Abstract
Background
Aseptic necrosis of the femoral head (ANFH) has a high incidence in the community and causes substantial problems with health as well as economic and social stress. Core decompression is the most commonly used treatment for early ANFH. Although many studies have reported on the efficacy of femoral head core decompression surgery for ANFH, there are still some shortcomings in assessing the severity of femoral head necrosis, the location distribution, and changes in necrotic lesions before and after surgery. Magnetic resonance imaging (MRI) and equivalent sphere model analysis were used to further clarify the clinical efficacy of percutaneous multiple small-diameter drilling core decompression in patients with ANFH.
Methods
From July 2013 to November 2016, 24 patients (32 cases of the hip joint) with ANFH who underwent percutaneous multiple small-diameter drilling core decompression were selected, and a retrospective analysis was conducted. MRI as well as VAS, OHS-C, and HHS scores were used to evaluate joint function in all patients before and 6, 12, and 24 months after the operation.
Results
Twenty-four months after the operation, 10 hips were amputated. The survival rates of alcoholic femoral head necrosis (AFNH), idiopathic femoral head necrosis (IFHN), and steroid-induced femoral head necrosis (SIFHN) patients at 24 months were 100%, 85.7% (− 2 hips), and 0.0% (− 8 hips), respectively. The MRI and equivalent sphere analysis results revealed that the anterior superior medial quadrant was the area most prone to osteonecrosis, and the posterior superior medial quadrant was the area second most prone to necrosis. After the operation, the average percentage of the AFHN necrosis area in the total volume of the femoral head decreased from 14.5 to 10.3%, and the average percentage of the IFHN necrosis area decreased from 16.3 to 9.2%; however, the average percentage of the necrosis area for SIFHN increased from 30.4 to 33.1%.
Conclusion
Percutaneous multiple small-diameter drilling core decompression significantly reduced the lesion volume for AFHN and IFHN, but the effect on SIFHN was not good.
Similar content being viewed by others
Background
Aseptic necrosis of the femoral head (ANFH), also known as nontraumatic femoral head necrosis, is a pathological process caused by impaired blood supply to the femoral head [1]. This process induces demineralization, trabecular thinning, and subsequent collapse of the joint surface with fracture of subchondral bone [2]. It can be classified as alcoholic femoral head necrosis (AFNH), steroid-induced femoral head necrosis (SIFHN), and idiopathic femoral head necrosis (IFHN) depending on the causes. ANFH has a high incidence in young and middle-aged populations and eventually leads to a severe loss of hip function [3]. In the USA, approximately 600,000 people are affected by ANFH [4]. The incidence of ANFH is also rising in Asian countries [5, 6]. The total population of individuals with ANFH in China over 15 years old is about 8.12 million [6]. This evidence suggests that ANFH has a high incidence in the community and causes substantial problems with health as well as economic and social stress.
Studies have shown that approximately 85% of patients have clinical symptoms, and 67% of patients without clinical symptoms experience a subsequent collapse of the femoral head; ultimately, these patients need to undergo artificial joint replacement [7]. To delay and reduce the probability of hip replacement in patients with ANFH, a series of interventions can be performed in patients with early femoral head necrosis, including biophysical therapy, drug intervention, bone flap transplantation with vascular pedicles, and core decompression of the femoral head [8]. Core decompression is the most commonly used treatment for early ANFH [9]. It improves local microvascular circulation by reducing the high pressure of the femoral head caused by tissue edema and promotes the healing of necrosis. Ultimately, core decompression relieves pain, improves joint function, and improves quality of life [10,11,12]. Although many studies have reported on the efficacy of femoral head core decompression surgery for ANFH, there are still some shortcomings in assessing the severity of femoral head necrosis, the location distribution, and changes in necrotic lesions before and after surgery.
The volume and location of femoral head necrosis are the main influencing factors associated with femoral head collapse [13]. However, the anatomical features of the femoral head limit our ability to accurately describe the differences between individuals with different types of femoral head necrosis. Magnetic resonance imaging (MRI) has a higher sensitivity and specificity for diagnosing early ANFH than X-ray and computed tomography (CT) examinations [14]. In addition, based on the definition of an equivalent sphere model for the femoral head [15], we can calculate the percentage of lesion volume in the equivalent sphere to represent the actual lesion volume across the femoral head [16]. Thus, we can assess the severity and prognosis of femoral head necrosis accurately and objectively.
