Abstract
Neuroendocrine neoplasms (NENs), which are characterized by neuroendocrine differentiation, can arise in various organs. NENs have been divided into well-differentiated neuroendocrine tumors (NETs) and poorly differentiated neuroendocrine carcinomas (NECs) based on morphological differentiation, each of which has a distinct etiology, molecular profile, and clinicopathological features. While the majority of NECs originate in the pulmonary organs, extrapulmonary NECs occur most predominantly in the gastro-entero-pancreatic (GEP) system. Although platinum-based chemotherapy is the main therapeutic option for recurrent or metastatic GEP-NEC patients, the clinical benefits are limited and associated with a poor prognosis, indicating the clinically urgent need for effective therapeutic agents. The clinical development of molecular-targeted therapies has been hampered due to the rarity of GEP-NECs and the paucity of knowledge on their biology. In this review, we summarize the biology, current treatments, and molecular profiles of GEP-NECs based on the findings of pivotal comprehensive molecular analyses; we also highlight potent therapeutic targets for future precision medicine based on the most recent results of clinical trials.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Neuroendocrine neoplasms (NENs), which are characterized by neuroendocrine differentiation, can arise in various organs. NENs have generally been divided into two types based on morphological differentiation: neuroendocrine tumors (NETs) and neuroendocrine carcinomas (NECs) [1], each of which is associated with a distinct etiology, molecular profile, clinicopathological features, and treatment strategies. NECs in particular are defined by their poorly differentiated morphology and high proliferative activity [1, 2]. The transformation from a well-differentiated NET to a poorly differentiated NEC is an extremely rare event. A majority of NECs originate de novo. Alternatively, they emerge through trans-neuroendocrine differentiation of non-neuroendocrine epithelial cancers via the acquisition of genomic and epigenetic alterations during disease progression and under selective pressure, as in the case of targeted therapies within the tumor microenvironment [3,4,5]. Although approximately 90% of NECs originate from pulmonary organs, extrapulmonary NECs occur most commonly in the gastro-entero-pancreatic (GEP) system [6]. GEP-NEC is often diagnosed at advanced disease stages with distant metastases due to the highly aggressive behavior associated with rapid disease progression [6, 7]. Although systemic chemotherapy is the main therapeutic option for patients with metastatic GEP-NEC, the prognosis is extremely poor, with a 5-year overall survival (OS) rate of less than 5% [6]. In addition, the advancement of therapeutic strategies has seen very limited progress. Therefore, further development of novel agents is required to improve prognostic outcomes.
The existing strategy for treating GEP-NEC has been extrapolated from methods directed toward small-cell lung cancer (SCLC) that is the most predominant histology among NECs, because of the rarity of GEP-NEC and their biological similarities with SCLC [6,7,8]. However, pivotal studies based on comprehensive molecular analyses have shed some light on the complex molecular scenarios of GEP-NECs as well as SCLC, which have revealed some differences in their molecular profiles [6, 9]. While NECs share some genomic features, despite their different anatomical sites of origin, considerable differences also exist between sites of tumor origin [10,11,12]. Improved knowledge of GEP-NECs may lead to more effective therapeutic strategies, including molecular-targeted agents and immunotherapy.
In this review, we summarize the biology and current treatments of GEP-NEC, as well as the state-of-the-art knowledge of its molecular landscape that has emerged from existing comprehensive analyses. Site-specific genetic alterations are also addressed according to the organ of origin. In addition, the similarities and differences between GEP-NEC and SCLC are highlighted, where appropriate, in terms of clinicopathological and molecular features. Finally, we discuss potential therapeutic targets from both basic and clinical viewpoints.
2 Clinicopathological and molecular features of GEP-NEC
NETs and NECs are distinct entities with widely differing etiologies, clinicopathologies, and genomic profiles.
2.1 Classification of neuroendocrine neoplasms
While GEP-NENs share a neuroendocrine phenotype, they are heterogenous malignancies that can originate from different anatomical sites. Based on grading of the Ki-67 proliferation index of the World Health Organization (WHO) classification in 2010, GEP-NENs can be categorized as low grade (G1), intermediate grade (G2), or high grade (G3), with Ki-67 values of < 3%, 3–20%, and > 20%, respectively [13]. Furthermore, the WHO 2017 and 2019 classifications separated the G3 GEP-NENs into well-differentiated G3 NETs and poorly differentiated G3 NECs based on their morphological differentiation as two distinct entities in terms of prognostic and molecular features [2, 10, 12,13,14]. Consequently, GEP-NENs are now classified as well-differentiated G1–G3 NETs and poorly differentiated G3 NEC based on proliferative grading and differentiation (Table 1 and Fig. 1). GEP-NECs are histopathologically subdivided into small-cell NEC (SCNEC) and large-cell NEC (LCNEC) [15].
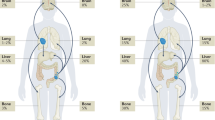
Characteristics and treatment of GEP-NET, GEP-NEC, and SCLC. For patients with GEP-NET, synthetic somatostatin analogs (SSAs) are used due to their favorable biology, including relatively low Ki-67, slow growth, and positive somatostatin receptor (SSTR) expression. Chemotherapy regimens recommended for advanced GEP-NETs and G3 GEP-NETs include streptozotocin-based, temozolomide-based, and platinum-based treatments. Molecular-targeted agents such as everolimus (Eve) and sunitinib (Sun) are also available, with Sun currently approved for pancreatic NETs only. Peptide receptor radionuclide therapy (PRRT) is an option for patients with progressive NETs expressing SSTR after first-line therapy. For patients with GEP-NEC, the standard first-line regimen remains cisplatin plus etoposide or cisplatin plus irinotecan. For patients with SCLC, the standard regimen consists of platinum-based chemotherapy combined with an immune checkpoint inhibitor (ICI) such as atezolizumab or durvalumab. NE, neuroendocrine; TFs, transcription factors
2.2 Clinicopathological features of GEP-NEC
The clinicopathological features of NECs and NETs are shown in Table 2 and Fig. 1. Morphologically, NECs present with solid “sheet-like” growth, partial or complete loss of cyto-architecture, irregular nuclei, less secretory granules, high mitoses, and abundant necrosis [2]. The expression of neuroendocrine markers is extremely limited in NECs [14, 16,17,18]. Although G3 NENs are defined by a Ki-67 proliferation index > 20%, NECs usually have a high Ki-67 index value of ≥ 55% compared to G3 NETs with a Ki-67 index of 21–50% [7, 14, 19, 20].
Approximately 10% of all NECs originate from the extrapulmonary organs, among which one-third develop in the GEP system [6, 8, 17]. The main primary locations of GEP-NECs have been identified as the colorectum, pancreas, and esophagus-stomach [6, 7, 14, 21], and large-cell morphology is the predominant subtype, except for a few tumor sites, such as the esophagus, the gall bladder, and the anal canal, in contrast to pulmonary NECs, which exhibit the highest percentage of small-cell morphologies (95%) [6]. Hormone-induced symptoms are rare [7, 16]. NECs are aggressive phenotypes that are identified as metastatic diseases in 60–85% of cases at the time of diagnosis [6,7,8, 14, 17, 21, 22]. Metastases are often found in the liver, lymph node, or peritoneum, and the incidence of brain metastases is considerably lower in GEP-NEC compared with pulmonary NEC [7, 8, 14, 22,23,24]. Although improved survival for GEP-NECs has been reported [17, 25, 26], the prognosis of patients with metastatic NECs is still unfavorable, with a median OS of 5–8 months [6, 8, 17]. The survival rate for GEP-NEC patients has been found to be worse than that for G3 NETs, even among G3 NENs [1, 12, 19, 27, 28, 40, 41]. Therefore, further development of novel therapies for GEP-NECs is warranted.
2.3 Aberrant molecular profiles of GEP-NEC
Developments in high-throughput genomic technologies have led to a better understanding of the molecular profiles of GEP-NEC compared with SCLC or GEP-NET (Table 3 and Fig. 1). SCLC is the most predominant histology among pulmonary NECs [6], and it is characterized by ubiquitous inactivating mutations in both TP53 and RB transcriptional corepressor 1 (RB1) [42,43,44,45,46]. NEC can develop as a result of lineage plasticity in response to selective pressure from targeted therapies, a process that is also associated with the loss of TP53 and RB1 [3, 47,48,49,50]. Genetically engineered mouse models demonstrated that inactivation of Trp53 and Rb1 induced lineage plasticity by converting from an epithelial phenotype to a NEC phenotype [5, 48, 51]. Genomic aberrations in TP53 and RB1 have also been observed in GEP-NEC at frequencies ranging from 57 to 89% and 9 to 46%, respectively [10,11,12, 29, 52,53,54,55,56,57], thus supporting the idea that the NEC phenotype shares part of the genetic processes of tumor evolution, regardless of the anatomic site of tumor origin [5, 30]. Chromothripsis is a single catastrophic event in the genome that is associated with TP53 mutation in GEP-NEC [10]. Although RB1 mutations emerge at a much lower rate in GEP-NEC compared to SCLC, the RB1 pathway appears to be suppressed by other mechanisms, such as copy number alterations affecting RB1, silencing of p16 via promoter methylation of cyclin-dependent kinase inhibitor 2A (CDKN2A), and amplifications of MYC or cyclin E1 (CCNE1) as an RB1 antagonist [10, 12, 45, 56, 58, 59]. In addition, a loss of RB1 protein expression has been reported in 33–80% of GEP-NEC cases [20, 60,61,62,63]. Thus, the loss of TP53 and RB1 pathways is a prerequisite for both the pathogenesis and lineage plasticity of NEC, but these alterations are likely to be insufficient to drive lineage reprogramming of the NEC phenotype [3, 5, 56, 64, 65]. Additional oncogenic factors are needed to transform normal epithelial cells into SCNEC [5, 56].
In addition to the mutations of TP53 and RB1, other frequently mutated genes in GEP-NECs are KRAS, BRAF, adenomatosis polyposis coli (APC), CCNE1, CDKN2A, Notch receptor 1 (NOTCH1), F-box and WD repeat domain containing-7 (FBXW7), catenin beta 1 (CTNNB1), and phosphatidylinositol-4,5-bisphosphate 3-kinase catalytic subunit alpha (PIK3CA)/phosphatase and tensine homolog (PTEN) [10,11,12, 29, 54, 55, 57] (Table 3). The ataxia telangiectasia-mutated (ATM) gene was subject to frequent copy number losses, whereas the MYC gene was frequently amplified [12]. In a systematic review of 41 studies assessing the molecular features of GEP-NECs, common alterations were observed in the signaling cascades of the mitogen-activated protein kinase (MAPK), p16/cyclin D1/RB1, and Notch pathways [66]. Notably, these molecular features had limited similarities to SCLC. In a clustering analysis of the COSMIC single-base substitution signatures, GEP-NECs exhibited no smoking-related signatures that are representative in SCLC, indicating distinct mutational processes between GEP-NEC and SCLC [10].
SCLC has typically been classified into four molecular subtypes based on the expression status of distinct neuroendocrine-lineage-specific transcription factors, including achaete-scute family bHLH transcription factor 1 (ASCL1), neuronal differentiation 1 (NEUROD1), POU class 2 homeobox 3 (POU2F3), and yes1-associated transcriptional regulator (YAP1) [76]. These subtypes have distinct features of a neuroendocrine phenotype, epithelial-mesenchymal transition, a tumor immune microenvironment, expression profiles, and therapeutic vulnerabilities [76, 77]. In a DNA-binding motif enrichment analysis of the reprogrammed SCNEC, motifs corresponding to ASCL1, NEUROD1, and NKX homeodomain, including NKX2.5 were hyper-accessible transcription factor binding regions [5]. Similarly, in GEP-NECs, ASCL1, NEUROD1, POU3F2, YAP1, and NKX2-5 have been identified as potential master regulators of neuroendocrine lineage reprogramming [56, 58, 78]. However, the expression pattern has been found to differ from that of SCLC [56]. Recently, special attention has been paid to SRY-box transcription factor 2 (SOX2), which acts not only as a transcriptional target of ASCL1 [79], but also as a prominent transcription factor that promotes pluripotency in embryonic stem cells [80] and cancer stem cells [81,82,83]. The SOX2 gene is recurrently amplified in SCLC [43] and has been implicated in the phenotypic switch as lineage plasticity [48]. In GEP-NECs, SOX2 is frequently overexpressed via the hypermethylation of its promoter region [10]. Thus, specific transcription factors can govern neuroendocrine differentiation and transformation in GEP-NECs.
Epigenetic aberrations are among the most oncogenic processes in SCLC [42] and GEP-NECs [11]. Histone-modifying genes, including lysine methyltransferase 2D (KMT2D), lysine methyltransferase 2C (KMT2C), CREB-binding protein (CREBBP), and E1A-binding protein p300 (EP300), have been shown to be frequently altered in SCLC [42], and mutations of these genes are largely mutually exclusive in GEP-NEC [11, 56, 58] (Table 3 and Fig. 1). In addition, alterations of switch/sucrose nonfermentable (SWI/SNF) chromatin remodeling genes, including AT-rich interaction domain 1A (ARID1A), are more common in GEP-NEC and GEP-NET, but rare in SCLC [10,11,12, 42, 52]. Therefore, epigenetic regulation may be a viable therapeutic target in GEP-NECs.
Although GEP-NECs share some genomic alterations characterized by neuroendocrine lineage regardless of different primary organ sites, they also have organ-specific mutational signatures [10]. A pivotal comprehensive molecular analysis has shown the different genomic features and methylation statuses between pancreatic NECs and non-pancreatic NECs in GEP systems [10]. Compared to pancreatic NECs, non-pancreatic NECs have a larger number of structural variations and nonsynonymous mutations [10]. Regarding the Notch signaling pathway, which acts as a tumor suppressor and master regulator of neuroendocrine differentiation in SCLC [42], aberrations of Notch family genes were frequently observed in non-pancreatic NECs, especially esophageal NECs [10, 11, 57]. Importantly, GEP-NECs exhibit key genetic aberrations identical to the non-neuroendocrine carcinomas arising in the same sites, such as BRAF and APC mutations in colorectal NECs [11, 12, 29, 45, 57, 84,85,86,87,88], KRAS mutation in colorectal and pancreatic NECs [9, 11, 12, 20, 29, 45, 55, 57], NOTCH1 mutation in esophageal NECs [11, 12, 57], and E74-like ETS transcription factor 3 (ELF3) mutation in ampullary NECs [10, 89] (Table 4 and Fig. 1), suggesting the hypothesis that GEP-NECs and non-neuroendocrine carcinomas originate from common clonal precursors in the same organ [3, 10, 90].
In pulmonary NEC, LCNECs are genetically more heterogeneous than SCNECs, with frequent inactivation of both TP53 and RB1 [42]. In GEP-NECs, mutations of the RB1 gene were more prevalent in SCNECs than in LCNECs, whereas structural variants in the RB1 gene were more frequent in LCNECs, indicating different mechanisms of RB1 inactivation [10]. However, the genetic profiles were highly concordant between GEP-SCNECs and GEP-LCNECs [9, 12, 57].
Both the alpha-thalassemia/mental retardation syndrome X-linked (ATRX) and death-domain-associated protein (DAXX) play a role in chromatin remodeling at telomeres and other genomic sites [99], and the multiple endocrine neoplasia type 1 (MEN1) interacts with DNA damage repair, chromatin remodeling, telomere alteration, and the phosphatidylinositol-4,5-bisphosphate 3-kinase (PI3K)/mechanistic target of rapamycin kinase (mTOR) pathway [67]. In pancreatic NENs, most NETs harbor genetic mutations of MEN1, ATRX, or DAXX, but mutations of the TP53 and RB1 genes are not observed frequently in NECs [2, 7, 9,10,11, 13, 67, 68, 100]. Among G3 GEP-NENs, G3 NETs share common genetic and epigenetic alterations with a hallmark of G1/G2 NETs, but not of NECs [10, 12, 52, 101]. In fact, G3 NET has frequent mutations in MEN1, ATRX, or DAXX, but extremely rare mutations in TP53, RB1, and KRAS [9, 12, 13, 20, 52, 61, 62, 102]. The frequency of mutations is substantially higher in GEP-NECs than in GEP-NETs [10, 13, 55].
Collectively, GEP-NECs adopt a subset of genomic and epigenomic characteristics of SCLCs, but some key molecular alterations are organ specific, even in the GEP system. In addition, distinct molecular profiles between NECs and NETs support the notion that NECs are not derived directly from NETs [3, 9].
3 Current treatment of patients with GEP-NEC
GEP-NEC patients are often diagnosed at advanced stages and are not eligible for curative treatment. For such patients, systemic treatment is the main therapeutic option for prolonging survival and improving their symptoms and quality of life. The current therapeutic strategies for GEP-NENs differ according to NET and NEC subtypes (Fig. 1). Systemic treatment for NETs includes four types of treatment: (1) synthetic somatostatin analogs (SSAs), (2) peptide receptor radionuclide therapy (PRRT), (3) molecular-targeted agents, and (4) cytotoxic agents. For NECs, cytotoxic chemotherapy is the only established treatment [31, 103].
