Abstract
Purpose
During orthodontic tooth movement, pressure and tension zones develop in the periodontal ligament, and periodontal ligament fibroblasts (PDLF) become exposed to mechanical strain. Enhanced salt (NaCl) concentrations are known to modulate responses of PDLF and immune cells to different stimuli like mechanical strain. Here, we investigated the impact of tensile strain on the gene expression profile of PDLF under normal (NS) and high salt (HS) conditions.
Methods
After preincubation under NS or HS (+40 mM NaCl in medium) conditions for 24 h, PDLF were stretched 16% for 48 h using custom-made spherical cap silicone stamps using an established and published setup. After determination of cell number and cytotoxicity, we analyzed expression of genes involved in extracellular matrix reorganization, angiogenesis, bone remodeling, and inflammation by quantitative real-time polymerase chain reaction (RT-qPCR).
Results
Tensile strain did not affect the expression of genes involved in angiogenesis or extracellular matrix reorganization by PDLF, which however modulate inflammatory responses and bone remodeling in reaction to 16% static tensile strain. Salt (NaCl) treatment triggered enhanced extracellular matrix formation, expression of cyclooxygenase 2 and bone metabolism in PDLF during tensile strain.
Conclusions
Salt (NaCl) consumption may influence orthodontic tooth movement and periodontal bone loss via modulation of extracellular matrix and bone metabolism. Excessive salt intake during orthodontic therapy may cause adverse effects regarding periodontal inflammation and bone resorption.
Zusammenfassung
Ziel
Während der kieferorthopädischen Zahnbewegung entwickeln sich Druck- und Zugzonen im Parodontalligament, und parodontale Ligamentfibroblasten (PDLF) werden mechanischer Belastung ausgesetzt. Es ist bekannt, dass erhöhte Salzkonzentrationen (NaCl) die Reaktionen von PDLF und Immunzellen auf verschiedene Stimuli wie mechanische Beanspruchung modulieren. Hier untersuchten wir den Einfluss von Dehnung auf das Genexpressionsprofil von PDLF unter Normal- (NS) und unter Hochsalzbedingungen (HS).
Methoden
Nach 24 h Vorinkubation unter NS- bzw. HS-Bedingungen (+40 mM NaCl im Medium) wurden PDLF 48 h lang unter Verwendung von Silikonstempeln unter Verwendung eines etablierten und veröffentlichten Protokolls um 16 % gestreckt. Nach Bestimmung der Zellzahl und der Zytotoxizität analysierten wir durch RT-qPCR („quantitative real-time polymerase chain reaction“) die Expression von Genen, die an der Reorganisation der extrazellulären Matrix, der Angiogenese, dem Knochenumbau und der Entzündung beteiligt sind.
Ergebnisse
Dehnung hatte keinen Einfluss auf die Expression von Genen, die an der Angiogenese oder der Reorganisation der extrazellulären Matrix durch PDLF beteiligt sind. In Reaktion auf statische Dehnung modulierten PDLF jedoch die Expression von Genen, die an Entzündungsreaktionen und am Knochenumbau beteiligt sind. Eine Behandlung mit Salz (NaCl) bewirkte während der Zugbelastung eine vermehrte Bildung von extrazellulärer Matrix sowie eine verstärkte Expression von Cyclooxygenase 2 und von Markern des Knochenmetabolismus durch PDLF.
Schlussfolgerungen
Salzkonsum kann die kieferorthopädische Zahnbewegung und den parodontalen Knochenverlust durch Modulation der extrazellulären Matrix und des Knochenstoffwechsels beeinflussen. Eine übermäßige Salzaufnahme während der kieferorthopädischen Therapie könnte daher nachteilige Auswirkungen auf parodontale Entzündungen und die Knochenresorption haben.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
During orthodontic tooth movement, pressure and tension zones develop in the periodontal ligament (PDL), a connective tissue responsible for the attachment of the tooth to the alveolar bone [25]. Periodontal ligament fibroblasts (PDLF) make up the majority of cells within the periodontal ligament and are the first cells exposed to mechanical stimuli occurring during orthodontic tooth movement. The main function of PDLF is the maintenance of tissue homeostasis and production of collagenous structural proteins and glycosaminoglycans. Furthermore, they sustain regulatory functions in innate immune defense [16, 25].
After an orthodontic force is applied to the tooth, PDLF are subjected to mechanical strain and play an important regulatory role in orthodontic tooth movement. As an early response to compressive forces, PDLF increase prostaglandin production via enhancement of cyclooxygenase 2 (COX-2) activity, resulting in enhanced expression of RANKL (receptor activator of NF-κB ligand) [16, 38, 48], while simultaneously secretion of RANKL decoy receptor osteoprotegerin (OPG) is reduced [38]. This promotes osteoclastogenesis in pressure areas of the PDL resulting in alveolar bone resorption. In contrast, in tension areas bone formation by osteoblastic activity is promoted [25].
Malocclusions have a negative impact on oral-health-related quality of life and mental well-being of children leading to reduced self-confidence [8, 42]. Often these psychological effects triggered by malocclusions are the reason to improve esthetics through orthodontic treatment [42]. Therapy of malocclusions is of distinct medical importance, as recent studies associated malpositioned teeth with the development of caries or periodontitis [2, 37, 41]. Therefore, orthodontic corrections are helpful to prevent the development and progression of these oral diseases. Despite the importance of orthodontic treatment for oral health, many aspects of orthodontic therapy remain uninvestigated, and many problems that arise during an ongoing orthodontic therapy are still unresolved.
