Abstract
Background
Cenobamate is a novel tetrazole-derived carbamate compound with a dual mechanism of action. This drug can enhance the inactivated state of voltage-gated sodium channels, preferentially inhibiting the persistent component of the sodium channel current, and acts as a positive allosteric modulator of GABAA receptors, binding at a non-benzodiazepine site.
Objective
We assessed the efficacy and safety of adjunctive cenobamate for the treatment of focal-onset seizures in adult patients with epilepsy using meta-analytical techniques.
Methods
We systematically searched (May, week 4, 2020) MEDLINE (accessed by PubMed), the Cochrane Central Register of Controlled Trials (CENTRAL), and the US National Institutes of Health Clinical Trials Registry (http://www.clinicaltrials.gov). There were no date limitations or language restrictions. Randomized, placebo-controlled, single or double-blinded, add-on trials of cenobamate in adult patients with uncontrolled focal-onset seizures were identified. Main outcomes included the proportion of patients with ≥ 50 and 100% reduction in seizure frequency during the maintenance treatment period compared with baseline and the incidence of treatment withdrawal and adverse events (AEs). Risk ratio (RR) with 95% confidence interval (CI) was estimated for each outcome.
Results
Two trials were included, overall enrolling 659 patients (442 for the add-on cenobamate group and 217 for the add-on placebo group). Seizure frequency reduction by at least 50% occurred during the maintenance phase in 50.1% of the patients randomized to cenobamate and 23.5% of the placebo-treated participants (RR 2.18, 95% CI 1.67–2.85; p < 0.001). The pooled estimated RR to achieve seizure freedom for the cenobamate group in comparison with placebo was 3.71 (95% CI 1.93–7.14; p < 0.001). Withdrawal from randomized treatment occurred in 16.7 and 11.1% of participants receiving cenobamate and placebo, respectively (RR 1.34, 95% CI 0.85–2.09; p = 0.205). Treatment was discontinued due to AEs in 12.2 and 4.1% of the patients in the active and control arms (RR 2.27, 95% CI 1.08–4.79; p = 0.031). AEs were reported in 76.9 and 66.8% of the patients during treatment with cenobamate and placebo (RR 1.14, 95% CI 1.02–1.26; p = 0.021). The cenobamate-associated AEs included somnolence, dizziness, fatigue, balance disorder, and diplopia.
Conclusions
Adjunctive cenobamate in adult patients with uncontrolled focal-onset seizures is associated with a greater reduction in seizure frequency and a higher rate of AEs than placebo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Cenobamate is a novel tetrazole-derived carbamate compound. |
Cenobamate acts as a modulator of voltage-gated sodium channels and GABA currents. |
Adjunctive cenobamate reduces the frequency of focal seizures in patients with uncontrolled epilepsy. |
The most common adverse events include somnolence, dizziness, fatigue, balance disorder, and diplopia. |
1 Introduction
With an estimated incidence of about 80 cases per 100,000 people and a prevalence of 5–10 cases per 1000 people, epilepsy affects approximately 70 million people worldwide [1, 2]. The management of epilepsy is mainly symptomatic. Although the majority of patients with epilepsy reaches sustained seizure control, seizures remain uncontrolled in more than one third of the cases [3,4,5,6]. Uncontrolled epilepsy is often disabling, with patients experiencing significant psychological and social dysfunction, reduced educational and employment prospects, impaired quality of life, and risk of premature death [7, 8]. Despite the increased availability of antiseizure medications (ASMs) over the past 25 years, the burden of treatment-resistant epilepsy has remained fairly stable and there is still the need for novel, more effective therapeutic options [9].
Cenobamate is a new ASM that has been recently approved by the US Food and Drug Administration for the treatment, and is currently being reviewed by the European Medicines Agency for the adjunctive treatment, of focal-onset seizures in adults [10]. Cenobamate is a novel tetrazole-derived carbamate compound with one chiral center and is structurally different from carisbamate. Dual, complementary mechanisms of action may contribute to its antiseizure activity [11]. Cenobamate has been shown to reduce neuronal excitability by enhancing the fast and slow inactivation of sodium channels and preferentially inhibiting the persistent component of the sodium channel current [12]. Moreover, cenobamate acts as a positive allosteric modulator of high affinity GABAA receptors, binding at a non-benzodiazepine site [13].
This systematic review and meta-analysis aimed to assess the efficacy and safety of adjunctive cenobamate for the treatment of focal seizures in patients with epilepsy.
