Abstract
Background
Due to a limited patient sample size, substantial data on robotic rectal resection (RRR) is lacking. Here, we reported a large consecutive cases from the real word data to assess the safety and efficacy of RRR.
Methods
From September 2010 to June 2017, a total of 1145 consecutive RRR procedures were performed in patients with stage I–IV disease. We conducted an analysis based on information from a prospectively designed database to evaluate surgical outcomes, urogenital function, and long-term oncological outcomes.
Results
Of three types of RRR performed, 227 (24.2%) were abdominoperineal resections, 865 (75.5%) were anterior resections, and 3 (0.3%) were Hartmann. Conversion to an open procedure occurred in 5.9% of patients. The overall positive circumferential margin rate was 1.3%. Surgical complication rate and mortality were 16.2% and 0.8% within 30 days of surgery, respectively. Mean hospital stay after surgery and hospital cost were 6.3 ± 2.9 days and 10442.5 ± 3321.5 US dollars, respectively. Risk factors for surgical complications included male gender, tumor location (mid-low rectum), combined organ resection, and clinical T category (cT3–4). Urinary function and general sexual satisfaction decreased significantly 1 month after surgery for both sexes. Subsequently, both parameters increased progressively, and the values 1 year after surgery were comparable to those measured before surgery. At a median follow-up of 34.6 months, local recurrence and distant metastases occurred in 2.3% and 21.1% of patients, respectively.
Conclusions
Robotic rectal resection was safe with preserved urogenital function and arrived equivalent oncological outcomes in a nonselected group of patients with rectal cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
A robotic approach with superior dexterity and precise movements of the robotic arms provides the surgeon with better exposure and greater ergonomic comfort during dissection of small anatomical structures [1, 2]. Robotic rectal resection (RRR) has been proven to be a valid option with a lower open conversion rate than that of conventional laparoscopy for patients with rectal cancer [3]. Furthermore, robotic total mesorectal excision may overcome some difficulties associated with conventional laparoscopic rectal resection (LRR) [4] primarily in patients with mid-low rectal cancer [5]. However, the benefit of robotic rectal resection for urogenital function protection and oncologic outcomes remains controversial due to the limited sample size in reported studies [6, 7].
Previous studies show LRR is associated with similar [8] or higher [9] rates of sexual and urinary dysfunction compared to open rectal resection (ORR). The incidence of urinary and sexual complications after RRR is still not well known. Limited data indicated robotic total mesorectal excision (TME) may allow for better preservation of urinary and sexual functions when compared with both ORR and LRR [10]. Furthermore, regarding oncological outcomes of RRR, based on evidence from a limited number of cases and initial experiences, substantive data are still lacking [11]. Few centers worldwide have the capacity to perform real world large-scale studies of RRR because of low-volume sample sizes. However, colorectal surgeons at Zhongshan Hospital were early adopters of RRR and have performed more than 1700 such procedures in a nonselected group of patients with rectal tumors.
The purpose of this study was to define the safety and function preservation of the robotic rectal surgery base on a real-world database from a single center over an 8-year period in China. The surgical complication and risk factors, sexual and urinary function, and long-term oncological outcomes are described in this study.
Materials and methods
Patients
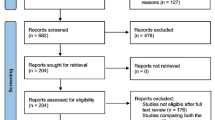
From September 2010 to June 2017, a total of 1211 consecutive patients are slated to undergo robotic rectal resection (RRR) with the Da Vinci S or Da Vinci Si Robot Surgical System. Of those, the robotic procedure was canceled in 66 cases after laparoscopic exploration revealed severe abdominal adhesions and intraperitoneal tumor dissemination. Ultimately, data from 1145 patients who underwent RRR were analyzed for this study. Patients were admitted to the study regardless of sex, age, AJCC/UICC (American Joint Committee on Cancer/Union for International Cancer Control) stage, type of intervention performed, or history of previous abdominal surgery. Data from patient hospital records were prospectively collected in a predesigned Excel file. Other clinical data were collected from computerized and archived patient charts. Postoperative data as well as surgical complications (30-day morbidity and mortality), sexual function, urinary function, and long-term oncological outcomes were assessed during follow-up.
