Abstract
The newest data on metallic gold have placed the noble metal central in the fight for the safe treatment of autoimmune inflammation. There are two different ways to use gold for the treatment of inflammation: gold microparticles > 20 µm and gold nanoparticles. The injection of gold microparticles (µGold) is a purely local therapy. µGold particles stay put where injected, and gold ions released from them are relatively few and taken up by cells within a sphere of only a few millimeters in diameter from their origin particles. The macrophage-induced release of gold ions may continue for years. Injection of gold nanoparticles (nanoGold), on the other hand, is spread throughout the whole body, and the bio-released gold ions, therefore, affect multitudes of cells all over the body, as when using gold-containing drugs such as Myocrisin. Since macrophages and other phagocytotic cells take up and transport nanoGold and remove it after a short period, repeated treatment is necessary. This review describes the details of the cellular mechanisms that lead to the bio-release of gold ions in µGold and nanoGold.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Robert Koch discovered the oligodynamic effect of gold salts and started treatment of rheumatoid arthritis (RA) with gold thiocompounds believing that the cause of RA was bacterial infection (Koch 1890; Richards et al. 2002; Rau 2005). Later it became clear that gold-containing drugs inhibit autoimmune inflammation (Forestier 1932; Freyberg and Block 1941; Fricker 1996). Gold thiocompounds were important for many decades in treating RA and are still used when modern drugs fail (Balfourier et al. 2020a; Castro et al. 2022).
Metallic gold was until recently perceived insoluble in the human body, but research has shown that this is not the case (Danscher 2002) (Fig. 1). Gold ions are proven to be bio-released from metallic gold implants, and it is these dicyanogold ions [Au(CN)2−] that are responsible for the anti-inflammatory effects of metallic gold (Larsen et al. 2007; Zainali et al. 2010; Danscher and Larsen 2010; Pedersen et al. 2012; Rasmussen et al. 2022) (Figs. 2, 3).
Autometallographic (AMG) silver enhancement of gold ion accumulation in the tissue. The tissue sections are exposed to UV light to reduce the gold ions to metallic gold atoms (Au0). The resulting nanosized gold particle is enhanced in an AMG developer to study at LM and EM levels. The AMG-enhanced nanoGold-sized particles accumulate in the lysosomes of macrophages, fibroblasts, mast cells, and secretory granules of the mast cells. In this AMG picture, part of a gold grid is shown in the upper part. The dusty appearance of the tissue close to the gold implant represents gold clusters outside cells. The two loaded cells further away are believed to be macrophages (Danscher 2002)
Autometallographic (AMG) illustration of the dissolucytotic release of the gold ions from a gold grid. a Light micrograph of AMG silver-enhanced J774 cells, grown on a gold grid, packed with silver-enhanced gold nanoparticles (after UV radiation). (1) Heavily loaded cell (arrow). (2) Cell filled with tiny AMG grains (black arrowhead). Such gold-dusted cells were recorded already after 2 days of exposure. (3) Dissolucytes containing coarse AMG grains after 5 days of exposure (white arrowhead). The picture is a mosaic composed of J774 cells grown on gold surfaces for 2 and 5 days, respectively. Scale bar, 20 µm. b Liberation of gold ions into the dissolution membrane. Electron micrograph of a macrophage and its dissolution membrane. The grid to which the cell was attached is removed during the tissue preparation. Notice the AMG-enhanced gold nanoparticles within the membrane. Scale bar, 3 µm. c Electron micrograph of the dissolution membrane to show the AMG grains at higher magnification. Dissolution membrane (dm), cytoplasm (cyt), and nucleus (nuc). Scale bar, 200 nm (Larsen et al. 2007)
μGold particles (> 20 µm) stay put where they are injected and attract macrophages that liberate gold ions into the intracellular space through dissolucytosis. In contrast, nanoGold particles spread systemically, and in the macrophage lysosomal compartment, there is oxidation to gold ions. The bio-released gold ions (Au+), most likely present as dicyanoaurate ions (Au(CN)2–) that pharmaceutically influence the intracellular microenvironment as well as macrophages, mast cells, and fibroblasts, that is, the bio-released gold ions affect the immune response, inflammation, and regeneration (Rasmussen et al. 2022)
Historical use in medicine
Several papers prove the immunosuppressing effects of gold by analyzing the outcome of gold-containing drugs on autoimmune diseases (e.g., join inflammation/arthrosis, psoriasis, asthma, psoriasis), impact on cancer, and their antimicrobial (oligodynamic) effects (Chakravarty and Kundu 2019). Gold ions inhibit the cell growth of certain infectious microbes and make these organisms more susceptible to oxidative stress and death (Harbut et al. 2015). Laboratory researchers have demonstrated that even low concentrations of gold nanoparticles exhibit definite inhibitory action against cultures of methicillin-resistant Staphylococcus aureus (Kalita et al. 2018).
