Abstract
Background
The delivery mode for pregnant women with uteruses scarred by prior caesarean section (CS) is a controversial issue, even though the CS rate has risen in the past 20 years. We performed this retrospective study to identify the factors associated with preference for CS or vaginal birth after CS (VBAC).
Methods
Pregnant women (n = 679) with scarred uteruses from Moulay Ali Cherif Provincial Hospital, Rashidiya, Morocco, were enrolled. Gestational age, comorbidity, fetal position, gravidity and parity, abnormal amniotic fluid, macrosomia, placenta previa or abruptio, abnormal fetal presentation, premature rupture of fetal membrane with labor failure, poor progression in delivery, and fetal outcomes were recorded.
Results
Out of 679 pregnant women ≥28 gestational weeks, 351 (51.69%) had a preference for CS. Pregnant women showed preference for CS if they were older (95% CI 1.010–1.097), had higher gestational age (95% CI 1.024–1.286), and a shorter period had passed since the last CS (95% CI 0.842–0.992). Prior gravidity (95% CI 0.638–1.166), parity (95% CI 0.453–1.235), vaginal delivery history (95% CI 0.717–1.818), and birth weight (95% CI 1.000–1.001) did not influence CS preference. In comparison with fetal preference, maternal preference was the prior indicator for CS. Correlation analysis showed that pregnant women with longer intervals since the last CS and history of gravidity, parity, and vaginal delivery showed good progress in the first and second stages of vaginal delivery.
Conclusions
We concluded that maternal and gestational age and interval since the last CS promoted CS preference among pregnant women with scarred uteruses.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Background
One of the most controversial issues in modern obstetrics is how to deliver the second baby of women with uteruses scarred by caesarean section (CS). The CS rate has risen in most countries over the past 20 years. Worldwide, it accounted for 5% of total deliveries in 1970 [1] and increased to over 30% in 2010 [2]. However, this rate ranged from 6.0 to 27.2% in the least and more developed regions in 2014 [2]. In 2008, 64.1% of urban women gave birth by CS in China [3]. The general CS rate was 29% in 2008, and increased to 35% in 2014 [4] and 41.1% in 2016 [5]. This tendency in CS might be due to worldwide socioeconomic change. As previously mentioned, the increased rate of CS has brought about the controversy about the delivery mode for the second baby in cases of uteruses scarred after CS.
It is known that the incidence of uterine rupture (UR) is higher in women with uteruses scarred by CS or laparoscopic surgery for removing salpingectomy (ectopic pregnancy), uterine leiomyomas, and other lesions [6, 7]. Pregnant women with scarred uteruses have higher risk for UR and emergency admission during their pregnancy, and UR during early-stage pregnancy usually ends with pregnancy termination or fetal death [8]. URs during the late stage of pregnancy often end with premature infants with low Apgar scores or transfer to intensive care [9,10,11,12]. Despite the increased UR rate due to CS [6], CS shows advantages in newborn and maternal outcomes, in particular for pregnant women with protracted labor, abruptio placentae, placenta previa, fetal embarrassment, or macrosomia, as well as women with abnormal pelvis or poor progress in the first and second stages of labor [1, 13, 14].
Upon introduction of the second-child policy in China in Nov 2013, the controversial issue on how to give birth from a scarred uterus has been put on the table. It has been reported that women with scarred uteruses due to uncompleted CS are often advised to have vaginal birth after CS (VBAC), rather than elective repeat CS (ERCS) [15]. However, this trend reversed from 1996 to 2010 due to worldwide socioeconomic change [16, 17], and then rose to 50% in 2012 [15]. These differences depend on the national healthcare system, clinical guidelines and patient preferences. However, there are no clear guidelines for choosing the second delivery mode after CS.
We performed this retrospective study using data from pregnant women with scarred uteruses at ≥28 gestational weeks to identify the factors associated with CS or VBAC preferences. Factors including maternal age, gestational age, interval since the last CS delivery, and number of vaginal deliveries prior to and after the last CS, as well as the episodes related to childbirth, were recorded and analyzed. We believe that this summary will facilitate decision-making regarding vaginal vs. CS delivery for women with prior CS.
