Abstract
Purpose
To evaluate the effects of percutaneous vertebroplasty (PVP) with conventional transpedicle approach (CTA) or basal transverse process-pedicle approach (BTPA) on the treatment of thoracolumbar osteoporotic vertebral compression fractures (TL-OVCFs) with narrow pedicles.
Methods
A retrospective study of TL-OVCFs with narrow pedicles was performed, including 78 cases of CTA and 84 cases of BTPA. The surgical outcomes, radiographic parameters [the width and height of the pedicle (PW, PH), the inclination angle of puncture (PIA)] and clinical indicators [visual analog scale (VAS) score, Oswestry Disability Index (ODI)] of two groups were compared.
Results
In terms of surgical outcomes of them, there was no difference in operation time (P > 0.05), while the volume of bone cement, the incidence of bone cement leakage and rate of good bone cement distribution were significantly worse in the CTA group (4.4 ± 0.6 ml vs. 5.5 ± 0.5 ml, 37.2% vs. 20.2%, 52.6% vs. 79.8%, P < 0.05). As for radiographic parameters and clinical indicators of them, the differences were not observed in the PH, PW, preoperative VAS score and ODI (P > 0.05), whereas the PIA, VAS score and ODI at 1 day postoperatively were significantly better in the BTPA group (17.3 ± 2.1° vs. 29.6 ± 2.8°, 2.7 ± 0.7 vs. 2.1 ± 0.8, 32.8 ± 4.6 vs. 26.7 ± 4.0, P < 0.05).
Conclusion
The study provided solid evidence that PVP with BTPA had more advantages in the treatment of TL-OVCFs with narrow pedicles, which can better relieve postoperative pain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Global aging is unstoppable and has resulted in a serious situation of osteoporosis [1, 2]. Osteoporosis is characterized by increasing bone fragility and can easily lead to osteoporotic vertebral compression fractures (OVCFs) [3], which have become a severe health problem because of high mortality and disability rate [4,5,6]. Thoracolumbar vertebra usually refers to the T11-L2 spinal level, which is the most common location of OVCFs because of the anatomical characteristics [7]. Nowadays, percutaneous vertebroplasty (PVP) has achieved good clinical results in the treatment of thoracolumbar OVCFs (TL-OVCFs) [8, 9]. The classic puncture approach of PVP is conventional transpedicle approach (CTA). However, due to the anatomical specificity of the thoracolumbar pedicles, its inner inclination angle is smaller than that of the lower lumbar spine [10]. Besides, a few pedicles are narrow due to anatomic variation, and its width is lower than normal value [11]. Therefore, the anatomical characteristics of narrow pedicles not only greatly increase the puncture difficulty of PVP with CTA, but also cause poor distribution and inadequate injection of bone cement, which can lead to poor postoperative symptom relief. Basal transverse process-pedicle approach (BTPA) is performed at the base of transverse process, which enters the vertebral body through the transverse process and pedicle. The inclination angle of puncture (PIA) of BTPA is larger than that of CTA [10], which can help the puncture needles to reach the center area of the vertebral body. Thus, the purpose of this study was to compare the clinical effects of two different puncture approaches on the treatment of TL-OVCFs with narrow pedicles.
Methods
Patient characteristics
This study was approved by our hospital’s Institutional Review Board, and informed consent was waived due to the retrospective nature of this study. The clinical data of single-segment TL-OVCFs (T11-L2) with narrow pedicles from March 2017 to March 2020 were retrospectively analyzed. Based on previous measurements of the normal value of thoracolumbar pedicles [12, 13], the diameter of the narrowest area in most thoracolumbar pedicles is generally greater than 7.5 mm. Therefore, in this study, if the width of the narrowest area of the pedicle measured on cross-sectional computed tomography (CT) is ≤ 6 mm, it is defined as the narrow pedicle. According to the different puncture approaches, they were divided into CTA group (78 cases) and BTPA group (84 cases). The surgical outcomes, radiographic parameters and clinical indicators of the two groups were compared. The inclusion criteria were as follows: (1) Single-segment fresh TL-OVCFs; (2) The width of the narrowest part of the bilateral pedicles ≤ 6 mm; (3) Mild vertebral collapse, loss of vertebral height < 25%; (4) No spinal cord injury; (5) The osteoporotic fracture (OF) classification of German Society for Orthopaedics and Trauma was OF1-OF2, and the score was ≥ 6 points [14, 15]. The exclusion criteria were as follows: (1) Pathological fractures caused by tuberculosis, tumor and infection; (2) With severe degenerative diseases such as scoliosis and lumbar disc herniation; (3) Combined with posterior fascia edema; (4) Inability to operate due to serious diseases; (5) Incomplete follow-up data.
