Abstract
Objectives
The present study investigated the effectiveness of an 8-week mindfulness mobile phone app on women’s depression, anxiety, stress and mindful attention/awareness in the postnatal period.
Methods
The study enrolled 99 mothers of a child under 1 year old, and randomly assigned them to intervention (n = 49, mean age = 31.11, SD = 4.30, years) and control (n = 50, mean age = 31.35, SD = 5.29, years) groups. Multiple regression examined intervention effects on depression, anxiety, stress and mindful attention/awareness measured post-intervention and at 4-week follow-up, controlling for the baseline and post-intervention measurement of the specific outcome, respectively.
Results
The intervention group showed significant decreases in depression, anxiety and stress levels and an increase of mindful attention/awareness post-intervention compared to the control group, with medium to large effect sizes after controlling for effects of corresponding variables at baseline. The intervention group showed further decrease in depression and stress levels and an increase in mindful attention/awareness at 4 weeks post-intervention compared to the control group, with small to medium effect sizes, after controlling for effects of corresponding variables at post-intervention.
Conclusions
The outcomes of the study suggest that delivery of mindfulness via smartphones could be a viable and affordable resource for reducing postnatal depression, anxiety and stress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Having a child is a significant life shift experienced by new parents. This involves changes in roles, responsibilities and expectations within families and their intimate partner relationships, while at the same time developing a bond with their infant. While there might be expectations that parenthood will be a time of joy and fulfilment, there are substantial stressors that accompany this period that place mothers at risk for emotional and cognitive distress (Yelland et al., 2010).
There are common stressors that accompany the postnatal period, which refers to the first year after birth. The most common stressors are recovering from birth, challenges with breastfeeding and bottle-feeding, lack of sleep, changes in hormones, coping with an unsettled baby, and disturbances in parent and infant bond (Milgrom et al., 2007). These stressors manifest in addition to ongoing household duties, and, for many mothers, resuming work outside the home (Biaggi et al., 2016). Due to these stressors, it is no surprise that there is a substantial body of research evidence demonstrating that a subset of mothers experience a range of mental health problems in the first year after a child’s birth, including anxiety, depression and stress (Camisasca et al., 2021; O’Hara & Swain, 2009; Yelland et al., 2010). To decrease the likelihood of these stressors leading to adverse mental health outcomes, there is a real need for accessible and effective treatments.
Postnatal depression (PND) is a common and serious postpartum mental disorder, affecting an estimated 10–20% of birthing parents during the postpartum period (Corbally & Wilkinson, 2021; Woody et al., 2017), with a disproportionately higher prevalence for those with middle-low income compared to high income (Woody et al., 2017). Beck et al. (2011) found that up to 42% of women experienced elevated postpartum depressive symptoms which did not meet a clinical threshold. However, it has been suggested that less than 50% of women who experience postnatal depressive symptoms will seek any formal assistance (Signal et al., 2017). Women who develop PND have an increased risk of experiencing further episodes of depression, and up to a 41% rate of experiencing PND again with a subsequent child (Cooper & Murray, 1998; Tharwat et al., 2018).
The impact of postnatal depression extends beyond the parent, with associated negative repercussions for the child (Heron et al., 2004). PND can lead to a disruption to healthy mother-infant bonding (Kerstis et al., 2015). Mothers with PND also report significantly higher rates of problematic patterns or perceptions of their infants’ behaviour in relation to feeding, crying and sleeping (Trevarthen & Aitken, 2001), and infants of mothers with PND have a higher risk of delayed motor, neurological, cognitive, language and emotional development, as well as displaying higher rates of distress and avoidance behaviour (O’Connor et al., 2002; Weissman et al., 2006). These adverse consequences can continue well past infancy and into adulthood (Weissman et al., 2006).
Postnatal anxiety is common and frequently co-occurs with postnatal depression, yet it is often neglected in studies of pregnancy and the postnatal period (Heron et al., 2004). Problematic levels of anxiety in the postnatal period have an estimated prevalence of 5–33% (Leach et al., 2017). Those experiencing postnatal anxiety can show impaired decision-making and reduced social functioning (Highet et al., 2014). In some instances, mothers report having feelings of panic, sometimes accompanied with severe and recurrent intrusive thoughts that often focus on their baby (Dennis et al., 2017). Evidence for adverse outcomes for the infants of anxious mothers is growing. Postnatal maternal anxiety has been linked with emotional and behavioural maladjustment of the infant (Bauer et al., 2015; Bekkhus et al., 2011; O’Connor et al., 2002; Rees et al., 2019).
Stress is a distinct adverse emotional state involving heightened arousal and impaired function (Lovibond & Lovibond, 1995). Significantly elevated stress levels in the postpartum period have been shown to affect approximately 40% of women in developed nations (Anniverno et al., 2013; Beck et al., 2011; Miller et al., 2006). Postnatal depression, anxiety and stress are all unique and separate experiences of distress that can interact and influence each other. Meta-analytic reviews have consistently identified stress within the postnatal period to be a significant risk factor that can contribute to the development of and precipitate PND and anxiety (Bernazzani et al., 1997; O’Hara & Swain, 2009). Research examining the course of postnatal depression suggests that anxiety may develop into depression as a result of the inability to manage stress (Heron et al., 2004). Another study found the symptoms of depression to be linked to the degree of stress (Terry et al., 1996).
Mindfulness-based interventions (MBIs) are structured psychological interventions that incorporate mindfulness practice. MBIs are designed with the intent to teach the individual to cultivate mindfulness and incorporate its practice into everyday life (Kabat-Zinn, 2003). They have been found beneficial for many conditions and issues, such as decreasing stress (Economides et al., 2018), anxiety (Quinones & Griffiths, 2019), depression (Flett et al., 2018), aggression (Shastri et al., 2017), compulsive internet use (Quinones & Griffiths, 2019) and job strain (Bostock et al., 2019) and increasing well-being (Howells et al., 2016), resilience (Flett et al., 2018), self-compassion (Dunn et al., 2012) and perceptions of workplace social support (Bostock et al., 2019). Dispositional mindfulness has been found to be inversely predictive of perinatal distress, with lower levels of mindfulness associated with elevated levels of depression, stress and anxiety (Kalmbach et al., 2020; Khan & Laurent, 2019).
There is growing evidence that MBIs have the potential to reduce depression, anxiety and stress for mothers in the perinatal period. A meta-analysis and systemic review of the effectiveness of MBIs in the perinatal period revealed significant reduction of depression, anxiety and stress concurrent with increases in mindfulness skills (Taylor et al., 2016). Of the studies assessed in this review, the majority (94%) were group-administered, in-person interventions. A recent meta-analysis of the effectiveness of MBIs delivered in the prenatal period also found them to be effective in reducing depression, anxiety and stress in pregnant participants (Corbally & Wilkinson, 2021). Moreover, MBIs have been shown to further improve well-being outcomes when combined with pharmacological treatment (Shulman et al., 2018). Notably, research has shown that that 8-week MBIs produced significant reductions in postnatal participants’ overall distress, depression and stress at follow-ups ranging from 8 weeks to 18 months (Ahmadpanah et al., 2018; Dimidjian et al., 2016; Felder et al., 2018; Pan et al., 2019). Even further decreases of PND have been seen at 3-month follow-up (Shulman et al., 2018).
