Abstract
Patient acceptability of a medicinal product is a key aspect in the development and prescribing of medicines. Children and older adults differ in many aspects from the other age subsets of population and require particular considerations in medication acceptability. This review highlights the similarities and differences in these two age groups in relation to factors affecting acceptability of medicines. New and conventional formulations of medicines are considered regarding their appropriateness for use in children and older people. Aspects of a formulation that impact acceptability in these patient groups are discussed, including, for example, taste/smell/viscosity of a liquid and size/shape of a tablet. A better understanding of the acceptability of existing formulations highlights opportunities for the development of new and more acceptable medicines and facilitates safe and effective prescribing for the young and older populations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Appropriate pharmaceutical design of oral medicines can improve acceptability and patient outcomes in paediatric and geriatric populations. |
Similar considerations should be given to physical characteristics affecting swallowability of tablets and capsules for use in children and older patients. |
Whilst formulation factors such as taste and smell are important features for paediatric medicines, safe swallowing is the key formulation factor in designing medicines for older patients. |
1 Introduction
Acceptability has previously been defined as “an overall ability of the patient and caregiver (defined as ‘user’) to use a medicinal product as intended (or authorised)” [1]. This terminology is used as the basis for this review article. Additional consideration is required in developing medicines for young and older patients as their physiological and cognitive responses may differ due to the developing and deteriorating conditions of the body, respectively. Oral administration is the most common route of drug delivery to both young and older patients. However, there are obstacles for young and older patients to accept their oral medicines, e.g. swallowing difficulties or dysphagia, the involvement of caregivers, child recalcitrance and polypharmacy in the older population, to name just a few. While these barriers may not be considered major issues for adults, they could potentially affect adherence in young and older patients. In many cases, oral medicines are modified to ease administration in these patients, ranging from simple removal from packaging to dispensing in a dosette box, to more complex alterations including crushing or splitting of solid oral dosage forms [2–6]. Altering medication dosage forms, whether for children or adults, leads to unlicensed use of medicines and can potentially change bioavailability, toxicity and stability of the medicines.
Guidance issued by the European Medicines Agency (EMA) highlighted that acceptability must be an integral part of paediatric formulation development [7]. Recently, the EMA Geriatric Expert Group has issued a concept paper on the need for a reflection paper on the quality requirements of medicines for older adults [8]. The EMA Quality Working Party is currently looking into drafting the reflection paper. Similar principles might apply to assess the acceptability of medicines in children and older adults; however, a duplicate approach might not be appropriate due to the different patient-centred issues in these two populations. The aim of this review is to highlight the similarities and differences between children and older adults in relation to the acceptability of oral medicines. A detailed analysis of barriers associated with administration of oral medicines guides the choice and development of appropriate medicines to meet the needs of both patient groups (see the Electronic Supplementary Material for a description of the search strategy).
2 Patient-Centred Factors Affecting Acceptability of Oral Medicines
Table 1 summarises the most important patient-related factors that affect oral medication acceptability in children and older adults.
2.1 Patient Characteristics
There is no such thing as a standard paediatric or geriatric patient. As the physiological and cognitive systems continue to develop or be impaired, chronological age is not the best indicator to predict the characteristics of the patient. Frailty does not always accompany very old age nor do all infants mature at the same rate. The heterogeneity is higher in the older adult group as the definition and recognition of the physiological changes with advanced age is diverse.
2.2 Drug Therapy-Associated Factors
The duration of treatment and the required number of medicines potentially increase the complexity of acceptance to medicines in older adults. Many older adults are on multiple medications to treat their multi-morbidities [9]. The dose regimen further complicates adherence and acceptance of medicines [10]. In this respect, multi-compartment adherence aids are promising in terms of helping patients to remember to take their medicines at the right time [11].
2.3 Socio-Cultural Factors
In both populations the involvement of a caregiver is common; therefore, there is a need for the directions on usage of a medicine to be clear both to the patient and the caregiver. Older adults living in their own home may be the sole person responsible for their medicine management, whereas seniors living in nursing homes are often helped by formal carers or by nurses at hospitals. The majority of paediatric populations, except adolescents, are typically dependent on their parents/carers to take their medicines. As such, the ability and willingness of the carer to administer a medicine to these patients as intended could determine the acceptability of the medicine and outcome of the treatment [12–16].
The acceptability of medicines may be influenced by the setting in which the administration of the medicine takes place. Children with minor diseases may need to take medications during nursery/school hours. Chronically ill children may need to take their regular medicines or medicines for the treatment of acute problems at school. Peer pressure and child recalcitrance are potential factors affecting their acceptance of a medication form in these cases.
2.4 Dysphagia in Children and Older Adults
The ability to swallow determines the acceptability of conventional medication forms such as tablets and capsules. Swallowing is a rapid, albeit complex, process that involves two essential actions: bolus transport and airway protection. The process of deglutition is generally divided into three main phases: the oral phase, the pharyngeal phase and the oesophageal phase. Dysphagia is defined as difficulty in swallowing and can occur in both children and older adults [18]. While swallowing reflexes can be observed as early as in utero, significant maturation related to deglutition occurs between 6 months and 3 years of age, with complete maturation generally believed to have occurred by 6 years of age [19, 20].
The prevalence of paediatric dysphagia is difficult to ascertain given the wide variations in how swallowing impairments are defined and the assessment measures used to identify them. The causes of paediatric dysphagia can be medical, developmental, behavioural, psychological, or it may indeed be a multidimensional disorder. Common aetiologies include prematurity, developmental disorders, neurological disorders, reflux and craniofacial abnormalities [21, 22]. Although the exact incidence of dysphagia is unknown, it is reportedly becoming more common given the improved prognosis of pre-mature infants and of children with chronic medical conditions [23, 24]. Nevertheless, it has been reported that as many as 25–45 % of typically developing children and up to 80 % of children with developmental disabilities exhibit some form of feeding disorders [21].
In contrast to children, the natural process of aging is associated with a decline in swallowing function affecting all three phases of deglutition [25]. Poor dentition and reduction in masticatory strength in older age are the main causes of increases in oral-phase duration and the amount of oral residue during swallowing. Age-related neuromuscular decline contributes to a delay in triggering pharyngeal swallowing reflex and decreases in bolus movement and clearance in the oesophageal phase. It was estimated that 70–90 % of the older population experience some degree of dysphagia [26]. In one study, 87 % of residents in a care home (average age of 87 years) reported mealtime difficulties related to swallowing and 68 % showed signs of dysphagia [27]. The prevalence of dysphagia is particularly high in patients with age-related diseases such as Parkinson’s disease (80 %), Alzheimer’s disease (40–70 %) and acute stroke (50 %) [28–31].
3 Factors Affecting Acceptability of Tablets and Capsules
3.1 Acceptability of Tablets and Capsules in Children
The age at which most children acquire the skills to swallow tablets and capsules safely has been the subject of much debate. Early literature widely quotes 6 years as a general age from which these dosage forms may be considered suitable for children [32]. Recent evidence suggests that some children may have already acquired the ability to swallow tablets and capsules from an earlier age, or in some cases can be taught using behavioural training interventions. For example, Yeung and Wong [33] found that children with HIV as young as 3 years were prescribed stavudine as a solid dosage form. In a recent study in Uganda and Zimbabwe, 36 % of children were able to swallow antiretroviral tablets intact (mean age 3.3 years), while 64 % required them to be crushed or dispersed (mean age 2.9 years) [34]. Behavioural techniques to aid swallowing of both tablets and capsules involving children as young as 2–3 years old have also been described; however, such reports are limited to specific diseases and small sample sizes [35–41].
Although swallowing ability may be perceived to improve with age, some studies have reported swallowing difficulties in adolescence. In a general paediatric clinic in Denmark, nearly half (43 %) of parents surveyed reported children aged 12 years and younger experienced difficulties taking both liquids and tablets, primarily due to taste and swallowability; problems in administering tablets were more pronounced [42]. In a qualitative study, Hansen et al. [43] found that more than one-third of adolescents described difficulties in taking oral medications, particularly swallowing tablets, primarily due to taste and size. Polaha et al. [44] similarly reported that around one-third of children and adolescents had refused and rejected tablets at least once; interestingly, frequent medication users were more likely to refuse them despite reportedly having better tablet swallowing skills. Difficulties in swallowing have nonetheless been implicated as a barrier to adherence in children in various chronic conditions [38, 45–47].