Therapeutic strategies for patients with GEP-NECs originated from those designed for SCLCs because of their close tumoral entity and the rarity of GEP-NEC [8, 31, 103]. Platinum-based chemotherapy is recommended as a first-line treatment extrapolation from SCLC [8, 24, 31, 103]. The impact of cytotoxic chemotherapy on GEP-NECs has mostly been evaluated by retrospective studies (Table 5). The treatment efficacy of platinum-based chemotherapy is generally modest, with a reported overall response rate (ORR) of 14–75% and a median progression-free survival (PFS) of 1.8–8.9 months. The median OS is approximately 12 months [14, 22, 104,105,106]. In a national cancer database study comprising 1861 patients with GEP-NECs, patients treated with palliative chemotherapy had significantly improved survival outcomes, compared to those who did not receive this treatment, with median OS of 11.2 months and 1.7 months, respectively (hazard ratio [HR], 0.43; 95% confidence interval [CI], 0.39–0.48) [22]. Similar results were observed in the NORDIC NEC study [14]. Of note, the Ki-67 proliferation index was a predictive marker for platinum-based chemotherapy (median ORR, 15% for patients with Ki-67 < 55% and 42% for those with Ki-67 ≥ 55%). This finding also supports the idea that platinum-based chemotherapy has limited efficacy for G3 NETs, whose Ki-67 index values are usually less than 55% [7, 19, 20]. Although the prognostic difference between organ sites remains controversial [14, 104], there was no difference found between cisplatin (CDDP) and carboplatin among platinum compounds in terms of treatment efficacy [14]. The two most commonly used chemotherapy regimens are etoposide (ETP) plus CDDP (EP) and irinotecan (CPT-11) plus CDDP (IP) [8, 31, 103]. In a phase III TOPIC-NEC trial of EP versus IP for GEP-NEC in a first-line setting, superiority was not demonstrated because of the median OS with an HR of 1.04 (95% CI: 0.79–1.37) [104]. Thus, both EP and IP remain standard first-line regimens.
Unfortunately, there is no standard chemotherapy for a second-line setting. In a systematic review and meta-analysis of second-line treatment in 582 patients with advanced extrapulmonary NEC, the ORR and median PFS were 18% and 2.5 months, respectively [139]. Similarly, the NORDIC NEC study showed an ORR of 18% in second-line chemotherapy for 84 patients with GEP-NEC [14]. Several chemotherapeutic agents have been proposed based on the results of small studies conducted on the second or later line (Table 5). Special attention should be paid to these results because of heterogeneous populations, including cases of well-differentiated G3 NET and poorly differentiated G3 NEC, which show that 5-fluorouracil (5-FU), oxaliplatin, and CPT-11 are likely to have antitumor activity in cases of GEP-NEC. Therefore, FOLFIRINOX, consisting of these three agents, may be a promising regimen, as demonstrated in cases of pancreatic cancer [140]. A randomized phase II trial to compare the efficacy and safety of first-line FOLFIRINOX treatment versus EP in GEP or unknown primary NECs is ongoing (NCT04325425). It should also be noted that temozolomide is active in pancreatic NETs [8, 31, 103], and a combination of capecitabine and temozolomide (CAPTEM) demonstrated a high ORR and long PFS compared to temozolomide alone [141]. In a multicenter retrospective review of 130 patients with G3 GEP-NENs, including NEC (35% of the study population), the ORR of the CAPTEM regimen was 26% [142]. Currently, randomized phase II trials of CAPTEM versus platinum plus ETP in the first-line setting (NCT02595424) and CAPTEM or FOLFIRI as a second-line therapy (NCT03387592) in GEP-NECs are ongoing.
4 Potent molecular-targeted therapy for patients with GEP-NEC
Although many molecular-targeted agents are currently approved for various solid tumors, no targeted therapies have been established for the clinical management of NECs. Therefore, novel therapies tailored to their molecular composition are urgently required to improve prognosis. A growing number of comprehensive molecular analyses have provided potential targets for GEP-NEC [10,11,12, 29, 54, 55, 57], which may lead to therapeutic breakthroughs with a personalized approach. As the molecular landscapes and transcriptional signatures of GEP-NECs are partially similar to those of SCLCs because of the neuroendocrine lineage, treatment strategies for GEP-NEC may be inferred from clinical trials conducted in cases of SCLC, such as immune checkpoint inhibitors (ICIs). As another approach, some molecular aberrations are organ-specific and similar to the corresponding conventional cancer; targeted treatments for conventional cancer may also be indicated for patients with NECs from the same site of origin. Recently, drug sensitivity and gene dependency screens have revealed a common therapeutic vulnerability between SCNECs and hematologic malignant tumors, thus supporting the extrapolation of targeted therapies that have been established for hematologic malignant tumors [4]. In this section, we summarize the results of previous trials (Table 6) and discuss potential therapeutic targets (Fig. 2), as well as other ongoing trials (Table 7).
Summary of potent therapeutic strategies for GEP-NEC. The potent approaches are composed of both neuroendocrine-specific and site-specific treatment. ADC, antibody–drug conjugate; BiTE, bispecific T-cell engager; CAR-T, chimeric antigen receptor-T cell therapy; PRRT, peptide receptor radionuclide therapy; HDAC, histone deacetylase; ICI, immune checkpoint inhibitor; DDR, DNA damage response. The “anti- “ means blockade of indicated molecule. The “α” includes other ICIs, chemotherapy, HDAC inhibitor, anti-angiogenic therapy, and DDR inhibitors targeting AURK, WEE1, ATR, ATM, AXL, CHK1, or PARP. The “β” includes other DDR inhibitors, and chemotherapy
4.1 RAS/BRAF-targeted therapy
Aberrant activation of receptor tyrosine kinase (RTK) pathways is common in non-neuroendocrine epithelial cancers, and KRAS mutational activation leads to downstream signaling of the MAPK and PI3K/v-akt murine thymoma viral oncogene homolog (Akt) pathways, which play crucial roles in tumorigenesis, proliferation, survival, angiogenesis, and metastasis. In GEP-NECs, KRAS mutations are reported at a similar frequency as in conventional cancers arising at the same sites: KRAS genes are frequently mutated in colorectal and pancreatic NECs, while they are less common in esophageal NECs [11, 12] (Table 4). Novel KRAS G12C allele-specific covalent inhibitors demonstrated a profound clinical impact in KRAS G12C-mutated non-small-cell lung cancer (NSCLC) [143, 144]. The accurate frequency remains unclear in GEP-NEC, but KRAS G12C mutations have been observed in NENs [145, 146]. Although KRAS G12C mutation may represent a potential target even for GEP-NEC, the efficacy is likely to be contingent upon RTK dependency and signaling rebound kinetics [147, 148]. As there is currently insufficient scientific evidence to establish the therapeutic strategy for KRAS G12C-mutated GEP-NEC, further preclinical and clinical studies are needed for GEP-NEC. In addition, the success of targeting KRAS G12C will provide hope that a range of mutant RAS allele-specific targeted therapies could become therapeutically tractable [149].
An activating missense mutation in codon 600 of exon 15 (V600E) of the BRAF gene has been identified in various tumor types, and BRAF inhibitors have yielded clinical benefits for patients with BRAF V600E-mutated cancers, especially melanoma and NSCLC [150,151,152]. However, in colorectal adenocarcinoma (CRC), the BRAF inhibitor vemurafenib alone only led to a 5% ORR, indicating insufficient single-agent activity [153]. Based on preclinical findings showing that reactivation of MAPK signaling through feedback activation of epidermal growth factor receptor (EGFR) was an escape mechanism responsible for intrinsic resistance to a BRAF inhibitor alone [154], a combination therapy of the BRAF inhibitor encorafenib and the EGFR inhibitor cetuximab resulted in significantly improved survival in CRC patients with BRAF V600E mutation [155]. In melanoma, a combination of the BRAF inhibitor dabrafenib and mitogen-activated protein kinase kinase (MEK) inhibitor trametinib showed superior efficacy over dabrafenib alone [156]. Thus, susceptibility to BRAF inhibitors alone and the success of a combinatorial approach are tumor-lineage-dependent.
BRAF V600E mutations are rare events in SCLCs, but the alterations are tumor site-dependent in GEP-NECs and especially enriched in colorectal NECs (Tables 3 and 4). BRAF mutations are more frequent genetic events in colorectal NEC than CRC, with frequency ranging from 15 to 59% of colorectal NECs [11, 12, 29, 45, 57, 84,85,86,87,88]. Similar to CRC, the predominant location of BRAF mutations is the right side of the colon [12]. EGFR expression is repressed by gene methylation in melanomas, which confers sensitivity to BRAF inhibitors alone [157]. Colorectal NECs have similar EGFR methylation signatures to melanoma, unlike CRC, and BRAF inhibitor monotherapy showed much higher tumor regression in colorectal NECs than CRC in patient-derived xenograft models [88]. In addition, treatment with a dual blockade of BRAF and MEK suppressed cell proliferation and tumor growth by inducing apoptosis and cell cycle arrest at the G1 phase in BRAF V600E-mutated colorectal NEC cell lines and xenograft models [87]. In a phase II basket trial of the BRAF inhibitor vemurafenib in non-melanoma BRAF V600 mutation-positive solid tumors, two NEC patients had PFS of 7.8 months and 5.7 months, respectively [151]. Recently, several case series have reported the benefits of BRAF inhibition in monotherapy or with the addition of an MEK inhibitor in colorectal NECs [84, 88, 158]. Thus, BRAF inhibitors are emerging as the most promising therapeutic strategies for BRAF V600E-mutated GEP-NECs (Fig. 2).
4.2 mTOR-targeted therapy
mTOR signaling is aberrantly activated via overexpression of phosphorylated mTOR and dysregulations of the PI3K/Akt pathway, which are implicated in the modulation of cell proliferation, metabolism, and angiogenesis in GEP-NETs [68]. The mTOR inhibitor everolimus showed a significantly prolonged PFS compared to a placebo in GEP-NETs [159], and it has consequently been recommended as a second- or third-line treatment [8, 31, 103]. The PI3K/mTOR pathway is also activated as a recurrent event in GEP-NECs [12, 59, 86]. However, everolimus failed to show efficacy for pancreatic NEC, with an ORR of 0% and median PFS of 1.2 months, in a phase II NECTOR trial [160]. There are ongoing phase II trials of everolimus monotherapy (NCT02113800 and NCT02687958) and a combination of everolimus with temozolomide (NCT02248012) in NEC (Table 7).
4.3 MYC-targeted therapy
MYC is a transcription factor that acts as a master regulator of genes involved in cell cycle progression, cell proliferation, apoptosis, and neuroendocrine lineage plasticity [161, 162]. MYC genetic alterations have been frequently reported in GEP-NECs across primary sites [11, 12] (Tables 3 and 4). A pivotal preclinical study demonstrated that MYC overexpression drove trans-neuroendocrine differentiation by binding to neuroendocrine-related genes in genetically engineered pancreatic adenocarcinoma mouse models [161], suggesting a rational target for GEP-NECs (Fig. 2). The direct approach of targeting MYC remains a major clinical challenge due to the unclear structure, absence of intrinsic enzymatic activity, lack of targetable binding pockets, and compensatory activation of the other MYC family members [163]. Therefore, indirect inhibition of MYC is considered an alternative pharmacological approach, such as by targeting its transcription. Cyclin-dependent kinase 7 (CDK7) regulates transcription by affecting the stability of preinitiation complexes, leading to altered gene expression, cell cycle progression, and cell survival [164]. The inhibition of CDK7 has been found to reduce MYC expression by interfering with RNA polymerase II and subsequently inhibiting the super enhancers of MYC [164, 165]. Knockdown or inhibitor treatment of CDK7 showed efficacy in in vitro and in vivo SCLC models [4].
Of note, tumors with MYC aberrations have unique biological vulnerabilities, which represents the potential of precision medicine in these cases [76, 77]. Potent synthetic lethal partners that have preclinically shown promising efficacy in MYC-driven tumors include checkpoint kinase 1 (CHK1), aurora kinase (AURK), WEE1 G2 checkpoint kinase (WEE1), and arginine deprivation. Inactivation of the TP53 and RB1 pathways causes disruption of G1/S cell cycle checkpoint function [42, 43], and MYC activation induces replicative stress, resulting in dependence on G2/M cell cycle checkpoint regulators upon cellular DNA damage [166]. CHK1 is a critical player in regulating the G2/M checkpoint that facilitates cell cycle arrest and DNA damage repair in cells with TP53 aberration [167]. MYC activation is capable of inducing CHK1 overexpression, leading to “CHK1 addiction” in MYC-driven cancers, especially with concurrent inactivation of TP53 [168, 169]. Since GEP-NECs have nearly ubiquitous inactivation of TP53, the CHK1 inhibitor may be more effective in GEP-NECs with MYC amplification or overexpression, as shown in cases of SCLC [169]. AURK stabilizes MYC via the regulation of proteasomal degradation mediated by ubiquitin ligases FBXW7 [170, 171]. Stabilized MYC also promotes the transcription of AURK, constituting a positive feedforward loop between MYC and AURK [170]. In a phase II trial of paclitaxel with or without the AURK inhibitor alisertib in SCLC, MYC expression was a predictive biomarker for sensitivity [172]. Thus, MYC-driven cancer cells may be susceptible to AURK inhibitors [173, 174].
Another key component of the G2/M checkpoint is WEE1, which blocks entry into mitosis for proper DNA repair by inhibiting the cyclin-dependent kinase (CDK1 and CDK2) in response to cellular DNA damage [175]. Preclinically, WEE1 inhibition has demonstrated an antitumor effect via cell cycle arrest and apoptosis in SCLC and other neuroendocrine-associated malignancies [176,177,178], thereby emerging as a therapeutic target for NECs. However, in a biomarker-driven phase II umbrella trial for patients with SCLC after platinum-based chemotherapy, a selective small-molecule WEE1 inhibitor AZD1775 monotherapy showed no objective response in SCLC with MYC amplification or co-alterations of CDKN2A and TP53 [179]. Thus, the limited clinical efficacy of WEE1 inhibitor monotherapy suggests an urgent need for novel combination strategies, such as chemotherapy plus AZD1775 for TP53-mutant ovarian cancer [180], chemotherapy followed by AZD1775 maintenance for TP53/KRAS-mutant CRC [181], AZD1775 plus an inhibitor of histone deacetylase (HDAC) or bromodomain-containing protein 4 (BRD4) for acute leukemia [182], or dual blockade of WEE1/AXL receptor tyrosine kinase (AXL) or WEE1/mTOR for SCLC [177].
Metabolic rewiring evokes cellular mechanisms that reduce therapeutic mightiness. Aberration of MYC also leads to reprogramming of cellular metabolism, which creates reliance on arginine biosynthetic pathways, including polyamine biosynthesis and mTOR pathway activation [183, 184]. Arginine depletion with PEGylated arginine deiminase has been found to dramatically suppress the tumor growth of MYC-driven SCLCs in genetically engineered mouse models and a patient-derived xenograft from a relapsed SCLC patient [184]. Depleting arginine may act as a therapeutic strategy for MYC-aberrant GEP-NECs.
While MYC-targeted therapies have emerged as a promising approach for GEP-NEC treatment, they have been hampered due to the lack of available clinical data, highlighting the need for further clinical trials for GEP-NEC.
4.4 DNA damage response-targeted therapy
Recently, targeting components of DNA repair pathways has emerged as a therapeutic strategy [185, 186]. DNA damage response (DDR) pathways play a critical role in cell survival through the activation of DNA repair signaling and their interaction with cell cycle checkpoints [185]. In cancer, DDR pathways are frequently disrupted by alterations in DDR-related genes, causing genomic instability as one of the hallmarks of cancer [186]. The poly (ADP-ribose) polymerase (PARP) enzyme acts as a highly sensitive sensor for DNA damage, which recruits DNA repair proteins to damage sites to facilitate efficient repair [185]. PARP is activated in response to DNA double-strand breaks (DSBs), but DSBs are normally repaired by homologous recombination repair (HRR). Cancer cells with HRR deficiency rely on an alternative repair system mediated by PARP, leading to susceptibility to PARP inhibitors via enhanced synthetic lethality due to a blockade of the repair system [187]. The clinical success of PARP inhibitors in BRCA-mutated breast, ovarian, prostate, and pancreatic cancers has provided proof-of-concept for synthetic lethality as a novel therapeutic strategy. DDR pathways are also sometimes deficient in SCLC and extrapulmonary NEC [188, 189]. In addition, the targeted sequencing in 152 GEP-NEC samples showed that the majority of potentially targetable alterations were related to defects in DNA repair [12]. In a randomized phase II trial of the PARP inhibitor veliparib in combination with EP chemotherapy in extensive-stage SCLC, the PFS as a primary endpoint was met, with an improvement in median PFS of 6.1 months for veliparib versus 5.5 months for the placebo [190]. A phase I/II trial of the PARP inhibitor rucaparib plus a PEGylated conjugate of SN-38 (PLX038) acting as a DNA-damaging chemotherapy is ongoing in solid tumors and small-cell cancers, including GEP-NEC (NCT04209595) (Table 7). The combined blockade of DDR proteins, such as PARP and WEE1, may also enhance therapeutic efficacy because of their crosstalk [186, 191].
