Abstract
Purpose
Dorsal screw-rod instrumentations are used for a variety of spinal disorders. Cross-links (CL) can be added to such constructs, however, no clear recommendations exist. This study aims to provide an overview of the available evidence on the effectiveness of CL, potentially allowing to formulate recommendations on their use.
Methods
A systematic literature review was performed on PubMed and 37 original articles were included and grouped into mechanical, biomechanical, finite element and clinical studies. The change in range of motion (ROM) was analyzed in mechanical and biomechanical studies, ROM, stiffness and stress distribution were evaluated in finite element studies and clinical outcome parameters were analyzed in clinical studies.
Results
A relative consistent reduction in ROM in axial rotation with CL-augmentation was reported, while minor and less consistent effects were observed in flexion–extension and lateral bending. The use of CLs was clinical beneficial in C1/2 fusion, while the limited clinical studies on other anatomic regions show no significant benefit for CL-augmentation.
Conclusion
While CL provides some additional axial rotation stability in most situations, lateral bending and flexion–extension are less affected. Based on clinical data, CL-augmentation can only be recommended for C1/2 instrumentations, while for other cases, further clinical studies are needed to allow for evidence-based recommendations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Dorsal instrumentation is an effective tool in the surgical treatment of various spinal disorders. It is generally based on a screw-rod construct composed of pedicle or lateral mass screws combined with vertically oriented connecting rods. It has been shown that the rigidity of instrumentations correlates with fusion rate [1] and consequently, high rigidity in all loading directions is aspired. A large plethora of implants like plates, hooks, cerclages, cross-links and interbody devices were developed to be added to a dorsal screw-rod construct or to be used as a substitute for certain parts of such constructs. Finally, the configuration chosen must be safe and effective, and therefore, the optimal compromise between construct rigidity, surgical exposure, surgical time and implant cost must be aspired.
Cross-links (CL), connecting the contralateral rods or screw heads, can be added to virtually all configurations of dorsal instrumentation. Despite a large amount of the literature on CL, its application remains controversial in the clinical practice, since the biomechanical benefit must be weighed against the additional implant, larger exposure, increased surgical time and implant cost. So far, guidelines on the use of CL-augmentation in dorsal screw-rod constructs are lacking.
The aim of this systematic review was to provide an overview of the mechanical, biomechanical, numerical and clinical effect of CL-augmentation on dorsal screw-rod constructs. This information could help develop recommendations for the use of CLs in specific clinical situations.
Materials and methods
A systematic review in accordance with the PRISMA statement was conducted on PubMed (https://www.ncbi.nlm.nih.gov/pubmed/) with the search terms “crosslink spine”, cross-link spine”, “transfixation spine” and “transverse connector spine” on July 2019. Excluding duplicates, 195 studies were identified and evaluated in accordance with the process shown in Fig. 1. Abstracts, case reports and conference presentations as well as studies on instrumentations other than dorsal screw-rod constructs and studies not analyzing the effect of CL were excluded. Studies in languages other than English or German, and studies published before 1990 were excluded as well. To be included into the review, studies had to compare dorsal screw-rod constructs with the same construct with one or more CLs within a mechanical or biomechanical setting, or they had to compare clinical outcome parameters of patients treated with dorsal instrumentations with or without CLs. Studies found through reference lists were evaluated with the same process. The included studies were grouped into mechanical experiments on synthetic bone models, biomechanical experiments on animal cadavers, biomechanical experiments on human cadavers, finite element simulations and in vivo studies with human patients.
Most mechanical and biomechanical studies reported the relative change in range of motion (ROM) due to addition of the CL as their primary outcome parameter [2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18]. Most other studies [19,20,21,22,23,24,25,26] reported change in stiffness over the whole loading magnitude. In these cases, the change in stiffness was converted into change in ROM for better comparability. Other outcome parameters like change in neutral zone, stiff zone and lax zone were not incorporated into the review. To reduce the amount of data, independently reported values for flexion and extension were pooled to one value for flexion–extension (FE). The types of CL were grouped into horizontal rod-rod cross-links (hR-R CL), horizontal screw-screw cross-links (hS-S CL) and diagonal screw-screw cross-links (dS-S CL) (Fig. 2).
