Abstract
Objectives
This systematic review aimed to quantify differences in loneliness levels between autistic and neurotypical samples and investigate the association between loneliness and mental health in autistic individuals.
Methods
Three meta-analyses were conducted. Studies were methodologically appraised using established tools.
Results
Overall, 39 studies were included. The majority of these achieved moderate methodological quality ratings. The primary meta-analysis (N = 23) found autistic samples reported higher loneliness compared with neurotypical samples (Hedges’ g = .89). The meta-analyses on the associations between loneliness and anxiety (N = 14) and depression (N = 11) in autistic samples found significant pooled correlations (r = .29 and r = .48, respectively).
Conclusions
This review highlights numerous limitations within current autism and loneliness research. Nevertheless, loneliness in autism merits targeted clinical and research attention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Loneliness has been conceptualised as either a uni- or a multi-dimensional construct (Heinrich & Gullone, 2006), but can broadly be defined as ‘A subjective unpleasant or distressing feeling of a lack of connection to other people, along with a desire for more, or more satisfying, social relationships.’ (Badcock et al., 2022). Within a multidimensional approach, ‘social loneliness’ indicates the recognised shortage of desired social relationships with accompanying feelings of exclusion and boredom, whereas ‘emotional loneliness’ indicates the absence of emotional connection/attachment and a sense of sadness and emptiness (DiTommaso & Spinner, 1997; Weiss, 1973). Importantly, loneliness is distinct from — though may be related to — objective social isolation, i.e. those who have objectively small social networks may not feel lonely, and likewise, loneliness can be felt by those with a seemingly large social network (Hawkley & Cacioppo, 2010). The experience of loneliness is thought to drive the formation and maintenance of relationships necessary for the survival of the human species, therefore acting as a motivator of social connection (Cacioppo et al., 2006).
Occasional feelings of loneliness are commonplace, with reports of between 10 and 80% of people in the general population experiencing loneliness at least sometimes (Beutel et al., 2017). Rates of loneliness are unevenly distributed across the life-course with peaks in prevalence often found in both older and younger adults (Hawkley et al., 2020; Shovestul et al., 2020). Some research has delineated ‘chronic loneliness’ (i.e. feeling lonely for at least 2 years; Martín-María et al., 2020; Peplau & Perlman, 1982) and ‘pathological loneliness’ (i.e. increased distress resulting from loneliness; Tiwari, 2013). Research demonstrates between 2 and 38% of the general population in the UK may feel lonely ‘most’ or ‘all of the time’ and may feel moderately to severely distressed by loneliness (Victor & Yang, 2012).
Loneliness and Mental Health
Loneliness is not a mental health condition; therefore, estimating the prevalence of — and threshold for — clinically relevant loneliness has been challenging in both research and clinical practice. Persistent and/or distressing feelings of loneliness can negatively impact on quality of life and wellbeing. A recent overview of 40 systematic reviews pertaining to the public health consequences of loneliness and social isolation found a consistent association with worse mental health outcomes, including depression and anxiety (Leigh-Hunt et al., 2017). Feelings of loneliness have also been found to be more prevalent among those with mental illnesses such as psychosis (Badcock et al., 2020). The association between loneliness and depressive symptoms has been shown to be moderate-large across the lifespan (r = 0.50–0.63; Erzen & Çikrikci, 2018; Matthews et al., 2016; Richardson et al., 2017). Similarly, the association between loneliness and anxiety has been found to be moderate-large in children and adult samples (r = 0.41–0.67; Beutel et al., 2017; Danneel et al., 2019; Richardson et al., 2017).
Loneliness in ASD
Individuals with autism spectrum disorder (ASD) may be at an increased risk of having fewer social relationships (Milton & Sims, 2016). This lifelong neurodevelopmental condition affects approximately 1% of the global population (Zeidan et al., 2022), and is characterised by difficulties in social communication and interaction, and engagement in restricted, repetitive behaviours or interests (American Psychiatric Association; APA, 2013). The characterisations of autism itself, as well as comparisons between autisticFootnote 1 and neurotypical (non-autistic) samples, may have maintained a narrative that autistic individuals are content in being alone; indeed, autistic individuals were historically considered to have ‘a powerful desire for aloneness’ (Kanner, 1943, p.249). Autism diagnostic criteria emphasise individuals’ deficits in social skills and interaction, including the lack of social-emotional reciprocity and a failure to develop developmentally appropriate peer relationships (APA, 2013). In line with the social motivation theory of autism, some researchers have posited that autistic individuals have less desire for — and may derive less pleasure from — social interactions, which subsequently decreases the likelihood of successful relationship development and maintenance (Chevallier et al., 2012). Research suggests autistic people have fewer, or no friendships in comparison to neurotypical peers (Orsmond et al., 2004; Shattuck et al., 2011) and in both child and adult samples, friendships have been reported to be of lower quality, result in less enjoyment and be defined in terms of social proximity rather than emotional connectedness (Baron-Cohen et al., 2001; Bauminger et al., 2004; Whitehouse et al., 2009). Nevertheless, research demonstrates that autistic individuals not only desire social interaction but may experience loneliness to a greater degree without it, compared to neurotypical individuals. For example, Bauminger et al. (2003) found autistic adolescents reported increased feelings of both social and emotional loneliness compared to neurotypical peers. Much of the research on loneliness in autism pertains to children and adolescents, in line with broader autism research (Evans, 2013). However, studies within adult samples have also reported the occurrence of loneliness among autistic adults (Hickey et al., 2018; Mazurek, 2014) and suggest that this is higher than neurotypical adults (Sundberg, 2018). However, evidence for increased loneliness in autistic compared to neurotypical samples is not ubiquitous in the literature, e.g. Chamberlain et al. (2007) and Bottema-Beutel et al. (2019) did not find any significant differences in loneliness levels between autistic and neurotypical children. It is notable that these studies had small sample sizes (17–21 participants per group) which may have compromised statistical power (Cohen, 1992).
Loneliness may be understood, experienced and expressed differently in autistic individuals compared with neurotypical individuals (Bauminger & Kasari, 2001). Moreover, the current methods used for measuring loneliness may be unsuitable for autistic individuals. In a study of 7–12 year olds, an experimental approach-avoidance task demonstrated autistic children showed an implicit desire for social interaction which was not captured in explicit questionnaire responses (Deckers et al., 2014). In their study of loneliness in 8–14-year-old high-functioning autistic children, Bauminger and Kasari (2000) found neurotypical children defined and understood loneliness as being alone with accompanying feelings of sadness, whereas the majority of autistic children defined loneliness as being alone without attributing an affective component.
There are several important factors which may influence loneliness experiences in autistic individuals. Co-occurring intellectual disability (ID) is prevalent in those diagnosed with autism, with reported rates between 30 and 70% (Thurm et al., 2019). Those with higher intellectual functioning may have greater self-awareness and awareness of social isolation (Volkmar et al., 2005), increasing susceptibility to loneliness (Bauminger & Kasari, 2001). Additionally, gender and age may influence loneliness experiences in autistic samples. For example, research has suggested autistic adolescent males have lower social motivation and friendship quality compared to autistic females (Sedgewick et al., 2016). There is also evidence of changes in the number and quality of friendships in autistic samples across the lifespan, with fewer friends in adolescence and adulthood compared to childhood (Howlin et al., 2004), which may also impact on feelings of loneliness (Kasari & Sterling, 2013).
Loneliness and Mental Health in ASD
Autistic populations experience a disproportionately high incidence and prevalence of anxiety and depression, in comparison to neurotypical populations (Joshi et al., 2013). A recent systematic review and meta-analysis of 30 studies measuring anxiety and 29 studies measuring depression suggested a pooled estimate of current and lifetime prevalence of 27% and 42% for anxiety disorders, and 23% and 37% for depressive disorders in autistic adults, respectively (Hollocks et al., 2019). Similar rates of comorbid anxiety and depression are reported across child and adolescent autistic samples (Hudson et al., 2019; Vasa & Mazurek, 2015; Wigham et al., 2017), and higher rates are reported in females compared to males (Sedgewick et al., 2020).
Loneliness in autism may be especially important to investigate considering research has evidenced significant associations between loneliness and depression (Han et al., 2019; Hedley et al., 2018a, b) and anxiety (Schiltz et al., 2020) in autistic individuals. It is possible that risk, causal and maintaining mechanisms for both loneliness and mental health difficulties reflect the core socio-communicative differences inherent in ASD. Additionally, the bi-directional influence of loneliness and mental health difficulties is also important to consider (Nuyen et al., 2020), as negative feelings associated with loneliness, anxiety and/or depression may limit the opportunities to develop meaningful relationships with others, which in turn exacerbate such feelings, impede socio-communication and drive social withdrawal (Magnuson & Constantino, 2011).
Despite increasing recognition within the autism community that loneliness is experienced by autistic people (National Autistic Society, 2018), the occurrence and degree of loneliness in this population in comparison to neurotypical individuals have not been systematically reviewed or quantitatively synthesised. Understanding the prevalence of loneliness in autism could have important clinical implications, especially given the increasing provision of psychosocial interventions to reduce social isolation and enhance social functioning and integration of autistic individuals (Pallathra et al., 2019). The disproportionate prevalence of anxiety and depression in the autistic population, and the potential influencing role of loneliness, indicates synthesis of the current evidence is imperative in directing future research in this emerging field.
The primary aim of this review is therefore to examine differences in loneliness levels between autistic and neurotypical samples. The secondary aim is to explore the association between loneliness and anxiety and depression in autistic individuals. To address these aims, three meta-analyses were employed to evaluate the following questions: (1) Is there a difference in loneliness levels between autistic and neurotypical individuals? (2) What is the strength of association between loneliness and anxiety among autistic people? (3) What is the strength of association between loneliness and depression among autistic people?
Method
Search Strategy
As is recommended by the Centre for Reviews and Dissemination (CRD, 2009), this review was undertaken following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Liberati et al., 2009). A protocol was published on the PROSPERO database prior to this review’s formal commencement.Footnote 2 Four bibliographic electronic databases (Scopus, PsycINFO, MEDLINE and ProQuest Dissertations and Theses) were searched from their inception until 01st September 2021. Forward and backward citation searches were conducted, as well as manual searching of the reference lists of included articles and relevant reviews (see Table 1 for a search syntax example).
Eligibility Criteria
Table 2 lists the eligibility criteria specific to the primary review and meta-analysis. Inclusion and exclusion criteria for the second review were identical to those in the first review with the following exceptions: studies did not need to include a neurotypical comparison group or to report loneliness levels; however, they must have measured anxiety or depression via a symptom severity questionnaire.