Materials and methods
Ethical approval and data protection
The de-identified data collected were obtained directly from this hospital’s database. Consent was obtained from patients before data collection. The Moulay Ali Cherif Provincial Hospital Ethics Committee ruled that ethical approval was not needed for the study. A confidentiality statement of data protection was completed with the data protection officer at the Moulay Ali Cherif Provincial Hospital.
Patient profile
This retrospective study was based on data from pregnant women with scarred uteruses admitted to Moulay Ali Cherif Provincial Hospital, Rashidiya, Morocco, between October 2016 and September 2018.
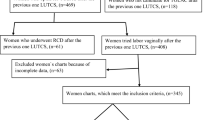
Women were included in our study if they met the following inclusion criteria: (1) age 19 or over, (2) with history of single-scar uterus, and (3) at ≥28 gestational weeks. The womens’ medical histories (gynecology and obstetrics), surgical indications for the last CS, number of vaginal deliveries prior to and after the last CS, as well as the interval between the last CS and this pregnancy (years), were recorded. The episodes related to childbirth captured the number of gravidity and parity, delivery method, and outcome.
Upon admission, we recorded the pregnant womens’ demographic characteristics, including gestational age (≥ 28 weeks), comorbidity history (including chronic hypertension, diabetes and gestational diabetes, and hypertension), electronic fetal heart monitoring, and fetal position, number, and presentation. Pregnant women with opening or opened cervical canals were prepared for VBAC. Pregnant women with indications for ERCS (pre-labor CSs) or intrapartum CS were not indicated, but the indications for CS were presented, including multifetation (≥ 2); suspected UR (with indications of abdominal pain, preeclampsia or eclampsia, and vaginal bleeding); abnormal amniotic fluid (pollution or less); macrosomia (evaluated over birthweight); placenta previa or abruptio placentae; abnormal fetal presentation; premature rupture of fetal membrane with labor failure; comorbidity (as mentioned above); and protracted active phase dilatation, protracted descent pattern, and prolonged latent phase of labor.
All episodes related to childbirth, including Apgar score (0–5 min), amount of bleeding during delivery (mL), and first- and second-stage labor duration (hour and minute; only for vaginal birth) were captured.
Statistical analysis
Pregnant women with CS and vaginal delivery were assigned to two groups accordingly. SPSS 22.0 software was used for statistical analysis. The difference in normally distributed data (age) between groups was analyzed using the unpaired t-test and that of abnormally distributed data (including gravidity and parity numbers, gestational age, and interval from the last CS) was analyzed using the Mann-Whitney U test. Differences in descriptive data (prior vaginal delivery, maternal demographics, indications for CS, and fetal outcomes) between the two groups were analyzed using the χ2 test with or without weighted case (frequency). To evaluate the correlation between maternal demographics, CS indicators, and fetal outcomes, we calculated the Spearman correlation coefficients. The 95% confidence intervals (95% CI) were analyzed. Logistic regression analysis was performed to identify indicators for CS preference. For all analyses, p < 0.05 was defined as statistical difference.
Results
Demographic characteristics of participants in the CS and VBAC groups
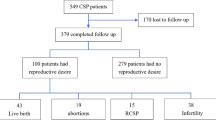
Out of the 679 pregnant women ≥28 gestational weeks, 351 women were assigned to CS (51.69%) and the other 328 women were assigned to VBAC (48.31%). There was no difference in age between the two groups (29.68 ± 6.04 vs. 29.70 ± 5.36, p = 0.979, Table 1). Women in the CS group showed significantly lower gravidity number, prior vaginal delivery number, shorter interval since the last CS, higher parity frequency, and older gestational age compared to women assigned to the vaginal delivery group (p < 0.01 for all). There were no significant differences in CS preference among ages (p = 0.169; χ2 test), interval since the last CS (p = 0.535), and newborn Apgar score (p = 0.222) between the women assigned to the CS and VBAC groups (Table 2).
