Abstract
Purpose
The aim of this study was to collect and analyze information from pregnancies of organ transplanted women and partners of organ transplanted men. The goal was to enhance counseling regarding pregnancy planning and management and to enable more targeted monitoring to improve maternal and child health.
Methods
In this retrospective, multicenter cohort study, women and men aged 18 to 45 who had undergone organ transplantation in Germany, Austria, and Switzerland were surveyed about their pregnancies before and after transplantation by using a self-developed questionnaire.
Results
Even through transplanted women planned their pregnancies more carefully than before transplantation, they still experienced more pregnancy complications afterward. The live birth rate for pregnancies of partners of transplanted men, especially men who received a thoracic organ, was lower compared to before transplantation. Furthermore, this study showed that pregnancies of the partners of male transplant recipients occurred significantly less by spontaneous conception in comparison to pregnancies of transplanted women.
Conclusion
Pregnancies after organ transplantation are possible but associated with an increased risk of pregnancy complications. Therefore, early counseling for transplanted women and men who wish to have children, along with extensive monitoring during pregnancy, is necessary.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
This study highlights the increased pregnancy complication rates among women after organ transplantation and the lower live birth rates in pregnancies of partners of transplanted men. Despite these risks, many patients are willing to accept them to become parents, emphasizing the need for comprehensive risk information and close monitoring before, during, and after pregnancy. |
Introduction
In recent decades, the number of organ transplants for the treatment of organ failure has increased [1,2,3,4]. In addition to treating the patient’s underlying disease, the main aim of transplantation is to enable the recipient to live a life as fulfilling as possible [5], so that family planning is also becoming increasingly important. A notable proportion of recipients are of childbearing age [6,7,8,9].
When it comes to family planning and contraception, there are numerous unique challenges to address. For instance, women facing end-stage renal disease, particularly during dialysis, often experience irregular menstruation, and in some cases, infertility leading to amenorrhea [10,11,12]. Lower fertility also occurs with end-stage liver, lung and heart disease [12]. Conversely, fertility typically normalizes shortly after a successful organ transplant, potentially leading to pregnancies [10, 12,13,14,15]. Careful consideration should be given to the timing of pregnancy. In this regard, established guidelines for post-transplant pregnancies, such as those provided by the American Society of Transplantation, serve as valuable resources for physicians and aid in patient consultations [15]. However, there are still gaps in society’s knowledge of contraception. So unintended pregnancies are more common among women with lower levels of knowledge about contraception [16].
Men who have undergone organ transplantation should receive counseling if they are considering fatherhood. It is important to note that there is a documented higher risk of erectile dysfunction among patients with end-stage chronic renal failure and post-transplant individuals [17, 18]. Immunosuppressants can indeed affect fertility, sperm count, and testosterone levels [18, 19]. However, recent studies have not described an increased risk of fetal malformations [20]. Overall, it is important to recognize that fatherhood after organ transplantation is feasible [18].
Due to the overall small number of conceptions and pregnancies after organ transplantation, information is still limited, and most studies primarily focus on pregnancies in women following kidney and liver transplantation. It is established that pregnancies following transplantation tend to have higher complication rates compared to pregnancies in the general population [21]. These pregnancies are associated with increased risk of preterm birth, low birth weight, and preeclampsia [5, 12, 21, 22]. Additionally, the rate of cesarean sections after transplantation is elevated compared to the general population [21]. While pregnancies in women who have undergone liver transplantation are generally well tolerated, those in women who have undergone heart or lung transplantation are considered high-risk. In this patient group an increased risk of premature birth, low birth weight of the children or the risk of organ rejection has been described [5, 23]. In contrast to this the maternal mortality rate during pregnancy seems not to be higher than overall mortality after thoracic organ transplantation [23].
Studies show that even in the general population preeclampsia during pregnancy increases the cardiovascular risk and the risk of chronic hypertension for affected mothers after pregnancy [24]. Counseling in this regard already appears to be widely established [25]. It is unclear whether this is also the case for pregnancies of organ transplanted mothers with an increased risk of complications overall.
In contrast, there are fewer studies examining the risk of pregnancies in partners of men who have undergone organ transplantation. While there is some evidence suggesting an increased risk of preeclampsia, the rates of stillbirth and spontaneous abortion seem to be similar to those in the general population [20, 26].