Screening
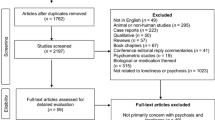
The search yielded 906 articles following deduplication. Study titles and abstracts were screened for relevance and those considered likely to meet selection criteria were reviewed in full (n = 83). Some studies were deemed to include overlapping participant samples,Footnote 3 which resulted in three being excluded from inclusion in this review. Full-text review excluded 44 articles, resulting in 39 studies (38 unique cohorts) included in the final reviews. Figure 1 summarises the selection process. Note. n, number; SR, Systematic Review; MA, Meta-Analysis. *The corresponding author of this study (Pak, 2019) was unable to provide the necessary information for inclusion in the review. Several studies were included in more than one review.
Data Extraction
As is recommended for systematic reviews, a data extraction tool was developed a priori and amended following piloting on four randomly selected included studies (Boland et al., 2014). Data were extracted verbatim onto an excel spreadsheet to minimise transcription errors. This included information on study characteristics (i.e. authors, date, publication status, country, objectives and population), sample characteristics (i.e. sample size, age, gender, ethnicity and IQ) and study results (i.e. procedures for ascertaining autism diagnosis, loneliness and anxiety or depression measures, key findings and statistical data). Where relevant data were not reported, authors were contacted via email. Data extracted for the primary meta-analysis included differences between loneliness rates (%) or levels (means; including F, t or Z statistics) between autistic and neurotypical samples. If this was not reported, sample sizes, loneliness mean scores and standard deviations were extracted to allow an effect size to be calculated. For the secondary meta-analyses, correlation values (r) or t statistics were extracted from studies. Studies were synthesised narratively where appropriate statistical data were not reported for inclusion in the meta-analyses.
Quality Assessment
Study quality was appraised using the Effective Public Health Practice Project (EPHPP) Tool for Quantitative Studies (Thomas et al., 2004), which was adapted for use within this review. The EPHPP has established content and construct validity (Thomas et al., 2004), fair inter-rater agreement (Cohen’s kappa = 0.60) for individual domains and excellent final rating agreement (Intra-class correlation coefficient = 0.77; Armijo-Olivo et al., 2012). This tool includes the essential criteria for methodological quality appraisal (CRD, 2009) and aligns with the recommended reporting of observational studies in epidemiology (Vandenbroucke et al., 2007). Additional criteria were included from the quality evaluation grid developed by Glod et al. (2015) which tailored methodological appraisal for studies including autistic samples. Criteria included as follows: how ASD diagnosis was confirmed for the study, whether cognitive functioning was assessed and reported and whether the measures used were validated for ASD populations.
Overall, studies were rated across seven domains: selection bias, study design, potential confounders (for studies including an NT comparison group), data collection (validity and reliability of measures used), management of participant drop-out/missing data, ASD diagnosis confirmation and cognitive functioning. In line with the EPHPP tool, criteria were rated as follows: Strong, Moderate or Weak. The overall quality of studies consisted of a rating of ‘Strong’ if no weak ratings were present, ‘Moderate’ if one weak rating was present and ‘Weak' if two or more weak ratings were present. It was decided a priori that no studies would be excluded from the review or meta-analysis based on weak global ratings. Due to the nature of this review including studies pertaining to different research questions, an additional ‘Not Applicable’ option was added to criteria (see supplementary table 1 for details on how component ratings were assigned to studies).
All studies were quality appraised by the first author, with a subset (12 papers; 31%) appraised by an independent reviewer. Agreement in component and overall ratings was evaluated using weighted Cohen’s KappaFootnote 4 (Schuck, 2004), with any disagreements resolved following discussion. Inter-rater reliability before consensus ranged between ‘fair’ and ‘very good’ (see supplementary table 2 for agreement statistics).
Meta-analytic Strategy
Meta-analyses were conducted using Comprehensive Meta-Analysis (CMA-Version 3; Borenstein et al., 2013). Random effects models were employed to account for expected within-study and between-study variance in true effect size estimates (Borenstein et al., 2010). For the primary meta-analysis, Hedges g was selected as the effect size for standardised mean difference due to its increased (weighted) accuracy when used with small sample sizes (n < 20) compared to Cohen’s d (Ellis, 2010). For the secondary meta-analyses, correlation coefficients (r) were selected as the effect size due to being easily interpretable and due to their inclusion in prior meta-analyses of associations between loneliness and mental health in neurotypical samples (Erzen & Çikrikci, 2018). Correlational statistics were transformed into Fisher’s Z scores during meta-analytic computations to account for possible skewed data distributions (Cox, 2008). Effect size magnitudes were interpreted according to Cohen (1992), i.e. small, medium and large effect size estimates of 0.10, 0.30 and 0.50 for r and 0.2, 0.5 and 0.8 for Hedges’ g, respectively.
Heterogeneity
Effect size variance between studies was assessed using the Cochran Q and I2 statistics. A significant Q statistic indicates that statistical heterogeneity is present. An adjusted alpha level of 0.10 was used due to the low power of this statistical test when few studies are analysed (Israel & Richter, 2011). The I2 statistic was used to quantify the proportion of variance across studies that was due to true heterogeneity rather than chance, whereby 25%, 50% and 75% indicate low, moderate and high heterogeneity respectively (Higgins et al., 2003).
Moderator Analysis
To investigate sources of heterogeneity, moderator analyses (including subgroup analysis for categorical variables and meta-regression for continuous variables) were planned (Borenstein et al., 2010). This included assessing the influence of age, gender, population (child or adult), presence of intellectual disability (ID), publication status (given the existence of larger effects being found in published as compared with unpublished studies; Boland et al., 2014) and the methodological quality of studies (Ioannidis, 2008). In line with previous systematic reviews and meta-analyses in autistic populations, the type of outcome measures used and the ASD diagnostic procedures reported (i.e. the diagnostic tools and procedures used to confirm autism) were also planned to be analysed as potential moderating variablesFootnote 5 (Hollocks et al., 2019; Spain et al., 2018). For subgroup analyses, summary effects for each group were computed and compared through a random effects approach to allow the total variance to be investigated with respect to within- and between-subgroup means. Meta-regression allowed calculation of the relationship between continuous variables and variation in effect-sizes (Israel & Richter, 2011).
Where multiple outcome measures were reported, the most comprehensive construct and/or reliable measure was selected for meta-analytic computations, due to the reported invalidity of effect size estimates that may occur through averaging effect-sizes (Park & Beretvas, 2019). Where studies provided both self- and other-reported measures (e.g. child and parent), self-reported data were included in meta-analyses. Of note, gender could not be investigated via subgroup analyses due to fewer than three studies providing outcome data separately for males/females; Card, 2015). Subgroup analysis based on ID could not be conducted due to insufficient studies including participants with ID.
Publication Bias
Publication bias was mitigated through inclusion of unpublished studies and use of subgroup analyses based on publication status. Egger et al.’s (1997) regression test was also conducted, along with fail-safe analysis to quantify the number of missing studies that would be required to invalidate a significant result (the threshold of which was met if N > 5 k + 10, where k is the number of included studies; Rosenthal, 1979). A funnel plot provided graphical representation of the assessment of each study’s precision (i.e. standard error) plotted against its effect-size, whereby asymmetrical patterns of effect-sizes around the mean effect-size indicate publication bias (Sterne & Egger, 2005). Finally, trim and fill methods were employed to account for missing studies and provided an unbiased effect size estimate (Duval & Tweedie, 2000). The significance level of these publication tests was set to 10% due to their low power (Lin & Chu, 2018).
Results
Studies retrieved for the primary review (differences in loneliness levels between ASD and NT samples; N = 24) and secondary review (associations between loneliness and anxiety; N = 16, associations between loneliness and depression; N = 14) are described separately in the summary tables, narrative syntheses and meta-analyses.
Loneliness Levels Between ASD and NT Samples
Study and Participant Characteristics
As can be seen in Table 3, of the 24 studies with unique cohorts included in this review, 23 utilised a cross-sectional design and one (Chiang, 2003) employed a pre-post experimental design (the baseline cross-sectional data were used in this review). All studies apart from one (Schalbroeck et al., 2021) provided appropriate data for inclusion in the meta-analysis. Studies were published between 2000 and 2021 and were conducted across 11 different countries, with the majority conducted in America (N = 11). Most studies used child and/or adolescent populations (N = 15).
Collectively, studies included 2944 participants (ASD = 1251; NT = 1693); sample sizes varied from 12 to 373 and ages ranged from 7 to 80 years. Of those that reported the ethnicity of the included sample (N = 10), the most represented ethnicity was White/Caucasian. Males were disproportionately represented in the ASD samples in 15 studies and in the NT sample in one study; gender distributions were equal in six studies and unreported in two.
Outcomes
Quality appraisal of each study is reported in supplementary material 3. Eleven different self-report loneliness measures were used across the 24 studies, the most frequently used (N = 5) was the Children’s Loneliness Scale (CLS; Asher et al., 1984). Of the 24 studies, 21 showed significantly higher average loneliness scores in the ASD sample compared to the NT sample. The remaining three reported no significant differences between groups, although all displayed a trend towards higher loneliness scores in the ASD group.
Four studies reported loneliness prevalence according to predetermined cut-off rates (Bauminger & Kasari, 2000; Bossaert et al., 2012; Chang et al., 2019; Lasgaard et al., 2010), of which three statistically compared rates between ASD and NT samples. Results showed ASD samples reported significantly higher levels of loneliness (i.e. reported feeling a higher magnitude of loneliness or felt lonely more often) (see Table 4 for an overview of study measures, outcomes and overall quality appraisal score).
Meta-Analysis
Figure 2 shows individual studies’ mean effect sizes and the pooled mean effect size. As predicted, autistic samples reported significantly higher loneliness than NT samples, with a large weighted pooled effect (Hedges’ g = 0.89; 95% CI [0.76, 1.02]; Z = 13.66, p < 0.001). Effect sizes ranged between g = 0.18 and 1.58. Two studies (Deckers et al., 2017; Nomura et al., 2012) included differing age groups. As the subgroups were all aged < 18, these were combined within each study for the purpose of meta-analytic computations at the study-level.