2 Materials and Methods
2.1 Search Strategy
The results of this systematic review and meta-analysis were reported according to the recommendations of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [14]. We systematically searched (May, week 4, 2020) MEDLINE (accessed by PubMed), the Cochrane Central Register of Controlled Trials (CENTRAL), and the US National Institutes of Health Clinical Trials Registry (http://www.clinicaltrials.gov) (search strategies are outlined in the electronic supplementary material [ESM]). Additional data were sought in the Drug Approval Package of cenobamate by the US Food and Drug Administration [15]. There were no date limitations or language restrictions. The reference lists of retrieved studies were reviewed to identify additional reports of relevant trials. The protocol was not registered previously.
2.2 Eligibility Criteria
Studies were selected when they met the following entry criteria: randomized, single- (masking of participants) or double-blinded (masking of investigator and participants), placebo-controlled, parallel-group, add-on studies with active and control arms receiving oral cenobamate and matched placebo, respectively, in addition to the existing ASM regimen. Participants had to meet the following criteria: any sex, any ethnicity, adult age (≥ 18 years), diagnosis of focal epilepsy, and seizures uncontrolled by one or more concomitant ASMs at stable doses at the time of randomization as defined within the original studies.
2.3 Outcome Measures
The efficacy outcomes were the proportions of patients with ≥ 50, ≥ 75, ≥ 90, and 100% reduction in monthly seizure frequency during the maintenance treatment period compared with the pre-randomization baseline. The safety and tolerability outcomes included the proportions of participants who withdrew from treatment for any reason and for adverse events (AEs) and who experienced any AE, any treatment-related AE, and any serious AE (SAE). AEs reported in at least 5% of patients in either treatment arm were also assessed. The effects on laboratory tests, ECG, vital signs, and physical and neurologic examinations were narratively reviewed.
2.4 Study Selection, Data Extraction and Assessment of the Risk of Bias
Two review authors independently assessed trials for inclusion and extracted the following information from included studies: main study author and age of publication, methodology and trial design (methods of randomization, allocation concealment and blinding, duration of baseline and treatment periods, dose/s of cenobamate tested), number and demographics of participants (age, sex, ethnicity, concomitant ASMs, seizure frequency during the baseline period), and number of patients experiencing any outcome per randomized group. Any disagreement was resolved by discussion with a third review author. The risk of bias of the identified studies was assessed following the recommendations of the Cochrane Collaboration [16].
2.5 Statistical Analysis
Heterogeneity among the trials was assessed through the Chi squared test and the I2 statistics for heterogeneity [17, 18]. Provided no substantial heterogeneity was present (p > 0.10), results were synthesized using a fixed-effects model; if the probability value was ≤ 0.10, a fixed- or random-effects model was chosen for I2 < 40% or ≥ 40%, respectively [19,20,21,22,23,24,25]. We presented heterogeneity statistics for all analyses unless only one trial contributed data and heterogeneity was not applicable. The modified intention-to-treat (ITT) maintenance phase population data (all randomized patients who had taken at least one dose of study drug and had any maintenance phase seizure data) were used for the efficacy analyses. The risk ratios (RRs) with 95% confidence intervals (CIs) were used as the measures of associations between treatment and outcomes with significance set at p < 0.05, unless otherwise specified. Results were presented according to cenobamate daily dosages, where sufficient data were available. Data analysis was performed using STATA/IC 13.1 (StataCorp LP, College Station, TX, USA).
3 Results
3.1 Results of the Search and Characteristics of Included Studies
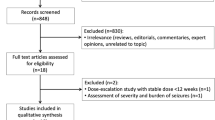
Thirty-seven records were identified by database and trial register searching, and two trials were included in the review and meta-analysis [26, 27] (Fig. 1). The studies assessed both the efficacy and safety of cenobamate, which was added once daily to the pre-existing antiseizure regimen at the dosage of 200 mg [26] or 100, 200, and 400 mg [27]. Details of the studies are provided in Table 1. The studies included 659 patients, of which 442 were randomized to add-on cenobamate and 217 to add-on placebo. Characteristics of the participants are summarized in Table 2.
All trials used adequate methods of sequence generation and allocation concealment. We judged all included trials at low risk of performance and detection bias since blinding was ensured by matching placebo, and patients, investigators, and study personnel were all masked to the treatment assignment. The risks of attrition and selective reporting bias were rated low as patients lost to follow-up and withdrawals were documented, and there was no suspicion of selective outcome reporting. All trials were sponsored by the cenobamate manufacturer.
