Abstract
Background
Interleukin-38 (IL-38), an inflammatory cytokine discovered in recent years, has been implicated in the pathogenesis of systemic lupus erythematosus (SLE). IL-38 is encoded by the IL1F10 (interleukin 1 family member 10) gene. Genetic variants of this gene have been associated with susceptibility to a number of autoimmune and inflammatory diseases, while their association with SLE risk has not been explored. In this case–control study, two novel variants of the 5 prime untranslated region (5′UTR) of the IL1F10 gene, rs3811050 C/T and rs3811051 T/G, were investigated in 120 women with SLE and 120 age-matched control women. The TaqMan allelic discrimination assay was used for genotyping of rs3811050 and rs3811051.
Results
The frequency of the rs3811050 CT genotype was significantly lower in SLE patients compared to controls (30.8 vs. 50.0%; odds ratio = 0.49; 95% confidence interval = 0.28–0.86; corrected probability = 0.045). The rs3811051 genotype frequencies did not show significant differences between patients and controls. Rs3811050 and rs3811051 showed weak linkage disequilibrium (LD) as indicated by the estimated LD coefficient and correlation coefficient values (0.32 and 0.05, respectively), and two-locus haplotype analysis revealed no significant differences between patients and controls. The frequencies of the rs3811050 T allele (38.8 vs. 20.6%; probability = 0.029) and the rs3811051 G allele (56.3 vs. 38.2%; probability = 0.038) were significantly higher in patients with mild/moderate disease activity than in patients with high disease activity, but significance was not maintained after applying Bonferroni correction (corrected probability = 0.058 and 0.076, respectively). Serum IL-38 concentrations (median and interquartile range) were significantly decreased in patients compared with controls (69.5 [64.1–74.8] vs. 73.5 [66.1–82.9] pg/mL; probability = 0.03), but were not influenced by SNP genotypes.
Conclusions
The heterozygous genotype of rs3811050, a 5'UTR variant, of the IL-38 encoding gene, IL1F10, is associated with a reduced risk of SLE among women. Furthermore, the rs3811050 T and rs3811051 G alleles may influence disease activity. In addition, serum IL-38 concentrations were down-regulated in SLE patients but were not affected by the rs3811050 and rs3811051 genotypes.
Similar content being viewed by others
Background
Systemic lupus erythematosus (SLE) is an inflammatory autoimmune disease, with an estimated global incidence of 5.14 per 100,000 population per year. The incidence varies widely between women and men (8.82 versus 1.53 per 100,000 population per year) and across ethnic and geographic regions [1]. SLE is a complex and heterogeneous disease in terms of etiology and clinical manifestations. Although the exact etiopathogenesis of SLE is not well understood and defined, several factors have been described to participate in the initiation and progression of the disease, including genetic, epigenetic, hormonal, infectious, lifestyle, and environmental factors [2]. Theoretical evidence suggests that the interaction of these factors can lead to immune dysregulation, actively contributing to preclinical autoimmunity and accelerating the clinical manifestations of SLE. In fact, it has been increasingly recognized that the onset of SLE is associated with dysregulated function of cells involved in innate and adaptive immunity, including dendritic cells, neutrophils, T helper cells, and B cells [3]. Ultimately, autoreactive B cells are activated by CD4 + T cells to produce pathogenic autoantibodies, particularly anti-double stranded DNA (anti-dsDNA) antibodies, which are serum markers that are indispensable for the diagnosis of SLE [4]. The crosstalk between these cells is mediated by cytokines, a network of soluble low-molecular-weight glycoproteins that act by binding to their receptors on target cells and activating a downstream signaling cascade that ends in the expression of a set of genes required to perform certain functions [5]. There is increasing evidence suggesting a critical role for various cytokines in the pathogenesis of SLE during disease onset and progression through pro-inflammatory and anti-inflammatory functions [6]. In addition, cytokines have also been shown to contribute to extra-articular manifestations of SLE, including nephritis and arthritis, along with their association with disease severity [7].
