Abstract
Background
Surgeons may cause tissue damage by incorrect laparoscopic pinch force control. Unpredictable tissue and grasper properties may cause slips or ruptures. This study investigated how different forms of haptic feedback influence the surgeon’s ability to generate a safe laparoscopic grasp while pulling tissues of variable stiffness using graspers with different force transmission ratios. The results will help define design requirements for training facilities and instruments.
Methods
For this study, 10 participants lifted an object barehanded, with tweezers, or with one of two laparoscopic graspers until they where able to complete five consecutive safe lifts under different tissue stiffness conditions. The participants were presented with indirect visual feedback of pinch force, object location, and target location.
Results
Lifting with instruments (tweezers or graspers) required 4.5 to 14.5 times as many practice trials as barehanded lifting, where no slips were recorded. Additionally, slips occurred more often with a decreasing force transmission ratio of the graspers and with increasing tissue stiffness. The maximal pinch force was higher in lifting with instruments than in barehanded lifting (26–60%) irrespective of the stiffness conditions. Using a grasper, the slip margin often was not high enough in the stiffest condition, resulting in slippage of up to 84%.
Conclusions
Without the direct tactile feedback that occurs with normal skin–tissue contact, subjects using graspers have trouble anticipating slippage when lifting tissue with variable stiffness. Performance drops with a decreased force transmision ratio of the instrument and increased tissue stiffness. Furthermore, the pinch forces are not adapted to the variable stiffness conditions. The same pinch force is applied irrespective of tissue stiffness. It takes participants longer to learn a safe laparoscopic grasp than to learn barehanded lifts. Additionally, to perform safe laparoscopic surgery, care should be taken when graspers with a low force transmission ratio are used.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
During laparoscopic tissue manipulation, surgeons have to grasp organs and tissues with variable properties, one of which is stiffness. Stiffness is important because it determines the magnitude of the force required by a surgeon for pulling and pinching to manipulate the tissue. Incorrect pinch force control causes tissue slippage, damage, or both [1].
Heijnsdijk et al. [2] found during a study of 10 laparoscopic colectomies and 15 cholecystectomies that the bowel and the gallbladder slipped out of the grasper during 7% and 17% of the grasp actions, respectively. Thus, it seems that even experienced surgeons have difficulty maintaining an accurate pinch force.
Accurate pinch force control relies to a great extent on haptic perception, which combines tactile perception (through tactile mechanoreceptors in the glabrous skin of our fingers) and kinesthetic perception (through muscle, tendons, and joint sensory receptors). If an unpredictable load force (unknown tissue stiffness) occurs during barehanded grasping, humans are able to adjust their pinch force to prevent slippage while avoiding exceedingly large forces [3–10].
During laparoscopic surgery, the surgeon’s hands are not directly in contact with the tissue but with the handle of the laparoscopic grasper. Therefore, next to visual cues, the only way to receive information about applied pinch forces is through the forces and positions transmitted to the grasper handle. The transmission of forces from the tip of the instrument to the handle is limited and significantly disturbed, depending on the type of grasper and the kind of manipulation action (e.g. trocar friction, abdominal wall resistance, scaling factors, mechanical construction, and efficiency) [1, 11–15].
It is unclear which factors contribute to the surgeon’s ability to adjust pinch force appropriately using a laparoscopic grasper if the load force is unpredictable. A safe grasp can be maintained if the internal mental reference model about the instrument and its interaction with the grasped object is correct. Mental models are used to estimate the input and output relations of systems and transform sensory signals into motor commands. Mental models have been generated for all motor actions and can be modified as new environments (e.g., new tools) are encountered [16]. The level of haptic feedback is thought to play a role in generating a correct mental reference model.
This study therefore aimed to investigate how different levels of haptic feedback influence a participant’s ability to generate a laparoscopic grasp with no excessive force and no slippage while pulling an object of unknown stiffness. To compare different levels of haptic feedback, the study tested grasp control using two commercially available laparoscopic graspers, anatomic tweezers, and bare hands.
