Abstract
Introduction
Sex-difference in types of cardiac organ damage has been reported in subjects with increased body mass index (BMI). However less is known about sex-differences in left ventricular (LV) myocardial function assessed by global longitudinal strain (GLS) in these subjects.
Methods
493 subjects (mean age 47 ± 9 years, 61% women) with BMI > 27.0 kg/m2 and without known cardiac disease underwent 24-hour (24h) ambulatory blood pressure (BP) recording, body composition analysis, carotid-femoral pulse wave velocity (PWV) measurement and echocardiography. LV peak systolic GLS was measured by two-dimensional speckle tracking echocardiography and LV ejection fraction (EF) by biplane Simpson’s method. Insulin sensitivity was assessed by homeostatic model of insulin resistance (HOMA-IR).
Results
Women had higher prevalence of increased waist circumference (99% vs. 82%), lower prevalence of hypertension (59 vs. 74%), and lower serum triglycerides (1.3 ± 0.7 vs. 1.7 ± 0.9 mmol/L) and carotid-femoral PWV (7.3 ± 1.6 vs. 7.7 ± 1.6 m/s) compared to men (all p < 0.05). Women also had higher (more negative) GLS compared to men (− 19.9 ± 3.0 vs. − 18.6 ± 3.0%, p < 0.001), while EF did not differ between sexes. In multivariable linear regression analyses, lower GLS in women was associated with higher waist circumference and PWV and with lower EF (all p < 0.05). In men, lower GLS was associated with higher waist circumference and HOMA-IR, and with lower EF (all p < 0.05).
Conclusions
Among subjects with increased BMI, GLS was higher in women than men. Lower GLS was associated with abdominal obesity in both sexes, and with impaired glucose metabolism in men, and with higher arterial stiffness in women.
Trial registration
https://www.clinicaltrials.gov NCT02805478, first registered 20.06.16.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
The obesity epidemic has resulted in an increasing prevalence of cardiometabolic disorders both in women and men [1, 2]. Underlying mechanisms include obesity-associated left ventricular (LV) volume and pressure overload, chronic inflammation and clustering of cardiovascular risk factors like hypertension, impaired glucose metabolism and dyslipidemia [3,4,5]. Previous studies in subjects with increased body mass index (BMI) have demonstrated that although systolic LV function measured by ejection fraction (EF) often is normal, myocardial function assessed by global longitudinal strain (GLS) or stress-corrected midwall shortening is often reduced [4, 6,7,8]. This has been attributed to interstitial fat infiltration and triglyceride accumulation in the contractile elements in the obese heart, affecting both LV mass, systolic function and myocardial energetic efficiency [9, 10]. Recently, an association between increased epicardial adipose tissue, higher myocardial fat content and reduced LV GLS was published [11].
Sex differences in prevalence and type of subclinical cardiac disease in subjects with increased BMI have previously been reported [3, 12]. Both in healthy subjects and in patients with hypertension, previous studies have found lower LV GLS in men than women [13, 14]. The Hypertension Genetic Epidemiology Network study found that higher waist circumference and waist-hip ratio was associated with lower LV GLS, but did not report sex-specific results [15]. Taken together, these results indicate that LV GLS is lower in subjects with increased BMI, but sex specific confounders of LV GLS are not well documented. Thus, the aim of the current study was to explore LV GLS and its covariates in women and men with increased BMI.
