Abstract
Buruli ulcer (BU), one of the skin-related neglected tropical diseases (skin NTDs), is a necrotizing and disabling cutaneous disease caused by subcutaneous infection with Mycobacterium ulcerans. Leading on from the World Health Organization’s (WHO) establishment of a global BU initiative in 1998, >67,000 cases of BU have been reported from over 32 countries, mostly from West Africa and Australia. While treatment is currently in the transition period from rifampicin plus streptomycin (injection) to an all-oral regimen, it cannot hope to eradicate this opportunistic environmental pathogen. M. ulcerans is genetically very similar to related pathogenic organisms M. marinum, M. leprae and M. tuberculosis. However, M. ulcerans carries a unique megaplasmid, pMUM001, encoding the biosynthetic machinery responsible for production of a lipid-like exotoxin virulence factor, mycolactone. This diffusible compound causes the substantial divergence in BU’s pathogenic aetiology from other mycobacterial infections. Hence, mycolactone is cytotoxic and immunosuppressive and causes vascular dysfunction in infected skin. A major recent advance in our understanding of BU pathogenesis has been agreement on the mycolactone’s mechanism of action in host cells, targeting the Sec61 translocon during a major step in secretory and membrane protein biogenesis. While vaccine development for all mycobacteria has been challenging, mycolactone production likely presents a particular challenge in the development of a BU vaccine. The live-attenuated vaccine BCG is known to provide only partial and transient protection in humans but provides a convenient baseline in mouse preclinical studies where it can delay, but not prevent, disease progression. No experimental vaccine strategy has yet conferred greater protection than BCG. However, there is now the prospect of developing a vaccine against mycolactone itself, which may provide hope for the future.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
1 Buruli Ulcer
The neglected tropical disease (NTD) Buruli ulcer (BU) is caused by subcutaneous infection with Mycobacterium ulcerans, resulting in necrosis of subcutaneous fatty tissue and the formation of ulcers with undermined edges which can extend to 15% of body surface area [1]. Much of its obscurity may be attributed to the fact that it predominantly affects the poor [2, 3], usually in remote rural areas with limited access to health services [4, 5]. Hence, while BU is considered a rare disease on a global scale, its impact on endemic communities should not be underestimated. BU is associated with social stigma [6] and presents a large financial [7, 8] and psychological [9] burden to patients and their care-givers, especially since most patients are young teenagers. A major global intervention came in 1998 when the WHO launched its Global BU Initiative (GBUI). This served as a forum for disease control and research efforts. Its success is clear from the global decrease in BU prevalence since 2010 [4], although this does not take into account under-reporting in countries without effective national control programmes [5]. Moreover, it brought about much of the research described in this chapter, and its success has underpinned the WHO’s most recent integrated approach to control all skin NTDs [10].
1.1 Epidemiology and Transmission
Infections that were most likely BU were first described by Sir Albert Cook at the turn of the twentieth century [11]. However, it was not until 1948 that the causative organism was identified by Peter MacCallum [12], due to the fortuitous breakdown of an incubator. To date, a total of >67,000 cases of BU have been reported worldwide in 32 countries including Japan, Papua New Guinea and Central and South America. At present, the highest prevalence of BU is in West Africa although there has recently been a worrying increase in cases in Australia’s state of Victoria [13]. The disease burden is difficult to objectively assess in many endemic countries (especially those that are lower-middle-income countries or least developed countries) due to the remote location of affected communities and lack of credible health system data [5] (Fig. 5.1).
Evidence consensus for Buruli ulcer presence and absence worldwide. These findings were based on a comprehensive systematic review of peer-reviewed evidence in the scientific literature as well as surveillance and laboratory data from country programmes. (From Simpson et al. [5])
The exact mode of transmission of M. ulcerans is unknown; however it seems almost certain that this opportunistic environmental pathogen enters the body by mechanical transfer. No incidences of person-to-person transmission have been reported, with the notable exception of a case involving a human bite [14]. Cases linked to other types of minor trauma, such as abrasions and even snake bite [15, 16], suggest that skin surface contamination may be important. Insects have been implicated in both Australia and West Africa, but this topic remains controversial and may vary between different environments (recently reviewed in [17,18,19]).
1.2 Clinical Presentations and Current Treatments
BU presents clinically as painless skin lesion(s) in one of five forms, nodule, papule, plaque or oedema and ulcers (Fig. 5.2), and, in some cases, bone involvement can result in osteomyelitis [20]. Nodules/papules are the first sign of (localised) infection, and the WHO has categorised more advanced lesions according to severity, with Category I including single small ulcers <5 cm diameter; Category II including larger ulcers of 5–15 cm, as well as plaques and oedema; and Category III including large ulcers >15 cm, multiple ulcers or ulcers that have spread to include particularly sensitive sites such as the eyes, bones, joints or genitals [20]. The more serious manifestations are much more common in African countries than Australia, most likely due to differences in health infrastructure.
Clinical presentations of Buruli ulcer. BU can present clinically through a spectrum including a papule or nodule a painless palpable lump under the skin; (a) or plaque an area of tough necrotic skin which can be of any size, but the epidermis remains intact; (b), which can also be found with or without oedema (c). If the epidermis breaks down, ulcers of varying sizes can form, but due to the characteristic undermined edges (d), the true lesion size is often much larger than the ulcerated region. Images by kind courtesy of Prof Richard Phillips. (Kumasi Centre for Collaborative Research, Ghana)
Hence, the most common presentation of BU is a necrotising skin ulcer [1, 20]. Typically, the edges of these ulcers are ‘undermined’ due to subcutaneous necrosis, meaning that ulcers are frequently larger than the area of dermal breakdown. Remarkably, given the extensive tissue loss that can occur, BU patients are usually otherwise well, rarely experiencing the severe pain that might be expected based on the physical appearance of the lesions.
Until 2004, the only medical intervention available was radical surgery, either in the form of wide excision and debridement some 10 cm beyond the extent of affected tissue, or even limb amputation [21]. Although M. ulcerans was known to be sensitive to a range of antimycobacterial antibiotics from an early stage [22,23,24,25], a key success of the WHO GBUI was the testing [26] and introduction [20] of effective antibiotic regimens. Initially, a combination of rifampicin and streptomycin (for 8 weeks) was used [27,28,29]. To tackle the poor compliance and ototoxicity from injectable streptomycin [30], this is now transitioning to an all-oral combination including clarithromycin [31]. While antibiotic therapy can cause so-called paradoxical reactions, where lesions can appear to worsen or appear in new locations, this should not be confused as treatment failure [1, 32]. Fortunately, antimicrobial resistance has not yet been reported in Buruli ulcer, which supports its classification as an opportunistic environmental pathogen and argues against ‘re-seeding’ of environmental niches from patient lesions.
Since antibiotics were introduced, there has been a significant reduction in surgical intervention for BU [33, 34]. Indeed, antibiotic treatment of BU at an early nodule/papule stage can result in healing before ulceration [35]. Therefore, surgery is now usually reserved for patients with severe disease [36], although clinical decision-making varies from clinic to clinic [37]. With or without surgery, BU comes with a high burden of disability and deformity due to the extensive tissue damage caused and the risk of contractures [20]. Careful wound management and physiotherapy are critical to minimise these risks. Consequently, improved diagnostic tools and public health measures aimed at early detection of BU are now a key goal of the WHO.
2 Mycobacterium ulcerans
The closest genetic relative of M. ulcerans is M. marinum, another pathogenic mycobacterium that causes ‘fish tank granuloma’, to which its genome is 98% identical [38, 39]. Despite this phylogenetic similarity, major changes in the M. ulcerans genome have altered its interaction with the host [38, 39]. First, ‘reductive evolution’ has occurred with pseudogene accumulation and gene deletion due to the accumulation of single nucleotide polymorphisms (SNPs). Second, two different insertion sequences (IS2404 and IS2606 [40]) have proliferated throughout the genome leading to disruption and loss of virulence regions. These include the well-characterised Early Secreted Antigenic Target 6 kDa (ESAT-6) secretion system 1 (ESX-1) that allows other mycobacteria to escape the phagosome [41, 42]. Third, it has acquired a plasmid, pMUM, which carries the only virulence genes identified to date [43]. These genes encode the polyketide synthases and accessory proteins that manufacture mycolactone. Notably, there are two lineages of M. ulcerans, which may explain some of the divergence between findings in Africa and Australia [44], including subtle differences in mycolactone structure and function [45].