Possible influences of nutrition on orthodontic treatment have hardly been investigated. Since orthodontic tooth movement comprises a local sterile-inflammatory process, numerous possibilities exist for the immune system and general metabolism to modulate these processes [18, 53]. Components of nutrition are reported to influence not only chronic diseases like hypertension [22, 23] or osteopenia [44], but also have an impact on the oral microflora [52] and periodontal bone loss [29]. In Western societies electrolytes such as sodium are consumed to a high degree as food supplements in the form of salt (sodium chloride, NaCl) and are known to modulate tissue response to different stimuli by their local tissue concentration [28]. It can be assumed that about 70–80% of the salt intake comes from “hidden” salts in processed foods such as cheese, bread, and ready-to-eat meals [6]. Most people in Europe consume significantly more salt (8–11 g/day) than recommended by the German Nutrition Society (1.5 g/day) [6, 51]. Therefore, it can be assumed that salt-related effects on orthodontic tooth movement in industrialized nations are relevant to the vast majority of patients.
Consumption of high salt diet or inflammation induces Na+ accumulation in various tissues, thereby, modulating the activity of cells of the mononuclear phagocytic system [3, 14, 22, 23]. Furthermore, Na+ accumulation may also occur in tissues of the oral cavity, especially the gingiva, the oral mucous membrane, and the periodontal ligament [39]. As salt (sodium chloride) is known to have a direct impact on the activity of cells of the mononuclear phagocytic system [14, 23, 32] and osteoclasts [54], it may also have an effect on the response of PDLF to tensile strain.
Materials and methods
In vitro cell culture experiments
All experiments were performed in accordance with the relevant guidelines and regulations. Approval for the collection and use of PDLF was obtained from the ethics committee of the University of Regensburg, Germany (approval number 12-170-0150). We obtained informed consent from all patients or their legal guardians.
Periodontal ligament fibroblasts (PDLF) were isolated from periodontal ligament tissue scraped off the middle third of human teeth. For these experiments we used a pool of PDLF from six different patients (3 male, 3 female, age range 17–27 years). Isolation and characterization was performed as previously described [17, 38]. For our experiments, we used PDLF of the 3rd to 6th passage. We determined cell number with a Beckman Coulter Counter Z2™ (Beckman Coulter GmbH, Krefeld, Germany) according to the manufacturer’s instructions.
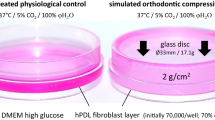
A total of 70,000 PDLF in 2 ml media (Dulbecco’s Modified Eagle Medium [DMEM] high glucose, D5796, Sigma-Aldrich, Munich, Germany); 10% FBS (fetal bovine serum, P30-3306, PAN-Biotech, Aidenbach, Germany), 1% L‑glutamine (SH30034.01, GE Healthcare Europe, Munich, Germany), 100 µM ascorbic acid (A8960, Sigma-Aldrich, Munich, Germany), and 1% antibiotics/antimycotics (A5955, Sigma-Aldrich, Munich, Germany) were seeded onto 6‑well collagen-I-coated bioflex plates (BF-3001C, Dunn Labortechnik, Asbach, Germany). After 24 h preincubation time without (normal salt [NS] conditions) or with addition of 40 mM NaCl (high salt [HS] conditions, 1162241000, Sigma-Aldrich, Munich, Germany), we performed 16% static isotropic cell stretching for an additional 48 h by using custom-made spherical cap silicone stamps (Fig. 1a) according to an established and published method [30] consisting of two-component silicone (43004,490068, Turbosil, Klasse 4, Dental GmbH, Augsburg, Germany; mixed 1:1 with Dosper evo, Dreve GmbH, Unna, Germany). In a previous study using the same setup, this tensile strain magnitude was shown to be the minimum magnitude to significantly affect the expression of proinflammatory genes in PDLF [30].
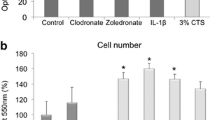
a In vitro simulation of tensile strain by isotropic stretching of adherently growing periodontal ligament fibroblasts (PDLF). Determination of cell number (b) and cytotoxicity by LDH assay (c). NS normal salt conditions, HS high salt conditions, AU arbitrary units, error bars error of the mean. Statistics: Analysis of variance (ANOVA) using the Games–Howell post hoc test: *p ≤ 0.05
a In-vitro-Simulation der Zugspannung durch isotrope Dehnung von adhärent wachsenden PDLF (parodontale Ligamentfibroblasten). Bestimmung der Zellzahl (b) und der Zytotoxizität durch LDH(Laktatdehydrogenase)-Assay (c). (NS Normalsalz-, HS Hochsalzbedingungen, AU arbiträre Einheiten, Fehlerbalken Fehler des Mittelwerts. Statistik: ANOVA („analysis of variance“) mit Games-Howell-Post-hoc-Test: *p ≤ 0,05)
Assessment of cell number
After 48 h of isotropic tensile strain, the medium was removed and PDLF were scraped off the bioflex membrane in 1 ml phosphate buffered saline (PBS) for cell number determination. Cells were counted automatically using a Beckman Coulter Counter Z2™ (Beckman Coulter GmbH, Krefeld, Germany) according to the manufacturer’s instructions.
