Abstract
Introduction
Office blood pressure (OBP) and low-density lipoprotein cholesterol (LDL-C) calculated by the Friedewald formula (F) are the cornerstones of the cardiovascular risk (CVR) assessment and management based on the SCORE2/SCORE2-OP model proposed by the 2021 ESC Guidelines on Cardiovascular Disease Prevention.
Aim
We compared the CVR stratification estimated by the old SCORE and the SCORE2/SCORE2-OP using OBP and ambulatory blood pressure measurement (ABPM), and we evaluated the prevalence of LDL-C control, after calculating it using three validated equations, in outpatients referred for arterial hypertension.
Methods
A cross-sectional study on 1539 consecutive patients with valid ABPM. LDL-C was calculated using the Friedewald formula (F), its modification by Martin (M), and the Sampson (S) equation. SCORE and SCORE2/SCORE2-OP were estimated using OBP, mean daytime (+ 5 mmHg adjustment), and mean 24-hour systolic blood pressure (+ 10 mmHg adjustment). Individual CVR by 2021 ESC Guidelines (and SCORE2/SCORE2-OP) was compared to the 2019 ESC/EAS Guidelines (and SCORE). Differences in the prevalence of LDL-C control according to the three methods to calculate LDL-C were also analysed.
Results
Mean age was 60 ± 12 years, with male prevalence (54%). Mean LDL-C values were 118 ± 38 mg/dL (F), 119 ± 37 mg/dL (M), and 120 ± 38 mg/dL (S), respectively. Within the same population, SCORE and SCORE2/SCORE2-OP significantly varied, but no differences emerged after comparing the average SCORE2/SCORE2-OP calculated with OBP (6% IQR 3–10), mean 24-hour systolic BP (7% IQR 4–11), and mean daytime systolic BP (7% IQR 4–11). SCORE2/SCORE2-OP and 2021 ESC Guidelines reclassified the CVR independently of the method used for BP measurement. The low-moderate risk group decreased by 32%, whereas the high and veryhighrisk groups increased by 18% and 12%, respectively. We found a significant reduction in reaching the LDL-C goals regardless of the equation used to calculate it, except for those > 65 years, in whom results were confirmed only by using the M.
Conclusion
SCORE2/SCORE2-OP and 2021 ESC Guidelines recommendations led to a non-negligible CVR reclassification and subsequent lack of LDL-C goal, regardless of estimating SCORE2 using OBP or ABPM. Calculating the LDL-C with the M may be the best choice in specific settings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Cardiovascular diseases (CVD) are the leading cause of death and disability worldwide [1]. To enhance healthcare and prevention, the European Society of Cardiology (ESC) provided a 10-year individual cardiovascular risk (CVR) prediction algorithm known as the Systematic COronary Risk Evaluation (SCORE) [2]. SCORE was developed from cohorts recruited before 1986, including only fatal CVD outcomes and considering only low-density lipoprotein cholesterol (LDL-C), eventually underestimating the total CVR burden. For these reasons, the ESC has developed an updated prediction model, SCORE2, that estimates 10-year fatal and non-fatal CVD risk in European individuals, considering the non-high-density lipoprotein cholesterol (non-HDL) and the office systolic blood pressure (SBP) as measurements of total atherogenic cholesterol and arterial blood pressure, respectively [3]. Despite its limitations due to several potential sources of measurement inaccuracy and variability (patient-, device-, or procedure-related) and its lower performance regarding CV outcomes and mortality prediction compared to home blood pressure monitoring (HBPM) and 24-hour ambulatory blood pressure monitoring (ABPM), conventional office blood pressure (OBP) measurement is the most widely available, studied and recommended method for assessing BP when it comes to diagnose hypertension, estimate the goals of anti-hypertensive treatment according to the risk and benefits profile and when considering BP in individual global CVR assessment [4]. Recently, an observational cohort study including 59,124 patients referred for evaluation of hypertension in primary care in Spain compares clinic SBP with mean 24-hour SBP (24h-SBP) to predict all-cause death and cardiovascular death over a decade follow-up. The authors evidenced a stronger association between ABPM parameters and all-cause and cardiovascular death than OBP. Adjusted HR for 24h-SBP was 1.51 (95% CI 1.41–1.62) vs. 1.04 (95% CI 0.96–1.12) for OBP [5].