Laparoscopic graspers have different frictional losses and different force multiplication factors. Inexperienced participants were used because they had no preconceived mental model for laparoscopic tissue handling. This research contributes to the knowledge of the effects that the limited and distorted force transmission of laparoscopic graspers have on grasp control and will help to define requirements for training facilities and instruments.
Methods
Participants
This study recruited 10 right-handed participants ages 21 to 41 years with no laparoscopic experience. The participants were not aware of the experiment’s purpose.
Task
The participants had to grasp an object either barehanded between the thumb and index finger (H), with tweezers (T), or with one of two laparoscopic graspers (GHFTR and GLFTR) and move the object to a predefined target location.
Experimental setup
A robotic device, Omega (Force Dimension, Lausanne, Switzerland), was used to generate computer-controlled load forces for the object to be grasped that simulated stretching of different tissue types. The object was randomly subjected to three different stiffness profiles: 80, 120, and 160 N/m. With human tissue, elasticity becomes noticeable only when the tissue is stretched, so the object was attached to a slack wire (Fig. 1) for better simulation of tissue grasping. Therefore, in moving the object, the wire first had to be made taut before the object was subjected to the various forces.
The object used was an aluminium wedge (17 × 30 mm with an angle of 15º) to generate pinch surfaces parallel to the jaws of the graspers and tweezers. The wedge was covered with a layer of rubber (0.5 mm) and attached with the wire to the end plate of the Omega (Figs. 1 and 2). To measure pinch forces, two thin (0.2 mm) FlexiForce force sensors (Tackscan, South Boston, MA, USA) were inserted into the pinch surfaces between the aluminium and the rubber. The sensors were covered with a thin steel plate (0.1 mm) to ensure an even distribution of the pinch force.
The participant could not see the object to generate similar visual feedback in all four test conditions. A curtain was used to prevent the participant from seeing the object in conditions H and T or the Pelvi-trainer in conditions GHFTR and GLFTR (Fig. 2). Visual feedback on both the object and the target locations was graphically presented to the participant on a monitor. A blue dot (diameter, 20 mm) represented the grasped object, and a red dot represented the target location.
The laparoscopic graspers were placed through a trocar (type Xcel 5; Ethicon ENDO-Surgery Inc., Cincinnati, OH, USA) with low friction to minimize the disturbance of forces caused by other elements [15]. Figure 1 shows the experimental setup for the condition of a laparoscopic grasper.
Instruments used
Two reusable laparoscopic graspers (types 33321 MH and 33321; C. Karl Storz, Tuttlingen, Germany) and a pair of anatomic tweezers were used. The force transmission ratios (combining frictional losses, force multiplication factors, and hysteresis) of each grasper were determined by measuring pinch force at the tip when handle forces were varied (with a fixed jaw opening of 15º).
Figure 3 shows that there were large differences in the force transmission ratios of the two laparoscopic graspers. To generate the same tip force, the grasper with a high force transmission ratio (GHFTR) required less effort from the participant than the grasper with a low force transmission ratio (GLFTR). The surface areas of the instrument tips were approximately the same for all the instruments (tweezers and laparoscopic graspers).
General procedure
The experimental setup was ergonomically adjusted individualy to the participants. The participant stood in front of the setup and grasped the object either barehanded using the thumb and index finger (H), with tweezers (T), or with one of the two laparoscopic graspers (GHFTR and GLFTR) and moved it to a predefined target location (Fig. 1). After the lift, the participant had to keep the object at the target location for 2 s before releasing it. To guarantee that the pinch surface was at the predefined starting position before the participant pinched and pulled, the experimenter placed the object in the participant’s instrument or hand each time the participant had to regrasp it.
