Abstract
Background
Secondary hyperparathyroidism (sHPT), a complication of chronic kidney disease (CKD) characterized by persistently elevated parathyroid hormone (PTH), alterations in calcium-phosphorus homeostasis, and vitamin D metabolism, affects 50% of children receiving dialysis. A significant proportion of these children develop CKD-mineral and bone disorder (CKD-MBD), associated with an increased risk of fractures and vascular calcification. The standard of care for sHPT in children includes vitamin D sterols, calcium supplementation, and phosphate binders. Several agents are approved for sHPT treatment in adults undergoing dialysis, including vitamin D analogs and calcimimetics, with limited information on their safety and efficacy in children. The calcimimetic cinacalcet is approved for use in adults with sHPT on dialysis, but is not approved for pediatric use outside Europe.
Methods
This review provides dosing, safety, and efficacy information from Amgen-sponsored cinacalcet pediatric trials and data from non-Amgen sponsored clinical studies.
Results
The Amgen cinacalcet pediatric clinical development program consisted of two Phase 3 randomized studies, one Phase 3 single arm extension study, one open-label Phase 2 study, and two open-label Phase 1 studies. Effects of cinacalcet on PTH varied across studies. Overall, 7.4 to 57.1% of subjects who received cinacalcet in an Amgen clinical trial attained PTH levels within recommended target ranges and 22.2 to 70.6% observed a ≥ 30% reduction in PTH. In addition, significant reductions in PTH were demonstrated in all non-Amgen-supported studies.
Conclusions
To help inform the pediatric nephrology community, this manuscript contains the most comprehensive review of cinacalcet usage in pediatric CKD patients to date.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
End-stage renal disease (ESRD) in children is rare with 18–100 per million patients requiring renal replacement therapy globally [1]. Children are priority candidates for kidney transplantation; as a result, the point prevalence of pediatric patients on dialysis is relatively low (e.g., < 1% [3,151]) of all US patients on dialysis (466,607) [2].
Secondary hyperparathyroidism (sHPT) is a compensatory complication of chronic kidney disease (CKD). sHPT is characterized by persistently elevated parathyroid hormone (PTH) concentrations in serum or plasma, and it represents an adaptive response that serves primarily to maintain calcium homeostasis systemically as kidney function declines [3]. Early alterations in fibroblast growth factor 23 (FGF23), vitamin D metabolism, and calcium and phosphorus regulation lead to a reduction in signaling through the calcium-sensing receptor (CaSR) and an increase in PTH secretion, resulting in higher PTH concentrations. Late in the course of CKD, phosphorus retention and overt hyperphosphatemia, together with skeletal resistance to the calcemic action of PTH, can also affect calcium metabolism adversely and further increase PTH secretion among patients with more advanced CKD [3,4,5,6]. Collectively, these changes in calcium and phosphorus concentrations and vitamin D metabolism contribute to the progression of sHPT, which generally worsens in severity over time if left untreated. sHPT affects 50% of children receiving dialysis [7].
The consequences of sHPT include the development of CKD-mineral bone disorder (CKD-MBD), defined as a systemic disorder of mineral and bone metabolism due to CKD that is manifested by either one or a combination of the following: (1) abnormalities in calcium, phosphorus, PTH, or vitamin D metabolism; (2) abnormalities in bone turnover, mineralization, volume, linear growth, or strength; and (3) vascular or other soft tissue calcification [8]. In children, CKD-MBD develops early during CKD, such that 50% of children with stage 3 CKD, and 60% with stage 4/5 CKD have manifestations of CKD-MBD [9]. Moreover, these patients can experience either calcium deficiency, potentially causing impaired mineralization and an increased fracture risk [9,10,11], or calcium excess, linked with vascular calcification [7].
The recommended standard of care (SOC) for the treatment of sHPT includes the use of vitamin D sterols, calcium supplementation, and phosphate binders (calcium-based and non-calcium-based, with the exception of aluminum salts that are contraindicated) [12]. Current pediatric consensus guidelines recommend that the SOC for pediatric patients should specifically focus on maintaining serum calcium and phosphate within the age-appropriate normal range [12,13,14]. Additionally, the National Kidney Foundation Kidney Disease Outcomes Quality Initiative (NKF K/DOQI) recommends PTH levels within a target range (> 150 to 300 pg/mL) [15], while the European Pediatric Dialysis Working Group (EPDWG) has recommended that PTH be monitored monthly and kept at two to three times the upper limit of the normal range in advanced CKD [12].
Several agents have been approved by the US Food and Drug Administration (FDA) and the European Medicines Agency (EMA) for the treatment of sHPT in adult patients undergoing dialysis. These include the vitamin D analogs doxercalciferol, paricalcitol, calcitriol, and the calcimimetics cinacalcet and etelcalcetide. Despite the availability of these therapies for adults, there is limited information on the safety and efficacy of these products in children, and pediatric formulations are generally not commercially available. Treatment with vitamin D sterols may not completely control sHPT in children with CKD, either due to insufficient efficacy or limited use resulting from the subsequent development of hypercalcemia and hyperphosphatemia. Furthermore, different therapeutic approaches to sHPT have differential effects on FGF23. Vitamin D tends to increase FGF23, and cinacalcet tends to lower FGF23, while the effects of calcium and non-calcium-based phosphate binders are variable [16,17,18].
The calcimimetic cinacalcet is an allosteric modulator of the CaSR, increasing receptor sensitivity to calcium and thereby increasing the potency of extracellular calcium resulting in decreased PTH secretion and production [19,20,21]. Cinacalcet has been approved by the FDA and EMA for use in adults with sHPT on dialysis [20]. In the EU, cinacalcet is approved for patients aged 3 years and older with ESRD on maintenance dialysis therapy in whom sHPT is not adequately controlled with SOC therapy [22]. To help address the unmet clinical need for additional therapies to treat sHPT in children, Amgen conducted an extensive pediatric development program for cinacalcet to investigate the dosing, safety, and efficacy in pediatric patients with sHPT on dialysis. Overall, 142 children were enrolled in interventional clinical trials in the Amgen-sponsored pediatric clinical development program; 103 of whom received cinacalcet. An additional 113 children received cinacalcet in observational studies that were part of the cinacalcet pediatric development program. Finally, safety and efficacy data are available from 60 children who received cinacalcet in five non-Amgen-supported clinical studies [23,24,25,26,27]. Herein, we provide a comprehensive review of all cinacalcet clinical studies in pediatric subjects to help inform the pediatric nephrology community.
