Abstract
Currently available guidelines on the daily formula milk requirements of infants are based on the needs of infants with their growth pattern following the 50th percentile of the weight-for-age growth curve. Hence, current recommendations may not thoroughly detail the needs of infants across the broad spectrum of body weight percentiles. This study aimed to provide stratified recommendations for daily formula milk intake of fully formula-fed infants, across different weight-for-age categories from 0 to 4 months. At first, theoretical age- and gender-specific weight ranges were constructed for infants across five pre-defined weight-for-length percentile categories of the WHO growth standard. Thereafter, total daily energy requirements for each category were calculated and converted to daily formula milk needs. Subsequently, these stratified age- and weight-formula milk recommendations were compared to actual daily and relative formula milk of infants in these categories, retrieved from pooled individual infant formula milk intake data derived from 13 clinical intervention trials. A fitted regression model was used to evaluate differences in volume intakes across body weight categories as well as between theoretically derived and actual intake values. Median daily formula milk volume intake (ml/day) of infants differed significantly across the increasing weight-for-age categories at each time point, with significant differences between small and large infants. Interestingly, the relative daily formula milk volume intake (ml/kg/day) was higher for smaller infants compared to larger infants. The mean daily and relative formula milk intakes demonstrated the same pattern based on theoretical calculations as well as for the actual formula milk intake values retrieved from 13 pooled clinical intervention trials. Conclusions: Based on theoretical calculations and actual formula intake data, we conclude that larger infants require a significantly higher daily formula milk intake than smaller infants, and we postulate that infants could benefit from more tailored formula milk intake recommendations.
What is Known: |
• Adequate energy intake during the infancy period is crucial to support optimal growth and organ development, with the potential for long-lasting health effects. • Current available guidelines on the daily formula milk requirements of infants are based on the needs of infants with their growth pattern following the 50th percentile of the weight-for-age growth curve. |
What is New: |
• Based on using both theoretical calculations and actual formula intake data, larger infants require a significantly higher daily formula milk intake than smaller infants. • Exclusive formula-fed infants could benefit from more tailored formula milk intake recommendations, in early infancy. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The first 1000 days of life represent a critical period for establishing metabolic programming, corresponding with a rapid phase of growth and development in infancy. During this time, infants experience the fastest growth rate, reaching up to 30 g per day, and then slowing down to approximately 15 g per day by 3–6 months [1]. Therefore, ensuring adequate intake and nutritional quality during this period is crucial to support optimal growth and organ development, with the potential for long-lasting effects on later-life health outcomes [2].
Exclusive breastfeeding is the recommended source of nutrition for infants, providing all the necessary energy and nutrients during the first few months of life [3]. However, when breastfeeding is not feasible, infant formulas are considered the suitable alternative. Nonetheless, studies have shown different growth patterns between breastfed and formula-fed infants [4]. Formula-fed infants are more likely to experience higher weight gain in their first year of life, which has been associated with a higher overweight or obesity risk in childhood [4]. Rapid weight gain (RWG) during infancy has been linked to 3.6 times greater risk of becoming overweight or obese later in life [5]. The increased risk for RWG in formula-fed infant populations may be due to several different mechanisms [6,7,8,9,10]. These include the higher total energy and protein content in formula compared to breast milk and/or inaccurate formula milk dispensing resulting in higher energy intake from formula milk [11,12,13]. It is postulated that formula-fed infants show less variability in volume intake between feedings, larger total daily volume of feeding, and have reduced self-regulation of energy intake [14, 15] which ultimately affects their growth patterns in early life [16]. Overfeeding during this early period of life could also lead to hyperinsulinemia and impaired insulin signaling, resulting in rapid weight gain and adipose hyperplasia and affecting a baby’s health throughout life [17].
Hence, introducing more precise daily formula milk volume recommendations that match the growth and nutritional requirements of formula-fed infants can be beneficial in avoiding excessive as well as suboptimal energy intakes.
Currently, available guidelines on the daily formula milk requirements of infants, including those from the Institute of Medicine (IOM) or Food and Agriculture Organization/World Health Organization/United Nations University (FAO/WHO/UNU), are based on the needs of infants with median body weight and the assumption that their growth patterns follow the 50th percentile of weight-for-age growth curve [18,19,20]. Therefore, current recommendations might not be sufficiently tailored to the needs of infants growing across the broader spectrum of body weight percentiles for each month.