In addition to PARP, DDR kinases, such as ataxia telangiectasia and RAD3-related (ATR), ATM, CHK1, and WEE1, have emerged as attractive targeted molecules because of their central roles in DNA repair [192, 193]. ATR is activated by DNA damage or DNA replication stress, which not only stabilizes replication forks but also activates the G2/M checkpoint. A subset of cancer cells under replication stress may be susceptible to ATR inhibitors, as well as other DDR inhibitors, such as CHK1 [168, 169] or WEE1 [177, 180] under MYC- or CCNE1-induced replication stress. Based on the preclinical results indicating that the dual inhibition of ATR and topoisomerase I was synergistically cytotoxic in SCLC, a proof-of-concept phase II trial of the ATR inhibitor berzosertib plus topotecan was conducted in the second or latter line of SCLC, which showed an ORR of 36% and a median PFS of 4.8 months [194]. Given that extrapulmonary SCNECs share a common molecular profile with SCLC [4, 5, 30], the trial was amended to assess the efficacy of berzosertib plus topotecan in extrapulmonary SCNECs. In this case, the ORR was 20% in 10 patients with extrapulmonary SCNECs from distinct primary sites, including the GEP system, and responses were observed even in tumors refractory to prior treatment with the topoisomerase I inhibitor [194]. In an exploratory analysis using pre-treatment samples from both SCLC and extrapulmonary SCNEC, most responders exhibited high neuroendocrine differentiation, such as ASCL1 or NEUROD1 subtypes, and somatic copy number alterations in genes driving replication stress, including CCNE1 gain and ARID1A loss [194]. Collectively, exacerbating DNA replication stress may induce the therapeutic vulnerability of GEP-NECs to DDR inhibitors (Fig. 2). Currently, several early-phase trials of agents targeting ATR in combination with a topoisomerase I inhibitor (NCT04514497, NCT02487095, and NCT03896503) are ongoing in cancers, including GEP-NECs (Table 7).
4.5 Angiogenesis-targeted therapy
Most pancreatic NETs have an extraordinary tumor vascularization due to overexpression of pro-angiogenic factors, including vascular endothelial growth factor receptor (VEGFR) and platelet-derived growth factor receptor (PDGFR) [195]. In fact, the multi-targeted tyrosine kinase inhibitor (TKI), mainly targeting VEGFRs and PDGFRs, sunitinib [196], and the mTOR inhibitor everolimus [159] have proven to be of clinical benefit in pancreatic NETs, and the promising antitumor activity of anti-angiogenic TKIs, such as pazopanib [197], cabozantinib [198], lenvatinib [199], and surufatinib [200, 201], has also been demonstrated in NETs.
Although there are no approved anti-angiogenetic agents for NECs, a preclinical study has demonstrated potent antitumor activity for two anti-VEGF antibodies, bevacizumab and aflibercept, in xenograft models of SCLC and colon NEC cell lines [202]. Clinically, a retrospective study reported the potent efficacy of the anti-VEGFR2 antibody ramucirumab in combination with chemotherapy compared to chemotherapy alone, possibly due to high expression levels of VEGFR2 in metastatic gastric NEC [203]. In a randomized phase II PRODIGE41-BEVANEC trial of bevacizumab in combination with second-line 5-FU, leucovorin, and CPT-11 (FOLFIRI) after the failure of a platinum plus ETP regimen in patients with GEP-NECs, the primary endpoint was met, with ≥ 50% of patients alive at 6 months following treatment with FOLFIRI plus bevacizumab. However, there seemed to be no additional efficacy of bevacizumab when added to FOLFIRI, given the median OS of 8.9 months and 7.0 months in FOLFIRI alone versus FOLFIRI plus bevacizumab, respectively [204]. In a phase II trial of first-line capecitabine, oxaliplatin, and CPT-11 (CAPOXIRI) plus bevacizumab, followed by maintenance treatment with pazopanib plus capecitabine, for colon or small intestinal NECs, great efficacy was shown, with an ORR of 47.4%, median PFS of 13 months, and median OS of 29 months [205]. In addition, phase II trials in cases of GEP-NEN showed clinical activity of sunitinib, with a disease control rate (DCR) of 55% in 20 patients with GEP-NEC [206], and pazopanib with an ORR of 23% and median PFS of 5.8 months in 13 patients with GEP-NEC [207]. There are ongoing trials of agents targeting angiogenic molecules in cancers, including GEP-NECs: a phase II trial of bevacizumab plus nab-paclitaxel in NEC (NCT04705519), a phase II trial of multi-targeted TKI (mainly targeting VEGFRs and PDGFRs), anlotinib in G3 GEP-NET including NEC (NCT03457844), and a phase II trial of cabozantinib targeting VEGFR2/MET proto-oncogene/AXL in G3 NENs including NEC (NCT04412629) (Table 7 and Fig. 2).
4.6 DLL3-targeted therapy
Delta-like canonical Notch ligand 3 (DLL3) is an inhibitory ligand of the Notch receptor pathway and is highly expressed in most pulmonary NECs [208, 209], which drives neuroendocrine differentiation [42]. DLL3 is a downstream target of ASCL1 [210], which acts as a prominent transcription factor in GEP-NECs [56, 58, 78]. In fact, DLL3 and ASCL1 have been molecularly and clinically characterized as the same subgroup among extrapulmonary NECs [78]. DLL3 was frequently expressed in 76.9% of GEP-NECs, but not in G1-G3 NETs [211]. In addition, DLL3 was found to be differentially upregulated in esophageal NEC compared to matched normal esophagi, accounting for approximately 85% of esophageal NECs [58]. Considering the high prevalence of NEC-specific cell surface molecules, DLL3 could be a compelling therapeutic opportunity for an antigen targeted by antibody–drug conjugates (ADCs), bispecific T-cell engager (BiTE), and chimeric antigen receptor (CAR) T cells in GEP-NECs (Fig. 2).
DLL3 is an attracted molecule that delivers cytotoxic compounds selectively and directly to NEC cells. Rovalpituzumab tesirine is an ADC comprising the cytotoxic payload pyrrolobenzodiazepine, which is conjugated by a linker to a monoclonal DLL3 antibody. Despite promising preclinical and early-phase clinical antitumor activity [208, 210], phase III trials of DLL3-positive SCLC have failed to demonstrate significantly improved OS of rovalpituzumab tesirine as a maintenance therapy versus a placebo after platinum-based therapy [212] and as a second-line treatment versus topotecan [213]. In a phase I/II trial of DLL3-expressing solid tumors, including GEP-NECs, patients with NEC/NET had an ORR of 13%, with a median PFS of 4.1 months [214]. These results led to the discontinuation of the further development of rovalpituzumab tesirine. The development of another DLL3-targeting ADC with cytotoxic pyrrolobenzodiazepine, SC-002, was also discontinued because of systemic toxicity [215]. However, the toxicity profiles of both rovalpituzumab tesirine and SC-002 were attributed to the cytotoxic pyrrolobenzodiazepine, suggesting that DLL3 still remains a research interest as a target of ADC.
Tarlatamab (AMG 757) is a half-life extended BiTE designed to specifically bind DLL3 on cancer cells and CD3 on T cells, resulting in T-cell-dependent killing of cancer cells with DLL3 expression in the SCLC patient-derived xenograft models [216]. A phase I trial of tarlatamab showed a confirmed ORR of 13%, with the estimated duration of response ≥ 6 months in 71% of cases of SCLC [217]. BI 764532 is a novel IgG-like DLL3/CD3 BiTE, resulting in T-cell-mediated complete tumor regression in a human T-cell engrafted xenograft model [218]. A first-in-human phase I trial of BI 764532 is ongoing in patients with SCLC and other NECs expressing DLL3 (NCT04429087). HPN328 is a tri-specific T-cell-engager designed as three binding domains with anti-albumin for half-life extension in addition to DLL3/CD3. Interim results of an ongoing phase I/II trial (NCT04471727) of HPN328 showed any tumor shrinkage in 40% of 15 patients with SCLC and other NECs expressing DLL3 [219]. Treatment with DLL3-targeted CAR-T cells also resulted in preclinical antitumor activity in SCLC xenograft models [220], and the DLL3-targeting CAR-T cells AMG 119 are in clinical development [221]. Thus, DLL3-targeted products may lead to a tremendous breakthrough in treating GEP-NECs (Table 7).
4.7 Epigenetic-targeted therapy
Epigenetic alternations, including DNA methylation, histone acetylation, and histone methylation, regulate gene expression and interact with numerous transcription factors that have fundamental functions in cancer progression [222]. The enhancer of the zeste 2 polycomb repressive complex 2 subunit (EZH2) is an enzymatic catalytic subunit of the polycomb repressive complex that can epigenetically alter gene expression via histone methyltransferase [223]. EZH2 overexpression and specific methylation patterns frequently occur in SCLC and other NECs, including the GEP system, which contribute to cellular lineage plasticity [10, 48, 49, 189]. DNA-damaging chemotherapy was found to induce genome-wide EZH2 activity, which in turn drove chemoresistance through epigenetically silencing the cell cycle regulator Schlafen family member 11 (SLFN11) [224]. The addition of EZH2 inhibitors to cytotoxic chemotherapy prevented the emergence of acquired resistance and augmented chemotherapeutic efficacy in both chemosensitive and chemoresistant SCLC patient-derived models. Although a phase I trial of selective EZH2 inhibitor PF-06821497 monotherapy failed to show a treatment response in two SCLC patients [225], these preclinical findings provide a rationale for further development of epigenetic targeting strategies.
Bromodomain and extra-terminal (BET) proteins bind acetylated histones and recruit protein complexes to promote transcription, among which BRD4 serves as a transcriptional regulator of MYC [226, 227]. BET inhibitors preclinically impaired tumor growth in MYC-dependent cancers, including SCLC [227, 228]. In addition, ASCL1 was downregulated by binding the BET inhibitor to the ASCL1 enhancer [229]. Of note, hematologic malignant tumors have been found to have more similarities to SCNECs in terms of expression profiles and drug sensitivity-based phenotypes, and SCNECs are more sensitive to HDAC inhibitors approved in hematologic malignancies [4]. To evaluate the additive and potentially synergistic effects of combining an HDAC inhibitor with chemotherapy, a phase I study of the HDAC inhibitor belinostat in combination with EP chemotherapy was conducted in advanced solid cancer [230]. In 15 patients with NECs, including 4 GEP-NECs, the ORR and DCR were 47% and 93%, respectively. A phase II trial of a novel subtype-selective HDAC inhibitor, tucidinostat, in combination with chemotherapy is ongoing in NECs (NCT05076786) (Table 7 and Fig. 2).
4.8 Somatostatin-targeted therapy
Somatostatin receptors (SSTRs) are a family of G protein-coupled receptors that are implicated in the regulation of hormone secretion and tumor proliferation in NET [231]. Since SSTRs are frequently expressed in NET, SSAs, such as octreotide and lanreotide autogel, have been established as a first-line therapy for ameliorating secretory symptoms and tumor growth in patients with SSTR expressing NET [232,233,234]. PRRT is a radiolabeled SSA, conjugated with a chelator and β/γ-emitting 177Lutetium (177Lu) or β-emitting 90Yttrium (90Y), in order to kill neoplastic cells with lethal radiation [235]. A phase III NETTER-1 trial showed significantly improved PFS and ORR in PRRT with [232]Lu labeled-tetraazacyclododecanetetraacetic acid (DOTA) modified Tyr [3] octreotate (TATE) compared to high-dose octreotide long-acting release (LAR) for patients with midgut NETs [236]. Based on this trial, PRRT is a second-line therapeutic option for GEP-NETs.
Although NECs have generally absent or reduced SSTR expression [1, 7, 16, 30, 31], a subset of NECs presents SSTR expression, especially for LCNECs and NECs, with a Ki-67 value of 21–55% [41, 91, 237]. In a multicenter retrospective cohort of 149 patients with G3 GEP-NENs treated with PRRT, the median PFS was 19 months in G3 NET, 11 months for NEC with Ki-67 ≤ 55%, and 4 months for NEC with Ki-67 > 55% [237, 238]. Of note, the ORR was similar between the NECs with Ki-67 ≤ 55% and > 55% (43% vs. 46%), and the median OS was 9 months, even in NECs with Ki-67 > 55%. PRRT may thus be considered a promising therapeutic option for selected NEC patients [7, 238]. Currently, several phase II trials have investigated the treatment efficacy of SSAs or PRRT in GEP-NECs, including octreotide LAR (NCT02409849), PRRT with [145]Y-DOTA modified somatostatin analog Tyr [3]-octreotide (TOC) and [232]Lu-DOTA-TOC (NCT00978211), and a combination of PRRT with [232]Lu-DOTA-TATE and the anti-PD-1 antibody nivolumab (NCT04525638) (Table 7 and Fig. 2).
SSTR2 is one of the most frequently expressed subtypes of SSTRs in GEP-NENs. PEN-221 is a small peptide drug conjugate that selectively targets SSTR2, with a cleavable linker to a cytotoxic payload DM1. Treatment with PEN-221 was found to enable efficient drug delivery to SSTR2-positive cells, resulting in complete and durable regressions in SSTR2-positive SCLC xenograft mouse models [239]. A phase I/IIa trial assessed the preliminary antitumor activity and safety of PEN-221 in patients with SSTR2-expressing NENs, including GEP-NEC (NCT02936323) (Table 7 and Fig. 2).
4.9 Other potent molecular-targeted therapies
Other potential cellular targets in GEP-NECs have been identified, such as exportin-1 (XPO1), the BCL2 apoptosis regulator (BCL2), and lurbinectedin (Fig. 2).
XPO1 is a key nuclear export protein that regulates the nucleocytoplasmic trafficking of a growing number of tumor suppressor proteins, growth regulatory proteins, and chemotherapeutic agents [240, 241]. XPO1 aberration leads to the functional inactivation of tumor suppressor proteins through exportation from the nucleus to the cytoplasm via the nuclear pore complex, which is implicated in tumorigenesis in various tumor types [241]. In a screening of potential therapeutic vulnerabilities using clustered regularly-interspaced short palindromic repeats (CRISPR)/CRISPR-associated protein (Cas)9 technology in SCLC cell lines, XPO1 was identified as a promising target for CDDP sensitization [242]. Selinexor is a selective inhibitor of nuclear export compounds that forms a reversible covalent bond with the cysteine residue of the XPO1 cargo-binding pocket, leading to nuclear retention and functional activation of tumor suppressor proteins and hindering DDR mechanisms [243]. Selinexor has been granted U.S. Food and Drug Administration (FDA) approval for the treatment of multiple myeloma and diffuse large B-cell lymphoma, and synergistic effects between selinexor and DNA-damaging agents have been preclinically demonstrated in cases of SCLC [242]. A phase II trial also investigated the efficacy of selinexor in SCLC and GEP-NEC (NCT02250885) (Table 7).
BCL2 plays an important role in blocking apoptotic cell death [244]. Accordingly, BCL2 was identified as a druggable target with conserved expression across the site of origin in NECs [176]. BCL2 inhibitors have demonstrated remarkable clinical benefit in hematologic malignant tumors and have been included in the shared predicted drug sensitivity profiles between hematologic malignancies and SCNECs [4]. SCLC cells with the ASCL1 molecular subtype predominantly exhibited BCL2 overexpression, and they were sensitive to BCL2 inhibitors [173, 245]. BCL2 inhibitors may also promote synergistic antitumor activity in combination with WEE1 inhibitors or BET inhibitors in cases of NECs [176, 246]. In GEP-NECs, BCL2 overexpression has also been observed at a high prevalence, partially due to the predominance of ASCL1 [9, 63], thus indicating a potential therapeutic target.
Lurbinectedin is a selective inhibitor of oncogenic transcription through preferential binding to CpG-rich sequences around promoters of protein-coding genes, degradation of elongating RNA polymerase II, generation of DNA damage, and subsequent apoptosis [247]. Lurbinectedin abrogates the expression of ASCL1 and NEUROD1 transcription factors and their target genes, such as BCL2, INSM1, MYC, and AURK in SCLC [248], which has been approved as a second-line therapy of SCLC by the FDA, with an ORR of 35% in patients with relapsed SCLC [249]. In a cohort of NEN patients from a phase II basket trial of lurbinectedin, two of the 31 evaluable participants had confirmed PR, and one patient with PR was diagnosed with NEC [250]. The efficacy of lurbinectedin monotherapy was assessed in a phase II trial that included a cohort of patients with NEC (NCT05126433). In a drug screening of lurbinectedin in combination with 43 other agents in SCLC, the top synergistic agent was the ATR inhibitor berzosertib, with a 3.5-fold increase in DNA damage compared to lurbinectedin alone [251]. Currently, a phase I/II trial of lurbinectedin plus the ATR inhibitor berzosertib is ongoing in NECs (NCT04802174) (Table 7).
Liquid biopsy has attracted considerable attention as a less-invasive approach that can identify high-level and clonal alterations among tumors with intratumoral heterogeneity [252]. The feasibility of next-generation sequencing using circulating tumor DNA (ctDNA) has also been demonstrated in GEP-NECs [253,254,255], suggesting the potential to provide precision medicine for patients with more homogenous alterations in the near future.
4.10 Immunotherapy
Inhibitory immune checkpoint molecules, such as programmed death-1 (PD-1) and its ligand PD-L1, promote antitumor immune escape during the cancer–immunity cycle process [256, 257]. Clinically, ICIs targeting PD-1/PD-L1 have exhibited a durable response by disrupting immune tolerance and activating cytotoxic T cells in various tumor types. While ICIs already constitute a standard treatment modality for patients with SCLC [258], ICI monotherapy has limited antitumor efficacy [77, 259,260,261,262]. The clinical benefit of ICIs has been evaluated for patients previously treated for extrapulmonary NECs in several early trials (Table 6). Consistent with SCLC, ICI monotherapy was unfortunately less effective in the unselected populations of GEP-NECs, with an ORR of 0–18.7% [262,263,264,265,266,267,268]. PD-L1 expression was associated with high-grade classification in NENs [266, 269, 270], but the association between PD-L1 expression and the treatment efficacy of ICI remains controversial [263, 266, 268, 271]. PD-L1 expression is commonly weak and restricted to tumor-infiltrating lymphocytes (TILs) rather than tumor cells in GEP-NECs [69, 269]. TILs have also been found to be abundant in GEP-NEC compared to GEP-NET [270, 272], but usually at a low density and located at the tumor edges or at the surrounding stroma without infiltrating the tumor parenchyma [58, 273]. In addition, adaptive immunity in a subset of NEC cases was counteracted by immune escape mechanisms, such as loss of major histocompatibility complex (MHC) class I, and by negative regulation of adaptive immunity via cyclooxygenase-2 and β-catenin signaling [270]. In a systemic review and meta-analysis of ICIs in 464 patients with NENs, the ORR was higher in NECs versus NETs and in the ICI combination versus monotherapy, although GEP-NENs had lower ORRs than pulmonary NENs [274]. Collectively, these findings likely indicate the limited potential of ICI monotherapy in GEP-NECs. Therefore, there is an urgent need for improved biomarkers for patient selection and the identification of synergistic therapeutic combinations.
