Abstract
An overexpression of CXCR4 receptors is reported in at least 30 different human solid tumors and hematological malignancies. This overexpression is often associated with tumor aggressiveness, increased risk of metastasis, and a higher probability of recurrence, which in turn leads to a poor prognosis. No in vivo method suitable for whole-body CXCR4 disease quantification has been described and this unmet clinical need or the scientific question has been reported recently. 68Ga-Pentixafor which is a CXCR4 targeting high-affinity PET imaging probe and the tracer has been evaluated in multiple myeloma, lymphoproliferative disorders, and in lung carcinoma, and the imaging results are extremely promising. Human dosimetry studies demonstrated excellent pharmacokinetics and low radiation burden to patients. The clinical applications of 68Ga-Pentixafor/177Lu/213Bi-Pentixather as a “theranostics pair” for the diagnosis and treatment of CXCR4-expressing cancers are emerging. CXCR4-based theranostics, which had not been investigated in clinical practice till now (except few preliminary proof-of-concept studies), may be a potential game changer both in the diagnosis and treatment of CXCR4 overexpressing solid tumors and hematological malignancies in which all other available treatment options have eventually failed.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
- 68Ga-Pentixafor PET/CT
- CXCR4 expression
- Lung cancer
- Multiple myeloma
- Glioblastoma
- PRRT
- Radionuclide theranostics
31.1 Background
A knowledge of receptor expression on the tumor is the key for therapy directed at these receptors and traditionally has been obtained by assay of biopsy material. Advances in molecular cancer biology have demonstrated that many of these tumor targets are receptors and have been reported as earliest targets for cancer diagnosis as well as therapy, with notable success in the effective treatment in few cancers [1]. One such important class of molecules/targets is a class of chemokine receptors, and the human chemokine system includes more than 50 chemokines and 20 chemokine receptors [2]. These receptors play an important role in cancer progression in terms of tumor growth, senescence, angiogenesis, epithelial-mesenchymal transition, metastasis, and evading the host immune system [3]. Among these chemokine receptors, CXCR4 is the most widely expressed receptor on malignant tumors, and its role in tumor biology has been studied extensively [4]. The chemokine CXCL12 is the sole ligand of CXCR4 and the majority of research focusing on the role of CXCR4 in cancer relates to this chemokine/chemokine-receptor pair [5, 6]. Upregulation of CXCR4 has been reported in at least 23 different epithelial, mesenchymal, and hematopoietic cancers [7, 8]. CXCR4 overexpression in tumor tissues has also been correlated with tumor aggressiveness, increased risk of metastasis, and a higher probability of recurrence [9].
It has been reported that an increased CXCR4 receptor density is often associated with metastatic disease which in turn leads to a poor prognosis [10]. Tumor receptor imaging offers a complementary role not only in providing a noninvasive evidence of tumor receptor expression but also in the evaluation of the entire tumor burden and characterization of the tumor heterogeneity. Therefore, noninvasive imaging using high-throughput PET probes targeting CXCR4 receptors may yield important diagnostic and prognostic information pertinent to the disease process [11]. Plerixafor (AMD-3100), an immunostimulant is a peptide that has been approved by Food and Drug Administration (FDA, USA) as a CXCR4-targeted therapy for hematopoietic stem cell mobilization in AML (Acute Myeloid Leukemia) and non-Hodgkin’s Lymphoma (NHL) patients [12]. Several CXCR4-specific PET (64Cu; 68Ga) tracers (AMD-3100; Trade Name—Plerixafor) have been developed but were restricted to preclinical applications [13]. However, the only PET tracer that has undergone the transition to clinical applications is 68Ga-labeled Pentixafor. This PET tracer (developed by a German group) was developed after certain modifications (without changing the physiochemical properties in the motif (Plerixafor—the parent compound)) allowing chemical binding with the metal chelator (DOTA) for achieving effective coupling with 68Ga [14]. These authors in their extensive animal and preliminary human studies have shown that the tracer localizes in the CXCR4-expressing tumors (lymphoma) with high target to nontarget ratios [15]. Further, these authors have shown that 68Ga-Pentixafor offers favorable dosimetry exhibiting whole-body radiation exposure of 2.3 mSv to patients which is almost one-third of that received from a conventional 18F-FDG PET scan [16].
The use of Gallium-68 (half-life t1/2 = 68 min; positron emission intensity—87%) is on the rise [17]. Several favorable properties of this radionuclide include superior image quality compared to SPECT radionuclides (e.g., indium-111) and the potential for an on-demand production via generator technologies that provide reliable and high-purity 68Ga in sufficient quantities for routine radiopharmaceutical production without the need for expensive cyclotron operations [18, 19]. Generator technologies for 68Ga production, chemistry of gallium, and emerging applications for 68Ga radiopharmaceuticals have been reviewed in detail [18, 20]. These physicochemical properties provide a strong basis for developing specific 68Ga-labeled probes for molecular imaging in various human cancers including solid tumors and hematological malignancies [15, 21,22,23].