Mindfulness refers to the ability to maintain attention to and awareness of present-moment experiences, emotions, thought and physical sensations as they unfold while maintaining a non-judgmental attitude (Kabat-Zinn, 2003). In the clinical context, there are various operational definitions, but the general consensus is that mindfulness levels can be described as the non-judgmental observation of the continuing surge of internal and external stimuli as they occur (Feng et al., 2018). Mindfulness levels can be measured as state and dispositional factors. State mindfulness is the quality of mindful presence at a given moment, or within a narrow window of time (e.g. the past 5 min), whereas dispositional or trait mindfulness refers to the general, cross-situational frequency of mindful states over time (Brown & Ryan, 2003).
In perinatal research on the effects of mindfulness, levels of stress, depression and anxiety are often studied separately, but rarely together (Felder et al., 2016; Fontein-Kuipers et al., 2014; Khan & Laurent, 2019; Townshend & Caltabiano, 2019; Townshend et al., 2018). It has been argued that research within the perinatal period frequently labels coexisting symptoms of postpartum depression and anxiety as PND without differentiating between these experiences (Miller et al., 2006). Because these factors are separate and affect the individual uniquely, research measuring all three symptoms is important to better understand how these separate experiences distinctively respond to interventions. Within the literature reviewed, one study was located that investigated the effect of an 8-week mindful parenting intervention on levels of stress, depression and anxiety, using a pre-post design method. They assessed symptoms of depression, anxiety and stress via the DASS21 at pre-test, post-test and 8-week follow-up (Potharst et al., 2022). They found significant reductions in all outcome variables at both measurement points apart from anxiety at the 8-week follow-up.
Evidence has showed that in-person, group-based MBIs can have a significant impact on perinatal well-being. However, Taylor et al. (2016) noted that retention rates in these interventions average about 75%, highlighting barriers to accessing this type of programmes. There are accessibility barriers for mothers that may limit the ability to physically attend face-to-face treatment. Interviews have revealed structural barriers to services to be greater obstacles than knowledge and attitudinal barriers, with the greatest structural barriers reported being lack of time, finances, transport and childcare (Goodman, 2009; O’Mahen & Flynn, 2008).
In response to overcoming these structural barriers, MBIs delivered on an application (app) via a smartphone are growing in popularity (Marshall et al., 2020). MBIs delivered via app (aMBI) have been shown to significantly reduce anxiety and depressive symptoms (Gál et al., 2021), irritability, affect and stress resulting from personal vulnerability, external pressure (Economides et al., 2018) and compulsive internet use (Quinones & Griffiths, 2019). In addition, they have been found to increase job-related well-being (Bostock et al., 2019), resilience (Flett et al., 2018) and positive affect (Howells et al., 2016). There has been little research examining the effectiveness of aMBIs in the postnatal period, highlighting a gap in literature. A recent scoping review of mobile-based psychological interventions for perinatal depression and anxiety only identified one study of the effectiveness of aMBI, from the 22 studies reviewed (Hussain-Shamsy et al., 2020).
The current study sought to investigate the effectiveness of an 8-week aMBI aiming to reduce experiences of depression, anxiety and stress in mothers during the postnatal period. It was hypothesised that depression, anxiety and stress levels in mothers who participate in the 8-week app-based mindfulness intervention would be significantly reduced compared to the active control condition, with further improvements seen at 4-week follow-up. It was also hypothesised that levels of mindful attention/awareness in those who participated in the 8-week mindfulness intervention would be significantly increased compared to the control condition, with further improvements seen at 4-week follow-up.
Method
Participants
Recruitment of participants was conducted through social media posts on pages that targeted mothers, primarily focusing on New Zealand mothers, but with some dissemination in Australian groups. Recruitment took place between October 14, 2019, and March 25, 2020. Inclusion criteria consisted of (a) being the mother of a child aged 0–12 months and (b) access to a smartphone that can download applications. New Zealand went into a strict lockdown on March 25, 2020, in response to the COVID-19 pandemic. Due to this major disruption and its unknown effects on social and psychological functioning, recruitment was discontinued at that point.
A total of 99 participants enrolled in the study and were randomly assigned to treatment and control groups. There were 49 participants assigned to the experimental group, with 50 participants assigned to the control group. Demographic characteristics of the mothers for each condition are shown in Table 1. Preliminary analysis confirmed that there were no statistically significant differences between the two groups at baseline for age, mindful attention/awareness and distress outcome variables.
Procedures
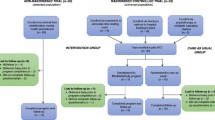
The study used a pre- to post-RCT design that tested the effect of a mindfulness app (Smiling Mind) on distress levels in the postnatal period, relative to a control app (Baby + Tracker). This study required women to use an app for 8 weeks, and respond to a battery of assessment tools to measure baseline (T1), post-intervention (T2) and 4-week follow-up scores (T3). See Fig. 1 for flow diagram. The trial was not preregistered.
There were a total of four formal withdrawals from the study citing inadequate time to use the app (2), the app being incompatible with their phone (1) and no reason given (1). A further 38 dropped out of the study by not completing the post-intervention (T2) survey. A total of 56 participants completed the T2 survey, with 27 participants in the experimental group and 29 participants in the control group. A further 27 did not complete the 4-week follow-up (T3) survey, resulting in a total of 30 participants completing both the intervention and follow-up survey with 15 participants in the experimental group and 15 participants in the control group.
Using the online survey platform Qualtrics, participants read the information sheet and gave informed consent by confirming they had read the information provided and were ready to begin the study. The participants then completed the questionnaires and were randomly assigned to either the experimental or control condition. Participants were instructed to download the applicable app and use it for 8 weeks. Participants in the experimental condition were encouraged to complete one session per day (session duration in minutes: M = 9.20), with the request to complete a minimum of three sessions per week. The control condition was encouraged to use the smartphone application that offers a combination of postnatal support and information unrelated to mindfulness for about 10 min per day, with the request to use it a minimum of three sessions per week. Participants were sent out a weekly SMS reminding them to use the app. On completion of the 8 weeks and at 4-week follow-up, participants were sent a link to complete measures of distress and mindful attention/awareness. If surveys were not completed, then up to two reminder SMS were sent. Participants were debriefed on the study after the final scale was completed.