Based on the clinical benefit of anti-PD-1 Ab pembrolizumab for patients with microsatellite instability-high (MSI-H)/deficient mismatch repair (dMMR) tumors in pivotal clinical trials [275], the FDA granted first tumor-agnostic approval for pembrolizumab for MSI-H/dMMR tumors. The frequency of MSI-H has been reported as ranging between 0 and 13% of GEP-NECs [12, 27, 52, 54, 66, 69, 70]. Like the corresponding conventional adenocarcinoma at the site of origin [71,72,73], MSI-H has been found to predominantly have small intestinal, gastric, and colorectal origins among GEP-NECs, mostly subsequent to MHL1 promoter methylation [11, 54, 66, 70]. The tumor mutational burden (TMB), defined as the total number of mutations per coding area of a tumor genome, is an emerging biomarker response to pembrolizumab [276], which led the FDA to approve it for patients with TMB-high tumors (≥ 10 mutations/megabase). TMB-high status is also more pronounced in high-grade GEP-NENs [52], but an analysis of a diverse cohort of 100,000 cancer cases showed a TMB-high designation in only 1.7–8.5% of extrapulmonary NECs, depending on primary tumor sites [277]. In addition, the prevalence of TMB-high and median values of TMB is generally lower in GEP-NECs than in SCLCs [11, 12, 42, 52, 53, 58, 69, 277]. ARID1A is a more common altered gene in GEP-NEC [10,11,12, 52]. ARID1A is a subunit of SWI/SNF chromatin remodeling complex, and its aberration induces the dysregulation of transcription, DNA repair, and chromatin segregation [278]. ARID1A deficiency impairs the MMR system, resulting in an increased MSI-H genomic signature, TMB, TILs, and PD-L1 expression [279]. Preclinically, ARID1A-deficient tumors, but not ARID1A-wild-type tumors, were regressed by treatment with ICI in xenograft models [279]. Clinically, in a phase I trial of NENs, in which 80% of patients had NECs, 3 of 8 (37.5%) responders to anti-PD-1 Ab toripalimab had ARID1A mutations, while only one of 27 non-responders harbored mutations [268]. Thus, a subset of GEP-NEC with MSI-H, TMB-high, or ARID1A deficiencies may preferentially benefit from ICIs (Fig. 2) [268].
Several treatment strategies have been examined to turn immunologically “cold” tumors with poor immune activation into “hot” tumors with strong immune infiltration in clinical trials combining the anti-PD-1/PD-L1 antibody with other immune-modulating treatments, including other ICIs, chemotherapy, angiogenetic inhibitors, and molecular-targeted agents (Table 7 and Fig. 2). Currently, the most promising strategy for the ICI combination is a dual blockade of PD-1 and cytotoxic T-lymphocyte-associated antigen-4 (CTLA-4). CTLA-4 acts as a negative regulator of the initial priming of T cells in the early stage of the immune response process, whereas PD-1/PD-L1 acts in later stages by turning off antitumor T-cell responses [280]. Therefore, dual inhibitors synergistically promote an antitumor immune response by blocking complementary mechanisms. In SCLC, a combination of anti-PD-1 Ab nivolumab plus anti-CTLA-4 Ab ipilimumab showed more favorable ORRs than nivolumab monotherapy, but the combined regimen was more toxic and similar OS to nivolumab monotherapy [259]. In a phase III CASPIAN trial of anti-PD-L1 Ab durvalumab with or without anti-CTLA-4 Ab tremelimumab in combination with first-line platinum-based chemotherapy, durvalumab plus chemotherapy demonstrated additional survival benefits compared to chemotherapy alone, whereas the addition of tremelimumab to durvalumab plus chemotherapy did not significantly improve outcomes [281]. The efficacy of anti-CTLA-4 Ab may be enriched in patients with TMB-high status [282]. The initial report of the dual inhibition of PD-1/PD-L1 and CTLA-4 was from a phase II multi-cohort trial of nivolumab plus ipilimumab in 32 patients with non-pancreatic NEN, where all responders were observed in an NEC cohort, with an ORR of 44% and a 6-month PFS rate of 44% [283]. Among 8 patients with GEP-NEC, two patients had tumor response. Subsequently, clinical activity was reported in several phase II trials for NENs, including cases of GEP-NEC, ranging from 9 to 50% in terms of ORR [262, 271, 284, 285] (Table 6). The antitumor efficacy of ICIs, including bispecific monoclonal antibodies of PD-1 and CTLA-4, XmAb20717 (NCT05337735 and NCT03517488), as well as anti-PD-L1 Ab avelumab monotherapy (NCT03147404), is currently under investigation in NECs (Table 7).
The PD-1/PD-L1 interaction is not the only immune checkpoint pathway that regulates T-cell activation in the tumor microenvironment (TME). Lymphocyte activation gene 3 protein (LAG3), T-cell immunoglobulin mucin receptor 3 (TIM3), and T-cell immunoreceptor with Ig and ITIM domains (TIGIT) are overexpressed on effector CD4 + and CD8 + T cells, regulatory T cells (Tregs), and natural killer cells, which act as inhibitory immune checkpoint modulators [286]. In fact, TIM3 and LAG3 in immune cells likely hamper the response to ICIs in NECs [287, 288]. TIGIT binds to CD155 with high affinity and competes with its activating counterreceptor CD226, which contributes to the local suppression of immune surveillance. A preclinical model showed that dual blockade of TIGIT and PD-L1 synergistically and specifically enhanced CD8 + T-cell effector function [289]. However, in a phase III SKYSCRAPER-02 trial of anti-PD-L1 Ab atezolizumab plus first-line chemotherapy with or without anti-TIGIT Ab tiragolumab in SCLC, tiragolumab did not provide an additional survival benefit [290]. Further studies of the ICI combination are required for NEC.
Chemotherapy can promote immune responses by increasing the immunogenicity of cancer cells or inhibiting immunosuppressive circuitries [291]. The clinical benefits of anti-PD-1/PD-L1 Ab in combination with first-line chemotherapy for patients with SCLC have been demonstrated [258, 281]. In a phase II NICE-NEC trial of nivolumab plus first-line platinum-based chemotherapy for 38 patients with unresectable G3 NENs of GEP or unknown origin, including 26 patients with NEC, nivolumab plus chemotherapy showed promising activity, with a 12-month PFS rate of 17.5%, a 12-month OS rate of 53.8%, and an ORR of 54% [292]. The median OS seemed to vary according to the primary site, with 6.4 months being reported for colorectal NENs and not reached for esophagogastric and small intestinal NENs. In another study, pembrolizumab plus chemotherapy failed to demonstrate treatment efficacy for 22 patients with previously treated extrapulmonary NECs, including 16 patients with GEP-NECs, with an ORR of 9% and a median PFS of 2 months [293]. The therapeutic strategy combining ICIs with chemotherapy is currently under investigation in several trials (NCT05058651, NCT05142865, and NCT03992911) (Table 7).
As the VEGF/VEGFR signaling pathway induces immunosuppressive effects via the downregulation of MHC expression, the activation of inhibitory immune checkpoint molecules, and the inhibition of TILs and dendritic cell differentiation in addition to angiogenesis [257], the combination of anti-angiogenetic agents with ICI has emerged as a promising strategy with immunomodulatory effects. In fact, the most compatible partners of ICIs have been found to be anti-angiogenetic inhibitors and platinum chemotherapy in a cross-sectional study of 98 clinical trials that included 24,915 patients [294]. Surufatinib is a small-molecule kinase inhibitor that primarily acts on VEGFR 1, 2, and 3; fibroblast growth factor receptor 1 (FGFR 1); and colony-stimulating factor 1 receptor (CSF-1R). Among 13 evaluable patients with NEC in a phase I trial of surufatinib plus toripalimab for advanced solid tumors, the ORR and median PFS were 23.1% and 4.0 months, respectively [295]. In an NEC cohort of the subsequent phase II trial, similar results were observed, with an ORR of 20% and a median PFS of 3.9 months [296], which was a favorable result compared to those of previous trials of ICI monotherapy in NECs (Table 6). Currently, a phase III SURTORI-01 trial (NCT05015621) is ongoing to evaluate the efficacy of surufatinib plus toripalimab versus FOLFIRI chemotherapy in a second-line setting for patients with NEC. In addition, there are several ongoing trials combining anti-PD-1/PD-L1 Ab with surufatinib plus anti-CTLA-4 Ab IBI310 (NCT05165407), cabozantinib (NCT04400474), and cabozantinib plus ipilimumab (NCT04079712) (Table 7).
HDAC inhibitors have been found to enhance tumor immunogenicity through not only increased MHC presentation [297] but also the reduced number and function of myeloid-derived suppressor cells and Tregs [298, 299]. On the other hand, treatment with HDAC inhibitors resulted in the upregulation of PD-L1 [300], which provides a rationale for combining HDAC inhibitors with anti-PD-1/PD-L1 Ab. In fact, early clinical trials have shown encouraging effects of the combined treatment in lung cancer and head and neck cancer [301, 302], and a phase II trial of tucidinostat plus anti-PD-1 antibody sintilimab is ongoing in advanced G3 NENs (NCT05113355).
The DDR pathway is sometimes deficient in NECs [12, 188, 189], which may contribute to the efficacy of ICIs through increased mutation load and neoantigen burden due to the loss of normal DNA repair function [303]. Thus, the DDR pathway and immune responses are connected and potentially synergistic, and combined treatment with ICI and DDR inhibitors, therefore, may have the potential to reinforce antitumor immune activity. As PARP inhibitors also promote host immunosuppression by upregulating PD-L1 expression, a dual blockade of PARP and PD-1/PD-L1 may be a relevant strategy to induce greater antitumor efficacy than inhibition alone [304, 305]. A phase II trial of the PARP inhibitor niraparib plus anti-PD-1 Ab dostarlimab is currently being conducted for SCLC and other NECs (NCT04701307). In addition, CHK1 [304], CDK7 [306], and WEE1 [178] have been shown to be compatible partners of ICIs in preclinical studies of SCLC.
5 Conclusion
NEC is a rare histological subtype among cancers in the GEP system, and the unsatisfying prognosis highlights the clinically urgent need for effective therapeutic compounds. NEC partially shares molecular features specific to SCLC across primary organ sites, whereas NEC also has key genetic aberrations similar to the non-neuroendocrine conventional cancer arising in the same organ sites. Thus, the molecular landscape of GEP-NECs is composed of both neuroendocrine-specific and site-specific alterations, indicating that there is potential in the extrapolation of effective treatment strategies, not only from SCLC but also from conventional cancers at the same site of origin. A better understanding of GEP-NEC biology could reveal a population vulnerable to specific molecular inhibition, which may pave the way for the establishment of personalized medicine. In addition, the assessment of ctDNA will guide the selection of patients who may benefit from molecular-targeted agents by identifying clonally altered genes in GEP-NECs with intratumoral heterogeneity.
References
Rindi, G., Klimstra, D. S., Abedi-Ardekani, B., et al. (2018). A common classification framework for neuroendocrine neoplasms: An International Agency for Research on Cancer (IARC) and World Health Organization (WHO) expert consensus proposal. Modern Pathology., 31, 1770–1786.
Nagtegaal, I. D., Odze, R. D., Klimstra, D., et al. (2020). The 2019 WHO classification of tumours of the digestive system. Histopathology, 76, 182–188.
Rickman, D. S., Beltran, H., Demichelis, F., & Rubin, M. A. (2017). Biology and evolution of poorly differentiated neuroendocrine tumors. Nature Medicine, 23, 1–10.
Balanis, N. G., Sheu, K. M., Esedebe, F. N., et al. (2019). Pan-cancer convergence to a small-cell neuroendocrine phenotype that shares susceptibilities with hematological malignancies. Cancer Cell, 36, 17-34.e17.
Park, J. W., Lee, J. K., Sheu, K. M., et al. (2018). Reprogramming normal human epithelial tissues to a common, lethal neuroendocrine cancer lineage. Science, 362, 91–95.
Dasari, A., Mehta, K., Byers, L. A., Sorbye, H., & Yao, J. C. (2018). Comparative study of lung and extrapulmonary poorly differentiated neuroendocrine carcinomas: A SEER database analysis of 162,983 cases. Cancer, 124, 807–815.
Janson, E. T., Knigge, U., Dam, G., et al. (2021). Nordic guidelines 2021 for diagnosis and treatment of gastroenteropancreatic neuroendocrine neoplasms. Acta Oncologica, 60, 931–941.
Garcia-Carbonero, R., Sorbye, H., Baudin, E., et al. (2016). ENETS consensus guidelines for high-grade gastroenteropancreatic neuroendocrine tumors and neuroendocrine carcinomas. Neuroendocrinology, 103, 186–194.
Yachida, S., Vakiani, E., White, C. M., et al. (2012). Small cell and large cell neuroendocrine carcinomas of the pancreas are genetically similar and distinct from well-differentiated pancreatic neuroendocrine tumors. American Journal of Surgical Pathology, 36, 173–184.
Yachida, S., Totoki, Y., Noë, M., et al. (2022). Comprehensive genomic profiling of neuroendocrine carcinomas of the gastrointestinal system. Cancer Discovery, 12, 692–711.
Frizziero, M., Kilgour, E., Simpson, K. L., et al. (2022). Expanding therapeutic opportunities for extrapulmonary neuroendocrine carcinoma. Clinical Cancer Research, 28, 1999–2019.
Venizelos, A., Elvebakken, H., Perren, A., et al. (2021). The molecular characteristics of high-grade gastroenteropancreatic neuroendocrine neoplasms. Endocrine-Related Cancer, 29, 1–14.
Assarzadegan, N., & Montgomery, E. (2021). What is new in the 2019 World Health Organization (WHO) classification of tumors of the digestive system: Review of selected updates on neuroendocrine neoplasms, appendiceal tumors, and molecular testing. Archives of Pathology and Laboratory Medicine, 145, 664–677.
Sorbye, H., Welin, S., Langer, S. W., et al. (2013). Predictive and prognostic factors for treatment and survival in 305 patients with advanced gastrointestinal neuroendocrine carcinoma (WHO G3): The NORDIC NEC study. Annals of Oncology., 24, 152–160.
Walenkamp, A. M., Sonke, G. S., & Sleijfer, D. T. (2009). Clinical and therapeutic aspects of extrapulmonary small cell carcinoma. Cancer Treatment Reviews, 35, 228–236.
Basturk, O., Tang, L., Hruban, R. H., et al. (2014). Poorly differentiated neuroendocrine carcinomas of the pancreas: A clinicopathologic analysis of 44 cases. American Journal of Surgical Pathology, 38, 437–447.
Sorbye, H., Strosberg, J., Baudin, E., Klimstra, D. S., & Yao, J. C. (2014). Gastroenteropancreatic high-grade neuroendocrine carcinoma. Cancer, 120, 2814–2823.
Bellizzi, A. M. (2020). Immunohistochemistry in the diagnosis and classification of neuroendocrine neoplasms: What can brown do for you? Human Pathology, 96, 8–33.
Heetfeld, M., Chougnet, C. N., Olsen, I. H., et al. (2015). Characteristics and treatment of patients with G3 gastroenteropancreatic neuroendocrine neoplasms. Endocrine-Related Cancer, 22, 657–664.
Hijioka, S., Hosoda, W., Matsuo, K., et al. (2017). Rb loss and KRAS mutation are predictors of the response to platinum-based chemotherapy in pancreatic neuroendocrine neoplasm with grade 3: A Japanese Multicenter Pancreatic NEN-G3 Study. Clinical Cancer Research, 23, 4625–4632.
Walter, T., Tougeron, D., Baudin, E., et al. (2017). Poorly differentiated gastro-entero-pancreatic neuroendocrine carcinomas: Are they really heterogeneous? Insights from the FFCD-GTE national cohort. European Journal of Cancer, 79, 158–165.
Alese, O. B., Jiang, R., Shaib, W., et al. (2019). High-grade gastrointestinal neuroendocrine carcinoma management and outcomes: A National Cancer Database study. The Oncologist, 24, 911–920.
Cicin, I., Karagol, H., Uzunoglu, S., et al. (2007). Extrapulmonary small-cell carcinoma compared with small-cell lung carcinoma: A retrospective single-center study. Cancer, 110, 1068–1076.
Stelwagen, J., de Vries, E. G. E., & Walenkamp, A. M. E. (2021). Current treatment strategies and future directions for extrapulmonary neuroendocrine carcinomas: A review. JAMA Oncology, 7, 759–770.
Dasari, A., Shen, C., Halperin, D., et al. (2017). Trends in the incidence, prevalence, and survival outcomes in patients with neuroendocrine tumors in the United States. JAMA Oncology, 3, 1335–1342.
