Abstract
Ongoing technical innovation in combination with a broad research activity has resulted in increased adoption and widespread utilization of magnetic resonance imaging (MRI) of the prostate. The Prostate Imaging Reporting and Data System (PI-RADS), first introduced in 2012 and subsequently updated in 2015 and 2019, standardized image acquisition and reporting and facilitated the communication of imaging findings to referring physician teams and is now considered an obligatory key element in prostate MRI. This has had a tremendous impact on the diagnostic workup of patients with suspected prostate cancer. Indications for MRI have been incorporated in multiple prostate cancer guidelines (e.g., NICE, AUA, EAU, German S3-Guideline), and in turn imaging-based targeted prostate biopsy has markedly increased. Referring physicians not only heavily rely on accurate interpretation of MRI of the prostate but actively seek high-quality MRI scans for their daily practice because prostate MRI has direct impact on their cancer detection rate. Furthermore, a paradigm shift is taking place in the prostate cancer community regarding the care of low-risk prostate cancer patients, where active surveillance (AS) is increasingly favored over definitive therapy. Prostate MRI plays an important role in AS not only during the initial assessment to determine eligibility but also over the course of follow-up of the disease.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
-
To learn about the advancing role of MR imaging for the management of prostate cancer.
-
To learn how to optimize multiparametric prostate MR imaging.
-
To know common pitfalls in MR imaging of the prostate.
-
To understand how the PI-RADS classification system is applied and interpreted.
-
To know the relevance of structured reporting in prostate cancer.
16.1 Introduction
Ongoing technical innovation in combination with a broad research activity has resulted in increased adoption and widespread utilization of magnetic resonance imaging (MRI) of the prostate. The Prostate Imaging Reporting and Data System (PI-RADS), first introduced in 2012 and subsequently updated in 2015 and 2019, standardized image acquisition and reporting and facilitated the communication of imaging findings to referring physician teams and is now considered an obligatory key element in prostate MRI. This has had a tremendous impact on the diagnostic workup of patients with suspected prostate cancer. Indications for MRI have been incorporated in multiple prostate cancer guidelines (e.g., NICE, AUA, EAU, German S3-Guideline), and in turn imaging-based targeted prostate biopsy has markedly increased. Referring physicians not only heavily rely on accurate interpretation of MRI of the prostate but actively seek high-quality MRI scans for their daily practice because prostate MRI has direct impact on their cancer detection rate. Furthermore, a paradigm shift is taking place in the prostate cancer community regarding the care of low-risk prostate cancer patients, where active surveillance (AS) is increasingly favored over definitive therapy. Prostate MRI plays an important role in AS not only during the initial assessment to determine eligibility but also over the course of follow-up of the disease.
All abdominal and genitourinary radiologists require training and skill in performing and interpreting prostate MRI, especially as prostate MRI has become an indispensable diagnostic tool for all patients with clinical suspicion of prostate cancer, during surveillance of low-risk disease and follow-up after prostate cancer treatment.
16.2 The Prostate Imaging Reporting and Data System (PI-RADS)
PI-RADS was introduced by the European Society of Uroradiology (ESUR) in 2012. An updated version (PI-RADS v2) was published in 2015 in collaboration with the American College of Radiology (ACR) and the AdMeTech Foundation. Further refinements through the same collaboration were conducted in 2019 and published as PI-RADS version 2.1. PI-RADS is not based on evidence from clinical research trials but rather on expert knowledge; however, several studies have confirmed that the PI-RADS system improves the diagnostic accuracy of multiparametric (mp) MRI. The overall rationale for implementation of PI-RADS was to ´improve detection, localization, characterization, and risk stratification in patients with suspected cancer in treatment naïve prostate glands´. PI-RADS is currently not applicable to post-treatment assessment in prostate cancer patients, although there are now other efforts proposed specifically for this purpose. The following specific definitions and aims regarding MR imaging and reporting are targeted by PI-RADS:
16.2.1 Clinical Considerations
Timing of mpMRI after prostate biopsy does not necessarily need to be postponed since clinically significant cancer is less likely affected by post biopsy changes when the biopsy was negative, a phenomenon referred to as the “hemorrhage exclusion sign.” For local staging of prostate cancer a delay of a minimum of 6 weeks might be advantageous. No specific patient preparation is necessary; however, the administration of a spasmolytic drug may be beneficial. Bowel cleaning is not recommended, but the patient should evacuate the rectum if possible to reduce the occurrence of susceptibility-related imaging artifacts.