Intervention
Smiling Mind Application
Smiling Mind (Smiling Mind, 2021) is a smartphone application that offers hundreds of hours of guided and unguided mindfulness meditation practices across several different mindfulness programmes. Smiling Mind is available free of charge on iOS and Android platforms and through the Smiling Mind website. Participants randomised to the Smiling Mind condition were instructed to download the app and use the ‘Mindfulness Foundations’ programme. The ‘Mindfulness Foundations’ programme features 10 modules over 41 sessions. The meditation sessions vary in duration from 1 to 43 min (M = 9.20). The ten modules cover the topics of the following: the Breath, Sound and Taste, Thoughts, Emotions, Everyday Mindfulness, Curiosity and Beginner’s Mind, Stress, Sleep and Gratitude, Relationships and Mindful Listening. The ‘Mindfulness Foundations’ programme is an introduction to mindfulness and not aimed specially for the postnatal period.
Control Condition
Baby + Tracker Application
Baby + Tracker (Philips Electronics UK, 2021) is a smartphone application that offers a combination of postnatal support and information, tracking infant progress, milestones and daily routine, and capturing memorable moments. Baby + Tracker is available free of charge on iOS and Android platforms. The support and information component includes information such as week by week development information, parenting and breastfeeding guides. The tracking of infant progress and milestones and daily routine components includes a baby growth and sleep tracker, milestones log and health tracker. The capture memorable moments component gives options to store and retrieve photos and videos of the infant.
Measures
Participants completed three scales to assess levels of distress and mindful attention/awareness, as well as a demographic questionnaire. Demographic information collected included the age of participant and infant, ethnicity, relationship status, country of residence, history of practising mindfulness and current use of support apps for postpartum support.
Depression Anxiety and Stress Scale Short Form (DASS21)
The DASS21 (Lovibond & Lovibond, 1995) is a 21-item self-report measure that assesses symptoms of depression, anxiety and stress. Using a 4-point Likert-type scale ranging from 0 (did not apply to me at all) to 3 (applied to me very much, most of the time), participants were asked to indicate how much each statement applied to them over the past 7 days. The DASS21 produces subscales of Depression (DASS-D), Anxiety (DASS-A) and Stress (DASS-S) by summing the scores for each of the seven relevant items for each subscale. Scores range from 0 to 21 for each subscale, with higher scores indicating higher symptomatology. The raw score of the DASS21 were used for interpretation. Scores can be categorised into normal, mild, moderate, severe and extremely severe. The DASS21 was developed in Australia and is commonly used in Australasia (Crawford et al., 2011). The depression subscale does not include somatic symptoms and therefore is appropriate for use in postnatal assessment (Barber & Steadman, 2018). The DASS21 has been previously shown to have high internal consistency for all subscales: DASS-D (α = 0.94; McDonald’s ω = 0.86), DASS-A (α = 0.87; McDonald’s ω = 0.82) and DASS-S (α = 0.91; McDonald’s ω = 0.88; Antony et al., 1998; Osman et al., 2012). Internal consistency in the current study was high for all subscales: DASS-D (α = 0.95), DASS-A (α = 0.93) and DASS-S (α = 0.90).
Mindful Attention Awareness Scale (MAAS)
The MAAS (Brown & Ryan, 2003) is a 15-item scale that measures core characteristics of mindful attention/awareness. Using a 6-point Likert-type scale ranging from 1 (Almost always) to 6 (Almost never), participants were asked to indicate how frequently or infrequently they had each experience. The scores range from 0 to 90, with higher scores indicating higher levels of mindful attention/awareness. The MAAS is widely used in studying mindfulness interventions and has been previously shown to have high internal consistency (α = 0.92; McDonald’s ω = 0.93; González-Blanch et al., 2022). Internal consistency in the current study was high (α = 0.94).
Data Analyses
Statistical analyses were conducted using IBM SPSS v. 26 for Windows. Preliminary analyses examined baseline group differences and found no statistically significant difference between the groups on any measure. The hypotheses and research questions were subsequently examined by conducting separate sets of hierarchical multiple regression while controlling for baseline levels of outcome variables. The presented descriptions of the magnitude of the effects of R2 follow the general definitions of R2 of 0.02 as small, 0.15 as medium and 0.26 as large (Cohen, 1988). Statistical significance was also evaluated and significance levels of less than 0.05 are reported as significant.
The target sample size was determined based on previous research by Taylor et al. (2016), who conducted a meta-analysis of studies on mindfulness-based interventions on distress in the perinatal period, yielding average medium effect sizes of Hedge’s g = 0.47 for depression, 0.36 for anxiety and 0.51 for stress. Minimum required sample size for regression analyses (n = 52) was determined using G*Power based on 85% certainty to detect a medium effect size (R2 = 0.15) under p = 0.05 (Faul et al., 2007). Regression analyses were used in order to maximise statistical power while still allowing to control for initial level on the outcome variables.
Tests of statistical assumptions were independently conducted for each analysis at post-intervention and follow-up and are only reported where violations of these assumptions were observed. For the regressions of intervention on DASS-depression, DASS-anxiety and DASS-stress, an inspection of distributions indicated there was a positive skew on DASS-depression, DASS-anxiety and DASS-stress. Square root transformations resulted in normal distributions; therefore, the transformed data for these variables were used for inferential statistics. The remaining variables were normally distributed and free from univariate outliers.
Inspection of the normal probability plot of standard residuals as well as the scatter plot of standardised residuals against standardised predicted values indicated that assumptions of normality, linearity and homoscedasticity of residuals were met. There was no evidence of multicollinearity, as assessed by tolerance values greater than 0.1. There were no studentised residuals greater than ± 3 standard deviations, leverage values greater than 0.2 and values for Cook’s distance above 1. Prior to calculating r of the associations between mindful attention/awareness and distress levels, the assumptions of normality, linearity and homoscedasticity were assessed. Visual inspection of the normal Q-Q plots of each variable confirmed that both were normally distributed.
To check for differential dropout, a comparison was conducted between the participants that completed and dropped out at T2, and those that completed and dropped out at T3 on MAAS, DASS-depression, DASS-anxiety and DASS-stress subscales, age of child and age of participant. Two significant differences were found at T2, suggesting that completers scored higher than dropouts on initial ratings of DASS-depression and DASS-anxiety (DASS-D, F(1, 56) = 4.91, p = 0.03, completers M = 6.07, SD = 6.3, drop outs M = 3.65, SD = 3.84; DASS-S, F(1, 56) = 8.21, p = 0.005, completers M = 9.80, SD = 5.35, drop outs M = 7.00, SD = 3.84).