Results
Biomechanical studies on synthetic bone models
Four studies analyzed the effect of CL using synthetic bone models [2, 19,20,21] (Table 1). All four studies added one and two hR-R CL to synthetic models instrumented with a dorsal pedicle screw-rod construct. The results of three studies were converted from stiffness values to relative change in ROM (Fig. 3) [19,20,21]
The change in range of motion (ROM) due to the addition of one and two horizontal rod-rod cross-links (1 CL) are plotted for axial rotation, flexion–extension and lateral bending for the mechanical studies performed on synthetic bone models. Changes reported as statistically significant are marked with an asterisk (*)
A significant decrease in AR-ROM of up to 31% for one and up to 44% for two regular hR-R CL was reported. In FE, ROM was measured to be reduced less than 8% with one and less than 12% with two regular R-R CL. Minimal changes in LB-ROM were reported with one and two regular hR-R CL. In two of the studies, the effect of vertical rod length was investigated [2, 20]. Both studies demonstrated that AR-rigidity decreases with longer construct, while the addition of a hR-R CL had a stronger effect on such longer and more unstable constructs [2, 20]. Custom built cross-links with very large cross-sectional areas were observed to be more effective in AR and FE compared to regular cross-links [20].
Biomechanical studies on animal cadavers
Eight biomechanical studies on animal cadavers were included [3, 11, 12, 22,23,24,25, 27] (Table 2). Three studies were performed on porcine and five studies on calf cadavers. Vertebrae originated from the thoracic, the thoracolumbar and the lumbar spine. Uni-segmental as well as multi-level (segmental and non-segmental) instrumentations were analyzed. Reported changes in stiffness were converted into ROM for four studies [22, 24, 25, 27].
The application of one hR-R CL led to a reduction in AR-ROM ranging from 5 to 59%, while the addition of two hR-R CL reduced AR-ROM between 10 and 30%. In FE, one hR-R CL led to a reduction in ROM from − 1 to 18%, while two hR-R CL reduced ROM from 1 to 6%. In LB, one hR-R CL reduced ROM from 1 to 16%, while two hR-R CL reduced ROM from 8 to 14% (Fig. 4).
The change in range of motion (ROM) due to the addition of one and two horizontal cross-links (1 CL) are plotted for axial rotation, flexion–extension and lateral bending for all biomechanical studies on animal cadavers. Changes reported as statistically significant in the studies are marked with an asterisk (*)
Comparing the effectiveness of hR-R CL on single-level to multi-level instrumentations, here, the included animal cadaver studies did not show a consistent difference. The effect of hR-R CL was more pronounced in segmental than in non-segmental instrumentations in LB [24]. This trend was however not seen to the same extent in AR, FE and AC [24, 27].
One study compared different CL-configurations: double hR-R CL, double hS-S CL and double dS-S CL. The greatest increase in AR-stability was observed with double dS-S CL, followed by double hS-S CL and double hR-R CL [22]. In another study, however, single hS-S CL was observed to be more effective in AR and LB compared to single dS-S CL, while the opposite relation was observed for FE [12].
Biomechanical studies on human cadavers
Fifteen biomechanical studies with human cadavers were included. They were grouped into occipitocervical [13, 14], cervical [15, 17, 18, 28], cervicothoracic [4], thoracic [5, 16], thoracolumbar [6,7,8, 26] and lumbar [9, 10] (Table 3). All studies used either hR-R CL or hS-S CL. Conversion from stiffness to ROM was done for one study (Fig. 5) [26].
The change in range of motion (ROM) due to the addition of one and two horizontal rod-rod cross-links (1 CL) are plotted for axial rotation, flexion–extension and lateral bending for all biomechanical studies on human cadavers. Changes reported as statistically significant in the studies are marked with an asterisk (*)
Occipitocervical
Two studies analyzed the effect of CL-augmentation on dorsal occipitocervical instrumentations [13, 14]. In both studies, the effect of one hR-R CL on the ROM was reported to be non-significant. Specific values were however not provided in the manuscripts.
Cervical
Of the four biomechanical studies on human cervical spines, two analyzed the effect of CL on the atlantoaxial region with one study using C1 and C3 lateral mass screws [15] and the other using a special implant configuration at C1–C2 [28]. In both studies, the addition of one hR-R CL reduced ROM in AR in the presence of an odontoidectomy significantly (−54% and −37%, respectively). The effect of CL in the intact situation (without odontoidectomy) was not quantified in the first and described as non-significant in the second study (− 15%). LB-ROM was reduced significantly in the second study only in the odontoidectomy situation (− 43%), while the effect was non-significant in the first study (− 13%) and in the intact situation of the second study (−24%). The effects in FE were non-significant in both studies with values below − 21%.
