Abstract
The current work explored the influences of time dependent Sildenafil (SILD) administration, and the possible outcomes from its concomitant administration with dexamethasone against acetic acid-induced ulcerative colitis in rats. Rats were assigned into six random groups: diseased group (AA), injected once with 2 ml acetic acid (3%) intrarectally, 2 days before sacrification. SILD + AA, received sildenafil (25 mg/kg, orally) for 6 days starting 3 days pre-injection of AA; SILD-t + AA, received sildenafil (25 mg/kg, orally), starting at time of AA injection and continued for 3 days; DEXA + AA, received dexamethasone (2 mg/kg, i.p.) for 3 days, starting at time of AA injection; SILD-t + DEXA + AA, received sildenafil (25 mg/kg, orally) and dexamethasone (2 mg/kg, i.p.), as mentioned. Sildenafil markedly ameliorated disease activity index (DAI), ulcer scores, colon length shortening and colonic histopathological changes. Mechanistically, Sildenafil markedly attenuated immunoexpression of NF-κB p65/ TNF-α and COX-2, diminished oxidative stress (↓ MDA/NO levels and ↑ GSH level and SOD activity), increased levels of Nrf-2/HO-1, compared to untreated group. Taken together, Sildenafil treatment suppressed acetic acid-induced ulcerative colitis, probably via inhibiting NF-κB/TNF-α signaling dependent of Nrf-2/HO-1 pathway, reducing oxidative stress and attenuating inflammation. Surprisingly, effects of sildenafil were unpromoted in a time dependant manner. Short term treatment with sildenafil was sufficient to exert its coloprotective effect, while longer term pretreatment was only superior among other treatments in the macroscopical changes. Moreover, concurrent administration of sildenafil and dexamethasone had the preference in boosting the antioxidant defense and anti-inflammatory mechanisms, visualized by histopathological/immunohistochemical changes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ulcerative colitis (UC) is a recurrent, chronic inflammatory disease of the colon of unknown etiopathogenesis at present (Brown and Mayer 2007). There is convincing evidence that excessive inflammation and oxidative stress are extremely involved in its pathogenesis (Jena et al. 2012). Acetic acid-induced UC animal model, is optimum as it resembles UC in humans in pathology, clinical course, increased release of inflammatory mediators, localized involvement and damage to the inflamed mucosa (Randhawa, Singh et al. 2014).
Nuclear erythroid-related factor 2 (Nrf-2) is a key antioxidant-mediated transcription factor that regulates downstream cytoprotective pathways, through interconnection with antioxidant response elements (ARE), which are localized upstream enhancer area of detoxification enzyme genes (Venugopal and Jaiswal 1998). Heme oxygenase-1 (HO-1) is one of the antioxidant enzymes, elevated following oxidative stress. HO-1 initiates the oxidative degradation of heme to carbon monoxide and bilirubin, both are potent antioxidants (Clark, Foresti et al. 2000). The activity of the transcription factor Nrf-2 is suppressed by Kelch-like ECH-associated protein-1 (KEAP-1), which physically segregates Nrf-2 in the cytosol, while electrophilic and oxidative stress destabilized this connection. Nrf-2 is then transfered to the nucleus, where it triggers downstream cytoprotective genes like HO-1 to be transcribed. Therefore, drugs that target Nrf-2 may be able to alleviate UC.
Nuclear erythroid-related factor 2 (Nrf-2) is greatly implicated in the transcription of genes responsible for management of cellular anti-inflammatory and antioxidant machinery (Ma 2013). Increased oxidative stress in absence of Nrf-2 induces NF-κB-over mediated cytokine expression, since NF-κB is more readily generated in an oxidative media (Ganesh Yerra, Negi et al. 2013). Nuclear factor kappa B (NF-κB) is a heterodimer protein complex constitute diverse subunits including P65 (Lingappan 2018). NF-κB signaling, and its downstream production of various proinflammatory cytokines, cyclooxygenase-2 (COX-2) enzyme, nitrosative and oxidative stress, perform a vital part in the pathogenesis of UC. These factors interact together, leading to exaggerated inflammatory reactions, thus contributed to colonic injury in UC (Jobin and Sartor 2000; Surh et al. 2001).
Overproduction of COX-2 due to disturbances in arachidonic acid metabolic pathway is well related to colitis development. COX-2 triggers overproduction of prostaglandin E2 (PGE-2) and thromboxane B2 (TXB2), which are two of the vital inflammatory mediators in colitis-associated colonic cell damage, inflammation, and edema, in addition to TXB2-induced vasoconstriction, platelet aggregation, and thrombosis (Dong et al. 2003) Previous studies confirmed their role in UC pathogenesis in animal models of colitis (Auwerda et al. 2001, Medina 2001, Appleyard et al. 2002).
Sildenafil (SILD) is a potent selective inhibitor of PDE5 and is widely being used for the treatment of erectile dysfunction in men (Yaseen, Darwich et al. 2012). More recently it has been experimented for treating other diseases. SILD is known to significantly decrease oxidative stress and inflammation in several models (Ali et al. 2011, El-Mahdy et al. 2016, LUNA 2016, Mohey et al. 2016, Sikandaner et al. 2017), thus yields a remarkable anti-inflammatory and antioxidant properties. It was thought of interest to examine the power of SILD to mitigate the effects of acetic acid-induced UC. In this research, we postulated that SILD could suppress UC in rats via Nrf-2/HO-1 pathway. Therefore, the current study was designed to compare three different regimens of SILD with or without dexamethasone to detect the most effective regimen.