2.1 Mycolactone
The identification of mycolactone [46], and the subsequent understanding of its effects on host cells and tissues, has been critical to the understanding of BU pathogenesis [47]. Mycolactone is a lipid-like molecule with a 12-membered lactone ring that can vary in the hydroxylation and methylation pattern on the longer polyketide side chain. The most potent congener found in most African strains is known as mycolactone A/B (Fig. 5.3a). Purified mycolactone can replicate the ulceration caused by M. ulcerans [46, 49], and strains that cannot produce it lose their virulence [50]. To date, the best characterised consequences of mycolactone exposure are cytopathic/cytotoxic effects and immune suppression, although vascular dysfunction has also recently been described [51, 52]. All of these have now been shown to be dependent on activity of mycolactone against the normal function of the Sec61 translocon [53,54,55,56,57], which is the main entry point to the canonical secretory pathway of secreted proteins, type I and type II transmembrane proteins and multi-pass membrane proteins [58, 59] (Fig. 5.3b). Indeed, the structure of mycolactone bound to Sec61 has recently been solved (Fig. 5.3c) [57].
Structure and function of mycolactone, the M. ulcerans virulence exotoxin. (a) The chemical structure of mycolactone. (b) Sec61-dependent co-translational translocation of proteins into the ER involves recognition of a signal peptide or signal anchor by the signal recognition particle and its receptor (not shown), which transfers it to Sec61. This results in reorganization of the translocon and movement of the Sec61α plug domain, opening the central pore and allowing transit of the translating protein into the ER. Mycolactone binds Sec61α, preventing the signal peptide from accessing its binding site at the lateral gate. Although the lateral gate is open, the plug remains closed, and the translocon is locked in an inactive state. (c) The structure of inhibited Sec61, with mycolactone bound inside the lateral gate of Sec61α. Dark purple, Sec61α; light purple, Sec61β; pink. Sec61γ; yellow/red, mycolactone (from PDB:6Z3T). Two views are shown, looking down from the cytosol towards the ER and from the side, as in (a). (Adapted from [48])
Mycolactone has a cytopathic effect on cultured mammalian cells characterized by cytoskeletal rearrangement, followed by rounding up and detachment from tissue culture plates [50, 60, 61]. It is also cytotoxic and induces apoptosis several days after exposure [50, 62,63,64] as well as cell cycle arrest in G0/G1 phase [46, 65]. We now know that the pathway to apoptosis involves changes in intracellular Ca2+ gradients [66, 67], the so-called integrated stress response [64, 68], and autophagy [69]. Cells carrying mutations in the gene encoding the major Sec61 subunit, Sec61α, are highly resistant to the cytopathic and cytotoxic effects of mycolactone and can proliferate in its presence [54, 57, 64, 67].
Mycolactone’s immunosuppressive effects are wide-ranging, which is unsurprising considering its inhibition of Sec61 and the consequent loss of secretory proteins (most cytokines and chemokines) and receptors (constitutive and induced), which normally act in elegant concert to mediate both innate and adaptive immune responses [48, 70]. Mycolactone has been shown to strongly suppress innate immunity by limiting phagocytosis [71] and inflammatory responses by monocytes, macrophages and dendritic cells [53, 71,72,73,74]. It limits adaptive immunity by suppressing both antigen presentation by dendritic cells and T cell activation [75,76,77]. Specific evidence demonstrated Sec61-dependent effects on TNF, IL-6 and Cox-2 production, antigen processing mediated by invariant chain during MHC class II processing and T cell activation [53, 54, 78]. A notable exception here is the recent discovery that mycolactone can induce the production of the cytokine IL-1β, by acting as the ‘second signal’ during inflammasome activation [48, 79]. This observation is entirely in line with Sec61 inhibition by mycolactone, since IL-1β does not use the canonical secretory pathway for its production.
Yet, there are no drugs described that can counteract the effect of mycolactone on the Sec61 translocon. Indeed, other inhibitors of Sec61 recapitulate the effects of mycolactone [80, 81] (R Simmonds, unpublished observation), and so this is not a viable treatment option. However, inhibitors of apoptosis such as Z-VAD-FMK, or genetic deletion of Bim, are able to at least delay cytotoxicity, both in vitro and in vivo [63, 82].
2.2 Immune Response to M. ulcerans Infection
The immunosuppressive properties of mycolactone described above are thought to explain the histopathology of BU lesions. Here, the lesions display coagulative necrosis, with clusters of extracellular acid-fast bacilli visible at the base of the subcutaneous tissue, and epidermal hyperplasia [3]. The cellular infiltrate of immune cells, normally expected in a microbial infection, is reduced and limited to the periphery of the lesion. In their elegant work, Ruf and Pluschke have shown that, in both humans and pigs, the infiltrating leukocytes are restricted to a ‘belt’ outside the necrotic core of the early ulcerative lesions [83, 84]. This contains T cells, CD68-positive macrophages and neutrophils, as well as clusters of B cells [83]. However, the immune cells are not able to access the necrotic core containing M. ulcerans, which contains neutrophilic debris and stains strongly and diffusely for apoptotic markers [83, 84]. Notably this picture changes remarkably during antibiotic therapy [85,86,87], which is presumed to be a result of a drop in mycolactone production.
Despite this, there is considerable evidence that both human and animal hosts can mount an immune response to M. ulcerans [88]. Critically, spontaneous recovery from BU without treatment reported in both humans [89,90,91,92] and animal models [93, 94] shows that the immune system can contain the infection in some circumstances. Both T cell [95,96,97,98,99] and serological [100,101,102] responses to M. ulcerans antigens have been demonstrated in the blood of BU patients. Moreover, their household contacts also display similar responses although they had never experienced clinical disease [100, 102,103,104]. Experimentally, IFN-γ protects against M. ulcerans infection in mice [105], and similarly a human genome SNP in the IFNG gene increases susceptibility to BU [106]. Such genetic studies in BU patients have identified a range of disease-modifying SNPs in genes involved in the cellular response to infection, including iNOS, the inducible nitric oxide synthase that generates bactericidal NO in macrophages [106]. Although the intra-macrophage stage of M. ulcerans infection is thought to be transient [71], SNPs in genes involved in this response also impact BU, including in PARK2, NOD2 and ATG16L1 [106,107,108].
3 Vaccine Candidates
Notwithstanding the obvious serious sequelae of infection, the motivation for a BU vaccine also encompasses the origins of the infection from the environment. It is now clear that there are certain environments where M. ulcerans is highly prevalent, especially those disturbed by human activity, such as mining or agricultural land use [109, 110]. Unfortunately those living in such environments are at high risk of developing BU [111], even if they adhere to risk-reducing guidance [112,113,114,115]. Therefore, a vaccine may be the only realistic hope of BU eradication.
Although studies aimed at developing a vaccine against M. ulcerans infection date back to the 1950s and the work of the Australian microbiologist Frank Fenner [116, 117] (https://www.science.org.au/learning/general-audience/history/interviews-australian-scientists/professor-frank-fenner), there is still currently no effective vaccine that provides long-term protection from BU [118]. Early attention focussed on the Bacillus Calmette-Guérin (BCG) strain of M. bovis that is primarily known as the vaccine for M. tuberculosis [119]. Indeed, most countries endemic for BU have a current national BCG vaccination policy for all citizens (www.bcgatlas.org), although Australia now only vaccinates special groups.
3.1 Human Studies with BCG
In two early randomised controlled trials using BCG in Uganda, there was evidence that BCG did confer some protection against BU even though this was thought to be short-lived [120, 121]. However, it should be noted that these studies were confounded by many factors. For example, in the first randomised trial with Rwandan refugees [120], participants were selected based on their tuberculin skin test (TST) negativity, which ruled out TB and latent TB infection, but almost certainly included both BCG-vaccinated and unvaccinated individuals (as TST in response to BCG wanes dramatically over time [122]). Moreover, this trial could not be fully completed, as the participants were lost to follow-up due to relocation of refugees. The second [121] was more successful in that the trial aims were fully achieved, but the outcomes were similar, in that partial and short-term protection was observed. Thus, an overall efficacy of BCG vaccination of 47% was reported, which declined sharply after 12 months, and was also notably highly variable depending on the immune status of participants on the outset. In that study, included participants had a broad spectrum of immune status, including those with known previous BU disease, presence or absence of BCG scar and even individuals with latent TB infection [121].
Since then, multiple other clinical studies found no evidence that BCG confers any long-term protection. For example, an observational study by Phillips et al. [123] found no association between BCG (presence of scar) and BU disease incidence amongst participants recruited from Congo, Ghana and Togo, replicating results from Benin [124]. For further reading on these studies, we refer the readers to two excellent recent reviews on the subject [125, 126].
