Abstract
Purpose
Staple line leak following sleeve gastrectomy is a significant problem and has been hypothesised to be related to hyperpressurisation in the proximal stomach. There is, however, little objective evidence demonstrating how these forces could be transmitted to the luminal wall. We aimed to define conditions in the proximal stomach and simulate the transmission of stress forces in the post-operative stomach using a finite element analysis (FEA).
Materials and Methods
The manometry of fourteen patients post sleeve gastrectomy was compared to ten controls. Manometry, boundary conditions, and volumetric CT were integrated to develop six models. These models delineated luminal wall stress in the proximal stomach. Key features were then varied to establish the influence of each factor.
Results
The sleeve gastrectomy cohort had a significantly higher peak intragastric isobaric pressures 31.58 ± 2.1 vs. 13.49 ± 1.3 mmHg (p = 0.0002). Regions of stress were clustered at the staple line near the GOJ, and peak stress was observed there in 67% of models. A uniform greater curvature did not fail or concentrate stress under maximal pressurisation. Geometric variation demonstrated that a larger triangulated apex increased stress by 17% (255 kPa versus 218 kPa), with a 37% increase at the GOJ (203kPA versus 148kPA). A wider incisura reduced stress at the GOJ by 9.9% (128 kPa versus 142 kPa).
Conclusion
High pressure events can occur in the proximal stomach after sleeve gastrectomy. Simulations suggest that these events preferentially concentrate stress forces near the GOJ. This study simulates how high-pressure events could translate stress to the luminal wall and precipitate leak.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Staple line leak is a morbid complication after sleeve gastrectomy and frequently results in a protracted recovery, significant morbidity, and occasionally mortality [1, 2]. Leaks almost always occur in the proximal staple line within 1–2 cm of the gastro-oesophageal junction [3, 4]; however, the precise pathophysiology is not well delineated [5]. An understanding of the precipitating factors driving leak could provide technical insights into sleeve construction that could reduce the incidence of chronic leak and aid decision making during their management.
Various mechanisms have been proposed to be the driver of leak; however, no single factor has been determined to be the sole contributory factor. Ischaemia and hyperpressurisation of the proximal stomach have been proposed to be the two main causative factors for leak. In-flow hypoperfusion, and a paucity of vasculature in the proximal staple line, has been suggested to drive ischaemia in the post-operative period [6]. Other theories, including thermal injury to the gastric wall or compromise to vascular supply during dissection, have been postulated.
Evidences of high-pressure events in the stomach after sleeve gastrectomy have led to the hypothesis that they play a role in the initiation and perpetuation of sleeve leak [7,8,9]. There have been multiple studies investigating staple line burst pressures and buttressing methods in an effort to reduce the incidence of leak [10]; however, the transmission of stress forces to the luminal wall has not been examined at length.
We utilised the finite element method (FEM) in order to predict the behaviour of the post-operative stomach under specific biological conditions. FEM is a commonly used mathematical method to solve complex mechanical and biological problems using sophisticated computing [11, 12]. A larger structure is reduced into individual finite elements and their behaviour under specific conditions is solved during repeated simulation. Accurate simulation of events requires a precise understanding of anatomy, pressure events, and tissue strength.
Our hypothesis is that using finite element analysis (FEA), we can develop a model of the post-operative stomach and using specific boundary conditions, we will be able to simulate the transmission of stress forces to the luminal wall. This will give us insights into the influence of the geometry of the sleeve on stress forces.
Methods
Patient Selection
There were two components to this study. In part 1, we established boundary conditions to accurately inform our intended finite element analysis. This involved compiling intraluminal pressure and anatomical data. In part 2, we conducted finite element analysis under different conditions with boundary conditions informed with data from part 1.
Part 1: Boundary Conditions
We utilised data from a prospective clinical trial from within our unit [13]. This involved patients who had undergone a sleeve gastrectomy from between 2014 and 2019. Patients were included if they were aged between 18 and 65 years, at least 6 weeks post-operative, and had an anatomically unremarkable gastric sleeve on contrast swallow. An unremarkable sleeve was defined as a tubular-shaped stomach without a retained fundus or evidence of obstruction or contrast leak. Patients were excluded if they had previous non-bariatric oesophago-gastric surgery or had a pre-existing oesophago-gastric motility disorder.
