Abstract
The failure of cartilage healing is a major impediment to recovery from joint disease or trauma. Growth factors play a central role in cell function and have been proposed as potential therapeutic agents to promote cartilage repair. Decades of investigation have identified many growth factors that promote the formation of cartilage in vitro and in vivo. However, very few of these have progressed to human trials. A growth factor that robustly augments articular cartilage healing remains elusive. This is not surprising. Articular cartilage repair involves multiple cellular processes and it is unlikely that any single agent will be able to optimally regulate all of them. It is more likely that multiple regulatory molecules may be required to optimize the maintenance and restoration of articular cartilage. If this is the case, then interactions among growth factors may be expected to play a key role in determining their therapeutic value. This review explores the hypothesis that growth factor interactions could help optimize articular cartilage healing.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Articular cartilage provides the gliding surface that enables pain-free joint motion. Articular cartilage damage due to disease or trauma is among the most disabling conditions affecting American adults [1]. This tissue has a particularly poor intrinsic repair capacity compared to most other tissues and damage tends to be progressive over time. There is currently no disease modifying agent that prevents, arrests or reverses cartilage damage.
Growth factors are essential regulators of cell behavior. Numerous growth factors have been shown to augment the repair capacity of articular chondrocytes in in vitro and in vivo models [2, 3]. Among these are insulin-like growth factor 1 (IGF-1), [4, 5] Fibroblast growth factor 2 (FGF-2), [6,7,8,9,10,11] Fibroblast growth factor 18 (FGF-18), [12,13,14,15] bone morphogenetic proteins 2 and 7 (BMP-2, BMP-7), [16,17,18,19,20] and transforming growth factor beta (TGF-β) [21, 22]. These growth factors regulate critical chondrocyte reparative functions by distinct and overlapping signal transduction pathways.
The sheer number of chondrogenic growth factors poses the challenge of determining which among them is the best one to pursue in translational studies toward clinical application. To date, few growth factors have progressed through clinical trials to test their potential as therapeutic agents. One of these is TGF-β1. A phase III study delivered non-transformed and retrovirally transduced juvenile human chondrocytes carrying the TGF-β1 gene to subjects with moderate (Kellgren-Lawrence grade III) osteoarthritis of the knee. The effect on articular cartilage was a trend toward greater cartilage thickness at one year [23]. A second example is FGF-18. A phase II study delivered a series of recombinant FGF-18 injections to knees of subjects with mild or moderate (Kellgren-Lawrence grade II-III) osteoarthritis. The results showed a statistically significant increase of 0.05 mm in mean tibiofemoral cartilage thickness compared to placebo at two years that persisted to 5 years [24]. These studies reflect substantial progress in the search for disease-modifying growth factors. Although encouraging, these results also suggest that further improvement could be achievable.
The regulation of the multiple, distinct chondrocyte functions that are involved in chondrogenesis is sufficiently complex that a single regulatory factor is unlikely to optimally promote articular cartilage healing. Indeed, an extensive literature has shown that two or more growth factors can improve chondrocyte biosynthesis compared to just one growth factor [7, 25,26,27,28,29]. These data suggest that, instead of attempting to identify the best growth factor for cartilage healing, perhaps it would be better to attempt to identify the best growth factor combination for cartilage healing. Central to such an approach is understanding how growth factors interact with each other in regulating articular chondrocyte reparative functions.
2 Multiple Growth Factors
To test the hypothesis that growth factors interact in chondrocyte regulation, a study delivered the genes encoding IGF-1, FGF-2, BMP-2, BMP-7 and TGF-β by transfection using an adeno-associated virus-based vector individually, or in combination, to primary adult bovine articular chondrocytes in culture, and measured their effect on chondrocyte aggrecan, type II collagen and type I collagen gene expression. The results showed that the growth factor transgenes differentially regulated the magnitude and time course of expression of all three chondrocyte matrix protein genes. The data further demonstrated interactions among the growth factors that ranged from inhibitory to synergistic. Maximum stimulation of type II collagen gene expression (35 fold) and also of aggrecan gene expression (16-fold) was by the combination of IGF-1, BMP-2 and BMP-7 transgenes. Interestingly, the FGF-2 transgene, individually and in combination with other growth factor transgenes, tended to stimulate aggrecan gene expression, but nearly abolished the expression of both type I and type II collagen gene expression [30].