The central role of CXCR4 in cancer pathogenesis and metastasis is proven beyond doubt; however, no in vivo method suitable for whole-body CXCR4 disease quantification has been described till late. This unmet clinical need or the scientific question has been addressed and 68Ga-Pentixafor having high affinity for CXCR4 receptors have been developed. They synthesized and developed 68Ga-Pentixafor which is a CXCR4 targeting high-affinity nuclear probe and have evaluated the radiotracer in small-cell lung cancer models [22]. Further, proof of concept (POC) studies with 68Ga-Pentixafor in lymphoma-xenografted animal models and in first human hematological malignancies are highly encouraging [23, 24]. And human dosimetry studies demonstrated excellent pharmacokinetics and low radiation burden to patients [16]. In expanding clinical applications of this novel tracer, it has been shown both in preclinical and clinical studies that the tracer provides a high contrast image in comparison to 18F-FDG PET in advanced stage multiple myeloma patients [23]. The other diagnostic applications of 68Ga-Pentixafor in glioma and some other cancers known to have higher degrees of CXCR4 expression are also emerging. We will discuss in this chapter the CXCR4 theranostics in lung cancer, multiple myeloma, and glioma.
31.2 CXCR4-Targeted PET Imaging in Lung Cancer
Lung cancer is one of the most common (after breast cancer) malignancies globally and within India amongst males alone as well as in the combined male and female population [25, 26]. Lung cancer (LC) alone causes higher number of deaths than that caused by the combination of the other four (breast, colon, pancreas, and prostate) common malignancies [25]. Both epidemiological data and molecular understanding of the disease pathophysiology has shown that LC is associated with cigarette smoking and occupational/environmental factors [26,27,28,29]. Approximately, 80% of the LC cases are of the non-small cell lung cancer (NSCLC) and frequently present with advanced disease at initial diagnosis (stages IIIB and IV) where the traditional treatment options like chemotherapy and radiation therapy are aimed at disease and symptom control rather than at achieving a cure [27, 28].
The diagnostic workup of suspected lung cancer depends upon the type, that is, NSCLC or small-cell lung cancer (SCLC), the size and site of the primary lung cancer. This approach involves accurate tissue diagnosis (histopathology and advanced immune-histochemical analysis), staging, and functional evaluation by radiological imaging techniques with high sensitivity and specificity. Amongst, over 150 factors, the tumor stage which guides the therapeutic options (surgery/radiation therapy/chemotherapy) is considered as the most significant prognostic indicator in LC patients [30,31,32,33]. Despite significant advances in diagnostic, staging, and surgical techniques as well as availability of newer targeted (both chemo/radio) therapies, the death rate from lung carcinoma has remained high [34, 35].
Hybrid 18F-FDG PET/CT imaging remains the mainstay of the diagnostic workup of patients with lung cancer [36]. This imaging technique scores high over the conventional radiological techniques for example, computed tomography (CT) and magnetic resonance imaging (MRI) in terms of both sensitivity and specificity [37]. Although 18F-FDG/PET imaging has proven its utility in monitoring response to appropriate therapies at early time intervals, yet this technique has fewer limitations. These include its inability to differentiate inflammatory/infectious pathologies from tumor recurrence/relapse, and the high background FDG uptake interferes with the detection of metastatic lesions in the brain [38, 39]. On the other hand, 18F-FLT, a marker of cell proliferation has high specificity for solid tumors. However, this imaging technique has inherent problem of lower uptake thereby poor image contrast, not making it an ideal PET tracer especially for response assessment [40, 41].
Philips et al. reported that distant metastases from NSCLC require a CXCL12 chemotactic gradient [42]. Furthermore, they found CXCL12 levels to be significantly higher in metastatic organs than that in the primary tumors. Likewise, SCLC preferentially metastasizes to the marrow, which has high constitutive CXCL12 expression [43]. The signaling via CXCR4 on SCLC cells induces activation and signaling of tumor-associated integrins that apparently play an important role in tumor progression [44]. A positive correlation between CXCR4 expression and clinical outcome in lung cancer has been reported. In a very interesting study by Spano et al. [45], it was observed that the patients having CXCR4-positive nuclear staining demonstrated confinement of CXCR4 presence in the nucleus and is associated with better patients’ survival than those having the receptor expression on the cytoplasmic membrane with absent nuclear staining.
In a recent study, Vag et al. reported their first experience on the use of 68Ga-Pentixafor PET imaging, targeting CXCR4 receptors in solid tumors [21]. These authors concluded that the detectability of solid cancers was found to be lower for 68Ga-Pentixafor than for 18F-FDG PET. However, this study included a small and heterogeneous cohort of 21 patients out of which only two were of NSCLC. The highest SUVmax of 10.9 was observed in a NSCLC patient followed by pancreatic cancer (6.2), HCC (5.0), and breast cancer (3.3). On the other hand, highest SUVmax of 13.8 was noted in the cervical metastases of the patient with cancer of unknown primary (CUP). In another study, Lapa et al. [22] studied the feasibility of CXCR4-directed 68Ga-Pentixafor PET/CT imaging in ten patients of small-cell lung carcinoma (SCLC) and compared results with 18F-FDG PET/CT or 68Ga-DOTA-TOC PET/CT. These authors concluded that noninvasive imaging of CXCR4 expression in SCLC is feasible and 68Ga-Pentixafor as a novel PET tracer might serve as a readout for confirming the CXCR expression which might serve as a prerequisite for potential CXCR4-directed radio-chemotherapies.