Cytokines are classified into families, and one proposed to have a role in the pathophysiology of SLE is the interleukin (IL)-1 family of cytokines. Cytokines belonging to the IL-1 family consist of two members with anti-inflammatory action (IL-37 and IL-38) and seven members with pro-inflammatory activity (IL-1α, IL-1β, IL-18, IL-33, IL-36α, IL-36β, and IL-36γ) [8]. IL-38, known as IL-1F10 or IL-1HY2 at the time of its discovery, is a 17 kDa cytokine that has been assigned to the IL-1 family in recent years and is mostly known for its anti-inflammatory properties [9]. Numerous immune cells have been shown to express IL-38, including monocytes, macrophages, fibroblast-like synoviocytes, keratinocytes and B cells, as well as some organs and tissues such as the spleen, thymus, tonsils, and skin [10]. Dysregulated production of IL-38 has been associated with the pathogenesis of autoimmune and inflammatory diseases, such as rheumatoid arthritis, psoriasis, inflammatory bowel disease, and SLE [11].
IL-38 is encoded by IL1F10 (interleukin 1 family member 10), a gene located in the long arm of human chromosome 2 at position 2q14.1. The gene consists of five exons and six introns to which more than 40 naturally occurring single nucleotide polymorphisms (SNPs) have been assigned with a minor allele frequency (MAF) ≥ 10% (https://www.ncbi.nlm.nih.gov/gene/84639; https://www.ensembl.org). Recent studies have revealed that polymorphisms in the IL1F10 gene are associated with susceptibility to a number of autoimmune and inflammatory diseases, including rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, and juvenile systemic arthritis [12, 13]. In SLE, genetic polymorphisms of the IL1F10 gene have not been explored.
In the current study, two novel 5 prime untranslated region (5'UTR) variants of the IL1F10 gene, rs3811050 C/T and rs3811051 T/G, were examined in Iraqi women with SLE with the aim of assessing their role in susceptibility to disease. In addition, serum IL-38 concentrations were determined and the effect of IL1F10 SNP genotypes on systemic levels of IL-38 was evaluated.
Materials and methods
Patients and controls
A case–control study was conducted on 240 women (120 women diagnosed with SLE and 120 healthy control women [HCW]) to evaluate the association of two novel IL1F10 gene variants with susceptibility to SLE. Patients (mean age = 34.0; standard deviation [SD] = 10.2; range = 17.0–57.0 years) and HCW (mean age = 35.9; SD = 9.6; range = 22.0–68.0 years) were matched for age (p = 0.157). SLE diagnosis was made at the Rheumatology Unit and Nephrology and Renal Transplantation Centre (Baghdad Medical City Complex) during January-November 2022 following the American College of Rheumatology (ACR) revised criteria for SLE [14]. The included patients were females who were at least 17 years old and followed the diagnostic criteria (inclusion criteria). Patients with other diseases, such as diabetes, cardiovascular disease and cancer, were excluded. The SLE Disease Activity Index (SLEDAI) was used to assess disease activity. The SLEDAI score ranges from 0 (no activity) to 20 (very high activity) [15]. In the current study, the SLEDAI was simplified into two categories, mild/moderate (score ≤ 10) and high activity (score > 10). All patients were on treatment with prednisolone (10 mg/day) plus mycophenolate mofetil (2 mg/day) or tacrolimus (1 mg/day).
Selection and detection of IL1F10 variants
We were interested in variants located in the 5'UTR of the IL1F10 gene (Gene ID: 84639) that had a MAF ≥ 10% (selection criteria). The complete sequence of the IL1F10 gene with variant data was downloaded (https://www.ensembl.org). Two 5'UTR variants were consistent with our selection criteria; rs3811050 C/T (MAF = 23%) and rs3811051 T/G (MAF = 36%). The gen map of the two SNPs is shown in Supplementary Fig. 1.
The EasyPure Blood gDNA kit was used to isolate genomic DNA following the protocol provided by the manufacturer (Transgen Biotech, China). The real-time polymerase chain reaction (RT-PCR)-based TaqMan allelic discrimination assay was adopted for genotyping rs3811050 and rs3811051 using primers and allele-specific fluorescent probes designed with Primer3Plus software (https://www.bioinformatics.nl/cgi-bin/primer3plus/primer3plus.cgi). The efficiency and specificity of primers and probes were tested using online in-silico PCR analysis (https://genome.ucsc.edu/cgi-bin/hgPcr). Primers and probes were synthesized by Alpha DNA (Canada) and are detailed in Table 1.The RT-PCR mix consisted of 6 µL PerfectStart II Probe qPCR SuperMix UDG (TransgenBiotech, China), 1 µL forward primer, 1 µL reverse primer, 0.8 µL probe 1, 0.8 µL probe 2, 4 µL DNA and 6.4 µL nuclease-free water (total volume: 20 µL). Table 1 illustrates the optimized conditions and protocol for RT-PCR amplification, which was performed using the MxPro 3005P qPCR system and the built-in MxPro software was used to interpret the collected data (Stratagene, USA).