The present study was characterized by a quantitative study of femoral head necrosis in ANFH patients treated with percutaneous multiple small-diameter drilling core decompression using MRI examination and equivalent sphere analysis. At the same time, the pain, function, and quality of life of ANFH patients were objectively described by various internationally recognized evaluation scales. Finally, a comprehensive assessment of the effect of percutaneous multiple small-diameter drilling core decompression on the prognosis of ANFH was conducted. This study is helpful for further clarifying the clinical efficacy of percutaneous multiple small-diameter drilling core decompression in patients with ANFH. It provides a theoretical basis for the treatment of ANFH by percutaneous multiple small-diameter drilling core decompression.
Material and methods
General information
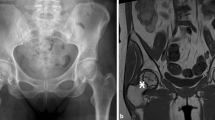
From July 2013 to November 2016, 24 patients (32 cases of the hip joint) with ANFH who underwent percutaneous multiple small-diameter drilling core decompression at the Zhongnan Hospital of Wuhan University were selected and subjected to retrospective analysis. All patients were examined with MRI and X-ray before admission, and the degree of necrosis of the femoral head was graded according to the method of the University of Pennsylvania. At the same time, the VAS score [17], OHS-C score [18], and HHS score [19] were used for preoperative evaluation. The inclusion process of the patients is shown in Fig. 1. The inclusion criteria were as follows: (a) patients with ANFH below stage IIc, (b) patients who voluntarily underwent core decompression surgery, (c) adult patients over 18 years old with no previous trauma or operation history of the lower limbs and spine, and (d) no contraindications such as severe cardiopulmonary insufficiency, poor control of blood pressure, diabetes, or blood system diseases.
Operation method
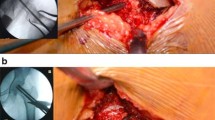
The patient was placed in a supine position after combined spinal-epidural anesthesia, which was convenient for intraoperative fluoroscopy. A 1% active iodine solution was used to disinfect the operation area, and then, a sterile dressing was used to cover the operation field. Three 2.5-mm-diameter Kirschner wires and two 3.0-mm-diameter Steinman pins were drilling through the femoral neck and femoral head under the trochanter to establish five decompression channels. Intraoperative fluoroscopy was used to ensure that the tip of the nail reached the necrotic area (Fig. 2).
Postoperative rehabilitation
Patients were asked to perform a non-weight-bearing rehabilitation exercise in bed and allowed to walk with non-weight-bearing crutch for 12 weeks after surgery. Isometric leg contraction and ankle rotation training were carried out on the bed, following the principle of step-by-step strengthening. After 12 weeks, the patient began partial weight-bearing rehabilitation training with the help of a professional rehabilitation physician.
Assessment instrument
VAS, OHS-C, and HHS scores were used to evaluate joint function within 1 week before the operation and at the 6, 12, and 24 months follow-up after the operation.
Quantification of lesions based on the concept of MRI and equivalent sphere analysis
MRI and X-ray examinations were performed in all the subjects before the surgery and 6, 12, and 24 months after the operation. Cases of femoral head collapse and artificial joint replacement were recorded. Based on the concept of the equivalent sphere proposed by Malizos et al. [15], the equivalent sphere volume of the femoral head was larger than that of the corresponding anatomic entity. The equivalent sphere was divided into eight quadrants from the horizontal, coronal, and sagittal positions: anterior superior lateral (ASL), anterior superior medial (ASM), anterior inferior lateral (AIL), anterior inferior medial (AIM), posterior superior lateral (PSL), posterior superior medial (PSM), posterior inferior lateral (PIL), and posterior inferior medial (PIM). The volume percentage of lesions on the equivalent sphere was used to describe the volume ratio of the actual lesion size in the whole femoral head. Further, the severity of femoral head necrosis between different individuals was standardized and compared with each other. Two imaging specialists and one joint surgeon completed the measurement. Each person repeated the analysis twice, with an interval of at least 1 week each time. Controversial results were debated and measured by another senior joint surgeon. Finally, all the results were summarized, and the average value was calculated for analysis.