We anticipate that more specific formula milk intake recommendations using stratification based on gender, age, and weight of infants could more adequately guide daily energy intake and eventually result in more optimal growth. This approach could be of particular interest for smaller or larger infants who are at higher risk for underweight or overweight development, respectively, during infancy.
This study aimed to define stratified recommendations on the required daily formula milk intake for exclusive formula-fed infants across different weight-for-age categories from 0 to 4 months. As a proof-of-concept, the validity of the stratified recommendations was evaluated using real-life intake data, based on pooled data analysis from 13 clinical intervention trials.
Methods
This study was conducted in a stepwise approach with three phases. In the first phase, daily energy and formula milk volume requirements were theoretically calculated for infants from five pre-defined percentiles weight for length percentiles according to the WHO 2006 growth standards as small (10th percentile), medium-small (15th and 25th percentiles), medium (50th percentile), medium-large (75th and 85th percentiles), and large (90th percentile) infants [18, 21]. As an example, Fig. 1 presents a calculation of the daily energy and formula milk volume requirements for girls at birth using the WHO weight-for-length growth chart, from different growth percentiles. In the second phase, actual daily formula intakes were retrieved anonymously from 13 intervention clinical trials done by Danone Nutricia Research, and stratified intake data was generated according to the different weight percentile categories [22,23,24,25,26,27,28,29,30,31,32,33,34,35]. As a final step, we compared our calculated formula milk intakes with real-life formula milk intakes. These three phases have been explained in detail in Supplementary A.
Statistical analysis
To assess potential differences in formula intake across weight classes, we fitted linear regression models with weight class as a predictor and formula milk intake (either total daily formula milk (ml/day) or relative formula milk volume (ml/kg/day) as response variable). The models were fitted separately for each age/sex combination, and both for theoretical and actual intake from the pooled dataset of clinical studies. The details regarding null hypotheses and sample size calculations are presented in Supplementary B.
All inferential statistics were performed using R version 4.3.3 for Windows. Power and sample size calculations were generated using the pwr.r.test function from the pwr package (version 1.3–0) for R. Figures were generated using Prism 9.0.
Results
First phase: Calculation of stratified formula milk volume intake recommendation
The median daily formula milk volume intake requirements (ml/day) for infants with smaller body weight categories were found to be significantly lower compared to those infants with larger body weight categories at each month (p < 0.0001). However, there was still a small overlap in the daily formula milk requirements of infants with different body weight categories (Fig. 2). Over time, the difference in required daily formula volume intake ranges between the groups increased due to larger differences in weight-for-age values across the 10th to 90th percentile. For example, the difference in required median formula milk intake between smaller and larger baby girls at birth was 211 ml/day compared to 305 ml/day at 4 months.
Median (min–max) daily formula milk volume requirements (ml/day) based on the Institute of Medicine (IOM) equation, for boys (A) and girls (B) with different weight-for-length percentile categories, from 0 to 4 months. *Significant differences comparing large and small categories, at all-time point p < 0.0001
Furthermore, smaller infants required significantly higher relative median formula milk (ml/kg/day) compared to larger infants (p < 0.0001), with small overlap for infants with different body weight categories (Fig. 3).
Median (min–max) relative formula milk volume requirements (ml/kg/day) based on the Institute of Medicine (IOM) equation, for boys (A) and girls (B) with different weight-for-length percentile categories, from 0 to 4 months. *Significant differences comparing large and small categories at all-time points, p < 0.0001
Second phase: Actual formula milk intake in pooled data from 13 clinical studies
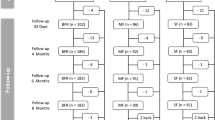
Our analysis was designed cross-sectionally and as such only included data of infants who were exclusively formula fed at each time point (irrespective of prior feeding history). It means, before enrolment and randomization, infants could have been breastfed exclusively or partially. Hence, given the high prevalence of breastfeeding immediately after birth, we have only limited available data points of formula-fed infants at birth (0–2 weeks of age). Infants had to be exclusively or at least predominantly formula fed at the time of allocation to one of the randomized formula intervention groups. In a substantial number of studies (8 out of 13), randomization of infants to the intervention formulas took place before 5 weeks of age. In the remaining studies, randomization occurred before 2 to 4 months of age (4 of 13 studies), and in one study, the start of infant formula intervention took place before 7 months of age. As a result, the total number of data points increased over time, with numbers at 1 month (2–6 weeks of age) of 1877, at 2 months (6–10 weeks of age) of 2044, at 3 months (10–14 weeks of age) of 2482, and at 4 months (14–18 weeks of age) of 2372. These higher data points reflect a greater proportion of available formula intake information of infants who were exclusive formula feeding during these periods (Supplementary Fig. 1).