For movement of the object in this experiment realistic, the target location was placed such that the object had to be moved over a distance of 50 mm along a travel path 60º relative to the horizontal plane, similar to reported pull directions for the colon [17]. To prevent the participants from automatically moving to the target location, the location was changed randomly during the trials (0 mm, 5 mm to the left, or 5 mm to the right relative to the sagittal plane). The different pull forces required for reaching the target location were 4, 6, and 8 N, respectively.
The participants were instructed to handle the object as if it were very delicate tissue. To prevent damage, the participants had to lift and pinch the tissue with the minimal force required to prevent slippage. To prevent the participant from adapting a strategy of applying as much force as possible to prevent slippage, a maximum pinch force level of 10 N was allowed. This was the level at which Heijnsdijk et al. [18] found perforation forces of 10.3 ± 2.9 N for a small human bowel. Visual feedback indicated whether the pinch force was approaching 10 N by changing the color of the dot representing the object gradually from blue to white with increasing force.
It was assumed that the participant had generated a correct mental model after performing five safe lifts in a row. A safe lift was defined as a lift performed without slippage or without exceeding 10 N of pinch force. The task had to be repeated until five consecutive safe lifts were performed. The grasps in the four different conditions were performed randomly with a resting period of 5 min between.
Performance assessment
For each of the four conditions, the number of safe and unsafe lifts performed by the participant before completing five consecutive safe lifts were counted and defined as the number of attempts. The number of slips also were noted. To determine whether the variable tissue stiffness influenced the number of slips, the percentage of slips within the attempts were calculated for each stiffness condition.
To estimate the pinch force used by the participant, the output of the two force sensors were averaged. The inaccuracy of the combined output from the two sensors was about 5%. To determine the maximal force levels used by the participants, the average peak pinch force during the five safe lifts was calculated.
Statistical analysis
A Friedman test was used to compare the number of required attempts and the percentage of slips during the trials among the different conditions. The influence of the variable tissue stiffness was tested as well. A two-way analysis of variance (ANOVA) was used to compare the mean maximal pinch force used during the five consecutive safe lifts and the influence of the variable tissue stiffness. Multi-comparison procedures using Tukey’s honestly significant difference criterion were preformed to determine which pairs of means were significantly different and which were not. Significance was set at a p value less than 0.05. If the data were not normally distributed, medians were used. Otherwise, the average and standard deviation were calculated for each condition.
Results
Influence of the instrument type
Compared with barehanded lifting (H) (median, 0 attempts), the participants required significantly more median attempts using one of the three instruments (T: 4.5 attempts, GHFTR: 10 attempts, GLFTR: 14.5 attempts) before performing five consecutive safe lifts (Friedman χ2 = 18.09, df = 3; p < 0.001). For condition GLFTR, the participant required significantly more attempts than for condition T (Fig. 4).
Total required attempts during the practice period. Data are presented as notched box and whisker plots, in which every box has a line at every quartile, median, and upper quartile value. The whiskers are presented as lines that extend from each end of the box to show the extent of the remaining data. The notches represent the 95% confidence interval for the median. The boxes whose notches do not overlap are significantly different (p < 0.05)
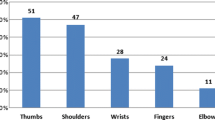
The participants experienced significantly more slips using one of the three instruments (T: 4.5%, GHFTR: 28%, GLFTR: 51% of the total median attempts required; Friedman χ2 = 20.7, df = 3; p < 0.001). than when lifting barehanded (H: 0%). For condition GLFTR, the participants had significantly more slips than for condition T (Fig. 5).
Percentage of slips during the practice period. Data are presented as notched box and whisker plots, in which every box has a line at every quartile, median, and upper quartile value. The whiskers are presented as lines that extend from each end of the box to show the extent of the remaining data. The notches represent the 95% confidence interval for the median. The boxes whose notches do not overlap are significantly different (p < 0.05)
Influence of the stiffness variable
The influence of the stiffness condition on the percentage of slips and on the average maximal pinch force applied to the object during the five safe lifts is presented in Table 1. The maximal forces did not differ significantly between the objects with different simulated stiffness conditions. The pinch forces used during conditions GHFTR and T were significantly higher than for condition H (F = 8.2; p < 0.001).