The poor efficacy of BCG from these human studies is most likely due to insufficient immune cross-reactivity with M. ulcerans and suboptimal performance of BCG in countries with high exposure to non-tuberculous mycobacteria (NTM). In the case of cross-protection, this is likely the result of the divergent pathophysiologies of the infections they cause despite a high degree of genetic homology between different mycobacterial species. Thus, similarly to M. ulcerans, BCG vaccine offers only partial protection against M. leprae in human clinical trials [127, 128]. Furthermore, while multiple other environmental and non-environmental factors are undoubtedly involved, it is well known that BCG efficacy against TB is drastically reduced in geographical settings with high burden of non-pathogenic mycobacteria due to immunological interference (reviewed in [129]). In other words, the reasons for failure of BCG to impart better, longer-lasting protection against BU disease may be the same as those that also undermine its efficacy against TB.
3.2 Mouse Studies of BU Vaccine Candidates
Development of BU vaccines that offer improved protection over BCG has frequently involved in vivo models of M. ulcerans infection [130]. The mouse hind footpad model of M. ulcerans infection was originally developed by Fenner [116] and continually refined over many decades, predominantly in the BALB/c and C57BL/6 strains of mice. Today, it is the gold standard for studying treatment interventions and new vaccine candidates against BU disease. M. ulcerans bacteria are injected subcutaneously into the footpad, and (depending on the injected dose and mouse strain) the initial signs of swelling may appear over the metatarsal area approximately 2–5 weeks later. If untreated, the swelling progresses and then extends into the leg, finally leading to onset of ulceration. These stages of experimental pathogenesis of M. ulcerans infection in mouse footpads can be graded according to their physical appearance, according to a process originally proposed by Stanford [23] and later refined by Converse [34] in line with modern animal welfare legislation (Fig. 5.4). This allows for experimental humane points to be achieved without causing undue suffering to animals, usually before the point of ulceration. Notably, the analgesic effects of mycolactone [131, 132] mean that the animals do not experience inflammatory, hypoxic or tissue pressure pain even at the more severe grades. Objective measures of the intervention can also be taken in terms of physical parameters (footpad diameter), enumeration of bacteria in footpad via either culturable bacilli or quantification of bacterial DNA and measurement of inflammatory markers in blood or tissue.
Pathogenesis after subcutaneous M. ulcerans injection in the mouse (BALB/c) footpad. Subcutaneous (s.c.) injection of M. ulcerans into the healthy mouse footpad (0) leads to progressive swelling and inflammation. (1) Grade 1, slight swelling; (2 and 2+) Grade 2, swelling with inflammation; (3 and 3+) Grade 3, swelling with inflammation of the leg; (4) Grade 4, swelling with inflammation and possible ulceration [130]. For most vaccine studies, the human endpoint is when cage bedding is observed sticking to the sole of the foot, indicating ulceration. Despite the dramatic appearance, the analgesic effects of mycolactone mean that the mice do not display signs of pain nor lose mobility
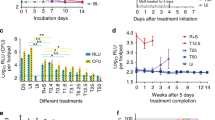
An alternative model involving subcutaneous injection of M. ulcerans into the central portion of the tail has also been described [71]. The main outcome measure here was time to ulceration in days (60–70 days in unvaccinated C57BL/6 and BALB/c mice, respectively) [133, 134]. A low-dose infection model using a recombinant bioluminescent strain of M. ulcerans allowing for bacteria enumeration in live animals [135, 136] has also been used [137].
Here, we have categorised the various vaccine candidates tested in mice under two broad arms: whole bacteria and subunit vaccines, including those based on mycolactone (Table 5.1). Despite its lack of efficacy in human clinical trials, BCG has proven useful as a baseline to compare the efficacy of other vaccine candidates (recently reviewed in [125, 126]), as it provides short-lived but measurable protection against mouse footpad infections. This has been reproducible since Fenner’s first attempts at a vaccine in the 1950s [116, 117] and is seen even when BCG booster approaches are used [148]. These studies showed that vaccine-mediated protection from M. ulcerans infection may be Th1-mediated, via sustained levels of IFN-γ and TNF and the absence of IL-4, IL-10 and IL-17 [139].
3.2.1 Whole Bacteria Vaccines
In concert with the earliest BCG studies in mice, several reports have attempted to use M. marinum as a vaccine against M. ulcerans infection. Early attempts showed increased efficacy over BCG, but these were also still short-lived and waned with time [116, 117]. More recently, there has been some interest in overexpressing antigens in BCG and M. marinum and using these recombinant strains as whole bacteria vaccines. By this design, M. ulcerans-specific antigens were presented in a vaccine which lacked the virulent and immunomodulatory potential of mycolactone. These studies have focused on antigens that are known to be immunodominant in M. tuberculosis including EsxH, the M. ulcerans ortholog of M. tuberculosis TB10.4 antigen and proteins of the Ag85 complex. The latter is made up of Ag85A, Ag85B and Ag85C and is known to be secreted from BCG and to elicit strong Th1 responses [149]. Each of these 30–32 kDa proteins is highly conserved between different species of mycobacteria, being involved in the synthesis of cord factor and the organisation of mycolic acids in the bacterial cell wall. Notably Ag85A induced measurable, but relatively weak, IFN-γ responses during whole blood restimulations of BU patients and their household contacts [103].
Hart et al. [142] used recombinant M. marinum expressing M. ulcerans Ag85A (MU-Ag85A). Although this did not seem to delay the onset of ulceration (the experimental endpoint), it did significantly reduce the bacterial load of the challenged footpads. Hart et al. applied this same technology to generate BCG expressing M. ulcerans Ag85B with and without a fusion with EsxH. Mice challenged with M. ulcerans following a single subcutaneous vaccination with BCG MU-Ag85B-EsxH [144] or BCG MU-Ag85B [143] displayed significantly less bacterial burden at 6 and 12 weeks post-infection, reduced histopathological tissue damage and significantly delayed (but not prevented) onset in ulceration compared to vaccination with BCG.
Others have attempted vaccines using various doses and strains of M. ulcerans itself. Once again, Fenner paved the way and found that low, but not high, doses of M. ulcerans (1615E) provided protection against footpad infections [117]. Though not explained, this may have been due to the immunomodulatory action of mycolactone. In an attempt to bypass this, Fraga et al. [139] used a mycolactone-deficient strain of M. ulcerans (5114) that had lost the MUP038 gene involved in mycolactone biosynthesis [150]. This strain delayed the onset of footpad swelling post-challenge similarly to BCG. Finally, an interesting approach was taken by Watanabe et al. [138], who inactivated and dewaxed M. ulcerans by organic solvent treatments, prior to using it as a vaccine in mice. This candidate conferred complete protection against swelling at 28 days post-challenge, though the authors did not investigate if this protection was long-lasting.
3.2.2 Subunit Vaccines for BU
An alternative approach has been the use of acellular/subunit vaccines formulated with adjuvants and delivered as proteins or DNA. Tanghe et al. [140] demonstrated that a DNA vaccine based on BCG-Ag85A was able to confer partial protection (like BCG) against M. ulcerans infection in mice, as measured by reduced bacterial load. This was further improved on with MU-Ag85A, particularly when used as a DNA-prime protein-boost regimen, with a 100-fold reduction of bacterial load compared to unvaccinated mice [141]. These experiments also demonstrated that the protective immune responses were localised and Th1-mediated, with strong roles for IL-2 and IFN-γ. However, while this vaccine delayed the onset of footpad ulceration, it was less effective than BCG, a finding later replicated by Roupie et al. [147].
Other immunodominant antigens of M. ulcerans that have been investigated as vaccine candidates include MUL_2232 (also known as Hsp18, homologous to an immunodominant cell wall antigen of M. leprae that is reactive with the sera of patients with BU [100]) and MUL_3720 (a highly expressed 21 kDa protein with unknown function [151, 152]). However, despite their strong induction of IgG antibodies, they failed to provide any protection in either the footpad or tail infection models [133, 145]. No further improvement was reported when vesicular stomatitis virus-based RNA replicon particles encoding these proteins were used [146]. Prior to this, Coutanceau et al. [134] had tried a DNA vaccine using M. leprae Hsp65 antigen, but this did not confer any protection despite inducing strong IgG antibody responses. These studies give credence to the thinking that T cell responses, rather than antibodies, may have a more significant role in M. ulcerans immunity.
Moreover, different domains of the three large mycolactone polyketide synthases mlsA1, mlsA2 and mlsB encoded by pMUM001 and found associated with the M. ulcerans cell wall [150] have been investigated as vaccine candidates. These included the acyl carrier protein type 1, 2 and 3 (ACP-1, ACP-2 and ACP-3), type 1 and type 2 acyltransferases (acetate) (ATac-1 and ATac-2), acyltransferase (propionate) (ATp), enoylreductase (ER), ketoreductase A (KR-A) and the load module ketosynthase domain (KS). Many of these domains have been shown to induce humoral or cellular responses, supporting their immunogenicity. Of these, ER, ATp and KR-A have been shown to discriminate serological responses between BU patients and controls in non-endemic regions [102]. Other domains, particularly ER and KS, were able to successfully induce IFN-γ and IL-5 during whole blood restimulations of BU patients and their household contacts [103].