The baseline data of patients are shown in Table 1. There were no significant differences in age, gender, bone mineral density, injured vertebral segment, fracture time, OF classification and score between the two groups (P > 0.05).
Surgical procedures and postoperative management
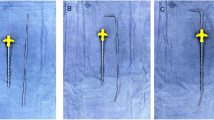
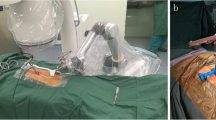
Both groups underwent bilateral puncture approach. The C-arm X-ray machine was used to locate the projection point of the pedicle on both sides of the injured vertebra (CTA group) or the projection point of the base of the transverse process (BTPA group) (Fig. 1). After disinfection and local anesthesia, incisions were made about 5 mm at the bilateral projection points. The puncture needles were inserted into the pedicles (CTA group) or the center of the basal transverse processes (BTPA group). Under C-arm X-ray machine guidance, the puncture needles of two groups were placed into the appropriate position of the vertebral body. Then, the bone cement was carefully injected guided by the C-arm X-ray machine. During the operation, bone cement leakage was observed. When the bone cement had solidified, the incisions were covered with gauze.
CTA group (A–C) and BTPA group (D–F). A and D The blue arrow represented the projection point and the puncture point. B and E The red arrow showed the location of the intraoperative puncture. C and F The black line indicated the puncture channel, and the blue area symbolized the direction of bone cement diffusion (CTA group: from the lateral area to the periphery, BTPA group: from the center to the periphery)
All patients were given standard anti-osteoporosis therapy after surgery, including basal therapy (Calcitriol capsules and calcium carbonate D3 were taken orally) and anti-osteoporosis therapy (Zoledronic acid was given intravenously). At 1 day postoperatively, the patients got out of bed with waist brace for rehabilitation.
Clinical and radiologic assessment
Clinical indicators included visual analog scale (VAS) score and Oswestry Disability Index (ODI), which were used to evaluate value of pain and impact of life, respectively. Radiographic parameters included the width and height of the pedicle (PW, PH) and PIA. The PW, PH and PIA were measured based on cross-sectional and sagittal CT (Fig. 2). The values of radiographic parameters were averaged by two experienced spinal surgeons as final results. The criteria for good bone cement distribution include that the bone cement evenly dispersed in the vertebral body on the lateral X-ray and in the central part of the vertebral body on the anteroposteric X-ray, and dispersed to the upper and lower endplates.
A The width of the narrowest area of the bilateral pedicles on cross-sectional CT represented PW (bilateral red lines). B The height of the medial area of the pedicle on sagittal CT was measured as PH (the red line). C, D PIA was formed by the intersection of the midline of the vertebral body and the puncture approach (C for CTA and D for BTPA)
Statistical analysis
The SPSS26.0 statistical software was applied for data analysis. The quantitative data were expressed as mean ± standard deviation. When the data were normally distributed, the independent sample T test was used for inter-group comparison. The count data were expressed as frequency, and the Chi-square test was used for comparison between two groups. P value < 0.05 was considered statistically significant.
Results
Surgical outcomes
The surgical outcomes are summarized in Table 2. All patients were operated on successfully without severe complications such as spinal cord injury and pulmonary embolism related to bone cement leakage. There was no statistical difference in the operation time between the two groups (P > 0.05), while the volume of bone cement in the CTA group was less than that in the BTPA group (4.4 ± 0.6 ml vs. 5.5 ± 0.5 ml, P < 0.05). As for rate of good bone cement distribution, the BTPA group was better than CTA group (79.8% vs. 52.6%, P < 0.001). In the CTA group, bone cement leakage occurred in 29 cases, while the BTPA group had 17 cases of bone cement leakage. The incidence of bone cement leakage in the CTA group was higher than that in the BTPA group (37.2% vs. 20.2%, P < 0.05).
Radiographic parameters
The comparison of radiographic parameters between the two groups is shown in Table 3. There were no significant differences in the PH and PW between the two groups (P > 0.05). The PIA of CTA group was 17.3 ± 2.1°, while that of BTPA group was 29.6 ± 2.8°, and there was a statistical difference between them (P < 0.001).
Clinical indicators
The comparison of clinical indicators between the two groups is presented in Table 4. The clinical indicators of both groups were significantly improved at 1 day postoperatively. The VAS score and ODI in CTA group and BTPA group decreased from (7.5 ± 0.8, 73.7 ± 5.5, 7.4 ± 0.9, 74.2 ± 5.3) at preoperation to (2.7 ± 0.7, 32.8 ± 4.6, 2.1 ± 0.8, 26.7 ± 4.0) at 1 day postoperatively, respectively. There were no differences in preoperative VAS score and ODI between the two groups (P > 0.05). However, the VAS score and ODI of BTPA group was better than those of CTA group at 1 day postoperatively (P < 0.05). Typical cases are shown in Figs. 3 and 4.