2 Methods
2.1 Study Population
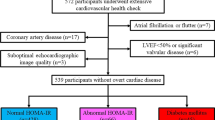
A total of 620 women and men between 30 and 65 years of age, with BMI > 27.0 kg/m2 were prospectively recruited to the FAT associated CardiOvasculaR dysfunction (FATCOR) study at Haukeland University Hospital in Bergen, Norway, between 2009 and 2017. In the present analysis, a total of 127 participants were excluded due to incomplete echocardiographic data (n = 51), insufficient echocardiographic image quality (n = 49), hardware mismatch (n = 25) and withdrawal of consent (n = 2). Details about methods used in the FATCOR study have been published previously [3, 16,17,18]. In short, recruitment of participants was done in collaboration with a primary health care center with particular interest in management of obesity. Most subjects were recruited through a local newspaper advertisement. Exclusion criteria in the FATCOR study were previous myocardial infarction, gastrointestinal disorders, severe psychiatric illness or inability to understand Norwegian language. The included group was older than the excluded group (49.7 ± 8.9 vs. 47.3 ± 9.2 years, p < 0.01), while sex, BMI, or prevalence of hypertension and diabetes mellitus did not differ between the included and the excluded groups. The FATCOR study was conducted in accordance with the Declaration of Helsinki from 1975 and was approved by the Regional Ethics Committee. All participants signed a written informed consent form.
2.2 Cardiovascular Risk Assessment
All study participants underwent a standardized clinical examination at the general practitioner center. A standardized questionnaire was used for self-reported health and use of medication. This information was quality assured by a study nurse.
Tetrapolar bioelectrical impedance analysis (Tatina-TBF-300A, Tanita Corporation of America, Arlington Heights, USA) was used to analyze body composition including total body weight, BMI, fat and muscle mass. Obesity was considered present if BMI ≥ 30.0 kg/m2 [19].
Clinic blood pressure (BP) was measured with an Omron M4 sphygmomanometer (Omron Healthcare Co. Ltd., Hoofdorp, Netherlands) using a correctly sized cuff in the individual participant. Attended clinic BP was measured in triplets after 5 minutes initial rest in seated position with 1-min intervals between the measurements [20]. The average of the two last BP measurements was taken as the clinic BP.
Ambulatory 24-hour (24h) BP (24hBP) recording was performed with a correctly sized cuff on the non-dominant arm in the individual participant, using Diasys Integra II recorders (Novacor, Cedex, France). Measurements were done with 20 min interval during daytime and 30 min interval during nighttime. Participants were instructed to follow their daily routine during the recording and relax the arm during cuff expansion. Hypertension was considered present if participants used anti-hypertensive medication or had elevated 24hBP (24h systolic BP ≥ 130 mmHg and/or 24h diastolic BP ≥ 80 mmHg).
Serum lipid profile was measured in fasting venous blood samples [16]. A standardized 2-h oral glucose tolerance test was performed in participants without previously diagnosed diabetes mellitus. Diabetes mellitus was considered present if any of the following factors were present in the individual participant: history of diabetes, fasting plasma glucose ≥ 7.0 mmol/L, glycated hemoglobin A1c (HbA1c) ≥ 6.5% or a 2-h plasma glucose ≥ 11.1 mmol/L after oral glucose tolerance test [21]. The homeostatic model of insulin resistance (HOMA-IR) was calculated as the product of fasting plasma insulin and glucose divided by 22.5 [22]. The metabolic syndrome (MetS) was considered present if any 3 of the 5 following criteria were met in the individual participant: increased waist circumference (≥ 102 cm in men, ≥ 88 cm in women), elevated serum triglycerides (TG) (≥ 1.7 mmol/L), reduced serum HDL cholesterol (< 1.03 mmol/L in men, < 1.3 mmol/L in women), elevated BP (≥ 130 mmHg systolic and/or ≥ 85 mmHg diastolic BP or the use of antihypertensive treatment), and elevated fasting glucose (≥ 5.6 mmol/L) or drug treatment for elevated glucose [23].
2.3 Arterial Stiffness Assessment
Applanation tonometry (SphygmoCor, AtCor Medical, Sydney, West Ryde, Australia) was used to measure carotid-femoral pulse wave velocity (PWV). A PWV > 10 m/s was considered increased [20].