LDL-C is causally involved in atherosclerotic CVD (ASCVD) [6], and its evaluation is critical for an accurate CVR assessment and prevention [7]. The gold standard for LDL-C measurement is ultracentrifugation and beta-quantification [8]. Although this method is the highest-order reference procedure, it is expensive and time-consuming for most laboratories, so several formulas have been used to calculate LDL-C. Friedewald and colleagues developed the first equation in 1972 (hereafter referred to as the Friedewald formula, or F) [9]. This formula requires the standard lipid panel, including fasting plasma HDL-C, total cholesterol (TC) and triglycerides (TG). It is calculated as LDL-C = TC − HDL − (TG / 5) for mg/dL (or 2.2 when using mmol/L). The final term of the formula assumes a mean fixed ratio of TG levels to very low-density lipoprotein cholesterol (TG:VLDL-C) of 5:1. Nevertheless, the actual TG:VLDL-C ratio varies significantly across the range of TG and cholesterol levels, making the F less accurate in two increasingly common situations: higher TG levels (usually found in overweight/obesity and diabetes mellitus); lower LDL-C levels (particularly <100 mg/dL), a commonplace in contemporary clinical practice when aggressive lipid-lowering-therapy (LLT) is used [10, 11]. In 2013, Martin et al. developed a novel method (hereafter referred to as the Martin method, or M) for estimating LDL-C from F, based on data from over 1.35 million plasma samples analysed by ultracentrifugation [12]. Rather than assuming a fixed TG denominator of 5, the M applies to the F an empirical and adjustable factor for the TG:VLDL-C ratio that varies depending on TG and non–HDL-C levels. This method is more accurate than the former one, particularly for low–LDL-C samples [13]. Finally, in 2020, Sampson et al. [14] proposed another equation for calculating LDL-C [hereafter referred to as the Sampson formula or S, also known as the National Institute of Health (NIH) 2 method]. They suggested that this formula is more accurate than all the others currently available in patients with low LDL-C levels or hypertriglyceridemia [15]. In a recent study on serum lipid panels of 1179 patients, the Martin formula and, to a lesser extent, the Sampson formula showed significantly higher correlation coefficients than the Friedewald formula with apolipoprotein B and, thereby, with the number of circulating atherogenic LDL particles [16]. This study investigated the differences between average SCORE and SCORE2/SCORE2-OP calculated using systolic OBP, adjusted mean daytime SBP and 24h-SBP from ABPM and the impact on CVR stratification. We compared the CVR estimated by the 2019 ESC/EAS Dyslipidemia Guidelines (and SCORE) and the 2021 ESC Guidelines on Cardiovascular Disease Prevention (and SCORE2/SCORE2-OP). After calculating LDL-C with the three validated equations, we also assessed the prevalence of LDL-C control according to the individual goal. To the best of our knowledge, this is the first study that has jointly compared CVR models and equations for LDL-C calculation to evaluate their combined impact on the prevalence of lipid control in a large population whose BP has been evaluated by both OBP and ABPM.
2 Methods
2.1 Study Design and Population
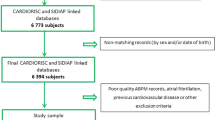
We conducted a cross-sectional study on 1539 consecutive outpatients referred to our "Hypertension Excellence Centre" of the European Society of Hypertension (ESH) from January 2022 to March 2023 because of suspected high BP or hypertension management, but not for dyslipidemia. Most patients were referred to our Hypertension Centre by general practitioners, while only a minority were by other specialists. Therefore, our sample reflects well the community-dwelling population. All patients in this study were tested with accurate OBP measurements and ABPM. Patients enrolled were in primary or secondary CV prevention, and other inclusion criteria were the following: age > 40 years, a valid ABPM, and a full lipid panel (TC, HDL-C and TG) non-suggestive for familial autosomal dominant hypercholesterolemia (FH), all performed within the previous month. We excluded patients with TG > 400 mg/dL because F was not applicable. All participants gave their informed consent, and clinical investigations were conducted according to the principles of the Declaration of Helsinki and its later amendments. This study was approved by the local institutional ethics committee (INRCA Ethics Committee).
2.2 Clinical and Laboratory Parameters
We collected all recruited patients' medical history, anthropometric measurements (body mass index, BMI, defined as the body mass divided by the square of the body height and expressed in units of kilogram per square meter, waist circumference), cardiovascular drug therapy, and complete laboratory tests. The CKD-EPI creatinine equation estimated the glomerular filtration rate (eGFR). The lipid profile was obtained after fasting sampling, and then LDL-C was calculated using the three validated equations: F, M and S. Non-HDL-C was calculated by subtracting the HDL-C from TC. Type 2 diabetes mellitus (T2DM) was defined based on documented medical history or the use of antidiabetic drugs. Smoking status was ascertained during recruitment, and the smoking habit was defined as the current or previous smoking of at least 100 cigarettes in a lifetime [17]. Chronic kidney disease (CKD) was determined by stable eGFR< 60 ml/min/1.73 m2.