Results
Descriptive statistics for the outcome variables by condition at T1, T2 and T3 for all participants who completed the assessments are presented in Table 2. At the T3 assessment, all participants were asked if they were still using the applicable app. Sixty percent (9/15) of the intervention group participants that completed T3 and 13% (2/15) of the control group participants that completed T3 reported they were still using the app. Treatment adherence data was collected at T2 and T3. At T2, 90% (44/49) of the intervention group and 86% (43/50) of the control group participants reported 3 ≥ sessions per week, 6% (3/49) of the intervention group and 4% (2/50) of the control group participants reported 1–2 sessions per week, and 4% (2/49) of the intervention group and 10% (5/50) of the control group participants reported ≤ 1 session per week. At T3, 93% (14/15) of the intervention group and 93% (14/15) of the control group participants reported 3 ≥ sessions per week, 7% (1/15) of the intervention group and 0% (0/15) of the control group participants reported 1–2 sessions per week, and 0% (0/15) of the intervention group and 7% (1/15) of the control group participants reported ≤ 1 session per week.
Several linear regression models were tested with intervention (vs control) as a predictor variable and outcomes of T2 depressive (DASS-D-T2), anxiety (DASS-A-T2), stress (DASS-S-T2) and mindful attention/awareness levels (MAAS-T2), at post-intervention. The mindfulness intervention demonstrated a large effect on DASS-D-T2, accounting for 45% of variance, large effect on DASS-A-T2, accounting for 41% of variance, a large effect on DASS-S-T2, accounting for 56% of variance, and a large effect on MAAS-T2, accounting for 63% of variance These findings were all statistically significant (Table 3).
Several linear regression models were tested with intervention (vs control) as a predictor variable and outcomes of T2 depressive (DASS-D-T3), anxiety (DASS-A-T3), stress (DASS-S-T3) and mindful attention/awareness levels (MAAS-T2), at the 3-month follow-up. The mindfulness intervention demonstrated a large effect on DASS-D-T3, accounting for 48% of variance, large effect on DASS-A-T3, accounting for 27% of variance, a large effect on DASS-S-T3, accounting for 53% of variance, and a large effect on MAAS-T3, accounting for 62% of variance. These findings were all statistically significant (Table 4).
A percentage of participants scored in the mild and higher above depression, anxiety and stress symptoms at all time points in both conditions. The percentage decreased after the intervention and at 4-week follow-up in the intervention but not in the control group (Table 2).
Discussion
This study examined the effectiveness of participation in the 8-week app-based mindfulness course, compared to an active control, on distress and mindful attention/awareness levels during the postpartum period. The results demonstrated that the app-based mindfulness intervention significantly decreased depression, anxiety and stress and increased mindful attention/awareness post-intervention and at the 4-week follow-up, all showing large effect sizes. These findings suggest that delivery of mindfulness via smartphones could be beneficial for reducing postnatal depression, anxiety and stress while enhancing mindful attention and awareness. Overall, these results are consistent with the findings of previous studies in which an 8-week face-to-face mindfulness intervention resulted in significantly lower levels of depression, anxiety and stress (Fontein-Kuipers et al., 2014; Potharst et al., 2017, 2022).
Previous research with women with postnatal depression has found an 8-week face-to-face mindfulness intervention paired with pharmacological treatment resulted in significantly lower levels of depression than pharmacological treatment alone (Ahmadpanah et al., 2018). These findings suggest that women prescribed medication for postnatal depression could benefit from concurrently using an app that supports mindfulness such as the Smiling Mind app and merits further investigation.
The positive effect of the mindfulness intervention on stress levels is consistent with research by Potharst et al. (2017) showing 8 weeks of mindfulness classes resulted in significant reductions on levels of postnatal stress. The postnatal period has been found to be characterised by increased levels of stress (Anniverno et al., 2013; Beck et al., 2011; Miller et al., 2006); however, depression and anxiety have received much more attention in the literature on interventions in the postnatal period (Felder et al., 2016; Fontein-Kuipers et al., 2014; Khan & Laurent, 2019; Townshend & Caltabiano, 2019; Townshend et al., 2018). This neglect of stress measurements results in the paucity of information around the effect of interventions on subjective stress. Elevated stress is more prominent in the perinatal period than depression and anxiety, affecting 40% of women in developed nations (Anniverno et al., 2013; Beck et al., 2011; Miller et al., 2006). Mothers in the postnatal period may experience high levels of stress without having high levels of depression or anxiety. This study suggests that the use of a mindfulness app can decrease levels of stress in the postnatal period.
The intervention had a large effect on anxiety, which is consistent with published literature, which found that 8-week MBIs resulted in significant decreases in levels of postpartum anxiety (Fontein-Kuipers et al., 2014; Shulman et al., 2018; Taylor et al., 2016). Anxiety can be very disruptive during the postnatal period, so an accessible, effective intervention that addresses it in addition to helping to manage stress and mood is promising and merits further investigation.
The percentage of participants scoring in the mild and higher above depression, anxiety and stress symptoms decreased after the intervention and at 4-week follow-up in the intervention but not in the control group. The trends in the current study show the strongest effects on stress, followed by depression, with the least impact being on anxiety. These patterns of effectiveness are consistent with the meta-analysis by Taylor et al. (2016), showing the same pattern of effectiveness of MBI on stress, depression and anxiety.
A significant and large increase in mindful attention/awareness levels was observed at both post-intervention and the 4-week follow-up for the treatment group. Meta-analytic reviews found that MBIs that failed to increase levels of mindfulness were ineffective in decreasing depression and stress in the perinatal period (Corbally & Wilkinson, 2021; Taylor et al., 2016). The similarities in the findings of the current study and previous research suggest that MBIs delivered face-to-face or via an app may result in similar mechanisms of change, with increases in mindfulness resulting in positive outcomes.
Recent systematic reviews and meta-analyses showed that mobile-based psychological interventions can be effective to prevent depression, anxiety and stress in the general population (Rigabert et al., 2020; Sander et al., 2016), but the evidence is scarce concerning outcomes in the postnatal period. The positive findings of this study suggest that app-based mindfulness interventions may be as effective as face-to-face MBI, with the additional benefit of reducing the barriers to physically attending interventions.
The delivery method of using the app and the free cost mean this intervention can be done in private, which is accessible to anyone with a smartphone, with the only costs being data to download and use the app. This overcomes the barriers to treatment of affordability, transportation, stigma and childcare issues (Ashford et al., 2018; Goodman, 2009; O’Mahen & Flynn, 2008), and may help overcome the barrier to treatment of lack of time (Ashford et al., 2018; Goodman, 2009; O’Mahen & Flynn, 2008). With regard to sustained improvement after the intervention, we observed a continuation of large treatment effects on all factors.
The improvements on depression, anxiety stress and mindful attention/awareness levels continued after the end of the formal intervention; 60% of those who responded at T3 were continuing to use the aMBI app (versus 13% of controls), so this may be an effect of continuing mindfulness practice, rather than true post-intervention change. In the Shulman et al. (2018) study of an in-person MBI that found even further improvements in levels of mindfulness and depression after the intervention, the participants were encouraged to practise mindfulness at home (Shulman et al., 2018). However, Shulman et al. did not report whether participants were practising at home after the intervention ceased. The app for the current mindfulness intervention offered a variety of different mindfulness sessions, rather than being a specific 8-week mindfulness course. This does highlight an opportunity to investigate what characteristics of mindfulness programmes or sessions (e.g. length of sessions, guided vs. unguided, gamification/reinforcement) are associated with continued practice.