LDH cytotoxicity assay
To test for cytotoxicity, we performed lactate dehydrogenase (LDH) assays (04744926001, Roche, Mannheim, Germany) using cell culture supernatants according to the manufacturer’s instructions. A total of 100 µl of cell culture supernatant was mixed with 100 µl freshly prepared LDH solution (consisting of 22 µl catalyst in 1 ml dye). After an incubation period of 30 min at room temperature in the dark, 50 µl stop solution was added and absorbance was measured at 490 nm using an ELISA reader (Multiscan GO Microplate Spectrophotometer, Thermo Fisher Scientific, Waltham, MA, USA), subtracting background absorbance at 690 nm.
RNA isolation and cDNA synthesis
RNA isolation was performed as previously described according to MIQE (Minimum Information for Publication of Quantitative Real-Time PCR Experiments) guidelines [17, 30]. A total of 500 µl peqGOLD TriFastTM (PEQLAB Biotechnology GmbH, Erlangen, Germany) was added per well and further processed according to the manufacturer’s instructions. The resulting RNA pellet was resuspended in 20 µl nuclease-free doubly distilled water (H2Odd; T143, Carl Roth, Karlsruhe, Germany). RNA was quantified using a NanoPhotometer (N60; Implen, Munich, Germany). A total of 100 ng RNA per sample was transcribed into cDNA using 1 µl oligo-dT18 primer (SO131, Thermo Fisher Scientific Inc., Waltham, MA, USA), 1 µl random hexamer primer (SO142, Thermo Fisher Scientific Inc.), 1 µl dNTP mix (L785.2, Roti®-Mix PCR3, Carl Roth), 1 µl RNase inhibitor (EO0381, Thermo Fisher Scientific Inc.), 1 µl MLV-reverse transcriptase (M1705, Promega, Fitchburg, WI, USA), 4 µl 5 × M-MLV-buffer (M1705, Promega) in a total volume of 20 µl by addition of nuclease-free H2Odd (T143, Carl Roth). Samples were incubated for 60 min at 37 °C and 2 min at 95 °C. Reverse transcription was performed for all samples at the same time to minimize experimental variation.
Quantitative real-time polymerase chain reaction
Quantitative real-time polymerase chain reaction (RT-qPCR) was performed according to MIQE guidelines [17, 30]. For RT-qPCR the Mastercycler® ep realplex‑S thermocycler (Eppendorf AG, Hamburg, Germany) was used in combination with 96-well PCR plates (TW-MT, 712282, Biozym Scientific GmbH, Hessisch Oldendorf, Germany) and BZO cover sheeting (712350, Biozym Scientific GmbH). Mastermix contained 7.5 µl SYBR®Green JumpStartTM Taq ReadyMixTM (S4438, Sigma-Aldrich, Munich, Germany), 0.75 µl of each primer in a total amount of 13.5 µl by addition of nuclease-free H2Odd (T143, Carl Roth, Karlsruhe, Germany) for each sample. Finally 1.5 µl cDNA in duplet per sample was added to the mastermix. RT-qPCR was performed in 45 cycles (initial: 5 min at 95 °C, each cycle: 10 s at 95 °C, 8 s at 60 °C, 8 s at 72 °C). At the end of each extension step SYBR®Green I fluorescence was measured at 521 nm. For calculation of relative gene expression, we used a set of two reference genes (TBP and PPIB), which have been shown to be stably expressed in PDLF under the conditions investigated [30]. Relative gene expression was calculated as 2−∆Cq with ∆Cq = Cq (target gene) − Cq (geometric mean TBP/PPIB) [21]. All primers (Eurofins MWG, Huntsville, AL, USA) are listed in Table 1 and were constructed using NCBI PrimerBLAST according to MIQE guidelines as previously described [17, 19, 30]. For each primer pair and RT-qPCR run, a no-template-control without cDNA was performed. Experiments were repeated two to three times (N = 2–3) with at least two to three biological replicates (n = 2–3).
Statistical methods
One-way analysis of variance (ANOVA) followed by Games–Howell post hoc tests was performed using GraphPad Prism version 8.0.0 for Windows (GraphPad Software, San Diego, CA, USA). Welch tests were performed in case of heterogeneity of variance. The significance level was set at p ≤ 0.05.
Results
Impact of tensile strain and sodium chloride on cell number and cytotoxicity
First, we assessed the PDLF number and possible cytotoxic effects after 48 h of tensile strain and 72 h of sodium chloride treatment. Tensile strain significantly increased cell numbers under normal salt treatment (NS, p = 0.035), while high salt treatment (HS; p = 0.036) with an additional 40 mM NaCl in the medium had no effect on cell number (Fig. 1b). Neither tension treatment nor addition of 40 mM NaCl showed any cytotoxic effects as no significantly increased LDH activity could be detected (p = 0.889) in the cell culture supernatant throughout the tested conditions (Fig. 1c).