Materials and methods
Drugs and chemicals
Sildenafil (Sild) was purchased from (Pfizer, Egypt) and was dissolved in water. Acetic acid was purchased from (EL-Goumhouria Co. for trading medicines, Egypt) and Dexamethasone was purchased from (AMRIYA pharmaceuticals, Egypt). These drugs were dissolved in normal saline. Other chemicals were of high analytical grade.
Animals
Adult male SD rats weighting 250 ± 20 g were maintained in a room at standard conditions and were provided food and water ad libitum.
Experimental design
The experimental design is shown in Fig. 1. Rats were assigned randomly into 6 groups (n = 9): Control, received 2 ml normal saline intrarectally at the induction day; diseased group (AA), injected once with 2 ml acetic acid (3%) intrarectally, 2 days before sacrification to induce colitis; SILD + AA, received sildenafil (25 mg/kg, orally) for 6 days starting 3 days pre-injection of AA; SILD-t + AA, received sildenafil (25 mg/kg, orally), starting at the time of AA injection and continued for 3 days; DEXA + AA, received dexamethasone (2 mg/kg, i.p.) for 3 days, starting at the time of AA injection; SILD-t + DEXA + AA, received sildenafil (25 mg/kg, orally) and dexamethasone (2 mg/kg, i.p.), for 3 days, starting at the time of AA injection. This dose of 25 mg/kg of SILD showed beneficial effect in several studies (Lee et al. 2010; Jasińska-Stroschein et al. 2013, Huang, Liu et al. 2022), in addition to optimal coloprotective effect according to our preliminary experiment (where two doses of sildenafil 25 and 30 mg/kg were used, supplementary file). All rats were deprived from food with free access to water 48 h before induction of colitis.
At the time of the experiment, anesthesia was achieved by thiopental (40 mg/kg, i.p.). Colitis was induced according to a published protocol (Matuszyk et al. 2016) by slow rectal injection of a 2 ml diluted solution of acetic acid (3%) using a flexible plastic rubber catheter with an outside diameter of 8 mm inserted rectally 8 cm into the colon via the anus. The animals were maintained in the supine trendelenburg position for 30 s to prevent early leakage of the intracolonic instillation.
One hour after the last drug administration, rats were sacrificed, under anesthesia. The entire colon, from the cecum to the anus, was immediately excised and the colon length was measured and observed as an indirect marker of inflammation, then washed, opened longitudinally and digital pictures were taken.
Finally, colon was cut into two parts, one part was homogenized in phosphate buffer solution (PBS), then homogenates were centrifuged at 4000 × g at 4 °C for 15 min. The supernatant was kept in − 80 °C until needed for subsequent analyses. The other part of colon was fixed in 10% buffered formalin for histopathological and immunohistochemical analyses.
Assessment of disease activity index (DAI)
Animals were kept in cages and were observed for body weight change, stool consistency and bleeding for 2 days post induction of colitis, to score the disease activity index (DAI) using a protocol previously described by (Cooper et al. 1993) with little modification, as shown in Table 1.
Assessment of macroscopic ulcer score
Colons were examined visually, to score the ulceration. The damage was assessed by the colon mucosal damage index (CMDI) scored on a scale of 0–10 according to a reported scoring system (Bell et al. 1995).
The following scores were applied: Grade 0: normal appearance; Grade 1: focal hyperemia, no ulcers; Grade 2: ulcer with no significant inflammation (hyperemia and bowel wall thickening); Grade 3: ulcer with inflammation at one site; Grade 4: two or more sites of ulceration and inflammation; Grade 5: major sites of damage extending > 1 cm along the length of the colon; and Grade 6–10:, if major sites of damage extending > 2 cm along the colon, the score was increased by 1 for each additional cm of involvement.
Estimation of antioxidant status and nitrosative stress
Levels of malondialdehyde (MDA), reduced glutathione (GSH) and superoxide dismutase (SOD) activity were assessed spectrophotometrically according to methods described by Ohkawa et al. (1979), Ellman (1959) and Marklund and Marklund (1974) respectively.
Evaluation of the antioxidant-related markers (Nrf-2, HO-1) by ELISA assay
Levels of the oxidant-related marker: iNOS and levels of the antioxidant-related markers: nuclear erythroid-related factor 2 (Nrf-2) and heme oxygenase-1(HO-1) were evaluated in colon homogenate by ELISA assay using commercial kits obtained from (Bioassay Technology Laboratory, Shanghai Crystal Day Biotech Co., Ltd., Shanghai, China), according to manufacturer’s instructions.
Briefly, a specific biotinylated antibody reagent was added to the plates, which were filled with the homogenized tissue and incubated at 37∘C in CO2 for 2 h. After washing with phosphate-buffered saline (PBS), streptavidin horseradish peroxidase (HRP) solution was added, and the plates were incubated for 30 min at room temperature. Then, using a microplate reader, absorbance was measured at 450 nm.