Unfortunately, vaccine trials using this strategy have been disappointing. Roupie et al. [147] used a DNA prime/protein boost protocol and found that the antibody and cellular (IL-2 and IFN-γ) immune responses to these antigens varied, with ATp providing the strongest response amongst the nine domains in line with, or better than, the MU-Ag85A control. However, this did not significantly extend the time for mice to display 4 mm footpad swelling or reduce bacterial numbers in infected feet. More recently, an approach that involved electrostatically coupling the ER domain to the Toll-Like receptor 2 (TLR-2) agonist adjuvant R4Pam2Cys was tested [137]. In this low-dose challenge tail model, this vaccine provided reduced protection compared to BCG and was associated with ER-specific serum IgG titres and IL-2/IL-4 in the draining lymph nodes.
With limited success so far with both whole bacteria and subunit protein candidates, it has been postulated that a vaccine design based on mycolactone could provide the much sought-after protection against BU. Evidence that such a toxin-blocking vaccine might be fruitful comes from the successful generation of mycolactone-neutralising antibodies using a truncated and non-cytotoxic mycolactone derivative. This compound (PG-203) lacking the so-called ‘Southern’ chain and conjugated to BSA via a diethylene glycol-based linker, it elicited protein-based immune responses as determined by ELISA and other neutralisation assays [153]. The vaccine potential of mycolactone has also been demonstrated using in vitro display methods comprising both phage and yeast [154].
4 Prospects
So, what are the prospects of a BU vaccine in the future? Based on the available evidence with BCG, a BU-specific vaccine is needed. While none of the promising preclinical candidates described here fully meet the criteria to be advanced to human studies, these partial successes strongly suggest that, with further improvements, such a vaccine may yet be achievable.
To that end, we would like to conclude this review with a preliminary report from our own attempts of developing a subunit-based vaccine against BU. Using our expertise from BCG-boost subunit vaccines studies for TB [155,156,157], we have recently developed several formulations that were tested in the mouse footpad model of M. ulcerans infection. These formulations contain individual or combinations of M. ulcerans antigens, as well as mycolactone itself, mixed with different types of adjuvants and delivery systems. While the data are yet to be published, we were very encouraged to observe that one of these formulations, which we have termed ‘BuruliVac’, was particularly effective in preventing swelling and ulceration of the mouse footpad and completely prevented footpad swelling in all experimental animals. This was corroborated by absence of C-reactive protein and other inflammatory markers in the tissue (Boakye-Appiah and Reljic, unpublished).
These ongoing proof-of-principle vaccine studies demonstrate that it is feasible to prevent M. ulcerans infection in this experimental model and that future efforts should be concentrated on further optimising and advancing such second-generation vaccine candidates against BU. Recent developments in vaccination strategies that allow specific targeting of skin resident memory T cells may be of value here [158]. However, it should also be noted that unlike BCG, a new BU-specific vaccine will come with a significant caveat, in that its clinical development and eventual licensure will depend on it being able to attract sufficient interest from pharmaceutical industry. BU, despite being the most significant mycobacterial disease after TB and leprosy, is an NTD that affects a relatively small proportion of population, mostly in the endemic areas in Western Africa. Vaccine development is an extremely costly undertaking for the pharmaceutical industry, amounting to hundreds of millions of US dollars. This investment can only be recouped by selling enough doses and over a prolonged period. The battle to develop a BU vaccine will therefore be fought on two separate fronts, in research laboratories and in the commercial arena. We, the scientific community, have the responsibility to ensure that if it comes to that second battle, we have something to fight with, a vaccine that has a real chance to eradicate the terrible affliction that is BU.
References
Yotsu RR, Suzuki K, Simmonds RE, Bedimo R, Ablordey A, Yeboah-Manu D, et al. Buruli ulcer: a review of the current knowledge. Curr Trop Med Rep. 2018;5(4):247–56.
Garchitorena A, Ngonghala CN, Guegan JF, Texier G, Bellanger M, Bonds M, et al. Economic inequality caused by feedbacks between poverty and the dynamics of a rare tropical disease: the case of Buruli ulcer in sub-Saharan Africa. Proc Biol Sci. 1818;2015(282):20151426.
WHO W. Laboratory diagnosis of Buruli ulcer; a manual for healthcare providers. Geneva: WHO; 2014.
Röltgen K, Pluschke G. Epidemiology and disease burden of Buruli ulcer: a review. Res Rep Trop Med. 2015;6:59–73.
Simpson H, Deribe K, Tabah EN, Peters A, Maman I, Frimpong M, et al. Mapping the global distribution of Buruli ulcer: a systematic review with evidence consensus. Lancet Glob Health. 2019;7(7):e912–e22.
Stienstra Y, van der Graaf WT, Asamoa K, van der Werf TS. Beliefs and attitudes toward Buruli ulcer in Ghana. Am J Trop Med Hyg. 2002;67(2):207–13.
Amoakoh HB, Aikins M. Household cost of out-patient treatment of Buruli ulcer in Ghana: a case study of Obom in Ga south municipality. BMC Health Serv Res. 2013;13:507.
Grietens KP, Boock AU, Peeters H, Hausmann-Muela S, Toomer E, Ribera JM. “It is me who endures but my family that suffers”: social isolation as a consequence of the household cost burden of Buruli ulcer free of charge hospital treatment. PLoS Negl Trop Dis. 2008;2(10):e321.
Amoako YA, Ackam N, Omuojine JP, Oppong MN, Owusu-Ansah AG, Abass MK, et al. Caregiver burden in Buruli ulcer disease: evidence from Ghana. PLoS Negl Trop Dis. 2021;15(6):e0009454.
Hay RJ, Asiedu K. Skin-related neglected tropical diseases (skin NTDs)-a new challenge. Trop Med Infect Dis. 2018;4(1):4.
Chany AC, Tresse C, Casarotto V, Blanchard N. History, biology and chemistry of Mycobacterium ulcerans infections (Buruli ulcer disease). Nat Prod Rep. 2013;30(12):1527–67.
MacCallum P, Tolhurst JC, Buckle G, Sissons HA. A new mycobacterial infection in man. J Pathol Bacteriol. 1948;60(1):93–122.
Johnson PDR. Buruli ulcer in Australia. In: Pluschke G, Roltgen K, editors. Buruli ulcer: Mycobacterium ulcerans disease. Cham: Springer; 2019. p. 61–76.
Debacker M, Zinsou C, Aguiar J, Meyers W, Portaels F. Mycobacterium ulcerans disease (Buruli ulcer) following human bite. Lancet. 2002;360(9348):1830.
Hofer M, Hirschel B, Kirschner P, Beghetti M, Kaelin A, Siegrist CA, et al. Brief report: disseminated osteomyelitis from Mycobacterium ulcerans after a snakebite. N Engl J Med. 1993;328(14):1007–9.
Meyers WM, Shelly WM, Connor DH, Meyers EK. Human Mycobacterium ulcerans infections developing at sites of trauma to skin. Am J Trop Med Hyg. 1974;23(5):919–23.
Dhungel L, Benbow ME, Jordan HR. Linking the Mycobacterium ulcerans environment to Buruli ulcer disease: progress and challenges. One Health. 2021;13:100311.
Receveur JP, Bauer A, Pechal JL, Picq S, Dogbe M, Jordan HR, et al. A need for null models in understanding disease transmission: the example of Mycobacterium ulcerans (Buruli ulcer disease). FEMS Microbiol Rev. 2021;46(1):fuab045.
Muleta AJ, Lappan R, Stinear TP, Greening C. Understanding the transmission of Mycobacterium ulcerans: a step towards controlling Buruli ulcer. PLoS Negl Trop Dis. 2021;15(8):e0009678.
WHO W. Treatment of Mycobacterium ulcerans disease (Buruli ulcer); guidance for health workers. Geneva: Wold Health Organisation; 2012.
Portaels F, Silva MT, Meyers WM. Buruli ulcer. Clin Dermatol. 2009;27(3):291–305.
Havel A, Pattyn SR. Activity of rifampicin on Mycobacterium ulcerans. Ann Soc Belg Med Trop. 1975;55(2):105–8.
Stanford JL, Phillips I. Rifampicin in experimental Mycobacterium ulcerans infection. J Med Microbiol. 1972;5(1):39–45.
Thangaraj HS, Adjei O, Allen BW, Portaels F, Evans MR, Banerjee DK, et al. In vitro activity of ciprofloxacin, sparfloxacin, ofloxacin, amikacin and rifampicin against Ghanaian isolates of Mycobacterium ulcerans. J Antimicrob Chemother. 2000;45(2):231–3.