Statistical methods
All data in this study were analyzed with SPSS 23.0 (IBM Corp., USA) software. In this study, the t test was used for statistical analysis. Statistical significance was designated at P < 0.05.
Results
General information about the research subjects
In this study, a total of 24 patients (including 32 hips) with ANFH were included, 18 males (24 hips) and 6 females (8 hips), with an average age of 47.1 ± 10.3 (20–62) years. Eight patients (10 hips) had AFNH, six patients (8 hips) had SIFHN, and ten patients (14 hips) had IFHN. According to the Pennsylvania stage of femoral head necrosis, there were 4 hips with stage Ia, 6 hips with stage Ib, 4 hips with stage Ic, 4 hips with stage IIa, 4 hips with stage IIb, and 10 hips with stage IIc disease. All patients were followed up for more than 6 months. The mean follow-up time was 25.9 ± 15.0 months (9.0–55.0 months) (Table 1).
Comparison of VAS, OHS-C, and HHS scores before and after the operation
The average VAS score was 2.4 ± 0.9 6 months after the core decompression operation, which was significantly lower than the score before the operation (Table 2, P < 0.01). At the end of the follow-up, the average VAS score was 3.1 ± 3.2, which was significantly lower than the score before core decompression (Table 2, P < 0.05).
The mean value of the OHS-C score of the hip joint at the 6-month follow-up was 35.6 ± 7.8, which was much higher than the score before the operation (Table 3, P < 0.01). At the end of the follow-up, the total average OHS-C score of the hip joint was 34.6 ± 13.7, which was significantly higher than the score before the operation (Table 3, P < 0.05).
At the 6-month follow-up, the average HHS score of the hip joint was 78.2 ± 9.1, which was much higher than the score before the operation (Table 4, P < 0.01). At the end of the follow-up, the average HHS score of the hip joint was 78.7 ± 17.4, which was higher than the score before the operation (Table 4, P < 0.05).
When analyzed according to pathogeny, the results suggested that percutaneous multiple small-diameter drilling core decompression significantly improved VAS, OHS-C, and HHS scores in patients with AFHN or IFHN. However, as shown in Tables 2, 3, and 4, core decompression only helped for the VAS, OHS-C, and HHS scores of patients with SIFHN within 6 months and did not improve hip pain or function in the middle period (more than 12 months).
Survival analysis of the hips
Twenty-four months after core decompression, 10 hips were amputated (femoral head collapse), and all of them had stage II disease before the operation. Among them, 2 hips collapsed at 9th month, 4 hips collapsed at 12th month, 2 hips collapsed at 20th month, and 2 hips collapsed at 24th month after the surgery. The overall survival rates at 12 and 24 months in this study were 81.3% and 68.6%, respectively (Fig. 3). The 24-month survival rate for stage I ANFH was 100%. The survival rates for stage II ANFH at 12 and 24 months were 66.7% and 44.4%, respectively (Fig. 4). The 24-month survival rate of AFHN was 100%. The survival rates of IFHN at 12 and 24 months were 92.6% (− 1 hip) and 85.7% (− 2 hips), respectively. The survival rates of SIFHN at 12 and 24 months were 37.5% (− 5 hips) and 0.0% (− 8 hips), respectively (Fig. 5).
Volume and distribution of femoral head necrosis area before the operation
The preoperative evaluation showed that the average volume in focus in AFHN was 14.1 ± 4.3 cm3, accounting for 24.8% ± 7.2% of the total volume of the femoral head. The average volume of the necrosis area for SIFHN was 16.5 ± 2.4 cm3, accounting for 30.4% ± 5.4% of the total volume of the femoral head. The average volume of the necrosis area for IFHN was 14.7 ± 6.0 cm3, accounting for 25.6% ± 8.7% of the total volume of the femoral head (Table 5). The average percentage of the total necrosis area in the volume of the femoral head in the study was 26.5% ± 7.5% (Table 5). Among these areas, the ASM quadrant was the most prone area for osteonecrosis. The average percentage of the volume of osteonecrosis area in the total volume of this quadrant was 55.2% ± 18.6% (Table 5/Fig. 6). The smallest affected area was the PIL quadrant, and the mean volume percentages of the dead and damaged objects were 7.7% ± 3.1% (Table 5/Fig. 6).
