Abstract
Heart failure (HF) is characterized by molecular and cellular defects which jointly contribute to decreased cardiac pump function. During the development of the initial cardiac damage which leads to HF, adaptive responses activate physiological countermeasures to overcome depressed cardiac function and to maintain blood supply to vital organs in demand of nutrients. However, during the chronic course of most HF syndromes, these compensatory mechanisms are sustained beyond months and contribute to progressive maladaptive remodeling of the heart which is associated with a worse outcome. Of pathophysiological significance are mechanisms which directly control cardiac contractile function including ion- and receptor-mediated intracellular signaling pathways. Importantly, signaling cascades of stress adaptation such as intracellular calcium (Ca2+) and 3′-5′-cyclic adenosine monophosphate (cAMP) become dysregulated in HF directly contributing to adverse cardiac remodeling and depression of systolic and diastolic function. Here, we provide an update about Ca2+ and cAMP dependent signaling changes in HF, how these changes affect cardiac function, and novel therapeutic strategies which directly address the signaling defects.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Congestive heart failure (HF) is a condition in which heart function is insufficient to supply the organs with enough blood nutrients. The consequence is a progressive cascade of changes that lead to fatigue, shortness of breath and, ultimately, death. Much progress has been made in understanding the molecular and cellular processes that contribute to HF. Despite these insights and modern treatment options, chronic HF remains a major cause of illness and death and generally has a poor prognosis. Because HF is more common with increasing age, the number of affected individuals is rising rapidly with the ageing population. Thus, new treatments directed at critical disease mechanisms are needed to halt and reverse the devastating consequences of this disease.
Here, we focus on chronic HF and our understanding of molecular disease mechanisms related to Ca2+ metabolism. Many insights into HF stem from the elucidation of intracellular signaling pathways that mediate cardiac performance as well as contribute to cardiac dysregulation under disease conditions. The clinically critical transition occurs when the heart can no longer provide adequate blood flow and/or pressure to meet the body’s demands. Consequently, physiological countermeasures include the stimulation of neurohormonal outflow and the activation of intracellular signaling cascades. These acute responses may initially offset reduced cardiac performance. However, sustained stimulation of the heart by cellular stress signaling cascades ultimately increases the likelihood of organ failure and contributes to a worse prognosis.
Cardiac remodeling and changes in intracellular signaling
HF is characterized by chronic activation of neuro-hormonal pathways representing a compensatory response to overcome depressed cardiac function. However, over weeks to months, a chronic hyperadrenergic state ensues with elevated plasma catecholamine levels, which contribute to maladaptive cardiac chamber remodeling, progressive deterioration of pump function, and deadly arrhythmias. Due to the chronic hyperadrenergic state, desensitization of β-adrenoreceptors (β-ARs) and reduced global intracellular cAMP synthesis occur in the failing heart [1–3]. However, stimulation of β-ARs and other signaling pathways is maintained and continues to affect the remodeled cells and proteins.
A broad range of molecular pathways are involved in the development of HF, and there is likely to be substantial overlap between these pathways. Typically, cell-surface receptors are activated by ligands leading to the activation of stress-response protein kinases and phosphatases such as cAMP-dependent protein kinase A (PKA), protein kinase C (PKC), protein kinase D (PKD), mitogen activated kinases (MAPKs), Ca2+ calmodulin-dependent kinase II (CaMKII), and calcineurin. Chronic activation of these stress pathways and their cellular effectors including transcription factors, which target multiple genes, result in changes in cellular structure, function, and overall regulation of the heart, collectively referred to as cardiac remodeling. Additionally, an imbalance between cell survival and cell death pathways results in a low rate of cardiomyocyte apoptosis which may contribute to cell loss in HF [4, 5]. A different form of cell death, necrosis, may contribute to HF, for example through mitochondrial damage mediated by increased cytosolic Ca2+ concentrations in cardiomyocytes.
HF causes changes in intracellular calcium signals
HF is a syndrome which results from different insults, typically following myocardial infarction (MI), viral myocarditis, toxic cardiomyopathy, or other less frequent causes such as genetic defects. However, following chronic remodeling of the heart, cardiac phenotypes occurring from different causes show important similarities, including depressed intracellular Ca2+ metabolism.
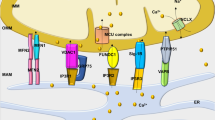
Ca2+ is the central regulator of excitation-contraction (EC) coupling, which controls muscle contraction during each heartbeat. EC coupling is activated by an incoming action potential wavefront and the subsequent opening of voltage-dependent L-type Ca2+ channels (CaV1.2). A relatively small Ca2+ influx current (I Ca) triggers a quantitatively larger intracellular Ca2+ release from sarcoplasmic reticulum (SR) Ca2+ stores through ryanodine receptor (RyR2) Ca2+ release channels by the process of Ca2+ induced Ca2+ release (CICR) (Fig. 1a). CICR is followed by re-uptake of Ca2+ into the SR by Ca2+ pumps (SERCA2) and removal of Ca2+ from the cytosol by the Na+/Ca2+ exchanger (NCX) (Fig. 1a). The activity of SERCA2 is regulated by phospholamban (PLN). Unphosphorylated PLN inhibits SERCA2 activity, and phosphorylation by PKA and/or CaMKII increases SR Ca2+ uptake. Similarly, RyR2 phosphorylation by PKA and/or CaMKII increases SR Ca2+ release [6, 7]. Within the approximately 12 nm wide compartment between the plasma membrane and the terminal SR membrane (junctional SR) where SR Ca2+ release occurs, CICR is organized within Ca2+ release units representing functional microdomains between T-tubuli and the terminal SR (junctional subspace). Strikingly, all components essential for CICR, including the SR Ca2+ release microdomain, the Ca2+ storage organelles, and the Ca2+ transport proteins themselves (Table 1), become significantly altered during remodeling of the failing heart [8].