IL-38 immunoassay
Serum IL-38 concentrations were measured using an enzyme-linked immunosorbent assay kit and the manufacturer's protocol was followed (MyBioSource, USA). The standard curve range for the kit was 0–1000 pg/mL.
Statistical analysis
Alleles and genotypes were expressed as number and frequency (percentage). SHEsis software was used to test genotype frequencies for Hardy–Weinberg equilibrium (HWE). It was also used to construct two-locus haplotypes and to determine linkage disequilibrium (LD), LD coefficient (D') and correlation coefficient (R2) [16]. Odds ratio (OR) and 95% confidence interval (CI) were used to evaluate the association of alleles and genotypes with susceptibility to SLE. Logistic regression analysis was used to calculate the OR and 95% CI using five genetic models (allele, co-dominant, dominant, recessive, and over-dominant). Serum IL-38 concentrations were expressed as median and interquartile range (IQR: 25–75%) and significance was assessed using the Mann–Whitney U test. Statistical significance was set at probability (p) < 0.05, and the p-value was corrected (pc) for multiple comparisons using the Bonferroni correction method [17]. IBM SPSS Statistics 25.0 (Armonk, NY: IBM Corp.) was used accomplish statistical analyses. G*power software (version 3.1.9.7) was used to calculate the power of the sample size [18].
Results
Power of sample size
Sample size power was analyzed using G*power software with the following inputs: 0.05 two-tailed α error p, 0.49 OR (determined in the current study), 120 SLE patients, and 120 HCW. The calculated sample size power (1-β error p) was 0.78, which is slightly lower than the ideal power of 0.8 [19].
HWE analysis of IL1F10 variants
The rs3811050 and rs3811051 genotype frequencies were consistent with HWE in the HCW group as there were no statistically significant differences between the observed and expected frequencies (p = 0.402 and 0.903, respectively). Regarding SLE patients, the rs3811051 genotype frequencies were also consistent with HWE as there were no significant differences between observed and expected frequencies (p = 0.112), while rs3811050 genotype frequencies significantly deviated from HWE (p = 0.001) (Table 2).
IL1F10 rs3811050 variant
Three genotypes of rs3811050 (CC, CT, and TT) were identified with frequencies of 48.3, 30.8 and 20.8%, respectively in SLE patients and 38.3, 50.0 and 11.7%, respectively in HCW. Logistic regression analysis for rs3811050 was conducted under five genetic models (allele, co-dominant, dominant, recessive, and over-dominant). Statistically significant differences were observed only under analysis of the co-dominant (CT vs. CC) and over-dominant (CT vs. CC + TT) models (pc = 0.045 and 0.01, respectively). In both models, a significant reduction in the frequency of the CT genotype was observed in SLE patients compared with HCW (30.8 vs. 50.0%). The calculated OR (95% CI) for the CT genotype under the co-dominant and over-dominant models was 0.49 (0.28–0.86) and 0.45 (0.26–0.75), respectively (Table 3).
IL1F10 rs3811051 variant
Three genotypes of rs3811051 (TT, TG, and GG) were identified with frequencies of 25.0, 42.5 and 32.5%, respectively, in SLE patients and 21.7, 49.2 and 29.2%, respectively in HCW. This variant appears not to be associated with SLE risk as logistic regression analysis demonstrated no significant association under any of the five genetic models (Table 4).
Haplotype analysis of IL1F10 rs3811050 and rs3811051variants
The SHEsis online software platform (http://analysis.bio-x.cn/myanalysis.php) was used to determine LD and generate two-locus haplotype for IL1F10 variants (in the order rs3811050 and rs3811051). Rs3811050 and rs3811051 showed weak LD as indicated by the estimated D' and R2 values (0.32 and 0.05, respectively) (Fig. 1). Four haplotypes (C-T, C-G, T-T, and T-G) were established but their frequencies did not show significant differences between SLE patients and HCW (p = 0.565, 0.48, 0.39 and 0.46, respectively) (Table 5).
