Abstract
The heterogeneous nature of multiple sclerosis (MS) and the unavailability of treatments addressing its intricate network and reversing the disease state is yet an area that needs to be elucidated. Liraglutide, a glucagon-like peptide-1 analogue, recently exhibited intriguing potential neuroprotective effects. The currents study investigated its potential effect against mouse model of MS and the possible underlying mechanisms. Demyelination was induced in C57Bl/6 mice by cuprizone (400 mg/kg/day p.o.) for 5 weeks. Animals received either liraglutide (25 nmol/kg/day i.p.) or dorsomorphin, an AMPK inhibitor, (2.5 mg/Kg i.p.) 30 min before the liraglutide dose, for 4 weeks (starting from the second week). Liraglutide improved the behavioral profile in cuprizone-treated mice. Furthermore, it induced the re-myelination process through stimulating oligodendrocyte progenitor cells differentiation via Olig2 transcription activation, reflected by increased myelin basic protein and myelinated nerve fiber percentage. Liraglutide elevated the protein content of p-AMPK and SIRT1, in addition to the autophagy proteins Beclin-1 and LC3B. Liraglutide halted cellular damage as manifested by reduced HMGB1 protein and consequently TLR-4 downregulation, coupled with a decrease in NF-κB. Liraglutide also suppressed NLRP3 transcription. Dorsomorphin pre-administration indicated a possible interplay between AMPK/SIRT1 and NLRP3 inflammasome activation as it partially reversed liraglutide’s effects. Immunohistochemical examination of Iba+ microglia emphasized these findings. In conclusion, liraglutide exerts neuroprotection against cuprizone-induced demyelination via anti-inflammatory, autophagic flux activation, NLRP3 inflammasome suppression, and anti-apoptotic mechanisms, possibly mediated, at least in part, via AMPK/SIRT1, autophagy, TLR-4/ NF-κB/NLRP3 signaling.
Graphical abstract

The potential mechanistic insight of Lira in alleviating Cup-induced neurotoxicity via: (1) AMPK/SIRT1 pathways activation resulting in the stimulation of brain autophagy flux (confirmed by lowering Beclin-1 and LC3-B protein expression). (2) Inhibition of NLRP3 inflammasome activation, as evidenced by reduced HMGB1, TLR-4, NF-κB and NLRP3 protein expression, alongside diminishing the activation of its downstream cascade as reflected by reduced levels of caspase-1 and IL-1β protein expression. (3) A possible modulating interplay between the previously mentioned two pathways.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multiple sclerosis (MS) is a neurodegenerative disease of the central nervous system (CNS) featured by chronic cardinal progressive immune-mediated neuro-inflammatory events that lead to neuronal demyelination, loss of myelin-producing oligodendrocytes (OLGs), and eventually nerve fibers destruction (Khan et al. 2014). Nowadays, MS is manifested as the most prevalent cause of non-traumatic progressive neurological disabilities in youth—about 2.3 million affected individuals globally (Browne et al. 2014)—impairing movement, sensory functions and cognition (Omotoso et al. 2018; Zidan et al. 2018). The currently available treatments mostly target the manipulation of immune response although improving oligodendrocyte progenitor cells (OPCs) differentiation into mature myelin-producing OLGs, which is a crucial step in reversing the degeneration by re-myelination, is an emerging yet elusive therapeutic strategy (Kremer et al. 2016; Plemel et al. 2017).
Sirtuin 1 (SIRT1), a histone deacetylase-Sirtuin family member, is a key modulator of the inflammatory responses. SIRT1 suppresses immunoinflammation via nuclear factor-κB (NF-κB) expression attenuation (Matsushita et al. 2013). The AMP-activated protein kinase (AMPK) is a critical regulator of mitochondrial energy homeostasis (Largani et al. 2019). AMPK exerts anti-inflammatory activity in a SIRT1-dependent manner (Peixoto et al. 2017). Additionally, AMPK and SIRT1 mutually modulate each other showing synergistic activity (Lan et al. 2008). Previous studies elucidated that the AMPK/SIRT1 pathway mediates neuroprotection, partially, through inducing the autophagy machinery hence suppressing cellular damage and apoptotic processes especially via mitochondrial-specific autophagy (mitophagy) (Jin et al. 2014; Yan et al. 2017; Kruppa et al. 2018). In this context, cuprizone (Cup), a copper chelator, has been reported to exert a reproducible neurotoxicity that results from perpetuating mitochondrial energy homeostasis (Zatta et al. 2005) and copper-dependent enzymes inhibition (Messori et al. 2007). Accordingly, it generates a drastic metabolic oxidative stress leading to apoptosis of OLGs, microgliosis and astrogliosis (Hillis et al. 2016).
Nucleotide-binding and oligomerization domain-like receptors-pyrin domain-containing protein 3 (NLRP3) inflammasome is damage motifs sensitive cytosolic protein complex that is expressed by phagocytes including macrophages and dendritic cells (Guo et al. 2015). They are essential part of the protective innate immune response, on the other hand, their over-activation is a key factor in multiple neurodegenerative diseases including MS through copious inflammatory cytokines production including interleukin-1β (IL-1β) and IL-18 (Swanson et al. 2019). IL-1β, a profound mature inflammatory cytokine processed by inflammasomes in microglia, has a pivotal role in cell death and the disturbance of blood–brain barrier integrity (Schrijver et al. 2003; Wang et al. 2014). Noteworthy, targeting NLRP3 inflammasome is an emerging strategy in manipulating MS (Shao et al. 2018).
Data suggest that a cross-talk between AMPK/SIRT1 and NLRP3 inflammasome pathways may occur through NF-κB modulation and/or mitigating mitochondrial damage via mitochondrial reactive oxygen species (mtROS) (Yan et al. 2017; Zou et al. 2018). Furthermore, previous studies revealed that AMPK activation may have a suppressive activity on Toll-like receptor-4 (TLR-4) expression, subsequently attenuating NLRP3 activation (Soraya et al. 2012, 2014). The previous findings cast light on targeting both AMPK/SIRT1 and NLRP3 as an outstanding strategy in the treatment of MS.
Liraglutide (Lira) is a glucagon-like peptide-1 (GLP-1) analogue that is characterized by a high amino acid sequence similarity, 97%, with the human GLP-1. It’s approved for type-2 diabetes mellitus, as a once-daily antidiabetic agent, without hypoglycemic side effects (Jacobsen et al. 2016). Its kinetic properties allow it to pass the blood–brain barrier and subsequently activate the widely distributed GLP-1 receptors (GLP-1R) in the brain (Hunter and Hölscher 2012; McGovern et al. 2012; Cork et al. 2015). Previous studies have reported some neuroprotective effects of Lira in animal models of Alzheimer’s disease (Hansen et al. 2016), Parkinson’s disease (Badawi et al. 2017), cognitive impairment (Liu et al. 2020), cerebral ischemia (Briyal et al. 2014), and diabetic peripheral neuropathy (Moustafa et al. 2018a, b).
The Cup model is a widely used mouse model imitating demyelination–re-myelination events in different brain regions (Klein et al. 2018). Therefore, we hypothesized that Lira has a possible neuroprotective effect against the Cup demyelinating model and a potential to induce re-myelination, suggesting its dual benefit for MS patients with diabetic co-morbidity. Herein, we focused on AMPK/SIRT1 and NLRP3 inflammasome pathways as well as the subsequent defective autophagy, inflammation, and apoptosis.