Immunohistochemical examination
Antibodies were used to evaluate colon expression of tumor necrosis factor alpha (TNF-α) (ABclonal Technology, MA, USA, catalog number: A0277), nuclear factor kappa beta p65 (NF-κB p65) (Bioss antibodies, MA, USA, catalog number: bs-20159R), and COX-2 (ABclonal Technology, MA, USA, catalog number: A1253), using Avidin–Biotin Complex (ABC), immunohistochemical staining protocol, according to the manufacturer's instructions.
Sections (4 μm) of colons were incubated for 20 min in 0.3% H2O2 to block the endogenous peroxidase activity. The section slides were incubated in a 100 °C water bath for 10 min in 0.01 M PBS buffer solution, then blocked with 2% BSA for 30 min. Then, the sections were incubated with the anti-rat antibodies overnight at 4 °C. The slides were washed and then incubated with HRP secondary antibody at 37 °C for 1 h. The sections were subsequently treated with DAB working solution for 4 min and finally counterstained with Mayer’s hematoxylin. Tissue sections were observed, photographed with a microscope (400 × magnification) and were semi-quantified.
Histopathological examination of colon tissues
The colons were dissected and fixed with 10% formaldehyde solution for 48 h. The tissues were embedded in paraffin wax and sliced (5 μm). The sections were stained with hematoxylin–eosin (H&E) and were evaluated blindly by the pathologist under a microscope (100 × magnification).
Statistical analysis
Results are presented as the mean ± standard error of the mean (SEM). Statistical evaluation was carried out by GraphPad Prism 5 (GraphPad Software, San Diego, CA, USA). One-way analysis of variance (ANOVA), followed by Tukey Kramer's post-hoc test was used to compare the measures between the experimental groups. Kruskal–Wallis test followed by Dunn's multiple comparison post-hoc test was used for analysis of histopathological and histochemical scores of rats. Significance level was set at p < 0.05.
Results
Effect of sildenafil on DAI, colon length, and macroscopic ulcer score
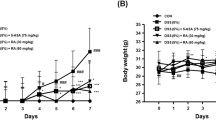
Acetic acid treatment caused a significant increase in DAI and macroscopic ulcer score with a significant reduction in colon length compared to control group. DEXA + AA group significantly reduced intensity of DAI by 58% with a significant increase in colon length by 1.1-fold, and exerted insignificant decrease in ulcer score, compared to AA group. Meanwhile, other treated groups: SILD + AA, SILD-t + AA, and SILD-t + DEXA + AA showed a higher marked decrease in intensity of DAI by 76.4, 58.8, 58.8%, and ulcer score by 57.1, 53, 42.8%, respectively, with a more significant increase in colon length by 1.26-fold, compared to AA group (Fig. 2), indicating the highest preference for the longer term pretreatment with sildenafil over other treated groups; SILD > SILD-t > SILD-t + DEXA > DEXA, in order of improvement of all macroscopical features.
Effect of sildenafil on DAI, colon length, and macroscopic ulcer score. Data are expressed as mean ± SEM (n = 9) AA Acetic acid, SILD Sildenafil, DEXA Dexamethasone, DAI disease activity index. Statistically significant: # p < 0.05, compared to control group, *p < 0.05, compared to AA group, using one-way ANOVA followed by Tukey–Kramer multiple comparisons post-hoc test
Effect of sildenafil on antioxidant status and nitrosative stress
To ascertain whether SILD can affect oxidative/nitrosative stress, we compared MDA, NO levels, SOD, and GSH activity within treated groups: SILD + AA, SILD-t + AA, DEXA + AA, and SILD-t + DEXA + AA (Fig. 3).
Effect of sildenafil on antioxidant status and nitrosative stress. Data are expressed as mean ± SEM (n = 9) AA Acetic acid, SILD Sildenafil, DEXA Dexamethasone, MDA malondialdehyde, NO nitric oxide, GSH reduced glutathione, SOD Superoxide dismutase. Statistically significant: #p < 0.05, compared to control group, *p < 0.05, compared to AA group, using one-way ANOVA followed by Tukey–Kramer multiple comparisons post-hoc test
Acetic acid treatment caused a significant elevation in MDA and NO (by 1.7 and twofold, respectively), whereas SOD and GSH activity were significantly decreased (by 23% and 46%, respectively) when compared to control group.
Herein, uncombined dexamethasone treated group and longer term pretreatment with sildenafil produced the least significant effects among other treated groups. DEXA + AA group showed a significant increase in SOD activity and GSH level by 3 and 1.6 folds respectively, in addition to a significant decrease in MDA level by 24%. Meanwhile, it produced the most significant reduction in NO level by 15.7% compared to AA group, indicating that nitrosative stress can be highly enhanced with dexamethasone treatment.
SILD + AA group showed the least significant increase in SOD activity and GSH level by 2.9 and 1.5 folds respectively, however, its high significant reduction in MDA level by 43.6% among other groups indicated that lipid peroxidation can be highly enhanced in the pre-diseased state with this drug, whereas no change was recorded in NO level, compared to AA group.