3.2 Proportions of Patients with ≥ 50, ≥ 75, ≥ 90 and 100% Reduction in Baseline Seizure Frequency
The seizure frequency reduction by at least 50% during the treatment maintenance phase occurred across the trials in 50.1% of the patients randomized to add-on cenobamate and 23.5% of the placebo-treated participants (RR 2.18, 95% CI 1.67–2.85; p < 0.001) (Chi squared = 0.14, df = 1, p = 0.706; I2 = 0.0%]. The overall pooled estimated RRs to achieve 75% or more, 90% or more, and 100% reduction in seizure frequency for the add-on cenobamate group in comparison with add-on placebo were 2.25 (95% CI 1.57–3.24; p < 0.001) (Chi squared = 1.77, df = 1, p = 0.184; I2 = 43.4%), 4.34 (95% CI 2.42–7.78; p < 0.001) (Chi squared = 0.47, df = 1, p = 0.495; I2 = 0.0%), and 3.71 (95% CI 1.93–7.14; p < 0.001) (Chi squared = 1.55, df = 1, p = 0.214; I2 = 35.3%) (Figs. 2, 3, 4, 5).
Adjunctive cenobamate at either 100, 200, or 400 mg per day was associated with a significantly greater decrease in baseline seizure frequency of 50% or more in comparison with the inactive treatment (Fig. 2). When given at the daily dosage of 200 and 400 mg, add-on cenobamate was more effective than placebo in reducing seizure frequency by 75% or more (Fig. 3) and 90% or more (Fig. 4) and achieving seizure freedom (Fig. 5).
3.3 Treatment Withdrawal
Across the trials, withdrawal from randomized treatment for any reason occurred in 16.7 and 11.1% of the participants receiving cenobamate and placebo, respectively (RR 1.34, 95% CI 0.85–2.09; p = 0.205) (Chi squared = 0.44, df = 1, p = 0.506; I2 = 0.0%). The RRs to discontinue treatment were 0.93 (95% CI 0.46–1.88; p = 0.837), 1.26 (95% CI 0.77–2.08; p = 0.357) (Chi squared = 0.28, df = 1, p = 0.595; I2 = 0.0%), and 2.09 (95% CI 1.17–3.71; p = 0.012) for cenobamate at the daily doses of 100, 200, and 400 mg, compared with placebo.
Treatment was discontinued due to AEs in 12.2 and 4.1% of patients in the active and control arms (RR 2.27, 95% CI 1.08–4.79; p = 0.031) (Chi squared = 2.17, df = 1, p = 0.140; I2 = 54.0%). The corresponding RRs for cenobamate at the doses of 100, 200, and 400 mg/day were 2.40 (95% CI 0.88–6.58; p = 0.089), 2.02 (95% CI 0.91–4.46; p = 0.083) (Chi squared = 1.71, df = 1, p = 0.191; I2 = 41.4%), and 4.48 (95% CI 1.77–11.35; p = 0.002) (Table 3).
3.4 Adverse Events
AEs were reported in 76.9 and 66.8% of the patients during add-on cenobamate and placebo treatment, respectively (RR 1.14, 95% CI 1.02–1.26; p = 0.021) (Chi squared = 0.65, df = 1, p = 0.420; I2 = 0.0%). Adjunctive CBD was associated with a higher incidence of treatment-related AEs (66.3% vs 44.2%) compared with placebo (Table 4). The AEs significantly associated with add-on cenobamate were somnolence, dizziness, fatigue, balance disorder, and diplopia (Tables 4, 5).
Hypersensitivity reactions were reported in four patients treated with cenobamate. Three cases occurred at day 1, 10, and 57 of treatment and were of a moderate entity, mainly characterized by dermatologic manifestations (reddening of palms and soles and itching of ears; pruritic rash and pyrexia; rash and facial swelling); one patient developed a serious case of drug reaction with eosinophilia and systemic symptoms (DRESS) on day 24 of treatment. Treatment was discontinued in all cases, and patients recovered. No deaths occurred during the double-blind treatment phases.