a Physiology of excitation-contraction (EC) coupling. An incoming action potential (AP) rapidly depolarizes the cell membrane potential (V m) in phase 0 through opening of voltage-dependent Na+ channels (NaV1.5). Subsequently, EC coupling is initiated through the opening of voltage-dependent L-type Ca2+ channels (CaV1.2) and the plasma membrane Ca2+ influx current (I Ca). I Ca activates ryanodine receptors (RyR2s) and intracellular Ca2+ release from sarcoplasmic reticulum (SR) stores, also known as Ca2+ induced Ca2+ release (CICR). CICR is followed by extrusion of Ca2+ from the cytosol into the SR by Ca2+ pumps (SERCA2) and to the extracellular compartment by the Na+/Ca2+ exchanger (NCX) operating in its forward mode (3 Na+ in for each Ca2+ out), which creates an electrogenic inward current. SR Ca2+ leak is inhibited by the calstabin2 (Cab2) subunit which stabilizes the RyR2 closed state. The SERCA2 pump rate is inhibited by the phospholamban (PLN) subunit in its dephosphorylated state. Ca2+ release and uptake occur cyclically during each heart beat and represent 60–90% of Ca2+ signaling during EC coupling depending on the species studied. b EC coupling abnormalities in CPVT. RyR2 missense mutations significantly increase the propensity for intracellular Ca2+ leak in resting cardiomyocytes (during diastole) with filled SR Ca2+ stores. Stimulation of β-adrenergic receptors (β-ARs) during stress adaptation results in RyR2 and PLN phosphorylation by PKA (indicated by ⊗) which increases SR Ca2+ release and uptake, respectively. However, RyR2 mutations (as indicated by green star) in the PKA phosphorylated Ca2+ release channel lead to partial calstabin2 depletion, a significant gain-of-function defect of RyR2, and intracellular Ca2+ leak. RyR2 Ca2+ leak activates depolarizing transient inward currents (I TI) supposedly through abnormal forward mode NCX activity. If I TI currents reach a critical threshold of membrane potential instability in phase 4 of the cardiac AP, Na+ channels are activated leading to delayed after depolarizations (DADs) which underly triggered activity. c EC coupling abnormalities in HF. HF is a chronic hyperadrenergic state which results in downregulation of β-AR signaling and reduced intracellular cAMP synthesis. However, maintained hyperadrenergic stimulation of β-ARs during HF results in chronic RyR2 PKA hyperphosphorylation (indicated by large ⊗), depletion of the stabilizing calstabin2 subunits as well as other components of the channel complex including phosphodiesterase 4D3 (PDE4D3). PDE4D3 depletion causes a chronically reduced cAMP hydrolysis in the channel complex and contributes to RyR2 PKA hyperphosphorylation induced intracellular Ca2+ leak. On the other hand, PLN is chronically PKA hypophosphorylated (indicated by small ⊗) creating constitutively inhibited state of SERCA2 and reduced SR Ca2+ uptake. Additionally, NCX expression is significantly increased leading to abnormally increased Ca2+ extrusion to the extracellular side and depletion of intracellular Ca2+ stores. Despite Ca2+ store depletion, DADs and triggered activity are frequent in HF possibly due to increased SR Ca2+ leak and proarrhythmogenic inward NCX and late I Na,L currents
Milestones toward imaging of intracellular calcium metabolism
The study of intracellular Ca2+ concentration, [Ca2+]i, in heart function requires to monitor the dynamics of [Ca2+]i in living cells. However, the free [Ca2+]i is heterogeneous even in resting cells and ranges from nanomolar to micromolar concentrations in the cytoplasm and SR Ca2+ stores, respectively [9]. During electrical cell activation or stimulation by hormone receptors, the resultant changes in the cytoplasmic and organellar Ca2+ concentrations occur as spatially and temporally defined patterns within cellular microdomains [10]. Thus, understanding of changes in Ca2+ signaling during HF has been largely dependent on methods to monitor Ca2+ concentrations in living cells.
Ca2+ indicators form selective and reversible complexes with free Ca2+ ions. The physicochemical differences of the free and bound indicator allow for the fluorescence detection of changes in ∆[Ca2+]i usually by the absorbance and/or emission of light [11]. Thus, the concentration of free Ca2+ is measured indirectly by monitoring the amount of the free versus the Ca2+ complexed indicator. The chemiluminescent photoprotein aequorin purified from jellyfish can be microinjected into tissues or cells and applied as a Ca2+ indicator [12]. Moreover, recombinant aequorin can be targeted to specific subcellular compartments through signal sequences [13]. However, recombinant aequorin emits a relatively small signal upon Ca2+ binding which compromises the measurement of Ca2+ concentrations in smaller cells at the cost of low time resolution [14]. Tsien and colleagues synthesized the first, rationally designed, fluorescent Ca2+ indicator for intracellular use based on the Ca2+-chelator EGTA [15]. The widespread and successful use of fluorescent polycarboxylate dyes started with the introduction of lipophilic acetoxymethyl (AM) ester derivatives allowing efficient and stable indicator loading of living cells without potentially damaging pipette injection techniques [16].
Global intracellular calcium abnormalities in heart failure
Pioneering studies used injection of the aequorin Ca2+ sensor into physiologically contracting muscle preparations from explanted human hearts. Aequorin loaded muscles from failing hearts showed a reduced capacity to restore nanomolar resting Ca2+ levels during diastole in conjunction with depressed muscle contraction and relaxation [17]. Different from healthy heart muscle and pronounced at faster rates, the aequorin injected failing heart muscle showed a reduced amplitude of the intracellular Ca2+ transient (∆[Ca2+]i) together with diminished force production [18]. Additionally, myothermal measurements in isolated muscle strip preparations from failing and non-failing human hearts showed that the thermal equivalent of total Ca2+ cycling is reduced significantly in HF [19]. The rate of heat production was significantly reduced indicating reduced SR Ca2+ uptake [19].
Consistent with multicellular muscle preparations, dissociated single cardiomyocytes from failing human hearts displayed a prolonged relaxation, depressed systolic contraction, and elevated diastolic tension [20]. Contractile dysfunction of failing cardiomyocytes occurred in conjunction with abnormal [Ca2+]i metabolism including reduced SR Ca2+ release, elevated resting [Ca2+]i, and a reduced rate of Ca2+ removal [21, 22]. For late stage HF it is now accepted that cardiomyocytes and/or muscle preparations from explanted patient or animal hearts exhibit a reduced Δ[Ca2+]i amplitude and a slowed decay of the global intracellular Ca2+ transient [17, 23–25]. Thus, depressed contractility in HF appears to be associated with cellular signaling abnormalities at the level of the global intracellular Ca2+ transient.
Notably, the combination of an abnormal intracellular Ca2+ transient together with depressed contractile function all occur from quite different forms of cardiac insults. Such phenotypic changes have been documented in dilated human cardiomyopathy [23, 26], hypertension induced hypertrophy HF in salt-sensitive rats [24], rats with myocardial infarction [27], mice with muscle LIM protein knockout [28], mice with replication-restricted full-length Coxsackievirus B3 overexpression and myocarditis [29], and mice overexpressing either the catalytic protein kinase A (PKA)-Cα subunit [30] or the cytosolic CaMKIIδc splice variant [31]. Thus, different HF models appear to agree that qualitatively similar changes of the intracellular Ca2+ transient and subsequent alterations of EC coupling and contractile dysfunction occur.
Local intracellular calcium abnormalities in heart failure
While cardiac contraction and relaxation cycles are controlled by a cell-wide (global) signaling event, the Ca2+ transient, intracellular Ca2+ release occurs within local (subcellular) Ca2+ release units as evidenced by elementary Ca2+ release events measured with bright fluorescent polycarboxylate dyes [8, 32]. How do local, elementary Ca2+ release events, known as Ca2+ sparks, modulate the intracellular Ca2+ transient? At a diastolic [Ca2+]i of approximately 100 nM, Ca2+ sparks occur at a very low rate (100 s−1 cell−1). When the AP occurs, Ca2+ influx causes a large increase in cytosolic [Ca2+]i within the tight junctional subspace (Fig. 1a). A raise of junctional [Ca2+]i above nanomolar concentrations increases the spark rate 103 to 106 fold. Therefore, the I Ca influx current becomes amplified by a dramatic increase in Ca2+ spark rate during CICR. This implies that modulation of the Ca2+ spark rate may control the Ca2+ transient amplitude and cardiac force development (inotropy). Indeed, imaging experiments of subcellular Ca2+ signaling have provided evidence that β-adrenergic stimulation increases local Ca2+ release possibly due to RyR2 phosphorylation [33].