Meanwhile, short term treatment with sildenafil alone or combined with dexamethasone produced the highest significant effects among other treated groups. SILD-t + AA and SILD-t + DEXA + AA groups showed a significant increase in SOD activity by 4.7 and 2.9 folds, respectively, in addition to a significant increase in GSH level by 1.7 and 2.6 folds, respectively. Moreover, they exerted a significant reduction in MDA level by 47.8, and 22%, respectively, in addition to a 15% significant decrease in NO level with the combined group, while no change was recorded in NO level in SILD-t + AA group, compared to AA group.
Effect of sildenafil on expression of the antioxidant-related markers (NRF-2 and HO-1)
In comparison to the normal control group, AA injection decreased NRF-2 and HO-1 levels by 15.7% and 13.3%, respectively) (Fig. 4). All treatment exerted a significant elevation in NRF-2 and HO-1 levels, compared to AA group, with the highest preference for time dependant sildenafil treatments, followed by single and combined DEXA treatments; SILD-t > SILD > DEXA and SILD-t + DEXA.
Effect of sildenafil on expression of the antioxidant-related markers (NRF-2 and HO-1). Data are expressed as mean ± SEM (n = 9) AA Acetic acid, SILD Sildenafil, DEXA Dexamethasone, Nrf-2 Nuclear erythroid-related factor 2, HO-1 Heme oxygenase-1. Statistically significant: #p < 0.05, compared to control group, *p < 0.05, compared to AA group, using one-way ANOVA followed by Tukey–Kramer multiple comparisons post-hoc test
Effect of sildenafil on immunohistochemical evaluation of the inflammatory mediators (TNF-α, NF-κB and COX-2)
Microscopic picture of immunostained colonic sections against TNF-α showing weak expression in control group. Colonic TNF-α positive expression appear as brown cytoplasmic color in leukocytes (macrophages & neutrophils) infiltrating mucosa and submucosa and there was also a sparse distribution in epithelial cells and vascular endothelial cells. The numbers of positively stained cells were predominantly located within the mucosa and submucosa and were significantly decreased in all treated group. The positive reaction appears the lowest in SILD-t + DEXA + AA (Fig. 5a).
Effect of sildenafil on immunohistochemical evaluation of the inflammatory mediators (TNF-α, NF-κB and COX-2). a Tumor necrosis factor alpha (TNF-α), b Nuclear factor kappa B (NF-κB), c Cyclooxygenase-2 (COX-2) expression in colonic tissues assessed by immunohistochemistry (X 400, bar = 50 µm), d Bar graphs showing immunohistopathological score of TNF-α, NF-κB and COX-2 in colonic tissue of rats. Statistically significant: #p < 0.05, compared to control group, *p < 0.05, compared to AA group, using Kruskal–Wallis test followed by Dunn's multiple comparison test. AA Acetic acid, SILD Sildenafil, DEXA Dexamethasone
Microscopic pictures of immunostained colonic sections against NF-κB showing normal expression in mucosa with negative expression in submucosa in control group. In contrast, intense positive staining appears in affected areas with necrosis & ulceration in mucosa (yellow arrows) and underlying submucosa (*) in AA group. Treated groups: SILD + AA, SILD-t + AA and DEXA + AA showed marked decrease of positive expression in mucosa (yellow arrows) with persistence of positive expression in submucosa (*). This decrease appeared the lowest in DEXA + AA group when compared to AA group. The treated group: SILD-t + DEXA + AA showed marked decrease of positive expression in mucosa (yellow arrows) and submucosa (*), when compared to AA group. IHC counterstained with Mayer's hematoxylin (Fig. 5b).
Microscopic pictures of immunostained colonic sections against COX-2 showing normal expression in mucosa (area in square) with negative expression in submucosa in control group. In contrast, intense positive staining appears in affected areas with necrosis & ulceration in mucosa (area in square) and underlying submucosa (*) in AA group. Treated groups showed lowered positive staining in affected mucosa (area in square) and underlying submucosa (*) when compared with AA group. The positive reaction appeared the lowest in SILD-t + DEXA + AA followed by SILD-t + AA followed by DEXA + AA followed by SILD + AA. IHC counterstained with Mayer's hematoxylin (Fig. 5c).
Effect of sildenafil on histopathological examination of the colon
Microscopic pictures of H&E-stained colonic sections showing normal layers: mucosa, submucosa and muscles in control group. Colonic sections from colitis group (AA) showed an extensive transmural necrosis reaching muscular layer, mucosal necrosis with ulceration accompanied with marked submucosal edema, congestion, hemorrhage and inflammation. Colonic sections from treated group (SILD + AA) showed mild focal mucosal erosion, markedly reduced submucosal edema, congestion and inflammation. Colonic sections from treated groups: (SILD-t + AA), followed by (DEXA + AA) showed small focal area of mucosal necrosis, submcosal edema and inflammation with few leukocytic cells infiltration. Colonic sections from treated group (SILD-t + DEXA + AA) showed markedly reduced submucosal edema and inflammation. Transmural necrosis (long black arrow), erosion/ulceration (dashed arrows), mucosal necrosis (short black arrow), submucosal edema (*), congestion (red arrow), hemorrhage (red arrowhead) and inflammation (yellow arrow) (Fig. 6).
