Abstract
The morbidity and mortality rates of cardiovascular diseases (CVDs) are increasing; thus, they impose substantial health and economic burdens worldwide, and effective interventions are needed for immediate resolution of this issue. Recent studies have suggested that noncoding RNAs (ncRNAs) play critical roles in the occurrence and development of CVDs and are potential therapeutic targets and novel biomarkers for these diseases. Newly discovered modes of cell death, including necroptosis, pyroptosis, apoptosis, autophagy-dependent cell death and ferroptosis, also play key roles in CVD progression. However, ferroptosis, which differs from the other aforementioned forms of regulated cell death in terms of cell morphology, biochemistry and inhereditability, is a unique iron-dependent mode of nonapoptotic cell death induced by abnormal iron metabolism and excessive accumulation of iron-dependent lipid peroxides and reactive oxygen species (ROS). Increasing evidence has confirmed that ncRNA-mediated ferroptosis is involved in regulating tissue homeostasis and CVD-related pathophysiological conditions, such as cardiac ischemia/reperfusion (I/R) injury, myocardial infarction (MI), atrial fibrillation (AF), cardiomyopathy and heart failure (HF). In this review, we summarize the underlying mechanism of ferroptosis, discuss the pathophysiological effects of ncRNA-mediated ferroptosis in CVDs and provide ideas for effective therapeutic strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
CVDs remain major causes of death and disability in developing and developed countries [1, 2]; these diseases mainly include atherosclerosis, coronary artery diseases, myocardial I/R injury, hypertension, arrhythmia, heart valve disorders, cardiomyopathy and HF [3]. However, the heart is primarily composed of terminally differentiated cardiomyocytes that have limited regenerative capacity and physiological significance in regulating cardiac development, senescence and homeostasis [4, 5]. Therefore, a clear understanding of cardiovascular pathophysiology is need for the prevention, diagnosis, treatment and prognosis of CVDs.
A myriad of studies have indicated that cell death plays a central role in regulating tissue and cellular homeostasis and the pathogeneses of various diseases. Fundamentally, cell death is classified into two different types: accidental cell death (ACD) and regulated cell death (RCD) [6]. ACD is a passive process in which severe damage to cells is incurred via stimulation by various pathogenic factors. However, RCD, also known as programmed cell death, is an active process under physiological conditions and can be further classified into apoptotic and nonapoptotic forms. Many nonapoptotic forms of RCD, such as necroptosis, pyroptosis, apoptosis, autophagy-dependent cell death and ferroptosis, have been identified, and they exert a significant influence on the occurrence and progression of numerous diseases, particularly CVDs [6, 7]. Additionally, recent studies have identified other RCD modes, such as cuproptosis [8, 9] and PANoptosis [10, 11]. However, ferroptosis is the most recently discovered type of RCD. In 2012, Dixon et al. [12] first proposed ferroptosis as a unique iron-dependent form of nonapoptotic cell death that is triggered by the oncogenic RNA-selective lethal (RSL) small-molecule erastin in rat RAS-mutant tumor cells. Ferroptosis, which is distinct from other forms of RCD in terms of morphology, biochemistry, genetics and metabolic manifestations, is dependent on the intracellular iron level but not the level of other metals [7, 12]. Intriguingly, ferroptotic cell death is associated with significant abnormal changes in mitochondrial morphology, including shrinkage, swelling, a reduction in the number or disappearance of cristae, a decrease in the membrane density and rupture of the outer membranes, while the morphology of the nucleus remains unchanged [13, 14].
Studies have shown that ferroptosis is extensively involved in the pathophysiology of various conditions, such as neurodegenerative diseases [15], cancer [16], acute kidney injury [17], liver disease [18] and I/R injury [19], and it is closely related to iron, lipid and antioxidant metabolism pathway impairment. Moreover, recent studies have uncovered links between ferroptosis and CVDs. For example, histochrome treatment decreases intracellular and mitochondrial ROS levels which rescues the myocardium from I/R injury by preventing ferroptotic cell death [20]. Therefore, insight into the mechanism underlying cardiac cell ferroptosis is crucial for obtaining an in-depth understanding of the pathogenesis of CVDs.
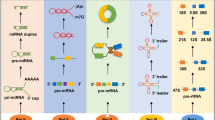
ncRNAs, a class of RNA molecules that do not encode proteins, are generally classified into two categories based on their nucleotide length: short or small-chain ncRNAs (including microRNAs, miRNAs) comprising approximately 18–200 nucleotides and long-chain ncRNAs (lncRNAs), comprising more than 200 nucleotides [21, 22]. In addition, lncRNAs can be further classified into six types according to their relative position to neighboring coding regions in the genome: sense lncRNAs, antisense lncRNAs, intergenic lncRNAs, intronic lncRNAs, enhancer lncRNAs and bidirectional lncRNAs [23]. In addition to linear ncRNAs, nonlinear ncRNAs, called circular RNAs (circRNAs), has been identified; circRNAs can be classified into three categories depending on their source: intronic circRNAs (circular intronic RNAs, ciRNAs), exonic circRNAs (exonic circular RNAs, ecRNAs), and exonic and intronic circRNAs (exon_intron circular RNAs, EIciRNAs) [24,25,26]. ncRNAs can function either alone or with other ncRNAs by acting as competitive endogenous RNAs (ceRNAs) to sponge miRNAs, which prevents them from interacting with target genes or proteins. In recent years, a large number of studies have demonstrated that both ncRNAs and ferroptosis are involved in the occurrence and progression of various CVDs and that ncRNAs regulate ferroptosis through key factors, such as SLC7A11, TFR, GPX4 and ACSL4. However, further analysis is needed to identify the pathophysiological mechanisms of CVDs that are affected by the regulatory actions of ncRNAs on ferroptosis.
In this review, we summarize the ferroptosis-related signaling pathways and discuss recent developments related to and perspectives on the role of ncRNA-regulated ferroptosis in CVD pathophysiology to identify potential therapeutic strategies for CVDs.
Ferroptosis signaling pathways and their roles in CVDs
In recent years, significant achievements have been made in elucidating the molecular mechanism of ferroptosis. Ferroptosis is defined as a newly discovered form of RCD that involves various processes and metabolic pathways, including iron homeostasis, amino acid, lipid metabolism and the antioxidant system (Fig. 1). However, the regulatory mechanisms of ferroptosis are intricate. Accumulating experimental evidence indicates that ferroptosis has a vital role in the pathogenesis of various CVDs, including atherosclerosis, MI, I/R, AF, cardiomyopathy, cardiac hypertrophy and HF [27]. Studies have shown that ferroptosis contributes to the occurrence and development of CVDs by impairing the structure and function of the heart and blood vessels and disrupting their normal function [28]. However, the precise underlying mechanisms of various CVDs are not completely clear. Fully elucidating the association of ferroptosis with CVD pathogenesis will provide novel insights for developing effective therapeutic strategies for patients with CVDs.
Molecular signaling mechanisms and pathways involved in ferroptosis. Different physiological processes and pathological stresses may trigger ferroptosis. Abnormal iron metabolism, excess ROS production and excessive accumulation of lipid peroxide are important factors that induce ferroptosis. Abbreviations: DcytB: duodenal cytochrome B reductase; EPO: erythropoietin; GSSG: glutathione disulfide; iFSP: inhibitor of FSP1; L-OOH: lipid peroxide; L-OH: lipid alcohol; and NADPH: nicotinamide adenine dinucleotide phosphate
Iron metabolism and homeostasis
Iron is an essential trace element in the human body due to its participation in the synthesis of many proteins and enzymes [29]. Iron is stored in hemoglobin (72%), myoglobin (3%), and other compounds (0.2%), reserve iron (25%) is stored in ferritin in the liver, spleen and bone marrow [30]. Iron is involved in various metabolic processes and life activities, and it is an indispensable cofactor for certain enzymes required for oxygen transport, cell respiration and electron transfer, energy metabolism, DNA synthesis and immune regulation [31, 32]. The complex and precise mechanisms of iron homeostasis regulation ensure that the iron concentration in a cell remains stable and prevent intracellular iron overload from triggering the Fenton reaction, which in turn leads to ferroptosis [13] (Fig. 1A). The main source of iron in the body is hemoglobin, and iron is recovered from hemoglobin by macrophages that phagocytose senescent red blood cells. Simultaneously, the duodenum absorbs dietary iron ions in the human body. However, chronic inflammation and HF-related generalized edema reduce iron absorption in gastrointestinal system and macrophage phagocytosis of red blood cells, resulting in functional iron deficiency which is associated with HF, cerebrovascular diseases, AF and pulmonary hypertension [33]. The effects of iron supplementation have been evaluated in patients with HF, and it has been reported that iron supplementation can improve quality of life and reduce hospitalization [34].
Iron obtained through these two pathways is transported in the plasma by ferroportin (FPN), also known as SLC40A1, which is widely distributed on the surface of duodenal epithelial cells, macrophages and hepatocytes. FPN function is regulated by hepcidin, a 25-amino acid liver -secreted peptide hormone that binds to FPN to promote FPN internalization and degradation when the iron concentration is high [30, 35]. However, overexpression of miR-124 inhibits the expression of FPN, leading to intracellular iron accumulation and triggering ferroptosis [36]. Bao and colleagues [37] showed that cigarette tar caused severe iron overload and lipid peroxidation, upregulated hepcidin expression and downregulated FPN and SLC7A11 in macrophages, resulting in the promotion of atherosclerosis progression. These regulatory changes can be reversed by ferroptosis inhibitors or hepcidin knockdown, while NF-κB inhibitors have the opposite effect and then inhibit macrophage ferroptosis.
The iron metabolism pathway is necessary for the intracellular accumulation of lipid peroxides and ferroptosis. Ferrous iron (Fe2+) in the extracellular space can be oxidized into ferric iron (Fe3+) by ceruloplasmin or hephaestin on the basolateral side of a cell, and Fe3+ is endocytosed into the cell by binding to transferrin (TF) and the membrane protein TF receptor 1 (TFR1) [38]. Within a cell, Fe3+ is located in endosomes and then reduced to Fe2+ by the iron oxide reductase six-transmembrane epithelial antigen of prostate 3 (STEAP3) and ultimately transported from endosomes to the cytosol by divalent metal transporter 1 (DMT1). Intracellular Fe2+ is stored in unstable labile iron pools (LIPs), and iron stored in ferritin is reduced to Fe2+ and consumed during the synthesis of iron-dependent enzymes [39]. Moreover, iron input is increased by iron transporter 1 (FPN1), poly copper-iron oxidase (e.g., ceruloplasmin) and ion transporter lipocalin 2 (LCN2). Once the balance between iron absorption, utilization and recycling is disrupted, cells can undergo iron overload. Iron in unstable LIPs, especially that obtained by the ferrous iron-induced Fenton reaction in the presence of hydrogen peroxide (H2O2), contributes to lipid peroxidation and ROS generation, ultimately triggering ferroptosis.