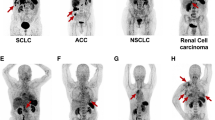
In a preliminary study [46], we have shown that 68Ga-Pentixafor PET/CT demonstrated higher CXCR4 density in SCLC compared to NSCLC and had superior performance in detection of brain metastases which is a known limitation of 18F-FDG PET imaging. We expanded our initial cohort to image 100 lung cancer patients with 68Ga-Pentixafor PET/CT. We found that the SUVmax values on 68Ga-pentixafor PET/CT were 6.14 ± 2.14 and 8.0 ± 1.9 in squamous (n = 60) and adenocarcinoma (n = 20) variants of the NSCLC, respectively. The corresponding values were highest in SCLC (n = 20; SUVmax 10.30 ± 5.0). Similarly, the CXCR4 quantitative values expressed as Mean Fluorescence Index (MFI) for in vivo measure of CXCR4 receptor density were 136.0 ± 80; 288 ± 121, and 348 ± 99 in squamous, adenocarcinoma, and SCLC respectively. These findings highlight that the uptake of the tracer increased as a function of the receptor density which in turn supports the specific binding of the tracer to CXCR4 receptors (Fig. 31.1). A representative IHC-stained slide showing CXCR4+ SCLC patient and a control (CXCR4-negative) slide is shown in Fig. 31.2. We have reported that 68Ga-Pentixafor PET/CT targets CXCR4 receptors non-invasively and its uptake varies as a function of CXCR4 receptors’ density in different lung cancer subtypes [47]. This imaging technique can thus be used for lung cancer disease assessment and for patient selection for appropriate CXCR inhibitor therapies and, especially, α/β-targeted radionuclide therapies. Further, this novel PET tracer has the potential of becoming a powerful tool for monitoring therapy response to CXCR4 inhibitors and also for the development of emerging alpha/beta-targeted therapies in advanced stage lung carcinoma.
31.3 CXCR4-Targeted PET Imaging in Multiple Myeloma
Multiple myeloma (MM) is characterized by the clonal proliferation of malignant plasma cells and accounts for 1.0% of all the cancers and 10.0% of all the hematological malignancies [48, 49]. MM patients often present with skeletal and renal involvement and immunodeficiency [50]. Despite significant advances in treatment for MM, most patients will eventually go into relapse or become refractory to the chemotherapeutic interventions [51]. Therefore, the prognosis for MM patients remains poor and the 5-year survival rate is around 45.0% [52]. This underscores the need to properly understand the tumor biology and find new targets for diagnosis and treatment of MM [53]. 18F-FDG PET has a proven role in the diagnosis, staging, response assessment, and management of MM [54, 55]. However, 18F-FDG PET has its own limitations, as a significant decrease in the SUVmax value (versus the baseline value) on the post-therapy follow-up has been reported to be not correlating with the progression-free survival [56].
The clinical utility of 68Ga-Pentixafor PET/CT imaging for in vivo imaging of CXCR4 whole-body disease burden has been reported in few recent studies. 68Ga-Pentixafor as a novel PET tracer having high affinity for CXCR4 has been shown to be superior or equal to 18F-FDG for the detection of myeloma lesions [57,58,59]. Herrmann et al. [23] in their first preliminary clinical experience reported that after disease mapping with 68Ga-Pentixafor PET/CT, CXCR4-targeted radiotherapy with Pentixather appears to be a promising novel treatment option in combination with cytotoxic chemotherapy and autologous stem cell transplantation, especially for patients with advanced multiple myeloma. Therefore, 68Ga-Pentixafor/177Lu/90Y-Pentixather is emerging as a potential theranostics’ pair for treatment of CXCR4-targeting therapies when other available treatment options in advanced stage MM patients have failed.
Our experience [59] with 68Ga-Pentixafor PET/CT in MM at PGIMER, Chandigarh, India, showed a higher lesion detection rate with 68Ga-Pentixafor PET compared to 18F-FDG PET (Fig. 31.3). We concluded that the dual tracer imaging may provide additional information on spatial and temporal heterogeneity of MM and may have significance for response evaluation to CXCR4-targeting pharmacologic or endo-radiotherapeutic therapies in CXCR4-positive and FDG-negative disease variants of multiple myeloma. In a recent study [60] in 30 MM patients, 68Ga-Pentixafor PET/CT showed a higher positive disease detection rate than 18F-FDG PET/CT (93.3 vs. 53.3%, p = 0.005). They further observed that the bone marrow tracer uptake of 68Ga-Pentixafor correlated positively (p < 0.05) with the end organ damage, staging, and laboratory markers of tumor disease burden including serum β2-microglobulin, serum-free light chain, and 24 h urine light chain. They concluded that 68Ga-Pentixafor PET/CT is a promising tracer in the assessment of newly diagnosed MM patients. The application of 68Ga-Pentixafor PET/CT in other hematological malignancies is emerging. In a recent study by Luo et al., the application of 68Ga-Pentixafor PET/CT was expanded in patients with Waldenstrom macroglobulinemia/lymphoplasmacytic lymphoma (WM/LPL) and compared results with 18F-FDG PET/CT [61]. 18F-FDG PET/CT has limitations in the evaluation of WM/LPL which is an indolent B-cell lymphoma and primarily involves the bone marrow. They reported that 68Ga-Pentixafor PET/CT had a higher positive rate for disease detection than 18F-FDG PET/CT (100.0% vs. 58.8%; p = 0.023).
