Abstract
Purpose
Oral symptoms are common in patients with advanced cancer. The aim of this scoping review was to identify oral symptom assessment tools that have been specifically utilised in patients with “advanced cancer”.
Methods
The review was conducted/reported according to international guidelines for undertaking scoping reviews. PubMed, Embase, and CINAHL were searched for articles involving adult patients with advanced cancer, which involved assessment of ≥ 2 oral symptoms, and which involved patients with > 1 type of cancer.
Results
The review identified four validated symptom assessment scales, including one cancer-specific quality of life scale (EORTC QLQ OH-15), one generic tool for assessing the “social impact” of specific oral problems (OHIP), one cancer-specific generic symptom assessment scale (MSAS), and one cancer-specific oral symptom assessment scale (OSAS).
Conclusion
Symptom assessment tools can facilitate good symptom control in clinical practice, and are an integral component of clinical research. The review identified four validated symptom assessment scales that could be utilised to assess oral symptoms in patients with advanced cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
One of the main aspects of palliative care is the management of “pain and other distressing symptoms” [1]. Patients with advanced cancer experience a range of different symptoms, including a variety of different oral symptoms [2]. Thus, Davies et al. [3] reported that 97.5% of participants in their multicentre study experienced at least one oral symptom, and that the median number of oral symptoms experienced was five (range 1–18). Moreover, many of these oral symptoms had a high frequency and a high intensity, and were associated with significant distress/ “bothersomeness” (and negative impact on quality of life). For example, 79.6% of participants experienced xerostomia/dry mouth, and this was the third most common symptom overall (after “lack of energy” and “feeling drowsy”) [3].
Investigators have identified discrepancies between the recorded prevalence of oral symptoms and the true (higher) prevalence of these symptoms in patients with advanced cancer [4]. The reasons for the latter are unclear. Healthcare professionals may not enquire about a symptom if (a) they perceive the symptom to be uncommon; (b) they perceive the symptom to be unimportant; (c) they perceive there is no treatment for the symptom; and/or (d) time does not permit. Similarly, patients may not volunteer a symptom if (a) they perceive the symptom to be inevitable; (b) they perceive there is no treatment for the symptom; (c) they sense that healthcare professionals perceive the symptom to be unimportant; and/or (d) other symptoms predominate.
Symptom assessment tools can facilitate good clinical practice by improving the thoroughness of the assessment (and re-assessment) of common symptoms. Furthermore, validated symptom assessment tools are essential to undertaking robust research studies. However, many generic symptom assessment scales contain no oral symptoms (e.g., Edmonton Symptom Assessment Scale/ESAS [5]), or only a limited number of oral symptoms (e.g., Memorial Symptom Assessment Scale/MSAS [6]). For example, the MSAS, which consists of 32 symptoms (26 physical, 6 psychological), includes only four oral symptoms, i.e. “dry mouth”, “change in the way food tastes”, “difficulty swallowing”, and “mouth sores”. Interestingly, the Norwegian version of ESAS does include xerostomia, as this is one of the “10 common symptoms of advanced cancer” [7].
The aim of this scoping review was to identify/describe oral symptom assessment tools that have been specifically utilised in patients with “advanced cancer” [8], and particularly in cancer patients receiving symptom-oriented treatment (i.e. palliative care).
Methods
The function of a scoping review is to identify the available evidence rather than to produce critically appraised answers to research questions [9, 10]. The Arksey and O’Malley methodological framework [11], which has been enhanced/developed by Levac et al. [12] and the Joanna Briggs Institute [13], was used as a framework to conduct this scoping review. The PRISMA Extension for Scoping Reviews (PRISMA-ScR) checklist was used as a guide in reporting this scoping review [14].
Study eligibility criteria
We used the Population, Intervention, Comparator/control, Outcome and Study design (PICOS) framework to identify relevant research studies [15]. Eligible studies included adult patients with advanced cancer (as defined by the National Cancer Institute/NCI, USA): “cancer that is unlikely to be cured or controlled with treatment” [8]. Studies involving patient-rated oral symptom assessment tools, as well as quality of life (QoL) instruments that contain oral symptom items, were included. However, studies involving assessment of a single oral symptom (e.g., xerostomia), or a single cancer site (e.g., head and neck cancer), were not included. Observational and experimental studies were included. Perspective, commentary or opinion articles without original data were excluded.