There were no clinically meaningful changes from baseline in hematology, vital signs, physical and neurological examination. There was a signal for a dose-related shortening of the QT interval associated with cenobamate treatment, with a negative change in group mean QTcB values and an excess of QTcB decline > 30 ms. There was an association of elevation of serum potassium values > 5 meq/L (upper reference range) with cenobamate treatment—out-of-range high values were in excess of placebo in a dose-related distribution and the maximum value observed was 5.9 meq/L. There were no excursions above the critical value of 6.0 meq/L.
4 Discussion
4.1 Summary of Main Results
Randomized controlled trials provided substantial evidence of the efficacy of adjunctive cenobamate to treat focal-onset seizures in adult patients with uncontrolled epilepsy, and the greatest effect was observed at the dosage of 400 mg/day. Post-hoc analyses conducted as part of the original trials also provided evidence of a significant efficacy of cenobamate across all assessed focal seizures, including focal aware with a motor component, focal with impaired awareness, and focal to bilateral tonic–clonic seizures, with the highest reduction occurring in the latest [26, 27]. The control of this seizure subtype is noteworthy, as persistent generalized tonic–clonic seizures increase the risk for sudden unexpected death in epilepsy [28].
A remarkable finding is the high percentage of patients who achieved seizure freedom during the maintenance treatment phase. The seizure-free rate of 20% or higher observed with cenobamate compares very favorably with the rates of individual and pooled pivotal clinical studies of adjunctive ASMs in patients with uncontrolled focal seizures, which ranged from 0 to 6.5% [29, 30]. Few patients achieved 100% seizure reduction, particularly in the placebo groups. Accordingly, even though the results are statistically significant and very encouraging, some of the estimates have a very wide confidence interval, which does introduce uncertainty regarding the magnitude of the treatment effect over placebo. Although no accurate comparisons can be made between studies carried out with different protocols at different times and locations, cenobamate appears as one of the most efficacious available drugs. Seizure freedom is a major target of epilepsy treatment and one of the main issues accountable for an independent lifestyle and favorable quality of life [8]. Real-life data overcoming the constraints of the randomized controlled trial (RCT) design will help to address how long patients maintain seizure control with cenobamate and whether freedom rates will be borne out in clinical practice. Mechanisms of action and potential additive or synergistic interactions of cenobamate with concomitant ASMs also warrant further investigation.
The overall rates of patients withdrawing cenobamate for any reason and AEs were consistent with those reported with other available add-on ASMs [29], and a meaningful difference with placebo emerged when cenobamate was administered at the highest daily dosage. Cenobamate was generally well tolerated, with the majority of AEs rated as mild or moderate in severity. The most common AEs associated with cenobamate included typical central nervous system-related symptoms, primarily somnolence, dizziness, and disturbances in gait and coordination, and their incidence increased with the dose and tended to abate as treatment was maintained. The rapid cenobamate titration of 100 mg/week from 200 to 400 mg and the impossibility as per study protocol to adjust the dose of concomitant treatments might have also contributed to the higher rates of AEs in the 400-mg group. Interestingly, a somewhat higher incidence of AEs has been observed among patients treated with cenobamate and concomitantly taking sodium channel blockers compared with those not taking them [26]. Definitive conclusions cannot be drawn as the number of patients was small and unbalanced between groups. Further research is needed to explore how the potentially unique combination of mechanisms of action of cenobamate may affect the tolerability profile according to various co-administered ASMs.
Four cases of readily identifiable hypersensitivity adverse reactions occurred during the RCTs, including one serious event of DRESS. Three of these events, including the case of DRESS, occurred early during treatment, at the start of the drug or during the titration schedule. During early clinical development, three confirmed cases of DRESS were also identified among the first 953 participants exposed to cenobamate, including one fatality [31]. Cutaneous, idiosyncratic AEs have been reported with ASMs. Reactions are generally mild in severity, but serious and potentially life-threatening events can occur [32]. Serious skin adverse reactions including DRESS, Stevens-Johnson syndrome (SJS), and toxic epidermal necrosis (TEN) are most frequently reported with phenytoin, carbamazepine, lamotrigine, and phenobarbital; however, other ASMs have been identified to carry a significantly elevated risk [32,33,34]. Notably, no cases of DRESS, SJS, or TEN were reported among the 1339 patients exposed to cenobamate in the ongoing phase III, open-label, safety trial (ClinicalTrials.gov identifier NCT02535091) at data cutoff, after a median treatment duration of 9 months [35]. These ad interim results suggest that the titration schedule of cenobamate is crucial for managing the risk of allergic drug reactions and reducing the initial dose to 12.5 mg/day and slowing the up-titration rate to biweekly increments can substantially lower the likelihood of serious rash and DRESS. The “start-low and go-slow” strategy has been already shown to reduce the risk of immune-mediated hypersensitivity reactions with other drugs, possibly by the development of immune tolerance [32, 36]. Many more exposures are needed, however, to better assess the true safety profile of cenobamate, as a sample size of around 1350 patients can only rule out a 1/450 rate of DRESS [37]. The ongoing phase III study, open-label portions of the phase II RCTs [38, 39], as well as post-marketing surveillance will provide additional data to evaluate the incidence of rare AEs.