For conditions T and GHFTR, the percentage of slips during the pulls of the stiffest object differed significantly from that for the object with the lowest stiffness (p = 0.024 vs p = 0.018). The percentage of slips during the lifts of the object with a stiffness of 120 N/m did not differ from that of the other two. For condition GLFTR, the percentage of slips during the pulls of the object with stiffness conditions of 120 and 160 N/m differed significantly from that for the object with the lowest stiffness (p < 0.001).
Discussion
This research aimed to investigate how different forms of haptic feedback influence the surgeon’s ability to generate a safe laparoscopic grasp for an object of unpredictable stiffness. The type of instrument (bare hand, tweezers, or laparoscopic graspers with high and low transmission ratios) used to lift the object and the different stiffness profiles influenced slippage occurrence and the amount of force applied. The results show that the number of trials required to perform five consecutive safe lifts was higher with the use of instruments than with barehanded lifting. Furthermore, slips occurred more often when the force transmission ratio of the laparoscopic grasper was lower. No slippage occurred with barehanded lifting. When an instrument was used, more slips occurred as the stiffness of the object increased.
We defined slip margin as the difference between the exact slip force and the force used to prevent slip. The amount of force used to prevent slippage compared with the slip force was higher for lifting with the aid of instruments than for barehanded lifting (26–60%). This did not differ for the varied stiffness conditions. The fact that the slip margin was not adjusted to the variable object stiffness demonstrates that when an object is grasped with the aid of instruments (tweezers or laparoscopic graspers), load force is not taken into account. However much load is applied, the pinch force remains the same. The slip margin, therefore, often was not great enough in the stiffest condition, with the result that slippage occurred for up to 84% of the required attempts during condition GLFTR.
The results of condition H are consistent with results from studies in which objects were lifted barehanded and load forces were changed to induce pinch force modifications. The pinch force modifications were in phase with the changes in load force [19]. Slips rarely occurred as the pinch force exceeded the minimum force required to prevent slippage according to a slip margin determined by the skin object friction [20].
The literature shows that a lack of cutaneous sensation of applied pinch force generally results in a higher slip margin. However, the pinch force is reduced during a static hold period [21]. The cause of the slips in this study were partly due to this reduction in force during the static hold period. In general, a high slip margin can lead to the application of unacceptably high forces to the tissue during laparoscopic surgery or to unwanted slips resulting from the reduction in force during the static hold period.
This study suggests that as haptic perception is distorted by instruments (tweezers and laparoscopic graspers), it is more difficult to control a safe grasp. Haptic feedback can be divided into kinesthetic feedback and tactile feedback. All three instruments used in this study considerably disturb tactile feedback because no contact exists between tissue and the cutaneous sensors in the skin. Because the hands are in contact with the instrument handle, slippage must be detected by movements, forces, and vibrations distributed by the instrument handle as a result of object movement at the tip of the instrument. The cutaneous sensors in the skin can detect pressure and vibrations of the handle, and sensors in the muscles and joints can detect force and position changes. However, the results show that the participants could not react in a timely manner to this limited amount of haptic feedback and often could not prevent slippage using an instrument (tweezers or laparoscopic grasper).
Kinesthetic feedback distortion can be attributed to the following disturbance factors: trocar friction, abdominal wall resistance, scaling factors, mechanical construction, and efficiency [1]. Of the three instruments used in this experiment, tweezers caused the least kinesthetic distortion. However, the maximal pinch force, the number of attempts required, and the percentage of slips resulting from the use of tweezers were similar to those of the grasper with a high force transmission ratio. This shows that the effects of haptic distortion on performance using these two instruments are comparable.