2.3 Blood Pressure Measurement
During office evaluation, we performed three sequential oscillometric automatic BP measurements on both arms using validated devices (Microlife® model BP3MQ1-2D and BP A200 AFib, Widnau, Switzerland). Correct cuff sizes (range 22–32 cm or 32–42 cm) were selected according to arm circumference, and BP measurements were performed after at least 5 min of rest in the sitting position. The patient's arm was kept at the heart level during the measurement. The higher average systolic BP value between arms was used for the analysis and to position the ABPM, thus avoiding errors due to interarm BP differences. The 24-hour ABPM was performed within one month before the office evaluation without therapeutic changes, using Spacelabs 90207 and 90217 (SpaceLabs Healthcare, Snoqualmie, Washington, USA). An appropriate cuff dimension was used according to the arm circumference. Minimum quality criteria for a satisfactory ABPM recording were based on recommendations by Omboni et al. [18]. For each patient, 24-hour BP, daytime BP (defined as the BP values from 06:00 to 22:00), and night-time BP (defined as the BP values from 22:00 to 06:00) were considered. The definitions of "day" and "night" periods were based on the most common answers to a questionnaire in which patients were asked about their sleeping behaviour. In our patients, ABPM was performed to diagnose hypertension in suspected cases and assess BP control in treated patients. According to OBP, some patients had a high-normal BP, and ABPM was performed to evaluate possible masked hypertension, as suggested by the 2018 ESC/ESH guidelines [19]. Thus, not all enrolled patients were hypertensive at the end of the assessments.
2.4 Individual CVR Stratification and Control
The individual 10-year CVR, reported in Supplemental Table S1, was estimated according to SCORE and SCORE2 (as calibrated for moderate risk European regions) and its equivalent for patients older than 70 years (SCORE2-OP) after taking into account other major CVR factors or ASCVD as suggested by both 2019 ESC/EAS Guidelines for the management of dyslipidemias and 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice [20, 21]. Concerning the classification proposed by the 2019 ESC/EAS Dyslipidemia guidelines, we merged the low and moderate-risk groups into the low-moderate group for better comparisons. Also, we did not take into account the extreme risk because it was not present in the former 2019 classification and because none of our patients would have fallen into this group. Office SBP, clinically adjusted mean daytime (+ 5 mmHg), and mean 24h-SBP (+ 10 mmHg) obtained by ABPM were used to calculate SCORE2/SCORE2-OP. At the same time, for the global individual CVR assessment, hypertension was defined if the patient was on anti-hypertensive therapy or if ABPM reported a mean 24h-SBP ≥ 130 mmHg and/or a mean 24-hour diastolic blood pressure (24h-DBP) ≥ 80 mmHg [22]. The duration of T2DM and additional laboratory or imaging information on target organ damage (TOD) (i.e., urine albumin-to-creatinine ratio, cardiac or vascular ultrasound evaluation, etc.) was unavailable in many patients for further CVR assessment. Patients' LDL-C levels were defined at goal based on the following targets, according to the individual CVR stratification: LDL-C below 100 mg/dL for patients at low-moderate CVR, LDL-C below 70 mg/dL for patients at high CVR and LDL-C below 55 mg/dL for patients at very high CVR.
2.5 Statistical Analyses
Continuous variables were checked for normality and expressed as mean ± standard deviation or as median and interquartile range (IQR) if markedly skewed. Categorical variables were expressed as numbers and percentages. Variables were compared using Wilcoxon's Signed Rank Test and General Linear Model for repeated measures within subjects and Bonferroni adjustment. Pearson's and Spearman's methods were used for correlations between variables. Differences in frequencies within the same group were evaluated using the Mc Nemar or Marginal Homogeneity Test. A p-value < 0.05 was considered statistically significant. All statistical analyses were conducted with SPSS version 23 [SPSS Inc., Chicago, IL, USA], Microsoft Windows version.