Distribution of the femoral head necrosis area before the operation. ASM: anterior superior medial; PSM: posterior superior medial; ASL: anterior superior lateral; PSL: posterior superior lateral; AIM: anterior inferior medial; PIM: posterior inferior medial; AIL: anterior inferior lateral; PIL: posterior inferior lateral; AFHN: alcoholic femoral head necrosis; SIFHN: steroid-induced femoral head necrosis; IFHN: idiopathic femoral head necrosis
Volume and distribution of the femoral head necrosis area after the operation
Six months after core decompression, the average percentage of the total necrosis volume of the femoral head was 19.9% ± 10.1%, which was 6.5% ± 7.9% lower than the average before core decompression (Table 6). The most significant reduction in necrosis area volume was seen in the ASM quadrant. In the ASM quadrant, the average percentage of the necrosis area volume in the total volume of this quadrant was 41.8% ± 23.3%, which was 13.4% ± 17.4% lower than the average before the operation (Table 6/Fig. 7). The average percentage of the AFHN necrosis area in the total volume of the femoral head was 14.5% ± 6.6%, which was 10.3% ± 0.9% less than the average before the operation; the average percentage of the IFHN necrosis area was 16.3% ± 7.5%, which was 9.2% ± 8.7% less than the average before the operation. However, the mean volume percentage of the necrosis area for SIFHN was 33.1% ± 5.1%, which increased by 2.7% ± 2.6% compared with the average before surgery. The results of the subgroup analysis showed that the volume of the necrosis area in the ASM quadrant for SIFHN increased significantly (6.5% ± 6.6%) (Table 6/Fig. 7).
Volume and distribution of the femoral head necrosis area at the 6th month after the operation. Anterior superior medial (ASM), posterior superior medial (PSM), anterior superior lateral (ASL), posterior superior lateral (PSL), anterior inferior medial (AIM), posterior inferior medial (PIM), anterior inferior lateral (AIL), posterior inferior lateral (PIL). AFHN: alcoholic femoral head necrosis; SIFHN: steroid-induced femoral head necrosis; IFHN: idiopathic femoral head necrosis
Clinical information of patients with amputation
In order to further explore the factors affecting the efficacy of percutaneous multiple small-diameter drilling core decompression, we summarized the clinical characteristics of the patients with tail amputation events in this study. As shown in Table 7, a total of 10 tail amputations occurred in this study, among which 8 were SIFN and 2 were IFHN, suggesting that the effect of decompression of SIFN with percutaneous fine-needle core was not good. VAS, OHS-C, and HHS in patients with tail amputation events were not significantly improved compared with those before surgery. In terms of the distribution of collapse area, 10 cases of hip joints collapsed in ASM, 9 cases collapsed in PSM, 8 cases collapsed in ASL, and 5 cases collapsed in PSL. The collapse area was mainly concentrated in the weight-bearing area. It was suggested that percutaneous multiple small-diameter drilling core decompression was not effective for SIFN, and the load-bearing area was the main area when the collapse occurred.
