Abstract
Purpose
To compare bacterial findings in pain-generating degenerated discs in adults operated on for lumbar disc herniation (LDH), and mostly also suffering from low back pain (LBP), with findings in adolescent patients with non-degenerated non-pain-generating discs operated on for scoliosis, and to evaluate associations with Modic signs on magnetic resonance imaging (MRI). Cutibacterium acnes (Propionibacterium acnes) has been found in painful degenerated discs, why it has been suggested treating patients with LDH/LBP with antibiotics. As multidrug-resistant bacteria are a worldwide concern, new indications for using antibiotics should be based on solid scientific evidence.
Methods
Between 2015 and 2017, 40 adults with LDH/LBP (median age 43, IQR 33–49) and 20 control patients with scoliosis (median age 17, IQR 15–20) underwent surgery at seven Swedish hospitals. Samples were cultured from skin, surgical wound, discs and vertebrae. Genetic relatedness of C. acnes isolates was investigated using single-nucleotide polymorphism analysis. DNA samples collected from discs/vertebrae were analysed using 16S rRNA-based PCR sequencing. MRI findings were assessed for Modic changes.
Results
No bacterial growth was found in 6/40 (15%) LDH patients, compared with 3/20 (15%) scoliosis patients. Most positive samples in both groups were isolated from the skin and then from subcutis or deep within the wound. Of the four disc and vertebral samples from each of the 60 patients, 235/240 (98%) were DNA negative by bacterial PCR. A single species, C. acnes, was found exclusively in the disc/vertebra from one patient in each group. In the LDH group, 29/40 (72%) patients had at least one sample with growth of C. acnes, compared to 14/20 (70%) in the scoliosis group. Bacterial findings and Modic changes were not associated.
Conclusions
Cutibacterium acnes found in discs and vertebrae during surgery for disc herniation in adults with degenerated discs may be caused by contamination, as findings in this group were similar to findings in a control group of young patients with scoliosis and non-degenerated discs. Furthermore, such findings were almost always combined with bacterial findings on the skin and/or in the wound. There was no association between preoperative Modic changes and bacterial findings. Antibiotic treatment of lumbar disc herniation with sciatica and/or low back pain, without signs of clinical discitis/spondylitis, should be seriously questioned.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Low back pain (LBP) frequently accompanies lumbar disc herniation (LDH) with sciatica. Globally, LBP is currently the leading cause of disability and poses a heavy burden to healthcare systems [1, 2]. In a recent issue of the Lancet, several task forces present a major overview of LBP including the challenges faced by professionals, administrators and politicians [3, 4].
It has been suggested that LBP may be the result of a low-grade infection caused by the anaerobic skin bacterium Cutibacterium acnes (formerly Propionibacterium acnes). This is based on studies that have found this bacterium using culture of degenerative lumbar disc material, and researchers have suggested that some patients with LDH/LBP could be treated with antibiotics [5,6,7,8,9]. Hypothetically, haematogenous spread of bacteria to a disc may cause pain through host release of pro-inflammatory substances [10]. Some researchers have argued that we indeed may face a paradigm shift in the treatment of LDH/LBP [11]. Others argue that isolation of bacteria from discs during LDH surgery is likely due to contamination [12, 13]. A causative relationship has been suggested between a low-grade infection in vertebrae adjacent to a degenerated disc and an inflammatory process identified on magnet resonance imaging (MRI), i.e. Modic type 1 changes [14, 15]. Regardlessly, severe and disabling LBP seems to be associated with Modic changes [16].
In view of worldwide concern about the increase in bacterial resistance to both common and critically important antibiotics [17], it is crucial to question new indications for antibiotic treatment unless backed by substantial scientific evidence. Such a treatment strategy in LBP/LDH could have far-reaching consequences for the development and spread of antibiotic resistance [18]. Thus, the association, and causal relationship, between LBP/LDH and low-grade infections must be confirmed [19].
The primary aim of this surgical, prospective, observational, comparative, multicentre and multidisciplinary study (surgery–microbiology–radiology) was to investigate the presence of bacteria in disc/vertebra in adult patients with painful LDH and compare these findings with findings in control patients without painful degenerative discs, here adolescents with scoliosis. Our hypothesis was that bacteria were not present in the scoliosis group.