A positive circumferential resection margin was defined as ≤ 1 mm from the specimen surface to the primary tumor or any tumor deposit. [12] Dissection planes are registered according to the description by Quirke. [13] The postoperative complications were defined as adverse events that occurred within 30 days after surgery. Complications were diagnosed and categorized according to patients’ symptoms, with the aid of laboratory and radiological evaluation to confirm clinical suspicions. Grading of complications was scored based on the detailed tables of the Surgical Complications Severity Scoring System proposed by Mazeh et al. [14].
The study was approved by the Fudan University Ethics Committee, and all patients were asked to provide informed consent. Urinary and sexual dysfunctions affecting quality of life (QoL) were assessed by means of specific self-administered questionnaires in all patients undergoing robotic TME. For evaluating urinary tract symptoms and the impact on QoL, the International Consultation on Incontinence Male/Female Lower Urinary Tract Symptoms questionnaires (ICIQ-FLUTS and ICIQ-MLUTS) were used [15]. Each module uses a common question format. Most questions use 5-point Likert scales to assess the presence or absence of a symptom and its severity, followed by a scale to assess the associated degree of bother, which is measured by a visual analog scale. For assessing male sexual function, the International Index of Erectile Function (IIEF) questionnaire [16] was adopted, and for female sexual function, the Female Sexual Function Index (FSFI) questionnaire [17] was adopted. These are 15-item self-administered questionnaires that analyze five factors: erectile function (sexual function for female), orgasmic function, sexual desire, intercourse satisfaction, and overall satisfaction. All of these questionnaires can effectively assess urinary and sexual function after prostate cancer [18] and rectal surgery [19, 20] as reported previously.
Robotic rectal resection
The single-docking technique with four or five ports was used as described in our previous studies [21]. We performed the high dissection and low ligation for lymph node dissection and preserved the left colic artery in most patients. The splenic flexure of the colon was not routinely mobilized, depending on the tension of the anastomosis. Once the sigmoid colon, mesocolon, entire rectum, and mesorectum were mobilized completely, anterior resection (AR) with the double-staple technique or abdominoperineal resection (APR) was performed accordingly.
We routinely used a standardized approach to prevent anastomotic leakage (AL) for mid-low rectal tumors, which included preserving the left colonic artery to improve the blood supply to the anastomosis. A transanal drainage tube was placed to reduce anastomotic tension in patients with robotic LAR. A diversion stoma was not routinely performed except in those patients at a substantial risk of AL. If the anastomosis was below the peritoneal reflex, the dissected pelvic peritoneum was sutured to avoid leakage of feces, which could cause intraperitoneal peritonitis following AL. At the same time, a double cannula was placed near the anastomosis to monitor the occurrence of AL. When AL occurred, the double cannula located near the anastomoses could be used to wash and drain the feces, promote anastomotic healing, and avoid a salvage ileostomy.
Statistical analysis
Statistical analysis was conducted with IBM SPSS Statistics software version 19 (SPSS Inc., IBM, Chicago, IL, USA). Categorical variables were analyzed using the χ2 test, and continuous variables were analyzed using the Student t test. The nonparametric Kruskal–Wallis test was employed to compare the qualitative variables for urinary and sexual function analysis. One-way analysis of variance with least significant difference multiple comparisons was used for analysis of quantitative differences between multiple groups. A logistic regression was used for multivariate analysis. Overall survival was calculated using the Kaplan–Meier method. P values less than 0.05 were considered statistically significant.
Results
Perioperative and pathological data
The 1145 patients who underwent robotic rectal resections (RRR) are summarized in Table 1. Briefly, they included 714 (62.4%) males and 431 (37.6%) females. The median age and body mass index (BMI) were 63 years (range 24–91) and 23.1 kg/m2 (range 15.1–35.0), respectively. A total of 138 (12.1%) patients are considered to have American Society of Anesthesiologists scores (ASA) of III–IV, 231 (20.2%) patients had a history of abdominal surgery, and 516 (45.1%) patients had comorbidities.