The ability to swallow tablets and capsules is one of the factors that influence the age at which children convert from liquid to solid formulations. Following analysis of community prescription data in Netherlands, Schirm et al. [48] found that the use of tablets and capsules exceeded liquids from the age of 7 years for licensed products, 3 years for off-label medicines and 9 years for unlicensed, pharmacy-compounded medicines. Similarly, in the UK, the average age of conversion from liquid to solid antiretroviral formulations was 7.3 years [33]. It is worth noting that many factors can potentially affect this conversion age, e.g. the availability of tablets of the right size and strength for paediatric use and the acceptance of prescribing an unlicensed medicine when an authorised formulation is available. Comparison of the practice in different countries would be an interesting topic for future study.
The ability of children to swallow tablets and capsules is strongly related to the size of these dosage forms, alongside age. However, current guidance on the suitability of tablet sizes for different age groups in children is based upon anecdotal feedback and perception [7]. Direct evidence in this area is scarce and future research in this area is required. Table 2 summarises the published evidence on the ability of children to swallow tablets of different dimensions based upon age. Mini-tablets (1–4 mm in diameter) are relatively new dosage forms with considerable promise in paediatrics [17, 49]. Mini-tablets can be administered directly (swallowed whole) or could be labelled for sprinkling onto food. Various research studies have recently assessed the acceptability of mini-tablets in infants and children (Table 2). While these exploratory studies demonstrate their proof of concept, each involved administration of single mini-tablets, whereas multiple mini-tablets are more likely to be used clinically to provide the appropriate dose. Further research is required to demonstrate the application of mini-tablets in practice.
3.2 Acceptability of Tablets and Capsules in Older Patients
In older patients, age- or disease-related swallowing difficulties affect their ability to take solid oral medicines. In a survey involving 17 community pharmacies from England and Northern Ireland, 60 % of patients aged between 60 and 89 years experienced difficulties in swallowing tablets and capsules [56]. A recent study reported that 37.4 % of adult patients (mean age 62 years) attending their general practices had difficulties in swallowing medicines [57]. Polypharmacy (taking ≥5 medicines) is common in older patients [9]. A study conducted in Switzerland showed that community-dwelling polypharmacy patients (mean age 67 years) reported ongoing (9.0 %) or past (13.4 %) swallowing difficulties that resulted in intentional non-adherence in 23 % of these patients [58].
Anxiety, previous bad experiences and disliking the idea of taking medicines could all contribute to difficulties for older patients in taking tablets and capsules [57]. Effortful swallowing, a process of swallowing ‘hard’ using oral and pharyngeal muscles, is commonly advised by speech and language therapists to help dysphagia patients and could increase the oral swallowing pressure to propel the swallowed object more effectively [59]. It was shown that targeted training using swallow-related exercises significantly improved swallowing performance of patients with Parkinson’s disease [60]. Indeed, some patients with dysphagia found that concentrating on swallowing improved their ability to swallow solid dosage forms [61].
3.3 Factors Affecting Swallowability and Oesophageal Transit of Tablets and Capsules in Adults
During the swallow process, there is a risk for tablets and capsules to adhere to the oesophagus, causing prolonged or incomplete oesophageal transit. A trapped dosage form can start to disintegrate or dissolve within the oesophagus and cause oesophageal injury, often due to altered local pH or hyper-osmolarity [62]. The swallowability and oesophageal transit of tablets and capsules are affected by many physical characteristics of the dosage form. However, literature reports on swallowability of tablets and capsules were typically conducted in the adult population and data from children and older adults are scarce. Difficulties in swallowing and oesophageal retention of tablets and capsules are expected to be magnified in children and older adults; therefore, the findings of studies in adults provide useful guidance. Nevertheless, studies that are directly conducted in paediatric and geriatric populations would be valuable to guide the design of medicines for these patients.
Tablet size was found to affect the swallowability and oesophageal transit in adults; smaller tablets were considered easier to swallow and showed faster oesophageal transit than larger tablets (Table 3). Shape, density, surface characteristics and type of formulation can all affect the swallowability and oesophageal transit of tablets and capsules (Table 3). Visual aspects of medicines such as colour can be adapted not only to provide an aesthetic dosage form that is acceptable to patients, but to aid users in recognising and differentiating medicines. The colour of tablets is associated with flavour perceptions and there are many reviews on the topic [63]. Tablet colour has been linked with taste, where pink is considered to be sweeter than red, and yellow is considered to be salty irrespective of its actual ingredients [64]. The colour of a medication has also been connected with specific ailments and can affect patient adherence. A change in tablet colour was associated with non-adherence in adult patients with epilepsy [65]. There have been reviews on the effect of colour of tablets and perceptions of efficacy [66]. Colour preferences among children have shown to be stereotypically gender dependent [67], and they seem to prefer brightly coloured medicines. In older patients, white was seen as the most popular colour choice for tablets; however, those patients who take more than ten tablets every day prefer brighter colours than patients who take fewer tablets [68].
The ability of a patient to swallow tablets and capsules is also affected by patient-related factors. The retention of a tablet or capsule in the oesophagus is affected by the body position of the patient while taking the medicine and the volume of fluid taken with the medication (Table 3). It was recommended that medications should be taken with at least 100 mL of fluid and the patient remains standing for at least 90 s to prevent oesophageal retention [69]. Although useful guidance, some older patients may not be able to follow this advice, as they may be bedridden or may have difficulty in swallowing a large amount of fluid [70]. Similarly, this volume may be too large for children to take.
3.4 New ‘Easy-to-Swallow’ Technologies to Aid in Swallowability of Tablets and Capsules
Several technologies have been developed to aid the swallowing of solid oral dosage forms. A disposable device called MedCoat® (Med Coat AB, Stockholm, Sweden) can be used by the patient to apply a thin coat on the tablet before swallowing [71]. The coating contains gelatine, sweeteners and flavouring agents and can improve the taste of the tablet. In a clinical trial (average age 30 years), the coating improved the ease of swallowing of tablets, especially bitter-flavoured placebo tablets [71]. A similar flavoured spray product Pill Glide® (FLAVORx Inc., Columbia, MD, USA) requires the patient to apply the spray to the back of the mouth and tongue before taking tablets or capsules [72]. The spray creates a lubricated surface in the mouth and thus facilitates swallowing. Pill Glide® has been found to be helpful in adolescents with difficulties in swallowing tablets.
4 Factors Affecting Acceptability of Oral Liquid Dosage Forms
Oral liquids are generally regarded to be the most appropriate dosage form for children despite having issues including taste masking, portability, stability and the inclusion of excipients that are not always appropriate for all paediatric patients. The challenge in using liquid formulations in older patients, particularly those with dysphagia, is aspiration, which is caused by inadequate protection of the airway during swallowing. The prevalence of aspiration was reported as 51 % in dysphagia patients and 36 % of healthy older adults showed some degree of aspiration during normal swallowing [83, 84].
Patient acceptability of a liquid dosage form is inevitability affected by many of its characteristics (Table 4). Modifications in these formulation factors can improve swallowing of a liquid by moderating the timing and response of oral, pharyngeal and oesophageal phases.
4.1 Taste, Smell and Palatability of a Liquid
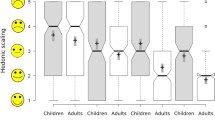
Taste is regarded as the most important factor determining the acceptability of a liquid medicine in children. There have been several studies undertaken that investigated the taste of liquid medicines in paediatric populations. These typically use face-rating scoring systems to evaluate the taste in this population and an example study was conducted by Cohen et al. [108]. Review articles have been published on this area and the reader is directed to the review by Ernest et al. for additional information [109].
Research has linked smell of a liquid to flavour and it has been argued that the majority of the flavour of food actually comes from its smell [110]. It is likely that certain medicines do smell unpleasant, yet there is very limited work done in this area, particularly in linking medication odour to compliance/adherence (Table 5).