3 Results
The general characteristics of the study population are reported in Table 1. We included 1539 patients in the analyses. The mean age was 60 ± 12 years, and male prevalence was 54%. The mean BMI was 28 ± 5 Kg/m2, and the mean waist circumference was 95 ± 11 cm in women and 103 ± 11 in men, respectively. Overweight (OW) and obese (OB) patients were 35% and 27%, respectively. The prevalence of T2DM was 13%. The mean office SBP was 140 ± 13 mmHg, and the mean office DBP was 86 ± 11 mmHg. Regarding ABPM parameters, the mean 24h-SBP was 131 ± 11 mmHg, the mean 24h-DBP was 78 ± 10 mmHg, the mean daytime SBP was 138 ± 14 mmHg, and the mean daytime DBP was 80 ± 12 mmHg. The prevalence of arterial hypertension, considering those in anti-hypertensive therapy, was 68% (1044 patients). In hypertensives, the mean office SBP was 134 ± 13 mmHg, the mean office DBP was 81 ± 10 mmHg, the mean 24h-SBP was 136 ± 10 mmHg, the mean 24h-DBP was 83 ± 9 mmHg, the mean daytime SBP was 130 ± 12 mmHg, and the mean daytime DBP was 79 ± 11 mmHg. Patients in primary prevention were 1236 (80% of the study population). Regarding the serum lipid profile, the mean TC was 196 ± 43 mg/dL, mean HDL-C was 54 ± 14 mg/dL, and median TG was 105 (IQR 80-150) mg/dL, respectively. Mean LDL-C values significantly varied depending on the formula used for their calculation (p < 0.001 for comparisons). Indeed, mean LDL-C values were the following: 118 ± 38 mg/dL according to F, 119 ± 37 mg/dL according to M, and 120 ± 38 mg/dL according to S, respectively. M and S showed a significant and almost total correlation with F (r = 0.998 for S and r = 0.991 for M). The clinical meaningfulness of one mg difference from F to M and one mg difference from M to S is likely to be irrelevant considering mean values; still, it was relevant for individual risk evaluation, as shown below.
3.1 Impact of BP Measurement Methods on CVR Stratification and LDL-C at Goal Prevalence
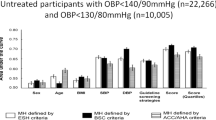
SCORE2/SCORE2-OP estimated with office SBP, adjusted mean daytime SBP and 24h-SBP were strongly correlated (SCORE2 with office SBP vs SCORE2 with adjusted daytime SBP: r = 0.979; SCORE2 with office SBP vs SCORE2 with adjusted 24h-SBP: r = 0.977, all p<0.001). The average SCORE2/SCORE2-OP estimated with office SBP (6%, IQR 3-10) or with adjusted 24h-SBP (7%, IQR 4–11) or with adjusted daytime SBP (7% IQR 4–11) showed no meaningful differences. After classifying the individual CVR according to the SCORE2/SCORE2-OP and the 2021 ESC Guidelines on cardiovascular disease prevention, we found a substantial rearrangement compared to the classification based on the SCORE and the 2019 ESC/EAS Guidelines for the management of dyslipidemias, regardless of the BP measurement method used to estimate SCORE2/SCORE2-OP. Patients at low-moderate risk decreased from 826 (55%) to 356 (23%), patients at high risk increased from 307 (20%) to 582 (38%), and patients at very high risk rose from 380 (25%) to 575 (37%) (Fig. 1 Panel A). Fifty-seven percent of those who were at low-moderate risk were redistributed among high (51%) and very-high risk (6%); 47% of individuals previously in the high risk were reclassified as very-high; all patients in the very-high risk group were confirmed belonging to the very-high risk. Consequently, we found meaningful changes in the proportion of patients achieving LDL-C goals based on the reclassified individual CVR, considering all three equations used for the LDL-C calculation (from 26 to 20% applying F, from 25 to 18% applying M, and from 24 to 18% with S, p < 0.001 for comparisons) (Fig. 1 Panel B). Notably, the lowest prevalence of patients with adequate risk-based LDL-C control was only 18% when using M and S. As expected, we found that by calculating the LDL-C using the S or the M, the proportion of patients at goal was significantly lower than when the F was used (Fig. 2). The results were also confirmed to be independent of the LDL-C formula after considering those patients (524, 34% of the study population) already taking a lipid-lowering therapy (LLT) with statins or ezetimibe, in hypertensives, as well as in other subgroups. The only exception was the subgroup of patients over 65 years, in whom despite showing the same trend, we found a significant decrease in the prevalence of LDL-C at goal only if considering the M, but not the F and S. A complete overview of these findings is reported in Table 2.