Recent studies have shown that multiple regulators of iron metabolism are involved in ferroptosis. For example, nuclear receptor coactivator 4 (NCOA4), a cargo receptor involved in ferritin autophagy, maintains intracellular and systemic iron homeostasis by delivering ferritin to lysosomes and degrading ferritin via selective cargo-mediated autophagy (a specific form of autophagy called ferritinophagy). Inhibition of ferritinophagy or knockdown of NCOA4 effectively ameliorates cellular or mitochondrial iron overload, lipid peroxide production and ROS accumulation, which protects cardiomyocytes from ferritinophagy-mediated ferroptosis and alleviates myocardial inflammation and fibrosis [40,41,42]. Heat shock protein beta 1 (HSPB1), a member of the small heat shock protein family, acts as a negative regulator of ferroptosis by inhibiting iron intake and the production of lipids. HSPB1 phosphorylation, regulated by protein kinase C, reduces the rate of iron-dependent production of lipid ROS to resist ferroptosis [43]. Emerging evidence indicates that overexpression of HSBP1 can accelerate recovery from tachypacing-induced structural damage and contractile dysfunction in HL-1 cardiomyocytes. Furthermore, HSBP1 can shield myofibrils from degradation by binding to them and stabilize sarcomeric proteins, indicating that HSBP1 induction is a potential target to reverse AF-induced cardiac remodeling [44]. In contrast, iron regulatory protein (IRP) and hypoxia-inducible factor-1 (HIF-1) increase cellular iron uptake by elevating TFR1 expression, thereby increasing cell sensitivity to ferroptosis [45,46,47]. Heme oxygenase 1 (Hmox1) is an essential enzyme in heme catabolism. Mechanistically, upregulation of Hmox1 promotes heme degradation and the release of free iron, and free iron accumulates in mitochondria and triggers lipid peroxidation, ultimately resulting in ferroptosis and myocardial injury in the presence of doxorubicin (DOX) [48, 49].
However, in recent years, a series of key regulators that pharmacologically inhibit ferroptosis have been identified. Most ferroptosis inhibitors include iron chelators and lipophilic RTAs. Iron chelators, such as deferoxamine (DFO), dexrazoxane (DXZ), deferiprone and ciclopirox, can reduce labile iron levels and block the Fenton chain reaction, thereby preventing the activation and spreading of lipid peroxidation to protect against ferroptosis [50, 51]. DXZ is the only FDA-approved drug for preventing DOX-induced cardiotoxicity in patients with cancer; DXZ can cross the cell membrane, directly enter mitochondria in cardiomyocytes and chelate intracellular free iron [52, 53].
GSH metabolism
Glutathione peroxidases (GPxs) plays a predominant role in a variety of human diseases by decreasing hydroperoxide levels. A substantial body of evidence has shown that the GPx family consists of eight members: cytosolic GPX (cGPX, GPX1), plasma GPX (pGPX, GPX3), gastrointestinal GPx (GI‐GPx, GPX2), GPX6, and phospholipid hydroperoxide GPx (PHGPX, GPX4) [54, 55]. GPX4, a monomeric protein, is expressed as three isoforms: cytosolic (cGPX4), mitochondrial (mGPX4) and sperm nuclear GPX4 (snGPX4) [56,57,58]. GPX4 plays an indispensable role in maintaining membrane lipid homeostasis by preventing excess accumulation of toxic lipid peroxides and the formation of free radicals, thereby attenuating ferroptosis (Fig. 1B). Notably, these outcomes can be driven by the direct inhibition of GPX4 and by inhibition of glutathione (GSH) synthesis which involves cysteine, glutamate and glycine and proceeds in two steps. System Xc−, a cystine-glutamate transport receptor, is composed of two proteins, 12 channel transmembrane protein transporter solute vector family 7 member 11 (SLC7A11) and single-channel transmembrane regulatory protein solute vector family 3 members 2 (SLC3A2), which are expressed on the cell membrane and capable of maintaining redox homeostasis [59]. Extracellular cystine is exchanged for intracellular glutamate at an equal ratio by System Xc−. Regardless of the pathway, ultimately, an increase in GPX levels reduces the levels of lipid-based ROS, which increase unsaturated fatty acid levels on the cell membrane and ultimately cause liposome peroxidation and ferroptosis. Studies have shown that DOX and sorafenib can decrease the levels of GPX and SLC7A11 and accelerate ferroptosis [60, 61]. As a result, targeting ferroptosis might be a novel therapeutic approach for preventing DOX- or sorafenib-induced cardiotoxicity in the future.
However, the high extracellular concentrations of glutamate and other molecules, such as erastin, sulfoximine, sulfasalazine and sorafenib, deplete intracellular cystine content by suppressing the function of System Xc−, which activates GPX4 by depleting GSH and initiating ferroptosis [62, 63]. Additionally, treating cells with direct inhibitors of GPX4, such as RSL3, ML162, FIN56, DPI 10, DPI12, DPI13 or DPI7, initiates ferroptosis by inactivating GPX4 [62, 64]. Certain synthetic compounds can suppress GPX4 and increase the peroxide level in cardiomyocytes.
Lipid peroxidation
The lipid bilayer of the cell membrane is essential for maintaining membrane function. Cell membranes are composed mainly of lipids, proteins and carbohydrates, polyunsaturated fatty acids (PUFAs) are important components of the cell membrane [65]. The location and content of PUFAs can be used to assess the degree of ferroptosis because this mode of cell death affects the extent of intracellular lipid peroxidation. PUFAs are the lipids most susceptible to peroxidation during ferroptosis. Lipoxygenases and phosphorylase kinase G2 are two key regulators of lipid peroxidation during ferroptosis [66, 67]. PUFA-containing phospholipids (PLs) are the major substrates in ferroptotic lipid peroxidation, and PL hydroperoxides, including phosphatidylcholine, cardiolipin and phosphatidylethanolamine (PE), are involved in ferroptosis [68, 69].
Two key lipid metabolism-associated enzymes, acyl-CoA synthase long-chain family member 4 (ACSL4) and lysophosphatidylcholine acyltransferase 3 (LPCAT3), are involved in the synthesis of PUFA-PLs [70]. ACSL4 catalyzes the binding of PUFAs and adrenergic acid to coenzyme A (CoA) to generate PUFA-CoA, and then LPCAT3 catalyzes the incorporation of PUFAs from PUFA-CoA into membrane PLs to generate PUFA-PLs, resulting in the remodeling of membrane phospholipids and influencing ferroptosis [71]. ACSL4 catalyzes PUFA-CoA formation to influence ferroptosis and is a marker of ferroptotic cell death sensitivity [47, 72, 73]. ACSL4 knockout decreases PUFA-PL generation, decreasing the percentage of cell undergoing RSL3-induced ferroptosis. Knockout of ACSL4 exerts a cardioprotective effect by decreasing iron accumulation, oxidative stress and ferroptosis after myocardial ischemia in rat [74]. In addition, PUFA-PL is oxidized by lipoxygenases (LOXs) or cytochrome P450 oxidoreductase (POR) into the harmful lipid peroxidation products PUFA-PL-OH and PUFA-PL-OOH, respectively, which induce lipid peroxidation and ROS production [75,76,77]. Ferroptosis is activated by cellular lipid hydroperoxides through LOXs and autoxidized peroxyl radicals. Therefore, inhibiting LOX enzyme activity with flavonoids and members of the vitamin E family can reduce cell damage caused by ferroptosis [68]. Moreover, the level of the aforementioned harmful substances can be reduced by GPX4, which converts them into nontoxic lipid alcohols and water. From the opposite point of view, reducing GPX4 levels via GPX4 treatment with inhibitors such as RSL3 can promote the excessive accumulation of peroxide products and thus induce ferroptosis [78, 79] (Fig. 1C).
Other signaling pathways
The FSP1-CoQ-NAD(P)H axis, which protects the myocardium in CVDs, is important in the GSH and GPX4 pathways. CoQ10 is mainly found in two forms, ubiquinone (the oxidized form) and ubiquinol (the reduced form); among these two forms, ubiquinol plays the main role in inhibiting oxidation. CoQ10 is a lipophilic electron carrier that participates in the mitochondrial respiratory chain and is a lipophilic radical scavenger at the plasma membrane [80]. Randomized controlled trials and meta-analyses have suggested that CoQ10 can improve cardiac function by reducing systemic oxidative stress, which is associated with a reduction in hospitalizations and the risk of cardiovascular mortality [81, 82]. Moreover, ferroptosis suppressor protein 1 (FSP1), also known as p53-responsive gene3 (PRG3), binds membranous structures in cells such as the Golgi apparatus, plasma membrane and perinuclear structures. Studies have found that FSP1 is a key component of nonmitochondrial CoQ10 and is recruited to the plasma membrane through the myristoylation of specific N-terminal sequences to capture lipotropic free radicals and exert antioxidant effects [83, 84], thereby mediating NADH-dependent CoQ reduction, suppressing CoQ activity in cells, and eventually inhibiting phospholipid peroxidation and ferroptosis via the FSP1-CoQ-NAD(P)H axis. Ara et al. [85] found that iFSP, an inhibitor of FSP1, can be used to eliminate lung cancer cells and induce ferroptosis. Upregulating FSP1 was found to alleviate septicemia-induced myocardial injury by inhibiting ferroptosis in vivo [86]. The combination of GPX4 and FSP1 serves as a separate defense system to suppress lipid peroxidation in the cytoplasmic and mitochondrial membranes, effectively alleviating CVDs by defending against ferroptosis [87]. CoQ10H2, the product of CoQ10 reduction, suppressed adipocyte differentiation and inhibited lipid ROS accumulation. In summary, elucidating the mechanism by which ferroptosis is regulated may provide new insights for the development of strategies to prevent and treat CVDs.