Materials and methods
Animals
This in-vivo study utilized male C57Bl/6 mice (8–10 weeks old, 20–25 g in weight). Mice were kept in the animal facility of the Faculty of Pharmacy, The British University in Egypt (BUE) (Cairo, Egypt) 1 week before the start of the experiment. They were maintained under standard conditions of five mice per cage and 12/12 h light/dark cycle (with lights on at 6 am) at a constant temperature (23 ± 2 °C). Animals were allowed free access to standard chow diet and water ad libitum. The experiment followed the guidelines of the animal facility and the experimental protocol was approved by the ethical committees at the British University in Egypt (Approval No. EX-1901, September 2019) and the faculty of pharmacy, Cairo University (Approval No. PT-2421, April 2019).
Drugs
Cuprizone (Bis (cyclohexanone) Oxaldihydrazone) and dorsomorphin (Dorso) (6-[4-(2-Piperidin-1-ylethoxy) phenyl]-3-pyridin-4-ylpyrazolo [1, 5-a]pyrimidine) were purchased from Sigma–Aldrich Co. USA. Liraglutide was acquired from Novo Nordisk pharmaceutical company, USA. Any other chemical used was of analytical grade with the highest purity.
Demyelination induction
Cuprizone suspension was prepared by mixing the powder with 0.1% methylcellulose (MC) and vortexed to obtain a homogenous suspension. Animals received Cup (400 mg/kg/day p.o) using oral gavage throughout a period of 5 weeks to induce acute demyelination (Zhen et al. 2017).
Experimental design and study time scale
Animals were assigned randomly into four groups (n = 15); thereafter they were subjected to the following treatments: (i) Normal control group: received 0.1% MC (10 ml/kg p.o.) (Zhen et al. 2017). (ii) Positive control group: received daily oral Cup suspension as described before. (iii) Liraglutide-treated group: received Cup + Lira (25 nmol/kg/day i.p.) for 4 weeks. (iv) Liraglutide and Dorso-treated group: received Cup + Lira + Dorso (2.5 mg/kg i.p.) 30 min right before Lira injection and it was dissolved with normal saline (Lee et al. 2019). A power analysis of power = 0.8 and α = 0.05 was performed to determine the group size with an effect size used previously by Elbaz et al. (2018).
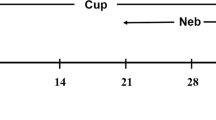
Treatment with Lira and Dorso was introduced at the second week of the regimen and continued for 4 weeks. This design is illustrated in Fig. 1. Liraglutide dose has been selected as it was reported to have a neuroprotective effect in previous animal studies (Hunter and Hölscher 2012; McClean and Hölscher 2014).
Behavioral assessments were conducted 24 h after the last dose injection. Eventually, animals were euthanized by decapitation under light anesthesia; afterwards, the whole-brain tissues were rapidly excised and weighed. Within each group, tissues were randomly divided into two subsets: one for histopathological examination and immunohistochemical analysis (n = 3) and the other for the investigation of biochemical parameters (n = 12).
Behavioral studies
Animals’ locomotor and motor coordination activities were assessed using open field test (OFT), rotarod and grip strength tests. Worthy of note, behavioral tests were performed with a minimum of 30 min rest interval in between and during animals’ light cycle to avoid any discrepancies due to circadian changes.
Open field test
Animals were allocated centrally in a square white wooden box arena, 40 × 40 × 25 cm, illuminated by white dim light, and allowed free uninterrupted movement. The testing apparatus was cleaned using 70% ethanol between subjects to eliminate any bias by left odors. The locomotor activity of each mouse was recorded within a noise-attenuated room for 3 min period, tracked and analyzed via ANY-maze software (version 6.0, Stoelting Co., Wood Dale, USA). The test arena was virtually divided into (4 × 4 cm) 16 equal squares and locomotor parameters including distance traveled, mean speed, mobility time, ambulation frequency (line crossings) and rearing frequency for each animal were assessed (Walsh and Cummins 1976; Keller et al. 2018).
Rotarod test
Assessment of motor coordination was performed using a standard rotarod apparatus (rotating at 25 rpm around a 3-cm diameter rod). At first, mice were allowed to acclimatize to maintain their posture on the rotating rod through three 5 min-training sessions on three consecutive days. After assessing the locomotor activity via open field test, animals were placed on the rotating rod and the time each mouse took before falling off the rod was determined as the latency period with a maximum cut-off value of 300 s (Jones and Roberts 2011; Gilli et al. 2016).
String test
String test has been used as a method to assess grip strength implicating the neuromuscular function (Brooks and Dunnett 2009; Takeshita et al. 2017). Mice were allowed to hang on a horizontal steel wire (35 cm in length and 2 mm in diameter) by their forelimbs. The latency period through which each mouse was hanging on the wire before losing grip was recorded (Cut-off value 3 min).
Sample preparation
Brain tissues were collected, rinsed with ice-cold phosphate buffered saline (PBS) to remove any blood residues, and dissected into two hemispheres through the midline. Then, tissues were immersed in liquid nitrogen to snap freeze and stored at − 80 °C till the analysis of the biochemical parameters. Brain hemispheres were homogenized with radioimmunoprecipitation assay (RIPA) buffer (25 mM Tris–HCl pH 7.6, 150 mM NaCl, 1% NP-40, 1% sodium deoxycholate, 0.1% SDS) and protease and phosphatase inhibitor cocktail (Pierce, ThermoFisher Scientific, USA) for protein extraction, and the homogenate was then constantly agitated for 1 h at 4 °C. The mixture was centrifuged for 30 min at 12,000 rpm at 4 °C and the supernatant was aspirated and stored at − 80 °C. Total protein content was quantified using bicinchoninic acid protein quantification kit (ThermoFisher Scientific, USA, Catalogue No. 23225). Protein extracts were used for western blot analysis and enzyme-linked immunosorbent assay (ELISA).
Biochemical analysis
Determination of brain p-AMPK, HMGB1, NF-κB, NLRP3, Caspase-1, and IL-1β via enzyme-linked immunosorbent assay
Mouse p-AMPK (Thr 172) (Catalogue No. MBS7230575, My BioSource, USA), NF-κB (P65) (Catalogue No. MBS775083, My BioSource, USA), high mobility group box protein-1 (HMGB1, catalogue No. CSB-E08224r, CUSABIO Technology LLC, China,), NLRP3 (Catalogue No. LS-F39627, LSBio, USA), caspase-1 (Catalogue No. NBP2-75014, Novus Biologicals, USA) and IL-1β (Catalogue No. MLB00C, R&D systems, USA) protein expression were determined and quantified using ELISA kits according to the manufacture’s protocol.
Western blot analysis of SIRT1, TLR-4, MBP, Olig2, and autophagy biomarkers (Beclin-1 and LC3B) protein expression
Equal amounts of protein samples (30 μg) were allowed to separate on 4–20% Precast polyacrylamide (SDS–PAGE) gels (ThermoFisher Scientific, USA). Thereafter, into a nitrocellulose membranes (Optitran®, Whatman), the separated proteins were transferred. Following the transfer, the nitrocellulose membranes were washed with 1X Tris Buffered Saline (1X TBS) and then blocked with 3% milk in 1X TBS for 1 h at room temperature. Subsequently, membranes were incubated overnight at 4 °C with the recommended dilutions of primary antibodies against SIRT1 (Catalogue No. MA5-32912), myelin basic protein (MBP, Catalogue No. MA5-27818), Olig2 (Catalogue No. P21954), Beclin-1 (Catalogue No. PA5-20171), and LC-3B (Catalogue No. PA5-85081) from ThermoFisher Scientific (USA) as well as TLR-4 (Catalogue No. 14358S) and GAPDH (Catalogue No. 2118) from Cell Signaling (USA). After washing with 0.1% tween in TBS, membranes were incubated with the corresponding peroxidase-labeled secondary antibodies at room temperature for 1 h. Finally, the protein-antibody complexes were visualized using enhanced chemiluminescent horseradish peroxidase (HRP) substrate (SuperSignal West Pico plus Chemiluminescent, ThermoFisher Scientific, USA) by scanning the membrane for chemiluminescent bands at the expected molecular weight of the protein via C-DIGIT® blot Scanner (Li-Cor Biosciences, USA). The protein bands density was finally analyzed using Image studio digits software version 5.0 (Li-Cor Biosciences, USA) and the results were then normalized with GAPDH protein expression.