Gold compounds like aurothiomalate (Myocrisin) are known to reduce inflammation related to rheumatoid arthritis (RA) by releasing gold ions. Treatment with gold thiocompounds did play a significant role in rheumatology for many years. Several clinical trials show that gold ions reduce RA inflammation, reduce radiographic progression, and often induce sustained remission (Williams et al. 1984; Yamashita et al. 1999; Roche 2006).
Mode of action
In vitro experiments on activated macrophages (Zetterström et al. 2008) showed that aurothiomalate inhibits the extracellular release of high mobility group box chromosomal protein 1 (HMGB1) and has no effect on the secretion of tumor necrosis factor (TNF). They found that aurothiomalate inhibits the endogenous mediators of HMGH1 translocation, interferon beta (IFN-β), and nitrous oxygen (NO). HMBG1 provokes inflammation and is possibly the key process underlying the development of rheumatoid arthritis. HMBG1 is a molecule with dual function. It behaves in one way inside the cell and in another outside (Zetterström et al. 2008; Pisetsky 2017).
Inside the nucleus, HMGB1 plays a role in the transcription of DNA to RNA (Zetterström et al. 2008; Pisetsky 2017). When released from the cell, HMGB1 stimulates the immune system and induces inflammation. There is an unusually high amount of HMGB1 in the synovial tissues and the fluid around inflamed joints. The authors (Zetterström et al. 2008) stimulated mouse and human immune system cells to secrete HMGB1, and then they were treated with aurothiomalate. They found that gold ions blocked the release of HMGB1 from the nucleus reducing the amount available to provoke the body’s immune system and attenuating the inflammatory response. They suggest that gold inhibits the release of HMGB1 by interfering with the activity of two helper molecules, INF and NO, that ease the release of HMGB1 from the cell.
Based on the accumulation of gold in lysosomes of macrophages, fibroblasts, and mast cells (Wojtecka-Lukasik et al. 1986; Shalit and Levi-schaffer 1990; Danscher 2002; Pisetsky 2017), it is tempting to hypothesize that gold ions may have a similar effect on HMGB1 in fibroblasts, mast cells, and other cells of inflammation and may influence the intercellular matrix composition of collagen, reticular, and elastin fibers. Gold-ion-loaded macrophages and mast cells move away over time, and new cells take over (Fig. 3). The µGold particles stay put and continuously expose the matrix and the new cells to gold ions and influence the production of a new intercellular matrix. Contrarily, the macrophages and mast cells will remove the nanoGold from the connective tissue as these cells move away over time (Sadauskas et al. 2007; Balfourier et al. 2020b).
Aurosomes in macrophages, mast cells, and fibroblasts
A lysosome that contains gold is called an aurosome. The almost explosive increase in our understanding of macrophages (Maruotti et al. 2007), mast cells, and the effect of gold ions on autoimmune inflammation make the introduction of metallic gold implants, e.g., µGold, even more exciting from a treatment point of view (Shapouri-Moghaddam et al. 2018).
Because of its chemical inertness, it was a common belief that metallic gold remains untouched in the body. However, as has been described, gold particles larger than 20 µm, and macro-implants, have been proven to be slowly dissolved by macrophages through a process coined dissolucytosis (Danscher 2002; Larsen et al. 2007, 2008; Seifert et al. 2012) (Fig. 3). Dissolucytosis is a continuous process, dependent only on the number of macrophages, i.e., the inflammatory status, inflammation, or no inflammation of the tissue, and the available gold surfaces at a given location.
The amount of bio-released gold ions is so discrete that all the biologically active Au+ or Au (CN)2− (Graham and Dale 1990) remain in a millimeter-sized sphere around the injected µGold particles (Graham 1990). Mast cells, fibroblasts, and other macrophages within this sphere take up the gold ions. The fact that only cells close to the µGold particles become loaded with gold implies that no gold ions are spread to gold-sensitive organs and exclude any toxic effects. The use of µGold, therefore, is considered a safe technique (Danscher 2002; Larsen et al. 2007; Danscher and Larsen 2010).
