Abstract
Posttraumatic stress disorder (PTSD) is among the common mental disorders in refugees and asylum seekers; however, it is unclear if population prevalence declines or persists after resettlement. Therefore, this study aimed to identify longitudinal studies reporting PTSD among refugees and asylum seekers in upper-middle and high-income countries and to conduct a meta-analysis to map the trajectory of PTSD prevalence over time in order to inform policymakers. Seven electronic databases were searched for relevant prospective longitudinal studies. The Joanna Briggs Institute (JBI) scale was used to assess the quality of studies, and we excluded studies with a high risk of bias leaving 21 studies: 13 with moderate and 8 with a low risk of bias. The total follow-up period ranged from 1 to 7 years. Random effects meta-analysis pooling all studies suggested a baseline prevalence of 17.65% in the immediate period after resettlement (up to 1 year after arrival) and a trend for decreasing prevalence to 11.64% over time. However, studies with over 6 years of follow-up indicated a higher longitudinal prevalence of 13–17%, and in the low-risk-of-bias study subgroup, the prevalence did not decrease (ranging between 27.54 and 30.10%), which raises the possibility that PTSD prevalence may not substantially decrease in the first 6 years after resettlement. The finding that studies with a low risk of bias reported a larger prevalence of PTSD persisting over time highlights the importance of conducting high-quality longitudinal studies to inform policy. Appropriate long-term interventions are needed to decrease the impact of traumatic events on the mental health of refugees and asylum seekers.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
According to the 2022 United Nations High Commissioner for Refugees (UNHCR) report (UNHCR, 2022), an estimated one hundred million individuals globally were displaced at the end of 2021, which is about one in eighty of the global population. These people were displaced due to instability in the country, war, and human rights violations. Approximately two-thirds of these people were internally displaced, meaning they remained inside their home country although not at their original home address. One-third of refugees and asylum seekers were displaced outside their home country, 25.9 and 3.5 million, respectively (UNHCR, 2022).
Challenges experienced during any stage of forced migration (including premigration, during and after migration) are known to affect refugee and asylum seekers’ mental health. Refugees and asylum seekers are at risk of experiencing posttraumatic stress disorder (PTSD) and other mental health disorders due to many factors that may be experienced, including xenophobia, stigma, poor living, housing, assault, sexual violence, and working conditions (Seglem et al., 2011; Walg et al., 2016).
After resettlement in the host country, the occurrence of PTSD can be influenced by the traumatic experience before and during the migration process and stressors experienced after resettlement in the destination country, including the challenges of adaptation to a new environment and cultural differences (Lindert et al., 2009; Milloy & Wood, 2015; Porter & Haslam, 2005; Pöyhönen & Kokkonen, 2019). Challenges faced by refugees and asylum seekers during the adaptation processes may include racial discrimination and complex legal immigration processes. A systematic review and meta-analysis showed that despite the frequent experience of mental health problems, refugees and asylum seekers often have underutilization of mental health care in host countries (Satinsky et al., 2019).
It has been suggested that the rate of PTSD might change over time across the period after resettlement (Jensen & Skårdalsmo 2014; Seglem et al., 2011, 2014; Spallek & Razum, 2008; Walg et al., 2016). However, the evidence is unclear whether the number of refugees and asylum seekers with symptoms of PTSD declines or persists over time after resettlement. Several primary studies have been conducted to measure the prevalence of PTSD among refugees and asylum seekers. However, across studies, the rate of PTSD over time is inconsistent, and the timeframes studied after resettlement are varied (Fazel et al., 2005; Lindert et al., 2009). Even though understanding the prevalence of PTSD prospectively is important for early prevention and management, there are no clear study findings on the long-term course of PTSD in refugees and asylum seekers, including whether it significantly increases or decreases in the years following resettlement (Fazel et al., 2005). Critically, no systematic review and meta-analysis have been conducted on the course of PTSD following resettlement in host countries (Fazel et al., 2005; Hauff & Vaglum, 1995; Steel et al., 2002).
This systematic review and meta-analysis aimed to assess the prevalence of PTSD among refugee and asylum seekers over time at multiple points of data collection in upper-middle- and high-income countries. We focussed this review on higher-income resettlement countries to provide program planners and policymakers with evidence for designing strategies and access to care for refugees and asylum seekers in these countries.
Methods
The systematic review protocol was developed based on the PROSPERO registration format and registered to PROSPERO (CRD42022327740) on May 5, 2022. Throughout this systematic review, the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) were followed (Page et al., 2021a, 2021b) to report the findings of this systematic review and meta-analysis.
Search Strategy
Seven databases were searched for the relevant literature, including Ovid MEDLINE, Ovid EMBASE, Ovid CINAHL, Scopus, Web of Science, PsycINFO, and Google Scholar, from April 2, 2022, to May 10, 2022. In collaboration with a specialist librarian from Monash University with expertise in high-quality, systematic literature searches, the search strategy was developed using a combination of MeSH (Medical Subject Headings) terms and variations of free-text keywords. The detailed search strategy is a supplement as a supplementary file (Supplementary file 1). Moreover, we supplemented electronic database searches by checking lists of references from relevant review articles, and a forward citation tracking process was used for the important papers in the field.
Inclusion Criteria
We listed all inclusion and exclusion criteria following the recommended Condition-Context-Population-Framework (CoCoPop) for the review (Munn et al., 2017). The included studies for this review were longitudinal or follow-up based; had a minimum of 1 year of follow-up, had a minimum of two data collection points; involved adult study participants; used validated data collection instruments to assess PTSD, which were administered by clinicians or trained data collectors or undertaken via self-report, with a sample size of greater than forty; and were conducted in upper-middle and high-income countries based on world bank classification (Giacco et al., 2018; World Bank, 2022).