Surgical Technique
We performed a laparoscopic sleeve gastrectomy using a 36 French ViSiGi™ bougie and stapled with a tri-stapler (Echelon Flex ™ GST). Once the stomach was mobilised, stapling began 4 cm from the pylorus and finished at least 2 cm away from the GOJ. The staple line was imbricated with a running suture.
High Resolution Manometry
A 16-channel manometry catheter, attached to a water perfused system, was inserted transnasally. The distal sensor was positioned in the proximal stomach 2 cm below the inferior border of the lower oesophageal sphincter (Fig. 1). Data were recorded in real time using TRACE!1.2 (written by G. Hebbard using LabVIEW, National Instruments, Austin, TX). Our technique has been previously described [9]. We used a standardised protocol for each patient: (1) supine basal recording for 60 s, (2) 5 deep breaths, (3) 10 swallows with 5 ml water, (4) volume stress test (5 swallows of 10 ml water). Basal pressure was defined as end expiratory pressure.
Stress Barium
A retrospective analysis of sleeve gastrectomy patients who had undergone a stress barium at our institution was undertaken. The technique for stress barium was adapted from a previous technique [14]. Two swallows of 5 mL liquid barium were taken, with anterior radiographs taken. This process was repeated for the lateral view. In order to distend the stomach, patients ingested two spoonsful of barium-soaked porridge followed by 80 mL of undiluted porridge.
Volumetric CT Analysis
We used a standardised procedure for each patient’s volumetric CT. Each patient was fasted for a minimum of 6 h prior to CT scan. Immediately prior to the scan, patients were provided a two-part oral contrast solution of X-EVESS™ (MCI Forrest, West Footscray, Vic, Australia) containing a CO2 producing mixture of sodium bicarbonate and citric acid.
Part 2: Establishment of Finite Element Models
Finite Element Analysis
FEA simulation was undertaken using ANSYS Software (Fluent, ANSYS 18.0, PA, USA). Baseline gastric geometry was determined using parameters from volumetric CT. Anatomical features of importance were considered to be triangulated apex (‘dog-ear’), narrow incisura, tapered apex, and leak. Gastric geometry was included in the study based on the presence of the aforementioned key anatomical features which have previously been implicated in staple line leak such as stenosis in the proximal stomach and retained fundus.
Additional fixed parameters across each model included the following: 1 mm uniform wall thickness, internal pressure of 4000 Pa (~ 30 mmHg) in the proximal and distal compartment, and a fixed oesophagus and pyloric sphincter. Tensile strength data of fresh gastric tissue were extracted from previously published work [15]. The tensile ultimate strength was 0.67 MPa. We assumed a density of 1040 kg/m3 and Poisson ratio 0.3.
Part 3: Simulation Conditions
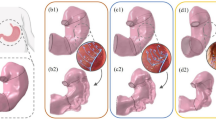
We simulated the conditions of a dry swallow by using longitudinal oesophageal displacement (shortening) of 3.5 cm during pressurisation [16]. The geometry of three models was also varied to evaluate the influence of key anatomical features on luminal wall stress (Fig. 2): proximal stenosis, triangulated apex, and the diameter of the incisura. A proximal stenosis was identified and dilated until it was a more consistent calibre (Fig. 2A). Similarly, a triangulated apex was created by enlarging a smaller apex (Fig. 2B), and the incisura of a model was widened from 42 to 50 Ch (Fig. 2C).
Statistical Analysis
All statistical analysis was performed with GraphPad Prism version 9.2.0 (GraphPad Software, San Diego, CA, USA). Continuous parametric data were analysed using Students t test. Where comparisons of repeated measures within the same subject were used, we used a repeated measures ANOVA. A p value < 0.05 was considered significant. Data were presented as mean ± standard deviation.
Results
Part 1: Establishment of Boundary Conditions
-
i.