The study was approved by the ethical committee in Linköping (EPN, ref. no. 2015/152–31). All patients gave their written informed consent.
Methods
Study design
To identify bacteria, culturing in one independent university laboratory was performed. In addition, DNA analyses were performed in two independent university laboratories. Preoperative Modic changes were assessed.
A video describing the sampling procedures was distributed to the participating centres before study start (Supplement 2). The same research nurse visited all centres prior to the first surgery to show the video and to discuss topics such as sampling details, transportation of samples and other aspects with the involved staff. This nurse also participated in the first surgical procedure at each clinic and provided phone and/or e-mail support during subsequent procedures as needed.
Anonymised data were stored in a database according to national healthcare regulations.
Patients
The study was conducted in 2015–2017. Sixty patients were included. Forty adults with degenerated discs and LDH/LBP: 23 males and 17 females, median age 43 years (IQR 33–49), and 20 adolescent control scoliosis patients without degenerated discs: 7 males and 13 females, median age 17 years (IQR 15–20). Seven Swedish centres performed the surgery.
Inclusion: Any surgical candidate with LDH, or with scoliosis, who agreed to participate and who would have undergone surgery regardless of the study.
Exclusion: Ongoing infection with or without antibiotic treatment, antibiotic treatment within two weeks of study start, prior treatment for discitis/spondylitis, attenuated immune response, autoimmune disease, rheumatic arthritis, prior back surgery, prior epidural pain injections or other reasons for ineligibility (language problems).
Bacterial samples–collection, culturing and DNA analyses
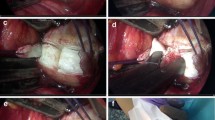
Samples were collected with swabs from skin taken after the patients “self-washing”, but before the preop skin disinfection by the scrub nurse, subcutaneous tissue and from over the vertebral laminae. Biopsies were obtained from the vertebra and the disc. All samples were sent for culturing and DNA analyses at the Clinical Microbiology Laboratory at Sahlgrenska University Hospital in Gothenburg. Samples from disc/vertebra were also sent to Department of Cell and Molecular Biology, Biomedical Center, Uppsala University, for DNA analyses. Polymerase chain reaction (PCR) was used to independently analyse the samples using universal 16S rRNA primers in these two laboratories (Supplement 3).
Samples for culturing were transported in ESwab tubes (Copan Diagnostics, Murrieta, CA), whilst samples from disc/vertebra were transported refrigerated in sterile saline.
Scoliosis patients operated with an anterior approach (n = 14) had their discs exposed as part of routine procedure, whilst patients operated with a posterior approach (n = 6) were sampled in the same way as LDH patients. The routine prophylactic antibiotics used at each centre were administered immediately prior to obtaining biopsy samples from the disc/vertebra in the LDH group, and immediately before skin incision in the scoliosis patients.
MRI. Preoperative MRI findings were assessed by a single experienced radiologist. The classification scheme advocated by the Nordic Modic Consensus Group Classification was used, which has a high intra- and interobserver reliability [20] (Supplement 4). Patients in the LDH group were analysed for Modic endplate changes at the operated disc level (Fig. 1), but Modic changes at adjacent disc levels (above and below the LDH level) were also reported (Supplement 5). In the scoliosis control group, MRI classification was performed at the biopsy level.
Statistical analysis
To yield a statistical power of 95% with an alpha of 0.05, enrolment ratio of 2:1 and an anticipated incidence of 44% in the LDH group and 0% in the control group, 29 patients were to be included in the LDH group and 14 in the control group. To allow for possible loss of samples during transportation or handling, the respective groups were decided to 40 and 20 patients each. Fisher’s exact test (two-tailed) was used for comparisons. A P-value < 0.05 was considered statistically significant.
Results
Patients
Low back pain and sciatica
Preoperatively, in the LDH group sciatica and LBP occurred simultaneously in well over 90%.