Exclusion Criteria
Letters to the editors, commentaries, systematic reviews, qualitative studies, studies with high risk of bias, and short communications were excluded from the study. Full-text publications which could not be accessed were excluded if there was no response from two email contacts made to the corresponding author.
Study Selection Process
Two authors (DW and YB) independently screened and identified eligible papers by title, abstract, and full text against prespecified criteria. Disagreements were resolved by discussion. All articles identified from the databases were exported to Endnote version X9. After removing the duplicates in Endnote, the articles were exported to Covidence (2022) (Veritas Health Innovation, 2022) for title and abstract screening and for full-text screening.
Outcome Measures
The primary outcome of this study was the prevalence of PTSD in refugee and asylum seekers identified using validated instruments. We included studies which fulfilled the quality and inclusion criteria. The identification of PTSD could be made by completing a validated scale or an interview with trained data collectors or health professionals.
Risk of Bias Assessment of the Studies
The quality of the included studies was evaluated independently by two authors (DW and YB); ratings were compared, and any disagreements were resolved by discussion. Quality was assessed using the Joanna Briggs Institute (JBI) scale for prevalence studies (Munn et al., 2017). This appraisal instrument has nine paraments: (1) appropriate sampling frame, (2) proper sampling technique, (3) adequate sample size, (4) detailed study subject and setting description, (5) sufficient data analysis, (6) valid methods to identify condition, (7) reliable measurement of condition for all participants, (8) appropriate statistical analysis, and (9) adequate response rate. If a study failed to satisfy a parameter, it resulted in a 1 otherwise a 0 score. The risk of bias was categorized as low (score 0–2), moderate (score 3–4), or high (score higher than 5).
Data Extraction
A standardized data extraction sheet was used to extract data from the included articles. Primary author, year of publication, study area, points of data collection, sample size, response rate, the proportion of refugee and asylum seekers with PTSD at the four points of data collection, the instrument used for measurement of PTSD, follow-up periods, and country of origin were extracted.
Data Analysis
Data analysis was undertaken using STATA version 17 (StataCorp, Texas, USA) after importing the extracted data. I-Square statistics and the Cochran Q test were used to evaluate the heterogeneity of the included studies. DerSimonian and Laird methods were used to compute the random effect meta-analysis model (LairdN, 1986). The overall pooled estimate was computed for the first and final point of data collection. In addition to estimating the pooled prevalence of the first/final time-point of meta-analysis (FTM) (Peters & Mengersen, 2008), the all-time-points meta-analysis (ATM) was estimated at 1 year of follow-up, 1–2 years of follow-up, 2–3 years of follow-up, 3–4 years of follow-up, 4–5 years of follow-up, 5–6 years of follow up, and more than 6 years of follow-up. The FTM and ATM approaches were chosen as they are recommended to provide useful effect estimates to address our study aim (Peters & Mengersen, 2008). Binomial distribution assumptions were used to the standard error from the reported estimates and population denominators. The pooled proportions for PTSD and their corresponding 95% CI were presented using tables and forest plots. Subgroup analyses were performed by the continent of the host country, migration status, risk of bias, study diagnostic tool, data collection method, and type of data collector to identify factors that might explain variability in study outcomes. Moreover, sensitivity and meta-regression analyses were conducted to find the potential sources of heterogeneity in the included studies.
Publication Bias and Sensitivity Analysis
The funnel plot and Egger’s test analysis were used to check the existence of publication bias with the significance level set to 0.05. A non-parametric analysis trim and fill method was used to identify the studies that caused asymmetry in the funnel plot. Then, the overall effect estimate produced by the rest of the studies can be considered minimally affected by bias, and finally, to fill imputed missing studies in the funnel plot based on the publication bias corrected overall estimate (Shi & Lin, 2019).
To assess the effect of single studies on the overall pooled estimate of PTSD among refugee and asylum seekers, a sensitivity analysis was performed using the random effects model.
Presentation and Reporting of Results
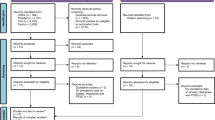
The Preferred Reporting Item for Systematic Reviews and Meta-analysis (PRISMA) guideline and PRISMA checklist (Supplementary file 2) were used to report the findings of this systematic review and meta-analysis (Page et al., 2021b) and are presented as a flow diagram in Fig. 1.
Results
Characteristics of Included Studies
The PRISMA diagram (Fig. 1) shows the study selection process for this study. A total of 7109 papers were identified from seven databases: Ovid Medline (1474), Ovid EMBASE (2423), Ovid CINAHL (875), Scopus (957), Web of Science (281), PsychInfo (403), and Google Scholar (689). Of the identified papers, 2331 were duplicates and were removed. For the remaining papers, 4764 were screened through a review of titles and abstracts, and a further 4330 papers were excluded. Following the screening of titles and abstracts, 434 studies were eligible for full-text assessment, and of these, 21 articles were included in the final analysis. The studies included 7638 participants at the baseline of the study, with 13 studies from Europe, three from North America, one from Asia, and four from Australia (see Table 1). Thirteen studies were assessed as having moderate risk, and eight had a low risk of bias. Ten studies were excluded from the analysis due to the high risk of bias as assessed by the Joanna Briggs Institute (JBI) scale. These studies had inadequate sample sizes, invalid methods for identifying conditions, incomplete descriptions of study subjects and settings, and unreliable measurements of conditions. Fifteen studies involved PTSD assessed by interviewer-administered validated tools and six with self-administered validated scales. In 13 of the studies, data collection was carried out by healthcare professionals, whereas in eight studies, non-healthcare professionals were responsible for collecting the data. Furthermore, the majority of the studies were carried out on refugees (15), with four studies focusing on asylum seekers and two studies encompassing both refugees and asylum seekers without differentiation.