Search strategy
A comprehensive search of three electronic databases including PubMed, Embase, and CINAHL was conducted from inception to 11 June 2021. The literature review was adapted to meet the requirements of each database searched with guidance from a health sciences librarian. The search was limited to English language articles. Reference lists of all eligible full texts were hand searched for other relevant articles. In addition, handsearching of reference lists of relevant chapters in academic textbooks was undertaken to ensure a comprehensive search of the literature was conducted.
Data management and synthesis
The EndNote 20™ (Clarivate) bibliographic software was used to store the records retrieved from all the literature searches. This software enables duplicates to be removed. We then used the Covidence software to screen these records. Two reviewers (NC, OM) independently screened the titles and abstracts using the PICOS criteria. Where an abstract was unavailable, the paper was included in the full text review process. If there was any conflict between the two reviewers, a third reviewer was available to determine inclusion. The same two reviewers independently reviewed the full texts, and extracted the relevant information using a review-specific proforma. Again, if there was any conflict between the two reviewers, a third reviewer was available to determine inclusion.
Results
Search results
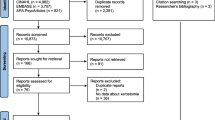
The search strategy identified 1179 unique references (Fig. 1). Fourteen papers were included in the full data extraction. One reference was a conference abstract and the authors confirmed that this was the same study as an included article. Five further articles were included following handsearching of the included full text articles. No further articles were included following handsearching of relevant chapters in academic textbooks.
Symptoms assessed
The number of oral symptoms assessed in each study varied from two [22, 23] to 20 [3, 36]. Xerostomia (“dry mouth”) was universally assessed, which is unsurprising as studies in patients with advanced cancer demonstrate a very high prevalence (i.e. 82–83.5%) [3, 36, 37]. Other commonly assessed symptoms included oral discomfort (18/18 studies), taste disturbance (15/18 studies), and denture problems (8/18 studies) (see Table 1).
It should be noted that the wording of the questions differed amongst the oral assessment tools: for example, taste disturbance was variously described as “altered taste”, “sour taste”, “disturbance of taste”, “taste disturbance(s)”, “unpleasant or altered taste sensation”, “bad or altered taste”, “change in the way food tastes”, “taste change”, “food and drink tasted different from usual”, and “dysgeusia” (although unclear as to the term used with the participants) [35].
Davies et al. [3] assessed 20 oral symptoms, many of which were not included in other studies (e.g. “sensitivity of teeth”, “altered sensation in mouth”, “burning sensation in mouth”, “bleeding from mouth”), and all of which were present in \(\ge 7.5\%\) of participants. Moreover, Davies et al. [3] identified a number of so-called oral symptom “clusters” in this cohort of patients, i.e. symptoms that frequently co-existed.
Dimensions assessed
Many of the (generally older) studies simply assessed the presence or absence of specific oral symptoms [7, 16,17,18,19, 23]. However, many of the (generally newer) studies assessed one or more dimensions, including frequency [3, 24, 27, 31, 36], intensity/severity [3, 21, 22, 24, 25, 27, 30, 31, 35, 36], level of distress or bothersomeness [3, 24, 36], level of limitation [30], and relative importance [22].
Symptom time frames
Many of the studies did not specify the time frames used in the questions. Of the studies that did specify a time frame, this varied from “in the previous 24 h” [31], to “during the past week” [3, 26, 34, 36]. Nevertheless, some studies appear to have used longer time frames based upon the results reported (e.g., up to 1 year [22]).
Discussion
As highlighted, oral symptoms are common in patients with advanced cancer. Furthermore, these symptoms are often frequent in occurrence, moderate to severe in intensity, and cause significant levels of distress (and so have a negative impact on quality of life). However, observational studies suggest that oral problems are not well-managed in this group of patients [38]. The reasons for the latter are several, and include inadequate assessment (including non-identification of oral symptoms/problems), inappropriate treatment, and inadequate re-assessment.