68Ga-Pentixafor PET/CT in a 60-year-old man with mutiple myeloma and diffuse bony pains. PET/CT images show diffuse and focal tracer uptake in the axial and appendicular skeleton (MIP image a), fused PET/CT (trans-axial c, sagittal d) images show diffuse and focal increased tracer uptake in multiple marrow and lytic skeletal lesions. The corresponding 18F-FDG PET/CT images (e, f) did not show any abnormal uptake in marrow and anywhere in the skeleton
31.4 CXCR4-Targeted PET Imaging in Glioblastoma Multiforme (GBM)
Gliomas are the most common primary tumors of the central nervous system (CNS) with a reported annual incidence of 20.5/100,000 [62]. Glioblastoma multiforme (GBM) usually have a infiltrative pattern of growth, and surgery is often incomplete, so radiotherapy with or without concurrent chemotherapy has become part of the current treatment regimens to significantly improve the survival in such patients [63]. In the post-surgery/chemoradiation follow-up of glioma, an accurate identification of the disease recurrence and radiation necrosis is important as the treatment strategy for recurrence warrants a change in treatment, whereas radiation necrosis will require continuation of the standard treatment [64]. So, there is a need for noninvasive imaging techniques for the accurate differentiation of tumor necrosis from recurrence and for response assessment to chemoradiation [65, 66].
Over the past few decades, different amino acid-based PET tracers, such as 18F-fluoro-ethyl-tyrosine (18F-FET), 18F-fluoro-choline (18F-FCH), and 11C-methionine (11C-MET) have been used in targeting various metabolic and molecular pathways that may add valuable diagnostic information especially in clinically challenging situations to improve diagnosis, detect tumor extent, and to help in therapy planning [67]. Among these tracers, 11C-MET is one of the most extensively investigated PET tracers in the diagnostic workup of glioma. 11C-MET accumulates extensively in proliferating tumors by the mechanism of increased amino acid transport and protein synthesis [68]. Undoubtedly, 18F-FDG PET/CT is not of much use in GBM and all other PET tracers have their own limitations in terms of logistical and cumbersome radiolabeling issues. Therefore, alternative tracers which are easy to synthesize and can be made widely available widely with “ready to label” strategies are needed for the accurate detection and postsurgical/chemoradiation follow-up in GBM.
There has been growing evidence that CXCR4 is overexpressed in GBM and is associated with tumor angiogenesis as well as associated with poor survival outcomes [7,8,9, 69, 70]. It has also been shown in animal xenograft models that treatment with CXCR4 antagonist significantly inhibits tumorigenicity and tumor growth and proliferation [71]. The latter suggests that CXCR4 may play a crucial role in promoting the growth of gliomas in humans. Therefore, the CXCR4/CXCL12 axis represents a highly relevant molecular target of cancer biology and offers promising new approaches and techniques for targeted cancer therapy [72, 73].
In a recent study [74], 68Ga-Pentixafor PET/CT was used for the detection of primary/recurrent glioma in 15 patients. In this pilot study, the tracer retention was noted in the vast majority of patients, and histological analysis from the tumor areas with high 68Ga-Pentixafor uptake confirmed the CXCR4 expression. On the other hand, regions of the same tumor without apparent tracer uptake showed no or low receptor expression. Further, in this study, head-to-head comparison with 18F-FET PET/CT in 11/15 cases showed similar SUVmean and SUVmax values of the two tracers; however, the TBR (target-to-background ratio) for SUVmean and SUVmax values were higher for 68Ga-pentixafor by multiples of 37 and 19, thereby resulting in excellent image contrast. It was concluded in this study that 68Ga-Pentixafor PET served as readout for visualization of intracranial CXCR4 expression which might prove as a useful theranostic tool for sensitive noninvasive in vivo quantification of CXCR4 tumor phenotyping. The latter may serve as a useful guide for prognostication and selection of patients who might benefit from CXCR4-directed therapies including β/α radionuclide therapies.
We conducted a pilot study [75] at PGIMER, Chandigarh, India, using 68Ga-Pentixafor PET/CT for quantitative imaging of CXCR4 expression in 28 GBM patients having clinical suspicion of recurrent/residual disease. All the patients received radical radiotherapy (54.0–60.0 Gy) after surgery with or without concurrent temozolomide as indicated and underwent 68Ga-Pentixafor PET/CT and conventional ceMRI of the brain. 68Ga-Pentixafor PET/CT findings with focally increased uptake of the radiotracer were interpreted as positive for recurrent/residual disease in 13/14 patients. The mean SUVmax value in these patients (n = 13) was 5.25 ± 2.07 (range: 2.71–9.69). PET/CT findings were concurrent with MRI findings in all the 14 patients. A representative 68Ga-Pentixafor PET image in a patient (58 yrs., female) with recurrent tumor in central primary GBM disease showing intense uptake of the radiotracer (SUVmax = 7.9) is presented in Fig. 31.4. The only (1/14) patient who had no focal uptake anywhere in the brain on 68Ga-Pentixafor PET was interpreted as negative for any residual/recurrent disease. The ceMRI finding in this patient was also negative and was reported as gliosis. The results of this preliminary study demonstrated that 68Ga-Pentixafor PET imaging in GBM (known to have high CXCR4 expression) is viewed to open up new theranostics applications (with beta and alpha radionuclides) for long-term survival benefits. However, the diagnostic utility of this tracer needs to be validated in a large cohort of patients through multicentric trials.