Boyar Cetinkaya, R., Aagnes, B., Myklebust, T., & Thiis-Evensen, E. (2018). Survival in neuroendocrine neoplasms; a report from a large Norwegian population-based study. International Journal of Cancer, 142, 1139–1147.
Milione, M., Maisonneuve, P., Spada, F., et al. (2017). The clinicopathologic heterogeneity of grade 3 gastroenteropancreatic neuroendocrine neoplasms: Morphological differentiation and proliferation identify different prognostic categories. Neuroendocrinology, 104, 85–93.
Sorbye, H., Baudin, E., Borbath, I., et al. (2019). Unmet needs in high-grade gastroenteropancreatic neuroendocrine neoplasms (WHO G3). Neuroendocrinology, 108, 54–62.
Takayanagi, D., Cho, H., Machida, E., et al. (2022). Update on epidemiology, diagnosis, and biomarkers in gastroenteropancreatic neuroendocrine neoplasms. Cancers (Basel), 14, 1119.
Rindi, G., Mete, O., Uccella, S., et al. (2022). Overview of the 2022 WHO classification of neuroendocrine neoplasms. Endocrine Pathology, 33, 115–154.
Pavel, M., Öberg, K., Falconi, M., et al. (2020). Gastroenteropancreatic neuroendocrine neoplasms: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Annals of Oncology., 31, 844–860.
Fang, C., Wang, W., Feng, X., et al. (2017). Nomogram individually predicts the overall survival of patients with gastroenteropancreatic neuroendocrine neoplasms. British Journal of Cancer, 117, 1544–1550.
Janson, E. T., Sørbye, H., Welin, S., et al. (2010). Nordic Guidelines 2010 for diagnosis and treatment of gastroenteropancreatic neuroendocrine tumours. Acta Oncologica, 49, 740–756.
Kessel, E., Naparst, M., Alpert, N., et al. (2021). Racial differences in gastroenteropancreatic neuroendocrine tumor treatment and survival in the United States. Pancreas, 50, 29–36.
Koizumi, T., Otsuki, K., Tanaka, Y., & Kanda, S. (2022). Epidemiology of neuroendocrine neoplasmas in Japan: Based on analysis of hospital-based cancer registry data, 2009–2015. BMC Endocrine Disorders, 22, 105.
Man, D., Wu, J., Shen, Z., & Zhu, X. (2018). Prognosis of patients with neuroendocrine tumor: A SEER database analysis. Cancer Management and Research., 10, 5629–5638.
Riihimäki, M., Hemminki, A., Sundquist, K., Sundquist, J., & Hemminki, K. (2016). The epidemiology of metastases in neuroendocrine tumors. International Journal of Cancer, 139, 2679–2686.
van der Zwan, J. M., Siesling, S., van Velthuysen, L., Links, T., Walenkamp, A., & Tesselaar, M. (2018). Extra-pulmonary neuroendocrine carcinomas: A population-based study in the Netherlands. Neuroendocrinology, 107, 50–59.
Yao, J. C., Hassan, M., Phan, A., et al. (2008). One hundred years after “carcinoid”: Epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. Journal of Clinical Oncology, 26, 3063–3072.
Basturk, O., Yang, Z., Tang, L. H., et al. (2015). The high-grade (WHO G3) pancreatic neuroendocrine tumor category is morphologically and biologically heterogenous and includes both well differentiated and poorly differentiated neoplasms. American Journal of Surgical Pathology, 39, 683–690.
Vélayoudom-Céphise, F. L., Duvillard, P., Foucan, L., et al. (2013). Are G3 ENETS neuroendocrine neoplasms heterogeneous? Endocrine-Related Cancer, 20, 649–657.
George, J., Lim, J. S., Jang, S. J., et al. (2015). Comprehensive genomic profiles of small cell lung cancer. Nature, 524, 47–53.
Rudin, C. M., Durinck, S., Stawiski, E. W., et al. (2012). Comprehensive genomic analysis identifies SOX2 as a frequently amplified gene in small-cell lung cancer. Nature Genetics, 44, 1111–1116.
Peifer, M., Fernández-Cuesta, L., Sos, M. L., et al. (2012). Integrative genome analyses identify key somatic driver mutations of small-cell lung cancer. Nature Genetics, 44, 1104–1110.
Bergsland, E. K., Roy, R., Stephens, P., Ross, J. S., Bailey, M., & Olshen, A. (2016). Genomic profiling to distinguish poorly differentiated neuroendocrine carcinomas arising in different sites. Journal of Clinical Oncology., 34, 4020–4020.
Lou, G., Yu, X., & Song, Z. (2017). Molecular profiling and survival of completely resected primary pulmonary neuroendocrine carcinoma. Clinical Lung Cancer, 18, e197–e201.
Marcoux, N., Gettinger, S. N., O’Kane, G., et al. (2019). EGFR-mutant adenocarcinomas that transform to small-cell lung cancer and other neuroendocrine carcinomas: Clinical outcomes. Journal of Clinical Oncology, 37, 278–285.
Ku, S. Y., Rosario, S., Wang, Y., et al. (2017). Rb1 and Trp53 cooperate to suppress prostate cancer lineage plasticity, metastasis, and antiandrogen resistance. Science, 355, 78–83.
Beltran, H., Prandi, D., Mosquera, J. M., et al. (2016). Divergent clonal evolution of castration-resistant neuroendocrine prostate cancer. Nature Medicine, 22, 298–305.
Rubin, M. A., Bristow, R. G., Thienger, P. D., Dive, C., & Imielinski, M. (2020). Impact of lineage plasticity to and from a neuroendocrine phenotype on progression and response in prostate and lung cancers. Molecular Cell, 80, 562–577.
Sutherland, K. D., Proost, N., Brouns, I., Adriaensen, D., Song, J. Y., & Berns, A. (2011). Cell of origin of small cell lung cancer: Inactivation of Trp53 and Rb1 in distinct cell types of adult mouse lung. Cancer Cell, 19, 754–764.
Puccini, A., Poorman, K., Salem, M. E., et al. (2020). Comprehensive genomic profiling of gastroenteropancreatic neuroendocrine neoplasms (GEP-NENs). Clinical Cancer Research, 26, 5943–5951.
Chen, L., Liu, M., Zhang, Y., Guo, Y., Chen, M. H., & Chen, J. (2021). Genetic characteristics of colorectal neuroendocrine carcinoma: More similar to colorectal adenocarcinoma. Clinical Colorectal Cancer, 20, 177-185.e113.
Sahnane, N., Furlan, D., Monti, M., et al. (2015). Microsatellite unstable gastrointestinal neuroendocrine carcinomas: A new clinicopathologic entity. Endocrine-Related Cancer, 22, 35–45.
Vijayvergia, N., Boland, P. M., Handorf, E., et al. (2016). Molecular profiling of neuroendocrine malignancies to identify prognostic and therapeutic markers: A Fox Chase Cancer Center Pilot Study. British Journal of Cancer, 115, 564–570.
Kawasaki, K., Toshimitsu, K., Matano, M., et al. (2020). An organoid biobank of neuroendocrine neoplasms enables genotype-phenotype mapping. Cell, 183, 1420-1435.e1421.
Wu, H., Yu, Z., Liu, Y., et al. (2022). Genomic characterization reveals distinct mutation landscapes and therapeutic implications in neuroendocrine carcinomas of the gastrointestinal tract. Cancer Commun (Lond), 42, 1367–1386.
Li, R., Yang, Z., Shao, F., et al. (2021). Multi-omics profiling of primary small cell carcinoma of the esophagus reveals RB1 disruption and additional molecular subtypes. Nature Communications, 12, 3785.
Shamir, E. R., Devine, W. P., Pekmezci, M., et al. (2019). Identification of high-risk human papillomavirus and Rb/E2F pathway genomic alterations in mutually exclusive subsets of colorectal neuroendocrine carcinoma. Modern Pathology., 32, 290–305.
Li, A. F., Li, A. C., Tsay, S. H., Li, W. Y., Liang, W. Y., & Chen, J. Y. (2008). Alterations in the p16INK4a/cyclin D1/RB pathway in gastrointestinal tract endocrine tumors. American Journal of Clinical Pathology, 130, 535–542.
Busico, A., Maisonneuve, P., Prinzi, N., et al. (2020). Gastroenteropancreatic high-grade neuroendocrine neoplasms: Histology and molecular analysis, two sides of the same coin. Neuroendocrinology, 110, 616–629.
Konukiewitz, B., Jesinghaus, M., Steiger, K., et al. (2018). Pancreatic neuroendocrine carcinomas reveal a closer relationship to ductal adenocarcinomas than to neuroendocrine tumors G3. Human Pathology, 77, 70–79.
Takizawa, N., Ohishi, Y., Hirahashi, M., et al. (2015). Molecular characteristics of colorectal neuroendocrine carcinoma; similarities with adenocarcinoma rather than neuroendocrine tumor. Human Pathology, 46, 1890–1900.
Mu, P., Zhang, Z., Benelli, M., et al. (2017). SOX2 promotes lineage plasticity and antiandrogen resistance in TP53- and RB1-deficient prostate cancer. Science, 355, 84–88.
Park, K. S., Liang, M. C., Raiser, D. M., et al. (2011). Characterization of the cell of origin for small cell lung cancer. Cell Cycle, 10, 2806–2815.
Girardi, D. M., Silva, A. C. B., Rêgo, J. F. M., Coudry, R. A., & Riechelmann, R. P. (2017). Unraveling molecular pathways of poorly differentiated neuroendocrine carcinomas of the gastroenteropancreatic system: A systematic review. Cancer Treatment Reviews, 56, 28–35.
Scarpa, A., Chang, D. K., Nones, K., et al. (2017). Whole-genome landscape of pancreatic neuroendocrine tumours. Nature, 543, 65–71.
Jiao, Y., Shi, C., Edil, B. H., et al. (2011). DAXX/ATRX, MEN1, and mTOR pathway genes are frequently altered in pancreatic neuroendocrine tumors. Science, 331, 1199–1203.
Xing, J., Ying, H., Li, J., et al. (2020). Immune checkpoint markers in neuroendocrine carcinoma of the digestive system. Frontiers in Oncology, 10, 132.
Fraune, C., Simon, R., Hube-Magg, C., et al. (2020). Homogeneous MMR deficiency throughout the entire tumor mass occurs in a subset of colorectal neuroendocrine carcinomas. Endocrine Pathology, 31, 182–189.
Akagi, K., Oki, E., Taniguchi, H., et al. (2021). The real-world data on microsatellite instability status in various unresectable or metastatic solid tumors. Cancer Sci, 12, 1105–1113.
Le, D. T., Durham, J. N., Smith, K. N., et al. (2017). Mismatch repair deficiency predicts response of solid tumors to PD-1 blockade. Science, 357, 409–413.
Vanderwalde, A., Spetzler, D., Xiao, N., Gatalica, Z., & Marshall, J. (2018). Microsatellite instability status determined by next-generation sequencing and compared with PD-L1 and tumor mutational burden in 11,348 patients. Cancer Medicine, 7, 746–756.
Ichikawa, Y., Kobayashi, N., Goto, A., et al. (2018). Abstract 3134: Pilot study of immune status of GEP-NETs in tumor microenvironment. Cancer Research, 78, 3134–3134.
Chung, H. C., Lopez-Martin, J. A., Kao, S.C.-H., et al. (2018). Phase 2 study of pembrolizumab in advanced small-cell lung cancer (SCLC): KEYNOTE-158. Journal of Clinical Oncology., 36, 8506–8506.
Rudin, C. M., Poirier, J. T., Byers, L. A., et al. (2019). Molecular subtypes of small cell lung cancer: A synthesis of human and mouse model data. Nature Reviews Cancer, 19, 289–297.
Gay, C. M., Stewart, C. A., Park, E. M., et al. (2021). Patterns of transcription factor programs and immune pathway activation define four major subtypes of SCLC with distinct therapeutic vulnerabilities. Cancer Cell, 39, 346-360.e347.
Metovic, J., La Salvia, A., Rapa, I., et al. (2022). Molecular subtypes of extra-pulmonary neuroendocrine carcinomas identified by the expression of neuroendocrine lineage-specific transcription factors. Endocrine Pathology, 33, 388–399.
Borromeo, M. D., Savage, T. K., Kollipara, R. K., et al. (2016). ASCL1 and NEUROD1 reveal heterogeneity in pulmonary neuroendocrine tumors and regulate distinct genetic programs. Cell Reports, 16, 1259–1272.
Bylund, M., Andersson, E., Novitch, B. G., & Muhr, J. (2003). Vertebrate neurogenesis is counteracted by Sox1-3 activity. Nature Neuroscience, 6, 1162–1168.
Ooki, A., Begum, A., Marchionni, L., et al. (2018). Arsenic promotes the COX2/PGE2-SOX2 axis to increase the malignant stemness properties of urothelial cells. International Journal of Cancer, 143, 113–126.
Ooki, A., Del Carmen Rodriguez Pena, M., Marchionni, L., et al. (2018). YAP1 and COX2 coordinately regulate urothelial cancer stem-like cells. Cancer Res., 78, 168–181.
Ooki, A., Dinalankara, W., Marchionni, L., et al. (2018). Epigenetically regulated PAX6 drives cancer cells toward a stem-like state via GLI-SOX2 signaling axis in lung adenocarcinoma. Oncogene, 37, 5967–5981.
Klempner, S. J., Gershenhorn, B., Tran, P., et al. (2016). BRAFV600E mutations in high-grade colorectal neuroendocrine tumors may predict responsiveness to BRAF-MEK combination therapy. Cancer Discovery, 6, 594–600.
Olevian, D. C., Nikiforova, M. N., Chiosea, S., et al. (2016). Colorectal poorly differentiated neuroendocrine carcinomas frequently exhibit BRAF mutations and are associated with poor overall survival. Human Pathology, 49, 124–134.
Lee, S. M., & Sung, C. O. (2021). Comprehensive analysis of mutational and clinicopathologic characteristics of poorly differentiated colorectal neuroendocrine carcinomas. Science and Reports, 11, 6203.
Dizdar, L., Werner, T. A., Drusenheimer, J. C., et al. (2019). BRAF(V600E) mutation: A promising target in colorectal neuroendocrine carcinoma. International Journal of Cancer, 144, 1379–1390.
Capdevila, J., Arqués, O., Hernández Mora, J. R., et al. (2020). Epigenetic EGFR gene repression confers sensitivity to therapeutic BRAFV600E blockade in colon neuroendocrine carcinomas. Clinical Cancer Research, 26, 902–909.
Yachida, S., Wood, L. D., Suzuki, M., et al. (2016). Genomic sequencing identifies ELF3 as a driver of ampullary carcinoma. Cancer Cell, 29, 229–240.
Gao, H. L., Wang, W. Q., Yu, X. J., & Liu, L. (2020). Molecular drivers and cells of origin in pancreatic ductal adenocarcinoma and pancreatic neuroendocrine carcinoma. Experimental Hematology & Oncology, 9, 28.
Konukiewitz, B., Schlitter, A. M., Jesinghaus, M., et al. (2017). Somatostatin receptor expression related to TP53 and RB1 alterations in pancreatic and extrapancreatic neuroendocrine neoplasms with a Ki67-index above 20. Modern Pathology, 30, 587–598.
Koh, J., Nam, S. K., Kwak, Y., et al. (2021). Comprehensive genetic features of gastric mixed adenoneuroendocrine carcinomas and pure neuroendocrine carcinomas. The Journal of Pathology, 253, 94–105.
Ooki, A., & Yamaguchi, K. (2022). The dawn of precision medicine in diffuse-type gastric cancer. Therapeutic Advances in Medical Oncology., 14, 17588359221083048.
Ishida, M., Sekine, S., Taniguchi, H., Fukagawa, T., Katai, H., & Kushima, R. (2014). Consistent absence of HER2 expression, regardless of HER2 amplification status, in neuroendocrine carcinomas of the stomach. Histopathology, 64, 1027–1031.
Ooki, A., Osumi, H., Chin, K., Watanabe, M., & Yamaguchi, K. (2023). Potent molecular-targeted therapies for advanced esophageal squamous cell carcinoma. Ther Adv Med Oncol., 15, 17588359221138376.
Vanoli, A., La Rosa, S., Klersy, C., et al. (2017). Four neuroendocrine tumor types and neuroendocrine carcinoma of the duodenum: Analysis of 203 cases. Neuroendocrinology, 104, 112–125.
Liu, F., Li, Y., Ying, D., et al. (2021). Whole-exome mutational landscape of neuroendocrine carcinomas of the gallbladder. Signal Transduction and Targeted Therapy, 6, 55.
Lee, S. M., & Sung, C. O. (2020). Neuroendocrine carcinomas of the gallbladder: A clinicopathologic and immunohistochemical analysis of 34 resected cases. American Journal of Surgical Pathology, 44, 1308–1321.
Heaphy, C. M., de Wilde, R. F., Jiao, Y., et al. (2011). Altered telomeres in tumors with ATRX and DAXX mutations. Science, 333, 425.
Singhi, A. D., Liu, T. C., Roncaioli, J. L., et al. (2017). Alternative lengthening of telomeres and loss of DAXX/ATRX expression predicts metastatic disease and poor survival in patients with pancreatic neuroendocrine tumors. Clinical Cancer Research, 23, 600–609.
Simon, T., Riemer, P., Jarosch, A., et al. (2022). DNA methylation reveals distinct cells of origin for pancreatic neuroendocrine carcinomas and pancreatic neuroendocrine tumors. Genome Medicine., 14, 24.