Effects of tensile strain and sodium chloride on extracellular-matrix-forming genes
Next, we investigated expression of genes involved in remodeling and formation of the extracellular matrix (prolyl-4-hydroxylase‑1 [P4HA1], collagen-1-α‑2 [COL1A2], fibronectin1 [FN1], and matrix-metalloproteinase‑8 [MMP8]). Neither tensile strain nor salt treatment showed significant effects on the gene expression of P4HA1 (p = 0.553, Fig. 2a). In contrast, gene expression of COL1A2 (p = 0.038, Fig. 2b) and FN1 was significantly elevated under HS conditions (p = 0.024, Fig. 2c) without additional tensile strain. Tension had no significant effect on COL1A2 or FN1 gene expression under NS conditions (COL1A2: p = 0.120, FN1: p = 0.173) or under high salt conditions (COL1A2: p = 0.998, FN1: p = 0.780). Gene expression of MMP8 was elevated after addition of 40 mM NaCl without (p = 0.004) and with stretching (p < 0.001) of PDLF (Fig. 2d). Tensile strain itself had no significant effect on MMP8 gene expression levels (NS: p = 0.904, HS: p = 0.769).
Changes in expression of the extracellular-matrix-reorganizing genes P4HA1 (a), COL1A2 (b), FN1 (c), and MMP8 (d). NS normal salt conditions, HS high salt conditions, AU arbitrary units, error bars error of the mean. Statistics: Analysis of variance (ANOVA) using the Games-Howell post hoc test: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Veränderungen in der Expression der extrazellulären-Matrix-reorganisierenden Gene P4HA1 (a), COL1A2 (b), FN1 (c) und MMP8 (d). (NS Normalsalzbedingungen, HS Hochsalzbedingungen, AU arbiträre Einheiten, Fehlerbalken Fehler des Mittelwerts. Statistik: ANOVA („analysis of variance“) mit Games-Howell-Post-hoc-Test: *p ≤ 0,05, **p ≤ 0,01, ***p ≤ 0,001)
Effects of tensile strain and sodium chloride on angiogenetic and bone-forming genes
The vascular endothelial growth factor A (VEGFA) is involved in tissue neoformation and responsible for growth of blood vessels. Surprisingly, neither tensile strain (NS: p = 0.170, HS: p = 0.262) nor addition of NaCl (without tension: p = 0.972, tension: p = 0.979) showed a significant effect on gene expression of VEGFA (Fig. 3a), although an increase of VEGFA gene expression under tensile strain was observed by tendency. The alkaline phosphatase (ALP) gene is involved in bone formation. We observed a significant increase in ALP gene expression after tensile strain under NS conditions (p = 0.002, Fig. 3b). Treatment of PDLF with 40 mM NaCl also increased ALP gene expression significantly (p < 0.001). However, we no longer detected an increased ALP gene expression due to tensile strain under HS conditions (p = 0.312, Fig. 3b).
Changes in expression of the angiogenesis-inducing gene VEGFA (a) and the osteoblastogenesis-inducing gene ALP (b). NS normal salt conditions, HS high salt conditions, AU arbitrary units, error bars error of the mean. Statistics: Analysis of variance (ANOVA) using the Games–Howell post hoc test: **p ≤ 0.01, ***p ≤ 0.001
Veränderungen in der Expression des Angiogenese-induzierenden Gens VEGFA (a) und des Osteoblastogenese-induzierenden Gens ALP (b). (NS Normalsalzbedingungen, HS Hochsalzbedingungen, AU arbiträre Einheiten, Fehlerbalken Fehler des Mittelwerts. Statistik: ANOVA („analysis of variance“) mit Games-Howell-Post-hoc-Test: **p ≤ 0,01, ***p ≤ 0,001)
Effects of tensile strain and HS on proinflammatory genes
Next we focused on the gene expression of proinflammatory genes like cyclooxygenase 2 (COX‑2) and interleukin 6 (IL‑6). Tensile strain resulted in a significant increase of COX‑2 gene expression (p = 0.017, Fig. 4a), whereas IL‑6 gene expression was significantly reduced (p = 0.019, Fig. 4b) under NS conditions. Salt treatment enhanced COX‑2 gene expression (p < 0.001, Fig. 4a) and also reduced IL‑6 gene expression (p = 0.031, Fig. 4b) compared to NS conditions.
Changes in expression of the proinflammatory genes COX‑2 (a) and IL‑6 (b). NS normal salt conditions, HS high salt conditions, AU arbitrary units, error bars error of the mean. Statistics: Analysis of variance (ANOVA) using the Games–Howell post hoc test: *p ≤ 0.05, ***p ≤ 0.001
Veränderungen in der Expression der proinflammatorischen Gene COX‑2 (a) und IL‑6 (b). (NS Normalsalzbedingungen, HS Hochsalzbedingungen, AU arbiträre Einheiten, Fehlerbalken Fehler des Mittelwerts. Statistik: ANOVA („analysis of variance“) mit Games-Howell-Post-hoc-Test: *p ≤ 0,05, ***p ≤ 0,001)
Effects of cell stretching and salt treatment on the RANKL/OPG ratio
The RANKL/OPG ratio plays a major regulating role during bone resorption. Tensile strain reduced gene expression of RANKL significantly (p = 0.008, Fig. 5a), whereas OPG gene expression was not affected by PDLF stretching (p = 0.355, Fig. 5b). This resulted in a significantly reduced RANKL/OPG ratio (p = 0.044, Fig. 5c) during tensile strain under NS conditions. HS conditions increased RANKL gene expression without (p = 0.023) and with additional tensile strain (p < 0.001). OPG gene expression was also increased under HS conditions without tensile strain (p = 0.042, Fig. 5b), whereas OPG expression was not affected under HS conditions with tension treatment (p = 0.815). This led to a significantly increased RANKL/OPG ratio under HS conditions during tensile strain compared to NS conditions with cell stretching (p = 0.033, Fig. 5c).