Follow-up Period
The total follow-up period ranged from 1 to 7 years. Twenty-one studies had two data collection points, six had three time-points, and only one from Australia had four time-points (Wu et al., 2021). The included studies collected data at different time intervals for each data collection point. For example, the second point of data collection occurred from 6 months to 3 years after the first point of data collection, and the third point of data collection occurred 6 months to 7 years after the second point of data collection (Fig. 2). The overall attrition rate of the study participants was 20.1% (95% CI: 19.58, 21.56) at the second point of data collection and 59.8% (95% CI: 57.87, 61.84) at the third point of data collection (Table 1).
Included studies with year of follow-up and points of data collection for systematic review and meta-analysis of longitudinal studies on PTSD in refugees and asylum seekers. T1 is baseline data collection time-point (21 studies); T2 is the second time-point (21 studies); T3 is the third time-point (six studies); and T4 is the fourth time-point (one study)
Four Time Periods
Only one longitudinal study of permanently resettled refugees reported data that included four time-points, which was a study conducted in Australia (Wu et al., 2021). An earlier publication reporting mental health findings using three time-points from this same longitudinal database (Cooper et al., 2019) was excluded from this systematic review to avoid duplication.
Pooled Prevalence of Post-Traumatic Stress Disorder
Twenty-one studies reported the prevalence of PTSD for the first and second points of data collection, and six studies reported PTSD for the third point of data collection (see Table 1). The pooled prevalence of the first/final time-point of meta-analysis (FTM) was estimated and indicated that the prevalence of PTSD decreased from the first point of data collection to the third point. About one-fifth of the study participants had PTSD at the first point of data collection, 17.65% (95% CI:12.99, 22.30) and 11.64% (95% CI: 6.70, 16.58) of participants had PTSD at the third point of data collection (Fig. 3). Only one study (Wu et al., 2021) had four time-points (collected within a 3 year follow-up period), and prevalence also decreased over time from 30.3% (95% CI: 28.5, 32.2) at T1 to 21.36% (95% CI: 19.2, 23.7) at the final fourth data point (Table 2).
In addition to estimating the pooled prevalence of the first/final time-point of meta-analysis (FTM), the all-time-points meta-analysis (ATM) was estimated for the included studies. After baseline, at 1 year, the pooled prevalence was PTSD 15.74%; at 2 years, the pooled prevalence of PTSD was 16.64; at 3 years, the pooled prevalence was 16.9%; and at 5 years, the prevalence was 13.2% (Supplementary file-4, Fig. 1). A meta-regression was conducted to assess the significant difference between the initial and second data collection points across 21 studies (p = 0.78). Conversely, a meta-regression was employed to evaluate the significant difference between the second and third data collection points, revealing no statistically significant difference between these two points of data collection (p = 0.65). Ultimately, when comparing the proportions of PTSD-positive refugees and asylum seekers, it was found that there were no significant differences observed between the various data collection points, including both the first and second data collection points and the second and third data collection points.
Heterogeneity for the Pooled Prevalence of PTSD
Subgroup Analysis
Included studies had heterogeneity at the three data collection points assessed in the meta-analysis. Subgroup analysis was done by strata of the continent of the host country (Europe, North America, Australia, Asia), migration status (refugee or asylum seeker), risk of bias (low or moderate), tool used by the study (diagnostic or screening tool), data collection method (interviewer or self-administered), and type of data collector (trained or non-trained) (Table 3).
The subgroup analysis showed that, at the first time point of data collection, the highest pooled prevalence of PTSD was reported from Australia and the lowest was from Asia. At T2, the pooled prevalence of PTSD was significantly higher in Asia compared to Europe (but note that there was only one study at T2 from Asia). At T3, the pooled prevalence was higher in Europe, followed by Australia, and both were significantly higher than in North America. In the subgroup analysis examining the risk of bias classification at T2 and T3, the prevalence of PTSD was significantly higher in those with a low risk of bias compared to those with moderate risk. Of the 21 studies included, 14 used screening tools and seven used diagnostic tools. Studies that used a screening tool had a higher pooled prevalence of PTSD than the studies that used diagnostic tools at all three data collection points; however, a significant difference was observed only at T2. No significant differences were found for migration status, data collection method, or type of data collector (Table 3).
Sensitivity Analysis
To explore the influence of a single study on the pooled prevalence of PTSD, a sensitivity analysis was conducted. The random-effects model sensitivity analysis revealed that no single study influenced the overall pooled prevalence of PTSD at the three points of data collection (Supplementary file 4, Figs. 2, 3, and 4).
