Abstract
Epidemiological studies in recent years have identified an association between exposure to air pollutants and acute myocardial infarction (AMI); however, the association between short-term ozone (O3) exposure and AMI hospitalization remains unclear, particularly in developing countries. Therefore, this study collected information on 24,489 AMI patients, including daily air pollutant and meteorological data in Henan, China, between 2016 and 2021. A distributed lagged nonlinear model combined with a Poisson regression model was used to estimate the nonlinear lagged effect of O3 on AMI hospitalizations. We also quantified the effects of O3 on the number of AMI hospitalizations, hospitalization days, and hospitalization costs. The results showed that single- and dual-pollution models of O3 at lag0, lag1, and lag (01–07) were risk factors for AMI hospitalizations, with the most significant effect at lag03 (RR = 1.132, 95% CI:1.083–1.182). Further studies showed that males, younger people (15–64 years), warm seasons, and long sunshine duration were more susceptible to O3. Hospitalizations attributable to O3 during the study period accounted for 11.66% of the total hospitalizations, corresponding to 2856 patients, 33,492 hospital days, and 90 million RMB. Maintaining O3 at 10–130 µg/m3 can prevent hundreds of AMI hospitalizations and save millions of RMB per year in Henan, China. In conclusion, we found that short-term exposure to O3 was significantly associated with an increased risk of hospitalization for AMI in Henan, China, and that further reductions in ambient O3 levels may have substantial health and economic benefits for patients and local healthcare facilities.
Graphical Abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Acute myocardial infarction (AMI) is known for its high morbidity and mortality (Hoole and Bambrough 2020, Reed et al. 2017); in China, AMI mortality has more than doubled in the past 20 years (Yang et al. 2013). The World Bank estimates that the number of patients with AMI in China will reach 23 million by 2030 (Bank. 2013). There is increasing evidence that exposure to ambient air pollutants is associated with an increased incidence of AMI (Chen et al. 2018; Ishii et al. 2021; Liu et al. 2021). However, most of these are studies on particulate matter and AMI incidence, with few involving ozone (O3), particularly in developing countries, and inconsistent outcomes. O3 is a secondary pollutant with strong oxidizing properties (Liu et al. 2022). The consequent temperature increase may lead to increased O3 concentrations in the future owing to the increased greenhouse gas emissions in the environment, accelerating global warming (Pu et al. 2017). Wang et al. (2017) reported that this process may further accelerate with the rapid consumption of fossil fuels in China. The World Health Organization (WHO) updated the WHO Global Air Quality Guidelines in 2021 to address the health hazards of O3 exposure by adding a new target of ambient seasonal O3 concentrations of less than 60 µg/m3 (Burki 2021); thus, ambient O3 pollution is a serious global public health problem.
In environmental ecology studies, short-term exposure to O3 increases the risk of cardiovascular disease, stroke, respiratory disease onset, and mortality (EPA US 2020). Recently, large cohort studies in the USA and Canada have shown that long-term exposure to O3 may be associated with mortality from cardiovascular diseases (Cakmak et al. 2016; Lim et al. 2019). In addition, a meta-study reported evidence of increased all-cause and cardiovascular mortalities associated with exposure to high O3 levels (Stafoggia et al. 2010). However, most of these studies were conducted at long-term O3 exposure levels and in developed countries where O3 concentrations are mostly below 60 µg/m3 (the ambient air quality standard for O3 in China is 160 µg/m3 (Guan et al. 2016)). In contrast, few studies have been conducted on short-term O3 exposure; no studies have analyzed the relationship between short-term O3 exposure and AMI hospitalization in China. Therefore, we conducted a multicenter time-series study in Henan Province, China, to explore the effect of short-term O3 exposure on AMI hospitalization. In addition, this study quantified the fraction of hospitalizations attributable to O3; the number of AMI-related hospitalizations and hospitalization costs saved by falling below China’s national secondary air quality standards was quantified to make appropriate recommendations for relevant public health policies.
Materials and methods
Study population
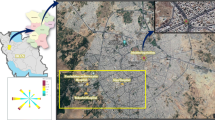
In this study, data were obtained from seven large general hospitals (Table S1) in Henan Province, China (31°23′–36°22′N, 110°21′–116°39′E), located in five cities: Anyang, Xinxiang, Luoyang, Kaifeng, and Nanyang (Figure S1). The coordinates of the monitoring stations and hospitals were determined on regional maps using ArcGIS (version 10.5). The selected hospitals were ranked as the top tertiary hospitals in prefecture-level cities and were located in densely populated areas with convenient transportation. With advanced equipment, complete medical departments, and strong diagnosis and treatment capabilities, they have a reputation for diagnosing and treating cardiovascular diseases. Therefore, they reflect the incidence of common cardiovascular diseases in the local area (Wang et al. 2020a). Between January 1, 2016, and October 31, 2021, 24,489 patients with AMI in the study sites mentioned above were enrolled in this study; all acute myocardial infarctions were clinically diagnosed and validated (Thygesen et al. 2018) with diagnosis code I21, from the 10th edition of the International Classification of Diseases (ICD-10). We collected information on these inpatients, including hospitalization number, inpatient medical records, sex, age, home address, and first diagnosis information. Each patient’s hospital address was geocoded to longitude and latitude and matched to the nearest monitoring station (Table S2). These data were also categorized according to sex, age, season, and sunshine duration. The age groups were as follows: younger (15–64 years) and older adults (≥ 65 years). The cold season was from November to April (next year), and the warm season was from May to October. We set the short (≤ 6.3 h) and long sunshine duration groups (> 6.3 h) based on the average sunshine duration in the warm season (6.33 h).