Heterogeneity
Significant heterogeneity was identified Q(22) = 41.12, p = 0.008. The I2 statistic indicated low-moderate heterogeneity with 46.50% of the dispersion between studies estimated to be real differences in the study effects. Heterogeneity was explored through categorical moderator analyses and meta-regression and outlined in Table 5. Across studies, 11 unique loneliness measures were used, with only one (the CLS; Asher et al., 1984) being used in enough studies to warrant sub-group analyses; the moderator analysis, therefore, investigated CLS against the other measures used. An insufficient number of studies (N = 3) received ‘strong’ ratings of overall methodological quality to enable them to occupy a separate subgroup, based on a priori criteria (Card, 2015). Therefore, subgroup analyses were conducted on studies appraised as methodologically ‘moderate-strong’ (N = 13) or ‘weak’ (N = 10). Only one moderator was evidenced to significantly explain between-group heterogeneity; studies that reported using gold-standard methods (i.e. using ADOS and/or ADI) to confirm ASD diagnosis of included participants (N = 5) attained a significantly higher pooled effect size than studies that did not. In line with the moderator analysis that investigated whether loneliness prevalence differed according to population (i.e. child or adult), meta-regression analysis showed age was not a significant moderator of effect-size across the 21 studies that provided relevant statistical information on participant ages (Q(1) = 0.00, b = 0.00, p = 0.98, 95% CI [− 0.02, 0.02], Z = 0.03).
Publication Bias
The funnel plot in Fig. 3 shows some asymmetry of study effect sizes around the effect size mean, with three studies falling outside of the 95% confidence limits. Trim and fill analysis corrected for asymmetry by imputing 6 studies to the left of the mean; however, this did not significantly alter the overall effect (t(21) = 2.34, p = 0.03). Moreover, fail-safe analysis indicated that 2116 missing studies with a mean effect of zero would be required to nullify the overall effect, exceeding the fail-safe threshold of k = 125. Taken together, these findings suggest no evidence of publication bias in this meta-analysis.
Loneliness and Mental Health in ASD
The results outlined below relate to the second review pertaining to studies reporting associations between loneliness and anxiety and/or depression within autistic samples.
Study and Participant Characteristics
Table 6 outlines the characteristics of each study. Of the 21 studies with unique cohorts included in the second review, seven measured anxiety only, five depression only and nine measured both anxiety and depression. Overall, 14 utilised a cross-sectional design and seven employed a longitudinal or pre-post experimental design, for which baseline cross-sectional data were extracted. Of the 16 studies measuring anxiety, 14 provided appropriate data for inclusion in the meta-analysis (N = 1224) and 11 out of 14 studies were included in the loneliness and depression meta-analysis (N = 980).
Studies were published between 2009 and 2021 and were conducted across five different countries, with the majority conducted in America (N = 13). Most studies were conducted using child samples (N = 11). Collectively, studies included 1752 participants; sample sizes varied from 18 to 220 participants and ages ranged from 7 to 80 years. In the 14 studies that reported sample ethnicity, the most represented ethnicity was White/Caucasian.
Outcomes
Quality appraisal of each study is reported in supplementary material 4. Eight different self-report loneliness measures were used across the 21 studies, the most frequently used were the Children’s Loneliness Scale (CLS; Asher et al., 1984) and the UCLA Loneliness Scale-8 (ULS-8; Hays & Dimatteo, 1987), both used in five studies. Thirteen different anxiety measures and 10 depression measures were used across studies; the most common were the Multidimensional Anxiety Scale for Children (MASC; March et al., 1997) and the Patient Health Questionnaire-9 (PHQ-9; Kroenke et al., 2001), used in three and four studies respectively. Two studies (Jackson et al., 2018; Wendler, 2019) did not report appropriate anxiety or depression subscale scores for inclusion in meta-analytic computations; however, they both reported at least one positive correlation between measures of emotional distress and loneliness. Two studies recruited participants from an overlapping source (Ee et al., 2019; Hedley et al., 2018a) resulting in only the latter being included in the depression meta-analysis (see Table 7 for an overview of study measures, outcomes and overall quality appraisal score. Where multiple measures and/or outcomes were reported, those in bold were used in the meta-analyses).
Meta-Analyses
Anxiety
As can be seen in Fig. 4, and in line with expectations, there was a significant positive association between mean loneliness scores and mean anxiety scores across most studies, with a low-medium pooled effect size (r = 0.29; 95% CI [0.15, 0.41]; Z = 4.09, p < 0.001). Effect sizes ranged between r = − 0.17 and r = 0.59. Of note, one study found a significant negative correlation between loneliness and anxiety (La Buissonniere Ariza et al., 2021). Significant heterogeneity was identified between studies Q(13) = 57.86, p < 0.001. The I2 statistic indicated high heterogeneity, with 77.53% of the dispersion between studies suggested to be due to real differences in the study effects. The relatively small number of studies in the secondary meta-analyses (< 20) precluded the use of comprehensive moderator analyses to investigate this heterogeneity (Rubio-Aparicio et al., 2017).
Publication Bias
Some asymmetry of study effect sizes around the effect size mean were apparent in the funnel plot in Fig. 5, with five studies falling outside of the 95% confidence limits. Trim and fill analysis corrected for asymmetry by imputing 6 studies to the left of the mean; however, this did not significantly alter the overall effect (t(12) = 1.13, p = 0.28). Fail-safe analysis indicated that 229 missing studies with a mean effect of zero would necessitate nullifying the overall effect, exceeding the fail-safe threshold of k = 80. Therefore, there is no evidence of publication bias in this meta-analysis.
Depression
Figure 6 outlines the significant positive relationship, with medium-large effect, between loneliness and depression (r = 0.48; 95% CI [0.40, 0.55]; Z = 10.6, p < 0.001). Effect sizes of studies ranged between r = 0.27 and r = 0.81, all in the expected direction. Again, there was evidence of significant heterogeneity identified between studies, (Q(10) = 19.72, p = 0.03). The I2 statistic indicated low-moderate heterogeneity, with 49.29% of the dispersion between studies suggested to be due to real study effect differences. This was not investigated further due to insufficient number of studies (Rubio-Aparicio et al., 2017).
Publication Bias
Some asymmetry of study effect sizes around the effect size mean was apparent in the funnel plot in Fig. 7, with three studies falling outside of the 95% confidence limits. However, no studies were imputed to correct for asymmetry based on trim and fill analysis and the regression test was non-significant (t(9) = 1.33, p = 0.22). Fail-safe analysis indicated that 660 missing studies with a mean effect of zero would necessitate nullifying the overall effect, exceeding the fail-safe threshold of k = 65. Overall, this demonstrated a lack of publication bias in this meta-analysis.
Discussion
Of the 23 studies included in the initial meta-analysis — investigating differences in loneliness levels between autistic and neurotypical samples, all found increased loneliness in autistic compared to neurotypical samples (this was a significant difference in 21 studies). The combined weighted effect size for this difference was large (Hedges’ g = 0.89). Eight of the 14 studies included in the meta-analysis of loneliness and anxiety found a significant correlation between loneliness and anxiety (seven in the expected direction) with an overall low-medium effect size (r = 0.29). In the final meta-analysis, a pooled medium-large effect (r = 0.48) was found for the association between loneliness and depression, with all 11 studies finding a significant positive correlation.
This is the first review to quantify differences in loneliness ratings between autistic and neurotypical samples. The consistent finding that autistic individuals report increased loneliness compared to neurotypical individuals contradicts literature that implies autistic individuals are compromised in their desire to seek social connection (Chevallier et al., 2012). It may be that autistic individuals’ ‘atypical’ social behaviour is not indicative of social disinterest (Jaswal & Akhtar, 2018), but manifests from reciprocal interactions within multiple ecological contexts (Bronfenbrenner, 1977). For example, autistic individuals are more susceptible to experiencing negative social interaction, e.g. through direct bullying and victimisation experiences and indirect broader societal stigmatisation (Schroeder et al., 2014). Such aversive experiences may lead to social withdrawal and fewer opportunities for social skill development and successful social experiences — yet the desire for more, or more meaningful, social connection remains.
The finding that loneliness was significantly positively correlated with both anxiety and depression is in line with previous research in neurotypical populations (Danneel et al., 2019; Erzen & Çikrikci, 2018; Leigh-Hunt et al., 2017). However, the cross-sectional nature of studies included in the meta-analyses precludes the interpretation of the direction of causality between loneliness, anxiety and depression. In the neurotypical population, the causal association between loneliness and mental health is considered to be bidirectional (Flett et al., 2016; Hawkley & Cacioppo, 2010), although evidence from longitudinal research has indicated loneliness being unidirectionally predictive of depressive symptoms over 1-year intervals (Cacioppo et al., 2010). Future research is required to establish whether loneliness shows a similar predictive effect in autistic individuals.
Significant between-study heterogeneity was found in all meta-analyses. Due to the number of studies included in meta-analytic computations, this could only be explored through moderator analysis in the first meta-analysis. In this analysis, only the use of gold standard diagnostic procedures, e.g. ADOS and ADI, for confirming autism diagnosis was found to significantly explain some between-study heterogeneity, suggesting that studies employing gold-standard procedures, with more accurate characterisation of autistic participants, had a greater effect size of mean differences in loneliness scores. The lack of significant findings for the other moderators is notable. For example, quality variance may not have significantly explained between-study heterogeneity due to the majority of included studies being considered as methodologically weak-moderate, with very few achieving strong ratings. Most studies utilised differing loneliness measures which were not validated in autistic samples which may explain why moderator analysis on loneliness measures did not explain significant heterogeneity. Likewise, most studies were conducted on younger samples (namely adolescents), potentially inflating the occurrence of type 2 errors for the moderator analyses on age and population type.
Strengths and Limitations of This Review
This review is strengthened by the employment of a comprehensive search strategy and the use of stringent eligibility criteria which fosters confidence that the included studies are representative of the current evidence base. The inclusion of unpublished literature reduces the likelihood of publication bias (Sterne & Egger, 2005); indeed, there was no evidence of publication bias within any of the meta-analyses. In addition, having independent ratings of methodological bias which resulted in ‘fair’ to ‘very good’ inter-rater agreement across all domains gives credibility to the reliability of the quality appraisal results.
Nevertheless, bias may have been inadvertently introduced during selection of studies due to this being conducted by only the first author, and a subsample was not cross-checked against the eligibility criteria by an independent reviewer (Boland et al., 2014). A further limitation is that due to the limited number of studies available for the meta-analyses on the association between loneliness and mental health, the influence of potential moderators in explaining the moderate-high between-study heterogeneity was not investigated. Additional data is therefore required to support further exploration of between-study heterogeneity.
Strengths and Limitations of Included Studies and Research Implications
There were numerous limitations in the literature included in this review. Measurement and reporting of participant characteristics across studies was inconsistent. Some studies did not report ethnicity data; in those that did, there appeared to be an over-representation of Caucasian participants from western cultures. As the meaning, experience and presentation of loneliness may vary across cultures, the findings of this review may not be generalisable to non-Caucasian participants (Barreto et al., 2021). Most participants were male, and although this aligns with gender ratios in autism research (Loomes et al., 2017), the findings of the review may not accurately capture the experiences of autistic females. Furthermore, the lack of subgroup analysis by gender within studies and the non-inclusion of individuals diagnosed with ID or reporting of IQ scores across studies, prevents confidence that these were appropriately controlled for in studies and precluded investigation of these as potential sources of heterogeneity.