16.2.2 Technical Considerations
Magnetic field strengths of 1.5 or 3 Tesla can both be used (even without an endorectal coil at 1.5 Tesla) when the scan parameters are tailored to small field-of-view imaging of the prostate and contemporary scanner technology is used (specifically multi-channel phased-array surface coils and high=performance gradients). In general, latest generation 3 Tesla systems are preferred (higher signal-to-noise ratio, shorter scan time), although an optimized acquisition protocol is considered even more important than field strength.
mpMRI of the prostate should include the following sequences:
T2-weighted imaging: 2D turbo spin-echo sequence, slice thickness ≤ 3 mm (no interslice gap), in-plane spatial resolution ≤0.7 mm (phase-encoding direction) x ≤ 0.4 mm (frequency-encoding direction). Images in the axial plane (either straight axial to the patient or oblique axial perpendicular to the long axis of the prostate) should be acquired as well as images in at least one additional orthogonal plane (sagittal and/or coronal).
Diffusion-weighted imaging (DWI): spin-echo EPI (echo planar imaging) sequence with fat saturation, slice thickness ≤ 4 mm (no interslice gap), in-plane spatial resolution ≤2.5 mm (phase- and frequency-encoding direction), at least two b-values (low b-value of 50–100 s/mm2 and an intermediate b-value of 800–1000 s/mm2). Additional b-values in the range of 100–1000 s/mm2 are optional. A high b-value (≥1400 s/mm2) image set is also mandatory (preferably should be obtained from a separate acquisition rather than from the abovementioned sequence (used for ADC map calculation), or calculated from the low and intermediate b-value images.
Dynamic contrast-enhanced (DCE) imaging: 2D or 3D (3D preferred) gradient-echo sequence with a temporal resolution below 15 s (preferably below 10 s) per acquisition, slice thickness ≤ 3 mm (no interslice gap), in-plane spatial resolution ≤2 mm (phase- and frequency-encoding direction).
Slice orientation and slice thickness should match for all mpMRI sequences to allow side-by-side comparison. Also, a large field-of-view sequence covering the pelvic lymph nodes and the skeleton should be acquired.
16.2.3 Assessment of Prostatic Lesions
One major key element of PI-RADS is scoring the likelihood of a prostatic lesion to be clinically significant prostate cancer on a 5-point Likert-type scale (Table 16.1).
Since several different definitions of clinically significant prostate cancer exist PI-RADS defines it as “Gleason score ≥7 (including 3 + 4 with prominent but not predominant Gleason 4 component), and/or tumor volume ≥0.5cc, and/or tumor extra prostatic extension (EPE).” The scoring system is based on typical imaging findings on the respective multiparametric MR sequence (exact definitions according to PI-RADS see Tables 16.2, 16.3, and 16.4, for examples see Figs. 16.1, 16.2, 16.3, 16.4, 16.5, 16.6, 16.7, 16.8, 16.9, 16.10, 16.11, 16.12, and 16.13). For this purpose, typical examples for each score and sequence are included in the PI-RADS publication. The goal is to increase the diagnostic accuracy for detection of prostate cancer and to reduce the variability in image interpretation. Most preliminary studies report good reader agreement, which is higher for peripheral zone (PZ) lesions than transition zone (TZ) lesions. Also, agreement is higher for PI-RADS scores 4 and 5 compared to lower scores.