31.5 Conclusion
CXCR4 and its ligand CXCL12 are intricately involved in the growth and proliferation of both solid tumors as well as hematologic malignancies. Noninvasive assessment of CXCR4 expression by PET/CT imaging can provide a useful tool in the management of a variety of oncologic conditions, both in terms of diagnostic and theranostic capabilities. Solid malignancies such as lung, breast, brain, prostate, and colorectal cancer and hematologic malignancies such as multiple myeloma, Waldenstrom macroglobulinemia, acute and chronic leukemia, and non-Hodgkin’s lymphoma have shown to overexpress CXCR4. Further large and prospectively planned studies can explore the diagnostic performance of 68Ga-Pentixafor PET/CT versus the conventional imaging techniques.
The need of the hour in aggressive malignancies such as glioblastoma multiforme is the development of novel therapies that can prolong survival, improve quality of life, and potentially offer a cure in these patients. Radionuclide therapies, such as intralesional injection of 213Bi-labled substance-P in GBM has shown some promising results [76]. In this context, the increased expression of CXCR4 in GBM has been utilized to develop novel peptide-based theranostics with beta/alpha emitters [77, 78]. This approach may expand our future PRRT armamentarium in GBM healthcare as an alternative to radio-immunotherapy.
References
Mankoff DA, Link JM, Linden HM, Sundararajan L, Krohn KA. Tumor receptor imaging. J Nucl Med. 2008;49(4):149S–63S.
Sarvaiya PJ, Guo D, Ulasov I, Gabikian P, Lesniak MS. Chemokines in tumor progression and metastasis. Oncotarget. 2013;4(12):2171–85.
Furusato B, Mohamed A, Uhlén M, Rhim JS. CXCR4 and cancer. Pathol Int. 2010;60(7):497–505.
Zlotnik A, Burkhardt AM, Homey B. Homeostatic chemokine receptors and organ-specific metastasis. Nat Rev Immunol. 2011;11(9):597–606.
Bleul CC, Farzan M, Choe H, Parolin C, Clark-Lewis I, Sodroski J, et al. The lymphocyte chemoattractant SDF-1 is a ligand for LESTR/fusin and blocks HIV-1 entry. Nature. 1996;382(6594):829–33.
Burger JA, Stewart DJ, Wald O, Peled A. Potential of CXCR4 antagonists for the treatment of metastatic lung cancer. Expert Rev Anticancer Ther. 2011;11(4):621–30.
Balkwill FR. The chemokine system and cancer. J Pathol. 2012;226:48–57.
Fulton AM. The chemokine receptors CXCR4 and CXCR3 in cancer. Curr Oncol Rep. 2009;11:125–31.
Jiang YP, Wu XH, Shi B, Wu WX, Yin GR. Expression of chemokine CXCL12 and its receptor CXCR4 in human epithelial ovarian cancer: an independent prognostic factor for tumor progression. Gynecol Oncol. 2006;103:226–33.
Liao WC, Wang HP, Huang HY, Wu MS, Chiang H, Tien YW, et al. CXCR4 expression predicts early liver recurrence and poor survival after resection of pancreatic adenocarcinoma. Clin Transl Gastroenterol. 2012;3:e22.
Kuil J, Buckle T, van Leeuwen FW. Imaging agents for the chemokine receptor 4 (CXCR4). Chem Soc Rev. 2012;41:5239–61.
Domanska UM, Kruizinga RC, Nagengast WB, Timmer-Bosscha H, Huls G, de Vries EG, et al. A review on CXCR4/CXCL12 axis in oncology: no place to hide. Eur J Cancer. 2013;49(1):219–30.
Nguyen QD, Aboagye EO. Imaging the life and death of tumors in living subjects: preclinical PET imaging of proliferation and apoptosis. Integr Biol. 2010;2:483–95.
Gourni E, Demmer O, Schottelius M, D'Alessandria C, Schulz S, Dijkgraaf I, et al. PET of CXCR4 expression by a (68)Ga-labeled highly specific targeted contrast agent. J Nucl Med. 2011;52(11):1803–10.
Wester HJ, Keller U, Schottelius M, Beer A, Philipp-Abbrederis K, Hoffmann F, et al. Disclosing the CXCR4 expression in lymphoproliferative diseases by targeted molecular imaging. Theranostics. 2015;5(6):618–30.
Herrmann K, Lapa C, Wester HJ, Schottelius M, Schiepers C, Eberlein U, et al. Biodistribution and radiation dosimetry for the chemokine receptor CXCR4-targeting probe 68Ga-Pentixafor. J Nucl Med. 2015;56(3):410–6.