Currently, there are only a limited number of studies that examined the desire for parenthood among organ transplanted women and men. Existing research suggests that women after transplantation have a similar desire to have children as women in the general population [27, 28] and transplanted men also express a wish to become father in the future [26]. Despite this strong desire, there is often a significant need for counselling among transplanted individuals who wish to have children. Nevertheless, many transplant recipients have apprehension about discussing this topic with their treating physician [28]. These findings underscore the importance of providing comprehensive counseling and education regarding pregnancy and contraception after transplantation. Additionally, there is a clear need for systematic documentation of pregnancies that have already occurred in this population.
The objective of this study was to gather data on the occurrence, progression, and complications of pregnancies or conceptions in transplant recipients, while also identifying potential variations between genders, organ categories, and pre- and post-transplantation phases. Such an approach is intended to streamline the counseling process for patients seeking guidance on family planning following an organ transplantation.
Material and methods
Participants and recruitment
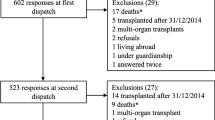
This study was conducted as a retrospective, multi-center cohort utilizing an online questionnaire available from July 2020 to December 2020. Ethical approval was granted by the Institutional Review Board of Hannover Medical School (Nr. 8900_BO_K_2020), and participants provided informed consent. The target group included women and men of reproductive age between 18 and 45 years after an organ or an allogeneic stem cell transplantation. Exclusion criteria encompassed individuals outside the specific age range, individuals solely listed for transplantation at the time of participation, and patients with autologous stem cell transplantation.
Potential participants were informed about the study through various channels, including posters and flyers distributed in several outpatient clinics across Germany, as well as through social media platforms such as Facebook and Instagram. Additionally, the study was introduced to support groups, and transplant patients received information from their medical care providers during regular follow-up care visits at transplant centers or at Hannover Medical School, supplemented by phone call.
Questionnaire
The survey was developed in cooperation with the Department of Obstetrics and Gynecology and the Department of Psychosomatics and Psychotherapy at Hannover Medical School. Data collection was conducted through an anonymous online questionnaire hosted on the Unipark platform.
The self-developed questionnaire compromised six thematic sections covering various aspects: demographic information, history of previous conceptions and pregnancies, current relationship status, desire for parenthood, attitude towards future pregnancies, mental health status and satisfaction with medical consultations regarding these topics. The focus of this study was to assess the past pregnancies and conceptions of the participating women and men. The questionnaire included a mix of single- and multiple-choice, free-text- and ranking questions.
Statistical analysis
Comparisons were conducted regarding gender, organ groups and pregnancies before and after transplantation.
These comparisons were analyzed using non-parametric tests, such as Mann–Whitney U or Kruskal–Wallis test, as appropriate. Relationships between variables were assessed using the chi-square test or Fisher’s exact test in cases of small sample size.
To ensure a more robust evaluation of individual groups, participants who had undergone allogenic stem cell transplantation (n = 23) or those with transplantation of more than one organ (n = 22) were subsequently excluded from the analysis due to small sample size. As a result, data from a total of n = 251 solid organ transplant recipients were available for analysis. Statistical analysis was performed using IBM SPSS Statistics 28.0.
Results
A total of n = 172 women and n = 79 men participated in the study. Gender comparison revealed a comparable age distribution of participants at the time of pregnancy before (p = 0.08), but a significant difference was observed after transplantation. Male participants were significantly older than females at the time of pregnancy after transplantation (p < 0.01). Whereas heart transplant patients represented the smallest group, the kidney, liver and lung transplant patients had nearly similar group sizes (p = 0.2). Significantly more men worked in full-time positions compared to women, who predominantly reported working in half time positions (p = 0.01) (Table 1).
Evaluation of pregnancies and conceptions before and after transplantation
A detailed overview of pregnancies before and after transplantation is presented in Table 2. Regarding the assessment of pregnancies among female participants before and after transplantation, a significantly higher number of pregnancies were planned after transplantation compared to before (p = 0.01). Specifically, it was observed that in cases where the disease was not yet known at the time of pregnancy, a higher proportion of pregnancies were planned (p = 0.05).