Symptom assessment tools can improve clinical practice through the improved/earlier identification of troublesome “orphan” symptoms (i.e. symptoms not usually reported or assessed) [39]. The “ideal” symptom assessment tool should be valid, reliable, relevant (for the population/specific scenario), comprehensive (for the specific scenario), multidimensional, and easy to administer/complete [40]. Symptom assessment tools also have a role in research, in both observational studies, and in interventional studies (as a means of demonstrating improvements in symptom control).
Currently, there is no consensus on the number of symptoms that should be included in symptom assessment tools. Longer (more comprehensive) symptom assessment tools may be more suited to research settings, whilst shorter assessment tools may be preferable for clinical practice due to related issues of patient burden, and inadequate completion.
Symptom assessment tools that only ask about the presence (or absence) of a symptom, or are limited to the assessment of a single dimension (e.g. frequency), risk under-estimating, and equally over-estimating, the importance of certain symptoms. For example, although a symptom may be frequent in nature, it may not cause significant distress (and so may not require any intervention). It should be noted that the level of distress of a symptom is often a very good indicator of its impact on the person’s quality of life (although frequency, and especially intensity/severity, is also important) [40].
Many of the included studies used study-specific questionnaires, which had not been validated, although some contained elements from other validated assessment tools (see Table 1). Validated tools included the MSAS [24], the EORTC QLQ-OH17 [26], the EORTC QLQ-OH15 [34], and the OSAS [3, 36]. One study used the OHIP [31], although related results were not presented (and it was unclear which version was used). Of note, another study used selected elements from the OHIP [27].
The MSAS is a 32-item multidimensional generic symptom assessment scale, which has been extensively validated in cancer patients [6]. It contains four oral symptoms (i.e. “dry mouth”, “difficulty swallowing”, “mouth sores” and “change in the way food tastes”). The MSAS also provides blank spaces for the patient to add additional symptoms not mentioned within the tool. Davies et al. [24] supplemented the MSAS with three further oral symptoms (“oral discomfort”, “difficulty chewing” and “difficulty speaking”). The MSAS involves patients rating the frequency, severity, and distress caused by each of the physical symptoms.
The EORTC QLQ oral health module is a validated quality of life instrument, which includes a number of oral symptoms. It was initially developed as the EORTC QLQ OH-17 (a 17-item tool) [26], but was subsequently refined to the EORTC QLQ-15 (a 15-item tool) [34]. This oral health module must be completed alongside the core EORTC QLQ C-30 instrument. The EORTC QLQ-15 assesses 12 oral symptoms with three further items pertaining to the wearing of dentures, and information received about dental or mouth problems.
The OSAS is a novel 20-item multidimensional oral symptom assessment tool, which has undergone initial validation in patients with advanced cancer (and is currently undergoing further validation in this group of patients) [3, 36]. The OSAS was modelled on the MSAS. The symptoms assessed are shown in Table 1, and it also provides blank spaces for the patient to add any additional oral symptoms not mentioned within the tool. The OSAS involves patients rating the frequency, severity, and distress caused by each of the oral symptoms.
Conclusion
Symptom assessment tools can facilitate good symptom control in clinical practice, and are an integral component of clinical research.This scoping review identified four validated symptom assessment scales that could be utilised to assess oral symptoms in patients with advanced cancer, including one cancer-specific quality of life scale (EORTC QLQ OH-15), one generic tool for assessing the “social impact” of specific oral problems (OHIP), one cancer-specific generic symptom assessment scale (MSAS), and one cancer-specific oral symptom assessment scale (OSAS).