Methods
After establishing cinacalcet bioavailability and bioequivalence of a pediatric formulation (Study 20070293), Amgen undertook a series of clinical trials. The Amgen cinacalcet pediatric clinical development program consisted of two phase 3 randomized studies, one phase 3 single arm extension study, one open-label phase 2 study, and two open-label phase 1 studies. Study details, including study objective, dosing regimen, and study populations, are provided in Table 1. In all multidose studies, the cinacalcet starting dose was titrated based on PTH and calcium thresholds, and safety assessments. Additional real-world observational data were available from a multicenter, retrospective, chart review study and a prospective cohort registry study. To summarize data outside of Amgen-supported studies, we undertook a comprehensive PubMed literature review (through 03 January 2019) of studies evaluating the use of cinacalcet in pediatric subjects on dialysis (Table 2). Preclinical studies, case reports, and review articles were omitted from this manuscript. Studies were also excluded if subjects had primary or tertiary hyperparathyroidism, hyperparathyroidism due to CaSR mutations, parathyroid carcinoma or malignancy, were not on dialysis, or had CKD 4 or lower. All Amgen study protocols, subject information, and informed consent forms were reviewed and approved by the IRB/IEC for each study center. All Amgen studies were conducted in accordance with applicable country regulations and International Conference on Harmonisation (ICH) Good Clinical Practice (GCP) regulations/guidelines.
Results
Collectively, 79 subjects received cinacalcet within the Amgen-supported phases 2 and 3 studies, with most subjects (57%) receiving cinacalcet for 16 weeks or longer (demographic details are presented in Table S1a). Across these studies, cinacalcet was initiated at a dose of 0.06–0.29 mg/kg/day (mean 0.16 mg/kg/day). Subjects received a mean cumulative dose of 1794 mg and a maximum weight–adjusted daily dose ranging from 0.1 to 5.7 mg/kg/day. Dosing with cinacalcet in the first phase 3 pediatric study (Study 20070208) was stopped due to a fatality in a cinacalcet-treated individual. The patient was noted to be severely hypocalcemic at the time of death. The cause of death was multifactorial and a contribution of cinacalcet to the death could not be excluded. The program was placed on a partial clinical hold by the US FDA for 14 months following the fatality while changes to cinacalcet dosing were implemented to further minimize the risk of severe hypocalcemia. Study 20070208 was terminated, and changes to cinacalcet dosing were implemented in Study 20130356 and Study 20110100. Dose adjustments of cinacalcet (reduction, withholding, or maintenance) were based on monthly assessments of iPTH and corrected serum calcium levels as well as weekly assessments using ionized calcium. Dose decisions were also based on adverse signs and symptoms (e.g., related to hypocalcemia), investigational product compliance, and administration of medications known to prolong the QT interval.
Adverse events (AEs) were frequent (70/79 patients; 88.6%) and mostly grade 3 or lower (63/79 patients; 79.7%), with the frequency and severity of AEs being similar between the control and test arms of the two controlled studies. No AEs resulted in the discontinuation of cinacalcet. A summary of the treatment-emergent AEs in all pediatric subjects treated with cinacalcet in Amgen-sponsored studies are described in Tables 5 and 6, and those in controlled studies are provided in Table S2. The most common AEs (occurring in > 10% of subjects) were hypocalcemia (18 subjects [22.8%]), vomiting (13 subjects [16.5%]), nausea (12 subjects [15.2%]), systemic hypertension (9 subjects [11.4%]), pyrexia (8 subjects [10.1%]), and muscle spasms (8 subjects [10.1%]). Accounting for cinacalcet exposure and treatment duration, the overall exposure- and follow-up-adjusted subject incidence rate of AEs was 478.5 per 100 subject years and 520.2 per 100 subject years, respectively. Approximately one-third of all subjects reported a serious AE, with the exposure-adjusted incidence of those most commonly reported (by > 1 subject) being device-related infection (10.8 per 100 subject years), peritonitis (7.3 per 100 subject years), overdose, systemic hypertension (each 7.2 per 100 subject years), and complication associated with catheter (7.0 per 100 subject years). Details of safety follow-up and the adjusted incidence of treatment-emergent AEs occurring in ≥ 5% of subjects in any treatment group by system organ class and preferred term are provided in Tables S3 and S4. Most subjects were receiving a phosphate binder and/or a vitamin D sterol at baseline. The proportion of subjects who had a phosphate binder or a vitamin D sterol added to their treatment regimen post-baseline was low and similar between the treatment and control arms. Details on concomitant phosphate binder and vitamin D use are presented in Table S5. The study specific safety data are described below.
Efficacy data from the Amgen-sponsored phases 2 and 3 studies are summarized in Table 3. Overall, the efficacy of cinacalcet in pediatric subjects enrolled in studies before the partial clinical hold was similar across pediatric age groups to that seen in adults. Lower-than-expected efficacy was observed in patients enrolled after the partial clinical hold; dose titration to achieve adequate cinacalcet exposure expected to result in PTH reduction was limited primarily because of frequent dose interruptions and reductions due to more conservative calcium thresholds. Despite limited cinacalcet exposure, twenty-one subjects (75%) achieved a ≥ 30% reduction in PTH after the first dose of cinacalcet during the combined Studies 20130356, 20110100, and 20140159. Furthermore, reductions in PTH were observed in individual subjects with increasing exposure to cinacalcet. Where assessed, no clinically significant results were observed regarding the impact of cinacalcet on bone turnover markers (e.g., serum-specific bone alkaline phosphatase [BALP], type 1 collagen cross-linked N-telopeptide [NTx], amino-terminal propeptide of type 1 collagen [P1NP], and type 1 collagen cross-linked C-telopeptide [CTx]).
Phases 2 and 3 safety findings
Study 20070208
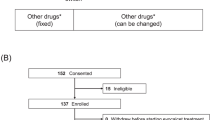
A randomized, double-blind, placebo-controlled Phase 3 study to assess the safety and efficacy of cinacalcet in 43 pediatric subjects with CKD and sHPT receiving dialysis [28].
The mean (standard deviation [SD]) duration of exposure during the double-blind phase was 109.7 (65.9) days in the cinacalcet group and 123.4 (80.4) days in the placebo group. The mean (SD) actual weight-adjusted daily dose of cinacalcet taken during the efficacy assessment phase (EAP; period between weeks 25 and 30, inclusive) was 1.54 (2.04) mg/kg/day. The mean (SD) maximum actual weight-adjusted daily dose of cinacalcet during the double-blind phase was 0.99 (1.26) mg/kg/day. In the double-blind phase, 81.8% of subjects in the cinacalcet group and 85.7% of subjects in the placebo group had at least one AE. The most common AEs in the cinacalcet group were vomiting (31.8% cinacalcet, 23.8% placebo), hypocalcemia (22.7% cinacalcet, 19.0% placebo), and nausea (18.2% cinacalcet, 14.3% placebo). No subjects in the cinacalcet group experienced an AE that led to cinacalcet withdrawal. Nine subjects in both the cinacalcet group (40.9%) and the placebo group (42.9%) had a serious AE. No serious AE was experienced by more than 1 subject. One subject in the cinacalcet group experienced a fatal AE (reported preferred term: cardiopulmonary failure) in the setting of severe hypocalcemia. Although the fatality was determined to be multifactorial, a causal role for hypocalcemia associated with cinacalcet treatment could not be excluded. Due to this fatality, the clinical program was placed on a partial clinical hold for 14 months. Based on a review of the case and in consultation with the Data Monitoring Committee and the FDA, changes were made to the cinacalcet pediatric program to include additional safety measures focused on further minimizing the risk of hypocalcemia in Study 20110100 (restarted after the partial clinical hold) and in new Studies 20130356 and 20140159. Study 20070208 was terminated following the partial clinical hold.