Air pollution and weather data
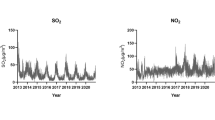
Air pollutant concentrations in the study area: O3, particulate matter with aerodynamic matter ≤ 2.5 μm (PM2.5), particulate matter with aerodynamic matter ≤ 10 μm (PM10), carbon monoxide (CO), nitrogen dioxide (NO2), and sulfur dioxide (SO2) from the China General Environmental Monitoring Station (http://www.cnemc.cn/). Air pollution data were collected from the 28 fixed-site monitoring stations mentioned above, located away from emission sources, such as roads, industries, and factories, and whose measurements reflect overall city averages rather than local pollution sources. For PM2.5, PM10, CO, NO2, and SO2, the daily concentrations are 24-h averages, while the diurnal concentrations of O3 vary significantly; therefore, the maximum 8-h averages of all effective monitoring stations were selected (Liu et al. 2022).
Meteorological data were obtained from the China National Meteorological Information Center (http://data.cma.cn/). Two meteorological parameters (daily average relative humidity and daily average temperature) were introduced as covariates in the model to adjust for confounding factors. This study was approved by the ethical review committee of The First Affiliated Hospital of Xinxiang Medical University (No. 2020097; Xinxiang, China).
Statistical analysis
Modeling the association between O3 and AMI hospitalizations and subgroup analysis
Daily AMI hospitalizations, O3, and meteorological data were linked by admission date for time-series analysis. The number of admissions of patients with AMI followed a Poisson distribution. A proposed Poisson regression model based on a generalized summation linear model and a distributed lag nonlinear model (DLMN) was used to evaluate the association between air pollutants and AMI hospitalizations (Chang et al. 2022). The association between AMI hospitalizations and O3 was fitted using the “DLMN” analysis package in R software (version 4.12). This was combined with the Akaike information criterion (Dziak et al. 2020). We included the following covariates in the model: a natural cubic spline (NS) function with 2 degrees of freedom (df) per year was used to control for long-term trends and seasonality; the effects of humidity and temperature were controlled with 2 and 5 df NS functions, respectively; the day-of-week effect (Dow) was set as a covariate; and the Chinese holiday effect was also considered in the model to eliminate the effect of public holidays.
The algebraic expression of the model is as follows:
where \(E\left({Y}_{t}\right)\) is the number of AMI hospitalizations on day t, \(\alpha\) is the intercept, and \(\beta {X}_{t,l}\) is the cross-basis matrix for air pollution. ns() represents the NS function.
To explore the lag association between AMI hospitalizations and O3, we set the pollutant as a cross-matrix and used a polynomial function for the lags. We set the lag days to 7 days (Raza et al. 2018; Stafoggia et al. 2010) and rated the lagged cumulative effect of each 10 µg/m3 increase in airborne O3 concentration using single-day lag (lag0–lag7) and multi-day cumulative lags (lag01–lag07). In addition, we stratified the study by sex (male and female), age (young and older patients), season (warm and cool seasons), and warm season sunshine duration (long and short sunshine durations) to identify potentially susceptible subgroups for O3 exposure.
Calculation of AMI hospitalizations, hospitalization days, and hospitalization costs attributable to O3
Based on the attribution fraction calculation method in previous studies (Chen et al. 2017a; Cheng et al. 2017; Deubner et al. 1975), we estimated the total attribution fraction (AF) and the number of attributions (AN) for AMI hospitalizations. Therefore, the formulae are as follows:
where \(AF\) is the attribution fraction for O3, \(A{N}_{i}\) is the number of attributions on day i, and \({N}_{i}\) is the total number of AMI hospitalizations, hospitalization days, and hospitalization costs. According to Steenland and Armstrong (2006), formulae (1) can be simplified to AF = (RR—1)/RR, RR is the cumulative maximum relative risk.