The effect of taste on medication acceptability in older patients has not been extensively investigated compared to the paediatric population. However, the unpleasant taste of liquid medicines was identified as one of the barriers for older patients with dysphagia to taking their medications [61]. Swallowing is modulated by the nervous inputs generated from sensory receptors in the oral, pharyngeal and laryngeal regions via trigeminal, glossopharyngeal and vagus nerves [111]. Taste, thermal and chemical properties of the ingested fluid act as stimuli of these nerves and are known to affect swallowing activities (Table 4). However, the effect of taste was likely to decrease in older adults due to the reduced taste sensitivity in older individuals [112].
Beneficial effects of a sour bolus, consisting of 50 % lemon juice and water, on the oropharyngeal swallowing in patients with neurogenic dysphagia were reported by Logemann et al. [87] (Table 4). It was suggested that the sour taste acted as an “alerting” stimulus and enhanced or altered the sensory input to the nervous system and thus facilitated oropharyngeal swallowing in neurogenic dysphagia patients. The strong sour taste was deemed unpleasant by most participants and changing the liquid into a palatable sweet and sour taste did not significantly improve swallowing [91]. It is the challenge for future research to utilise the benefit of the sour taste and improve the palatability in the design of oral liquid medicines to promote safe swallowing in older dysphagic patients.
4.2 Texture and Viscosity of a Liquid
The texture and mouth feel of particles is acknowledged as important in food products as it affects mastication and overall taste sensation [113]. Grittiness of particles has previously been linked to particles >12 μm [113]. Texture effects on acceptability of liquid medicines have not been extensively investigated (Table 4) and it is an important subject for future research.
The consistency and rheology of the swallowed bolus affect the safety of swallowing [114, 115]. In particular, liquids and thin pastes initiate significantly different muscle activities during swallowing compared with thick pastes, which could be associated with a higher risk of aspiration in dysphagia patients [98]. Thin liquids pose a high risk of aspiration due to their lack of resistance to flow and they usually arrive at the hypopharynx before the onset of the pharyngeal swallow. Increasing the viscosity of the liquid slows the oropharyngeal transit of the bolus and thus prevents the premature emptying from the mouth before the pharyngeal swallow response [97–99].
4.3 Volume of a Liquid Administered
Small volumes are normally better tolerated for preparations with known palatability issues, unless a more diluted preparation may allow better taste masking. There are issues in very small volumes of oral liquids for administration in children; these are generally related to the accuracy of dosing relative to the devices available [116]. Minimal volumes are normally used when dosing very young children via enteral tubes to ensure that sufficient nutrition can be administered in addition to medication. The typical volume of medicine administered in a child is expected to be swallowable in one unit; therefore, the maximum volume should equate to the volume of a swallow. The volume of a swallow is reported to be 4.5 mL for children from 15 months to 3.5 years of age and this equates to a typical volume of 0.27 mL/kg [117].
The volume of the liquid to be swallowed can affect the safety of swallowing in older adults. A normal sip size for healthy adults has been reported to be in the range of 17–21 mL [117, 118]. However, the sip size is much smaller (9.8 mL ± 6.0) in patients with neurogenic oropharyngeal dysphagia [91]. Increasing the liquid bolus volume has been shown to increase the risk of aspiration (Table 4). Interestingly, too small a volume can also be a problem for dysphagia patients to swallow (Table 4) [102]. This is likely due to the reduced sensory awareness in these patients and because increased bolus volume increases the sensory input into the nervous system.
4.4 Administration Devices
The device used to administer an oral liquid is critical in ensuring that the dose administered is accurate. There are many alternatives available for the delivery of oral liquids including oral syringes, measuring spoons and measuring cups. In general, drinking from a spoon is considered safer for patients with dysphagia than cup and straw drinking (Table 4). The front edge of the bolus was reported to be frequently in the hypopharynx before the initiation of the swallowing during straw drinking and this distal bolus location was associated with greater occurrences of airway penetration in dysphagia patients [119].
4.5 Packaging and Storage
Preservatives are required in multidose oral preparations; however, preservatives are often associated with bitterness and this needs to be balanced with the overall palatability of the medicine. The safety and toxicity of the preservatives used need careful consideration, particularly for neonates. Packaging liquid medicines in a single-use sachet has benefits in terms of reducing the requirement for preservatives and also increasing the portability of a medicine. This packaging is used within the UK for paracetamol suspensions and Gaviscon® products. Anecdotal evidence suggest that carers prefer sachets of certain drugs due to the portability and also eliminating the need for an additional measuring device as the medicine can be transferred directly from the sachet to the patient’s mouth. Oral liquids may require refrigeration, which is a further hurdle for patients who may require frequent administration of a liquid.
4.6 Patient Posture
Postural changes of the head and body have been frequently used as compensatory treatments for oropharyngeal dysphagia, especially for eliminating aspiration of thin liquids. The most effective postural techniques include head rotation and chin-down posture—touching the chin to the front of the neck (Table 4) [105, 106, 120, 121]. The effectiveness of the chin-down posture in reducing the risk of aspiration is related to a significant narrowing of the laryngeal entrance and a posterior shift of the epiglottis, and thus providing a more effective protection of the airway entrance [122–124]. This technique was seen to be most helpful in the oldest patients (ages 80–95 years), probably relating to the changes in the natural neck posture with age [101]. Head rotation was shown to lateralise the bolus away from the direction of the head turn during swallowing [107, 125]. This technique is therefore useful for patients with unilateral neurologic or structural damage to the pharynx, by bypassing the damaged area and improving the efficiency of swallow. The effect of posture in the very young has not been examined with respect to medicines administration but may be of significant importance for babies and infants who often feed in a horizontal position.
5 Acceptability of Other Flexible Oral Solid Dosage Forms
Alternatives to liquid medicines are often sought where liquid medicines are not acceptable to patients; for example, where taste issues cannot be overcome, more sophisticated formulation approaches such as encapsulation of drug particles may be required. Many disadvantages associated with taking oral liquids can be avoided by the use of flexible oral solid medicines that are convenient to use by patients who cannot swallow tablets and capsules. Table 5 describes studies investigating the acceptability of these formulations in children and older adults and Table 6 summarises the advantages and challenges of using these formulations in these patient groups.
5.1 Multiparticulate Dosage Forms
Multiparticulates include powders, granules and pellets and are usually presented in sachets or capsules that can be reconstituted in a drink to provide solutions or suspensions, or applied onto food as ‘sprinkles’. They can also be further processed to produce other solid formulations including conventional, orally disintegrating or chewable tablets. Based on recent US FDA guidance, multiparticulates that are labelled for administration via sprinkling should have a target size of 2.5 mm, with no more than 10 % variation over this to a maximum size of 2.8 mm [160]. These formulations are typically considered as paediatric formulations; however, older patients can also benefit from their use, such as for the treatment of Parkinson’s disease, osteoporosis and phenylketonuria [132, 133, 161].
5.2 Dispersible, Soluble and Effervescent Tablets
Dispersible, soluble and effervescent tablets are solid dosage forms that can be dispersed or dissolved in a liquid to form a solution or suspension. These dosage forms require effective taste masking, as reviewed in Sect. 4.1 relating to oral liquid medicines. These dosage forms are beneficial in the delivery of large doses of active drug substances as they are easier to swallow than large tablets. The acceptability and safety of using dispersible and soluble tablets in older adults, especially those with dysphagia, have not been fully studied. However, effervescent formulations may be a useful technology to promote safe swallowing in older patients due to the production of carbon dioxide in water. Carbonated water has been found to be able to improve swallowing in dysphagia patients by exciting chemical stimulation in the oral cavity (Table 4) [88, 93, 153]. A national survey in the UK showed that 90 % of the prescribed and issued over-the-counter ‘easy to swallow’ solid formulations were effervescent tablets for long-term use in older people [162].