Study 20130356
A randomized, multicenter, open-label, controlled (cinacalcet + SOC vs. SOC) Phase 3 study in 55 pediatric subjects with CKD and sHPT receiving dialysis.
The mean (SD) duration of exposure in the cinacalcet + SOC group was 112.8 (41.0) days. The mean (SD) actual weight-adjusted daily dose of cinacalcet taken was 0.3 (0.3) mg/kg/day during weeks 11 to 15, and 0.4 (0.5) mg/kg/day during weeks 17 to 20. The mean (SD) maximum actual weight-adjusted daily dose was 0.6 (0.5) mg/kg/day. During the entire treatment period, 23 of 25 subjects (92.0%) had at least 1 cinacalcet dose withheld or reduced.
Twenty-one subjects (84.0%) in the cinacalcet + SOC group and 17 subjects (56.7%) in the SOC group experienced AEs. The most common AEs were hypocalcemia (6 subjects [24.0%] cinacalcet + SOC, 2 subjects [6.7%] SOC), muscle spasms (3 [12.0%], 2 [6.7%]), nausea (3 [12.0%], 1 [3.3%]), headache (1 [4.0%], 4 [13.3%]), and vomiting (0, 3 [10.0%]). All other AEs were reported for ≤2 subjects in either treatment group. Most subjects had AEs that were grade > 2 in severity, and most were considered not related to study treatment. None of the subjects died or were withdrawn from the study due to an AE. Serious AEs were reported for 4 subjects (16.0%) in the cinacalcet + SOC group and 2 subjects (6.7%) in the SOC group. Each serious AE was reported by a single subject, and none were considered related to study treatment. Review of laboratory parameters, including corrected serum calcium, ionized calcium, and phosphate, revealed no unexpected safety concerns in either treatment group. More subjects in the cinacalcet + SOC group (6 subjects [24.0%]) experienced low corrected serum calcium < 8.4 mg/dL compared with the SOC group (2 subjects [6.9%]); however, the incidences of low corrected serum calcium < 8.0 mg/dL and < 7.5 mg/dL were comparable. The incidence of low ionized calcium was similar between treatment groups.
Study 20110100
An open-label, single-arm phase 2 study of cinacalcet in addition to SOC in 18 pediatric subjects aged 28 days to < 6 years.
Seventeen subjects received ≥ 1 cinacalcet dose. Data were assessed before partial clinical hold (cohort 1; n = 7) and after partial clinical hold (cohort 2; n = 10). The mean total cinacalcet dose administered was 516.9 mg for cohort 1 and 371.3 mg for cohort 2. The higher exposure in cohort 1 was achieved despite a shorter mean (SD) exposure to cinacalcet for cohort 1 (66.0 [50.9] days) compared with cohort 2 (101.2 [42.4] days). The mean (SD) maximum weight–adjusted daily dose was 0.98 (0.94) mg/kg/day and 0.55 (0.31) mg/kg/day for cohorts 1 and 2, respectively. Serious AEs were reported in 9 subjects (52.9%), 4 in cohort 1 and 5 in cohort 2. Complication associated with catheter and systemic hypertension each occurred in 2 subjects (11.8%; 1 subject each per cohort). None of the serious AEs were treatment-related. One subject in cohort 2 experienced a grade 2 serious AE of a seizure 14 days after discontinuation of cinacalcet treatment. The seizure occurred at the end of a hemodialysis session. This event was considered not to be related to cinacalcet treatment by the investigator.
Study 20140159
An open-label, phase 3 extension study of cinacalcet in the treatment of sHPT in pediatric subjects with CKD receiving dialysis (extension of Studies 20130356 and 20110100). The final analyses included 27 subjects rolled over from the parent Study 20130356 and 1 subject rolled over from Study 20110100. Of the 27 subjects from Study 20130356, 14 subjects previously received cinacalcet and SOC in the parent study (hereinafter referred to as the Study 20130356 cinacalcet + SOC group), and 13 subjects previously received SOC alone in the parent study (referred to as Study 20130356 SOC hereafter).
The mean (SD) maximum weight-adjusted exposure to cinacalcet during the extension study was 0.78 (0.66) mg/kg/day, across 169.8 (52.4) days. Nine subjects (32.1%; 6 subjects from Study 20130356 cinacalcet + SOC, 2 subjects from Study 20130356 SOC, and 1 subject from Study 20110100 cinacalcet + SOC) had at least 1 serious adverse event and at least 1 grade ≥3 adverse event. Nine subjects (32.1%; 4 subjects from Study 20130356 cinacalcet + SOC and 5 subjects from Study 20130356 SOC) had adverse events that were considered treatment related by the investigator. A 2-year 7-month-old boy died; it was determined by autopsy that the death was due to bronchopneumonia and acute exacerbation of chronic pyelonephritis. According to the investigator, there was no reasonable possibility that the fatal event was related to cinacalcet.
Phase 1 pharmacokinetic studies
Two phase 1 pharmacokinetic (PK) studies (Study 20090005 and Study 20030227) have been conducted and the PK findings published. Study 20090005 was an open-label, single-dose study (0.25 mg/kg) of cinacalcet in 14 pediatric subjects aged 28 days to < 6 years with CKD receiving dialysis [29]. Study 20030227 was an open-label study of a single dose (15 mg) of cinacalcet in 12 pediatric subjects age 6 to < 18 years with CKD receiving dialysis [30].
Safety and efficacy data from observational studies
Study 20090198
A retrospective chart review to evaluate biochemical markers and safety in children < 6 years of age with sHPT and CKD receiving dialysis at the time of initiation of cinacalcet treatment.
Safety
This study included a total of 23 subjects on dialysis who received cinacalcet. Nineteen of the 23 subjects (83%) received cinacalcet as a crushed tablet. The route of administration was oral for 15 subjects (65%), by nasogastric tube for 7 subjects (30%), and through a percutaneous endoscopic gastrostomy for 1 subject (4%). The mean (SD) duration of exposure was 274.17 (245.53) days, with an exposure range of 34–1036 days. The mean (SD) initial weight-adjusted daily dose was 0.81 (0.54) mg/kg/day (median [range] 0.61 [0.1, 1.9] mg/kg/day). The mean (SD) maximum weight–adjusted daily dose over the course of treatment was 1.87 (1.30) mg/kg/day (median [range] 1.40 [0.4, 5.6] mg/kg/day). Seventeen subjects (74%) had at least 3 months of cinacalcet treatment. A review of dose administration by individual subject showed variable dosing regimens with doses ranging from 2.5 to 60 mg. The frequency of administration changed over time for some subjects, although the most common frequency was once daily. Two subjects had adverse drug reactions (i.e., cinacalcet-related AEs): decreased level of consciousness and intermittent mild hypocalcemia; the decreased level of consciousness event occurred in the setting of marked hypocalcemia and was considered serious.