Tang, L. H., Basturk, O., Sue, J. J., & Klimstra, D. S. (2016). A practical approach to the classification of WHO grade 3 (G3) well-differentiated neuroendocrine tumor (WD-NET) and poorly differentiated neuroendocrine carcinoma (PD-NEC) of the pancreas. American Journal of Surgical Pathology, 40, 1192–1202.
The National Comprehensive Cancer Network (2023) NCCN clinical practice guidelines in neuroendocrine and adrenal tumors. https://www.nccn.org/professionals/physician_gls/pdf/neuroendocrine.pdf. 2023;version 1. Accessed 15 Apr 2023.
Morizane, C., Machida, N., Honma, Y., et al. (2022). Effectiveness of etoposide and cisplatin vs irinotecan and cisplatin therapy for patients with advanced neuroendocrine carcinoma of the digestive system: the TOPIC-NEC phase 3 randomized clinical trial. JAMA Oncology, 8, 1447–1455.
Yamaguchi, T., Machida, N., Morizane, C., et al. (2014). Multicenter retrospective analysis of systemic chemotherapy for advanced neuroendocrine carcinoma of the digestive system. Cancer Science, 105, 1176–1181.
Ali, A. S., Grönberg, M., Langer, S. W., et al. (2018). Intravenous versus oral etoposide: Efficacy and correlation to clinical outcome in patients with high-grade metastatic gastroenteropancreatic neuroendocrine neoplasms (WHO G3). Medical oncology (Northwood, London, England)., 35, 47–47.
Mitry, E., Baudin, E., Ducreux, M., et al. (1999). Treatment of poorly differentiated neuroendocrine tumours with etoposide and cisplatin. British Journal of Cancer, 81, 1351–1355.
Moertel, C. G., Kvols, L. K., O’Connell, M. J., & Rubin, J. (1991). Treatment of neuroendocrine carcinomas with combined etoposide and cisplatin. Evidence of major therapeutic activity in the anaplastic variants of these neoplasms. Cancer., 68, 227–232.
Iwasa, S., Morizane, C., Okusaka, T., et al. (2010). Cisplatin and etoposide as first-line chemotherapy for poorly differentiated neuroendocrine carcinoma of the hepatobiliary tract and pancreas. Japanese Journal of Clinical Oncology, 40, 313–318.
Imai, H., Shirota, H., Okita, A., et al. (2016). Efficacy and safety of carboplatin and etoposide combination chemotherapy for extrapulmonary neuroendocrine carcinoma: A retrospective case series. Chemotherapy, 61, 111–116.
Frizziero, M., Spada, F., Lamarca, A., et al. (2019). Carboplatin in combination with oral or intravenous etoposide for extra-pulmonary, poorly-differentiated neuroendocrine carcinomas. Neuroendocrinology, 109, 100–112.
Brandi, G., Paragona, M., Campana, D., et al. (2018). Good performance of platinum-based chemotherapy for high-grade gastroenteropancreatic and unknown primary neuroendocrine neoplasms. Journal of Chemotherapy, 30, 53–58.
Hainsworth, J. D., Spigel, D. R., Litchy, S., & Greco, F. A. (2006). Phase II trial of paclitaxel, carboplatin, and etoposide in advanced poorly differentiated neuroendocrine carcinoma: A Minnie Pearl Cancer Research Network Study. Journal of Clinical Oncology, 24, 3548–3554.
Mani, M. A., Shroff, R. T., Jacobs, C., et al. (2008). A phase II study of irinotecan and cisplatin for metastatic or unresectable high grade neuroendocrine carcinoma. Journal of Clinical Oncology., 26, 15550–15550.
Okita, N. T., Kato, K., Takahari, D., et al. (2011). Neuroendocrine tumors of the stomach: Chemotherapy with cisplatin plus irinotecan is effective for gastric poorly-differentiated neuroendocrine carcinoma. Gastric Cancer, 14, 161–165.
Nakano, K., Takahashi, S., Yuasa, T., et al. (2012). Feasibility and efficacy of combined cisplatin and irinotecan chemotherapy for poorly differentiated neuroendocrine carcinomas. Japanese Journal of Clinical Oncology, 42, 697–703.
Okuma, H. S., Iwasa, S., Shoji, H., et al. (2014). Irinotecan plus cisplatin in patients with extensive-disease poorly differentiated neuroendocrine carcinoma of the esophagus. Anticancer Research, 34, 5037–5041.
Lu, Z. H., Li, J., Lu, M., et al. (2013). Feasibility and efficacy of combined cisplatin plus irinotecan chemotherapy for gastroenteropancreatic neuroendocrine carcinomas. Medical oncology (Northwood, London, England)., 30, 664.
Ramella Munhoz, R., de Mendonça Rego, J. F., de Celis Ferrari, A. R., et al. (2013). Combination of irinotecan and a platinum agent for poorly differentiated neuroendocrine carcinomas. Rare Tumors., 5, e39.
Li, J., Lu, M., Lu, Z., et al. (2017). Irinotecan plus cisplatin followed by octreotide long-acting release maintenance treatment in advanced gastroenteropancreatic neuroendocrine carcinoma: IPO-NEC study. Oncotarget, 8, 25669–25678.
Raj, N., Valentino, E., Capanu, M., et al. (2017). Treatment response and outcomes of grade 3 pancreatic neuroendocrine neoplasms based on morphology: Well differentiated versus poorly differentiated. Pancreas, 46, 296–301.
Zhang, P., Li, J., Li, J., et al. (2020). Etoposide and cisplatin versus irinotecan and cisplatin as the first-line therapy for patients with advanced, poorly differentiated gastroenteropancreatic neuroendocrine carcinoma: A randomized phase 2 study. Cancer, 126(Suppl 9), 2086–2092.
Du, Z., Wang, Y., Zhou, Y., Wen, F., & Li, Q. (2013). First-line irinotecan combined with 5-fluorouracil and leucovorin for high-grade metastatic gastrointestinal neuroendocrine carcinoma. Tumori, 99, 57–60.
Hentic, O., Hammel, P., Couvelard, A., et al. (2012). FOLFIRI regimen: An effective second-line chemotherapy after failure of etoposide-platinum combination in patients with neuroendocrine carcinomas grade 3. Endocrine-Related Cancer, 19, 751–757.
Sugiyama, K., Shiraishi, K., Sato, M., Nishibori, R., Nozawa, K., & Kitagawa, C. (2021). Salvage chemotherapy by FOLFIRI regimen for poorly differentiated gastrointestinal neuroendocrine carcinoma. Journal of Gastrointestinal Cancer, 52, 947–951.
Hadoux, J., Malka, D., Planchard, D., et al. (2015). Post-first-line FOLFOX chemotherapy for grade 3 neuroendocrine carcinoma. Endocrine-Related Cancer, 22, 289–298.
Bajetta, E., Catena, L., Procopio, G., et al. (2007). Are capecitabine and oxaliplatin (XELOX) suitable treatments for progressing low-grade and high-grade neuroendocrine tumours? Cancer Chemotherapy and Pharmacology, 59, 637–642.
Olsen, I. H., Sørensen, J. B., Federspiel, B., et al. (2012). Temozolomide as second or third line treatment of patients with neuroendocrine carcinomas. ScientificWorldJournal., 2012, 170496.
Welin, S., Sorbye, H., Sebjornsen, S., Knappskog, S., Busch, C., & Oberg, K. (2011). Clinical effect of temozolomide-based chemotherapy in poorly differentiated endocrine carcinoma after progression on first-line chemotherapy. Cancer, 117, 4617–4622.
Rogowski, W., Wachuła, E., Gorzelak, A., et al. (2019). Capecitabine and temozolomide combination for treatment of high-grade, well-differentiated neuroendocrine tumour and poorly-differentiated neuroendocrine carcinoma - retrospective analysis. Endokrynologia Polska, 70, 313–317.
Ando, T., Hosokawa, A., Yoshita, H., et al. (2015). Amrubicin monotherapy for patients with platinum-refractory gastroenteropancreatic neuroendocrine carcinoma. Gastroenterol Res Pract., 2015, 425876.
Nio, K., Arita, S., Isobe, T., et al. (2015). Amrubicin monotherapy for patients with extrapulmonary neuroendocrine carcinoma after platinum-based chemotherapy. Cancer Chemotherapy and Pharmacology, 75, 829–835.
Araki, T., Takashima, A., Hamaguchi, T., et al. (2016). Amrubicin in patients with platinum-refractory metastatic neuroendocrine carcinoma and mixed adenoneuroendocrine carcinoma of the gastrointestinal tract. Anti-Cancer Drugs, 27, 794–799.
Kitagawa, Y., Osumi, H., Shinozaki, E., et al. (2019). Safety and efficacy of amrubicin monotherapy in patients with platinum-refractory metastatic neuroendocrine carcinoma of the gastrointestinal tract: A single cancer center retrospective study. Cancer Manag Res., 11, 5757–5764.
Apostolidis, L., Bergmann, F., Jäger, D., & Winkler, E. C. (2016). Efficacy of topotecan in pretreated metastatic poorly differentiated extrapulmonary neuroendocrine carcinoma. Cancer Medicine, 5, 2261–2267.
Olsen, I. H., Knigge, U., Federspiel, B., et al. (2014). Topotecan monotherapy in heavily pretreated patients with progressive advanced stage neuroendocrine carcinomas. Journal of Cancer, 5, 628–632.
Chen, M. H., Chou, W. C., Hsiao, C. F., et al. (2020). An open-label, single-arm, two-stage, multicenter, phase II study to evaluate the efficacy of TLC388 and genomic analysis for poorly differentiated neuroendocrine carcinomas. The Oncologist, 25, e782–e788.
McNamara, M. G., Swain, J., Craig, Z., et al. (2022). NET-02: A multicenter, randomized, phase II trial of liposomal irinotecan (nal-IRI) and 5-fluorouracil (5-FU)/folinic acid or docetaxel as second-line therapy in patients (pts) with progressive poorly differentiated extra-pulmonary neuroendocrine carcinoma (PD-EP-NEC). Journal of Clinical Oncology., 40, 4005–4005.
McNamara, M. G., Frizziero, M., Jacobs, T., et al. (2020). Second-line treatment in patients with advanced extra-pulmonary poorly differentiated neuroendocrine carcinoma: A systematic review and meta-analysis. Therapeutic Advances in Medical Oncology., 12, 1758835920915299.
Conroy, T., Desseigne, F., Ychou, M., et al. (2011). FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. New England Journal of Medicine, 364, 1817–1825.
Kunz, P. L., Graham, N. T., Catalano, P. J., et al. (2023). A randomized study of temozolomide or temozolomide and capecitabine in patients with advanced pancreatic neuroendocrine tumors (ECOG-ACRIN E2211). Journal of Clinical Oncology, 41, 1359–1369.
Chan, D. L., Bergsland, E. K., Chan, J. A., et al. (2021). Temozolomide in grade 3 gastroenteropancreatic neuroendocrine neoplasms: A multicenter retrospective review. The Oncologist, 26, 950–955.
Jänne, P. A., Riely, G. J., Gadgeel, S. M., et al. (2022). Adagrasib in non-small-cell lung cancer harboring a KRAS(G12C) mutation. New England Journal of Medicine, 387, 120–131.
Skoulidis, F., Li, B. T., Dy, G. K., et al. (2021). Sotorasib for lung cancers with KRAS p.G12C mutation. The New England Journal of Medicine., 384, 2371–2381.
Wang, S., Li, Q., Ma, P., et al. (2022). KRAS mutation in rare tumors: A landscape analysis of 3453 Chinese patients. Frontiers in Molecular Biosciences, 9, 831382.
Thein, K. Z., Biter, A. B., Banks, K. C., et al. (2022). Identification of KRAS(G12C) mutations in circulating tumor DNA in patients with cancer. JCO Precision Oncology, 6, e2100547.
Hong, D. S., Fakih, M. G., Strickler, J. H., et al. (2020). KRAS(G12C) Inhibition with sotorasib in advanced solid tumors. New England Journal of Medicine, 383, 1207–1217.
Amodio, V., Yaeger, R., Arcella, P., et al. (2020). EGFR blockade reverts resistance to KRAS(G12C) inhibition in colorectal cancer. Cancer Discovery, 10, 1129–1139.
Moore, A. R., Rosenberg, S. C., McCormick, F., & Malek, S. (2020). RAS-targeted therapies: Is the undruggable drugged? Nature Reviews. Drug Discovery, 19, 533–552.
Chapman, P. B., Hauschild, A., Robert, C., et al. (2011). Improved survival with vemurafenib in melanoma with BRAF V600E mutation. New England Journal of Medicine, 364, 2507–2516.
Subbiah, V., Puzanov, I., Blay, J. Y., et al. (2020). Pan-cancer efficacy of vemurafenib in BRAF (V600)-mutant non-melanoma cancers. Cancer Discovery, 10, 657–663.
Planchard, D., Kim, T. M., Mazieres, J., et al. (2016). Dabrafenib in patients with BRAF(V600E)-positive advanced non-small-cell lung cancer: A single-arm, multicentre, open-label, phase 2 trial. The lancet Oncology, 17, 642–650.
Kopetz, S., Desai, J., Chan, E., et al. (2015). Phase II pilot study of vemurafenib in patients with metastatic BRAF-mutated colorectal cancer. Journal of Clinical Oncology, 33, 4032–4038.
Prahallad, A., Sun, C., Huang, S., et al. (2012). Unresponsiveness of colon cancer to BRAF(V600E) inhibition through feedback activation of EGFR. Nature, 483, 100–103.
Kopetz, S., Grothey, A., Yaeger, R., et al. (2019). Encorafenib, binimetinib, and cetuximab in BRAF V600E-mutated colorectal cancer. New England Journal of Medicine, 381, 1632–1643.
Long, G. V., Stroyakovskiy, D., Gogas, H., et al. (2014). Combined BRAF and MEK inhibition versus BRAF inhibition alone in melanoma. New England Journal of Medicine, 371, 1877–1888.
Wang, J., Huang, S. K., Marzese, D. M., et al. (2015). Epigenetic changes of EGFR have an important role in BRAF inhibitor-resistant cutaneous melanomas. The Journal of Investigative Dermatology, 135, 532–541.
Burkart, J., Owen, D., Shah, M. H., et al. (2018). Targeting BRAF mutations in high-grade neuroendocrine carcinoma of the colon. Journal of the National Comprehensive Cancer Network, 16, 1035–1040.
Yao, J. C., Shah, M. H., Ito, T., et al. (2011). Everolimus for advanced pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 514–523.
Okuyama, H., Ikeda, M., Okusaka, T., et al. (2020). A phase II trial of everolimus in patients with advanced pancreatic neuroendocrine carcinoma refractory or intolerant to platinum-containing chemotherapy (NECTOR Trial). Neuroendocrinology, 110, 988–993.
Farrell, A. S., Joly, M. M., Allen-Petersen, B. L., et al. (2017). MYC regulates ductal-neuroendocrine lineage plasticity in pancreatic ductal adenocarcinoma associated with poor outcome and chemoresistance. Nature Communications, 8, 1728.
Dang, C. V. (2012). MYC on the path to cancer. Cell, 149, 22–35.
Martínez-Martín, S., & Soucek, L. (2021). MYC inhibitors in multiple myeloma. Cancer Drug Resistance., 4, 842–865.
Kelso, T. W., Baumgart, K., Eickhoff, J., et al. (2014). Cyclin-dependent kinase 7 controls mRNA synthesis by affecting stability of preinitiation complexes, leading to altered gene expression, cell cycle progression, and survival of tumor cells. Molecular and Cellular Biology, 34, 3675–3688.
Nilson, K. A., Guo, J., Turek, M. E., et al. (2015). THZ1 reveals roles for Cdk7 in co-transcriptional capping and pausing. Molecular Cell, 59, 576–587.
Sen, T., Gay, C. M., & Byers, L. A. (2018). Targeting DNA damage repair in small cell lung cancer and the biomarker landscape. Translational Lung Cancer Research., 7, 50–68.
Zhang, Y., & Hunter, T. (2014). Roles of Chk1 in cell biology and cancer therapy. International Journal of Cancer, 134, 1013–1023.
Höglund, A., Nilsson, L. M., Muralidharan, S. V., et al. (2011). Therapeutic implications for the induced levels of Chk1 in Myc-expressing cancer cells. Clinical Cancer Research, 17, 7067–7079.
Sen, T., Tong, P., Stewart, C. A., et al. (2017). CHK1 inhibition in small-cell lung cancer produces single-agent activity in biomarker-defined disease subsets and combination activity with cisplatin or olaparib. Cancer Research, 77, 3870–3884.
Dauch, D., Rudalska, R., Cossa, G., et al. (2016). A MYC-aurora kinase A protein complex represents an actionable drug target in p53-altered liver cancer. Nature Medicine, 22, 744–753.
Jiang, J., Wang, J., Yue, M., et al. (2020). Direct phosphorylation and stabilization of MYC by aurora B kinase promote T-cell leukemogenesis. Cancer Cell, 37, 200-215.e205.
Owonikoko, T. K., Niu, H., Nackaerts, K., et al. (2020). Randomized phase II study of paclitaxel plus alisertib versus paclitaxel plus placebo as second-line therapy for SCLC: Primary and correlative biomarker analyses. Journal of Thoracic Oncology, 15, 274–287.
Gay, C. M., Tong, P., Cardnell, R. J., et al. (2019). Differential sensitivity analysis for resistant malignancies (DISARM) identifies common candidate therapies across platinum-resistant cancers. Clinical Cancer Research, 25, 346–357.