Most studies adequately reported their recruitment procedures; however, the reporting of participant selection and attrition was particularly weak across studies. The rate of participation in the studies out of those selected was unclear, and rates of non-completers or missing data were not reported which may have biased findings, e.g. participants who were particularly lonely may be more motivated to take part and complete the studies. It is important to note that the findings of this review may be more generalisable to autistic individuals in the community, as opposed to clinical samples, given most samples were recruited from non-treatment seeking populations. Consistent with other systematic reviews on autistic individuals across the lifespan, most studies recruited child or adolescent samples (Spain 2018), which reduces the generalisability of these findings to adult samples; nevertheless, findings were consistent across age groups in this review.
The varied assessment and outcome measures used across studies may have resulted in different operationalisations of constructs (Offord & Kraemer, 2000). For example, the lack of gold standard procedures in confirming ASD diagnoses decreases the assurance of the diagnostic characterisation of most participants included in this review. Moreover, few studies reported whether the measures used to assess anxiety and depression had been validated within an autistic population, and participants exceeding clinical cut-off in studies were rarely reported, limiting the generalisation of findings in this review to participants with sub-clinical anxiety and/or depression.
Studies may also have introduced bias by not considering diagnostic overshadowing, i.e. the overlapping symptomatology of anxiety, depression and ASD inflating estimates of association (Rosen et al., 2018). This is further confounded by the greater co-occurrence of alexithymia in autistic individuals, characterised by difficulties in identifying and/or describing ones emotional experiences (Poquérusse et al., 2018), which can lead to inaccurate self-reporting on measures that have only been validated in neurotypical samples. Only one study reported accounting for diagnostic overshadowing (Maddox et al., 2017) and they found no significant correlation between anxiety and loneliness. It is notable that no studies reported accounting for possible alexithymia in participants. Using gold-standard procedures for confirming autism diagnoses such as the ADOS (Gotham et al., 2006) and ADI-R (Rutter et al., 2008) would enable better generalisation of study findings to diagnosed autistic individuals. The lack of current valid and reliable measures of mental health in autism is a recognised research gap, especially within adult populations (Brugha et al., 2015), although recent research is addressing this (Rodgers et al., 2020). Future studies would benefit from including validated mental health and alexithymia measures.
Importantly, despite autistic individuals scoring higher on loneliness measures compared to neurotypical individuals across included studies, we cannot infer that the magnitude of loneliness is severe and/or clinically relevant. Only three studies reported loneliness prevalence according to predetermined cut-off rates, which all reported autistic individuals had increased prevalence of ‘high’ loneliness. However, all studies used different loneliness measures and cut-off criteria, and achieved weak or moderate quality ratings, making comparisons between studies difficult. Future studies would benefit from including a standardised measure of loneliness duration, intensity, distress and frequency, in line with recommendations for measuring loneliness in the general population (Office for National Statistics, 2018). This will aid understanding of the clinical magnitude of loneliness felt by autistic individuals.
Moreover, this review cannot confirm that autistic individuals define, experience or express loneliness in the same way that neurotypical individuals may. Only three studies utilised loneliness measures which encapsulated multiple loneliness dimensions, precluding this from being meta-analytically explored as a potential moderator. Future studies would benefit from exploring differing dimensions of loneliness through utilisation of multidimensional measures of loneliness, especially when comparing autistic and neurotypical samples, as it may be that autistic individuals score higher than neurotypical individuals on a certain dimension of loneliness, rather than loneliness as a global construct. Future studies should also implement outcome measures that have been validated in autistic populations. Given the absence of validated loneliness measures in autistic people, it is necessary to ascertain how loneliness can be measured in autistic individuals, and whether loneliness measures are comparable between autistic and neurotypical samples (e.g. conducting measurement invariance studies). This should be done in collaboration with autistic people to more accurately capture their understanding and experiences (Cassidy et al., 2018).
Finally, longitudinal research could advance understanding of the mechanisms, course and predictors of loneliness, as well as factors which may mediate or moderate its association with anxiety and depression. This would help identify autistic individuals most vulnerable to experiencing loneliness and anxiety or depression, thus allowing early intervention to help mitigate the potential deleterious consequences.
Conclusions
Loneliness is an important yet overlooked construct in the socio-emotional experiences of autistic individuals. This is the first systematic review using meta-analytic procedures to compare loneliness levels between autistic and neurotypical samples. This is also the first review to quantify the associations between loneliness and anxiety and loneliness and depression in autistic individuals. Unexplained heterogeneity as well as the variance in study quality should be considered when interpreting these findings. Nevertheless, this review demonstrates consistently elevated loneliness scores reported by autistic individuals compared with neurotypical individuals, and significant correlations between loneliness scores and anxiety and depressive symptoms in autistic individuals, highlighting the importance of further research and awareness of loneliness in autism.
Notes
The term ‘autistic’ is used following research by Kenny et al. (2016) who found this term is preferred by the majority of UK autistic community respondents.
This review was registered on PROSPERO on 09.09.2020: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020205493
Where studies were thought to have overlapping samples, the first published study or those with most participants were selected (highlighted here in bold) for inclusion in summary tables e.g., (Bauminger et al., 2003; Bauminger et al., 2004); (Bohnert et al., 2019; Lieb & Bohnert, 2017; Ward et al., 2017). Of note, two studies with overlapping participants (Lin & Huang, 2019; Syu & Lin, 2018) were included in separate meta-analyses and have been presented separately in tables.
The Byrt (1996) criteria were used to interpret the weighted kappa values as follows: none < 0.01, poor = 0.01–0.20; slight = 0.21–0.40; fair = 0.41–0.60; good = 0.61–0.80; very good = 0.81–0.92 and excellent = 0.93–1.00. The weighted kappa allows consideration of the closeness of agreement between raters (i.e. a disagreement of ‘strong’ vs ‘moderate’ is closer than ‘strong’ vs ‘weak’) and may not corresponded to the % of exact agreement.
The following moderators were prespecified in the registered protocol: age, gender, population, presence of intellectual disability and the measures/procedures used to assess ASD and loneliness.
References
Achenbach, T. M., Dumenci, L., & Rescorla, L. A. (2003). Ratings of relations between DSM-IV diagnostic categories and items of the Adult Self-Report (ASR) and Adult Behavior Checklist (ABCL).
Achenbach, T. M., & Rescorla, L. A. (2001). Manual for the ASEBA school-age forms & profiles. Research Center for Children, Youth & Families. https://doi.org/10.1007/978-0-387-79948-3_1529
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders, fifth edition: DSM 5 (Fifth). American Psychiatric Publishing. http://www.psyweb.com/content/main-pages/dsm-5-fifth-edition-of-the-diagnostic-and-statistical-manual-of-mental-disorders
Armijo-Olivo, S., Stiles, C. R., Hagen, N. A., Biondo, P. D., & Cummings, G. G. (2012). Assessment of study quality for systematic reviews: A comparison of the Cochrane Collaboration Risk of Bias Tool and the Effective Public Health Practice Project Quality Assessment Tool: Methodological research. Journal of Evaluation in Clinical Practice, 18, 12–18. https://doi.org/10.1111/j.1365-2753.2010.01516.x
Asher, S., Hymel, S., & Renshaw, P. D. (1984). Loneliness in children. Child Development, 55(4), 1464. https://doi.org/10.2307/1130015
Asher, S., & Weeks, M. S. (2013). Loneliness and belongingness in the college years. In R. Coplan & J. Bowker (Eds.), The handbook of solitude (pp. 283–301). Wiley. https://doi.org/10.1002/9781118427378.ch16
Asher, S., & Wheeler, V. (1985). Children’s loneliness: A comparison of rejected and neglected peer status. Journal of Consulting and Clinical Psychology, 53(4), 500–505. https://psycnet.apa.org/buy/1985-30488-001
Badcock, J.C., Holt-Lunstad, J., Garcia, E., Bombaci, P., & Lim, M. H. (2022). Position statement: Addressing social isolation and loneliness and the power of human connection. Global Initiative on Loneliness and Connection. www.gilc.global
Badcock, Johanna C., Adery, L. H., & Park, S. (2020). Loneliness in psychosis: A practical review and critique for clinicians. Clinical Psychology: Science and Practice, 27(4). https://doi.org/10.1111/CPSP.12345
Baron-Cohen, S., Wheelwright, S., Skinner, R., Martin, J., & Clubley, E. (2001). The autism-spectrum quotient (AQ): Evidence from asperger syndrome/high-functioning autism, males and females, scientists and mathematicians. Journal of Autism and Developmental Disorders, 31(1), 5–17. https://doi.org/10.1023/A:1005653411471
Barreto, M., Victor, C., Hammond, C., Eccles, A., Richins, M. T., & Qualter, P. (2021). Loneliness around the world: Age, gender, and cultural differences in loneliness. Personality and Individual Differences, 169. https://doi.org/10.1016/j.paid.2020.110066
Bauminger, N. (1997). Loneliness, friendship and theory of mind in high-functioning children with autism. [ProQuest Information & Learning]. In ProQuest Dissertations and Theses (Vol. 57, Issues 10-A). http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc3&NEWS=N&AN=1997-95007-036
Bauminger, N., & Kasari, C. (2000). Loneliness and friendship in high-functioning children with autism. Child Development, 71(2), 447–456. https://doi.org/10.1111/1467-8624.00156
Bauminger, N., & Kasari, C. (2001). The experience of loneliness and friendship in autism: Theoretical and practical issues. In E. Schopler, N. Yirmiya, C. Shulman, & L. M. Marcus (Eds.), The research basis for autism intervention. (pp. 151–168). Kluwer Academic/Plenum Publishers. http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc3&NEWS=N&AN=2001-18055-010
Bauminger, N., Shulman, C., & Agam, G. (2003). Peer interaction and loneliness in high-functioning children with autism. Journal of Autism and Developmental Disorders, 33(5), 489–507. https://doi.org/10.1023/A:1025827427901
Bauminger, N., Shulman, C., & Agam, G. (2004). The link between perceptions of self and of social relationships in high-functioning children with autism. Journal of Developmental and Physical Disabilities, 16(2), 193–214. https://doi.org/10.1023/B:JODD.0000026616.24896.c8
Beck, A. T., Steer, R. A., & Brown, G. (1996). Manual for the Beck Depression Inventory-II. In Psychological Corporation. https://doi.org/10.1037/t00742-000
Beutel, M. E., Klein, E. M., Brähler, E., Reiner, I., Jünger, C., Michal, M., Wiltink, J., Wild, P. S., Münzel, T., Lackner, K. J., & Tibubos, A. N. (2017). Loneliness in the general population: Prevalence, determinants and relations to mental health. BMC Psychiatry, 17(1). https://doi.org/10.1186/s12888-017-1262-x
Bodden, D. H. M., Bögels, S. M., & Muris, P. (2009). The diagnostic utility of the Screen for Child Anxiety Related Emotional Disorders-71 (SCARED-71). Behaviour Research and Therapy, 47(5), 418–425. https://doi.org/10.1016/j.brat.2009.01.015
Boland, A., Cherry, M. G., & Dickson, R. (2014). Doing a systematic review : A student’s guide (1st ed.). SAGE Publications Ltd.