A 74-year-old female suffering from TL-OVCFs (L1) underwent PVP with BTPA. A Anteroposterior radiograph presented narrow projection of the bilateral pedicles. B The cross-sectional CT showed the width of the narrowest area of the bilateral pedicles was less than 6 mm and vertebral body wall damage. C Magnetic resonance imaging (MRI) suggested that vertebral compression fracture of L1. D The intersection between the edge of the vertebral body and the base of the transverse process was used as the puncture point. E, F Two needles reached the inner wall of the pedicle projection with a larger PIA on the anteroposterior radiograph and the posterior edge of the vertebral body on the lateral radiograph. G, H Postoperative radiographs showed good bone cement distribution without bone cement leakage
A 72-year-old female suffering from TL-OVCFs (L2) underwent PVP with CTA. A Anteroposterior radiograph showed narrow projection of the bilateral pedicles. B The cross-sectional CT presented the width of the narrowest area of the bilateral pedicles was less than 6 mm and vertebral body wall damage. C MRI suggested that vertebral compression fracture of L2. D The location of external wall of the pedicle projections were used as the puncture points. E, F Two needles reached the inner wall of the pedicle projection with a smaller PIA on the anteroposterior radiograph and the posterior edge of the vertebral body on the lateral radiograph. G, H Postoperative radiographs showed poor distribution and bone cement leakage
Discussion
It has confirmed that the morphology and anatomical structures of the pedicles are crucial for puncture of PVP [10]. In clinical practice, it is obvious that thoracolumbar narrow pedicles are not rare and more common in short women [11], which increase the difficulty of puncture, operative time and trauma. Based on anatomical and mechanical characteristics, TL-OVCFs are different from the lower lumbar spine and prone to kyphosis and collapse with improper treatment [16, 17]. Therefore, it is necessary to accurately understand the anatomical characteristics of narrow pedicles and important to explore the optimal puncture approach of PVP.
Good distribution of bone cement in PVP is required to achieve better clinical effects [18]. However, it is closely related to the ideal puncture point and larger PIA [10], which should be paid more attention to especially for TL-OVCFs with narrow pedicles. During the process of CTA, the puncture needles should be completely inside the pedicle to avoid enter the spinal canal. Due to the anatomical characteristics of TL-OVCFs with narrow pedicles, the PIA of CTA is significantly smaller [11]. However, the puncture point of BTPA group was located at the base of the transverse process and more outward than that of CTA group. Thus, the PIA was significantly higher than that of the CTA, and it was easier to reach the central area of the damaged vertebra where stress was concentrated on.
Bone cement leakage is one of the common complications of PVP [19], which can lead to biomechanical changes of injured vertebra and even spinal cord injury in severe cases [20]. For TL-OVCFs with perivertebral wall damage, the incidence of soft tissue leakage, intravascular leakage and intervertebral disk leakage is significantly increased [21, 22]. When PVP was performed with CTA, the channel of bone cement could not get close to the central area due to the smaller PIA. Then, the dispersion direction was from bilateral area of the vertebral body to the periphery during bone cement perfusion, which not only easily resulted in poor distribution of bone cement in the central area, but also significantly increased risk of bone cement leakage. Once bone cement leakage occurs during operation, surgeons often stop or reduce the injection of bone cement in order to avoid complications, which may lead to hypoperfusion of bone cement. However, in the BTPA group, the bone cement could reach the central area and diffuse from the central area to the periphery due to the larger PIA. Therefore, BTPA not only ensured the effective perfusion and facilitated the good distribution, but also reduced the risk of bone cement leakage.
The short-term purpose in the treatment of TL-OVCFs is to rapidly reduce pain and eliminate incapacitation [9]. The results of this study showed that clinical indicators in both groups were obviously improved at 1 day postoperatively. However, the postoperative VAS and ODI of CTA group were worse than those of BTPA group. The reason was the difference of bone cement perfusion and distribution between the two groups. It has concluded that the analgesic effect of high-dose bone cement is better than that of low-dose bone cement [23]. Besides, if bone cement is completely distributed in the fracture area, it can effectively strengthen the vertebral body and significantly relieve postoperative pain [24]. Therefore, how to effectively inject high-dose of bone cement and distribute it in the fracture area during PVP are particularly important. In this study, because of the smaller PIA of CPA group, bone cement distribution was poor, especially the fracture area in the center of vertebral body. Whereas in the BTPA group, the distribution of bone cement in the central area was good due to the larger PIA. Therefore, the postoperative clinical indicators of BTPA group were better than those of CTA group after surgery.