Mollaoglu, G., Guthrie, M. R., Böhm, S., et al. (2017). MYC drives progression of small cell lung cancer to a variant neuroendocrine subtype with vulnerability to aurora kinase inhibition. Cancer Cell, 31, 270–285.
Matheson, C. J., Backos, D. S., & Reigan, P. (2016). Targeting WEE1 kinase in cancer. Trends in Pharmacological Sciences, 37, 872–881.
Corella, A. N., Cabiliza Ordonio, M. V. A., Coleman, I., et al. (2020). Identification of therapeutic vulnerabilities in small-cell neuroendocrine prostate cancer. Clinical Cancer Research, 26, 1667–1677.
Sen, T., Tong, P., Diao, L., et al. (2017). Targeting AXL and mTOR pathway overcomes primary and acquired resistance to WEE1 inhibition in small-cell lung cancer. Clinical Cancer Research, 23, 6239–6253.
Taniguchi, H., Caeser, R., Chavan, S. S., et al. (2022). WEE1 inhibition enhances the antitumor immune response to PD-L1 blockade by the concomitant activation of STING and STAT1 pathways in SCLC. Cell Reports, 39, 110814.
Park, S., Shim, J., Mortimer, P. G. S., et al. (2020). Biomarker-driven phase 2 umbrella trial study for patients with recurrent small cell lung cancer failing platinum-based chemotherapy. Cancer, 126, 4002–4012.
Leijen, S., van Geel, R. M., Sonke, G. S., et al. (2016). Phase II study of WEE1 inhibitor AZD1775 plus carboplatin in patients with TP53-mutated ovarian cancer refractory or resistant to first-line therapy within 3 months. Journal of Clinical Oncology, 34, 4354–4361.
Seligmann, J. F., Fisher, D. J., Brown, L. C., et al. (2021). Inhibition of WEE1 is effective in TP53- and RAS-mutant metastatic colorectal cancer: A randomized trial (FOCUS4-C) comparing adavosertib (AZD1775) with active monitoring. Journal of Clinical Oncology, 39, 3705–3715.
Garcia, T. B., Uluisik, R. C., van Linden, A. A., et al. (2020). Increased HDAC activity and c-MYC expression mediate acquired resistance to WEE1 inhibition in acute leukemia. Frontiers in Oncology, 10, 296.
Stine, Z. E., Walton, Z. E., Altman, B. J., Hsieh, A. L., & Dang, C. V. (2015). MYC, metabolism, and cancer. Cancer Discovery, 5, 1024–1039.
Chalishazar, M. D., Wait, S. J., Huang, F., et al. (2019). MYC-driven small-cell lung cancer is metabolically distinct and vulnerable to arginine depletion. Clinical Cancer Research, 25, 5107–5121.
Pearl, L. H., Schierz, A. C., Ward, S. E., Al-Lazikani, B., & Pearl, F. M. (2015). Therapeutic opportunities within the DNA damage response. Nature Reviews Cancer, 15, 166–180.
Groelly, F. J., Fawkes, M., Dagg, R. A., Blackford, A. N., & Tarsounas, M. (2023). Targeting DNA damage response pathways in cancer. Nature Reviews Cancer, 23, 78–94.
Pommier, Y., O’Connor, M. J., & Bono, J. D. (2016). Laying a trap to kill cancer cells: PARP inhibitors and their mechanisms of action. Science Translational Medicine., 8, 362ps317-362ps317.
Chedgy, E. C., Vandekerkhove, G., Herberts, C., et al. (2018). Biallelic tumour suppressor loss and DNA repair defects in de novo small-cell prostate carcinoma. The Journal of Pathology, 246, 244–253.
Byers, L. A., Wang, J., Nilsson, M. B., et al. (2012). Proteomic profiling identifies dysregulated pathways in small cell lung cancer and novel therapeutic targets including PARP1. Cancer Discovery, 2, 798–811.
Owonikoko, T. K., Dahlberg, S. E., Sica, G. L., et al. (2019). Randomized phase II trial of cisplatin and etoposide in combination with veliparib or placebo for extensive-stage small-cell lung cancer: ECOG-ACRIN 2511 study. Journal of Clinical Oncology, 37, 222–229.
Lallo, A., Frese, K. K., Morrow, C. J., et al. (2018). The combination of the PARP inhibitor olaparib and the WEE1 inhibitor AZD1775 as a new therapeutic option for small cell lung cancer. Clinical Cancer Research, 24, 5153–5164.
Cleary, J. M., Aguirre, A. J., Shapiro, G. I., & D’Andrea, A. D. (2020). Biomarker-guided development of DNA repair inhibitors. Molecular Cell, 78, 1070–1085.
Blackford, A. N., & Jackson, S. P. (2017). ATM, ATR, and DNA-PK: The trinity at the heart of the DNA damage response. Molecular Cell, 66, 801–817.
Thomas, A., Takahashi, N., Rajapakse, V. N., et al. (2021). Therapeutic targeting of ATR yields durable regressions in small cell lung cancers with high replication stress. Cancer Cell, 39, 566-579.e567.
Sennino, B., Ishiguro-Oonuma, T., Wei, Y., et al. (2012). Suppression of tumor invasion and metastasis by concurrent inhibition of c-Met and VEGF signaling in pancreatic neuroendocrine tumors. Cancer Discovery, 2, 270–287.
Raymond, E., Dahan, L., Raoul, J. L., et al. (2011). Sunitinib malate for the treatment of pancreatic neuroendocrine tumors. New England Journal of Medicine, 364, 501–513.
Bergsland, E. K., Mahoney, M. R., Asmis, T. R., et al. (2019). Prospective randomized phase II trial of pazopanib versus placebo in patients with progressive carcinoid tumors (CARC) (Alliance A021202). Journal of Clinical Oncology., 37, 4005–4005.
Chan, J. A., Faris, J. E., Murphy, J. E., et al. (2017). Phase II trial of cabozantinib in patients with carcinoid and pancreatic neuroendocrine tumors (pNET). Journal of Clinical Oncology., 35, 228–228.
Capdevila, J., Fazio, N., Lopez, C. L., et al. (2019). Final results of the TALENT trial (GETNE1509): A prospective multicohort phase II study of lenvatinib in patients (pts) with G1/G2 advanced pancreatic (panNETs) and gastrointestinal (giNETs) neuroendocrine tumors (NETs). Journal of Clinical Oncology., 37, 4106–4106.
Xu, J., Shen, L., Bai, C., et al. (2020). Surufatinib in advanced pancreatic neuroendocrine tumours (SANET-p): A randomised, double-blind, placebo-controlled, phase 3 study. The lancet Oncology, 21, 1489–1499.
Xu, J., Shen, L., Zhou, Z., et al. (2020). Surufatinib in advanced extrapancreatic neuroendocrine tumours (SANET-ep): A randomised, double-blind, placebo-controlled, phase 3 study. The lancet Oncology, 21, 1500–1512.
Rodríguez-Remírez, M., Del Puerto-Nevado, L., Fernández Aceñero, M. J., et al. (2020). Strong antitumor activity of bevacizumab and aflibercept in neuroendocrine carcinomas: In-depth preclinical study. Neuroendocrinology, 110, 50–62.
Mishima, S., Kawazoe, A., Matsumoto, H., et al. (2018). Efficacy and safety of ramucirumab-containing chemotherapy in patients with pretreated metastatic gastric neuroendocrine carcinoma. ESMO open., 3, e000443.
Walter, T., Lievre, A., Coriat, R., et al. (2023). Bevacizumab plus FOLFIRI after failure of platinum-etoposide first-line chemotherapy in patients with advanced neuroendocrine carcinoma (PRODIGE 41-BEVANEC): A randomised, multicentre, non-comparative, open-label, phase 2 trial. The Lancet Oncology, 24, 297–306.
Alifieris, C. E., Griniatsos, J., Delis, S. G., et al. (2020). Capecitabine, oxaliplatin, irinotecan, and bevacizumab combination followed by pazopanib plus capecitabine maintenance for high-grade gastrointestinal neuroendocrine carcinomas. American Journal of Clinical Oncology, 43, 305–310.
Pellat, A., Dreyer, C., Couffignal, C., et al. (2018). Clinical and biomarker evaluations of sunitinib in patients with grade 3 digestive neuroendocrine neoplasms. Neuroendocrinology, 107, 24–31.
Ahn, H. K., Choi, J. Y., Kim, K. M., et al. (2013). Phase II study of pazopanib monotherapy in metastatic gastroenteropancreatic neuroendocrine tumours. British Journal of Cancer, 109, 1414–1419.
Rudin, C. M., Pietanza, M. C., Bauer, T. M., et al. (2017). Rovalpituzumab tesirine, a DLL3-targeted antibody-drug conjugate, in recurrent small-cell lung cancer: A first-in-human, first-in-class, open-label, phase 1 study. The lancet Oncology, 18, 42–51.
Hermans, B. C. M., Derks, J. L., Thunnissen, E., et al. (2019). DLL3 expression in large cell neuroendocrine carcinoma (LCNEC) and association with molecular subtypes and neuroendocrine profile. Lung Cancer, 138, 102–108.
Saunders, L. R., Bankovich, A. J., Anderson, W. C., et al. (2015). A DLL3-targeted antibody-drug conjugate eradicates high-grade pulmonary neuroendocrine tumor-initiating cells in vivo. Science Translational Medicine., 7, 302136.
Liverani, C., Bongiovanni, A., Mercatali, L., et al. (2021). Diagnostic and predictive role of DLL3 expression in gastroenteropancreatic neuroendocrine neoplasms. Endocrine Pathology, 32, 309–317.
Johnson, M. L., Zvirbule, Z., Laktionov, K., et al. (2021). Rovalpituzumab tesirine as a maintenance therapy after first-line platinum-based chemotherapy in patients with extensive-stage-SCLC: Results from the phase 3 MERU study. Journal of Thoracic Oncology, 16, 1570–1581.
Blackhall, F., Jao, K., Greillier, L., et al. (2021). Efficacy and safety of rovalpituzumab tesirine compared with topotecan as second-line therapy in DLL3-high SCLC: Results from the phase 3 TAHOE study. Journal of Thoracic Oncology, 16, 1547–1558.
Mansfield, A. S., Hong, D. S., Hann, C. L., et al. (2021). A phase I/II study of rovalpituzumab tesirine in delta-like 3-expressing advanced solid tumors. NPJ Precision Oncology., 5, 74.
Morgensztern, D., Johnson, M., Rudin, C. M., et al. (2020). SC-002 in patients with relapsed or refractory small cell lung cancer and large cell neuroendocrine carcinoma: Phase 1 study. Lung Cancer, 145, 126–131.
Giffin, M. J., Cooke, K., Lobenhofer, E. K., et al. (2021). AMG 757, a half-life extended, DLL3-targeted bispecific T-cell engager, shows high potency and sensitivity in preclinical models of small-cell lung cancer. Clinical Cancer Research, 27, 1526–1537.
Owonikoko, T. K., Champiat, S., Johnson, M. L., et al. (2021). Updated results from a phase 1 study of AMG 757, a half-life extended bispecific T-cell engager (BiTE) immuno-oncology therapy against delta-like ligand 3 (DLL3), in small cell lung cancer (SCLC). Journal of Clinical Oncology., 39, 8510–8510.
Hipp, S., Voynov, V., Drobits-Handl, B., et al. (2020). A bispecific DLL3/CD3 IgG-like T-cell engaging antibody induces antitumor responses in small cell lung cancer. Clinical Cancer Research, 26, 5258–5268.
Johnson, M. L., Dy, G. K., Mamdani, H., et al. (2022). Interim results of an ongoing phase 1/2a study of HPN328, a tri-specific, half-life extended, DLL3-targeting, T-cell engager, in patients with small cell lung cancer and other neuroendocrine cancers. Journal of Clinical Oncology., 40, 8566–8566.
Chen, X., Amar, N., Zhu, Y., et al. (2020). Combined DLL3-targeted bispecific antibody with PD-1 inhibition is efficient to suppress small cell lung cancer growth. Journal for Immunotherapy of Cancer, 8, e000785.
Byers, L., Heymach, J., Gibbons, D., et al. (2022). 697 A phase 1 study of AMG 119, a DLL3-targeting, chimeric antigen receptor (CAR) T cell therapy, in relapsed/refractory small cell lung cancer (SCLC). Journal for Immunotherapy of Cancer, 10, A728–A728.
Ellis, L., Atadja, P. W., & Johnstone, R. W. (2009). Epigenetics in cancer: Targeting chromatin modifications. Molecular Cancer Therapeutics, 8, 1409–1420.
Pasini, D., & Di Croce, L. (2016). Emerging roles for Polycomb proteins in cancer. Current Opinion in Genetics & Development, 36, 50–58.
Gardner, E. E., Lok, B. H., Schneeberger, V. E., et al. (2017). Chemosensitive relapse in small cell lung cancer proceeds through an EZH2-SLFN11 axis. Cancer Cell, 31, 286–299.
Schweizer, M., Penkov, K. D., Tolcher, A. W., et al. (2022). 488P phase I trial of PF-06821497, a potent and selective inhibitor of enhancer of zeste homolog 2 (EZH2), in follicular lymphoma (FL), small cell lung cancer (SCLC) and castration-resistant prostate cancer (CRPC). Annals of Oncology., 33, S763–S764.
Donati, B., Lorenzini, E., & Ciarrocchi, A. (2018). BRD4 and cancer: Going beyond transcriptional regulation. Molecular Cancer, 17, 164.
Puissant, A., Frumm, S. M., Alexe, G., et al. (2013). Targeting MYCN in neuroblastoma by BET bromodomain inhibition. Cancer Discovery, 3, 308–323.
Jahchan, N. S., Lim, J. S., Bola, B., et al. (2016). Identification and targeting of long-term tumor-propagating cells in small cell lung cancer. Cell Reports, 16, 644–656.
Lenhart, R., Kirov, S., Desilva, H., et al. (2015). Sensitivity of small cell lung cancer to BET inhibition is mediated by regulation of ASCL1 gene expression. Molecular Cancer Therapeutics, 14, 2167–2174.
Balasubramaniam, S., Redon, C. E., Peer, C. J., et al. (2018). Phase I trial of belinostat with cisplatin and etoposide in advanced solid tumors, with a focus on neuroendocrine and small cell cancers of the lung. Anti-Cancer Drugs, 29, 457–465.
Modlin, I. M., Pavel, M., Kidd, M., & Gustafsson, B. I. (2010). Review article: Somatostatin analogues in the treatment of gastroenteropancreatic neuroendocrine (carcinoid) tumours. Alimentary Pharmacology & Therapeutics, 31, 169–188.
Rinke, A., Müller, H. H., Schade-Brittinger, C., et al. (2009). Placebo-controlled, double-blind, prospective, randomized study on the effect of octreotide LAR in the control of tumor growth in patients with metastatic neuroendocrine midgut tumors: A report from the PROMID Study Group. Journal of Clinical Oncology, 27, 4656–4663.
Kvols, L. K., Moertel, C. G., O’Connell, M. J., Schutt, A. J., Rubin, J., & Hahn, R. G. (1986). Treatment of the malignant carcinoid syndrome. Evaluation of a long-acting somatostatin analogue. The New England Journal of Medicine., 315, 663–666.
Caplin, M. E., Pavel, M., Ćwikła, J. B., et al. (2014). Lanreotide in metastatic enteropancreatic neuroendocrine tumors. New England Journal of Medicine, 371, 224–233.
Villard, L., Romer, A., Marincek, N., et al. (2012). Cohort study of somatostatin-based radiopeptide therapy with [(90)Y-DOTA]-TOC versus [(90)Y-DOTA]-TOC plus [(177)Lu-DOTA]-TOC in neuroendocrine cancers. Journal of Clinical Oncology, 30, 1100–1106.
Strosberg, J., El-Haddad, G., Wolin, E., et al. (2017). Phase 3 trial of (177)Lu-dotatate for midgut neuroendocrine tumors. New England Journal of Medicine, 376, 125–135.
Carlsen, E. A., Fazio, N., Granberg, D., et al. (2019). Peptide receptor radionuclide therapy in gastroenteropancreatic NEN G3: A multicenter cohort study. Endocrine-Related Cancer, 26, 227–239.
Sorbye, H., Kong, G., & Grozinsky-Glasberg, S. (2020). PRRT in high-grade gastroenteropancreatic neuroendocrine neoplasms (WHO G3). Endocrine-Related Cancer, 27, R67-r77.
Whalen, K. A., White, B. H., Quinn, J. M., et al. (2019). Targeting the somatostatin receptor 2 with the miniaturized drug conjugate, PEN-221: A potent and novel therapeutic for the treatment of small cell lung cancer. Molecular Cancer Therapeutics, 18, 1926–1936.
Hill, R., Cautain, B., de Pedro, N., & Link, W. (2014). Targeting nucleocytoplasmic transport in cancer therapy. Oncotarget, 5, 11–28.
Benkova, K., Mihalyova, J., Hajek, R., & Jelinek, T. (2021). Selinexor, selective inhibitor of nuclear export: Unselective bullet for blood cancers. Blood Reviews, 46, 100758.
Quintanal-Villalonga, A., Taniguchi, H., Hao, Y., et al. (2022). Inhibition of XPO1 sensitizes small cell lung cancer to first- and second-line chemotherapy. Cancer Research, 82, 472–483.
Kashyap, T., Argueta, C., Unger, T., et al. (2018). Selinexor reduces the expression of DNA damage repair proteins and sensitizes cancer cells to DNA damaging agents. Oncotarget, 9, 30773–30786.