A subsequent study sought to determine whether these growth factors interact to modulate articular chondrocyte proliferation and the production of cartilage matrix. As in the prior study, the genes encoding IGF-1, FGF-2, TGF-β1, BMP-2 and BMP-7, individually and in various combinations, were delivered to primary adult bovine articular chondrocytes in culture. Dependent variables included changes in DNA content, an index of chondrocyte proliferation, and changes in glycosaminoglycan (GAG) and collagen content, indices of cartilage matrix synthesis. Glycosaminoglycan that was released into the culture medium or retained in the cell layer were measured separately [31]. This distinction is important because retained matrix molecules contribute to the formation of new cartilage, while released molecules do not provide structural benefit.
The results showed that, in concert, the growth factors interacted to generate widely divergent effects on both chondrocyte proliferation and matrix synthesis. As was seen for the regulation of gene expression, these interactions ranged from inhibitory to synergistic. The IGF-1 transgene synergistically stimulated proliferation when combined with any of the other growth factor transgenes, and synergistic stimulation by the combination of IGF-1 and FGF-2 transgenes maximized cell proliferation (8.5 fold). Synergistic stimulation by the combination of the IGF-1, BMP-2 and BMP-7 transgenes maximized matrix production (14.9 fold), and also maximized the proportion of GAG retained in the cell layer. Similar results were obtained for collagen, the other major component of articular cartilage matrix. In contrast to the other growth factor transgenes, the FGF-2 transgene, when combined with any of the other transgenes, increased the proportion of collagen that was lost into the medium such that the majority of the newly synthesized collagen did not contribute to matrix formation. Further, when added to the combination of the IGF-1 transgene and either of the BMP transgenes, the FGF-2 transgene abolished their synergistic stimulation of both cell-associated GAG and collagen [31].
These and other studies reveal imitations to the use of growth factor combinations for articular cartilage repair. First, some growth factor combinations inhibited chondrocyte biosynthesis [32, 33]. Second, the optimal combination for proliferation was poor at augmenting matrix production (IGF-I plus FGF-2), and the optimal combination for matrix production was only a mediocre mitogen (IGF-I plus BMP-2 plus BMP-7). Thus, no combination of growth factors was found that optimized both of these key chondrocyte reparative functions.
3 Multiple Combinations of Growth Factors
Taken together, the foregoing results suggest that instead of attempting to identify the best growth factor combination for cartilage healing, perhaps it would be better to attempt to identify the best combination of growth factor combinations for cartilage healing. Using data from the above studies, one example would be to select the combination of IGF-1 and FGF-2 to increase the number of chondrocytes and use the combination of IGF-1, BMP-2 and BMP-7 to increase matrix production.
This approach fits the conceptual framework of chondrogenesis as a four-dimensional process. During cartilage development and repair, cell functions change over time. These changes are effected, in part, by changes in the signaling factors that regulate those functions. As a result, interventions that deliver different agents in sequence may be superior to those that deliver different agents simultaneously, or to the same agent delivered repeatedly. However, treatments that deliver combinations of growth factors simultaneously take advantage of their synergistic interactions, a benefit that would likely be lost when multiple growth factors are delivered sequentially. These are not mutually exclusive options. Multiple combinations of sequentially delivered growth factor combinations offer the dual advantages of both synergistically activating distinct sets of signal transduction pathways to optimize cellular responses, and of doing so at times appropriate to distinct phases of cartilage repair.
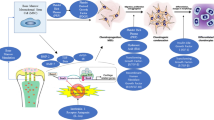
In its simplest form, this approach would involve a combination of just two distinct combinations of regulatory factors. If the first combination of growth factors optimized cell proliferation and the second combination optimized matrix production, the combination of two combinations of factors would first increase the number of cells and then stimulate that enlarged population of cells to generate matrix. In such cases, the order of delivery of the combinations would be important (Fig. 10.1). To address more than two cell-regulatory phases during repair or regeneration, the model would require additional combinations and sequences of delivery over the course of treatment.