Schultz MK, Donahue P, Musgrave NI, Zhernosekov K, Naidoo K, Razbash A, et al. An increasing role for 68Ga-PET imaging: a perspective on the availability of parent 68Ge material for generator manufacturing in an expanding market. Postgrad Med Edu Res. 2013;47(1):26–30.
Roesch F. Maturation of a key resource - the germanium-68/gallium-68 generator: development and new insights. Curr Radiopharm. 2012;5(3):202–11.
Buchmann I, Henze M, Engelbrecht S, Eisenhut M, Runz A, Schafer M, et al. Comparison of 68Ga-DOTATOC PET and 111In-DTPAOC (Octreoscan) SPECT in patients with neuroendocrine tumours. Eur J Nucl Med Mol Imaging. 2007;34(10):1617–26.
Prata MI. Gallium-68: a new trend in PET Radiopharmacy. Curr Radiopharm. 2012;5(2):142–9.
Vag T, Gerngross C, Herhaus P, Eiber M, Philipp-Abbrederis K, Graner FP, et al. First experience with chemokine receptor CXCR4-targeted PET imaging of patients with solid cancers. J Nucl Med. 2016;57(5):741–6.
Lapa C, Lückerath K, Rudelius M, Schmid JS, Schoene A, Schirbel A, et al. [68Ga]-Pentixafor-PET/CT for imaging of chemokine receptor 4 expression in small cell lung cancer--initial experience. Oncotarget. 2016;7(8):9288–95.
Herrmann K, Schottelius M, Lapa C, Osl T, Poschenrieder A, Hänscheid H, et al. First-in-human experience of CXCR4 directed Endoradiotherapy with 177Lu- and 90Y-labeled Pentixather in advanced-stage multiple myeloma with extensive intra and extramedullary disease. J Nucl Med. 2016;57(2):248–51.
Demmer O, Gourni E, Schumacher U, Kessler H, Wester HJ. PET imaging of CXCR4 receptors in cancer by a new optimized ligand. Chem Med Chem. 2011;6(10):1789–91.
Singh N, Aggarwal AN, Gupta D, Behera D, Jindal SK. Unchanging clinico-epidemiological profile of lung cancer in North India over three decades. Cancer Epidemiol. 2010;34:101–4.
Behera D, Balamugesh T. Lung cancer in India. Indian J Chest Dis Allied Sci. 2004;46:269–81.
Singh N, Aggarwal AN, Gupta D, Behera D, Jindal SK. Quantified smoking status and non-small cell lung cancer stage at presentation: analysis of a north Indian cohort and a systematic review of literature. J Thorac Dis. 2012;4:474–84.
Singh N, Mootha VK, Madan K, Aggarwal AN, Behera D. Tumor cavitation among lung cancer patients receiving first-line chemotherapy at a tertiary care Centre in India: association with histology and overall survival. Med Oncol. 2013;30:602.
Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, 2010. CA Cancer J Clin. 2010;60(5):277–300.
Pao W, Girard N. New driver mutations in non-small-cell lung cancer. Lancet Oncol. 2011;12(2):175–80.
Pao W, Hutchinson KE. Chipping away at the lung cancer genome. Nat Med. 2012;18(3):349–51.
Alberg AJ, Ford JG, Samet JM. Epidemiology of lung cancer: ACCP evidence-based clinical practice guidelines. Chest. 2007;132(3 Suppl):29S–55S.
Siegel R, Desantis C, Virgo K, Stein K, Mariotto A, Smith T, et al. Cancer treatment and survivorship statistics, 2012. CA Cancer J Clin. 2012;62(4):220–41.
Spiro SG, Silvestri GA. One hundred years of lung cancer. Am J Respir Crit Care Med. 2005;172(5):523–9.
Barker JM, Silvestri GA. Lung cancer staging. Curr Opin Pulm Med. 2002;8:287–93.
Cuaron J, Dunphy M, Rimner A. Role of FDG-PET scans in staging, response assessment, and follow-up care for non-small cell lung cancer. Front Oncol. 2013;2:208.
Gupta NC, Graeber GM, Rogers JS, Bishop HA. Comparative efficacy of positron emission tomography with FDG and computed tomographic scanning in preoperative staging of non-small cell lung cancer. Ann Surg. 1999;229:286–91.
Weber WA, Avril N, Schwaiger M. Relevance of positron emission tomography (PET) in oncology. Strahlenther Onkol. 1999;175:356–73.
Marom EM, McAdams HP, Erasmus JJ, Goodman PC, Culhane DK, Coleman RE, et al. Staging non-small cell lung cancer with whole-body PET. Radiology. 1999;212:803–9.
Bhoil A, Singh B, Singh N, Kashyap R, Watts A, Sarika S, et al. Can 3′-deoxy-3′-(18)F-fluorothymidine or 2′-deoxy-2′-(18)F-fluoro-d-glucose PET/CT better assess response after 3-weeks treatment by epidermal growth factor receptor kinase inhibitor, in non-small lung cancer patients? Preliminary results. Hell J Nucl Med. 2014;17(2):90–6.
Sohn HJ, Yang YJ, Ryu JS, Oh SJ, Im KC, Moon DH, et al. 18F-Fluorothymidine positron emission tomography before and 7 days after Gefitinib: treatment predicts response in patients with advanced adenocarcinoma of the lung. Clin Cancer Res. 2008;14:7423–9.