Tumor locations are detailed in Table 2. There were 367 (32.1%) patients with upper rectal tumors, 423 (36.9%) with middle rectal tumors, and 355 (31.0%) with low rectal tumors. Anterior resection (AR), low anterior resection (LAR), and abdominoperineal resection (APR) procedures were performed in 365 (31.9%), 500 (43.6%), and 277 (24.2%) patients, respectively. The mean operative time and estimated blood loss were 166.8 ± 31.6 min (range 106–720) and 73.8 ± 30.5 mL (range 5–400), respectively. Overall blood transfusion events totaled 16 (1.4%) within 30 days of surgery (Due to improve preoperative serious anemia (hemoglobin < 70 g/L) in 14 patients, and 2 patients suffered from major bleeding after operation). A diverting stoma was completed in 3 of 500 patients with LAR. The number of conversions to open procedures was 68 (5.9% conversion rate), of which, 60 cases were due to combined organ resection, and 8 for major bleeding or difficult tumor dissection. Following laparoscopic exploration, robotic procedures were canceled for 66 patients with severe abdominal adhesions or intraperitoneal tumor dissemination. The adjusted conversion rate was 11.1% (134/1211) if these 66 patients were calculated. The 133 (11.6%) patients accepted for combined organ resections are summarized in Table 1. A total of 181(23.7%) patients with T4 or N2 mid-low rectal cancer accepted preoperative radiotherapy or chemoradiotherapy. After surgery, 406 patients at high risk of relapse accepted adjuvant chemoradiotherapy, another 90 patients with unrespectable distant metastases accepted chemotherapy/target therapy after the primary tumor resection. The mean time of liquid diet and first flatus passage after surgery were 1.6 ± 0.1 days and 2.1 ± 0.5 days, respectively. The mean hospital stay after surgery and total hospital cost were 6.3 ± 2.9 days and 10442.5 ± 3321.5 US dollars, respectively (Table 2).
The mean number of harvested lymph nodes was 17 ± 10.5 (range 5–54). The positive rates of circumferential margin (CRM) and distant margin (DRM) were 15 (1.3%) and 6 (0.5%), respectively. The surgical quality of mesorectal excision calculated in 777 patients who underwent LAR or APR, according to Quirkes’ criteria, with “complete” in 706 (90.2%) patients and “near complete” in 71 (9.1%). No case was the mesorectum defined as “incomplete” by the pathologist. The pathological data are summarized in Table 3.
Surgical complication and risk factors
The number of overall surgical complications was 187 (16.3%). Grade 1 and grade 2 complications together accounted for 13.8%, while grade 3 and grade 4 complications were 2.0% and 0.4%, respectively. One patient died of hepatic failure after simultaneous hepatectomy for liver metastases within 30 days of the operation. The rehospitalization rate and reoperation rate associated with surgical complications within 90 days of surgery were 26 (2.3%) and 9 (0.8%), respectively.
We evaluated risk factors for surgical complications associated with RRR using a multivariate model, including factors that were statistically significant (P < 0.05) in a univariate analysis (Table 4). The male gender, tumors located at the mid-low rectum, combined organ resection, and clinical T category (cT3-4) were confirmed as the independent risk factors for surgical complications by multivariate analysis.
Sexual and urinary function
The analysis of the questionnaires completed by 81% of patients who underwent robotic TME or APR. It shows that sexual function and general sexual satisfaction decreased significantly 1 month, 6 months, and 1 year after intervention, respectively. In male patients, the scores for erectile function were 18.8 ± 2.7 (preoperation) versus 12.1 ± 4.6 (P = 0.008) at 1 month and 14.2 ± 5.1 (P = 0.021) at 6 months; for general satisfaction, 6.7 ± 1.2 (preoperation) versus 5.1 ± 1.2 (P = 0.017) at 1 month and 5.2 ± 1.2 (P = 0.023) at 6 months. In female patients, the values for arousal were 2.5 ± 0.9 (preoperation) versus 0.8 ± 0.4 (P = 0.024) at 1 month and 1.9 ± 0.6 (P = 0.068) at 6 months for general satisfaction. Both parameters then increased progressively, and at 1 year after surgery, the values were comparable to those measured before surgery. These data are presented in Table 5.