An important advance why changes in the intracellular Ca2+ transient occur in HF come from combined voltage-clamp and Ca2+ spark imaging experiments to assess if changes in EC coupling are responsible for depressed cardiac function. A rat model of hypertension induced HF with preserved Ca2+ influx current (I Ca) density showed that the ability of any given I Ca to activate SR Ca2+ sparks (Δ[Ca2+]i) was significantly decreased [24]. Thus, HF is accompanied by a decrease in the gain of EC coupling (Δ[Ca2+]i/ICa) which has been confirmed in rats with myocardial infarction [27], dogs with pacing-induced HF [34], mice with viral myocarditis [29], and muscle LIM protein knockout mice [35]. Additionally, structural changes of the T-tubules, SR storage organelles, and/or the architecture of the junctional microdomain cleft are all likely contributors to defective EC coupling by altering the geometry of the Ca2+ release unit potentially resulting in orphaned RyR2 release channels and/or abnormal CICR [36, 37].
Abnormal calcium release triggers fatal arrhythmias
Sudden unexpected death accounts for up to 50% of all deaths in HF patients and is most often due to ventricular tachyarrhythmias [38]. Both reentry and focal mechanisms have been documented in patients with ischemic cardiomyopathy [39]. At the cellular level, arrhythmias have been associated with Ca2+ induced electrical abnormalities including SR Ca2+ overload leading to intracellular Ca2+ waves and Ca2+ activated transient inward current (I TI) [40–42]. In digitalis treated cells, I TI was shown to initiate delayed after depolarizations (DADs) [43]. Association of SR Ca2+ leak with activation of a depolarizing Na+/Ca2+ exchange current is a likely mechanism of arrhythmogenic I TI in HF [44–46].
Genetic linkage and translational studies have significantly advanced our understanding about specific Ca2+ dependent arrhythmia mechanisms (Table 1). For instance, RyR2 missense mutations may cause stress-induced syncope and sudden death in a syndrome called Catecholaminergic Polymorphic Ventricular Tachycardia (CPVT) [47, 48]. Consistent with a β-AR and cAMP mediated stress mechanism, PKA phosphorylated RyR2 channels containing CPVT mutations showed a significant gain-of-function defect and a Ca2+ leak mediated arrhythmia trigger mechanism [49, 50]. Indeed, cardiomyocytes from knockin mice with the RyR2-R2474S mutation identified earlier in CPVT patients [47] showed Ca2+ leak mediated I TI currents and DADs during stimulation with catecholamines (Fig. 1b) [51]. While we have to anticipate additional mechanisms of Ca2+ leak in HF, mechanistic linkage of CPVT mutant RyR2 dependent Ca2+ leak to arrhythmia initiation [51] provides a specific mechanism of Ca2+ dependent arrhythmia initiation which can be targeted and tested by a novel class of RyR2 stabilizing compounds [51] (Table 2).
Storage organelle and calcium transport dysfunction
Ca2+ is the central intracellular messenger which links an incoming action potential to myofilament activation and cardiac contraction. Apart from EC coupling, [Ca2+]i is subject to physiological stress adaptation and a higher systolic ∆[Ca2+]i increases force development and cardiac output (inotropy) [33]. Following the realization that SR Ca2+ uptake might be depressed in failing cardiomyocytes, the intracellular storage organelles and SR Ca2+ content became a focus of intense research interest.
HF has been associated with decreased function of different Ca2+ transport mechanisms (Table 1) including the sarcoendoplasmic reticulum (SR) Ca2+ ATPase (SERCA2) [52, 53] and with increased function of the Na+/Ca2+ exchanger (NCX) [54]. The ratio of PLN:SERCA2 is a critical determinant of cardiac Ca2+ homeostasis, and increases in this ratio have been suggested to contribute to increased diastolic Ca2+ levels and cardiac dysfunction [53, 55, 56]. On the other hand, due to the changes in the relative expression and function of NCX and SERCA2, a net shift toward increased Ca2+ extrusion to the extracellular space and a net decrease in SR Ca2+ uptake occurs (Fig. 1c). Therefore, intracellular Ca2+ stores may develop a relatively Ca2+ depleted state which has been confirmed experimentally in cardiomyocytes from dogs and humans with HF [26, 34]. Decreased SR Ca2+ load may result in a decreased amplitude and slower upstroke of the intracellular Ca2+ transient. Since ∆[Ca2+]i is an important mediator of cardiac force development, a decreased ∆[Ca2+]i due to decreased SR load may result in decreased force development. However, SR Ca2+ store depletion in HF does not necessarily prevent an increase in Ca2+ spark frequency [31] likely due to chronically increased RyR2 phosphorylation [57] and consistent with an increased propensity for Ca2+ induced arrhythmias in HF.
Molecular mechanisms of depressed SR calcium uptake
Decreased SERCA2 function has been associated with changes in the regulatory subunit PLN (Fig. 1c). PLN is a phosphoprotein which inhibits SERCA2 in its dephosphorylated state, while phosphorylation of PLN during β-AR stimulation relieves this inhibitory effect. The regulatory role of PLN in myocardial contractility has been established through the generation and characterization of genetically altered mouse models, which revealed a correlation between PLN expression and contractile function [58–60]. PLN phosphorylation in HF is chronically decreased (PLN hypophosphorylation) which may directly contribute to depressed SR Ca2+ uptake [61]. Chronic PLN hypophosphorylation can be predicted to compromise cardiac stress adaptation mediated by cAMP and PKA. Overexpression of the cardiac SERCA2a isoform or the constitutively PKA phosphorylated PLN-Ser16 improved function in rats following aortic banding-induced HF [62] and decreased arrhythmia susceptibility following ischemia-reperfusion cardiomyopathy in pigs [63].
Phospholamban is potently inhibited by phosphatase 1 (PP1), which in turn is inhibited by phosphatase inhibitor I-1 following PKA phosphorylation and I-1 activation. Consistent with this mechanism, overexpression of an activated I-1 form in mice protects the animals from HF development [64]. Moreover, the identification of PLN mutations in patients with dilated cardiomyopathy has strengthened its critical role in cardiac function. Thus, inhibition of PLN activity and restoration of SR Ca2+ cycling were suggested to hold promise for treating heart failure [65].
Molecular mechanisms of intracellular calcium leak
In samples from patients and animals with HF, RyR2 is chronically PKA hyperphosphorylated contributing to intracellular Ca2+ leak and remodeling of the macromolecular channel complex [7, 66, 67]. If the hyperadrenergic state in HF leads to secondary downregulation of β-adrenergic signaling and globally reduced intracellular cAMP synthesis, which molecular mechanism maintains RyR2 PKA hyperphosphorylation and intracellular Ca2+ leak? During HF, phosphatases (PP1 and PP2A) are depleted from the RyR2 complex which may contribute to a reduced rate of RyR2 dephosphorylation [61, 66]. In human HF, the cAMP-specific phosphodiesterase isoform PDE4D3 was found to be decreased in the RyR2 complex paralleled by a decrease in cAMP hydrolyzing activity [57]. Thus, PKA hyperphosphorylation and calstabin2 depletion may both contribute to chronic RyR2 activation and intracellular Ca2+ leak (Fig. 1c). Indeed, single RyR2 channels from human failing hearts showed an increased open probability consistent with intracellular Ca2+ leak [66].