Two-locus linkage disequilibrium (LD) plot for the Interleukin 1 family member 10 (IL1F10) gene variants rs3811050 T/C and rs3811051 G/T showing the LD coefficient (D'; 0.32; left) and correlation coefficient (R2; 0.05; right). Plots were generated using SHEsis software (http://analysis.bio-x.cn/myanalysis.php)
Association of IL1F10 variants with disease activity
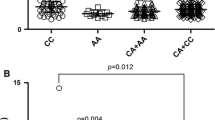
To examine whether rs3811050 and rs3811051 are associated with SLE activity as determined by SLEDAI, allele and genotype frequencies of both variants were compared between patients with mild/moderate disease activity (n = 103) and patients with high disease activity (n = 17). The frequencies of the rs3811050 T allele (38.8 vs. 20.6%; p = 0.029) and the rs3811051 G allele (56.3 vs. 38.2%; p = 0.038) were significantly higher in patients with mild/moderate disease activity than in patients with high disease activity, but significance was not maintained after applying Bonferroni correction (pc = 0.058 and 0.076, respectively). The frequencies of the rs3811050 and rs3811051 genotypes did not show significant differences between the two groups of patients, although there was a tendency for the rs3811050 TT genotype (22.3 vs. 11.8%; p = 0.179) and the rs3811051 GG genotype (35.0 vs. 17.6%; p = 0.194) to show an increased frequency in patients with mild/moderate disease activity compared to patients with high disease activity (Table 6).
IL-38 concentrations
Serum IL-38 concentrations were significantly lower in SLE patients than in HCW (69.5 [IQR: 64.1–74.8] vs. 73.5 [IQR: 66.1–82.9] pg/mL; p = 0.03) (Additional file 1: Supplementary Figure II). When IL-38 concentrations were stratified by rs3811050 and rs3811051 genotypes, there were no significant differences and concentrations were nearly similar in the three genotypes of each SNP (Additional file 1: Supplementary Figure III).
Discussion
In the current study, the association of two novel variants located in the 5'UTR of the IL1F10 gene, rs3811050 C/T and rs3811051 T/G, with susceptibility to SLE was analyzed. It was found that the frequency of the CT genotype of rs3811050 was significantly lower in SLE patients compared to HCW and was associated with a lower risk of developing SLE under co-dominant and over-dominant genetic models. It should be noted that genotype frequencies of rs3811050 deviated significantly from HWE in SLE patients, and the observed low level of heterozygosity could have contributed to this deviation. The observed frequency of the rs3811050 TC genotype was 30.8% in SLE patients, while the expected frequency was significantly higher and was 45.8%. Deviation from HWE can be attributed to several factors, such as genotyping errors, small sample size, disease association and others [20]. Genotyping errors could be excluded because we adopted a highly sensitive method in genotyping rs3811050 and all genotyping steps were well verified. Regarding sample size, we agree that the current number of SLE patients (n = 120) may be relatively small and could have contributed to departure from HWE. However, disease association may be considered an important factor in the deviation of HWE because although the included patients were selected at random, the disease itself may represent selection bias and thus affected individuals are overrepresented in the ascertained sample. As a result, when a genetic variant is associated with the risk of a disease, the type I error rate of the HWE test can be inflated [21].
Although SLE is a multifactorial disease, the genetic contribution to its etiology is high with heritability up to 66% as revealed by twin studies. Genome-wide association studies have confirmed the role of genetic predisposition in the development of SLE and approximately hundred susceptibility SNPs have been identified. Many of these SNPs are localized in non-coding regions of the human genome and are proposed as potential disease-causing variants [22, 23]. Rs3811050 is a genetic variant located in a non-coding sequence, 5′UTR, of the IL1F10 gene, and the present study reported for the first time an association of the rs3811050 CT genotype with a reduced risk of SLE among women. The 5′UTR is an RNA sequence located immediately upstream of the encoded RNA and contains the translation initiation codon. It may also include several regulatory elements, such as CpG methylation sites, upstream open reading frames (ORFs), internal ribosome entry sites, and RNA binding protein sites [24]. Alterations in these regulatory elements may modify the molecular pathways of gene expression and thus cellular processes, which may lead to a disease phenotype. Therefore, 5′UTR genetic variants, due to nucleotide substitution, may modify these regulatory pathways and can impact overall protein production by influencing several molecular aspects of RNA, such as transcription, translation, and stability [25].