The knowledge about the gold ions while in the intercellular space is sparse. They may present as dicyanoaurate, the gold compound found in the urine of Myocrisin-treated patients (Tepperman et al. 1994; Minakata et al. 2009). The continuous supply of gold ions into the intercellular space by µGold influences the extracellular environment continuously (Figs. 3, 4). Comprehensive studies are required to understand the changes they impose on the extracellular molecules and elements such as collagen, reticular fibers, or elastic fibers. Gold ions may suppress the amount of granulation tissue as the gold ions suppress the production of collagen probably by a reduction in the number of macrophages (Wojtecka-Łukasik et al. 1986; Larsen et al. 2007; Danscher 2017; Balfourier et al. 2020a). It is worth noting that macrophages produce the cytokines PDGF and TGF. They activate fibroblasts producing procollagen, trigger reendothelialization, and stimulate the formation of new blood vessels (Wynn and Barron 2010).
Once in the intercellular fluid and the intracellular compartment, the gold ions act in the same ways as systemically administered gold ions. One of the pharmacological effects may be related to the ability of the gold ions to change the folding of the protein structures. (Rasmussen et al. 2022)
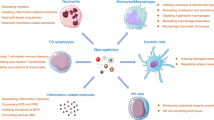
During the inflammatory process, macrophages acquire a plastic phenotype ranging from being pro-inflammatory (M1) to anti-inflammatory (M2) (Fernandes et al. 2020). Different stimuli polarize the macrophages. IFN-g, LPA, and TNF-a polarize to M1, and IL-4, Il-3, Il-10, and TLRs polarize against M2. The M2 macrophage has wound-healing capacities and is pro-chondrogenic. Gold ions initiate an anti-inflammatory response (Seifert et al. 2012), and a clinical pilot study shows this impact of gold ions on the macrophages (Rasmussen et al. 2022) (Figs. 4, 5), though further analysis concerning the polarization is needed.
Proteome changes in SF and serum found during treatment indicate involvement of multiple functional pathways and signaling processes, including wound healing, regulation of the humoral and adaptive immune system, and neutrophil degranulation (Rasmussen et al. 2022)
nanoGold
With the increasing popularity and use of nanometer-sized gold particles (nanoGold), the impact of the smaller metal particles on inflammation has received considerable attention (Brown et al. 2007; James et al. 2015; Han et al. 2022). When the gold particles are bigger than 20 µm, they are too big for the macrophages to engulf, and the macrophages thus proceed to secrete cyanide compounds and dissolve the gold into cyanide–gold complexes such as Au(CN)2− (Larsen et al. 2008; Zainali et al. 2010; Danscher and Larsen 2010) (Figs. 2, 3). The macrophages degrade nanoGold in a fundamentally different way than µGold. nanoGold particles are oxidized in the lysosomes of the macrophages after being phagocytosed (Carlander et al. 2019) or extracellularly by way of reactive nitrogen species from macrophages (McCarrick et al. 2021). The gold ions diffuse from the lysosomes into the intracellular cytoplasm and nuclei, where they exert their influence on inflammation. nanoGold particles are a possible treatment for rheumatoid arthritis and have a temporal beneficial effect on inflammation (Balfourier et al. 2020a, b).
Lysosomal disintegration of nanoGold causes an intracellular creation of gold ions, having the same effect as gold ions arriving from gold complexes (e.g., Myocrisin) or bio-released gold ions from µGold. While gold complexes and nanoGold spread to all parts of the body and need repeated injections to keep the number of gold ions at a pharmaceutical level (Balfourier et al. 2020b), gold ions released from µGold particles are a purely local process that slowly, but continuously release local pharmaceutical levels of active gold ions into the intercellular space (Rasmussen et al. 2022).
For more than 50 years, gold-containing drugs like Myocrisin have been in use for the treatment of different autoimmune maladies, and an overwhelming amount of literature has been gathered proving that gold ions are potent immune suppressors (Petersen and Bendtzen 1983). Dicyanogold ions (Au(CN)2–) affect lymphokine production and are a common metabolite found in blood and urine samples from patients treated with different gold-based drugs (Tepperman et al. 1994, 1999).