Using site-directed mutagenesis of RyR2, a specific Ca2+/calmodulin-dependent protein kinase II (CaMKII) phosphorylation site (Ser2814) distinct from the PKA phosphorylation site (Ser2808) has been identified [6]. CaMKII phosphorylation increased RyR2 Ca2+ sensitivity and open probability. Since CaMKII was activated by higher cardiac pacing rates, RyR2 CaMKII phosphorylation may contribute to enhanced CICR and enhanced contractility at higher heart rates. However, the rate-dependent increase in RyR2 phosphorylation by CaMKII as seen in sham-operated, healthy rat hearts was compromised in rat hearts with HF [6]. Transgenic mice overexpressing the cytosolic CaMKIIδc isoform develop cardiac hypertrophy, HF, and intracellular Ca2+ leak [68]. Acute overexpression of CaMKIIδc in cardiomyocytes resulted in significant SR Ca2+ leak without changes in contractile function [69]. Adenoviral CaMKII overexpression was not associated with calstabin2 dissociation from RyR2 [69] confirming earlier results [6]. On the other hand, PKA phosphorylation of RyR2 resulted in depletion of the stabilizing calstabin2 subunit [6], and decreased calstabin2 levels have been linked to Ca2+ triggered arrhythmias in the structurally normal heart [49]. Disruption of RyR2 PKA phosphorylation in Ser2808Ala knockin mice with myocardial infarct induced HF has provided evidence that PKA hyperphosphorylation induced SR Ca2+ leak may directly contribute to HF progression [70]. However, the significance of concomitant PKA and/or CaMKII RyR2 phosphorylation in Ca2+ dysregulation during HF has not been addressed conclusively.
Altered sodium handling in heart failure
Intracellular Na+ and Ca2+ concentrations are intricately coupled through the NCX current. In addition, Na+ influx through sarcolemmal NaV1.5 channels contributes to intracellular [Na+]i homeostasis (Fig. 1a). Studies about [Na+]i in human myocardium showed a stimulation rate dependent increase in [Na+]i [71, 72]. For any given stimulation rate, human end-stage failing myocardium showed a shift toward higher intracellular [Na+]i [71]. In a rabbit HF model with elevated [Na+]i, the function of the Na+/K+-ATPase function was found normal [73]. A potential role of altered Na+ channel inactivation and a significantly increased late I Na,L in HF as a cause of intracellular [Na+]i overload has been documented in animal models of HF and human failing myocardium [74, 75]. Slow pacing of failing cardiomyocytes with increased [Na+]i may enhance Ca2+ influx from the extracellular side through reverse mode NCX contributing to increased SR Ca2+ load and force development. Indeed, at higher pacing rates failing cardiomyocytes with high [Na+]i are prone to diastolic Ca2+ overload and contractile dysfunction. Interestingly, pharmacological inhibition of I Na,L was found to improve diastolic dysfunction in failing human myocardium [76]. Additionally, increased late I Na,L may result in Ca2+ induced electrical cardiomyocyte dysfunction as shown in SCN5A-∆KPQ knockin mice resembling the Long-QT3 syndrome [77].
Altered force frequency relation in the failing human heart
Pathophysiological consequences of altered EC coupling have an immediate impact on cardiac stress adaptation during higher heart rates. The force–frequency relation (FFR) or staircase phenomenon of healthy human myocardium and within physiological limits describes a heart rate dependent increase in contractile force and cardiac output. However, in failing human hearts or isolated muscle preparations, the frequency-dependent potentiation of contractile force is blunted or, even worse, inversed [78]. Alteration of the FFR in the failing human heart has been accepted as a functional milestone which may partially explain the decreased exercise capacity of symptomatic HF patients.
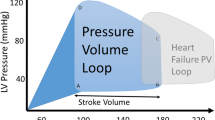
Using aequorin Ca2+ measurements it has been shown that a positive FFR in normal healthy myocardium is associated with a positive ∆[Ca2+]i transient amplitude–frequency relation, and vice versa, a negative FFR in the failing myocardium is associated with an inverted ∆[Ca2+]i–frequency relation [18]. Alterations of the frequency response of contractile performance have been confirmed in vivo in HF patients [79]. A different experimental protocol which is thought to enable increased Ca2+ accumulation into the SR stores in diastole, uses post-rest pacing which typically produces an increase in developed force in healthy myocardium also referred to as ‘post-rest potentiation’. However, alterations in post-rest potentiation that may underlie reduced stress adaptation and the FFR inversion have been associated with a blunted post-rest ∆[Ca2+]i increase of SR Ca2+ content (Fig. 2) [80]. While in healthy human myocardium a pronounced upregulation of SR Ca2+ content occurs at higher heart rates, failing human myocardium shows a blunted regulation of SR Ca2+ content [26]. Therefore, the chronic hyperadrenergic state and associated higher heart rates in HF patients may create an increased risk for Ca2+ induced cardiac dysfunction and arrhythmias. Accordingly, novel therapeutic strategies have successfully used pharmacological heart rate reduction in HF patients to improve prognostic outcome [81].
Representative traces of aequorin-based Ca2+ signals and corresponding isometric forces from human nonfailing (top) and failing (bottom) myocardial muscle preparations. Upper panel: Nonfailing myocardium shows post-rest potentiation of the intracellular Ca2+ transient and force development which increases from 10 to 120 s rest period. Lower panel: Failing myocardium shows depressed post-rest intracellular Ca2+ transient and force development after 120 s rest. Steady-state pre-rest signals are shown on the left of each trace; first and second post-rest signals are shown afterwards; post-rest signals represent 10 s (left) and 120 s (right), dimensions as indicated. Reproduced with permission from the Journal of Clinical Investigation (Pieske et al. [80])
Therapeutic rationales to modulate calcium handling in heart failure
Several therapeutic rationales exist which aim to correct known molecular Ca2+ signaling abnormalities in HF as summarized in Table 2. Among these strategies, NCX blockers may have therapeutic utility if mode-selective block can be established and/or risks for disturbing intracellular Ca2+ metabolism can be avoided. Partial inhibition of NCX by SEA-0400 in MLP−/− knockout cardiomyocytes with heart failure showed a net gain of [Ca2+]i and SR load but no improvement in contractility whereas cardiomyocytes from mice with aortic-banding induced hypertrophy and HF showed improved contractile function [82]. Further development of NCX blockers for HF will depend on the critical assessment of the potential benefits of NCX reduction versus effects on [Ca2+]i by refining mode dependence and/or including additional targeting strategies.
Some traditional ion channel blockers like tetracaine inhibit ion permeation through RyR2 channels, however, lack of specificity and potential side effects on contractile function indicate significant limitations toward therapeutic applicability [83, 84]. Recently, the efficacy of novel RyR2 channel stabilizing drugs of the 1,4-benzothiazepine class (JTV519 or K201) which stabilize the RyR2 closed state but do not block ion permeation has been established in animal models of heart failure where they inhibit progression of cardiac remodeling and dysfunction [57, 85, 86]. RyR2 stabilizing compounds with high specificity and cardiac activity have been developed [51] and their efficacy as potential HF treatment is under investigation. Additionally, β-blockers and angiotensin-II receptor blockers have been associated with beneficial effects on RyR2 channel dysfunction in HF through mechanisms which indirectly prevent excess post-translational modification of RyR2, e.g. by PKA hyperphosphorylation or nitrosylation [87–89].