Efficacy
PTH
The proportion of subjects with ≥ 30% reduction in PTH from baseline was 33% (6 of 18 subjects), 42% (5 of 12 subjects), and 58% (7 of 12 subjects) of subjects at months 1, 2, and 3, respectively. Mean PTH concentrations decreased from baseline at every time point, except month 4. The mean (SD) decreases at months 1, 2, and 3 were − 86.8 (815.9), − 533.3 (1055.3), and − 473.5 (871.7) pg/mL, respectively.
Calcium
In general, mean serum calcium concentrations remained within normal limits during treatment and ranged from 8.72 (1.11) mg/dL at month 1 to 9.76 (1.13) mg/dL at month 2. Mean decreases from baseline in total calcium were observed at every time point, except month 2. The mean (SD) changes from baseline at months 1, 2, and 3 were − 0.6 (0.8), 0.4 (1.3), and − 0.2 (0.8) mg/dL, respectively. The maximum mean (SD) decreases were at months 1 and 5 (− 0.6 [0.8] mg/dL; − 0.6 [0.7]mg/dL), respectively.
Phosphate
Mean decreases from baseline in phosphate were observed at every time point. The largest mean (SD) decrease from baseline was − 1.48 (2.32) mg/dL observed at month 2. The mean (SD) percent decrease from baseline at this same time point was − 20.79% (30.52%). Unexpectedly, the overall group mean percent change from baseline increased at months 1, 5, 6, and 7. This increase is likely skewed by substantial percent increases over baseline for 2 subjects. Median percent decreases in phosphorus from baseline were observed at all time points except month 1 and ranged in value from − 5.60% at month 4 to − 24.24% at month 2. In general, mean serum phosphate concentrations remained within normal limits (i.e., 4.5 to 8.0 mg/dL) during treatment.
Study 20120116
A prospective cohort study to describe the use and safety of cinacalcet in pediatric subjects receiving dialysis in the North American Pediatric Renal Trials and Collaborative Studies (NAPRTCS) registry.
This study evaluated 538 subjects on dialysis, including 90 who received cinacalcet and 448 who did not receive cinacalcet. Data collected from this study contributed to the evaluation of the safety rather than the efficacy of cinacalcet. The incidence of AEs of interest (hypocalcemia, seizure, and infection [requiring hospitalization]) was estimated separately in cinacalcet-treated and untreated subjects enrolled in the pediatric dialysis registry. Patients were followed for up to 3 years. Patients were censored at 3 years, transplant, death, loss to follow-up, or if no longer participating in NAPRTCS, whichever occurred first.
Hypocalcemia
The incidence of subjects who were treated for or had a modification of treatment for hypocalcemia was similar between subjects who received cinacalcet and subjects who did not. Ten of 90 subjects (11.1%) who received cinacalcet were treated for or had a modification of treatment for hypocalcemia a total of 28 times during the study; 20 therapy modification episodes involved a change in cinacalcet therapy. In subjects not receiving cinacalcet, 48 of 448 (10.7%) had a total of 95 hypocalcemia treatments or modification of treatment for hypocalcemia.
Seizure
The incidence of seizure was similar between subjects receiving cinacalcet and subjects not receiving cinacalcet. In subjects receiving cinacalcet, 5 of 90 subjects (5.6%) reported 5 seizure episodes; 4 subjects experienced seizures while taking cinacalcet, 1 subject experienced a seizure while not actively taking cinacalcet. The incidence rate (95% CI) of seizures per follow-up year was 0.04 (0.01, 0.08) in participants receiving cinacalcet and 0.08 (0.06, 0.11) in participants not receiving cinacalcet.
Infection
Bacterial infections were reported in 89% (34 of 38) of the hospitalizations in the cinacalcet group and in 65% (116 of 179) of the hospitalizations in the group that did not receive cinacalcet. Viral infections were reported in 8% (3 of 38) of the hospitalizations in the cinacalcet group and 22% (39 of 179) of the hospitalizations in the group that did not receive cinacalcet. Three of the 8 subjects who died in this study had received cinacalcet. Of these three subjects, one subject with focal segmental glomerulosclerosis collapsed and was unable to be resuscitated. The cause of death was noted as “unknown”. Cinacalcet dosing information was not available, and the subject was not taking cinacalcet at last follow-up. The second subject died of hemorrhagic pancreatitis. The subject received therapy with cinacalcet for 5 months and had discontinued cinacalcet therapy 7 months before death. The third subject had acute lymphoblastic leukemia-multiple complications; the subject was receiving cinacalcet at last follow-up (86 days before death).
Bayesian extrapolation analysis
Innovative study designs and advanced analysis methods including Bayesian approaches are encouraged by the FDA and EMA to improve efficiency and optimize pediatric drug development by minimizing exposure of children to studies and by addressing feasibility issues such as the limited available pediatric population. Accordingly, a Bayesian hierarchical model was used to synthesize information from the adult cinacalcet Studies 20000172, 20000183, and 20000188 and the pediatric cinacalcet Studies 20070208 and 20110100 (specifically, subjects enrolled before the partial clinical hold) to make statistical inference on the treatment effect of cinacalcet in the pediatric population. Bayesian extrapolation demonstrated a higher proportion of pediatric subjects in the cinacalcet group who achieved a ≥ 30% reduction from baseline in mean PTH compared with the placebo-controlled group in both the overall pediatric population and in the younger age group between 28 days and < 6 years of age.
Physiologically-based PK modeling
Physiologically-based PK modeling analyses were conducted to predict the PK characteristics of cinacalcet in pediatric subjects < 1 year old and their consistency with those observed in older children (1 year to < 18 years old) and adults. Physiologically-based PK simulations projected that the average, weight-normalized oral clearance of cinacalcet in subjects 28 days to 1 year and in subjects 28 days to < 18 years varied < 1.5-fold. At the lowest dose analyzed (0.2 mg/kg), the average Cmax, AUC, and weight-normalized oral clearance of cinacalcet were projected to vary < 1.5-fold in subjects 28 days to 1 year, supporting its selection as the weight-based starting dose for subjects aged 28 days to 1 year. Thus, cinacalcet PK data are similar between pediatric and adult subjects with CKD and secondary HPT receiving dialysis and between pediatric age groups (28 days to < 6 years and 6 years to < 18 years).
PK/PD model of cinacalcet, in adults and pediatric patients with sHPT on dialysis [31]
Cinacalcet PK parameters were described by a two-compartment linear model with delayed first-order absorption-elimination (apparent clearance = 287.7 L/h). Simulations suggested that pediatric starting doses (1, 2.5, 5, 10, and 15 mg) would provide PK exposures less than or similar to a 30-mg adult dose. The titrated dose simulations suggested that the mean (prediction interval) proportion of pediatric and adult subjects achieving ≥ 30% reduction in PTH from baseline at week 24 was 49% (36%, 62%) and 70% (63%, 77%), respectively. Additionally, the mean (confidence interval) proportion of pediatric and adult subjects achieving corrected calcium ≤ 8.4 mg/dL at week 24 was 8% (2%, 18%) and 24% (18%, 31%), respectively. Model-based simulations showed that the pediatric cinacalcet starting dose (0.2 mg/kg/day, based on the subject’s dry weight, rounded down to the lowest protocol-specified dose [PSD]), titrated to effect, would provide the desired pharmacodynamic efficacy (PTH suppression > 30%) while minimizing safety concerns (hypocalcemia).
