Abstract
Background
The removal of common bile duct stones by endoscopic retrograde cholangiopancreatography (ERCP) shows excellent results with low complication rates and is therefore considered a gold standard. However, in case of stones non-removable by ERCP, surgical extraction is needed. The surgical approach is still controversial and clinical guidelines are missing. This study aims to analyze the outcomes of patients treated with choledochotomy or hepaticojejunostomy for common bile duct stones.
Methods
All patients who underwent choledochotomy or hepaticojejunostomy for common bile duct stones at a tertiary referral hospital over 11 years were included. The analyzed data contains basic demographics, diagnostics, surgical parameters, length of hospitalization, and morbidity and mortality.
Results
Over the study period, 4375 patients underwent cholecystectomy, and 655 received an ERCP with stone extraction, with 48 of these patients receiving subsequent surgical treatment. ERCP was attempted in 23/30 (77%) of the choledochotomy patients pre/intraoperatively and 11/18 (56%) in hepaticojejunostomy patients. The 30-day major complication rate (Clavien-Dindo > II) was 1/30 (3%) in the choledochotomy group and 2/18 (11%) in the hepaticojejunostomy group. Complications after 30 days occurred in 3/30 (10%) patients and 2/18 (11%), respectively, and no mortality occurred.
Conclusion
ERCP should still be considered the gold standard, although due to low short- and long-term morbidity rates, choledochotomy and hepaticojejunostomy represent effective surgical solutions for common bile duct stones.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Common bile duct stones (CBDS) are present in about 10–20% of patients with symptomatic gallstones [1,2,3,4]. Occlusion of the common bile duct (CBD) can lead to pathologic liver function tests with a cholestatic picture and complications such jaundice, cholangitis, liver abscesses, or pancreatitis [5, 6]. Recurrence of CBDS is the most common long-term complication after gallstone surgery, and patients usually present with acute cholangitis [7, 8].
Since the National Institutes of Health Consensus Conference in 1993, laparoscopic cholecystectomy is the current gold standard for gallstone disease [9]. In obstructive cholelithiasis, ERCP with endoscopic sphincterotomy as well as laparoscopic surgery has replaced open cholecystectomy (CCY) with choledochotomy or sphincterotomy in combination with bile duct clearance [10, 11]. In modern days with significant advances of the endoscopic standard techniques, CBDS clearance rates above 80% should be expected. In combination with further advanced techniques such as mechanical lithotripsy, success rates increased to more than 90%. In the remaining cases, additional specific endoscopic procedures (i.e., electrohydraulic, laser, or extracorporeal shockwave lithotripsy) or surgery is needed [12].
Apart from the gold standard of ERCP and laparoscopy [13, 14], several studies describe open cholecystectomy with bile duct exploration as a safe and feasible alternative in challenging cases [15,16,17,18,19]. Interestingly, some studies specify open choledochotomy as superior in clearing CBDS without a negative impact on morbidity or mortality [20,21,22].
Furthermore, Roux-en-Y hepaticojejunostomy (HJS) is a surgical modality for the treatment of recurrent CBDS after unsuccessful interventional therapy to allow bile drainage [23, 24].
Clinical guideline recommendations for the surgical management of recurrent CBDS are missing [24]. Therefore, the aim of this study was to describe the short- and long-term outcomes as well as the recurrence of CBDS after surgical management with choledochotomy and HJS.