Recent evidence suggests that the 5'UTR variant rs3811050 (-143C > T) may affect IL1F10 gene expression in cardiovascular disorders due to allelic replacement of C with T, where T is predicted to create an elongated coding sequence (603 nucleotides) while the canonical coding sequence is shorter (459 nucleotides). This allelic alternation may ultimately contribute to disease susceptibility [26]. In the current study, the rs3811050 T allele showed a decreased frequency in SLE patients with high disease activity compared to patients with mild/moderate disease activity. A similar observation was also made for the G allele of rs3811051, which was in weak LD with rs3811050 (D' = 0.32). Although the pc-value was not significant, which could be attributed to the low sample size of patients with high disease activity SLE (n = 17), these results suggest an association between both alleles (rs3811050 T and rs3811051 G) and a reduced risk of developing active disease. In the heterozygous state, the rs3811050 T allele may also contribute to reduced susceptibility to SLE.
Since 5'UTR variants can affect RNA transcription and translation processes, gene expression and corresponding protein synthesis may also be dysregulated [25]. Therefore, we measured serum IL-38 concentrations in SLE patients and HCW, and the effect of IL1F10 SNP genotypes was evaluated. Serum IL-38 concentrations were significantly decreased in SLE patients compared to HCW. These results are not consistent with previous studies, which reported elevated levels of IL-38 in the serum of patients [27, 28]. However, consistent with our findings, Takeuchi and colleagues studied 19 SLE patients with early-onset disease and found that 18 patients showed undetectable concentrations of IL-38 and only one patient showed elevated levels of IL-38. Interestingly, the concentration of IL-38 in this patient gradually decreased with treatment [29]. In our study, all SLE patients were on treatment and this may explain the low IL-38 concentrations. It has also been reported that serum IL-38 levels are affected by genetic variants in the promoter of the IL1F10 gene [30]. In the present study, this observation was not confirmed, and the genotypes of both SNPs in the 5'UTR of the IL1F10 gene, rs3811050 and rs3811051, showed no significant effects on serum IL-38 concentration. Regardless of these conflicting results, IL-38 appears to play an essential role in the pathogenesis of SLE and its prognostic significance in SLE cannot be ruled out, and further studies are needed to explore and understand the underlying molecular mechanisms.
An important limitation of the current study is the lack of IL1F10 gene expression analysis in SLE patients. In addition, the relatively small sample size of SLE patients, especially those with high disease activity, is another limitation, and the need for replication in larger cohorts is certainly justified. Furthermore, confounding factors that may influence results should be addressed and taken into account when analyzing IL1F10 genetic variants such as extra-articular manifestations of SLE. In addition, newly diagnosed SLE cases should be included.