Differences in CVR stratification and LDL-C control according to 2019 ESC/EAS and 2021 ESC Guidelines. Panel A shows how applying the 2021 Guidelines on Cardiovascular Prevention changed the CVR stratification; most of the population was reclassified as higher risk. Panel B shows how the CVR reclassification reduced the proportion of patients reaching low-density lipoprotein cholesterol (LDL-C) goals independently of the formula used to calculate LDL-C
4 Discussion
Increasingly lower LDL-C goals and recently approved lipid-lowering therapies (LLTs) to improve further the treatment efficacy led to a renewed emphasis on CV preventive strategies and to the need for a more reliable and precise individual CVR assessment of the adult population to guarantee the optimal and most personalized therapy approach. The 2021 ESC Guidelines on cardiovascular disease prevention have proposed new recommendations and tools for better estimating the CVR, especially for primary prevention, which achieved broad consensus and have been widely adopted [23]. Adopting the SCORE2/SCORE2-OP by these Guidelines is the most important novelty. Differently and more accurately than the previous SCORE algorithm, SCORE2/SCORE2-OP estimate the 10-year risk of CVD death and non-fatal CVD events (such as myocardial infarction and stroke) using non-HDL cholesterol in patients over 40 years. Although without additional laboratory tests or imaging information about TOD, but strongly supported by the availability of ABPM in each patient (used not only to define hypertension in non-treated patients but also to assess any potential impact on CVR stratification), our results highlighted how a significant portion of the study population underwent a reclassification of the CVR based on SCORE2/SCORE2-OP and 2021 ESC Guidelines, regardless of using OBP or ABPM to estimate CVR. A clear overall trend emerged, showing a decreased prevalence of those defined at low-moderate risk and an increased prevalence of those defined at high or very high CVR. Recent investigations conducted on similarly sized European cohorts found the same results [24], and one study on more than 85000 patients aged 40-65 found that whenever the SCORE2 instead of the SCORE was used, 44% of the population was reclassified with a higher risk [25]. Likewise, the same applies concerning other major CV risk factors, such as hypertension. Among the 512 hypertensive patients evaluated by Del Pinto et al., with the application of the new parameters for fatal and non-fatal CVR assessment proposed by the 2021 ESC Guidelines, the proportion of individuals at high or very high risk rose from 49 to 77% of cases [26]. Most of the population in the study (62%) resulted in the overweight (OW) and obese (OB) range of BMI, with mean waist circumference suggestive of excess visceral adipose tissue for both genders. Previous data from our group have demonstrated that dyslipidemia is common and too often neglected in OW and OB hypertensive patients despite they present a more atherogenic lipid pattern likely driven by metabolic derangement pivoting around excess adipose tissue and insulin resistance. In such population, only one-third of OW/OB patients had a LDL-C at goal, while BP was controlled in only about 40% of patients. Moreover, only 12% of OW/OB patients had both mean 24-hour BP and LDL-C at target. Likewise, the higher the CVR, the lower the rate of LDL-C control and individuals in secondary prevention had worse LDL-C control than patients in primary prevention [27].
The immediate consequence of such a radical increase in the number of patients with high or very high CVR is that the LDL-C goal dramatically changed for many patients, and we observed an even worse LDL-C control among all three classes of CVR after the reclassification. Results were replicable in almost all the other subgroups considered in the analyses, including patients already treated with LLT and hypertensives, representing nearly half of our population. In hypertensives, 20% were on LLT (18% on statin and 2% on ezetimibe), and we observed LDL-C at goal only in the 13–15% range. These real-life data are discouraging and in evident contrast to the great body of evidence that suggests, on the one hand, an exponentially increased CVR when multiple uncontrolled risk factors coexist and, on the other hand, the benefits that could derive from tackling hypertension and dyslipidemia with a synergistic combination of metabolically neutral anti-hypertensive and lipid-lowering drugs, often offered in single-pill formulation, thus increasing efficacy and adherence [28, 29].
In this regard, individual CVR estimation in each hypertensive patient has recently been stressed and endorsed by the latest 2023 ESH Guidelines because of its relevance in hypertension management, especially in individuals with a high-normal BP or grade 1 hypertension, in whom it may influence the decision of whether or how fast to initiate BP-lowering drug treatment. In assessing individual CVR, ESH Guidelines recommend using the more accurate SCORE2/SCORE2-OP tool based on office SBP. Excluding the DBP in the risk chart has been criticized, and the potential role of ABPM in estimating the CVR more accurately needs further clarification and validation [4].