Material and methods
In this retrospective single-center analysis, we included all patients who underwent choledochotomy or HJS for CBDS between 2009 and 2020 at St. Clara Hospital in Basel, Switzerland. Additionally, total numbers of CCY and acute cholecystitis cases were documented. Patient records of hospitalization for choledochotomy/HJS and all relevant clinical follow-up information concerning recurrence, surgery, or death were compiled. The data included demographics such as age, gender, previous abdominal surgeries, details about the choledochotomy and HJS procedure, complications, duration of total hospital stay, revisional surgery and/or reintervention rate, morbidity, and mortality [25, 26]. Complications were classified according to the Clavien-Dindo (CD) classification and divided into short- and long-term complications [27,28,29]. In this study, we defined short-term complications within a period of 30 days postoperative and long-term complications after 30 days. Follow-up data was collected through patient’ readmission at St. Clara Hospital Basel or University Hospital Basel in any subspecialty unit. Furthermore, preoperative ERCP were analyzed. The total amount of CCY and ERCP over the same period served as a reference value. Reporting followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guideline where appropriate [30].
Data were extracted retrospectively in dedicated electronic databases (CGM PHOENIX) by trained contributors with regular auditing and guidance by the principal investigator from a prospective consecutive institutional database (Microsoft Office created ACCESS-database, version 14.0.7015. 1000, Office 2013; Microsoft Corporation, Redmond, Washington, USA).
We used descriptive statistics to summarize patient, treatment, and disease characteristics. Baseline differences between the two groups were calculated using the χ2 test, the t-test, or the Welch test as appropriate. Data are shown as mean ± SD. Ethical approval was granted by the ethics commission of North West Switzerland with the registration number EKNZ 2020–00076.
Results
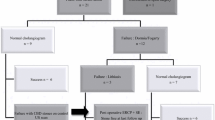
In the reported time period of 11 years, 4375 patients underwent CCY, and 1801 patients received ERCP, of which 655 had a stone extraction. 48 patients underwent surgery for open bile duct exploration because of CBDS, resulting in either choledochotomy (30; 63%) or hepaticojejunostomy (18; 37%). Further information about the patient characteristics at the time of the first presentation can be found in Table 1.
Surgery time was significantly longer in the HJS group with a mean time of 291 ± 72 min (95% CI: 219–363) compared to 174 ± 25 min (95% CI: 149–199) in the choledochotomy group (p value < 0.01). In the HJS group, the gallbladder was removed prior to bile duct resection in 13/18 cases (72%) whereas in the choledochotomy group this was the case in 8/30 patients (27%) (p value = 0.01).
Within 30 days after surgery, 16/48 patients (33%) needed treatment due to complications. Grade I and II complications occurred in 13/48 (25%) patients, grade IIIa and IIIb in three patients (6%), and one patient (2%) suffered a grade IVa complication and had to be transferred to intensive care unit. One patient needed postoperative abscess drainage, in one patient the HJS had to be refashioned after 10 days, and one patient developed postoperative heart failure. There was no reported mortality within the first 30 postoperative days.
5/48 patients (10%) were readmitted > 30 days after surgery, three (10%) in the choledochotomy group and two (11%) in the HJS group. All three complications in the choledochotomy group were due to recurrent cholelithiasis and could be treated with ERCP. In the HJS group, one patient (5.6%) presented to our department again after 295 days due to recurrent choledocholithiasis and was treated by drainage and removal of the bile duct stone through balloon extraction. In one patient, recurrent cholangitis occurred after more than two years and was treated conservatively with antibiotics. Interestingly, one patient initially presented with an existing HJS which had been done 23 years earlier in a different hospital. A stricture could be identified radiologically, and new HJS with further bile duct resection was done (Tables 2 and 3).
Discussion
Minimally invasive methods such as ERCP have been well established as the gold standard for the treatment of CBDS. However, even with an increase of reliability over the past decades, some CBDS cannot be successfully treated with ERCP. This study demonstrates that choledochotomy and HJS are both well-established methods for the management of CBDS. Even though choledochotomy and HJS are usually used in highly complicated cases of CBDS, complication rates are relatively low and represent a valid alternative to laparoscopic bile duct surgery. Based on our findings, shorter operation times, lower short-term complication rates, a sufficient long-term outcome considering CBDS recurrence, and additional surgical options seem to be the main advantages of choledochotomy over the establishment of a hepaticojejunostomy.