The dropout rate for the present study was 43% at T2. Although this is substantial, this rate is not unusual compared to a similar app-based 8-week MBCT intervention aimed at postpartum women, which recorded a dropout rate of 92% at post-intervention (Sun et al., 2021). In the current study, the apps used were chosen based on high user ratings, and this may have contributed to higher retention. In addition, the weekly reminder SMS text messages may have influenced participation. In terms of differential dropout, there were some notable differences between the participants that dropped out and those that completed the interventions. Participants that completed the interventions had significantly higher self-reported levels of depression and stress at the initial assessment point. This suggests that people with depression may be more motivated to complete MBI in app format than mothers who are feeling less distress.
To the best of our knowledge, there is lack of research investigating the effect of an aMBI on mothers’ depression, anxiety and stress levels in postnatal period. The randomised assignment and use of an active control are central strengths of the study. Meta-analytic reviews on MBI in the perinatal period highlighted a lack in rigorous methods and consistency in intervention and outcome measures. One issue frequently highlighted was lack of randomised controlled trials; even in those with control groups, most were assigned to treatment as usual or waitlist (Corbally & Wilkinson, 2021; Taylor et al., 2016). The postnatal period may show a trend of decreased distress over time even without treatment (Takehara et al., 2020), so a control group is particularly important to minimise the chance of overstating gains. Another strength was measurement of depression, anxiety and stress as separate experiences. The segregation of the components of distress is important to be able to investigate treatment effects on differing negative emotions. This allows recommendations of interventions that are suitable for the particular individual’s type of emotional distress.
Limitations and Directions of Future Research
One major challenge this study faced was the context of the COVID-19 pandemic that was starting to escalate during the time many of the women in this study were participating in the intervention. This affected the sample size and may have affected levels of stress and anxiety. Another limitation was the dropout rate of the present study, of 43% at T2 and 70% at T3. This poses a threat to the validity of results as participants that completed the intervention may differ from the participants that dropped out, and may have benefited more from the intervention. A larger sample size would allow for more detailed evaluation of patterns of change, and more confidence to detect small-sized effects. It is possible that the minimal impact on anxiety found in this study may be in part related to the overall context of high anxiety, but this cannot be examined with the data collected. It is notable that significant effects were found even in the context of this very stressful and isolating context.
A limitation of using multiple self-report measures, which potentially increases the risk of common methods bias, should also be acknowledged. The DASS21 and MAAS require the participants to report their own perceptions, which can be influenced by bias such as priming effects and social desirability, leading to spurious effects as a result of the measurement instruments rather than to the constructs being measured (Podsakoff et al., 2012).
Another limitation of this study is the assessment of mindfulness using the MAAS scale, which is not capturing all relevant facets of mindfulness. For instance, psychometric research has established mindfulness as a multidimensional construct consisting of distinct facets such as observing, describing, acting with awareness, nonreacting and non-judging (Baer et al., 2006). Brown and Ryan (2003) have suggested the MAAS scale more accurately records acting with awareness rather than true mindfulness. A disadvantage of the unidimensional MAAS is that it only allows investigation of mechanisms involved in acting with awareness, which neglects a comprehensive investigation of the overarching mindfulness.
In the initial assessment, participants that completed the intervention reported higher levels of depression and stress than those that dropped out. This indicated those with higher levels of depression and stress may be more likely to persist with this kind of intervention. It would be worth investigating which aspects of mobile applications are related to participants continuing their use.
The current intervention is both remote and autonomous, and relied on participants to report their estimated usage. It would be beneficial to implement tracking of the meditation sessions to improve accuracy. Gathering more precise information into the usage of sessions could give some further insight regarding dropouts, optimal number of sessions for maximum efficacy and optimal session times for retention.
The current study’s inclusion criteria were exclusively targeted at mothers. This is consistent with much of the previous research on mindfulness in the perinatal period, but it would be beneficial to extend research to include the experience of new fathers, who are coping with increased levels of transition and stress at this time, and are often neglected in research on the perinatal mental health (Wong et al., 2016).
App-based mindfulness interventions are a promising tool to support new parents in the complex, stressful, but also rich and rewarding process of transition to parenthood. This study has demonstrated that a freely available mindfulness app can have a substantial impact on levels of depression, anxiety and stress for mothers of infants, and thus constitutes a viable option for promoting well-being in early parenthood.
Data Availability
The data that support the findings of this study are openly available in Open Science Framework at DOI 10.17605/OSF.IO/QPUZW.
References
Ahmadpanah, M., Nazaribadie, M., Aghaei, E., Ghaleiha, A., Bakhtiari, A., Haghighi, M., Bahmani, D. S., Akhondi, A., Bajoghli, H., Jahangard, L., Holsboer-Trachsler, E., & Brand, S. (2018). Influence of adjuvant detached mindfulness and stress management training compared to pharmacologic treatment in primiparae with postpartum depression. Archieves of Womens Mental Health, 21(1), 65–73. https://doi.org/10.1007/s00737-017-0753-6