Furthermore, it was noted that a significantly higher rate of pregnancy complications was reported after transplantation compared to before (p = 0.04). Pregnancy complications after transplantation mainly involved preterm birth, preterm labor and gestational hypertension.
The comparison of pregnancies of female partners of participants (Table 3) revealed a statistically significant difference regarding the pregnancy outcome of the female partners of the study participants. Live births were observed in 89.7% of pregnancies (n = 26) before and in 67.6% of pregnancies (n = 25) after transplantation (p = 0.03).
Gender-specific comparison of pregnancies before and after transplantation
In the gender comparison (Table 4, Supplements Table 1) pre-transplant pregnancies exhibited a significant difference in childbirth outcomes. While 89.7% (n = 26) of conceptions achieved by transplanted men resulted in live births, only 64.1% (n = 25) of pregnancies among female participants did (p = 0.02). In contrast to the pre-transplantation period, a significant gender difference was noted after transplantation regarding the method of conception. While 94.3% (n = 50) of female participants conceived spontaneously, spontaneous conception occurred less frequently in male transplant recipients (75.7%, n = 28), (p = 0.02).
Organ group specific evaluation of pregnancies from female participants before and after transplantation
Furthermore, pregnancies of female participant who received abdominal and thoracic organ transplants were compared. No significant difference was observed when comparing pregnancies of women who underwent abdominal transplantation with those who underwent thoracic transplantation, either before or after transplantation, in terms of method of conception, pregnancy outcome, mode of delivery or pregnancy complication rate (Tables 5, 6).
Organ group specific evaluation of pregnancies of partners from male participants before and after transplantation
At last pregnancies of partners from male participants who received an abdominal and thoracic organ transplant were compared. There was no significant difference found before transplantation (Table 7). After transplantation (Table 8) significantly less pregnancies of thoracic organ transplant recipients resulted in live births compared to those of abdominal organ transplant recipients (p = 0.03). Particularly, miscarriage was a more frequent pregnancy outcome among female partners of thoracic organ transplant recipients.
Discussion
The primary objective of this study was to gather comprehensive data on the frequency, progression, and complications of pregnancies or conceptions in transplant recipients. We aimed to identify potential variations between genders, organ categories, and pre- and post-transplantation phases. Our findings revealed that despite transplanted women planned their pregnancies more carefully than before transplantation, there were still more pregnancy complications after transplantation. Furthermore, pregnancies of partners of transplanted men, especially those who received a thoracic organ transplant, exhibited lower live birth rates compared to partners of men before transplantation. Additionally, our study highlighted that pregnancies of partners of male transplant recipients occurred significantly less frequently through spontaneous conception compared to transplanted women.
This study revealed that more pregnancies among female participants were planned after transplantation compared to before, regardless of the transplanted organ. However, it’s crucial to emphasize the importance of birth control, especially since unplanned pregnancies in the absence of clarification of current organ function pose greater risks [29]. Depending on the medication regimen, adjustments to immunosuppressants may be necessary to prevent adverse outcomes such as early abortion [29]. Particularly, pregnancies among thoracic organ recipients are categorized as extreme risk pregnancies. Therefore, comprehensive counseling on contraceptive methods and pregnancy planning, as well as close monitoring during pregnancy, are of paramount importance [5].
Consequently, the results observed in this study suggest that education regarding pregnancy planning while taking immunosuppressants may already be prevalent among the analyzed group of participants. However, it remains unclear whether this counseling occurs sufficiently during doctor-patient discussion or via self-help groups. A closer examination of the organ groups regarding pregnancy outcome reveals a higher rate of miscarriage in pregnancies of the female participants before transplantation compared to afterwards. This trend is particularly pronounced in the group of abdominally transplanted participants. In approximately half of this group, the underlying disease leading to transplantation was already present at the time of pregnancy. The occurrence of pregnancy at an unplanned time, potentially coinciding with poor organ function due to the disease leading to transplantation, could be a contributing factor to this observation. Simultaneously, the higher rate of planned pregnancies after transplantation also suggests a lower rate of induced abortions. When comparing the induced abortion rates in this study with those of the general population [30], it is noteworthy that the abortion rate before transplantation is higher than in the general population, while the abortion rate after transplantation is lower.
A limiting factor of this study is, that the reason for induced abortion was not recorded.