Our analysis on the pooled data from clinical studies demonstrated that the daily and relative daily formula milk volume intake of smaller and larger infants differs significantly. Larger infants had higher daily formula milk intake but lower relative formula milk intake compared to smaller infants, between 1 and 4 months (p < 0.0001). No significant difference in formula intake outcomes was observed based on the limited available data points at birth (0–2 weeks) (p > 0.05) (Figs. 4 and 5 and Supplementary Figs. 3 and 4).
Median (min–max) of daily actual formula milk volume intake (ml/day), for boys (A) and girls (B) based on pool data from 13 clinical studies, with different weight-for-age percentile categories from 0 to 4 months. *Significant differences between large and small categories, at all-time points, except at birth, p < 0.0001. × No data presented for girl (orange bar) at birth, due to the limited numbers
Median (min–max) of relative actual formula milk volume intake (ml/kg/day) for boys (A) and girls (B), based on pool data from 13 clinical studies, with different weight-for-age percentile categories, 0–4 months. *Significant differences between large and small categories, at all-time points with p < 0.0001, except at birth. × No data presented for girl (orange bar) at birth, due to limited numbers
Supplementary Tables 2 and 3 present the calculated and actual formula milk intakes, from 0 to 4 months.
We also assessed comparability between the mean weight of the pooled clinical dataset and the WHO growth chart [4]. The details of this comparison are presented in Supplementary C.
Third phase: Comparison of theoretical and actual milk intake from pooled clinical studies
To assess the trend of theoretical calculation for daily formula milk intake for infants of different body sizes, we compared them with the actual daily formula milk volume intake (ml/day) and relative intake (ml/kg/day) from our pooled dataset based on 13 clinical studies (Figs. 6 and 7 and Supplementary Figs. 3 and 4).
Qualitative comparisons of the median (Q1–Q3) for theoretical calculations and actual daily formula milk intakes (ml/day), across weight-for-age categories, boys (A) and girls (B) from 0 to 4 months. Significant differences between the trends of calculated and actual formula milk intake (ml/day) from pooled dataset only at specific time points, *p < 0.05, **p < 0.0001. × Due to the limited numbers, no data was presented for girl (orange bar) at birth
Qualitative comparisons of the median (Q1–Q3) for theoretical calculations and relative formula milk intakes (ml/kg/day), across weight-for-age categories, boys (A) and girls (B) from 0 to 4 months. Significant differences between the trends of calculated and actual formula milk intake (ml/day) from pooled dataset at specific time points, *p < 0.05, **p < 0.0001. × Not presented at birth due to the limited numbers
A fitted regression model was conducted to compare theoretical and actual formula milk intake within the Q1–Q3 interquartile range. The results clearly showed that the slopes exhibit the same trend between actual and theoretical intakes with milk volume intake of infants increasing across weight categories at each time point, for boys and girls. However, at specific time points, the slope of the actual daily formula intake data is significantly steeper for boys (at 1–3 months) or shallower for girls (at 4 months (p < 0.001)) compared to theoretical calculated required daily formula intake data (Supplementary Figs. 3 and 4).
Discussion
This study, for the first time, provides theoretical calculations for daily formula intake and compared them with actual intakes based on pooled data from 13 clinical studies, across a wider range of weight percentiles.
We showed that larger infants on average tend to consume significantly more formula milk than smaller infants based on the pooled formula intake data from 13 clinical studies. This observation was in line with theoretical calculations across the five pre-defined stratified infant weight categories. In addition, the slopes of mean formula intakes across weight categories based on actual and theoretical calculations were generally in the same direction, although it was significantly steeper for boys and shallower for girls at specific time points (based on actual intake). We confirmed that the required formula volume intakes between smaller and larger infants are substantially different from infants growing at the 50th percentiles and considering both sex and weight categories is essential.