5.3 Orally Disintegrating Formulations
Orally disintegrating formulations include tablets, films and thin wafers. These formulations are relatively new innovations in improving patient compliance and acceptance, especially for paediatric and geriatric patients. These preparations may be applicable for use across the paediatric population, including infants and young children; however, evidence of their use and acceptability in these subsets is lacking. A number of orally disintegrating tablet and film formulations have been developed for the treatment of diseases that are common in the older population such as pain, depression, Parkinson’s disease and Alzheimer’s disease [163, 164].
5.4 Chewable Tablets
Chewable tablets are another dosage form useful for paediatric and geriatric patients who are unable to swallow conventionally sized monolithic dosage forms intact. In typically developing children, deciduous (primary) teeth begin to erupt from 6 months of age and the complete set of 20 have usually erupted between the ages of 2 and 3 years. Exfoliation of deciduous teeth begins from 6 to 7 years of age, with complete replacement by permanent teeth usually completed by the age of 12–13 years. Recent research suggests continual refinement of chewing skills occurs until at least the age of 3 years, at which time chewing patterns and efficiency also stabilise [165].
Despite the recent popularity of chewable tablets in children, their usage in older adults may be limited due to the deteriorations of chewing ability in this age group. The prevalence of chewing problems was observed to be 40 % among older Tanzanian citizens (aged 50–100 years) [166]. In Finland, chewing ability was considered poor in 55 % of long-term hospitalised older individuals and 65 % could eat mashed food only [167]. The loss of teeth is regarded as the primary factor accounting for the deterioration of the chewing ability and the possession of more than 20 teeth is essential for retaining good chewing capacity. However, a survey in Japan showed that 65 % of older people (aged 75–100 years) had less than 20 teeth [168]. In Denmark, half of the 75- and 85-year-old men and women in a suburban area were edentulous and only 15 % still had more than 20 teeth [169]. As a result, chewing problems were shown in three-quarters of those very old men and women who have lost all of their natural teeth.
5.5 Films and Jellys
A film formulation provides easy swallow through the application of a dry film that turns into a jelly instantaneously in the mouth by absorbing a small amount of saliva [170]. The film consists of an inner layer that contains the active drug and two gelling layers covering the drug layer (Fig. 1). The dissolution of the drug in the mouth was limited by the gel layer which swells by absorbing water (Fig. 2). The oesophageal transit of the film was significantly quicker than gelatin capsules [170]. The technology may be difficult to use in older people with xerostomia, which is a common symptom in the older population, particularly related to the increased use of medications [171]. A drug-containing oral jelly was developed to improve swallowing for older patients [172]. The formulation comprises a jelly portion and an air portion which can be pushed to extrude the jelly when opening the package.
Schematic structure of the easy-swallowing film formulation (reproduced from Okabe et al. [170], with permission)
The swelling behaviour of the film formulation in purified water (reproduced from Okabe et al. [170], with permission)
6 Acceptability of Dosage Forms Designed for Particular Therapeutic Effects
6.1 Modified-Release Formulations
Oral modified-release formulations enable longer and more patient-friendly dosing intervals. This can be beneficial in children to avoid the need to take medicines at school or nursery settings and to improve adherence in older patients. More simplified dose regimens with fewer daily doses have been associated with higher patient adherence [10]. It was found that patient adherence was significantly higher with once- and twice-daily regimens than three and four times daily regimens. Further evidence shows that adherence can be improved by switching from twice-daily to once-daily therapy [173]. Adherence to antiretroviral therapy was significantly improved when patients were switched from twice-daily to once-daily stavudine treatments for HIV [174]. However, for extended-release formulations, patients need to be reminded that doses should be taken at approximately equal time intervals, e.g. the same time of the day for once-daily preparations. Taking doses too far apart or too close together for these formulations may result in decreased efficacy or increased adverse effects.
Conventionally, modified-release formulations are designed as single-unit dosage forms that contain the active ingredient in a single tablet or capsule. These formulations are challenging for children and older patients to swallow (see Sect. 3.1). Crushing modified-release tablets prior to administration poses an additional risk of toxicity due to the high level of active drug contents. There have been reports of patient deaths resulting from administrating crushed modified-release tablets to older dysphagia patients [175]. Modified-release multiparticulate systems offer a more flexible method for administration to children and older patients and exist as granules, pellets, beads, mini-tablets, microspheres and microcapsules [176–179]. These multiple-unit modified-release systems can be filled into capsules/sachets or compressed into orally disintegrating tablets as the final dosage form [180, 181].
6.2 Fixed-Dose Combinations
Fixed-dose combinations could be useful to reduce pill burden in older patients and could be beneficial for paediatric patients with combined drug therapies such as treatment for HIV. However, this could increase the size of the tablet and cause further swallowing issues. A potential solution could be different coloured pellets that could be mixed together at different strengths by the manufacturer or pharmacist. Fixed-dose combinations in the forms of oral suspensions and dispersible tablets have been proposed in paediatrics for the treatment of HIV [182]. Kayitare et al. [183] have developed a fixed-dose combination tablet of zidovudine and lamivudine for paediatric use that allows dose flexibility and easy administration to children. The rectangular tablet can be broken into eight subunits for dose adjustment according to body weight and each subunit disintegrates rapidly in a small volume of liquid to aid administration. It was suggested that the tablet is suitable for children from infants (from 1 month old) to adolescents (up to 18 years of age) [183].
7 Concluding Remarks
Children and older adults share similarities in oral medication acceptability, particularly difficulties in swallowing conventional tablets and capsules. Appropriate formulation design and selection affect the acceptability of medicines in these two age groups and have an impact on patient safety, therapeutic outcomes and adherence. However, distinct differences in relation to drug therapy are notable in children and older people, and separate considerations in prescribing and formulation development should be given to the two populations. Whilst taste, smell and palatability are major concerns in developing paediatric formulations, characteristics of a medicine affecting safe swallowing are of significant importance in older patients, especially to prevent oesophageal retention and risk of aspiration. Nevertheless, both the young and older populations benefit enormously from the advances in pharmaceutical technology which offers bespoke and appropriate formulations of choice to meet their needs.
References
Kozarewicz P. Regulatory perspectives on acceptability testing of dosage forms in children. Int J Pharm. 2014;469:245–8.
Paradiso LM, Roughead EE, Gilbert AL, et al. Crushing or altering medications: what’s happening residential aged-care facilities? Australas J Ageing. 2002;21:123–1270.
Cuzzolin L, Atzei A, Fanos V. Off-label and unlicensed prescribing for newborns and children in different settings: a review of the literature and a consideration about drug safety. Expert Opin Drug Saf. 2006;5:703–18.
Richey RH, Shah UU, Peak M, et al. Manipulation of drugs to achieve the required dose is intrinsic to paediatric practice but is not supported by guidelines or evidence. BMC Pediatr. 2013;13:81.
Standing JF, Tuleu C. Paediatric formulations—getting to the heart of the problem. Int J Pharm. 2005;300:56–66.
Wright D. Medication administration in nursing homes. Nurs Stand. 2002;16:33–8.
European Medicines Agency (EMA). Guideline on pharmaceutical development of medicines for paediatric use 2011. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2011/06/WC500107908.pdf. Accessed 11 Jul 2014.
European Medicines Agency (EMA). Concept paper on the need of a reflection paper on the quality requirements of medicines for older adults, 2013. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2014/01/WC500159545.pdf. Accessed 11 Sep 2014.
Hajjar ER, Cafiero AC, Hanlon JT. Polypharmacy in elderly patients. Am J Geriatr Pharmacother. 2007;5:345–51.
Claxton AJ, Cramer J, Pierce C. A systematic review of the associations between dose regimens and medication compliance. Clin Ther. 2001;23:1296–310.
Salzman C. Medication compliance in the elderly. J Clin Psychiatry. 1995;56(Suppl 1):18–22 (discussion 23).
Bernabei R, Rossini PM, Di Cioccio L, et al. Compliance and caregiver satisfaction in Alzheimer’s disease: results from the AXEPT Study. Dement Geriatr Cogn Dis Extra. 2012;2:418–32.
Cloyd JC, Kriel RL, Jones-Saete CM, et al. Comparison of sprinkle versus syrup formulations of valproate for bioavailability, tolerance, and preference. J Pediatr. 1992;120:634–8.