Delivery sequences of two combinations of growth factor combinations. Delivery of a two-growth factor combination that increases the number of chondrocytes, which are then stimulated to produce matrix by a three-growth factor combination (upper sequence) would likely generate more robust neocartilage than the delivery of the same two growth factor combinations in the reverse (lower) sequence. The reverse sequence would be expected to produce a comparatively matrix-deficient tissue
4 Multifunctional Growth Factors
The application of growth factors to cartilage repair will also require a more complete understanding of their actions on chondrocytes. Many growth factors are pleiotropic and regulate multiple chondrocyte functions. As illustrated by FGF-2, some of these functions may mitigate against chondrogenesis. Although FGF-2 is an asset as a potent mitogen for articular chondrocytes, and has been shown to promote chondrogenesis, it is also a potential liability as a potent stimulus of cartilage matrix catabolism, [34,35,36,37] an effect that is mediated, at least in part, by MMP-13 [38].
A recent study tested the catabolic effect of IGF-1, FGF-2, BMP-2, BMP-7 and TGF-β by transferring individual or combinations of the genes encoding these factors to primary bovine articular chondrocytes, and measuring the expression of A disintegrin and metalloproteinase with thrombospondin motifs-4 (ADAMTS)-4, ADAMTS-5, matrix metalloproteinase-3 (MMP)-3, MMP-13, and interleukin 6 (IL-6). Unexpectedly, the growth factor transgenes generally increased the expression of these catabolic genes. Further, interactions among these growth factors transgenes produced a wide range of synergistic and inhibitory effects on these genes. The regulation of IL-6 and MMP-13 are illustrative. Individually, IGF-1 and FGF-2 increased IL-6 gene expression to 3.0-fold and 10.8-fold respectively. In combination, they synergistically increased IL-6 expression to 40-fold. In the case of MMP-13, IGF-1 initially reduced MMP-13 expression and then increased it to 2.3-fold, while FGF-2 progressively increased MMP-13 expression to 71-fold. In concert, the addition of IGF-1 to FGF-2 brought the stimulation by FGF-2 down to 5.4-fold. Thus, the interaction between IGF-1 and FGF-2 was opposite for the two catabolic genes: synergistic for IL-6 and inhibitory for MMP-13. Conversely, the different growth factor transgenes all tended to produce similar effects on ADAMTS-4 and ADAMTS-5 gene expression, but in opposite directions. They upregulated ADAMTS-4 and down-regulated ADAMTS-5 [39].
Taken together, available evidence indicates that growth factor interactions are remarkably diverse with respect the direction, magnitude, time course and specific genes that they regulate, including degradative functions. This diversity extends beyond the previously noted inhibitory-to-synergistic range of interactive effects on reparative functions. The competing actions of growth factors on reparative and degradative chondrocyte behaviors add an additional level of complexity to the development of these regulatory molecules as therapeutic agents for restoring articular cartilage homeostasis or promoting repair. The diversity of these actions could also offer a potential benefit. It provides the opportunity to select specific growth factor combinations, and specific phases of cartilage repair that can be tailored to produce specific outcomes.
5 Opportunities for Progress
A major obstacle to identifying growth factor combinations for translational studies is the current lack of ability to predict the actions of a combination of growth factors based on their individual actions. This problem reflects a deficient understanding of the mechanisms underlying growth factor interactions. While the mechanisms of action of individual growth factors have been fairly well established, the mechanisms of interaction among the networks formed by these pathways are only beginning to be elucidated. One approach to this problem is to identify the sites of cross-talk in the growth factor signal transduction networks that mediate their interactions. An omics approach to understanding of the specific determinants of growth factor interaction will be enhanced by the application of advanced machine learning, high-throughput combinatorial experimental methods, and bioinformatic analytics. For example, characterization of the articular chondrocyte interactome could facilitate the development of therapeutic agents designed to elicit specific chondrocyte behaviors.
Another approach to identifying these mechanisms is to better understand the interactions between growth factors and the subcellular anatomic structures that contribute to their function. A recent study employed a novel approach to elucidating structure-function relationships among intracellular proteins and their environment [40]. The authors combined imaging and biophysical data on the intracellular location of several hundred proteins. They employed neural networks to relate the proteins to each other and to subcellular structures. The study identified multiple previously unknown subcellular functional systems, including cross talk between them [40]. Such information obtained for growth factor networks might lend insight into the mechanisms underlying the interactions in their regulation of chondrocytes.
