Abstract
Aim
The aim of this study was to estimate the prevalence, possible risk factors, patterns of resistance, and fate of multidrug-resistant pulmonary tuberculosis (MDR-TB) in Alexandria governorate as a representative part of Egypt during the period between July 2008 and December 2012.
Patients and methods
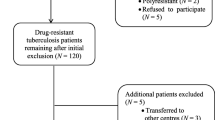
This retrospective study included all patients with pulmonary TB that was recorded in Alexandria governorate during the period between July 2008 (the time that MDR ward was held in Alexandria) and December 2012. They were divided into two groups: group I included patients with pulmonary TB that was recorded in Alexandria governorate (1893 cases), and group II included patients with pulmonary TB who were admitted in El-Maamoura Chest Hospital (509 cases). They were subdivided into two subgroups: group IIa included patients with MDR pulmonary TB (82 cases), and group IIb included patients with pulmonary TB not categorized as MDR-TB (427 cases).
Results
All patients with MDR-TB had acquired resistance. MDR-TB was more common in the male population, diabetic patients, and those with chronic chest disease. The effect of treatment of MDR-TB cases was as follows: cured patients, 49 (59.8%); patients under treatment, 10 (12.2%); treatment failure, four cases (4.9%); deceased patients, 10 (12.2%); and defaulters, nine (10.9%). The overall total prevalence rate of MDR-TB in Alexandria governorate from 2008 to 2012 was 4.3%.
Conclusion
There was a decreasing trend of MDR-TB cases. History of anti-TB treatment is the strongest independent predictor of MDR-TB. The highest figures of resistance in the MDR group besides isoniazide and rifampicin were for streptomycin, whereas the lowest resistance was for ethambutol.
Article PDF
Similar content being viewed by others
References
Ormerod LP. Multidrug-resistant tuberculosis (MDR-TB): epidemiology, prevention, and treatment. Br Med Bull 2009; 73–74:17–24.
WHO. Multidrug and extensively drug-resistant TB (M/XDR-TB): 2010 global report on surveillance and response (2010).
Zignol M, Hosseini S, Wright A, van Weezenbeek CL, Nunn P, Watt CJ, et al. Global incidence of multi-drug resistant tuberculosis. J Infect Dis 2006; 194:479–485.
CDC. Emergence of Mycobacterium tuberculosis with extensive resistance to second-line drugs worldwide, 2000–2004. MMWR 2006; 55:301–305.
Sayed H. Interferon gamma release assay (IGRA) in diagnosis of pulmonary tuberculosis [MSc thesis in Chest diseases]. Egypt: Alexandria University, 2013.
Abdel Fatah M. Outcome of multi-drug resistant tuberculosis treatment in patients admitted to Abassia Chest Hospital between July 2006 to June 2008 [MSc Thesis in Chest Diseases]. Egypt: Ain Shams University, 2009.
Abdel-Azim A. Identification of gene mutation in Mycobacterium tuberculosis isolated from patients unreasoned to rifampicin and isoniazid treatment [MSc Thesis in Chest Diseases]. Egypt: Ain Shams University, 2003.
Bellamy R. Identifying susceptibility factors for tuberculosis in Africans: a candidate gene study and genome wide screen. Clin Sci (Lond) 2000; 98:245–250.
Safwat TM, Elmasry AA, Abdel Kader M. Prevalence of multi drug resistance tuberculosis in Abassia Chest Hospital from July 2006 to December 2009. Egypt J Bronchol 2011; 5:124–130.
Hamdy ABE, Wagdan AA. Role of patient compliance during the treatment of tuberculosis. Med J Cairo University 1991; 59:721.
Kamal M. Multiple drug resistant tuberculosis in Abassia Chest Hospital from January 2005 to December 2006 [MSc Thesis in Chest Diseases]. Egypt: Ain Shams University, 2006.
Fawzy M. Resistance to INH and rifampicin in pulmonary tuberculous patients [MSc Thesis in Chest Diseases]. Egypt: Ain Shams University, 2005.
WHO. Global tuberculosis report, The burden of disease caused by TB. Geneva, Switzerland: WHO; 2012.
Nada M. Outcome of multi-drug resistant antituberculous treatment in Abassia Chest Hospital between July 2006 to June 2008 [MSc Thesis in Chest Diseases]. Egypt: Ain Shams University, 2009.
Author information
Authors and Affiliations
Corresponding author
Additional information
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Rights and permissions
This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mohammad, O.I., Okab, A.A. & Zaki, M.E. Situation of multidrug-resistant pulmonary tuberculosis in Alexandria governorate from July 2008 to December 2012. Egypt J Bronchol 10, 64–68 (2016). https://doi.org/10.4103/1687-8426.176792
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.4103/1687-8426.176792