Abstract
Aeromonas species (spp.) are well-known fish pathogens, several of which have been recognized as emerging human pathogens. The organism is capable of causing a wide spectrum of diseases in humans, ranging from gastroenteritis, wound infections, and septicemia to devastating necrotizing fasciitis. The systemic form of infection is often fatal, particularly in patients with underlying chronic diseases. Indeed, recent trends demonstrate rising numbers of hospital-acquired Aeromonas infections, especially in immuno-compromised individuals. Additionally, Aeromonas-associated antibiotic resistance is an increasing challenge in combating both fish and human infections. The acquisition of antibiotic resistance is related to Aeromonas’ innate transformative properties including its ability to share plasmids and integron-related gene cassettes between species and with the environment. As a result, alternatives to antibiotic treatments are desperately needed. In that vein, many treatments have been proposed and studied extensively in the fish-farming industry, including treatments that target Aeromonas quorum sensing. In this review, we discuss current strategies targeting quorum sensing inhibition and propose that such studies empower the development of novel chemotherapeutic approaches to combat drug-resistant Aeromonas spp. infections in humans.
Key points
• Aeromonas notoriously acquires and maintains antimicrobial resistance, making treatment options limited.
• Quorum sensing is an essential virulence mechanism in Aeromonas infections.
• Inhibiting quorum sensing can be an effective strategy in combating Aeromonas infections in animals and humans.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Aeromonas species (spp.) are ubiquitous in nature predominately found in freshwater habitats and estuarine ecosystems. The organism commonly infects fish, amphibians, and reptiles, wreaking havoc on the fish-farming industry. The first documented case of a human Aeromonas infection was recorded in 1951 when the organism was cultured from cerebral spinal fluid during a patient’s autopsy in Jamaica (Caselitz 1996). Since this landmark case, 36 spp. have been added to the genus, and at least 19 of them have been classified as emerging human pathogens (Fernández-Bravo and Figueras 2020). Unlike many other human pathogens, Aeromonas spp. are unique in their ability to inhabit an enormous range of hosts. In addition to humans, they have been isolated from leeches, insects, mollusks, birds, livestock, fresh produce, preserved food, domestic animals, drinking water, and wastewater sludge (Didugu et al. 2015; Govender et al. 2021; Janda and Abbott 2010; McMahon and Wilson 2001; Wang et al. 2011; Wu et al. 2019). The organism’s ability to grow at refrigeration temperatures is an added concern in the food industry (Hoel et al. 2019). Alarmingly, human Aeromonas infections are not associated with just one predictable tissue type or set of symptoms but rather have been implicated in an impressive array of clinical syndromes including wound/soft tissue infections, septicemia/bacteremia, gastroenteritis, colitis, intraabdominal infections/peritonitis, urinary tract infections, pneumonia, and even dreaded necrotizing fasciitis (Janda and Abbott 2010). Historically, symptomatic infections have mostly been associated with immuno-compromised patients, and a number of comorbidities are commonly correlated with severe infection, mostly liver disease (Clark and Chenoweth 2003; Valcarcel et al. 2021; Xu et al. 2022). While the majority of Aeromonas research is focused on aquaculture and relieving the economic burden of fish disease, there is a pressing need to understand this pathogen in a human-disease context and to innovate and develop novel, clinically relevant treatments as antimicrobial resistance (AMR) continues to spread in this pathogen.
Overuse/misuse of antibiotics, both clinically and commercially, has accelerated AMR development world-wide in a large number of human bacterial pathogens. This has resulted in bacterial infections that are increasingly difficult to treat, leading to higher mortality rates and longer hospital stays (Orosz et al. 2022; Wagenlehner and Dittmar 2022). The seemingly unchecked emergence of AMR pathogens poses a significant global threat to public health, prompting the need for a better understanding of the molecular mechanisms of resistance and the development of novel countermeasures. Aeromonas spp. are no exception to this emerging trend and have demonstrated their ability to rapidly acquire and share new AMR genes. Identifying/developing solutions to this problem requires a multifaceted approach including achieving a better understanding of Aeromonas spp. acquisition and retention of AMR genes, as well as identifying and characterizing virulence factors/mechanisms as potential drug targets. One promising antibiotic-alternative drug target is quorum sensing (QS), an essential virulence mechanism for Aeromonas spp. during human infections.
Antibiotic resistance in Aeromonas: an ongoing problem
Considering Aeromonas’ pervasiveness in both ecological and clinical environments, promiscuity, and ability to cope with (and endure) environmental stressors, it should not be overlooked as a potentially significant source and/or reservoir of clinically relevant AMR genes. AMR mechanisms, particularly the presence of ß-lactams, including carbapenemases (Hayes et al. 1994, 1996), have been well characterized in Aeromonas spp. over the years. Chromosomally encoded ß-lactams were among the first to be detected and genetically characterized in Aeromonas (Iaconis and Sanders 1990; Ko et al. 1998; Walsh et al. 1997). Today, AMR genes that encode penicillinases, cephalosporinases, and metallo-ß-lactamases are of common occurrence in many Aeromonas spp. (Nwaiwu and Aduba 2020; Pourmohsen et al. 2023; Hilt et al. 2020). AMR genes do not observably accumulate in one species of Aeromonas more than another (Bertran et al. 2021). This is, in part, due to the fact that accurate identification of Aeromonas on a species level is historically problematic due to standard diagnostic techniques that are not tailored to Aeromonas spp. and shifting taxonomic definitions (Zhang et al. 2023; Fernández-Bravo and Figueras 2020). For example, A. dhakensis is being reevaluated in recent years for clinical significance, especially as a culprit in monomicrobial, systemic infections because of frequent misidentification as A. hydrophila (Wu et al. 2015, Puah et al. 2022). These factors combine to make studying species-specific AMR trends difficult.
Importantly, clinical AMR Aeromonas strains have been isolated across the globe; 3rd-generation cephalosporin-resistant Aeromonas has been isolated in Southern India (Bhaskar et al. 2015), and 3rd-generation cephalosporin and carbapenem-resistant isolates have been found in Croatia (Drk et al. 2023). Two broad-spectrum carbapenemase KPC-24-producing A. veronii strains were isolated recently from hospital sewage in China (Yang et al. 2022). Indeed, AMR profiles have been characterized in Aeromonas spp. isolated from India (Indra et al. 2015), including North Bengal (Dey Bhowmick and Bhattacharjee 2017), Tunisia (Bargui et al. 2023), Egypt (El-Hossary et al. 2023), Thailand (Hatrongjit et al. 2020), European countries, and Brazil, just to name a few (Table 1). Sequence analysis of nine independent A. veronii isolates from fish, humans, and Brazilian environments found all isolates to be remarkably similar to the uploaded Aeromonas genomes found in NCBI, demonstrating that widespread distribution of AMR genes in Aeromonas can originate from vastly different sources and geographic locations (Maia et al. 2023). Environmental isolates unassociated with human/clinical disease also demonstrate an alarmingly high rate of AMR. This suggests a possible ecological reservoir of AMR genes with the potential to be transferred to human-associated strains (Canellas et al. 2023; Goñi-Urriza et al. 2000; Igbinosa et al. 2015). It is clear that Aeromonas spp. are formidable enemies capable of horizontally spreading AMR genes, and it is important to understand how and why such propensity for AMR acquisition and retention exists.
Sources and selective pressures for AMR acquisition
As alluded to earlier, one commonly studied mechanism of AMR acquisition in Aeromonas is horizontal gene transfer from other bacteria. A. caviae, for example, has been shown to be naturally competent and readily acquires DNA from its environment (Sayeed et al. 1996). In one study, 73% of environmental Aeromonas isolates were able to serve as recipients of donor DNA, while 100% of tested isolates were able to act as donors to at least some other aeromonads under optimal laboratory conditions (Tris buffer with magnesium or calcium, pH 5–8, and a saturating concentration of 0.5 μg of DNA per assay, at 30 °C; sodium was also required) (Huddleston et al. 2013). On account of this naturally transformative state, it is no surprise that so many AMR genes have been found in Aeromonas spp. that are derived from other common but unrelated pathogens. For example, a Verona integron-encoded family metallo-β-lactamase (VIM) producing A. hydrophila strain carrying a VIM-4 gene was described in a case report from Budapest in 2008. Sequencing showed an identical match to a previously characterized integron in Pseudomonas aeruginosa from southern Hungary, suggesting DNA transfer between the two (Libisch et al. 2008). Temoniera-24 (TEM-24), a prominent extended-spectrum β-lactamase gene variant, was observed in a clinical isolate of Aeromonas for the first time in 2003. TEM-24 is typically isolated across Western Europe from Enterobacter spp. and Pseudomonas spp., and since this particular Aeromonas spp. was isolated alongside Enterobacter aerogenes, this also suggests cross-species horizontal AMR gene acquisition (Marchandin et al. 2003).
Another mechanism that could be promoting the alarming rate of AMR acquisition is the presence of AMR genes in the context of mobile genetic elements (MGE) such as plasmids and integrons. Aeromonas spp. are known to possess a collection of plasmids constituting its plasmidome. The Aeromonas plasmidome is of particular interest in the context of AMR genes and other virulence factors (Vincent et al. 2021). Virulence-related plasmids released by bacterial cells have been shown to persist in harsh environments such as treated wastewater and can readily be acquired by nearby pathogens (Drk et al. 2023). Additionally, integrons, small sections of chromosome that can capture gene cassettes from the environment and incorporate them into the genome via integrase genes and site-specific recombination, have been found to play an important role in the acquisition and spread of antibiotic resistance genes (Fluit and Schmitz 1999). Such integrons have been found within multiple species of the Aeromonas genus. Characterization of 133 Aeromonas spp. isolates (50 A. caviae, 45 A. hydrophila, 31 A. sobria, 6 A. encheleia, and 1 A. veronii) revealed the presence of several different class I integrons, including 10 different gene cassettes, encoding resistance to a variety of antibiotics including trimethoprim, aminoglycosides, ß-lactams, and phenicol. As to be expected, antibiotic resistance rates were different between integron-positive and integron-negative strains. Specifically, resistance to trimethoprim and trimethoprim–sulphamethoxazole was more commonly associated with integron-positive isolates, and all integron-positive isolates were resistant to more than 3 antibiotics. In fact, resistance to as many as 10 antimicrobial chemotherapeutics was observed in some integron-positive strains (Chang et al. 2007). Additionally, a global study of 38 A. salmonicida isolates revealed that 21/38 isolates contained a class I integron with all gene cassettes described in the study being associated with human bacterial infections (L'Abée-Lund and Sørum 2001).