Assessment of the potential health and economic effects of O3 concentrations below the current Chinese ambient air quality standard for O3 (8 h: 160 µg/m3) during the study period
Daily O3 concentrations below the secondary standard for ambient air quality in China (8 h: 160 µg/m3) accounted for 84.2% (1795/2131) of the total study period. We maintained the O3 concentrations in the range of 10‒160 µg/m3 (every 30 unit increment). The potential health and economic effects were estimated based on five O3 concentrations (10–40–70–100–130 µg/m3). The magnitude of the health benefit (i.e., the number of preventable cases per year) was measured as the difference between the annual number of attributed cases at the O3 concentration level of the Chinese ambient air quality secondary standard and the number of cases below the five O3 concentration limits developed. Similarly, the magnitude of the economic benefit, that is, the annual hospitalization cost savings (in RMB), is measured as the difference between the annual attributable hospitalization cost at the O3 concentration level of the Chinese ambient air quality secondary standard and the hospitalization cost below the five established O3 concentration limits.
We used a cumulative lag of 3 days for risk assessment in constructing the dual-pollution model, subgroup analysis, and assessment of population attribution because O3 produced the most significant effect estimate at a cumulative lag of 3 days.
Sensitivity analysis
First, we constructed a dual-pollution model to test the effect of using the lag of the co-pollution model by adjusting for common pollutants (PM2.5, PM10, CO, NO2, and SO2) in the model. Second, the stability of the results was tested by varying the df values (3, 4, 5, 6, and 7) of the long-term trends.
The statistical analysis for this study was performed using the “dlnm” package in R software (version 4.12). This function reports the effect of every 10 µg/m3 increase in O3 on the daily AMI hospitalizations, estimated as relative risk (RR) and 95% confidence interval (95% CI). A two-sided test p-value < 0.05 was considered statistically significant.
Results
Study patients and exposure characteristics
Table 1 shows the descriptive statistics for daily AMI hospitalizations, hospitalization days, total hospitalization costs, meteorological factors, and air pollution during the study period. Between January 1, 2016, and October 31, 2021, we recorded 24,489 patients diagnosed with AMI (ICD10: I21) in these hospitals, with an average of 11.49 admissions daily. The patients were predominantly male (8.35 cases daily) and aged 15–64 years (6.18 cases daily). The daily maximum 8-h average O3 concentration during the study period was 104.29 µg/m3 (range:4–277 µg/m3).
Figure 1 shows the time series patterns of daily AMI hospitalizations, O3 concentrations, and meteorological indicators between 2016 and 2021. The number of AMI admissions showed seasonal characteristics of high in winter and low in summer, with an overall increasing trend between 2016 and 2021. O3, average daily temperature, and sunshine duration showed clear seasonal patterns of variation. Figure S2 shows the interval percentages of O3 concentrations and monthly O3 trends in the different cities during the study period. Table S3 shows the Spearman correlations between all pollutant indicators and some meteorological indicators, indicating a significant positive correlation between O3 and temperature (r = 0.78), the same positive correlation with sunshine duration (r = 0.54), and a negative correlation between O3 and the remaining air pollution indicators.
Effects of O3 in single- and dual-pollutant models
Table S4 shows the association between different air pollutants of O3, PM2.5, PM10, CO, NO2, and SO2 and AMI hospitalization at different lag days, with short-term O3 exposure being the most significantly associated with increased risk of AMI hospitalization in this study area compared to other air pollutants. Table 2 and Figure S3 show the single- and dual-pollution models of the association between O3 on different lag days and AMI hospitalization. We observed that lag0, lag1, and lag (01–07) were all risk factors for AMI hospitalization in the single- and dual-pollution models, with statistically significant differences and the largest effect at lag03 (RR = 1.132, 95% CI:1.083–1.182).
Figure 2 shows the results of the dual-pollution model at lag03, which are insignificantly different from those of the O3 single-pollution model.
Associations between O3 and AMI in different subgroups
Figure 3 reports the RR (95% CI) values of O3-related AMI hospitalizations by sex, age, season, and different sunshine hours in the warm season. The mean sunshine duration in the warm season is shown in Table S6 as 6.33 h; we defined warm season sunshine duration ≤ 6.3 has short sunshine duration (SSD) and > 6.3 has long sunshine duration (LSD) (Table S7). Among the different subgroups, AMI hospitalizations in the male, younger patients, warm season, and LSD groups were more susceptible to O3 effects.
RR (95% CI) of AMI hospitalizations expose to O3 (every 10 µg/m3 increase) in different subgroups at different lag days. A The single-day and cumulative relative risk effects in males and females. B The single-day and cumulative relative risk effects in young and elderly. C The single-day and cumulative relative risk effects in warm season and cold season. D The single-day and cumulative relative risk effects of LSD (long sunshine duration) and SSD (short sunshine duration) in warm season
In the sex stratification, the largest effect of O3 on AMI hospitalizations was estimated in lag03 (RR = 1.117, 95% CI:1.058–1.180) for males and lag02 (RR = 1.104, 95% CI:1.028–1.185) for females. In age stratification, the largest effect of O3 on AMI hospitalizations was estimated in lag02 (RR = 1.154, 95% CI:1.095–1.215) for younger patients and lag03 (RR = 1.109, 95% CI:1.054–1.176) for older adult patients. In seasonal stratification, the largest effect value of O3 on AMI hospitalizations during the warm season was estimated at lag03 (RR = 1.190, 95% CI:1.124–1.259); the difference was not statistically significant in the cold season. In the stratification of different daylight hours in the warm season, the largest effect value of O3 on AMI hospitalizations in the LSD group was estimated at lag02 (RR = 1.201, 95% CI:1.077–1.339) and in the SSD group at lag06 (RR = 1.163, 95% CI:1.015–1.286) (Table S5).