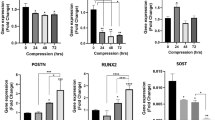
Changes in expression of the bone remodeling genes RANKL (a) and OPG (b) as well as RANKL/OPG ratio (c). NS normal salt conditions, HS high salt conditions, AU arbitrary units, error bars error of the mean. Statistics: Analysis of variance (ANOVA) using the Games–Howell post hoc test: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Veränderungen der Expression der am Knochenumbau beteiligten Gene RANKL (a) und OPG (b) sowie des RANKL/OPG-Verhältnisses (c). (NS Normalsalzbedingungen, HS Hochsalzbedingungen, AU arbiträre Einheiten, Fehlerbalken Fehler des Mittelwerts. Statistik: ANOVA („analysis of variance“) mit Games-Howell-Post-hoc-Test: *p ≤ 0,05, **p ≤ 0,01, ***p ≤ 0,001)
Discussion
In this study, we investigated the effects of tensile strain and salt (sodium chloride) on the expression levels of genes involved in extracellular matrix reorganization, angiogenesis, bone remodeling, and inflammation in PDLF. We could show that application of tension resulted in a reduced RANKL/OPG ratio, which was accompanied by enhanced ALP gene expression indicating elevated bone formation. Tensile strain increased COX‑2, but concurrently reduced IL‑6 gene expression. Surprisingly, we detected no effects of tension on genes involved in extracellular matrix remodeling or angiogenesis, whereas salt had a significant impact.
During orthodontic tooth movement, PDLF are suspected to be involved in extracellular matrix remodeling especially in the formation and breakdown of collagen fibrils [25]. For that reason, we analyzed expression of genes involved in collagen formation (COL1A2, P4HA1) and degradation (MMP8), but also fibronectin 1 (FN1), which interacts with collagen and other molecules of the extracellular matrix like heparin sulfate and serves as an adhesion molecule [36]. Furthermore, FN1 has already been associated before with extracellular matrix remodeling during orthodontic tooth movement [1]. We detected no changes in expression of genes involved in collagen synthesis after application of tension. Howard et al. reported increased FN1 expression after 10% cyclic tensile strain; however, COL1 expression was not changed by PDLF stretching [11], supporting our data. A recent study investigated collagen and fibronectin expression in histological samples. They observed a downregulation of FN1, while COL1 was upregulated at the tension side [26]. Compressive force treatment was reported to affect collagen formation within 24 h because of increased gene expression of COL1A2 and P4HA1 [38]. In contrast to genes involved in collagen formation, FN1 was not affected by compressive force treatment [38]. MMPs are proteolytic enzymes, which degenerate different components of the extracellular matrix [4]. In this study we investigated the gene expression of MMP8, which acts as collagenase and is expressed by PDLF [46]. Contrary to our results it was reported that collagenases like MMP8 were upregulated by tensile forces with the strength of the tensile strain playing a crucial role [5, 13, 31], whereas MMP8 was downregulated after compressive force treatment in PDLF [39, 43]. In the current study, salt (sodium chloride) treatment affected gene expression of COL1A2, FN1 and MMP8 in PDLF, as reported previously [39]. Salt consumption has already been reported to be involved in extracellular matrix reorganization, as it impacts on glycosaminoglycan sulfatation [45, 49].
Application of orthodontic forces changes the blood flow in the surrounding tissue. To avoid hypoxic conditions, vascular endothelial growth factor A (VEGFA) expression is induced in the periodontal ligament (PDL) due to mechanical strain. VEGFA is a growth factor involved in the reshaping of blood vessels and angiogenesis [7]. Increased VEGFA expression was reported at compression and tension areas of the PDL in histological samples after tooth movement [27]. In this study, however, we detected no significant effect of tensile strain or salt on VEGFA gene expression. As increased VEGFA gene expression, however, occurred quite early after the onset of mechanical strain [38], our timing of detection might have been too late, as we analyzed VEGFA gene expression not earlier than after 48 h of tensile strain.
According to the common pressure–tension theory during orthodontic tooth movement, bone resorption happens at the pressure areas, while bone formation occurs at tension areas of the PDL [25]. Alkaline phosphatase (ALP) activity is elevated in the periodontal ligament compared to other connective tissues and is associated with bone formation [10]. In line with our data, static and cyclic tensile strain increased ALP expression dependent on the applied magnitude of tensile strain [12, 30, 31, 50], which may enhance the osteoblastic phenotype of PDLF and prompt bone formation [12, 55]. Furthermore, increased ALP levels were observed in human crevicular fluid after orthodontic treatment [15, 24, 35]. Salt treatment enhanced ALP gene expression, suggesting that NaCl promotes an osteoblastic phenotype of PDLF.