Portaels F, Traore H, De Ridder K, Meyers WM. In vitro susceptibility of Mycobacterium ulcerans to clarithromycin. Antimicrob Agents Chemother. 1998;42(8):2070–3.
Dega H, Robert J, Bonnafous P, Jarlier V, Grosset J. Activities of several antimicrobials against Mycobacterium ulcerans infection in mice. Antimicrob Agents Chemother. 2000;44(9):2367–72.
Etuaful S, Carbonnelle B, Grosset J, Lucas S, Horsfield C, Phillips R, et al. Efficacy of the combination rifampin-streptomycin in preventing growth of Mycobacterium ulcerans in early lesions of Buruli ulcer in humans. Antimicrob Agents Chemother. 2005;49(8):3182–6.
Chauty A, Ardant MF, Adeye A, Euverte H, Guedenon A, Johnson C, et al. Promising clinical efficacy of streptomycin-rifampin combination for treatment of buruli ulcer (Mycobacterium ulcerans disease). Antimicrob Agents Chemother. 2007;51(11):4029–35.
Sarfo FS, Phillips R, Asiedu K, Ampadu E, Bobi N, Adentwe E, et al. Clinical efficacy of combination of rifampin and streptomycin for treatment of Mycobacterium ulcerans disease. Antimicrob Agents Chemother. 2010;54(9):3678–85.
Klis S, Stienstra Y, Phillips RO, Abass KM, Tuah W, van der Werf TS. Long term streptomycin toxicity in the treatment of Buruli ulcer: follow-up of participants in the BURULICO drug trial. PLoS Negl Trop Dis. 2014;8(3):e2739.
Phillips RO, Robert J, Abass KM, Thompson W, Sarfo FS, Wilson T, et al. Rifampicin and clarithromycin (extended release) versus rifampicin and streptomycin for limited Buruli ulcer lesions: a randomised, open-label, non-inferiority phase 3 trial. Lancet. 2020;395(10232):1259–67.
O'Brien DP, Robson ME, Callan PP, McDonald AH. “Paradoxical” immune-mediated reactions to Mycobacterium ulcerans during antibiotic treatment: a result of treatment success, not failure. Med J Aust. 2009;191(10):564–6.
WHO W. Provisional guidance on the role of specific antibiotics in the management of Mycobacterium ulcerans disease (Buruli ulcer). Geneva: WHO; 2008.
Converse PJ, Nuermberger EL, Almeida DV, Grosset JH. Treating Mycobacterium ulcerans disease (Buruli ulcer): from surgery to antibiotics, is the pill mightier than the knife? Future Microbiol. 2011;6(10):1185–98.
Klis S, Ranchor A, Phillips RO, Abass KM, Tuah W, Loth S, et al. Good quality of life in former Buruli ulcer patients with small lesions: long-term follow-up of the BURULICO trial. PLoS Negl Trop Dis. 2014;8(7):e2964.
Degboe B, Sopoh GE, Alimi M, Koudoukpo C, Akpadjan F, Agbéssi N, et al. Buruli ulcer: evaluation of its medical and surgical management at the Allada (Benin) screening and treatment Center, 2010-2014. Med Sante Trop. 2019;29(4):402–8.
Wadagni AC, Steinhorst J, Barogui YT, Catraye PM, Gnimavo R, Abass KM, et al. Buruli ulcer treatment: rate of surgical intervention differs highly between treatment centers in West Africa. PLoS Negl Trop Dis. 2019;13(10):e0007866.
Stinear TP, Seemann T, Pidot S, Frigui W, Reysset G, Garnier T, et al. Reductive evolution and niche adaptation inferred from the genome of Mycobacterium ulcerans, the causative agent of Buruli ulcer. Genome Res. 2007;17(2):192–200.
Demangel C, Stinear TP, Cole ST. Buruli ulcer: reductive evolution enhances pathogenicity of Mycobacterium ulcerans. Nat Rev Microbiol. 2009;7(1):50–60.
Stinear T, Ross BC, Davies JK, Marino L, Robins-Browne RM, Oppedisano F, et al. Identification and characterization of IS2404 and IS2606: two distinct repeated sequences for detection of Mycobacterium ulcerans by PCR. J Clin Microbiol. 1999;37(4):1018–23.
Hsu T, Hingley-Wilson SM, Chen B, Chen M, Dai AZ, Morin PM, et al. The primary mechanism of attenuation of bacillus Calmette-Guerin is a loss of secreted lytic function required for invasion of lung interstitial tissue. Proc Natl Acad Sci U S A. 2003;100(21):12420–5.
Tiwari S, Casey R, Goulding CW, Hingley-Wilson S, Jacobs WR, Jr. Infect and inject: how Mycobacterium tuberculosis exploits its major virulence-associated type VII secretion system, ESX-1. Microbiol Spectr. 2019;7(3).
Stinear TP, Mve-Obiang A, Small PL, Frigui W, Pryor MJ, Brosch R, et al. Giant plasmid-encoded polyketide synthases produce the macrolide toxin of Mycobacterium ulcerans. Proc Natl Acad Sci U S A. 2004;101(5):1345–9.
Doig KD, Holt KE, Fyfe JA, Lavender CJ, Eddyani M, Portaels F, et al. On the origin of Mycobacterium ulcerans, the causative agent of Buruli ulcer. BMC Genomics. 2012;13:258.
Kishi Y. Chemistry of mycolactones, the causative toxins of Buruli ulcer. Proc Natl Acad Sci U S A. 2011;108(17):6703–8.
George KM, Chatterjee D, Gunawardana G, Welty D, Hayman J, Lee R, et al. Mycolactone: a polyketide toxin from Mycobacterium ulcerans required for virulence. Science. 1999;283(5403):854–7.
Sarfo FS, Phillips R, Wansbrough-Jones M, Simmonds RE. Recent advances: role of mycolactone in the pathogenesis and monitoring of Mycobacterium ulcerans infection/Buruli ulcer disease. Cell Microbiol. 2016;18(1):17–29.
Hall BS, Hsieh LTH, Sacre S, Simmonds RE. The one that got away: how macrophage-derived IL-1 beta escapes the mycolactone-dependent Sec61 blockade in Buruli ulcer. Front Immunol. 2022;22:788146.
Adusumilli S, Mve-Obiang A, Sparer T, Meyers W, Hayman J, Small PL. Mycobacterium ulcerans toxic macrolide, mycolactone modulates the host immune response and cellular location of M. ulcerans in vitro and in vivo. Cell Microbiol. 2005;7(9):1295–304.
George KM, Pascopella L, Welty DM, Small PL. A Mycobacterium ulcerans toxin, mycolactone, causes apoptosis in guinea pig ulcers and tissue culture cells. Infect Immun. 2000;68(2):877–83.
Ogbechi J, Ruf MT, Hall BS, Bodman-Smith K, Vogel M, Wu HL, et al. Mycolactone-dependent depletion of endothelial cell thrombomodulin is strongly associated with fibrin deposition in Buruli ulcer lesions. PLoS Pathog. 2015;11:e1005011.
Hsieh LT, Dos Santos SJ, Hall BS, Ogbechi J, Loglo AD, Salguero FJ, et al. Aberrant stromal tissue factor localisation and mycolactone-driven vascular dysfunction, exacerbated by IL-1β, are linked to fibrin formation in Buruli ulcer lesions. PLoS Pathog. 2022;18(1):e1010280.
Hall BS, Hill K, McKenna M, Ogbechi J, High S, Willis AE, et al. The pathogenic mechanism of the Mycobacterium ulcerans virulence factor, mycolactone, depends on blockade of protein translocation into the ER. PLoS Pathog. 2014;10(4):e1004061.
Baron L, Paatero AO, Morel JD, Impens F, Guenin-Mace L, Saint-Auret S, et al. Mycolactone subverts immunity by selectively blocking the Sec61 translocon. J Exp Med. 2016;213(13):2885–96.
McKenna M, Simmonds RE, High S. Mechanistic insights into the inhibition of Sec61-dependent co- and post-translational translocation by mycolactone. J Cell Sci. 2016;129(7):1404–5.
McKenna M, Simmonds RE, High S. Mycolactone reveals the substrate-driven complexity of Sec61-dependent transmembrane protein biogenesis. J Cell Sci. 2017;130(7):1307–20.
Gérard SF, Hall BS, Zaki AM, Corfield KA, Mayerhofer PU, Costa C, et al. Structure of the inhibited state of the sec translocon. Mol Cell. 2020;79(3):406–15.e7.
Voorhees RM, Hegde RS. Toward a structural understanding of co-translational protein translocation. Curr Opin Cell Biol. 2016;41:91–9.
Zimmermann R, Eyrisch S, Ahmad M, Helms V. Protein translocation across the ER membrane. Biochim Biophys Acta. 2011;1808(3):912–24.