The Publication Biases
The asymmetric distribution of funnel plots suggested publication bias among the included studies in three data collection points (Figs. 4, 5, and 6). Moreover, objective measurement Egger’s tests were used to confirm the publication bias. The tests showed significant publication bias at the first and second points of data collection. At the outset, our intention was to incorporate unpublished articles. However, as part of the screening and quality assessment, these unpublished papers were subsequently excluded. This may account for the potential presence of significant publication bias. However, there was no significant publication bias at the third data collection point, p = 0.025 at T1, p = 0.012 at T2, and p = 0.659 at T3. Trim and fill analysis was performed to adjust publication bias and to estimate the number of missing studies that might exist for the first and second points of data collection (Figs. 7 and 8). After adjusting publication bias, the pooled prevalence of PTSD among refugees and asylum seekers was 17.62% at the first point and 15.14% at the second data collection point.
Meta-Regression
Meta-regression analysis was used to examine potential sources of heterogeneity using variables such as the continent of the study conducted, year of publication, methods of data collection, and risk of bias of the included studies. Based on this meta-regression result, none of these variables was statistically associated with the pooled prevalence of PTSD at the three time-points of data collection (Supplementary file 4, Table 4); however, it is noted that the number of included studies is relatively low and meta-regression may be underpowered.
Discussion
Overall Findings
This systematic review and meta-analysis identified 21 longitudinal studies with moderate or low risk of bias that examined the time-varying prevalence of PTSD reported among refugees and asylum seekers resettled in an upper-middle or high-income host country. Overall, a relatively high prevalence of PTSD was found even at follow-up periods of up to 7 years. Pooled prevalence indicated that 17.65% of the refugee and asylum seekers likely had PTSD at baseline in the first years of resettlement and might be as high as one-in-four people as indicated by the studies assessed as having a low risk of bias. Pooling all studies showed a trend for a decrease in prevalence of PTSD over timepoints to approximately one-in-ten people; however, studies having over 6 years of follow-up suggested that the longitudinal prevalence is 13–17%, which is closer to the pooled prevalence at baseline.
Decreasing or Stable Prevalence of PTSD
This meta-analysis of longitudinal studies provides some evidence that the prevalence of PTSD may decline over time in refugees who are newly resettled within upper-mid and high-income host countries. Decreasing prevalence over time has been found in other studies conducted in Norway and the Netherlands (Betancourt et al., 2013; Blackmore et al., 2020; Lamkaddem et al., 2014; Oppedal & Idsoe, 2015) and other longitudinal studies (Hauff & Vaglum, 1994; Lie, 2002). Access to new jobs and reduced stressful events are reported to be contributing factors to the decline of PTSD prevalence over time (Beiser & Hou, 2001). Additionally, the reduction could be associated with declining post-migration difficulties, including overcoming any initial financial hardship, family integration, and loneliness in the host country (Beiser & Wickrama, 2004).
The sub-group analyses did raise the possibility that the prevalence of PTSD may not substantially decrease in the first decade after resettlement from baseline. The subgroup of studies with over 6 years of follow-up had a pooled longitudinal prevalence of 13–17%, while in the subgroup of nine studies with low risk of bias, there was a relatively stable prevalence between 25 and 30% at all data collection points. Another study conducted in Switzerland also found that the prevalence of PTSD did not change over time after resettlement (Schick et al., 2018). A possible reason for the persistence of PTSD could be that the symptoms of PTSD can also have an intermittent or delayed onset, whereby symptoms only become apparent several years after the traumatic events have occurred (Smid et al., 2009, 2011). Moreover, exposure to interpersonal stressors and trauma during premigration and also post-migration may increase the risk for the onset and persistence of PTSD (Priebe et al., 2010; Steel et al., 2009). Post-migration stresses are widely reported, such as socio-economic difficulties, social integration problems, weak social networks, housing and accommodation problems, discrimination, and financial difficulties (Carswell et al., 2011; Lecerof et al., 2015; Teodorescu et al., 2012).
Other Findings
Of the included studies, all had at least two points of data collection, six studies (27.27%) had three time-points of data collection, and only one study (4.5%) had a fourth time data collection point. The rate of PTSD varied across continents of the host countries at three data collection points; in the first data collection point, the pooled prevalence of PTSD was higher in studies conducted in Australia than the studies conducted in other continents. At the second point of data collection, the prevalence of PTSD was found to be highest in those conducted within Asia. Additionally, the pooled prevalence of PTSD observed during the first point of data collection surpassed the findings from a sub-group analysis conducted by Blackmore in their study within the systematic review and meta-analysis (Blackmore et al., 2020). The possible reasons for this could be the year of the study conducted, the tools used to screen for or diagnose PTSD, the method of data collection, and methodological differences. Moreover, the intervention measures and health care access could be the potential source of the differences. Screening instruments have been known to inflate PTSD prevalence rates, and in this analysis, studies that used a screening tool had higher pooled prevalence than the studies that used a diagnostic tool. Adopting or developing a method that can reliably estimate the expected population-level percentage differences between screening and diagnostic tools would be useful for the detection of a more reliable estimate of PTSD among refugee and asylum seekers in research.
Policy Implications
Studies with refugee and asylum seeker are often complex and expensive to conduct due to factors such as the need for interpreters and difficulties locating participants over time, as these are often highly mobile groups. This suggests that prevalence estimates from lower quality studies might be erroneously low, which then decrease the overall pooled prevalence when included in a meta-analysis like this one. This new evidence from this systematic review indicates that high-quality longitudinal studies are warranted to obtain policy-informing data, which is valuable information for program planners and policymakers in middle- and high-income countries who need to justify the costs and resources put towards such studies.