Figure 4 shows the exposure–response curves between O3 and AMI hospitalizations in different subgroups at lag03. Except for the curves in the cold season, which were not statistically significant, the O3 curves showed a linear trend in all subgroups, and the cumulative RR increased with increasing O3 concentration.
Attributable burden of AMI hospitalizations due to O3
Table 3 shows the total attributable fraction (AF) and attributable number (AN) of AMI and different subgroups of hospitalizations attributable to O3. We estimated that O3 accounted for 11.66% of the total cases (2,856), 33,492 days of total hospitalization, and 90 million RMB of the total hospitalization costs. Among the different subgroups, the AF and AN were higher in males, younger patients, and warm seasons. When we adjusted for the dual air pollution factors, the AF decreased slightly, as shown in Table S8.
Figure S4 illustrates that if O3 concentrations could be reduced to levels below current Chinese ambient air quality standards during the study, such as maintaining 130 µg/m3, 185 AMI cases could be prevented yearly, resulting in savings of 6 million RMB. If O3 were maintained at even lower levels (below 10 µg/m3), 1056 AMI hospitalizations could be prevented yearly, saving more than 30 million RMB and yielding substantial health and economic benefits. These results varied significantly across the subgroups.
Sensitivity analyses
The sensitivity analysis results are reported in Table S9; we varied the df range of the long-term trend (3, 4, 5, 6, 7) between total AMI hospitalizations, sex, age, and different seasons and found similar results to our main analysis, indicating that the outcome estimates are robust.
Discussion
This study was performed in the north-central provinces of China, with four seasons of the year. It is representative of China as a major agricultural province with low per capita income levels, and is one of the most polluted provinces in China (Zhang et al. 2022). We first constructed single-pollution models for different air pollutants of O3, PM2.5, PM10, CO, NO2, and SO2 and the risk of AMI hospitalization (Table S4), and found that short-term O3 exposure was associated with a more significant increase in the risk of AMI hospitalization than other air pollutants, and therefore, the analysis was focused on short-term O3 pollution exposure. We found that AMI hospitalization and short-term O3 exposure in Henan were significantly associated with a lag effect, with the greatest risk at a cumulative lag of 3 days (RR = 1.132, 95% CI:1.083–1.182) and a linear exposure–response curve (Figure S3). In addition, males, younger patients, warm season, and LSD groups were more susceptible to O3 levels. To our knowledge, this is the first time that DLMN analysis has been used to explore the relationship between short-term O3 exposure and AMI hospitalization in China and to attempt to quantify the number of O3-attributable AMI hospitalizations, hospitalization days, and hospitalization costs.
In epidemiological studies, O3 exposure is associated with the risk of cardiovascular and cerebrovascular diseases and mortality (Nuvolone et al. 2013; Raza et al. 2019; Wen et al. 2022; Zhang et al. 2019, 2021). A multicenter study from Italy showed that short-term exposure to O3 increased all-cause mortality in a population with an RR of 1.0043 (95% CI:1.0029, 1.0057) (Wen et al. 2022). Raza et al. (2019) found that short-term exposure to O3 increases the risk of out-of-hospital cardiac arrest. Henrotin et al. (2010) showed that short-term exposure to even low levels of O3 may cause ischemic cerebrovascular events and myocardial infarction (MI) and was most significant at a cumulative lag of 3 days with an RR of 1.115 (95% CI:1.027–1.209), consistent with our findings; however, Henrotin et al. included fewer patients with MI. Furthermore, it has been shown that there is no significant association between hourly O3 exposure and the onset of acute coronary syndromes (Chen et al. 2022), which may be due to various reasons, such as the study period, study site, and differences in O3 exposure levels. Most previous studies on O3 and cardiovascular disease were conducted in developed countries, where the mean 8-h O3 concentrations were generally below 60 µg/m3, which is significantly lower than the mean 8-h O3 concentration in our study area (104.3 µg/m3). The outcome supports this study’s results and points to a need for further control of O3 levels to lower levels in our study area.