Non-Amgen-supported studies
Five non-Amgen-supported clinical studies of cinacalcet use in pediatric subjects with CKD and sHPT receiving dialysis were identified and are described in Table 2. These studies comprised two single-center studies, one retrospective chart review, one retrospective case series, and one prospective cohort analysis. Overall, these studies reported safety and efficacy data from 60 children (age 0.5–19 years; see Table S1b) following cinacalcet treatment with starting dose ranging from 0.25 to 1.1 mg/kg/day. No cases of overt symptoms of hypocalcemia such as tremor, paresthesia, or seizure were reported. Across these studies, cinacalcet reduced PTH levels by 60 to 98% from baseline values. Interestingly, all children with refractory sHPT attained K/DOQI PTH target goal (150–300 pg/ml) within 8 months of cinacalcet initiation [23]. Patients with lower baseline PTH were reported to attain target PTH levels quicker than those with high PTH levels. Furthermore, a “rebound” in PTH levels was reported in patients with a baseline PTH > 1000 pg/mL. One study demonstrated improved linear growth in 80% (8/10) of patients during 6 months of cinacalcet treatment [23]. Overall, findings on changes in serum calcium and phosphate levels were inconclusive.
Discussion
Treatment strategies for sHPT in children need to account for their higher calcium requirements and bone development. KDIGO recognizes that children may be uniquely vulnerable to calcium restriction and provides guidelines to account for the higher calcium requirements of the growing skeleton, recommending serum calcium be maintained within the age-appropriated normal range and that phosphate-lowering treatment selection be informed by the serum calcium level. Childhood and adolescence are critical periods for bone development with the approximate calcium content of the skeleton increasing from 25 g at birth to 1000 g in adults, and approximately 25% of total skeletal mass is laid down during the 2-year interval of peak height velocity at adolescence [32]. Furthermore, medication recommendations must consider the fact that the capacity to metabolize drugs in children varies throughout development of CYP enzymes and is completed by approximately 6 years of age [30]. Given the extensive weight range common in children and our conservative dosing requirements, a weight-adjusted dosing schema was deemed warranted for cinacalcet.
Six interventional studies have been conducted to obtain information about the safety and efficacy of cinacalcet in pediatric subjects. We have assembled the data here to provide pediatric nephrologists with information that can improve patient care.
The clinical data that have been generated are generally consistent with model-based simulations that showed the pediatric cinacalcet starting dose (0.2 mg/kg/day [based on subject’s dry weight at enrolment, rounded down to the lowest PSD]), when titrated to effect, would provide the desired pharmacodynamic efficacy (PTH suppression > 30%) while minimizing safety concerns (hypocalcemia) [31]. All phases 2 and 3 clinical studies reported here used weight-based dosing to minimize exposure variability between subjects at different developmental stages. Adjusting cinacalcet doses to correct and maintain PTH within target levels [15] and to maintain calcium concentrations within age-appropriate levels [13, 14] was an effective treatment strategy that also showed an AE profile consistent with the known safety profile of cinacalcet in the treatment of adults with sHPT as listed in the prescribing information [20].
The effect of cinacalcet on PTH varied across studies. Overall, 7.4 to 57.1% of subjects who received cinacalcet in an Amgen Inc. clinical trial attained PTH levels within the K/DOQI target range and 22.2 to 70.6% observed a ≥ 30% reduction in PTH. In addition, significant reductions in PTH were demonstrated in all non-Amgen-supported studies. Furthermore, the real-world effectiveness and safety data from the retrospective chart review and the prospective registry supported the safety and efficacy findings from the clinical studies. This real-world data demonstrated that cinacalcet treatment had expected effects on biochemical markers of sHPT and no unexpected safety concerns observed, despite varied doses (mean range 0.8 to 1.9 mg/kg/day) and frequency of administration among children < 6 years of age with CKD and sHPT. The variability in PTH response may, in part, be due to the success of the dose titration. As mentioned above, in Study 20130356, the dose titration rules were conservative, and dose titration was limited based on calcium levels. This may have contributed to a smaller proportion of subjects achieving target PTH levels or at least a 30% reduction in PTH in this study. Interestingly, no significant trends in changes in calcium or phosphate levels were observed in either the Amgen or non-Amgen-supported studies. Serum calcium levels need to be closely monitored and managed during treatment with cinacalcet in children to minimize the risk of hypocalcemia.
Although not evaluated here, bone-related complications and vascular or other soft tissue calcifications are clinically important aspects of CKD-MBD. High turnover skeletal lesions in sHPT cause disproportionate bone loss that leads to thinning of cortical tissue, reductions in cortical bone mass, and an increased risk of skeletal fracture both in adults and in children with advanced CKD [4, 11, 33,34,35,36,37]. Similarly, alterations in the epiphyseal growth plate cartilage architecture can adversely affect endochondral bone formation and impair linear bone growth [38] contributing to growth retardation and to skeletal deformity in children with CKD. Data from one non-Amgen-sponsored study has suggested that cinacalcet may improve linear growth [23]; however, further validation of this finding is required. The addition of cinacalcet to SOC may offer protection against these bone-related complications. The recent BONAFIDE study showed that high rates of bone formation and several biochemical markers of high-turnover bone disease decreased toward normal as PTH was reduced during the treatment of sHPT with cinacalcet [39], potentially due to CaSR activation in osteoblasts promoting bone turnover [40]. However, these benefits should be viewed cautiously as concurrent treatment with vitamin D sterols was allowed throughout the BONAFIDE study, and their impact on bone turnover was not determined [39]. Despite advances in CKD-MBD management, subjects with CKD-MBD receiving maintenance hemodialysis, including children, still experience cardiovascular (CV) morbidity and mortality. High serum phosphorus contributes to the development of vascular calcifications in subjects undergoing dialysis [41, 42]. Indeed, due to this high CV morbidity in children with ESRD, the American Heart Association recently recommended that mineral metabolism abnormalities (i.e., high phosphorus level, sHPT) should be screened for and treated to prevent coronary artery calcification, and children should undergo regular echocardiographic monitoring for LVH [43]. Whether cinacalcet provides CV benefit remains to be fully elucidated. One systematic review of calcimimetics for sHPT in CKD patients concluded that cinacalcet had uncertain effects on CV mortality for CKD stage 5 adult patients on dialysis [44]. Additionally, the EVOLVE study failed to show significant survival benefit for adult patients with cinacalcet in the unadjusted primary analysis [45]. However, secondary analyses of EVOLVE data demonstrated lower rates of CV death and major CV events associated with treatment-induced reductions in serum FGF23 [46]. Furthermore, in two large cohort studies, cinacalcet was shown to reduce overall and CV mortality in adult patients with PTH > 300 pg/mL [47] and adult patients with moderate sHPT (PTH 300–599 pg/mL), younger age, and without diabetes [48].