Concerning urinary function, the grade of incontinence measured 1 year after the intervention was statistically unchanged when compared with the preoperative status for both sexes. These data are summarized in Table 6. In particular, in male patients, we observed no significant deterioration of voiding or incontinence during the entire study period. Filling symptoms and incontinence function in women were both statistically worse 1 month after intervention, 2.3 ± 0.6 versus 3.2 ± 0.8 (P = 0.024) and 1.5 ± 0.6 versus 2.9 ± 0.8 (P = 0.019), respectively, whereas at 1 year after surgery, all scores were comparable to preoperative values. We observed the same results when comparing the total number of male and female patients with severe or moderate urinary incontinence (score ≥ 9) before and 1 year after surgery.
With regards to the impact of urinary symptoms on patient’s QoL, no difference was measured in either sex at 1 year compared to preoperative status (Table 7). For example, the scores of voiding QoL were 3.7 ± 1.1 (preoperation) versus 3.3 ± 1.1 (1 year, P = 0.162) for male and 3.7 ± 0.9 (preoperation) versus 3.7 ± 1.0 (1 year, P = 0.955) for female.
Long-term oncological outcomes
The median follow-up duration from primary treatment was 34.6 months (25th–75th percentile 18–79). A total 1034 of 1145 patients underwent R0 resection. Local recurrence and distant metastases occurred in 24 (2.3%) and 218 (21.1%) patients, respectively. The 3-year disease free-survival (DFS) rate was 81.0%, and the 3-year overall survival (OS) rate was 87.2%.
Discussion
We reported here the results of a large consecutive nonselected number of robotic rectal resections from real world to evaluate the safety and efficacy of robotic procedure for rectal cancer in China. In this study, we contributed to followed data analysis: (1) we analyzed the patients’ short-term outcomes and identified high-risk patients for robotic rectal surgery. (2) We summarized the sexual and urinary function data, as well as the long-term oncologic outcomes in detail. All this data demonstrated that the robotic procedure was safe and efficacious for patients with rectal cancer, when performed in an experienced medical unit.
This study summarized the complication and identified the risk factor of surgical complications during RRR. The incidence of grade 3 and grade 4 complications together was 2.4% in this RRR study, which was lower than rates reported in previous laparoscopic rectal resection (LRR) studies of 7.4% [22] and 9.5% [23]. A systematic review demonstrated no differences in postoperative morbidity and mortality between LRR and ORR [2]. RRR may help to reduce severe surgical complications; therefore, we recommended patients at a high risk for surgical complications undergo robotic surgery for rectal cancer.
More importantly, by applying a standardized robotic approach as described, we effectively reduced the incidence of anastomotic leakage (totally 4.2%) without including a routine diverting stoma. The rate of AL was 0.8% for AR and 6.6% for LAR, which was obviously lower than the reported 10–13% in recent studies [6, 8, 20]. It is worth noting that previous studies, even multicenter RCT studies, had low operative numbers performed by a single doctor; for example, 30 units completed 739 cases of LRR in the COLOR II study [8] and 40 surgeons completed 237 cases of RRR in the ROLARR study [6]. Limited case volume and inadequate surgical experience may compromise the quality of surgery [24, 25], which may be a potential reason possibly responsible for the high rate of AL in previous studies.
Independent risk factors for surgical complications during RRR were male gender, tumors located at the mid-low rectum, combined organ resection, and clinical T category (cT3–4). Risk factors previously reported in LRR or ORR [22, 26] studies, BMI ≥ 28, age ≥ 75, history of comorbidity, preoperative radiotherapy (RT) or chemoradiotherapy (CRT), and tumor size ≥ 5 cm, were not significant in our robotic procedure. These differences may be due to the diversity of patient characteristics: (1) The neoadjuvant RT or CRT was associated with an increased rate of anastomotic leakage (AL) as reported previously [26]. In this study, only patients with T4 or N2 disease received preoperative RT or CRT, and other patients with a high risk of relapse received chemoradiotherapy after radical surgery. The number of patients with mid-low rectal cancer who received neoadjuvant RT or CRT was 23.7% (181/778) in this study, unlike a greater proportion of CRT (46–58%) in Western countries [6, 8]. (2) Regarding a history of comorbidities, this study only collected data from cardiovascular disease and diabetes; therefore, some data associated with other organ systems were missed. (3) The percentage of patients with a BMI ≥ 28 was about 18% in this study. BMI was significantly lower in Asian people than the patients in western who have a high proportion of obese patients. [27, 28].