Spontaneous pregnancies were significantly more common among female transplant participants compared to the partners of male transplant participants. A notable proportion of male participants utilized intracytoplasmic sperm injection (ICSI) for achieving a pregnancy, with a majority of these participants being thoracic transplant recipients. The underlying diseases of thoracic transplant recipients, such as cystic fibrosis and muscular dystrophy, shed light on this observation. Research indicated that over 98% of men with cystic fibrosis experience azoospermia, rendering them infertile or necessitating assisted reproductive techniques for conception [31]. Moreover, muscular dystrophy is frequently associated with hypogonadism [32]. Therefore, it is plausible that the gender difference observed in this study can be attributed to the underlying diseases of the participants.
There is a significant decrease in live births after transplantation compared to before in pregnancies involving partners of male transplant participants. Specifically, miscarriages, stillbirths, and induced abortions were more frequently reported after transplantation. As previously mentioned, research on pregnancy outcomes of female partners of male organ transplant recipients has been limited. However, a cohort study by Morken et al. [20] suggests an increased risk of preeclampsia in pregnancies fathered by male transplant recipients across all transplanted organ groups. Unfortunately, complications of pregnancies fathered by male transplant recipients were not examined in this study. Nevertheless, our study expands upon this research by demonstrating an increased rate of miscarriage and stillbirth after transplantation. It is unclear whether there is an association between the decrease in live births after transplantation and the increased preeclampsia rate observed in Morken’s study. Nonetheless, this finding underscores the importance of further investigation in future studies.
At this point, it is important to highlight the increased risk of pregnancy complications leading to abortions due to immunosuppressant intake in female transplant recipients [5]. Conversely, a study by Jones concluded that the pregnancy outcomes in conceptions by males treated with mycophenolic acid products were similar to the general population [33]. This finding could potentially explain the higher live birth rates observed in pregnancies resulting from transplanted men. However, further investigation into other potential causes of this sex-specific difference is warranted and should be the focus of future studies.
Regarding pregnancy complication rates, this study revealed a significant difference before and after transplantation. After transplantation, more than half of the participants reported complications, whereas the proportion before transplantation represented approximately one third.
An increased preterm birth rate was observed after transplantation compared to before. This finding aligns with existing literature documenting higher preterm birth rates after transplantation. The results of this study highlight that preterm birth accounts for a significant portion of pregnancy complications after transplantation. Moreover, this underscores the importance of close monitoring during pregnancy, including ultrasound examinations and regular fetal growth assessments, as emphasized in previous studies [5, 15, 22].
One reason for the equally high rate of pregnancy complications before transplantation could be attributed to the presence of the disease that led to transplantation in approximately half of the abdominally transplanted participants before transplantation. Abdominal transplanted participants represented the largest share of the group. Studies indicate that women with chronic kidney or liver disease not only experience impaired fertility due to dysfunction of the hypothalamic-pituitary-ovarian axis but also face an increased risk of pregnancy complications [34].
Furthermore, research suggests that stable graft function is typically unaffected by pregnancy. However, in cases of chronic rejection before pregnancy, there is an increased risk of graft loss during pregnancy [35]. Additionally, graft function at the onset of pregnancy plays a significant role in determining risks and outcomes [29, 36]. The participants in this study exhibited a relatively low rate of graft rejections during pregnancy after transplantation and no occurrences of graft failure were reported. However, it is important to note that graft function at the beginning of pregnancy was not determined, which is a limiting factor of our study.
Our study builds upon existing research on pregnancies in female organ transplant recipients, with a unique focus on comparing pregnancies grouped by transplanted organs. What sets our study apart is its reliance on self-reported data, allowing for comparisons between abdominal and thoracic transplanted organ groups, as well as a gender-specific analysis of pregnancies among transplanted women and partners of transplanted men.
Initiated with primary data collection at Hannover Medical School, the largest transplant center in Germany, our study expanded its reach to encompass the entirety of Germany, Austria and Switzerland. This approach facilitated the recruitment of a large cohort of participants and provided a comprehensive overview of common pregnancy complications and patterns. Notably, our study also addresses a gap in the literature by documenting the obstetric outcomes of partners of male transplant recipients.