PDLF modulate the expression of proinflammatory genes in reaction to orthodontic forces [16, 30, 38]. In this study gene expression of COX‑2 was increased after 48 h of tensile strain. This was in line with Shimizu et al. who reported that enhanced COX‑2 expression was accompanied by increased PG-E2 levels in PDLF after stimulation with cyclic stretching [40]. As already reported, salt treatment of PDLF also enhanced COX‑2 gene expression [39]. As it is well established that NaCl increases expression of the osmoprotective transcription factor NFAT5 [23, 33] and that COX‑2 is an NFAT5 target gene [9], this is not by surprise. In contrast to COX‑2, gene expression of IL‑6 was reduced with tension treatment and NaCl addition. This is in line with prior publications reporting simultaneous increase of COX‑2 and reduction of IL‑6 expression upon tensile strain [30, 39]. IL‑6 modulates the extent of immune responses during inflammation [34] and can influence osteoclastogenesis [20]. Reduction of IL‑6 expression after stretching and NaCl could contribute to the osteoblastic phenotype of PDLF.
Bone metabolism strongly depends on the interaction of RANKL (receptor activator of NF-κB ligand) and OPG (osteoprotegerin) [47]. While binding of RANKL to the RANK receptor on osteoclast precursor cells is critical for osteoclast formation and activation, secretion of the decoy receptor OPG inhibits this interaction [47]. In contrast to pressure application [38, 39], tensile strain resulted in reduced RANKL expression, while OPG gene expression remained unaffected. This resulted in a shifting of the RANKL/OPG ratio towards OPG suggesting less bone resorption. As already reported, salt treatment increased gene expression of RANKL and OPG in PDLF without tensile strain [39]. In contrast to the normal salt-treated PDLFs, we observed a reduction of OPG gene expression under high salt treatment with additional tensile strain, resulting in an increased RANKL/OPG ratio upon salt treatment with stretching. Therefore salt, that is sodium chloride, may modulate bone metabolism at the tension site as well.
For our in vitro experiments, we used salt concentrations (40 mM) corresponding to the local Na+ accumulation measured under high salt diet in the murine mandible including the associated mucosa [39] to maximize transferability of results to the in vivo situation within the PDL and surrounding alveolar bone. The addition of 40 mM NaCl to the cell culture medium did have an impact on the expression of genes involved in extracellular matrix and bone remodeling as well as prostaglandin synthesis supporting previous results [39]. A high salt environment in combination with force application affected the RANKL/OPG ratio under tensile strain as well as during compressive force treatment, indicating a stimulating role of salt on osteoclastogenesis and thereby bone resorption [39]. To further investigate the role of salt on orthodontic tooth movement, in vivo experiments with animals receiving low, normal, and high salt diets with and without orthodontic tooth movement are required. Based on our in vitro results, we surmise that increased sodium concentrations due to high salt intake or possibly a local therapeutic injection into the periodontal ligament may accelerate orthodontic tooth movement due to an increase in osteoclastogenesis in pressure areas as well as elevated osteoblastic activity in tensile areas, but this might also have detrimental effects such as periodontal bone loss or dental root resorptions, which needs to be clarified in further in vivo studies.
Conclusions
-
Salt (NaCl) treatment has an impact on extracellular matrix formation, expression of proinflammatory cytokines and bone metabolism during tensile strain in PDLF (periodontal ligament fibroblasts).
-
Additional NaCl exposure increased ALP (alkaline phosphatase) expression by PDLF and could thereby promote bone formation at tension areas of the PDL (periodontal ligament).
-
Excessive salt intake during orthodontic therapy may cause stimulatory effects on periodontal inflammation and bone resorption, possibly leading to increased tooth movement, but also periodontal bone loss and dental root resorptions.
-
Tensile strain did not affect expression of genes involved in angiogenesis or extracellular matrix reorganization in PDLFs.
-
PDLFs modulate inflammatory responses and bone remodeling in reaction to static tensile strain.
Change history
25 October 2021
A Correction to this paper has been published: https://doi.org/10.1007/s00056-021-00362-7
References
Anastasi G, Cordasco G, Matarese G et al (2008) An immunohistochemical, histological, and electron-microscopic study of the human periodontal ligament during orthodontic treatment. Int J Mol Med 21:545–554
Bernhardt O, Krey K‑F, Daboul A et al (2019) New insights in the link between malocclusion and periodontal disease. J Clin Periodontol 46:144–159
Binger KJ, Gebhardt M, Heinig M et al (2015) High salt reduces the activation of IL-4- and IL-13-stimulated macrophages. J Clin Invest 125:4223–4238
Birkedal-Hansen H, Moore WG, Bodden MK et al (1993) Matrix metalloproteinases: a review. Crit Rev Oral Biol Med 4:197–250
Bolcato-Bellemin AL, Elkaim R, Abehsera A et al (2000) Expression of mRNAs encoding for alpha and beta integrin subunits, MMPs, and TIMPs in stretched human periodontal ligament and gingival fibroblasts. J Dent Res 79:1712–1716