Effect of sildenafil on histopathological examination of the colon. Right panel: Representative photomicrographs of H&E-stained colonic sections (X 100, bar = 100 µm). Left panel: Bar graphs showing colon injury score. Statistically significant: #p < 0.05, compared to control group, *p < 0.05, compared to AA group, using Kruskal–Wallis test followed by Dunn's multiple comparison test. AA Acetic acid, SILD Sildenafil, DEXA Dexamethasone
Discussion
AA-induced colitis is like human UC in cytokine profile and histopathological features and is characterized by neutrophil infiltration, that contributes substantially to the development of colon tissue damage via the formation of different reactive species (Elshazly, Elhassanny et al. 2020). Findings from this study show that the identified potent selective inhibitor of PDE5, sildenafil, attenuated AA-induced colitis in rat. SILD treatment produced the following beneficial effects: a) it improved macroscopic appearance of colon tissue and markedly reduced histopathological changes in colon tissue; b) it reduced colon oxidative stress (↓ MDA, NO levels and ↑ GSH level and SOD activity); c) it increased level of antioxidant-related markers Nrf-2 and HO-1; d) it decreased colon immunodepression of inflammatory markers TNF-α, NF-κB p65, and COX-2 (Fig. 7).
Graphical representation of the coloprotective mechanisms for Sildenafil against AA-induced UC in rats. AA Acetic acid, SILD Sildenafil, DAI disease activity index, MDA malondialdehyde, NO nitric oxide, GSH reduced glutathione, SOD Superoxide dismutase, Nrf-2 Nuclear erythroid-related factor 2, HO-1 Heme oxygenase-1, TNF-α: Tumor necrosis factor alpha, NF-κB Nuclear factor kappa B, COX-2 Cyclooxygenase-2
Nuclear erythroid-related factor 2 (Nrf-2) is a distinct antioxidant-mediated transcription factor that controls downstream cytoprotective targets, through encoded coordinated expression of antioxidant and cytoprotective genes, which is essential for body’s defense against inflammatory tissue injuries (He, Ru et al. 2020). Among which is HO-1, a significant cellular defense enzymatic antioxidant facing oxidative tissue damage that is considered as a protective mechanism through initiation of several antioxidants and bilirubin formation, which are capable of sequestering ROS (Bauer, Huse et al. 2008). Therefore, initiation of this enzyme could be a target to protect against inflammatory processes and oxidative tissue damage.
To pinpoint the exact mechanism of SLID. We investigated its role in modulating the Nrf-2/HO-1 pathway. The Nrf-2/ HO-1 pathway has been a recent attractive target in addressing AA-induced colitis (Khodir et al. 2019, Jeong, Kang et al. 2021). Indeed, in our study SILD treatment increased antioxidant-related markers Nrf-2 and HO-1, implying that it could be used to prevent oxidative damage and improve healing. Several studies reported antioxidant activities of SILD in experimental disease models through the Nrf-1/HO-1 cytoprotective pathway (Zahran et al. 2015, Behiry et al. 2018, Fang et al. 2020).
Inflammation is a major effector of AA-induced colitis. NF-κB is involved in the regulation of many genes involved in the inflammatory response (Liu et al. 2017). Increased NF-κB expression has been linked to increased cyclooxygenase-2 (COX-2) (Ahmed et al. 2014), TNF-α and IL-6 expression (Chamanara et al. 2019, Ansari et al. 2021), which are directly involved in colon tissue destruction. TNF-α may also increase the inflammatory cascade by activating NF-κB (Parameswaran and Patial 2010). Nrf-2 activators have been reported to be capable of preventing IK/IB phosphorylation and NF-κB p65 nuclear translocation, hence inactivating NF-κB signaling (Wardyn et al. 2015). Furthermore, it is thought that activating Nrf-2 antioxidant signaling inhibits inflammatory signaling pathways like NF-κB (Abdelrahman and Abdel-Rahman 2019). As a result, there is a possibility of crosstalk between the Nrf-2 and NF-κB pathways. In the current study AA-induced increase in inflammatory markers in line with previous studies (Elshazly et al. 2020, Ansari et al. 2021, Jeong et al. 2021, Salim et al. 2021), SILD reduced colon expression of TNF-α, NF-κB p65 and COX-2 consistent with previous studies (Yaseen et al. 2012, Zahran et al. 2015, Sikandaner et al. 2017, Fang et al. 2020).
Another point of view, AA-induced oxidative stress was indicated by significantly higher levels of NO and MDA, an index of lipid peroxidation, and significantly lower levels of the antioxidants GSH and SOD (Ansari et al. 2021, Salim et al. 2021, Zaghloul et al. 2022). SILD treatment has significantly reduced NO and MDA and elevated GSH and SOD levels and alleviated the oxidative stress status. SILD may potentially exert its action through potentiating the antioxidant Nrf-2 pathway. Moreover, SILD treatment reduced histopathological and score changes in colon tissue.