µGold
As the release of gold ions from gold microparticles is carried out by macrophages that settle on the gold surface, the surface area per weight of gold must be as high as possible. The microparticles must not be smaller than particles ≥ 20 µm, or they will be phagocytosed by the macrophages and treated in the lysosomes like gold nanoparticles. When placed into the tissue, proteins are adsorbed to the surface, creating a nanometer-thick membrane (Danscher 2002; Seifert et al. 2012).
The macrophages organize the initial molecular “membrane” between themselves and the gold surface, creating a dissolution membrane (Danscher 2002; Larsen et al. 2007) (Figs. 1, 2). The macrophages control the chemical conditions and milieu in the dissolution membrane and secrete, among others, cyanide ions into the membrane. At the surface of the gold microparticle and the optimal oxygen tension and pH, the macrophages oxidate gold atoms to monovalent gold ions (Au+). The gold ions then extracellularly in the dissolution membrane bind to cyanide ions (CN)− and create dicyanoaurate ions [Au(CN)2−]. The dicyanoaurate ions diffuse from the dissolution membrane into the intercellular space, bind to soluble and membrane-bound proteins containing sulfur, and are taken up and concentrated in the lysosomes of the cells (Larsen et al. 2007; Minakata et al. 2009; Danscher and Larsen 2010). Some of the gold-loaded proteins, positioned in the cellular membrane of the dissolucytotic macrophages, themselves, in local mast cells, fibroblasts, and the interstitial fluid, are found in the lysosomes and mast cells, additionally in the basophilic granules (Danscher 2002; Danscher and Larsen 2010) Using the histochemical technique autometallography (AMG) (Jacobsen et al. 1989; Danscher 2002; Danscher and Stoltenberg 2006), gold ions liberated from gold implants can be traced in macrophages, mast cells, and fibroblasts and fibers, the same cells that take up gold ions in patients injected with aurothiomalate (Myocrisin) (Møller-Madsen et al. 1987; Graudal and Møller-Madsen 1988; Jacobsen et al. 1989).
If the tissue is in a state of inflammation when injecting the gold microparticles, or if the inflamed tissues already contain gold microparticles, there may be a higher release of gold ions compared with tissues not affected by inflammation. The reason for this effect is not yet determined but is likely in part related to the significant increase in the number of macrophages associated with inflammation. This may explain the clinical findings in patients with knee osteoarthritis and effusion (Rasmussen et al. 2022).
Another important observation is that metal implants in animal studies stay well fixed when there is a partial coating with gold (Zainali et al. 2013) but exhibit inferior fixation when there is a complete gold coating (Zainali et al. 2009). A third study using particulate gold in bone allograft influenced the cells adjacent to the gold microparticles without reducing the implant fixation (Zainali et al. 2010). These studies indicate that gold ions reduce inflammation and the number of granular cells, fibroblasts, and collagen (Danscher and Larsen 2010) and may reduce the capsular membrane around the implants. Adding gold to the surface of an implant may cause a substantial prolongation of the stability of the bone-metal zone (Zainali et al. 2010, 2013). This observation calls for further evaluation.
An important issue when applying metallic gold is whether magnetic resonance imaging (MRI) may cause a negative effect. One study investigated the matter using upper eyelid gold weight implants placed in an open chamber exposed to 1.5 T and subcutaneously in six rats (Marra et al. 1995). There were no displacements or adverse effects, suggesting that it is safe to perform MRI on patients treated with µGold particles.
nanoGold versus µGold
There is a temporary and beneficial effect of nanoGold on autoimmune inflammation (Balfourier et al. 2020b). In contrast, µGold induce a long-lasting up to 2-year suppression or even a shutdown effect on the inflammation in joints suffering from osteoarthritis (Rasmussen et al. 2022) (Fig. 5). nanoGold may be less acutely toxic than gold-containing drugs such as Myocrisin. However, there are no studies of the long-termed effects of gold nanoparticle treatment on humans, but one study on acute and chronic administration of nanoGold finds they cause DNA damage in the cerebral cortex of adult rats (Cardoso et al. 2014). It is general knowledge that nanoGold will enter an unknown multitude of cells, including neurons and tubular cells of the kidney, that might make long-term treatment problematic. Moreover, the liver is known to be central in the accumulation of nanoGold (Sadauskas et al. 2007, 2009).