Non-pathogenic, environmental/aquatic Aeromonas spp. have also proven to be significant sources/reservoirs of AMR gene acquisition of clinically relevant strains. In one such example, the transfer of oxytetracycline-resistant plasmids between Aeromonas spp. found in fish hatcheries and Aeromonas spp. recovered from hospital effluent was observed in A. hydrophila (8 isolates), A. sobria (6 isolates), and A. caviae (1 isolate) (Rhodes et al. 2000). Additionally, A. veronii isolated from catfish ponds in the South-Eastern USA was found to harbor tetracycline resistance gene on a MGE, similar to ones found in Vibrio parahaemolyticus and other Aeromonas spp. isolated from human stool (Dubey et al. 2023). When 66 Aeromonas isolates [A. caviae (58%), A. hydrophila (17%), A. media (11%), and A. veronii (11%)] from both untreated hospital wastewater and treated municipal water were examined, almost all of them (65/66) demonstrated multidrug-resistant phenotypes. Prevalent carbapenem genes found among the isolates included blaKPC-2, blaVIM-2, blaOXA-48, and blaIMP-13, with the latter three being described for the first time in Aeromonas. This same study demonstrated the ability of some of these Aeromonas isolates to transfer these resistance phenotypes to susceptible recipients (Escherichia coli), suggesting conventionally treated municipal and untreated hospital wastewater may be a reservoir for AMR, and that Aeromonas spp. could be mediating the spread of AMR to other pathogens in that environment (Drk et al. 2023). By demonstrating overlap between aquatic and clinical Aeromonas spp., these findings warn of the perils of compartmentalizing human and agricultural/environmental niches and conversely suggest that they should be considered as one combined environment since the transfer of genetic information can occur between them (Jones et al. 2023). Roh and Kannimuthu (2023) in a recent genomic analysis of the resistomes of 400 Aeromonas aquaculture strains found resistance against carbapenem, fluoroquinolone, cephalosporin, elfamycin, aminoglycoside, and tetracycline was “more or less evenly distributed across all species, while resistance against the other classes varied between species” (Roh and Kannimuthu 2023). This distribution highlights the genetic promiscuity displayed by Aeromonas across species and underscores its potentially global relevance as an indicator organism of the spread of antibiotic resistance (Usui et al. 2016).
Mechanisms of Aeromonas-associated drug resistance
Aeromonas employs a multivariate platform of strategies that confer antimicrobial resistance. One such strategy is through the exploitation of escape mutations in genes encoding the protein targets of the antibiotics. For example, quinolone resistance observed in an A. caviae human isolate was a result of an accumulation of point mutations in the type II topoisomerase genes gyrA and parC allowing for the continued function of the enzymes while reducing antibiotic binding affinity (Sinha et al. 2004). Another AMR mechanism employed by Aeromonas is the use of substrate-specific antibiotic degrading enzymes such as ß-lactamases (Majiduddin et al. 2002; Rasmussen and Bush 1997). For example, MOX-9, a class C enzyme belonging to a novel sub-lineage of MOX ß-lactamases, was found to be encoded by a chromosomal transposon in A. media. Biochemical characterization of this MOX-9 gene revealed a strong binding preference for cephalosporins and cephamycins. By comparing MOX-9 binding affinity and its hydrolysis activity to other more common MOX-type enzymes, this study not only demonstrated the variations that exist within this family of resistance genes but also provided a genetic context by which resistance genes can be easily mobilized onto transmissible plasmids and horizontally shared among other organisms (Piccirilli et al. 2022).
A third strategy is the use of broad-spectrum, non-specific AMR techniques such as drug uptake resistance, efflux pumps, and/or enhanced biofilm production. In one demonstration, when the ompR gene encoding an outer membrane protein (OMP) was deleted in an A. veronii isolate, increased sensitivity of the mutant culture to both ceftriaxone and neomycin, two different classes of drugs, was observed. Interestingly, the ΔompR mutant was shown to exhibit reduced biofilm production as well. It was speculated that this increased antibiotic susceptibility may be due, in part, to the reduction in biofilm formation since biofilm typically impedes an antibiotic’s access to the bacteria (Wang et al. 2023b). Indeed, when 29 OMP knockout strains were created in A. hydrophila, 22 gene deletions affected susceptibility levels to at least one of the 20 antibiotics tested. That being said, no OMP mutant exhibited consistent responses to all the tested antibiotics, eluding to more complicated downstream signaling/regulatory mechanisms underlying OMP-related drug uptake (Li et al. 2019). Additionally, when the porin protein Aha1 was mutated in A. hydrophila at its lysine-acetylation sites, increased resistance to tetracyclines and ß-lactams was observed, presumably due to decreased drug uptake (Zhang et al. 2022d). Recently, in China, a resistance-nodulation-division (RND)-type efflux pump gene cluster named tmexCD1-toprJ1636 was discovered in a related Gram-negative enteric pathogen Klebsiella pnuemoniae which confers resistance to different classes of antibiotics including tetracyclines, cephalosporins, aminoglycosides, phenicol, quinolones, and the last-resort antibiotic tigecycline (Lv et al. 2020). Such an efflux pump has since been shown to play a role in Aeromonas spp. drug resistance as well; in an environmental study, 36 of the 636 Aeromonas spp. isolated from livestock, meat, water, and humans [A. caviae ( 22), A. hydrophila (5), A. salmonicida (1), and A. veronii ( 8)] were positive for the multidrug-resistant gene cluster mentioned above, either encoded chromosomally or on a plasmid. Importantly, the characterized tmexCD-toprJ genes were associated with different Aeromonas spp., phylogenetic lineages, environments, and genetic locations and were surrounded by varying MGEs, demonstrating alarming diversity (Wu et al. 2023).
In reality, AMR in Aeromonas likely results from many different complicated factors, all playing simultaneous and even interactive roles. Employing a proteomic approach, a quinolone, norfloxacin (NOR), stress response study in A. hydrophila revealed 186 downregulated proteins and 220 upregulated proteins following exposure. Interestingly, many of the differentially expressed proteins were involved in sulfur metabolism and homologous recombination. Seven of these differentially expressed proteins were chosen as targets for site-directed mutagenesis in their encoding genes. Some mutants exhibited increased sensitivity to NOR such as ΔAHA_0904 (an uncharacterized protein) and ΔcirA (colicin I receptor), whereas the ΔhlyD (in the secretion family) mutant significantly increased NOR resistance. Other mutants, ΔAHA_4275 (a ferrichrome receptor), Δicd (isocitrate dehydrogenase [NADP]), ΔcheV (chemotaxis coupling protein), and ΔppsA (phosphoenolpyruvate synthase) displayed no differences compared to the parental A. hydrophila strain (Liu et al. 2023). This suggests that genes with no apparent ties to AMR can play an important role in an organism’s resistance/susceptibility to antibiotic stress.
Transcriptional regulators have also been shown to influence Aeromonas spp. drug resistance. More specifically, the transcriptional regulator AhslyA was shown to play a role in fluoroquinolone resistance. In an A. hydrophila ΔahslyA mutant, increased fluoroquinolone Enoxacin (ENX) sensitivity was observed. Proteomic analysis revealed differentially produced proteins involved in DNA metabolism, the SOS response, and cell communication following ENX treatment. Site-specific mutations were then engineered in several targets’ encoding genes, three genes related to decreasing protein abundance (AHA_0655, AHA_1195, and AHA_3721), and three genes related to increasing protein abundance (AHA_1239, AHA_2114, and narQ). The ΔAHA_2114 and ΔnarQ mutants had slightly decreased resistance to ENX at 0.01 μg/mL, and mutants ΔAHA_1239 and ΔAHA_3721 demonstrated an increase in resistance to ENX at 0.01 μg/mL. This further demonstrates the genetic diversity of expression/regulation involved in conferring drug resistance (Li et al. 2021). Collectively, these studies underscore the complex network of overlapping known pathways and mechanisms involved in AMR. When considering the potential contributions of yet unknown pathways, the network becomes even more complex.
Quorum sensing
Quorum sensing (QS), broadly, is a sophisticated mechanism of communication utilized by bacteria to coordinate behavior in a population. There are three major types of quorum sensing systems in Aeromonas known as autoinducers 1, 2, and 3. Autoinducer 1 (AI-1) QS is a system found exclusively in Gram-negative bacteria and is thought to detect and respond to the population density of members of the same species in an environment (Vanetti et al. 2020). Autoinducer 2 (AI-2) QS is a mechanism thought to mediate cross-species communication, given the machinery for this system is found in both Gram-positive and Gram-negative bacteria (Zhao et al. 2018). Autoinducer 3 (AI-3) QS is a two-component response system found in bacteria that responds to signals produced by members of the eukaryotic kingdom, demonstrating its use as an inter-kingdom mode of communication (Fan et al. 2022) (Fig. 1).
A schematic demonstrating the basic mechanisms that govern the three QS systems: AI-1 QS (far left) is only found in Gram-negative bacteria and is thought to be the mode of intra-species communication. Bacteria in a community simultaneously produce AI-1 signal via an AI-1 synthase (AhyI) where the signal is then sensed and responded to via the response regulator AhyR. AI-2 QS (center) is found in both Gram-positive and Gram-negative bacteria and is thought to be the mechanism of communication between different bacterial species. AI-2 signal is produced by all members of the bacterial community via LuxS. LuxR is responsible for sensing and responding to AI-2 signals. AI-3 QS (far right) is a two-component phosphorylative response system thought to be a mode of communication between prokaryotes and eukaryotes (inter-kingdom). Signals produced by a eukaryotic host collectively known as AI-3 cause a conformational change in membrane-bound sensor kinase (QseC), allowing for phosphorylation of the cytoplasmic response regulator (QseB), which activates it. (Image produced in BioRender)
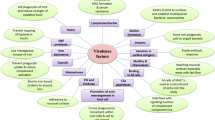
In many pathogenic bacteria, including Aeromonas spp., QS has been shown to globally regulate virulence gene expression and/or disease-causing mechanisms. Some of these virulence factors/mechanisms, utilized by Aeromonas and regulated by QS, include biofilm formation, motility, and effector protein secretion through various (e.g., types 2, 3, and 6) secretion systems (Table 2).
Autoinducer 1 quorum sensing: AhyRI
A QS system homologous to the LuxRI system in V. fischeri (Kempner and Hanson 1968) was first described in Aeromonas in 1997 (Swift et al. 1997). The system produces acyl-homoserine lactones (AHLs), molecular signals collectively known as AI-1, which are synthesized by the AHL synthase AhyI. A corresponding response regulator, AhyR, is then modulated by this signal (Chu et al. 2013; Swift et al. 1999; Van Houdt et al. 2007) to alter downstream gene expression. By far the most studied of the 3 Aeromonas-associated QS systems, AI-1 QS is ubiquitous across Aeromonas spp. (Jangid et al. 2007) and has been shown to influence the development of biofilm (Lynch et al. 2002), exo-proteases production (Khajanchi et al. 2009; Swift et al. 1999), outer membrane protein profiles, S (surface)-layer thickness (Bi et al. 2007), and type 6 secretion system (T6SS) effector secretion (Khajanchi et al. 2009) (Table 2). It has also been shown that mutations in this QS system result in decreased virulence potential of Aeromonas. More specifically, the virulence of a ΔahyRΔahyI double mutant was reduced by 50% when compared to its parental strain A. hydrophila SSU [since re-classified as A. dhakensis (Grim et al. 2014)] in a murine model of infection (Khajanchi et al. 2009). In a fish infection model using a challenge dose of 109 colony forming units (CFU)/ml, A. hydrophila J-1 mutant ΔahyR was rendered avirulent, as evidenced by the 100% survival of challenged fish. In contrast, 100% fish mortality was observed when challenged with the parental strain at the same dose (Bi et al. 2007). To better understand the AI-1 QS pathway, an AHL lactonase was used to block AI-1 signaling. Further evaluation of the data revealed differential expression of genes, post AHL lactonase treatment, that were involved in a myriad of metabolic pathways including metabolite transport, amino acid metabolism, central metabolism, and respiration, suggesting universal metabolic regulation by AI-1 QS (Gui et al. 2017).
