Abstract
Purpose
This study evaluates the use of the needle arthroscopy in anatomical reconstruction of the lateral ankle. We hypothesized that the needle arthroscopy would allow anatomical reconstruction to be performed under arthroscopy.
Methods
Three patients underwent treatment of chronic ankle instability. The comparative procedure was performed in the following four steps: 1) anteromedial articular exploration (medial/lateral gutter/anterior chamber/syndesmosis); 2)creation of the talar tunnel via the anteromedial arthroscopic approach; 3) anterolateral fibular tunneling; and 4) positioning of the graft by the anteromedial arthroscopic approach.
For each of these steps, the planned procedure using the needle arthroscope was compared to the standard arthroscope. For each step, the planned procedure using the needle arthroscopy was compared to the standard arthroscope and the act was classified based on level of difficulty: facilitated, similar, complicated and impossible.
Results
The exploration of the medial and lateral gutter, the creation of the tunnel of the talus and graft positioning were not accomplished using the needle arthroscope. While the syndesmosis visualization was facilitated by the needle arthroscope in comparison to the standard arthroscope.
Conclusion
The anatomical reconstruction of the lateral ankle, using the needle arthroscopy-only approach, was impossible in all three cases, regarding: ankle joint exploration, creation of the tunnel of the talus and graft positioning. The needle arthroscope should not be considered as a "mini arthroscope" but as a new tool with which it is necessary to rethink procedures to take advantage of the benefits of this instrument.
Similar content being viewed by others
Case presentation
Three patients underwent surgery for the treatment of chronic lateral ankle instability.
The demographic data of the patients are presented in Table 1.
The procedure was performed according to a previously described technique [13] and based on previously cadaveric study [14] under general anesthesia. In the light of minimally invasive surgery, less tissue damage and consequently better recovery, the same anatomical reconstruction technique was tested with needle-arthroscopy. During this procedure, the standard arthroscope was sequentially replaced by the needle arthroscopy (NanoScopeTM, Arthrex, Naples, FL) (Fig. 1).
The needle arthroscopy is a video system consisting of a handpiece provided in a single-use kit (Fig. 2) connected to a 13-inch handheld console (Fig. 3).
The handpiece includes an LED light and video capture system. Inserted in a 2.2-mm trocar connected to an irrigation system, its tip has no obliquity and offers a 120° viewing angle. The needle arthroscope is 4.1 cm wide and 25.4 cm long, weighs 150 g and offers an image resolution of 400 × 400 pixels. The overall characteristics of the needle arthroscope are compared with those of the standard arthroscope used during the procedure in Table 2.
The comparative procedure was performed in the following four steps:
-
1)
anteromedial articular exploration (medial/lateral gutter/anterior chamber/syndesmosis) (supplementary video) [5, 11, 24];
-
2)
creation of the talar tunnel via the anteromedial arthroscopic approach;
-
3)
anterolateral fibular tunneling; and
-
4)
positioning of the graft by the anteromedial arthroscopic approach.
For each of these steps, the planned procedure using the needle arthroscope was compared to the standard arthroscope, and the act was classified based on level of difficulty: facilitated, similar, complicated and impossible. The 4 possible task difficulty levels were predefined by the senior author. This comparison is presented in Table 3.
The exploration of the anterior chamber is presented in the video (supplementary material).
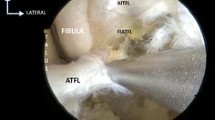
The view of the lateral talar gutter at different times during the procedure was compared with the 2 instruments (Figs. 4, 5, and 6).
The exploration of the medial and lateral gutter, the creation of the tunnel of the talus and graft positioning were not accomplished using the needle arthroscope. While the syndesmosis visualization was facilitated by the needle arthroscope in comparison to the standard arthroscope.
Discussion
The main finding of this study was that the needle arthroscopy-only approach did not allow the performance of the anatomical reconstruction of the lateral ankle in the three cases evaluated. This is the first is the first non-cadaveric study that compares step-by-step the surgery with the needle arthroscopy to standard ankle arthroscopy. In the present study, the authors evaluated only the feasibility and not other aspects of interest compared to a standard arthroscope. Overall, the perceived advantages of the needle arthroscope in this study were: ergonomics, smaller diameter, and optics flexibility, which could lead to less iatrogenic risk, and the limitations were: absence of obliquity and low resolution.