Motte J, Pedespan JM, Sevestre M, et al. Acceptability and tolerance of sodium valproate, a new sustained-action granule formulation, in monotherapy for epileptic children from 3 years old [in French]. Arch Pediatr. 2005;12:1533–9.
Sevilla C, Jimenez Caballero PE, Alfonso V, et al. Current treatments of Alzheimer disease: are main caregivers satisfied with the drug treatments received by their patients? Dement Geriatr Cogn Disord. 2009;28:196–205.
Jefferds MED, Ogange L, Owuor M, et al. Formative research exploring acceptability, utilization, and promotion in order to develop a micronutrient powder (Sprinkles) intervention among Luo families in western Kenya. Food Nutr Bull. 2010;31:S179–85.
European Medicines Agency (EMA). Guideline on pharmaceutical development of medicines for paediatric use. 2013. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2013/07/WC500147002.pdf. Accessed 18 Sep 2014.
Stegemann S, Gosch M, Breitkreutz J. Swallowing dysfunction and dysphagia is an unrecognized challenge for oral drug therapy. Int J Pharm. 2012;430:197–206.
Kramer SS, Eicher PM. The evaluation of pediatric feeding abnormalities. Dysphagia. 1993;8:215–24.
Foy TM, Czyzewski DI. Feeding difficulties. In: Duggan CW, Watkins JB, Walker WA, editors. Nutrition in pediatrics: basic science, clinical applications. Hamilton: BC Decker; 2008.
Lefton-Greif MA, Arvedson JC. Pediatric feeding and swallowing disorders: State of health, population trends, and application of the International Classification of Functioning, Disability, and Health. Semin Speech Lang. 2007;28:161–5.
Prasse JE, Kikano GE. An overview of pediatric dysphagia. Clin Pediatr (Phila). 2009;48:247–51.
Kakodkar K, Schroeder JW. Pediatric dysphagia. Pediatr Clin North Am. 2013;60:969–77.
Arvedson JC. Assessment of pediatric dysphagia and feeding disorders: clinical and instrumental approaches. Dev Disabil Res Rev. 2008;14:118–27.
Khan A, Carmona R, Traube M. Dysphagia in the elderly. Clin Geriatr Med. 2014;30:43–53.
Kelly J, Wright D. Administering medication to adult patients with dysphagia. Nurs Stand. 2009;23:62–8.
Steele CM, Greenwood C, Ens I, et al. Mealtime difficulties in a home for the aged: not just dysphagia. Dysphagia. 1997;12:45–50.
Easterling C, Robbins E. Dementia and dysphagia. Geriatr Nurs. 2008;29:275–85.
Crary MA, Humphrey JL, Carnaby-Mann G, et al. Dysphagia, nutrition, and hydration in ischemic stroke patients at admission and discharge from acute care. Dysphagia. 2013;28:69–76.
Gordon C, Hewer RL, Wade DT. Dysphagia in acute stroke. Br Med J (Clin Res Ed). 1987;295:411–4.
Eggenberger SK, Nelms TP. Artificial hydration and nutrition in advanced Alzheimer’s disease: facilitating family decision-making. J Clin Nurs. 2004;13:661–7.
Committee for Medicinal Products for Human Use (CHMP). Reflection paper: formulations of choice for the paediatric population. 2006. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2009/09/WC500003782.pdf. Accessed 11 Sep 2014.
Yeung VW, Wong ICK. When do children convert from liquid antiretroviral to solid formulations? Pharm World Sci. 2005;27:399–402.
Nahirya-Ntege P, Cook A, Vhembo T, et al. Young HIV-infected children and their adult caregivers prefer tablets to syrup antiretroviral medications in Africa. PLoS One. 2012;7:e36186.
Babbitt RL, Parrish JM, Brierley PE, et al. Teaching developmentally disabled children with chronic illness to swallow prescribed capsules. J Dev Behav Pediatr. 1991;12:229–35.
Beck MH, Cataldo M, Slifer KJ, et al. Teaching children with attention deficit hyperactivity disorder (ADHD) and autistic disorder (AD) how to swallow pills. Clin Pediatr (Phila). 2005;44:515–26.
Czyzewski D, Runyan D, Lopez M, et al. Teaching and maintaining pill swallowing in HIV-infected children. AIDS Read. 2000;10:88–94.
Garvie PA, Lensing S, Rai SN. Efficacy of a pill-swallowing training intervention to improve antiretroviral medication adherence in pediatric patients with HIV/AIDS. Pediatrics. 2007;119:E893–9.
Ghuman JK, Cataldo MD, Beck MH, et al. Behavioral training for pill-swallowing difficulties in young children with autistic disorder. J Child Adolesc Psychopharmacol. 2004;14:601–11.
Kaplan BJ, Steiger RA, Pope J, et al. Successful treatment of pill-swallowing difficulties with head posture practice. Paediatr Child Health. 2010;15:e1–5.
Meltzer EO, Welch MJ, Ostrom NK. Pill swallowing ability and training in children 6 to 11 years of age. Clin Pediatr (Phila). 2006;45:725–33.
Steffensen GK, Pachai A, Pedersen SE. Peroral drug administration to children—are there any problems? Ugeskr Laeger. 1998;160:2249–52.
Hansen DL, Tulinius D, Hansen EH. Adolescents’ struggles with swallowing tablets: barriers, strategies and learning. Pharm World Sci. 2008;30:65–9.
Polaha J, Dalton WT III, Lancaster BM. Parental report of medication acceptance among youth: implications for everyday practice. South Med J. 2008;101:1106–12.
Hommel KA, Baldassano RN. Brief report: barriers to treatment adherence in pediatric inflammatory bowel disease. J Pediatr Psychol. 2010;35:1005–10.
Modi AC, Quittner AL. Barriers to treatment adherence for children with cystic fibrosis and asthma: what gets in the way? J Pediatr Psychol. 2006;31:846–58.
Modi AC, Zeller MH, Xanthakos SA, et al. Adherence to vitamin supplementation following adolescent bariatric surgery. Obesity. 2013;21:E190–5.
Schirm E, Tobi H, de Vries TW, et al. Lack of appropriate formulations of medicines for children in the community. Acta Paediatr. 2003;92:1486–9.
Tissen C, Woertz K, Breitkreutz J, et al. Development of mini-tablets with 1 mm and 2 mm diameter. Int J Pharm. 2011;416:164–70.
Kokki H, Nikanne E, Ahonen R. The feasibility of pain treatment at home after adenoidectomy with ketoprofen tablets in small children. Paediatr Anaesth. 2000;10:531–5.
Kreeftmeijer-Vegter AR, de Meijer M, Wegman KA, et al. Development and evaluation of age-appropriate film-coated tablets of levamisole for paediatric use (2–18 years). Expert Opin Drug Deliv. 2013;10:293–300.
Thomson SA, Tuleu C, Wong ICK, et al. Minitablets: new modality to deliver medicines to preschool-aged children. Pediatrics. 2009;123:E235–8.
Klingmann V, Spomer N, Lerch C, et al. Favorable acceptance of mini-tablets compared with syrup: a randomized controlled trial in infants and preschool children. J Pediatr. 2013;163:1728–32.
Van de Vijver E, Desager K, Mulberg AE, et al. Treatment of infants and toddlers with cystic fibrosis-related pancreatic insufficiency and fat malabsorption with pancrelipase MT. J Pediatr Gastroenterol Nutr. 2011;53:61–4.
van Riet-Nales DA, de Neef BJ, Schobben AFAM, et al. Acceptability of different oral formulations in infants and preschool children. Arch Dis Child. 2013;98:725–31.
Strachan I, Greener M. Medication-related swallowing difficulties may be more common than we realise. Pharm Pract. 2005;15:411–4.
Schiele JT, Quinzler R, Klimm HD, et al. Difficulties swallowing solid oral dosage forms in a general practice population: prevalence, causes, and relationship to dosage forms. Eur J Clin Pharmacol. 2013;69:937–48.
Marquis J, Schneider MP, Payot V, et al. Swallowing difficulties with oral drugs among polypharmacy patients attending community pharmacies. Int J Clin Pharm. 2013;35:1130–6.