The study shows that open surgery such as choledochotomy for complex bile duct stones is a rare procedure. This is in line with the guidelines of using ERCP as the gold standard and shows that surgery was only suggested if previous interventions failed or were not possible [13, 14, 32].
Taking into account our results, open surgery can be considered a safe and feasible procedure in the treatment of CBDS, even in a hospital without a specialized hepatobiliary surgeon. It has to be noted that training can be challenging, since with the advances in ERCP procedures case numbers have become rare. Consequently, the method of choice should be based on the preference and experience of the operating surgeon.
Comparing choledochotomy with HJS shows that complications within 30 days after surgery are more frequent in the HJS group. Long-term complications after more than 30 days postsurgery as well as recurrence rates of CBDS were similar throughout both study groups. In line with these results, the current literature describes complication rates between 3 and 41% for open choledochotomy, with a trend toward lower rates after primary closure compared to T-tube-insertion [33,34,35,36,37,38]. When consulting literature concerning the overall short-term complication rates for HJS, numbers between 9 and 29% are found. Mortality is described in up to 3% [24, 39]. To our knowledge, this study seems to be the first study in which the short- as well as the long-term complications of HJS compared to open choledochotomy specifically for CBDS are systematically investigated.
Regardless of the excellent stone clearance rates with modern endoscopy, several authors report a recurrence rate between 3 and 15% of CBDS after an initially successful endoscopic clearance [24, 40,41,42]. Xia et al. observed that the main reason for CBDS recurrences seems to be related to structural and functional abnormalities or damages of the duodenal papilla (sphincter Oddi). This can be caused by interventional incision of the duodenal papilla as it is performed in a sphincterotomy during ERCP [24]. Furthermore, repeated ERCP procedures have been shown to increase the complication rate during the intervention [39].
In their study, Abdelmajid et al. have defined main indicators for biliary enteric bypass: age > 65 years (90% of the cases), multiple stones (55%), and unremovable stones (16%) [23]. In our study population, main reasons for establishing a HJS were recurrent symptoms of obstructive bile duct disease, such as CBDS, choledochal stenosis/sclerosis, and complications occurring during treatment. Interestingly, based on the presented data and the literature, HJS seems to be a widely adoptable method for terminal bile duct disease or challenging anatomic sites even though it is a more invasive procedure [23, 43, 44]. Ultimately, it has to be noted that even though there are some indicators pointing toward the establishment of an HJS rather than to perform a choledochotomy, the final decision should be the surgeon’s preference.
HJS was technically successful in all of the cases in our cohort. Despite its technical success, it should be noted that open biliodigestive anastomoses inhibit any further efforts for minimal invasive treatment of CBDS and are therefore considered as a last option for CBDS, pre- or post-CCY [6]. Additionally, since the resection line of the bile duct should be as high as possible to decrease the risk for bile duct stricture, there are very limited options in case the HJS fails [45].
According to the literature, strictures are the most frequent long-term complications of HJS, resulting in bile duct obstruction potentially causing recurrent cholangitis [45,46,47,48,49,50,51]. Commonly, stricture rates range between 5 to 14%, are usually diagnosed around 17 to 18 months after surgery, and are mostly caused by scar-tissue contraction [49, 50]. Consequently, the higher the biliodigestive anastomosis is placed, the lower the possibility of stricture formation [45, 52, 53].
This study has several limitations. First of all, this is a retrospective study and data was not documented for research purpose, so potential confounders might be missing. Secondly, this is a single-center study; therefore, the outcome might be biased on the surgical team’s skill and experience of the procedure. Additionally, there are only few patients with choledochotomy or HJS for CBDS, and statistics are only descriptive. Lastly, the loss to follow-up was quite high, possibly due to the tertiary hospital with an outsourced aftercare. Fixed follow-up appointments or reports could have been helpful. Further research with a higher number of patients is needed to fully investigate the best use of either choledochotomy or HJS and their outcomes.