Histopathological examination
Using 10% neutral buffered formalin, whole-brain tissues were fixed for 72 h. Afterwards, brain tissue samples were processed in serial dilutions of ethanol (100–95%), cleared in xylene and embedded into Paraplast tissue embedding media. Five-micron thick sagittal brain sections were cut from the paraffin tissue blocks by rotatory microtome. Then, the processed tissue sections were deparaffinized and stained with Harris Hematoxylin and Eosin (H&E) stain for general tissue examination, in addition to Luxol fast blue (LFB) for evaluation of myelinated nerve fibers percentage in corpus callosum regions from different samples of all groups. Samples fixation and processing were applied according to (Culling 2013). The histopathological examination was performed by an experienced investigator who was blinded to samples’ identity to eliminate any bias in the results.
Immunohistochemical assessment of Iba+ microglial cells
Unstained deparaffinized 5 μm-thick brain tissue sections were cut and processed with 3% hydrogen peroxide for 20 min, washed by PBS, and incubated with ionized calcium-binding adaptor molecule 1 (Iba-1) primary antibody (Abcam, USA, Catalogue No. ab108539) overnight at 4 °C after 1:100 dilution. HRP performed complex and 3,3̀-diaminobenzidine (DAB) were used for detection of Iba+ microglia according to manufacturer’s instructions (Dako, Denmark). After washing by PBS, tissue slides were counter-stained with hematoxylin for microscopic analysis. Micrographs were captured by Full HD microscopic camera processed by Leica application module (Leica Microsystems GmbH, Wetzlar, Germany). The immunohistochemical examination was performed by an experienced investigator who was blinded to samples’ identity to eliminate any bias in the results.
Statistical analysis
A Shapiro–Wilk test was performed to check for the normality of distribution of all parametric data sets. Data that passed the requirements for parametric criteria were then analyzed by one-way analysis of variance (one-way ANOVA) followed by Tukey–Kramer posts hoc statistical tests and presented as mean ± standard deviation (S.D.). However, data sets that did not meet the parametric requirements were analyzed using non-parametric Kruskal–Wallis ANOVA followed by Dunn’s post hoc statistical tests and presented as median and range. Data were analyzed and visualized using GraphPad Prism software (Version 9, San Diego, CA, USA). A cut-off value of less than 0.05 was accepted as a statistically significant P value level. Additionally, to confirm that, sample sizes had the sufficient power to detect a statistically significant effect, Mead’s “Resource Equation” was applied (Mead et al. 2012).
Results
Lira ameliorated cuprizone-induced behavioral abnormalities
Behavioral tests demonstrated that Cup administration resulted in a significant deterioration in the locomotor activity and motor coordination parameters compared to the normal control group as displayed in Fig. 2a & b. Treatment with Lira significantly reversed the behavioral changes as it depicted an increase in the total distance traveled by mice, mean speed, time being mobile, and rearing frequency (OFT test) reaching levels approximately 4-, 3-, 3- and 4-fold, respectively, greater than those in the cuprizone-treated group. Interestingly, Lira increased the retention time of animals on the rotating rod before falling (rotarod test) and the latency period the mice took hanging on the steel wire (string test) reaching approximately 5- and 8-fold the cuprizone-treated group values, respectively, compared to the Cup-treated group. Meanwhile, combining Lira with Dorso caused worsening in the behavioral parameters compared to the Lira-treated group.
Effect of Lira on Cup-induced alterations in locomotion & motor ability in C57Bl/6 mice through OFT, rotarod and string test. a Table of the behavioural analysis results. Each value represents the mean ± S.D. except for the rearing frequency, values represent the median and range of 12 mice in the open field arena. b Represents track plots showing the position of the centre of the mice in OFT test. Statistical significance between groups was detected using one-way ANOVA followed by Tukey–Kramer post hoc tests except for rearing frequency, which was analyzed using Kruskal–Wallis ANOVA followed by Dunn’s post hoc statistical tests. aSignificantly different from Normal group, bSignificantly different from Cup group, cSignificantly different from Cup + Lira group at P < 0.05
Lira reversed cuprizone-induced brain weight alterations
As shown in Fig. 3a, a significant reduction of 14.7% in brain weight was induced by Cup administration in comparison to normal control group. Whereas, Lira significantly increased the brain weight by 15% compared to the Cup group and almost maintained the brain weight compared to normal group. Combining Lira with Dorso decreased brain weight by 3% compared to Lira-treated group.
Effect of Lira on Cup-induced alterations in brain weight and brain myelination biomarkers of C57Bl/6 mice. Vertical bars represent the mean ± S.D. of 12 mice for a brain weight, as well as six mice for b MBP and c Olig2 relative protein expression. Values are statistically significant at P < 0.05 using one-way ANOVA followed by Tukey–Kramer post hoc tests
Lira improved cuprizone-induced alteration in the brain myelination status.
The percent of myelinated nerve fibers in different corpus callosum fields as well as MBP and Olig2 relative protein expression were measured to assess the effect of Lira administration on C57Bl/6 mice brain myelination status.
As shown in Fig. 4, Cup administration significantly evoked a defect in the myelination status of mice brain tissues, which is evidenced by the significant decrease in the percentage of myelinated nerve fibers in different corpus callosum brain sections by 46.7%, as depicted by LFB-staining. In contrast, Lira treatment significantly increased the intensity of LFB-staining by 35% and consequently increased the percentage of myelinated nerve fibers in comparison to the Cup group. Worthy of note, Dorso co-administration reduced the percentage of myelinated nerve fibers in comparison to Lira-treated group.
Representative images showing the effect of Lira on Cup-induced deterioration in myelinated nerve fibers percentage. LFB-stained brain corpus callosum coronal sections (magnification, × 50) of: a Normal control group, b Cup-, c Lira-, d Lira + Dorso-treated groups LFB-staining intensities and e Bar chart for the percentage of myelinated nerve fibres in six random corpus callosum fields/tissue section. Vertical bars represent the mean ± S.D. of each group. Values are statistically significant at P < 0.05 using one-way ANOVA followed by Tukey–Kramer post hoc tests
Fig. 3a and b also shows that Lira administration significantly improved the myelination markers in C57Bl/6 mice brains as manifested by the increased levels of MBP and Olig2 relative protein expression reaching approximately 1.5- and 2-fold, respectively, compared to the Cup group. Interestingly, by combining Lira + Dorso, MBP protein expression significantly decreased, while it showed almost the same level of Olig2 in comparison to the Lira-treated group.
Lira activated AMPK/SIRT1 pathway in cuprizone-induced neurotoxicity
Fig. 5a and b presents the experimental data where Cup administration showed a marked reduction in p-AMPK and SIRT1 levels by 53.6 and 68.8%, respectively, compared to normal control group. Interestingly, Lira almost normalized p-AMPK and SIRT1, when compared with normal control group. In addition, it caused a significant augmentation in both proteins expression reaching approximately 2- and 3-fold, respectively, when compared to the Cup-treated group. On the other hand, combining Lira + Dorso was able to partially block Lira-induced stimulation of p-AMPK/SIRT1 proteins as confirmed by the significant reduction of p-AMPK and SIRT1 by 28.9 and 51.1%, respectively, when compared to Lira-treated rats.