In addition, in this study, AA-induced UC which was manifested by a significant rise in DAI score, colon length, and macroscopic ulcer score that correlated with histopathological examination that revealed extensive transmural necrosis reaching muscular layer, mucosal necrosis with ulceration accompanied with marked submcosal edema, congestion, hemorrhage and inflammation. These results are in line with previous studies that confirmed the ability of AA to induce UC in rats closely comparable to the human UC ((Elshazly et al. 2020, Zaghloul et al. 2022). Interestingly, the administration of SILD significantly improved colon tissue architecture and reversed AA-induced UC.
Therefore, this work was the first to design a time dependent study on sildenafil, in addition to the concomitant sildenafil/dexamethasone effects. Three regimens: SILD/DEXA combination, short and longer term SILD treatments, were able to exert downregulation of inflammatory mediators, increased colon antioxidant defense machinery, with a preference for the combination group, while the longer term sildenafil pretreatment regimen was the least significant, except for macroscopical changes. In addition, the underlying coloprotective mechanisms of sildenafil were primarily explained in our study.
Conclusion
In conclusion, sildenafil ameliorated colon injury and its associated oxidant and inflammatory features through multiple mechanisms. SILD down-regulated expression of TNF-α, NF-κB p65, and COX-2. In addition, SILD acted as an activator of Nrf-2/HO-1, and inhibitor of inflammation signaling pathways. Hence, sildenafil could serve as a promising candidate for the treatment of ulcerative colitis in humans. It may be nonessential to take sildenafil as a protective medicine, and its short term treatment could produce the desired coloprotective effect.
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ARE:
-
Antioxidant response elements
- Cyclooxygenase-2:
-
COX-2
- GSH:
-
Glutathione
- H&E:
-
Hematoxylin and eosin
- HO-1:
-
Heme oxygenase-1
- MDA:
-
Malondialdeyhde
- NF-κB:
-
Nuclear factor kappa B
- NOx:
-
Nitrite/nitrate
- Nrf-2:
-
Nuclear erythroid-related factor 2
- PGE-2:
-
Prostaglandin E2
- SILD:
-
Sildenafil
- SOD:
-
Superoxide dismutase
- TNF-α:
-
Tumor necrosis factor alpha
- TXB2:
-
Thromboxane B2
- UC:
-
Ulcerative colitis
References
Abdelrahman RS, N. Abdel-Rahman (2019) Dimethyl fumarate ameliorates acetaminophen-induced hepatic injury in mice dependent of Nrf-2/HO-1 pathway. Life Sci 217: 251–260.http://www.ncbi.nlm.nih.gov/pubmed/30550888
Ahmed S, Dewan MZ, Xu RJAJDD (2014) Nuclear factor-kappaB in inflammatory bowel disease and colorectal cancer. 1: 84–96
Ali BH, Abdelrahman AM, Al-Salam S, Sudhadevi M, AlMahruqi AS, Al-Husseni IS, Beegam S, Dhanasekaran S, Nemmar A, Al-Moundhri M (2011) The effect of sildenafil on cisplatin nephrotoxicity in rats. Basic Clin Pharmacol Toxicol 109(4):300–308
Ansari MN, Rehman NU, Karim A, Soliman GA, Ganaie MA, Raish M, Hamad AM (2021). Role of oxidative stress and inflammatory cytokines (TNF-α and IL-6) in acetic acid-induced ulcerative colitis in rats: ameliorated by otostegia fruticosa. 11(3): 195. https://www.mdpi.com/2075-1729/11/3/195
Appleyard CB, Alvarez A, Percy WH (2002) Temporal Changes in Colonic Vascular Architecture and Inflammatory Mediator Levels in Animal Models of Colitis. Digestive Diseases and Sciences 47(9): 2007–2014.https://doi.org/10.1023/A:1019660526241
Auwerda JJA, Zijlstra FJ, Tak CJAM, van den Ingh HFGM, Wilson JHP, Ouwendijk RJT (2001) Ridogrel enemas in distal ulcerative colitis. Euro J Gastroenterol Hepatol 13(4): 397–400. https://journals.lww.com/eurojgh/Fulltext/2001/04000/Ridogrel_enemas_in_distal_ulcerative_colitis.16.aspx
Bauer M, Huse K, Settmacher U, Claus RA (2008) The heme oxygenase-carbon monoxide system: regulation and role in stress response and organ failure. Intensive Care Med 34(4): 640–648.http://www.ncbi.nlm.nih.gov/pubmed/18286266, https://springerlink.fh-diploma.de/article/10.1007%2Fs00134-008-1010-2
Behiry, S., A. Rabie, M. Kora, W. Ismail, D. Sabry and A. Zahran (2018). "Effect of combination sildenafil and gemfibrozil on cisplatin-induced nephrotoxicity; role of heme oxygenase-1." Renal Failure 40(1): 371–378.https://doi.org/10.1080/0886022X.2018.1455596
Bell CJ, Gall DG, Wallace JL (1995) Disruption of colonic electrolyte transport in experimental colitis. Am J Physiol 268(4 Pt 1):G622-630