Borenstein, M, Hedges, L., Higgins, J., & Rothesteing, H. (2013). Comprehensive meta-analysis: Version 3. Biostat. https://www.meta-analysis.com
Borenstein, M., Hedges, L. V., Higgins, J. P. T., & Rothstein, H. R. (2010). A basic introduction to fixed-effect and random-effects models for meta-analysis. Research Synthesis Methods, 1(2), 97–111. https://doi.org/10.1002/jrsm.12
Bossaert, G., Colpin, H., Pijl, S. J., & Petry, K. (2012). Loneliness among students with special educational needs in mainstream seventh grade. Research in Developmental Disabilities, 33(6), 1888–1897. https://doi.org/10.1016/j.ridd.2012.05.010
Bottema-Beutel, K., Malloy, C., Cuda, J., Kim, S. Y., & MacEvoy, J. P. (2019). Friendship expectations may be similar for mental age-matched children with autism spectrum disorder and typically developing children. Journal of Autism and Developmental Disorders, 49(10), 4346–4354. https://doi.org/10.1007/s10803-019-04141-7
Bronfenbrenner, U. (1977). Toward an experimental ecology of human development. American Psychologist, 32(7), 513–531. http://content.apa.org/journals/amp/32/7/513
Brooks, W. T. (2014). Gender differences in social skills, peer relationships, and emotional correlates in adults with high functioning autism spectrum disorders. [The Ohio State University]. In ProQuest Dissertations and Theses (Vol. 76). https://search.proquest.com/dissertations-theses/gender-differences-social-skills-peer/docview/1699717702/se-2?accountid=13828
Brugha, T. S., Doos, L., Tempier, A., Einfeld, S., & Howlin, P. (2015). Outcome measures in intervention trials for adults with autism spectrum disorders; A systematic review of assessments of core autism features and associated emotional and behavioural problems. International Journal of Methods in Psychiatric Research, 24(2), 99–115. https://doi.org/10.1002/mpr.1466
Byrt, T. (1996). How good is that agreement? Epidemiology (Cambridge, Mass.), 7(5), 561. http://www.ncbi.nlm.nih.gov/pubmed/8862998
Cacioppo, J. T., Hawkley, L. C., Ernst, J. M., Burleson, M., Berntson, G. G., Nouriani, B., & Spiegel, D. (2006). Loneliness within a nomological net: An evolutionary perspective. Journal of Research in Personality, 40(6), 1054–1085. https://doi.org/10.1016/j.jrp.2005.11.007
Cacioppo, J. T., Hawkley, L. C., & Thisted, R. A. (2010). Perceived social isolation makes me sad: 5-year cross-lagged analyses of loneliness and depressive symptomatology in the chicago health, aging, and social relations study. Psychology and Aging, 25(2), 453–463. https://doi.org/10.1037/a0017216
Capriola-Hall, N. N., Brewe, A. M., Golt, J., & White, S. W. (2021). Anxiety and depression reduction as distal outcomes of a college transition readiness program for adults with autism. Journal of Autism and Developmental Disorders, 51(1), 298–306. https://doi.org/10.1007/s10803-020-04549-6
Card, N. (2015). Applied meta-analysis for social science research (S. Ahn, B. Bushman, & J. Worley (eds.); 1st ed.). Guilford Press. https://www.routledge.com/Applied-Meta-Analysis-for-Social-Science-Research/Card/p/book/9781462525003
Cassidy, S., Bradley, L., Shaw, R., & Baron-Cohen, S. (2018). Risk markers for suicidality in autistic adults. Molecular Autism, 9(1), 1–14. https://doi.org/10.1186/s13229-018-0226-4
Centre for Reviews and Dissemination. (2009). Systematic reviews: CRD’s guidance for undertaking reviews in health care. CRD, University of York.
Chamberlain, B., Kasari, C., & Rotheram-Fuller, E. (2007). Involvement or isolation? The social networks of children with autism in regular classrooms. Journal of Autism and Developmental Disorders, 37(2), 230–242. https://doi.org/10.1007/s10803-006-0164-4
Chang, Y.-C., Chen, C.-H., Huang, P.-C., & Lin, L.-Y. (2019). Understanding the characteristics of friendship quality, activity participation, and emotional well-being in Taiwanese adolescents with autism spectrum disorder. Scandinavian Journal of Occupational Therapy, 26(6), 452–462. https://doi.org/10.1080/11038128.2018.1449887
Che, H.-H., Lu, M.-L., Chen, H.-C., Chang, S.-W., & Lee, Y.-J. (2006). Validation of the Chinese version of the Beck Anxiety Inventory. Taipei Medical University, 10(4), 447–454. https://doi.org/10.6320/FJM.2006.10(4).05
Chevallier, C., Kohls, G., Troiani, V., Brodkin, E. S., & Schultz, R. T. (2012). The social motivation theory of autism. In Trends in Cognitive Sciences (Vol. 16, Issue 4, pp. 231–239). Elsevier Ltd. https://doi.org/10.1016/j.tics.2012.02.007
Chiang, I.-T. (2003). Effects of a therapeutic recreation intervention within a technology-based physical activity context on the social interaction of male youth with autism spectrum disorders [Indiana University]. In ProQuest Dissertations and Theses. https://search.proquest.com/dissertations-theses/effects-therapeutic-recreation-intervention/docview/305332304/se-2?accountid=13828
Clarke, G., Lewinsohn, P., Hyman, H., & Seeley, J. (1992). A self- and parent-report measure of adolescent depression: The Child Behavior Checklist Depression scale (CBCL-D). Behavioral Assessment, 14(3), 443–463. https://psycnet.apa.org/record/1993-24114-001
Cohen, J. (1992). A power primer. Psychological Bulletin, 112, 155–159. https://doi.org/10.1037/0033-2909.112.1.155
Connor, K. M., Davidson, J. R. T., Erik Churchill, L., Sherwood, A., Foa, E., & Weisler, R. H. (2000). Psychometric properties of the social phobia inventory (SPIN) New self- rating scale. British Journal of Psychiatry, 17(6), 379–386. https://doi.org/10.1192/bjp.176.4.379
Constantino, J. (2012). Social Responsiveness Scale, Second Edition (SRS-2). Western Psychological Services. https://www.pearsonclinical.co.uk/Psychology/ChildMentalHealth/ChildAutisticSpectrumDisorders/srs-2/social-responsiveness-scale-second-edition.aspx
Cox, N. J. (2008). Speaking Stata: Correlation with confidence, or Fisher’s z revisited. In Stata Journal (Vol. 8, Issue 3, pp. 413–439). DPC Nederland. https://doi.org/10.1177/1536867x0800800307
Craske, M., Wittchen, U., Bogels, S., Stein, M., Andrews, G., & Lebeu, R. (2013). Severity Measure for Generalized Anxiety Disorder-Adult.
Danneel, S., Bijttebier, P., Bastin, M., Colpin, H., Van Den Noortgate, W., Karla, •, Leeuwen, V., Verschueren, K., & Goossens, • Luc. (2019). Loneliness, social anxiety, and depressive symptoms in adolescence: Examining their distinctiveness through factor analysis. Journal of Child and Family Studies, 28, 1326–1336https://doi.org/10.1007/s10826-019-01354-3
De Gennaro, L. M. (2016). Loneliness in adolescents with high-functioning autism spectrum disorder. [ProQuest Information & Learning]. In Dissertation Abstracts International: Section B: The Sciences and Engineering (Vol. 77). http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc13&NEWS=N&AN=2016-37853-094
de Jong-Gierveld, J., & Kamphuls, F. (1985). The development of a rasch-type loneliness scale. Applied Psychological Measurement, 9(3), 289–299. https://doi.org/10.1177/014662168500900307
Deckers, A., Muris, P., & Roelofs, J. (2017). Being on your own or feeling lonely? Loneliness and other social variables in youths with autism spectrum disorders. Child Psychiatry and Human Development, 48(5), 828–839. https://doi.org/10.1007/s10578-016-0707-7
Deckers, A., Roelofs, J., Muris, P., & Rinck, M. (2014). Desire for social interaction in children with autism spectrum disorders. Reseach in Autism Spectrum Disorders, 8, 449–453. https://doi.org/10.1016/j.rasd.2013.12.019
DiTommaso, E., & Spinner, B. (1997). Social and emotional loneliness: A reexamination of weiss’ typology of loneliness. Personality and Individual Differences, 22(3), 417–427. https://doi.org/10.1016/S0191-8869(96)00204-8
Duval, S., & Tweedie, R. (2000). Trim and fill: A simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics, 56(2), 455–463. https://doi.org/10.1111/j.0006-341X.2000.00455.x
Ee, D., Hwang, Y. I., Reppermund, S., Srasuebkul, P., Trollor, J. N., Foley, K.-R., & Arnold, S. R. C. (2019). Loneliness in adults on the autism spectrum. https://Home.Liebertpub.Com/Aut. https://doi.org/10.1089/AUT.2018.0038
Egger, M., Smith, G. D., Schneider, M., & Minder, C. (1997). Bias in meta-analysis detected by a simple, graphical test. British Medical Journal, 315(7109), 629–634. https://doi.org/10.1136/bmj.315.7109.629
Ellis, P. D. (2010). The essential guide to effect sizes. Cambridge University Press. https://doi.org/10.1017/CBO9780511761676
Eriksson, J. M., Andersen, L. M., & Bejerot, S. (2013). RAADS-14 screen: Validity of a screening tool for autism spectrum disorder in an adult psychiatric population. Molecular Autism, 4, 49. https://doi.org/10.1186/2040-2392-4-49