In both RCTs, cenobamate shortened the electrocardiogram QT interval in a dose-dependent manner. Similar findings were observed in a placebo-controlled QT study in healthy volunteers administered cenobamate [10]. This effect is likely due to the inhibition of the cardiac sodium channels and raises potential safety concerns in patients at risk for further QT-interval shortening. Accordingly, cenobamate is contraindicated in patients with familial short QT syndrome, and caution is required in co-administration with other drugs known to reduce QT interval since a synergistic effect can occur [40, 41]. Finally, a trend of hyperkalemia was identified with the administration of cenobamate. The events of raised potassium values tended to be sporadic, and there were no critical outlier values associated with adverse cardiac AEs in controlled study data [15]. The sporadic occurrence leads to uncertainty about the causal association, and clinical chemistry monitoring is not strictly required [15].
4.2 Pharmacological Interactions
Earlier pharmacokinetic studies indicated that cenobamate can significantly increase plasma exposures of phenytoin and phenobarbital via inhibition of CYP2C19 [42]. Remarkably, the interim report from the ongoing phase III safety study provided dosing guidance for the real-world management of patients taking cenobamate and concomitant phenytoin or phenobarbital, who instead were excluded from the RCTs. In this study, which allows dose adjustment of concomitant ASMs based on the patient’s clinical condition and plasma levels, around 45 and 30% of patients taking phenytoin and phenobarbital had their doses decreased [35]. At the end of the titration, the mean plasma levels of phenytoin and phenobarbital were generally comparable to those obtained before the start of cenobamate, suggesting that periodic dose reductions of 25–33% in response to AEs can be effective to maintain stable plasma levels [35]. In the same way, a reduction in dosage of clobazam should be considered, as clinically appropriate, to counteract the increase in plasma concentrations of desmethylclobazam, the active metabolite of clobazam, that occurs when cenobamate is concomitantly prescribed [10]. Cenobamate has been also shown to decrease the plasma exposure to carbamazepine by around 25% through the induction of CYP3A4 [42], and carbamazepine dose adjustment may be necessary when these drugs are used in combination. Similarly, an increase in the dosage of lamotrigine may be required when cenobamate is added to the therapeutic drug regimen [10].
4.3 Strengths and Limitations
This systematic review with meta-analysis is a comprehensive synthesis of the efficacy and safety of adjunctive cenobamate in adult patients with focal-onset seizures. Efficacy and safety analyses were also performed according to cenobamate daily dosages and the estimates of seizure responses during the maintenance phase could reflect steady-state drug levels at the target dose more accurately than data referring to the entire treatment period, including the titration phase. Nonetheless, different shortcomings need to be acknowledged. Only two trials met the eligibility criteria, a single pharmaceutical company funded both of them, and the efficacy of cenobamate at the highest dose was explored in one single study. The meta-analysis inherited the general limitations and assumptions of the RCTs of adjunctive ASMs, including the short duration of the maintenance phase, the highly selected inclusion and exclusion criteria for enrollment, and the potential effect of concomitant medications whose dosage must be kept unchanged throughout the double-blind period. Although cenobamate demonstrated a broad spectrum of activity and was efficacious in several animal models of epilepsy, including the maximal electroshock seizure test, seizures produced by picrotoxin and pentylenetetrazol, the hippocampal kindled rat model, and the mouse 6-Hz psychomotor seizure model [30], this review focused only on the use of cenobamate in focal epilepsy. In this regard, ongoing phase III trials are recruiting patients with primary generalized tonic–clonic seizures (NCT03678753, NCT03961568). Likewise, this meta-analysis cannot provide information about the efficacy and tolerability of cenobamate as monotherapy, the safety of cenobamate during pregnancy and lactation, or the quality of life or health economic outcomes.