Barium Swallow
Barium swallow studies after a sleeve gastrectomy appear to suggest a bicompartmental appearance of the post-operative stomach (Fig. 3). Swallowing is characterised by the filling of the proximal compartment, subsequent pressurisation, and emptying into the distal compartment. We surmised that previously reported intragastric hyper-pressurisations were related to this distention of the proximal compartment as this has been noted during concurrent fluoroscopy and intraluminal pressure measurements [9].
-
ii.
Measurement of Intraluminal Pressure in the Fasting State (Prolonged Study)
In order to establish the range of intragastric pressurisation, we assessed the high-resolution manometry (HRM) of fourteen patients after sleeve gastrectomy and compared then to ten obese controls. The results are described in Table 1. The median time between sleeve gastrectomy and manometry was 6 months (range: 5–31). The immediate post-operative period was uncomplicated for all these patients, and none developed staple line leak post operatively. Twelve of these patients underwent HRM for investigation of new reflux symptoms post operatively; the remaining two patients report new symptoms of dysphagia after their operation.
Ten obese control patients underwent manometry as a preoperative investigation prior to bariatric surgery. The demographic details of the control and sleeve gastrectomy groups were respectively: age 40.5 ± 17.7 vs 42.5 ± 15.7 (p = 0.22), gender 9 (90%) vs 11 (78.5%) female (p = 0.615), weight 122.3 ± 21.0 kg vs 110.6 ± 18.9 kg (p = 0.771), BMI 48 ± 11.7 vs 38.3 ± 3.8 (p = 0.023). BMI was significantly lower in the sleeve gastrectomy cohort (p = 0.023).
The sleeve gastrectomy cohort had a significantly higher peak intragastric isobaric pressures after normally structured swallows than those in the obese control group 31.58 ± 2.1 vs. 13.49 ± 1.3 mmHg (p = 0.0002) (Fig. 4). The IG/MO ratio at each point of hyperpressurisation was more negative after a swallow in the sleeve gastrectomy patients −4.36 ± 7.4 versus −1.17 ± 1.4 mmHg (p = 0.01). There was no significant difference between intragastric pressure in sleeve gastrectomy patients who had hiatus hernias 35.3 ± 11.3 mmHg versus 28.8 ± 8.4 mmHg in those without (p = 0.435).
During the basal stage of monitoring, there was no significant difference in peak pressures at end expiration 3.28 ± 3.4 vs. 5.78 ± 6.5 mmHg (p = 0.236). Similarly, there was no difference in the IG/MO ratio during the basal phase −0.123 ± 0.8 vs. −1.0 ± 1.8 mmHg (p = 0.081) (Fig. 4).
We delineated using HRM that the sleeve demonstrated isobaric pressurisations relating to distension of the proximal compartment. This led us to construct a model in which the distended pressurised state would exist even when swallowing minimal volumes.
Evaluation of high-resolution manometry. Peak intragastric isobaric pressures measured at A immediately after a normally structured wet swallow of 5 ml of water, and B at end expiration during the basal recording period. Intragastric/mid-oesophageal ratio of C peak intragastric pressure during a normally structured swallow and D at end expiration during the basal recording period
Part 2: Model Geometry Using Volumetric CT
The volumetric CT of 22 patients were assessed post sleeve gastrectomy. The median time after surgery was 2 years (range: 6 months–12 years).
Of the 22, 21 patients (95.5%) had a bicompartmental appearance. Four patients had a smoothly contoured proximal stomach. The remaining 18 patients had features of irregular contouring along the greater curvature of the proximal compartment. This included 2 patients with a tapered GOJ, 5 with a triangulated apex, 4 with a proximal stenosis, and 5 with a narrow incisura. One patient had a leak, which was known prior to the study.
We established that the post-operative stomach has a varied appearance which has implications for the transmission of mechanical forces to the gastric wall.
Part 3: Simulation of Model Using Finite Element Analysis (FEA)
-
i.
Simulation of a Dry Swallow
From the information delineated in parts 1 and 2, five distinct models of post-operative stomachs were established and underwent finite element analysis (Fig. 5). These models underwent a simulation of a dry swallow with oesophageal shortening and uniform pressurisation. During these simulations, we were able to determine luminal wall stress on different components of these models.