While it is well established that AI-1 QS plays a crucial role in the virulence of Aeromonas (Bi et al. 2007; Khajanchi et al. 2009), little is known about the specifics of AHL synthesis or substrate specificity. It was historically thought Aeromonas only had the ability to synthesize two AHLs, N-butanoyl-L-homoserine lactone (C4-HSL) and N-hexanoyl-L-homoserine lactone (C6-HSL) (Kirke et al. 2004; Swift et al. 1997, 1999). To expand that knowledge, one study successfully purified 6 unique AHLs from A. hydrophila, although C4-HSL and C6-HSL continued to be the most abundant signals. The mechanism by which AhyI is able to catalyze the formation of the various AHLs was proposed to likely employ small molecules S-adenosyl-L-methionine (SAM) and butyryl-acyl carrier protein (ACP) as facilitators. If indeed SAM and ACP are involved in AHL synthesis, then AHL synthesis utilizes an acyl-ACP-derived fatty-acyl substrate and not acyl-CoA, as previously thought (Jin et al. 2020).
Autoinducer 2 quorum sensing: LuxS
The LuxS universal QS system mediated by AI-2 has also been described in the Aeromonas genus as early as 2008 (Kozlova et al. 2008). Unlike AI-1, this QS system is found in both Gram-positive and Gram-negative bacteria and is thought to be the means of cross-species communication (Xavier and Bassler 2003). Since its discovery, other publications have corroborated the existence of AI-2 systems in Aeromonas (Zhao et al. 2015); however, less research has focused on this QS system in Aeromonas spp. compared with AI-1 QS. The phenomenon generally observed has been an overall increase in virulence when AI-2 (luxS gene) is deleted. This is in sharp contrast to the deletion of the AI-1 system components. More specifically, an A. dhakensis SSU ΔluxS mutant exhibited decreased motility, increased virulence (as observed by increased lethality in a murine model), and altered biofilm structure. Surprisingly, the increased virulence in a septic mouse model of infection was not due to alterations/enhancements in hemolytic activity, AexU (a type 3 section system effector) translocation, or T6SS effector translocation (Kozlova et al. 2008) (Table 2). Furthermore, LuxS deficiency negatively affected expression levels of the A-layer gene encoding VapA, potentially reducing survivability in host macrophages (Meng et al. 2017). In an effort to uncover the mechanism(s) for these phenotypes, the DNA adenine-methyltransferase (Dam) encoding gene was overexpressed in both the parental and the ΔluxS mutant. The overexpression of dam caused the ΔluxS mutant to become hyper-motile and demonstrated increased hemolytic activity as compared to the isogenic dam-overexpressing parental strain. However, the overexpression of dam did not alter the virulence potential of the ΔluxS mutant in vivo. Taken together, these results suggest that the methylation of LuxS may play a role in the regulation of the AI-2 QS system (Kozlova et al. 2008) and needs further investigation.
To gain more insight into the signaling pathway downstream of AI-2 QS, the LuxS-regulated gene B protein (LsrB) was investigated in A. veronii. This protein belongs to the high-affinity substrate-binding protein family and is one of the two D-type receptors (LuxP and LsrB) of the AI-2 molecule in the AI-2 QS system. The major role of LsrB is to internalize extracellular AI-2 (Reading and Sperandio 2006). When this receptor was deleted in A. veronii, there was no apparent impact on growth, hemolytic activity, or antibiotic sensitivity. Motility was slightly decreased, likely on account of reduced flagellar gene expression, and a significant reduction in biofilm formation was also observed. Interestingly, the subsequent interruption of the AI-2 signaling pathway following LsrB deletion resulted in an unexpected decrease in virulence in a zebrafish model (as measured by an increased LD50) (Gao et al. 2023) contradicting the previous murine study (Kozlova et al. 2008). Additionally, AI-2 QS signaling seems to be affected by post-translation modifications (PTMs). By mapping out lysine-acetylation and lysine-succinylation sites in A. hydrophila, the sites were found to be largely overlapping. One such overlap was in the amino acid K165 in the luxS gene. Acetylated LuxS was found to negatively regulate LuxS enzymatic activity in A. hydrophila, while conversely, succinylated LuxS (at the same residue) positively regulated enzymatic activity. Interestingly, two distinct PTMs of LuxS on a specific residue oppositely influenced bacterial AI-2 QS activity (Sun et al. 2019), suggesting that the role LuxS plays in Aeromonas’ biological functions may be partially dependent on PTM status. This aspect may potentially contribute to the difference in phenotypic virulence in murine versus Zebra fish models and requires further investigation.
Autoinducer 3 quorum sensing: QseB/QseC
A third QS system mediated by two-component regulatory proteins QseB and QseC, which respond to AI-3 molecules, was identified in A. dhakensis SSU in 2012 (Khajanchi et al. 2012). Since then, 15 environmental Aeromonas isolates from China have been found to possess qseBC genes, demonstrating the widespread nature of this system within the genus (Sarkodie et al. 2019). Of the three QS systems identified in Aeromonas spp., the QseB/QseC system is the most poorly understood. Upon discovery, a ΔqseB mutant was constructed in A. dhakensis SSU, and the mutant exhibited diminished swarming and swimming motility, increased biofilm density, reduced protease production, and a slightly decreased virulence with 30% lower mortality over a test period of 16 days in an in vivo murine model of septicemic infection compared to the parental strain (Khajanchi et al. 2012). In contradiction to this study, a recent 2023 study reported that AI-3 QS component deletions in A. hydrophila did not affect motility, decreased biofilm production, and promoted increased virulence in an in vivo fish model (Qin et al. 2023a). Given the contrary nature of these two reports in different animal models, clearly, more studies are needed to better understand this complicated QS system.
One interesting finding in a fish model of infection study (Qin et al. 2023a) was its use of the host-derived stress hormone norepinephrine (NE). QseBC has previously been shown to enable many entero-bacteria to sense and interact with the host-derived environment (Lustri et al. 2017; Moreira and Sperandio 2016). This may also be true for Aeromonas spp. since the addition of NE to the medium of A. hydrophila increased its growth rate and dramatically increased biofilm production. However, ΔqseB and ΔqseC mutants did not display the aforementioned NE-mediated responses, suggesting that host signaling molecules are, in some way, associated with Aeromonas behavior, likely through the AI-3 QS (Qin et al. 2023a).
Interactions between QS systems
To complicate matters further, the three QS systems described above could possibly interact with one another, creating a complicated network of QS pathways replete with crosstalk and overlap. In an attempt to elucidate the ambiguity, one study systematically compared QS-related gene expression in mutants of all three QS systems. It was found that individual component deletions resulted in altered expression levels of the other QS system genes. In the ΔahyRI mutant, qseB, qseC, and luxS genes were all upregulated. In the ΔqseB mutant, ahyR and ahyI gene expression levels were downregulated; however, no changes were observed in luxS expression. Finally, in the ΔluxS mutant, no changes were observed in qseB and qseC expression levels. Taken together, these findings demonstrate that crosstalk and/or compensatory interactions between/among the various Aeromonas spp. QS systems occur (Kozlova et al. 2012).
Role of C-di-GMP in QS system interactions
C-di-GMP is a small signaling molecule that plays a crucial role in the regulation of bacterial behavior and physiology including all three Aeromonas spp. QS systems. An initial report demonstrated a link between c-di-GMP and AI-1 QS in A. sobria (Rahman et al. 2007). C-di-GMP overexpression in A. hydrophila was shown to enhance biofilm formation and reduce motility in the ΔluxS mutant and its parental strain. In contrast, the ΔahyRI mutant only showed a marginal increase in biofilm formation with no effect on motility when c-di-GMP was overexpressed (Kozlova et al. 2011). Overexpression of c-di-GMP reduced protease activity in the ΔqseB mutant when compared to the isogenic parental strain, and no changes in protease activity in the ΔahyRI mutant were observed. Furthermore, increased c-di-GMP expression in parental A. dhakensis SSU produced denser biofilms while increased c-di-GMP in the ΔqseB mutant decreased biofilm density (Kozlova et al. 2012). Collectively, the varying regulations each QS system exerts on one another, either positively or negatively, may be mediated by this small signaling molecule that has the demonstrable ability to communicate with all three.
Investigating the role of c-di-GMP in QS regulation led to the discovery that both AI-1 and AI-2 QS systems in Aeromonas affect expression levels of the transcriptional regulator LitR (Kozlova et al. 2011). The LitR homolog, HapR, has been shown to universally regulate virulence factors in V. cholerae (Kovacikova and Skorupski 2002). LitR has since been shown to bind to the promoter regions of the hemolysin and serine protease genes, as well as T6SS effector protein VrgG in A. hydrophila. LitR was also found to positively regulate hemolytic and extracellular protease activities (Zhao et al. 2023). This establishes LitR as a master transcriptional regulator used to control the expression of many essential virulence factors, and the expression level of LitR is regulated by both AI-1 and AI-2 QS systems, further demonstrating the overlap between the systems.
QS inhibition: an alternative therapeutic to antibiotics
Understanding the Aeromonas spp. QS systems and their crosstalk could enable exploitations that may result in promising alternative therapeutics for Aeromonas infections and beyond. The need for alternative therapeutics is especially apparent in Aeromonas spp. on account of their being both the cause of severe infections in humans and reservoirs of AMR genes. In that vein, the first use of a QS inhibitor in Aeromonas appears in 2009 when Truchado et al. (2009) found culturing A. hydrophila with chestnut honey resulted in the degradation of AHLs and decreased biofilm production. Since then, many natural and synthetic compounds have been shown to decrease QS-mediated virulence factors including biofilm, motility, protease production, and hemolysis to great effect via QS inhibition in Aeromonas (Table 3). AI-1 QS inhibitor cinnamaldehyde was shown to significantly decrease virulence phenotypes of A. hydrophila (Li et al. 2023). The plant-derived citrus flavonoid, hesperidin methyl chalcone (HMC), was found to not only downregulate the QS gene ahyR but also reduce the overall virulence potential of A. hydrophila in an in vivo fish model (Roshni et al. 2023). Tannic acid has been proven to be an effective QS inhibitor in A. hydrophila with demonstrably lower expression levels of ahyI and ahyR post-treatment and reduced hemolysis, motility, and biofilm formation. Tannic acid treatment also resulted in decreased virulence potential in an in vivo fish model (Patel et al. 2017). Genistein caused the downregulation of ahyRI expression levels, decreased virulence factors like biofilm and aerolysin production, and increased survival in an in vivo fish model (Dong et al. 2021). Another compound, carvacrol, a naturally derived monoterpenoid present in many herbs, was found to decrease the virulence potential of A. hydrophila by inducing decreased biofilm formation, protease production, hemolytic activity, and AHL production. The transcriptional analysis uncovered the downregulation of ahyR with carvacrol treatment in two separate studies, suggesting the involvement of AI-1 QS inhibition (Wang et al. 2022; Lu et al. 2023).
High-throughput screening for QS inhibitory molecules is becoming increasingly common to discover novel QS inhibitors (Zhang et al. 2022c). In silico methodologies can be used to do this via predicted 3-dimensional structures of the proteins involved. In that vein, the protein structure of AhyI was predicted and functionally characterized. Following that, the AI-1 synthase inhibitor N-cis-octadec-9Z-enoyl-L-homoserine lactone was then identified using high-throughput virtual screening. When tested, this molecule was found to effectively inhibit AI-1 activity at a concentration of 40 mM (Ali et al. 2022). Work has also been carried out to uncover novel AI-2 QS inhibiting compounds. In silico modeling of the AI-2 QS LuxS protein structure facilitated the prediction of putative binders and inhibitors of LuxS. From those predictions, a compound named ( −)-dimethyl 2,3-O-isopropylidene-l-tartrate was chosen for downstream testing, and it was shown to be an effective AI-2 QS inhibitor also at a concentration of 40 μM. Furthermore, A. hydrophila growth was significantly reduced when AI-2 QS inhibitor was added in conjunction with 1 mg/ml of oxytetracycline treatment (Ali et al. 2018). The use of in silico predictive models can more efficiently inform the discovery/design of novel drug candidates, especially when used synergistically with sub-lethal concentrations of bonafide antibiotics.