The effect of different CL locations and types of CL on the ROM of C3–C7 lateral mass screw instrumentations was analyzed in another study [17]. Without laminectomy, no CL-configuration changed the ROM in a statistically significant way. After laminectomy, however, the addition of two CL in three of the tested configurations led to a significant reduction of ROM in AR. The two types of CL used in this study (hS-S CL, hR-R CL) showed no statistically significant difference in effectiveness [17].
Analyzing the cervical region with C3–C6 lateral mass screws and pedicle screws at C7, a significant reduction in AR-ROM with one (− 29%) and two hS-S CL (− 44%) as well as a significant reduction of LB-ROM with two hS-S CL (− 13%) was observed in both, the intact and the destabilized situation [18]. The relative effect of the CL remained relatively constant with an increasing extent of decompression and facetectomy [18].
Cervicothoracic
In dorsal instrumentations of C6–T2, the addition of 2 h-R CL led to a significant reduction in AR-ROM in the 3-column injury model at C7/T1 (− 27%). A similar trend was observed in the 2-column-injury model at C7/T1. Thoracic hR-R CL showed a trend of being more effective than the cervical hR-R CL [4].
Thoracic
In thoracic instrumentations of T4–T10, the addition of one and two hR-R CL reduced ROM significantly (average 21% for one and 34% for two CL) [5]. In LB and FE, the addition of one and two hR-R CL did not reduce the ROM significantly [5]. Analogously, another study analyzing the same anatomical region with an additional pedicle subtraction osteotomy at T7 found a reduction of AR-ROM with one (26%, ns.) and two hR-R CL (48%, *), while no relevant effect was observed in FE and LB [16].
Thoracolumbar
The thoracolumbar region has been investigated in four biomechanical studies performed on human cadaveric spines [6,7,8, 26]. In testing of embalmed specimens, completely destabilized at L1 and instrumented at T12 and L2, the addition of one and two CL decreased ROM in AR up to 38% and in LB up to 89%, whereas only a subgroup of the differences were statistically significant [26]. In another study on specimens destabilized and dorsally instrumented at T12/L1, the addition of one hR-R CL reduced ROM significantly in AR (21%), while LB and FE were not affected to the same extent [7]. In a study on cadavers with corpectomy and spacer instrumentation at T12, the addition of one hR-R CL to two different types of dorsal instrumentations led to a reduction in AR-ROM of 44% and 51%, while the effect in LB and FE was below 18% and 12%, respectively [6]. ROM after T12 corpectomy and instrumentations at T11 and L1 was significantly reduced in AR by the addition of one and two CL (16% and 31%, respectively), while the effects in FE and LB were non-significant [8].
Lumbar
The biomechanical effects on the lumbar spine have been investigated by two groups [9, 10]. In destabilized specimens at L3/4 and L4/5, the addition of one hR-R CL to a dorsal instrumentation at L3 and L5 reduced ROM in AR significantly (21%) only with CoCr vertical rods, while the effect with Titanium rods was similar (18%), but statistically non-significant. The non-significant effects in FE and LB were below 1% and 4%, respectively [9]. In specimens with corpectomy L3 and dorsal instrumentation at L2 and L4, the change in ROM due to one hR-R CL was not altered significantly in AR, LB and FE, while the observed effect was most prominent in LB with 16% [10].
Biomechanical studies with numerical simulations
Six studies were included that used finite element simulations to evaluate the biomechanical effect of CL-augmentation on dorsal instrumentations [11, 12, 29,30,31,32] (Table 4). One study focused on the thoracolumbar region [29], four studies on the lumbar region [11, 12, 30, 31], and one study evaluated a long instrumentation from T1-sacrum [32]. The values reported for change in ROM are illustrated in Fig. 6.
One study analyzed the stiffness of constructs with one hR-R CL, one dR-R- CL and two dR-R CL (X-shaped) effects of CL on longer constructs, while the largest effect was seen in AR and LB when simulating the augmentation with an X-shaped CL configuration.[29].
Bone loads (von Mises) were observed to decrease with the use of a CL [12, 29]. Similarly, loads (von Mises) on the pedicle screw neck decreased [29]. This is opposed by another study in which a general increase in screw loads (strain energy) in AR and LB was observed [12]. Peak loads (peak von Mises) on the vertical rod were seen to increase in one study [31], while another study calculated better stress dispersion on the rod in situations with CL-implantation [32].