Brown SJ, Mayer L (2007) The immune response in inflammatory bowel disease. Am J Gastroenterol 102(9):2058–2069
Chamanara M, Abdollahi A, Rezayat SM, Ghazi-Khansari M, Dehpour A, Nassireslami E, Rashidian A (2019) Thymol reduces acetic acid-induced inflammatory response through inhibition of NF-kB signaling pathway in rat colon tissue. Inflammopharmacology 27(6):1275–1283
Clark JE, Foresti R, Green CJ, Motterlini R (2000) Dynamics of haem oxygenase-1 expression and bilirubin production in cellular protection against oxidative stress. Biochem J 348 Pt 3: 615–619.http://www.ncbi.nlm.nih.gov/pubmed/10839994https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1221105/pdf/10839994.pdf
Cooper HS, Murthy SN, Shah RS, Sedergran DJ (1993) Clinicopathologic study of dextran sulfate sodium experimental murine colitis. Lab Invest 69(2):238–249
Dong WG, Liu SP, Yu BP, Wu DF, Luo HS, Yu JP (2003) Ameliorative effects of sodium ferulate on experimental colitis and their mechanisms in rats. World J Gastroenterol 9(11):2533–2538
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82(1):70–77
El-Mahdy NA, El-Sayad ME-S, El-Kadem AH (2016) Combination of telmisartan with sildenafil ameliorate progression of diabetic nephropathy in streptozotocin-induced diabetic model. Biomed Pharmacotherapy 81: 136–144. https://www.sciencedirect.com/science/article/pii/S0753332216301767
Elshazly SM, Elhassanny AEM, Mahmoud NM (2020) Cilostazol protects against acetic acid-induced colitis in rats: Possible role for cAMP/SIRT1 pathway. Euro J Pharmacol 881: 173234.https://www.sciencedirect.com/science/article/pii/S0014299920303265
Fang D, Lin Q, Wang C, Zheng C, Li Y, Huang T, Ni F, Wu Z, Chen B, Sun L (2020) Effects of sildenafil on inflammatory injury of the lung in sodium taurocholate-induced severe acute pancreatitis rats. Int Immunopharmacol 80: 106151. https://www.sciencedirect.com/science/article/pii/S1567576919317941
Ganesh Yerra V, Negi G, Sharma SS, Kumar A (2013) Potential therapeutic effects of the simultaneous targeting of the Nrf2 and NF-κB pathways in diabetic neuropathy. Redox Biol 1(1): 394–397. https://www.sciencedirect.com/science/article/pii/S2213231713000578
He F, Ru X, Wen T (2020) NRF2, a Transcription Factor for Stress Response and Beyond. Int J Mol Sci 21(13): 4777. https://pubmed.ncbi.nlm.nih.gov/32640524, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7369905/
Huang W, Liu N, Tong X, Du Y (2022) Sildenafil protects against pulmonary hypertension induced by hypoxia in neonatal rats via activation of PPARγ‑mediated downregulation of TRPC. Int J Mol Med 49(2): 19. https://doi.org/10.3892/ijmm.2021.5074
Jasińska-Stroschein M, Owczarek J, Łuczak A, Orszulak-Michalak D (2013) The beneficial impact of fasudil and sildenafil on monocrotaline-induced pulmonary hypertension in rats: a hemodynamic and biochemical study. Pharmacology 91(3–4):178–184
Jena G, Trivedi PP, Sandala B (2012) Oxidative stress in ulcerative colitis: an old concept but a new concern. Free Radic Res 46(11):1339–1345
Jeong S, Kang C, Park S, Ju S, Yoo JW, Yoon IS, Yun H, Jung Y (2021) Eletrophilic Chemistry of Tranilast Is Involved in Its Anti-Colitic Activity via Nrf2-HO-1 Pathway Activation. Pharmaceuticals (Basel) 14(11)
Jobin C, Sartor RB (2000) NF-kappaB signaling proteins as therapeutic targets for inflammatory bowel diseases. Inflamm Bowel Dis 6(3):206–213
Khodir AE, Said E, Atif H, ElKashef HA, Salem HA (2019) Targeting Nrf2/HO-1 signaling by crocin: role in attenuation of AA-induced ulcerative colitis in rats. Biomed Pharmacother 110:389–399
Lee DS, Kim YK, Jung YW (2010) Simvastatin, sildenafil and their combination in monocrotaline induced pulmonary arterial hypertension. Korean Circ J 40(12):659–664
Lingappan, K. (2018). "NF-κB in Oxidative Stress." Current opinion in toxicology 7: 81–86.https://pubmed.ncbi.nlm.nih.gov/29862377, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5978768/
Liu, T., L. Zhang, D. Joo and S.-C. Sun (2017). "NF-κB signaling in inflammation." Signal transduction and targeted therapy 2: 17023.https://pubmed.ncbi.nlm.nih.gov/29158945, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5661633/
Luna RLdA (2016) Influência de citocinas e fatores de crescimento em modelos murinos de pré-eclampisia de perda gestacional: alvos-terapêuticas alternativos na prevenção do aborto e na má-formação vascular fetal.