This review of cinacalcet use in pediatrics has several strengths and limitations. Children with sHPT represent a very small population of subjects that frequently receive kidney transplants, creating difficulty for clinical trials in pediatric dialysis to enroll large numbers of patients, and to evaluate hard outcomes that are present in adult studies such as CV morbidity or death. Furthermore, trial data are limited by subjects discontinuing treatment for transplant. In turn, to obtain data in this patient population, it was important to consider information from multiple sources and conduct novel analyses to evaluate dosing, safety, and efficacy. We have provided the largest pediatric clinical trial data collection assessing the safety and efficacy of cinacalcet use in children with sHPT receiving dialysis in one report. Furthermore, these data are supported with findings from a comprehensive review of clinical trial and real-world data on cinacalcet use in pediatric subjects. Whereas the provision of all available data to pediatric nephrologists is warranted, the conclusions are limited by the fact that data are assessed from multiple sources and are not directly comparable. Additionally, the theoretical corrected calcium inclusion criteria used in the randomized trials (corrected calcium ≥ 8.8 mg/dL) may not reflect real-world treatment decision values guided by the summary of product characteristics and KDIGO and K/DOQI guidelines which suggest the corrected calcium should be in the upper range of, or above, the age-specified reference range prior to administration of the first dose of cinacalcet [13, 15, 22]. Furthermore, whether vitamin D sterols utilized with calcium-free phosphate binders diminish episodes of hypercalcemia was not assessed and warrants further clarification. However, the frequency of hypocalcemia in subjects receiving cinacalcet was similar between Studies 20070208 (22.7%, Table S4) and 20130356 (24.0%, Table S4) despite the presence of 2-fold more subjects in 20070208 (68.2%, Table S5) using calcium-containing phosphate binders than in 20130356 (33.3%, Table S5). Finally, due to study designs, no conclusions can be drawn on the potential impact of cinacalcet on bone density, fracture risk, and CV comorbidities.
In summary, this manuscript contains the most comprehensive review of cinacalcet usage in pediatric patients to date. A patient registry in Europe will provide additional information about the occurrence of hypocalcemia and its management in children receiving cinacalcet. In the meantime, data presented here together with recently published European guidelines [49] will aid in the management of pediatric patients with sHPT on dialysis.
References
Harambat J, van Stralen KJ, Kim JJ, Tizard EJ (2012) Epidemiology of chronic kidney disease in children. Pediatr Nephrol 27:363–373. https://doi.org/10.1007/s00467-011-1939-1
National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda, MD (2015) 2015 USRDS Annual Data Report Volume 2: ESRD in the United States. https://www.usrds.org/2015/view/. Accessed 12 June 2019
Goodman WG, Quarles LD (2008) Development and progression of secondary hyperparathyroidism in chronic kidney disease: lessons from molecular genetics. Kidney Int 74:276–288. https://doi.org/10.1038/sj.ki.5002287
Slatopolsky E, Brown A, Dusso A (2001) Role of phosphorus in the pathogenesis of secondary hyperparathyroidism. Am J Kidney Dis 37(1 Suppl 2):S54–S57
Wetmore JB, Quarles LD (2009) Calcimimetics or vitamin D analogs for suppressing parathyroid hormone in end-stage renal disease: time for a paradigm shift? Nat Clin Pract Nephrol 5:24–33. https://doi.org/10.1038/ncpneph0977
de Francisco AL, Cobo MA, Setien MA, Rodrigo E, Fresnedo GF, Unzueta MT, Amado JA, Ruiz JC, Arias M, Rodriguez M (1998) Effect of serum phosphate on parathyroid hormone secretion during hemodialysis. Kidney Int 54:2140–2145. https://doi.org/10.1046/j.1523-1755.1998.00221.x
Rees L, Schaefer F, Schmitt CP, Shroff R, Warady BA (2017) Chronic dialysis in children and adolescents: challenges and outcomes. Lancet Child Adolesc Health 1:68–77. https://doi.org/10.1016/s2352-4642(17)30018-4
KDIGO (2009) KDIGO Clinical practice guideline for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD) Kidney Int Suppl (113):S1–130. doi:https://doi.org/10.1038/ki.2009.188
Wesseling-Perry K, Pereira RC, Tseng CH, Elashoff R, Zaritsky JJ, Yadin O, Sahney S, Gales B, Juppner H, Salusky IB (2012) Early skeletal and biochemical alterations in pediatric chronic kidney disease. Clin J Am Soc Nephrol 7:146–152. https://doi.org/10.2215/cjn.05940611
Wetzsteon RJ, Kalkwarf HJ, Shults J, Zemel BS, Foster BJ, Griffin L, Strife CF, Foerster DL, Jean-Pierre DK, Leonard MB (2011) Volumetric bone mineral density and bone structure in childhood chronic kidney disease. J Bone Miner Res 26:2235–2244. https://doi.org/10.1002/jbmr.427
Denburg MR, Kumar J, Jemielita T, Brooks ER, Skversky A, Portale AA, Salusky IB, Warady BA, Furth SL, Leonard MB (2016) Fracture burden and risk factors in childhood CKD: results from the CKiD cohort study. J Am Soc Nephrol 27:543–550. https://doi.org/10.1681/asn.2015020152
Klaus G, Watson A, Edefonti A, Fischbach M, Ronnholm K, Schaefer F, Simkova E, Stefanidis CJ, Strazdins V, Vande Walle J, Schroder C, Zurowska A, Ekim M (2006) Prevention and treatment of renal osteodystrophy in children on chronic renal failure: European guidelines. Pediatr Nephrol 21:151–159. https://doi.org/10.1007/s00467-005-2082-7
KDIGO (2017) Clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD) (2017). Kidney Int Suppl 7:1–59. https://doi.org/10.1016/j.kisu.2017.04.001
Dasgupta I, Shroff R, Bennett-Jones D, McVeigh G (2013) Management of hyperphosphataemia in chronic kidney disease: summary of National Institute for Health and Clinical Excellence (NICE) guideline. Nephron Clin Pract 124:1–9. https://doi.org/10.1159/000354711
Isakova T, Nickolas TL, Denburg M, Yarlagadda S, Weiner DE, Gutierrez OM, Bansal V, Rosas SE, Nigwekar S, Yee J, Kramer H (2017) KDOQI US commentary on the 2017 KDIGO clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD). Am J Kidney Dis 70:737–751. https://doi.org/10.1053/j.ajkd.2017.07.019
