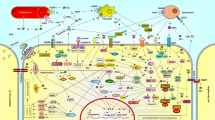
Abstract
This book’s contribution deals with the delicious fruits of the exciting and hard work performed by Prof. Richard Baum and his team in the Zentralklinik Bad Berka, Germany. Herein the fruits from his work as a scientist in the field of theranostics, as a physician in the clinic, and the fruits from a dear friendship are dealt with.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
8.1 Introduction
A small German city named Bad Berka, which is situated in the south of the Weimar region, brought forth many famous people over time. These include both sons and daughters of Bad Berka and those strongly connected to the town (adapted from Wikipedia):
-
Otto Fries (1849–1905), politician National Liberal Party (Germany), member of Reichstag
-
Hugo Günther (1891–1954), party functionary (SPD/KPD/KPO/SED) and insurance director
-
Hans Carl Nipperdey (1895–1968), law professor, first president of the Federal Labour Court
-
Hartmut Griesmayr (born 1945), screenwriter and director
-
Johann Wolfgang von Goethe (1749–1832), writer, stayed there often as a bathing guest
-
Jakob Michael Reinhold Lenz (1751–1792), poet of Sturm und Drang
-
Dietrich Georg von Kieser (1779–1862), medical doctor, worked as a physician in Berka
-
Adolf Brütt (1855–1939), sculptor, worked in Bad Berka, since 1928 honorary citizen
-
Martin Hellberg (1905–1999), author, actor and director
-
Henry Augustus Siebrecht, florist, “Father of Fifth Avenue”
-
Richard Baum, professor, physician, and scientist, Chef of the clinic for Molecular Radiotherapy at the Zentralklinik Bad Berka
The last person on this list, Prof. Richard Baum, is quite a special person. To describe him, I thought of a metaphor and expression taken from the bible (Luke 6:43-44): “An der Frucht erkennt man den Baum”. That is because Richard Baum reminds me of a cherry tree; a firm tree, a highlight in the garden, solidly rooted in fertile ground, self-pollinating, but benefitting from other trees in the garden, and rich in delicious fruits that come in pairs. Paired fruits refer here to the field of theranostics (see below). For this contribution, I chose three themes:
-
Fruits of Scientist Baum
-
Fruits of Physician Baum
-
Fruits of Friend Baum
8.2 Fruits of Scientist Baum
Radiolabeled somatostatin analogs were introduced more than 20 years ago for theranostics of patients with somatostatin receptor (especially subtype 2) expressing neuroendocrine tumors. After injection into the body these small somatostatin peptide analogs can guide attached radioactivity to their target receptors overexpressed on tumor cells, enabling imaging or radionuclide therapy, dependent on the radionuclide of choice.
A few years later, the first clinical studies were carried out, also paving the way for the development of a variety of different radiolabeled peptide analogs for the diagnosis and treatment of tumors in many collaborative studies [1,2,3,4,5,6,7,8,9,10] (review: 11). Promising radiolabeled analogs used for positron emission tomography (PET) or peptide receptor radiotherapy (PRRT) include peptides targeting somatostatin receptors (SSTR), integrins, chemokine receptors, fibroblast activating protein (FAP), gastrin-releasing peptide receptor (GRPR), or the prostate-specific membrane antigen (PSMA) [11]. They are excellent examples of so-called theranostics, a combination of the terms therapeutics and diagnostics. It refers to the combination of a paired diagnostic/imaging tool or tracer used to identify a second tool (which may in fact be the same tracer now radiolabeled with a therapeutic radionuclide) for therapy, like the paired cherries in the cherry tree. Using this concept, “We can see what we treat and we can treat what we see”. Theranostics comprise an interesting part of personalized or precision medicine: “The right treatment for the right patient at the right time and at the right dose”.