Discussion
Femoral head core decompression is the most commonly used surgery for the treatment of early ANFH. It reduces the internal pressure of the femoral head caused by tissue edema and promotes bone regeneration, healing, and remodeling, and thus reduces pain, improves joint function, and improves quality of life [10,11,12]. Studies have proven that the percutaneous multiple small-diameter drilling core decompression can relieve the pain of the hip joint in patients and delay the progress of femoral head necrosis [20,21,22]. According to Mont et al., 63.5% of reviewed hips achieved a well clinical result after core decompression. Stage predicted outcome, with a survival rate of 84% of hips with stage I ANFH and 65% of hips with stage II ANFH [23]. According to the results of Song et al., the survival rate of stage I ANFH and stage II ANFH was 79% and 77%, respectively, after multiple drilling core decompression for 5 years [24]. In this study, after the operation, the VAS scores decreased, and the HHS and OHS-C scores increased in all patients with AFHN or IFHN. These results suggested that percutaneous multiple small-diameter drilling core decompression significantly improved the pain, quality of life, and hip function of patients with AFHN or IFHN. However, for patients with SIFHN, percutaneous multiple small-diameter drilling core decompression improved the VAS, HHS, and OHS-C scores in a short period, but had no effect on the long-term VAS, HHS, and OHS-C scores. In general, percutaneous multiple small-diameter drilling core decompression significantly improved the short-term and long-term joint health and quality of life of patients with AFHN or IFHN. However, for SIFHN, percutaneous multiple small-diameter drilling core decompression only improved the local symptoms of the joint in the short term and had limited long-term effects. In addition, the survival rate of stage I ANFH was 100% and stage II ANFH was 44% at 2 years after the percutaneous multiple small-diameter drilling core decompression in this study. The results were similar to previous reports.
In current clinical studies, early treatment of ANFH emphasizes comprehensive treatment. The conventional methods of treatment include core decompression combined with weight-bearing restriction and drug [25, 26]. Most studies have shown that after core decompression surgery, patients need to undergo a 3–6-month weight-bearing restriction to achieve better outcomes [27,28,29]. The post-operative weight-bearing restriction is helpful for the recovery of blood circulation in the femoral head of the affected limb. Moreover, it can promote the regeneration and remodeling of the internal bone of the femoral head, delay the further necrosis of the femoral head, and ultimately improve the success rate of core decompression surgery [26]. However, it has been reported that for non-surgical patients, the survival rate of the femoral head could not be improved simply by weight-bearing restriction, and the progression of femoral head necrosis was not significantly delayed [25, 30]. A retrospective study by Mont et al. showed that more than 74% of patients with femoral head necrosis were further aggravated after 34 months of weight-bearing restriction [25]. In addition, animal experiments showed that there was no significant difference in the progression of steroid-induced femoral head necrosis in the rat model between the control group and the weight-bearing-restricted group [31]. In this study, all patients underwent core decompression. After 6 months of weight-bearing restriction, the hip joint score was significantly improved and femoral head necrosis progression was significantly delayed. Therefore, we speculated that the improvement in various clinical scores of patients after core decompression surgery was mainly caused by the surgery, rather than the long-term non-weight bearing.
The volume and location of femoral head necrosis are the main factors related to the collapse of the femoral head. However, the anatomical characteristics of the femoral head often limit researchers in describing the differences between different individuals. MRI demonstrates the volume and location distribution of femoral head necrosis foci in three dimensions, which can more accurately evaluate the severity and prognosis of femoral head necrosis. Based on the definition of an equivalent sphere model for the femoral head, MRI can help calculate the volume percentage of femoral head tissue affected by avascular necrosis in different regions and compare the differences between different individuals [15]. The prognosis of ANFH is related to the volume and location distribution of femoral head necrosis lesions [32,33,34]. ANFH patients with micronecrotic lesions far from the articular surface may have a good prognosis even without additional therapeutic intervention. However, the prognosis of ANFH patients with large necrotic lesions involving subchondral bone in the weight-bearing region is poor whether treated or not [32, 35]. Therefore, it is of great significance for the treatment of ANFH to accurately describe the lesion distribution in the femoral head with three-dimensions by using the equivalent sphere-volume method. In this study, we found that the focus of ischemic necrosis in ANFH patients was mainly located in the ASM quadrant, which was basically consistent with previous studies. These findings also suggest that the direction of the decompression guidewire should be as close as possible to the anterior-upper part of the femoral head when performing femoral head core decompression.