Bacterial growth
Abundant growth was reported from the skin (presterilisation), and subcutaneously in both groups, with a wide range of bacterial species, and there was a tendency towards a growth gradient of C. acnes from the skin to the disc/vertebrae (Supplements 6 and 7). Only sparse growth was found in the discs/vertebrae, and in contrast to skin samples, almost all bacterial findings in the discs/vertebrae belonged to the species C. acnes.
Nine patients (15%) had no growth at any site, with no prominence associated with any of the seven operating centres; 6/40 (15%) were LDH patients and 3/20 (15%) were scoliosis patients. Of the LDH patients, 29/40 (72%) had at least one sample with growth of C. acnes, compared with 14/20 (70%) in the control group. The positive samples in both groups were mainly isolated from skin, subcutis or deep within the wound. Of the 29 LDH patients with at least one sample of C. acnes growth at any site outside the disc/vertebra, 13 (43%) also showed growth of C. acnes in at least one sample from the disc/vertebra, compared with 4/14 patients (29%) in the control group (ns). In all, 26/40 LDH patients (65%) and 15/20 control patients (75%) showed no growth of C. acnes in the disc/vertebra (ns). In one single patient from each group, C. acnes grew only in the disc/vertebra (Fig. 2).
Analysis of bacterial DNA
Of the four disc and vertebral samples from each of the 60 patients, 235/240 (98%) were DNA negative. None of the five remaining samples, but one, yielded a positive PCR product of the same bacterial species as detected by culturing. Two biopsies, both from LDH patients, yielded a PCR product in Gothenburg, one of which was culture negative but contained DNA from Streptococcus sp. and Lactococcus lactis, whilst the other was positive for C. acnes both by culture and 16S rRNA PCR. Three biopsies were positive in Uppsala, two of which were from LDH patients (DNA from the species Corynebacterium and Burkholderiales was detected, respectively) and one from a scoliosis patient (in which specimen DNA from the species Corynebacterium was detected).
Genetic relatedness between C. acnes isolates
In 15 patients (including both groups), one C. acnes isolate from discs and/or vertebrae and one isolate from the skin and/or soft tissues were investigated for genetic relatedness. The isolates from the different tissues in 5/11 LDH patients (45%) belonged to the same strain, suggesting contamination from the skin to the disc/vertebrae, whereas 6/11 LDH and 4/4 scoliosis patients had different strains at the sampling sites. The differences in single-nucleotide polymorphisms (SNPs) between isolates of the same strain were 17 or less. Non-genetically related isolates had at least 10 times this difference in SNPs, usually in the range of 100–1000 × as many.
Modic changes on MRI and association to bacterial findings
In the LDH group, 23/40 patients (58%) had some type of Modic change in one or both vertebrae adjacent to the LDH level: Modic 1 = 5/40 (13%) and Modic 2 = 18/40 (45%); none had Modic 3 (sclerosis). Most endplate changes showed little extension in maximum height; 81% extended less than 25% of vertebral height. The distribution between Modic changes and no Modic changes was equivalent in the four “bacterial findings groups”: (0) no bacteria in any samples; (1) bacteria only in disc/vertebra; (2) bacteria only in surrounding soft tissues; and 3. bacteria in surrounding soft tissues and in disc/vertebra (Fig. 3). For distribution of Modic changes, see Supplement 8.
Association between Modic changes and bacterial findings in the two groups; (0) no bacteria anywhere, (1) bacteria only in disc/vertebra, (2) bacteria only in soft tissues, (3) bacteria in soft tissues and in disc or vertebra. The bacterium found in one scoliosis patient was not in the disc/vertebra
Modic 1 was not detected in any patient who was culture positive for bacteria in discs/vertebrae. In the control group, 18/20 scoliosis patients underwent MRI before surgery. One patient had a minor Modic 2 change adjacent to a Schmorl’s node with no bacterial findings in the disc/vertebra (Fig. 3).