5 Conclusions
Adjunctive cenobamate appears an effective treatment option for focal-onset seizures. Despite the development of many ASMs in the past decades, little has changed in the rate of patients who can achieve seizure freedom. In this context, trial data suggest that cenobamate stands out against the compounds approved in the last 25 years and brings promise for patients who have difficult-to-control seizures, mainly if the higher dosages can be tolerated [30, 37]. As cenobamate seizure-freedom rates appear substantially higher than those of other ASMs, it will be important to make sure that patients tolerate the introduction of this drug into the existing therapeutic regimen. Special caution and slower titration or stepwise tapering off should be considered in patients on other sodium channel blockers to increase tolerability and reduce the risk of treatment failure due to AEs. Real-world evidence will complement and further clarify the true therapeutic potentialities and clinical relevance of this newest anti-seizure drug.
References
Hirtz D, Thurman DJ, Gwinn-Hardy K, Mohamed M, Chaudhuri AR, Zalutsky R. How common are the “common” neurologic disorders? Neurology. 2007;68:326–37.
Cagnetti C, Lattanzi S, Foschi N, Provinciali L, Silvestrini M. Seizure course during pregnancy in catamenial epilepsy. Neurology. 2014;83:339–44.
Cockerell OC, Johnson AL, Sander JW, Hart YM, Shorvon SD. Remission of epilepsy: results from the national general practice study of epilepsy. Lancet. 1995;346:140–4.
Lattanzi S, Zaccara G, Giovannelli F, Grillo E, Nardone R, Silvestrini M, Trinka E, Brigo F. Antiepileptic monotherapy in newly diagnosed focal epilepsy. A network meta-analysis. Acta Neurol Scand. 2019;139:33–41.
Kwan P, Brodie MJ. Early identification of refractory epilepsy. N Engl J Med. 2000;342:314–9.
Lattanzi S, Cagnetti C, Foschi N, Provinciali L, Silvestrini M. Lacosamide monotherapy for partial onset seizures. Seizure. 2015;27:71–4.
Laxer KD, Trinka E, Hirsch LJ, Cendes F, Langfitt J, Delanty N, Resnick T, Benbadis SR. The consequences of refractory epilepsy and its treatment. Epilepsy Behav. 2014;37:59–70.
Josephson CB, Patten SB, Bulloch A, Williams JVA, Lavorato D, Fiest KM, Secco M, Jette N. The impact of seizures on epilepsy outcomes: a national, community-based survey. Epilepsia. 2017;58:764–71.
Chen Z, Brodie MJ, Liew D, Kwan P. Treatment outcomes in patients with newly diagnosed epilepsy treated with established and new antiepileptic drugs: a 30-year longitudinal cohort study. JAMA Neurol. 2018;75:279–86.
FDA. Cenobamate. Full prescribing information. https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/212839s000lbl.pdf. Accessed May 2020.
Bialer M, Johannessen SI, Levy RH, Perucca E, Tomson T, White HS. Progress report on new antiepileptic drugs: a summary of the Eleventh Eilat Conference (EILAT XI). Epilepsy Res. 2013;103:2–30.
Nakamura M, Cho JH, Shin H, Jang IS. Neuropharmacology and analgesia effects of cenobamate (YKP3089), a newly developed anti-epileptic drug, on voltage-gated sodium channels in rat hippocampal CA3 neurons. Eur J Pharmacol. 2019;855:175–82.
Sharma R, Nakamura M, Neupane C, Jeon BH, Shin H, Melnick SM, Glenn KJ, Jang IS, Park JB. Positive allosteric modulation of GABA(A) receptors by a novel antiepileptic drug cenobamate. Eur J Pharmacol. 2020;879:173117.
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
FDA. Drug approval package: Xcopri (Cenobamate), NDA 212839, FDA Center for Drug Evaluation and Research. https://www.accessdata.fda.gov/drugsatfda_docs/nda/2019/212839Orig1s000TOC.cfm. Accessed May 2020.
Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. In: Higgins JPT, Green S, editors. The Cochrane Collaboration, 2011. http://handbook-5-1.cochrane.org/. Accessed May 2020.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
Lattanzi S, Brigo F, Trinka E, Zaccara G, Cagnetti C, Del Giovane C, Silvestrini M. Efficacy and safety of cannabidiol in epilepsy: a systematic review and meta-analysis. Drugs. 2018;78:1791–804.