Although the prevalence of PTSD may decrease over time, the rate of those affected remains high. These findings therefore support the need for appropriate interventions to decrease the impact of traumatic events on the mental health of refugees and asylum seekers. This is essential information for program planners and policymakers in upper-middle- and high-income countries suggesting that targeted efforts should remain sustained and not just focussed early in resettlement. The following points are recommended to alleviate these problems in refugees and asylum seekers. First, implement systematic and regular screening for PTSD and other mental health issues among refugees and asylum seekers during their resettlement process. This can help identify individuals who may need intervention and support as early as possible (Magwood et al., 2022). Second, train healthcare and social service providers in trauma-informed care approaches. This includes understanding the impact of trauma on individuals’ mental health, creating safe and supportive environments, and avoiding re-traumatization. Third, establish support groups and peer-led initiatives where refugees and asylum seekers can share their experiences, coping strategies, and advice with one another. This can foster a sense of belonging and reduce feelings of isolation (Murray et al., 2010). Finally, establish long-term monitoring systems to track the mental health progress of refugees and asylum seekers over time. This can help identify trends, evaluate the effectiveness of interventions, and make necessary adjustments (Thiel de Bocanegra et al., 2018).
Limitations of the study
Although this systematic review and meta-analysis is the first of its type in the specified study area, it has limitations. These include the differences in follow-up and data collection time points, which we examined within two meta-analysis approaches (FTM and ATM) recommended to help us answer our study aim (Peters & Mengersen, 2008). Importantly, this review showed that studies with a low risk of bias produced the highest estimates for PTSD, which were significantly higher at the later time-points examined in the meta-analysis. This underscores the necessity for cautious interpretation and generalization of these findings. It is important to recognize that this conclusion is drawn from a limited number of included studies, and the meta-analysis did not encompass all potential factors that might influence the risk of PTSD. Other limitations include the inability to consider the effect of any interventions during the resettlement period, such as clinical, psychological, and religious interventions as well as gaining employment. Moreover, this review had higher effect size heterogeneity; however, we conducted a subgroup analysis to control such heterogeneity in the included studies, which is an example of what future meta-analyses with heterogenous populations and studies can do to strengthen their findings. Furthermore, the potential source of heterogeneity of the pooled prevalence in this study could be the country of origin, ethnicities of included groups, and sex of the study participants. It is important to note that the number of incorporated studies is relatively low at the third data collection point. As a consequence, the meta-regression findings during this particular data collection point might lack sufficient statistical power. Finally, no studies in this review reported on PTSD prevalence during the premigration phase. Hence, this could be the limitation of this systematic review and meta-analysis.
Conclusion
Longitudinal studies show that the prevalence of PTSD is relatively high in refugee and asylum seekers resettled in upper-middle and high-income countries. Although there may be a decline in PTSD over time, the rate of PTSD varied across continents of the host country. Importantly, this review underscored that studies exhibiting a low risk of bias demonstrated a persistently higher prevalence of PTSD compared to the overall pooled prevalence at each stage of data collection. This emphasizes the crucial role of conducting high-quality longitudinal studies to provide informed insights for shaping policies. Appropriate interventions are needed to decrease the impact of traumatic events on the mental health of refugees and asylum seekers because, although the prevalence of PTSD may decrease in the first decade after resettlement, the rate of those affected remains high.
Data Availability
The data extracted from the included studies and the analytic code are available upon request to the authors. The dataset is available upon application and approval by the corresponding author, Associate Professor Joanne C. Enticott (Joanne.Enticott@monash.edu).
Abbreviations
- AOR :
-
Adjusted odds ratio
- PRISMA :
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PTSD :
-
Posttraumatic stress disorder
References
Beiser, M., & Hou, F. (2001). Language acquisition, unemployment and depressive disorder among Southeast Asian refugees: A 10-year study. Social Science & Medicine, 53(10), 1321–1334. https://doi.org/10.1016/S0277-9536(00)00412-3
Beiser, M., & Wickrama, K. A. S. (2004). Trauma, time and mental health: A study of temporal reintegration and depressive disorder among Southeast Asian refugees. Psychological Medicine, 34(5), 899–910. https://doi.org/10.1017/S0033291703001703