Guenin-Mace L, Veyron-Churlet R, Thoulouze MI, Romet-Lemonne G, Hong H, Leadlay PF, et al. Mycolactone activation of Wiskott-Aldrich syndrome proteins underpins Buruli ulcer formation. J Clin Invest. 2013;123(4):1501–12.
Gama JB, Ohlmeier S, Martins TG, Fraga AG, Sampaio-Marques B, Carvalho MA, et al. Proteomic analysis of the action of the Mycobacterium ulcerans toxin mycolactone: targeting host cells cytoskeleton and collagen. PLoS Negl Trop Dis. 2014;8(8):e3066.
Bozzo C, Tiberio R, Graziola F, Pertusi G, Valente G, Colombo E, et al. A Mycobacterium ulcerans toxin, mycolactone, induces apoptosis in primary human keratinocytes and in HaCaT cells. Microbes Infect. 2010;12(14–15):1258–63.
Bieri R, Scherr N, Ruf MT, Dangy JP, Gersbach P, Gehringer M, et al. The macrolide toxin mycolactone promotes Bim-dependent apoptosis in Buruli ulcer through inhibition of mTOR. ACS Chem Biol. 2017;12(5):1297–307.
Ogbechi J, Hall BS, Sbarrato T, Taunton J, Willis AE, Wek RC, et al. Inhibition of Sec61-dependent translocation by mycolactone uncouples the integrated stress response from ER stress, driving cytotoxicity via translational activation of ATF4. Cell Death Dis. 2018;9(3):397.
George KM, Barker LP, Welty DM, Small PL. Partial purification and characterization of biological effects of a lipid toxin produced by Mycobacterium ulcerans. Infect Immun. 1998;66(2):587–93.
Snyder DS, Small PL. Uptake and cellular actions of mycolactone, a virulence determinant for Mycobacterium ulcerans. Microb Pathog. 2003;34(2):91–101.
Bhadra P, Dos Santos S, Gamayun I, Pick T, Neumann C, Ogbechi J, et al. Mycolactone enhances the Ca2+ leak from endoplasmic reticulum by trapping Sec61 translocons in a Ca2+ permeable state. Biochem J. 2021;478(22):4005–24.
Morel JD, Paatero AO, Wei J, Yewdell JW, Guenin-Mace L, Van Haver D, et al. Proteomics reveals scope of mycolactone-mediated Sec61 blockade and distinctive stress signature. Mol Cell Proteomics. 2018;17(9):1750–65.
Hall BS, Dos Santos SJ, Hsieh LT, Manifava M, Ruf MT, Pluschke G, et al. Inhibition of the SEC61 translocon by mycolactone induces a protective autophagic response controlled by EIF2S1-dependent translation that does not require ULK1 activity. Autophagy. 2021;18:1–19.
Hall BS, Simmonds RE. Pleiotropic molecular effects of the Mycobacterium ulcerans virulence factor mycolactone underlying the cell death and immunosuppression seen in Buruli ulcer. Biochem Soc Trans. 2013;42(1):177–83.
Coutanceau E, Marsollier L, Brosch R, Perret E, Goossens P, Tanguy M, et al. Modulation of the host immune response by a transient intracellular stage of Mycobacterium ulcerans: the contribution of endogenous mycolactone toxin. Cell Microbiol. 2005;7(8):1187–96.
Pahlevan AA, Wright DJ, Andrews C, George KM, Small PL, Foxwell BM. The inhibitory action of Mycobacterium ulcerans soluble factor on monocyte/T cell cytokine production and NF-kappa B function. J Immunol. 1999;163(7):3928–35.
Simmonds RE, Lali FV, Smallie T, Small PL, Foxwell BM. Mycolactone inhibits monocyte cytokine production by a posttranscriptional mechanism. J Immunol. 2009;182(4):2194–202.
Torrado E, Adusumilli S, Fraga AG, Small PL, Castro AG, Pedrosa J. Mycolactone-mediated inhibition of tumor necrosis factor production by macrophages infected with Mycobacterium ulcerans has implications for the control of infection. Infect Immun. 2007;75(8):3979–88.
Coutanceau E, Decalf J, Martino A, Babon A, Winter N, Cole ST, et al. Selective suppression of dendritic cell functions by Mycobacterium ulcerans toxin mycolactone. J Exp Med. 2007;204(6):1395–403.
Boulkroun S, Guenin-Mace L, Thoulouze MI, Monot M, Merckx A, Langsley G, et al. Mycolactone suppresses T cell responsiveness by altering both early signaling and posttranslational events. J Immunol. 2010;184(3):1436–44.
Guenin-Mace L, Carrette F, Asperti-Boursin F, Le Bon A, Caleechurn L, Di Bartolo V, et al. Mycolactone impairs T cell homing by suppressing microRNA control of L-selectin expression. Proc Natl Acad Sci U S A. 2011;108(31):12833–8.
Grotzke JE, Kozik P, Morel JD, Impens F, Pietrosemoli N, Cresswell P, et al. Sec61 blockade by mycolactone inhibits antigen cross-presentation independently of endosome-to-cytosol export. Proc Natl Acad Sci U S A. 2017;114(29):E5910–e9.
Foulon M, Robbe-Saule M, Manry J, Esnault L, Boucaud Y, Alcaïs A, et al. Mycolactone toxin induces an inflammatory response by targeting the IL-1β pathway: mechanistic insight into Buruli ulcer pathophysiology. PLoS Pathog. 2020;16(12):e1009107.
Hau AM, Greenwood JA, Löhr CV, Serrill JD, Proteau PJ, Ganley IG, et al. Coibamide a induces mTOR-independent autophagy and cell death in human glioblastoma cells. PLoS One. 2013;8(6):e65250.
Zong G, Hu Z, O'Keefe S, Tranter D, Iannotti MJ, Baron L, et al. Ipomoeassin F binds Sec61α to inhibit protein translocation. J Am Chem Soc. 2019;141(21):8450–61.
Förster B, Demangel C, Thye T. Mycolactone induces cell death by SETD1B-dependent degradation of glutathione. PLoS Negl Trop Dis. 2020;14(10):e0008709.
Ruf MT, Steffen C, Bolz M, Schmid P, Pluschke G. Infiltrating leukocytes surround early Buruli ulcer lesions, but are unable to reach the mycolactone producing mycobacteria. Virulence. 2017;8(8):1918–26.
Bolz M, Ruggli N, Borel N, Pluschke G, Ruf MT. Local cellular immune responses and pathogenesis of Buruli ulcer lesions in the experimental Mycobacterium ulcerans pig infection model. PLoS Negl Trop Dis. 2016;10(4):e0004678.
Ruf MT, Sopoh GE, Brun LV, Dossou AD, Barogui YT, Johnson RC, et al. Histopathological changes and clinical responses of Buruli ulcer plaque lesions during chemotherapy: a role for surgical removal of necrotic tissue? PLoS Negl Trop Dis. 2011;5(9):e1334.
Ruf MT, Schutte D, Chauffour A, Jarlier V, Ji B, Pluschke G. Chemotherapy-associated changes of histopathological features of Mycobacterium ulcerans lesions in a Buruli ulcer mouse model. Antimicrob Agents Chemother. 2012;56(2):687–96.
Andreoli A, Ruf MT, Sopoh GE, Schmid P, Pluschke G. Immunohistochemical monitoring of wound healing in antibiotic treated Buruli ulcer patients. PLoS Negl Trop Dis. 2014;8(4):e2809.
Fevereiro J, Fraga AG, Pedrosa J. The immunology of Buruli ulcer. In: Pluschke G, Röltgen K, editors. Buruli ulcer: Mycobacterium ulcerans disease. Cham: Springer; 2019. p. 135–58. Copyright 2019, The Author(s).
van der Werf TS, van der Graaf WT, Tappero JW, Asiedu K. Mycobacterium ulcerans infection. Lancet. 1999;354(9183):1013–8.
Beissner M, Piten E, Maman I, Symank D, Jansson M, Nitschke J, et al. Spontaneous clearance of a secondary Buruli ulcer lesion emerging ten months after completion of chemotherapy—a case report from togo. PLoS Negl Trop Dis. 2012;6(7):e1747.
Gordon CL, Buntine JA, Hayman JA, Lavender CJ, Fyfe JA, Hosking P, et al. Spontaneous clearance of Mycobacterium ulcerans in a case of Buruli ulcer. PLoS Negl Trop Dis. 2011;5(10):e1290.
O'Brien DP, Murrie A, Meggyesy P, Priestley J, Rajcoomar A, Athan E. Spontaneous healing of Mycobacterium ulcerans disease in Australian patients. PLoS Negl Trop Dis. 2019;13(2):e0007178.