In ANFH patients without early intervention, deformation and collapse of the femoral head will occur within 2 years of onset as the necrosis volume of the femoral head expands. These patients develop osteoarthritis of the hip and eventually require an artificial joint replacement. Therefore, the volume of the necrotic area of the femoral head is an important indicator of the degree of necrosis of the femoral head [36]. In this study, compared with the preoperative volume, the volume of the total necrotic lesion of the hip decreased 6 months after decompression surgery. Among these volumes, the necrotic volume of the ASM region in the main load area was significantly reduced, while the necrotic volumes of other areas were decreased to varying degrees. These results suggest that percutaneous multiple small-diameter drilling core decompression reduces the lesion volume of patients with femoral head necrosis, thus delaying the progress of femoral head necrosis. However, all 6 patients (8 hips) with SIFHN included in this study were found to have a larger volume of osteonecrosis of the femoral head on MRI 6 months after surgery compared with that of before surgery. All 6 patients (8 hips) with SIFHN had undergone artificial joint replacement at the end of the follow-up. SIFHN is associated with angiogenic dysfunction, decreased bone repair ability, and inhibited BMP-2 receptor expression [37,38,39]. Although decompression with a femoral head core drill releases intramedullary pressure and improves intramedullary microcirculation, it cannot improve bone cell metabolism and bone regeneration function for SIFHN. Therefore, the effect of percutaneous multiple small-diameter drilling core decompression on SIFHN is limited.
Limitations of this study
This study is a retrospective study, and the quality of evidence is lower than that of prospective studies and randomized controlled trials. Further, the number of cases included in the study was small. The lack of stage I SIFHN cases may be a factor affecting the prognosis of SIFHN. Further expansion of the sample size and a long-term follow-up are needed in the future.
Conclusion
The equivalent sphere method based on MRI can accurately describe the location distribution of ANFH lesions, as well as the volume change of the necrotic area before and after the operation. The short-term (within 6 months) and long-term (more than 12 months) VAS, HHS, and OHS-C scores after surgery for AFHN and IFHN were significantly improved by percutaneous multiple small-diameter drilling core decompression, while the effect of SIFHN on long-term hip pain relief and functional improvement was limited. Percutaneous multiple small-diameter drilling core decompression significantly reduced the lesion volume for AFHN and IFHN, but the effect on SIFHN was not good.
Availability of data and materials
All the data of the manuscript are presented in the paper.
Abbreviations
- ANFH:
-
Aseptic necrosis of the femoral head
- MRI:
-
Magnetic resonance imaging
- AFHN:
-
Alcoholic femoral head necrosis
- IFHN:
-
Idiopathic femoral head necrosis
- SIFHN:
-
Steroid-induced femoral head necrosis
- CT:
-
Computed tomography
- ASL:
-
Anterior superior lateral
- ASM:
-
Anterior superior medial
- AIL:
-
Anterior inferior lateral
- AIM:
-
Anterior inferior medial
- PSL:
-
Posterior superior lateral
- PSM:
-
Posterior superior medial
- PIL:
-
Posterior inferior lateral
- PIM:
-
Posterior inferior medial
References
Boksenbaum M. Aseptic necrosis of the femoral head associated with steroid therapy. Jama. 1963;184:262.
Kramer J, Scheurecker G, Scheurecker A, Stöger A, Hofmann S. Femoral head necrosis. 2009;49:410–8.
Mont MA, Jones LC, Hungerford DS. Nontraumatic osteonecrosis of the femoral head: ten years later. J Bone Joint Surg Am. 2006;88(5):1117–32.
Lieberman JR, Berry DJ, Mont MA, Aaron RK, Callaghan JJ, Rajadhyaksha AD, Urbaniak JR. Osteonecrosis of the hip: management in the 21st century. Instr Course Lect. 2003;84:337.
Kazuma I, Yukiharu H, Taisuke S, Yasuhiko T, Takafumi A, Naoki I. Epidemiology of nontraumatic osteonecrosis of the femoral head in Japan. Mod Rheumatol. 2015;25(2):278–81.
Zhao DW, Yu M, Hu K, Wang W, Yang L, Wang BJ, Gao XH. Prevalence of nontraumatic osteonecrosis of the femoral head and its associated risk factors in the Chinese population: results from a nationally representative survey. Chin Med J. 2015;128(21):2843–50.