Furthermore, LDL-C control also seemed to depend on the formula used for its calculation. As described by several authors, while assessing the accuracy of different LDL-C formulas by comparing the calculation with the direct measurement of serum LDL-C and in various clinical scenarios such as non-fasting, high levels of TG, and low LDL-C, the S and the M emerged as the best performing [30]. Estimating the accuracy of the three considered LDL-C equations is beyond the scope of this investigation. We instead wanted to explore the potential impact of assessing LDL-C by different equations on the proportion of patients reaching the LDL-C goal. In our real-life analyses, we pointed out meaningful differences in estimated LDL-C between the three equations, with both the M and S constantly calculating higher LDL-C values than the F. Within and between the two CVR assessment models considered in the study, overall LDL-C control resulted different after comparing the three equations (non-significant only between S and M within the 2021 model, p = 0.786), Fig. 2. Also, based on the 2021 ESC Guidelines and SCORE2/SCORE2-OP CVR stratification, only 18% of the overall population would achieve the LDL-C goal using the M and the S. Moreover, the proportion of patients at LDL-C goal in all the subgroups considered in the study was significantly reduced, regardless of the method used to calculate LDL-C. The only exception was the group > 65 years, in whom differences in LDL-C control between the former and the latter CVR stratification emerged when using the M, but not the F or the S. Actually, older patients represented more than one-third of our sample (n. 578, 38%) and had higher CVR than the younger group (median SCORE2 12% vs 4%, p < 0.001; very-high CVR 67% vs 19%, p < 0.001), were more treated with LLT (52% vs 23%, p < 0.001; statin 47% vs 21%) and consequently showed lower LDL-C (patients with LDL-C < 100 mg/dL 48% vs 25%, p < 0.001). In cases of very high CVR and low LDL-C, the enhanced accuracy of the M may help isolating those who would benefit from a more aggressive reduction of LDL-C to improve outcomes [13, 30]. This approach could be adequately applied in the old population in whom an appropriately aggressive LLT may reduce ASCVD [31, 32], and over-treatment may have a negative impact, given the risk of medication adverse effects and the burden of polypharmacy.
Eventually, in our study, we highlighted that the proportion of patients with suboptimal CVR management regarding dyslipidemia depended more on the accuracy of the risk assessment strategies than the method used for calculating LDL-C values and that there is still a lack of awareness about the critical role of a systematic application of updated methods of individual global CVR assessment.
To render CVR evaluation a very rapid task with broader use in clinical practice, we recently developed an open free-to-use web-app (www.humtelemed.it) based on the 2019 ESC/EAS Guidelines for the management of dyslipidemias updated with SCORE2/SCORE2-OP (that is most useful in primary prevention) and using the M for LDL-C calculation. Easy-to-use apps can be the way to further spread and optimize the appropriate individual CVR evaluations in daily clinical practice.
4.1 Study Strengths and Limitations
Although our sample referred to a Hypertension Excellence Centre, it reflects the community-dwelling population at CV risk well. This aspect could strengthen the work since the data can be better extended to the general population. Assessing the BP profile by more accurate ABPM and calculating LDL-C by the three most used equations provide a more comprehensive picture of the extent of their impact on CVR assessment and management compared to conventional methods. As stated in the Materials and Methods section, the individual CVR could be partially biased by the absence of data regarding the systematic TOD evaluation (i.e., albuminuria, left ventricular hypertrophy, carotid atherosclerosis, coronary calcium score).
5 Conclusions
The potential for a significant impact of CVR reclassification follows the application of the 2021 ESC Guidelines on cardiovascular disease prevention. The reclassification occurs due to the more accurate assessment of individual CVR using new tools such as SCORE2/SCORE2-OP, algorithms and risk charts, and additional risk factors in the prediction models. In a first analysis, ABPM and OBP seem to share similar abilities in estimating CVR; thus, if correctly carried out, OBP remains the most accessible and straightforward method. A non-negligible proportion of individuals previously classified as low-moderate risk may be reclassified as high or very risk, and this should lead to earlier and more intensive preventive interventions with personalized strategies, aiming at increasing adherence and reducing CVD burden. More awareness about the strengths and limitations of the methods used for LDL-C calculation will help CVR classification and treatment decisions. In specific conditions, such as low LDL-C values due to LLT or whenever considering risks and benefits of more aggressive interventions (i.e. in older patients), the modified Friedewald equation by Martin could represent the more suitable choice. Apps for a quick and easy CVR evaluation (such as the web app www.humtelemed.it developed by our group) may be helpful to a broader application of CVR evaluation in clinical practice.
References
Roth GA, Mensah GA, Johnson CO, Addolorato G, Ammirati E, Baddour LM, et al. Global Burden of Cardiovascular Diseases and Risk Factors, 1990–2019: Update From the GBD 2019 Study. J Am Coll Cardiol. 2020;76(25):2982–3021.
