Abstract
The cause of fetal death by sulfonylureas (SUs), used for diabetes in pregnancy in the early 1960s, remained unsolved for decades. In 1993, Nakanishi discovered constriction of ductus arteriosus (DA) strips in rabbit fetuses with glibenclamide, a SU and inhibitor of the KATP channel. Later, Momma showed dose-dependent fetal DA constriction by glibenclamide injected directly into the fetus in rats. Every first-generation SU constricted the fetal DA by oral administration to the pregnant rat. DA constriction with the clinical dose of these SUs was mild, whereas a 100 times larger dose was needed to close the DA completely. Coadministration of SUs and cylooxygenase inhibitors caused additive severe constriction and complete closure of the fetal DA. These data suggested that the aforementioned high fetal death rate (63% in 1962) with chlorpropamide was due to the coadministration of this SU and aspirin-like drugs.
You have full access to this open access chapter, Download conference paper PDF
Similar content being viewed by others
Keywords
- Ductus arteriosus
- KATP channel inhibitor
- Glibenclamide
- Sulfonylurea
- Premature closure of ductus arteriosus
1 Transplacental Fetal Death by Sulfonylureas
Sulfonylureas (SUs) were used for diabetes treatment in the early 1950s. In 1962, it was reported from South Africa that chlorpropamide, a first-generation SU (an inhibitor of the KATP channel) administered to diabetic pregnant women caused 63% fetal death rate during the latter half of gestation [1]. Fetal autopsies revealed no malformations and the mechanism of death remained uncertain. In 1964, a survey of diabetic pregnant patients in the United Kingdom confirmed the association of chlorpropamide and tolbutamide with fetal death. Although the mechanism of fetal death was unknown, the use of these SUs became contraindicated during pregnancy from then onward.
2 Closure of Fetal Ductus Arteriosus with Non-Steroidal Anti-Inflammatory Drugs
Aspirin was discovered in 1901. Cardiac catheterization and angiography was the major cardiovascular diagnostic methods in the 1960s. In 1969, the first case of transplacental premature fetal DA closure was reported by Arcilla [2]. In this case, a full-term mother had severe arthritis and she took massive doses of salicylates for 11 days. The neonate was severely cyanotic, and cardiac catheterization and angiography at 4 h postpartum revealed pulmonary hypertension, atrial right-to-left shunting, and a closed DA at the aortic end. Since 1978, we studied fetal rat DA with a rapid whole-body freezing method, and we showed transplacental constriction of the fetal DA with all 50 non-steroidal anti-inflammatory drugs (NSAIDs) [3,4,5] (Fig. 36.1). Experimentally, constriction was absent in mid-gestation, but it increased in late gestation [6].
Fetal DA diameters following orogastric administration of non-steroidal anti-inflammatory drugs to the near-term rat. Time course of fetal DA constriction by 14 mg/kg Acetoaminophen (black squares) and 14 mg/kg Aspirin (white squares), 0.7 mg/kg Indomethacin (black circles), and 6 mg/kg Ibuprofen (white circles) to d21 pregnant rats (mean ± SEM)
3 Constriction of Ductus Arteriosus with Glibenclamide
In 1993, Nakanishi discovered constriction of DA strips in rabbit fetuses with glibenclamide, a second-generation SU and inhibitor of the KATP channel. Glibenclamide passed into the placenta slowly [7]. Since 2012, we studied direct intraperitoneal injection of glibenclamide into the rat fetus and demonstrated dose-dependent DA constriction in the preterm and term fetus [8]. The DA constriction with the clinical doses was mild, and the DA inner diameter decreased to 70% in 30 min. The DA closed completely with a 100 times larger dose compared to the clinical dose (Figs. 36.2 and 36.3).