Despite the innovative evolutionary features of the needle arthroscopy in ankle surgery [3, 4, 4, 7, 15, 17], the poorer image resolution compared to a standard arthroscope, and most importantly, the absence of distal obliquity and the 120° field of view made the lateral ankle ligament complex anatomical reconstruction using the needle arthroscopy-only approach, impossible in all three cases. The needle arthroscopy has as its main purpose to be an alternative to MRI imaging and second-look arthroscopy. However, this less invasive advent still presents crucial limitations in ankle ligament reconstruction in its classic arthroscopic form which, in this study, could not be performed using exclusively the needle arthroscopy. Although the small diameter and flexibility of the new tool seemed to be particularly well suited to the ankle joint, the different views obtained with the needle arthroscope, under the usual technical conditions (patient position and identical approaches), did not allow the completion of the surgical procedure. Exploration of the medial and lateral gutters by the anteromedial portal was always complicated, if not impossible, with the needle arthroscope. On the other hand, the evaluation of syndesmosis was always easier. The anterior chamber was also easily visualized with both tools.
An anatomical study had previously shown the interest of a different obliquity (70° optics) to better visualize certain areas of the ankle, particularly the very anterior and posterior part of the articular surface of the distal tibia [22]. A recent cadaveric study [18] confirmed these data with an exploration allowing in all cases (n = 10) the visibility of all anatomical elements (deep fibers of the medial collateral ligament, anterior bundle of the lateral collateral ligament, medial, lateral and anterior gutter, the entire talus) by standard anteromedial or anterolateral approaches as described by previous authors [6, 10]. Additionally, Stornebrink et al. [18] reported that it was possible to see an average of 96% of the talus dome and 85% of the articular surface of the distal tibia. Accordingly, in the present study, the articular surfaces were largely visualized, and we were able to move from the anterior to the posterior joint chamber without any difficulty. This feature seems to us to be particularly interesting in the context of the endoscopic treatment of osteochondral lesions because of the technical difficulties known to be related to reduced accessibility. Needle arthroscopy is also an option as the initial step in the management of a suspected joint reported 11 cases of bacterial arthritis of native joints (ankle, wrist, shoulder and knee) and needle arthroscopic led to successful lavage in all cases, requiring no further surgical interventions [19].
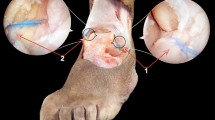
Iatrogenicity was also evaluated in a previous cadaveric study using the needle arthroscopy, and only in one case was an intermediate dorsal cutaneous branch of the superficial fibular nerve in contact with the anterolateral approach without macroscopic lesions [18]. The average distance between this nerve and this approach was 2.2 mm. The average distance between the anterolateral approach and the anterior vasculonervous pedicle was 8.8 mm [18]. The same authors performed the same cadaveric study evaluating fibular, posterior tibial, and calcaneal tendinoscopies and found similar results [20].
Although superficial nerve iatrogenic injury has a lower rate when the approach is limited to 2.2 mm, it cannot be eliminated because anatomical variability in the distal branches of the superficial fibular nerve is significant and unpredictable [8, 9, 21]. Contrary to what was reported by Stornebrink [18], it has been shown that transillumination does not reliably limit nerve damage in ankle arthroscopy [12]. To limit this superficial nerve damage, the position of the ankle in dorsiflexion seems to be important [6, 9], but ultrasound identification is reported to be the best solution [1, 2, 16]. No cartilage iatrogenic injury was reported in this same study [18], compared with the 31% found by Vega et al. [23]. The semirigid nature and the small diameter seemed to be major advantages in limiting cartilage damage.
Finally, another important factor for ankle arthroscopy is ergonomics. The needle arthroscope is four times lighter than a standard arthroscope (Table 2), making its management easier, however stabilization in the three spatial planes is much more difficult (Fig. 7). Additionally, a learning curve is necessary to master the gestures particular to this camera.
The limitations of this study are mainly the fact that a single surgeon performed the all the procedures, and the small number of cases.
In conclusion, despite the innovative evolutionary features of the needle arthroscopy in ankle surgery, the poorer image resolution compared to a standard arthroscope, and most importantly, the absence of distal obliquity and the 120° field of view made the anatomical reconstruction of the lateral ankle, using the needle arthroscopy-only approach, impossible in all three cases.
The needle arthroscope should not be considered as a "mini arthroscope" but as a new tool with which it will probably be necessary to rethink and describe truly new surgical procedures to take advantage of the benefits of this instrument.