Increased release of gold ions in inflammatory tissue
If the tissue containing µGold is or becomes inflammatory, the amount of released gold ions increases, most likely because the amount of dissolucytotic macrophages increases until the inflammation has ceased (Danscher et al. 2008 unpublished results). In a transplantation study of the ability of gold microparticles to suppress inflammation and delay rejection of the transplanted tissue, gold microparticles cause a pronounced decrease in the formation of granulation tissue (Danscher et al. 2006). As both macrophages and mast cells are major players in the inflammatory process (Tamang et al. 2012; Xu and Shi 2012), placement of pure metallic gold (99.99%) in inflammatory tissues will interact profoundly with the inflammatory processes, leading to repression or even to a total cessation of the inflammation (Rasmussen et al. 2022) (Fig. 5).
More speculative is the notion that the gold ions cause the formation of new chondrocytes in the gold-treated joints, but the finding that gold particles injected into brain lesions evoke neogenesis of glial cells supports the possibility (Pedersen et al. 2012). Whether osteophytes may be affected by treating a diseased joint with µGold or may stay unaffected and not increase in size is not known.
As mentioned above, gold nanoparticles are taken up by macrophages and concentrated in the lysosomes (Sadauskas et al. 2007). In the lysosomes of the macrophages, oxidation turns nanoparticles into monovalent gold ions (Au+) (Carlander et al. 2019). The lysosomes end up having a load of gold ions as after the extracellular dissolucytosis of µGold or after injection of Myocrisin. Electron microscopy detects the presence of gold ions in the lysosomes (Danscher 2002; Carlander et al. 2019) (Figs. 1, 2).
Conclusion
Pain or nociception is a protective sensation that, in physiological conditions, is of paramount importance to humans and other living organisms to the extent that it must be considered essential for survival.
Thus, finding an effective treatment that suppresses inflammation and reduces pain is a topic for basic researchers and clinical doctors. A safe local gold cure might comprehend such qualities as the goal of the ongoing research on bio-released gold ions from gold implants.
From experimental and empirical evidence, and soon hopefully supported by more clinical studies, we know that the number of gold ions released from metallic gold implants is sufficient to cause a local effect around the implant (Seifert et al. 2012; Pedersen et al. 2012; Rasmussen et al. 2022) (Fig. 5).
We do now know whether the pain-reducing effect of gold ions results from anti-inflammatory characteristics or includes a direct impact of gold ions on pain perception. However, the visible decline in the local edema suggests that inhibition of histamine release from mast cells by monovalent gold ions might play a role (Shalit and Levi-Schaffer 1990). Since the scientific proof of macrophage-caused liberation of gold ions in connective tissue and the brain is established (Danscher 2002), several animal models of such maladies (Lie et al. 2011; Jæger et al. 2012; Pedersen et al. 2012; Märki et al. 2018) and a human trial (Rasmussen et al. 2022) prove the rational use of gold as treatment of noninfectious or autoimmune inflammation.
Data availability
The references and data analysed during the current study are available from the corresponding author on reasonable request.
References
Balfourier A, Kolosnjaj-Tabi J, Luciani N et al (2020a) Gold-based therapy: from past to present. Proc Natl Acad Sci USA 117:22639–22648. https://doi.org/10.1073/pnas.2007285117
Balfourier A, Luciani N, Wang G et al (2020b) Unexpected intracellular biodegradation and recrystallization of gold nanoparticles. Proc Natl Acad Sci USA 117:103–113. https://doi.org/10.1073/pnas.1911734116
Brown C, Bushell G, Whitehouse M, Agrawal DS, Tuoe SG, Paknikar KM, Tiekink E (2007) Nanogold-pharmaceutics. Gold Bull 40:245–250