Most women (60.67% in the VBAC group and 66.67% in the CS group) were 24–34 years old; approximately 22% of women were older than 34 years in the two groups. More than 93% women (93.29% in the VBAC group and 93.16% in the CS group) had over a 2-year interval since the last CS, suggesting good health consciousness. Most fetuses (approximately 97%) showed good outcomes, with Apgar score above 8′-8′. Pregnant women with newborns weighing over 4000 g had CS selection preference (p = 0.043, Table 2).
Indicators for CS preference
The factors that might impact maternal preference for CS were analyzed using logistic regression analysis. Maternal age (β = 0.043, 95% CI 1.010–1.097, p = 0.010), gestational age (β = 0.138, 95% CI 1.024–1.286, p = 0.018), and interval since the last CS (β = − 0.090, 95% CI 0.842~0.992, p = 0.031) were indicators for CS (Table 3). Higher maternal and gestational ages and shorter interval since the last CS were shown to promote maternal preference for CS. The history of gravidity and parity, vaginal delivery, and high birth weight were not indicators for CS preference (p > 0.05; Table 3).
Out of 351 women in the CS group, 144 participants (41.03%) chose CS delivery facing certain fetal conditions, including postmature birth (n = 57, 39.58%), followed by abnormal amniotic fluid (n = 37, 25.69%; Table 4). Of the risk factors in pregnant women, abnormal pelvis (n = 58, 28.02%), poor active phase (including protracted active phase dilatation, protracted descent pattern and prolonged latent phase of labor; n = 50, 24.15%), and malpresentation (n = 28, 13.53%) were the first three reasons for CS preference. Of the 16 participants with suspected UR, 7 (43.75%) had hemorrhoea (> 500 ml).
Risk factors associated with outcomes of CS delivery
Next, we analyzed the correlation between episodes related to CS, including suspected UR, abnormal amniotic fluid, birthweight, maternal age, gestational age, retarded birth, abnormal fetal presentation, comorbidity (including hypertension, diabetes, and preeclampsia or eclampsia), and Apgar score. Spearman correlation analysis showed that the presence of birth defects was negatively correlated with amniotic fluid abnormity (β = − 0.172, p < 0.01) and UR (β = − 0.167, p < 0.01) and positively correlated with birthweight (β = 0.170, p < 0.01; Table 5). Moreover, suspected UR showed negative correlations with gestational age (β = − 0.231, p < 0.01), abnormal active phase (β = − 0.145, p < 0.05), and birthweight (β = − 0.197, p < 0.01). Women with abnormal fetal presentation often had lower gestational age (β = − 0.110, p < 0.05), abnormal amniotic fluid (β = − 0.110, p < 0.05), and abnormal active phase (β = − 0.126, p < 0.05). Increased gestational age was only correlated with incidence of macrosomia (β = 0.307, p < 0.01), and abnormal amniotic fluid was negatively associated with fetal Apgar scores (β = − 0.268, p < 0.01; Table 5).
Factors associated with outcomes of vaginal delivery
Spearman correlation analysis was also performed to identify the correlations between factors associated with VBAC (Table 6). We found that the duration of first-stage and second-stage deliveries was significantly correlated (β = 0.452, p < 0.01). The delivery of macrosomia might increase duration of second-stage deliveries (β = 0.340, p < 0.01). Pregnant women with higher number of vaginal deliveries and longer intervals since the last CS showed shorter delivery duration (p < 0.01). In addition, we noted that older women showed shorter duration of first-stage (β = − 0.153, p < 0.05) and second-stage (β = − 0.245, p < 0.01) deliveries. Higher number of parity correlated with shorter delivery duration (β = − 0.307, p < 0.01; Table 6).
Discussion
Our study confirmed that most pregnant women with scarred uteruses chose CS delivery (51.69%), which was consistent with the worldwide trend. Of 679 CS deliveries, 41.03% were compelled by fetal conditions, including breech presentation, transverse presentation, reduced amniotic fluid, and amniotic fluid pollution. Of the other cases, 58.97% were caused by maternal conditions, 28.02% had abnormal pelvic, 24.15% developed abnormal active phase (protracted active phase dilatation, protracted descent pattern, and prolonged latent phase of labor), and 13.53% showed malpresentation during vaginal delivery. This was in accordance with the generally reported reasons for CS delivery, including protracted labor, abruptio placentae, previous CS, eclampsia, placenta previa, and malpresentation [1].