Marion E, Jarry U, Cano C, Savary C, Beauvillain C, Robbe-Saule M, et al. FVB/N mice spontaneously heal ulcerative lesions induced by Mycobacterium ulcerans and switch M. ulcerans into a low mycolactone producer. J Immunol. 2016;196(6):2690–8.
Silva-Gomes R, Marcq E, Trigo G, Gonçalves CM, Longatto-Filho A, Castro AG, et al. Spontaneous healing of Mycobacterium ulcerans lesions in the Guinea pig model. PLoS Negl Trop Dis. 2015;9(12):e0004265.
Nausch N, Antwi-Berko D, Mubarik Y, Abass KM, Owusu W, Owusu-Dabo E, et al. Analysis of Mycobacterium ulcerans-specific T-cell cytokines for diagnosis of Buruli ulcer disease and as potential indicator for disease progression. PLoS Negl Trop Dis. 2017;11(2):e0005415.
Gooding TM, Johnson PD, Campbell DE, Hayman JA, Hartland EL, Kemp AS, et al. Immune response to infection with Mycobacterium ulcerans. Infect Immun. 2001;69(3):1704–7.
Gooding TM, Kemp AS, Robins-Browne RM, Smith M, Johnson PD. Acquired T-helper 1 lymphocyte anergy following infection with Mycobacterium ulcerans. Clin Infect Dis. 2003;36(8):1076–7.
Phillips R, Sarfo FS, Guenin-Mace L, Decalf J, Wansbrough-Jones M, Albert ML, et al. Immunosuppressive signature of cutaneous Mycobacterium ulcerans infection in the peripheral blood of patients with buruli ulcer disease. J Infect Dis. 2009;200(11):1675–84.
Phillips R, Horsfield C, Kuijper S, Sarfo SF, Obeng-Baah J, Etuaful S, et al. Cytokine response to antigen stimulation of whole blood from patients with Mycobacterium ulcerans disease compared to that from patients with tuberculosis. Clin Vaccine Immunol. 2006;13(2):253–7.
Diaz D, Döbeli H, Yeboah-Manu D, Mensah-Quainoo E, Friedlein A, Soder N, et al. Use of the immunodominant 18-kiloDalton small heat shock protein as a serological marker for exposure to Mycobacterium ulcerans. Clin Vaccine Immunol. 2006;13(12):1314–21.
Dobos KM, Spotts EA, Marston BJ, Horsburgh CR Jr, King CH. Serologic response to culture filtrate antigens of Mycobacterium ulcerans during Buruli ulcer disease. Emerg Infect Dis. 2000;6(2):158–64.
Pidot SJ, Porter JL, Marsollier L, Chauty A, Migot-Nabias F, Badaut C, et al. Serological evaluation of Mycobacterium ulcerans antigens identified by comparative genomics. PLoS Negl Trop Dis. 2010;4(11):e872.
Loglo AD, Frimpong M, Sarpong Duah M, Sarfo F, Sarpong FN, Agbavor B, et al. IFN-γ and IL-5 whole blood response directed against mycolactone polyketide synthase domains in patients with Mycobacterium ulcerans infection. Peer J. 2018;6:e5294.
Gooding TM, Johnson PD, Smith M, Kemp AS, Robins-Browne RM. Cytokine profiles of patients infected with Mycobacterium ulcerans and unaffected household contacts. Infect Immun. 2002;70(10):5562–7.
Bieri R, Bolz M, Ruf MT, Pluschke G. Interferon-γ is a crucial activator of early host immune defense against Mycobacterium ulcerans infection in mice. PLoS Negl Trop Dis. 2016;10(2):e0004450.
Bibert S, Bratschi MW, Aboagye SY, Collinet E, Scherr N, Yeboah-Manu D, et al. Susceptibility to Mycobacterium ulcerans disease (Buruli ulcer) is associated with IFNG and iNOS gene polymorphisms. Front Microbiol. 2017;8:1903.
Capela C, Dossou AD, Silva-Gomes R, Sopoh GE, Makoutode M, Menino JF, et al. Genetic variation in autophagy-related genes influences the risk and phenotype of Buruli ulcer. PLoS Negl Trop Dis. 2016;10(4):e0004671.
Stienstra Y, van der Werf TS, Oosterom E, Nolte IM, van der Graaf WT, Etuaful S, et al. Susceptibility to Buruli ulcer is associated with the SLC11A1 (NRAMP1) D543N polymorphism. Genes Immun. 2006;7(3):185–9.
Campbell LP, Finley AO, Benbow ME, Gronseth J, Small P, Johnson RC, et al. Spatial analysis of anthropogenic landscape disturbance and Buruli ulcer disease in Benin. PLoS Negl Trop Dis. 2015;9(10):e0004123.
Combe M, Velvin CJ, Morris A, Garchitorena A, Carolan K, Sanhueza D, et al. Global and local environmental changes as drivers of Buruli ulcer emergence. Emerg Microb Infect. 2017;6(1):1–11.
Williamson HR, Benbow ME, Campbell LP, Johnson CR, Sopoh G, Barogui Y, et al. Detection of Mycobacterium ulcerans in the environment predicts prevalence of Buruli ulcer in Benin. PLoS Negl Trop Dis. 2012;6(1):e1506.
Stienstra Y, van der Graaf WT, te Meerman GJ, The TH, de Leij LF, van der Werf TS. Susceptibility to development of Mycobacterium ulcerans disease: review of possible risk factors. Trop Med Int Health. 2001;6(7):554–62.
Aiga H, Amano T, Cairncross S, Adomako J, Nanas OK, Coleman S. Assessing water-related risk factors for Buruli ulcer: a case-control study in Ghana. Am J Trop Med Hyg. 2004;71(4):387–92.
Lavender CJ, Fyfe JA, Azuolas J, Brown K, Evans RN, Ray LR, et al. Risk of Buruli ulcer and detection of Mycobacterium ulcerans in mosquitoes in southeastern Australia. PLoS Negl Trop Dis. 2011;5(9):e1305.
Raghunathan PL, Whitney EA, Asamoa K, Stienstra Y, Taylor TH Jr, Amofah GK, et al. Risk factors for Buruli ulcer disease (Mycobacterium ulcerans infection): results from a case-control study in Ghana. Clin Infect Dis. 2005;40(10):1445–53.
Fenner F. The pathogenic behavior of Mycobacterium ulcerans and Mycobacterium balnei in the mouse and the developing chick embryo. Am Rev Tuberc. 1956;73(5):650–73.
Fenner F. Homologous and heterologous immunity in infections of mice with Mycobacterium ulcerans and Mycobacterium balnei. Am Rev Tuberc. 1957;76(1):76–89.
Huygen K. Prospects for vaccine development against Buruli disease. Expert Rev Vaccines. 2003;2(4):561–9.
Zwerling A, Behr MA, Verma A, Brewer TF, Menzies D, Pai M. The BCG world atlas: a database of global BCG vaccination policies and practices. PLoS Med. 2011;8(3):e1001012.
Anon. BCG vaccination against Mycobacterium ulcerans infection (Buruli ulcer). First results of a trial in Uganda. Lancet. 1969;1(7586):111–5.
Smith PG, Revill WD, Lukwago E, Rykushin YP. The protective effect of BCG against Mycobacterium ulcerans disease: a controlled trial in an endemic area of Uganda. Trans R Soc Trop Med Hyg. 1977;70(5–6):449–57.
Seddon JA, Paton J, Nademi Z, Keane D, Williams B, Williams A, et al. The impact of BCG vaccination on tuberculin skin test responses in children is age dependent: evidence to be considered when screening children for tuberculosis infection. Thorax. 2016;71(10):932–9.
Phillips RO, Phanzu DM, Beissner M, Badziklou K, Luzolo EK, Sarfo FS, et al. Effectiveness of routine BCG vaccination on buruli ulcer disease: a case-control study in the Democratic Republic of Congo, Ghana and Togo. PLoS Negl Trop Dis. 2015;9(1):e3457.
Nackers F, Dramaix M, Johnson RC, Zinsou C, Robert A, et al. BCG vaccine effectiveness against Buruli ulcer: a case-control study in Benin. Am J Trop Med Hyg. 2006;75(4):768–74.
Muhi S, Stinear TP. Systematic review of M. Bovis BCG and other candidate vaccines for Buruli ulcer prophylaxis. Vaccine. 2021;39(50):7238–52.
Ishwarlall TZ, Okpeku M, Adeniyi AA, Adeleke MA. The search for a Buruli ulcer vaccine and the effectiveness of the Bacillus calmette–Guérin vaccine. Acta Trop. 2022;228:106323.