References
Radbruch L, De Lima L, Knaul F, Wenk R, Ali Z, Bhatnaghar S et al (2020) Redefining palliative care - a new consensus-based definition. J Pain Symptom Manag 60:754–764
Teunissen SC, Wesker W, Kruitwagen C, de Haes HC, Voest EE, de Graeff A (2007) Symptom prevalence in patients with incurable cancer: a systematic review. J Pain Symptom Manag 34:94–104
Davies A, Buchanan A, Todd J, Gregory A, Batsari KM (2021) Oral symptoms in patients with advanced cancer: an observational study using a novel oral symptom assessment scale. Support Care Cancer 29:4349–4356
Shah S, Davies AN (2001) Re: Medical records vs. patient self-rating. J Pain Symptom Manag 22:805–806
Chang VT, Hwang SS, Feuerman M (2000) Validation of the Edmonton Symptom Assessment Scale. Cancer 88:2164–2171
Portenoy RK, Thaler HT, Kornblith AB, McCarthy Lepore J, Friedlander-Klar H, Kiyasu E et al (1994) The Memorial Symptom Assessment Scale: an instrument for the evaluation of symptom prevalence, characteristics and distress. Eur J Cancer 30:1326–1336
Wilberg P, Hjermstad MJ, Ottesen S, Herlofson BB, Wilberg P, Hjermstad MJ et al (2012) Oral health is an important issue in end-of-life cancer care. Support Care Cancer 20:3115–3122
National Cancer Institute Dictionary of Cancer Terms (2022) NCI website. https://www.cancer.gov/publications/dictionaries/cancer-terms/def/advanced-cancer. Accessed February 2022
Munn Z, Peters MDJ, Stern C, Tufanaru C, McArthur A, Aromataris E (2018) Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol 18:143
Lau J, Mazzotta P, Fazelzad R, Ryan S, Tedesco A, Smith AJ et al (2021) Assessment tools for problematic opioid use in palliative care: a scoping review. Palliat Med 35:1295–1322
Arksey H, O’Malley L (2005) Scoping studies: towards a methodological framework. Int J Soc Res Methodol 8:19–32
Levac D, Colquhoun H, O’Brien KK (2010) Scoping studies: advancing the methodology. Implement 5:69
Daudt HML, Van Mossel C, Scott SJ (2013) Enhancing the scoping study methodology: a large, inter-professional team’s experience with Arksey and O’Malley’s framework. BMC Med Res Methodol 13:48
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med 169:467–473
Schardt C, Adams MB, Owens T, Keitz S, Fontelo P (2007) Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inform Decis Mak 7:16
Pople J, Oliver D (1986) Oral thrush in hospice patients. Nurs Times 3986:34–35
Clarke J, Wilson J, Von Haacke N, Milne L (1987) Oral candidiasis in terminal illness. Health Bull 45:268–271
Aldred M, Addy M, Bagg J, Finlay I (1991) Oral health in the terminally ill: a cross-sectional pilot survey. Spec Care Dentist 11:59–62
Jobbins J, Bagg J, Finlay IG, Addy M, Newcombe RG (1992) Oral and dental disease in terminally ill cancer patients. Br Med J 304:1612
Sweeney M, Bagg J, Baxter W, Aitchison T (1997) Clinical trial of a mucin-containing oral spray for treatment of xerostomia in hospice patients. Palliat Med 11:225–232
Sweeney MP, Bagg J, Baxter WP, Aitchison TC (1998) Oral disease in terminally ill cancer patients with xerostomia. Oral Oncol 34:123–126
Oneschuk D, Hanson J, Bruera E (2000) A survey of mouth pain and dryness in patients with advanced cancer. Support Care Cancer 8:372–376
Milligan S, McGill M, Sweeney MP, Malarkey C (2001) Oral care for people with advanced cancer: an evidence-based protocol. Int J Palliat Nurs 7:418–426
Davies AN, Broadley K, Beighton D (2001) Xerostomia in patients with advanced cancer. J Pain Symptom Manag 22:820–825
Alt-Epping B, Nejad RK, Jung K, Groß U, Nauck F (2012) Symptoms of the oral cavity and their association with local microbiological and clinical findings - a prospective survey in palliative care. Support Care Cancer 20:531–537