Adeno-associated viruses (AAVs) are currently best suited for myocardial gene delivery due to minimal pathogenicity and several serotypes exhibit tropism for the heart. Following identification and comprehensive characterization of SERCA2a as a potential therapeutic target in HF, cardiac gene therapy trials using replication-deficient viral vectors (AAV-SERCA2a) have been approved by the US Food and Drug Administration and are under review with the UK regulatory authorities for clinical trials [90].
Summary and future perspectives
HF is characterized by chronic maladaptive changes and a poor prognosis. Chronic activation of intracellular signaling pathways mediates structural and functional remodeling of the failing heart. Changes in EC coupling at the level of local and global Ca2+ signals represent a key mechanism of contractile depression and arrhythmia propensity. It has become increasingly clear that cardiac remodeling in HF occurs within cytosolic Ca2+ signaling microdomains. Translational approaches about the local and global Ca2+ signaling mechanisms, remodeling mechanisms, and related disease processes will be of key importance to develop novel and specific therapeutic rationales. We anticipate that Ca2+ imaging techniques will significantly increase our understanding of the cardiac pathophysiology underlying HF and boost development of novel therapeutic strategies in the future.
Abbreviations
- AAV:
-
Adeno-associated virus
- AP:
-
Action potential
- β-AR:
-
β-Adrenergic receptor
- Ca2+ :
-
Free ionized calcium
- [Ca2+]i :
-
Intracellular Ca2+ concentration
- CaMKII:
-
Ca2+ calmodulin dependent protein kinase II
- CICR:
-
Ca2+ induced Ca2+ release
- cAMP:
-
3′-5′-Cyclic adenosine monophosphate
- CaV1.2:
-
L-type Ca2+ channels
- DAD:
-
Delayed after depolarization
- EC coupling:
-
Excitation-contraction coupling
- HF:
-
Heart failure
- I Ca :
-
Ca2+ influx current
- I TI :
-
Ca2+ activated transient inward current
- I-1:
-
Phosphatase inhibitor 1
- MI:
-
Myocardial infarction
- NCX:
-
Na+/Ca2+ exchanger
- PKA:
-
cAMP-dependent protein kinase A
- PLN:
-
Phospholamban
- PP1:
-
Phosphatase 1
- SERCA2a:
-
Sarco-endoplasmic reticulum Ca2+ pump
- SR:
-
Sarcoplasmic reticulum Ca2+ storage organelle
- RyR2:
-
Cardiac ryanodine receptor
References
Bristow MR, Ginsburg R, Umans V, Fowler M, Minobe W, Rasmussen R, Zera P, Menlove R, Shah P, Jamieson S et al (1986) Beta 1- and beta 2-adrenergic-receptor subpopulations in nonfailing and failing human ventricular myocardium: coupling of both receptor subtypes to muscle contraction and selective beta 1-receptor down-regulation in heart failure. Circ Res 59:297–309
Cohn JN, Levine TB, Olivari MT, Garberg V, Lura D, Francis GS, Simon AB, Rector T (1984) Plasma norepinephrine as a guide to prognosis in patients with chronic congestive heart failure. N Engl J Med 311:819–823
Feldman MD, Copelas L, Gwathmey JK, Phillips P, Warren SE, Schoen FJ, Grossman W, Morgan JP (1987) Deficient production of cyclic AMP: pharmacologic evidence of an important cause of contractile dysfunction in patients with end-stage heart failure. Circulation 75:331–339
Foo RS, Mani K, Kitsis RN (2005) Death begets failure in the heart. J Clin Invest 115:565–571. doi:10.1172/JCI200524569
Wencker D, Chandra M, Nguyen K, Miao W, Garantziotis S, Factor SM, Shirani J, Armstrong RC, Kitsis RN (2003) A mechanistic role for cardiac myocyte apoptosis in heart failure. J Clin Invest 111:1497–1504
Wehrens XH, Lehnart SE, Reiken SR, Marks AR (2004) Ca2+/calmodulin-dependent protein kinase II phosphorylation regulates the cardiac ryanodine receptor. Circ Res 94:e61–e70. doi:10.1161/01.RES.0000125626.33738.E2
Marx SO, Reiken S, Hisamatsu Y, Jayaraman T, Burkhoff D, Rosemblit N, Marks AR (2000) PKA phosphorylation dissociates FKBP12.6 from the calcium release channel (ryanodine receptor): defective regulation in failing hearts. Cell 101:365–376. doi:10.1016/S0092-8674(00)80847-8
Guatimosim S, Dilly K, Santana LF, Saleet Jafri M, Sobie EA, Lederer WJ (2002) Local Ca(2+) signaling and EC coupling in heart: Ca(2+) sparks and the regulation of the [Ca(2+)](i) transient. J Mol Cell Cardiol 34:941–950. doi:10.1006/jmcc.2002.2032
Pozzan T, Rizzuto R, Volpe P, Meldolesi J (1994) Molecular and cellular physiology of intracellular calcium stores. Physiol Rev 74:595–636
Berridge MJ, Lipp P, Bootman MD (2000) The versatility and universality of calcium signalling. Nat Rev Mol Cell Biol 1:11–21. doi:10.1038/35036035
Rudolf R, Mongillo M, Rizzuto R, Pozzan T (2003) Looking forward to seeing calcium. Nat Rev Mol Cell Biol 4:579–586. doi:10.1038/nrm1153
Shimomura O, Johnson FH, Saiga Y (1962) Extraction, purification and properties of aequorin, a bioluminescent protein from the luminous hydromedusan, Aequorea. J Cell Comp Physiol 59:223–239. doi:10.1002/jcp.1030590302
Rizzuto R, Brini M, Pozzan T (1994) Targeting recombinant aequorin to specific intracellular organelles. Methods Cell Biol 40:339–358. doi:10.1016/S0091-679X(08)61121-8
Rutter GA, Burnett P, Rizzuto R, Brini M, Murgia M, Pozzan T, Tavare JM, Denton RM (1996) Subcellular imaging of intramitochondrial Ca2+ with recombinant targeted aequorin: significance for the regulation of pyruvate dehydrogenase activity. Proc Natl Acad Sci USA 93:5489–5494. doi:10.1073/pnas.93.11.5489
Tsien RY (1980) New calcium indicators and buffers with high selectivity against magnesium and protons: design, synthesis, and properties of prototype structures. Biochemistry 19:2396–2404. doi:10.1021/bi00552a018
Tsien RY (1981) A non-disruptive technique for loading calcium buffers and indicators into cells. Nature 290:527–528. doi:10.1038/290527a0
Gwathmey JK, Copelas L, MacKinnon R, Schoen FJ, Feldman MD, Grossman W, Morgan JP (1987) Abnormal intracellular calcium handling in myocardium from patients with end-stage heart failure. Circ Res 61:70–76
Pieske B, Kretschmann B, Meyer M, Holubarsch C, Weirich J, Posival H, Minami K, Just H, Hasenfuss G (1995) Alterations in intracellular calcium handling associated with the inverse force-frequency relation in human dilated cardiomyopathy. Circulation 92:1169–1178