Effect of Lira on brain p-AMPK/SIRT1 and autophagy biomarkers in Cup-induced demyelination in C57Bl/6 mice. Vertical bars represent the mean ± S.D. of six mice for a p-AMPK level, b SIRT1, c Beclin-1 and d LC3B (II/I) relative protein expression. Values are statistically significant at P < 0.05 using one-way ANOVA followed by Tukey–Kramer post hoc tests
Lira augmented autophagic flux in cuprizone-induced demyelination
To investigate the effect of Lira administration on C57Bl/6 mice brain autophagy, Beclin-1 and LC3B proteins expression was measured. As presented in Fig. 5c & d, Cup administration inhibited the autophagy pathway as manifested by the reduction of Beclin-1 and LC3B-B (II/I ratio) proteins expression by nearly 2- and 3.3-fold, respectively, compared to normal control group. Lira treatment augmented the brain autophagy process as evidenced by the significant increase in the protein expression of both Beclin-1 and LC3B (II/I ratio) reaching levels approximately 3- and 6-fold, respectively, when compared to the Cup group. Meanwhile, co-administration of Dorso with Lira gave rise to a defect in brain autophagy, a finding that was confirmed by a concomitant decrease in both Beclin-1 and LC3B-B (II/I ratio) protein expression by 1.5- and 4.4-fold compared to Lira-treated group.
Lira inhibited NLRP3 inflammasome activation and OLGs apoptotic biomarkers in cuprizone-induced neurotoxicity
Cuprizone intoxication significantly evoked the protein expression of HMBG1 and upregulation of TLR-4, hence increased the expression of NF-κB (Fig. 6). Consequently, the NLRP3 downstream cascade proteins were highly expressed. Also, Cup augmented the apoptotic flux as evidenced by increasing the expression of caspase-1 and IL-1β by 2- and 1.5-fold, respectively, compared to normal mice. On the other hand, Lira was capable of curtaining the inflammation induced by Cup ingestion via NLRP3 inflammasome. In the Lira-treated group, HMGB1, TLR-4, NF-κB and NLRP3 proteins expression were decreased by 1.4-, 4.1-, 3- and 1.3-fold, respectively, compared to the Cup-treated group. Furthermore, Lira exhibited a suppression of the apoptotic process as depicted by the significant decrease in apoptotic biomarkers caspase-1 and IL-1β by 3- and 1.6-fold, respectively, less than that observed in Cup-treated group.
Effect of Lira on Cup-induced inflammation and apoptosis via NLRP3 inflammasome activation in C57Bl/6 mice. Vertical bars represent the mean ± S.D. of six mice for a HMGB1, b & c TLR-4, d NF-κB, e NLRP3, f caspase-1 and g IL-1β protein expression. Values are statistically significant at P < 0.05 using one-way ANOVA followed by Tukey–Kramer post hoc tests
Histopathologic evaluation of different brain coronal sections
According to Fig. 7, corpus callosum sections of normal control mice showed normal histological structures with normal myelinated nerve fibers and minimal abnormal glial cells infiltrates. The administration of Cup elicited focal regions of reactive astroglial and microglial cells infiltrates. Moreover, it showed moderate demyelination, vacuolization and axonal damage showing higher inter-axonal spaces all-over corpus callosum. Lira-treated corpus callosum sections presented a significant reduction in glial cells infiltrates with mild focal axonal demyelination. However, most of the fields showed intact and more organized morphological features. On the other hand, sections from Lira + Dorso-treated mice demonstrated almost the same histological records as Cup-treated sections.
Effect of Lira on histopathological alterations in Cup-induced neurotoxicity. Representative images of H&E stained brain corpus callosum sections of C57Bl/6 mice, (magnification, × 50). a Normal control group, b Cup-, c Lira- and d Lira + Dorso-treated groups. Black arrow indicates abnormal glial cells infiltrates, yellow arrow indicates astroglial and microglial cells infiltrates and red arrow indicates demyelination, vacuolization and axonal damage
Lira ameliorated cuprizone-induced microgliosis
To investigate the relative activation of microglial cells in brain corpus callosum sections, Anti-Iba-1 immunohistochemical staining was performed. According to Fig. 8, Cup-treated sections showed an elevated Iba-1 positive staining reaching approximately 8-fold compared to normal control. Interestingly, treatment with Lira was able to reduce the Iba+ stained microglial cells by 73.7% compared to the Cup-treated group. However, combing Lira + Dorso caused an increase in the number of Iba-1 positively stained microglia reaching 3-fold compared to the Lira-only treated group.
Effect of Lira on Cup-induced microgliosis. Representative images of anti-Iba-1 Immunohistochemical staining of brain corpus callosum sections of C57Bl/6 mice (magnification, × 50). a Normal control group, b Cup-, c Lira-, d Lira + Dorso-treated groups, and e Box plot chart for the count of active microglial cells that positively express Iba-1 in six random corpus callosum fields per tissue section. Vertical bars represent the median and range of each group. ( +) represents the mean. Values are statistically significant at P < 0.05 using Kruskal–Wallis ANOVA followed by Dunn’s post hoc statistical tests
Discussion
The current study divulged, for the first time, new mechanistic insights of the ameliorative effects of Lira on Cup-induced demyelination through the modulation of AMPK/SIRT1, autophagy flux, and NLRP3 inflammasome neuro-inflammatory pathways, and its potential effect to trigger neuronal re-myelination via OPCs differentiation induction (Greenberg and Jin 2006). Dorsomorphin, a pyrazolopyrimidine derivative immensely used as an AMPK inhibitor (Zhou et al. 2001), was used in the current work to investigate the involvement of P-AMPK/SIRT1 signaling in Lira-induced autophagy. Herein, Dorso was not able to abolish the neuroprotective effects of Lira completely, which implies that the neuroprotective effects of Lira involve not only AMPK-dependent but also AMPK-independent mechanisms.
There are several lines of evidence supporting the crucial role of GLP-1R in the growth and vitality of neuronal cells (Duarte et al. 2013; Hölscher 2014; Yildirim Simsir et al. 2018; Elbassuoni and Ahmed 2019). Moreover, GLP-1 knock-out mice showed impaired neuronal functions such as cognition, learning, and memory (Perry et al. 2003; Abbas et al. 2009). It was reported that GLP-1 has a pivotal effect in the stimulation of neuronal progenitor cells proliferation (During et al. 2003), an effect that is beneficial for the restoration of neuronal networks in different CNS diseases such as Alzheimer’s (Greenberg and Jin 2006; Hansen et al. 2016) and Parkinson’s diseases (Badawi et al. 2017; Safar et al. 2021). Indeed, the aforementioned data cast light on GLP-1R as an emerging potential target of new drug discovery in the treatment of MS.
Our findings depicted that, Cup was able to induce multiple behavioral and motor dysfunctions as observed in OFT, rotarod and string testing. These results are explained by the observed abnormally affected corpus callosum regions, in parallel to previous findings (Zhen et al. 2017; Zhang et al. 2020). Whereas, treatment with Lira reversed the impairments in animals’ behavioral profile in addition to histopathological abnormalities. Moreover, the findings were accompanied by a significant Cup-induced decrease in brain weight, which might be attributed to the reported ability of Cup to induce neuronal demyelination through the perturbation of brain mitochondrial metabolic state in mice (Matsushima and Morell 2001; Liu et al. 2010). Whereas, treatment with Lira amended Cup-induced reduction in brain weight, suggesting its potential repurposing in the treatment of MS. Moreover, Dorso has partially blocked the effect of Lira on motor and behavioral dysfunctions, as mice received Dorso showed better behavioral profiles but to a lesser extent than Lira-treated mice. On the other hand, Dorso failed to reverse Lira-induced normalized brain weight.