6 Biochemical and Biophysical Factor Combinations
Growth factor actions are not determined just by interactions with each other. They are also determined by interactions with a variety of other cell-regulatory stimuli. Prominent among these are mechanical forces. Bonassar et al. tested the hypothesis that the mechanical regulator, static compression, and the biochemical regulator, IGF-1, modulate each other’s effects on articular chondrocyte biosynthesis. Bovine articular cartilage explants were treated with IGF-1 (0–300 ng/ml), static compression (0–50%), or the combination of both, and the incorporation of [35S]sulfate and [3H]proline into the cartilage matrix was measured. As expected, [41] IGF-1 increased, and static compression decreased, both [35S]sulfate and [3H]proline incorporation in a dose-dependent fashion. When delivered together, static compression progressively inhibited the stimulatory effect of IGF-1 and 50% compression nearly eliminated the effect of IGF-1. The time course of action of the two stimuli differed; IGF-1 stimulation plateaued at 24 hours while static compression reached a steady state by 4 hours. Static compression also reduced the concentration of IGF-I in the tissue at equilibrium [42].
Expanding on the study of static compression, Bonassar et al. tested the hypothesis that dynamic compression and IGF-1 modulate each other’s actions on articular chondrocyte biosynthesis. Bovine articular cartilage explants were treated with IGF-1 (0–300 ng/ml), dynamic compression (2% strain, 0.1 Hz), or both, and [35S]sulfate and [3H]proline incorporation were measured. IGF-1 and dynamic compression each increased both [35S]sulfate and [3H]proline incorporation. When given together, the stimulation was greater than the maximum stimulation by either IGF-1 or dynamic compression alone. Further, the time constant of stimulation for IGF-1 and dynamic compression was 12.2 hours and 2.9 hours respectively, and 5.6 hours for the combination. Dynamic compression also increased the rate of diffusion of IGF-1 into the cartilage matrix [43].
To extend these studies from static and dynamic compression to shear deformation, Jin et al. employed a similar model as above but applied shear strains (0–6.0%) rather than compression. IGF-1 and dynamic shear each increased both [35S]sulfate and [3H]proline incorporation. When given together, the stimulation was greater than the maximum stimulation by either IGF-1 or dynamic shear alone. Unlike static compression, shear did not change the concentration of IGF-1 in the cartilage tissue and unlike dynamic compression, it did not change the transport of IGF-1 into the tissue [44].
Taken together, the results of all three of the above studies indicate that IGF-1 and mechanical stimuli regulate the same articular chondrocyte reparative functions and that these two classes of stimuli act through distinct signal transduction pathways.
A recent illustration of growth factor interaction with mechanosensors is the observation by Trompeter et al. that IGF-1 regulates the mechanosensitivity of chondrocyte-like ATDC5 cells by modulating TRPV4 (transient receptor potential vanilloid 4) ion channel. TRPV4 is central to chondrocyte mechanotransduction and may play a role in osteoarthritis. This study demonstrated that IGF-1 suppressed hypotonic-induced TRPV4 currents and intracellular calcium flux by increasing apparent cell stiffness associated with actin stress fiber formation. IGF-1 also abrogated the release of ATP that is mediated by TRPV4 in response to mechanical stimulation [45]. This study demonstrates a direct connection between a growth factor and a mechanotransduction pathway in chondrocyte-like cells. A second illustration of interaction between growth factor and mechanotransduction pathways is provided by the chondrocyte primary cilium, an organelle that serves, in part, as an interface between extracellular forces and intracellular growth factor signaling [46].
7 Growth Factor – Matrix Interaction: Role in Growth Factor Delivery
The clinical application of growth factors requires an effective delivery system. Methods will be needed to deliver the desired growth factor combinations in the desired sequence over the desired time periods to the desired locations. They must be retained at the desired site of action long enough to produce their effect and focal enough to avoid off-target effects. This will involve another class of growth factor interactions: those between the growth factor(s), the delivery vehicle and the site of cartilage damage to be treated. Free growth factors generally have a relatively short residence time (t½ = hours to ±1 day) when delivered by intra-articular injection [47, 48] and, for better or for worse, have at least as good access to synovial cells as to articular chondrocytes. Articular chondrocytes reside in a dense, highly anionic matrix. For growth factors such as FGF-18 that have a high isoelectric point (pI~10), this can facilitate binding to the negatively charged proteoglycan sulfate groups in cartilage matrix, a property that may account for the articular cartilage localization of intra-articular FGF-18 when delivered to rat knees [48].