Regarding optimal CL-positions, larger effects on the rigidity were computed for placement in the proximal part of the construct [11, 33] and at an osteotomy-site [33].
In vivo studies
Six in vivo studies on human patients were identified [33,34,35,36,37,38] (Table 5). Two studies were performed on atlantoaxial instrumentations and found earlier bony fusion in the hS-S CL group [34] and in the hR-R CL group [33] compared to the no-CL groups. Furthermore, favorable neurological scores were observed in the hR-R CL group compared to the no-CL group [33].
In the thoracolumbar region, two studies on patients with adolescent idiopathic scoliosis treated with dorsal instrumentations found no clinical, radiologic or surgical differences for the groups with and without hR-R CL [36, 37]. Another study suggests to omit CL-augmentation since no rotational instability was observed without the use of CL [38]. Comparing the effectiveness of different types of CL, lower reoperation rates were observed in closed drop entry CL compared to other types of CL [35].
Discussion
The stability of dorsal instrumentation is of great importance for bony fusion and consequently for a good clinical outcome [1]. To achieve the required stiffness, a plethora of augmenting components like interbody cages, pedicle hooks, cerclages, end-to-end and side-to-side connectors as well as CLs have been proposed for the use in certain clinical settings. For the application of CLs, no clear recommendations or guidelines exist, and the use of these components is based on the subjective evaluation of the surgeon. The addition of elements to a biomechanical construct can be argued to generally increase stability, while also cost, surgical exposure, surgical time and additional foreign body implantation have to be considered and weighed against the beneficial effects. The aim of this systematic review was to create an overview of the effect of CL-augmentation to contribute to a more informed decision on whether or not to include CL in dorsal instrumentations.
Synthetic models
Synthetic models, having the advantage of eliminating anatomical variability, show a clear effect of horizontal R-R CL with up to 30% reduction in ROM in axial rotation. The effects in FE and LB were found to be much smaller with values below 12% and 3%, respectively.
Animal cadaver studies
Animal cadaver studies show very similar results to the synthetic models with the largest effect of CL-augmentation in AR. While these studies integrate factors like the screw-bone interface, morphology and bone density can vary from humans.
Human cadaver studies
The biomechanical studies on the different parts of the human spine showed similar results with the largest effects of CL-augmentation being observed in AR, while only minimal effects were recorded in FE and more irregular results were observed in LB.
Numeric simulations
The general stress in the vertebral bodies and the mean stress in the instrumentations were observed to be reduced by CL-augmentation. However, peak loads and stress accumulation in the vertical rods were increased, which might be problematic in situations where material failure poses a problem.
Several generally applicable biomechanical observations can be stated:
-
CL-augmentation adds stability to the construct mainly in AR.
-
Two CLs are more effective than a single CL [2, 4, 5, 8, 11, 16, 17, 19,20,21, 26].
-
A CL with a larger cross section is more effective than a smaller one [19, 20].
-
Longer single-level constructs are less rigid in AR and CL-augmentation is more effective in such situations [2, 20].
-
In destabilized situations, CL-augmentation is observed to be more effective by the majority of studies [3, 15, 17, 28], while this correlation was less evident in other studies [4, 14, 18].
-
CLs are not more effective in multi-level constructs (segmental and non-segmental) compared to single-level constructs [24, 27, 39].
-
CLs do not provide the same stability as segmental screws in multi-level instrumentations [39].
-
The biomechanical effectiveness of screw-screw and rod-rod CLs is generally not different [17].
-
Diagonal CL shows higher effectiveness in FE and LB, while horizontal CL are more effective in AR [12, 29].
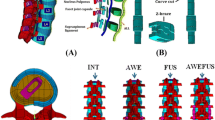
Based on the mechanical, biomechanical and numerical studies, we evaluate the effectiveness of CL to be based on the prevention of shear deformation of the screw-rod construct, also described as the “windshield wiper” effect. As illustrated in Fig. 7, such deformation primarily occurs during AR, less during LB and only minimally during FE. In conclusion, the largest effect of CL-augmentation can be expected in AR, less in LB and only minimal effects in FE, which agrees with the literature.