Sprague SM, Wetmore JB, Gurevich K, Da Roza G, Buerkert J, Reiner M, Goodman W, Cooper K (2015) Effect of cinacalcet and vitamin D analogs on fibroblast growth Factor-23 during the treatment of secondary hyperparathyroidism. Clin J Am Soc Nephrol 10:1021–1030. https://doi.org/10.2215/cjn.03270314
Cozzolino M, Ketteler M, Martin KJ, Sharma A, Goldsmith D, Khan S (2014) Paricalcitol- or cinacalcet-centred therapy affects markers of bone mineral disease in patients with secondary hyperparathyroidism receiving haemodialysis: results of the IMPACT-SHPT study. Nephrol Dial Transplant 29:899–905. https://doi.org/10.1093/ndt/gfu011
Ketteler M, Martin KJ, Wolf M, Amdahl M, Cozzolino M, Goldsmith D, Sharma A, Marx S, Khan S (2012) Paricalcitol versus cinacalcet plus low-dose vitamin D therapy for the treatment of secondary hyperparathyroidism in patients receiving haemodialysis: results of the IMPACT SHPT study. Nephrol Dial Transplant 27:3270–3278. https://doi.org/10.1093/ndt/gfs018
Walter S, Baruch A, Dong J, Tomlinson JE, Alexander ST, Janes J, Hunter T, Yin Q, Maclean D, Bell G, Mendel DB, Johnson RM, Karim F (2013) Pharmacology of AMG 416 (velcalcetide), a novel peptide agonist of the calcium-sensing receptor, for the treatment of secondary hyperparathyroidism in hemodialysis patients. J Pharmacol Exp Ther 346:229–240. https://doi.org/10.1124/jpet.113.204834
Sensipar® (cinacalcet) prescribing information. (2011). https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/021688s017lbl.pdf Accessed 12 June 2019
Nemeth EF, Heaton WH, Miller M, Fox J, Balandrin MF, Van Wagenen BC, Colloton M, Karbon W, Scherrer J, Shatzen E, Rishton G, Scully S, Qi M, Harris R, Lacey D, Martin D (2004) Pharmacodynamics of the type II calcimimetic compound cinacalcet HCl. J Pharmacol Exp Ther 308:627–635. https://doi.org/10.1124/jpet.103.057273
Sensipar® (cinacalcet) Summary of Product Characteristics. (2018). https://www.ema.europa.eu/en/documents/product-information/mimpara-epar-product-information_en.pdf. Accessed 12 June 2019
Arenas Morales AJ, DeFreitas MJ, Katsoufis CP, Seeherunvong W, Chandar J, Zilleruelo G, Freundlich M, Abitbol CL (2019) Cinacalcet as rescue therapy for refractory hyperparathyroidism in young children with advanced chronic kidney disease. Pediatr Nephrol 34:129–135. https://doi.org/10.1007/s00467-018-4055-7
Alharthi AA, Kamal NM, Abukhatwah MW, Sherief LM (2015) Cinacalcet in pediatric and adolescent chronic kidney disease: a single-center experience. Medicine 94:e401. https://doi.org/10.1097/md.0000000000000401
Platt C, Inward C, McGraw M, Dudley J, Tizard J, Burren C, Saleem MA (2010) Middle-term use of cinacalcet in paediatric dialysis patients. Pediatr Nephrol 25:143–148. https://doi.org/10.1007/s00467-009-1294-7
Muscheites J, Wigger M, Drueckler E, Fischer DC, Kundt G, Haffner D (2008) Cinacalcet for secondary hyperparathyroidism in children with end-stage renal disease. Pediatr Nephrol 23:1823–1829. https://doi.org/10.1007/s00467-008-0810-5
Silverstein DM, Kher KK, Moudgil A, Khurana M, Wilcox J, Moylan K (2008) Cinacalcet is efficacious in pediatric dialysis patients. Pediatr Nephrol 23:1817–1822. https://doi.org/10.1007/s00467-007-0742-5
Warady BA, Iles JN, Ariceta G, Dehmel B, Hidalgo G, Jiang X, Laskin B, Shahinfar S, Vande Walle J, Schaefer F (2019) A randomized, double-blind, placebo-controlled study to assess the efficacy and safety of cinacalcet in pediatric patients with chronic kidney disease and secondary hyperparathyroidism receiving dialysis. Pediatr Nephrol 34:475–486. https://doi.org/10.1007/s00467-018-4116-y
Sohn WY, Portale AA, Salusky IB, Zhang H, Yan LL, Ertik B, Shahinfar S, Lee E, Dehmel B, Warady BA (2019) An open-label, single-dose study to evaluate the safety, tolerability, pharmacokinetics, and pharmacodynamics of cinacalcet in pediatric subjects aged 28 days to < 6 years with chronic kidney disease receiving dialysis. Pediatr Nephrol 34:145–154. https://doi.org/10.1007/s00467-018-4054-8
Padhi D, Langman CB, Fathallah-Shaykh S, Warady BA, Salusky IB, Lee E, Wang C, Posvar E (2012) An open-label study to evaluate a single-dose of cinacalcet in pediatric dialysis subjects. Pediatr Nephrol 27:1953–1959. https://doi.org/10.1007/s00467-012-2186-9
Chen P, Sohn W, Narayanan A, Gisleskog PO, Melhem M (2019) Bridging adults and paediatrics with secondary hyperparathyroidism receiving haemodialysis: a pharmacokinetic-pharmacodynamic analysis of cinacalcet. Br J Clin Pharmacol 85:1312–1325. https://doi.org/10.1111/bcp.13900
Baxter-Jones AD, Faulkner RA, Forwood MR, Mirwald RL, Bailey DA (2011) Bone mineral accrual from 8 to 30 years of age: an estimation of peak bone mass. J Bone Miner Res 26:1729–1739. https://doi.org/10.1002/jbmr.412
Cundy T, Hand DJ, Oliver DO, Woods CG, Wright FW, Kanis JA (1985) Who gets renal bone disease before beginning dialysis? Br Med J (Clin Res Ed) 290:271–275. https://doi.org/10.1136/bmj.290.6464.271
Salusky IB, Fine RN, Kangarloo H, Gold R, Paunier L, Goodman WG, Brill JE, Gilli G, Slatopolsky E, Coburn JW (1987) “High-dose” calcitriol for control of renal osteodystrophy in children on CAPD. Kidney Int 32:89–95
Coen G, Mazzaferro S, Ballanti P, Sardella D, Chicca S, Manni M, Bonucci E, Taggi F (1996) Renal bone disease in 76 patients with varying degrees of predialysis chronic renal failure: a cross-sectional study. Nephrol Dial Transplant 11:813–819. https://doi.org/10.1093/oxfordjournals.ndt.a027404
Spasovski GB, Bervoets AR, Behets GJ, Ivanovski N, Sikole A, Dams G, Couttenye MM, De Broe ME, D'Haese PC (2003) Spectrum of renal bone disease in end-stage renal failure patients not yet on dialysis. Nephrol Dial Transplant 18:1159–1166. https://doi.org/10.1093/ndt/gfg116
Sanchez CP (2003) Secondary hyperparathyroidism in children with chronic renal failure: pathogenesis and treatment. Paediatr Drugs 5:763–776. https://doi.org/10.2165/00148581-200305110-00005
Kuizon BD, Salusky IB (1999) Growth retardation in children with chronic renal failure. J Bone Miner Res 14:1680–1690. https://doi.org/10.1359/jbmr.1999.14.10.1680