2.4 Conventional Echocardiography
A transthoracic two-dimensional (2D) echocardiogram was performed following a standardized imaging protocol on a Vivid E9 echocardiograph (GE Vingmed Ultrasound, Horten, Norway) as previously described [3]. The echocardiographic images were digitally stored and post-processed offline in the Echocardiography Core Laboratory at the University of Bergen, Norway using Image Arena software version 4.6 (TomTec Imaging Systems GmbH, Unterschleissheim, Germany). Quantitative echocardiographic analyses were performed in accordance with current guidelines for chamber quantification [24]. Relative wall thickness was calculated from posterior wall thickness/LV internal radius ratio and considered increased if ≥ 0.43 [20, 25]. LV mass was calculated using Devereux’s formula and indexed for body height in the allometric power of 2.7. LV hypertrophy was defined by the prognostically validated cut-off values; LV mass index > 46.7 g/m2.7 in women and > 49.2 g/m2.7 in men, respectively [24, 26]. LV EF was calculated by the biplane Simpson method [24]. All conventional image analyses were proof read by a single expert reader (EG) as recommended for clinical trials [27].
2.5 Speckle Tracking Echocardiography
Analysis was performed by a single junior reader (NP) on a workstation equipped with EchoPAC version BT202 software (GE Vingmed Ultrasound, Horten, Norway) and quality assured by a single experienced reader (SS). Peak systolic LV GLS was measured by Automated Function Imaging in each LV segment using an 18-segment model and apical 4-, 2- and 3-chamber views. The region of interest (ROI) was automatically generated based on three manual points set by the reader. To include the myocardium and avoid the pericardium or optimize tracking, the reader manually adjusted the ROI when necessary.
2.6 Statistical Analysis
Statistical analyses were performed using the IBM SPSS Statistics software version 25 (IBM, Armonk, New York, USA). The cohort was split by sex. For the descriptive analyses, continuous variables were presented as mean ± standard deviation and categorical variables as percentages. Uni- and multivariable linear regression analyses with collinearity tools were used to identify the covariables of LV GLS. Results are reported as standardized beta coefficients and p-values. Inter-observer reproducibility of LV GLS was evaluated by reanalysis of 26 randomly selected study participants and reported as interclass correlation coefficient and 95% confidence interval (CI). A p-value < 0.05 was considered statistically significant in all analyses.
3 Results
The total study population was on average 47 ± 9 years, included 61% women, and the mean BMI was 32.1 ± 4.2 kg/m2. Women had higher BMI and higher prevalence of increased waist circumference, but lower prevalence of hypertension, serum TG and blood glucose compared to men (all p < 0.05), while HOMA-IR and the prevalence of diabetes mellitus did not differ between sexes (Table 1). Although LV EF did not differ between sexes, average LV GLS was significantly lower in men than women (p < 0.001) (Table 2).
The inter-observer reproducibility of GLS was excellent with interclass correlation coefficient 0.96 [95% CI 0.95–0.98]. In the total study population, lower LV GLS was independently associated with male sex both in univariable (β = 0.21) and multivariable analyses (β = 0.25) (both p < 0.05). In women, lower LV GLS was significantly associated with higher waist circumference, serum TG, HOMA-IR, PWV and hypertension in univariable analyses (all p < 0.05) (Table 3). In multivariable linear regression analysis, lower LV GLS remained associated with higher waist circumference and PWV and with lower LV EF in women (all p < 0.05) (Table 3). In men, lower LV GLS was associated with higher HOMA-IR and waist circumference and with lower LV EF analysis both in uni- and multivariable linear regression analysis (all p < 0.05) (Table 3).
There was an inversed, linear correlation between GLS and serum triglyceride in women, r = 0.15, p = 0.010, but not in men (Fig. 1a). However, the negative, linear correlation between GLS and C-peptide was stronger in men than women, r = 0.28, p = 0.001 and r = 0.16, p = 0.006 (Fig. 1b).