Although in vitro experiments are crucial to understand and predict the biomechanical effect of CL-augmentation, this information is not sufficient to predict the effect on clinical outcome. To answer this question, in vivo studies are indispensable, however, only a limited number of studies is available. In the setting of C1/2-instrumentation, CL-augmentation has been observed to result in earlier bony fusion, superior clinical outcome and in no additional complications. The reduced number of clinical and radiologic follow-up controls and the improved patient satisfaction was stated to possibly compensate for the additional cost of about 1000 dollars per CL [33, 34]. In retrospective analysis, CL-augmented instrumentations in idiopathic scoliosis patients were not associated with a better clinical or radiologic outcome [36, 37]. While biomechanically, CLs provide some benefits in such constructs, CL-augmentation was also observed to be associated with soft tissue irritation and delayed infection [40] and with an increased risk of pseudarthrosis due to the reduced bone graft volume at the CL position [41].
In conclusion, based on clinical data, the general use of CL-augmentation can only be recommended for C1/2 instrumentations. In the surgical treatment of idiopathic scoliosis, CL-augmentation cannot be recommended as a standard measure. Based on biomechanical studies, an increase in AR-stability can be expected for many other clinical situations, however, no clinical data is available. The increase in AR-stability could be especially beneficial in situation of relevant AR-instability (e.g., after bilateral facetectomy), however, due to the fact that CL-augmentations provides potential drawbacks, such as the risk of irritation, delayed infection, pseudoarthrosis, increased costs, surgery time and exposure, clear clinical evidence is required to justify the usage of CL. Therefore, further clinical research on this topic is strongly suggested to further assess the benefit of CL in distinct clinical situations and to legitimate its usage.
Abbreviations
- AR:
-
Axial rotation
- CL:
-
Cross-link
- dS-S CL:
-
Diagonal screw-screw cross-links
- FE:
-
Flexion–extension
- hR-R CL:
-
Horizontal rod-rod cross-links
- hS-S CL:
-
Horizontal screw-screw cross-links
- LB:
-
Lateral bending
- ROM:
-
Range of motion
References
Zdeblick TA (1993) A prospective, randomized study of lumbar fusion: priliminary results. Spine Phila Pa 1976 18:983–991
Pintar FA, Maiman DJ, Yoganandan N et al (1995) Rotational stability of a spinal pedicle screw/rod system. J Spinal Disord 8:49–55. https://doi.org/10.1097/00002517-199502000-00007
Chutkan NB, Zhou H, Akins JP, Wenger KH (2008) Effects of facetectomy and crosslink augmentation on motion segment flexibility in posterior lumbar interbody fusion. Spine J 33:E828–E835. https://doi.org/10.1097/BRS.0b013e318183bb6d
O’Brien JR, Dmitriev AE, Yu W et al (2009) Posterior-only stabilization of 2-column and 3-column injuries at the cervicothoracic junction: a biomechanical study. J Spinal Disord Tech 22:340–346. https://doi.org/10.1097/BSD.0b013e31816f68d9
Kuklo TR, Dmitriev AE, Cardoso MJ et al (2008) Biomechanical contribution of transverse connectors to segmental stability following long segment instrumentation with thoracic pedicle screws. Spine Phila Pa 1976 33:E482–E487. https://doi.org/10.1097/BRS.0b013e31817c64d5
Arand M, Wilke HJ, Schultheiss M et al (2000) Comparative stability of the “internal fixator” and the “universal spine system” and the effect of crosslinking transfixating systems. a biomechanical in vitro study. Biomed Tech 45:311–316. https://doi.org/10.1515/bmte.2000.45.11.311
Bastian L, Knop C, Lange U, Blauth M (1999) Einfluß eines Querverbinders oder einer cerclage auf die mechanische stabilität des fixateur interne. Orthopade 28:714. https://doi.org/10.1007/s001320050401
Wahba GM, Bhatia N, Bui CNH et al (2010) Biomechanical evaluation of short-segment posterior instrumentation with and without crosslinks in a human cadaveric unstable thoracolumbar burst fracture model. Spine Phila Pa 1976 35:278–285. https://doi.org/10.1097/BRS.0b013e3181bda4e6