Alternatively, some research efforts have focused on exploring the role of commensal bacteria in pathogenic QS degradation. For example, one study reported that co-culturing A. hydrophila with three separate fish-gut-derived probiotic bacteria decreased AHL production by A. hydrophila and increased survival in an in vivo tilapia model when challenged (Omar et al. 2023). Similar results are found when a Streptomyces commensal (Liang et al. 2022) and a Bacillus commensal (Chen et al. 2020) were used in a zebrafish model and challenged with A. hydrophila. Because these studies have all focused on aquaculture and fish models, the efficacy of this technique in a mammalian model and the use of human commensals remain unexplored.
The emerging body of literature strongly suggests that blocking QS can be an effective way to reduce Aeromonas-related disease burden in aquaculture. Unfortunately, its potential in humans is left almost entirely unexplored. Given that all in vivo QS inhibition studies to date have been performed in a fish model of infection, a more clinically relevant understanding of many of these QS inhibitors needs to be established. Toward that end, some QS inhibitors have been tested in mammalian cell lines. Resveratrol, while effective in fish, demonstrated cytotoxicity in the murine macrophage cell line J774A.1 at higher concentrations (Qin et al. 2023b). One group observed that the plant extract, sanguinarine, was successful at reducing QS-regulated virulence factors like biofilm production and hemolysis at concentrations of 4 mg/ml. Sanguinarine was found to provide significant protection to human A549 cells from aerolysin-induced cell injury at this same concentration (Zhang et al. 2022b). In fact, thymol, genistein, and cinnamaldehyde have all demonstrated anti-QS activity and reduced cytotoxicity in human A549 cells (Dong et al. 2020a, b; Dong et al. 2021; Li et al. 2023). So, what little evidence we do have of these inhibitors in mammalian cell lines is, at best, varied. To further complicate the situation in a mammalian model, it has been shown that pre-treating mice with QS AI-1 signaling molecule AHL before challenging with A. dhakensis prevents clinical sequelae and produces increased survival in a septicemic model of infection (Khajanchi et al. 2011). While QS inhibition is a demonstrably effective way to reduce pathogenicity in a fish model, more research needs to be performed to ascertain its effectiveness in humans. Furthermore, the vast majority of QS inhibitory studies have been conducted using A. hydrophila as the model pathogen. Studies on this topic need to shift from the discovery of new compounds with anti-QS activity to fully characterizing the known compounds in different Aeromonas spp. and infection models.
Conclusion
Aeromonas spp. are well-established aquatic fish and emerging human pathogens (Fernández-Bravo and Figueras 2020; Hayatgheib et al. 2020). Control of these aquatic pathogens is critical to both protecting aquaculture and its associated economy, as well as to prevent potential human disease. When considering treatment, antibiotic resistance is a major global threat in all bacterial pathogens, and Aeromonas infections are no exception. In fact, antibiotic resistance of various types has been globally documented in Aeromonas spp. (Bargui et al. 2023; Bhaskar et al. 2015; Hayes et al. 1994). Unfortunately, Aeromonas spp. have been shown to acquire resistance from other pathogens as well as readily share resistance with other species/strains (Canellas et al. 2023; Goñi-Urriza et al. 2000; Igbinosa et al. 2015). On account of this, Aeromonas, being aquatic by nature, has rendered aquatic environments including treated waters, significant reservoirs for AMR acquisition and retention (Drk et al. 2023; Rhodes et al. 2000). This is particularly challenging given the potential economic impact of disrupting the aquaculture industry. Furthermore, in serving as potential reservoirs for AMR, these hardy aquatic pathogens can not only cause drug-resistant human diseases but also facilitate the spread of AMR to other unrelated bacterial pathogens. Viewed in this light, AMR Aeromonas could become a major contributor to the problem, setting the stage for nightmarish scenarios associated with the post-antibiotic era.
When facing antimicrobial challenges, Aeromonas spp. employ numerous AMR strategies of evasion including mutations of the drug targets themselves and, in some cases, expression of specific antibiotic degrading enzymes (if their encoding genes are present) (Piccirilli et al. 2022; Rasmussen and Bush 1997; Sinha et al. 2004). Aeromonas spp. also employ a number of highly effective broad-spectrum AMR strategies such as efflux pumps and drug uptake inhibition (Wu et al. 2023; Zhang et al. 2022d). When attempting to acquire a clear picture of AMR pathways involved in antimicrobial evasion, some ambiguity is found on account of pathway crosstalk, synergy, and even, at times, antagonism. Indeed, proteomic analysis reveals the truly complicated nature of Aeromonas’ phenotypic resistance to antibiotic-associated stress which further complicates the issue (Li et al. 2021; Liu et al. 2023). Because there are so many different strategies employed to this effect, a complete understanding of antibiotic resistance in Aeromonas spp. cannot be reached by examining each strategy/pathway independently. As a result, this remains a fruitful area of study.
Aeromonas spp. have also been shown to harbor AI-1, AI-2, and AI-3 QS systems (Khajanchi et al. 2012; Kozlova et al. 2008; Swift et al. 1997). All three systems are essential for the regulation of each other and overall virulence potential (Talagrand-Reboul et al. 2017). Without them, infection cannot be established (Natrah et al. 2012). Because of its essential and ubiquitous nature, QS may be a point of vulnerability to be exploited from a therapeutic perspective. In that vein, many pharmaceutical/natural alternatives to conventional antibiotics/antimicrobials therapies have been proposed specifically targeting the QS systems in Aeromonas spp. to great effect (Li et al. 2023; Patel et al. 2017; Qin et al. 2023b; Roshni et al. 2023; Tan et al. 2019; Wang et al. 2022). The limitation of these therapeutic studies has been their primary focus on aquaculture and fish health. In large part, these studies have employed in vivo fish models with the ecological and economic health of fish culturing in mind, thereby limiting data available on efficacy for use in a human context. Unfortunately, Aeromonas spp. infections continue to pose a challenge to human health, and when considering multiple-drug-resistant Aeromonas spp. infections, treatment alternatives become critical. In fact, the post-antibiotic era has created a pressing need for the development of alternative therapeutics for bacterial infections extending well beyond those caused by Aeromonas spp. alone. Ultimately, additional investigations on the use of these alternative therapeutics in a clinically relevant context are warranted for Aeromonas spp. infections and beyond.
Funding
This work was supported by the National Institutes of Health (NIH) R21 AI135453 grant and the pilot grants from the Institute for Human Infections and Immunity, UTMB, as well as the John S. Dunn chair in Global health Endowment to AKC, and the National Science Foundation (NSF) HRD-1345173 (JAR), HRD-1400962 (JAR), and HRD-1622993 (JAR) awards. The authors declare there are no conflicts of interest.
References
Ali F, Cai Q, Hu J, Zhang L, Hoare R, Monaghan SJ, Pang H (2022) In silico analysis of AhyI protein and AI-1 inhibition using N-cis-octadec-9z-enoyl-l-homoserine lactone inhibitor in Aeromonashydrophila. Microb Pathog 162:105356. https://doi.org/10.1016/j.micpath.2021.105356
Ali F, Yao Z, Li W, Sun L, Lin W, Lin X (2018) In-silico prediction and modeling of the quorum sensing luxs protein and inhibition of ai-2 biosynthesis in Aeromonas hydrophila. Molecules 23(10). https://doi.org/10.3390/molecules23102627
Bakken JS, Sanders CC, Clark RB, Hori M (1988) ß-lactam resistance in Aeromonas spp. caused by inducible ß-lactamases active against penicillins, cephalosporins, and carbapenems. Antimicrob Agents Chemother 32(9):1314–9. https://doi.org/10.1128/AAC.32.9.1314
Barger PC, Liles MR, Beck BH, Newton JC (2021) Differential production and secretion of potentially toxigenic extracellular proteins from hypervirulent Aeromonas hydrophila under biofilm and planktonic culture. BMC Microbiol 21(1):8. https://doi.org/10.1186/s12866-020-02065-2
Bargui H, Marzouk M, Hannachi N, Boukadida J (2023) Antimicrobial resistance and molecular determination of virulence genes of Aeromonas isolates from clinical patients and hydric samples. Euro-Mediterr J Environ 8(3):705–716. https://doi.org/10.1007/s41207-023-00369-z
Bertran X, Rubio M, Gómez L, Llovet T, Muñoz C, Navarro F, Miro E (2021) Taxonomic identification of different species of the genus Aeromonas by whole-genome sequencing and use of their species-specific β-Lactamases as phylogenetic markers. Antibiotics (Basel) 10(4). https://doi.org/10.3390/antibiotics10040354
Bhaskar M, Dinoop KP, Mandal J (2015) Characterization of ceftriaxone-resistant Aeromonas spp. isolates from stool samples of both children and adults in Southern India. J Health Popul Nutr 33:26. https://doi.org/10.1186/s41043-015-0036-7
Bhattacherjee R, Mandal S, Banerjee S, Saha KK, Sarkar J, Banerjee D, Mandal NC (2021) Structural-genetic insight and optimization of protease production from a novel strain of Aeromonas veronii CMF, a gut isolate of Chrysomya megacephala. Arch Microbiol 203(6):2961–2977. https://doi.org/10.1007/s00203-021-02282-x
Bi ZX, Liu YJ, Lu CP (2007) Contribution of AhyR to virulence of Aeromonas hydrophila J-1. Res J Vet Sci 83(2):150–156. https://doi.org/10.1016/j.rvsc.2007.01.003