Anniverno, R., Bramante, A., Mencacci, C., & Durbano, F. (2013). Anxiety disorders in pregnancy and the postpartum period. In F. Durbano. (Ed.) New insights into anxiety disorders 259–285. InTech Open Book Series. https://doi.org/10.5772/52786
Antony, M. M., Bieling, P. J., Cox, B. J., Enns, M. W., & Swinson, R. P. (1998). Psychometric properties of the 42-item and 21-item versions of the Depression Anxiety Stress Scales in clinical groups and a community sample. Psychological Assessment, 10(2), 176–181. https://doi.org/10.1037/1040-3590.10.2.176
Ashford, M. T., Olander, E. K., & Ayers, S. (2016). Computer- or web-based interventions for perinatal mental health: A systematic review. Journal of Affective Disorders, 197, 134–146. https://doi.org/10.1016/j.jad.2016.02.057
Ashford, M. T., Olander, E. K., Rowe, H., Fisher, J. R., & Ayers, S. (2018). Feasibility and acceptability of a web-based treatment with telephone support for postpartum women with anxiety: Randomized controlled trial. JMIR Mental Health, 5(2), e19. https://doi.org/10.2196/mental.9106
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13(1), 27–45. https://doi.org/10.1177/1073191105283504
Barber, C. C., & Steadman, J. (2018). Distress levels in pregnant and matched non-pregnant women. Australian & New Zealand Journal of Obstetrics & Gynaecology, 58(1), 128–131. https://doi.org/10.1111/ajo.12712
Bauer, A., Knapp, M., & Parsonage, M. (2015). Lifetime costs of perinatal anxiety and depression. Journal of Affective Disorders, 192, 83–90. https://doi.org/10.1016/j.jad.2015.12.005
Beck, C. T., Gable, R. K., Sakala, C., & Declercq, E. R. (2011). Posttraumatic stress disorder in new mothers: Results from a two‐stage U.S. national survey. Birth: Issues in Perinatal Care, 38(3), 216–227. https://doi.org/10.1111/j.1523-536X.2011.00475.x
Bekkhus, M., Rutter, M., Barker, E. D., & Borge, A. I. H. (2011). The role of pre- and postnatal timing of family risk factors on child behavior at 36 months. Journal of Abnormal Child Psychology, 39(4), 611–621. https://doi.org/10.1007/s10802-010-9477-z
Bernazzani, O., Saucier, J.-F., David, H., & Borgeat, F. (1997). Psychosocial predictors of depressive symptomatology level in postpartum women. Journal of Affective Disorders, 46(1), 39–49. https://doi.org/10.1016/S0165-0327(97)00077-3
Biaggi, A., Conroy, S., Pawlby, S., & Pariante, C. M. (2016). Identifying the women at risk of antenatal anxiety and depression: A systematic review. Journal of Affective Disorders, 191, 62–77. https://doi.org/10.1016/j.jad.2015.11.014
Bostock, S., Crosswell, A. D., Prather, A. A., & Steptoe, A. (2019). Mindfulness on-the-go: Effects of a mindfulness meditation app on work stress and well-being. Journal of Occupational Health Psychology, 24(1), 127–138. https://doi.org/10.1037/ocp0000118
Brown, K. W. & Ryan, R. M. (2003). The benefits of being present: Mindfulness and its role in psychological well-being. Journal of Personality and Social Psychology, 84, 822–848. https://doi.org/10.1037/t04259-000
Camisasca, E., Di Blasio, P., Milani, L., & Miragoli, S. (2021). Postpartum depressive symptoms as a linking mechanism between maternal sleep and parenting stress: The conditional indirect effect by social support. Children’s Health Care, 50(1), 64–82. https://doi.org/10.1080/02739615.2020.1824675
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd Ed.). Routledge. https://ci.nii.ac.jp/naid/10029716665/
Cooper, P. J., & Murray, L. (1998). Postnatal depression. BMJ : British Medical Journal, 316(7148), 1884. https://doi.org/10.1136/bmj.316.7148.1884
Corbally, L., & Wilkinson, M. (2021). The effect of mindfulness-based interventions on stress, depression and anxiety during the perinatal period in women without pre-existing stress, depressive or anxiety disorders: A systematic review and meta-analysis of controlled trials. Mindfulness, 12(10), 2357–2370. https://doi.org/10.1007/s12671-021-01697-3
Crawford, J., Cayley, C., Lovibond, P. F., Wilson, P. H., & Hartley, C. (2011). Percentile norms and accompanying interval estimates from an Australian general adult population sample for self-report mood scales (BAI, BDI, CRSD, CES-D, DASS, DASS-21, STAI-X, STAI-Y, SRDS, and SRAS). Australian Psychologist, 46(1), 3–14. https://doi.org/10.1111/j.1742-9544.2010.00003.x
Dennis, C.-L., Brown, H. K., Falah-Hassani, K., Marini, F. C., & Vigod, S. N. (2017). Identifying women at risk for sustained postpartum anxiety. Journal of Affective Disorders, 213, 131–137. https://doi.org/10.1016/j.jad.2017.02.013
Dimidjian, S., Goodman, S., Felder, J., Gallop, R., Brown, A., & Beck, A. (2016). Staying well during pregnancy and the postpartum: A pilot randomized trial of mindfulness-based cognitive therapy for the prevention of depressive relapse/recurrence. Journal of Consulting and Clinical Psychology, 84(2), 134. https://doi.org/10.1037/ccp0000068
Dunn, C., Hanieh, E., Roberts, R., & Powrie, R. (2012). Mindful pregnancy and childbirth: Effects of a mindfulness-based intervention on women’s psychological distress and well-being in the perinatal period. Archives of Women’s Mental Health, 15(2), 139–143. https://doi.org/10.1007/s00737-012-0264-4
Economides, M., Martman, J., Bell, M. J., & Sanderson, B. (2018). Improvements in stress, affect, and irritability following brief use of a mindfulness-based smartphone app: A randomized controlled trial. Mindfulness, 9(5), 1584–1593. https://doi.org/10.1007/s12671-018-0905-4
Faul, F., Erdfelder, E., Lang, A. G., & Buchner, A. (2007). G* Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods, 39(2), 175–191. https://doi.org/10.3758/BF03193146
Felder, J. N., Lemon, E., Shea, K., Kripke, K., & Dimidjian, S. (2016). Role of self-compassion in psychological well-being among perinatal women. Archives of Womens’ Mental Health, 19(4), 687–690. https://doi.org/10.1007/s00737-016-0628-2
Felder, J. N., Roubinov, D., Bush, N. R., Coleman-Phox, K., Vieten, C., Laraia, B., Adler, N. E., & Epel, E. (2018). Effect of prenatal mindfulness training on depressive symptom severity through 18-months postpartum: A latent profile analysis. Journal of Clinical Psychology, 74(7), 1117–1125. https://doi.org/10.1002/jclp.22592
Feng, X. J., Krägeloh, C. U., Billington, D. R., & Siegert, R. J. (2018). To what extent is mindfulness as presented in commonly used mindfulness questionnaires different from how it is conceptualized by senior ordained Buddhists? Mindfulness, 9(2), 441–460. https://doi.org/10.1007/s12671-017-0788-9
Flett, J. A. M., Hayne, H., Riordan, B. C., Thompson, L. M., & Conner, T. S. (2018). Mobile mindfulness meditation: A randomised controlled trial of the effect of two popular apps on mental health. Mindfulness, 10(5), 863–876. https://doi.org/10.1007/s12671-018-1050-9