Doulgeris JJ, Aghayev K, Gonzalez-Blohm SA et al (2013) Comparative analysis of posterior fusion constructs as treatments for middle and posterior column injuries: an in vitro biomechanical investigation. Clin Biomech 28:483–489. https://doi.org/10.1016/j.clinbiomech.2013.05.001
Steffen R, Wittenberg R, Plafki C (2003) Biomechanische untersuchungen lumbaler spondylodesen mittels fixateur interne aus einer titanlegierung. Z Orthop Ihre Grenzgeb 141:73–78. https://doi.org/10.1055/s-2003-37301
Lim TH, Eck JC, An HS et al (1996) Biomechanics of transfixation in pedicle screw instrumentation. Spine Phila Pa 1976 21:2224–2229. https://doi.org/10.1097/00007632-199610010-00009
Lim TH, Kim JG, Fujiwara A et al (2001) Biomechanical evaluation of diagonal fixation in pedicle screw instrumentation. Spine Phila Pa 1976 26:2498–2503. https://doi.org/10.1097/00007632-200111150-00020
Finn MA, Fassett DR, Mccall TD et al (2008) The cervical end of an occipitocervical fusion: a biomechanical evaluation of 3 constructs - Laboratory investigation. J Neurosurg Spine 9:296–300
Scheer JK, Tang J, Eguizabal J et al (2010) Optimal reconstruction technique after C-2 corpectomy and spondylectomy: a biomechanical analysis. J Neurosurg Spine 12:517–524. https://doi.org/10.3171/2009.11.spine09480
Brasiliense LBC, Lazaro BCR, Reyes PM et al (2010) Stabilization of the atlantoaxial joint with C1–C3 lateral mass screw constructs: biomechanical comparison with standard technique. Neurosurgery 67:422–428. https://doi.org/10.1227/NEU.0b013e3181fb414c
Lehman RA, Kang DG, Wagner SC et al (2015) Biomechanical stability of transverse connectors in the setting of a thoracic pedicle subtraction osteotomy. Spine J 15:1629–1635. https://doi.org/10.1016/j.spinee.2015.03.010
Majid K, Gudipally M, Hussain M et al (2011) The biomechanical effect of transverse connectors use in a pre- and postlaminectomy model of the posterior cervical spine: an in vitro cadaveric study. Spine Phila Pa 1976 36:E1694–E1701. https://doi.org/10.1097/BRS.0b013e3182276735
Shaw MN, Morel EP, Utter PA et al (2011) Transverse connectors providing increased stability to the cervical spine rod-screw construct: an in vitro human cadaveric study. Lab invest J Neurosurg Spine 14:719–725. https://doi.org/10.3171/2011.1.SPINE10411
Dick JC, Zdeblick TA, Bartel BD, Kunz DN (1997) Mechanical evaluation of cross-link designs in rigid pedicle screw systems. Spine J 22:370–375
Korovessis P, Baikousis A, Deligianni D et al (2001) Effectiveness of transfixation and length of instrumentation on titanium and stainless steel transpedicular spine implants. J Spinal Disord 14:109–117. https://doi.org/10.1097/00002517-200104000-00004
Peltier C, Germaneau A, Dupré JC et al (2017) Biomechanical analysis of different cross-link configurations spinal instrumentation systems: a preliminary study. Comput Methods Biomech Biomed Engin 20:157–158. https://doi.org/10.1080/10255842.2017.1382909
Valdevit A, Kambic HE, McLain RF (2005) Torsional stability of cross-link configurations: a biomechanical analysis. Spine J 5:441–445. https://doi.org/10.1016/j.spinee.2005.03.010
Nakajima Y, Hara M, Umebayashi D et al (2016) Biomechanical analysis of a pedicle screw-rod system with a novel cross-link configuration. Asian Spine J 10:993–999. https://doi.org/10.4184/asj.2016.10.6.993
Brodke DS, Bachus KN, Mohr RA, Nguyen BK (2001) Segmental pedicle screw fixation or cross-links in multilevel lumbar constructs. a biomechanical analysis. Spine J 1:373–379. https://doi.org/10.1016/S1529-9430(01)00116-4
Hart R, Hettwer W, Liu Q, Prem S (2006) Mechanical stiffness of segmental versus nonsegmental pedicle screw constructs: The effect of cross-links. Spine Phila Pa 1976 31:E35–E38. https://doi.org/10.1097/01.brs.0000194835.89010.22
Lynn G, Mukherjee DP, Kruse RN et al (1997) Mechanical stability of thoracolumbar pedicle screw fixation: the effect of crosslinks. Spine Phila Pa 1976 22:1568–1573. https://doi.org/10.1097/00007632-199707150-00007