Hind JA, Nicosia MA, Roecker EB, et al. Comparison of effortful and noneffortful swallows in healthy middle-aged and older adults. Arch Phys Med Rehabil. 2001;82:1661–5.
Nagaya M, Kachi T, Yamada T. Effect of swallowing training on swallowing disorders in Parkinson’s disease. Scand J Rehabil Med. 2000;32:11–5.
Kelly J, D’Cruz G, Wright D. Patients with dysphagia: experiences of taking medication. J Adv Nurs. 2010;66:82–91.
Kikendall JW. Pill-induced esophageal injury. Gastroenterol Clin North Am. 1991;20:835–46.
Delwiche J. The impact of perceptual interactions on perceived flavor. Food Qual Prefer. 2004;15:137–46.
Srivastava RK, More AT. Some aesthetic considerations for over the‐counter (OTC) pharmaceutical products. Int J Biotechnol. 2010;11:267–83.
Kesselheim AS, Misono AS, Shrank WH, et al. Variations in pill appearance of antiepileptic drugs and the risk of nonadherence. JAMA Intern Med. 2013;173:202–8.
Craen AJ, Roos PJ, Vries AL, et al. Effect of colour of drugs: systematic review of perceived effect of drugs and of their effectiveness. BMJ. 1996;313:1624–6.
Smith CJ, Sammons HM, Fakis A, et al. A prospective study to assess the palatability of analgesic medicines in children. J Adv Nurs. 2013;69:655–63.
Overgaard AB, Hojsted J, Hansen R, et al. Patients’ evaluation of shape, size and colour of solid dosage forms. Pharm World Sci. 2001;23:185–8.
Hey H, Jorgensen F, Sorensen K, et al. Oesophageal transit of six commonly used tablets and capsules. Br Med J (Clin Res Ed). 1982;285:1717–9.
Suiter DM, Leder SB. Clinical utility of the 3-ounce water swallow test. Dysphagia. 2008;23:244–50.
Uloza V, Uloziene I, Gradauskiene E. A randomized cross-over study to evaluate the swallow-enhancing and taste-masking properties of a novel coating for oral tablets. Pharm World Sci. 2010;32:420–3.
Diamond S, Lavallee DC. Experience with a pill-swallowing enhancement aid. Clin Pediatr (Phila). 2010;49:391–3.
Yamamoto S, Taniguchi H, Hayashi H, et al. How do tablet properties influence swallowing behaviours? J Pharm Pharmacol. 2013;66:32–9.
Channer KS, Virjee JP. The effect of formulation on oesophageal transit. J Pharm Pharmacol. 1985;37:126–9.
Channer KS, Virjee JP. The effect of size and shape of tablets on their esophageal transit. J Clin Pharmacol. 1986;26:141–6.
Robertson CS, Hardy JG. Oesophageal transit of small tablets. J Pharm Pharmacol. 1988;40:595–6.
Perkins AC, Wilson CG, Blackshaw PE, et al. Impaired oesophageal transit of capsule versus tablet formulations in the elderly. Gut. 1994;35:1363–7.
Perkins AC, Wilson CG, Frier M, et al. Esophageal transit of risedronate cellulose-coated tablet and gelatin capsule formulations. Int J Pharm. 1999;186:169–75.
Evans KT, Roberts GM. The ability of patients to swallow capsules. J Clin Hosp Pharm. 1981;6:207–8.
Channer KS, Virjee J. Effect of posture and drink volume on the swallowing of capsules. Br Med J (Clin Res Ed). 1982;285:1702.
Osmanoglou E, Van Der Voort IR, Fach K, et al. Oesophageal transport of solid dosage forms depends on body position, swallowing volume and pharyngeal propulsion velocity. Neurogastroenterol Motil. 2004;16:547–56.
Bailey RT Jr, Bonavina L, McChesney L, et al. Factors influencing the transit of a gelatin capsule in the esophagus. Drug Intell Clin Pharm. 1987;21:282–5.
Butler SG, Stuart A, Leng X, et al. Factors influencing aspiration during swallowing in healthy older adults. Laryngoscope. 2010;120:2147–52.
Lundy DS, Smith C, Colangelo L, et al. Aspiration: cause and implications. Otolaryngol Head Neck Surg. 1999;120:474–8.
Chee C, Arshad S, Singh S, et al. The influence of chemical gustatory stimuli and oral anaesthesia on healthy human pharyngeal swallowing. Chem Senses. 2005;30:393–400.
Ding R, Logemann JA, Larson CR, et al. The effects of taste and consistency on swallow physiology in younger and older healthy individuals: a surface electromyographic study. J Speech Lang Hear Res. 2003;46:977–89.
Logemann JA, Pauloski BR, Colangelo L, et al. Effects of a sour bolus on oropharyngeal swallowing measures in patients with neurogenic dysphagia. J Speech Hear Res. 1995;38:556–63.
Miura Y, Morita Y, Koizumi H, et al. Effects of taste solutions, carbonation, and cold stimulus on the power frequency content of swallowing submental surface electromyography. Chem Senses. 2009;34:325–31.
Pelletier CA, Dhanaraj GE. The effect of taste and palatability on lingual swallowing pressure. Dysphagia. 2006;21:121–8.
Alves LM, Secaf M, Dantas RO. Effect of a bitter bolus on oral, pharyngeal and esophageal transit of healthy subjects. Arq Gastroenterol. 2013;50:31–4.
Pelletier CA, Lawless HT. Effect of citric acid and citric acid–sucrose mixtures on swallowing in neurogenic oropharyngeal dysphagia. Dysphagia. 2003;18:231–41.
Cola PC, Gatto AR, Silva RG, et al. The influence of sour taste and cold temperature in pharyngeal transit duration in patients with stroke. Arq Gastroenterol. 2010;47:18–21.
Michou E, Mastan A, Ahmed S, et al. Examining the role of carbonation and temperature on water swallowing performance: a swallowing reaction-time study. Chem Senses. 2012;37:799–807.
Sdravou K, Walshe M, Dagdilelis L. Effects of carbonated liquids on oropharyngeal swallowing measures in people with neurogenic dysphagia. Dysphagia. 2012;27:240–50.
Mitchell JC, Counselman FL. A taste comparison of three different liquid steroid preparations: prednisone, prednisolone, and dexamethasone. Acad Emerg Med. 2003;10:400–3.
Gee SC, Hagemann TM. Palatability of liquid anti-infectives: clinician and student perceptions and practice outcomes. J Pediatr Pharmacol Ther. 2007;12:216–23.
Dantas RO, Kern MK, Massey BT, et al. Effect of swallowed bolus variables on oral and pharyngeal phases of swallowing. Am J Physiol. 1990;258:G675–81.
Reimers-Neils L, Logemann J, Larson C. Viscosity effects on EMG activity in normal swallow. Dysphagia. 1994;9:101–6.
Steele CM, Van Lieshout PH. Influence of bolus consistency on lingual behaviors in sequential swallowing. Dysphagia. 2004;19:192–206.
Troche MS, Sapienza CM, Rosenbek JC. Effects of bolus consistency on timing and safety of swallow in patients with Parkinson’s disease. Dysphagia. 2008;23:26–32.
Logemann JA, Gensler G, Robbins J, et al. A randomized study of three interventions for aspiration of thin liquids in patients with dementia or Parkinson’s disease. J Speech Lang Hear Res. 2008;51:173–83.
Bisch EM, Logemann JA, Rademaker AW, et al. Pharyngeal effects of bolus volume, viscosity, and temperature in patients with dysphagia resulting from neurologic impairment and in normal subjects. J Speech Hear Res. 1994;37:1041–59.
Rasley A, Logemann JA, Kahrilas PJ, et al. Prevention of barium aspiration during videofluoroscopic swallowing studies: value of change in posture. AJR Am J Roentgenol. 1993;160:1005–9.
Logemann JA, Rademaker AW, Pauloski BR, et al. Effects of postural change on aspiration in head and neck surgical patients. Otolaryngol Head Neck Surg. 1994;110:222–7.