Noncoding RNAs that regulate ferroptosis in CVDs
To date, some ncRNAs have been found to play potentially critical roles in CVDs by directly or indirectly regulating iron metabolism and ferroptosis-related signaling pathways. Cardiac modeling, manifesting as abnormal deposition of collagen and dysregulated extracellular matrix homeostasis, is a common, persistent and irreversible pathological change associated with CVDs and results in cardiac structural changes, cardiac dysfunction, HF and even sudden death. Therefore, one strategy to prevent adverse cardiac remodeling and consequent cardiovascular events is to go upstream and decrease cardiac cell death. Recent reports suggest that ferroptosis is involved in the initial myocardial cell death caused by MI, I/R injury, AF, cardiac hypertrophy, aortic valve replacement, cardiomyopathy and HF [88]. For instance, inhibition or knockout of xCT can exacerbate cardiomyocyte hypertrophy and angiotensin II (Ang II)-induced cardiac fibrosis in mice and increase the levels of the ferroptosis biomarkers Ptgs2, MDA and ROD, while Fer-1 can alleviate the exacerbation of cardiac hypertrophy caused by inhibiting xCT in rat cells or ablating xCT in mice [89]. In addition, GPX4 also plays an important role in promoting the thrombospondin 1 (TSP1)/autophagy, insulin-like growth factor 1 (IGF1) or stimulator of interferon genes (STING) axis to inhibit cardiac fibrosis and the expression of the associated markers α-SMA, collagen type I (Col I) and Col III [55]. In this section, we describe the pathological roles of ferroptosis-related ncRNAs in CVDs (Tables 1 and 2).
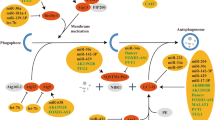
MiRNAs that regulate ferroptosis in CVDs
MiRNAs are a ubiquitous class of endogenous noncoding small RNA molecules, and there are many types of miRNAs in the body. They are generally 18–25 nucleotides in length and bind the 3’ untranslated region (UTR) of target mRNAs to regulate the expression of different genes by interfering with mRNA molecules at the posttranscriptional and translational levels. In recent years, the detailed molecular mechanisms underlying ncRNA-mediated ferroptosis in cancer have been explored [90, 91], but the function of ferroptosis-related miRNAs in CVDs remains largely unknown.
Acute MI (AMI) causes a series of pathological responses in cardiomyocytes, including ischemia, hypoxia, inflammatory reactions and necrosis in the early stage and persistent ventricular remodeling, ischemic cardiomyopathy, HF and even death in the late stage [92, 93]. Early restoration of vascular perfusion, such as through percutaneous coronary intervention (PCI) or thrombolytic therapy, can reduce the number of necrotic cardiomyocytes and the risk of adverse cardiovascular events. However, cardiomyocyte damage and dysfunction persist even after reperfusion of myocardial tissue, and reperfusion inducing myocardial necrosis and the development of cardiac fibrosis; these changes are collectively referred to as I/R injury [94]. Recent studies have revealed that iron homeostasis and miRNAs play indispensable roles in maintaining cardiac structure and function [68, 95, 96]. Either iron deficiency or iron overload can impair cardiac function. Fan et al. [97] verified that inhibition of miR-15a-5p by silencing the transcription factor early growth response-1 (Egr-1) can suppress ferroptosis and alleviate myocardial injury by increasing GPX4 and MDA levels and decreasing the activity of ROS in an AMI mouse model. MiR-23a-3p from the human umbilical cord blood (HUCB)-mesenchymal stem cell (MSC)-derived exosomes targets DMT1 to inhibit ferroptosis and attenuate myocardial injury [98]. Tang et al. [99] confirmed that targeting ATG5 by overexpression of miR-30d effectively inhibits autophagy upregulates FTH1 and GPX4 expression in H9C2 cells, and increases the content of GSH, protecting against ferroptosis-mediated myocardial injury. Furthermore, miR-375-3p expression is significantly upregulated in an I/R rat model, and miR-375-3p targets GPX4-related ferroptosis to promote cardiac fibrosis, which is associated with increased collagen I expression and ROS levels and inhibition of the oxidative scavenging by superoxide dismutase (SOD). However, this process was found to be reversed by a miR-375-3p inhibitor and the ferroptosis inhibitor ferrostatin-1 (Fer-1) [93].
As mentioned above, GPX4 acts as an important mediator of I/R injury in cardiac tissue by regulating ferroptosis and alleviating oxidative damage via the elimination of lipid peroxides from various membranes. Inhibition of miR-1224 and miR-135b-3p can alleviate myocardial injury by targeting GPX4 and suppressing hypoxia/reoxygenation (H/R)-induced oxidative stress [100, 101]. However, increased expression of miR-135b-3p exacerbates myocardial I/R injury in an iron-dependent manner in vitro [101]. Similarly, miR-29b-3p also aggravates cardiomyocyte injury and promotes the secretion of inflammatory cytokines such as TNF-α caused by I/R through targeted downregulation of pentraxin 3 (PTX3) [102]. Additionally, other miRNAs, such as miR-190a-5p, miR-199a-5p, miR-196c-3p and miR-210-3p play critical roles in myocardial I/R injury by regulating ferroptosis-related genes and proteins [103,104,105,106]. In the later stage of MI, MI will cause left ventricular enlargement and cardiac fibrosis progression occur, ultimately leading to HF. Ji et al. [105] found that an miR-196c-3p mimic improves cardiac function by inhibiting the expression of the ferroptosis hub genes NOX4, p53 and LOX in a myocardial I/R injury mouse model. Wang et al. [107] showed that a miR-351 agomir effectively inhibited mixed lineage kinase 3 (MLK3) protein and mRNA expression to regulate JNK/p53 signaling pathway-mediated oxidative stress, which significantly increased the left ventricular ejection fraction (LVEF) and left ventricular fractional shortening (LVFS), decreased the left ventricular end-diastolic diameter (LVEDD), the left ventricular end-systolic diameter (LVESD), LV mass and collagen deposition, improved cardiac function, and inhibited cardiac hypertrophy and fibrosis in the advanced stage of congestive heart failure (CHF).
AF, mainly characterized by persistent biventricular enlargement and cardiac diastolic dysfunction, is the most common arrhythmia. Recent reports have revealed that ncRNAs play significant roles in the pathophysiological mechanism of AF [108,109,110]. However, the molecular mechanisms underlying AF and ferroptosis remain to be fully elucidated. Liu et al. [111] suggested that inhibition of cardiac fibroblast-derived exon-miR-23a-3p upregulates SLC7A11 and protects H9C2 cardiomyocytes from ferroptosis, preventing persistent AF development. In addition, miR-143-3p overexpression in AF cardiomyocytes was found to increase cell proliferation and viability, inhibit lipid ROS production and mitochondrial superoxide formation and reduce the intracellular concentrations of total iron and Fe2+ by inhibiting glutamic-oxaloacetic transaminase 1 (GOT1)-mediated oxidative damage and cardiac ferroptosis [112]. As indicated above, miRNAs play key roles in CVDs by regulating ferroptosis-related signaling pathways, as shown in Table 1.
LncRNAs that regulate ferroptosis in CVDs
LncRNAs are transcripts exceeding 200 nucleotides in length that regulate different cellular pathways and the expression of genes by binding to DNA, mRNA, miRNA and protein. LncRNAs play important roles in regulating physiological and pathological processes in multiple CVDs mainly through cis- or trans-regulation of chromosome structure, translation, alternative splicing at the transcriptional and posttranscriptional levels, and mRNA transport, stability and translation [113]. Based on the current research evidence, we believe that lncRNAs play vital roles in CVDs, especially MI, by acting as ceRNAs and mediating cardiomyocyte ferroptosis (Table 2). For instance, silencing lncAABR07025387.1 can attenuate myocardial I/R injury by increasing cardiomyocyte activity and decreasing lipid ROS, Fe2+, ACSL4 and LPCAT3 levels, which can suppress ACSL4-mediated ferroptosis. In addition, lncAABR07025387.1 serves as a ceRNA to sponge miR-205 which directly targets ACSL4. Moreover, downregulation of miR-205 efficiently reverses the inhibition of ACSL4-mediated ferroptosis [114]. Zhang and colleagues found that the exo-lncRNA Mir9-3hg binds and downregulates pumilio RNA-binding family member 2 (Pum2). Pum2 is ribonucleic acid-binding protein (RBP) that inhibits peroxiredoxin 6 (PRDX6) protein expression by binding to the PRDX6 promoter region, so its downregulation facilitates cell proliferation, increases the GSH content, and reduces the iron ion concentrations, ROS levels and ferroptosis marker protein levels in H/R-treated HL-1 cells and the myocardial tissue of I/R model mice, ultimately attenuating I/R-induced cardiac injury by inhibiting cardiomyocyte ferroptosis [115]. Gao et al. [116] confirmed that overexpression of lncRNA Gm47283 significantly increases Ptgs2 expression and the levels of ROS and MDA and inhibits GPX4 expression. They also demonstrated that a stem cell membrane-coated short interfering RNA (siRNA) targeting the lncRNA Gm47283 increased miR-706 expression in the advanced phase, suppressing Ptgs2 expression to reduce lipid peroxide toxicity and attenuating myocardial injury by inhibiting cardiomyocyte ferroptosis.
Patients with diabetes are vulnerable to a series of cardiovascular complications, including cardiomyocytes dysfunction and left ventricular longitudinal dysfunction. Ni and team found that inhibiting the lncRNA ZFAS1 attenuates diabetic cardiomyopathy (DCM) progression via sponging of miR-150-5p to activate cyclin D2 (CCND2), which leads to reduced collagen deposition and inhibiting of cardiomyocyte apoptosis and ferroptosis. Moreover, overexpression of miR-150-5p and CCND2 can improve cardiac function by significantly increasing the LVEF and LVFS and decreasing the LVEDD and LVESD [117]. Cardiac hypertrophy is a common maladaptive characteristic of multiple types of advanced CVDs, including coronary heart disease, valvular heart disease and myocarditis. An increasing number of studies have shown that lncRNAs can inhibit cardiac fibrosis and are potential biomarkers and novel therapeutic targets because they regulate the proliferation and transformation of cardiac fibroblasts [110, 118, 119]. Shi and colleagues found that forced expression of the lncRNA AABR07017145.1 induces MMP9/TIMP1 imbalance, which leads to ferroptosis of cardiac microvascular endothelial cells (CMECs) mediated by activation of TFR-1 and increased Fe2+ levels in a rat model of cardiac hypertrophy. However, miR-30b-5p, which was found to be significantly downregulated in a rat model and to target TIMP1, was shown to suppress the effect of the lncRNA AAB on ferroptosis. Additionally, further research demonstrated that silencing the lncRNA AAB and overexpressing miR-30b-5p are novel therapeutic strategies for cardiac hypertrophy [120].