Betancourt, T. S., Borisova, I., Williams, T. P., Meyers-Ohki, S. E., Rubin-Smith, J. E., Annan, J., & Kohrt, B. A. (2013). Research review: Psychosocial adjustment and mental health in former child soldiers–a systematic review of the literature and recommendations for future research. Journal of Child Psychology and Psychiatry, 54(1), 17–36. https://doi.org/10.1111/j.1469-7610.2012.02620.x
Blackmore, R., Boyle, J. A., Fazel, M., Ranasinha, S., Gray, K. M., Fitzgerald, G., Misso, M., & Gibson-Helm, M. (2020). The prevalence of mental illness in refugees and asylum seekers: A systematic review and meta-analysis. PLoS Medicine, 17(9), e1003337. https://doi.org/10.1371/journal.pmed.1003337
Borho, A., Viazminsky, A., Morawa, E., Schmitt, G. M., Georgiadou, E., & Erim, Y. (2020). The prevalence and risk factors for mental distress among Syrian refugees in Germany: A register-based follow-up study. BMC Psychiatry, 20(1), 362. https://doi.org/10.1186/s12888-020-02746-2
Carlsson, J. M., Olsen, D. R., Mortensen, E. L., & Kastrup, M. (2006). Mental health and health-related quality of life: A 10-year follow-up of tortured refugees. The Journal of Nervous and Mental Disease, 194(10), 725–731. https://doi.org/10.1097/01.nmd.0000243079.52138.b7
Carswell, K., Blackburn, P., & Barker, C. (2011). The relationship between trauma, post-migration problems and the psychological well-being of refugees and asylum seekers. International Journal of Social Psychiatry, 57(2), 107–119. https://doi.org/10.1177/0020764009105699
Chernet, A., Probst-Hensch, N., Sydow, V., Paris, D. H., & Labhardt, N. D. (2021). Mental health and resilience among Eritrean refugees at arrival and one-year post-registration in Switzerland: A cohort study. BMC Research Notes, 14(1), 1–6. https://doi.org/10.1186/s13104-021-05695-5
Cooper, S., Enticott, J. C., Shawyer, F., & Meadows, G. (2019). Determinants of mental illness among humanitarian migrants: Longitudinal analysis of findings from the first three waves of a large cohort study. Frontiers in Psychiatry, 10, 545. https://doi.org/10.3389/fpsyt.2019.00545
Cwikel, J., Abdelgani, A., Goldsmith, J., Quastel, M., & Yevelson, I. (1997). Two-year follow up study of stress-related disorders among immigrants to Israel from the Chernobyl area. Environmental Health Perspectives, 105(suppl 6), 1545–1550. https://doi.org/10.1289/ehp.97105s61545
Drozdek, B., Kamperman, A. M., Tol, W. A., Knipscheer, J. W., & Kleber, R. J. (2014). Seven-year follow-up study of symptoms in asylum seekers and refugees with PTSD treated with trauma-focused groups. Journal of Clinical Psychology, 70(4), 376–387. https://doi.org/10.1002/jclp.22035
Ellis, B. H., Sideridis, G., Davis, S. H., Cardeli, E., Abdi, S. M., & Lincoln, A. K. (2022). Discrimination and mental health of Somali immigrants in North America: A longitudinal study from 2013 to 2019. Social Psychiatry and Psychiatric Epidemiology, 57(5), 1049–1059. https://doi.org/10.1007/s00127-022-02235-9
Fazel, M., Wheeler, J., & Danesh, J. (2005). Prevalence of serious mental disorder in 7000 refugees resettled in western countries: A systematic review. The Lancet, 365(9467), 1309–1314.
Giacco, D., Laxhman, N., & Priebe, S. (2018). 2018/05/01/). Prevalence of and risk factors for mental disorders in refugees. Seminars in Cell & Developmental Biology, 77, 144–152. https://doi.org/10.1016/j.semcdb.2017.11.030
Hauff, E., & Vaglum, P. (1994). Chronic posttraumatic stress disorder in Vietnamese refugees. A prospective community study of prevalence, course, psychopathology, and stressors. The Journal of Nervous and Mental Disease, 182(2), 85–90. https://doi.org/10.1097/00005053-199402000-00004
Hauff, E., & Vaglum, P. (1995). Organised violence and the stress of exil. Predictors of mental health in a community cohort of Vietnamese refugees three years after resettlement. British Journal of Psychiatry, 166(3), 360–367. https://doi.org/10.1192/bjp.166.3.360
Jensen, T. K., Skar, A. M. S., Andersson, E. S., & Birkeland, M. S. (2019). Long-term mental health in unaccompanied refugee minors: Pre- and post-flight predictors. European Child and Adolescent Psychiatry, 28(12), 1671–1682. https://doi.org/10.1007/s00787-019-01340-6
Jensen, T., & Skårdalsmo, B. BM & Fjermestad, KW (2014). Development of mental health problems-A follow-up study of unaccompanied refugee minors. Child and Adolescent Psychiatry and Mental Health, 8. https://doi.org/10.1186/1753-2000-8-29
Kaltenbach, E., Schauer, M., Hermenau, K., Elbert, T., & Schalinski, I. (2018). Course of mental health in refugees—A one year panel survey. Frontiers in Psychiatry, 9, 352. https://doi.org/10.3389/fpsyt.2018.00352
LairdN, D. (1986). Meta-analysis in clinical trials. Controlled Clinical Trials, 7(3), 177–188. https://doi.org/10.1016/0197-2456(86)90046-2
Lamkaddem, M., Stronks, K., Devillé, W. D., Olff, M., Gerritsen, A. A., & Essink-Bot, M.-L. (2014). Course of post-traumatic stress disorder and health care utilisation among resettled refugees in the Netherlands. BMC Psychiatry, 14(1), 1–7. https://doi.org/10.1186/1471-244X-14-90
Lecerof, S. S., Stafström, M., Westerling, R., & Östergren, P.-O. (2015). Does social capital protect mental health among migrants in Sweden? Health Promotion International, 31(3), 644–652. https://doi.org/10.1093/heapro/dav048
Lenferink, L. I., Liddell, B. J., Byrow, Y., O’Donnell, M., Bryant, R. A., Mau, V., McMahon, T., Benson, G., & Nickerson, A. (2022). Course and predictors of posttraumatic stress and depression longitudinal symptom profiles in refugees: A latent transition model. Journal of Psychiatric Research, 146, 1–10. https://doi.org/10.1016/j.jpsychires.2021.12.009
Lie, B. (2002). A 3-year follow-up study of psychosocial functioning and general symptoms in settled refugees. Acta Psychiatrica Scandinavica, 106(6), 415–425. https://doi.org/10.1034/j.1600-0447.2002.01436.x