Conclusion
This study has demonstrated that when ERCP does not show sufficient results for the management of CBDS, choledochotomy and HJS can both be considered a safe and effective procedure with low morbidity and mortality. With shorter operation times, lower short-term complication rates, a sufficient long-term outcome considering the CBDS recurrence, and further surgical options, choledochotomy seems to be the method of choice for choledocholithiasis. However, HJS plays a role in cases with complications after CCY or ERCP and can be discussed as a method of first choice for recurrent bile stones due to its possible positive effect on the formation of recurrent CBDS.
Data availability
The data that support the findings of this study are available on request from the corresponding author, [SDS]. The data are not publicly available due to [ethical restrictions].
Abbreviations
- APACHE:
-
Acute physiology and chronic health evaluation
- CBDS:
-
Common bile duct stones
- CCI:
-
Charlson Comorbidity Index
- CD:
-
Clavien-Dindo
- CCY:
-
Cholecystectomy
- CI:
-
Confidence interval
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- HJS:
-
Hepaticojejunostomy
- SD:
-
Standard deviation
References
Younis M, Pencovich N, El-On R et al (2022) Surgical treatment for choledocholithiasis following repeated failed endoscopic retrograde cholangiopancreatography. J Gastrointest Surg 26:1233–1240
Navaratne L, Martínez Cecilia D, Martínez Isla A (2020) The ABCdE score for PREdicting Lithotripsy Assistance during transcystic Bile duct Exploration by Laparoendoscopy (PRE-LABEL). Surg Endosc. https://doi.org/10.1007/s00464-020-08082-6
Wills VL, Gibson K, Karihaloot C, Jorgensen JO (2002) Complications of biliary T-tubes after choledochotomy. ANZ J Surg 72:177–180
Williams E, Beckingham I, El Sayed G et al (2017) Updated guideline on the management of common bile duct stones (CBDS). Gut 66:765–782
Santambrogio R, Bianchi P, Opocher E et al (1999) Prevalence and laparoscopic ultrasound patterns of choledocholithiasis and biliary sludge during cholecystectomy. Surg Laparosc Endosc Percutan Tech 9:129–134
Ko CW, Lee SP (2002) Epidemiology and natural history of common bile duct stones and prediction of disease. Gastrointest Endosc 56:S165–S169
Petelin JB (2003) Laparoscopic common bile duct exploration. Surg Endosc 17:1705–1715
Acosta JM, Ledesma CL (1974) Gallstone migration as a cause of acute pancreatitis. N Engl J Med 290:484–487
Costi R, Gnocchi A, Di Mario F, Sarli L (2014) Diagnosis and management of choledocholithiasis in the golden age of imaging, endoscopy and laparoscopy. World J Gastroenterol 20:13382–13401
Shapoval’iants SG, Myl’nikov AG, Pan’kov AG et al (2012) Recurrent choledocholithiasis. Diagnosis, prevention and treatment. Eksp Klin Gastroenterol 4:32–38
Oh CH, Dong SH (2015) Recent advances in the management of recurrent bile duct stones. Korean J Gastroenterol= Taehan Sohwagi Hakhoe chi 66:251–254
NIH consensus conference (1993) Gallstones and laparoscopic cholecystectomy. Surg Endosc 7:271–279
De Palma GD (2013) Minimally invasive treatment of cholecysto-choledocal lithiasis: The point of view of the surgical endoscopist. World J Gastrointest Surg 5:161–166
Neoptolemos JP, Carr-Locke DL, Fossard DP (1987) Prospective randomised study of preoperative endoscopic sphincterotomy versus surgery alone for common bile duct stones. Br Med J 294:470–474
Carr-Locke DL (2002) Therapeutic role of ERCP in the management of suspected common bile duct stones. Gastrointest Endosc 56:S170–S174
Cremer A, Arvanitakis M (2016) Diagnosis and management of bile stone disease and its complications. Minerva Gastroenterol Dietol 62:103–129