Myelin basic protein, is a main intrinsic component of the mature compacted myelin sheath covering the neuronal axons (Stinissen et al. 1998). It is well established as an indicative biomarker for the assessment of myelination status and re-myelination tendency (García-León et al. 2020). Herein, Cup administration caused demyelination as manifested by the profound reduction in MBP expression and hence myelin sheath loss, the major hallmark of MS, which lends support to previous reports (Clarner et al. 2012; Abd El Aziz et al. 2021). This finding is affirmed by LFB-staining of brain corpus callosum showing a reduced percentage of myelinated nerve fibers. Promisingly, the present study reveals the potential of Lira to hinder neuronal demyelination and its ability to stimulate re-myelination as Lira-treated group significantly restored Cup-deranged level of MBP sections (Carriel et al. 2017). Additionally, Lira treatment elevated the percentage of myelinated nerve fibers in brain corpus callosum sections. Furthermore, Dorso abated the effect of Lira treatment on myelination status as it showed a lower MBP level than the Lira-treated group, and almost blocked the protective effect of Lira on myelinated nerve fibers percent.
In parallel with re-myelination, Olig2, a master transcription factor, is believed to have a pivotal role in OPCs differentiation into mature myelin-producing OLGs (Szu et al. 2021). According to our results, Cup ingestion reduced OPCs re-myelination capacity through lowering Olig2 protein level, which emphasize previous findings (Zhan et al. 2020). However, Lira was able to restore the OPCs re-myelination ability via Olig2 transcription activation. On the contrary, administration of Dorso failed to significantly block the triggering effect of Lira on Olig2 protein expression. This reflects that Lira stimulates Olig2 via other multiple mechanisms. Results of brain weight, LFB-staining, MBP and Olig2 protein expression suggest that the mechanism by which Lira reverses Cup-induced neurotoxicity may be through its potential to induce re-myelination and prevent demyelination.
Upon activation of GLP-1R, it stimulates the phosphorylation of AMPK and activates the neuroprotective downstream signaling cascade (Carling et al. 2012). The current study clearly shows that Lira-treated group exhibited a significant increase in p-AMPK, which may explain the significant up-regulatory effect of Lira on SIRT1 suppression triggered by Cup intoxication (Peixoto et al. 2017). Previous research supports these findings (Elbaz et al. 2018; Houshmand et al. 2019), which revealed that Cup ingestion induced neurotoxicity via suppressing p-AMPK/SIRT1 markers. Moreover, Lira-modulatory effect is affirmed by Dorso co-administration as Lira + Dorso group showed significantly lower levels of p-AMPK and SIRT1 than Lira-treated group.
In line with its activation effect on AMPK/SIRT1 pathway, Lira markedly enhanced the autophagy machinery as verified by a significant increment in the autophagy biomarkers Beclin-1 and LC3B levels (Misrielal et al. 2020). In contrast, Cup was able to diminish the autophagic flux as shown in the reduced levels of Beclin-1 and LC3B, similar to what was formerly demonstrated (Dasgupta et al. 2013; Zhang et al. 2020). Based on the premise that autophagy activation participate in the regulation of mitochondrial homeostasis and neuroprotection (Kruppa et al. 2018; Misrielal et al. 2020), our findings depicted the suppressive effect of Lira on neuroinflammation through abolishing the Cup-induced mitochondrial damage and cellular debris via autophagy augmentation. This result is confirmed by the co-administration of Dorso as it lowered Beclin-1 and LC3B protein expression. Additionally, this may explain the significant decrement in HMGB1 level, as one of the most powerful damage-associated molecular patterns (DAMPs) (Shi et al. 2018), in Lira-treated group. In this context, we hypothesized that Lira may indirectly mitigate the activation of TLR-4 and subsequently NLRP3 inflammasomes via autophagy activation.
It is well established that Cup administration induces detrimental metabolic oxidative stress and primary OLGs apoptosis. A state that subsequently increases microglial activation and microgliosis significantly (Zatta et al. 2005; Blakemore and Franklin 2008; Hillis et al. 2016). It goes along with our results, as the Cup-treated group showed highly expressed Iba-1 in immunohistochemical pictures. However, Lira was able to mitigate the pathologic microgliosis as it showed a lower Iba-1 level.
The canonical NLRP3 activation is primed by the recognition of several DAMPs by the aid of pattern recognition receptors such as Toll-like receptors (TLRs) (Yuan et al. 2018). High mobility group box protein-1, a non-histone DNA-chaperone protein, is a key transcriptional modulator. It is released to the extracellular environment from the activated macrophages, monocytes, dendritic cells as well as apoptotic OLGs (Malhotra et al. 2015). Being a powerful DAMP, HMGB1 is detected by the surface TLR-4 and upregulates the transcription and activation of the inflammatory cytokine NF-κB. Thereafter, triggering NF-κB leads to the overexpression of inflammasome-related components such as NLRP3, pro-caspase-1, pro-IL-1β and pro-IL-18 as well (Agostini et al. 2004; Harris et al. 2011). Following the priming step, NLRP3 protein forms a heterogeneous oligomer with apoptosis-associated spec-like protein. Such oligomer, in turn, catalyzes the proteolysis of pro-caspase-1 into active caspase-1. This further gives rise to the formation and release of mature IL-1β and IL-18 (Ito et al. 2015; Birnbaum et al. 2018).
Cuprizone intoxication was able to provoke a heightened state of inflammation and apoptosis through elevating caspase-1 and IL-1β in brain tissue that is reflected in the histopathological pictures herein (Jha et al. 2010). The observed significant increase in HMGB1 in the Cup-treated group is attributed to the activation of immune cells and apoptotic OLGs, which is consistent with previous findings (Malhotra et al. 2015). In parallel, this was associated with upregulation of TLR-4 expression (Shi et al. 2018). The activation of GLP-1 resulted in inhibition of TLR-4 expression by the tested macrophages (Dai et al. 2014). More importantly, the current study shows the anti-inflammatory action of Lira via preventing Cup-induced overexpression of HMGB1 and TLR-4, indirectly and directly, respectively. Hence, it promisingly ameliorates the concomitant increases in NF-κB expression. These findings are in accordance with the literature data, which clearly showed that the activation of upregulated TLR-4 by overly expressed HMGB1 is assumed to trigger several cell responses. It markedly increased NF-κB level (Shi et al. 2018), as demonstrated in the Cup-treated group in our study. Accordingly, it may elucidate the overexpression of NLRP3, activated caspase-1 and activated IL-1β, as a downstream cascade, following Cup intoxication.
According to our findings, Lira treatment markedly attenuated the activation and release of the inflammatory cytokines such as caspase-1 and IL-1β via mitigating the Cup-induced NLRP3 overexpression. Indeed, IL-1β has been recognized as a significant contributor to the cellular apoptosis cascade (Cai et al. 2004; Prins et al. 2013). Therefore, the observed suppressive effect of Lira on IL-1β may contribute to its anti-apoptotic effect and consequently its anti-inflammatory effect.
Accumulating body of evidence presumed that both HMGB1/TLR-4 and AMPK/SIRT1 cascades tightly control NF-κB, which is a crucial transcriptional regulator of neuroinflammation (Liu et al. 2017). Moreover, previous studies reported the suppressive effect of both SIRT1 on NF-κB (Kuhlmann et al. 2008) and AMPK on TLR-4 expression (Soraya et al. 2012, 2014). In line with this, the current study depicted that Lira can mitigate neuroinflammation in Cup-treated mice through NLRP3 inflammasomes modulation both directly via GLP-1R and indirectly via AMPK/SIRT1 and autophagy, a finding that is verified by Dorso administration. Herein, Lira neuroprotective effect is partially abolished by pre-treatment with Dorso as it presented a significant decrement in HMGB1, TLR-4, and NF-κB levels in addition to NLRP3 expression and its downstream cascade, caspase-1, and IL-1β.