Because pollutants in the atmosphere usually exist simultaneously, we constructed a dual-pollution model for PM2.5, PM10, CO, NO2, and SO2, and included covariates such as temperature, humidity, Dow, and public holidays in the model. The results showed no significant difference compared with the single-pollution model for O3, and the RR of the dual-pollution model was slightly lower than that of the single-pollution model, probably due to the significant negative correlation between O3 and other air pollutants (Table S3). O3 and temperature were significantly positively correlated (r = 0.78), with significantly higher O3 concentrations in the warm season than in the cold season (Table S6). The results of the subgroup analysis indicated that short-term exposure to O3 was associated with a significantly higher risk of AMI hospitalization in the warm season than in the cold season, similar to the findings of Wen et al. (2022). Similarly, we found that O3 and sunshine duration were also positively correlated (r = 0.54), which may be related to the involvement of ultraviolet light in the formation of O3 (Chang et al. 2022; Wang et al. 2020b). As we found that the association between O3 and the risk of AMI hospitalization was insignificant in the cold season, we further divided the patients into the LSD and SSD groups according to the mean sunshine hours in the warm season (6.33 h) (Table S7). We found that patients in the LSD group were associated with a higher risk of AMI, supporting the association between O3 concentration and the risk of AMI hospitalization. Concerning the age and sex of the susceptible population, the findings of current studies are mostly inconsistent; Wen et al. in Italy did not find differences between age and sex groups exposed to O3 and all-cause mortality (Wen et al. 2022). In a multi-community study, Schwartz et al. reported that for every 10 µg/m3 increase in O3 (mean 0–2 day lag), cardiovascular disease mortality was higher in people aged ≥ 65 years than in younger people, and females and blacks were more likely to be affected (Medina-Ramón and Schwartz 2008). In this study, we have found that males and younger patients are more likely to be affected by O3, possibly because there were more males and patients with AMI aged 14–64 years in this study and that this population would be more likely to expose themselves to higher levels of O3 through outdoor activities or by engaging in occupations (such as policeman and delivery-man) (Chang et al. 2022); at the meantime, males were more likely to suffer from respiratory disease (Wang et al. 2022b), which in turn affects cardiorespiratory function, which may also increase the risk of AMI hospitalization due to O3 exposure in this population.
The mechanism of O3 and the occurrence of AMI is unclear, and the results of some studies are inconsistent (Goodman et al. 2015). Michaudel et al. found that O3 dissolved in plasma generates reactive oxygen species (Michaudel et al. 2018), causing apoptosis of endothelial cells and damaging blood vessels (Emon et al. 2021). In addition, a study on healthy individuals showed that exposure to O3 resulted in elevated plasma levels of inflammatory markers (Kim et al. 2011; Pirozzi et al. 2015) and that inflammatory mediators can enter the circulatory system and stimulate platelet activation (Day et al. 2017) and the release of coagulation factors (Münzel et al. 2017), increasing the chances of thrombosis and promoting coronary events. O3 exposure may also be associated with changes in the autonomic nervous system (Arjomandi et al. 2015; Jia et al. 2011) and blood pressure (Niu et al. 2022); however, some studies have found a protective effect of O3 on ischemic myocardium (Wang et al. 2022a; Yu et al. 2021).
To complement the traditional exposure risk assessment, we evaluated the number of AMI hospitalizations, hospitalization days, and hospitalization costs attributable to O3. The results showed that 11.66% of AMI hospitalizations were attributable to the effects of O3 in the environment, equivalent to 2856 patients and 90 million RMB (Table 3). A modelling study of 12,946 cities included globally showed that the fraction of global O3-attributable mortality occurring in urban areas gained in their share of global O3-attributable burden from 2000 to 2019 (from 35 to 37%) (Malashock et al. 2022). Another study of the global burden of chronic obstructive pulmonary disease (COPD) attributable to ambient O3 exposure, conducted in 204 countries around the world, showed that among COPD-related deaths, attributable O3 exposure is generally on the rise globally, from 8.22% in 1990 to 11.13% in 2019 (Wang et al. 2022b). In contrast, a study by Chen et al. (2017b) in area of Zhejiang Province, China, found that the population attributable fractions for O3 exposure to COPD is 5.32%. This study fills a research gap in China in terms of AMI hospitalizations attributable to O3 exposure. The medical burden on local hospitals is enormous, and the local economic loss to the government and patients is huge. The Chinese government promulgated the Ambient Air Quality Standard (GB 3095–2012) in 2012, in which the secondary standard applicable to general areas sets the 8-h average concentration of O3 at 160 µg/m3; even below this standard, short-term exposure to O3 exhibits a significant association with an increased risk of AMI hospitalization. In September 2021, the World Health Organization released the latest unprecedentedly stringent “Air Quality Guidelines” (AQG) (Burki 2021), which set higher requirements for atmospheric O3 concentrations and added a new indicator of O3 concentrations less than 60 µg/m3 in the warm season, compared to the warm season in Henan, where O3 concentrations are much higher than this standard. If more stringent measures could be implemented to control O3 to lower concentrations, as shown in Figure S4, hundreds of AMI cases could be prevented yearly, and millions of RMB could be saved. This study is the first to analyze the relationship between short-term exposure to O3 and the risk of AMI hospitalization in areas of China with more severe O3 pollution, providing a basis for the prevention of AMI and environmental improvement in Henan Province.