Lies, J., Drummond, S. P., & Jobson, L. (2020). Longitudinal investigation of the relationships between trauma exposure, post-migration stress, sleep disturbance, and mental health in Syrian refugees. European Journal of Psychotraumatology, 11(1), 1825166. https://doi.org/10.1080/20008198.2020.1825166
Lindert, J., von Ehrenstein, O. S., Priebe, S., Mielck, A., & Brähler, E. (2009). Depression and anxiety in labor migrants and refugees–A systematic review and meta-analysis. Social Science & Medicine, 69(2), 246–257. https://doi.org/10.1016/j.socscimed.2009.04.032
Magwood, O., Kassam, A., Mavedatnia, D., Mendonca, O., Saad, A., Hasan, H., Madana, M., Ranger, D., Tan, Y., & Pottie, K. (2022). Mental health screening approaches for resettling refugees and asylum seekers: A scoping review. International Journal of Environmental Research and Public Health, 19(6), 3549. https://doi.org/10.3390/ijerph19063549
Milloy, M. J., & Wood, E. (2015). Withdrawal from methadone in US prisons: Cruel and unusual? Lancet, 386(9991), 316–318. https://doi.org/10.1016/S0140-6736(15)60073-3
Mollica, R. F., Caridad, K. R., & Massagli, M. P. (2007). Longitudinal study of posttraumatic stress disorder, depression, and changes in traumatic memories over time in Bosnian refugees. Journal of Nervous and Mental Disease, 195(7), 572–579. https://doi.org/10.1097/NMD.0b013e318093ed2c
Munn, Z., Moola, S., Lisy, K., Riitano, D., & Tufanaru, C. (2017). Systematic reviews of prevalence and incidence. Joanna Briggs Institute reviewer’s manual. Adelaide, South Australia: The Joanna Briggs Institute, 5.1–5.5. https://doi.org/10.46658/JBIMES-20-06
Murray, K. E., Davidson, G. R., & Schweitzer, R. D. (2010). Review of refugee mental health interventions following resettlement: Best practices and recommendations. American Journal of Orthopsychiatry, 80(4), 576–585. https://doi.org/10.1111/j.1939-0025.2010.01062.x
Oppedal, B., & Idsoe, T. (2015). The role of social support in the acculturation and mental health of unaccompanied minor asylum seekers. Scandinavian Journal of Psychology, 56(2), 203–211. https://doi.org/10.1111/sjop.12194
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., & Brennan, S. E. (2021a). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. International Journal of Surgery, 88, 105906.
Page, M. J., Moher, D., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., & Brennan, S. E. (2021). PRISMA 2020 explanation and elaboration: Updated guidance and exemplars for reporting systematic reviews. Bmj, 372. https://doi.org/10.1136/bmj.n160
Peters, J. L., & Mengersen, K. L. (2008). Meta-analysis of repeated measures study designs. Journal of Evaluation in Clinical Practice, 14(5), 941–950. https://doi.org/10.1111/j.1365-2753.2008.01010.x
Porter, M., & Haslam, N. (2005). Predisplacement and postdisplacement factors associated with mental health of refugees and internally displaced persons: A meta-analysis. Jama, 294(5), 602–612. https://jamanetwork.com/journals/jama/article-abstract/201335.
Pöyhönen, A., & Kokkonen, E. (2019). Psychosocial well-being and mental health service utilization of immigrant background women who are at home and employed - Population study in Russian, Kurdish, and Somali groups. University of Eastern Finland]. Finland. http://urn.fi/urn:nbn:fi:uef-20191172
Priebe, S., Bogic, M., Ashcroft, R., Franciskovic, T., Galeazzi, G. M., Kucukalic, A., Lecic-Tosevski, D., Morina, N., Popovski, M., & Roughton, M. (2010). Experience of human rights violations and subsequent mental disorders–A study following the war in the Balkans. Social Science & Medicine, 71(12), 2170–2177. https://doi.org/10.1016/j.socscimed.2010.09.029
Sarajlić Vuković, I., Jovanović, N., Kolarić, B., Vidović, V., & Francis Mollica, R. (2014). Psychological and somatic health problems in Bosnian refugees: A three year follow-up. Psychiatria Danubina, 26(suppl 3), 442–449.
Satinsky, E., Fuhr, D. C., Woodward, A., Sondorp, E., & Roberts, B. (2019). Mental health care utilisation and access among refugees and asylum seekers in Europe: A systematic review. Health Policy, 123(9), 851–863. https://doi.org/10.1016/j.healthpol.2019.02.007
Schick, M., Morina, N., Mistridis, P., Schnyder, U., Bryant, R. A., & Nickerson, A. (2018). Changes in Post-migration living difficulties predict treatment outcome in traumatized refugees [Original Research]. Frontiers in Psychiatry, 9. https://doi.org/10.3389/fpsyt.2018.00476
Seglem, K. B., Oppedal, B., & Raeder, S. (2011). Predictors of depressive symptoms among resettled unaccompanied refugee minors. Scandinavian Journal of Psychology, 52(5), 457–464. https://doi.org/10.1111/j.1467-9450.2011.00883.x
Seglem, K. B., Oppedal, B., & Roysamb, E. (2014). Daily hassles and coping dispositions as predictors of psychological adjustment: A comparative study of young unaccompanied refugees and youth in the resettlement country. International Journal of Behavioral Development, 38(3), 293–303. https://doi.org/10.1177/0165025414520807
Shi, L., & Lin, L. (2019). The trim-and-fill method for publication bias: Practical guidelines and recommendations based on a large database of meta-analyses. Medicine, 98(23). https://doi.org/10.1097/MD.0000000000015987
Smid, G. E., Mooren, T. T., Van Der Mast, R. C., Gersons, B. P., & Kleber, R. J. (2009). Delayed posttraumatic stress disorder: Systematic review, meta-analysis, and meta-regression analysis of prospective studies. The Journal of Clinical Psychiatry, 70(11), 4091.