This study supplied larger cases analysis by questionnaires to evaluate the role of robotic TME on preservation of urogenital function. We recorded no difference in terms of incontinence, filling, or voiding symptoms at 1 year after surgery compared to the preoperative status for both sexes. This result was similar to that of a previous robotic study [10] and better than that of a LRR study, which was associated with a rate of sexual and urinary dysfunction higher [8] or comparable [29] to that following open surgery. Limitations of LRR can be explained by the technical complexities of laparoscopy surgery, including the unstable view of the operative field and the poor ergonomics of the surgical tools that render complex operations more difficult with a higher degree of surgeon fatigue. However, robotic surgery can overcome the limitations of laparoscopic surgery for rectal cancer, offering the surgeon a stable camera platform with a 3-dimensional operative field, precise and dexterous control of the wristed instruments to improve endo-wrist function, and reduced operator fatigue. As reported previously [30], the technical characteristics of a robotic system permits extended lymph node dissection and an accurate dissection of the smaller anatomical structures, thereby protecting the pelvic autonomic nerves.
In terms of the oncologic aspects, we found the 3-years DFS and OS were 81.0% and 87.2%, respectively, which was comparable to recent reports of LRR and ORR results [23, 31]. This outcome can be interpreted as confirmation that the therapeutic effectiveness of RRR is equivalent to laparoscopic and open surgery. Interestingly, the local recurrence rate and positive circumferential margin rate were better than that of LRR [7, 23] and ORR [31] in previous studies. Lim et al. [7] reported a lower local recurrence rate in RRR (2.7%) than that of LRR (6.3%) for patients with mid-low rectal cancer following neoadjuvant chemoradiation therapy. Baek et al. [32] classified 182 patients who underwent robotic surgery for rectal cancer into easy, moderate, and difficult groups by MRI-based pelvimetry and there was no difference between the groups in terms of operative and pathologic outcomes. Thus, an advantage of RRR may be its ability to overcome challenges associated with difficult pelvic anatomy and allow for a high quality of tumor resection.
The current study has several limitations in that it is single-arm large cases analysis with data from only a single center and is not a head-to-head designed study.
Conclusion
Based on the results, we determined robotic rectal resection to be a safe and adequate technique for the treatment of rectal cancer, with a low incidence of serious complications and anastomotic leakage. Robotic TME allows for preservation of urinary and sexual functions in patients with mid-low rectal cancer.