References
Canella C, Demondion X, Guillin R, Boutry N, Peltier J, Cotten A (2009) Anatomic Study of the Superficial Peroneal Nerve Using Sonography. Am J Roentgenol 193:174–179. https://doi.org/10.2214/AJR.08.1898
Causeret A, Ract I, Jouan J, Dreano T, Ropars M, Guillin R (2018) A review of main anatomical and sonographic features of subcutaneous nerve injuries related to orthopedic surgery. Skeletal Radiol 47:1051–1068. https://doi.org/10.1007/s00256-018-2917-5
Colasanti CA, Kaplan DJ, Chen JS, Kanakamedala A, Dankert JF, Hurley ET, Mercer NP, Stone JW, Kennedy JG (2022) In-Office Needle Arthroscopy for Anterior Ankle Impingement. Arthrosc Tech 11:e327–e331. https://doi.org/10.1016/j.eats.2021.10.025
Colasanti CA, Mercer NP, Garcia JV, Kerkhoffs GMMJ, Kennedy JG (2022) In-Office Needle Arthroscopy for the Treatment of Anterior Ankle Impingement Yields High Patient Satisfaction With High Rates of Return to Work and Sport. Arthrosc J Arthrosc Relat Surg 38:1302–1311. https://doi.org/10.1016/j.arthro.2021.09.016
Cordier G, Lebecque J, Vega J, Dalmau-Pastor M (2020) Arthroscopic ankle lateral ligament repair with biological augmentation gives excellent results in case of chronic ankle instability. Knee Surg Sports Traumatol Arthrosc 28:108–115. https://doi.org/10.1007/s00167-019-05650-9
Dalmau-Pastor M, Malagelada F, Kerkhoffs GM, Karlsson J, Guelfi M, Vega J (2020) Redefining anterior ankle arthroscopic anatomy: medial and lateral ankle collateral ligaments are visible through dorsiflexion and non-distraction anterior ankle arthroscopy. Knee Surg Sports Traumatol Arthrosc 28:18–23. https://doi.org/10.1007/s00167-019-05603-2
Dankert JF, Mercer NP, Kaplan DJ, Kanakamedala AC, Chen JS, Colasanti CA, Hurley ET, Stone JW, Kennedy JG (2022) In-Office Needle Tendoscopy of the Tibialis Posterior Tendon with Concomitant Intervention. Arthrosc Tech 11:e339–e345. https://doi.org/10.1016/j.eats.2021.10.027
Darland AM, Kadakia AR, Zeller JL (2015) Branching Patterns of the Superficial Peroneal Nerve: Implications for Ankle Arthroscopy and for Anterolateral Surgical Approaches to the Ankle. J Foot Ankle Surg 54:332–337. https://doi.org/10.1053/j.jfas.2014.07.002
DeLee JC (1985) Complications of arthroscopy and arthroscopic surgery: results of a national survey. Committee on Complications of Arthroscopy Association of North America. Arthrosc J Arthrosc Relat Surg Off Publ Arthrosc Assoc N Am Int Arthrosc Assoc 1:214–220
Golanó P, Vega J, de Leeuw PAJ, Malagelada F, Manzanares MC, Götzens V, van Dijk CN (2010) Anatomy of the ankle ligaments: a pictorial essay. Knee Surg Sports Traumatol Arthrosc 18:557–569. https://doi.org/10.1007/s00167-010-1100-x
Guillo S, Cordier G, Sonnery-Cottet B, Bauer T (2014) Anatomical reconstruction of the anterior talofibular and calcaneofibular ligaments with an all-arthroscopic surgical technique. Orthop Traumatol Surg Res 100:S413–S417. https://doi.org/10.1016/j.otsr.2014.09.009
Harnroongroj T, Chuckpaiwong B (2017) Is the Arthroscopic Transillumination Test Effective in Localizing the Superficial Peroneal Nerve? Arthrosc J Arthrosc Relat Surg 33:647–650. https://doi.org/10.1016/j.arthro.2016.10.011
Lopes R, Decante C, Geffroy L, Brulefert K, Noailles T (2016) Arthroscopic anatomical reconstruction of the lateral ankle ligaments: A technical simplification. Orthop Traumatol Surg Res 102:S317–S322. https://doi.org/10.1016/j.otsr.2016.09.003
Lopes R, Noailles T, Brulefert K, Geffroy L, Decante C (2018) Anatomic validation of the lateral malleolus as a cutaneous marker for the distal insertion of the calcaneofibular ligament. Knee Surg Sports Traumatol Arthrosc 26:869–874. https://doi.org/10.1007/s00167-016-4250-7