Ferroptosis also plays a critical role in doxorubicin (DOX)-induced cardiomyopathy. Zhuang et al. [121] reported that DOX induces cardiomyocyte ferroptosis by activating the METL14/lncRNA KCNQ1OT1 signaling pathway and inhibiting miR-7-5p expression, which leads to an increase in TF levels, promoting iron absorption and lipid ROS production. Currently, cardiopulmonary bypass, coronary artery bypass grafting, cardiac valve replacement and heart transplantation are the main treatments for many complex CVDs, such as cardiac tumors. Cardiac injury during surgery is mainly associated with the stress response, hemodynamic instability and I/R-induced injury [122] and previous studies have shown that lncRNAs play functional roles in the injury process [123,124,125]. Overexpression of lncRNA SEMA5A-1T1 protects cardiomyocytes from H/R injury and against ferroptosis by sponging miR-143-3p to upregulate the expression of B-cell CLL/lymphoma 2 (BCL2) and SLC7A11 [126].
CircRNAs that regulate ferroptosis in CVDs
As newly discovered critical ncRNAs, circRNAs, considered secondary products of canonical linear mRNA splicing, have been increasingly reported to participate in fundamental pathological and physiological processes in CVDs. Depending on their mode of biogenesis, circRNAs can be classified into three types, i.e., ciRNAs, ecRNAs and EIciRNAs [25, 26], and the biological functions of circRNAs have been gradually revealed. For example, circRNAs contain multiple binding sites for individual or multiple miRNAs to target other RNAs. They also interact with RNA-binding proteins and play roles in the assembly of scaffold components, splicing, gene transcription regulation and the translation of miRNAs into proteins or peptides.
In recent years, circRNAs have become a popular topic in biological research since they are highly conserved, show stable and specific expression in tissues and cells, can act as endogenous sponges to bind miRNAs and show regulatory capacity [131]. Through in-depth exploration of the molecular mechanisms underlying the effects of circRNAs on ferroptosis, researchers have confirmed their roles as potential molecular biomarkers and novel targets for the diagnosis and treatment of CVDs. For example, in an MI mouse model and hypoxia-treated cardiomyocytes, circRNA1615 and lipoprotein receptor-related protein 6 (LRP6) expression is significantly downregulated, while miR-152-3p expression is increased. A previous study showed that cardiac LRP6 is downregulated in patients with dilated cardiomyopathy, and cardiomyocyte-specific depletion of LRP6 causes lethal dilated cardiomyopathy, such as acute HF and cardiac dysfunction, resulting from the suppression of autophagy-mediated degradation and fatty acid utilization through Drp1/mTOR/TFEB signaling [127, 132]. Further research confirmed that siR-LRP6 increases the expression of the autophagy-regulated proteins LC3-A/B and ATG5 and decreases p62 expression. That is LRP6 plays a critical role in CVDs. Mechanistically, circRNA1615 sponges miR-152-3p to prevent LRP6-mediated autophagy-related ferroptosis in cardiomyopathy [127].
It has been reported that iron overload can impair heart function by increasing ROS levels via the Fenton reaction, which directly affects cardiac mitochondrial dynamics and promotes cardiac mitochondrial damage. Zheng et al. [128] found that the iron content in an HF mouse model was noticeably increased compared to that in the sham group, and decreased expression of GPX4 and increased expression of NOX1, ACSL4 and MDA indicated the occurrence of lipid peroxidation during HF. More importantly, FTH1 expression was markedly downregulated, and low circSnx12 expression and high miR-224-5p expression caused cardiac cell death by downregulating FTH1 and directly regulating iron overload in cardiomyocytes. However, in a mouse model of I/R, circ FEACR overexpression protected cardiomyocytes from I/R-induced ferroptosis by decreasing the levels of SLC7A11, GPX4, and MDA and lipid ROS production [129]. Mechanistically, FEACR directly binds to nicotinamide phosphoribosyltransferase (NAMPT) to increase NAMPT-dependent Sirtuin1 (Sirt1), which promotes the transcriptional activity of forkhead box protein O1 (FOXO1), which can upregulate FTH1, leading to the amelioration of MI and improvements cardiac function by inhibiting ferroptosis [129].
Maladaptive cardiac remodeling is an important determinant of morbidity and mortality that significantly affects life expectancy and quality of life. Knocking down circCmass1 was shown to decrease Ang II-induced neonatal cardiomyocyte hypertrophy in vitro and pressure overload-induced cardiac hypertrophy in TAC mice via the EIF4A3/TFR1 signaling axis to regulate ferroptosis [130] (Table 2). Notably, research on the role of ferroptosis-related circRNAs in CVDs is still lacking. Most of the recently published studies focus on cancer and cells [133]. Therefore, animal research clinical trials on CVDs are needed to ensure the safety and efficacy of the candidate molecules and methods.
Conclusions and perspectives
CVDs represent a global health problem and have high rates of morbidity, mortality and disability. An understanding of how cardiomyocyte damage is involved in the pathology of CVDs and new viable therapeutic strategies are needed. On the role of ferroptosis in CVDs has attracted the attention of researchers. Recently accumulating evidence has revealed that various physiological processes and pathological stresses can trigger ferroptosis in humans and animals. Among these processes and stress, abnormal iron metabolism, amino acid metabolism, ROS production and excessive accumulation of lipid peroxides are critical ferroptosis inducers. However, research on ferroptosis is still in the initial stages, and many unanswered questions remain and need to be urgently answered.
First, there are multiple published studies on ferroptosis based on animal and cellular models, but experimental verification in vivo is lacking since it is difficult to accurately detect ferroptosis progression. However, recent studies have shown that we can detect morphological changes in ferroptotic cells at the subcellular level, including by analyzing plasma membranes, mitochondrial viscosity and the dynamic structure of nucleic acids during ferroptosis through probes, transmission electron microscopy and nucleic acid-responsive carbon dots [134]. And ferroptosis-related molecules, such as labile Fe (II), lipid peroxides, ROS, GSH and TFR1 can be detected through fluorescence probe, quantitative polymerase chain reaction, western blotting and flow cytometry [135, 136]. In clinical practice, positron emission tomography (PET) imaging can provide quantitative, three-dimensional images for in vivo assessment of labile Fe(II) ions levels [134], and cardiac magnetic resonance (CMR) combined with a processing workstation (Cvi42) can be used to analyze iron levels, cardiac structure and function, and the degree of fibrosis through the techniques of late gadolinium enhancement (LGE) and T1 and T2 mapping [137]. Moreover, the molecular mechanisms underlying ferroptosis and ferroptosis biomarkers remain to be identified. Clinical ferroptosis-related biomarkers for diagnosing CVDs and predicting the prognosis of CVDs patients have not yet been discovered. Finally, inhibitors of ferroptosis, such as Fer-1 and RSL3, have been proposed to effectively ameliorate cardiomyocyte injury, but their targets, the mechansims underlying their effects, their potential toxicity to untargeted organs and their feasibility for use in clinical settings remain unclear.
In recent years, ncRNAs have been shown to be important regulators of CVDs and to be involved in the life cycle of cardiomyocytes by affecting their differentiation, transcription and apoptosis rate. Additionally, the use of ncRNAs as biomarkers has increased due to their specificity, accessibility, stability and other distinguishing features. Specifically, ncRNAs crosslink ferroptosis and CVD markers, which helps in monitoring and interfering with ferroptosis-related CVDs. Through more in-depth research and the rapid development of bioinformatics technologies, the role of ferroptosis-associated ncRNAs in CVDs will be further elucidated in the future, and more databases will be established as integrated analysis platforms for researchers to study ferroptosis [138,139,140]. However, the role of ncRNA-mediated ferroptosis in CVDs and the mechanisms underlying pathophysiology of CVD remain to be further elucidated. Fewer ferroptosis-related studies have focused on lncRNAs and circRNAs than on miRNAs. In addition, cardiac fibrosis is a common pathological feature of various CVDs that results in cardiac systolic and diastolic dysfunction, conduction abnormalities and reduced patient compliance, ultimately leading to arrhythmias and HF. Sufficient evidence has indicated that ncRNAs are differentially expressed in myocardial fibrosis [141, 142], but further confirmation of these findings is need to identify the signaling pathways that ameliorate cardiac remodeling via ferroptosis and the potential roles of other pathways [93, 143]. Therefore, identifying ferroptosis-related ncRNAs involved in cardiac fibrosis may aid in preventing and treating of CVDs and predicting the prognosis of CVD patients.
In conclusion, both ferroptosis and ncRNAs play pivotal roles in the occurrence and development of numerous CVDs, but the underlying molecular mechanisms of ncRNA-induced ferroptosis in cardiomyocytes remain to be fully elucidated. As basic and clinical research on the molecular mechanisms of ferroptosis and interventions for inhibiting ferroptosis is being conducted, we believe that effective therapeutic strategies for CVDs are forthcoming.
Data availability
Not applicable.