References
Speicher PJ, Englum BR, Ganapathi AM, Nussbaum DP, Mantyh CR, Migaly J (2015) Robotic low anterior resection for rectal cancer: a national perspective on short-term oncologic outcomes. Ann Surg 262(6):1040–1045
Martinez-Perez A, Carra MC, Brunetti F, de’Angelis N (2017) Short-term clinical outcomes of laparoscopic vs open rectal excision for rectal cancer: a systematic review and meta-analysis. World J Gastroenterol 23(44):7906–7916
Prete FP, Pezzolla A, Prete F, Testini M, Marzaioli R, Patriti A, Jimenez-Rodriguez RM, Gurrado A, Strippoli GFM (2018) Robotic versus laparoscopic minimally invasive surgery for rectal cancer: a systematic review and meta-analysis of randomized controlled trials. Ann Surg 267(6):1034–1046
Baek JH, McKenzie S, Garcia-Aguilar J, Pigazzi A (2010) Oncologic outcomes of robotic-assisted total mesorectal excision for the treatment of rectal cancer. Ann Surg 251(5):882–886
Eftaiha SM, Pai A, Sulo S, Park JJ, Prasad LM, Marecik SJ (2016) Robot-assisted abdominoperineal resection: clinical, pathologic, and oncologic outcomes. Dis Colon Rectum 59(7):607–614
Jayne D, Pigazzi A, Marshall H, Croft J, Corrigan N, Copeland J, Quirke P, West N, Rautio T, Thomassen N, Tilney H, Gudgeon M, Bianchi PP, Edlin R, Hulme C, Brown J (2017) Effect of robotic-assisted vs conventional laparoscopic surgery on risk of conversion to open laparotomy among patients undergoing resection for rectal cancer: the ROLARR randomized clinical trial. JAMA 318(16):1569–1580
Lim DR, Bae SU, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2017) Long-term oncological outcomes of robotic versus laparoscopic total mesorectal excision of mid-low rectal cancer following neoadjuvant chemoradiation therapy. Surg Endosc 31(4):1728–1737
van der Pas MH, Haglind E, Cuesta MA, Furst A, Lacy AM, Hop WC, Bonjer HJ, Group COcLoORIS (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14(3):210–218
Jones OM, Stevenson AR, Stitz RW, Lumley JW (2009) Preservation of sexual and bladder function after laparoscopic rectal surgery. Colorectal Dis 11(5):489–495
Luca F, Valvo M, Ghezzi TL, Zuccaro M, Cenciarelli S, Trovato C, Sonzogni A, Biffi R (2013) Impact of robotic surgery on sexual and urinary functions after fully robotic nerve-sparing total mesorectal excision for rectal cancer. Ann Surg 257(4):672–678
Sammour T, Malakorn S, Bednarski BK, Kaur H, Shin US, Messick C, You YN, Chang GJ (2018) Oncological outcomes after robotic proctectomy for rectal cancer: analysis of a prospective database. Ann Surg 267:521–526
Wibe A, Rendedal PR, Svensson E, Norstein J, Eide TJ, Myrvold HE, Soreide O (2002) Prognostic significance of the circumferential resection margin following total mesorectal excision for rectal cancer. Br J Surg 89(3):327–334
Quirke P (2003) Training and quality assurance for rectal cancer: 20 years of data is enough. Lancet Oncol 4(11):695–702
Mazeh H, Samet Y, Abu-Wasel B, Beglaibter N, Grinbaum R, Cohen T, Pinto M, Hamburger T, Freund HR, Nissan A (2009) Application of a novel severity grading system for surgical complications after colorectal resection. J Am Coll Surg 208(3):355–361
Abrams P, Avery K, Gardener N, Donovan J, Board IA (2006) The International Consultation on Incontinence Modular Questionnaire. J Urol 175(3 Pt 1):1063–1066 (discussion 1066)
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 49(6):822–830
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R, Ferguson D, D’Agostino R Jr (2000) The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26(2):191–208
Collettini F, Enders J, Stephan C, Fischer T, Baur ADJ, Penzkofer T, Busch J, Hamm B, Gebauer B (2019) Image-guided irreversible electroporation of localized prostate cancer: functional and oncologic outcomes. Radiology 292(1):250–257
Saito S, Fujita S, Mizusawa J, Kanemitsu Y, Saito N, Kinugasa Y, Akazai Y, Ota M, Ohue M, Komori K, Shiozawa M, Yamaguchi T, Akasu T, Moriya Y, Colorectal Cancer Study Group of Japan Clinical Oncology, Group (2016) Male sexual dysfunction after rectal cancer surgery: results of a randomized trial comparing mesorectal excision with and without lateral lymph node dissection for patients with lower rectal cancer: Japan Clinical Oncology Group Study JCOG0212. Eur J Surg Oncol 42(12):1851–1858