However, our study does have limitations. Being retrospective in nature, there is potential for recall bias, particularly when participants are asked to recall events from the distant past. Additionally, some questions in the questionnaire were not mandatory, leading to missing values. Participation in the study was voluntary, introducing the possibility of selection bias. Furthermore, important factors such as organ function at the time of conception/pregnancy, use of immunosuppressive medication, exposure to harmful substances during or before pregnancy, prior medical conditions of participants, and pregnancy complications of male participants’ partners were not recorded. These limitations should be taken into account when interpreting the results of our study.
Data availability
Data are available on reasonable demand to the corresponding author.
References
Boenink R, Kramer A, Tuinhout RE, Savoye E, Åsberg A et al (2023) Trends in kidney transplantation rate across Europe: study from the ERA registry. Nephrol Dial Transplant 38(6):1528–1539. https://doi.org/10.1093/ndt/gfac333
Chambers DC, Yusen RD, Cherikh WS, Goldfarb SB, Kucheryavaya AY, Khusch K, Levvey BJ, Lund LH, Meiser B, Rossano JW, Stehlik J (2017) The registry of the international society for heart and lung transplantation: thirty-fourth adult lung and heart-lung transplantation report—2017; focus theme: allograft ischemic time. J Heart Lung Transplant 36(10):1047–1059. https://doi.org/10.1016/j.healun.2017.07.016
Dutkowski P, De Rougemont O, Müllhaupt B, Clavien P (2010) Current and future trends in liver transplantation in Europe. Gastroenterology 138(3):802-809.e4. https://doi.org/10.1053/j.gastro.2010.01.030
Manla Y, Badarin FJ, Soliman M, Gobolos L, Alsindi F, Bader F (2021) Twenty-year temporal and regional trends in heart transplantation in Europe: results from the global observatory on donation and transplantation (GODT). Eur Heart J 42(1):ehab724.0968. https://doi.org/10.1093/eurheartj/ehab724.0968
Coscia LA, Constantinescu S, Moritz MJ, Frank AM, Ramirez CB, Maley WR, Doria C, McGrory CH, Armenti VT (2010) Report from the National Transplantation Pregnancy Registry (NTPR): outcomes of pregnancy after transplantation. Clin Transpl. 105730:65–85. https://terasaki.org/store/CH7-Coscia_2010
Durand F, Levitsky J, Cauchy F, Gilgenkrantz H, Soubrane O, Francoz C (2019) Age and liver transplantation. J Hepatol 70(4):745–758. https://doi.org/10.1016/j.jhep.2018.12.009
Knoll G (2008) Trends in kidney transplantation over the past decade. Drugs 68(1):3–10. https://doi.org/10.2165/00003495-200868001-00002
Rossano JW, Cherikh WS, Chambers DC, Goldfarb S, Hayes D, Khush KK, Kucheryavaya AY, Toll AE, Levvey BJ, Meiser B, Stehlik J (2018) The international thoracic organ transplant registry of the international society for heart and lung transplantation: twenty-first pediatric heart transplantation report—2018; focus theme: multiorgan transplantation. J Heart Lung Transplant 37(10):1184–1195. https://doi.org/10.1016/j.healun.2018.07.018
Yusen RD, Christie JD, Edwards LB, Kucheryavaya AY, Benden C, Dipchand AI, Dobbels F, Kirk R, Lund LH, Rahmel AO, Stehlik J (2013) The registry of the international society for heart and lung transplantation: thirtieth adult lung and heart-lung transplant report—2013; focus theme: age. J Heart Lung Transplant 32(10):965–978. https://doi.org/10.1016/j.healun.2013.08.007
Lessan-Pezeshki M, Ghazizadeh S, Khatami MR, Mahdavi M, Razeghi E, Seifi S, Ahmadi F, Maziar S (2004) Fertility and contraceptive issues after kidney transplantation in women. Transpl Proc 36(5):1405–1406. https://doi.org/10.1016/j.transproceed.2004.04.090
Lim VS, Henriquez C, Sievertsen G, Frohman LA (1980) Ovarian function in chronic renal failure: evidence suggesting hypothalamic anovulation. Ann Intern Med 93(1):21. https://doi.org/10.7326/0003-4819-93-1-21