Solazzo A, Monaco L, Del Vecchio L, et al. Investigation of compensatory postures with videofluoromanometry in dysphagia patients. World J Gastroenterol. 2012;18:2973–8.
Terre R, Mearin F. Effectiveness of chin-down posture to prevent tracheal aspiration in dysphagia secondary to acquired brain injury. A videofluoroscopy study. Neurogastroenterol Motil. 2012;24(414–9):e206.
Ohmae Y, Ogura M, Kitahara S, et al. Effects of head rotation on pharyngeal function during normal swallow. Ann Otol Rhinol Laryngol. 1998;107:344–8.
Cohen R, Rocque F, Lécuyer A, et al. Study of the acceptability of antibiotic syrups, suspensions, and oral solutions prescribed to pediatric outpatients. Eur J Pediatr. 2009;168:851–7.
Ernest TB, Elder DP, Martini LG, et al. Developing paediatric medicines: identifying the needs and recognizing the challenges. J Pharm Pharmacol. 2007;59:1043–55.
Zampini M, Spence C. Assessing the role of visual and auditory cues in multisensory perception of flavor. In: Murray MM, Wallace MT, editors. The neural bases of multisensory processes. Boca Raton: CRC Press; 2012. Chapter 37. http://www.ncbi.nlm.nih.gov/books/NBK92852/. Accessed 18 Sep 2104.
Miller AJ. Deglutition. Physiol Rev. 1982;62:129–84.
Bartoshuk LM. Taste. Robust across the age span? Ann N Y Acad Sci. 1989;561:65–75.
Shabir Q, Skaria C, Brien H, et al. Taste and mouthfeel assessment of porous and non-porous silicon microparticles. Nanoscale Res Lett. 2012;7:1–6.
Coster ST, Schwarz WH. Rheology and the swallow-safe bolus. Dysphagia. 1987;1:113–8.
Leonard RJ, White C, McKenzie S, et al. Effects of bolus rheology on aspiration in patients with dysphagia. J Acad Nutr Diet. 2014;114(4):590–4.
Morecroft CW, Caldwell NA, Gill A. Prescribing liquid medication: can the dose be accurately given? Arch Dis Child. 2013;98:831–2.
Jones DV, Work CE. Volume of a swallow. Am J Dis Child. 1961;102:427.
Adnerhill I, Ekberg O, Groher ME. Determining normal bolus size for thin liquids. Dysphagia. 1989;4:1–3.
Daniels SK, Corey DM, Hadskey LD, et al. Mechanism of sequential swallowing during straw drinking in healthy young and older adults. J Speech Lang Hear Res. 2004;47:33–45.
Balou M, McCullough GH, Aduli F, et al. Manometric measures of head rotation and chin tuck in healthy participants. Dysphagia. 2014;29(1):25–32.
Sakuma T, Kida I. Relationship between ease of swallowing and deglutition-related muscle activity in various postures. J Oral Rehabil. 2010;37:583–9.
Ekberg O. Posture of the head and pharyngeal swallowing. Acta Radiol Diagn (Stockh). 1986;27:691–6.
Shanahan TK, Logemann JA, Rademaker AW, et al. Chin-down posture effect on aspiration in dysphagic patients. Arch Phys Med Rehabil. 1993;74:736–9.
Welch MV, Logemann JA, Rademaker AW, et al. Changes in pharyngeal dimensions effected by chin tuck. Arch Phys Med Rehabil. 1993;74:178–81.
Logemann JA, Kahrilas PJ, Kobara M, et al. The benefit of head rotation on pharyngoesophageal dysphagia. Arch Phys Med Rehabil. 1989;70:767–71.
Motte J, Pedespan JM, Sevestre M, et al. Acceptability and tolerance of sodium valproate, a new sustained-action granule formulation, in monotherapy for epileptic children from 3 years old. Arch Pediatr. 2005;12:1533–9.
Zlotkin S, Arthur P, Antwi KY, et al. Treatment of anemia with microencapsulated ferrous fumarate plus ascorbic acid supplied as sprinkles to complementary (weaning) foods. Am J Clin Nutr. 2001;74:791–5.
Zlotkin S, Antwi KY, Schauer C, et al. Use of microencapsulated iron(II) fumarate sprinkles to prevent recurrence of anaemia in infants and young children at high risk. Bull World Health Organ. 2003;81:108–15.
Hirve S, Bhave S, Bavdekar A, et al. Low dose ‘sprinkles’—an innovative approach to treat iron deficiency anemia in infants and young children. Indian Pediatr. 2007;44:91–100.
Adu-Afarwuah S, Lartey A, Brown KH, et al. Home fortification of complementary foods with micronutrient supplements is well accepted and has positive effects on infant iron status in Ghana. Am J Clin Nutr. 2008;87:929–38.
Geltman PL, Hironaka LK, Mehta SD, et al. Iron supplementation of low-income infants: a randomized clinical trial of adherence with ferrous fumarate sprinkles versus ferrous sulfate drops. J Pediatr. 2009;154:738–43.
den Uyl D, Geusens PP, van Berkum FN, et al. Patient preference and acceptability of calcium plus vitamin D3 supplementation: a randomised, open, cross-over trial. Clin Rheumatol. 2010;29:465–72.
MacDonald A, Lilburn M, Davies P, et al. ‘Ready to drink’ protein substitute is easier is for people with phenylketonuria. J Inherit Metab Dis. 2006;29:526–31.
Nasrin D, Larson CP, Sultana S, et al. Acceptability of and adherence to dispersible zinc tablet in the treatment of acute childhood diarrhoea. J Health Popul Nutr. 2005;23:215–21.
Winch PJ, Gilroy KE, Doumbia S, et al. Short report: prescription and administration of a 14-day regimen of zinc treatment for childhood diarrhea in Mali. Am J Trop Med Hyg. 2006;74:880–3.
Ameen VZ, Pobiner BF, Giguere GC, et al. Ranitidine (Zantac) syrup versus ranitidine effervescent tablets (Zantac) EFFERdose) in children: a single-center taste preference study. Paediatr Drugs. 2006;8:265–70.
Bayer AJ, Day JJ, Finucane P, et al. Bioavailability and acceptability of a dispersible formulation of levodopa-benserazide in parkinsonian patients with and without dysphagia. J Clin Pharm Ther. 1988;13:191–4.
Tolia V, Han C, North JD, et al. Taste comparisons for lansoprazole strawberry-flavoured delayed-release orally disintegrating tablet and ranitidine peppermint-flavoured syrup in children. Clin Drug Investig. 2005;25:285–92.
Cohen IT, Joffe D, Hummer K, et al. Ondansetron oral disintegrating tablets: acceptability and efficacy in children undergoing adenotonsillectomy. Anesth Analg. 2005;101:59–63.
Freedman SB, Adler M, Seshadri R, et al. Oral ondansetron for gastroenteritis in a pediatric emergency department. N Engl J Med. 2006;354:1698–705.
Danileviciute V, Sveikata A, Adomaitiene V, et al. Efficacy, tolerability, and preference of mirtazapine orally disintegrating tablets in depressed patients: a 17-week naturalistic study in Lithuania. Medicina (Kaunas). 2009;45:778–84.
Wade AG, Crawford GM, Young D. A survey of patient preferences for a placebo orodispersible tablet. Patient Prefer Adherence. 2012;6:201–6.
Kinon BJ, Hill AL, Liu H, et al. Olanzapine orally disintegrating tablets in the treatment of acutely ill non-compliant patients with schizophrenia. Int J Neuropsychopharmacol. 2003;6:97–102.
Nelson JC, Hollander SB, Betzel J, et al. Mirtazapine orally disintegrating tablets in depressed nursing home residents 85 years of age and older. Int J Geriatr Psychiatry. 2006;21:898–901.
Nausieda PA. A multicenter, open-label, sequential study comparing preferences for carbidopa-levodopa orally disintegrating tablets and conventional tablets in subjects with Parkinson’s disease. Clin Ther. 2005;27:58–63.
Michele TM, Knorr B, Vadas EB, et al. Safety of chewable tablets for children. J Asthma. 2002;39:391–403.