Phillips RJ, Burdick MD, Lutz M, Belperio JA, Keane MP, Strieter RM. The stromal derived factor-1/CXCL12-CXC chemokine receptor 4 biological axis in non-small cell lung cancer metastases. Am J Respir Crit Care Med. 2003;167(12):1676–86.
Hartmann TN, Burger JA, Glodek A, Fujii N, Burger M. CXCR4 chemokine receptor and integrin signaling co-operate in mediating adhesion and chemoresistance in small cell lung cancer (SCLC) cells. Oncogene. 2005;24:4462–47.
Sethi T, Rintoul RC, Moore SM, MacKinnon AC, Salter D, Choo C, et al. Extracellular matrix proteins protect small cell lung cancer cells against apoptosis: a mechanism for small cell lung cancer growth and drug resistance in vivo. Nat Med. 1999;5:662–8.
Spano J, Andre F, Morat L, Sabatier L, Besse B, Combadiere C, et al. Chemokine receptor CXCR4 and early-stage non-small cell lung cancer: pattern of expression and correlation with outcome. Ann Oncol. 2004;15:613–7.
Watts A, Singh B, Basher R, Singh H, Bal A, Kapoor R, et al. 68Ga-Pentixafor PET/CT demonstrating higher CXCR4 density in small cell lung carcinoma than in non-small cell variant. Eur J Nucl Med Mol Imaging. 2017;44(5):909–10.
Watts A, Singh B, Singh H, Bal A, Kaur H, Dhanota N, et al. (68Ga)Ga-Pentixafor PET/CT imaging for in vivo CXCR4 receptor mapping in different lung cancer histologic sub-types: correlation with quantitative receptors’ density by immunochemistry techniques. Eur J Nucl Med Mol Imaging. 2023;50:1216–27.
Raab MS, Podar K, Breitkreutz I, Richardson PG, Anderson KC. Multiple myeloma. Lancet. 2009;374(9686):324–39.
Jemal A, Clegg LX, Ward E, Ries LA, Wu X, Jamison PM, et al. Annual report to the nation on the status of cancer, 1975–2001, with a special feature regarding survival. Cancer. 2004;101(1):3–27.
Hanrahan CJ, Christensen CR, Crim JR. Current concepts in the evaluation of multiple myeloma with MR imaging and FDG PET/CT. Radiographics. 2010;30(1):127–42.
Laubach JP, Mahindra A, Mitsiades CS, Schlossman RL, Munshi NC, Ghobrial IM, et al. The use of novel agents in the treatment of relapsed and refractory multiple myeloma. Leukemia. 2009;23(12):2222–32.
Lütje S, de Rooy JW, Croockewit S, Koedam E, Oyen WJ, Raymakers RA. Role of radiography, MRI and FDG-PET/CT in diagnosing, staging and therapeutical evaluation of patients with multiple myeloma. Ann Hematol. 2009;88(12):1161–8.
Domanska UM, Kruizinga RC, Nagengast WB, Timmer-Bosscha H, Huls G, de Vries EG, Walenkamp AM. A review on CXCR4/CXCL12 axis in oncology: no place to hide. Eur J Cancer. 2013;49(1):219–30.
Bartel TB, Haessler J, Brown TL, Shaughnessy JD, van Rhee F, Anaissie E, et al. F18-fluorodeoxyglucose positron emission tomography in the context of other imaging techniques and prognostic factors in multiple myeloma. Blood. 2009;114(10):2068–76.
Dimitrakopoulou-Strauss A, Hoffmann M, Bergner R, Uppenkamp M, Haberkorn U, Strauss LG. Prediction of progression-free survival in patients with multiple myeloma following anthracycline-based chemotherapy based on dynamic FDG-PET. Clin Nucl Med. 2009;34(9):576–84.
Bredella MA, Steinbach L, Caputo G, Segall G, Hawkins R. Value of FDG PET in the assessment of patients with multiple myeloma. AJR Am J Roentgenol. 2005;184(4):1199–204.
Philipp-Abbrederis K, Herrmann K, Knop S, Schottelius M, Eiber M, Lückerath K, et al. In vivo molecular imaging of chemokine receptor CXCR4 expression in patients with advanced multiple myeloma. EMBO Mol Med. 2015;7(4):477–87.
Lapa C, Schreder M, Schirbel A, Samnick S, Kortüm KM, Herrmann K, et al. [68Ga]Pentixafor-PET/CT for imaging of chemokine receptor CXCR4 expression in multiple myeloma - comparison to [18F]FDG and laboratory values. Theranostics. 2017;7(1):205–12.
Shekhawat AS, Singh B, Malhotra P, et al. Imaging CXCR4 receptors expression for staging multiple myeloma by using 68Ga-Pentixafor PET/CT: comparison with 18F-FDG PET/CT. Br J Radiol. 2022;95:20211272.
Pan Q, Cao X, Luo Y, Li J, Feng J, Li F. Chemokine receptor-4 targeted PET/CT with 68Ga-Pentixafor in assessment of newly diagnosed multiple myeloma: comparison to 18F-FDG PET/CT. Eur J Nucl Med Mol Imaging. 2020;47(3):537–46.