McKay DB, Josephson MA (2006) Pregnancy in recipients of solid organs effects on mother and child. N Engl J Med 354:1281. https://doi.org/10.1056/NEJMra050431
Al-Badri M, Kling JM, Vegunta S (2017) Reproductive planning for women after solid-organ transplant. CCJM 84(9):719–728. https://doi.org/10.3949/ccjm.84a.16116
De Koning ND, Haagsma EB (1990) Normalization of menstrual pattern after liver transplantation: consequences for contraception. Digestion 46(4):239–241. https://doi.org/10.1159/000200352
Deshpande NA, Coscia LA, Gomez-Lobo V, Moritz MJ, Armenti VT (2013) Pregnancy after solid organ transplantation: a guide for obstetric management. Rev Obstet Gynecol 6(3–4):116–125. https://doi.org/10.3909/riog0230
Allerstorfer C, Reiter E, Shebl O, Oppelt P, Reid AM, Schimetta W, Binder H, Beckmann MW (2024) Influence of basic knowledge about female health, physiology, and contraception on unintended pregnancies: an international multicenter survey among women in Austria, Germany and Switzerland. Arch Gynecol Obstet 310(2):1267–1273. https://doi.org/10.1007/s00404-024-07441-1
Antonucci M, Palermo G, Recupero SM, Bientinesi R, Presicce F, Foschi N, Bassi PF, Gulino G (2015) Male sexual dysfunction in patients with chronic end-stage renal insufficiency and in renal transplant recipients. Archivio Italiano di Urologia e Andrologia. 87:299. https://doi.org/10.4081/aiua.2015.4.299
Thirumavalavan N, Scovell JM, Link RE, Lamb DJ, Lipshultz LI (2018) Does solid organ transplantation affect male reproduction? Eur Urol Focus 4(3):307–310. https://doi.org/10.1016/j.euf.2018.08.012
Tainio J, Jahnukainen K, Nurmio M, Pakarinen M, Jalanko H, Jahnukainen T (2014) Testicular function, semen quality, and fertility in young men after renal transplantation during childhood or adolescence. Transplantation 98(9):987–993. https://doi.org/10.1097/TP.0000000000000173
Morken N-H, Diaz-Garcia C, Reisaeter AV, Foss A, Leivestad T, Geiran O, Hervás D, Brännström M (2015) Obstetric and neonatal outcome of pregnancies fathered by males on immunosuppression after solid organ transplantation: pregnancies fathered by transplanted males. Am J Transplant 15(6):1666–1673. https://doi.org/10.1111/ajt.13159
Mohamed-Ahmed O, Nelson-Piercy C, Bramham K, Gao H, Kurinczuk JJ, Brocklehurst P, Knight M (2014) Pregnancy outcomes in liver and cardiothoracic transplant recipients: a UK national cohort study. PLoS ONE 9(2):e89151. https://doi.org/10.1371/journal.pone.0089151
Bedin A, Carbonnel M, Snanoudj R, Roux A, Vanlieferinghen S, Marchiori C, Hertig A, Racowsky C, Ayoubi J-M (2022) Pregnancies and gynecological follow-up after solid organ transplantation: experience of a decade. J Clin Med 11(16):4792. https://doi.org/10.3390/jcm11164792
Jha N, Jha A, Mishra S, Parida S (2023) Thoracic organ transplantation and pregnancy outcomes: systematic review and meta-analysis. Arch Gynecol Obstetr 309:385. https://doi.org/10.1007/s00404-023-07065-x
Haßdenteufel K, Müller M, Gutsfeld R, Goetz M, Bauer A, Wallwiener M, Brucker SY, Joos S, Colombo MG, Hawighorst-Knapstein S, Chaudhuri A, Kirtschig G, Saalmann F, Wallwiener S (2023) Long-term effects of preeclampsia on maternal cardiovascular health and postpartum utilization of primary care: an observational claims data study. Arch Gynecol Obstet 307(1):275–284. https://doi.org/10.1007/s00404-022-06561-w
Palmrich P, Binder C, Zeisler H, Kroyer B, Pateisky P, Binder J (2022) Awareness of obstetricians for long-term risks in women with a history of preeclampsia or HELLP syndrome. Arch Gynecol Obstet 305(3): 581-587. https://doi.org/10.1007/s00404-021-06181-w