Deutsche Gesellschaft für Ernährung e.V. (DGE) (2017) https://www.dge.de/presse/pm/dge-aktualisiert-die-referenzwerte-fuer-natrium-chlorid-und-kalium/
Di Domenico M, D’apuzzo F, Feola A et al (2012) Cytokines and VEGF induction in orthodontic movement in animal models. J Biomed Biotechnol 2012:201689
Dutra SR, Pretti H, Martins MT et al (2018) Impact of malocclusion on the quality of life of children aged 8 to 10 years. Dental Press J Orthod 23:46–53
Favale NO, Casali CI, Lepera LG et al (2009) Hypertonic induction of COX2 expression requires TonEBP/NFAT5 in renal epithelial cells. Biochem Biophys Res Commun 381:301–305
Grundt A, Grafe IA, Liegibel U et al (2009) Direct effects of osteoprotegerin on human bone cell metabolism. Biochem Biophys Res Commun 389:550–555
Howard PS, Kucich U, Taliwal R et al (1998) Mechanical forces alter extracellular matrix synthesis by human periodontal ligament fibroblasts. J Periodontal Res 33:500–508
Jacobs C, Grimm S, Ziebart T et al (2013) Osteogenic differentiation of periodontal fibroblasts is dependent on the strength of mechanical strain. Arch Oral Biol 58:896–904
Jacobs C, Walter C, Ziebart T et al (2014) Induction of IL‑6 and MMP‑8 in human periodontal fibroblasts by static tensile strain. Clin Oral Investig 18:901–908
Jantsch J, Schatz V, Friedrich D et al (2015) Cutaneous Na+ storage strengthens the antimicrobial barrier function of the skin and boosts macrophage-driven host defense. Cell Metab 21:493–501
Jeyraj Y, Katta AK, Vannala V et al (2015) Estimation of alkaline phosphatase in the gingival crevicular fluid during orthodontic tooth movement in premolar extraction cases to predict therapeutic progression. J Nat Sci Biol Med 6:343–346
Kanzaki H, Chiba M, Shimizu Y et al (2002) Periodontal ligament cells under mechanical stress induce osteoclastogenesis by receptor activator of nuclear factor kappaB ligand up-regulation via prostaglandin E2 synthesis. J Bone Miner Res 17:210–220
Kirschneck C, Batschkus S, Proff P et al (2017) Valid gene expression normalization by RT-qPCR in studies on hPDL fibroblasts with focus on orthodontic tooth movement and periodontitis. Sci Rep 7:14751
Kirschneck C, Maurer M, Wolf M et al (2017) Regular nicotine intake increased tooth movement velocity, osteoclastogenesis and orthodontically induced dental root resorptions in a rat model. Int J Oral Sci 9:174–184
Kirschneck C, Proff P, Fanghänel J et al (2016) Reference genes for valid gene expression studies on rat dental, periodontal and alveolar bone tissue by means of RT-qPCR with a focus on orthodontic tooth movement and periodontitis. Ann Anat 204:93–105
Kurihara N, Bertolini D, Suda T et al (1990) IL‑6 stimulates osteoclast-like multinucleated cell formation in long term human marrow cultures by inducing IL‑1 release. J Immunol 144:4226–4230
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(‑Delta Delta C(T)) Method. Methods 25:402–408
Machnik A, Dahlmann A, Kopp C et al (2010) Mononuclear phagocyte system depletion blocks interstitial tonicity-responsive enhancer binding protein/vascular endothelial growth factor C expression and induces salt-sensitive hypertension in rats. Hypertension 55:755–761
Machnik A, Neuhofer W, Jantsch J et al (2009) Macrophages regulate salt-dependent volume and blood pressure by a vascular endothelial growth factor-C-dependent buffering mechanism. Nat Med 15:545–552
Megat Abdul Wahab R, Md Dasor M, Senafi S et al (2013) Crevicular alkaline phosphatase activity and rate of tooth movement of female orthodontic subjects under different continuous force applications. Int J Dent 2013:245818
Meikle MC (2006) The tissue, cellular, and molecular regulation of orthodontic tooth movement: 100 years after Carl Sandstedt. Eur J Orthod 28:221–240
Militi A, Cutroneo G, Favaloro A et al (2019) An immunofluorescence study on VEGF and extracellular matrix proteins in human periodontal ligament during tooth movement. Heliyon 5:e2572
Miyagawa A, Chiba M, Hayashi H et al (2009) Compressive force induces VEGF production in periodontal tissues. J Dent Res 88:752–756
Müller DN, Wilck N, Haase S et al (2019) Sodium in the microenvironment regulates immune responses and tissue homeostasis. Nat Rev Immunol 19:243–254
Muluke M, Gold T, Kiefhaber K et al (2016) Diet-induced obesity and its differential impact on periodontal bone loss. J Dent Res 95:223–229
Nazet U, Schröder A, Spanier G et al (2019) Simplified method for applying static isotropic tensile strain in cell culture experiments with identification of valid RT-qPCR reference genes for PDL fibroblasts. Eur J Orthod. https://doi.org/10.1093/ejo/cjz052
Nettelhoff L, Grimm S, Jacobs C et al (2016) Influence of mechanical compression on human periodontal ligament fibroblasts and osteoblasts. Clin Oral Investig 20(3):621–629
Neubert P, Weichselbaum A, Reitinger C et al (2019) HIF1A and NFAT5 coordinate Na+-boosted antibacterial defense via enhanced autophagy and autolysosomal targeting. Autophagy 15:1899–1916
Neuhofer W, Woo SK, Na KY et al (2002) Regulation of TonEBP transcriptional activator in MDCK cells following changes in ambient tonicity. Am J Physiol Cell Physiol 283:C1604–C1611
Okada N, Kobayashi M, Mugikura K et al (1997) Interleukin‑6 production in human fibroblasts derived from periodontal tissues is differentially regulated by cytokines and a glucocorticoid. J Periodont Res 32:559–569