The formula milk intakes for infants are typically based on the standard recommended quantities indicated on formula packaging. These recommendations are tailored to meet the needs of infants with average body weight. The current formula recommendations may not be optimal and tailored to the needs of infants growing across the broad spectrum of body weight percentiles [19, 35]. For instance, we calculated the energy requirements for 3-month-old infants in five pre-defined weight categories using IOM equations. The results showed that the minimum energy needs of infants growing at the 10th percentile is 480 kcal/day, while the maximum energy needs of infants at the 90th percentile is 720 kcal/day. However, the recommended energy requirements for 3-month-old infants with average weight according to the WHO and EFSA are 583 and 479 kcal/day, respectively [19, 35]. Therefore, adjusting the intake recommendations based on the infant’s weight percentile may lead to more accurate and personalized feeding recommendations, and it could overcome the current limitations of “population average” energy and formula milk recommendations for formula-fed infants.
Adequate nutrition tailored to infants’ needs throughout infancy supports infants in achieving an appropriate growth trajectory and can help prevent adverse health effects later in life [5]. As such, both high or low formula milk intake during the first 4 months of life could be important factors contributing to the imbalanced infancy weight gain and subsequent higher body weight or underweight during childhood [2, 10, 19]. For example, Ong et al. found that formula milk providing 640 kcal/day at 4 months led to increased rapid weight gain until age 2 [10]. Therefore, more precise and personalized formula milk recommendations can serve as a strategy to help parents avoid underfeeding or overfeeding their infants.
Inevitably, infant biology and individual developmental needs play crucial roles in regulating milk consumption during early life. While breastfed infants often self-regulate their intake based on biological cues and individual developmental needs, among exclusive formula-fed infants, the total formula milk intake is more a complex interplay between infant biology, infant development plus parental behavior, and formula milk dispensing. Fildes et al. found that mothers tend to encourage lighter infants with smaller appetites to drink more, while restricting infants with larger appetites if they are bottle-fed [36]. Other studies have also shown that formula milk dispensing and parental feeding behavior significantly impact infants’ daily energy and nutrient intakes [35,36,37,38,39,40]. Ferguson et al. investigated the effects of following different formula-feeding guidelines advised by hospitals on infant weight gain. Using a “Virtual Infant” model, they found that caregivers following the first set of formula-feeding guidelines (with recommended a higher minimum daily amount of formula milk) might lead to overweight or obese infants. However, when caregivers followed the second set of guidelines, which allowed more flexibility in adjusting formula amounts, infants were able to maintain a healthier weight [37].
The early responsive parenting (RP) intervention study, which focused on feeding, infant soothing, and sleeping, also found that the RP group had 6% fewer overweight infants (weight for length ≥ 95th percentile) compared to the control group during the first year of life [38]. On the other hand, the mathematical model estimated that formula-fed infants with an 11% higher daily energy intake would reach the 75th percentile of weight-for-age at 6 months, starting from the 50th percentile at birth, with a higher level of adiposity [39]. Taken together, formula-fed infants could benefit from more accurate instructions for dispensing formula milk.
Stratified formula milk recommendations could also offer a valuable approach for future implementation through digital tools or as detailed guidelines on formula milk packaging to address the limitations of the existing guidelines. From a practical standpoint, it may be challenging for parents or caregivers to determine the actual weight of infants particularly for small-scale weight categories to classify them into the respective weight category and receive the recommended volume of formula milk. However, anticipating the rapid growth of digital applications for tracking nutrition and health, future innovative tools will likely simplify weight reporting for infants. Consequently, this advancement will provide the opportunity to implement more precise formula milk recommendations tailored to smaller, medium, and larger infants, rather than relying solely on generic recommendations based on medium-sized infants.
We should acknowledge that our study had certain limitations. The comparison between the theoretical and actual formula milk intakes was implemented only for 0–4 months of life due to the lower available data for the formula milk intakes after the 4 months from 13 clinical studies. In addition, we had a low number of exclusive formula-fed infants at birth (0–2 weeks) from clinical studies. The low number could potentially be caused due to the fact that women were still breastfeeding in the first days or weeks after birth. However, a second and probably main driver of this low number is that most of the intervention studies allowed the infants to be enrolled beyond 14 days of age, even up to 28, 35, or even 56 days of age, resulting in a lack of available data. Another related limitation was that our current recommendation is only for infants growing between the 10th and 90th percentiles. However, we acknowledge that there can be situations, such as very small or very large infants, or cases of faltering growth or catch-up growth that require tailored energy and dietary intakes from a pediatrician as well. Finally, the data in the current study were analyzed cross-sectionally. Considering the importance of monitoring longitudinal growth patterns in early life and their impact on limiting excessive weight gain during infancy and early childhood, collecting data on actual formula milk intake and growth outcomes for the same infant population over time could provide comprehensive insights.