To augment the delivery of growth factors to articular chondrocytes embedded in an anionic matrix, Geiger et al. engineered a charged PEGylated dendrimer and conjugated it to IGF-1 [49]. The authors demonstrated that this penetrated the full thickness of 1 mm thick bovine articular cartilage explants. Further, when injected into rat knees, the dendrimer-IGF-1 prolonged the residence time in the joint from a half-life of 0.41 days for unconjugated IGF-1 to 4.21 days. In a rat model of surgically induced knee osteoarthritis, the dendrimer-IGF-1 decreased the area of medial tibial degeneration to 8.4% from the 19.7% observed with unconjugated IGF-1 [49].
An alternative method to improve the delivery of growth factors to sites of articular cartilage damage is to create a fusion protein composed of a growth factor and a specific binding domain, and deliver it in a hydrogel functionalized with the binding domain target sequence. Zanotto et al. used a heparin-binding IGF-1 and delivered it in a self-assembling KLD hydrogel to articular cartilage defects treated by microfracture in equine femoropatellar joints [50]. The treatment also included preparation of the site with trypsin and delivery of platelet derived growth factor with the heparin-binding IGF-1. The results showed improvement in multiple histological parameters and overall quality of the repair tissue compared to microfracture alone [50].
8 Conclusions
Available evidence suggests that growth factor interactions have the potential to promote articular cartilage healing. Harnessing these interactions to help create effective therapies for damaged cartilage will require new research and development technologies that are able to elucidate and then take advantage of the complex mechanisms underlying those interactions. This enterprise will, in turn, require new interactions among representatives of various, currently under-connected disciplines.
In the meantime, sufficient information exists to suggest certain growth factor combinations for further study. One example is FGF-18 and IGF-1, with or without a member of the TGF-β family. A review of growth factors not referenced in this limited review is likely to suggest additional options.
This enterprise, if pursued, would not be without challenges. One is a prolonged time frame. Articular cartilage damage usually progresses slowly and clinical trials may require many years to generate useful results. Another is the regulatory challenge of gaining approval for multiple simultaneously and sequentially delivered agents, particularly if combined with other tissue engineered constructs.
It is important to put the field of biologic approaches to cartilage repair in context. There exists the possibility that progress in the fields of skeletal reconstruction, joint replacement, or other interventions will outpace those of biologics. Although such alternative solutions to preventing and/or treating articular cartilage damage would potentially reduce the need for biologic agents, growth factor-based interventions may well augment the benefits of the other forms of treatment. Further, different approaches would likely prove to be most useful for different conditions, or different stages of disease. Ideally, the elucidation of the causes of cartilage-damaging joint disease would enable the prevention of at least some of the conditions altogether. None of these options are mutually exclusive and all of them hold promise.
The field of cartilage repair, including the role of growth factors, owes an enormous debt of gratitude to Professor Alan Grodzinsky for his decades of innovative research, education of new researchers and collaboration with fellow investigators.