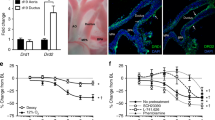
Frontal sections of the frozen rat fetus through aortic arch (Ao), ductus arteriosus (DA), and right and left pulmonary artery (RPA, LPA). The inner diameter of the Ao, DA, and main pulmonary artery (PA) were 0.8 mm, respectively. The DA/PA ratio was 1.0 in the control (a). A large dose (100 mg/kg, injected into the fetal abdomen) of glibenclamide constricted the DA severely in 30 min, the DA inner diameter diminished to 0.1 mm, and the DA/PA ratio was 0.1 (b)
Time courses of fetal DA constriction with maternal orogastric administration of chlorpropamide (a), and those with fetal intraperitoneal injection of glibenclamide (b) in rats. Time course of fetal DA constriction in rats exposed to chlorpromide, 1 mg/kg (black squares), 10 mg/kg (white squares), 100 mg/kg (black circles), and 1000 mg (white circles) (mean ± SEM)
4 Constriction of Fetal DA with Other Sulfonylureas
Since 2010, we demonstrated transplacental constriction of the fetal DA with first-generation sulfonylureas in the rat model (Table 36.1). Every SU constricted the fetal DA mildly in 4 h after orogastric administration of the drug to the near-term rats. The fetal DA constriction was severe, or the DA closed completely with 100 times larger doses (Table 36.1). Rat fetuses survived with clinical doses of SUs with associated mild DA constriction, whereas fetal death increased with closure of the DA. Severe DA constriction with 100 times larger doses of SUs persisted up to 24 h later.
5 Fetal DA Closure with Combined Administration of Cyclooxygenase Inhibitors and SUs
We studied the combined effects of indomethacin and glibenclamide in the fetal DA model (Fig. 36.4). Indomethacin (0.1, 1, and 10 mg/kg) was administered orogastrically to 19th day and 21st day rats. Glibenclamide (1 mg/kg) was administered to the fetus at 3 h, and the fetal DA was studied at 4 h. As shown in Fig. 36.4, indomethacin and glibenclamide constricted the DA additively. These data suggest that the aforementioned high fetal death rate with chlorpropamide was due to the additional intake of cyclooxygenase inhibitors (COX-I), used as analgesics and antipyretics, combined with the SU effects of KATP channel inhibition.
Fetal rat DA constriction in 4 h with three doses, 0.1 mg/kg (white circles), 1 mg/kg (white diamonds), and 10 mg/kg (white squares)、of indomethacin with orogastric administration to preterm rats on the 19th day (a) and to near-term rats on 21st day (b). Glibenclamide (1 mg/kg) was injected to the fetus intraperitoneally at 3 h after administration of indomethacin
6 Early Fetal Exposure to COX-I
Fetal DA contractility in the presence of oxygen is the basic mechanism of neonatal DA closure. In 1986, we discovered in rat experiments the following paradoxical phenomenon: early exposure to COX-Is impaired fetal DA contractility to late administration of COX-Is or oxygen, respectively [9]. The same phenomenon was reported in clinical patent DA in premature infants [10]. The molecular mechanism of this paradox was only clarified recently [11, 12]. We created a rat model with this paradox [13]: the fetal rats with exposure to large doses of indomethacin during the latter 30% of the total fetal gestational period showed much reduced DA contractility. Moreover, they showed eight times slower DA closure in the postpartum period. In this fetus model, DA constriction with glibenclamide was weak, and the DA constricted only moderately with a large dose (1000 mg/kg) of glibenclamide.
7 Effects of Massive Doses of Glibenclamide in Newborn Rat
As is shown in Fig. 36.3, glibenclamide constricted the fetal DA only mildly with clinical doses, and closed the DA completely with massive doses. The effects of massive doses of glibenclamide were studied with orogastric administration in one-day-old newborn rats under maternal nursing. Large doses of glibenclamide (100 mg and 1000 mg/kg) were well tolerated, and more than 90% of these rats survived with normal weight gain up to 3 weeks. Severe hypoglycemia, as low as 30 mg/dL of plasma glucose, developed and persisted for up to 3 days. The hypoglycemia was treated with large doses of orogastric glucose. Laboratory tests at 1 day after glibenclamide administration revealed hypoglycemia, but other parameters were normal.