References
Perk J, De Backer G, Gohlke H, Graham I, Reiner Z, Verschuren M, Albus C, Benlian P, Boysen G, Cifkova R et al (2012) European Guidelines on cardiovascular disease prevention in clinical practice (version 2012). The fifth joint task force of the european society of cardiology and other societies on cardiovascular disease prevention in clinical practice (constituted by representatives of nine societies and by invited experts). Eur Heart J 33:1635–1701. https://doi.org/10.1093/eurheartj/ehs092
Tsao CW, Aday AW, Almarzooq ZI, Alonso A, Beaton AZ, Bittencourt MS, Boehme AK, Buxton AE, Carson AP, Commodore-Mensah Y et al (2022) Heart disease and stroke statistics-2022 update: a report from the american heart association. Circulation 145:e153–e639. https://doi.org/10.1161/cir.0000000000001052
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, Himmelfarb CD, Khera A, Lloyd-Jones D, McEvoy JW et al (2019) 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the american college of cardiology/american heart association task force on clinical practice guidelines. Circulation 140:e596–e646. https://doi.org/10.1161/cir.0000000000000678
Del Re DP, Amgalan D, Linkermann A, Liu Q, Kitsis RN (2019) Fundamental mechanisms of regulated cell death and implications for heart disease. Physiol Rev 99:1765–1817. https://doi.org/10.1152/physrev.00022.2018
Patel P, Karch J (2020) Regulation of cell death in the cardiovascular system. Int Rev Cell Mol Biol 353:153–209. https://doi.org/10.1016/bs.ircmb.2019.11.005
Tang D, Kang R, Berghe TV, Vandenabeele P, Kroemer G (2019) The molecular machinery of regulated cell death. Cell Res 29:347–364. https://doi.org/10.1038/s41422-019-0164-5
Green DR (2019) The coming decade of cell death research: five riddles. Cell 177:1094–1107. https://doi.org/10.1016/j.cell.2019.04.024
Wang Y, Zhang L, Zhou F (2022) Cuproptosis: a new form of programmed cell death. Cell Mol Immunol 19:867–868. https://doi.org/10.1038/s41423-022-00866-1
Tsvetkov P, Coy S, Petrova B, Dreishpoon M, Verma A, Abdusamad M, Rossen J, Joesch-Cohen L, Humeidi R, Spangler RD et al (2022) Copper induces cell death by targeting lipoylated TCA cycle proteins. Science 375:1254–1261. https://doi.org/10.1126/science.abf0529
Yan WT, Zhao WJ, Hu XM, Ban XX, Ning WY, Wan H, Zhang Q, Xiong K (2023) PANoptosis-like cell death in ischemia/reperfusion injury of retinal neurons. Neural Regen Res 18:357–363. https://doi.org/10.4103/1673-5374.346545
Christgen S, Tweedell RE, Kanneganti TD (2022) Programming inflammatory cell death for therapy. Pharmacol Ther 232:108010. https://doi.org/10.1016/j.pharmthera.2021.108010
Dixon SJ, Lemberg KM, Lamprecht MR, Skouta R, Zaitsev EM, Gleason CE, Patel DN, Bauer AJ, Cantley AM, Yang WS et al (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149:1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Leng Y, Luo X, Yu J, Jia H, Yu B (2021) Ferroptosis: A potential target in cardiovascular disease. Front Cell Dev Biol 9:813668. https://doi.org/10.3389/fcell.2021.813668
Fang X, Ardehali H, Min J, Wang F (2022) The molecular and metabolic landscape of iron and ferroptosis in cardiovascular disease. Nat Rev Cardiol. https://doi.org/10.1038/s41569-022-00735-4
Ratan RR (2020) The chemical biology of ferroptosis in the central nervous system. Cell Chem Biol 27:479–498. https://doi.org/10.1016/j.chembiol.2020.03.007
Lei G, Zhuang L, Gan B (2022) Targeting ferroptosis as a vulnerability in cancer. Nat Rev Cancer 22:381–396. https://doi.org/10.1038/s41568-022-00459-0
Ni L, Yuan C, Wu X (2022) Targeting ferroptosis in acute kidney injury. Cell Death Dis 13:182. https://doi.org/10.1038/s41419-022-04628-9
Chen J, Li X, Ge C, Min J, Wang F (2022) The multifaceted role of ferroptosis in liver disease. Cell Death Differ 29:467–480. https://doi.org/10.1038/s41418-022-00941-0
Li X, Ma N, Xu J, Zhang Y, Yang P, Su X, Xing Y, An N, Yang F, Zhang G et al (2021) Targeting ferroptosis: pathological mechanism and treatment of ischemia-reperfusion injury. Oxid Med Cell Longev 2021:1587922. https://doi.org/10.1155/2021/1587922
Hwang JW, Park JH, Park BW, Kim H, Kim JJ, Sim WS, Mishchenko NP, Fedoreyev SA, Vasileva EA, Ban K et al (2021) Histochrome attenuates myocardial ischemia-reperfusion injury by inhibiting ferroptosis-induced cardiomyocyte death. Antioxidants (Basel). https://doi.org/10.3390/antiox10101624
Henshall DC, Hamer HM, Pasterkamp RJ, Goldstein DB, Kjems J, Prehn JHM, Schorge S, Lamottke K, Rosenow F (2016) MicroRNAs in epilepsy: pathophysiology and clinical utility. Lancet Neurol 15:1368–1376. https://doi.org/10.1016/s1474-4422(16)30246-0
Beermann J, Piccoli MT, Viereck J, Thum T (2016) Non-coding RNAs in development and disease: background, mechanisms, and therapeutic approaches. Physiol Rev 96:1297–1325. https://doi.org/10.1152/physrev.00041.2015
Zhu L, Li N, Sun L, Zheng D, Shao G (2021) Non-coding RNAs: the key detectors and regulators in cardiovascular disease. Genomics 113:1233–1246. https://doi.org/10.1016/j.ygeno.2020.10.024
Yousefi F, Soltani BM (2021) Circular RNAs as potential theranostics in the cardiac fibrosis. Heart Fail Rev 26:195–203. https://doi.org/10.1007/s10741-019-09908-9
Li Z, Huang C, Bao C, Chen L, Lin M, Wang X, Zhong G, Yu B, Hu W, Dai L et al (2015) Exon-intron circular RNAs regulate transcription in the nucleus. Nat Struct Mol Biol 22:256–264. https://doi.org/10.1038/nsmb.2959
Zhang Y, Zhang XO, Chen T, Xiang JF, Yin QF, Xing YH, Zhu S, Yang L, Chen LL (2013) Circular intronic long noncoding RNAs. Mol Cell 51:792–806. https://doi.org/10.1016/j.molcel.2013.08.017
Fang X, Ardehali H, Min J, Wang F (2023) The molecular and metabolic landscape of iron and ferroptosis in cardiovascular disease. Nat Rev Cardiol 20:7–23. https://doi.org/10.1038/s41569-022-00735-4
Liu Y, Ding W, Wang J, Ao X, Xue J (2023) Non-coding RNA-mediated modulation of ferroptosis in cardiovascular diseases. Biomed Pharmacother 164:114993. https://doi.org/10.1016/j.biopha.2023.114993
Ward DM, Cloonan SM (2019) Mitochondrial iron in human health and disease. Annu Rev Physiol 81:453–482. https://doi.org/10.1146/annurev-physiol-020518-114742
Ravingerová T, Kindernay L, Barteková M, Ferko M, Adameová A, Zohdi V, Bernátová I, Ferenczyová K, Lazou A (2020) The molecular mechanisms of iron metabolism and its role in cardiac dysfunction and cardioprotection. Int J Mol Sci. https://doi.org/10.3390/ijms21217889
Stoyanovsky DA, Tyurina YY, Shrivastava I, Bahar I, Tyurin VA, Protchenko O, Jadhav S, Bolevich SB, Kozlov AV, Vladimirov YA et al (2019) Iron catalysis of lipid peroxidation in ferroptosis: regulated enzymatic or random free radical reaction? Free Radic Biol Med 133:153–161. https://doi.org/10.1016/j.freeradbiomed.2018.09.008
Hirota K (2019) An intimate crosstalk between iron homeostasis and oxygen metabolism regulated by the hypoxia-inducible factors (HIFs). Free Radic Biol Med 133:118–129. https://doi.org/10.1016/j.freeradbiomed.2018.07.018
Savarese G, von Haehling S, Butler J, Cleland JGF, Ponikowski P, Anker SD (2023) Iron deficiency and cardiovascular disease. Eur Heart J 44:14–27. https://doi.org/10.1093/eurheartj/ehac569
Sawicki KT, De Jesus A, Ardehali H (2023) Iron metabolism in cardiovascular disease: physiology, mechanisms, and therapeutic targets. Circ Res 132:379–396. https://doi.org/10.1161/circresaha.122.321667
Billesbølle CB, Azumaya CM, Kretsch RC, Powers AS, Gonen S, Schneider S, Arvedson T, Dror RO, Cheng Y, Manglik A (2020) Structure of hepcidin-bound ferroportin reveals iron homeostatic mechanisms. Nature 586:807–811. https://doi.org/10.1038/s41586-020-2668-z
Bao WD, Zhou XT, Zhou LT, Wang F, Yin X, Lu Y, Zhu LQ, Liu D (2020) Targeting miR-124/Ferroportin signaling ameliorated neuronal cell death through inhibiting apoptosis and ferroptosis in aged intracerebral hemorrhage murine model. Aging Cell 19:e13235. https://doi.org/10.1111/acel.13235
Bao X, Luo X, Bai X, Lv Y, Weng X, Zhang S, Leng Y, Huang J, Dai X, Wang Y et al (2023) Cigarette tar mediates macrophage ferroptosis in atherosclerosis through the hepcidin/FPN/SLC7A11 signaling pathway. Free Radic Biol Med 201:76–88. https://doi.org/10.1016/j.freeradbiomed.2023.03.006
Zheng J, Conrad M (2020) The metabolic underpinnings of ferroptosis. Cell Metab 32:920–937. https://doi.org/10.1016/j.cmet.2020.10.011
Bogdan AR, Miyazawa M, Hashimoto K, Tsuji Y (2016) Regulators of iron homeostasis: new players in metabolism, cell death, and disease. Trends Biochem Sci 41:274–286. https://doi.org/10.1016/j.tibs.2015.11.012