Discussion
We conducted a multicentre study including 60 surgically treated patients. In all, 40 adults with a degenerated disc/painful lumbar disc herniation (LDH/LBP) and 20 adolescent scoliosis patients without painful lumbar discs (controls) were surgically treated for their scoliosis and compared for the presence of bacteria. Seven orthopaedic clinics participated under real-life conditions. The study was conducted as it has been suggested that low back pain (LBP) with or without lumbar disc herniation (LDH) may be due to low-grade infection caused by the common skin bacteria C. acnes (formerly Propionibacterium acnes) and may be treated with antibiotics. We found that such bacterial findings in discs and vertebrae were rare in both groups, and almost always detected in conjunction with abundance of the same agent on the skin or in the wound (Supplement 7). In short,
-
(1)
An equivalent abundant bacterial growth was found on the skin (the majority) and also in the surrounding tissues of the disc/vertebra in the LDH group and scoliosis group, 50% and 60%, respectively, and in combination with growth in the disc/vertebra, 33% and 20%. The overwhelmingly predominant species were C. acnes, 72% in the LDH group and 70% in the scoliosis group. Thus, we found approximately the same amount of C. acnes in both skin and other tissues as well as in disc/vertebrae in both degenerated discs with Modic changes and in young non-degenerated discs without Modic changes.
-
(2)
In all 98% of disc and vertebral biopsies showed no DNA related to bacterial species found in bacterial cultures. This contradicts bacterial growth in the biopsies.
-
(3)
In 5/11 patients in the LDH group, we found the same strains of C. acnes in samples from disc/vertebrae and surrounding tissues when isolated from the same patient, suggesting contamination from the skin to the disc/vertebrae. The reason why not all patients, none in the control group and 6/11 in the LDH group, had the same strain identified in disc/vertebrae and surrounding tissues is probably due to the existence of several strains of C. acnes on the skin simultaneously.
-
(4)
None of the five cases with Modic changes type 1 in the LDH group had positive bacterial growth in disc/vertebra.
Why some patients with LDH/LBP experience pain and others do not is not fully understood, but in patients with painful LDH, LBP is almost always present as well (in all but one patient in the current study) which is in accordance with the Swedish National Spine Register, Swespine [21]. The pain-producing mechanisms may be mechanical and/or biochemical. Theoretically a subclinical infection in the disc caused by low-virulence microorganisms could remain undiagnosed and still result in secretion of pro-inflammatory cytokines that activate pain-producing nociceptors [10]. Kahn et al. [22] reported that C. acnes could produce an autoimmune response in joints leading to inflammation and pain, and Stirling et al. hypothesised from serology and culturing studies that C. acnes could be responsible for sciatica in patients with disc herniation [9]. Other researchers found no C. acnes in disc material [13, 23]. In a double-blinded RCT with 162 patients suffering from chronic LBP after previous disc herniation and Modic type 1 changes (sic), Albert et al. reported that 100 days of treatment with broad-spectrum amoxicillin/clavulanic (Bioclavid) acid was significantly more effective than placebo in all primary and secondary outcomes [8].
The significance and aetiology of Modic changes on MRI as a diagnostic tool in patients with a possible, and potentially a painful infection in disc/vertebrae, are gaining interest, but remain controversial [15, 24,25,26,27].
In our study, the overwhelmingly predominant bacterial species growing in discs or vertebrae was C. acnes, which is in line with findings from other research groups [5,6,7, 9, 11] and explains why so much effort has been dedicated to evaluating its possible association with LBP/LDH. The reason for finding C. acnes may, however, be related to contamination during the surgical procedure since this organism is present in the skin of virtually all adolescents/adults. As an aerotolerant anaerobe, it resides in hair follicles and sebaceous glands, making it difficult to eliminate with presurgical disinfection [28]. Figure 2 illustrates the findings of any bacteria in the two groups, and in Supplement 8, we present an illustration with only C. acnes. The results are the same.
Over the past two decades, improved diagnostics have increasingly highlighted the role of C. acnes in implant-associated infections. The 16S rRNA gene PCR has played an important role in detecting the presence of bacteria in biofilm. Biofilm was not investigated in our study, although it has in fact been reported from disc material [29,30,31,32].
Culturing is the most sensitive method for detecting bacteria, for which reason it was selected as the primary method, with the addition of DNA analysis using PCR and sequencing.