We determined that pregnant women with newborns weighing over 4000 g had CS preference, suggesting that macrosomia was an indicator for CS. Guo et al. showed that there was significantly lower neonatal birth weight between women in the VBAC group and women who failed the trial of labor after caesarean section (TOLAC) [18]. That was true for the women both with successful and failed TOLAC [19]. They also showed that vaginal delivery history and birth weight (< 3300 g) were independent factors for VBAC or successful TOLAC [18, 19]. However, there is controversy about the choice for macrosomia delivery in the general population. Menticoglou et al. [20] showed that most macrosomia (78.7%) were delivered via labor in Melbourne, Australia, with good outcomes, based on general cohort not considering scarred uterus.
Through our analysis, we determined that age was not a causality for CS preference in pregnant women (95% 1.010–1.097). Actually, some studies showed that advanced maternal age correlated with failed TOLAC [19], and maternal age < 35 years correlated with trial of labor [21]. This was different from the correlation between older maternal age and VBAC preference reported by Guo et al. [18]. However, Minsart et al. showed that Chinese women had a higher vaginal birth rate after CS compared with North American and Australian women [21]. This showed that the rate of vaginal birth after CS is different between races regardless of the age effect [21].
Sudhof et al. [22] showed that spontaneous labor onset was an indicator for choosing vaginal delivery. However, many parous women with or without spontaneous labor onset are more likely to have a cesarean birth [23]. This is a consequence of the fear of vaginal pain among many women. Out of 679 pregnant women, we found that older participants showed shorter duration of delivery (both in the first and second stages). This fact is largely due to the higher number of previous vaginal delivery among older women. We also found that the age of pregnant women was positively correlated with shorter gestational age especially in women in the VBAC group, which might indirectly reduce the incidence of macrosomia. Similarly, a negative correlation between advanced maternal age and incidence of macrosomia was reported by Lin et al. [24]. Advanced maternal age and higher birth weight were reported to be correlated with higher rate of failed TOLAC [19]. However, advanced maternal age (> 30 years) may be associated with higher risk of small for gestational age < 10th percentile [25], while women aged 20 to 29 years old had low risk of small for gestational age < 10th percentile.
We found that history of prior vaginal delivery was not an indicator for the selection of vaginal delivery mode or that there was even a correlation between them. This was not in accordance with the results obtained by other investigators [26] who have shown that prior history of vaginal delivery was a major reason for vaginal delivery preference. Some investigations show that both maternal age and parity number are associated with increased incidence of UR [6] and placenta previa [27, 28]. However, our study did not present the correlation between maternal age and incidence of suspected UR.
Women with a longer interval since the last CS had a preference for vaginal delivery. This was in accordance with the results reported by Seffah and Adu-Bonsaffoh [19], who showed that a short inter-pregnancy interval was related to failed TOLAC. We noted that more than 93% women (93.29% in the VBAC group and 93.16% in the CS group) had over a 2-year interval since the last CS, suggesting good health consciousness in most pregnant women. It has been reported that the mature stage for scarring is approximately 2 years [29, 30], and the following pregnancies usually show good outcomes with low tendency toward UR. Pregnant women with earlier healing and hospital discharge had a preference for vaginal delivery [26]. Two of the 16 women with suspected UR in our study had shorter intervals (< 2 years; 12.5%). However, 15 of 16 participants showed good outcomes with high Apgar scores (10–10) due to CS. These results suggested that CS was effective for improving the outcomes of pregnant women with UR.
Conclusions
In summary, we concluded that increased maternal and gestational ages and a shorter interval since the last CS were indicators for CS delivery. There was a negative correlation between maternal and gestational age, which might reduce the frequency of macrosomia. Both CS and VBAC are viable options for childbirth, with comparable fetal outcomes. The selection of repeat CS delivery after CS may not depend on maternal age and gestational age, but may be associated with adequate patient education.