Blöcher R, Ramírez AR, Castro-Excarpulli G, Curiel-Quesada E, Reyes-Arellano A (2018) Design, synthesis, and evaluation of alkyl-quinoxalin-2(1 H)-one derivatives as anti-quorum sensing molecules, inhibiting biofilm formation in Aeromonas caviae Sch3. Molecules 23(12):3075. https://doi.org/10.3390/molecules23123075
Braun M, Stuber K, Schlatter Y, Wahli T, Kuhnert P, Frey J (2002) Characterization of an ADP-ribosyltransferase toxin (AexT) from Aeromonas salmonicida subsp. salmonicida. J Bacteriol 184(7):1851–8. https://doi.org/10.1128/jb.184.7.1851-1858.2002
Burr SR, Stuber K, Frey J (2003) The ADP-ribosylating toxin, AexT, from Aeromonas salmonicida subsp. Salmonicida is translocated via a type III secretion pathway. J Bacteriol 85(22):6583–91. https://doi.org/10.1128/JB.185.22.6583-6591.2003
Cai H, Yu J, Qiao Y, Ma Y, Zheng J, Lin M, Yan Q, Huang L (2022) Effect of the type vi secretion system secreted protein hcp on the virulence of aeromonas salmonicida. Microorganisms 10(12). https://doi.org/10.3390/microorganisms10122307
Canellas ALB, de Oliveira BFR, Laport MS (2023) Hiding in plain sight: characterization of aeromonas species isolated from a recreational estuary reveals the carriage and putative dissemination of resistance genes. Antibiotics 12(1). https://doi.org/10.3390/antibiotics12010084
Cascón A, Yugueros J, Temprano A, Sánchez M, Hernanz C, Luengo JM, Naharro G (2000) A major secreted elastase is essential for pathogenicity of Aeromonas hydrophila. Infect Immun 68(6):3233–3241. https://doi.org/10.1128/iai.68.6.3233-3241.2000
Caselitz (1996) How the Aeromonas story started in medical microbiology. Med Microbiol Lett (5):46–54
Chang YC, Shih DY, Wang JY, Yang SS (2007) Molecular characterization of class 1 integrons and antimicrobial resistance in Aeromonas strains from foodborne outbreak-suspect samples and environmental sources in Taiwan. Diagn Microbiol Infect Dis 59(2):191–197. https://doi.org/10.1016/j.diagmicrobio.2007.04.007
Chen B, Peng M, Tong W, Zhang Q, Song Z (2020) The quorum quenching bacterium bacillus licheniformis T-1 protects Zebrafish against Aeromonas hydrophila infection. Probiotics Antimicrob Proteins 12(10):160–171. https://doi.org/10.1007/s12602-018-9495-7
Cheng Z, Zhao X, Jiang X, Zhang J, Li L, Pei C, Zhou Y, Zeng L, Kong X (2023) Contribution of flagellar cap gene in virulence and pathogenicity of Aeromonas veronii. J Fish Dis 46(3):247–259. https://doi.org/10.1111/jfd.13739
Chopra AK, Xu X, Ribardo D, Gonzalez M, Kuhl K, Peterson JW, Houston CW (2000) The cytotoxic enterotoxin of Aeromonas hydrophila induces proinflammatory cytokine production and activates arachidonic acid metabolism in macrophages. Infect Immun 68(5):2808–2818. https://doi.org/10.1128/iai.68.5.2808-2818.2000
Chu W, Liu Y, Jiang Y, Zhu W, Zhuang X (2013) Production of n-acyl homoserine lactones and virulence factors of waterborne aeromonas hydrophila. Indian J Microbiol 53(3):264–268. https://doi.org/10.1007/s12088-013-0381-4
Clark NM, Chenoweth CE (2003) Aeromonas infection of the hepatobiliary system: report of 15 cases and review of the literature. Clin Infect Dis 37(4):506–513. https://doi.org/10.1086/376629
Dey Bhowmick U, Bhattacharjee S (2017) Status of antibiotic resistance in the aeromonads of North Bengal With A special reference to change in resistance pattern through altitudinal gradient. NBU J. Anim. Sc. 11:51–59. ISSN:0975–1424
Didugu H, Thirtham M, Nelapati K, Reddy KK, Kumbhar BS, Poluru A, Pothanaboyina G (2015) A study on the prevalence of Aeromonas spp. and its enterotoxin genes in samples of well water, tap water, and bottled water. Vet World 8(10):1237–42. https://doi.org/10.14202/vetworld.2015.1237-1242
Ding T, Li T, Wang Z, Li J (2017) Curcumin liposomes interfere with quorum sensing system of Aeromonas sobria and in silico analysis. Sci Rep 7(1):8612. https://doi.org/10.1038/s41598-017-08986-9
Ding T, Li T, Li J (2018) Impact of curcumin liposomes with anti-quorum sensing properties against foodborne pathogens Aeromonas hydrophila and Serratia grimesii. Microb Pathog 122:137–143. https://doi.org/10.1016/j.micpath.2018.06.009
Dong J, Zhang L, Liu Y, Xu N, Zhou S, Yang Q, Yang Y, Ai X (2020a) Thymol protexts channel catfish from Aeromonas hydrophila infection by inhibiting aerolysin expression and biofilm formation. Microorganisms 8(5):636. https://doi.org/10.3390/microorganisms8050636
Dong W, Cai Y, Xu Z, Fu B, Chen Q, Cui Y, Ruan Z, Liang Y, Peng N, Zhao S (2020b) Heterologous expression of AHL lactonase AiiK by Lactobacillus casei MCJΔ1 with great quorum quenching ability against Aeromonas hydrophila AH-1 and AH-4. Microb Cell Fact 19(1):191. https://doi.org/10.1186/s12934-020-01448-4
Dong J, Zhang D, Li J, Liu Y, Zhou S, Yang Y, Xu N, Yang Q, Ai X (2021) Genistein inhibits the pathogenesis of Aeromonas hydrophila by disrupting quorum sensing mediated biofilm formation and aerolysin production. Front Pharmacol 12:753581. https://doi.org/10.3389/fphar.2021.753581
Drk S, Puljko A, Dželalija M, Udiković-Kolić N (2023) Characterization of third generation cephalosporin- and carbapenem-resistant aeromonas isolates from municipal and hospital wastewater. Antibiotics 12(3). https://doi.org/10.3390/antibiotics12030513
Dubey S, Ager-Wiick E, Peng B, DePaola A, Sørum H, Munang’andu HM (2023) The mobile gene cassette carrying tetracycline resistance genes in Aeromonas veronii strain Ah5S-24 isolated from catfish pond sediments shows similarity with a cassette found in other environmental and foodborne bacteria. Front Microbiol 14:1112941. https://doi.org/10.3389/fmicb.2023.1112941
Ebanks RO, Goguen M, McKinnon S, Pinto DM, Ross NW (2005) Identification of the major outer membrane proteins of Aeromonas salmonicida. Dis Aqua Org 68(1):29–38. https://doi.org/10.3354/dao068029
El-Hossary D, Mahdy A, Elariny EYT, Askora A, Merwad AMA, Saber T, Dahshan H, Hakami NY, Ibrahim RA (2023) Antibiotic resistance, virulence gene detection, and biofilm formation in aeromonas spp. isolated from fish and humans in Egypt. Biology 12(3). https://doi.org/10.3390/biology12030421
Fan Q, Wang H, Mao C, Li J, Zhang X, Grenier D, Yi L, Wang Y (2022) Structure and signal regulation mechanism of interspecies and interkingdom quorum sensing system receptors. J Agric Food Chem 70(2):429–445. https://doi.org/10.1021/acs.jafc.1c04751
Feng C, Liu X, Hu N, Tang Y, Feng M, Zhou Z (2022) Aeromonas hydrophila Ssp1: a secretory serine protease that disrupts tight junction integrity and is essential for host infection. Fish Shellfish Immunol 127:530–541. https://doi.org/10.1016/j.fsi.2022.06.068
Fernández-Bravo A, Figueras MJ (2020) An update on the genus aeromonas: taxonomy, epidemiology, and pathogenicity. Microorganisms 8(1). https://doi.org/10.3390/microorganisms8010129
Fernández-Bravo A, Kilgore PB, Andersson JA, Blears E, Figueras MJ, Hasan NA, Colwell RR, Sha J, Chopra AK (2019) T6SS and ExoA of flesh-eating Aeromonas hydrophila in peritonitis and necrotizing fasciitis during mono- and polymicrobial infections. Proc Natl Acad Sci USA 116(48):24084–24092. https://doi.org/10.1073/pnas.1914395116
Fluit AC, Schmitz FJ (1999) Class 1 integrons, gene cassettes, mobility, and epidemiology. Eur J Clin Microbiol Infect Dis 18(11):761–770. https://doi.org/10.1007/s100960050398
Gao H, Wang H, Zhang M, Shan X, Qian A, Zhang L, Zhang D, Sun W (2023) Detection of changes in biological characteristics of Aeromonas veronii TH0426 after deletion of lsrB gene by homologous recombination. Microb Pathog 174:105938. https://doi.org/10.1016/j.micpath.2022.105938
Garg N, Sharma G, Saffarini D, Sharda S, Sahney R, Shirodkar S (2023) Role of type IV pilin biosynthesis genes in biofilm formation of Aeromonas hydrophila. Asia Pac J Mol Biol Biotechnol 31(1):89–96
Goñi-Urriza M, Pineau L, Capdepuy M, Roques C, Caumette P, Quentin C (2000) Antimicrobial resistance of mesophilic Aeromonas spp. isolated from two European rivers. J Antimicrob Chemother 46(2):297–301. https://doi.org/10.1093/jac/46.2.297
Govender R, Amoah ID, Adegoke AA, Singh G, Kumari S, Swalaha FM, Bux F, Stenström TA (2021) Identification, antibiotic resistance, and virulence profiling of Aeromonas and Pseudomonas species from wastewater and surface water. Environ Monit Assess 193(5):294. https://doi.org/10.1007/s10661-021-09046-6
Grim CJ, Kozlova EV, Ponnusamy D, Fitts EC, Sha J, Kirtley ML, van Lier CJ, Tiner BL, Erova TE, Joseph SJ, Read TD, Shak JR, Joseph SW, Singletary E, Felland T, Baze WB, Horneman AJ, Chopra AK (2014) Functional genomic characterization of virulence factors from necrotizing fasciitis-causing strains of Aeromonas hydrophila. Appl Environ Microbiol 80(14):4162–4183. https://doi.org/10.1128/aem.00486-14
Gui M, Wu R, Liu L, Wang S, Zhang L, Li P (2017) Effects of quorum quenching by AHL lactonase on AHLs, protease, motility and proteome patterns in Aeromonas veronii LP-11. Int J Food Microbiol 252:61–68. https://doi.org/10.1016/j.ijfoodmicro.2017.04.005
Gurkok S, Ozdal M (2021) Purification and characterization of a novel extracellular, alkaline, thermoactive, and detergent-compatible lipase from Aeromonas caviae LipT51 for application in detergent industry. Protein Expr Purif 180:105819. https://doi.org/10.1016/j.pep.2021.105819
Hatrongjit R, Kerdsin A, Takeuchi D, Wongsurawat T, Jenjaroenpun P, Chopjitt P, Boueroy P, Akeda Y, Hamada S (2020) Genomic analysis of aeromonas veronii c198, a novel mcr-3.41-harboring isolate from a patient with septicemia in Thailand. Pathogens 9(12). https://doi.org/10.3390/pathogens9121031
Hayatgheib N, Moreau E, Calvez S, Lepelletier D, Pouliquen H (2020) A review of functional feeds and the control of Aeromonas infections in freshwater fish. Aquac Int 28(3):1083–1123. https://doi.org/10.1007/s10499-020-00514-3
Hayes MV, Thomson CJ, Amyes SG (1994) Three beta-lactamases isolated from Aeromonas salmonicida, including a carbapenemase not detectable by conventional methods. Eur J Clin Microbiol Infect Dis 13(10):805–811. https://doi.org/10.1007/bf02111340