Only one patient in each group was culture positive exclusively for C. acnes in tissue samples from the disc/vertebra. DNA methodology failed to detect additional presence of C. acnes but was able to identify possible contaminants. None of the species identified through DNA sequencing was confirmed with other methodology except the one case of C. acnes, indicating that no bacteria were overlooked due to culturing problems or transportation delays.
Since C. acnes is usually not invasive and does not cause deep tissue infection, sequential findings of the same strain in the skin and in other tissues deeper within the surgical wound point towards contamination from the skin, as was the case with several patients in our study.
Proteomic analyses of removed disc material from patients operated for LDH have detected protein findings of C. acnes, and this has been suggested as a support for the “bacteria theory” and even as a “paradigm shift” in the treatment of LBP [11]. Such findings, however, could alternatively be due to contamination, as suggested by our present findings of larger amounts of the same bacteria on the skin and/or in the wounds of the patients that were positive also in discs or vertebras. Our findings demonstrate the capricious nature of culturing C. acnes and the unexpected findings of positive cultures in non-degenerated young discs. It was very common with bacteria on the skin and tissues surrounding the disc/vertebra, but it was very unusual with bacteria only in the disc/vertebrae, which indicates that the probability of contamination as an explanation of finding positive C. acnes cultures during surgery in discs is high.
Weakness of the study
We primarily explored whether an opportunistic organism like C. acnes found in disc/vertebra samples could be due to contamination. Universal 16S rRNA primers were used; in principle, such methodology should detect any bacterial species. It is possible that the sensitivity of the PCR assay would have been higher if primers specifically targeting the rRNA of C. acnes had been used. However, such an approach would only detect the predetermined species. Peak colonisation with C. acnes is found in males aged 15–19 years [33], and it is possible that positive findings from this group resulted in relative overrepresentation. However, the ratio of men/women in the scoliosis group was 7:13, with no relevant difference in findings.
Strength of the study
The strengths of this clinical study are that it is prospective, comparative, systematic and multicentre and that a sequential sampling strategy for bacterial detection was used during the operations. All this was demonstrated in a video and presented by a study nurse well in advance of the first operation at every centre. This study nurse also participated at the first operation at every centre. We have analysed samples from discs and vertebrae and from skin and surgical wound originating from patients operated for LDH, whilst using a unique control group with non-degenerated discs.
Conclusion
Cutibacterium acnes found in discs and vertebrae during surgery for disc herniation in adults with degenerated discs may be caused by contamination, as findings in this group were similar to findings in a control group of young patients with scoliosis and non-degenerated discs, and regularly combined with larger amounts of the same bacterial species in skin and wound. There was no association between preoperative Modic changes and bacteria. Antibiotic treatment of lumbar disc herniation with sciatica and/or low back pain, without signs of clinical discitis/spondylitis, should be seriously questioned.
Change history
29 October 2019
Unfortunately, the 5th author name was incorrectly published in the original paper. The complete correct name is given below.
References
Murray CJ, Lopez AD (2013) Measuring the global burden of disease. N Engl J Med 369(5):448–457
Clark S, Horton R (2018) Low back pain: a major global challenge. Lancet 391(10137):2302
Buchbinder R, van Tulder M, Oberg B et al (2018) Low back pain: a call for action. Lancet 391(10137):2384–2388
Foster NE, Anema JR, Cherkin D et al (2018) Prevention and treatment of low back pain: evidence, challenges, and promising directions. Lancet 391(10137):2368–2383
Capoor MN, Ruzicka F, Machackova T, Jancalek R, Smrcka M et al (2016) Prevalence of propionibacterium acnes in intervertebral discs of patients undergoing lumbar microdiscectomy: a prospective cross-sectional study. PLOS 11:e0161676