Mercer NP, Gianakos AL, Kaplan DJ, Dankert JF, Kanakamedala A, Chen JS, Colasanti CA, Hurley ET, Stone JW, Kennedy JG (2022) Achilles Paratenon Needle Tendoscopy in the Office Setting. Arthrosc Tech 11:e315–e320. https://doi.org/10.1016/j.eats.2021.10.024
Poggio D, Claret G, López AM, Medrano C, Tornero E, Asunción J (2016) Correlation Between Visual Inspection and Ultrasonography to Identify the Distal Branches of the Superficial Peroneal Nerve: A Cadaveric Study. J Foot Ankle Surg 55:492–495. https://doi.org/10.1053/j.jfas.2016.01.014
Shimozono Y, Ito H, Ryoki H, Sakai S, Ishie S, Arai I, Kuroda Y, Matsuda S (2022) Needle-Arthroscopic Ankle Lateral Ligament Repair Using a Knotless Suture Anchor. Foot Ankle Orthop 7:2473011421S0045. https://doi.org/10.1177/2473011421S00450
Stornebrink T, Altink JN, Appelt D, Wijdicks CA, Stufkens SAS, Kerkhoffs GMMJ (2020) Two-millimetre diameter operative arthroscopy of the ankle is safe and effective. Knee Surg Sports Traumatol Arthrosc 28:3080–3086. https://doi.org/10.1007/s00167-020-05889-7
Stornebrink T, Janssen SJ, Kievit AJ, Mercer NP, JohnG K, Stufkens SAS, Kerkhoffs GMMJ (2021) Bacterial arthritis of native joints can be successfully managed with needle arthroscopy. J Exp Orthop 8:67. https://doi.org/10.1186/s40634-021-00384-5
Stornebrink T, Stufkens SAS, Appelt D, Wijdicks CA, Kerkhoffs GMMJ (2020) 2-Mm Diameter Operative Tendoscopy of the Tibialis Posterior, Peroneal, and Achilles Tendons: A Cadaveric Study. Foot Ankle Int 41:473–478. https://doi.org/10.1177/1071100719895504
Takao M, Uchio Y, Shu N, Ochi M (1998) Anatomic bases of ankle arthroscopy: study of superficial and deep peroneal nerves around anterolateral and anterocentral approach. Surg Radiol Anat 20:317–320. https://doi.org/10.1007/BF01630612
Tonogai I, Hayashi F, Tsuruo Y, Sairyo K (2018) Comparison of Ankle Joint Visualization Between the 70° and 30° Arthroscopes: A Cadaveric Study. Foot Ankle Spec 11:72–76. https://doi.org/10.1177/1938640017733099
Vega J, Golanó P, Peña F (2016) Iatrogenic articular cartilage injuries during ankle arthroscopy. Knee Surg Sports Traumatol Arthrosc 24:1304–1310. https://doi.org/10.1007/s00167-014-3237-5
Vega J, Karlsson J, Kerkhoffs GMMJ, Dalmau-Pastor M (2020) Ankle arthroscopy: the wave that’s coming. Knee Surg Sports Traumatol Arthrosc 28:5–7. https://doi.org/10.1007/s00167-019-05813-8
Acknowledgements
None
Funding
The present study has no funding sources.
Author information
Authors and Affiliations
Contributions
Author’s participation using the ICMJE criteria for authorship. RL and TN Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work. RL, GP, NB, and TDV Drafting the work or revising it critically for important intellectual content. RL, TN, GP, NB and TDV Final approval of the version to be published. RL, TN, GP, NB and TDV Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Institutional review board approval (IRB #blinded for review) was granted for the study and all patients provided informed consent in order to participate.
Competing interests
One or more of the authors has declared a potential conflict of interest. RL. is a consultant for and receives research support from Arthrex.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lopes, R., Noailles, T., Padiolleau, G. et al. Needle arthroscopy in anatomical reconstruction of the lateral ankle: a report of three cases with a parallel comparison to the standard arthroscopy procedure. J EXP ORTOP 9, 75 (2022). https://doi.org/10.1186/s40634-022-00510-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40634-022-00510-x