All simulations showed lower stress in the distal stomach wall compared to the proximal stomach. Stress forces were also found to be clustered at staple line adjacent to the GOJ, and maximal wall stress was observed there in the majority of models (Fig. 6). Only one model, with a uniformly contoured greater curvature, did not show concentrated deformation or material failure under maximal pressurisation (Fig. 5A). The highest stress geometry was the small triangulated apex model (Fig. 5B) at 218 kPa. The uniformly contoured model had the lowest stress at the GOJ with 34 kPa (Fig. 7A). GOJ stress in the tapered apex simulation (Fig. 6F) had the highest stress along the staple line at the GOJ (188 kPa) (Fig. 7A).
-
ii.
Variation in Geometry
Three of the existing models (Fig. 5B–D) were then modified to assess the effect of variation in geometry on the stress patterns acting on the gastric wall (Fig. 8).
Stress distribution was more uniform in the model with a dilated proximal stenosis (Fig. 8A i–ii). Von-mises stress was found be similar in both models, with a 4% reduction in peak stress in the modified simulation (192 kPa versus 185 kPa respectively). The larger triangulated apex model had a 17% higher maximal stress compared to the smaller triangulated apex model (255 kPa versus 218 kPa respectively) (Fig. 7B i–ii). Widening of the incisura did not result in a shift of stress forces but resulted in a 2.7% reduction in maximal wall stress (188 kPa versus 183 kPa respectively) (Fig. 8C i–ii).
The large triangulated apex model had a 37% increase in peak stress at the GOJ compared to the smaller triangulated apex model (203 kPA versus 148 kPA) (Fig. 7B).
There was a 4.5% decrease in stress at the GOJ in the dilated proximal stenosis compared to the unmodified model (132 kPa versus 138 kPa). A wider incisura led to a 9.9% reduction in stress at the GOJ during simulation (128 kPa versus 142 kPa).
-
iii.
Simulation of the Leak Model
A simulation of a swallow after staple line leak showed the highest stress forces around the incisura at 282 kPa (Fig. 9). This was more than twice the stress simulated at the leak site (135 kPa). The peak wall stress at the site of leak was lower than each other simulated geometry, except for the smoothly contoured sleeve. Similarly, equivalent stress at the GOJ was lower in the leak model, except when compared to the smooth contoured sleeve (Fig. 7A).
Luminal wall (von-mises) stress of the stomach during a simulated dry swallow with maximal stress and site of tissue failure marked (A–E). A Anterior view of smoothly contoured greater curvature model without evidence of tissue failure during simulation. B Posterior view of small dog-ear model with maximal wall stress acting on the GOJ at 218 kPa. C Anterior view of model with proximal stenosis with maximal wall stress acting on the posterior GOJ of 192 kPa. D Anterior view of narrow incisura model demonstrating peak wall stress of 189 kPa at the staple line at the GOJ. E Posterior view of tapered apex model demonstrating peak wall stress of 204 kPA at the proximal staple line near the GOJ. There is a cluster stress forces at the site of a posterior indentation
Finite element model of proximal staple line leak. A Total gastrectomy and oesophagojejunostomy with the site of the leak cicatrizing the stomach. B Axial section of abdominal CT with extraluminal gas (arrow) tracking through fistula. C Rendered stomach from the volumetric CT taken of a patient with staple line leak after sleeve gastrectomy demonstrating leak cavity (arrow). D FEA simulation with maximal wall stress at the incisura of 282 kPa. Peak stress at the site of leak was 135 kPa
Discussion
This study shows that there are significant isobaric high-pressure episodes that occur in the sleeve during oesophageal contractions. We have described how maximal shear forces could be transmitted to the staple line and precipitate tissue failure. Simulations of high-pressure events predict how maximal strain could be transmitted to the staple line at the GOJ during these events.
The distribution of luminal wall stress can be influenced by the geometry of the greater curvature. A smoother staple line is less likely to concentrate stress forces during simulation. An enlarged triangulated apex appeared to be a higher stress geometry during simulation of the key variable features of construction.