(a–d) Normal peripheral zone. (a) Axial and (b) coronal T2-weighted sequence showing uniform hyperintense signal intensity of the peripheral zone (PI-RADS score 1). (c) Diffusion-weighted high b-value (calculated b = 1400 s/mm2) image and (d) ADC map (dominant sequence for the peripheral zone) with no abnormality consistent with an overall PI-RADS score of 1. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a, b) Normal transition zone. (a) Axial and (b) coronal T2-weighted sequence (dominant sequence for the transition zone) showing heterogeneous intermediate signal intensity of the non-enlarged transition zone (PI-RADS score 1). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–e) PI-RADS score 2 findings in the peripheral zone. (a) Axial and (b) coronal T2-weighted sequence showing linear hypointensities in the bilateral peripheral zone (PI-RADS score 2). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows no areas of increased signal intensity. (d) ADC map shows no focal hypointense areas (dominant sequence for the peripheral zone) in the peripheral zone (PI-RADS score 2). (e) DCE sequence shows no focal or early enhancement (DCE negative) consistent with an overall PI-RADS score of 2. Linear T2-hypointensities in the peripheral zone are a frequent finding and may represent changes related to chronic prostatitis or post biopsy scarring. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–d) PI-RADS 1 findings of the transition zone in a patient with benign prostatic hyperplasia (BPH). (a) Axial and (b) coronal T2-weighted sequence (dominant sequence for the transition zone) showing multiple circumscribed heterogeneous encapsulated nodules (dark T2-rim) within the enlarged transition zone (PI-RADS score 1). (c) Diffusion-weighted high b-value (calculated b = 1400 s/mm2) image shows no focal areas of moderately increased signal intensity. (d) ADC map shows no focal hypointense areas (PI-RADS score 1). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–e) Protruded BPH node in the right anterior gland. (a) Axial and (b) coronal T2-weighted sequence (dominant sequence for the transition zone) showing a circumscribed heterogeneous completely encapsulated nodule (overall PI-RADS score 1). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows increased signal intensity. (d) ADC map shows a focal hypointensity which is related to stromal BPH components which corresponds to the BPH nodule. (e) DCE sequence showing focal enhancement which corresponds to the lesion that demonstrates clear features of a BPH node (therefore DCE negative) consistent with an overall PI-RADS score of 1. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
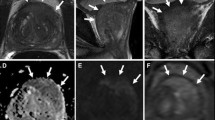
(a–e) PI-RADS 3 findings of the peripheral zone. (a) Axial and (b) coronal T2-weighted sequence showing heterogeneous non-circumscribed changes of the peripheral zone bilaterally (PI-RADS score 3). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows a mildly hyperintense signal intensity. (d) ADC map (dominant sequence for the peripheral zone) shows moderately hypointense changes in the bilateral peripheral zone (PI-RADS score 3). (e) DCE sequence shows no focal early enhancement (DCE negative) consistent with an overall PI-RADS score of 3. TRUS-guided prostate biopsy revealed mild chronic prostatitis with no evidence of prostate cancer. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–e) PI-RADS 3 changes of the transition zone in a patient with benign prostatic hyperplasia (BPH). (a) Axial and (b) coronal T2-weighted sequence (dominant sequence for the transition zone) showing heterogeneous signal intensity with obscured margins within the enlarged transition zone (overall PI-RADS score 3). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows mildly hyperintense signal intensity. (d) ADC map shows moderately hypointense areas (PI-RADS score 3). (e) DCE sequence shows diffuse enhancement not corresponding to a focal finding on any other sequence (DCE negative). Random TRUS-guided biopsy revealed no cancer, the findings were clinically attributed to BPH with predominantly stromal (T2 hypointense) components. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–e) PI-RADS 4 lesion in the peripheral zone. (a) Axial and (b) coronal T2-weighted sequence showing moderate diffuse (non-circumscribed) hypointensity of the bilateral peripheral zone (PI-RADS score 3). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows mildly hyperintense signal intensity in the right anterior and lateral peripheral zone (PI-RADS score 3). (d) ADC map correspondingly shows moderate hypointense signal intensity (dominant sequence for the peripheral zone) in the right anterior and lateral peripheral zone (PI-RADS score 3). (e) DCE sequence shows focal and contemporary enhancement (DCE positive) consistent with an upgrading to an overall PI-RADS score of 4. MRI/US fusion guided biopsy revealed a Gleason 3 + 4 = 7 adenocarcinoma (PSA level 6.9 ng/mL). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–e) PI-RADS 4 lesion in the peripheral zone. (a) axial and (b) coronal T2-weighted sequence showing a circumscribed 11 mm hypointense lesion in the left lateral peripheral zone (PI-RADS score 4). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows focal markedly hyperintense signal intensity. (d) ADC map (dominant sequence for the peripheral zone) correspondingly shows focal markedly hypointense signal intensity (PI-RADS score 4). (e)DCE sequence shows focal and early enhancement (DCE positive) corresponding to the lesion seen on T2w and DWI consistent with an overall PI-RADS score of 4. MRI/US fusion guided biopsy revealed a Gleason 4 + 3 = 7 adenocarcinoma (PSA level 8.1 ng/mL). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–c) PI-RADS 4 lesion in the transition zone. (a) Axial T2-weighted sequence (dominant sequence for the transition zone) showing a circumscribed lenticular 14 mm hypointense lesion in the left anterior transition zone with bulging of the fibromuscular stroma (PI-RADS score 4). (b) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows focal markedly hyperintense signal intensity. (c) ADC map correspondingly shows focal markedly hypointense signal intensity (PI-RADS score 4). MRI/US fusion guided biopsy revealed a Gleason 4 + 4 = 8 adenocarcinoma (PSA level 9.8 ng/mL). The patient had undergone a random TRUS-guided biopsy 3 months earlier with no evidence of malignancy. The anterior location is typical for adenocarcinoma missed by random prostate biopsies, thus MRI is particularly useful in patients with negative random biopsy and persisting clinical suspicion for prostate cancer. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
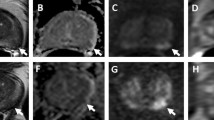
(a–e) PI-RADS 5 lesion in the peripheral zone. (a) Axial and (b) coronal T2-weighted images showing a circumscribed 18 mm hypointense lesion in the right lateral peripheral zone (PI-RADS score 5). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows focal markedly hyperintense signal intensity. (d) ADC map (dominant sequence for the peripheral zone) correspondingly shows focal markedly hypointense signal intensity (PI-RADS score 5). (e) DCE sequence shows focal and early enhancement (DCE positive) corresponding to the lesion seen on T2w and DWI consistent with an overall PI-RADS score of 5. MRI/US fusion guided biopsy revealed a Gleason 4 + 3 = 7 adenocarcinoma (PSA level 11.2 ng/mL). Also note the wedge-shaped T2-hypointensities in the left lateral peripheral zone which demonstrate moderately hypointense signal on the ADC map and no focal enhancement (PI-RADS 3). On biopsy multifocal prostate cancer was diagnosed with Gleason 3 + 3 = 6 pattern in the left side of the prostate. (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–d) PI-RADS 5 lesion in the transition zone. (a) Axial and (b) coronal T2-weighted images (dominant sequence for the transition zone) showing a circumscribed lenticular 20 mm hypointense mass the anterior transition zone with bulging of the prostatic capsule (PI-RADS score 5). (c) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows focal markedly hyperintense signal intensity. (d) ADC map correspondingly shows focal markedly hypointense signal intensity (PI-RADS score 4). MRI/US fusion guided biopsy revealed a Gleason 4 + 3 = 7 adenocarcinoma (PSA level 14.7 ng/mL). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
(a–c) Locally advanced prostate cancer with seminal vesicle invasion. (a) Axial T2-weighted sequence showing diffuse hypointensity of the entire prostate (zonal anatomy not visible) with extension into the bilateral seminal vesicles (PI-RADS score 5). (b) Diffusion weighted high b-value (calculated b = 1400 s/mm2) image shows markedly hyperintense signal intensity of the entire prostate. (c) ADC map correspondingly shows markedly hypointense signal intensity of the prostate (PI-RADS score 5). Randomized TRUS guided biopsy revealed a Gleason 4 + 5 = 9 adenocarcinoma (PSA level 26.5 ng/mL). (Reproduced from. https://doi.org/10.1007/978-3-319-75019-4_11)