The study has some imitations. First of all, this is a single-center, retrospective and controlled study, which need to be further validated by multicenter, prospective and randomized studies. Secondly, the sample size in this study is small and a larger-sample is needed to reduce errors. Finally, this study did not discuss the follow-up results, especially the comparisons of long-term complications. Therefore, we will conduct a large-sample size, multicenter controlled study and further compare the follow-up results to improve this study in the future.
Conclusion
In conclusion, both groups of PVP were safe and effective in the treatment of TL-OVCFs with narrow pedicles. However, BTPA group has the larger PIA, higher-dose bone cement perfusion, better bone cement distribution and lower bone cement leakage incidence, which can more effectively relieve pain after surgery.
References
Zeng Q, Li N, Wang Q, Feng J, Sun D, Zhang Q, Huang J, Wen Q, Hu R, Wang L, Ma Y, Fu X, Dong S, Cheng X (2019) The Prevalence of Osteoporosis in China, a Nationwide, Multicenter DXA Survey. J Bone Miner Res 34:1789–1797. https://doi.org/10.1002/jbmr.3757
Kanis JA, Cooper C, Rizzoli R, Reginster JY (2019) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 30:3–44. https://doi.org/10.1007/s00198-018-4704-5
Ballane G, Cauley JA, Luckey MM, El-Hajj Fuleihan G (2017) Worldwide prevalence and incidence of osteoporotic vertebral fractures. Osteoporos Int 28:1531–1542. https://doi.org/10.1007/s00198-017-3909-3
Si L, Winzenberg TM, Jiang Q, Chen M, Palmer AJ (2015) Projection of osteoporosis-related fractures and costs in China: 2010–2050. Osteoporos Int 26:1929–1937. https://doi.org/10.1007/s00198-015-3093-2
Edidin AA, Ong KL, Lau E, Kurtz SM (2015) Morbidity and mortality after vertebral fractures: comparison of vertebral augmentation and nonoperative management in the medicare population. Spine (Phila Pa 1976) 40:1228–1241. https://doi.org/10.1097/brs.0000000000000992
Edidin AA, Ong KL, Lau E, Kurtz SM (2011) Mortality risk for operated and nonoperated vertebral fracture patients in the medicare population. J Bone Miner Res 26:1617–1626. https://doi.org/10.1002/jbmr.353
Rajasekaran S, Kanna RM, Shetty AP (2015) Management of thoracolumbar spine trauma: an overview. Indian J Orthop 49:72–82. https://doi.org/10.4103/0019-5413.143914
Martikos K, Greggi T, Faldini C, Vommaro F, Scarale A (2018) Osteoporotic thoracolumbar compression fractures: long-term retrospective comparison between vertebroplasty and conservative treatment. Eur Spine J 27:244–247. https://doi.org/10.1007/s00586-018-5605-1
Sanli I, van Kuijk SMJ, de Bie RA, van Rhijn LW, Willems PC (2020) Percutaneous cement augmentation in the treatment of osteoporotic vertebral fractures (OVFs) in the elderly: a systematic review. Eur Spine J 29:1553–1572. https://doi.org/10.1007/s00586-020-06391-x
Wang S, Wang Q, Kang J, Xiu P, Wang G (2014) An imaging anatomical study on percutaneous kyphoplasty for lumbar via a unilateral transverse process-pedicle approach. Spine (Phila Pa 1976) 39:701–706. https://doi.org/10.1097/brs.0000000000000243
He W, Qian Y, Yang WL, Han WQ, Lu XY, Jin C, Li J (2017) Applied anatomic study of narrow pedicle in thoracolumbar spine of adults. Chin J Orthop 37:36–43. https://doi.org/10.3760/cma.j.issn.0253⁃2352.2017.01.006
Hou S, Hu R, Shi Y (1993) Pedicle morphology of the lower thoracic and lumbar spine in a Chinese population. Spine (Phila Pa 1976) 18:1850. https://doi.org/10.1097/00007632-199310000-00021
Shi R, Liu H, Yuan Y, Wu W (2005) The measurement and comparison of pedicle internal structure in different segments. Chin J Clin Anat 23:458–462. https://doi.org/10.3969/j.issn.1001-165X.2005.05.003
Schnake KJ, Blattert TR, Hahn P, Franck A, Hartmann F, Ullrich B, Verheyden A, Mörk S, Zimmermann V, Gonschorek O, Müller M, Katscher S, Saman AE, Pajenda G, Morrison R, Schinkel C, Piltz S, Partenheimer A, Müller CW, Gercek E, Scherer M, Bouzraki N, Kandziora F (2018) Classification of osteoporotic thoracolumbar spine fractures: recommendations of the spine section of the German society for orthopaedics and trauma (DGOU). Global Spine J 8:46s–49s. https://doi.org/10.1177/2192568217717972