Conclusions
The study results indicated that the heterozygous genotype of rs3811050, a 5'UTR variant, of the IL-38 encoding gene, IL1F10, is associated with a reduced risk of SLE among women. Furthermore, the rs3811050 T and rs3811051 G alleles may influence disease activity. In addition, serum IL-38 concentrations were down-regulated in SLE patients but were not affected by the rs3811050 and rs3811051 genotypes.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- 5'UTR:
-
5 Prime untranslated region
- CI:
-
Confidence interval
- D':
-
LD coefficient
- dsDNA:
-
Double stranded DNA
- HCW:
-
Healthy control women
- HWE:
-
Hardy–Weinberg equilibrium
- IL:
-
Interleukin
- IL1F10 :
-
Interleukin 1 family member 10
- LD:
-
Linkage disequilibrium
- MAF:
-
Minor allele frequency
- OR:
-
Odds ratio
- p :
-
Probability
- pc :
-
Bonferroni-corrected p
- R2 :
-
Correlation coefficient
- SD:
-
Standard deviation
- SLE:
-
Systemic lupus erythematosus
- SLEDAI:
-
SLE disease activity index
- SNP:
-
Single nucleotide polymorphism
References
Tian J, Zhang D, Yao X, Huang Y, Lu Q (2023) Global epidemiology of systemic lupus erythematosus: a comprehensive systematic analysis and modelling study. Ann Rheum Dis 82:351–356. https://doi.org/10.1136/ard-2022-223035
Akhil A, Bansal R, Anupam K, Tandon A, Bhatnagar A (2023) Systemic lupus erythematosus: latest insight into etiopathogenesis. Rheumatol Int 43:1381–1393. https://doi.org/10.1007/s00296-023-05346-x
Pan L, Lu MP, Wang JH, Xu M, Yang SR (2020) Immunological pathogenesis and treatment of systemic lupus erythematosus. World J Pediatr 16:19–30. https://doi.org/10.1007/s12519-019-00229-3
Choi MY, Costenbader KH (2022) Understanding the concept of pre-clinical autoimmunity: prediction and prevention of systemic lupus erythematosus: identifying risk factors and developing strategies against disease development. Front Immunol 13:890522. https://doi.org/10.3389/fimmu.2022.890522
Altan-Bonnet G, Mukherjee R (2019) Cytokine-mediated communication: a quantitative appraisal of immune complexity. Nat Rev Immunol 19:205–217. https://doi.org/10.1038/s41577-019-0131-x
Idborg H, Oke V (2021) Cytokines as biomarkers in systemic lupus erythematosus: Value for diagnosis and drug therapy. Int J Mol Sci 22:11327. https://doi.org/10.3390/ijms222111327
Richter P, Macovei LA, Mihai IR, Cardoneanu A, Burlui MA, Rezus E (2023) Cytokines in systemic lupus erythematosus—focus on TNF-α and IL-17. Int J Mol Sci 24:14413. https://doi.org/10.3390/ijms241914413
Wu YR, Hsing CH, Chiu CJ, Huang HY, Hsu YH. 2022 Roles of IL-1 and IL-10 family cytokines in the progression of systemic lupus erythematosus: Friends or foes? IUBMB Life, John Wiley & Sons, Ltd, p. 143–56. https://doi.org/10.1002/iub.2568.
van de Veerdonk FL, de Graaf DM, Joosten LAB, Dinarello CA (2018) Biology of IL-38 and its role in disease. Immunol Rev 281:191–196. https://doi.org/10.1111/IMR.12612
Xie L, Huang Z, Li H, Liu X, Zheng S, Su W (2019) IL-38: A new player in inflammatory autoimmune disorders. Biomolecules 9:345. https://doi.org/10.3390/biom9080345
Song XH, Liu Y, Fu Y, Li M, Qing WuY (2021) Biology of interleukin-38 and its role in chronic inflammatory diseases. Int Immunopharmacol 95:107528. https://doi.org/10.1016/j.intimp.2021.107528
Garraud T, Harel M, Boutet MA, Le Goff B, Blanchard F (2018) The enigmatic role of IL-38 in inflammatory diseases. Cytokine Growth Factor Rev 39:26–35. https://doi.org/10.1016/j.cytogfr.2018.01.001
Xu WD, Huang AF (2018) Role of interleukin-38 in chronic inflammatory diseases: A comprehensive review. Front Immunol 9:375574. https://doi.org/10.3389/fimmu.2018.01462
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40:1725. https://doi.org/10.1002/art.1780400928
Griffiths B, Mosca M, Gordon C (2005) Assessment of patients with systemic lupus erythematosus and the use of lupus disease activity indices. Best Pract Res Clin Rheumatol 19:685–708. https://doi.org/10.1016/j.berh.2005.03.010
Shi YY, He L (2005) SHEsis, a powerful software platform for analyses of linkage disequilibrium, haplotype construction, and genetic association at polymorphism loci. Cell Res 15:97–98. https://doi.org/10.1038/sj.cr.7290272