Availability of data and materials
The datasets generated and analyzed during the current study are not publicly available due to institutional confidentiality but are available from the corresponding author on reasonable request.
Abbreviations
- CS:
-
Cesarean section
- ERCS:
-
Elective repeat CS
- UR:
-
Uterus rupture
- VBAC:
-
Vaginal birth after CS
References
Dumont A, Bernis LD, Bouvier-Colle MH, Bréart G. Caesarean section rate for maternal indication in sub-Saharan Africa: a systematic review. Lancet. 2001;358(9290):1328–33.
Betrán AP, Ye J, Moller AB, Zhang J, Gülmezoglu AM, Torloni MR. The increasing trend in caesarean section rates: global, regional and National Estimates: 1990-2014. PLoS One. 2016;11(2):e0148343.
Lin FX, Ling X, Yan G, Carine R. Factors influencing rising caesarean section rates in China between 1988 and 2008. Bull World Health Organ. 2012;90(1):30–39A.
Li HT, Luo S, Trasande L, Hellerstein S, Kang C, Li JX, Zhang Y, Liu JM, Blustein J. Geographic variations and temporal trends in cesarean delivery rates in China, 2008-2014. Jama. 2017;317(1):69–76.
Liang J, Mu Y, Li X, Tang W, Wang Y, Liu Z, Huang X, Scherpbier R, Guo S, Li M, et al. Relaxation of the one child policy and trends in caesarean section rates and birth outcomes in China between 2012 and 2016: observational study of nearly seven million health facility births. Bmj. 2018;360:k817.
Al-Zirqi I, Stray-Pedersen B, Forsén L, Daltveit AK, Vangen S. Uterine rupture: trends over 40 years. BJOG Int J Obstet Gynaecol. 2016;123(5):780–7.
Chao A-S, Chang Y-L, Yang L-Y, Chao A, Chang W-Y, Su S-Y, Wang C-J. Laparoscopic uterine surgery as a risk factor for uterine rupture during pregnancy. PLoS One. 2018;13(5):e0197307.
Jiang S, Zhao J. Analysis of 12 cases of interstitial pregnancy after salpingectomy. Chinese J Fam Plann Gynecotokol. 2018;10(5):61–5 (in Chinese).
Lin B: The uterine rupture after laparoscopic surgery for ectopic interstitial pregnancy: report of 4 cases and literature review. Zhejiang University 2017:[Master's Thesis].
Gu X, Wang Y. Two cases of uterine rupture in ectopic pregnancy after laparoscopic surgery. Prog Obstet Gynecol. 2015;24(7):486 (in Chinese).
Paradise C, Carlan SJ, Holloman C. Spontaneous uterine cornual rupture at 26 weeks' gestation in an interstitial heterotopic pregnancy following in vitro fertilization. J Clin Ultrasound Jcu. 2016;44(5):322–5.
Yang X. One case of metrorrhexis caused by subsequent fetation after ectopic pregnancy surgery. China Modern Med. 2013;20(3):151–2 (in Chinese).
Menticoglou SM, Manning FA, Morrison I, Harman CR. Must Macrosomic fetuses be delivered by a caesarean section? A review of outcome for 786 babies ≥ 4,500 g. Aust N Z J Obstet Gynaecol. 2010;32(2):100–3.
Florica M, ., Stephansson O, Nordström L. Indications associated with increased cesarean section rates in a Swedish hospital. Int J Gynaecol Obstet 2006, 92(2):181–185.
Knight HE, Gurol-Urganci I, Van Der Meulen JH, Mahmood TA, Richmond DH, Dougall A, Cromwell DA. Vaginal birth after caesarean section: a cohort study investigating factors associated with its uptake and success. BJOG Int J Obstet Gynaecol. 2014;121(2):183–92.
Shiliang L, Rusen ID, Joseph KS, Robert L, Kramer MS, Wu WS, Robert K. Recent trends in caesarean delivery rates and indications for caesarean delivery in Canada. J Obstet Gynaecol Canada. 2004;26(8):735–42.