Erzen, E., & Çikrikci, Ö. (2018). The effect of loneliness on depression: A meta-analysis. In International Journal of Social Psychiatry (Vol. 64, Issue 5, pp. 427–435). SAGE Publications Ltd. https://doi.org/10.1177/0020764018776349
Evans, B. (2013). How autism became autism: The radical transformation of a central concept of child development in Britain. In History of the Human Sciences (Vol. 26, Issue 3, pp. 3–31). SAGE Publications. https://doi.org/10.1177/0952695113484320
Flett, G. L., Goldstein, A. L., Pechenkov, I. G., Nepon, T., & Wekerle, C. (2016). Antecedents, correlates, and consequences of feeling like you don’t matter: Associations with maltreatment, loneliness, social anxiety, and the five-factor model. Personality and Individual Differences, 92, 52–56. https://doi.org/10.1016/j.paid.2015.12.014
Glod, M., Riby, D. M., Honey, E., & Rodgers, J. (2015). Psychological correlates of sensory processing patterns in individuals with autism spectrum disorder: A systematic review. Review Journal of Autism and Developmental Disorders, 2, 199–221. https://doi.org/10.1007/s40489-015-0047-8
Gotham, K., Risi, S., Pickles, A., & Lord, C. (2006). The Autism Diagnostic Observation Schedule (ADOS). In Journal of Autism and Developmental Disorders. Springer Nature. https://www.research.manchester.ac.uk/portal/en/publications/the-autism-diagnostic-observation-schedule-ados(31646979-0428-4614-b727-e0052e1497ed)/export.html
Han, G. T., Tomarken, A. J., & Gotham, K. O. (2019). Social and nonsocial reward moderate the relation between autism symptoms and loneliness in adults with ASD, depression, and controls. Autism Research, 12(6), 884–896. https://doi.org/10.1002/aur.2088
Hawkley, L. C., Buecker, S., Kaiser, T., & Luhmann, M. (2020). Loneliness from young adulthood to old age: Explaining age differences in loneliness: International Journal of Behavioral Development, 46(1). https://doi.org/10.1177/0165025420971048
Hawkley, L. C., & Cacioppo, J. T. (2010). Loneliness matters: A theoretical and empirical review of consequences and mechanisms. Annals of Behavioral Medicine, 40(2), 218–227. https://doi.org/10.1007/s12160-010-9210-8
Hays, R. D., & Dimatteo, M. R. (1987). A short-form measure of loneliness. Journal of Personality Assessment, 51(1), 69–81. https://doi.org/10.1207/s15327752jpa5101_6
Hedley, D., Uljarević, M., Foley, K.-R., Richdale, A., & Trollor, J. (2018a). Risk and protective factors underlying depression and suicidal ideation in autism spectrum disorder. Depression and Anxiety, 35(7), 648–657. https://doi.org/10.1002/da.22759
Hedley, D., Uljarević, M., Wilmot, M., Richdale, A., & Dissanayake, C. (2018b). Understanding depression and thoughts of self-harm in autism: A potential mechanism involving loneliness. Research in Autism Spectrum Disorders, 46, 1–7. https://doi.org/10.1016/j.rasd.2017.11.003
Heimberg, R. G., Horner, # K J, Juster, H. R., Safren, S. A., Brown, E. J., Schneier, F. R., & Liebowitz, M R. (1999). Psychometric properties of the Liebowitz Social Anxiety Scale. Psychological Medicine, 29, 199–212
Heinrich, L. M., & Gullone, E. (2006). The clinical significance of loneliness: A literature review. In Clinical Psychology Review (Vol. 26, Issue 6, pp. 695–718). Pergamon. https://doi.org/10.1016/j.cpr.2006.04.002
Hickey, A., Crabtree, J., & Stott, J. (2018). ‘Suddenly the first fifty years of my life made sense’: Experiences of older people with autism. Autism, 22(3), 357–367. https://doi.org/10.1177/1362361316680914
Higgins, J. P. T., Thompson, S. G., Deeks, J. J., & Altman, D. G. (2003). Measuring inconsistency in meta-analyses. In British Medical Journal (Vol. 327, Issue 7414, pp. 557–560). BMJ Publishing Group. https://doi.org/10.1136/bmj.327.7414.557
Hoekstra, R. A., Vinkhuyzen, A. A. E., Wheelwright, S., Bartels, M., Boomsma, D. I., Baron-Cohen, S., Posthuma, D., & Van Der Sluis, S. (2011). The construction and validation of an abridged version of the autism-spectrum quotient (AQ-short). Journal of Autism and Developmental Disorders, 41(5), 589–596. https://doi.org/10.1007/s10803-010-1073-0
Hollocks, M. J., Lerh, J. W., Magiati, I., Meiser-Stedman, R., & Brugha, T. S. (2019). Anxiety and depression in adults with autism spectrum disorder: A systematic review and meta-analysis. Psychological Medicine, 49(4), 559–572. https://doi.org/10.1017/S0033291718002283
Howlin, P., Goode, S., Hutton, J., & Rutter, M. (2004). Adult outcome for children with autism. Journal of Child Psychology and Psychiatry and Allied Disciplines, 45(2), 212–229. https://doi.org/10.1111/j.1469-7610.2004.00215.x
Hoza, B., Bukowski, W. M., & Beery, S. (2000). Assessing peer network and dyadic loneliness. Journal of Clinical Child and Adolescent Psychology, 29(1), 119–128. https://doi.org/10.1207/S15374424jccp2901_12
Hudson, C. C., Hall, L., & Harkness, K. L. (2019). Prevalence of depressive disorders in individuals with autism spectrum disorder: A meta-analysis. Journal of Abnormal Child Psychology, 47(1), 165–175. https://doi.org/10.1007/s10802-018-0402-1
Hughes, M. E., Waite, L. J., Hawkley, L. C., & Cacioppo, J. T. (2004). A short scale for measuring loneliness in large surveys: Results from two population-based studies. Research on Aging, 26(6), 655–672. https://doi.org/10.1177/0164027504268574
Hymas, R. (2021). Loneliness, social identity and mental health in autistic individuals. DClinPsy Thesis, University of Sheffield. https://etheses.whiterose.ac.uk/29522/
Ioannidis, J. P. A. (2008). Why most discovered true associations are inflated. Epidemiology, 19(5), 640–648. https://doi.org/10.1097/EDE.0b013e31818131e7
Israel, H., & Richter, R. R. (2011). A guide to understanding meta-analysis. Journal of Orthopaedic & Sports Physical Therapy, 496(7), 496–504. https://doi.org/10.2519/jospt.2011.3333
Jackson, S. L. J., Hart, L., Brown, J. T., & Volkmar, F. R. (2018). Brief report: Self-reported academic, social, and mental health experiences of post-secondary students with autism spectrum disorder. Journal of Autism and Developmental Disorders, 48(3), 643–650. https://doi.org/10.1007/s10803-017-3315-x
Jaswal, V. K., & Akhtar, N. (2018). Being vs. appearing socially uninterested: Challenging assumptions about social motivation in autism. Behavioral and Brain Sciences, 42, 1–84. https://doi.org/10.1017/S0140525X18001826
Joshi, G., Wozniak, J., Petty, C., Martelon, M. K., Fried, R., Bolfek, A., Kotte, A., Stevens, J., Furtak, S. L., Bourgeois, M., Caruso, J., Caron, A., & Biederman, J. (2013). Psychiatric comorbidity and functioning in a clinically referred population of adults with autism spectrum disorders: A comparative study. Journal of Autism and Developmental Disorders, 43(6), 1314–1325. https://doi.org/10.1007/s10803-012-1679-5
Kalyva, E. (2010). Multirater congruence on the social skills assessment of children with asperger syndrome: Self, mother, father, and teacher ratings. Journal of Autism and Developmental Disorders, 40(10), 1202–1208. https://doi.org/10.1007/s10803-010-0978-y
Kanner, L. (1943). Autistic disturbances of affective contact. Nervous Child, 2, 217–250. https://psycnet.apa.org/record/1943-03624-001
Kasari, C., & Sterling, L. (2013). Loneliness and social isolation in children with autism spectrum disorders. In The Handbook of Solitude (pp. 409–426). Wiley. https://doi.org/10.1002/9781118427378.ch23
Kaufman, A., & Kaufman, N. (2004). Kaufman Brief Intelligence Test, Second Edition (KBIT-2). Pearson. https://www.pearsonclinical.co.uk/Education/Assessments/GeneralAbility/KaufmanBriefIntelligenceTestSecondEdition(KBIT-2)/KaufmanBriefIntelligenceTestSecondEdition(KBIT-2).aspx
Kellogg, C., & Morton, N. (1999). Revised Beta Examination (Beta III). The Psychological Corporation. https://www.pearsonclinical.co.uk/Psychology/AdultCognitionNeuropsychologyandLanguage/AdultGeneralAbilities/BetaIII/BetaIII.aspx
Kenny, L., Hattersley, C., Molins, B., Buckley, C., Povey, C., & Pellicano, E. (2016). Which terms should be used to describe autism? Perspectives from the UK autism community. Autism, 20, 442–462. https://doi.org/10.1177/1362361315588200
Kopp, S., & Gillberg, C. (2011). The Autism Spectrum Screening Questionnaire (ASSQ)-Revised Extended Version (ASSQ-REV): An instrument for better capturing the autism phenotype in girls? A preliminary study involving 191 clinical cases and community controls. Research in Developmental Disabilities, 32(6), 2875–2888. https://doi.org/10.1016/j.ridd.2011.05.017
Kovacs, M. (1992). Children’s depression inventory manual. Multi-health Systems, Inc.