Conclusion
In the current study, Lira exhibited neuroprotective effects against Cup-induced MS. The findings showed that Lira was able to restore the impaired behavioral and motor functions in Cup-treated mice. In addition, it revealed that Lira could activate autophagy, curtain inflammation, and suppress apoptosis. The current study also substantiates the possible interplay between AMPK/SIRT1, autophagy, and NLRP3 inflammasomes pathways and their role in the potential anti-inflammatory neuroprotective effect of Lira. At last, this study offers a new perspective for the use of Lira as a promising candidate in the management of MS and ameliorating its pathological consequences, especially for diabetic patients who suffer from multiple sclerosis co-morbidity. However, further investigations for its beneficial effects on humans through clinical trials are still needed.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Abbas T, Faivre E, Hölscher C (2009) Impairment of synaptic plasticity and memory formation in GLP-1 receptor KO mice: interaction between type 2 diabetes and Alzheimer’s disease. Behav Brain Res 205:265–271
Abd El Aziz AE, Sayed RH, Sallam NA, El Sayed NS (2021) Neuroprotective effects of telmisartan and nifedipine against cuprizone-induced demyelination and behavioral dysfunction in mice: roles of NF-κB and Nrf2. Inflammation 44:1629–1642. https://doi.org/10.1007/s10753-021-01447-6
Agostini L, Martinon F, Burns K et al (2004) NALP3 forms an IL-1β-processing inflammasome with increased activity in Muckle-Wells autoinflammatory disorder. Immunity 20:319–325. https://doi.org/10.1016/S1074-7613(04)00046-9
Badawi GA, Abd El Fattah MA, Zaki HF, El Sayed MI (2017) Sitagliptin and liraglutide reversed nigrostriatal degeneration of rodent brain in rotenone-induced Parkinson’s disease. Inflammopharmacology 25:369–382. https://doi.org/10.1007/s10787-017-0331-6
Birnbaum Y, Bajaj M, Yang HC, Ye Y (2018) Combined SGLT2 and DPP4 inhibition reduces the activation of the Nlrp3/ASC inflammasome and attenuates the development of diabetic nephropathy in mice with type 2 diabetes. Cardiovasc Drugs Ther 32:135–145. https://doi.org/10.1007/s10557-018-6778-x
Blakemore WF, Franklin RJM (2008) Remyelination in experimental models of toxin-induced demyelination. In: Rodriguez M (ed) Current topics in microbiology and immunology. Springer, Berlin Heidelberg, Berlin, Heidelberg, pp 193–212
Briyal S, Shah S, Gulati A (2014) Neuroprotective and anti-apoptotic effects of liraglutide in the rat brain following focal cerebral ischemia. Neuroscience 281:269–281. https://doi.org/10.1016/j.neuroscience.2014.09.064
Brooks SP, Dunnett SB (2009) Tests to assess motor phenotype in mice: a user’s guide. Nat Rev Neurosci 10:519–529. https://doi.org/10.1038/nrn2652
Browne P, Chandraratna D, Angood C et al (2014) Atlas of multiple sclerosis 2013: a growing global problem with widespread inequity. Neurology 83:1022–1024. https://doi.org/10.1212/WNL.0000000000000768
Cai Z, Lin S, Pang Y, Rhodes PG (2004) Brain injury induced by intracerebral injection of interleukin-1beta and tumor necrosis factor-alpha in the neonatal rat. Pediatr Res 56:377–384. https://doi.org/10.1203/01.PDR.0000134249.92944.14
Carling D, Thornton C, Woods A, Sanders MJ (2012) AMP-activated protein kinase: new regulation, new roles? Biochem J 445:11–27. https://doi.org/10.1042/BJ20120546
Carriel V, Campos A, Alaminos M et al (2017) Staining methods for normal and regenerative myelin in the nervous system. Methods Mol Biol 1560:207–218. https://doi.org/10.1007/978-1-4939-6788-9_15
Clarner T, Diederichs F, Berger K et al (2012) Myelin debris regulates inflammatory responses in an experimental demyelination animal model and multiple sclerosis lesions. Glia 60:1468–1480. https://doi.org/10.1002/glia.22367
Cork SC, Richards JE, Holt MK et al (2015) Distribution and characterisation of Glucagon-like peptide-1 receptor expressing cells in the mouse brain. Mol Metab 4:718–731. https://doi.org/10.1016/j.molmet.2015.07.008
Culling CFA (2013) Handbook of histopathological and histochemical techniques, 3rd edn. Butterworth-Heinemann, London, UK
Dai Y, Dai D, Wang X et al (2014) DPP-4 inhibitors repress NLRP3 inflammasome and interleukin-1beta via GLP-1 receptor in macrophages through protein kinase C pathway. Cardiovasc Drugs Ther 28:425–432. https://doi.org/10.1007/s10557-014-6539-4
Dasgupta A, Zheng J, Perrone-Bizzozero NI, Bizzozero OA (2013) Increased carbonylation, protein aggregation and apoptosis in the spinal cord of mice with experimental autoimmune encephalomyelitis. ASN Neuro 5:e00111. https://doi.org/10.1042/AN20120088
Duarte AI, Candeias E, Correia SC et al (2013) Crosstalk between diabetes and brain: glucagon-like peptide-1 mimetics as a promising therapy against neurodegeneration. Biochim Biophys Acta - Mol Basis Dis 1832:527–541. https://doi.org/10.1016/j.bbadis.2013.01.008
During MJ, Cao L, Zuzga DS et al (2003) Glucagon-like peptide-1 receptor is involved in learning and neuroprotection. Nat Med 9:1173–1179. https://doi.org/10.1038/nm919
Elbassuoni EA, Ahmed RF (2019) Mechanism of the neuroprotective effect of GLP-1 in a rat model of Parkinson’s with pre-existing diabetes. Neurochem Int 131:104583. https://doi.org/10.1016/j.neuint.2019.104583
Elbaz EM, Senousy MA, El-Tanbouly DM, Sayed RH (2018) Neuroprotective effect of linagliptin against cuprizone-induced demyelination and behavioural dysfunction in mice: a pivotal role of AMPK/SIRT1 and JAK2/STAT3/NF-κB signalling pathway modulation. Toxicol Appl Pharmacol 352:153–161. https://doi.org/10.1016/j.taap.2018.05.035
García-León JA, García-Díaz B, Eggermont K et al (2020) Generation of oligodendrocytes and establishment of an all-human myelinating platform from human pluripotent stem cells. Nat Protoc 15:3716–3744. https://doi.org/10.1038/s41596-020-0395-4
Gilli F, Royce DB, Pachner AR (2016) Measuring progressive neurological disability in a mouse model of multiple sclerosis. J vis Exp 117:54616. https://doi.org/10.3791/54616
Greenberg DA, Jin K (2006) Neurodegeneration and neurogenesis: focus on Alzheimer’s disease. Curr Alzheimer Res 3:25–28. https://doi.org/10.2174/156720506775697106
Guo H, Callaway JB, Ting JPY (2015) Inflammasomes: mechanism of action, role in disease, and therapeutics. Nat Med 21:677–687. https://doi.org/10.1038/nm.3893
Hansen HH, Barkholt P, Fabricius K et al (2016) The GLP-1 receptor agonist liraglutide reduces pathology-specific tau phosphorylation and improves motor function in a transgenic hTauP301L mouse model of tauopathy. Brain Res 1634:158–170. https://doi.org/10.1016/j.brainres.2015.12.052
Harris J, Hartman M, Roche C et al (2011) Autophagy controls IL-1β secretion by targeting Pro-IL-1β for degradation. J Biol Chem 286:9587–9597. https://doi.org/10.1074/jbc.M110.202911