Lattanzi S, Brigo F, Cagnetti C, Trinka E, Silvestrini M. Efficacy and safety of adjunctive cannabidiol in patients with Lennox–Gastaut syndrome: a systematic review and meta-analysis. CNS Drugs. 2018;32:905–16.
Lattanzi S, Brigo F, Trinka E, Zaccara G, Striano P, Del Giovane C, Silvestrini M. Adjunctive cannabidiol in patients with Dravet syndrome: a systematic review and meta-analysis of efficacy and safety. CNS Drugs. 2020;34:229–41.
Lattanzi S, Brigo F, Trinka E, Vernieri F, Corradetti T, Dobran M, Silvestrini M. Erenumab for preventive treatment of migraine: a systematic review and meta-analysis of efficacy and safety. Drugs. 2019;79:417–31.
Lattanzi S, Cagnetti C, Danni M, Provinciali L, Silvestrini M. Oral and intravenous steroids for multiple sclerosis relapse: a systematic review and meta-analysis. J Neurol. 2017;264:1697–704.
Lattanzi S, Brigo F, Cagnetti C, Di Napoli M, Silvestrini M. Patent foramen ovale and cryptogenic stroke or transient ischemic attack: to close or not to close? A systematic review and meta-analysis. Cerebrovasc Dis. 2018;45:193–203.
Lattanzi S, Grillo E, Brigo F, Silvestrini M. Efficacy and safety of perampanel in Parkinson’s disease. A systematic review with meta-analysis. J Neurol. 2018;265:733–40.
Chung SS, French JA, Kowalski J, Krauss GL, Lee SK, Maciejowski M, Rosenfeld WE, Sperling MR, Mizne S, Kamin M. Randomized phase 2 study of adjunctive cenobamate in patients with uncontrolled focal seizures. Neurology. 2020;94:e2311–22.
Krauss GL, Klein P, Brandt C, Lee SK, Milanov I, Milovanovic M, Steinhoff BJ, Kamin M. Safety and efficacy of adjunctive cenobamate (YKP3089) in patients with uncontrolled focal seizures: a multicentre, double-blind, randomised, placebo-controlled, dose-response trial. Lancet Neurol. 2020;19:38–48.
Hesdorffer DC, Tomson T, Benn E, Sander JW, Nilsson L, Langan Y, Walczak TS, Beghi E, Brodie MJ, Hauser A, ILAE Commission on Epidemiology, Subcommission on Mortality. Combined analysis of risk factors for SUDEP. Epilepsia. 2011;52:1150–9.
Costa J, Fareleira F, Ascenção R, Borges M, Sampaio C, Vaz-Carneiro A. Clinical comparability of the new antiepileptic drugs in refractory partial epilepsy: a systematic review and meta-analysis. Epilepsia. 2011;52:1280–91.
Vossler DG. Remarkably high efficacy of cenobamate in adults with focal-onset seizures: a double-blind, randomized, placebo-controlled trial. Epilepsy Curr. 2020;20:85–7.
Sperling M, Klein P, Kamin M. Safety of cenobamate (YKP3089) as adjunctive treatment for uncontrolled partial seizures in a large, multicenter, open-label study. In: The American Epilepsy Society annual meeting. New Orleans, LA, November 30–December 4, 2018. Abstract 1.303. https://www.aesnet.org/meetings_events/annual_meeting_abstracts/view/500991. Accessed May 2020.
Zaccara G, Franciotta D, Perucca E. Idiosyncratic adverse reactions to antiepileptic drugs. Epilepsia. 2007;48:1223–44.
Borrelli EP, Lee EY, Descoteaux AM, Kogut SJ, Caffrey AR. Stevens–Johnson syndrome and toxic epidermal necrolysis with antiepileptic drugs: an analysis of the US Food and Drug Administration Adverse Event Reporting System. Epilepsia. 2018;59:2318–24.
Tennis P, Stern RS. Risk of serious cutaneous disorders after initiation of use of phenytoin, carbamazepine, or sodium valproate: a record linkage study. Neurology. 1997;49:542–6.
Sperling MR, Klein P, Aboumatar S, Gelfand M, Halford JJ, Krauss GL, Rosenfeld WE, Vossler DG, Wechsler R, Borchert L, Kamin M. Cenobamate (YKP3089) as adjunctive treatment for uncontrolled focal seizures in a large, phase 3, multicenter, open-label safety study. Epilepsia. 2020;61:1099–108.