4 Discussion
The present study assessed the impact of sex on LV myocardial function measured by GLS in subjects with increased BMI and without known cardiovascular disease. In particular, the results demonstrate that: (1) women with increased BMI had higher LV GLS than men despite a comparable LV EF, (2) lower LV GLS was associated with male sex independent of higher PWV, HOMA-IR and waist circumference in the total study population, and (3) in sex-specific analyses, lower LV GLS was associated with higher waist circumference in both sexes, and particularly with higher HOMA-IR in men, and with higher arterial stiffness in women.
Sex differences in body fatness and fat distribution are well known [28]. While men are more prone to abdominal fat deposition around the internal organs, referred to as visceral obesity, women preferentially store fat subcutaneously in the gluteofemoral region [29]. Visceral obesity leads to insulin resistance and chronic low-grade systemic inflammation, contributing to development of preclinical and clinical cardiovascular disease [30]. However, a stronger influence of abdominal obesity on LV mass in women than men was demonstrated in the community-based Strong Heart Study which included a high proportion of subjects with obesity and type 2 diabetes [12]. Further, in treated hypertensive subjects followed in the Campania Salute Network project, obesity was identified as a more powerful risk factor for incident LV hypertrophy in women than men [31]. In our study LV GLS was higher in women than in men, independent of LV EF, in line with previous findings in community-based and hypertensive cohorts [13, 14, 32]. Interestingly, women had higher LV GLS despite the higher prevalence of abdominal obesity, reflected by increased waist circumference, in women compared to men. Furthermore, higher arterial stiffness, measured by carotid-femoral PWV, remained significantly associated with lower LV GLS after adjustment for confounders only in women, despite the higher PWV in men. Bell et al. demonstrated in the much larger Framingham Offspring and Omni study that higher PWV was associated with lower LV GLS in both women and men, while higher characteristic impedance was associated with lower LV GLS only in women [32]. Taken together, it may be suggested that LV long-axis function in women may be particularly sensitive to mechanical coupling in the proximal aorta. Of note, the 2495 participants in the Framingham Offspring and Omni study were on average 20 years older than the present study cohort and non-obese [32]. Thus, the present results expand previous findings to middle-aged women with increased BMI.
In the present study, HOMA-IR, a marker of insulin sensitivity, was particularly associated with lower LV GLS in men, independent of abdominal obesity. The observation adds to a previous report by Blomstrand et al. indicating a progressive reduction in LV GLS with increasing BMI in participants with type 2 diabetes [33]. However, sex-specific results were not provided in their report. In women, an association of higher serum TG, an important component of atherogenic dyslipidemia, with reduced LV GLS was found in univariable analysis, while no such correlation was identified in men. However, this association was attenuated when adjusted for HOMA-IR. A possible explanation for these diverging findings may be the higher estrogen level in women, which has been shown to decrease glucose oxidation, protect from insulin resistance and increase fatty acid oxidation in liver and skeletal muscles [34, 35]. Furthermore, Peterson et al. demonstrated in studies of myocardial metabolism using positron emission tomography that obesity was associated with increased myocardial oxygen demand and myocardial fatty acid metabolism [36], and that the influence of obesity on myocardial glucose metabolism was more pronounced in men than women [37]. Furthermore, in a study of healthy volunteers, Ng et al. found an association between increased epicardial adipose tissue, more extensive adipose infiltration in LV myocardium and reduced LV GLS [11]. From this it may be hypothesized that sex differences in epicardial and myocardial fat content may contribute to the observed sex difference in myocardial function found by LV GLS in the present study. However, neither computer tomography, nor positron emission tomography of the heart was performed in the FATCOR study.
4.1 Study Limitations
Due to the cross-sectional study design causality between LV GLS and the identified covariates cannot be claimed. The study participants were mostly recruited through an advertisement in the local newspaper, which may have caused some selection bias. Furthermore, in this cross-sectional study the duration of increased BMI and hypertension in the individual participant is unknown. Measurements of sex hormones and information regarding menopause-status were not included in our study.
5 Conclusion
In subjects with increased BMI without known cardiac disease participating in the FATCOR study, women had better myocardial function assessed by LV GLS compared to men, despite more pronounced visceral obesity. Lower LV GLS was associated with increased abdominal obesity and LV EF in both sexes, and particularly with arterial stiffness in women, and with insulin resistance in men.