Hayes MV, Thomson CJ, Amyes SG (1996) The ‘hidden’ carbapenemase of Aeromonas hydrophila. J Antimicrob Chemother 37(1):33–44. https://doi.org/10.1093/jac/37.1.33
Heiss C, Wang Z, Thurlow CM, Hossain MJ, Sun D, Liles MR, Saper MA, Azadi P (2019) Structure of the capsule and lipopolysaccharide O-antigen from the channel catfish pathogen Aeromonas Hydrophila. Carbohydr Res 486:107858. https://doi.org/10.1016/j.carres.2019.107858
Hilt E, Fitzwater S, Ward K, Maurice A, Chandrasekaran S, Garner O, Yang S (2020) Carbapenem resistant Aeromonas hydrophila carrying bla cphA7 isolated from two solid organ transplant patients. Front Cell Infect Microbiol 10:563482. https://doi.org/10.3389/fcimb.2020.563482
Hoel S, Vadstein O, Jakobsen AN (2019) The significance of mesophilic Aeromonas spp. in minimally processed ready-to-eat seafood. Microorganisms 7(3). https://doi.org/10.3390/microorganisms7030091
Huddleston JR, Brokaw JM, Zak JC, Jeter RM (2013) Natural transformation as a mechanism of horizontal gene transfer among environmental Aeromonas species. Syst Appl Microbiol 36(4):224–234. https://doi.org/10.1016/j.syapm.2013.01.004
Husain FM, Ahmad I, Khan MS, Al-Shabib NA (2015) trigonella foenum-graceum (seed) extract interferes with quorum sensing regulated traits and biofilm formation in the strains of Pseudomonas aeruginosa and Aeromonas hydrophila. Evid Based Complement Alternat Med 2015:879540. https://doi.org/10.1155/2015/879540
Husain FM, Ahmad I, Al-Thubiani AS, Abulreesh HH, AlHazza I, Aqil F (2017) leaf extracts of Mangifera indica L. inhibit quorum sensing-regulated production of virulence factors and biofilm in test bacteria. Front Microbiol 8:727. https://doi.org/10.3389/fmicb.2017.00727
Iaconis JP, Sanders CC (1990) Purification and characterization of inducible beta-lactamases in Aeromonas spp. Antimicrob Agents Chemother 34(1):44–51. https://doi.org/10.1128/aac.34.1.44
Igbinosa IH, Igbinosa EO, Okoh AI (2015) Detection of antibiotic resistance, virulence gene determinants and biofilm formation in Aeromonas species isolated from cattle. Environ Sci Pollut Res 22(22):17596–17605. https://doi.org/10.1007/s11356-015-4934-4
Indra U, Sureshkumar M, Kumar B, Vivekanandhan G (2015) Virulence determinants, drug and metal resistance of clinical and environmental Aeromonas species. J of Adv Res 3:573–587
Janda JM, Abbott SL (2010) The genus Aeromonas: taxonomy, pathogenicity, and infection. Clin Microbiol Rev 23(1):35–73. https://doi.org/10.1128/cmr.00039-09
Jangid K, Kong R, Patole MS, Shouche YS (2007) luxRI homologs are universally present in the genus Aeromonas. BMC Microbiol 7:93. https://doi.org/10.1186/1471-2180-7-93
Jin L, Zhang X, Shi H, Wang W, Qiao Z, Yang W, Du W (2020) Identification of a Novel N-Acyl homoserine lactone synthase, AhyI, in Aeromonas hydrophila and structural basis for its substrate specificity. J Agric Food Chem 68(8):2516–2527. https://doi.org/10.1021/acs.jafc.9b07833
Jones DC, LaMartina EL, Lewis JR, Dahl AJ, Nadig N, Szabo A, Newton RJ, Skwor TA (2023) One health and global health view of antimicrobial susceptibility through the “eye” of Aeromonas: systematic review and meta-analysis. Int J Antimicrob Agents 62(2):106848. https://doi.org/10.1016/j.ijantimicag.2023.106848
Kempner ES, Hanson FE (1968) Aspects of light production by Photobacterium fischeri. J Bacteriol 95(3):975–979. https://doi.org/10.1128/jb.95.3.975-979.1968
Khajanchi BK, Kirtley ML, Brackman SM, Chopra AK (2011) Immunomodulatory and protective roles of quorum-sensing signaling molecules N-acyl homoserine lactones during infection of mice with Aeromonas hydrophila. Infect Immun 79(7):2646–2657. https://doi.org/10.1128/iai.00096-11
Khajanchi BK, Kozlova EV, Sha J, Popov VL, Chopra AK (2012) The two-component QseBC signaling system regulates in vitro and in vivo virulence of Aeromonas hydrophila. Microbiology (reading) 158(Pt 1):259–271. https://doi.org/10.1099/mic.0.051805-0
Khajanchi BK, Sha J, Kozlova EV, Erova TE, Suarez G, Sierra JC, Popov VL, Horneman AJ, Chopra AK (2009) N-acyl-homoserine lactones involved in quorum sensing control the type VI secretion system, biofilm formation, protease production, and in vivo virulence in a clinical isolate of Aeromonas hydrophila. Microbiology (reading) 155(Pt 11):3518–3531. https://doi.org/10.1099/mic.0.031575-0
Kirke DF, Swift S, Lynch MJ, Williams P (2004) The Aeromonas hydrophila LuxR homolog AhyR regulates the N-acyl homoserine lactone synthase, AhyI positively and negatively in a growth phase-dependent manner. FEMS Microbiol Lett 241(1):109–117. https://doi.org/10.1016/j.femsle.2004.10.011
Ko WC, Wu HM, Chang TC, Yan JJ, Wu JJ (1998) Inducible beta-lactam resistance in Aeromonas hydrophila: therapeutic challenge for antimicrobial therapy. J Clin Microbiol 36(11):3188–3192. https://doi.org/10.1128/jcm.36.11.3188-3192.1998
Kovacikova G, Skorupski K (2002) Regulation of virulence gene expression in Vibrio cholerae by quorum sensing: HapR functions at the aphA promoter. Mol Microbiol 46(4):1135–1147. https://doi.org/10.1046/j.1365-2958.2002.03229.x
Kozlova EV, Khajanchi BK, Popov VL, Wen J, Chopra AK (2012) Impact of QseBC system in c-di-GMP-dependent quorum sensing regulatory network in a clinical isolate SSU of Aeromonas hydrophila. Microb Pathog 53(3–4):115–124. https://doi.org/10.1016/j.micpath.2012.05.008
Kozlova EV, Khajanchi BK, Sha J, Chopra AK (2011) Quorum sensing and c-di-GMP-dependent alterations in gene transcripts and virulence-associated phenotypes in a clinical isolate of Aeromonas hydrophila. Microb Pathog 50(5):213–223. https://doi.org/10.1016/j.micpath.2011.01.007
Kozlova EV, Popov VL, Sha J, Foltz SM, Erova TE, Agar SL, Horneman AJ, Chopra AK (2008) Mutation in the S-ribosylhomocysteinase (luxS) gene involved in quorum sensing affects biofilm formation and virulence in a clinical isolate of Aeromonas hydrophila. Microb Pathog 45(5–6):343–354. https://doi.org/10.1016/j.micpath.2008.08.007
L’Abée-Lund TM, Sørum H (2001) Class 1 integrons mediate antibiotic resistance in the fish pathogen Aeromonas salmonicida worldwide. Microb Drug Resist (larchmont, NY) 7(3):263–272. https://doi.org/10.1089/10766290152652819
Lau TV, Puah SM, Tan JMA, Merino S, Puthucheary SD, Chua KH (2023) Flagellar motility mediates biofilm formation in Aeromonas dhakensis. Microb Pathog 177:106059. https://doi.org/10.1016/j.micpath.2023.106059
Li S, Zhou S, Yang Q, Liu Y, Yang Y, Xu N, Ai X, Dong J (2023) Cinnamaldehyde decreases the pathogenesis of Aeromonas hydrophila by inhibiting quorum sensing and biofilm formation. Fishes 8(3):122
Li T, Sun X, Chen H, He B, Mei Y, Wang D, Li J (2020) Methyl anthranilate: a novel quorum sensing inhibitor and anti-biofilm agent against Aeromonassobria. Food Microbiol 83:103356. https://doi.org/10.1016/j.fm.2019.103356
Li Z, Wang Y, Li X, Lin Z, Lin Y, Srinivasan R, Lin X (2019) The characteristics of antibiotic resistance and phenotypes in 29 outer-membrane protein mutant strains in Aeromonas hydrophila. Environ Microbiol 21(12):4614–4628. https://doi.org/10.1111/1462-2920.14761
Li Z, Zhang L, Song Q, Wang G, Yang W, Tang H, Srinivasan R, Lin L, Lin X (2021) Proteomics analysis reveals bacterial antibiotics resistance mechanism mediated by ahslya against enoxacin in Aeromonashydrophila. Front Microbiol 12:699415. https://doi.org/10.3389/fmicb.2021.699415
Liang Q, Liu G, Guo Z, Wang Y, Xu Z, Ren Y, Zhang Q, Cui M, Zhao X, Xu D (2022) Application of potential probiotic strain Streptomyces sp. SH5 on anti-Aeromonas infection in zebrafish larvae. Fish Shellfish Immun 127:375–385. https://doi.org/10.1016/j.fsi.2022.06.049
Libisch B, Giske CG, Kovács B, Tóth TG, Füzi M (2008) Identification of the first VIM metallo-beta-lactamase-producing multiresistant Aeromonas hydrophila strain. J Clin Microbiol 46(5):1878–1880. https://doi.org/10.1128/jcm.00047-08
Liu Z, Zhang L, Song Q, Song H, Xu Y, Lu J, Xu Q, Tang Y, Liu Y, Wang G, Lin X (2023) Quantitative proteomics reveal the inherent antibiotic resistance mechanism against norfloxacin resistance in Aeromonas hydrophila. J Proteome Res 22(4):1193–1200. https://doi.org/10.1021/acs.jproteome.2c00663
Lu L, Wang J, Qin T, Chen K, Xie J, Xi B (2023) Carvacrol inhibits quorum sensing in opportunistic bacterium Aeromonas hydrophila. Microorganisms 11(8). https://doi.org/10.3390/microorganisms11082027
Lustri BC, Sperandio V, Moreira CG (2017) Bacterial chat: intestinal metabolites and signals in host-microbiota-pathogen interactions. Infect Immun 85(12). https://doi.org/10.1128/iai.00476-17
Lv L, Wan M, Wang C, Gao X, Yang Q, Partridge SR, Wang Y, Zong Z, Doi Y, Shen J, Jia P, Song Q, Zhang Q, Yang J, Huang X, Wang M, Liu JH (2020) Emergence of a plasmid-encoded resistance-nodulation-division efflux pump conferring resistance to multiple drugs, including tigecycline, in Klebsiella pneumoniae. mBio 11(2). https://doi.org/10.1128/mBio.02930-19
Lynch MJ, Swift S, Kirke DF, Keevil CW, Dodd CE, Williams P (2002) The regulation of biofilm development by quorum sensing in Aeromonas hydrophila. Environ Microbiol 4(1):18–28. https://doi.org/10.1046/j.1462-2920.2002.00264.x
Maia J, Silva GAA, Cunha LSB, Gouveia GV, Góes-Neto A, Brenig B, Araújo FA, Aburjaile F, Ramos RTJ, Soares SC, Azevedo VAC, Costa MMD, Gouveia JJS (2023) Genomic characterization of Aeromonas veronii provides insights into taxonomic assignment and reveals widespread virulence and resistance genes throughout the world. Antibiotics 12(6). https://doi.org/10.3390/antibiotics12061039
Majiduddin FK, Materon IC, Palzkill TG (2002) Molecular analysis of beta-lactamase structure and function. Int J Med Microbiol Suppl 2:127–137. https://doi.org/10.1078/1438-4221-00198
Mangoudehi HT, Zamani H, Shahangian SS, Mirzanejad L (2020) Effect of curcumin on the expression of ahyI/R quorum sensing genes and some associated phenotypes in pathogenic Aeromonas hydrophila fish isolates. World J Microbiol Biotechnol 36(5):70. https://doi.org/10.1007/s11274-020-02846-x