References
Centers for Disease C, Prevention (2010) Prevalence of doctor-diagnosed arthritis and arthritis-attributable activity limitation—United States, 2007–2009. MMWR Morb Mortal Wkly Rep 59(39):1261–1265
Trippel SB, Coutts RD, Einhorn TA, Mundy GR, Rosenfeld RD (1996) Growth factors as therapeutic agents. J Bone Joint Surg (Am Vol) 78:1272–1286
Kuo CK, Li W-J, Mauck RL, Tuan RS (2006) Cartilage tissue engineering: its potential and uses. Curr Opin Rheumatol 18(1):64–73
Trippel SB, Corvol MT, Dumontier MF, Rappaport R, Hung HH, Mankin HJ (1989) Effect of somatomedin-C/insulin-like growth factor I and growth hormone on cultured growth plate and articular chondrocytes. Pediatr Res 25(1):76–82
Fortier LA, Mohammed HO, Lust G, Nixon AJ (2002) Insulin-like growth factor-I enhances cell-based repair of articular cartilage. J Bone Joint Surg 84(2):276–288
Jentzsch KD, Wellmitz G, Heder G, Petzold E, Buntrock P, Oehme P (1980) A bovine brain fraction with fibroblast growth factor activity inducing articular cartilage regeneration in vivo. Acta Biol Med Ger 39(8–9):967–971
Osborn KD, Trippel SB, Mankin HJ (1989) Growth factor stimulation of adult articular cartilage. J Orthop Res 7(1):35–42
Henson FM, Bowe EA, Davies ME (2005) Promotion of the intrinsic damage-repair response in articular cartilage by fibroblastic growth factor-2. Osteoarthritis and cartilage/OARS, Osteoarthritis Research Society. 13(6):537–544
Cucchiarini M, Madry H, Ma C, Thurn T, Zurakowski D, Menger MD et al (2005) Improved tissue repair in articular cartilage defects in vivo by rAAV-mediated overexpression of human fibroblast growth factor 2. Mol Ther 12(2):229–238
Yokoo N, Saito T, Uesugi M, Kobayashi N, Xin KQ, Okuda K et al (2005) Repair of articular cartilage defect by autologous transplantation of basic fibroblast growth factor gene-transduced chondrocytes with adeno-associated virus vector. Arthritis Rheum 52(1):164–170
Sawaji Y, Hynes J, Vincent T, Saklatvala J (2008) Fibroblast growth factor 2 inhibits induction of aggrecanase activity in human articular cartilage. Arthritis Rheum 58(11):3498–3509
Ellsworth JL, Berry J, Bukowski T, Claus J, Feldhaus A, Holderman S et al (2002) Fibroblast growth factor-18 is a trophic factor for mature chondrocytes and their progenitors. [Erratum appears in Osteoarthritis Cartilage 2002 Oct;10(10):826]. Osteoarthr Cartil 10(4):308–320
Davidson D, Blanc A, Filion D, Wang H, Plut P, Pfeffer G et al (2005) Fibroblast growth factor (FGF) 18 signals through FGF receptor 3 to promote chondrogenesis. J Biol Chem 280(21):20509–20515
Moore EE, Bendele AM, Thompson DL, Littau A, Waggie KS, Reardon B et al (2005) Fibroblast growth factor-18 stimulates chondrogenesis and cartilage repair in a rat model of injury-induced osteoarthritis. Osteoarthr Cartil 13(7):623–631
Lohmander LS, Hellot S, Dreher D, Krantz EF, Kruger DS, Guermazi A et al (2014) Intra-articular Sprifermin (Recombinant Human Fibroblast Growth Factor 18) in Knee Osteoarthritis: randomized, double-blind, placebo-controlled trial. Arthritis & rheumatology (Hoboken, NJ) 66:1820–1831
Cook SD, Rueger DC (1996) Osteogenic protein-1: biology and applications. Clin Orthop Relat Res 324:29–38
Sailor LZ, Hewick RM, Morris EA (1996) Recombinant human bone morphogenetic protein-2 maintains the articular chondrocyte phenotype in long-term culture. J Orthop Res 14(6):937–945
Frenkel SR, Saadeh PB, Mehrara BJ, Chin GS, Steinbrech DS, Brent B et al (2000) Transforming growth factor beta superfamily members: role in cartilage modeling. Plast Reconstr Surg 105(3):980–990
van der Kraan PM, Vitters EL, van Beuningen HM, van de Loo FA, van den Berg WB (2000) Role of nitric oxide in the inhibition of BMP-2-mediated stimulation of proteoglycan synthesis in articular cartilage. Osteoarthritis and cartilage/OARS, Osteoarthritis Research Society. 8(2):82–86