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Kroenke, K., Spitzer, R. L., Williams, J. B. W., & Löwe, B. (2009). An ultra-brief screening scale for anxiety and depression: The PHQ-4. Psychosomatics, 50(6), 613–621. https://doi.org/10.1176/appi.psy.50.6.613
La Buissonniere Ariza, V., Schneider, S. C., Cepeda, S. L., Wood, J. J., Kendall, P. C., Small, B. J., Wood, K. S., Kerns, C., Saxena, K., & Storch, E. A. (2021). Predictors of suicidal thoughts in children with autism spectrum disorder and anxiety or cbsessive-compulsive disorder: The unique contribution of externalizing behaviors. Child Psychiatry and Human Development, 1–14https://doi.org/10.1007/s10578-020-01114-1
La Greca, A. M., & Lopez, N. (1998). Social anxiety among adolescents: Linkages with peer relations and friendships. Journal of Abnormal Child Psychology, 26(2), 83–94. https://doi.org/10.1023/A:1022684520514
Lasgaard, M., Nielsen, A., Eriksen, M. E., & Goossens, L. (2010). Loneliness and social support in adolescent boys with autism spectrum disorders. Journal of Autism and Developmental Disorders, 40(2), 218–226. https://doi.org/10.1007/s10803-009-0851-z
Lasgaard, M. (2007). Reliability and validity of the Danish version of the UCLA loneliness scale. Personality and Individual Differences, 42(7), 1359–1366. https://doi.org/10.1016/j.paid.2006.10.013
Leigh-Hunt, N., Bagguley, D., Bash, K., Turner, V., Turnbull, S., Valtorta, N., & Caan, W. (2017). An overview of systematic reviews on the public health consequences of social isolation and loneliness. In Public Health (Vol. 152, pp. 157–171). Elsevier B.V. https://doi.org/10.1016/j.puhe.2017.07.035
Liberati, A., Altman, D. G., Tetzlaff, J., Mulrow, C., Gøtzsche, P. C., Ioannidis, J. P. A., Clarke, M., Devereaux, P. J., Kleijnen, J., & Moher, D. (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ (Clinical Research Ed.), 339https://doi.org/10.1136/BMJ.B2700
Lieb, R. W., & Bohnert, A. M. (2017). Relations between executive functions, social impairment, and friendship quality on adjustment among high functioning youth with autism spectrum disorder. Journal of Autism and Developmental Disorders, 47(9), 2861–2872. https://doi.org/10.1007/s10803-017-3205-2
Lin, L.-Y., & Huang, P.-C. (2019). Quality of life and its related factors for adults with autism spectrum disorder. Disability and Rehabilitation, 41(8), 896–903. https://doi.org/10.1080/09638288.2017.1414887
Lin, L., & Chu, H. (2018). Quantifying publication bias in meta-analysis. Biometrics, 74(3), 785. https://doi.org/10.1111/BIOM.12817
Locke, J., Ishijima, E. H., Kasari, C., & London, N. (2010). Loneliness, friendship quality and the social networks of adolescents with high-functioning autism in an inclusive school setting. Journal of Research in Special Educational Needs, 10(2), 74–81. https://doi.org/10.1111/j.1471-3802.2010.01148.x
Loomes, R., Hull, L., & Mandy, W. P. L. (2017). What is the male-to-female ratio in autism spectrum disorder? A systematic review and meta-analysis. In Journal of the American Academy of Child and Adolescent Psychiatry (Vol. 56, Issue 6, pp. 466–474). Elsevier Inc. https://doi.org/10.1016/j.jaac.2017.03.013
Lovibond, P. F., & Lovibond, S. H. (1995). The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behaviour Research and Therapy, 33, 335–343. https://doi.org/10.1016/0005-7967(94)00075-U
Maddox, B. B., Miyazaki, Y., & White, S. W. (2017). Long-term effects of CBT on social impairment in adolescents with ASD. Journal of Autism and Developmental Disorders, 47(12), 3872–3882. https://doi.org/10.1007/s10803-016-2779-4
Magnuson, K. M., & Constantino, J. N. (2011). Characterization of depression in children with autism spectrum disorders. In Journal of Developmental and Behavioral Pediatrics (Vol. 32, Issue 4, pp. 332–340). Lippincott Williams and Wilkins. https://doi.org/10.1097/DBP.0b013e318213f56c
Mahjouri, S. (2011). A cross-sectional analysis of social engagement, isolation and loneliness for children and adolescents with autism. [ProQuest Information & Learning]. In ProQuest Dissertations and Theses (Issue 11). https://search.proquest.com/dissertations-theses/cross-sectional-analysis-social-engagement/docview/1033014349/se-2?accountid=13828
March, J. S., Parker, J. D., Sullivan, K., Stallings, P., & Conners, C. K. (1997). The Multidimensional Anxiety Scale for Children (MASC): Factor structure, reliability, and validity. Journal of the American Academy of Child and Adolescent Psychiatry, 36(4), 554–565. https://doi.org/10.1097/00004583-199704000-00019
Marcoen, A., Goossens, L., & Caes, P. (1987). Lonelines in pre-through late adolescence: Exploring the contributions of a multidimensional approach. Journal of Youth and Adolescence, 16(6), 561–577. https://doi.org/10.1007/BF02138821
Martín-María, N., Caballero, F. F., Miret, M., Tyrovolas, S., Haro, J. M., Ayuso-Mateos, J. L., & Chatterji, S. (2020). Differential impact of transient and chronic loneliness on health status. A Longitudinal Study. Psychology and Health, 35(2), 177–195. https://doi.org/10.1080/08870446.2019.1632312
Matson, J. L., Rotatori, A. F., & Helsel, W. J. (1983). Development of a rating scale to measure social skills in children: The matson evaluation of social skills with youngsters (MESSY). Behaviour Research and Therapy, 21(4), 335–340. https://doi.org/10.1016/0005-7967(83)90001-3
Matthews, T., Danese, A., Wertz, J., Odgers, C. L., Ambler, A., Moffitt, T. E., & Arseneault, L. (2016). Social isolation, loneliness and depression in young adulthood: A behavioural genetic analysis. Social Psychiatry and Psychiatric Epidemiology, 51(3), 339–348. https://doi.org/10.1007/s00127-016-1178-7
Mazurek, M. O. (2014). Loneliness, friendship, and well-being in adults with autism spectrum disorders. Autism, 18(3), 223–232. https://doi.org/10.1177/1362361312474121
Merkler, E. E. (2007). The experience of isolation and loneliness in young adults with high-functioning autism. Dissertation Abstracts International: Section B: The Sciences and Engineering, 68(3-B), 1936. http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc5&NEWS=N&AN=2007-99018-265
Milton, D., & Sims, T. (2016). How is a sense of well-being and belonging constructed in the accounts of autistic adults? Disability & Society, 31, 520–534. https://doi.org/10.1080/09687599.2016.1186529
National Academy of Sciences. (2015). Prevalence of autism spectrum disorder: Mental disorders and disabilities among low-income children. https://www.ncbi.nlm.nih.gov/books/NBK332896/
National Autistic Society. (2018, April 25). Hidden crisis: autism and loneliness. https://www.autism.org.uk/get-involved/media-centre/news/2018-04-25-hidden-crisis-autism-and-loneliness.aspx
Nomura, K., Beppu, S., & Tsujii, M. (2012). Loneliness in children with high functioning pervasive developmental disorders. Japanese Journal of Special Education, 49(6), 645–656. https://doi.org/10.6033/tokkyou.49.645
Nuyen, J., Tuithof, M., de Graaf, R., van Dorsselaer, S., Kleinjan, M., & ten Have, M. (2020). The bidirectional relationship between loneliness and common mental disorders in adults: Findings from a longitudinal population-based cohort study. Social Psychiatry and Psychiatric Epidemiology, 55(10), 1297–1310. https://doi.org/10.1007/s00127-019-01778-8
Office for National Statistics. (2018, December 5). Recommended national indicators of loneliness. https://www.ons.gov.uk/peoplepopulationandcommunity/wellbeing/compendium/nationalmeasurementofloneliness/2018/recommendednationalindicatorsofloneliness
Offord, D. R., & Kraemer, H. C. (2000). Risk factors and prevention. Evidence-Based Mental Health, 3, 70–71. https://doi.org/10.1136/ebmh.3.3.70
Orsmond, G. I., Krauss, M. W., & Seltzer, M. M. (2004). Peer relationships and social and recreational activities among adolescents and adults with autism. In Journal of Autism and Developmental Disorders (Vol. 34, Issue 3, pp. 245–256). J Autism Dev Disord. https://doi.org/10.1023/B:JADD.0000029547.96610.df
Pak, E. P. (2019). Self-perceptions of friendship quality and loneliness predicting social adaptivity of children with HFASD [University of California, Los Angeles]. In ProQuest Dissertations and Theses. https://search.proquest.com/dissertations-theses/self-perceptions-friendship-quality-loneliness/docview/2301477854/se-2?accountid=13828
Pallathra, A. A., Cordero, L., Wong, K., & Brodkin, E. S. (2019). Psychosocial interventions targeting social functioning in adults on the autism spectrum: A literature review. Current Psychiatry Reports, 21(5), 1–11. https://doi.org/10.1007/s11920-019-0989-0
Park, S., & Beretvas, S. N. (2019). Synthesizing effects for multiple outcomes per study using robust variance estimation versus the three-level model. Behavior Research Methods, 51(1), 152–171. https://doi.org/10.3758/s13428-018-1156-y
Peplau, L., & Perlman, D. (1982). Loneliness: A sourcebook of current theory, research, and therapy. (L. Peplau & D. Perlman (eds.)). Wiley. https://trove.nla.gov.au/work/14222510
Poquérusse, J., Pastore, L., Dellantonio, S., & Esposito, G. (2018). Alexithymia and autism spectrum disorder: A complex relationship. Frontiers in Psychology, 9https://doi.org/10.3389/fpsyg.2018.01196
Radloff, L. S. (1977). The CES-D scale: A self-report depression scale for research in the general population. Applied Psychological Measurement, 1(3), 385–401. https://doi.org/10.1177/014662167700100306
Richardson, T., Elliott, P., & Roberts, R. (2017). Relationship between loneliness and mental health in students. Journal of Public Mental Health, 16(2), 48–54. https://doi.org/10.1108/JPMH-03-2016-0013
Rodgers, J., Farquhar, K., Mason, D., Brice, S., Wigham, S., Ingham, B., Freeston, M., & Parr, J. R. (2020). Development and initial evaluation of the anxiety scale for autism-adults. Autism in Adulthood, 2(1), 24–33. https://doi.org/10.1089/aut.2019.0044
Rosen, T. E., Mazefsky, C. A., Vasa, R. A., & Lerner, M. D. (2018). Co-occurring psychiatric conditions in autism spectrum disorder. In International Review of Psychiatry (Vol. 30, Issue 1, pp. 40–61). Taylor and Francis Ltd. https://doi.org/10.1080/09540261.2018.1450229
Rosenthal, R. (1979). The file drawer problem and tolerance for null results. Psychological Bulletin, 86(3), 638–641. https://doi.org/10.1037/0033-2909.86.3.638
Rubio-Aparicio, M., Sánchez-Meca, J., López-López, J. A., Botella, J., & Marín-Martínez, F. (2017). Analysis of categorical moderators in mixed-effects meta-analysis: Consequences of using pooled versus separate estimates of the residual between-studies variances. British Journal of Mathematical and Statistical Psychology, 70(3), 439–456. https://doi.org/10.1111/bmsp.12092