Our study had some limitations. First, as an environmental ecological study, we could not include more comprehensive information on individuals in our study, such as disease history, complications, biochemical indicators, and medication use, which will need to be included in future in-depth clinical studies. Second, owing to the nature of the time-series study design and the uneven distribution of air monitoring stations in some study areas, there was variability in O3 exposure per patient, which may have led to reduced variability in exposure conditions and biased results. Third, in practical studies, the AF calculations we performed were often not univariate, and also, observational studies introduce certain confounding effects. This leads to some deviation from the true AF when we calculate AF. Fourth, we did not consider information related to hospitalization reimbursement for each patient with AMI when calculating the annual hospitalization costs that could be reduced by reducing O3 and the fact that reimbursement may vary across regions, which may have affected our estimates of O3-induced costs. Fifth, this study was conducted in only one province in central China; therefore, caution should be taken when generalizing to populations in other regions or countries.
Conclusions
We found that short-term exposure to O3 was significantly associated with an increased risk of hospitalization for AMI and that the exposure–response curve was linear at a cumulative lag of 3 days, particularly for males, younger patients, warm season, and long sunshine duration with greater risk. Further reductions in O3 levels, particularly in developing countries, may bring substantial health and economic benefits to patients and local healthcare institutions.
Data availability
All data were presented in our analytical results or please contact the first author or the corresponding author on reasonable request.
References
Arjomandi M, Wong H, Donde A, Frelinger J, Dalton S, Ching W, Power K, Balmes JR (2015) Exposure to medium and high ambient levels of ozone causes adverse systemic inflammatory and cardiac autonomic effects. Am J Physiol Heart Circ Physiol 308:H1499–H1509
Bank TW (2013) Toward a healthy and harmonious life in China: stemming the rising tide of non-communicable diseases. http://www.worldbank.org/content/dam/Worldbank/document/NCD_report_en.pdf (accessed Nov 27, 2013).
Burki T (2021) WHO introduces ambitious new air quality guidelines. Lancet 398:1117
Cakmak S, Hebbern C, Vanos J, Crouse DL, Burnett R (2016) Ozone exposure and cardiovascular-related mortality in the Canadian Census Health and Environment Cohort (CANCHEC) by spatial synoptic classification zone. Environ Pollut 214:589–599
Chang Z, Chen Y, Zhao Y, Fu J, Liu Y, Tang S, Han Y, Fan Z (2022) Association of sunshine duration with acute myocardial infarction hospital admissions in Beijing, China: a time-series analysis within-summer. Sci Total Environ 828:154528
Chen C, Zhu P, Lan L, Zhou L, Liu R, Sun Q, Ban J, Wang W, Xu D, Li T (2018) Short-term exposures to PM(2.5) and cause-specific mortality of cardiovascular health in China. Environ Res 161:188–194
Chen R, Yin P, Meng X, Liu C, Wang L, Xu X, Ross JA, Tse LA, Zhao Z, Kan H, Zhou M (2017) Fine particulate air pollution and daily mortality. A nationwide analysis in 272 Chinese cities. Am J Respir Crit Care Med 196:73–81
Chen R et al (2022) Hourly air pollutants and acute coronary syndrome Onset in 1.29 Million Patients. Circulation 145:1749–1760
Chen Y, Zang L, Chen J, Xu D, Yao D, Zhao M (2017) Characteristics of ambient ozone (O(3)) pollution and health risks in Zhejiang Province. Environ Sci Pollut Res Int 24:27436–27444
Cheng J, Xu Z, Bambrick H, Su H, Tong S, Hu W (2017) The mortality burden of hourly temperature variability in five capital cities, Australia: time-series and meta-regression analysis. Environ Int 109:10–19
Day DB, Xiang J, Mo J, Li F, Chung M, Gong J, Weschler CJ, Ohman-Strickland PA, Sundell J, Weng W, Zhang Y, Zhang JJ (2017) Association of ozone exposure with cardiorespiratory pathophysiologic mechanisms in healthy adults. JAMA Intern Med 177:1344–1353
Deubner DC, Tyroler HA, Cassel JC, Hames CG, Becker C (1975) Attributable risk, population attributable risk, and population attributable fraction of death associated with hypertension in a biracial population. Circulation 52:901–908
Dziak JJ, Coffman DL, Lanza ST, Li R, Jermiin LS (2020) Sensitivity and specificity of information criteria. Brief Bioinform 21:553–565
Emon ST, Unal S, Arslanhan A, Bozkurt SU, Meric ZC, Ziyal I (2021) Effects of ozone on injury after gamma knife radiosurgery. World Neurosurg 149:e982–e988
EPA US (2020): Integrated science assessment (ISA) for ozone and related photochemical oxidants (final report). Washington, DC: U.S. Environmental Protection Agency, 2020. https://cfpub.epa.gov/ncea/isa/recordisplay.cfm?deid=348522.