Hasenfuss G, Mulieri LA, Leavitt BJ, Allen PD, Haeberle JR, Alpert NR (1992) Alteration of contractile function and excitation-contraction coupling in dilated cardiomyopathy. Circ Res 70:1225–1232
Harding SE, Jones SM, O’Gara P, del Monte F, Vescovo G, Poole-Wilson PA (1992) Isolated ventricular myocytes from failing and non-failing human heart; the relation of age and clinical status of patients to isoproterenol response. J Mol Cell Cardiol 24:549–564. doi:10.1016/0022-2828(92)91843-T
Schmidt U, Hajjar RJ, Helm PA, Kim CS, Doye AA, Gwathmey JK (1998) Contribution of abnormal sarcoplasmic reticulum ATPase activity to systolic and diastolic dysfunction in human heart failure. J Mol Cell Cardiol 30:1929–1937. doi:10.1006/jmcc.1998.0748
Gwathmey JK, Slawsky MT, Hajjar RJ, Briggs GM, Morgan JP (1990) Role of intracellular calcium handling in force-interval relationships of human ventricular myocardium. J Clin Invest 85:1599–1613. doi:10.1172/JCI114611
Schlotthauer K, Schattmann J, Bers DM, Maier LS, Schutt U, Minami K, Just H, Hasenfuss G, Pieske B (1998) Frequency-dependent changes in contribution of SR Ca2+ to Ca2+ transients in failing human myocardium assessed with ryanodine. J Mol Cell Cardiol 30:1285–1294. doi:10.1006/jmcc.1998.0690
Gomez AM, Valdivia HH, Cheng H, Lederer MR, Santana LF, Cannell MB, McCune SA, Altschuld RA, Lederer WJ (1997) Defective excitation-contraction coupling in experimental cardiac hypertrophy and heart failure. Science 276:800–806. doi:10.1126/science.276.5313.800
Beuckelmann DJ, Nabauer M, Erdmann E (1992) Intracellular calcium handling in isolated ventricular myocytes from patients with terminal heart failure. Circulation 85:1046–1055
Pieske B, Maier LS, Bers DM, Hasenfuss G (1999) Ca2+ handling and sarcoplasmic reticulum Ca2+ content in isolated failing and nonfailing human myocardium. Circ Res 85:38–46
Gomez AM, Guatimosim S, Dilly KW, Vassort G, Lederer WJ (2001) Heart failure after myocardial infarction: altered excitation-contraction coupling. Circulation 104:688–693. doi:10.1161/hc3201.092285
Esposito G, Santana LF, Dilly K, Cruz JD, Mao L, Lederer WJ, Rockman HA (2000) Cellular and functional defects in a mouse model of heart failure. Am J Physiol Heart Circ Physiol 279:H3101–H3112
Wessely R, Klingel K, Santana LF, Dalton N, Hongo M, Jonathan Lederer W, Kandolf R, Knowlton KU (1998) Transgenic expression of replication-restricted enteroviral genomes in heart muscle induces defective excitation-contraction coupling and dilated cardiomyopathy. J Clin Invest 102:1444–1453. doi:10.1172/JCI1972
Antos CL, Frey N, Marx SO, Reiken S, Gaburjakova M, Richardson JA, Marks AR, Olson EN (2001) Dilated cardiomyopathy and sudden death resulting from constitutive activation of protein kinase a. Circ Res 89:997–1004. doi:10.1161/hh2301.100003
Maier LS, Zhang T, Chen L, DeSantiago J, Brown JH, Bers DM (2003) Transgenic CaMKIIdeltaC overexpression uniquely alters cardiac myocyte Ca2+ handling: reduced SR Ca2+ load and activated SR Ca2+ release. Circ Res 92:904–911. doi:10.1161/01.RES.0000069685.20258.F1
Cheng H, Lederer WJ, Cannell MB (1993) Calcium sparks: elementary events underlying excitation-contraction coupling in heart muscle. Science 262:740–744. doi:10.1126/science.8235594
Lindegger N, Niggli E (2005) Paradoxical SR Ca2+ release in guinea-pig cardiac myocytes after beta-adrenergic stimulation revealed by two-photon photolysis of caged Ca2+. J Physiol 565:801–813. doi:10.1113/jphysiol.2005.084376
Hobai IA, O’Rourke B (2001) Decreased sarcoplasmic reticulum calcium content is responsible for defective excitation-contraction coupling in canine heart failure. Circulation 103:1577–1584
Arber S, Hunter JJ, Ross J Jr, Hongo M, Sansig G, Borg J, Perriard JC, Chien KR, Caroni P (1997) MLP-deficient mice exhibit a disruption of cardiac cytoarchitectural organization, dilated cardiomyopathy, and heart failure. Cell 88:393–403. doi:10.1016/S0092-8674(00)81878-4
Schaper J, Froede R, Hein S, Buck A, Hashizume H, Speiser B, Friedl A, Bleese N (1991) Impairment of the myocardial ultrastructure and changes of the cytoskeleton in dilated cardiomyopathy. Circulation 83:504–514
Song LS, Sobie EA, McCulle S, Lederer WJ, Balke CW, Cheng H (2006) Orphaned ryanodine receptors in the failing heart. Proc Natl Acad Sci USA 103:4305–4310. doi:10.1073/pnas.0509324103
Grimm W, Maisch B (2002) Sudden cardiac death in dilated cardiomyopathy—therapeutic options. Herz 27:750–759. doi:10.1007/s00059-002-2425-0
Pogwizd SM, Hoyt RH, Saffitz JE, Corr PB, Cox JL, Cain ME (1992) Reentrant and focal mechanisms underlying ventricular tachycardia in the human heart. Circulation 86:1872–1887
Kass RS, Tsien RW, Weingart R (1978) Ionic basis of transient inward current induced by strophanthidin in cardiac Purkinje fibres. J Physiol 281:209–226
Kass RS, Lederer WJ, Tsien RW, Weingart R (1978) Role of calcium ions in transient inward currents and aftercontractions induced by strophanthidin in cardiac Purkinje fibres. J Physiol 281:187–208
Berlin JR, Cannell MB, Lederer WJ (1989) Cellular origins of the transient inward current in cardiac myocytes. Role of fluctuations and waves of elevated intracellular calcium. Circ Res 65:115–126
Lederer WJ, Tsien RW (1976) Transient inward current underlying arrhythmogenic effects of cardiotonic steroids in Purkinje fibres. J Physiol 263:73–100
Clusin WT (1983) Caffeine induces a transient inward current in cultured cardiac cells. Nature 301:248–250. doi:10.1038/301248a0
Lipp P, Pott L (1988) Voltage dependence of sodium-calcium exchange current in guinea-pig atrial myocytes determined by means of an inhibitor. J Physiol 403:355–366
Pogwizd SM, Qi M, Yuan W, Samarel AM, Bers DM (1999) Upregulation of Na(+)/Ca(2+) exchanger expression and function in an arrhythmogenic rabbit model of heart failure. Circ Res 85:1009–1019
Priori SG, Napolitano C, Tiso N, Memmi M, Vignati G, Bloise R, Sorrentino VV, Danieli GA (2001) Mutations in the cardiac ryanodine receptor gene (hRyR2) underlie catecholaminergic polymorphic ventricular tachycardia. Circulation 103:196–200