Radiolabeled small peptides are an important class of radiopharmaceuticals applied for diagnosis and therapy of tumors. These small compounds possess beneficial properties as targeting probes in nuclear medicine: they are not immunogenic and show fast diffusion and target localization. Additionally, peptides can be easily modified, improving metabolic stability and adjusting favorable pharmacokinetics. In contrast to small molecular weight compounds, peptides are more tolerant of modifications. Because of the presence of endogenous enzymes (peptidases) for the degradation of peptides and proteins, the major disadvantage of peptides compared to small molecular mass probes could be the lower metabolic stability. A variety of strategies can overcome this problem, including the introduction of unnatural amino acids, backbone cyclization, modifications, and the use of peptidase inhibitors [11, 12]. A relatively easy strategy for stability improvement toward peptidases is the application of d-amino acids or unnatural amino acids. In many cases, a combination of N/C-terminal modification with stabilization via d-amino acids or unnatural amino acids is used, as described for Tyr3-octreotide or different RGD-derivatives. For a variety of tracers, backbone cyclization could be combined with the introduction of d-amino acids. However, not all amino acids in a sequence can be replaced either by the corresponding d-amino acid or by an unnatural amino acid without influencing the binding affinity. So, for another pathway to stabilize peptides, we hypothesized that the in vivo co-administration of specific enzyme inhibitors would improve peptide bioavailability and hence tumor uptake. Through single coinjection of the neutral endopeptidase inhibitor phosphoramidon (PA), we indeed were able to provoke remarkable rises in the percentages of circulating intact somatostatin, gastrin, and bombesin radiopeptides in mouse models, resulting in a clear increase in uptake in tumor xenografts in mice [12]. These approaches have also been applied in our collaborative research with Prof. Baum, resulting in the following fruits:
Gastrin-releasing peptide receptors (GRPR) represent attractive targets for tumor diagnosis and therapy because of their overexpression in major human cancers. Internalizing GRPR agonists were initially proposed for prolonged lesion retention, but a shift of paradigm to GRPR antagonists has been made, as radioantagonists, such as 99mTcDB1 (99mTc-N4′-DPhe(6),Leu-NHEt(13)]BBN(6-13)), displayed better pharmacokinetics than radioagonists, in addition to their higher biosafety. We introduced 68GaSB3, a 99mTc-DB1 mimic, carrying the chelator DOTA for labeling with the PET radiometal 68Ga. SB3 and [(nat)Ga]SB3 bound to the human GRPR with high affinity, plus 67GaSB3 displayed good in vivo stability. 67GaSB3 showed high, GRPR-specific and prolonged retention in PC-3 xenografts in mice, but much faster clearance from the GRPR-rich pancreas. In patients in Bad Berka, 68GaSB3 clearly visualized cancer lesions without adverse effects. Thus, 4 out of 8 breast cancer and 5 out of 9 prostate cancer patients showed pathological uptake on PET/CT. We concluded imaging with 68GaSB3 to be promising in patients with primary breast or prostate cancer [13]. Afterward, we introduced, by replacement of the C-terminal Leu13-Met14-NH2 dipeptide of SB3 by Sta13-Leu14-NH2, the novel GRPR antagonist NeoBOMB1, labeled with different radiometals for theranostic use. NeoBOMB1 and natGa-, natIn-, and natLu-NeoBOMB1 bound again to GRPR with high affinity. They showed excellent metabolic stability in peripheral mouse blood. After injection in mice, all 3 tracers (67Ga-, 111In-, and 177Lu-NeoBOMB1) showed comparably high and GRPR-specific uptake in the PC-3 xenografts. During a translational study in prostate cancer patients, 68Ga-NeoBOMB1 rapidly localized in pathologic lesions, achieving high-contrast imaging, so the GRPR antagonist radioligands 67Ga-, 111In-, and 177Lu-NeoBOMB1, independent of the radiometal applied, have shown comparable and most promising behavior in prostate cancer models and patients, in favor of future theranostic use in GRPR-positive cancer patients [14].
In another series of collaborative studies, we focused on the use of the potent alpha emitter bismuth-213 for radionuclide therapy [15,16,17,18]. So, we optimized the labeling conditions of 213Bi-DOTATATE for preclinical applications of peptide receptor-targeted alpha therapy plus we evaluated whether 213Bi-DOTATATE was suitable for the treatment of both larger neuroendocrine tumors overexpressing SSTR2 in comparison to its effectiveness in smaller tumors. Based on the results of the studies we concluded that 213Bi-DOTATATE demonstrated a great therapeutic effect in both small and larger tumor lesions, whereas higher probability for stable disease was found in animals with small tumors.