Smid, G. E., Lensvelt-Mulders, G. J., Knipscheer, J. W., Gersons, B. P., & Kleber, R. J. (2011). Late-onset PTSD in unaccompanied refugee minors: Exploring the predictive utility of depression and anxiety symptoms. Journal of Clinical Child & Adolescent Psychology, 40(5), 742–755. https://doi.org/10.1080/15374416.2011.597083
Spallek, J., & Razum, O. (2008). Courtesy translation: Health inequalities. Determinants and mechanisms of health inequality. Health inequalities, 271–290.
Steel, Z., Silove, D., Phan, T., & Bauman, A. (2002). Long-term effect of psychological trauma on the mental health of Vietnamese refugees resettled in Australia: A population-based study. Lancet, 360(9339), 1056–1062. https://doi.org/10.1016/S0140-6736(02)11142-1
Steel, Z., Chey, T., Silove, D., Marnane, C., Bryant, R. A., & Van Ommeren, M. (2009). Association of torture and other potentially traumatic events with mental health outcomes among populations exposed to mass conflict and displacement: A systematic review and meta-analysis. JAMA, 302(5), 537–549. https://doi.org/10.1001/jama.2009.1132
Steel, Z., Momartin, S., Silove, D., Coello, M., Aroche, J., & Tay, K. W. (2011). Two year psychosocial and mental health outcomes for refugees subjected to restrictive or supportive immigration policies. Social Science & Medicine, 72(7), 1149–1156. https://doi.org/10.1016/j.socscimed.2011.02.007
Strømme, E. M., Haj-Younes, J., Hasha, W., Fadnes, L. T., Kumar, B., Igland, J., & Diaz, E. (2020). Changes in health among Syrian refugees along their migration trajectories from Lebanon to Norway: A prospective cohort study. Public Health, 186, 240–245. https://doi.org/10.1016/j.puhe.2020.07.016
Teodorescu, D.-S., Siqveland, J., Heir, T., Hauff, E., Wentzel-Larsen, T., & Lien, L. (2012). Posttraumatic growth, depressive symptoms, posttraumatic stress symptoms, post-migration stressors and quality of life in multi-traumatized psychiatric outpatients with a refugee background in Norway. Health and Quality of Life Outcomes, 10(1), 1–16. https://doi.org/10.1186/1477-7525-10-84
Thiel de Bocanegra, H., Carter-Pokras, O., Ingleby, J. D., Pottie, K., Tchangalova, N., Allen, S. I., Smith-Gagen, J., & Hidalgo, B. (2018). Addressing refugee health through evidence-based policies: A case study. Annals of epidemiology, 28(6), 411–419. https://doi.org/10.1016/j.annepidem.2017.05.010
UNHCR. (2022). Refugee data Finder UNHCR, The UN Refugee Agency. https://www.unhcr.org/refugee-statistics/
Veritas Health Innovation. (2022). Covidence systematic review software. http://www.covidence.org
Vervliet, M., Lammertyn, J., Broekaert, E., & Derluyn, I. (2014). Longitudinal follow-up of the mental health of unaccompanied refugee minors. European Child and Adolescent Psychiatry, 23(5), 337–346. https://doi.org/10.1007/s00787-013-0463-1
Vojvoda, D., Weine, S. M., McGlashan, T., Becker, D. F., & Southwick, S. M. (2008). Posttraumatic stress disorder symptoms in Bosnian refugees 3 1/2 years after resettlement. Journal of Rehabilitation Research & Development, 45(3). https://doi.org/10.1682/JRRD.2007.06.0083
Walg, M., Fink, E., Großmeier, M., Temprano, M., & Hapfelmeier, G. (2016). The proportion of unaccompanied refugee minors suffering from psychiatric disorders in Germany. Zeitschrift Fur Kinder-Und Jugendpsychiatrie Und Psychotherapie, 45(1), 58–68. https://doi.org/10.1024/1422-4917/a000459
World Bank. (2022). The world by income and region. Retrieved 27 July, 2022 from https://datatopics.worldbank.org
Wright, A. M., Aldhalimi, A., Lumley, M. A., Jamil, H., Pole, N., Arnetz, J. E., & Arnetz, B. B. (2016). Determinants of resource needs and utilization among refugees over time. Social Psychiatry and Psychiatric Epidemiology, 51(4), 539–549. https://doi.org/10.1007/s00127-015-1121-3
Wu, S., Renzaho, A. M., Hall, B. J., Shi, L., Ling, L., & Chen, W. (2021). Time-varying associations of pre-migration and post-migration stressors in refugees’ mental health during resettlement: A longitudinal study in Australia. The Lancet Psychiatry, 8(1), 36–47. https://doi.org/10.1016/S2215-0366(20)30422-3
Acknowledgements
We would like to acknowledge the Monash University Liberians for their advice and assistance. We also would like to thank Prof. Graham Meadows for his valuable insights into an earlier version of the paper.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Handiso, D., Belsti, Y., Boyle, J.A. et al. A Systematic Review and Meta-Analysis of Longitudinal Studies on Posttraumatic Stress Disorders in Refugees and Asylum Seekers. Int J Ment Health Addiction (2023). https://doi.org/10.1007/s11469-023-01172-1
Accepted:
Published:
DOI: https://doi.org/10.1007/s11469-023-01172-1