Homer CSE, Johnston R, Foureur MJ. Birth after caesarean section: changes over a nine-year period in one Australian state. Midwifery. 2011;27(2):165–9.
Guo N, Bai R, Qu P, Huang P, He Y, Wang C, Mi Y. Influencing factors and antenatal assessment of the vaginal birth after cesarean section. Zhonghua fu chan ke za zhi. 2019;54(6):369–74.
Seffah J, Adu-Bonsaffoh K. Vaginal birth after a previous caesarean section: current trends and outlook in Ghana. J West Afr Coll Surg. 2014;4(2):1.
Menticoglou SM, Manning FA, Morrison I, Harman CR. Must macrosomic fetuses be delivered by a caesarean section? A review of outcome for 786 babies greater than or equal to 4,500 g. Aust N Z J Obstet Gynaecol. 2010;32(2):100–3.
Minsart A-F, Liu H, Moffett S, Chen C, Ji N. Vaginal birth after caesarean delivery in Chinese women and Western immigrants in Shanghai. J Obstet Gynaecol. 2017;37(4):446–9.
Sudhof L, Has P, Rouse D, Hughes B. Choice of trial of labor after cesarean and association with likelihood of success. Am J Perinatol. 2018;35(9):892–7.
Neal JL, Lowe NK, Phillippi JC, Carlson NS, Knupp AM, Dietrich MS. Likelihood of cesarean birth among parous women after applying leading active labor diagnostic guidelines. Midwifery. 2018;67:64–9.
Lin J, Fu Y, Han Q, Yan J, Chen R, Zhang H. Gestational weight management and pregnancy outcomes among women of advanced maternal age. Exp Ther Med. 2019;18(3):1723–8.
Palatnik A, De Cicco S, Zhang L, Simpson P, Hibbard J, Egede L. The Association between Advanced Maternal Age and Diagnosis of Small for Gestational Age. Am J Perinatol. 2019. https://doi.org/10.1055/s-0039-1694775.
Buyukbayrak EE, Kaymaz O, Kars B, Karsidag AYK, Bektas E, Unal O, Turan C. Caesarean delivery or vaginal birth: preference of Turkish pregnant women and influencing factors. J Obstet Gynaecol. 2010;30(2):155–8.
Simi J, Bindu P, Uma T, Nirmala C. A comparative study on maternal and fetal outcome in cases of placenta Previa with previous cesarean section and without previous cesarean section. JMSCR. 2017;5(4):20657–65.
Bencaiova G, Burkhardt T, Beinder E. Abnormal placental invasion experience at 1 center. J Reprod Med. 2007;52(8):709–14.
Gong P, Es'Haghian S, Harms KA, Murray A, Rea S, Kennedy BF, Wood FM, Sampson DD, Mclaughlin RA. Optical coherence tomography for longitudinal monitoring of vasculature in scars treated with laser fractionation. J Biophotonics. 2016;9(6):626–36.
Es'Haghian S, Gong P, Chin L, Harms KA, Murray A, Rea S, Kennedy BF, Wood FM, Sampson DD, Mclaughlin RA. Investigation of optical attenuation imaging using optical coherence tomography for monitoring of scars undergoing fractional laser treatment. J Biophotonics. 2017;10(4):511–22.
Acknowledgements
We thank the staff of the Moulay Ali Cherif Provincial Hospital, Rashidiya, Morocco, for their generous help in obtaining the clinical data.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
Conception and design of the research: ZH. Acquisition and interpretation of data: ZH and FEO. Statistical analysis: ZH. Drafting the manuscript: ZH. Manuscript revision for important intellectual content: FEO. Both authors have read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethics approval was not required for this study. This study involved no human tissues and animal experiments or tissues. Written consent was obtained from patients before data collection. The Moulay Ali Cherif Provincial Hospital Ethics Committee ruled that ethical approval was not needed in this particular case.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Hua, Z., El Oualja, F. Indicators for mode of delivery in pregnant women with uteruses scarred by prior caesarean section: a retrospective study of 679 pregnant women. BMC Pregnancy Childbirth 19, 445 (2019). https://doi.org/10.1186/s12884-019-2604-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12884-019-2604-0