Schulz C, Schirra J, Mayerle J (2020) Indications for endoscopic retrograde cholangiopancreatography and cholecystectomy in biliary pancreatitis. Br J Surg 107:11–13
Clayton ESJ, Connor S, Alexakis N, Leandros E (2006) Meta-analysis of endoscopy and surgery versus surgery alone for common bile duct stones with the gallbladder in situ. Br J Surg 93:1185–1191
Sharp CF, Garza RZ, Mangram AJ, Dunn EL (2009) Partial cholecystectomy in the setting of severe inflammation is an acceptable consideration with few long-term sequelae. Am Surg 75:249–252
Elshaer M, Gravante G, Thomas K et al (2015) Subtotal cholecystectomy for “difficult gallbladders”: systematic review and meta-analysis. JAMA Surg 150:159–168
Karaliotas C, Sgourakis G, Goumas C et al (2008) Laparoscopic common bile duct exploration after failed endoscopic stone extraction. Surg Endosc 22:1826–1831
Singh AN, Kilambi R (2018) Single-stage laparoscopic common bile duct exploration and cholecystectomy versus two-stage endoscopic stone extraction followed by laparoscopic cholecystectomy for patients with gallbladder stones with common bile duct stones: systematic review and meta-analysis of randomized trials with trial sequential analysis. Surg Endosc 32:3763–3776
Dasari BVM, Tan CJ, Gurusamy KS et al (2013) Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev 2013(9):CD003327
Demling L, Koch H, Classen M et al (1974) Endoscopic papillotomy and removal of gall-stones: animal experiments and first clinical results (author’s transl). Dtsch Med Wochenschr 99:2255–2257
Chan DSY, Jain PA, Khalifa A et al (2014) Laparoscopic common bile duct exploration. Br J Surg 101:1448–1452
Abdelmajid K, Houssem H, Rafik G et al (2013) Open choldecho-enterostomy for common bile duct stones: is it out of date in laparo-endoscopic era? N Am J Med Sci 5:288–292
Xia H, Xin X, Yang T et al (2020) Surgical strategy for recurrent common bile duct stones: a 10-year experience of a single center. Updates Surg. https://doi.org/10.1007/s13304-020-00882-8
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Mayhew D, Mendonca V, Murthy BVS (2019) A review of ASA physical status - historical perspectives and modern developments. Anaesthesia 74:373–379
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Dindo D, Clavien P-A (2008) What is a surgical complication? World. J Surg 32:939–941
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
von Elm E, Altman DG, Egger M et al (2014) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg 12:1495–1499
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
ElGeidie AA, ElEbidy GK, Naeem YM (2011) Preoperative versus intraoperative endoscopic sphincterotomy for management of common bile duct stones. Surg Endosc 25:1230–1237
Yildirim M, Dasiran F, Ozsoy U et al (2020) The efficiency of laparoscopic common bile duct exploration in endoscopic retrograde-cholangiopancreatography-limited setting in a peripheral university hospital. J Laparoendosc Adv Surg Tech A. https://doi.org/10.1089/lap.2020.0525
Zhou X-D, Chen Q-F, Zhang Y-Y et al (2019) Outcomes of endoscopic sphincterotomy vs open choledochotomy for common bile duct stones. World J Gastroenterol 25:485–497
Nassar AHM, Ng HJ, Katbeh T, Cannings E (2020) Conventional surgical management of bile duct stones: a service model and outcomes of 1318 laparoscopic explorations. Ann Surg Publish Ahead of Print: https://doi.org/10.1097/SLA.0000000000004680
Prat F, Malak NA, Pelletier G et al (1996) Biliary symptoms and complications more than 8 years after endoscopic sphincterotomy for choledocholithiasis. Gastroenterology 110:894–899