In our simulations the smoothly contoured greater curvature did not concentrate stress forces at any point along the staple line, suggesting that high stress events are not intrinsic in the construction of a sleeve gastrectomy. This may be a key factor in mitigating the risk of protracted staple line leak. In contrast, simulations suggest that the leak creates a lower wall stress geometry. This is consistent with the paradigm of the high-pressure sleeve, suggesting that leak has a decompressive effect.
The decline in incidence of staple line leak has been made more notable by the rise in popularity of the sleeve gastrectomy procedure. The reported incidence of leak varies between surgeons and institution, however, is approximately between 0.2 and 4% [5, 17]. The decrease in incidence has been attributed in-part to advances in surgical technique [18] and technology [19].
Intragastric hyper-pressurisation has been previously described after sleeve gastrectomy [9, 20]; however, there have been few studies demonstrating how these forces could be translated to the luminal wall and precipitate leak. Mid-gastric stenosis or incisura stricture has been suggested to play a role in leak [5]; however, not all cases of leak have evidence of stenosis [21, 22]. Parikh et al.’s meta-analysis found that a larger bougie size was associated with a reduction the risk of leak, suggesting that there is an intraluminal mechanism driving leak [23]. No other studies have utilised finite element analysis of gastric geometry to evaluate the transmission of stress forces along the staple line, despite its widespread application in biomechanics.
Marie et al.’s [24] porcine study describes a preferential burst pattern in the proximal sleeve after insufflation. Natoudi et al. found that similar burst pressures were required in the resected stomach after a sleeve [25]. Burst pressures in resected sleeve specimens have also been observed in our HRM findings [26]; however, these do not account for the geometry and dynamic shortening of the oesophagus during normal physiology. While the pattern of pressurisation is likely to differ in vivo due to various anatomical and physiological factors, the isobaric hyper-pressurisations found during our study were significant enough to theoretically cause gastric tissue failure using these findings. Associations between a thinner fundal wall and leak, while not significant [27], correlate with the mechanical hypothesis of leak.
Impaired vascular supply has been proposed and implicated in staple line leak [5, 6] and is likely to be associated in some leaks, but there is limited objective evidence to suggest that it is the major precipitating factor driving leak. Preliminary angiography findings published by Furia et al. on a small cohort of patients found limited evidence of vascular compromise after sleeve [28]. Despite these findings, it is possible that perfusion may play a role in multifactorial leak, but it does not appear to be the main causative factor. Studies assessing the association between leak and technical choices are difficult to adequately power given varied technique and relatively low incidence of leak, but suggest that there is no strong association between the two variables [19].
The strength of our study is that it uses sophisticated computer modelling to simulate the transmission of stress forces using real world tensile stress data during swallowing. We developed precise boundary conditions in our model to incorporate realistic conditions during swallow events and pressurisation. Simulation allows us to understand the influence of variation in sleeve construction without having to utilise large sample sizes or control for independent variables.
While FEA allows for flexibility in repeated simulation in a multitude of different conditions, it is difficult to account all of the physiological and biological factors influencing leak. Strict boundary conditions are necessary to create a functional model, but also remove the influence of independent variables. This model does not account for gastric contraction during filling and emptying of the stomach.
Future studies could use in vivo animal models to establish the influence of a particular geometry to precipitate leak; this will determine which factors need to be avoided to reduce the incidence of intractable leak. Further simulation using additional factors such intrinsic muscle contractility may provide more insight into the influence of geometry and the bicompartmental sleeve on gastric pressurisation.
Conclusions
This study provides evidence of how high-pressure events in the proximal stomach can transmit stress forces preferentially to the luminal wall of the proximal stomach. It demonstrates how a smoothly contoured sleeve evenly distribute stress forces in the proximal stomach, and how the geometry of the sleeve can influence the distribution of these stress forces. It is possible that imbrication or other methods to vary the geometry after stapling may influence the distribution of stress forces. These findings provide evidence for the theoretical and scientific basis of the luminal wall stress model of staple line leak.
References
Chouillard E, Younan A, Alkandari M, Daher R, Dejonghe B, Alsabah S, et al. Roux-en-Y fistulo-jejunostomy as a salvage procedure in patients with post-sleeve gastrectomy fistula: mid-term results. Surg Endosc. 2016;30(10):4200–4.