Ma Q (2013) Role of nrf2 in oxidative stress and toxicity. Annual review of pharmacology and toxicology 53: 401–426. https://pubmed.ncbi.nlm.nih.gov/23294312, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4680839/
Marklund S, Marklund G (1974) Involvement of the superoxide anion radical in the autoxidation of pyrogallol and a convenient assay for superoxide dismutase. Eur J Biochem 47(3):469–474
Matuszyk A, Ceranowicz P, Warzecha Z, Cieszkowski J, Ceranowicz D, Gałązka K, Bonior J, Jaworek J, Bartuś K, Gil K, Olszanecki R, Dembiński A (2016) Exogenous ghrelin accelerates the healing of acetic acid-induced colitis in rats. Int J Mol Sci 17(9): 1455. https://pubmed.ncbi.nlm.nih.gov/27598133, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5037734/
Medina SVARMRMAFGJVASJRMC (2001) "Therapeutic effect of phenantroline in two rat models of inflammatory bowel disease. Scandinavian J Gastroenterol 36(12): 1314–1319. https://doi.org/10.1080/003655201317097182
Mohey V, Singh M, Puri N, Kaur T, Pathak D, Singh AP (2016) Sildenafil obviates ischemia-reperfusion injury–induced acute kidney injury through peroxisome proliferator–activated receptor γ agonism in rats. J Surg Res 201(1): 69–75. https://www.sciencedirect.com/science/article/pii/S0022480415009440
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95(2):351–358
Parameswaran N, Patial S (2010) Tumor necrosis factor-α signaling in macrophages. Critical Rev Eukaryotic Gene Expression 20(2): 87–103. https://pubmed.ncbi.nlm.nih.gov/21133840, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3066460/
Randhawa, P. K., K. Singh, N. Singh and A. S. Jaggi (2014). "A Review on Chemical-Induced Inflammatory Bowel Disease Models in Rodents." kjpp 18(4): 279–288. https://doi.org/10.4196/kjpp.2014.18.4.279http://www.e-sciencecentral.org/articles/?scid=1025952
Salim M, Amir N, Adeghate E, Ojha S (2021) Nerolidol, a sesquiterpene, attenuates oxidative stress and inflammation in acetic acid-induced colitis in rats. Mol Cell Biochem 476
Sikandaner HE, Park SY, Kim MJ, Park SN, Yang DW (2017) Neuroprotective effects of sildenafil against oxidative stress and memory dysfunction in mice exposed to noise stress. Behavioural Brain Res 319: 37–47. https://www.sciencedirect.com/science/article/pii/S0166432816307203
Surh YJ, Chun KS, Cha HH, Han SS, Keum YS, Park KK, Lee SS (2001) Molecular mechanisms underlying chemopreventive activities of anti-inflammatory phytochemicals: down-regulation of COX-2 and iNOS through suppression of NF-kappa B activation. Mutat Res 480–481:243–268
Venugopal R, Jaiswal AK (1998) Nrf2 and Nrf1 in association with Jun proteins regulate antioxidant response element-mediated expression and coordinated induction of genes encoding detoxifying enzymes. Oncogene 17(24): 3145–3156. http://www.ncbi.nlm.nih.gov/pubmed/9872330, https://www.nature.com/articles/1202237.pdf
Wardyn JD, Ponsford AH,. Sanderson CM (2015) Dissecting molecular cross-talk between Nrf2 and NF-κB response pathways. Biochem Soc Trans 43(4): 621–626 https://pubmed.ncbi.nlm.nih.gov/26551702, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4613495/
Yaseen H, Darwich M, Hamdy H (2012) Is sildenafil an effective therapy in the management of persistent pulmonary hypertension?. J Clin Neonatol 1(4): 171–175 https://pubmed.ncbi.nlm.nih.gov/24027721, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3762043/
Zaghloul MS, Elshal M, Abdelmageed ME (2022) Preventive empagliflozin activity on acute acetic acid-induced ulcerative colitis in rats via modulation of SIRT-1/PI3K/AKT pathway and improving colon barrier. Environ Toxicol Pharmacol: 103833. https://www.sciencedirect.com/science/article/pii/S1382668922000266
Zahran MH, Hussein AM, Barakat N, Awadalla A, Khater S, Harraz A, Shokeir AA (2015) Sildenafil activates antioxidant and antiapoptotic genes and inhibits proinflammatory cytokine genes in a rat model of renal ischemia/reperfusion injury. Int Urol Nephrol 47(11):1907–1915
Acknowledgements
The authors of the manuscript acknowledge Dr. Walla F. Awadin, Professor of Pathology at Mansoura University's Faculty of Veterinary Medicine, for helping in completing the histopathological and IHC portions of this research.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
GE designed the experiments; performed the experiments, analyzed the data, wrote the manuscript and designed the graphical abstract. RA designed the experiments; performed the experiments, analyzed the data, wrote the manuscript, and designed the graphical abstract.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval
The study and the animal care were approved by the Institutional Animal Care and Use Committee (IACUC) at Faculty of Pharmacy, Delta University for Science and Technology, Gamasa, Egypt, with approval number (FPDU 150321/4).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
El-Tanbouly, G.S., Abdelrahman, R.S. The emerging coloprotective effect of sildenafil against ulcerative colitis in rats via exerting counterbalance between NF-κB signaling and Nrf-2/HO-1 pathway. Inflammopharmacol 30, 1351–1362 (2022). https://doi.org/10.1007/s10787-022-01016-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-022-01016-9