Pereira-Lima JC, Jakobs R, Winter UH et al (1998) Long-term results (7 to 10 years) of endoscopic papillotomy for choledocholithiasis. Multivariate analysis of prognostic factors for the recurrence of biliary symptoms. Gastrointest Endosc 48:457–464
Kawaji Y, Isayama H, Nakai Y et al (2019) Multiple recurrences after endoscopic removal of common bile duct stones: a retrospective analysis of 976 cases. J Gastroenterol Hepatol 34:1460–1466
Zhu J, Zhang Y, Gong J et al (2020) Closure of choledochotomy with a barbed absorbable suture after laparoscopic common bile duct exploration. Am Surg. https://doi.org/10.1177/0003134820982861
Zhou B, Hu J, Zhong Y (2017) Surgical treatments for patients with recurrent bile duct stones and Oddis sphincter laxity. Intractable Rare Dis Res 6:172–176
Tsutsumi K, Kato H, Yabe S et al (2017) A comparative evaluation of treatment methods for bile duct stones after hepaticojejunostomy between percutaneous transhepatic cholangioscopy and peroral, short double-balloon enteroscopy. Therap Adv Gastroenterol 10(1):54–67
Böhm SA, Beckurts KTE, Landwehr P, Hölscher AH (1999) Anisoperistaltische Roux-Schlinge: Seltene Ursache rezidivierender Cholangitiden nach Hepaticojejunostomie. Chirurg 70:803–806
Tocchi A, Costa G, Lepre L et al (1996) The long-term outcome of hepaticojejunostomy in the treatment of benign bile duct strictures. Ann Surg 224:162–167
Parra-Membrives P, Martínez-Baena D, Sánchez-Sánchez F (2016) Late Biliary Complications after Pancreaticoduodenectomy. Am Surg 82:456–461
Dimou FM, Adhikari D, Mehta HB et al (2016) Incidence of hepaticojejunostomy stricture after hepaticojejunostomy. Surgery 160:691–698
Matthews JB, Baer HU, Schweizer WP et al (1993) Recurrent cholangitis with and without anastomotic stricture after biliary-enteric bypass. Arch Surg 128:269–272
Okabayashi T, Shima Y, Sumiyoshi T et al (2018) Incidence and risk factors of cholangitis after hepaticojejunostomy. J Gastrointest Surg 22:676–683
Geng Z-M, Yao Y-M, Liu Q-G et al (2005) Mechanism of benign biliary stricture: a morphological and immunohistochemical study. World J Gastroenterol 11:293–295
Terblanche J, Allison HF, Northover JM (1983) An ischemic basis for biliary strictures. Surgery 94:52–57
Terblanche J, Worthley CS, Spence RA, Krige JE (1990) High or low hepaticojejunostomy for bile duct strictures? Surgery 108:828–834
Funding
Open access funding provided by University of Basel
Author information
Authors and Affiliations
Contributions
Gabriel Fridolin Hess, Philipp Sedlaczek, Otto Kollmar, and Savas Deniz Soysal contributed to the study conception and design. Material preparation and data collection were performed by Gabriel Fridolin Hess, Philipp Sedlaczek, and Jasmin Zeindler. Analysis and interpretation were performed by Gabriel Fridolin Hess, Philipp Sedlaczek, Simone Muenst, Silvio Däster, and Andreas Michael Schmitt. The first draft of the manuscript was written by Gabriel Fridolin Hess and Philipp Sedlaczek. Critical revision of the manuscript was done by Silvio Däster, Martin Bolli, Simone Muenst, Otto Kollmar, and Savas Deniz Soysal. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Swiss ethics commission, registration number: EKNZ 2020–00076.
Consent to participate
All included individual participants were consented.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Gabriel F. Hess and Philipp Sedlaczek contributed equally as first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hess, G.F., Sedlaczek, P., Zeindler, J. et al. The short- and long-term outcome after the surgical management of common bile duct stones in a tertiary referral hospital. Langenbecks Arch Surg 408, 288 (2023). https://doi.org/10.1007/s00423-023-03011-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-03011-2