Laitinen PJ, Brown KM, Piippo K, Swan H, Devaney JM, Brahmbhatt B, Donarum EA, Marino M, Tiso N, Viitasalo M, Toivonen L, Stephan DA, Kontula K (2001) Mutations of the cardiac ryanodine receptor (RyR2) gene in familial polymorphic ventricular tachycardia. Circulation 103:485–490
Wehrens XH, Lehnart SE, Huang F, Vest JA, Reiken SR, Mohler PJ, Sun J, Guatimosim S, Song LS, Rosemblit N, D’Armiento JM, Napolitano C, Memmi M, Priori SG, Lederer WJ, Marks AR (2003) FKBP12.6 deficiency and defective calcium release channel (ryanodine receptor) function linked to exercise-induced sudden cardiac death. Cell 113:829–840. doi:10.1016/S0092-8674(03)00434-3
Lehnart SE, Wehrens XH, Laitinen PJ, Reiken SR, Deng SX, Cheng Z, Landry DW, Kontula K, Swan H, Marks AR (2004) Sudden death in familial polymorphic ventricular tachycardia associated with calcium release channel (ryanodine receptor) leak. Circulation 109:3208–3214. doi:10.1161/01.CIR.0000132472.98675.EC
Lehnart SE, Mongillo M, Bellinger A, Lindegger N, Chen BX, Hsueh W, Reiken S, Wronska A, Drew LJ, Ward CW, Lederer WJ, Kass RS, Morley G, Marks AR (2008) Leaky Ca2+ release channel/ryanodine receptor 2 causes seizures and sudden cardiac death in mice. J Clin Invest 118:2230–2245
Mercadier JJ, Lompre AM, Duc P, Boheler KR, Fraysse JB, Wisnewsky C, Allen PD, Komajda M, Schwartz K (1990) Altered sarcoplasmic reticulum Ca2(+)-ATPase gene expression in the human ventricle during end-stage heart failure. J Clin Invest 85:305–309. doi:10.1172/JCI114429
Meyer M, Schillinger W, Pieske B, Holubarsch C, Heilmann C, Posival H, Kuwajima G, Mikoshiba K, Just H, Hasenfuss G et al (1995) Alterations of sarcoplasmic reticulum proteins in failing human dilated cardiomyopathy. Circulation 92:778–784
Studer R, Reinecke H, Bilger J, Eschenhagen T, Bohm M, Hasenfuss G, Just H, Holtz J, Drexler H (1994) Gene expression of the cardiac Na(+)-Ca2+ exchanger in end-stage human heart failure. Circ Res 75:443–453
Kadambi VJ, Ponniah S, Harrer JM, Hoit BD, Dorn GW 2nd, Walsh RA, Kranias EG (1996) Cardiac-specific overexpression of phospholamban alters calcium kinetics and resultant cardiomyocyte mechanics in transgenic mice. J Clin Invest 97:533–539. doi:10.1172/JCI118446
Dash R, Frank KF, Carr AN, Moravec CS, Kranias EG (2001) Gender influences on sarcoplasmic reticulum Ca2+-handling in failing human myocardium. J Mol Cell Cardiol 33:1345–1353. doi:10.1006/jmcc.2001.1394
Lehnart SE, Wehrens XH, Reiken S, Warrier S, Belevych AE, Harvey RD, Richter W, Jin SL, Conti M, Marks AR (2005) Phosphodiesterase 4D deficiency in the ryanodine-receptor complex promotes heart failure and arrhythmias. Cell 123:25–35. doi:10.1016/j.cell.2005.07.030
Luo W, Wolska BM, Grupp IL, Harrer JM, Haghighi K, Ferguson DG, Slack JP, Grupp G, Doetschman T, Solaro RJ, Kranias EG (1996) Phospholamban gene dosage effects in the mammalian heart. Circ Res 78:839–847
Luo W, Grupp IL, Harrer J, Ponniah S, Grupp G, Duffy K, Doetschmann T, Kranias EG (1994) Targeted ablation of the phospholamban gene is associated with markedly enhanced myocardial contractility and loss of beta-agonist stimulation. Circ Res 75:401–409
Lorenz JN, Kranias EG (1997) Regulatory effects of phospholamban on cardiac function in intact mice. Am J Physiol 273:H2826–H2831
Reiken S, Gaburjakova M, Guatimosim S, Gomez AM, D’Armiento J, Burkhoff D, Wang J, Vassort G, Lederer WJ, Marks AR (2003) Protein kinase A phosphorylation of the cardiac calcium release channel (ryanodine receptor) in normal and failing hearts. Role of phosphatases and response to isoproterenol. J Biol Chem 278:444–453. doi:10.1074/jbc.M207028200
Miyamoto MI, del Monte F, Schmidt U, DiSalvo TS, Kang ZB, Matsui T, Guerrero JL, Gwathmey JK, Rosenzweig A, Hajjar RJ (2000) Adenoviral gene transfer of SERCA2a improves left-ventricular function in aortic-banded rats in transition to heart failure. Proc Natl Acad Sci USA 97:793–798. doi:10.1073/pnas.97.2.793
Prunier F, Kawase Y, Gianni D, Scapin C, Danik SB, Ellinor PT, Hajjar RJ, Del Monte F (2008) Prevention of ventricular arrhythmias with sarcoplasmic reticulum Ca2+ ATPase pump overexpression in a porcine model of ischemia reperfusion. Circulation 118:614–624. doi:10.1161/CIRCULATIONAHA.108.770883
Pathak A, del Monte F, Zhao W, Schultz JE, Lorenz JN, Bodi I, Weiser D, Hahn H, Carr AN, Syed F, Mavila N, Jha L, Qian J, Marreez Y, Chen G, McGraw DW, Heist EK, Guerrero JL, DePaoli-Roach AA, Hajjar RJ, Kranias EG (2005) Enhancement of cardiac function and suppression of heart failure progression by inhibition of protein phosphatase 1. Circ Res 96:756–766. doi:10.1161/01.RES.0000161256.85833.fa
MacLennan DH, Kranias EG (2003) Phospholamban: a crucial regulator of cardiac contractility. Nat Rev Mol Cell Biol 4:566–577. doi:10.1038/nrm1151
Marx SO, Reiken S, Hisamatsu Y, Jayaraman T, Burkhoff D, Rosemblit N, Marks AR (2000) PKA phosphorylation dissociates FKBP12.6 from the calcium release channel (ryanodine receptor): defective regulation in failing hearts. Cell 101(4):365–376. doi:10.1016/S0092-8674(00)80847-8
Ono K, Yano M, Ohkusa T, Kohno M, Hisaoka T, Tanigawa T, Kobayashi S, Matsuzaki M (2000) Altered interaction of FKBP12.6 with ryanodine receptor as a cause of abnormal Ca(2+) release in heart failure. Cardiovasc Res 48:323–331. doi:10.1016/S0008-6363(00)00191-7
Maier LS, Bers DM (2007) Role of Ca2+/calmodulin-dependent protein kinase (CaMK) in excitation-contraction coupling in the heart. Cardiovasc Res 73:631–640. doi:10.1016/j.cardiores.2006.11.005
Kohlhaas M, Zhang T, Seidler T, Zibrova D, Dybkova N, Steen A, Wagner S, Chen L, Brown JH, Bers DM, Maier LS (2006) Increased sarcoplasmic reticulum calcium leak but unaltered contractility by acute CaMKII overexpression in isolated rabbit cardiac myocytes. Circ Res 98:235–244. doi:10.1161/01.RES.0000200739.90811.9f
Wehrens XH, Lehnart SE, Reiken S, Vest JA, Wronska A, Marks AR (2006) Ryanodine receptor/calcium release channel PKA phosphorylation: a critical mediator of heart failure progression. Proc Natl Acad Sci USA 103:511–518. doi:10.1073/pnas.0510113103