Boyer A, Lobbedez T, Ouethrani M, Thurillier Lecouf A, Bouvier N, Châtelet V, Hurault de Ligny B (2020) Paternity in male kidney transplant recipients: a French national survey, the PATeRNAL study. BMC Nephrol 21:483. https://doi.org/10.1186/s12882-020-02115-x
Szpotanska-Sikorska M, Mazanowska N, Madej A, Kociszewska-Najman B, Wielgos M, Pietrzak B (2018) Reproductive life planning in women after kidney or liver transplantation. Clin Transplant 32(9):e13378. https://doi.org/10.1111/ctr.13378
van Buren MC, Beck DK, Lely AT, van de Wetering J, Massey EK (2021) EXPloring attitudes and factors influencing reproductive choices in kidney transplant patients (the EXPECT-study). Clin Transplant 35(12):e14473. https://doi.org/10.1111/ctr.14473
Blume C, Pischke S, von Versen-Höynck F, Günter HH, Gross MM (2014) Pregnancies in liver and kidney transplant recipients: a review of the current literature and recommendation. Best Pract Res Clin Obstet Gynaecol 28(8):1123–1136. https://doi.org/10.1016/j.bpobgyn.2014.07.021
Koch-Institut R, Hintzpeter B, Saß A-C, Prütz F, Krause L, Ziese T (2020). RKI Frauengesundheitsbericht. https://doi.org/10.25646/6585
Boyd JM, Mehta A, Murphy DJ (2004) Fertility and pregnancy outcomes in men and women with cystic fibrosis in the United Kingdom. Hum Reprod 19(10):2238–2243. https://doi.org/10.1093/humrep/deh405
Mastrogiacomo I, Bonanni G, Menegazzo E, Santarossa C, Pagani E, Gennarelli M, Angelini C (1996) Clinical and hormonal aspects of male hypogonadism in myotonic dystrophy. Ital J Neuro Sci 17(1):59–65. https://doi.org/10.1007/BF01995710
Jones A, Clary MJ, McDermott E, Coscia LA, Constantinescu S, Moritz MJ, Armenti VT (2013) Outcomes of pregnancies fathered by solid-organ transplant recipients exposed to mycophenolic acid products. Prog Transpl 23(2):153–157. https://doi.org/10.7182/pit2013636
Szymusik I, Warzecha D, Wielgoś M, Pietrzak B (2020) Infertility in female and male solid organ recipients–from diagnosis to treatment: an up-to-date review of the literature. Ann Transplant. https://doi.org/10.12659/AOT.923592
Armenti VT, Moritz MJ, Davison JM (1998) Drug safety issues in pregnancy following transplantation and immunosuppression: effects and outcomes. Drug Saf 19(3):219–232. https://doi.org/10.2165/00002018-199819030-00005
Deshpande NA, James NT, Kucirka LM, Boyarsky BJ, Garonzik-Wang JM, Montgomey RA, Segev DL (2011) Pregnancy outcomes in kidney transplant recipients: a systematic review and meta-analysis: pregnancy outcomes in kidney transplant recipients. Am J Transplant 11(11):2388–2404. https://doi.org/10.1111/j.1600-6143.2011.03656.x
Funding
Open Access funding enabled and organized by Projekt DEAL. This study was supported by departmental funds of the Department of Obstetrics, Gynecology and Reproductive Medicine, Hannover Medical School, Germany.
Author information
Authors and Affiliations
Contributions
F von Versen-Höynck: Project development, questionnaire development, management, manuscript editing. T Zimmermann: Project development, questionnaire development, manuscript editing. N Meyer: Project development, questionnaire development, management of data analysis, manuscript editing. N Schirm: Questionnaire development, data analysis, manuscript editing. L Böhm: Questionnaire development, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study was approved by the Institutional Review Board of Hannover Medical School (approval no. 8900_BO_K_2020).
Concern to participate
All participants gave their informed consent.
Concern to publication
Does not apply.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Böhm, L., Schirm, N., Zimmermann, T. et al. Examining the impact of solid organ transplantation on family planning: pre- and post-transplantation pregnancy evaluations for both women and men. Arch Gynecol Obstet (2024). https://doi.org/10.1007/s00404-024-07689-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00404-024-07689-7