Compared to PI-RADS version 1, PI-RADS version 2 introduced the diagnostic weighting of the multiparametric sequences to generate a combined score by introducing the concept of a dominant imaging sequence. The dominant sequence depends on the prostatic zone the lesion is located; therefore identification of the zonal anatomy is crucial. The area at the base of the prostate where the central zone borders the peripheral zone and the anterior gland where the anterior horn of the peripheral zone borders the transition zone and the anterior fibromuscular stroma might be challenging in this respect. DWI is the dominant sequence for the peripheral zone, where most prostate cancers are located. T2W is the dominant sequence for the transition zone. The dominant sequence defines the final PI-RADS score with the exception of PI-RADS 3 lesions, where for the peripheral zone, the DCE sequence and for the transition zone, the DWI sequence defines the final PI-RADS score (see Tables 16.5 and 16.6). PI-RADS version 2.1 also included a subcategorization of PI-RADS score 2 TZ lesions on T2-weighted images, as reflected in Table 16.6.
There is growing interest and support for the use of bi-parametric (bp) MRI (T2W + DWI), eliminating the need for DCE-MRI. The current PI-RADS version 2.1 contains no specific recommendations for the use of bpMRI; however, it does address situations where a particular sequence cannot be acquired or is non-diagnostic due to artifacts (e.g., DWI when certain hip implants are present). In these situations, the following rules apply:
Assessment without DWI (applies to PZ and TZ): the T2-weighted sequence defines the final PI-RADS score with the exception of PI-RADS 3 - if the lesion is DCE negative the final score remains 3, if the lesion is DCE positive the final score is 4.
Assessment without DCE (only applies to the peripheral zone since DCE is not used for transition zone scoring): the DWI score represents the final PI-RADS score.
16.2.4 Structured Reporting
A very important task of PI-RADS is to simplify and standardize the terminology and content of radiology reports and to enhance interdisciplinary communications with referring clinicians. A comprehensive mpMRI report should therefore include the following contents:
The volume of prostate should be reported according to the ellipsoid formula: maximum AP diameter × maximum transverse diameter × maximum longitudinal diameter × 0.52. PI-RADS version 2.1 suggests that maximum AP and longitudinal diameters be measured on a mid-sagittal T2W image if obtained, and that maximum transverse diameter measurement is made on an axial T2W image. PI-RADS scores are assigned to up to 4 intraprostatic lesions with overall score ≥ 3. In case of multiple lesions, an index lesion should be defined. The index lesion is the one with the highest PI-RADS score. In case multiple lesions qualify for the highest PI-RADS score, extraprostatic extension (EPE) outweighs lesion size. For each lesion a PI-RADS score is assigned to a visual snapshot, or the series and the image number where the lesion is best visualized should be reported to assist the selection of optimal images for MRI/US fusion-guided prostate biopsy. The lesion size also needs to be reported. Measurement of each lesion is preferred on the axial images, the DWI sequence should be used for peripheral zone lesions and the T2-weighted images for transition zone lesions. If a lesion is not well delineated on the axial sequences then another plane can be used.
Another crucial element of a full PI-RADS report is a sector map in which the lesions should be indicated, since this particularly enhances the communication with referring physician teams. For this matter, the prostate is subdivided into three axial regions craniocaudally, the base, the midgland and the prostatic apex. The seminal vesicles should also be included for cases of extraprostatic extension. The zonal anatomy (peripheral zone, transition zone, central zone and anterior fibromuscular stroma) and the urethra should also be incorporated into the sector map.
16.3 Conclusion
Comprehensive multiparametric MRI of the prostate should include lesion scoring and reporting according to the PI-RADS system. This will assist to achieve a high level of diagnostic accuracy and assure a thriving communication with the multidisciplinary care team.