Conclusion
Our study revealed that based on both theoretical calculation and actual pooled clinical studies, the estimated required formula milk intakes between smaller and larger infants growing between the 10th and 90th percentile of weight for age growth charts are substantially different. Therefore, given the critical nature of nutrition in early life, formula-fed infants, especially those who are not growing on the 50th percentiles, could benefit from introducing more precise and detailed daily formula milk recommendations that increase the accuracy of formula milk dispensing and daily caloric density from bottles. This could optimally meet the personalized growth and nutritional requirements of infants and avoid excessive (or suboptimal) energy intakes.
Data availability
No datasets were generated or analysed during the current study.
Abbreviations
- EFSA:
-
European Food Safety Authority
- FAO/WHO/UNU:
-
Food and Agriculture Organization/World Health Organization/United Nations University
- IOM:
-
Institute of Medicine
- RP:
-
Responsive parenting
- TEE:
-
Total energy expenditure
- RWG:
-
Rapid weight gain
References
Patel JK, Rouster AS (2022) Infant nutrition requirements and options. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing Copyright © 2022, StatPearls Publishing LLC. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560758/
Gluckman PD, Hanson MA, Cooper C, Thornburg KL (2008) Effect of in utero and early-life conditions on adult health and disease. N Engl J Med 359(1):61–73
Akre J (1994) WHO report on infant and young child nutrition: global problems and promising developments. Soz Praventivmed 39(6):397–398
Agostoni C, Grandi F, Giannì ML, Silano M, Torcoletti M, Giovannini M et al (1999) Growth patterns of breast fed and formula fed infants in the first 12 months of life: an Italian study. Arch Dis Child 81(5):395–399
Zheng M, Lamb KE, Grimes C, Laws R, Bolton K, Ong KK et al (2018) Rapid weight gain during infancy and subsequent adiposity: a systematic review and meta-analysis of evidence. Obes Rev 19(3):321–332
Andres A, Casey PH, Cleves MA, Badger TM (2013) Body fat and bone mineral content of infants fed breast milk, cow’s milk formula, or soy formula during the first year of life. J Pediatr 163(1):49–54
Bell KA, Wagner CL, Feldman HA, Shypailo RJ, Belfort MB (2017) Associations of infant feeding with trajectories of body composition and growth. Am J Clin Nutr 106(2):491
Sobik S, Sims CR, McCorkle G, Bellando J, Sorensen ST, Badger TM et al (2021) Early infant feeding effect on growth and body composition during the first 6 years and neurodevelopment at age 72 months. Pediatr Res 90(1):140–147
Heinig MJ, Nommsen LA, Peerson JM, Lonnerdal B, Dewey KG (1993) Energy and protein intakes of breast-fed and formula-fed infants during the first year of life and their association with growth velocity: the DARLING Study. Am J Clin Nutr 58(2):152–161
Ong KK, Emmett PM, Noble S, Ness A, Dunger DB (2006) Dietary energy intake at the age of 4 months predicts postnatal weight gain and childhood body mass index. Pediatrics 117(3):e503–e508
Hester SN, Hustead DS, Mackey AD, Singhal A, Marriage BJ (2012) Is the macronutrient intake of formula-fed infants greater than breast-fed infants in early infancy? J Nutr Metab 2012:891201
Huang J, Zhang Z, Wu Y, Wang Y, Wang J, Zhou L et al (2018) Early feeding of larger volumes of formula milk is associated with greater body weight or overweight in later infancy. Nutr J 17(1):12
Gilmore LA, Altazan AD, Flanagan EW, Beyer AG, Olson KN, O’Connell AA et al (2020) Modifications to infant formula instructions improve the accuracy of formula dispensing. Nutrients 12:4
Li R, Fein SB, Grummer-Strawn LM (2010) Do infants fed from bottles lack self-regulation of milk intake compared with directly breastfed infants? Pediatrics 125(6):e1386–e1393
Sievers E, Oldigs HD, Santer R, Schaub J (2002) Feeding patterns in breast-fed and formula-fed infants. Ann Nutr Metab 46(6):243–248