In real surgery, however, the distortion in transmission of haptic information for laparoscopic graspers is greater than for tweezers. The reason for this is that tweezers are used in an open setting without disturbing factors such as abdominal wall thickness, which can vary enormously in laparoscopy. Compared with the other instruments, the grasper, due to a low force transmission ratio, provided less feedback on force. Therefore, it was even more difficult to control pinch forces with the grasper.
These results lead to the expectation that the slip margin would be higher in condition GLFTR than in conditions GHFTR and T. This, however, was not found because with condition GLFTR, it was almost impossible to exceed the 10 N of pinch force. To achieve a force of 10 N at the tip, extreme force (~133 N) on the handle is required (Fig. 3). As a result of these extreme forces on the handle, it is possible that minor changes in handle position (due to slippage) were not noticed. Additionally, pain sensation could be the cause for disregarding tactile information provided through the handle, due to the inhibition of cutaneous sensors. With condition GLFTR, the participants complained of sore hands due to high handle forces, even after a holding period of only 2 s.
Heijnsdijk et al. [22] evaluated the effects from differences in the force transmission ratios of laparoscopic forceps and concluded that the efficiency is dependent on the task being performed. Whereas a low force transmission ratio is sufficient for tasks requiring little movement of the forceps, such as grasping and holding tissue, a high force transmission ratio is required for tasks requiring repeated movement of the forceps.
In our experiment, the GLFTR grasper caused a significant amount of slippage when the participant had to make a lift, but the maximum pinch force applied was acceptable. In a time–action analysis study of real surgery, Heijnsdijk et al. [2] found that 89% of the time, the colon was clamped for less than 1 min. The maximum clamping time was 7 min for the colon and 55 min for the gallbladder (often with use of the instrument handle ratchet). This suggests that graspers with a low force transmission ratio are suitable for situations in which the tissue is very elastic because the tissue does not have to be moved or held for a lengthy period. The literature shows that these conditions are rare during surgery [2]. Therefore, to perform safe surgery, the use of these laparoscopic graspers should be avoided. Because wear can cause the force transmission ratio of laparoscopic graspers to decrease, extra care should be taken with the use of older nondisposable laparoscopic graspers.
In this study, we did not provide the participants with a direct view of the instrument tip while they were holding the object. During surgery, the surgeon can view on a monitor the instrument tip holding the tissue, and tissue deformation can help the surgeon determine the pinch force required. However, if the tip is not visible, the surgeon must rely on haptic information to control pinch forces. Inexperienced surgeons find it difficult to use visual cues. They have not been trained to use visual cues as an indication of pinch force because the endoscopic view differs from the view in an open setting.
These findings are of value for the designing of new graspers or the development of training facilities. This study demonstrates that the greater the amount of haptic feedback (as with tweezers and graspers, which have high force transmision ratios), the quicker the development of a mental model required for application of a safe grasp, which results in less practice time. To prevent slippage, improved feedback on the minimal force required also may help to reduce practice time.
Conclusion
When grasping tissue with a variable stiffness, participants need 10 to 14.5 times more trials to achieve a safe grasp with a laparoscopic grasper than with their bare hands. Without tactile feedback, which results from normal skin–tissue contact, participants have trouble anticipating slippage during lifts of tissue with variable stiffness. Furthermore, with the use of a laparoscopic grasper, the pinch forces applied are not adjusted to suit the variable stiffness conditions. For this reason, the same pinch force is applied irrespective of the tissue stiffness. Applying these results to the field of laparascopic surgery, our experiments demonstrate that to improve laparoscopic surgery safety, care should be taken when graspers are used with a low force transmission ratio.