Urquhart DM, Zheng Y, Cheng AC, Rosenfeld JV, Chan P, Liew S, Hussain SM, Cicuttini FM (2015) Could low grade bacterial infection contribute to low back pain? A systematic review. BMC Med 13:13
Rollason J, McDowell A, Albert HB, Barnard E, Worthington T, Hilton AC, Vernallis A, Patrick S, Elliott T, Lambert P (2013) Genotypic and antimicrobial characterisation of Propionibacterium acnes isolates from surgically excised lumbar disc herniations. BioMed Res Int 20:530382
Albert HB, Sorensen JS, Christensen BS et al (2013) Antibiotic treatment in patients with chronic low back pain and vertebral bone edema (Modic type 1 changes): a double-blind randomized clinical controlled trial of efficacy. Eur Spine J 22(4):697–707
Stirling A, Worthington T, Rafiq M et al (2001) Association between sciatica and propionibacterium acnes. Lancet 357(9273):2024–2025
Brisby H, Olmarker K, Larsson K et al (2002) Proinflammatory cytokines in cerebrospinal fluid and serum in patients with disc herniation and sciatica. Eur Spine J 11(1):62–66
Rajasekaran S, Tangavel C, Aiyer SN et al (2017) ISSLS prize in clinical science 2017: Is infection the possible initiator of disc disease? An insight from proteomic analysis. Eur Spine J 26(5):1384–1400
Birkenmaier C (2013) Should we start treating chronic low back pain with antibiotics rather than with pain medications? Korean J Pain 4:327–335
Wedderkopp N, Thomsen K, Manniche C et al (2009) No evidence for presence of bacteria in modic type I changes. Acta Radiol 50(1):65–70
Modic MT, Steinberg PM, Ross JS et al (1988) Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 166(1 Pt 1):193–199
Albert HB, Lambert P, Rollason J et al (2013) Does nuclear tissue infected with bacteria following disc herniations lead to Modic changes in the adjacent vertebrae? Eur Spine J 22(4):690–696
Maatta JH, Wadge S, MacGregor A et al (2015) ISSLS prize winner: vertebral endplate (modic) change is an independent risk factor for episodes of severe and disabling low back pain. Spine 40(15):1187–1193
Tagliabue A, Rappuoli R (2018) Changing priorities in vaccinology: antibiotic resistance moving to the top. Front Immunol 9:1068
van Duin D, Paterson DL (2016) Multidrug-resistant bacteria in the community: trends and lessons learned. Infect Dis Clin N Am 30(2):377–390
Ganko R, Rao PJ, Phan K et al (2015) Can bacterial infection by low virulent organisms be a plausible cause for symptomatic disc degeneration? A systematic review. Spine 40(10):E587–E592
Jensen TS, Sorensen JS, Kjaer P (2007) Intra- and interobserver reproducibility of vertebral endplate signal (Modic) changes in the lumbar spine: the Nordic modic consensus group classification. Acta Radiol 48(7):748–754
Strömqvist B, Hägg PFO, Knutsson B, Sandén B (2014) Swespine—the swedish spine register 2014 report september 2014 swedish society of spinal surgeons. ISBN: 978-91-88017-00-0. http://www.4s.nu/pdf/Report_2014_Swespine_Engl_ver_141204.pdf
Kahn MF (1995) Why the “SAPHO” syndrome? J Rheumatol 22(11):2017–2019
Fritzell P, Bergstrom T, Welinder-Olsson C (2004) Detection of bacterial DNA in painful degenerated spinal discs in patients without signs of clinical infection. Eur Spine J 13(8):702–706
Albert HB, Kjaer P, Jensen TS, Sorensen JS, Bendix T, Manniche C (2008) Modic changes, possible causes and relation to low back pain. Med Hypothes 70:361–368 Epub 2007 Jul 10
Albert HB, Lambert P, Rollason J, Sorensen JS, Worthington T, Pedersen MB, Nørgaard HS, Vernallis A, Busch F, Manniche S, Elliott T (2013) Is nuclear tissue infected with bacteria following disc herniations which leads to Modic changes in the adjacent vertebrae? Eur Spine J 22:690–696
Crockett MT, Kelly BS, van Baarsel S et al (2017) Modic type 1 vertebral endplate changes: injury, inflammation, or infection? AJR Am J Roentgenol 209(1):167–170
Kanna RM, Shanmuganathan R, Rajagopalan VR et al (2017) Prevalence, patterns, and genetic association analysis of Modic vertebral endplate changes. Asian Spine J 11(4):594–600
Christensen GJ, Bruggemann H (2014) Bacterial skin commensals and their role as host guardians. Benef Microbes 5(2):201–215
Capoor MN, Ruzicka F, Schmitz JE et al (2017) Propionibacterium acnes biofilm is present in intervertebral discs of patients undergoing microdiscectomy. PLoS ONE 12(4):e0174518