Musso ES, Mitchell SN, Schink-Ascani M, Bassett CA. Results of conservative management of osteonecrosis of the femoral head. A retrospective review. Clin Orthop Relat Res. 1986;207:209–15.
Sen RK. Management of avascular necrosis of femoral head at pre-collapse stage. Indian J Orthop. 2009;43(1):6–16.
Dean MT, Cabanela ME. Transtrochanteric anterior rotational osteotomy for avascular necrosis of the femoral head. Long-term results. J Bone Joint Surg (Br). 1993;75(4):597–601.
Yamamoto T, Ikemura S, Iwamoto Y, Sugioka Y. The repair process of osteonecrosis after a transtrochanteric rotational osteotomy. Clin Orthop Relat Res. 2010;468(12):3186–91.
Eyb R, Kotz R. The transtrochanteric anterior rotational osteotomy of Sugioka. Early and late results in idiopathic aseptic femoral head necrosis. Arch Orthop Trauma Surg. 1987;106(3):161–7.
Hiranuma Y, Atsumi T, Kajiwara T, Tamaoki S, Asakura Y. Evaluation of instability after transtrochanteric anterior rotational osteotomy for nontraumatic osteonecrosis of the femoral head. J Orthop Sci. 2009;14(5):535–42.
Lieberman JR, Engstrom SM, Meneghini RM, SooHoo NF. Which factors influence preservation of the osteonecrotic femoral head? Clinical orthopaedics and related research. Clin Orthop Relat Res. 2012;470(2):525–34.
Beltran J, Burk JM, Herman LJ, Clark RN, Zuelzer WA, Freedy MR, Simon S. Avascular necrosis of the femoral head: early MRI detection and radiological correlation. Magn Reson Imaging. 1987;5(6):431–42.
Malizos KN, Siafakas MS, Fotiadis DI, Karachalios TS, Soucacos PN. An MRI-based semiautomated volumetric quantification of hip osteonecrosis. Skelet Radiol. 2001;30(12):686–93.
Mitchell DG, Rao VM, Dalinka MK, Spritzer CE, Alavi A, Steinberg ME, Fallon M, Kressel HY. Femoral head avascular necrosis: correlation of MR imaging, radiographic staging, radionuclide imaging, and clinical findings. Radiology. 1987;162(3):709–15.
Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale. Arthritis Care Res. 2011;63:S240–52.
Zheng W, Li J, Zhao J, Liu D, Xu W. Development of a valid simplified Chinese version of the Oxford Hip Score in patients with hip osteoarthritis. Clin Orthop Relat Res. 2014;472:1545–51.
Söderman P, Malchau H. Is the Harris hip score system useful to study the outcome of total hip replacement? Clin Orthop Relat Res. 2001;384:189–97.
Omran AA. Multiple drilling compared with standard core decompression for avascular necrosis of the femoral head in sickle cell disease patients. Arch Orthop Trauma Surg. 2013;133(5):609–13.
Bellot F, Havet E, Gabrion A, Meunier W, Lestang MD. Core decompression of the femoral head for avascular necrosis. Rev Chir Orthop Reparatrice Appar Mot. 2005;91(2):114–23.
Keizer BS. Treatment of avascular necrosis of the hip by a non-vascularised cortical graft. J Bone Joint Surg (Br). 2006;88(4):460–6.
Mont MA, Carbone JJ, Fairbank AC. Core decompression versus nonoperative management for osteonecrosis of the hip. Clin Orthop Relat Res. 1996;324:169–78.
Song WS, Yoo JJ, Kim Y-M, Kim HJ. Results of multiple drilling compared with those of conventional methods of core decompression. Clin Orthop Relat Res. 2007;454:139–46.
Mont MA, Hungerford DS. Non-traumatic avascular necrosis of the femoral head. J Bone Joint Surg Am. 1995;77(3):459–74.
Joaquin MA, Arianna LG, Jordan CV, Amelia N, Joseph ML. Current concepts on osteonecrosis of the femoral head. World J Orthop. 2015;6(8):590–601.