Chubinskaya S, Kuettner KE (2003) Regulation of osteogenic proteins by chondrocytes. Int J Biochem Cell Biol 35(9):1323–1340
Morales TI, Roberts AB (1988) Transforming growth factor beta regulates the metabolism of proteoglycans in bovine cartilage organ cultures. J Biol Chem 263(26):12828–12831
Rosier RN, O’Keefe RJ, Crabb ID, Puzas JE (1989) Transforming growth factor beta: an autocrine regulator of chondrocytes. Connect Tissue Res 20(1–4):295–301
Kim MK, Ha CW, In Y, Cho SD, Choi ES, Ha JK et al (2018) A multicenter, double-blind, Phase III clinical trial to evaluate the efficacy and safety of a cell and gene therapy in knee Osteoarthritis patients. Hum Gene Ther Clin Dev 29(1):48–59
Hochberg MC, Guermazi A, Guehring H, Aydemir A, Wax S, Fleuranceau-Morel P et al (2019) Effect of intra-articular sprifermin vs placebo on femorotibial joint cartilage thickness in patients with osteoarthritis: the FORWARD randomized clinical trial. JAMA 322(14):1360–1370
Inoue H, Kato Y, Iwamoto M, Hiraki Y, Sakuda M, Suzuki F (1989) Stimulation of cartilage-matrix proteoglycan synthesis by morphologically transformed chondrocytes grown in the presence of fibroblast growth factor and transforming growth factor-beta. J Cell Physiol 138(2):329–337
Tsukazaki T, Usa T, Matsumoto T, Enomoto H, Ohtsuru A, Namba H et al (1994) Effect of transforming growth factor-beta on the insulin-like growth factor-I autocrine/paracrine axis in cultured rat articular chondrocytes. Exp Cell Res 215(1):9–16
Chopra R, Anastassiades T (1998) Specificity and synergism of polypeptide growth factors in stimulating the synthesis of proteoglycans and a novel high molecular weight anionic glycoprotein by articular chondrocyte cultures. J Rheumatol 25(8):1578–1584
Loeser RF, Pacione CA, Chubinskaya S (2003) The combination of insulin-like growth factor 1 and osteogenic protein 1 promotes increased survival of and matrix synthesis by normal and osteoarthritic human articular chondrocytes. Arthritis Rheum 48(8):2188–2196
Leipzig ND, Eleswarapu SV, Athanasiou KA (2006) The effects of TGF-beta1 and IGF-I on the biomechanics and cytoskeleton of single chondrocytes. Osteoarthritis and cartilage/OARS, Osteoarthritis Research Society 14(12):1227–1236
Shi S, Mercer S, Eckert GJ, Trippel SB (2012) Regulation of articular chondrocyte aggrecan and collagen gene expression by multiple growth factor gene transfer. J Orthop Res 30(7):1026–1031
Shi S, Mercer S, Eckert GJ, Trippel SB (2013) Growth factor transgenes interactively regulate articular chondrocytes. J Cell Biochem 114(4):908–919
Sonal D (2001) Prevention of IGF-1 and TGFbeta stimulated type II collagen and decorin expression by bFGF and identification of IGF-1 mRNA transcripts in articular chondrocytes. Matrix Biol 20(4):233–242
Loeser RF, Chubinskaya S, Pacione C, Im HJ (2005) Basic fibroblast growth factor inhibits the anabolic activity of insulin-like growth factor 1 and osteogenic protein 1 in adult human articular chondrocytes. Arthritis Rheum 52(12):3910–3917
Sah RL, Chen AC, Grodzinsky AJ, Trippel SB (1994) Differential effects of bFGF and IGF-I on matrix metabolism in calf and adult bovine cartilage explants. Arch Biochem Biophys 308(1):137–147
Yan D, Chen D, Cool SM, van Wijnen AJ, Mikecz K, Murphy G et al (2011) Fibroblast growth factor receptor 1 is principally responsible for fibroblast growth factor 2-induced catabolic activities in human articular chondrocytes. Arthritis Res Ther 13(4):R130
Ellman MB, Yan D, Ahmadinia K, Chen D, An HS, Im HJ (2013) Fibroblast growth factor control of cartilage homeostasis. J Cell Biochem 114(4):735–742
Sah RL, Trippel SB, Grodzinsky AJ (1996) Differential effects of serum, insulin-like growth factor-I, and fibroblast growth factor-2 on the maintenance of cartilage physical properties during long-term culture. J Orthop Res 14(1):44–52