Pönnighaus JM, Fine PE, Sterne JA, Wilson RJ, Msosa E, Gruer PJ, et al. Efficacy of BCG vaccine against leprosy and tuberculosis in northern Malawi. Lancet. 1992;339(8794):636–9.
Glynn JR, Fielding K, Mzembe T, Sichali L, Banda L, McLean E, et al. BCG re-vaccination in Malawi: 30-year follow-up of a large, randomised, double-blind, placebo-controlled trial. Lancet Glob Health. 2021;9(10):e1451–e9.
Mangtani P, Abubakar I, Ariti C, Beynon R, Pimpin L, Fine PE, et al. Protection by BCG vaccine against tuberculosis: a systematic review of randomized controlled trials. Clin Infect Dis. 2014;58(4):470–80.
Bolz M, Ruf MT. Buruli ulcer in animals and experimental infection models. In: Pluschke G, Röltgen K, editors. Buruli ulcer: Mycobacterium ulcerans disease. Cham: Springer; 2019. p. 159–81.
Marion E, Song OR, Christophe T, Babonneau J, Fenistein D, Eyer J, et al. Mycobacterial toxin induces analgesia in buruli ulcer by targeting the angiotensin pathways. Cell. 2014;157(7):1565–76.
En J, Goto M, Nakanaga K, Higashi M, Ishii N, Saito H, et al. Mycolactone is responsible for the painlessness of Mycobacterium ulcerans infection (buruli ulcer) in a murine study. Infect Immun. 2008;76(5):2002–7.
Mangas KM, Tobias NJ, Marion E, Babonneau J, Marsollier L, Porter JL, et al. High antibody titres induced by protein subunit vaccines using Mycobacterium ulcerans antigens Hsp18 and MUL_3720 with a TLR-2 agonist fail to protect against Buruli ulcer in mice. Peer J. 2020;8:e9659.
Coutanceau E, Legras P, Marsollier L, Reysset G, Cole ST, Demangel C. Immunogenicity of Mycobacterium ulcerans Hsp65 and protective efficacy of a Mycobacterium leprae Hsp65-based DNA vaccine against Buruli ulcer. Microbes Infect. 2006;8(8):2075–81.
Omansen TF, Porter JL, Johnson PD, van der Werf TS, Stienstra Y, Stinear TP. In-vitro activity of avermectins against Mycobacterium ulcerans. PLoS Negl Trop Dis. 2015;9(3):e0003549.
Wallace JR, Mangas KM, Porter JL, Marcsisin R, Pidot SJ, Howden B, et al. Mycobacterium ulcerans low infectious dose and mechanical transmission support insect bites and puncturing injuries in the spread of Buruli ulcer. PLoS Negl Trop Dis. 2017;11(4):e0005553.
Mangas KM, Buultjens AH, Porter JL, Baines SL, Marion E, Marsollier L, et al. Vaccine-specific immune responses against Mycobacterium ulcerans infection in a low-dose murine challenge model. Infect Immun. 2020;88(3):e00753.
Watanabe M, Nakamura H, Nabekura R, Shinoda N, Suzuki E, Saito H. Protective effect of a dewaxed whole-cell vaccine against Mycobacterium ulcerans infection in mice. Vaccine. 2015;33(19):2232–9.
Fraga AG, Martins TG, Torrado E, Huygen K, Portaels F, Silva MT, et al. Cellular immunity confers transient protection in experimental Buruli ulcer following BCG or mycolactone-negative Mycobacterium ulcerans vaccination. PLoS One. 2012;7(3):e33406.
Tanghe A, Content J, Van Vooren JP, Portaels F, Huygen K. Protective efficacy of a DNA vaccine encoding antigen 85A from Mycobacterium bovis BCG against Buruli ulcer. Infect Immun. 2001;69(9):5403–11.
Tanghe A, Dangy JP, Pluschke G, Huygen K. Improved protective efficacy of a species-specific DNA vaccine encoding mycolyl-transferase Ag85A from Mycobacterium ulcerans by homologous protein boosting. PLoS Negl Trop Dis. 2008;2(3):e199.
Hart BE, Hale LP, Lee S. Immunogenicity and protection conferred by a recombinant Mycobacterium marinum vaccine against Buruli ulcer. Trials Vaccinol. 2016;5:88–91.
Hart BE, Hale LP, Lee S. Recombinant BCG expressing Mycobacterium ulcerans Ag85A imparts enhanced protection against experimental Buruli ulcer. PLoS Negl Trop Dis. 2015;9(9):e0004046.
Hart BE, Lee S. Overexpression of a Mycobacterium ulcerans Ag85B-EsxH fusion protein in recombinant BCG improves experimental Buruli ulcer vaccine efficacy. PLoS Negl Trop Dis. 2016;10(12):e0005229.
Bolz M, Benard A, Dreyer AM, Kerber S, Vettiger A, Oehlmann W, et al. Vaccination with the surface proteins MUL_2232 and MUL_3720 of Mycobacterium ulcerans induces antibodies but fails to provide protection against Buruli ulcer. PLoS Negl Trop Dis. 2016;10(2):e0004431.
Bolz M, Kerber S, Zimmer G, Pluschke G. Use of recombinant virus replicon particles for vaccination against Mycobacterium ulcerans disease. PLoS Negl Trop Dis. 2015;9(8):e0004011.
Roupie V, Pidot SJ, Einarsdottir T, Van Den Poel C, Jurion F, Stinear TP, et al. Analysis of the vaccine potential of plasmid DNA encoding nine mycolactone polyketide synthase domains in Mycobacterium ulcerans infected mice. PLoS Negl Trop Dis. 2014;8(1):e2604.
Tanghe A, Adnet PY, Gartner T, Huygen K. A booster vaccination with Mycobacterium bovis BCG does not increase the protective effect of the vaccine against experimental Mycobacterium ulcerans infection in mice. Infect Immun. 2007;75(5):2642–4.
Huygen K. The Immunodominant T-cell epitopes of the mycolyl-transferases of the antigen 85 complex of M. tuberculosis. Front Immunol. 2014;5:321.
Porter JL, Tobias NJ, Pidot SJ, Falgner S, Tuck KL, Vettiger A, et al. The cell wall-associated mycolactone polyketide synthases are necessary but not sufficient for mycolactone biosynthesis. PLoS One. 2013;8(7):e70520.
Dreyer A, Röltgen K, Dangy JP, Ruf MT, Scherr N, Bolz M, et al. Identification of the Mycobacterium ulcerans protein MUL_3720 as a promising target for the development of a diagnostic test for Buruli ulcer. PLoS Negl Trop Dis. 2015;9(2):e0003477.
Vettiger A, Scherr N, Ruf M, Röltgen K, Pluschke G. Localization of mycobacterial antigens by immunofluorescence staining of agarose embedded cells. Mycobact Dis. 2014;4:3–4.
Dangy JP, Scherr N, Gersbach P, Hug MN, Bieri R, Bomio C, et al. Antibody-mediated neutralization of the exotoxin mycolactone, the main virulence factor produced by Mycobacterium ulcerans. PLoS Negl Trop Dis. 2016;10(6):e0004808.
Naranjo L, Ferrara F, Blanchard N, Demangel C, D'Angelo S, Erasmus MF, et al. Recombinant antibodies against Mycolactone. Toxins. 2019;11(6):346.
Copland A, Diogo GR, Hart P, Harris S, Tran AC, Paul MJ, et al. Mucosal delivery of fusion proteins with Bacillus subtilis spores enhances protection against tuberculosis by bacillus Calmette-Guérin. Front Immunol. 2018;9:346.
Hart P, Copland A, Diogo GR, Harris S, Spallek R, Oehlmann W, et al. Nanoparticle-fusion protein complexes protect against Mycobacterium tuberculosis infection. Mol Ther. 2018;26(3):822–33.
Diogo GR, Hart P, Copland A, Kim MY, Tran AC, Poerio N, et al. Immunization with Mycobacterium tuberculosis antigens encapsulated in phosphatidylserine liposomes improves protection afforded by BCG. Front Immunol. 2019;10:1349.
Clegg J, Soldaini E, Bagnoli F, McLoughlin RM. Targeting skin-resident memory T cells via vaccination to combat Staphylococcus aureus infections. Trends Immunol. 2021;42(1):6–17.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2023 The Author(s)
About this chapter
Cite this chapter
Boakye-Appiah, J., Hall, B., Reljic, R., Simmonds, R.E. (2023). Current Progress and Prospects for a Buruli Ulcer Vaccine. In: Christodoulides, M. (eds) Vaccines for Neglected Pathogens: Strategies, Achievements and Challenges . Springer, Cham. https://doi.org/10.1007/978-3-031-24355-4_5
Download citation
DOI: https://doi.org/10.1007/978-3-031-24355-4_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-24354-7
Online ISBN: 978-3-031-24355-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)