Dulskas A, Samalavicius NE (2016) A prospective study of sexual and urinary function before and after total mesorectal excision. Int J Colorectal Dis 31(6):1125–1130
Xu JM, Wei Y, Wang XY, Fan H, Chang WJ, Ren L, Jiang W, Fan J, Qin XY (2015) Robot-assisted one-stage resection of rectal cancer with liver and lung metastases. World J Gastroenterol 21(9):2848–2853
Asa Z, Greenberg R, Ghinea R, Inbar R, Wasserberg N, Avital S (2013) Grading of complications and risk factor evaluation in laparoscopic colorectal surgery. Surg Endosc 27(10):3748–3753
Park EJ, Cho MS, Baek SJ, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2015) Long-term oncologic outcomes of robotic low anterior resection for rectal cancer: a comparative study with laparoscopic surgery. Ann Surg 261(1):129–137
Manilich E, Vogel JD, Kiran RP, Church JM, Seyidova-Khoshknabi D, Remzi FH (2013) Key factors associated with postoperative complications in patients undergoing colorectal surgery. Dis Colon Rectum 56(1):64–71
Asari SA, Cho MS, Kim NK (2015) Safe anastomosis in laparoscopic and robotic low anterior resection for rectal cancer: a narrative review and outcomes study from an expert tertiary center. Eur J Surg Oncol 41(2):175–185
Kang CY, Halabi WJ, Chaudhry OO, Nguyen V, Pigazzi A, Carmichael JC, Mills S, Stamos MJ (2013) Risk factors for anastomotic leakage after anterior resection for rectal cancer. JAMA Surg 148(1):65–71
Yang CS, Choi GS, Park JS, Park SY, Kim HJ, Choi JI, Han KS (2016) Rectal tube drainage reduces major anastomotic leakage after minimally invasive rectal cancer surgery. Colorectal Dis 18(12):O445–O452
Kang J, Yoon KJ, Min BS, Hur H, Baik SH, Kim NK, Lee KY (2013) The impact of robotic surgery for mid and low rectal cancer: a case-matched analysis of a 3-arm comparison–open, laparoscopic, and robotic surgery. Ann Surg 257(1):95–101
Andersson J, Abis G, Gellerstedt M, Angenete E, Angeras U, Cuesta MA, Jess P, Rosenberg J, Bonjer HJ, Haglind E (2014) Patient-reported genitourinary dysfunction after laparoscopic and open rectal cancer surgery in a randomized trial (COLOR II). Br J Surg 101(10):1272–1279
Pigazzi A, Luca F, Patriti A, Valvo M, Ceccarelli G, Casciola L, Biffi R, Garcia-Aguilar J, Baek JH (2010) Multicentric study on robotic tumor-specific mesorectal excision for the treatment of rectal cancer. Ann Surg Oncol 17(6):1614–1620
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MH, de Lange-de Klerk ES, Lacy AM, Bemelman WA, Andersson J, Angenete E, Rosenberg J, Fuerst A, Haglind E (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372(14):1324–1332
Baek SJ, Kim CH, Cho MS, Bae SU, Hur H, Min BS, Baik SH, Lee KY, Kim NK (2015) Robotic surgery for rectal cancer can overcome difficulties associated with pelvic anatomy. Surg Endosc 29(6):1419–1424
Acknowledgments
This project was supported by The National Natural Science Foundation of China (81602035); The Shanghai Municipal Commission of Health and Family Planning: Shanghai Outstanding Youth Specialist Training Program (Q2017-059); Clinical Science and Technology Innovation Project of Shanghai (SHDC12016104); Shanghai Science and Technology Committee Project (17411951300).
Funding
This project was supported by The National Natural Science Foundation of China (81602035); The Shanghai Municipal Health Commission (Q2017-059); Clinical Science and Technology Innovation Project of Shanghai (SHDC12016104); Shanghai Science and Technology Committee Project (17411951300).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Wenju Chang, Ye Wei, Li Ren, Mi Jian, Yijiao Chen, Jingwen Chen, Tianyu Liu, Wenbai Huang, Shangjin Peng, and Jianmin Xu have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Chang, W., Wei, Y., Ren, L. et al. Short-term and long-term outcomes of robotic rectal surgery—from the real word data of 1145 consecutive cases in China. Surg Endosc 34, 4079–4088 (2020). https://doi.org/10.1007/s00464-019-07170-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07170-6