In the text above, beautiful examples of translational research, from bench to bedside, have been shown. To further improve translational research, sophisticated cancer models are now available to address cancer-related research questions. Technological developments in probe synthesis and labeling have resulted in most promising imaging and therapeutic probes with the potential for basic research, as well as for translational and clinical applications. Moreover, translational collaborative studies as referred to above have shown that developments and improvements of multimodal imaging methods for use in animal research have substantially strengthened the field of preclinical theranostics. Improvements in all these research fields improved rapid translation of new therapies into the clinic [19].
We conclude that the future of radiopharmaceuticals for imaging and therapy is radiant. The field of theranostics will flourish even more when applying novel intra-arterial applications, targeting antagonists with better-targeting profiles, the application of novel radionuclides, including the powerful alpha emitters, and combination therapies.
8.3 Fruits of Doctor Baum
In Bad Berka, Prof. Baum and his team apply theranostics in cancer patients from all over the world with great success. Prof. Baum arrived in Bad Berka in 1997 to initiate a Nuclear Medicine department there; in the meantime, it became very well known for the application of theranostics. It has developed to an ENETS Center of Excellence where patients from many different parts of the world are being treated using PRRT with beta and alpha particle emitting radionuclides. PRRT is now approved by the European Medical Agency (EMA) and the Food and Drug Administration (FDA). In Bad Berka, around 1000 therapies are given each year in the large station with 22 beds. Not only patients with neuroendocrine tumors are being treated with PRRT, also patients suffering from other tumor types, like e.g. prostate cancer, can be treated now using novel theranostics, which is great news for all kinds of patients suffering from these cancers.
Prof. Baum is highly respected by his co-workers and patients, which is very understandable and well deserved, considering his enormous work load, enthusiasm, and drive to do the best possible for every patient. From the picture in Fig. 8.1 we can also clearly witness this. The successful theranostic work in Bad Berka is based on team work; like a cherry tree Prof. Baum can be self-pollinating, but he strongly benefits from fertile ground and the presence of other cherry trees around him.
8.3.1 Fruits of Our Friend Baum
Prof. Baum is a great colleague and friend, a treasure in our theranostic garden like a beautiful cherry tree: being considerate, very helpful, a source of inspiration, always in for a challenge, cheerful, and enthusiastic, albeit also demanding and ambitious. We both very much enjoyed the start of the theranostic adventure and I appreciate our collaborations, even though we worked in different steps of the development and introduction of new theranostic radiopharmaceuticals.
Now it is time for a new adventure: Prof. Baum will start the Theranostics Center for Radiomolecular Precision Oncology in Wiesbaden: Richard, I wish you all the best and please continue the good work!
References
Bodei L, Kidd M, Modlin IM, Prasad V, Severi S, Ambrosini V, et al. Gene transcript analysis blood values correlate with (6)(8)Ga-DOTA-somatostatin analog (SSA) PET/CT imaging in neuroendocrine tumors and can define disease status. Eur J Nucl Med Mol Imaging. 2015;42(9):1341–52.
Bodei L, Kidd M, Modlin IM, Severi S, Drozdov I, Nicolini S, et al. Measurement of circulating transcripts and gene cluster analysis predicts and defines therapeutic efficacy of peptide receptor radionuclide therapy (PRRT) in neuroendocrine tumors. Eur J Nucl Med Mol Imaging. 2016;43(5):839–51.
Bodei L, Kidd M, Paganelli G, Grana CM, Drozdov I, Cremonesi M, et al. Long-term tolerability of PRRT in 807 patients with neuroendocrine tumours: the value and limitations of clinical factors. Eur J Nucl Med Mol Imaging. 2015;42(1):5–19.
Bodei L, Kidd MS, Singh A, van der Zwan WA, Severi S, Drozdov IA, et al. PRRT genomic signature in blood for prediction of (177)Lu-octreotate efficacy. Eur J Nucl Med Mol Imaging. 2018;45(7):1155–69.
Bodei L, Kidd MS, Singh A, van der Zwan WA, Severi S, Drozdov IA, et al. PRRT neuroendocrine tumor response monitored using circulating transcript analysis: the NETest. Eur J Nucl Med Mol Imaging. 2020;47(4):895–906.
Caplin M, Sundin A, Nillson O, Baum RP, Klose KJ, Kelestimur F, et al. ENETS Consensus Guidelines for the management of patients with digestive neuroendocrine neoplasms: colorectal neuroendocrine neoplasms. Neuroendocrinology. 2012;95(2):88–97.