Cardoso E, Rezin GT, Zanoni ET, de Souza Notoya F, Leffa DD, Damiani AP, Daumann F, Rodriguez JC, Benavides R, da Silva L, Andrade VM, da Silva Paula MM (2014) Acute and chronic administration of gold nanoparticles cause DNA damage in the cerebral cortex of adult rats. Mutat Res 766–767:25–30. https://doi.org/10.1016/j.mrfmmm.2014.05.009
Carlander U, Midander K, Hedberg YS et al (2019) Macrophage-assisted dissolution of gold nanoparticles. ACS Appl Bio Mater 2:1006–1016. https://doi.org/10.1021/acsabm.8b00537
Chakravarty IKS (2019) Oligodynamic boons of daptomycin and noble metal nanoparticles packaged in an Anti-MRSA topical gel formulation. Curr Pharm Biotechnol 20:707–718. https://doi.org/10.2174/1389201020666190621103416
Danscher G (2002) In vivo liberation of gold ions from gold implants. Autometallographic tracing of gold in cells adjacent to metallic gold. Histochem Cell Biol 117:447–452. https://doi.org/10.1007/s00418-002-0400-8
Danscher G (2017) Gold particles for use in therapy to prevent or reduce capsular contracture. Eur Pat Off, pp 1–9
Danscher G, Larsen A (2010) Effects of dissolucytotic gold ions on recovering brain lesions. Histochem Cell Biol 133:367–373. https://doi.org/10.1007/s00418-010-0681-2
Danscher G, Stoltenberg M (2006) Silver enhancement of quantum dots resulting from (1) metabolism of toxic metals in animals and humans, (2) in vivo, in vitro and immersion created zinc-sulphur/zinc-selenium nanocrystals, (3) metal ions liberated from metal implants and particles. Prog Histochem Cytochem 41:57–139. https://doi.org/10.1016/j.proghi.2006.06.001
de Castro CT, de Queiroz MJ, Albuquerque FC et al (2022) Real-world effectiveness of biological therapy in patients with rheumatoid arthritis: Systematic review and meta-analysis. Front Pharmacol 13:1–16. https://doi.org/10.3389/fphar.2022.927179
Fernandes TL, Gomoll AH, Lattermann C et al (2020) Macrophage: a potential target on cartilage regeneration. Front Immunol 11:1–9. https://doi.org/10.3389/fimmu.2020.00111
Forestier J (1932) The treatment of rheumatoid arthritis with gold salts. Lancet 219:441–444
Freyberg RH, Block WD, Levey S (1941) Metabolism, toxicity and manner of action of gold compounds used in the treatment of arthritis. I. Human plasma and synovial fluid concentration and urinary excretion of gold during and following treatment with gold sodium thiomalate, gold sodium thiosulfate, and colloidal gold sulfide. J Clin Invest 20:401–412. https://doi.org/10.1172/JCI101235
Fricker SP (1996) Medical uses of gold compounds: past, present and future. Gold Bull 29:53–60. https://doi.org/10.1007/bf03215464
Graham GGDM (1990) The activation of gold complexes by cyanide produced by polymorphonuclear leukocytes—II. Evidence for the formation and biological activity of aurocyanide. Biochem Pharmacol 39:1697–1702. https://doi.org/10.1016/0006-2952(90)90113-y
Graudal H, Møller-Madsen BDG (1988) Autometallographic demonstration of gold in rheumatoid synovial tissue. Z Rheumatol 47:347–350
Han X, Avelar E, Mathai A et al (2022) A clinical study to evaluate the safety and efficacy of oral administration of microscopic dose gold nanoparticle (AuNP) on knee joint health and function in arthritis patients. J Funct Morphol Kinesiol 7:1–21. https://doi.org/10.3390/jfmk7030052
Harbut MB, Vilchèze C, Luo X et al (2015) Auranofin exerts broad-spectrum bactericidal activities by targeting thiol-redox homeostasis. Proc Natl Acad Sci USA 112:4453–4458. https://doi.org/10.1073/pnas.1504022112
Jacobsen E, Andreasen A, Graudal H, Danscher G (1989) Autometallographic demonstration of gold uptake in cultured synovial fluid cells from patients with rheumatoid arthritis. Scand J Rheumatol 18:161–164. https://doi.org/10.3109/03009748909095414
Jæger GT, Stigen Ø, Devor M, Moe L (2012) Gold bead implantation in acupoints for coxofemoral arthrosis in dogs: method description and adverse effects. Animals 2:426–436. https://doi.org/10.3390/ani2030426