References
Alpert MA, Lavie CJ, Agrawal H, Aggarwal KB, Kumar SA. Obesity and heart failure: epidemiology, pathophysiology, clinical manifestations, and management. Transl Res. 2014;164(4):345–56. https://doi.org/10.1016/j.trsl.2014.04.010.
Gerdts E, Regitz-Zagrosek V. Sex differences in cardiometabolic disorders. Nat Med. 2019;25(11):1657–66. https://doi.org/10.1038/s41591-019-0643-8.
Halland H, Lønnebakken MT, Pristaj N, Saeed S, Midtbø H, Einarsen E, et al. Sex differences in subclinical cardiac disease in overweight and obesity (the FATCOR study). Nutr Metab Cardiovasc Dis. 2018. https://doi.org/10.1016/j.numecd.2018.06.014.
Wong CY, O’Moore-Sullivan T, Leano R, Byrne N, Beller E, Marwick TH. Alterations of left ventricular myocardial characteristics associated with obesity. Circulation. 2004;110(19):3081–7. https://doi.org/10.1161/01.CIR.0000147184.13872.0F.
Muiesan ML, Paini A, Aggiusti C, Bertacchini F, Rosei CA, Salvetti M. Hypertension and organ damage in women. High Blood Press Cardiovasc Prev. 2018;25(3):245–52. https://doi.org/10.1007/s40292-018-0265-0.
Lund BP, Gohlke-Bärwolf C, Cramariuc D, Rossebo AB, Rieck AE, Gerdts E. Effect of obesity on left ventricular mass and systolic function in patients with asymptomatic aortic stenosis (a Simvastatin Ezetimibe in Aortic Stenosis [SEAS] substudy). Am J Cardiol. 2010;105(10):1456–60. https://doi.org/10.1016/j.amjcard.2009.12.069.
Tadic M, Cuspidi C, Majstorovic A, Pencic B, Backovic S, Ivanovic B, et al. Does the metabolic syndrome impact left-ventricular mechanics? A two-dimensional speckle tracking study. J Hypertens. 2014;32(9):1870–8. https://doi.org/10.1097/hjh.0000000000000257.
Rogge BP, Gerdts E, Cramariuc D, Bahlmann E, Jander N, Gohlke-Bärwolf C, et al. Impact of obesity and nonobesity on grading the severity of aortic valve stenosis. Am J Cardiol. 2014;113(9):1532–5. https://doi.org/10.1016/j.amjcard.2014.01.429.
Murdolo G, Angeli F, Reboldi G, Di Giacomo L, Aita A, Bartolini C, et al. Left ventricular hypertrophy and obesity: only a matter of fat? High Blood Press Cardiovasc Prev. 2015;22(1):29–41. https://doi.org/10.1007/s40292-014-0068-x.
Mancusi C, Losi MA, Izzo R, Canciello G, Manzi MV, Sforza A, et al. Effect of diabetes and metabolic syndrome on myocardial mechano-energetic efficiency in hypertensive patients. The Campania Salute Network. J Hum Hypertens. 2017;31(6):395–9. https://doi.org/10.1038/jhh.2016.88.
Ng ACT, Strudwick M, van der Geest RJ, Ng ACC, Gillinder L, Goo SY, et al. Impact of epicardial adipose tissue, left ventricular myocardial fat content, and interstitial fibrosis on myocardial contractile function. Circ Cardiovasc Imaging. 2018;11(8):e007372. https://doi.org/10.1161/CIRCIMAGING.117.007372.
De Simone G, Devereux RB, Chinali M, Roman MJ, Barac A, Panza JA, et al. Sex differences in obesity-related changes in left ventricular morphology: the Strong Heart Study. J Hypertens. 2011;29(7):1431–8. https://doi.org/10.1097/HJH.0b013e328347a093.