Oberg K, Krenning E, Sundin A, Bodei L, Kidd M, Tesselaar M, et al. A Delphic consensus assessment: imaging and biomarkers in gastroenteropancreatic neuroendocrine tumor disease management. Endocr Connect. 2016;5(5):174–87.
Strosberg J, El-Haddad G, Wolin E, Hendifar A, Yao J, Chasen B, et al. Phase 3 trial of (177)Lu-dotatate for midgut neuroendocrine tumors. N Engl J Med. 2017;376(2):125–35.
Strosberg J, Kunz PL, Hendifar A, Yao J, Bushnell D, Kulke MH, et al. Impact of liver tumour burden, alkaline phosphatase elevation, and target lesion size on treatment outcomes with (177)Lu-Dotatate: an analysis of the NETTER-1 study. Eur J Nucl Med Mol Imaging. 2020;47(10):2372–82.
Strosberg J, Wolin E, Chasen B, Kulke M, Bushnell D, Caplin M, et al. Health-related quality of life in patients with progressive midgut neuroendocrine tumors treated with (177)Lu-dotatate in the phase III NETTER-1 trial. J Clin Oncol. 2018;36(25):2578–84.
Rangger C, Haubner R. Radiolabelled peptides for positron emission tomography and endoradiotherapy in oncology. Pharmaceuticals. 2020;13(2):22.
Nock BA, Maina T, Krenning EP, de Jong M. “To serve and protect”: enzyme inhibitors as radiopeptide escorts promote tumor targeting. J Nucl Med. 2014;55(1):121–7.
Maina T, Bergsma H, Kulkarni HR, Mueller D, Charalambidis D, Krenning EP, et al. Preclinical and first clinical experience with the gastrin-releasing peptide receptor-antagonist [(6)(8)Ga]SB3 and PET/CT. Eur J Nucl Med Mol Imaging. 2016;43(5):964–73.
Nock BA, Kaloudi A, Lymperis E, Giarika A, Kulkarni HR, Klette I, et al. Theranostic perspectives in prostate cancer with the gastrin-releasing peptide receptor antagonist NeoBOMB1: preclinical and first clinical results. J Nucl Med. 2017;58(1):75–80.
Chan HS, de Blois E, Konijnenberg MW, Morgenstern A, Bruchertseifer F, Norenberg JP, et al. Optimizing labelling conditions of (213)Bi-DOTATATE for preclinical applications of peptide receptor targeted alpha therapy. EJNMMI Radiopharm Chem. 2017;1(1):9.
Chan HS, de Blois E, Morgenstern A, Bruchertseifer F, de Jong M, Breeman W, et al. In vitro comparison of 213Bi- and 177Lu-radiation for peptide receptor radionuclide therapy. PLoS One. 2017;12(7):e0181473.
Chan HS, Konijnenberg MW, Daniels T, Nysus M, Makvandi M, de Blois E, et al. Improved safety and efficacy of (213)Bi-DOTATATE-targeted alpha therapy of somatostatin receptor-expressing neuroendocrine tumors in mice pre-treated with L-lysine. EJNMMI Res. 2016;6(1):83.
Chan HS, Konijnenberg MW, de Blois E, Koelewijn S, Baum RP, Morgenstern A, et al. Influence of tumour size on the efficacy of targeted alpha therapy with (213)Bi-[DOTA(0),Tyr(3)]-octreotate. EJNMMI Res. 2016;6(1):6.
de Jong M, Essers J, van Weerden WM. Imaging preclinical tumour models: improving translational power. Nat Rev Cancer. 2014;14(7):481–93.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2024 The Author(s)
About this chapter
Cite this chapter
de Jong, M. (2024). A Tree Can Be Recognized by Its Fruit. In: Prasad, V. (eds) Beyond Becquerel and Biology to Precision Radiomolecular Oncology: Festschrift in Honor of Richard P. Baum. Springer, Cham. https://doi.org/10.1007/978-3-031-33533-4_8
Download citation
DOI: https://doi.org/10.1007/978-3-031-33533-4_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-33532-7
Online ISBN: 978-3-031-33533-4
eBook Packages: MedicineMedicine (R0)