Catchlove W, Johari Y, Forrest E, Au A, Shaw K, Nottle P, et al. Initial radiologic appearance rather than management strategy predicts the outcomes of sleeve gastrectomy leaks. Surg Obes Relat Dis. 2022;18(2):205–16.
Hughes D, Hughes I, Khanna A. Management of staple line leaks following sleeve gastrectomy—a systematic review. Obes Surg. 2019;29(9):2759–72.
Johari Y, Catchlove W, Tse M, Shaw K, Paul E, Chen R, et al. A 4-tier Protocolized Radiological Classification System for Leaks Following Sleeve Gastrectomy. Annals of Surgery. 2022;275(2):e401–9.
Iossa A, Abdelgawad M, Watkins BM, Silecchia G. Leaks after laparoscopic sleeve gastrectomy: overview of pathogenesis and risk factors. Langenbecks Arch Surg. 2016;401(6):757–66.
Saber AA, Azar N, Dekal M, Abdelbaki TN. Computed tomographic scan mapping of gastric wall perfusion and clinical implications. Am J Surg. 2015;209(6):999–1006.
Mion F, Tolone S, Garros A, Savarino E, Pelascini E, Robert M, et al. High-resolution impedance manometry after sleeve gastrectomy: increased intragastric pressure and reflux are frequent events. Obes Surg. 2016;26(10):2449–56.
Yehoshua RT, Eidelman LA, Stein M, Fichman S, Mazor A, Chen J, et al. Laparoscopic sleeve gastrectomy—volume and pressure assessment. Obes Surg. 2008;18(9):1083.
Johari Y, Wickremasinghe A, Kiswandono P, Yue H, Ooi G, Laurie C, et al. Mechanisms of esophageal and gastric transit following sleeve gastrectomy. Obes Surg. 2021;31(2):725–37.
Gagner M, Kemmeter P. Comparison of laparoscopic sleeve gastrectomy leak rates in five staple-line reinforcement options: a systematic review. Surg Endosc. 2020;34(1):396–407.
Erdemir A, Guess TM, Halloran J, Tadepalli SC, Morrison TM. Considerations for reporting finite element analysis studies in biomechanics. J Biomech. 2012;45(4):625–33.
Miftahof RN. Biomechanics of the human stomach. Manama: Springer International Publishing; 2017. p. 213–26.
Lim G, Johari Y, Ooi G, Playfair J, Laurie C, Hebbard G, et al. Diagnostic criteria for gastro-esophageal reflux following sleeve gastrectomy. Obes Surg. 2021;31(4):1464–74.
Burton PR, Brown WA, Laurie C, Hebbard G, O’Brien PE. Mechanisms of bolus clearance in patients with laparoscopic adjustable gastric bands. Obes Surg. 2010;20(9):1265–72.
Egorov VI, Schastlivtsev IV, Prut EV, Baranov AO, Turusov RA. Mechanical properties of the human gastrointestinal tract. J Biomech. 2002;35(10):1417–25.
Lee YY, Whiting JGH, Robertson EV, Derakhshan MH, Smith D, McColl KEL. Measuring movement and location of the gastroesophageal junction: research and clinical implications. Scand J Gastroenterol. 2013;48(4):401–11.
Iannelli A, Treacy P, Sebastianelli L, Schiavo L, Martini F. Perioperative complications of sleeve gastrectomy: review of the literature. J Min Access Surg. 2019;15(1):1.
Cesana G, Cioffi S, Giorgi R, Villa R, Uccelli M, Ciccarese F, et al. Proximal leakage after laparoscopic sleeve gastrectomy: an analysis of preoperative and operative predictors on 1738 consecutive procedures. Obes Surg. 2018;28(3):627–35.
Ali AB, Morris LM, Hodges J, Amirkhosravi F, Yasrebi S, Khoo A, et al. Postoperative bleeding and leaks in sleeve gastrectomy are independent of both staple height and staple line oversewing. Surgical Endoscopy. 2022;4:1–7.