Kocabay G, Muraru D, Peluso D, Cucchini U, Mihaila S, Padayattil-Jose S, et al. Normal left ventricular mechanics by two-dimensional speckle-tracking echocardiography. Reference values in healthy adults. Rev Esp Cardiol (Engl Ed). 2014;67(8):651–8. https://doi.org/10.1016/j.rec.2013.12.009.
Tadic M, Cuspidi C, Celic V, Ivanovic B, Pencic B, Grassi G. The influence of sex on left ventricular strain in hypertensive population. J Hypertens. 2019;37(1):50–6. https://doi.org/10.1097/HJH.0000000000001838.
Selvaraj S, Martinez EE, Aguilar FG, Kim KY, Peng J, Sha J, et al. Association of central adiposity with adverse cardiac mechanics: findings from the hypertension genetic epidemiology network study. Circ Cardiovasc Imaging. 2016. https://doi.org/10.1161/CIRCIMAGING.115.004396.
Strandheim A, Halland H, Saeed S, Cramariuc D, Hetland T, Lønnebakken MT, et al. Obesity-associated metabolic changes influence resting and peak heart rate in women and men. Scand Cardiovasc J. 2015;49(6):337–43. https://doi.org/10.3109/14017431.2015.1081273.
Halland H, Lønnebakken MT, Saeed S, Midtbø H, Cramariuc D, Gerdts E. Does fitness improve the cardiovascular risk profile in obese subjects? Nutr Metab Cardiovasc Dis. 2017;27(6):518–24. https://doi.org/10.1016/j.numecd.2017.04.006.
Halland H, Matre K, Einarsen E, Midtbø H, Saeed S, Pristaj N, et al. Effect of fitness on cardiac structure and function in overweight and obesity (the FATCOR study). Nutr Metab Cardiovasc Dis. 2019;29(7):710–7. https://doi.org/10.1016/j.numecd.2019.03.012.
WHO. Obesity and overweight. 2018. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Accessed 16 Dec 2018.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Cardiology and the European Society of Hypertension. J Hypertens. 2018;36(10):1953–2041. https://doi.org/10.1097/HJH.0000000000001940.
American Diabetes A. 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2018. Diabetes Care. 2018;41(Suppl 1):S13–27. https://doi.org/10.2337/dc18-S002.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28(7):412–9. https://doi.org/10.1007/BF00280883.
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute scientific statement: executive summary. Crit Pathw Cardiol. 2005;4(4):198–203. https://doi.org/10.1097/00132577-200512000-00018.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2015;16(3):233–70. https://doi.org/10.1093/ehjci/jev014.
Gerdts E, Cramariuc D, de Simone G, Wachtell K, Dahlof B, Devereux RB. Impact of left ventricular geometry on prognosis in hypertensive patients with left ventricular hypertrophy (the LIFE study). Eur J Echocardiogr. 2008;9(6):809–15. https://doi.org/10.1093/ejechocard/jen155.
Gerdts E, Rossebo AB, Pedersen TR, Cioffi G, Lønnebakken MT, Cramariuc D, et al. Relation of left ventricular mass to prognosis in initially asymptomatic mild to moderate aortic valve stenosis. Circ Cardiovasc Imaging. 2015;8(11):e003644. https://doi.org/10.1161/CIRCIMAGING.115.003644 (discussion e).
Galderisi M, Henein MY, D’Hooge J, Sicari R, Badano LP, Zamorano JL, et al. Recommendations of the European Association of Echocardiography: how to use echo-Doppler in clinical trials: different modalities for different purposes. Eur J Echocardiogr. 2011;12(5):339–53. https://doi.org/10.1093/ejechocard/jer051.
Palmer BF, Clegg DJ. The sexual dimorphism of obesity. Mol Cell Endocrinol. 2015;402:113–9. https://doi.org/10.1016/j.mce.2014.11.029.