Gao M, Monian P, Pan Q, Zhang W, Xiang J, Jiang X (2016) Ferroptosis is an autophagic cell death process. Cell Res 26:1021–1032. https://doi.org/10.1038/cr.2016.95
Hou W, Xie Y, Song X, Sun X, Lotze MT, Zeh HJ 3rd, Kang R, Tang D (2016) Autophagy promotes ferroptosis by degradation of ferritin. Autophagy 12:1425–1428. https://doi.org/10.1080/15548627.2016.1187366
Zhu M, Peng L, Huo S, Peng D, Gou J, Shi W, Tao J, Jiang T, Jiang Y, Wang Q et al (2023) STAT3 signaling promotes cardiac injury by upregulating NCOA4-mediated ferritinophagy and ferroptosis in high-fat-diet fed mice. Free Radic Biol Med 201:111–125. https://doi.org/10.1016/j.freeradbiomed.2023.03.003
Sun X, Ou Z, Xie M, Kang R, Fan Y, Niu X, Wang H, Cao L, Tang D (2015) HSPB1 as a novel regulator of ferroptotic cancer cell death. Oncogene 34:5617–5625. https://doi.org/10.1038/onc.2015.32
van Wijk SW, Ramos KS, Brundel B (2021) Cardioprotective role of heat shock proteins in atrial fibrillation: From mechanism of action to therapeutic and diagnostic target. Int J Mol Sci. https://doi.org/10.3390/ijms22010442
Zhang T, Sun L, Hao Y, Suo C, Shen S, Wei H, Ma W, Zhang P, Wang T, Gu X et al (2022) ENO1 suppresses cancer cell ferroptosis by degrading the mRNA of iron regulatory protein 1. Nat Cancer 3:75–89. https://doi.org/10.1038/s43018-021-00299-1
Yuan S, Wei C, Liu G, Zhang L, Li J, Li L, Cai S, Fang L (2022) Sorafenib attenuates liver fibrosis by triggering hepatic stellate cell ferroptosis via HIF-1α/SLC7A11 pathway. Cell Prolif 55:e13158. https://doi.org/10.1111/cpr.13158
Zhang Y, Xin L, Xiang M, Shang C, Wang Y, Wang Y, Cui X, Lu Y (2022) The molecular mechanisms of ferroptosis and its role in cardiovascular disease. Biomed Pharmacother 145:112423. https://doi.org/10.1016/j.biopha.2021.112423
Fang X, Wang H, Han D, Xie E, Yang X, Wei J, Gu S, Gao F, Zhu N, Yin X et al (2019) Ferroptosis as a target for protection against cardiomyopathy. Proc Natl Acad Sci USA 116:2672–2680. https://doi.org/10.1073/pnas.1821022116
Conrad M, Proneth B (2019) Broken hearts: Iron overload, ferroptosis and cardiomyopathy. Cell Res 29:263–264. https://doi.org/10.1038/s41422-019-0150-y
Li N, Wang W, Zhou H, Wu Q, Duan M, Liu C, Wu H, Deng W, Shen D, Tang Q (2020) Ferritinophagy-mediated ferroptosis is involved in sepsis-induced cardiac injury. Free Radic Biol Med 160:303–318. https://doi.org/10.1016/j.freeradbiomed.2020.08.009
Li N, Jiang W, Wang W, Xiong R, Wu X, Geng Q (2021) Ferroptosis and its emerging roles in cardiovascular diseases. Pharmacol Res 166:105466. https://doi.org/10.1016/j.phrs.2021.105466
Ichikawa Y, Ghanefar M, Bayeva M, Wu R, Khechaduri A, Naga Prasad SV, Mutharasan RK, Naik TJ, Ardehali H (2014) Cardiotoxicity of doxorubicin is mediated through mitochondrial iron accumulation. J Clin Invest 124:617–630. https://doi.org/10.1172/jci72931
Gammella E, Maccarinelli F, Buratti P, Recalcati S, Cairo G (2014) The role of iron in anthracycline cardiotoxicity. Front Pharmacol 5:25. https://doi.org/10.3389/fphar.2014.00025
Agassandian M, Tedrow JR, Sembrat J, Kass DJ, Zhang Y, Goncharova EA, Kaminski N, Mallampalli RK, Vuga LJ (2015) VCAM-1 is a TGF-β1 inducible gene upregulated in idiopathic pulmonary fibrosis. Cell Signal 27:2467–2473. https://doi.org/10.1016/j.cellsig.2015.09.003
Li Z, Zhu Z, Liu Y, Liu Y, Zhao H (2022) Function and regulation of GPX4 in the development and progression of fibrotic disease. J Cell Physiol 237:2808–2824. https://doi.org/10.1002/jcp.30780
Ursini F, Maiorino M, Valente M, Ferri L, Gregolin C (1982) Purification from pig liver of a protein which protects liposomes and biomembranes from peroxidative degradation and exhibits glutathione peroxidase activity on phosphatidylcholine hydroperoxides. Biochim Biophys Acta 710:197–211. https://doi.org/10.1016/0005-2760(82)90150-3
Maiorino M, Scapin M, Ursini F, Biasolo M, Bosello V, Flohé L (2003) Distinct promoters determine alternative transcription of gpx-4 into phospholipid-hydroperoxide glutathione peroxidase variants. J Biol Chem 278:34286–34290. https://doi.org/10.1074/jbc.M305327200
Azuma K, Koumura T, Iwamoto R, Matsuoka M, Terauchi R, Yasuda S, Shiraya T, Watanabe S, Aihara M, Imai H et al (2022) Mitochondrial glutathione peroxidase 4 is indispensable for photoreceptor development and survival in mice. J Biol Chem 298:101824. https://doi.org/10.1016/j.jbc.2022.101824
Kim DH, Kim WD, Kim SK, Moon DH, Lee SJ (2020) TGF-β1-mediated repression of SLC7A11 drives vulnerability to GPX4 inhibition in hepatocellular carcinoma cells. Cell Death Dis 11:406. https://doi.org/10.1038/s41419-020-2618-6
Li Y, Yan J, Zhao Q, Zhang Y, Zhang Y (2022) ATF3 promotes ferroptosis in sorafenib-induced cardiotoxicity by suppressing Slc7a11 expression. Front Pharmacol 13:904314. https://doi.org/10.3389/fphar.2022.904314
Wang M, Liu M, Tang L, Shen L, Xiao J, Li R (2023) Liquiritin reduces ferroptosis in doxorubicin-induced cardiotoxicity through targeting SLC7A11/GPX4 pathway. Naunyn Schmiedebergs Arch Pharmacol. https://doi.org/10.1007/s00210-023-02515-4
Hong X, Roh W, Sullivan RJ, Wong KHK, Wittner BS, Guo H, Dubash TD, Sade-Feldman M, Wesley B, Horwitz E et al (2021) The lipogenic regulator SREBP2 induces transferrin in circulating melanoma cells and suppresses ferroptosis. Cancer Discov 11:678–695. https://doi.org/10.1158/2159-8290.Cd-19-1500
Yang WS, SriRamaratnam R, Welsch ME, Shimada K, Skouta R, Viswanathan VS, Cheah JH, Clemons PA, Shamji AF, Clish CB et al (2014) Regulation of ferroptotic cancer cell death by GPX4. Cell 156:317–331. https://doi.org/10.1016/j.cell.2013.12.010
Angeli JPF, Shah R, Pratt DA, Conrad M (2017) Ferroptosis inhibition: mechanisms and opportunities. Trends Pharmacol Sci 38:489–498. https://doi.org/10.1016/j.tips.2017.02.005
Casares D, Escribá PV, Rosselló CA (2019) Membrane lipid composition: Effect on membrane and organelle structure, function and compartmentalization and therapeutic avenues. Int J Mol Sci. https://doi.org/10.3390/ijms20092167
Yang WS, Kim KJ, Gaschler MM, Patel M, Shchepinov MS, Stockwell BR (2016) Peroxidation of polyunsaturated fatty acids by lipoxygenases drives ferroptosis. Proc Natl Acad Sci USA 113:E4966-4975. https://doi.org/10.1073/pnas.1603244113
Hu H, Chen Y, Jing L, Zhai C, Shen L (2021) The link between ferroptosis and cardiovascular diseases: a novel target for treatment. Front Cardiovasc Med 8:710963. https://doi.org/10.3389/fcvm.2021.710963
Wu X, Li Y, Zhang S, Zhou X (2021) Ferroptosis as a novel therapeutic target for cardiovascular disease. Theranostics 11:3052–3059. https://doi.org/10.7150/thno.54113
Hassannia B, Van Coillie S, Vanden Berghe T (2021) Ferroptosis: biological rust of lipid membranes. Antioxid Redox Signal 35:487–509. https://doi.org/10.1089/ars.2020.8175
Feng H, Stockwell BR (2018) Unsolved mysteries: how does lipid peroxidation cause ferroptosis? PLoS Biol 16:e2006203. https://doi.org/10.1371/journal.pbio.2006203
Wang K, Chen XZ, Wang YH, Cheng XL, Zhao Y, Zhou LY, Wang K (2022) Emerging roles of ferroptosis in cardiovascular diseases. Cell Death Discov 8:394. https://doi.org/10.1038/s41420-022-01183-2
Feng J, Lu PZ, Zhu GZ, Hooi SC, Wu Y, Huang XW, Dai HQ, Chen PH, Li ZJ, Su WJ et al (2021) ACSL4 is a predictive biomarker of sorafenib sensitivity in hepatocellular carcinoma. Acta Pharmacol Sin 42:160–170. https://doi.org/10.1038/s41401-020-0439-x
Doll S, Proneth B, Tyurina YY, Panzilius E, Kobayashi S, Ingold I, Irmler M, Beckers J, Aichler M, Walch A et al (2017) ACSL4 dictates ferroptosis sensitivity by shaping cellular lipid composition. Nat Chem Biol 13:91–98. https://doi.org/10.1038/nchembio.2239
Yu Q, Zhang N, Gan X, Chen L, Wang R, Liang R, Jian J (2023) EGCG attenuated acute myocardial infarction by inhibiting ferroptosis via miR-450b-5p/ACSL4 axis. Phytomedicine 119:154999. https://doi.org/10.1016/j.phymed.2023.154999
Yan B, Ai Y, Sun Q, Ma Y, Cao Y, Wang J, Zhang Z, Wang X (2021) Membrane damage during ferroptosis is caused by oxidation of phospholipids catalyzed by the oxidoreductases POR and CYB5R1. Mol Cell 81:355-369.e310. https://doi.org/10.1016/j.molcel.2020.11.024
Shah R, Shchepinov MS, Pratt DA (2018) Resolving the role of lipoxygenases in the initiation and execution of ferroptosis. ACS Cent Sci 4:387–396. https://doi.org/10.1021/acscentsci.7b00589
Koppula P, Zhuang L, Gan B (2021) Cytochrome P450 reductase (POR) as a ferroptosis fuel. Protein Cell 12:675–679. https://doi.org/10.1007/s13238-021-00823-0