Goodman JE, Prueitt RL, Sax SN, Pizzurro DM, Lynch HN, Zu K, Venditti FJ (2015) Ozone exposure and systemic biomarkers: evaluation of evidence for adverse cardiovascular health impacts. Crit Rev Toxicol 45:412–452
Guan WJ, Zheng XY, Chung KF, Zhong NS (2016) Impact of air pollution on the burden of chronic respiratory diseases in China: time for urgent action. Lancet 388:1939–1951
Henrotin JB, Zeller M, Lorgis L, Cottin Y, Giroud M, Béjot Y (2010) Evidence of the role of short-term exposure to ozone on ischaemic cerebral and cardiac events: the Dijon Vascular Project (DIVA). Heart 96:1990–1996
Hoole SP, Bambrough P (2020) Recent advances in percutaneous coronary intervention. Heart 106:1380–1386
Ishii M, Seki T, Kaikita K, Sakamoto K, Nakai M, Sumita Y, Nishimura K, Miyamoto Y, Noguchi T, Yasuda S, Kanaoka K, Terasaki S, Saito Y, Tsutsui H, Komuro I, Ogawa H, Tsujita K, Kawakami K (2021) Association of short-term exposure to air pollution with myocardial infarction with and without obstructive coronary artery disease. Eur J Prev Cardiol 28:1435–1444
Jia X, Song X, Shima M, Tamura K, Deng F, Guo X (2011) Acute effect of ambient ozone on heart rate variability in healthy elderly subjects. J Expo Sci Environ Epidemiol 21:541–547
Kim CS, Alexis NE, Rappold AG, Kehrl H, Hazucha MJ, Lay JC, Schmitt MT, Case M, Devlin RB, Peden DB, Diaz-Sanchez D (2011) Lung function and inflammatory responses in healthy young adults exposed to 0.06 ppm ozone for 6.6 hours. Am J Respir Crit Care Med 183:1215–1221
Lim CC, Hayes RB, Ahn J, Shao Y, Silverman DT, Jones RR, Garcia C, Bell ML, Thurston GD (2019) Long-term exposure to ozone and cause-specific mortality risk in the United States. Am J Respir Crit Care Med 200:1022–1031
Liu S, Zhang Y, Ma R, Liu X, Liang J, Lin H, Shen P, Zhang J, Lu P, Tang X, Li T, Gao P (2022) Long-term exposure to ozone and cardiovascular mortality in a large Chinese cohort. Environ Int 165:107280
Liu Y, Pan J, Fan C, Xu R, Wang Y, Xu C, Xie S, Zhang H, Cui X, Peng Z, Shi C, Zhang Y, Sun H, Zhou Y, Zhang L (2021) Short-term exposure to ambient air pollution and mortality from myocardial infarction. J Am Coll Cardiol 77:271–281
Malashock DA, Delang MN, Becker JS, Serre ML, West JJ, Chang KL, Cooper OR, Anenberg SC (2022) Global trends in ozone concentration and attributable mortality for urban, peri-urban, and rural areas between 2000 and 2019: a modelling study. Lancet Planet Health 6:e958–e967
Medina-Ramón M, Schwartz J (2008) Who is more vulnerable to die from ozone air pollution? Epidemiology 19:672–679
Michaudel C, Fauconnier L, Julé Y, Ryffel B (2018) Functional and morphological differences of the lung upon acute and chronic ozone exposure in mice. Sci Rep 8:10611
Münzel T, Sørensen M, Gori T, Schmidt FP, Rao X, Brook FR, Chen LC, Brook RD, Rajagopalan S (2017) Environmental stressors and cardio-metabolic disease: part II-mechanistic insights. Eur Heart J 38:557–564
Niu Z, Duan Z, Wei J, Wang F, Han D, Zhang K, Jing Y, Wen W, Qin W, Yang X (2022) Associations of long-term exposure to ambient ozone with hypertension, blood pressure, and the mediation effects of body mass index: a national cross-sectional study of middle-aged and older adults in China. Ecotoxicol Environ Saf 242:113901
Nuvolone D, Balzi D, Pepe P, Chini M, Scala D, Giovannini F, Cipriani F, Barchielli A (2013) Ozone short-term exposure and acute coronary events: a multicities study in Tuscany (Italy). Environ Res 126:17–23
Pirozzi C, Sturrock A, Weng HY, Greene T, Scholand MB, Kanner R, Paine R 3rd (2015) Effect of naturally occurring ozone air pollution episodes on pulmonary oxidative stress and inflammation. Int J Environ Res Public Health 12:5061–5075
Pu X, Wang TJ, Huang X, Melas D, Zanis P, Papanastasiou DK, Poupkou A (2017) Enhanced surface ozone during the heat wave of 2013 in Yangtze River Delta region, China. Sci Total Environ 603–604:807–816
Raza A, Dahlquist M, Lind T, Ljungman PLS (2018) Susceptibility to short-term ozone exposure and cardiovascular and respiratory mortality by previous hospitalizations. Environ Health 17:37
Raza A, Dahlquist M, Jonsson M, Hollenberg J, Svensson L, Lind T, Ljungman PLS (2019) Ozone and cardiac arrest: the role of previous hospitalizations. Environ Pollut 245:1–8
Reed GW, Rossi JE, Cannon CP (2017) Acute myocardial infarction. Lancet 389:197–210
Stafoggia M, Forastiere F, Faustini A, Biggeri A, Bisanti L, Cadum E, Cernigliaro A, Mallone S, Pandolfi P, Serinelli M, Tessari R, Vigotti MA, Perucci CA (2010) Susceptibility factors to ozone-related mortality: a population-based case-crossover analysis. Am J Respir Crit Care Med 182:376–384