Niklas T (2014) Effects of feeding term infants low energy low protein formula supplemented with bovine milk fat globule membranes. Umeå University, Sweden
Diéguez E, Nieto-Ruiz A, Sepúlveda-Valbuena N, Herrmann F, Agil A, De-Castellar R et al (2023) Long-term effects and potential impact of early nutrition with breast milk or infant formula on glucose homeostasis control in healthy children at 6 years old: a follow-up from the COGNIS study. Nutrients 15:4
Butte NF (1996) Energy requirements of infants. Eur J Clin Nutr 50(Suppl 1):S24-36
FAO/WHO/UNU (1985) Energy and protein requirements. Report of a joint FAO/WHO/UNU expert consultation. World Health Organ Tech Rep Ser 724:1–206
Trumbo P, Schlicker S, Yates AA, Poos M (2002) Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein and amino acids. J Am Diet Assoc 102(11):1621–1630
World Health Organization (2020)Weight-for-length. https://www.who.int/tools/child-growth-standards/standards/weight-for-length-height
Abrahamse-Berkeveld M, Alles M, Franke-Beckmann E, Helm K, Knecht R, Köllges R, Sandner B, Knol J, Ben Amor K, Bufe A (2016) Infant formula containing galacto-and fructo-oligosaccharides and Bifidobacterium breve M-16V supports adequate growth and tolerance in healthy infants in a randomised, controlled, double-blind, prospective, multicentre study. J Nutr Sci 5:e42
Boyle RJ, Tang ML, Chiang WC, Chua MC, Ismail I, Nauta A, Hourihane JOB, Smith P, Gold M, Ziegler JJ, Peake J, Quinn P, Rao R, Brown N, Rijnierse A, Garssen J, Warner JO (2016) Prebiotic-supplemented partially hydrolysed cow’s milk formula for the prevention of eczema in high-risk infants: a randomized controlled trial. Allergy 71:701–710
Breij LM, Abrahamse-Berkeveld M, Vandenplas Y, Jespers SNJ, de Mol AC, Khoo PC, Kalenga M, Peeters S, van Beek RHT, Norbruis OF, Schoen S, Acton D, Hokken-Koelega ACS (2019) An infant formula with large, milk phospholipid-coated lipid droplets containing a mixture of dairy and vegetable lipids supports adequate growth and is well tolerated in healthy, term infants. Am J Clin Nutr 109:586–596
Huet F, Abrahamse-Berkeveld M, Tims S, Simeoni U, Beley G, Savagner C, Vandenplas Y, Hourihane JO (2016) Partly fermented infant formulae with specific oligosaccharides support adequate infant growth and are well-tolerated. J Pediatr Gastroenterol Nutr 63:e43-53
Lay C, Chu CW, Purbojati RW, Acerbi E, Drautz-Moses DI, de Sessions PF, Jie S, Ho E, Kok YJ, Bi X, Chen S, Mak SY, Chua MC, Goh AEN, Chiang WC, Rao R, Chaithongwongwatthana S, Khemapech N, Chongsrisawat V, Martin R, Roeselers G, Ho YS, Hibberd ML, Schuster SC, Knol J (2021) A synbiotic intervention modulates meta-omics signatures of gut redox potential and acidity in elective caesarean born infants. BMC Microbiol 21:191
Moro G, Arslanoglu S, Stahl B, Jelinek J, Wahn U, Boehm G (2006) A mixture of prebiotic oligosaccharides reduces the incidence of atopic dermatitis during the first six months of age. Arch Dis Child 91:814–819
Phavichitr N, Wang S, Chomto S, Tantibhaedhyangkul R, Kakourou A, Intarakhao S, Jongpiputvanich S, Roeselers G, Knol J (2021) Impact of synbiotics on gut microbiota during early life: a randomized, double-blind study. Sci Rep 11:3534
Piemontese P, Giannì ML, Braegger CP, Chirico G, Grüber C, Riedler J, Arslanoglu S, van Stuijvenberg M, Boehm G, Jelinek J, Roggero P (2011) Tolerance and safety evaluation in a large cohort of healthy infants fed an innovative prebiotic formula: a randomized controlled trial. PLoS ONE 6:e28010
Rigo J, Schoen S, Verghote M, van Overmeire B, Marion W, Abrahamse-Berkeveld M, Alliet P (2019) Partially hydrolysed whey-based formulae with reduced protein content support adequate infant growth and are well tolerated: results of a randomised controlled trial in healthy term infants. Nutrients 11(7):1654. https://doi.org/10.3390/nu11071654