Fontein-Kuipers, Y. J., Nieuwenhuijze, M. J., Ausems, M., Budé, L., & de Vries, R. (2014). Antenatal interventions to reduce maternal distress: A systematic review and meta-analysis of randomised trials. BJOG: An International Journal of Obstetrics & Gynaecology, 121(4), 389–397. https://doi.org/10.1111/1471-0528.12500
Gál, É., Ștefan, S., & Cristea, I. A. (2021). The efficacy of mindfulness meditation apps in enhancing users’ well-being and mental health related outcomes: A meta-analysis of randomized controlled trials. Journal of Affective Disorders, 279, 131–142. https://doi.org/10.1016/j.jad.2020.09.134
González-Blanch, C., Medrano, L. A., O’Sullivan, S., Bell, I., Nicholas, J., Chambers, R., Gleeson, J. F., & Alvarez-Jimenez, M. (2022). Psychometric properties of the Mindful Attention Awareness Scale (MAAS) in a first-episode psychosis sample. Psychological Assessment, 34(2), 188–196. https://doi.org/10.1037/pas0001077
Goodman, J. H. (2009). Women’s attitudes, preferences, and perceived barriers to treatment for perinatal depression. Birth: Issues in Perinatal Care, 36(1), 60–69. https://doi.org/10.1111/j.1523-536X.2008.00296.x
Heron, J., O’Connor, T. G., Evans, J., Golding, J., & Glover, V. (2004). The course of anxiety and depression through pregnancy and the postpartum in a community sample. Journal of Affective Disorders, 80(1), 65–73. https://doi.org/10.1016/j.jad.2003.08.004
Highet, N., Stevenson, A. L., Purtell, C., & Coo, S. (2014). Qualitative insights into women’s personal experiences of perinatal depression and anxiety. Women and Birth, 27(3), 179–184. https://doi.org/10.1016/j.wombi.2014.05.003
Howells, A., Ivtzan, I., & Eiroa-Orosa, F. J. (2016). Putting the ‘app’ in happiness: A randomised controlled trial of a smartphone-based mindfulness intervention to enhance wellbeing. Journal of Happiness Studies, 17(1), 163–185. https://doi.org/10.1007/s10902-014-9589-1
Hussain-Shamsy, N., Shah, A., Vigod, S. N., Zaheer, J., & Seto, E. (2020). Mobile health for perinatal depression and anxiety: Scoping review. Journal of Medical Internet Research, 22(4), e17011–e17011. https://doi.org/10.2196/17011
Kabat-Zinn, J. (2003). Mindfulness-based interventions in context: Past, present, and future. Clinical Psychology: Science and Practice, 10(2), 144–156. https://doi.org/10.1093/clipsy/bpg016
Kalmbach, D. A., Roth, T., Cheng, P., Ong, J. C., Rosenbaum, E., & Drake, C. L. (2020). Mindfulness and nocturnal rumination are independently associated with symptoms of insomnia and depression during pregnancy. Sleep Health, 6(2), 185–191. https://doi.org/10.1016/j.sleh.2019.11.011
Kerstis, B., Aarts, C., Tillman, C., Persson, H., Engström, G., Edlund, B., Öhrvik, J., Sylvén, S., & Skalkidou, A. (2015). Association between parental depressive symptoms and impaired bonding with the infant. Archives of Women’s Mental Health, 19(1), 87–94. https://doi.org/10.1007/s00737-015-0522-3
Khan, F., & Laurent, H. (2019). Assessing the impact of mindfulness and life stress on maternal well-being. Mindfulness, 10(1), 26–35. https://doi.org/10.1007/s12671-018-0943-y
Leach, L. S., Poyser, C., & Fairweather-Schmidt, K. (2017). Maternal perinatal anxiety: A review of prevalence and correlates. Clinical Psychologist, 21(1), 4–19. https://doi.org/10.1111/cp.12058
Lovibond, P. F., & Lovibond, S. H. (1995). The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behaviour Research and Therapy, 33(3), 335–343. https://doi.org/10.1016/0005-7967(94)00075-U
Marshall, J. M., Dunstan, D. A., & Bartik, W. (2020). Effectiveness of using mental health mobile apps as digital antidepressants for reducing anxiety and depression: Protocol for a multiple baseline across-individuals design. JMIR Research Protocols, 9(7), e17159. https://doi.org/10.2196/17159
Milgrom, J., Gemmill, A. W., Bilszta, J. L., Hayes, B., Barnett, B., Brooks, J., Ericksen, J., Ellwood, D., & Buist, A. (2007). Antenatal risk factors for postnatal depression: A large prospective study. Journal of Affective Disorders, 108(1), 147–157. https://doi.org/10.1016/j.jad.2007.10.014
Miller, R. L., Pallant, J. F., & Negri, L. M. (2006). Anxiety and stress in the postpartum: Is there more to postnatal distress than depression? BMC Psychiatry, 6(1), 12–12. https://doi.org/10.1186/1471-244x-6-12
Smiling Mind. (2021). Smiling Mind. (Version 4.0.1) [Mobile app]. https://play.google.com/store/apps/details?id=com.smilingmind.app
O’Connor, T. G., Heron, J., Glover, V., T Alspac Study. (2002). Antenatal anxiety predicts child behavioral/emotional problems independently of postnatal depression. The American Academy of Child and Adolescent Psychiatry, 41(12), 1470–1477. https://doi.org/10.1097/00004583-200212000-00019
O’Hara, M. W., & Swain, A. M. (2009). Rates and risk of postpartum depression—A meta-analysis. International Review of Psychiatry, 8(1), 37–54. https://doi.org/10.3109/09540269609037816
O’Mahen, H. A., & Flynn, H. A. (2008). Preferences and perceived barriers to treatment for depression during the perinatal period. Journal of Women’s Health, 17(8), 1301–1309. https://doi.org/10.1089/jwh.2007.0631
Osman, A., Wong, J. L., Bagge, C. L., Freedenthal, S., Gutierrez, P. M., & Lozano, G. (2012). The depression anxiety stress Scales—21 (DASS-21): Further examination of dimensions, scale reliability, and correlates. Journal of Clinical Psychology, 68(12), 1322–1338. https://doi.org/10.1002/jclp.21908
Pan, W.-L., Chang, C.-W., Chen, S.-M., & Gau, M.-L. (2019). Assessing the effectiveness of mindfulness-based programs on mental health during pregnancy and early motherhood - A randomized control trial. BMC Pregnancy and Childbirth, 19(1), 346–346. https://doi.org/10.1186/s12884-019-2503-4
Philips Electronics UK. (2021). Baby + Tracker (Version 2.6.2) [Mobile app]. https://play.google.com/store/apps/details?id=com.hp.babyapp&_branch_match_id=79403 7338836798686
Podsakoff, P. M., MacKenzie, S. B., & Podsakoff, N. P. (2012). Sources of method bias in social science research and recommendations on how to control it. Annual Review of Psychology, 63, 539–569. https://doi.org/10.1146/annurev-psych-120710-100452
Potharst, E. S., Aktar, E., Rexwinkel, M., Rigterink, M., & Bögels, S. M. (2017). Mindful with your baby: Feasibility, acceptability, and effects of a mindful parenting group training for mothers and their babies in a mental health context. Mindfulness, 8(5), 1236–1250. https://doi.org/10.1007/s12671-017-0699-9
Potharst, E. S., Veringa-Skiba, I., van Broekhuizen, E., & Bögels, S. M. (2022). Mindful with your baby for mothers of infants with (parental) stress in a non-clinical setting: A wait-list controlled pilot trial. BMC Pregnancy and Childbirth, 22(1), 1–11. https://doi.org/10.1186/s12884-022-04640-z