8 Future Direction and Clinical Implications
Recent studies of cord bloods at birth in neonates of diabetic mothers with glibenclamide treatment revealed the presence of the drug in concentrations at about 50% of the maternal levels [14]. This suggests mild DA constriction and increased risk of premature DA closure in the fetus of mothers treated with glibenclamide. The clinical application of glibenclamide to close patent DA in premature infants is difficult because of the associated prolonged hypoglycemia when used in large doses, and a decreased constrictive effect in DA with early exposure to COX-Is.
References
Jackson WPU, Campbell GD, Noteloviz M. Tolbutamide and chlorpropamide during pregnancy in human diabetes. Diabetes. 1962;11(Suppl):98–101.
Archilla RA, Thilenius OG, Ranniger K. Congestive heart failure from suspected ductus closure in utero. J Pediatr. 1969;75:74–8.
Momma K, Takeuchi H. Constriction of fetal ductus arteriosus by non-steroidal anti-inflammatory drugs. Prostaglandins. 1983;26:631–43.
Momma K, Hagiwara H, Konishi T. Constriction of fetal ductus arteriosus by non-steroidal anti-inflammatory drugs. Study of additional 34 drugs. Prostaglandins. 1984;28:527–36.
Momma K, Takao. Transplacental cardiovascular effects of four popular analgesics in rats. Am J Obstet Gynecol. 1990;162:1304–10.
Momma K, Takao A. In vivo constriction of the ductus arteriosus by non-steroidal anti-inflammatory drugs in near-term and preterm fetal rats. Pediatr Res. 1987;22:567–72.
Nakanishi T, Gu H, Hagiwara N, et al. Mechanisms of oxygen-induced contraction of ductus arteriosus isolated from the fetal rabbit. Circ Res. 1993;72:1218–28.
Momma K, Monma M, Toyoshima K, et al. Fetal and neonatal ductus arteriosus is regulated with ATP-sensitive potassium channel. In: Nakanishi T, et al., editors. Etiology and morphogenesis of congenital heart disease. Tokyo: Springer Japan; 2016. p. 263–5.
Konishi T, Momma K, Takao A. Inhibited maturation of fetal ductus arteriosus by indomethacin in rats. Jpn J Neonatol. 1986;22:430–5.. (in Japanese).
Norton ME, Merrill J, Cooper BAB, et al. Neonatal complication after the administration of indomethacin for preterm labor. N Engl J Med. 1993;329:1602–7.
Yokoyama U, Minamisawa S, Quan H, et al. Chronic activation of the prostaglandin receptor EP4 promotes hyaluronan-mediated neointimal formation in the ductus arteriosus. J Clin Invest. 2006;116:3026–34.
Reese J, Waleh SD, Poole SD, et al. Chronic in utero cyclooxygenase inhibition alters PGE2-regulated ductus arteriosus contractile pathways and prevents postnatal closure. Pediatr Res. 2009;66:155–61.
Momma K, Toyoshima K, Ito K, et al. Delayed neonatal closure of the ductus arteriosus following early in utero exposure to indomethacin in the rat. Neonatology. 2007;96:69–79.
Schwartz RA, Rosenn B, Katarina A, et al. Glyburide transport across the human placenta. Obstet Gynecol. 2015;125:583–8.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2020 The Author(s)
About this paper
Cite this paper
Momma, K., Toyoshima, K., Hayama, E., Nakanishi, T. (2020). Constriction of the Ductus Arteriosus with KATP Channel Inhibitors. In: Nakanishi, T., Baldwin, H., Fineman, J., Yamagishi, H. (eds) Molecular Mechanism of Congenital Heart Disease and Pulmonary Hypertension. Springer, Singapore. https://doi.org/10.1007/978-981-15-1185-1_36
Download citation
DOI: https://doi.org/10.1007/978-981-15-1185-1_36
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-15-1184-4
Online ISBN: 978-981-15-1185-1
eBook Packages: MedicineMedicine (R0)