Mohanty SP, Singh KA, Kundangar R, Shankar V. Management of non-traumatic avascular necrosis of the femoral head—a comparative analysis of the outcome of multiple small diameter drilling and core decompression with fibular grafting. Musculoskelet Surg. 2017;101(1):59–66.
Han Y, Zhenfeng Y, Dawei W. Multiple drilling combined with simvastatin versus multiple drilling alone for the treatment of avascular osteonecrosis of the femoral head: 3-year follow-up study. BMC Musculoskelet Disord. 2016;17(1):344.
Mont MA, Ragland PS, Etienne GJCO, Research R. Core decompression of the femoral head for osteonecrosis using percutaneous multiple small-diameter drilling. Clin Orthop Relat Res. 2004;429:131–8.
Castro FP Jr, Barrack RL. Core decompression and conservative treatment for avascular necrosis of the femoral head: a meta-analysis. Am J Orthop. 2000;29(3):187–94.
Okazaki S, Nagoya S, Katada R, Mizuo K, Sasaki. Inhibiton of IRF7 prevents developing corticosteroid-induced osteonecrosis of the femoral head. FASEB J. 2013;27:403–17.
Steinberg ME, Hayken GD, Steinberg DR. A quantitative system for staging avascular necrosis. J Bone Joint Surg (Br). 1995;77(1):34–41.
Urbaniak JR, Coogan PG, Gunneson EB, Nunley JA. Treatment of osteonecrosis of the femoral head with free vascularized fibular grafting. A long-term follow-up study of one hundred and three hips. J Bone Joint Surg Am. 1995;77(5):681–94.
Ohzono K, Saito M, Takaoka K, Ono K, Saito S, Nishina T, Kadowaki T. Natural history of nontraumatic avascular necrosis of the femoral head. J Bone Joint Surg (Br). 1991;73:68–72.
Koo KH, Kim R. Quantifying the extent of osteonecrosis of the femoral head. A new method using MRI. J Bone Joint Surg (Br). 1995;77(6):875–80.
Yoshida T, Kanayama Y, Okamura M, Negoro N, Yoshikawa J. Long-term observation of avascular necrosis of the femoral head in systemic lupus erythematosus: an MRI study. Clin Exp Rheumatol. 2002;20(4):525–30.
Sionek A, Czwojdziński A, Kowalczewski J, Okoń T, Marczak D, Sibiński M, Zlotorowicz M, Czubak J. Hip osteonecroses treated with calcium sulfate-calcium phosphate bone graft substitute have different results according to the cause of osteonecrosis: alcohol abuse or corticosteroid-induced. Int Orthop. 2018;42(7):1491–8.
Wang W, Liu L, Dang X, Ma S, Zhang M, Wang K. The effect of core decompression on local expression of BMP-2, PPAR-γ and bone regeneration in the steroid-induced femoral head osteonecrosis. BMC Musculoskelet Disord. 2012;13:142.
Hernigou P, Beaujean F, Lambotte JC. Decrease in the mesenchymal stem-cell pool in the proximal femur in corticosteroid-induced osteonecrosis. J Bone Joint Surg (Br). 1999;81:349–55.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (no. 81403027) and the Hubei Province Health and Family Planning Scientific Research Project (no. WJ2019Q051).
Funding
There was no external funding for this work.
Author information
Authors and Affiliations
Contributions
YT and HYH carried out the entire procedure including the literature search and data extraction. ZHW and JQ performed the statistical analysis, drafted the manuscript, and revised the submitted manuscript. LBC and HW conceived of the study, coordinated and participated in the entire process of drafting, and revised the manuscript. YXW and ZQP contributed to the statistical analysis and revision of the manuscript. All authors have contributed significantly. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The Ethics Committee of Zhongnan Hospital of Wuhan University approved this study, and all patients provided written informed consent.
Competing interests
There is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Tan, Y., He, H., Wan, Z. et al. Study on the outcome of patients with aseptic femoral head necrosis treated with percutaneous multiple small-diameter drilling core decompression: a retrospective cohort study based on magnetic resonance imaging and equivalent sphere model analysis. J Orthop Surg Res 15, 264 (2020). https://doi.org/10.1186/s13018-020-01786-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13018-020-01786-4