Hillis JM, Davies J, Mundim MV et al (2016) Cuprizone demyelination induces a unique inflammatory response in the subventricular zone. J Neuroinflammation 13:1–15. https://doi.org/10.1186/s12974-016-0651-2
Hölscher C (2014) Central effects of GLP-1: new opportunities for treatments of neurodegenerative diseases. J Endocrinol 221:T31–T41. https://doi.org/10.1530/JOE-13-0221
Houshmand F, Barati M, Golab F et al (2019) Metformin-induced AMPK activation stimulates remyelination through induction of neurotrophic factors, downregulation of NogoA and recruitment of Olig2+ precursor cells in the cuprizone murine model of multiple sclerosis. DARU, J Pharm Sci 27:583–592. https://doi.org/10.1007/s40199-019-00286-z
Hunter K, Hölscher C (2012) Drugs developed to treat diabetes, liraglutide and lixisenatide, cross the blood brain barrier and enhance neurogenesis. BMC Neurosci 13:4–9. https://doi.org/10.1186/1471-2202-13-33
Ito M, Shichita T, Okada M et al (2015) Bruton’s tyrosine kinase is essential for NLRP3 inflammasome activation and contributes to ischaemic brain injury. Nat Commun 6:1–11. https://doi.org/10.1038/ncomms8360
Jacobsen LV, Flint A, Olsen AK, Ingwersen SH (2016) Liraglutide in type 2 diabetes mellitus: clinical pharmacokinetics and pharmacodynamics. Clin Pharmacokinet 55:657–672. https://doi.org/10.1007/s40262-015-0343-6
Jha S, Srivastava SY, Brickey WJ et al (2010) The Inflammasome sensor, NLRP3, regulates CNS inflammation and demyelination via caspase-1 and interleukin-18. J Neurosci 30:15811–15820. https://doi.org/10.1523/JNEUROSCI.4088-10.2010
Jin X, Chen M, Yi L et al (2014) Delphinidin-3-glucoside protects human umbilical vein endothelial cells against oxidized low-density lipoprotein-induced injury by autophagy upregulation via the AMPK/SIRT1 signaling pathway. Mol Nutr Food Res 58:1941–1951. https://doi.org/10.1002/mnfr.201400161
Jones BJ, Roberts DJ (2011) The quantitative measurement of motor inco-ordination in naive mice using an accelerating rotarod. J Pharm Pharmacol 20:302–304. https://doi.org/10.1111/j.2042-7158.1968.tb09743.x
Keller SM, Doherty TS, Roth TL (2018) Pharmacological manipulation of dna methylation in adult female rats normalizes behavioral consequences of early-life maltreatment. Front Behav Neurosci 12:1–9. https://doi.org/10.3389/fnbeh.2018.00126
Khan N, Woodruff TM, Smith MT (2014) Establishment and characterization of an optimized mouse model of multiple sclerosis-induced neuropathic pain using behavioral, pharmacologic, histologic and immunohistochemical methods. Pharmacol Biochem Behav 126:13–27. https://doi.org/10.1016/j.pbb.2014.09.003
Klein B, Mrowetz H, Barker CM et al (2018) Age influences microglial activation after cuprizone-induced demyelination. Front Aging Neurosci 10:1–22. https://doi.org/10.3389/fnagi.2018.00278
Kremer D, Göttle P, Hartung HP, Küry P (2016) Pushing forward: remyelination as the new frontier in CNS diseases. Trends Neurosci 39:246–263. https://doi.org/10.1016/j.tins.2016.02.004
Kruppa AJ, Kishi-Itakura C, Masters TA et al (2018) Myosin VI-dependent actin cages encapsulate parkin-positive damaged mitochondria. Dev Cell 44:484–499. https://doi.org/10.1016/j.devcel.2018.01.007
Kuhlmann T, Miron V, Cuo Q et al (2008) Differentiation block of oligodendroglial progenitor cells as a cause for remyelination failure in chronic multiple sclerosis. Brain 131:1749–1758. https://doi.org/10.1093/brain/awn096
Lan F, Cacicedo JM, Ruderman N, Ido Y (2008) SIRT1 modulation of the acetylation status, cytosolic localization, and activity of LKB1: Possible role in AMP-activated protein kinase activation. J Biol Chem 283:27628–27635. https://doi.org/10.1074/jbc.M805711200
Largani SHH, Borhani-Haghighi M, Pasbakhsh P et al (2019) Oligoprotective effect of metformin through the AMPK-dependent on restoration of mitochondrial hemostasis in the cuprizone-induced multiple sclerosis model. J Mol Histol 50:263–271. https://doi.org/10.1007/s10735-019-09824-0
Lee YT, Lim SH, Lee B et al (2019) Compound C Inhibits B16–F1 tumor growth in a syngeneic mouse model via the blockage of cell cycle progression and angiogenesis. Cancers (basel) 11:823. https://doi.org/10.3390/cancers11060823
Liu L, Belkadi A, Darnall L et al (2010) CXCR2-positive neutrophils are essential for cuprizone-induced demyelination: relevance to multiple sclerosis. Nat Neurosci 13:319–326. https://doi.org/10.1038/nn.2491
Liu S, Jin Z, Zhang Y et al (2020) The glucagon-like peptide-1 analogue liraglutide reduces seizures susceptibility, cognition dysfunction and neuronal apoptosis in a mouse model of dravet syndrome. Front Pharmacol 11:1–17. https://doi.org/10.3389/fphar.2020.00136
Liu T, Zhang L, Joo D, Sun S-C (2017) NF-κB signaling in inflammation. Signal Transduct Target Ther 2:17023. https://doi.org/10.1038/sigtrans.2017.23
Malhotra S, Fissolo N, Tintoré M et al (2015) Role of high mobility group box protein 1 (HMGB1) in peripheral blood from patients with multiple sclerosis. J Neuroinflammation 12:48. https://doi.org/10.1186/s12974-015-0269-9
Matsushima GK, Morell P (2001) The neurotoxicant, cuprizone, as a model to study demyelination and remyelination in the central nervous system. Brain Pathol 11:107–116. https://doi.org/10.1111/j.1750-3639.2001.tb00385.x
Matsushita T, Sasaki H, Takayama K et al (2013) The overexpression of SIRT1 inhibited osteoarthritic gene expression changes induced by interleukin-1β in human chondrocytes. J Orthop Res 31:531–537. https://doi.org/10.1002/jor.22268
McClean PL, Hölscher C (2014) Liraglutide can reverse memory impairment, synaptic loss and reduce plaque load in aged APP/PS1 mice, a model of Alzheimer’s disease. Neuropharmacology 76:57–67. https://doi.org/10.1016/j.neuropharm.2013.08.005
McGovern SFJ, Hunter K, Hölscher C (2012) Effects of the glucagon-like polypeptide-1 analogue (Val8)GLP-1 on learning, progenitor cell proliferation and neurogenesis in the C57B/16 mouse brain. Brain Res 1473:204–213. https://doi.org/10.1016/j.brainres.2012.07.029
Mead R, Gilmour SG, Mead A (2012) Statistical Principles for the Design of Experiments: Applications to Real Experiments. Cambridge Series in Statistical and Probabilistic Mathematics. Cambridge University Press, Cambridge
Messori L, Casini A, Gabbiani C et al (2007) Unravelling the chemical nature of copper cuprizone. Dalt Trans 21:2112–2114. https://doi.org/10.1039/b701896g
Misrielal C, Mauthe M, Reggiori F, Eggen BJL (2020) Autophagy in multiple sclerosis: two sides of the same coin. Front Cell Neurosci 14:603710. https://doi.org/10.3389/fncel.2020.603710
Moustafa PE, Abdelkader NF, El Awdan SA et al (2018a) Extracellular matrix remodeling and modulation of inflammation and oxidative stress by sulforaphane in experimental diabetic peripheral neuropathy. Inflammation 41:1460–1476. https://doi.org/10.1007/s10753-018-0792-9