Ohrt-Nissen et al (2018) Bacterial biofilms: a possible mechanism for chronic infection in patients with lumbar disc herniation—a prospective proof-of-concept study using fluorescence in situ hybridization. APMIS 126(5):440–447
Coscia MF, Denys GA, Wack MF (2016) Propionibacterium acnes, coagulase-negative staphylococcus, and the “biofilm-like” intervertebral disc. Spine (Phila Pa 1976) 41(24):1860–1865
Ohrt-Nissen Fritz B, Walbom J et al (2018) Bacterial biofilms: a possible mechanism for chronic infection in patients with lumbar disc herniation—a prospective proof-of-concept study using fluorescence in situ hybridization. APMIS 126(5):440–447
Miura Y, Ishige I, Soejima N et al (2010) Quantitative PCR of Propionibacterium acnes DNA in samples aspirated from sebaceous follicles on the normal skin of subjects with or without acne. J Med Dental Sci 57(1):65–74
Acknowledgements
Open access funding provided by Jönköping University. Catharina Strömstedt, Study nurse, Uppsala university Hospital. Anastasios Charalampidis, MD, Karolinska University Hospital. Hans Möller, MD, PhD, Karolinska University Hospital. Kourosh Jalalpour, MD, Karolinska University Hospital. Panayiotis Savvides, MD, Karolinska University Hospital. Anna Granqvist BMA, Sahlgrenska University Hospital. Kerstin Florén, BMA, Sahlgrenska University Hospital. Feda Haj Salem, BMA, Sahlgrenska University Hospital. Per Jallinder Björkman BMA, Sahlgrenska University Hospital. Kamran Alavi, St Göran Hospital, Stockholm, Sweden.
Funding
The study was funded by FORSS, a Swedish regional research foundation: http://www.fou.nu/is/forss/, which had no role in any part of the study, including study design, data collection, analyses and interpretation of data, or in the writing of the report.
Author information
Authors and Affiliations
Contributions
PF MD, Associate Professor. Study design, literature search, drafting, figures, data acquisition, analysis and interpretation, writing, revising, final approval, accountable for all aspects of the study. HT, MD, Professor. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. PG, MD, Associate Professor. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. OH, MD, PhD. Spine Center Göteborg, Sweden. Study design, data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. HL, MD. Spine Center Göteborg, Göteborg, Sweden. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. BK MD, PhD. Sundsvalls Hospital, Sundsvall. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. AL MD, Örebro University Hospital, Örebro, Sweden. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. PE MD, PhD. Södersjukhuset, Stockholm, Sweden. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. ER MD. Södersjukhuset, Stockholm, Sweden. Data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. C-WO PhD. Study design, literature search, data acquisition, data analysis, data interpretation, writing revising, final approval and accountable for all aspects of the study. BJ PhD. Study design, literature search, data acquisition, data analysis, data interpretation, writing, revising, final approval and accountable for all aspects of the study. ÅM MD, Professor. Study design, literature search, data acquisition, data interpretation, writing, revising, final approval and accountable for all aspects of the study. SA Professor. Study design, literature search, data acquisition, data interpretation, writing, revising, final approval and accountable for all aspects of the study. TB MD, Professor. Study design, literature search, data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study. MS MD, PhD. Study design, literature search, data acquisition, data interpretation, revising, final approval and accountable for all aspects of the study.
Corresponding author
Ethics declarations
Conflict of interest
No author had any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original article was revised to update the 5th author name as Siv G.E. Andersson.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary file2 (MP4 363704 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Fritzell, P., Welinder-Olsson, C., Jönsson, B. et al. Bacteria: back pain, leg pain and Modic sign—a surgical multicentre comparative study. Eur Spine J 28, 2981–2989 (2019). https://doi.org/10.1007/s00586-019-06164-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06164-1