Rodriguez-Herrera A, Tims S, Polman J, Porcel Rubio R, Muñoz Hoyos A, Agosti M, Lista G, Corvaglia LT, Knol J, Roeselers G, Pérez Navero JL (2022) Early-life fecal microbiome and metabolome dynamics in response to an intervention with infant formula containing specific prebiotics and postbiotics. Am J Physiol Gastrointest Liver Physiol 322:G571–G582
Shek LP, Chong YS, Winokan A, Abrahamse-Berkeveld M, Van Der Beek EM, Teoh OH, and Group On Behalf Of The Venus Working (2021) Evaluation of an infant formula with large, milk-phospholipid coated lipid droplets on long-term growth and development of Singaporean infants: randomized controlled trial protocol. Nutrients 13:8
Teoh OH, Lin TP, Abrahamse-Berkeveld M, Winokan A, Chong YS, Yap F, Marintcheva-Petrova M, van der Beek EM, Shek LP (2022) An infant formula with large, milk phospholipid-coated lipid droplets supports adequate growth and is well-tolerated in healthy, term asian infants: a randomized, controlled double-blind clinical trial. Nutrients 14:3. https://doi.org/10.3390/nu14030634
van der Aa LB, Heymans HS, van Aalderen WM, Sillevis Smitt JH, Knol J, Ben Amor K, Goossens DA, Sprikkelman AB (2010) Effect of a new synbiotic mixture on atopic dermatitis in infants: a randomized-controlled trial. Clin Exp Allergy 40:795–804
EFSA. EFSA Panel on Dietetic Products, Nutrition and Allergies (NDA). Scientific opinion on dietary reference values for energy. EFSA Journal. 2013;European Food Safety Authority (EFSA), Parma, Italy.
Fildes A, van Jaarsveld CH, Llewellyn C, Wardle J, Fisher A (2015) Parental control over feeding in infancy. Influence of infant weight, appetite and feeding method. Appetite 91:101–6. https://doi.org/10.1016/j.appet.2015.04.004
Ferguson MC, O’Shea KJ, Hammer LD, Hertenstein DL, Syed RM, Nyathi S et al (2020) Can following formula-feeding recommendations still result in infants who are overweight or have obesity? Pediatr Res 88(4):661–667
Savage JS, Birch LL, Marini M, Anzman-Frasca S, Paul IM (2016) Effect of the INSIGHT responsive parenting intervention on rapid infant weight gain and overweight status at age 1 year: a randomized clinical trial. JAMA Pediatr 170(8):742–749
Altazan AD, Gilmore LA, Guo J, Rosenberg DM, Toupo D, Gowins A et al (2019) Unintentional error in formula preparation and its simulated impact on infant weight and adiposity. Pediatr Obes 14(12):e12564
Mennella JA, Smethers AD, Delahanty MT, Stallings VA, Trabulsi JC (2023) Glutamic acid intake by formula-fed infants: are acceptable daily intakes appropriate? Eur J Pediatr 182(12):5701–5705. https://doi.org/10.1007/s00431-023-05215-6
Acknowledgements
The authors acknowledge the significant contributions of Helene Thygesen for her application of statistical analyses and Femke Sijtsma for her work in extracting data from the pooled dataset of clinical studies.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data analysis were performed by S.S. and M.AB. All authors wrote, read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All studies were conducted in compliance with the principles of the Declaration of Helsinki and with the local laws and regulations of the countries where the studies were performed. All participating study centers in each of the study obtained approval from the relevant Ethical Review Board in each country and study sites.
Consent to participate
For all 13 studies, written informed consent was obtained from all parents/guardians before enrolment.
Competing interests
Shila Shafaeizadeh, Ardy van Helvoort, Martine Alles, Marieke Abrahamse-Berkeveld were employees of Danone Nutricia Research in the Netherlands at the time of writing the manuscript.
Additional information
Communicated by Gregorio Milani
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Shafaeizadeh, S., Henry, C.J., van Helvoort, A. et al. Tailored recommendations for infant milk formula intake results in more accurate feeding. Eur J Pediatr (2024). https://doi.org/10.1007/s00431-024-05726-w
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00431-024-05726-w