Camhi SM, Bray GA, Bouchard C, Greenway FL, Johnson WD, Newton RL, et al. The relationship of waist circumference and BMI to visceral, subcutaneous, and total body fat: sex and race differences. Obesity (Silver Spring). 2011;19(2):402–8. https://doi.org/10.1038/oby.2010.248.
Lyon CJ, Law RE, Hsueh WA. Minireview: adiposity, inflammation, and atherogenesis. Endocrinology. 2003;144(6):2195–200. https://doi.org/10.1210/en.2003-0285.
Gerdts E, Izzo R, Mancusi C, Losi MA, Manzi MV, Canciello G, et al. Left ventricular hypertrophy offsets the sex difference in cardiovascular risk (the Campania Salute Network). Int J Cardiol. 2018;258:257–61. https://doi.org/10.1016/j.ijcard.2017.12.086.
Bell V, McCabe EL, Larson MG, Rong J, Merz AA, Osypiuk E, et al. Relations between aortic stiffness and left ventricular mechanical function in the community. J Am Heart Assoc. 2017. https://doi.org/10.1161/JAHA.116.004903.
Blomstrand P, Sjoblom P, Nilsson M, Wijkman M, Engvall M, Lanne T, et al. Overweight and obesity impair left ventricular systolic function as measured by left ventricular ejection fraction and global longitudinal strain. Cardiovasc Diabetol. 2018;17(1):113. https://doi.org/10.1186/s12933-018-0756-2.
Lizcano F, Guzman G. Estrogen deficiency and the origin of obesity during menopause. Biomed Res Int. 2014;2014:757461. https://doi.org/10.1155/2014/757461.
Varlamov O, Bethea CL, Roberts CT Jr. Sex-specific differences in lipid and glucose metabolism. Front Endocrinol (Lausanne). 2014;5:241. https://doi.org/10.3389/fendo.2014.00241.
Peterson LR, Gropler RJ. Radionuclide imaging of myocardial metabolism. Circ Cardiovasc Imaging. 2010;3(2):211–22. https://doi.org/10.1161/CIRCIMAGING.109.860593.
Peterson LR, Herrero P, Coggan AR, Kisrieva-Ware Z, Saeed I, Dence C, et al. Type 2 diabetes, obesity, and sex difference affect the fate of glucose in the human heart. Am J Physiol Heart Circ Physiol. 2015;308(12):H1510–6. https://doi.org/10.1152/ajpheart.00722.2014.
Acknowledgements
We thank Hilde Jacobsen (staff engineer), Marina V. Kokorina (MD), Britt Gjellefall (RN), Synnøve Ygre Hauge (RN) and Liv Himle (RN) for technical assistance with data collection, registration, and participant management.
Funding
Open Access funding provided by University of Bergen.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The FATCOR study was funded by a grant from the Western Norwegian Regional Health Authorities [Grant number 911402]. The echocardiograph used in FATCOR was donated by the Grieg Foundation. The funding sources did not have any role in study design, in the collection, design and interpretation of data, in the writing of the report, or in the decision to submit the paper for publication.
Conflicts of interest
The authors have no conflicts of interest to disclose.
Ethics approval
The study was approved by Regional Ethics Committee number 17173 and performed in accordance with the 1964 Helsinki declaration and its later amendments.
Author contributions
EG conceptualized the current study. EG, HM, HH and SS acquired the data, and NP and SS analyzed strain-echocardiography. EG and NP interpreted the data and drafted the article. EG, NP, SS, HM, KM and HH critically reviewed the article and approved the final submission.
Data availability
The FATCOR file is currently being used in PhD projects and is not available for external researchers.
Additional information
All authors take responsibility for all aspects of the reliability and freedom from bias of the data presented and their discussed interpretation.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Pristaj, N., Saeed, S., Midtbø, H. et al. Covariables of Myocardial Function in Women and Men with Increased Body Mass Index. High Blood Press Cardiovasc Prev 27, 579–586 (2020). https://doi.org/10.1007/s40292-020-00418-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-020-00418-6