Kagan VE, Mao G, Qu F, Angeli JP, Doll S, Croix CS, Dar HH, Liu B, Tyurin VA, Ritov VB et al (2017) Oxidized arachidonic and adrenic PEs navigate cells to ferroptosis. Nat Chem Biol 13:81–90. https://doi.org/10.1038/nchembio.2238
Chen Z, Yan Y, Qi C, Liu J, Li L, Wang J (2021) The role of ferroptosis in cardiovascular disease and its therapeutic significance. Front Cardiovasc Med 8:733229. https://doi.org/10.3389/fcvm.2021.733229
Santoro MM (2020) The antioxidant role of non-mitochondrial CoQ10: mystery solved! Cell Metab 31:13–15. https://doi.org/10.1016/j.cmet.2019.12.007
Dunning BJ, Bourgonje AR, Bulthuis MLC, Alexander J, Aaseth JO, Larsson A, van Goor H, Alehagen U (2023) Selenium and coenzyme Q(10) improve the systemic redox status while reducing cardiovascular mortality in elderly population-based individuals. Free Radic Biol Med 204:207–214. https://doi.org/10.1016/j.freeradbiomed.2023.04.024
Alarcón-Vieco E, Martínez-García I, Sequí-Domínguez I, Rodríguez-Gutiérrez E, Moreno-Herráiz N, Pascual-Morena C (2023) Effect of coenzyme Q10 on cardiac function and survival in heart failure: an overview of systematic reviews and meta-analyses. Food Funct 14:6302–6311. https://doi.org/10.1039/d3fo01255g
Bersuker K, Hendricks JM, Li Z, Magtanong L, Ford B, Tang PH, Roberts MA, Tong B, Maimone TJ, Zoncu R et al (2019) The CoQ oxidoreductase FSP1 acts parallel to GPX4 to inhibit ferroptosis. Nature 575:688–692. https://doi.org/10.1038/s41586-019-1705-2
Doll S, Freitas FP, Shah R, Aldrovandi M, da Silva MC, Ingold I, Goya Grocin A, Xavier da Silva TN, Panzilius E, Scheel CH et al (2019) FSP1 is a glutathione-independent ferroptosis suppressor. Nature 575:693–698. https://doi.org/10.1038/s41586-019-1707-0
Jo A, Bae JH, Yoon YJ, Chung TH, Lee EW, Kim YH, Joh HM, Chung JW (2022) Plasma-activated medium induces ferroptosis by depleting FSP1 in human lung cancer cells. Cell Death Dis 13:212. https://doi.org/10.1038/s41419-022-04660-9
Zhang LL, Tang RJ, Yang YJ (2022) The underlying pathological mechanism of ferroptosis in the development of cardiovascular disease. Front Cardiovasc Med 9:964034. https://doi.org/10.3389/fcvm.2022.964034
Xie LH, Fefelova N, Pamarthi SH, Gwathmey JK (2022) Molecular mechanisms of ferroptosis and relevance to cardiovascular disease. Cells. https://doi.org/10.3390/cells11172726
Komai K, Kawasaki NK, Higa JK, Matsui T (2022) The role of ferroptosis in adverse left ventricular remodeling following acute myocardial infarction. Cells. https://doi.org/10.3390/cells11091399
Zhang X, Zheng C, Gao Z, Chen H, Li K, Wang L, Zheng Y, Li C, Zhang H, Gong M et al (2022) SLC7A11/xCT prevents cardiac hypertrophy by inhibiting ferroptosis. Cardiovasc Drugs Ther 36:437–447. https://doi.org/10.1007/s10557-021-07220-z
Valashedi MR, Bamshad C, Najafi-Ghalehlou N, Nikoo A, Tomita K, Kuwahara Y, Sato T, Roushandeh AM, Roudkenar MH (2022) Non-coding RNAs in ferroptotic cancer cell death pathway: meet the new masters. Hum Cell 35:972–994. https://doi.org/10.1007/s13577-022-00699-0
Balihodzic A, Prinz F, Dengler MA, Calin GA, Jost PJ, Pichler M (2022) Non-coding RNAs and ferroptosis: potential implications for cancer therapy. Cell Death Differ 29:1094–1106. https://doi.org/10.1038/s41418-022-00998-x
Bahit MC, Kochar A, Granger CB (2018) Post-myocardial infarction heart failure. JACC Heart Fail 6:179–186. https://doi.org/10.1016/j.jchf.2017.09.015
Zhuang Y, Yang D, Shi S, Wang L, Yu M, Meng X, Fan Y, Zhou R, Wang F (2022) MiR-375-3p promotes cardiac fibrosis by regulating the ferroptosis mediated by GPX4. Comput Intell Neurosci 2022:9629158. https://doi.org/10.1155/2022/9629158
Neri M, Riezzo I, Pascale N, Pomara C, Turillazzi E (2017) Ischemia/Reperfusion injury following acute myocardial infarction: a critical issue for clinicians and forensic pathologists. Mediators Inflamm 2017:7018393. https://doi.org/10.1155/2017/7018393
Hermann DM, Xin W, Bähr M, Giebel B, Doeppner TR (2022) Emerging roles of extracellular vesicle-associated non-coding RNAs in hypoxia: Insights from cancer, myocardial infarction and ischemic stroke. Theranostics 12:5776–5802. https://doi.org/10.7150/thno.73931
Wang X, Liu Y, Hou H, Shao W, Huang D, Hao Z, Xue H, Ye Y (2022) MiRNA-29 aggravates myocardial infarction via inhibiting the PI3K/mTOR/HIF1α/VEGF pathway. Aging (Albany NY) 14:3129–3142. https://doi.org/10.18632/aging.203997
Fan K, Huang W, Qi H, Song C, He C, Liu Y, Zhang Q, Wang L, Sun H (2021) The Egr-1/miR-15a-5p/GPX4 axis regulates ferroptosis in acute myocardial infarction. Eur J Pharmacol 909:174403. https://doi.org/10.1016/j.ejphar.2021.174403
Song Y, Wang B, Zhu X, Hu J, Sun J, Xuan J, Ge Z (2021) Human umbilical cord blood-derived MSCs exosome attenuate myocardial injury by inhibiting ferroptosis in acute myocardial infarction mice. Cell Biol Toxicol 37:51–64. https://doi.org/10.1007/s10565-020-09530-8
Tang S, Wang Y, Ma T, Lu S, Huang K, Li Q, Wu M, Yang H, Zhong J (2020) MiR-30d inhibits cardiomyocytes autophagy promoting ferroptosis after myocardial infarction. Panminerva Med. https://doi.org/10.23736/s0031-0808.20.03979-8
Li G, Jin J, Liu S, Ding K, Qian C (2021) Inhibition of miR-1224 suppresses hypoxia/reoxygenation-induced oxidative stress and apoptosis in cardiomyocytes through targeting GPX4. Exp Mol Pathol 121:104645. https://doi.org/10.1016/j.yexmp.2021.104645
Sun W, Shi R, Guo J, Wang H, Shen L, Shi H, Yu P, Chen X (2021) MiR-135b-3p promotes cardiomyocyte ferroptosis by targeting GPX4 and aggravates myocardial ischemia/reperfusion injury. Front Cardiovasc Med 8:663832. https://doi.org/10.3389/fcvm.2021.663832
He D, Yan L (2021) MiR-29b-3p aggravates cardiac hypoxia/reoxygenation injury via targeting PTX3. Cytotechnology 73:91–100. https://doi.org/10.1007/s10616-020-00446-z
Zhou X, Zhuo M, Zhang Y, Shi E, Ma X, Li H (2021) MiR-190a-5p regulates cardiomyocytes response to ferroptosis via directly targeting GLS2. Biochem Biophys Res Commun 566:9–15. https://doi.org/10.1016/j.bbrc.2021.05.100
Zhang GY, Gao Y, Guo XY, Wang GH, Guo CX (2022) MiR-199a-5p promotes ferroptosis-induced cardiomyocyte death responding to oxygen-glucose deprivation/reperfusion injury via inhibiting Akt/eNOS signaling pathway. Kaohsiung J Med Sci 38:1093–1102. https://doi.org/10.1002/kjm2.12605
Ji JJ, Chen SY, Yang ZW, Zhang R, Qian LL, Jiang Y, Guo JQ, Wu Y, Fan QL, Yao YY et al (2022) Delivery of Mir-196c-3p with NIR-II light-triggered gel attenuates cardiomyocyte ferroptosis in cardiac ischemia-reperfusion injury. Nanomedicine 47:102618. https://doi.org/10.1016/j.nano.2022.102618
Lei D, Li B, Isa Z, Ma X, Zhang B (2022) Hypoxia-elicited cardiac microvascular endothelial cell-derived exosomal miR-210-3p alleviate hypoxia/reoxygenation-induced myocardial cell injury through inhibiting transferrin receptor 1-mediated ferroptosis. Tissue Cell 79:101956. https://doi.org/10.1016/j.tice.2022.101956
Wang J, Deng B, Liu Q, Huang Y, Chen W, Li J, Zhou Z, Zhang L, Liang B, He J et al (2020) Pyroptosis and ferroptosis induced by mixed lineage kinase 3 (MLK3) signaling in cardiomyocytes are essential for myocardial fibrosis in response to pressure overload. Cell Death Dis 11:574. https://doi.org/10.1038/s41419-020-02777-3
Xiao J, Zhang Y, Tang Y, Dai H, OuYang Y, Li C, Yu M (2021) Hsa-miR-4443 inhibits myocardial fibroblast proliferation by targeting THBS1 to regulate TGF-β1/α-SMA/collagen signaling in atrial fibrillation. Braz J Med Biol Res 54:e10692. https://doi.org/10.1590/1414-431x202010692
Han X, Wang S, Yong Z, Zhang X, Wang X (2022) MiR-29b ameliorates atrial fibrosis in rats with atrial fibrillation by targeting TGFβRΙ and inhibiting the activation of Smad-2/3 pathway. J Bioenerg Biomembr 54:81–91. https://doi.org/10.1007/s10863-022-09934-7
Guo F, Tang C, Huang B, Gu L, Zhou J, Mo Z, Liu C, Liu Y (2022) LncRNA H19 drives proliferation of cardiac fibroblasts and collagen production via suppression of the miR-29a-3p/miR-29b-3p-VEGFA/TGF-β Axis. Mol Cells 45:122–133. https://doi.org/10.14348/molcells.2021.0066
Liu D, Yang M, Yao Y, He S, Wang Y, Cao Z, Chen H, Fu Y, Liu H, Zhao Q (2022) Cardiac fibroblasts promote ferroptosis in atrial fibrillation by secreting exo-miR-23a-3p targeting SLC7A11. Oxid Med Cell Longev 2022:3961495. https://doi.org/10.1155/2022/3961495
Song Y, Wei CAI, Wang J (2021) Upregulation of miR-143–3p attenuates oxidative stress-mediated cell ferroptosis in cardiomyocytes with atrial fibrillation by degrading glutamic-oxaloacetic transaminase 1. Biocell 45:733–744. https://doi.org/10.32604/biocell.2021.013236