Pieske B, Maier LS, Piacentino V 3rd, Weisser J, Hasenfuss G, Houser S (2002) Rate dependence of [Na+]i and contractility in nonfailing and failing human myocardium. Circulation 106:447–453. doi:10.1161/01.CIR.0000023042.50192.F4
Gray RP, McIntyre H, Sheridan DS, Fry CH (2001) Intracellular sodium and contractile function in hypertrophied human and guinea-pig myocardium. Pflugers Archiv 442:117–123. doi:10.1007/s004240000512
Despa S, Islam MA, Weber CR, Pogwizd SM, Bers DM (2002) Intracellular Na(+) concentration is elevated in heart failure but Na/K pump function is unchanged. Circulation 105:2543–2548. doi:10.1161/01.CIR.0000016701.85760.97
Valdivia CR, Chu WW, Pu J, Foell JD, Haworth RA, Wolff MR, Kamp TJ, Makielski JC (2005) Increased late sodium current in myocytes from a canine heart failure model and from failing human heart. J Mol Cell Cardiol 38:475–483. doi:10.1016/j.yjmcc.2004.12.012
Wagner S, Dybkova N, Rasenack EC, Jacobshagen C, Fabritz L, Kirchhof P, Maier SK, Zhang T, Hasenfuss G, Brown JH, Bers DM, Maier LS (2006) Ca2+/calmodulin-dependent protein kinase II regulates cardiac Na+ channels. J Clin Invest 116:3127–3138. doi:10.1172/JCI26620
Sossalla S, Wagner S, Rasenack EC, Ruff H, Weber SL, Schondube FA, Tirilomis T, Tenderich G, Hasenfuss G, Belardinelli L, Maier LS (2008) Ranolazine improves diastolic dysfunction in isolated myocardium from failing human hearts—role of late sodium current and intracellular ion accumulation. J Mol Cell Cardiol 45:32–43. doi:10.1016/j.yjmcc.2008.03.006
Fredj S, Lindegger N, Sampson KJ, Carmeliet P, Kass RS (2006) Altered Na+ channels promote pause-induced spontaneous diastolic activity in long QT syndrome type 3 myocytes. Circ Res 99:1225–1232. doi:10.1161/01.RES.0000251305.25604.b0
Mulieri LA, Hasenfuss G, Leavitt B, Allen PD, Alpert NR (1992) Altered myocardial force-frequency relation in human heart failure. Circulation 85:1743–1750
Hasenfuss G, Holubarsch C, Hermann HP, Astheimer K, Pieske B, Just H (1994) Influence of the force-frequency relationship on haemodynamics and left ventricular function in patients with non-failing hearts and in patients with dilated cardiomyopathy. Eur Heart J 15:164–170
Pieske B, Sutterlin M, Schmidt-Schweda S, Minami K, Meyer M, Olschewski M, Holubarsch C, Just H, Hasenfuss G (1996) Diminished post-rest potentiation of contractile force in human dilated cardiomyopathy. Functional evidence for alterations in intracellular Ca2+ handling. J Clin Invest 98:764–776. doi:10.1172/JCI118849
Fox K, Ford I, Steg PG, Tendera M, Robertson M, Ferrari R (2008) Heart rate as a prognostic risk factor in patients with coronary artery disease and left-ventricular systolic dysfunction (BEAUTIFUL): a subgroup analysis of a randomised controlled trial. Lancet 372:817–821. doi:10.1016/S0140-6736(08)61171-X
Ozdemir S, Bito V, Holemans P, Vinet L, Mercadier JJ, Varro A, Sipido KR (2008) Pharmacological inhibition of na/ca exchange results in increased cellular Ca2+ load attributable to the predominance of forward mode block. Circ Res 102:1398–1405. doi:10.1161/CIRCRESAHA.108.173922
Neary P, Duncan AM, Cobbe SM, Smith GL (2002) Assessment of sarcoplasmic reticulum Ca(2+) flux pathways in cardiomyocytes from rabbits with infarct-induced left-ventricular dysfunction. Pflugers Archiv 444:360–371. doi:10.1007/s00424-002-0794-0
Mason CA, Ferrier GR (1999) Tetracaine can inhibit contractions initiated by a voltage-sensitive release mechanism in guinea-pig ventricular myocytes. J Physiol 519(Pt 3):851–865. doi:10.1111/j.1469-7793.1999.0851n.x
Wehrens XH, Lehnart SE, Reiken S, van der Nagel R, Morales R, Sun J, Cheng Z, Deng SX, de Windt LJ, Landry DW, Marks AR (2005) Enhancing calstabin binding to ryanodine receptors improves cardiac and skeletal muscle function in heart failure. Proc Natl Acad Sci USA 102:9607–9612. doi:10.1073/pnas.0500353102
Yano M, Kobayashi S, Kohno M, Doi M, Tokuhisa T, Okuda S, Suetsugu M, Hisaoka T, Obayashi M, Ohkusa T, Matsuzaki M (2003) FKBP12.6-mediated stabilization of calcium-release channel (ryanodine receptor) as a novel therapeutic strategy against heart failure. Circulation 107:477–484. doi:10.1161/01.CIR.0000044917.74408.BE
Doi M, Yano M, Kobayashi S, Kohno M, Tokuhisa T, Okuda S, Suetsugu M, Hisamatsu Y, Ohkusa T, Matsuzaki M (2002) Propranolol prevents the development of heart failure by restoring FKBP12.6-mediated stabilization of ryanodine receptor. Circulation 105:1374–1379. doi:10.1161/hc1102.105270
Reiken S, Wehrens XH, Vest JA, Barbone A, Klotz S, Mancini D, Burkhoff D, Marks AR (2003) Beta-blockers restore calcium release channel function and improve cardiac muscle performance in human heart failure. Circulation 107:2459–2466. doi:10.1161/01.CIR.0000068316.53218.49
Okuda S, Yano M, Doi M, Oda T, Tokuhisa T, Kohno M, Kobayashi S, Yamamoto T, Ohkusa T, Matsuzaki M (2004) Valsartan restores sarcoplasmic reticulum function with no appreciable effect on resting cardiac function in pacing-induced heart failure. Circulation 109:911–919. doi:10.1161/01.CIR.0000115526.92541.D2
Lyon AR, Sato M, Hajjar RJ, Samulski RJ, Harding SE (2008) Gene therapy: targeting the myocardium. Heart (British Cardiac Society) 94:89–99. doi:10.1136/hrt.2007.116483
Acknowledgments
This work was supported by funds from the Deutsche Forschungsgemeinschaft (DFG) Grant KFO 155 (to S.E.L.: TP4 LE 1313/2-1; to L.S.M.: TP5; to G.H.: TP1), the American Heart Association (to S.E.L.), the Alfried Krupp von Bohlen and Halbach Foundation (to S.E.L.), by the European Commission FP6 project grant EUGeneHeart (to G.H.). L.S.M. is funded by the DFG Heisenberg Program, the German Society for Cardiology, and by the Fondation Leducq. The authors apologize to all colleagues if their work could not be represented adequately in this review due to space limitations.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Lehnart, S.E., Maier, L.S. & Hasenfuss, G. Abnormalities of calcium metabolism and myocardial contractility depression in the failing heart. Heart Fail Rev 14, 213–224 (2009). https://doi.org/10.1007/s10741-009-9146-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-009-9146-x