Perinetti G, Paolantonio M, D’Attilio M et al (2002) Alkaline phosphatase activity in gingival crevicular fluid during human orthodontic tooth movement. Am J Orthod Dentofacial Orthop 122:548–556
Romberger DJ (1997) Fibronectin. Int J Biochem Cell Biol 29:939–943
Sá-Pinto AC, Rego TM, Marques LS et al (2018) Association between malocclusion and dental caries in adolescents: a systematic review and meta-analysis. Eur Arch Paediatr Dent 19:73–82
Schröder A, Bauer K, Spanier G et al (2018) Expression kinetics of human periodontal ligament fibroblasts in the early phases of orthodontic tooth movement (Expression kinetics of human periodontal ligament fibroblasts in the early phases of orthodontic tooth movement). J Orofac Orthop 79:337–351. https://doi.org/10.1007/s00056-018-0145-1
Schröder A, Nazet U, Neubert P et al (2019) Sodium-chloride-induced effects on the expression profile of human periodontal ligament fibroblasts with focus on simulated orthodontic tooth movement. Eur J Oral Sci 127:386–395
Shimizu N, Ozawa Y, Yamaguchi M et al (1998) Induction of COX‑2 expression by mechanical tension force in human periodontal ligament cells. J Periodontol 69:670–677
Staufer K, Landmesser H (2004) Effects of crowding in the lower anterior segment—a risk evaluation depending upon the degree of crowding. J Orofac Orthop 65:13–25
Taibah SM, Al-Hummayani FM (2017) Effect of malocclusion on the self-esteem of adolescents. J Orthod Sci 6:123–128
Takahashi I, Nishimura M, Onodera K et al (2003) Expression of MMP‑8 and MMP-13 genes in the periodontal ligament during tooth movement in rats. J Dent Res 82:646–651
Titze J, Rittweger J, Dietsch P et al (2004) Hypertension, sodium retention, calcium excretion and osteopenia in Dahl rats. J Hypertens 22:803–810
Titze J, Shakibaei M, Schafflhuber M et al (2004) Glycosaminoglycan polymerization may enable osmotically inactive Na+ storage in the skin. Am J Physiol Heart Circ Physiol 287:H203–H208
Tsubota M, Sasano Y, Takahashi I et al (2002) Expression of MMP‑8 and MMP-13 mRNAs in rat periodontium during tooth eruption. J Dent Res 81:673–678
Tyrovola JB, Spyropoulos MN, Makou M et al (2008) Root resorption and the OPG/RANKL/RANK system: a mini review. J Oral Sci 50:367–376
Ullrich N, Schröder A, Jantsch J et al (2019) The role of mechanotransduction versus hypoxia during simulated orthodontic compressive strain-an in vitro study of human periodontal ligament fibroblasts. Int J Oral Sci 11:33
Volpi N, Maccari F, Titze J (2005) Simultaneous detection of submicrogram quantities of hyaluronic acid and dermatan sulfate on agarose-gel by sequential staining with toluidine blue and Stains-All. J Chromatogr B Analyt Technol Biomed Life Sci 820:131–135
Wescott DC, Pinkerton MN, Gaffey BJ et al (2007) Osteogenic gene expression by human periodontal ligament cells under cyclic tension. J Dent Res 86:1212–1216
WHO (2012) WHO guideling: sodium intake for adults and children. ISBN: 9789241504836
Woelber JP, Bremer K, Vach K et al (2016) An oral health optimized diet can reduce gingival and periodontal inflammation in humans—a randomized controlled pilot study. BMC Oral Health 17:28
Wolf M, Lossdörfer S, Römer P et al (2016) Short-term heat pre-treatment modulates the release of HMGB1 and pro-inflammatory cytokines in hPDL cells following mechanical loading and affects monocyte behavior. Clin Oral Investig 20:923–931
Wu L, Luthringer BJC, Feyerabend F et al (2017) Increased levels of sodium chloride directly increase osteoclastic differentiation and resorption in mice and men. Osteoporos Int 28:3215–3228
Yu H‑S, Kim J‑J, Kim H‑W et al (2016) Impact of mechanical stretch on the cell behaviors of bone and surrounding tissues. J Tissue Eng. https://doi.org/10.1177/2041731415618342
Acknowledgements
The authors wish to thank Ms. Zaglauer for her technical support. The authors want to thank the German Orthodontic Society (DGKFO, Kirschneck 2018) for their support and the German Research Foundation DFG (SCHR 1622/1‑1 and KI 2105/2-1) for funding of this study.
Funding
This study was funded by the German Research Foundation DFG (SCHR 1622/1‑1 and KI 2105/2-1).
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. Schröder, J. Gubernator, U. Nazet, G. Spanier, J. Jantsch, P. Proff and C. Kirschneck report no financial or other conflict of interest relevant to this article, which is the intellectual property of the authors.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Approval for the collection and usage of periodontal ligament fibroblasts was obtained from the ethics committee of the University of Regensburg, Germany (approval number 12-170-0150). This article does not contain any studies with animals.
Additional information
The original online version of this article was revised due to a retrospective Open Access order.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schröder, A., Gubernator, J., Nazet, U. et al. Effects of sodium chloride on the gene expression profile of periodontal ligament fibroblasts during tensile strain. J Orofac Orthop 81, 360–370 (2020). https://doi.org/10.1007/s00056-020-00232-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00056-020-00232-8
Keywords
- Periodontal ligament fibroblast
- Periodontal ligament (PDL)
- Orthodontic tooth movement
- Tensile strain
- Expression kinetics