Marchandin H, Godreuil S, Darbas H, Jean-Pierre H, Jumas-Bilak E, Chanal C, Bonnet R (2003) Extended-spectrum beta-lactamase TEM-24 in an Aeromonas clinical strain: acquisition from the prevalent Enterobacter aerogenes clone in France. Antimicrob Agents Chemother 47(12):3994–3995. https://doi.org/10.1128/aac.47.12.3994-3995.2003
Masuyer G (2020) Crystal structure of exotoxin a from Aeromonas pathogenic species. Toxins (Basel) 12(6). https://doi.org/10.3390/toxins12060397
Matys J, Turska-Szewczuk A, Sroka-Bartnicka A (2020) Role of bacterial secretion systems and effector proteins - insights into Aeromonas pathogenicity mechanisms. Acta Biochim Pol 67(3):283–293. https://doi.org/10.18388/abp.2020_5410
McMahon MA, Wilson IG (2001) The occurrence of enteric pathogens and Aeromonas species in organic vegetables. Int J Food Microbiol 70(1–2):155–162. https://doi.org/10.1016/s0168-1605(01)00535-9
Mendoza-Barberá E, Merino S, Tomás J (2021) Surface glucan structures in Aeromonas spp. Mar Drugs 19(11). https://doi.org/10.3390/md19110649
Meng L, Du Y, Liu P, Li X, Liu Y (2017) Involvement of LuxS in Aeromonas salmonicida metabolism, virulence, and infection in Atlantic salmon (Salmo salar L). Fish Shellfish Immun 64:260–269. https://doi.org/10.1016/j.fsi.2017.03.009
Moreira CG, Sperandio V (2016) The epinephrine/norepinephrine/autoinducer-3 interkingdom signaling system in Escherichia coli O157:H7. Adv Exp Med Biol 874:247–261. https://doi.org/10.1007/978-3-319-20215-0_12
Natrah FM, Alam MI, Pawar S, Harzevili AS, Nevejan N, Boon N, Sorgeloos P, Bossier P, Defoirdt T (2012) The impact of quorum sensing on the virulence of Aeromonas hydrophila and Aeromonas salmonicida towards burbot (Lota lota L.) larvae. Vet Microbiol 159(1–2):77–82. https://doi.org/10.1016/j.vetmic.2012.03.014
Neuwirth C, Siebor E, Robin F, Bonnet R (2007) First occurrence of an IMP metallo-beta-lactamase in Aeromonas caviae: IMP-19 in an isolate from France. Antimicrob Agents Chemother 51(12):4486–4488. https://doi.org/10.1128/aac.01462-06
Nwaiwu O, Aduba C (2020) An in silico analysis of acquired antimicrobial resistance genes in Aeromonas plasmids. AIMS Microbiol 6(1):75–91. https://doi.org/10.3934/microbiol.2020005
Omar N, Emilia S, Danish-Daniel M, Iehata S, Ikhsan N (2023) Probiotics bacteria as quorum sensing degrader control Aeromonas hydrophila pathogenicity in cultured red hybrid tilapia. Indones Aquac J 18(1):1–15. https://doi.org/10.15578/iaj.18.1.2023.1-15
Orosz N, Tóthné Tóth T, Vargáné Gyuró G, Tibor Nábrádi Z, Hegedűsné Sorosi K, Nagy Z, Rigó É, Kaposi Á, Gömöri G, Adi Santoso CM, Nagy A (2022) Comparison of length of hospital stay for community-acquired infections due to enteric pathogens, influenza viruses and multidrug-resistant bacteria: a cross-sectional study in Hungary. Int J Environ Res Public Health 19(23). https://doi.org/10.3390/ijerph192315935
Papulzai A, John N, kurinji V, Malla S, (2020) A genetic variability study of lipase producing gene among Aeromonas species isolated from clinical isolates by RAPD DNA markers. Sumerianz J Biotechnol 3(9):83–92
Paquet VE, Vincent AT, Moineau S, Charette SJ (2019) Beyond the A-layer: adsorption of lipopolysaccharides and characterization of bacteriophage-insensitive mutants of Aeromonas salmonicida subsp. salmonicida. Mol Microbiol 112(2):667–677. https://doi.org/10.1111/mmi.14308
Patel B, Kumari S, Banerjee R, Samanta M, Das S (2017) Disruption of the quorum sensing regulated pathogenic traits of the biofilm-forming fish pathogen Aeromonas hydrophila by tannic acid, a potent quorum quencher. Biofouling 33(7):580–590. https://doi.org/10.1080/08927014.2017.1336619
Piccirilli A, Antonelli A, D’Andrea MM, Cherubini S, Perilli M, Rossolini GM (2022) Molecular and kinetic characterization of MOX-9, a plasmid-mediated enzyme representative of a novel sublineage of MOX-type class C β-lactamases. Antimicrob Agents Chemother 66(9):e0059522. https://doi.org/10.1128/aac.00595-22
Pillai L (2006) Role of new virulence mechanisms/factors (type 3 secretion system and TOX-R regulated lipoprotein [TAGA]) in the pathogenesis of the emerging human pathogen Aeromonas hydrophila. University of Texas Medical Branch
Pourmohsen M, Shakib P, Zolfaghari M (2023) The prevealence of bla VIM, bla KPC, bla NDM, bla IMP, bla SHV, bla TEM, bla CTX-M, and class I and II integrons genes in Aeromonas hydrophila isolated from clincal specimens of Qom, Iran. Clin Lab 69(1). https://doi.org/10.7754/Clin.Lab.2022.220314
Puah SM, Khor WC, Aung KT, Lau TTV, Puthucheary SD, Chua KH (2022) Aeromonas dhakensis: clinical isolates with high carbapenem resistance. Pathogens 11(8):833. https://doi.org/10.3390/pathogens11080833
Qin T, Chen K, Xi B, Pan L, Xie J (2023a) QseBC regulates in vitro and in vivo virulence of Aeromonas hydrophila in response to norepinephrine. Microb Pathog 174:105914. https://doi.org/10.1016/j.micpath.2022.105914
Qin T, Chen K, Xi B, Pan L, Xie J, Lu L, Liu K (2023b) In vitro antibiofilm activity of resveratrol against Aeromonas hydrophila. Antibiotics 12(4). https://doi.org/10.3390/antibiotics12040686
Rahman M, Simm R, Kader A, Basseres E, Römling U, Möllby R (2007) The role of c-di-GMP signaling in an Aeromonas veronii biovar sobria strain. FEMS Microbiol Lett 273(2):172–179. https://doi.org/10.1111/j.1574-6968.2007.00803.x
Ran C, Qin C, Xie M, Zhang J, Li J, Xie Y, Wang Y, Li S, Liu L, Fu X, Lin Q, Li N, Liles MR, Zhou Z (2018) Aeromonas veronii and aerolysin are important for the pathogenesis of motile aeromonad septicemia in cyprinid fish. Environ Microbiol 20(9):3442–3456. https://doi.org/10.1111/1462-2920.14390
Rangel LT, Marden J, Colston S, Setubal JC, Graf J, Gogarten JP (2019) Identification and characterization of putative Aeromonas spp. T3SS effectors. PLoS One 14(6):e0214035. https://doi.org/10.1371/journal.pone.0214035
Rasmussen BA, Bush K (1997) Carbapenem-hydrolyzing beta-lactamases. Antimicrob Agents Chemother 41(2):223–232. https://doi.org/10.1128/aac.41.2.223
Rather MA, Willayat MM, Wani SA, Hussain SA, Shah SA (2019) Enterotoxin gene profile and molecular epidemiology of Aeromonas species from fish and diverse water sources. J Appl Microbiol 127(3):921–931. https://doi.org/10.1111/jam.14351
Reading NC, Sperandio V (2006) Quorum sensing: the many languages of bacteria. FEMS Microbiol Lett 254(1):1–11. https://doi.org/10.1111/j.1574-6968.2005.00001.x
Rhodes G, Huys G, Swings J, McGann P, Hiney M, Smith P, Pickup RW (2000) Distribution of oxytetracycline resistance plasmids between aeromonads in hospital and aquaculture environments: implication of Tn1721 in dissemination of the tetracycline resistance determinant tet A. Appl Environ Microbiol 66(9):3883–3890. https://doi.org/10.1128/aem.66.9.3883-3890.2000
Rho H, Kannimuthu D (2023) Comparative resistome analysis of Aeromonas species in aquaculture reveals antibiotic resistance patterns and phylogeographic distribution. Environ Res 239(pt2):117273. https://doi.org/10.1016/j.envres.2023.117273
Roshni PS, Alexpandi R, Abirami G, Durgadevi R, Cai Y, Kumar P, Ravi AV (2023) Hesperidin methyl chalcone, a citrus flavonoid, inhibits Aeromonas hydrophila infection mediated by quorum sensing. Microb Pathog 177:106029. https://doi.org/10.1016/j.micpath.2023.106029
Rossolini GM, Walsh T, Amicosante G (1996) The Aeromonas metallo-beta-lactamases: genetics, enzymology, and contribution to drug resistance. Microb Dug Resist 2(2):245–252. https://doi.org/10.1089/mdr.1996.2.245
Sakai DK (1985) Loss of virulence in a protease-deficient mutant of Aeromonas salmonicida. Infect Immun 48(1):146–152. https://doi.org/10.1128/iai.48.1.146-152.1985
Sarkodie E, Zhou S, Chu W (2019) N-Acylhomoserine Lactones (AHLs), QseB/C gene detection, virulence factors and antibiotics resistance of Aeromonas hydrophila. J Adv Microbiol 9(5)
Sayeed S, Saunders JR, Edwards C, Corkill JE, Hart CA (1996) Expression of Aeromonas caviae bla genes in Escherichia coli. J Antimicrob Chemother 38(3):435–441. https://doi.org/10.1093/jac/38.3.435
Sha J, Galindo CL, Pancholi V, Popov VL, Zhao Y, Houston CW, Chopra AK (2003) Differential expression of the enolase gene under in vivo versus in vitro growth conditions of Aeromonas hydrophila. Microb Pathog 34(4):195–204. https://doi.org/10.1016/s0882-4010(03)00028-7
Sha J, Wang SF, Suarez G, Sierra JC, Fadl AA, Erova TE, Foltz SM, Khajanchi BK, Silver A, Graf J, Schein CH, Chopra AK (2007) Further characterization of a type III secretion system (T3SS) and of a new effector protein from a clinical isolate of Aeromonas hydrophila—Part I. Microb Pathog 43(4):127–146. https://doi.org/10.1016/j.micpath.2007.05.002
Shao L, Chen S, Ning Z, Xu X, Wang H (2023) Characterization of effector protein Hap determining meat spoilage process from meat-borne Aeromonassalmonicida. Food Chem 410:135457. https://doi.org/10.1016/j.foodchem.2023.135457
Sinha S, Chattopadhyay S, Bhattacharya SK, Nair GB, Ramamurthy T (2004) An unusually high level of quinolone resistance associated with type II topoisomerase mutations in quinolone resistance-determining regions of Aeromonas caviae isolated from diarrhoeal patients. Res Microbiol 155(10):827–829. https://doi.org/10.1016/j.resmic.2004.06.008
Sierra JC, Giovanni S, Chopra AK (2011) An intriguing emerging human pathogen Aeromonas hydrophila: pathogenesis and vaccines. In: Vaccines against Bacterial Boithreat pathogens. Research Signpost, Kerala, India, pp 1–34 ISBN: 978–81–308–0463–7
Suarez G, Sierra JC, Sha J, Wang S, Erova TE, Fadl AA, Foltz SM, Horneman AJ, Chopra AK (2008) Molecular characterization of a functional type VI secretion system from a clinical isolate of Aeromonas hydrophila. Microb Pathog 44(4):344–361. https://doi.org/10.1016/j.micpath.2007.10.005
Sun B, Luo H, Jiang H, Wang Z, Jia A (2021) Inhibition of quorum sensing and biofilm formation of esculetin on Aeromonashydrophila. Font Microbiol 12:737626. https://doi.org/10.3389/fmicb.2021.737626