Further Reading
Ahmed HU, El-Shater Bosaily A, Brown LC, et al. Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet. 2017;389:815–22.
Barentsz JO, Richenberg J, Clements R, et al. ESUR prostate MR guidelines 2012. Eur Radiol. 2012;22:746–57.
Barrett T, Vargas HA, Goldman D, Akin O, Hricak H. The value of the “Hemorrhage exclusion” sign on T1-weighted prostate MRI for the detection of prostate cancer. Radiology. 2012;263(3):751–7.
Barth BK, De Visschere PJ, Cornelius A, Nicolau C, Vargas HA, Eberli D, Donati OF. Detection of clinically significant prostate cancer: short dual-pulse sequence versus standard multiparametric MR Imaging-A multireader study. Radiology. 2017;284(3):725–36.
Cash H, Günzel K, Maxeiner A, et al. Men with a negative real-time MRI/ultrasound-fusion guided targeted biopsy but prostate cancer detection on TRUS-guided random biopsy – what are the reasons for targeted biopsy failure? BJU Int. 2016a;118:35–43.
Cash H, Maxeiner A, Stephan C, et al. The detection of significant prostate cancer is correlated with the Prostate Imaging Reporting and Data System (PI-RADS) in MRI/transrectal ultrasound fusion biopsy. Word J Urol. 2016b;34:525–32.
Greer MD, Shih JH, Lay N, et al. Validation of the dominant sequence paradigm and role of dynamic contrast-enhanced imaging in PI-RADS version 2. Radiology in press. 2017;285(3):859–69.
Haas M, Gnzel K, Penzkofer T, et al. Implications of PI-RADS version 1 and updated version 2 on the scoring of prostatic lesions on multiparametric MRI. Aktuelle Urol. 2016;47:383–7.
Panebianco V, Villeirs G, Weinreb J, et al. Prostate Magnetic Resonance Imaging for Local Recurrence Reporting (PI-RR): International consensus-based guidelines on multiparametric magnetic resonance imaging for prostate cancer recurrence after radiation therapy and radical prostatectomy. Eur Urol Oncol. 2021;4(6):868–76.
Polanec S, Helbich TH, Bickel H, et al. Head-to-head comparison of PI-RADS v2 and PI-RADS v1. Eur J Radiol. 2016;85:1125–31.
Purysko AS, Bittencourt LK, Bullen JA, et al. Accuracy and interobserver agreement for Prostate Imaging Reporting and Data System, Version 2, for the characterization of lesions identified on multiparametric MRI of the prostate. AJR Am J Roentgenol. 2017;209:339–49.
Rosenkrantz AB, Ginocchio LA, Cornfeld D, et al. Interobserver reproducibility of the PI-RADS version 2 lexicon: a multicenter study of six experienced prostate radiologists. Radiology. 2016;280:793–804.
Turkbey B, Rosenkrantz AB, Haider MA, et al. Prostate Imaging Reporting and Data System Version 2.1: 2019 Update of Prostate Imaging Reporting and Data System Version 2. Eur Urol. 2019;76(3):340–51.
Ullrich T, Quentin M, Oelers C, et al. Magnetic resonance imaging of the prostate at 1.5 versus 3.0 T: a prospective comparison study of image quality. Eur J Radiol. 2017;90:192–7.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2023 The Author(s)
About this chapter
Cite this chapter
Vargas, A., Asbach, P., Hamm, B. (2023). Magnetic Resonance Imaging of the Prostate in the PI-RADS Era. In: Hodler, J., Kubik-Huch, R.A., Roos, J.E., von Schulthess, G.K. (eds) Diseases of the Abdomen and Pelvis 2023-2026. IDKD Springer Series. Springer, Cham. https://doi.org/10.1007/978-3-031-27355-1_16
Download citation
DOI: https://doi.org/10.1007/978-3-031-27355-1_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-27354-4
Online ISBN: 978-3-031-27355-1
eBook Packages: MedicineMedicine (R0)