Russell, D. W. (1996). UCLA Loneliness Scale (Version 3): Reliability, validity, and factor structure. Journal of Personality Assessment, 66(1), 20–40. https://doi.org/10.1207/s15327752jpa6601_2
Russell, N. (2020). The association of sleep quality and loneliness with perceived physical and mental health status in autistic adults. Dissertation Abstracts International: Section B: The Sciences and Engineering, 82(8-B), No-Specified. http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc17&NEWS=N&AN=2021-27916-080
Rutter, M., LeCouteur, A., & Lord, A. (2008). Autism Diagnostic Interview – Revised (ADI-R). Western Psychological Services. https://www.carautismroadmap.org/individual-test-summaries-and-review-autism-diagnostic-interview-revised-adi-r/
Schalbroeck, R., van Velden, F. H. P., de Geus-Oei, L.-F., Yaqub, M., van Amelsvoort, T., Booij, J., & Selten, J.-P. (2021). Striatal dopamine synthesis capacity in autism spectrum disorder and its relation with social defeat: An [18F]-FDOPA PET/CT study. Translational Psychiatry, 11(1). https://doi.org/10.1038/s41398-020-01174-w
Schiltz, H. K., McVey, A. J., Dolan Wozniak, B., Haendel, A. D., Stanley, R., Arias, A., Gordon, N., & Van Hecke, A. V. (2020). The role of loneliness as a mediator between autism features and mental health among autistic young adults. Autism, 25(2), 545–555. https://doi.org/10.1177/1362361320967789
Schopler, E., Van Bourgondien, M., Wellman, G., & Love, S. (2010). Childhood Autism Rating Scale - Second Edition (CARS-2). Western Psychological Services. https://www.pearsonclinical.co.uk/Psychology/ChildMentalHealth/ChildAutisticSpectrumDisorders/ChildhoodAutismRatingScale-SecondEdition(CARS2)/ChildhoodAutismRatingScale-SecondEdition(CARS2).aspx
Schroeder, J. H., Cappadocia, M. C., Bebko, J. M., Pepler, D. J., & Weiss, J. A. (2014). Shedding light on a pervasive problem: A review of research on bullying experiences among children with autism spectrum disorders. Journal of Autism and Developmental Disorders, 44(7), 1520–1534. https://doi.org/10.1007/s10803-013-2011-8
Schuck, P. (2004). Assessing reproducibility for interval data in health-related quality of life questionnaires: Which coefficient should be used? Quality of Life Research, 13(3), 571–585. https://doi.org/10.1023/B:QURE.0000021318.92272.2a
Scott, F. J., Baron-Cohen, S., Bolton, P., & Brayne, C. (2002). The CAST (childhood asperger syndrome test): Preliminary development of a UK screen for mainstream primary-school-age children. Autism, 6(1), 9–31. https://doi.org/10.1177/1362361302006001003
Sedgewick, F., Hill, V., Yates, R., Pickering, L., & Pellicano, E. (2016). Gender differences in the social motivation and friendship experiences of autistic and non-autistic adolescents. Journal of Autism and Developmental Disorders, 46(4), 1297–1306. https://doi.org/10.1007/s10803-015-2669-1
Sedgewick, F., Leppanen, J., & Tchanturia, K. (2020). Gender differences in mental health prevalence in autism. Advances in Autism. https://doi.org/10.1108/AIA-01-2020-0007
Shattuck, P. T., Orsmond, G. I., Wagner, M., & Cooper, B. P. (2011). Participation in social activities among adolescents with an autism spectrum disorder. PLoS ONE, 6(11), e27176. https://doi.org/10.1371/journal.pone.0027176
Shiovitz-Ezra, S., & Ayalon, L. (2010). Situational versus chronic loneliness as risk factors for all-cause mortality. International Psychogeriatrics, 22(3), 455–462. https://doi.org/10.1017/S1041610209991426
Shovestul, B., Han, J., Germine, L., & Dodell-Feder, D. (2020). Risk factors for loneliness: The high relative importance of age versus other factors. PLOS ONE, 15(2). https://doi.org/10.1371/JOURNAL.PONE.0229087
Silverman, W. K., & Albano, A. M. (1996). The anxiety disorders interview schedule for children and parents- DSM-IV version. . Graywind. https://www.scirp.org/(S(351jmbntvnsjt1aadkposzje))/reference/ReferencesPapers.aspx?ReferenceID=720677
Spain, D., & Blainey, S. H. (2015). Group social skills interventions for adults with high-functioning autism spectrum disorders: A systematic review. Autism, 19(7), 874–886. https://doi.org/10.1177/1362361315587659
Spain, D., Sin, J., Linder, K. B., McMahon, J., & Happé, F. (2018). Social anxiety in autism spectrum disorder: A systematic review. Research in Autism Spectrum Disorders, 52, 51–68. https://doi.org/10.1016/J.RASD.2018.04.007
Spitzer, R. L., Kroenke, K., & Williams, J. B. W. (1999). Validation and utility of a self-report version of PRIME-MD: The PHQ primary care study. Journal of the American Medical Association, 282(18), 1737–1744. https://doi.org/10.1001/jama.282.18.1737
Sterne, J. A. C., & Egger, M. (2005). Regression methods to detect publication and other bias in meta-analysis. In Publication Bias in Meta-Analysis: Prevention, Assessment and Adjustments (pp. 99–110). John Wiley & Sons, Ltd. https://doi.org/10.1002/0470870168.ch6
Sundberg, M. (2018). Online gaming, loneliness and friendships among adolescents and adults with ASD. Computers in Human Behavior, 79, 105–110. https://doi.org/10.1016/j.chb.2017.10.020
Syu, Y.-C., & Lin, L.-Y. (2018). Sensory overresponsivity, loneliness, and anxiety in taiwanese adults with autism spectrum disorder. Occupational Therapy International, 1–7https://doi.org/10.1155/2018/9165978
The Research Units on Pediatric Psychopharmacology Anxiety Study Group. (2002). The Pediatric Anxiety Rating Scale (PARS): Development and psychometric properties. Journal of the American Academy of Child and Adolescent Psychiatry, 41(9), 1061–1069. https://doi.org/10.1097/00004583-200209000-00006
Thomas, B. H., Ciliska, D., Dobbins, M., & Micucci, S. (2004). A process for systematically reviewing the literature: Providing the research evidence for public health nursing interventions. Worldviews on Evidence-Based Nursing, 1, 176–184. https://doi.org/10.1111/j.1524-475X.2004.04006.x
Thurm, A., Farmer, C., Salzman, E., Lord, C., & Bishop, S. (2019). State of the field: Differentiating intellectual disability from autism spectrum disorder. In Frontiers in Psychiatry (Vol. 10). Frontiers Media S.A. https://doi.org/10.3389/fpsyt.2019.00526
Tiwari, S. C. (2013). Loneliness: A disease? In Indian Journal of Psychiatry (Vol. 55, Issue 4, pp. 320–322). Wolters Kluwer -- Medknow Publications. https://doi.org/10.4103/0019-5545.120536
Vandenbroucke, J. P., von Elm, E., Altman, D. G., Gøtzsche, P. C., Mulrow, C. D., & Pocock, S. J. (2007). Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): Explanation and elaboration. PLoS Medicine, 4(10), 805–835. https://doi.org/10.1371/journal.pmed.0040297
Vasa, R. A., & Mazurek, M. O. (2015). An update on anxiety in youth with autism spectrum disorders. In Current Opinion in Psychiatry (Vol. 28, Issue 2, pp. 83–90). Lippincott Williams and Wilkins. https://doi.org/10.1097/YCO.0000000000000133
Victor, C. R., & Yang, K. (2012). The prevalence of loneliness among adults: A case study of the United Kingdom. Journal of Psychology: Interdisciplinary and Applied, 146(1–2), 85–104. https://doi.org/10.1080/00223980.2011.613875
Volkmar, F., Chawarska, K., & Klin, A. (2005). Autism in infancy and early childhood. Annual Review of Psychology, 56, 315–336. https://doi.org/10.1146/annurev.psych.56.091103.070159
Ward, A., Arola, N., Bohnert, A., & Lieb, R. (2017). Social-emotional adjustment and pet ownership among adolescents with autism spectrum disorder. Journal of Communication Disorders, 65, 35–42. https://doi.org/10.1016/j.jcomdis.2017.01.002
Wechsler, D. (2008). Wechsler Intelligence Scale for Children, Fourth Edition (WISC-IV). In Pearson. Springer US. https://doi.org/10.1007/978-0-387-79061-9
Wechsler, D. (2011). Wechsler Abbreviated Scale of Intelligence (2nd ed.). Psychological Corporation.
Weiss, R. S. (1973). Loneliness: The experience of emotional and social isolation. The MIT Press. https://psycnet.apa.org/record/1974-22306-000
Wendler, D. (2019). Improv theater as a social cognition intervention for autism. Dissertation Abstracts International: Section B: The Sciences and Engineering, 80. http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc16&NEWS=N&AN=2019-41141-135
White, S. W., & Roberson-Nay, R. (2009). Anxiety, social deficits, and loneliness in youth with autism spectrum disorders. Journal of Autism and Developmental Disorders, 39(7), 1006–1013. https://doi.org/10.1007/s10803-009-0713-8
Whitehouse, A. J. O., Durkin, K., Jaquet, E., & Ziatas, K. (2009). Friendship, loneliness and depression in adolescents with Asperger’s Syndrome. Journal of Adolescence, 32(2), 309–322. https://doi.org/10.1016/j.adolescence.2008.03.004
Wigham, S., Barton, S., Parr, J. R., & Rodgers, J. (2017). A systematic review of the rates of depression in children and adults with high-functioning autism spectrum disorder. Journal of Mental Health Research in Intellectual Disabilities, 10(4), 267–287. https://doi.org/10.1080/19315864.2017.1299267
Wood, H. (2014). Social anxiety and self-perceptions of social performance in adolescents and young adults with high functioning autism spectrum disorders [University of Bath (United Kingdom)]. In PQDT - UK & Ireland. https://search.proquest.com/dissertations-theses/doctorate-clinical-psychology-main-research/docview/1784057225/se-2?accountid=13828
Wright, M. F. (2017). Parental mediation, cyber victimization, adjustment difficulties, and adolescents with autism spectrum disorder. Cyberpsychology, 11(1), 1–12. https://doi.org/10.5817/CP2017-1-6
Yeung, A. W. (2009). The perception of friendships for children with Asperger’s disorder and its relationship with loneliness and depression. Dissertation Abstracts International: Section B: The Sciences and Engineering, 70(6-B). http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=psyc6&NEWS=N&AN=2009-99240-417
Zeidan, J., Fombonne, E., Scorah, J., Ibrahim, A., Durkin, M. S., Saxena, S., Yusuf, A., Shih, A., & Elsabbagh, M. (2022). Global prevalence of autism: A systematic review update. Autism Research, 13(1). https://doi.org/10.1002/AUR.2696
Acknowledgements
The research was conducted in partial fulfilment of doctoral level study by the first author under the supervision of the third author.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hymas, R., Badcock, J.C. & Milne, E. Loneliness in Autism and Its Association with Anxiety and Depression: A Systematic Review with Meta-Analyses. Rev J Autism Dev Disord 11, 121–156 (2024). https://doi.org/10.1007/s40489-022-00330-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40489-022-00330-w