Kaloni, D., Diepstraten, S. T., Strasser, A., & Kelly, G. L. (2023). BCL-2 protein family: attractive targets for cancer therapy. Apoptosis, 28, 20–38.
Lissa, D., Takahashi, N., Desai, P., et al. (2022). Heterogeneity of neuroendocrine transcriptional states in metastatic small cell lung cancers and patient-derived models. Nature Communications, 13, 2023–2023.
Lam, L. T., Lin, X., Faivre, E. J., et al. (2017). Vulnerability of small-cell lung cancer to apoptosis induced by the combination of BET bromodomain proteins and BCL2 inhibitors. Molecular Cancer Therapeutics, 16, 1511–1520.
Santamaría Nuñez, G., Robles, C. M., Giraudon, C., et al. (2016). Lurbinectedin specifically triggers the degradation of phosphorylated RNA polymerase II and the formation of DNA breaks in cancer cells. Molecular Cancer Therapeutics, 15, 2399–2412.
Costanzo, F., Martínez Diez, M., Santamaría Nuñez, G., et al. (2022). Promoters of ASCL1- and NEUROD1-dependent genes are specific targets of lurbinectedin in SCLC cells. EMBO Molecular Medicine, 14, e14841.
Trigo, J., Subbiah, V., Besse, B., et al. (2020). Lurbinectedin as second-line treatment for patients with small-cell lung cancer: A single-arm, open-label, phase 2 basket trial. The lancet Oncology, 21, 645–654.
Longo-Muñoz, F., Castellano, D., Alexandre, J., et al. (2022). Lurbinectedin in patients with pretreated neuroendocrine tumours: Results from a phase II basket study. European Journal of Cancer, 172, 340–348.
Schultz, C. W., Zhang, Y., Fu, H., et al. (2022). Abstract 2153: ATR inhibition augments the efficacy of the lurbinectedin in small cell lung cancer. Cancer Research, 82, 2153–2153.
Wan, J. C. M., Massie, C., Garcia-Corbacho, J., et al. (2017). Liquid biopsies come of age: Towards implementation of circulating tumour DNA. Nature Reviews Cancer, 17, 223–238.
Sorbye, H., Knappskog, S., Grob, T., et al. (2022). 890MO Mutation spectrum in liquid versus solid biopsies from advanced digestive neuroendocrine carcinoma patients. Annals of Oncology., 33, S955.
Zakka, K., Nagy, R., Drusbosky, L., et al. (2020). Blood-based next-generation sequencing analysis of neuroendocrine neoplasms. Oncotarget, 11, 1749–1757.
Gerard, L., Garcia, J., Gauthier, A., et al. (2021). ctDNA in neuroendocrine carcinoma of gastroenteropancreatic origin or of unknown primary: The CIRCAN-NEC pilot study. Neuroendocrinology, 111, 951–964.
Chen, D. S., & Mellman, I. (2013). Oncology meets immunology: The cancer-immunity cycle. Immunity, 39, 1–10.
Ooki, A., Shinozaki, E., & Yamaguchi, K. (2021). Immunotherapy in colorectal cancer: Current and future strategies. J Anus Rectum Colon., 5, 11–24.
The National Comprehensive Cancer Network (2023) NCCN clinical practice guidelines in oncology, small cell lung cancer. https://www.nccn.org/guidelines/guidelines-detail?category=1&id=1462. 2023;version 2. Accessed 1 Apr 2023.
Ready, N. E., Ott, P. A., Hellmann, M. D., et al. (2020). Nivolumab monotherapy and nivolumab plus ipilimumab in recurrent small cell lung cancer: Results from the CheckMate 032 randomized cohort. Journal of Thoracic Oncology, 15, 426–435.
Chung, H. C., Piha-Paul, S. A., Lopez-Martin, J., et al. (2020). Pembrolizumab after two or more lines of previous therapy in patients with recurrent or metastatic SCLC: Results from the KEYNOTE-028 and KEYNOTE-158 studies. Journal of Thoracic Oncology, 15, 618–627.
Hamilton, G., & Rath, B. (2019). Immunotherapy for small cell lung cancer: Mechanisms of resistance. Expert Opinion on Biological Therapy, 19, 423–432.
Girard, N., Mazieres, J., Otto, J., et al. (2021). LBA41 Nivolumab (nivo) & #xb1; ipilimumab (ipi) in pre-treated patients with advanced, refractory pulmonary or gastroenteropancreatic poorly differentiated neuroendocrine tumors (NECs) (GCO-001 NIPINEC). Annals of Oncology., 32, S1318.
Vijayvergia, N., Dasari, A., Deng, M., et al. (2020). Pembrolizumab monotherapy in patients with previously treated metastatic high-grade neuroendocrine neoplasms: Joint analysis of two prospective, non-randomised trials. British Journal of Cancer, 122, 1309–1314.
Chan, D. L., Rodriguez-Freixinos, V., Doherty, M., et al. (2022). Avelumab in unresectable/metastatic, progressive, grade 2–3 neuroendocrine neoplasms (NENs): Combined results from NET-001 and NET-002 trials. European Journal of Cancer, 169, 74–81.
Mulvey, C., Raj, N. P., Chan, J. A., et al. (2019). Phase II study of pembrolizumab-based therapy in previously treated extrapulmonary poorly differentiated neuroendocrine carcinomas: Results of part A (pembrolizumab alone). Journal of Clinical Oncology., 37, 363–363.
Yao, J. C., Strosberg, J., Fazio, N., et al. (2021). Spartalizumab in metastatic, well/poorly-differentiated neuroendocrine neoplasms. Endocrine-Related Cancer, 28, 161–172.
Fottner, C., Apostolidis, L., Ferrata, M., et al. (2019). A phase II, open label, multicenter trial of avelumab in patients with advanced, metastatic high-grade neuroendocrine carcinomas NEC G3 (WHO 2010) progressive after first-line chemotherapy (AVENEC). Journal of Clinical Oncology., 37, 4103–4103.
Lu, M., Zhang, P., Zhang, Y., et al. (2020). Efficacy, safety, and biomarkers of toripalimab in patients with recurrent or metastatic neuroendocrine neoplasms: A multiple-center phase Ib trial. Clinical Cancer Research, 26, 2337–2345.
Ferrata, M., Schad, A., Zimmer, S., et al. (2019). PD-L1 expression and immune cell infiltration in gastroenteropancreatic (GEP) and non-GEP neuroendocrine neoplasms with high proliferative activity. Frontiers in Oncology, 9, 343.
Milione, M., Miceli, R., Barretta, F., et al. (2019). Microenvironment and tumor inflammatory features improve prognostic prediction in gastro-entero-pancreatic neuroendocrine neoplasms. J Pathol Clin Res., 5, 217–226.
Capdevila, J., Landolfi, S., Hernando, J., et al. (2021). 1107P Durvalumab plus tremelimumab in patients with grade 3 neuroendocrine neoplasms of gastroenteropancreatic origin: Updated results from the multicenter phase II DUNE trial (GETNE 1601). Annals of Oncology., 32, S914–S915.
Takahashi, D., Kojima, M., Suzuki, T., et al. (2018). Profiling the tumour immune microenvironment in pancreatic neuroendocrine neoplasms with multispectral imaging indicates distinct subpopulation characteristics concordant with WHO 2017 classification. Science and Reports, 8, 13166.
Roberts, J. A., Gonzalez, R. S., Das, S., Berlin, J., & Shi, C. (2017). Expression of PD-1 and PD-L1 in poorly differentiated neuroendocrine carcinomas of the digestive system: A potential target for anti-PD-1/PD-L1 therapy. Human Pathology, 70, 49–54.
Park, E. J., Park, H. J., Kim, K. W., et al. (2022). Efficacy of immune checkpoint inhibitors against advanced or metastatic neuroendocrine neoplasms: A systematic review and meta-analysis. Cancers (Basel), 14, 794.
Le, D. T., Uram, J. N., Wang, H., et al. (2015). PD-1 blockade in tumors with mismatch-repair deficiency. New England Journal of Medicine, 372, 2509–2520.
Marabelle, A., Fakih, M., Lopez, J., et al. (2020). Association of tumour mutational burden with outcomes in patients with advanced solid tumours treated with pembrolizumab: Prospective biomarker analysis of the multicohort, open-label, phase 2 KEYNOTE-158 study. The lancet Oncology, 21, 1353–1365.
Chalmers, Z. R., Connelly, C. F., Fabrizio, D., et al. (2017). Analysis of 100,000 human cancer genomes reveals the landscape of tumor mutational burden. Genome Medicine., 9, 34.
Lo, Y. H., Kolahi, K. S., Du, Y., et al. (2021). A CRISPR/Cas9-engineered ARID1A-deficient human gastric cancer organoid model reveals essential and nonessential modes of oncogenic transformation. Cancer Discovery, 11, 1562–1581.
Shen, J., Ju, Z., Zhao, W., et al. (2018). ARID1A deficiency promotes mutability and potentiates therapeutic antitumor immunity unleashed by immune checkpoint blockade. Nature Medicine, 24, 556–562.
Zappasodi, R., Merghoub, T., & Wolchok, J. D. (2018). Emerging concepts for immune checkpoint blockade-based combination therapies. Cancer Cell, 33, 581–598.
Goldman, J. W., Dvorkin, M., Chen, Y., et al. (2021). Durvalumab, with or without tremelimumab, plus platinum-etoposide versus platinum-etoposide alone in first-line treatment of extensive-stage small-cell lung cancer (CASPIAN): Updated results from a randomised, controlled, open-label, phase 3 trial. The lancet Oncology, 22, 51–65.
Hellmann, M. D., Callahan, M. K., Awad, M. M., et al. (2018). Tumor mutational burden and efficacy of nivolumab monotherapy and in combination with ipilimumab in small-cell lung cancer. Cancer Cell, 33, 853-861.e854.
Patel, S. P., Othus, M., Chae, Y. K., et al. (2020). A phase II basket trial of dual anti-CTLA-4 and anti-PD-1 blockade in rare tumors (DART SWOG 1609) in patients with nonpancreatic neuroendocrine tumors. Clinical Cancer Research, 26, 2290–2296.
Patel, S. P., Mayerson, E., Chae, Y. K., et al. (2021). A phase II basket trial of dual anti-CTLA-4 and anti-PD-1 blockade in rare tumors (DART) SWOG S1609: High-grade neuroendocrine neoplasm cohort. Cancer, 127, 3194–3201.
Klein, O., Kee, D., Markman, B., et al. (2020). Immunotherapy of ipilimumab and nivolumab in patients with advanced neuroendocrine tumors: A subgroup analysis of the CA209-538 clinical trial for rare cancers. Clinical Cancer Research, 26, 4454–4459.
Anderson, A. C., Joller, N., & Kuchroo, V. K. (2016). Lag-3, Tim-3, and TIGIT: Co-inhibitory receptors with specialized functions in immune regulation. Immunity, 44, 989–1004.
Yao, J. C., Strosberg, J., Fazio, N., et al. (2018). Activity & safety of spartalizumab (PDR001) in patients (pts) with advanced neuroendocrine tumors (NET) of pancreatic (Pan), gastrointestinal (GI), or thoracic (T) origin, & gastroenteropancreatic neuroendocrine carcinoma (GEP NEC) who have progressed on prior treatment (Tx). Annals of Oncology., 29, viii467–viii468.
Owen, D. H., Benner, B., Wei, L., et al. (2023). A phase 2 clinical trial of nivolumab and temozolomide for neuroendocrine neoplasms. Clinical Cancer Research, 29, 731–741.
Johnston, R. J., Comps-Agrar, L., Hackney, J., et al. (2014). The immunoreceptor TIGIT regulates antitumor and antiviral CD8(+) T cell effector function. Cancer Cell, 26, 923–937.
Rudin, C. M., Liu, S. V., Lu, S., et al. (2022). SKYSCRAPER-02: primary results of a phase III, randomized, double-blind, placebo-controlled study of atezolizumab (atezo) + carboplatin + etoposide (CE) with or without tiragolumab (tira) in patients (pts) with untreated extensive-stage small cell lung cancer (ES-SCLC). Journal of Clinical Oncology., 40, LBA8507–LBA8507.
Galluzzi, L., Buqué, A., Kepp, O., Zitvogel, L., & Kroemer, G. (2015). Immunological effects of conventional chemotherapy and targeted anticancer agents. Cancer Cell, 28, 690–714.
Riesco Martinez, M. C., Capdevila Castillon, J., Alonso, V., et al. (2022). 496MO Final overall survival results from the NICE-NEC trial (GETNE-T1913): A phase II study of nivolumab and platinum-doublet chemotherapy (CT) in untreated advanced G3 neuroendocrine neoplasms (NENs) of gastroenteropancreatic (GEP) or unknown (UK) origin. Annals of Oncology., 33, S769.
Chan, J. A., Raj, N. P., Aggarwal, R. R., et al. (2021). Phase II study of pembrolizumab-based therapy in previously treated extrapulmonary poorly differentiated neuroendocrine carcinomas: Results of part B (pembrolizumab + chemotherapy). Journal of Clinical Oncology., 39, 4148–4148.
Schmidt, E. V., Chisamore, M. J., Chaney, M. F., et al. (2020). Assessment of clinical activity of PD-1 checkpoint inhibitor combination therapies reported in clinical trials. JAMA Network Open, 3, e1920833.
Cao, Y., Lu, M., Sun, Y., et al. (2023). Surufatinib plus toripalimab in patients with advanced solid tumors: a single-arm, open-label, phase 1 trial. Journal of Cancer Research and Clinical Oncology, 149, 779–789.
Shen, L., Yu, X., Lu, M., et al. (2021). Surufatinib in combination with toripalimab in patients with advanced neuroendocrine carcinoma: Results from a multicenter, open-label, single-arm, phase II trial. Journal of Clinical Oncology., 39, e16199–e16199.
Maio, M., Coral, S., Fratta, E., Altomonte, M., & Sigalotti, L. (2003). Epigenetic targets for immune intervention in human malignancies. Oncogene, 22, 6484–6488.
Shen, L., & Pili, R. (2012). Class I histone deacetylase inhibition is a novel mechanism to target regulatory T cells in immunotherapy. Oncoimmunology., 1, 948–950.
Orillion, A., Hashimoto, A., Damayanti, N., et al. (2017). Entinostat neutralizes myeloid-derived suppressor cells and enhances the antitumor effect of PD-1 inhibition in murine models of lung and renal cell carcinoma. Clinical Cancer Research, 23, 5187–5201.
Woods, D. M., Sodré, A. L., Villagra, A., Sarnaik, A., Sotomayor, E. M., & Weber, J. (2015). HDAC inhibition upregulates PD-1 ligands in melanoma and augments immunotherapy with PD-1 blockade. Cancer Immunology Research, 3, 1375–1385.
Gray, J. E., Saltos, A., Tanvetyanon, T., et al. (2019). Phase I/Ib study of pembrolizumab plus vorinostat in advanced/metastatic non-small cell lung cancer. Clinical Cancer Research, 25, 6623–6632.
Rodriguez, C. P., Wu, Q. V., Voutsinas, J., et al. (2020). A phase II trial of pembrolizumab and vorinostat in recurrent metastatic head and neck squamous cell carcinomas and salivary gland cancer. Clinical Cancer Research, 26, 837–845.
Mouw, K. W., Goldberg, M. S., Konstantinopoulos, P. A., & D’Andrea, A. D. (2017). DNA damage and repair biomarkers of immunotherapy response. Cancer Discovery, 7, 675–693.
Sen, T., Rodriguez, B. L., Chen, L., et al. (2019). Targeting DNA damage response promotes antitumor immunity through STING-mediated T-cell activation in small cell lung cancer. Cancer Discovery, 9, 646–661.
Jiao, S., Xia, W., Yamaguchi, H., et al. (2017). PARP inhibitor upregulates PD-L1 expression and enhances cancer-associated immunosuppression. Clinical Cancer Research, 23, 3711–3720.
Zhang, H., Christensen, C. L., Dries, R., et al. (2020). CDK7 inhibition potentiates genome instability triggering anti-tumor immunity in small cell lung cancer. Cancer Cell, 37, 37-54.e39.
Author information
Authors and Affiliations
Contributions
A.O. drew/developed the conceptual framework, searched the literature, and wrote the manuscript. H.O., K.F., and K.Y. revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
N/A.
Consent for publication
N/A.
Conflict of interest
AO received speaker honoraria from Bristol-Myers Squibb, Ono Pharmaceutical, Daiichi Sankyo, and Taiho Pharmaceutical Co. KY received speaker honoraria from Chugai Pharmaceutical Co. Ltd., Bristol-Myers Squibb, Merck Serono, Taiho Pharmaceutical Co., Takeda, and Eli Lilly; a consultant fee from Takeda Pharmaceutical Co. Ltd.; honoraria from Tsumura Co. Ltd., Nihon Kayaku Co. Ltd., and Chugai Pharmaceutical Co. Ltd; research grants from Sumitomo Dainippon Pharma, Gilead Sciences, MSD, Boehringer Ingelheim, Daiichi Sankyo, and Chugai Pharmaceutical Co. Ltd; and speaker honoraria, research grants, and scholarship grants from Ono Pharmaceutical, Yakult Honsha Co., Ltd., and Sanofi.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ooki, A., Osumi, H., Fukuda, K. et al. Potent molecular-targeted therapies for gastro-entero-pancreatic neuroendocrine carcinoma. Cancer Metastasis Rev 42, 1021–1054 (2023). https://doi.org/10.1007/s10555-023-10121-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10555-023-10121-2