Song C, Qi H, Liu Y, Chen Y, Shi P, Zhang S, Ren J, Wang L, Cao Y, Sun H (2021) Inhibition of lncRNA Gm15834 attenuates autophagy-mediated myocardial hypertrophy via the miR-30b-3p/ULK1 axis in mice. Mol Ther 29:1120–1137. https://doi.org/10.1016/j.ymthe.2020.10.024
Sun W, Wu X, Yu P, Zhang Q, Shen L, Chen J, Tong H, Fan M, Shi H, Chen X (2022) LncAABR07025387.1 enhances myocardial ischemia/reperfusion injury via miR-205/ACSL4-mediated ferroptosis. Front Cell Dev Biol 10:672391. https://doi.org/10.3389/fcell.2022.672391
Zhang JK, Zhang Z, Guo ZA, Fu Y, Chen XJ, Chen WJ, Wu HF, Cui XJ (2022) The BMSC-derived exosomal lncRNA Mir9-3hg suppresses cardiomyocyte ferroptosis in ischemia-reperfusion mice via the Pum2/PRDX6 axis. Nutr Metab Cardiovasc Dis 32:515–527. https://doi.org/10.1016/j.numecd.2021.10.017
Gao F, Zhao Y, Zhang B, Xiao C, Sun Z, Gao Y, Dou X (2022) Suppression of lncRNA Gm47283 attenuates myocardial infarction via miR-706/ Ptgs2/ferroptosis axis. Bioengineered 13:10786–10802. https://doi.org/10.1080/21655979.2022.2065743
Ni T, Huang X, Pan S, Lu Z (2021) Inhibition of the long non-coding RNA ZFAS1 attenuates ferroptosis by sponging miR-150-5p and activates CCND2 against diabetic cardiomyopathy. J Cell Mol Med 25:9995–10007. https://doi.org/10.1111/jcmm.16890
Li J, Zhang Q, Jiao H (2021) LncRNA NRON promotes M2 macrophage polarization and alleviates atrial fibrosis through suppressing exosomal miR-23a derived from atrial myocytes. J Formos Med Assoc 120:1512–1519. https://doi.org/10.1016/j.jfma.2020.11.004
Zhang S, Wang N, Ma Q, Fan F, Ma X (2021) LncRNA TUG1 acts as a competing endogenous RNA to mediate CTGF expression by sponging miR-133b in myocardial fibrosis after myocardial infarction. Cell Biol Int 45:2534–2543. https://doi.org/10.1002/cbin.11707
Shi P, Li M, Song C, Qi H, Ba L, Cao Y, Zhang M, Xie Y, Ren J, Wu J et al (2022) Neutrophil-like cell membrane-coated siRNA of lncRNA AABR07017145.1 therapy for cardiac hypertrophy via inhibiting ferroptosis of CMECs. Mol Ther Nucleic Acids 27:16–36. https://doi.org/10.1016/j.omtn.2021.10.024
Zhuang S, Ma Y, Zeng Y, Lu C, Yang F, Jiang N, Ge J, Ju H, Zhong C, Wang J et al (2021) METTL14 promotes doxorubicin-induced cardiomyocyte ferroptosis by regulating the KCNQ1OT1-miR-7-5p-TFRC axis. Cell Biol Toxicol. https://doi.org/10.1007/s10565-021-09660-7
Jayaram R, Jones M, Reilly S, Crabtree MJ, Pal N, Goodfellow N, Nahar K, Simon J, Carnicer R, DeSilva R et al (2022) Atrial nitroso-redox balance and refractoriness following on-pump cardiac surgery: a randomized trial of atorvastatin. Cardiovasc Res 118:184–195. https://doi.org/10.1093/cvr/cvaa302
Su Y, Zhu C, Wang B, Zheng H, McAlister V, Lacefield JC, Quan D, Mele T, Greasley A, Liu K et al (2021) Circular RNA Foxo3 in cardiac ischemia-reperfusion injury in heart transplantation: a new regulator and target. Am J Transplant 21:2992–3004. https://doi.org/10.1111/ajt.16475
Wang B, Zhou Q, Li A, Li S, Greasley A, Skaro A, Quan D, Min W, Liu K, Zheng X (2021) Preventing alloimmune rejection using circular RNA FSCN1-silenced dendritic cells in heart transplantation. J Heart Lung Transplant 40:584–594. https://doi.org/10.1016/j.healun.2021.03.025
Nog R, Gupta CA, Panza JA (2021) Role of micro RNA in heart transplant. Cardiol Rev. https://doi.org/10.1097/crd.0000000000000393
Wu T, Shi G, Ji Z, Wang S, Geng L, Guo Z (2022) Circulating small extracellular vesicle-encapsulated SEMA5A-IT1 attenuates myocardial ischemia-reperfusion injury after cardiac surgery with cardiopulmonary bypass. Cell Mol Biol Lett 27:95. https://doi.org/10.1186/s11658-022-00395-9
Li RL, Fan CH, Gong SY, Kang S (2021) Effect and mechanism of LRP6 on cardiac myocyte ferroptosis in myocardial infarction. Oxid Med Cell Longev 2021:8963987. https://doi.org/10.1155/2021/8963987
Zheng H, Shi L, Tong C, Liu Y, Hou M (2021) CircSnx12 Is involved in ferroptosis during heart failure by targeting miR-224-5p. Front Cardiovasc Med 8:656093. https://doi.org/10.3389/fcvm.2021.656093
Ju J, Li XM, Zhao XM, Li FH, Wang SC, Wang K, Li RF, Zhou LY, Liang L, Wang Y et al (2023) Circular RNA FEACR inhibits ferroptosis and alleviates myocardial ischemia/reperfusion injury by interacting with NAMPT. J Biomed Sci 30:45. https://doi.org/10.1186/s12929-023-00927-1
Xu QR, Liu JL, Zhu RR, Huang WX, Huang H, Liu JC, Xu XP, Zhou XL (2023) NSD2 promotes pressure overload-induced cardiac hypertrophy via activating circCmiss1/TfR1/ferroptosis signaling. Life Sci 328:121873. https://doi.org/10.1016/j.lfs.2023.121873
Liu B, Zhao N, Zhou Y, Lu Y, Chen W, Huang Z, Wang D, Xu Y, Wai Ping Yam J, Cui Y (2021) Circular RNA circ_ABCB10 in cancer. Clin Chim Acta 518:93–100. https://doi.org/10.1016/j.cca.2021.03.010
Chen Z, Li Y, Wang Y, Qian J, Ma H, Wang X, Jiang G, Liu M, An Y, Ma L et al (2018) Cardiomyocyte-restricted low density lipoprotein receptor-related protein 6 (LRP6) deletion leads to lethal dilated cardiomyopathy partly through Drp1 signaling. Theranostics 8:627–643. https://doi.org/10.7150/thno.22177
Li F, Li PF, Hao XD (2023) Circular RNAs in ferroptosis: Regulation mechanism and potential clinical application in disease. Front Pharmacol 14:1173040. https://doi.org/10.3389/fphar.2023.1173040
Zeng F, Nijiati S, Tang L, Ye J, Zhou Z, Chen X (2023) Ferroptosis detection: from approaches to applications. Angew Chem Int Ed Engl. https://doi.org/10.1002/anie.202300379
Chen N, Du N, Wang W, Liu T, Yuan Q, Yang Y (2022) Real-time monitoring of dynamic microbial Fe(III) respiration metabolism with a living cell-compatible electron-sensing probe. Angew Chem Int Ed Engl 61:e202115572. https://doi.org/10.1002/anie.202115572
Martinez AM, Kim A, Yang WS (2020) Detection of ferroptosis by BODIPY™ 581/591 C11. Methods Mol Biol 2108:125–130. https://doi.org/10.1007/978-1-0716-0247-8_11
Zeng F, Nijiati S, Liu Y, Yang Q, Liu X, Zhang Q, Chen S, Su A, Xiong H, Shi C et al (2023) Ferroptosis MRI for early detection of anticancer drug-induced acute cardiac/kidney injuries. Sci Adv 9:eadd8539. https://doi.org/10.1126/sciadv.add8539
Zhou N, Bao J (2020) FerrDb: A manually curated resource for regulators and markers of ferroptosis and ferroptosis-disease associations. Database (Oxford) 2020: https://doi.org/10.1093/database/baaa021
Zhou N, Yuan X, Du Q, Zhang Z, Shi X, Bao J, Ning Y, Peng L (2022) FerrDb V2: Update of the manually curated database of ferroptosis regulators and ferroptosis-disease associations. Nucleic Acids Res. https://doi.org/10.1093/nar/gkac935
Zhou S, Huang YE, Xing J, Zhou X, Chen S, Chen J, Wang L, Jiang W (2022) NcFO: a comprehensive resource of curated and predicted ncRNAs associated with ferroptosis. Genom Proteom Bioinform. https://doi.org/10.1016/j.gpb.2022.09.004
Thum T (2014) Noncoding RNAs and myocardial fibrosis. Nat Rev Cardiol 11:655–663. https://doi.org/10.1038/nrcardio.2014.125
Dong Y, Peng N, Dong L, Tan S, Zhang X (2022) Non-coding RNAs: important participants in cardiac fibrosis. Front Cardiovasc Med 9:937995. https://doi.org/10.3389/fcvm.2022.937995
Du X, Dong R, Wu Y, Ni B (2022) Physiological effects of ferroptosis on organ fibrosis. Oxid Med Cell Longev 2022:5295434. https://doi.org/10.1155/2022/5295434
Acknowledgements
Figure 1 was created with www.BioRender.com.
Funding
This article was supported by grants from the National Nature Science Foundation of China (Grant 82160439); Basic Research Plan Project of Yunnan Provincial Science and Technology Department (Grants 202001AY070001-028, H-2019053); Yunnan Provincial Training Project of High-level Talents (Grant RLMY-20200001); Medical leading Talents Training Program of Yunnan Provincial Health Commission (Grant L-2019026); Clinical Medical Center for Cardiovascular and Cerebrovascular Disease of Yunnan Province (Grant ZX2019-03-01).
Author information
Authors and Affiliations
Contributions
CYW and SLB: designed and wrote the manuscript. XCC and LY: performed the literature search, data collection and analysis. YZP, RJL and HS: commented and revised the manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interest
The authors declare that there is no competing interest.
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wu, C., Bao, S., Sun, H. et al. Noncoding RNAs regulating ferroptosis in cardiovascular diseases: novel roles and therapeutic strategies. Mol Cell Biochem (2023). https://doi.org/10.1007/s11010-023-04895-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11010-023-04895-w