Mion F, Tolone S, Garros A, Savarino E, Pelascini E, Robert M, et al. High-resolution impedance manometry after sleeve gastrectomy: increased intragastric pressure and reflux are frequent events. Obes Surg. 2016;26(10):2449–56.
Nimeri A, Ibrahim M, Maasher A, Al HM. Management algorithm for leaks following laparoscopic sleeve gastrectomy. Obes Surg. 2016;26(1):21–5.
Nedelcu M, Manos T, Cotirlet A, Noel P, Gagner M. Outcome of leaks after sleeve gastrectomy based on a new algorithm adressing leak size and gastric stenosis. Obes Surg. 2015;25(3):559–63.
Parikh M, Issa R, McCrillis A, Saunders JK, Ude-Welcome A, Gagner M. Surgical strategies that may decrease leak after laparoscopic sleeve gastrectomy: a systematic review and meta-analysis of 9991 cases. Ann Surg. 2013;257(2):231–7.
Marie L, Masson C, Gaborit B, Berdah SV, Bège T. An experimental study of intraluminal hyperpressure reproducing a gastric leak following a sleeve gastrectomy. Obes Surg. 2019;29(9):2773–80.
Natoudi M, Theodorou D, Papalois A, Drymousis P, Alevizos L, Katsaragakis S, et al. Does tissue ischemia actually contribute to leak after sleeve gastrectomy? An experimental study. Obes Surg. 2014;24(5):675–83.
Causey MW, Fitzpatrick E, Carter P. Pressure tolerance of newly constructed staple lines in sleeve gastrectomy and duodenal switch. Am J Surg. 2013;205(5):571–5.
Boeker C, Schneider B, Markov V, Mall J, Reetz C, Wilkens L, et al. Primary sleeve gastrectomy and leaks: the impact of fundus-wall thickness and staple heights on leakage—an observational study of 500 patients. Frontiers in Surgery. 2021; 496.
Di Furia M, Romano L, Salvatorelli A, Brandolin D, Lomanto D, Cianca G, et al. Indocyanine green fluorescent angiography during laparoscopic sleeve gastrectomy: preliminary results. Obes Surg. 2019;29(12):3786–90.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions This study was funded by a grant from The Henry O’Hara Surgical Research Trust (#19004).
Author information
Authors and Affiliations
Contributions
Author 1 was extensively involved in design, data collection, data analysis, presentation, and write up. Author 2 was extensively involved in the design, and data collection. Author 3 was extensively involved in the initial design and data collection. Author 4 was extensively involved in supervision, the design, and final approval of the paper. Author 5 was extensively involved in initial concept, design, supervision, data analysis, presentation, write up, and final approval of the paper.
Corresponding author
Ethics declarations
Ethical Approval and Informed Consent
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Ethics approval was obtained from the Hospital Human Research and Ethics Committee (HREC) no. 380/16 and The Avenue Hospital HREC no. 236.
Informed consent does not apply.
Conflict of Interest
Author 1 reports grants from The Henry O'Hara Surgical Research Trust, during the conduct of the study. Author 2: No conflicts of interest to disclose. Author 3: No conflicts of interest to disclose. Author 4 reports grants from Johnson and Johnson, grants from Medtronic, grants from GORE, personal fees from GORE, grants from Applied Medical, grants from Apollo Endosurgery, grants and personal fees from Novo Nordisc, personal fees from Merck Sharpe and Dohme, outside the submitted work. Author 5: No conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• Intragastric isobaric hyper pressurisations occur in the proximal stomach after sleeve gastrectomy, Producing a radially distending force.
• Simulations suggest that luminal wall stress is preferentially transmitted to the GOJ and proximal staple line.
• The combination of isobaric pressurisation and preferential transmission of shear force is a highly plausible mechanism for leaks occurring at the proximal staple line.
• A distorted luminal wall concentrates stress far more than a uniformly contoured sleeve.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Catchlove, W., Liao, S., Lim, G. et al. Mechanism of Staple Line Leak After Sleeve Gastrectomy via Isobaric Pressurisation Concentrating Stress Forces at the Proximal Staple Line. OBES SURG 32, 2525–2536 (2022). https://doi.org/10.1007/s11695-022-06110-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-06110-z