Bukstein DA, Bratton DL, Firriolo KM, et al. Evaluation of parental preference for the treatment of asthmatic children aged 6 to 11 years with oral montelukast or inhaled cromolyn: a randomized, open-label, crossover study. J Asthma. 2003;40:475–85.
Lazarus CL, Logemann JA, Rademaker AW, et al. Effects of bolus volume, viscosity, and repeated swallows in nonstroke subjects and stroke patients. Arch Phys Med Rehabil. 1993;74:1066–70.
Lee KL, Kim WH, Kim EJ, et al. Is swallowing of all mixed consistencies dangerous for penetration-aspiration? Am J Phys Med Rehabil. 2012;91:187–92.
Tsukada T, Taniguchi H, Ootaki S, et al. Effects of food texture and head posture on oropharyngeal swallowing. J Appl Physiol. 1985;2009(106):1848–57.
World Health Organization. Development of paediatric medicines: points to consider in pharmaceutical development (Working document QAS/08.257/Rev.3), 2012. http://www.who.int/medicines/areas/quality_safety/quality_assurance/Rev3-PaediatricMedicinesDevelopment_QAS08-257Rev3_17082011.pdf. Accessed 18 Sep 2014.
Gerrard SE, Orlu-Gul M, Tuleu C, et al. Modeling the physiological factors that affect drug delivery from a nipple shield delivery system to breastfeeding infants. J Pharm Sci. 2013;102:3773–83.
Dessirier JM, Simons CT, Carstens MI, et al. Psychophysical and neurobiological evidence that the oral sensation elicited by carbonated water is of chemogenic origin. Chem Senses. 2000;25:277–84.
Maguire A, Baqir W, Nunn JH. Are sugars-free medicines more erosive than sugars-containing medicines? An in vitro study of paediatric medicines with prolonged oral clearance used regularly and long-term by children. Int J Paediatr Dent. 2007;17:231–8.
George J, Majeed W, Mackenzie IS, et al. Association between cardiovascular events and sodium-containing effervescent, dispersible, and soluble drugs: nested case–control study. BMJ. 2013;347:f6954.
Ubeda A, Llopico J, Sanchez MT. Blood pressure reduction in hypertensive patients after withdrawal of effervescent medication. Pharmacoepidemiol Drug Saf. 2009;18:417–9.
Carnaby-Mann G, Crary M. Pill swallowing by adults with dysphagia. Arch Otolaryngol Head Neck Surg. 2005;131:970–5.
Montgomery W, Treuer T, Karagianis J, et al. Orally disintegrating olanzapine review: effectiveness, patient preference, adherence, and other properties. Patient Prefer Adherence. 2012;6:109–25.
Gupta A, Chidambaram N, Khan MA. An index for evaluating difficulty of chewing the chewable tablets. Drug Dev Ind Pharm. Epub 2013 Nov 19.
Food and Drug Administration (FDA). Guidance for industry size of beads in drug products labeled for sprinkle, 2012. http://www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/UCM240243.pdf. Accessed 11 Jul 2014.
An alternative medicine treatment for Parkinson’s disease: results of a multicenter clinical trial. HP-200 in Parkinson’s Disease Study Group. J Altern Complement Med. 1995;1:249–55.
Baqir W, Maguire A. Consumption of prescribed and over-the-counter medicines with prolonged oral clearance used by the elderly in the Northern Region of England, with special regard to generic prescribing, dose form and sugars content. Public Health. 2000;114:367–73.
Keith S. Advances in psychotropic formulations. Prog Neuropsychopharmacol Biol Psychiatry. 2006;30:996–1008.
Muramatsu RS, Litzinger MH, Fisher E, et al. Alternative formulations, delivery methods, and administration options for psychotropic medications in elderly patients with behavioral and psychological symptoms of dementia. Am J Geriatr Pharmacother. 2010;8:98–114.
Delaney AL, Rudolph C. Nascent oral phase. In: Shaker R, Belafsky PC, Postma GN, et al., editors. Principles of deglutition. New York: Springer; 2013.
Kida IA, Astrom AN, Strand GV, et al. Chewing problems and dissatisfaction with chewing ability: a survey of older Tanzanians. Eur J Oral Sci. 2007;115:265–74.
Peltola P, Vehkalahti MM. Chewing ability of the long-term hospitalized elderly. Spec Care Dentist. 2005;25:260–4.
Yoshioka M, Hinode D, Yokoyama M, et al. Relationship between subjective oral health status and lifestyle in elderly people: a cross-sectional study in Japan. ISRN Dent. 2013;2013:687139.
Avlund K, Holm-Pedersen P, Schroll M. Functional ability and oral health among older people: a longitudinal study from age 75 to 80. J Am Geriatr Soc. 2001;49:954–62.
Okabe H, Suzuki E, Sugiura Y, et al. Development of an easily swallowed film formulation. Int J Pharm. 2008;355:62–6.
Cassolato SF, Turnbull RS. Xerostomia: clinical aspects and treatment. Gerodontology. 2003;20:64–77.
Imai K. Alendronate sodium hydrate (oral jelly) for the treatment of osteoporosis: review of a novel, easy to swallow formulation. Clin Interv Aging. 2013;8:681–8.
Doesch AO, Mueller S, Konstandin M, et al. Increased adherence after switch from twice daily calcineurin inhibitor based treatment to once daily modified released tacrolimus in heart transplantation: a pre-experimental study. Transplant Proc. 2010;42:4238–42.
Portsmouth SD, Osorio J, McCormick K, et al. Better maintained adherence on switching from twice-daily to once-daily therapy for HIV: a 24-week randomized trial of treatment simplification using stavudine prolonged-release capsules. HIV Med. 2005;6:185–90.
Schier JG, Howland MA, Hoffman RS, et al. Fatality from administration of labetalol and crushed extended-release nifedipine. Ann Pharmacother. 2003;37:1420–3.
Vergote GJ, Vervaet C, Van Driessche I, et al. An oral controlled release matrix pellet formulation containing nanocrystalline ketoprofen. Int J Pharm. 2001;219:81–7.
Yamada T, Onishi H, Machida Y. Sustained release ketoprofen microparticles with ethylcellulose and carboxymethylethylcellulose. J Control Release. 2001;75:271–82.
Lopes CM, Lobo JM, Pinto JF, et al. Compressed matrix core tablet as a quick/slow dual-component delivery system containing ibuprofen. AAPS PharmSciTech. 2007;8:E76.
Shimokawa K, Saegusa K, Wada Y, et al. Physicochemical properties and controlled drug release of microcapsules prepared by simple coacervation. Colloids Surf B Biointerfaces. 2013;104:1–4.
Abdul S, Chandewar AV, Jaiswal SB. A flexible technology for modified-release drugs: multiple-unit pellet system (MUPS). J Control Release. 2010;147:2–16.
Wilson JT, Helms R, Pickering BD, et al. Acetaminophen controlled-release sprinkles versus acetaminophen immediate-release elixir in febrile children. J Clin Pharmacol. 2000;40:360–9.
Pensi T. Fixed dose combination of lamivudine, stavudine and nevirapine in the treatment of pediatric HIV infection: a preliminary report. Indian Pediatr. 2007;44:519–21.
Kayitare E, Vervaet C, Ntawukulilyayo JD, et al. Development of fixed dose combination tablets containing zidovudine and lamivudine for paediatric applications. Int J Pharm. 2009;370:41–6.
Author information
Authors and Affiliations
Corresponding author
Additional information
On behalf of European Paediatric Formulation Initiatives (EuPFI).
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, and provide a link to the Creative Commons license. You do not have permission under this license to share adapted material derived from this article or parts of it.
The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
To view a copy of this license, visit (http://creativecommons.org/licenses/by-nc-nd/4.0/)
About this article
Cite this article
Liu, F., Ranmal, S., Batchelor, H.K. et al. Patient-Centered Pharmaceutical Design to Improve Acceptability of Medicines: Similarities and Differences in Paediatric and Geriatric Populations. Drugs 74, 1871–1889 (2014). https://doi.org/10.1007/s40265-014-0297-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-014-0297-2