Behets GJ, Spasovski G, Sterling LR, Goodman WG, Spiegel DM, De Broe ME, D'Haese PC (2015) Bone histomorphometry before and after long-term treatment with cinacalcet in dialysis patients with secondary hyperparathyroidism. Kidney Int 87:846–856. https://doi.org/10.1038/ki.2014.349
Diaz-Tocados JM, Rodriguez-Ortiz ME, Almaden Y, Pineda C, Martinez-Moreno JM, Herencia C, Vergara N, Pendon-Ruiz de Mier MV, Santamaria R, Rodelo-Haad C, Casado-Diaz A, Lorenzo V, Carvalho C, Frazao JM, Felsenfeld AJ, Richards WG, Aguilera-Tejero E, Rodriguez M, Lopez I, Munoz-Castaneda JR (2019) Calcimimetics maintain bone turnover in uremic rats despite the concomitant decrease in parathyroid hormone concentration. Kidney Int 95:1064–1078. https://doi.org/10.1016/j.kint.2018.12.015
Shroff R, Long DA, Shanahan C (2013) Mechanistic insights into vascular calcification in CKD. J Am Soc Nephrol 24:179–189. https://doi.org/10.1681/asn.2011121191
Khouzam NM, Wesseling-Perry K, Salusky IB (2015) The role of bone in CKD-mediated mineral and vascular disease. Pediatr Nephrol 30:1379–1388. https://doi.org/10.1007/s00467-014-2919-z
de Ferranti SD, Steinberger J, Ameduri R, Baker A, Gooding H, Kelly AS, Mietus-Snyder M, Mitsnefes MM, Peterson AL, St-Pierre J, Urbina EM, Zachariah JP, Zaidi AN (2019) Cardiovascular risk reduction in high-risk pediatric patients: a scientific statement from the American Heart Association. Circulation 139:e603–e634. https://doi.org/10.1161/cir.0000000000000618
Ballinger AE, Palmer SC, Nistor I, Craig JC, Strippoli GF (2014) Calcimimetics for secondary hyperparathyroidism in chronic kidney disease patients. Cochrane Database Syst Rev (12):Cd006254. doi:https://doi.org/10.1002/14651858.CD006254.pub2
Chertow GM, Block GA, Correa-Rotter R, Drueke TB, Floege J, Goodman WG, Herzog CA, Kubo Y, London GM, Mahaffey KW, Mix TC, Moe SM, Trotman ML, Wheeler DC, Parfrey PS (2012) Effect of cinacalcet on cardiovascular disease in patients undergoing dialysis. N Engl J Med 367:2482–2494. https://doi.org/10.1056/NEJMoa1205624
Moe SM, Chertow GM, Parfrey PS, Kubo Y, Block GA, Correa-Rotter R, Drueke TB, Herzog CA, London GM, Mahaffey KW, Wheeler DC, Stolina M, Dehmel B, Goodman WG, Floege J (2015) Cinacalcet, fibroblast growth Factor-23, and cardiovascular disease in hemodialysis: the Evaluation of Cinacalcet HCl Therapy to Lower Cardiovascular Events (EVOLVE) trial. Circulation 132:27–39. https://doi.org/10.1161/circulationaha.114.013876
Akizawa T, Kurita N, Mizobuchi M, Fukagawa M, Onishi Y, Yamaguchi T, Ellis AR, Fukuma S, Alan Brookhart M, Hasegawa T, Kurokawa K, Fukuhara S (2016) PTH-dependence of the effectiveness of cinacalcet in hemodialysis patients with secondary hyperparathyroidism. Sci Rep 6:19612. https://doi.org/10.1038/srep19612
Friedl C, Reibnegger G, Kramar R, Zitt E, Pilz S, Mann JFE, Rosenkranz AR (2017) Mortality in dialysis patients with cinacalcet use: a large observational registry study. Eur J Intern Med 42:89–95. https://doi.org/10.1016/j.ejim.2017.05.002
Bacchetta J, Schmitt CP, Ariceta G, Bakkaloglu SA, Groothoff J, Wan M, Vervloet M, Shroff R, Haffner D (2019) Cinacalcet use in paediatric dialysis: a position statement from the European Society for Paediatric Nephrology and the Chronic Kidney Disease-Mineral and Bone Disorders Working Group of the ERA-EDTA. Nephrol Dial Transplant. https://doi.org/10.1093/ndt/gfz159
Acknowledgements
The authors acknowledge Jonathan Plumb, PhD (Fishawack Communications Inc., funded by Amgen Inc.), Kate Smigiel, PhD, and William W Stark, Jr., PhD (both employees and stockholders, Amgen, Inc.) for assistance with the writing of this manuscript.
Funding
This study was funded by Amgen Inc., Thousand Oaks, CA, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Bradley A. Warady has received consulting fees from Amgen, Inc. Eric Ng, Laura Bloss, and May Mo are employees of and own stock in Amgen Inc. Franz Schaefer has received personal fees from Amgen Inc. Justine Bacchetta has received research grants and consulting fees from Amgen, Inc.
Data sharing agreement
There is a plan to share data. This may include de-identified individual patient data for variables necessary to address the specific research question in an approved data-sharing request; also, related data dictionaries, study protocol, statistical analysis plan, informed consent form, and/or clinical study report. Data sharing requests relating to data in this manuscript will be considered after the publication date, and (1) this product and indication (or other new use) have been granted marketing authorization in both the USA and Europe, or (2) clinical development discontinues and the data will not be submitted to regulatory authorities. There is no end date for eligibility to submit a data sharing request for these data. Qualified researchers may submit a request containing the research objectives, the Amgen product(s) and Amgen study/studies in scope, endpoints/outcomes of interest, statistical analysis plan, data requirements, publication plan, and qualifications of the researcher(s). In general, Amgen does not grant external requests for individual patient data for the purpose of reevaluating safety and efficacy issues already addressed in the product labelling. A committee of internal advisors reviews requests. If not approved, requests may be further arbitrated by a Data Sharing Independent Review Panel. Requests that pose a potential conflict of interest or an actual or potential competitive risk may be declined at Amgen’s sole discretion and without further arbitration. Upon approval, information necessary to address the research question will be provided under the terms of a data sharing agreement. This may include anonymized individual patient data and/or available supporting documents, containing fragments of analysis code where provided in analysis specifications. Further details are available at the following: https://www.amgen.com/science/clinical-trials/clinical-data-transparency-practices/
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Warady, B.A., Ng, E., Bloss, L. et al. Cinacalcet studies in pediatric subjects with secondary hyperparathyroidism receiving dialysis. Pediatr Nephrol 35, 1679–1697 (2020). https://doi.org/10.1007/s00467-020-04516-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04516-4