Steenland K, Armstrong B (2006) An overview of methods for calculating the burden of disease due to specific risk factors. Epidemiology 17:512–519
Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD (2018) Fourth universal definition of myocardial infarction (2018). Circulation 138:e618–e651
Wang J, Lu M, An Z, Jiang J, Li J, Wang Y, Du S, Zhang X, Zhou H, Cui J, Wu W, Liu Y, Song J (2020) Associations between air pollution and outpatient visits for allergic rhinitis in Xinxiang, China. Environ Sci Pollut Res Int 27:23565–23574
Wang R, Liu F, Huang P, Zhang Y, He J, Pang X, Zhang D, Guan Y (2022) Ozone preconditioning protects rabbit heart against global ischemia-reperfusion injury in vitro by up-regulating HIF-1α. Biomed Pharmacother 150:113033
Wang T, Xue L, Brimblecombe P, Lam YF, Li L, Zhang L (2017) Ozone pollution in China: a review of concentrations, meteorological influences, chemical precursors, and effects. Sci Total Environ 575:1582–1596
Wang Y, Wang K, Cheng W, Zhang Y (2022) Global burden of chronic obstructive pulmonary disease attributable to ambient ozone in 204 countries and territories during 1990–2019. Environ Sci Pollut Res Int 29:9293–9305
Wang ZB, Li JX, Liang LW (2020) Spatio-temporal evolution of ozone pollution and its influencing factors in the Beijing-Tianjin-Hebei Urban Agglomeration. Environ Pollut 256:113419
Wen B, Wu Y, Ye T, Xu R, Yu W, Yu P, Guo Y, Li S (2022) Short-term exposure to ozone and economic burden of premature mortality in Italy: a nationwide observation study. Ecotoxicol Environ Saf 241:113781
Yang G, Wang Y, Zeng Y, Gao GF, Liang X, Zhou M, Wan X, Yu S, Jiang Y, Naghavi M, Vos T, Wang H, Lopez AD, Murray CJ (2013) Rapid health transition in China, 1990–2010: findings from the Global Burden of Disease Study 2010. Lancet 381:1987–2015
Yu S, Guo H, Luo Y, Chen H (2021) Ozone protects cardiomyocytes against ischemia/reperfusion injury: regulating the heat shock protein 70 (HPS70) expression through activating the JAK2/STAT3 Pathway. Bioengineered 12:6606–6616
Zhang H, Zhang X, Zhao X, Cheng G, Chang H, Ye X, Wang J, Yu Z, Wang Q, Huang C (2022) Maternal exposure to air pollution and congenital heart diseases in Henan, China: a register-based case-control study. Ecotoxicol Environ Saf 229:113070
Zhang J, Chen Q, Wang Q, Ding Z, Sun H, Xu Y (2019) The acute health effects of ozone and PM(2.5) on daily cardiovascular disease mortality: a multi-center time series study in China. Ecotoxicol Environ Saf 174:218–223
Zhang S, Lu W, Wei Z, Zhang H (2021) Air pollution and cardiac arrhythmias: from epidemiological and clinical evidences to cellular electrophysiological mechanisms. Front Cardiovasc Med 8:736151
Funding
This research was supported by the Key Specialized Research and Development Breakthrough in Henan province (No.212102310350, No.222102310442) and Research Projects of Higher Education Institutions in Henan Province (No.21A320012).
Author information
Authors and Affiliations
Contributions
Yulong Wei: conceptualization, methodology, data curation, formal analysis, writing — original draft; Lin Fei: funding acquisition, writing — review and editing; Yongbin Wang: conceptualization, methodology; Min Zhang: conceptualization, methodology, writing — review and editing; Zhigang Chen: conceptualization, methodology; Huige Ge: conceptualization, methodology, data curation; Shiqi Ge: conceptualization, methodology, data curation; Sen Zhu: conceptualization, methodology; Pingshuan Dong: conceptualization; Kan Yang: conceptualization; Na Xie: conceptualization; Guoan Zhao: conceptualization, funding acquisition, writing — review and editing.
Corresponding author
Ethics declarations
Consent to participate
Not applicable.
Consent for publication
The manuscript was approved by all authors.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Highlights
• Association between air pollutants exposure and acute myocardial infarction exists.
• Determining lagged effect of O3 on acute myocardial infarction using two models.
• Hospitalizations caused by O3 accounted for 11.66% of the total hospitalizations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wei, Y., Fei, L., Wang, Y. et al. A time-series analysis of short-term ambient ozone exposure and hospitalizations from acute myocardial infarction in Henan, China. Environ Sci Pollut Res 30, 93242–93254 (2023). https://doi.org/10.1007/s11356-023-28456-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-28456-2