Quinones, C., & Griffiths, M. D. (2019). Reducing compulsive internet use and anxiety symptoms via two brief interventions: A comparison between mindfulness and gradual muscle relaxation. Journal of Behavioral Addictictions, 8(3), 530–536. https://doi.org/10.1556/2006.8.2019.45
Rees, S., Channon, S., & Waters, C. S. (2019). The impact of maternal prenatal and postnatal anxiety on children’s emotional problems: A systematic review. European Child & Adolescent Psychiatry, 28(2), 257–280. https://doi.org/10.1007/s00787-018-1173-5
Rigabert, A., Motrico, E., Moreno-Peral, P., Resurrección, D. M., Conejo-Cerón, S., Cuijpers, P., Martín-Gómez, C., López-Del-Hoyo, Y., & Bellón, J. Á. (2020). Effectiveness of online psychological and psychoeducational interventions to prevent depression: Systematic review and meta-analysis of randomized controlled trials. Clinical Psychology Review, 82, 1–14. https://doi.org/10.1016/j.cpr.2020.101931
Sander, L., Rausch, L., & Baumeister, H. (2016). Effectiveness of internet-based interventions for the prevention of mental disorders: A systematic review and meta-analysis. JMIR Mental Health, 3(3), e38–e38. https://doi.org/10.2196/mental.6061
Shastri, V. V., Hankey, A., Sharma, B., & Patra, S. (2017). Investigation of yoga pranayama and Vedic Mathematics on mindfulness, aggression and emotion regulation. International Journal of Yoga, 10(3), 138–144. https://doi.org/10.4103/0973-6131.213470
Shulman, B., Dueck, R., Ryan, D., Breau, G., Sadowski, I., & Misri, S. (2018). Feasibility of a mindfulness-based cognitive therapy group intervention as an adjunctive treatment for postpartum depression and anxiety. Journal of Affective Disorders, 235, 61–67. https://doi.org/10.1016/j.jad.2017.12.065
Signal, T. L., Paine, S.-J., Sweeney, B., Muller, D., Priston, M., Lee, K., Gander, P., & Huthwaite, M. (2017). The prevalence of symptoms of depression and anxiety, and the level of life stress and worry in New Zealand Māori and non-Māori women in late pregnancy. Australian & New Zealand Journal of Psychiatry, 51(2), 168–176. https://doi.org/10.1177/0004867415622406
Sun, Y., Li, Y., Wang, J., Chen, Q., Bazzano, A. N., & Cao, F. (2021). Effectiveness of smartphone-based mindfulness training on maternal perinatal depression: Randomized controlled trial. Journal of Medical Internet Research, 23(1), e23410. https://doi.org/10.2196/23410
Takehara, K., Suto, M., & Kato, T. (2020). Parental psychological distress in the postnatal period in Japan: A population-based analysis of a national cross-sectional survey. Scientific Reports, 10(1), 13770–13770. https://doi.org/10.1038/s41598-020-70727-2
Taylor, L. B., Cavanagh, K., & Strauss, C. (2016). The effectiveness of mindfulness-based interventions in the perinatal period: A systematic review and meta-analysis. PLoS One, 11(5), e0155720. https://doi.org/10.1371/journal.pone.0155720
Terry, D. J., Mayocchi, L., & Hynes, G. J. (1996). Depressive symptomatology in new mothers: A stress and coping perspective. Journal of Abnormal Psychology, 105(2), 220. https://doi.org/10.1037//0021-843x.105.2.220
Tharwat, D., Trousselard, M., Balès, M., Sutter-Dallay, A.-L., Fromage, D., Spitz, E., Dallay, D., Harvey, T., Welter, E., Coatleven, F., Cherier, L., Teissèdre, F., Pouly, J.-L., Dutheil, F., & Duffaud, A. (2018). Chronic stress protection for postnatal depression prevention (SERENE): A protocol for an exploratory study. BMJ Open, 8(5). https://doi.org/10.1136/bmjopen-2017-018317
Townshend, K., & Caltabiano, N. (2019). Self-compassion and mindfulness: Modeling change processes associated with the reduction of perinatal depression. Journal of Child and Family Studies, 28(7), 1790–1802. https://doi.org/10.1007/s10826-019-01371-2
Townshend, K., Caltabiano, N. J., Powrie, R., & O’Grady, H. (2018). A preliminary study investigating the effectiveness of the caring for body and mind in pregnancy (CBMP) in reducing perinatal depression, anxiety and stress. Journal of Child and Family Studies, 27(5), 1556–1566. https://doi.org/10.1007/s10826-017-0978-z
Trevarthen, C., & Aitken, K. J. (2001). Infant intersubjectivity: Research, theory, and clinical applications. The Journal of Child Psychology and Psychiatry and Allied Disciplines, 42(1), 3–48. https://doi.org/10.1017/S0021963001006552
Weissman, M. M., Pilowsky, D. J., Wickramaratne, P. J., Talati, A., Wisniewski, S. R., Fava, M., Hughes, C. W., Garber, J., Malloy, E., & King, C. A. (2006). Remissions in maternal depression and child psychopathology: A STAR* D-child report. JAMA, 295(12), 1389–1398. https://doi.org/10.1001/jama.295.12.1389
Williams, J. M. G., & Kabat-Zinn, J. (2011). Mindfulness: Diverse perspectives on its meaning, origins, and multiple applications at the intersection of science and dharma. Contemporary Buddhism, 12(1), 1–18. https://doi.org/10.1080/14639947.2011.564811
Wong, O., Nguyen, T., Thomas, N., Thomson-Salo, F., Handrinos, D., & Judd, F. (2016). Perinatal mental health: Fathers-The (mostly) forgotten parent. Asia-Pacific Psychiatry, 8(4), 247–255. https://doi.org/10.1111/appy.12204
Woody, C. A., Ferrari, A. J., Siskind, D. J., Whiteford, H. A., & Harris, M. G. (2017). A systematic review and meta-regression of the prevalence and incidence of perinatal depression. Journal of Affective Disorders, 219, 86–92. https://doi.org/10.1016/j.jad.2017.05.003
Yelland, J., Sutherland, G., & Brown, S. J. (2010). Postpartum anxiety, depression and social health: Findings from a population-based survey of Australian women. BMC Public Health, 10(1), 771–771. https://doi.org/10.1186/1471-2458-10-771
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Contributions
KB: designed and executed the study, conducted data analyses, and wrote the paper. CB: collaborated with the design, writing of the paper, and editing of the final manuscript. OM: collaborated in the writing and editing of the final manuscript. All authors approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Ethics Approval
This research project has been approved by the Health Research and Ethics Committee of the Faculty of Arts and Social Sciences, University of Waikato. Ethics approval ID: HREC(Health)2019#69.
Consent to Participate
All participants provided informed consent to participate in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bear, K.A., Barber, C.C. & Medvedev, O.N. The Impact of a Mindfulness App on Postnatal Distress. Mindfulness 13, 2765–2776 (2022). https://doi.org/10.1007/s12671-022-01992-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-022-01992-7