Blattert TR, Schnake KJ, Gonschorek O, Katscher S, Ullrich BW, Gercek E, Hartmann F, Mörk S, Morrison R, Müller ML, Partenheimer A, Piltz S, Scherer MA, Verheyden A, Zimmermann V (2019) Nonsurgical and surgical management of osteoporotic vertebral body fractures : recommendations of the Spine Section of the German society for orthopaedics and trauma (DGOU). Orthopade 48:84–91. https://doi.org/10.1007/s00132-018-03666-6
Chou KN, Lin BJ, Wu YC, Liu MY, Hueng DY (2014) Progressive kyphosis after vertebroplasty in osteoporotic vertebral compression fracture. Spine (Phila Pa 1976) 39:68–73. https://doi.org/10.1097/brs.0000000000000042
Li YX, Guo DQ, Zhang SC, Liang D, Yuan K, Mo GY, Li DX, Guo HZ, Tang Y, Luo PJ (2018) Risk factor analysis for re-collapse of cemented vertebrae after percutaneous vertebroplasty (PVP) or percutaneous kyphoplasty (PKP). Int Orthop 42:2131–2139. https://doi.org/10.1007/s00264-018-3838-6
Sun HB, Jing XS, Liu YZ, Qi M, Wang XK, Hai Y (2018) The Optimal volume fraction in percutaneous vertebroplasty Evaluated by pain relief, cement dispersion, and cement leakage: a prospective cohort study of 130 patients with painful osteoporotic vertebral compression fracture in the thoracolumbar vertebra. World Neurosurg 114:e677–e688. https://doi.org/10.1016/j.wneu.2018.03.050
Nieuwenhuijse MJ, Van Erkel AR, Dijkstra PD (2011) Cement leakage in percutaneous vertebroplasty for osteoporotic vertebral compression fractures: identification of risk factors. Spine J 11:839–848. https://doi.org/10.1016/j.spinee.2011.07.027
Saracen A, Kotwica Z (2016) Complications of percutaneous vertebroplasty: an analysis of 1100 procedures performed in 616 patients. Medicine (Baltimore) 95:e3850. https://doi.org/10.1097/md.0000000000003850
Wang HD, Yao FC, Fu ZY, Wu YJ (2019) Factors related to bone cement leakage during percutaneous vertebroplasty for elderly osteoporotic thoracolumbar vertebral compression fractures. J Spinal Surg 17:192–197. https://doi.org/10.3969/j.issn.1672-2957.2019.03.009
Tang B, Cui L, Chen X, Liu Y (2021) Risk factors for cement leakage in percutaneous vertebroplasty for osteoporotic vertebral compression fractures: an analysis of 1456 vertebrae augmented by low-viscosity bone cement. Spine (Phila Pa 1976) 46:216–222. https://doi.org/10.1097/brs.0000000000003773
Fu Z, Hu X, Wu Y, Zhou Z (2016) Is There a dose-response relationship of cement volume with cement leakage and pain relief after vertebroplasty? Dose Resp 14:1559325816682867. https://doi.org/10.1177/1559325816682867
Xu K, Li YL, Song F, Liu HW, Yang HD, Xiao SH (2019) Influence of the distribution of bone cement along the fracture line on the curative effect of vertebral augmentation. J Int Med Res 47:4505–4513. https://doi.org/10.1177/0300060519864183
Funding
No funds, grants or other support were received.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study. XL collected all the data and wrote the manuscript. XL and XY analyzed the data. JT reviewed and edited the manuscript. ZS and HW designed the study and reviewed and edited the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declared that they had no conflict of interest.
Ethical approval
This study was approved by the ethics committee of the fourth affiliated hospital of Nanjing Medical University (Ethics approval number: 20230109-k083). The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liu, X., Tian, J., Yu, X. et al. Comparison of clinical effects of percutaneous vertebroplasty with two different puncture approaches on the treatment of thoracolumbar osteoporotic vertebral compression fractures with narrow pedicles: a retrospective controlled study. Eur Spine J 32, 2594–2601 (2023). https://doi.org/10.1007/s00586-023-07714-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07714-4