Conroy RM, Pyörälä K, Fitzgerald AP, Sans S, Menotti A, De Backer G, et al. Estimation of ten-year risk of fatal cardiovascular disease in Europe: the SCORE project. Eur Heart J. 2003;24(11):987–1003.
SCORE2 risk prediction algorithms. new models to estimate 10-year risk of cardiovascular disease in Europe. Eur Heart J. 2021;42(25):2439–54.
Mancia G, Kreutz R, Brunström M, Burnier M, Grassi G, Januszewicz A, et al. ESH Guidelines for the management of arterial hypertension The Task Force for the management of arterial hypertension of the European Society of Hypertension Endorsed by the European Renal Association (ERA) and the International Society of Hypertension (ISH). J Hypertens. 2023 Jun 21. https://doi.org/10.1097/HJH.0000000000003480. Online ahead of print.
Staplin N, de la Sierra A, Ruilope LM, Emberson JR, Vinyoles E, Gorostidi M, et al. Relationship between clinic and ambulatory blood pressure and mortality: an observational cohort study in 59 124 patients. Lancet 2023 Jun 17;401(10393):2041-2050.
Ference BA, Ginsberg HN, Graham I, Ray KK, Packard CJ, Bruckert E, et al. Low-density lipoproteins cause atherosclerotic cardiovascular disease. 1. Evidence from genetic, epidemiologic, and clinical studies. A consensus statement from the European Atherosclerosis Society Consensus Panel. Eur Heart J. 2017;38(32):2459–72.
Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation. 2002;106(25):3143-421.
Nakamura M, Kayamori Y, Iso H, Kitamura A, Kiyama M, Koyama I, et al. LDL cholesterol performance of beta quantification reference measurement procedure. Clin Chim Acta. 2014;431:288–93.
Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem. 1972;18(6):499–502.
Sajja A, Park J, Sathiyakumar V, Varghese B, Pallazola VA, Marvel FA, et al. Comparison of methods to estimate low-density lipoprotein cholesterol in patients with high triglyceride levels. JAMA Netw Open. 2021;4(10): e2128817.
Bolat S, Ertürk Zararsız G, Doğan K, Kochan N, Yerlitaş SI, Cephe A, et al. Concordance of LDL-C estimating equations with direct enzymatic measurement in diabetic and prediabetic subjects. J Clin Med . 2023 May 20;12(10):3570. https://doi.org/10.3390/jcm12103570.
Martin SS, Blaha MJ, Elshazly MB, Toth PP, Kwiterovich PO, Blumenthal RS, et al. Comparison of a novel method vs the Friedewald equation for estimating low-density lipoprotein cholesterol levels from the standard lipid profile. JAMA. 2013;310(19):2061–8.
Martin SS, Giugliano RP, Murphy SA, Wasserman SM, Stein EA, Ceška R, et al. Comparison of low-density lipoprotein cholesterol assessment by martin/hopkins estimation, friedewald estimation, and preparative ultracentrifugation: insights from the FOURIER Trial. JAMA Cardiol. 2018;3(8):749–53.
Sampson M, Ling C, Sun Q, Harb R, Ashmaig M, Warnick R, et al. A new equation for calculation of low-density lipoprotein cholesterol in patients with normolipidemia and/or hypertriglyceridemia. JAMA Cardiol. 2020;5(5):540–8.
Ginsberg HN, Rosenson RS, Hovingh GK, Letierce A, Samuel R, Poulouin Y, et al. LDL-C calculated by Friedewald, Martin-Hopkins, or NIH equation 2 versus beta-quantification: pooled alirocumab trials. J Lipid Res . 2022 Jan;63(1):100148. https://doi.org/10.1016/j.jlr.2021.100148. Epub 2021 Nov 11.
Briers PJ, Langlois MR. Concordance of apolipoprotein B concentration with the Friedewald, Martin-Hopkins, and Sampson formulas for calculating LDL cholesterol. Biochem Med (Zagreb). 2022;32(1): 010704.
Giulietti F, Filipponi A, Rosettani G, Giordano P, Iacoacci C, Spannella F, et al. Pharmacological approach to smoking cessation: an updated review for daily clinical practice. High Blood Press Cardiovasc Prev. 2020;27(5):349–62.
Omboni S, Palatini P, Parati G. Standards for ambulatory blood pressure monitoring clinical reporting in daily practice: recommendations from the Italian Society of Hypertension. Blood Press Monit. 2015;20(5):241–4.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39(33):3021–104.