Moustafa PE, Abdelkader NF, El Awdan SA et al (2018b) Liraglutide ameliorated peripheral neuropathy in diabetic rats: Involvement of oxidative stress, inflammation and extracellular matrix remodeling. J Neurochem 146:173–185. https://doi.org/10.1111/jnc.14336
Omotoso GO, Ukwubile II, Arietarhire L et al (2018) Kolaviron protects the brain in cuprizone-induced model of experimental multiple sclerosis via enhancement of intrinsic antioxidant mechanisms: Possible therapeutic applications? Pathophysiology 25:299–306. https://doi.org/10.1016/j.pathophys.2018.04.004
Peixoto CA, de Oliveira WH, da Araújo SMR, Nunes AKS (2017) AMPK activation: role in the signaling pathways of neuroinflammation and neurodegeneration. Exp Neurol 298:31–41. https://doi.org/10.1016/j.expneurol.2017.08.013
Perry TA, Lahiri DK, Sambamurti K et al (2003) Glucagon-like peptide-1 decreases endogenous amyloid-β peptide (Aβ) levels and protects hippocampal neurons from death induced by Aβ and iron. J Neurosci Res 72:603–612. https://doi.org/10.1002/jnr.10611
Plemel JR, Liu WQ, Yong VW (2017) Remyelination therapies: a new direction and challenge in multiple sclerosis. Nat Rev Drug Discov 16:617–634. https://doi.org/10.1038/nrd.2017.115
Prins M, Eriksson C, Wierinckx A et al (2013) Interleukin-1β and interleukin-1 receptor antagonist appear in grey matter additionally to white matter lesions during experimental multiple sclerosis. PLoS ONE 8:e83835–e83835. https://doi.org/10.1371/journal.pone.0083835
Safar MM, Abdelkader NF, Ramadan E et al (2021) Novel mechanistic insights towards the repositioning of alogliptin in Parkinson’s disease. Life Sci 287:120132. https://doi.org/10.1016/j.lfs.2021.120132
Schrijver HM, Van As J, Crusius JBA et al (2003) Interleukin (IL)-1 gene polymorphisms: relevance of disease severity associated alleles with IL-1β and IL-1ra production in multiple sclerosis. Mediators Inflamm 12:89–94. https://doi.org/10.1080/0962933031000097691
Shao B-Z, Cao Q, Liu C (2018) Targeting NLRP3 inflammasome in the treatment of CNS diseases. Front Mol Neurosci 11:1–10. https://doi.org/10.3389/fnmol.2018.00320
Shi Y, Zhang L, Teng J, Miao W (2018) HMGB1 mediates microglia activation via the TLR4/NF-κB pathway in coriaria lactone induced epilepsy. Mol Med Rep 17:5125–5131. https://doi.org/10.3892/mmr.2018.8485
Soraya H, Clanachan AS, Rameshrad M et al (2014) Chronic treatment with metformin suppresses toll-like receptor 4 signaling and attenuates left ventricular dysfunction following myocardial infarction. Eur J Pharmacol 737:77–84. https://doi.org/10.1016/j.ejphar.2014.05.003
Soraya H, Farajnia S, Khani S et al (2012) Short-term treatment with metformin suppresses toll like receptors (TLRs) activity in isoproterenol-induced myocardial infarction in rat: Are AMPK and TLRs connected? Int Immunopharmacol 14:785–791. https://doi.org/10.1016/j.intimp.2012.10.014
Stinissen P, Medaer R, Raus J (1998) Myelin reactive T cells in the autoimmune pathogenesis of multiple sclerosis. Mult Scler 4:203–211. https://doi.org/10.1177/135245859800400322
Swanson KV, Deng M, Ting JPY (2019) The NLRP3 inflammasome: molecular activation and regulation to therapeutics. Nat Rev Immunol 19:477–489. https://doi.org/10.1038/s41577-019-0165-0
Szu J, Wojcinski A, Jiang P, Kesari S (2021) Impact of the olig family on neurodevelopmental disorders. Front Neurosci 15:1–19. https://doi.org/10.3389/fnins.2021.659601
Takeshita H, Yamamoto K, Nozato S et al (2017) Modified forelimb grip strength test detects aging-associated physiological decline in skeletal muscle function in male mice. Sci Rep 7:1–9. https://doi.org/10.1038/srep42323
Walsh RN, Cummins RA (1976) The open-field test: a critical review. Psychol Bull 83:482–504. https://doi.org/10.1037/0033-2909.83.3.482
Wang Y, Jin S, Sonobe Y et al (2014) Interleukin-1β induces blood-brain barrier disruption by downregulating sonic hedgehog in astrocytes. PLoS ONE 9:e110024. https://doi.org/10.1371/journal.pone.0110024
Yan P, Bai L, Lu W et al (2017) Regulation of autophagy by AMP-activated protein kinase/sirtuin 1 pathway reduces spinal cord neurons damage. Iran J Basic Med Sci 20:1029–1036
Yildirim Simsir I, Soyaltin UE, Cetinkalp S (2018) Glucagon like peptide-1 (GLP-1) likes Alzheimer’s disease. Diabetes Metab Syndr Clin Res Rev 12:469–475. https://doi.org/10.1016/j.dsx.2018.03.002
Yuan X, Wang L, Bhat OM et al (2018) Differential effects of short chain fatty acids on endothelial Nlrp3 inflammasome activation and neointima formation: antioxidant action of butyrate. Redox Biol 16:21–31. https://doi.org/10.1016/j.redox.2018.02.007
Zatta P, Raso M, Zambenedetti P et al (2005) Copper and zinc dismetabolism in the mouse brain upon chronic cuprizone treatment. Cell Mol Life Sci 62:1502–1513. https://doi.org/10.1007/s00018-005-5073-8
Zhan J, Mann T, Joost S et al (2020) The cuprizone model: dos and do nots. Cells 9:843. https://doi.org/10.3390/cells9040843
Zhang N, Zhang R, Loers G et al (2020) Cuprizone-induced demyelination in mouse hippocampus is alleviated by ketogenic diet. J Agric Food Chem 68:11215–11228. https://doi.org/10.1021/acs.jafc.0c04604
Zhen W, Liu A, Lu J et al (2017) An alternative cuprizone-induced demyelination and remyelination mouse model. ASN Neuro 9:175909141772517. https://doi.org/10.1177/1759091417725174
Zhou G, Myers R, Li Y et al (2001) Role of AMP-activated protein kinase in mechanism of metformin action. J Clin Invest 108:1167–1174. https://doi.org/10.1172/JCI13505
Zidan A, Hedya SE, Elfeky DM, Abdin AA (2018) The possible anti-apoptotic and antioxidant effects of acetyl L-carnitine as an add-on therapy on a relapsing-remitting model of experimental autoimmune encephalomyelitis in rats. Biomed Pharmacother 103:1302–1311. https://doi.org/10.1016/j.biopha.2018.04.173
Zou P, Liu X, Li G, Wang Y (2018) Resveratrol pretreatment attenuates traumatic brain injury in rats by suppressing NLRP3 inflammasome activation via SIRT1. Mol Med Rep 17:3212–3217. https://doi.org/10.3892/mmr.2017.8241
Acknowledgements
The authors are grateful to Dr. Mohamed Abdel Razek (Associate Professor of Pathology, Faculty of Veterinary Medicine, Cairo University) for his assistance in histopathological examination.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). There is no funding sources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ammar, R.A., Mohamed, A.F., Kamal, M.M. et al. Neuroprotective effect of liraglutide in an experimental mouse model of multiple sclerosis: role of AMPK/SIRT1 signaling and NLRP3 inflammasome. Inflammopharmacol 30, 919–934 (2022). https://doi.org/10.1007/s10787-022-00956-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-022-00956-6