Hjermstad MJ, Bergenmar M, Fisher SE, Montel S, Nicolatou-Galitis O, Raber-Durlacher J et al (2012) The EORTC QLQ-OH17: a supplementary module to the EORTC QLQ-C30 for assessment of oral health and quality of life in cancer patients. Eur J Cancer 48:2203–2211
Fischer DJ, Epstein JB, Yao Y, Wilkie DJ (2014) Oral health conditions affect functional and social activities of terminally ill cancer patients. Support Care Cancer 22:803–810
Slade GD, Spencer AJ (1994) Development and evaluation of the Oral Health Impact Profile. Community Dent Health 11:3–11
Epstein JB, Emerton S, Kolbinson DA, Le ND, Phillips N, Stevenson-Moore P et al (1999) Quality of life and oral function following radiotherapy for head and neck cancer. Head Neck 21:1–11
Mercadante S, Aielli F, Adile C, Ferrera P, Valle A, Fusco F et al (2015) Prevalence of oral mucositis, dry mouth, and dysphagia in advanced cancer patients. Support Care Cancer 23:3249–3255
Nikles J, Mitchell GK, Hardy J, Agar M, Senior H, Carmont S-A et al (2015) Testing pilocarpine drops for dry mouth in advanced cancer using n-of-1 trials: a feasibility study. Palliat Med 29:967–974
Thomson WM, Chalmers JM, Spencer AJ, Williams SM (1999) The Xerostomia Inventory: a multi-item approach to measuring dry mouth. Community Dent Health 16:12–17
Nikles J, Mitchell GK, Hardy J, Agar M, Senior H, Carmont SA et al (2013) Do pilocarpine drops help dry mouth in palliative care patients: a protocol for an aggregated series of n-of-1 trials. BMC Palliat Care 12:39
Hjermstad MJ, Bergenmar M, Bjordal K, Fisher SE, Hofmeister D, Montel S et al (2016) International field testing of the psychometric properties of an EORTC quality of life module for oral health: the EORTC QLQ-OH15. Support Care Cancer 24:3915–3924
Magnani C, Mastroianni C, Giannarelli D, Stefanelli MC, Di Cienzo V, Valerioti T et al (2019) Oral hygiene care in patients with advanced disease: an essential measure to improve oral cavity conditions and symptom management. Am J Hosp Palliat Med 36:815–819
Davies A, Batsari K, Waghorn M (2016) An observational study of the frequency of oral symptoms in patients with advanced cancer. Support Care Cancer 16:S149
Tranmer JE, Heyland D, Dudgeon D, Groll D, Squires-Graham M, Coulson K (2003) Measuring the symptom experience of seriously ill cancer and noncancer hospitalized patients near the end of life with the Memorial Symptom Assessment Scale. J Pain Symptom Manag 25:420–429
Kvalheim SF, Strand GV, Husebø BS, Marthinussen MC (2016) End-of-life palliative oral care in Norwegian health institutions. An exploratory study. Gerodontology 33:522–529
Santini D, Armento G, Giusti R, Ferrara M, Moro C, Fulfaro F et al (2020) Management of orphan symptoms: ESMO Clinical Practice Guidelines for diagnosis and treatment. ESMO Open 5:e000933
Delgado-Guay MO, Bruera E (2015) Multidimensional patient assessment. In: Bruera E, Higginson I, von Gunten CF, Morita T (eds) Textbook of Palliative Medicine and Supportive Care, 2nd edn. CRC Press, Boca Raton, pp 323–340
Funding
Open Access funding provided by the IReL Consortium
Author information
Authors and Affiliations
Contributions
The conception and design of this scoping review were formulated by NC. Material collection was conducted by NC. NC and OM contributed to the article review process. NC and AD contributed to the data collection and synthesis. The first draft of the manuscript was written by NC and AD commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This is a scoping review. Ethics approval was not required.
Consent to participate
Not applicable.
Consent for publication
No applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cleary, N., Mulkerrin, O.M. & Davies, A. Oral symptom assessment tools in patients with advanced cancer: a scoping review. Support Care Cancer 30, 7481–7490 (2022). https://doi.org/10.1007/s00520-022-07169-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-022-07169-1