Mach F, Baigent C, Catapano AL, Koskinas KC, Casula M, Badimon L, et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS). Eur Heart J. 2019;41(1):111–88.
Visseren FLJ, Mach F, Smulders YM, Carballo D, Koskinas KC, Bäck M, et al. 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2021;42(34):3227–337.
Stergiou GS, Palatini P, Parati G, O’Brien E, Januszewicz A, Lurbe E, et al. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. J Hypertens. 2021;39(7):1293–302.
Volpe M, Gallo G, Modena MG, Ferri C, Desideri G, Tocci G. Updated recommendations on cardiovascular prevention in 2022: an executive document of the italian society of cardiovascular prevention. High Blood Press Cardiovasc Prev. 2022;29(2):91–102.
Boskovic N, Giga V, Djordjevic-Dikic A, Beleslin B, Stojkovic S, Nedeljkovic I, et al. Comparison of SCORE and SCORE 2 risk prediction tools in contemporary very high risk european population. European Heart Journal, Volume 43, Issue Supplement_2, October 2022, ehac544.2281, https://doi.org/10.1093/eurheartj/ehac544.2281
Csenteri O, Jancsó Z, Szöllösi GJ, Andréka P, Vajer P. Differences of cardiovascular risk assessment in clinical practice using SCORE and SCORE2. Open Heart . 2022 Nov;9(2):e002087. https://doi.org/10.1136/openhrt-2022-002087.
Del Pinto R, Giua C, Keber E, Grippa E, Tilotta M, Ferri C. Impact of 2021 ESC Guidelines for cardiovascular disease prevention on hypertensive patients risk: secondary analysis of save your heart study. High Blood Press Cardiovasc Prev. 2023;30(2):167–73.
Spannella F, Giulietti F, Di Pentima C, Sarzani R. Prevalence and control of dyslipidemia in patients referred for high blood pressure: the disregarded “Double-Trouble” lipid profile in overweight/obese. Adv Ther. 2019;36(6):1426–37.
Borghi C, Fogacci F, Agnoletti D, Cicero AFG. Hypertension and dyslipidemia combined therapeutic approaches. High Blood Press Cardiovasc Prev. 2022;29(3):221–30.
Sarzani R, Laureti G, Gezzi A, Spannella F, Giulietti F. Single-pill fixed-dose drug combinations to reduce blood pressure: the right pill for the right patient. Ther Adv Chronic Dis. 2022;13:20406223221102750.
Martins J, Steyn N, Rossouw HM, Pillay TS. Best practice for LDL-cholesterol: when and how to calculate. J Clin Pathol. 2023;76(3):145–52.
Mortensen MB, Nordestgaard BG. Elevated LDL cholesterol and increased risk of myocardial infarction and atherosclerotic cardiovascular disease in individuals aged 70–100 years: a contemporary primary prevention cohort. Lancet. 2020;396(10263):1644–52.
Gencer B, Marston NA, Im K, Cannon CP, Sever P, Keech A, et al. Efficacy and safety of lowering LDL cholesterol in older patients: a systematic review and meta-analysis of randomised controlled trials. Lancet. 2020;396(10263):1637–43.
Acknowledgements
The authors would like to express sincere gratitude to all the individuals and organizations contributing to this research paper.
Funding
Open access funding provided by Università Politecnica delle Marche within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
All patients included in the study provided informed consent, and the local ethical committee (INRCA IRCCS of Ancona, Italy) approved the investigation according to the declaration of Helsinki and its later amendments.
Consent for Publication
Not applicable.
Availability of data and Materials
The datasets used and analysed during the current study are available from the corresponding author upon reasonable request.
Conflict of Interests
The authors declare no conflict of interest.
Funding
This research was funded by "Politecnica delle Marche" University (Ricerca di Ateneo to Prof. Riccardo Sarzani). This research received no specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author's Contributions
ML made the analyses. ML and MA wrote the manuscript. ML elaborated tables and figures. FS, MA, AG, FG, and RS planned and supervised the whole study and revised the manuscript. ML and MA should both be considered as first authors. All the authors contributed equally to the data collection and preparation of the dataset.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Landolfo, M., Allevi, M., Spannella, F. et al. Cardiovascular Risk Assessment and Control in Outpatients Evaluated by 24-hour Ambulatory Blood Pressure and Different LDL-C Equations. High Blood Press Cardiovasc Prev 30, 551–560 (2023). https://doi.org/10.1007/s40292-023-00605-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-023-00605-1