Sun L, Yao Z, Guo Z, Zhang L, Wang Y, Mao R, Lin Y, Fu Y, Lin X (2019) Comprehensive analysis of the lysine acetylome in Aeromonas hydrophila reveals cross-talk between lysine acetylation and succinylation in LuxS. Emerg Microbes Infect 8(1):1229–1239. https://doi.org/10.1080/22221751.2019.1656549
Swift S, Karlyshev AV, Fish L, Durant EL, Winson MK, Chhabra SR, Williams P, Macintyre S, Stewart GS (1997) Quorum sensing in Aeromonas hydrophila and Aeromonas salmonicida: identification of the LuxRI homologs AhyRI and AsaRI and their cognate N-acyl-homoserine lactone signal molecules. J Bacteriol 179(17):5271–5281. https://doi.org/10.1128/jb.179.17.5271-5281.1997
Swift S, Lynch MJ, Fish L, Kirke DF, Tomás JM, Stewart GS, Williams P (1999) Quorum sensing-dependent regulation and blockade of exoprotease production in Aeromonas hydrophila. Infect Immun 67(10):5192–5199. https://doi.org/10.1128/iai.67.10.5192-5199.1999
Talagrand-Reboul E, Jumas-Bilak E, Lamy B (2017) The social life of Aeromonas through biofilm and quorum sensing systems. Front Microbiol 8:37. https://doi.org/10.3389/fmicb.2017.00037
Tekedar HC, Abdelhamed H, Kumru S, Blom J, Karsi A, Lawrence ML (2018) Comparative genomics of Aeromonas hydrophila secretion systems and mutational analysis of hcp1 and vgrg1 genes from T6SS. Front Microbiol 9:3216. https://doi.org/10.3389/fmicb.2018.03216
Truchado P, Gil-Izquierdo A, Tomás-Barberán F, Allende A (2009) Inhibition by chestnut honey of N-Acyl-L-homoserine lactones and biofilm formation in Erwinia carotovora, Yersinia enterocolitica, and Aeromonas hydrophila. J Agric Food Chem 57(23):11186–11193. https://doi.org/10.1021/jf9029139
Ueda M, Kobayashi H, Seike S, Takahashi E, Okamoto K, Yamanaka H (2022) Aeromonas sobria serine protease degrades several protein components of tight junctions and assists bacterial translocation across the T84 monolayer. Front Cell Infect Microbiol 12:824547. https://doi.org/10.3389/fcimb.2022.824547
Usui M, Tagaki C, Fukuda A, Okubo T, Boonla C, Suzuki S, Seki K, Takada H, Tamura Y (2016) Use of Aeromonas spp. as general indicators of antimicrobial susceptibility among bacteria in aquatic environments in Thailand. Front Microbiol 7:710. https://doi.org/10.3389/fmicb.2016.00710
Valcarcel B, De-la-Cruz-Ku G, Malpica L, Enriquez-Vera D (2021) Clinical features and outcome of Aeromonas sobria bacteremia in pediatric and adult patients with hematologic malignancies: a single-center retrospective study in Peru. PLoS ONE 16(8):e0255910. https://doi.org/10.1371/journal.pone.0255910
Van Houdt R, Aertsen A, Michiels CW (2007) Quorum-sensing-dependent switch to butanediol fermentation prevents lethal medium acidification in Aeromonas hydrophila AH-1N. Res Microbiol 158(4):379–385. https://doi.org/10.1016/j.resmic.2006.11.015
Vanetti M, Carneiro D, Almeida F, Vargas E, Lima E, Pinto U (2020) Autoinducer-1 quorum sensing communication mechanism in gram-negative bacteria trends in quorum sensing and quorum quenching. 1st Edition edn. CRC Press, p 21
Vincent AT, Hosseini N, Charette SJ (2021) The Aeromonas salmonicida plasmidome: a model of modular evolution and genetic diversity. Ann N.Y. Acad Sci 1488(1):16–32. https://doi.org/10.1111/nyas.14503
Wagenlehner FME, Dittmar F (2022) Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Eur Urol 82(6):658. https://doi.org/10.1016/j.eururo.2022.08.023
Walsh TR, Payne DJ, MacGowan AP, Bennett PM (1995) A clinical isolate of Aeromonas sobria with three chromosomally mediated inducible beta-lactamases: a cephalosporinase, a penicillinase and a third enzyme, displaying carbapenemase activity. J Antimicrob Chemother 35(2):271–279. https://doi.org/10.1093/jac/35.2.271
Walsh TR, Stunt RA, Nabi JA, MacGowan AP, Bennett PM (1997) Distribution and expression of beta-lactamase genes among Aeromonas spp. J Antimicrob Chemother 40(2):171–178. https://doi.org/10.1093/jac/40.2.171
Wang EW, Warren DK, Ferris VM, Casabar E, Nussenbaum B (2011) Leech-transmitted ciprofloxacin-resistant Aeromonas hydrophila. Arch Otolaryngol Head Neck Surg 137(2):190–193. https://doi.org/10.1001/archoto.2010.257
Wang G, Clark CG, Liu C, Pucknell C, Munro CK, Kruk TM, Caldeira R, Woodward DL, Rodgers FG (2003) Detection and characterization of the hemolysin genes in Aeromonas hydrophila and Aeromonas sobria by multiplex PCR. J Clin Microbiol 41(3):1048–1054. https://doi.org/10.1128/jcm.41.3.1048-1054.2003
Wang J, Qin T, Chen K, Pan L, Xie J, Xi B (2022) Antimicrobial and antivirulence activities of carvacrol against pathogenic Aeromonas hydrophila. Microorganisms 10(11). https://doi.org/10.3390/microorganisms10112170
Wang Y-d, Gong J-s, Guan Y-c, Zhao Z-l, Cai Y-n, Shan X-f (2023a) Hcp1 regulates flagella of Aeromonas veronii TH0426 to reduce virulence. Aquaculture 576:739899. https://doi.org/10.1016/j.aquaculture.2023.739899
Wang YD, Gong JS, Guan YC, Zhao ZL, Cai YN, Shan XF (2023b) OmpR (TCS response regulator) of Aeromonas veronii plays a major role in drug resistance, stress resistance, and virulence by regulating biofilm formation. Microb Pathog 181:106176. https://doi.org/10.1016/j.micpath.2023.106176
Wu CJ, Ko WC, Lee NY, Su SL, Li CW, Li MC, Chen YW, Su YC, Shu CY, Lin YT, Chen PL (2019) Aeromonas isolates from fish and patients in Tainan City, Taiwan: genotypic and phenotypic characteristics. Appl Environ Microbiol 85(21). https://doi.org/10.1128/aem.01360-19
Cj WU, Chen PL, Hsueh PR, Chang MC, Tsai PJ, Shih HI, Wang HC, Chou PH, Ko WC (2015) Clinical implications of species identification in monomicrobial Aeromonas bacteremia. PLoS ONE 10(2):e0117821. https://doi.org/10.1371/journal.pone.0117821
Wu Y, Dong N, Cai C, Zeng Y, Lu J, Liu C, Wang H, Zhang Y, Huang L, Zhai W, Shao D, Li R, Liu D, Chen S, Zhang R (2023) Aeromonas spp. from hospital sewage act as a reservoir of genes resistant to last-line antibiotics. Drug Resist Updat 67:100925. https://doi.org/10.1016/j.drup.2023.100925
Xavier KB, Bassler BL (2003) LuxS quorum sensing: more than just a numbers game. Curr Opin Microbiol 6(2):191–197. https://doi.org/10.1016/s1369-5274(03)00028-6
Xu C, Lin Q, Zhao Y, Zhu G, Jiang E, Li S, Mi Y, Zheng Y, Zhang F, Zhu X, Xiao Z, Han M, Wang J, Feng S (2022) Clinical characteristics and risk factors of Aeromonas bloodstream infections in patients with hematological diseases. BMC Infect Dis 22(1):303. https://doi.org/10.1186/s12879-022-07277-7
Yang C, Guo M, Yang H, Wen Y, Zhu Z, Wang T, Zhu J, Chen L, Du H (2022) bla(KPC-24)-Harboring Aeromonas veronii from the hospital sewage amples in China. Microbiol Spectr 10(3):e0055522. https://doi.org/10.1128/spectrum.00555-22
Zhang D, Li W, Hu X, Huang H, Zhang X (2023) Accurate identification and virulence detection of Aeromonas: a single-center retrospective study on the clinical features and outcomes associated with Aeromonas bacteremia in soutwestern China. Jpn J Infect Dis 76(1):7–13. https://doi.org/10.7883/yoken.JJID.2022.101
Zhang L, Jin S, Feng C, Song H, Raza SHA, Yu H, Zhang L, Chi T, Qi Y, Zhang D, Qian A, Liu N, Shan X (2022a) Aeromonas veronii virulence and adhesion attenuation mediated by the gene aodp. J Fish Dis 45(2):231–247. https://doi.org/10.1111/jfd.13544
Zhang L, Ma L, Yang Q, Liu Y, Ai X, Dong J (2022b) Sanguinarine protects channel catfish against Aeromonas hydrophila infection by inhibiting aerolysin and biofilm formation. Pathogens 11(3). https://doi.org/10.3390/pathogens11030323
Zhang L, Wu Y, Yao Z, Wang X, Chen J, Yang W, Yao J, Lin Y, Liu Z, Lin X (2022c) A high-throughput screening approach for bacterial quorum sensing inhibitors (QSIs) against Aeromonas hydrophila infection. Aquaculture 560:738488. https://doi.org/10.1016/j.aquaculture.2022.738488
Zhang L, Yao Z, Tang H, Song Q, Song H, Yao J, Li Z, Xie X, Lin Y, Lin X (2022d) The lysine acetylation modification in the porin Aha1 of Aeromonas hydrophila regulates the uptake of multidrug antibiotics. Mol Cell Proteom 21(9):100248. https://doi.org/10.1016/j.mcpro.2022.100248
Zhao J, Li Y, Huang Y, Jin L, Xu Y, Xu M, Quan C, Chen M (2023) Heterologous expression of quorum sensing transcriptional regulator LitR and its function in virulence-related gene regulation in foodborne pathogen Aeromonas hydrophila. Mol Biol Rep 50(3):2049–2060. https://doi.org/10.1007/s11033-022-07866-4
Zhao J, Quan C, Jin L, Chen M (2018) Production, detection, and application perspectives of quorum sensing autoinducer-2 in bacteria. J Biotechnol 268:53–60. https://doi.org/10.1016/j.jbiotec.2018.01.009
Zhao J, Zhang F, Cui Y, Xu Y, Chen M, Quan C, Fan S (2015) In vitro biosynthesis and activity detection of quorum sensing signal molecule AI-2 of Aeromonas hydrophila. Microbiol China 42(10):1858–1865
Acknowledgements
The McLaughlin Endowment Predoctoral Fellowship Award to BHN is greatly acknowledged.
Author information
Authors and Affiliations
Contributions
BHN and GLC performed the literature review and wrote the manuscript. JAR and JS reviewed and edited the manuscript. AKC provided financial support for the work, offered expertise in article’s topic, and provided final edits to the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Declarations
This study was funded by the US National Institutes of Health R21 AI135453, as well as by the John S. Dunn chair in Global health Endowment and the US National Science Foundation (HRD-1345173, HRD-1400962, and HRD-1622993).
Conflict of interest
All 4 authors (BHN, GLC, JAR, and AKC) declare that they have no conflict of interest to declare.
Human and animal studies
This article does not contain any studies with either animal or human subjects.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Neil, B., Cheney, G.L., Rosenzweig, J.A. et al. Antimicrobial resistance in aeromonads and new therapies targeting quorum sensing. Appl Microbiol Biotechnol 108, 205 (2024). https://doi.org/10.1007/s00253-024-13055-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00253-024-13055-z