James LRA, Xu ZQ, Sluyter R et al (2015) An investigation into the interactions of gold nanoparticles and anti-arthritic drugs with macrophages, and their reactivity towards thioredoxin reductase. J Inorg Biochem 142:28–38. https://doi.org/10.1016/j.jinorgbio.2014.09.013
Kalita S, Kandimalla R, Bhowal AC et al (2018) Functionalization of β-lactam antibiotic on lysozyme capped gold nanoclusters retrogress MRSA and its persisters following awakening. Sci Rep 8:1–13. https://doi.org/10.1038/s41598-018-22736-5
Koch R (1890) Ueber bakteriologische forschung. Verlag von August Hirschwald, Berlin, pp 1–15
Larsen A, Kolind K, Pedersen DS et al (2008) Gold ions bio-released from metallic gold particles reduce inflammation and apoptosis and increase the regenerative responses in focal brain injury. Histochem Cell Biol 130:681–692. https://doi.org/10.1007/s00418-008-0448-1
Larsen A, Stoltenberg M, Danscher G (2007) In vitro liberation of charged gold atoms: autometallographic tracing of gold ions released by macrophages grown on metallic gold surfaces. Histochem Cell Biol 128:1–6. https://doi.org/10.1007/s00418-007-0295-5
Lie KI, Jæger G, Nordstoga K, Moe L (2011) Inflammatory response to therapeutic gold bead implantation in canine hip joint osteoarthritis. Vet Pathol 48:1118–1124. https://doi.org/10.1177/0300985810381910
Märki N, Witte S, Kuchen S et al (2018) Safety of intra-articular gold microimplants in horses–a randomized, blinded, controlled experimental study. J Equine Vet Sci 60:59-66.e2. https://doi.org/10.1016/j.jevs.2017.03.005
Marra S, Konior RJ, Leonetti JP, Raslan W (1995) Effect of magnetic resonance imaging on implantable eyelid weights. Ann Otol Rhinol Laryngol 104:448–452. https://doi.org/10.1177/000348949510400606
Maruotti N, Cantatore FP, Crivellato E, Vacca ARD (2007) Macrophages in rheumatoid arthritis. Histol Histopathol 22:581–586. https://doi.org/10.14670/HH-22.581
McCarrick S, Midander K, Krausová M et al (2021) Gold nanoparticles dissolve extracellularly in the presence of human macrophages. Int J Nanomed 16:5895–5908. https://doi.org/10.2147/IJN.S314643
Minakata K, Nozawa H, Gonmori K et al (2009) Determination of cyanide, in urine and gastric content, by electrospray ionization tandem mass spectrometry after direct flow injection of dicyanogold. Anal Chim Acta 651:81–84. https://doi.org/10.1016/j.aca.2009.08.001
Møller-Madsen B, Danscher G, Uldbjerg NAJ (1987) Autometallographic demonstration of gold in human fetal liver and placenta. Rheumatol Int 7:47–48. https://doi.org/10.1007/BF00267342
Pedersen DS, Fredericia PM, Pedersen MO et al (2012) Metallic gold slows disease progression, reduces cell death and induces astrogliosis while simultaneously increasing stem cell responses in an EAE rat model of multiple sclerosis. Histochem Cell Biol 138:787–802. https://doi.org/10.1007/s00418-012-0996-2
Petersen J, Bendtzen K (1983) Immunosuppressive actions of gold salts. Scand J Rheumatol 12:28–35. https://doi.org/10.3109/03009748309095340
Pisetsky DS (2017) Antinuclear antibody testing - misunderstood or misbegotten? Nat Rev Rheumatol 13:495–502. https://doi.org/10.1038/nrrheum.2017.74
Rasmussen S, Kjær Petersen K, Kristiansen MK et al (2022) Gold micro-particles for knee osteoarthritis. Eur J Pain (UK) 26:811–824. https://doi.org/10.1002/ejp.1909
Rau R (2005) Have traditional DMARDs had their day? Effectiveness of parenteral gold compared to biologic agents. Clin Rheumatol 24:189–202. https://doi.org/10.1007/s10067-004-0869-8
Richards DG, McMillin DL, Mein EA, Nelson CD (2002) Gold and its relationship to neurological/glandular conditions. Int J Neurosci 112:31–53. https://doi.org/10.1080/00207450212018
Roche PA (2006) Gold-plating MHC class II molecules. Nat Chem Biol 2:178–179. https://doi.org/10.1038/nchembio0406-178
Sadauskas E, Danscher G, Stoltenberg M et al (2009) Protracted elimination of gold nanoparticles from mouse liver. Nanomed Nanotech Biol Med 5:162–169. https://doi.org/10.1016/j.nano.2008.11.002