Luo Y, Cao X, Pan Q, Li J, Feng J, Li F. 68Ga-Pentixafor PET/CT for imaging of chemokine receptor 4 expression in Waldenström Macroglobulinemia/Lymphoplasmacytic lymphoma: comparison to 18F-FDG PET/CT. J Nucl Med. 2019;60(12):1724–9.
Jessen KR. Glial cells. Int J Biochem Cell Biol. 2004;36:1861–7.
Ahmed R, Oborski MJ, Hwang M, Lieberman FS, Mountz JM. Malignant gliomas: current perspectives in diagnosis, treatment, and early response assessment using advanced quantitative imaging methods. Cancer Manag Res. 2014;6:149–70.
Parvez K, Parvez A, Zadeh G. The diagnosis and treatment of pseudoprogression, radiation necrosis and brain tumor recurrence. Int J Mol Sci. 2014;15:11832–46.
Kumar AJ, Leeds NE, Fuller GN, Van Tassel P, Maor MH, Sawaya RE, et al. Malignant gliomas: MR imaging spectrum of radiation therapy- and chemotherapy-induced necrosis of the brain after treatment. Radiology. 2000;217:377–84.
Deng SM, Zhang B, Wu YW, Zhang W, Chen YY. Detection of glioma recurrence by 11C-methionine positron emission tomography and dynamic susceptibility contrast-enhanced magnetic resonance imaging: a meta-analysis. Nucl Med Commun. 2013;34:758–66.
Huang C, McConathy J. Radiolabeled amino acids for oncologic imaging. J Nucl Med. 2013;54:1007–10.
Okubo S, Zhen HN, Kawai N, Nishiyama Y, Haba R, Tamiya T. Correlation of L-methyl-11 C-methionine (MET) uptake with L-type amino acid transporter 1 in human gliomas. J Neuro-Oncol. 2010;99:217–25.
Tabouret E, Tchoghandjian A, Denicolai E, Delfino C, Metellus P, Graillon T, et al. Recurrence of glioblastoma after radio-chemotherapy is associated with an angiogenic switch to the CXCL12-CXCR4 pathway. Oncotarget. 2015;6(13):11664–75.
Bian XW, Yang SX, Chen JH, Ping YF, Zhou XD, Wang QL, et al. Preferential expression of chemokine receptor CXCR4 by highly malignant human gliomas and its association with poor patient survival. Neurosurgery. 2007;61(3):570–8.
Rubin JB, Kung AL, Klein RS, Chan JA, Sun Y, Schmidt K, et al. A small-molecule antagonist of CXCR4 inhibits intracranial growth of primary brain tumors. Proc Natl Acad Sci U S A. 2003;100(23):13513–8.
Uy GL, Rettig MP, Motabi IH, McFarland K, Trinkaus KM, Hladnik LM, et al. A phase 1/2 study of chemosensitization with the CXCR4 antagonist plerixafor in relapsed or refractory acute myeloid leukemia. Blood. 2012;119:3917–24.
Kuhne MR, Mulvey T, Belanger B, Chen S, Pan C, Chong C, et al. BMS-936564/MDX-1338: a fully human anti-CXCR4 antibody induces apoptosis in vitro and shows antitumor activity in vivo in hematologic malignancies. Clin Can Res. 2013;19:357–66.
Lapa C, Lückerath K, Kleinlein I, Monoranu CM, Linsenmann T, Kessler AF, et al. (68) Ga-Pentixafor-PET/CT for imaging of chemokine receptor 4 expression in glioblastoma. Theranostics. 2016;6(3):428–34.
Watts A, Arora D, Kumar N, Thakur S, Basher R, Radotra B, et al. 68Ga-Pentixafor PET/CT offers high contrast image for the detection of CXCR4 expression in recurrent glioma. J Nucl Med. 2019;60(suppl 1):491.
Krolicki L, Bruchertseifer F, Kunikowska J, Koziara H, Królicki B, Jakuciński M, et al. Prolonged survival in secondary glioblastoma following local injection of targeted alpha therapy with 213Bi-substance P analogue. Eur J Nucl Med Mol Imaging. 2018;45(9):1636–44.
Schottelius M, Osl T, Poschenrieder A, Hoffmann F, Beykan S, Hänscheid H, et al. [177Lu] -pentixather: comprehensive preclinical characterization of a first CXCR4-directed endoradiotherapeutic agent. Theranostics. 2017;7(9):2350–62.
Buck AK, Stolzenburg A, Hänscheid H, Schirbel A, Lückerath K, Schottelius M, Wester HJ, Lapa C. Chemokine receptor—directed imaging and therapy. Methods. 2017;130:63–71.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2024 The Author(s)
About this chapter
Cite this chapter
Baljinder, S. et al. (2024). CXCR4 Theranostics: A Potential Game Changer in Solid Tumors and Hematological Malignancies. In: Prasad, V. (eds) Beyond Becquerel and Biology to Precision Radiomolecular Oncology: Festschrift in Honor of Richard P. Baum. Springer, Cham. https://doi.org/10.1007/978-3-031-33533-4_31
Download citation
DOI: https://doi.org/10.1007/978-3-031-33533-4_31
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-33532-7
Online ISBN: 978-3-031-33533-4
eBook Packages: MedicineMedicine (R0)