Dick JC, Jones MP, Zdeblick TA et al (1994) A biomechanical comparison evaluating the use of intermediate screws and cross-linkage in lumbar pedicle fixation. J Spinal Disord 7:402–407. https://doi.org/10.1097/00002517-199410000-00006
Lehman RA, Kang DG, Wagner SC et al (2012) Biomechanical analysis of the C2 intralaminar fixation technique using a cross-link and offset connector for an unstable atlantoaxial joint. Spine J 12:151–156. https://doi.org/10.1016/j.spinee.2012.01.020
Alizadeh M, Kadir MRA, Fadhli MM et al (2013) The use of X-shaped cross-link in posterior spinal constructs improves stability in thoracolumbar burst fracture: a finite element analysis. J Orthop Res 31:1447–1454. https://doi.org/10.1002/jor.22376
Fan CY, Hsu CC, Chao CK et al (2010) Biomechanical comparisons of different posterior instrumentation constructs after two-level ALIF: a finite element study. Med Eng Phys 32:203–211. https://doi.org/10.1016/j.medengphy.2009.12.002
Park TH, Woo SH, Lee SJ et al (2019) Cross-link is a risk factor for rod fracture at pedicle subtraction osteotomy site: a finite element study. J Clin Neurosci. https://doi.org/10.1016/j.jocn.2019.04.036
Wang T, Cai Z, Zhao Y et al (2019) The influence of cross-links on long-segment instrumentation following spinal osteotomy: a finite element analysis. World Neurosurg 123:e294–e302. https://doi.org/10.1016/j.wneu.2018.11.154
Wang H, Yin Y, Li T et al (2019) Effects of transverse connectors on reduction and fixation of atlantoaxial dislocation and basilar invagination using posterior C1–C2 screw rod technique. Spine J. https://doi.org/10.1016/j.spinee.2019.06.021
Mizutani J, Inada A, Kato K et al (2018) Advantages of an on-the-screwhead crosslink connector for atlantoaxial fixation using the Goel/Harms technique. J Clin Neurosci 50:183–189. https://doi.org/10.1016/j.jocn.2018.01.043
Asher MA, Lai SM, Burton DC (2010) Analysis of instrumentation/fusion survivorship without reoperation after primary posterior multiple anchor instrumentation and arthrodesis for idiopathic scoliosis. Spine J 10:5–15. https://doi.org/10.1016/j.spinee.2009.08.460
Garg S, Niswander C, Pan Z, Erickson M (2015) Cross-links do not improve clinical or radiographic outcomes of posterior spinal fusion with pedicle screws in adolescent idiopathic scoliosis: a multicenter cohort study. Spine Deform 3:338–344. https://doi.org/10.1016/j.jspd.2014.12.002
Dhawale AA, Shah SA, Yorgova P et al (2013) Effectiveness of cross-linking posterior segmental instrumentation in adolescent idiopathic scoliosis: A 2-year follow-up comparative study. Spine J 13:1485–1492. https://doi.org/10.1016/j.spinee.2013.05.022
Kulkarni AG, Dhruv AN, Bassi AJ (2013) Should we cross the cross-links? Spine Phila Pa 1976 38:E1128–E1134. https://doi.org/10.1097/BRS.0b013e31829af99f
Papagelopoulos PJ, Currier BL, Neale PG et al (2003) Biomechanical evaluation of posterior screw fixation in cadaveric cervical spines. Clin Orthop Relat Res 411:13–24
Richards BS, Emara KM (2001) Delayed infections after posterior TSRH spinal instrumentation for idiopathic scoliosis: revisited. Spine Phila Pa 1976 26:1990–1996. https://doi.org/10.1097/00007632-200109150-00009
Kim YJ, Bridwell KH, Lenke LG et al (2005) Pseudarthrosis in primary fusions for adult idiopathic scoliosis: Incidence, risk factors, and outcome analysis. Spine Phila Pa 1976 30:468–474
Acknowledgements
The authors gratefully acknowledge the contribution of Maria-Rosa Fasser in proofreading the manuscript.
Funding
Open access funding provided by University of Zurich.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cornaz, F., Widmer, J., Snedeker, J.G. et al. Cross-links in posterior pedicle screw-rod instrumentation of the spine: a systematic review on mechanical, biomechanical, numerical and clinical studies. Eur Spine J 30, 34–49 (2021). https://doi.org/10.1007/s00586-020-06597-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06597-z