Im H-J, Muddasani P, Natarajan V, Schmid TM, Block JA, Davis F et al (2007) Basic fibroblast growth factor stimulates matrix metalloproteinase-13 via the molecular cross-talk between the mitogen-activated protein kinases and protein kinase Cdelta pathways in human adult articular chondrocytes. J Biol Chem 282(15):11110–11121
Shi S, Mercer S, Eckert GJ, Trippel SB (2019) Regulation of articular chondrocyte catabolic genes by growth factor interaction. J Cell Biochem 120:11127
Qin Y, Huttlin EL, Winsnes CF, Gosztyla ML, Wacheul L, Kelly MR et al (2021) A multi-scale map of cell structure fusing protein images and interactions. Nature 600(7889):536–542
Kim YJ, Sah RL, Grodzinsky AJ, Plaas AH, Sandy JD (1994) Mechanical regulation of cartilage biosynthetic behavior: physical stimuli. Arch Biochem Biophys 311(1):1–12
Bonassar LJ, Grodzinsky AJ, Srinivasan A, Davila SG, Trippel SB (2000) Mechanical and physicochemical regulation of the action of insulin-like growth factor-I on articular cartilage. Arch Biochem Biophys 379(1):57–63
Bonassar LJ, Grodzinsky AJ, Frank EH, Davila SG, Bhaktav NR, Trippel SB (2001) The effect of dynamic compression on the response of articular cartilage to insulin-like growth factor-I. J Orthop Res 19(1):11–17
Jin M, Emkey GR, Siparsky P, Trippel SB, Grodzinsky AJ (2003) Combined effects of dynamic tissue shear deformation and insulin-like growth factor I on chondrocyte biosynthesis in cartilage explants. Arch Biochem Biophys 414(2):223–231
Trompeter N, Gardinier JD, DeBarros V, Boggs M, Gangadharan V, Cain WJ et al (2021) Insulin-like growth factor-1 regulates the mechanosensitivity of chondrocytes by modulating TRPV4. Cell Calcium 99:102467
Thompson CL, Plant JC, Wann AK, Bishop CL, Novak P, Mitchison HM et al (2017) Chondrocyte expansion is associated with loss of primary cilia and disrupted hedgehog signalling. Eur Cell Mater 34:128–141
Caldwell J (2000) A safety tolerability and pharmacokinetic study of intra-articular recombinant human insulin-like growth factor (rhIFG-I) in patients with severe osteoarthritis (OA) of the Knee. America College of Rheumatology 64th Annual Scientific Meeting; 2000:Abstract 941, Abstract Supplement 2000, p S233
Ladel CH, Barbero L, Riva S, Guehring H (2020) Tissue distribution of sprifermin (recombinant human fibroblast growth factor 18) in the rat following intravenous and intra-articular injection. Osteoarthritis and Cartilage Open 2:100068
Geiger BC, Wang S, Padera RF Jr, Grodzinsky AJ, Hammond PT (2018) Cartilage-penetrating nanocarriers improve delivery and efficacy of growth factor treatment of osteoarthritis. Sci Transl Med 10(469)
Zanotto G, Liebesny P, Barrett M, Zlotnick H, Grodzinsky A, Frisbie D (2019) Trypsin pre-treatment combined with growth factor functionalized self-assembling peptide hydrogel improves cartilage repair in rabbit model. J Orthop Res 37(11):2307–2315
Acknowledgements
Supported by the Department of Orthopaedic Surgery, Indiana University School of Medicine. The author thanks Sue Samson for assistance with manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Additional information
Dedication: This review is dedicated to Prof. Alan J. Grodzinsky on the occasion of his 75th birthday.
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2023 The Author(s)
About this chapter
Cite this chapter
Trippel, S.B. (2023). Harnessing Growth Factor Interactions to Optimize Articular Cartilage Repair. In: Connizzo, B.K., Han, L., Sah, R.L. (eds) Electromechanobiology of Cartilage and Osteoarthritis. Advances in Experimental Medicine and Biology, vol 1402. Springer, Cham. https://doi.org/10.1007/978-3-031-25588-5_10
Download citation
DOI: https://doi.org/10.1007/978-3-031-25588-5_10
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-25587-8
Online ISBN: 978-3-031-25588-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)