References
Westebring-van der Putten EP, Goossens RHM, Jakimowicz JJ, Dankelman J (2008) Haptics in minimally invasive surgery: a review. Minim Invasive Ther Allied Technol 17:3–16
Heijnsdijk EA, Dankelman J, Gouma DJ (2002) Effectiveness of grasping and duration of clamping using laparoscopic graspers. Surg Endosc 16:1329–1331
Monzee J, Lamarre Y, Smith AM (2003) The effects of digital anesthesia on force control using a precision grip. J Neurophysiol 89:672–683
Winstein CJ, Abbs JH, Petashnick D (1991) Influences of object weight and instruction on grip force adjustments. Exp Brain Res 87:465–469
Cole KJ, Johansson RS (1993) Friction at the digit–object interface scales the sensorimotor transformation for grip responses to pulling loads. Exp Brain Res 95:523–532
Johansson RS, Riso R, Hager C, Backstrom L (1992) Somatosensory control of precision grip during unpredictable pulling loads: I. Changes in load force amplitude. Exp Brain Res 89:181–191
Turrell YN, Li FX, Wing AM (1999) Grip force dynamics in the approach to a collision. Exp Brain Res 128:86–91
Jenmalm P, Dahlstedt S, Johansson RS (2000) Visual and tactile information about object-curvature control fingertip forces and grasp kinematics in human dexterous manipulation. J Neurophysiol 84:2984–2997
Jenmalm P, Johansson RS (1997) Visual and somatosensory information about object shape control manipulative fingertip forces. J Neurosci 17:4486–4499
Johansson RS, Westling G (1987) Signals in tactile afferents from the fingers eliciting adaptive motor responses during precision grip. Exp Brain Res 66:141–154
Zhou M, Perreault J, Schwaitzberg SD, Cao CG (2008) Effects of experience on force perception threshold in minimally invasive surgery. Surg Endosc 22:510–515
Tendick F, Jennings RW, Tharp G, Stark L (1993) Sensing and manipulation problems in endoscopic surgery: experiment, analysis, and observation. Presence 2:66–81
Sjoerdsma W, Herder JL, Horward MJ, Jansen A, Bannenberg JJG, Grimbergen CA (1997) Force transmission of laparoscopic grasping instruments. Minim Invasive Ther Allied Technol 6:274–278
Picod G, Jambon AC, Vinatier D, Dubois P (2005) What can the operator actually feel when performing a laparoscopy? Surg Endosc 19:95–100
van den Dobbelsteen JJ, Schooleman A, Dankelman J (2007) Friction dynamics of trocars. Surg Endosc 21:1338–1343
Witney AG (2004) Internal models for bi-manual tasks. Hum Mov Sci 23:747–770
de Visser H, Heijnsdijk EA, Herder JL, Pistecky PV (2002) Forces and displacements in colon surgery. Surg Endosc 16:1426–1430
Heijnsdijk EA, van der Voort M, de Visser H, Dankelman J, Gouma DJ (2003) Inter- and intraindividual variabilities of perforation forces of human and pig bowel tissue. Surg Endosc 17:1923–1926
Flanagan JR, Tresilian JR (1994) Grip-load force coupling: a general control strategy for transporting objects. J Exp Psychol Hum Percept Perform 20:944–957
Johansson RS, Westling G (1984) Roles of glabrous skin receptors and sensorimotor memory in automatic control of precision grip when lifting rougher or more slippery objects. Exp Brain Res 56:550–564
Augurelle AS, Smith AM, Lejeune T, Thonnard JL (2003) Importance of cutaneous feedback in maintaining a secure grip during manipulation of handheld objects. J Neurophysiol 89:665–671
Heijnsdijk EA, Pasdeloup A, Dankelman J, Gouma DJ (2004) The optimal mechanical efficiency of laparoscopic forceps. Surg Endosc 18:1766–1770
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Westebring-van der Putten, E.P., van den Dobbelsteen, J.J., Goossens, R.H.M. et al. Effect of laparoscopic grasper force transmission ratio on grasp control. Surg Endosc 23, 818–824 (2009). https://doi.org/10.1007/s00464-008-0107-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-008-0107-6