Sadauskas E, Wallin H, Stoltenberg M et al (2007) Kupffer cells are central in the removal of nanoparticles from the organism. Part Fibre Toxicol 4:1–7. https://doi.org/10.1186/1743-8977-4-10
Seifert O, Matussek A, Sjögren F et al (2012) Gene expression profiling of macrophages: implications for an immunosuppressive effect of dissolucytotic gold ions. J Inflamm (UK). https://doi.org/10.1186/1476-9255-9-43
Shalit M, Levi-schaffer F (1990) Auranofin inhibits histamine release from rat peritoneal mast cells. Int J Immunopharmaco 12:403–407. https://doi.org/10.1016/0192-0561(90)90022-f
Shapouri-Moghaddam A, Mohammadian S, Vazini H et al (2018) Macrophage plasticity, polarization, and function in health and disease. J Cell Physiol 233:6425–6440. https://doi.org/10.1002/jcp.26429
Tamang TL, Pullen N, Ryan J (2012) Mast cell-macrophage interactions alter inflammatory cytokine production. J Immunol 188:177.10
Tepperman K, Zhang Y, Roy PW et al (1994) Transport of the dicyanogold (I) anion. Met Based Drugs 1:433–443. https://doi.org/10.1155/MBD.1994.433
Tepperman K, Roy PW, Moloney BF, Elder RC (1999) Dicyanogold effects on lymphokine production. Met Based Drugs 6:301–309. https://doi.org/10.1155/MBD.1999.301
Williams HJ, Ward JR, Egger MJ, Reading JC, Samuelson CO, Altz-Smith M, Willkens RW, Solsky MA, Hayes SP, Furst D et al (1984) Auranofin, gold sodium thiomalate, and placebo in the treatment of rheumatoid arthritis. Cooperative systematic studies of rheumatic diseases. Clin Rheumatol. https://doi.org/10.1007/BF03342621
Wojtecka-Lukasik E, Sopata I, Maśliński S (1986) Auranofin modulates mast cell histamine and polymorphonuclear leukocyte collagenase release. Agents Actions 18:86–70. https://doi.org/10.1007/BF01987985
Wojtecka-Łukasik E, Sopata I, Maśliński S (1986) Auranofin modulates mast cell histamine and polymorphonuclear leukocyte collagenase release. Agents Actions 18:68–70. https://doi.org/10.1007/BF01987985
Wynn TABL (2010) Macrophages: master regulators of inflammation and fibrosis. Semin Liver Dis 30:245–257. https://doi.org/10.1055/s-0030-1255354
Xu JM, Shi GP (2012) Emerging role of mast cells and macrophages in cardiovascular and metabolic diseases. Endocr Rev 33:71–108. https://doi.org/10.1210/er.2011-0013
Yamashita M, Ichinowatari G, Yamaki K, Ohuchi K (1999) Inhibition by auranofin of the production of prostaglandin E2 and nitric oxide in rat peritoneal macrophages. Eur J Pharmacol 368:251–258. https://doi.org/10.1016/S0014-2999(99)00053-9
Zainali K, Danscher G, Jakobsen T, Jakobsen SS, Baas J, Møller P, Bechtold JESK (2009) Effects of gold coating on experimental implant fixation. J Biomed Mater Res A 88:274–280. https://doi.org/10.1002/jbm.a.31924
Zainali K, Baas J, Jakobsen T et al (2010) Particulate gold as an anti-inflammatory mediator in bone allograft-An animal study. J Biomed Mater Res - Part A 95:956–963. https://doi.org/10.1002/jbm.a.32928
Zainali K, Danscher G, Jakobsen T et al (2013) Assessment of modified gold surfaced titanium implants on skeletal fixation. J Biomed Mater Res - Part A 101A:195–202. https://doi.org/10.1002/jbm.a.34307
Zetterström CK, Jiang W, Wähämaa H et al (2008) Pivotal Advance: Inhibition of HMGB1 nuclear translocation as a mechanism for the anti-rheumatic effects of gold sodium thiomalate. J Leukoc Biol 83:31–38. https://doi.org/10.1189/jlb.0507323
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
Both authors had the idea for the article and contributed equally to the literature search, drafting and critically revised the work. Both authors have approved the manuscript before the submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
Both authors are involved in companies working with gold and inflammation, Berlock ApS and ReGold ApS.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Danscher, G., Rasmussen, S. nanoGold and µGold inhibit autoimmune inflammation: a review. Histochem Cell Biol 159, 225–232 (2023). https://doi.org/10.1007/s00418-023-02182-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-023-02182-9