Shi Q, Pavey ES, Carter RE (2012) Bonferroni-based correction factor for multiple, correlated endpoints. Pharm Stat 11:300–309. https://doi.org/10.1002/pst.1514
Kang H (2021) Sample size determination and power analysis using the G*Power software. J Educ Eval Health Prof 18:17. https://doi.org/10.3352/JEEHP.2021.18.17
Serdar CC, Cihan M, Yücel D, Serdar MA (2021) Sample size, power and effect size revisited: Simplified and practical approachin pre-clinical clinical and laboratory studies. Biochem Medica 31:1–27. https://doi.org/10.11613/BM.2021.010502
Sha Q, Zhang S (2011) A test of Hardy-Weinberg equilibrium in structured populations. Genet Epidemiol 35:671–678. https://doi.org/10.1002/gepi.20617
Li M, Li C (2008) Assessing departure from Hardy-Weinberg equilibrium in the presence of disease association. Genet Epidemiol 32:589–599. https://doi.org/10.1002/gepi.20335
Elghzaly AA, Sun C, Looger LL, Hirose M, Salama M, Khalil NM et al (2022) Genome-wide association study for systemic lupus erythematosus in an egyptian population. Front Genet 13:948505. https://doi.org/10.3389/fgene.2022.948505
Kwon YC, Chun S, Kim K, Mak A (2019) Update on the genetics of systemic lupus erythematosus: Genome-wide association studies and beyond. Cells 8:1180. https://doi.org/10.3390/cells8101180
Pichon XA, Wilson L, Stoneley M, Bastide AA, King H, Somers J, Willis A (2012) RNA binding protein/RNA element interactions and the control of translation. Curr Protein Pept Sci 13:294–304. https://doi.org/10.2174/138920312801619475
Steri M, Idda ML, Whalen MB, Orrù V (2018) Genetic variants in mRNA untranslated regions. Wiley Interdiscip Rev RNA 9:e1474. https://doi.org/10.1002/wrna.1474
Soukarieh O, Meguerditchian C, Proust C, Aïssi D, Eyries M, Goyenvalle A et al (2022) Common and rare 5′UTR variants altering upstream open reading frames in cardiovascular genomics. Front Cardiovasc Med 9:841032. https://doi.org/10.3389/fcvm.2022.841032
Xu WD, Su LC, Liu XY, Wang JM, Yuan ZC, Qin Z et al (2020) IL-38: a novel cytokine in systemic lupus erythematosus pathogenesis. J Cell Mol Med 24:12379–12389. https://doi.org/10.1111/jcmm.15737
Zhang J, Tabush N, Wei C, Luo L (2023) Regulatory effect of IL-38 on NF-κB pathway in systemic lupus erythematosus. Immunobiology 228:152322. https://doi.org/10.1016/j.imbio.2022.152322
Takeuchi Y, Seki T, Kobayashi N, Sano K, Shigemura T, Shimojo H et al (2018) Analysis of serum IL-38 in juvenile-onset systemic lupus erythematosus. Mod Rheumatol 28:1069–1072. https://doi.org/10.1080/14397595.2018.1436118
Al-Karaawi IA, Al-bassam WW, Ismaeel HM, Ad’hiah AH (2022) Interleukin-38 promoter variants and risk of COVID-19 among Iraqis. Immunobiology 227:152301. https://doi.org/10.1016/j.imbio.2022.152301
Acknowledgements
Firstly, we would like to express our sincere thanks and appreciation to the medical staff at the Rheumatology Unit and Center for Kidney Disease and Transplantation (Medical City Complex in Baghdad) for the kind cooperation. Second, we express our thanks to Dr. Ziarih Hawi (Monash University, Australia) for his help in designing the primers. Third, we owe SLE patients a debt of thanks for their understanding in conducting this study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
RAN and AAA contributed to laboratory work, data handling, writing and revising the manuscript. AHA managed data, carried out statistical analyses and wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval was obtained from the Ethics Committee of the Department of Biotechnology, College of Science, University of Baghdad (Reference Number: CSEC/1121/0078 dated 20 November 2021) and the Baghdad Medical City Complex (Reference Number: 2084 dated 16 January 2022). All participants provided written consent.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1:
Supplementary Figures.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nijeeb, R.A., Aljber, A.A. & Ad’hiah, A.H. Low heterozygosity for rs3811050, a 5 prime untranslated region variant of the gene encoding interleukin-38 (IL1F10), is associated with a reduced risk of systemic lupus erythematosus. Egypt J Med Hum Genet 25, 36 (2024). https://doi.org/10.1186/s43042-024-00503-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43042-024-00503-8