Hirsch LJ, Weintraub DB, Buchsbaum R, et al. Predictors of lamotrigine-associated rash. Epilepsia. 2006;47:318–22.
French JA. Cenobamate for focal seizures—a game changer? Nat Rev Neurol. 2020;16:133–4.
Chung SS, French J, Krauss GL, Lee SK, Maciejowski M, Rosenfeld WE, Sperling MR, Kamin M. Long-term safety of adjunctive cenobamate in patients with uncontrolled focal seizures: open-label extension of a randomized clinical study. In: The American Academy of Neurology annual meeting, Toronto, Canada, April 25–May 1, 2020. Abstract S25.006. https://index.mirasmart.com/AAN2020/SearchResults.php?Topic=&Author_Institution=&Author=&Title=Long-term+Safety+of+Adjunctive+Cenobamate+in+Patients+with+Uncontrolled+Focal+Seizures%3A+Open-label+Extension+of+a+Randomized+Clinical+Study+. Accessed July 2020.
Krauss G, Klein P, Aboumatar S, Kamin M. Long-term efficacy and safety of adjunctive cenobamate in patients with uncontrolled focal seizures: open-label extension of a randomized clinical study. The American Academy of Neurology annual meeting, Toronto, Canada, April 25–May 1, 2020. Abstract S59.009. https://index.mirasmart.com/AAN2020/SearchResults.php?text=&Topic=&Author_Institution=&Author=&Title=Long-term+Efficacy+and+Safety+of+Adjunctive+Cenobamate+in+Patients+With+Uncontrolled+Focal+Seizures%3A+Open-label+Extension+of+a+Randomized+Clinical+Study+. Accessed July 2020.
Zaccara G, Lattanzi S, Cincotta M, Russo E. Drug treatments in patients with cardiac diseases and epilepsy. Acta Neurol Scand. 2020;142:37–49.
Zaccara G, Lattanzi S. Comorbidity between epilepsy and cardiac arrhythmias: implication for treatment. Epilepsy Behav. 2019;97:304–12.
Vernillet L, Kamin M. Drug–drug interactions between cenobamate and other antiepileptic drugs: results from phase I studies with carbamazepine, phenobarbital, phenytoin, and divalproex sodium [abstract]. Clin Pharmacol Ther. 2018;103(Suppl S1):S91.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Open access funding provided by Università Politecnica delle Marche within the CRUI-CARE Agreement. No funding has been received for the conduct of this study.
Conflict of Interest
Simona Lattanzi has received speaker’s or consultancy fees from Eisai, UCB Pharma, and GW Pharmaceuticals and has served on an advisory board for GW Pharmaceuticals. Eugen Trinka received speaker’s honoraria from UCB Pharma, Biogen, Gerot-Lannach, Bial, Eisai, Takeda, Newbridge, Sunovion Pharmaceuticals Inc., LivaNova, and Novartis; consultancy funds from UCB Pharma, Biogen, Gerot-Lannach, Bial, Eisai, Takeda, Newbridge, GW Pharmaceuticals, Sunovion Pharmaceuticals Inc., and Novartis; and directorship funds from Neuroconsult GmbH. E. Trinka’s institution received grants from Biogen, Red Bull, Merck, UCB Pharma, European Union, FWF Österreichischer Fond zur Wissenschaftsförderung, and Bundesministerium für Wissenschaft und Forschung. Gaetano Zaccara received speaker’s or consultancy fees from Eisai, Sanofi-Aventis, and UCB Pharma. Pasquale Striano received fees and research grants from GW Pharmaceuticals, Zogenyx, Biomarin, and Kolfarma s.r.l. Cinzia Del Giovane and Mauro Silvestrini have no conflicts of interest directly relevant to the content of this study. Francesco Brigo acted as a consultant for Eisai.
Consent for Publication
All authors approved the final manuscript for submission.
Author Contributions
SL drafted the concept, analyzed data, and wrote the manuscript. SL and GZ performed the literature search. ET, GZ, PS, CDG, MS, and FB critically revised the work. All authors contributed to the final manuscript.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Lattanzi, S., Trinka, E., Zaccara, G. et al. Adjunctive Cenobamate for Focal-Onset Seizures in Adults: A Systematic Review and Meta-Analysis. CNS Drugs 34, 1105–1120 (2020). https://doi.org/10.1007/s40263-020-00759-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40263-020-00759-9