Abstract
Maintaining the telomere length is decisive for the viability and homeostasis process of all the cells of an organism, including human glial cells. Telomere shortening of microglial cells has been widely associated with the onset and progression of neurodegenerative diseases such as Parkinson’s and Alzheimer’s disease. Additionally, traumatic brain injury appears to have a positive correlation with the telomere-shortening process of microglia, and telomere length can be used as a non-invasive biomarker for the clinical management of these patients. Moreover, telomere involvement through telomerase reactivation and homologous recombination also known as the alternative lengthening of telomeres (ALT) has been described in gliomagenesis pathways, and particular focus has been given in the translational significance of these mechanisms in gliomas diagnosis and prognostic classification. Finally, glia telomere shortening is implicated in some psychiatric diseases. Given that telomere dysfunction of glial cells is involved in the central nervous system (CNS) disease pathogenesis, it represents a promising drug target that could lead to the incorporation of new tools in the medicinal arsenal for the management of so far incurable conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Telomeres constitute nucleoprotein structures composed of TTAGGG repeats forming G-overhangs and G-quadruplexes protecting chromosome ends during DNA replication which would otherwise undergo gradual shortening with each division. In that regard, telomeres, often termed the “molecular clock” of cells, shield the genome from the loss of invaluable genetic information through each replication cycle. Telomere integrity is protected by a complex of six proteins (TRF1, TRF2, RAP1, TPP1, TIN2, and POT1) called shelterin [1,2,3]. Telomere length shortening is a physiological process that predominantly occurs in mitotically active somatic cells due to the inability of DNA telomerase (a telomere maintenance enzyme which consists of TERC, an RNA template for DNA synthesis, and TERT, a rate-limiting subunit with reverse transcriptase, and RNA binding catalytic action) to replicate telomere ends. Eventually, they reach a point of no return, where the shelterin cap dissociates, leaving the 3′-overhang exposed to be recognized as DNA breaks, leading to cell cycle arrest or fusion with another chromosome [4]. Hence, perpetual replication is deterred in somatic cells, effectively preventing aberrant cell division and tumorigenesis, inducing replication arrest after a fixed cycle of cell divisions, known as the “Hayflick limit.” Thus, telomeres play a crucial role in physiologic cellular functions to preserve homeostasis through replication aging [1,2,3,4].
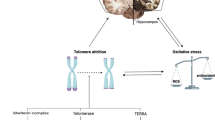
Telomere attrition is a central aspect of the telomere-cellular senescence-aging axis, resulting from semiconservative DNA replication. The consequence is genomic instability and subsequent activation of the DNA damage response pathway (DDR pathway) which drives the cell toward irreversible cell cycle arrest and the allostasis state of “senescence” [5]. Cellular senescence and telomere shortening consist typical hallmarks of cell aging, and consequently organ aging, compromising its regeneration capacity [6,7,8]. Stem cells like neural stem cells and neural progenitor cells maintain telomere length through a high level of telomerase activity and preserve their telomere length and proliferative capacity bypassing the Hayflick limit and achieving cellular immortality [9, 10]. Neurons are considered post-mitotic cells, incapable of dividing (although this statement’s legitimacy remains a controversial issue among scientists), whereas glial cells preserve their mitotic capability [11, 12]. Studies on normal cerebral tissues have shown that neurons demonstrate the longest telomeres and no age-related attrition contrary to telomeres of glial cells in the white matter which show age-related attrition [13]. Among CNS glial cells (astrocytes, microglia, oligodendrocytes), microglial cells are the most mitotically potent cells and thus prone to telomere shortening [14, 15].
Deciphering telomere dynamics is pivotal in unraveling the complex interplay between telomere shortening and various pathologies encountered in the CNS. The regulation of telomeres and telomerase holds significance in cancer neurobiology and age-related processes, shaping the physiological landscape of cell replication and longevity. The aim of this article is to overview the recent reports that refer to the role and possible implication of glial cell telomeres in neurodegenerative, and psychiatric diseases, gliomas, and traumatic brain injury as well as to present relevant telomere-targeting therapeutic strategies for these CNS human diseases.
The Role of Glia Telomere Dysfunction in CNS Neurodegeneration
Microglial cells play a major role in neuroprotection and immunological surveillance of the brain and are activated in various CNS pathologies, including injury, trauma, or stroke to maintain neuronal survival by reinforcing the secretion of trophic factors and cytokines [16]. Accumulating evidence reveals that during brain aging, microglia establish gradually an inflammatory and cytotoxic environment for neurons [17] and are subject to morphological and functional transformation [18]. Moreover, these changes may be predictive of the development of neurodegenerative conditions [18]. Since telomere shortening is one of the major features of aging, this could be considered inductive to the establishment of a dystrophic microglia phenotype [19]. The exact mechanism by which telomere shortening causes microglia senescence is not well-established. Herbig et al., through their experiments in human fibroblasts, demonstrated that the overexpression of the TRF-2 mutant form led to telomere uncapping in the 3′ guanine-rich sequence [20]. This exposed region may initiate DNA damage signals, resulting in the activation of phosphatidylinositol 3-kinase (PI3K)-like protein kinases (PI3KKs), mainly ATM and, to a lesser extent, ATR. These pathways activate the p53 protein and upregulate p21CIP1, a Cdk inhibitor, causing retinoblastoma (RB) hyperphosphorylation and, consequently, cell cycle arrest in the G1 phase. When ATM-P53 is deactivated, the cell cycle initiates again, highlighting its crucial role in cellular senescence including the brain as reviewed by Liu and Saez-Atienzar and Masliah [21, 22].
One of the primary consequences of DNA damage and subsequent cell cycle exit in microglia is the transition to a senescence-associated secretory phenotype (SASP) [23,24,25]. In this state, microglia produce pro-inflammatory cytokines (TNFα, IL-1β, IL-6, and IL-8), influenced by the expression of NF-κΒ, ROS, proteases, and other molecules that could damage the surrounding tissue, leading to apoptosis of neurons and other glial cells. Accumulation of Aβ deposition and neurofibrillary tangles (NFTs) may cause genetic, metabolic, and DNA damage, triggering SASP not only in microglia but also in other brain cell types [17, 18, 23,24,25]. However, it remains controversial whether proteinopathy or cellular senescence occurs first. Indeed, Khan et al. showed that telomere dysfunction in genetically altered mice with TERC gene knock-out (KO) mutations did not correlate with microglia aging or morphological changes of microglial cells although a reduction in microglial cell number was observed [26].
Another effect of aging in microglia is the amplification of its immunogenicity, a condition known as “priming” [27]. Microglial priming induces a neurodegenerative phenotype which demonstrates great relevance to Alzheimer’s disease. Specifically, primed microglia can induce excessive neuroinflammation and accumulation of neurofibrillary tangles due to phosphorylation of tau protein and production of amyloid β (Aβ) disrupting thus neuronal integrity as well as reduction of the release of neurotrophic factors resulting further in loss of normal neurons [28].
Raj et al. examined in a mouse model of telomere shortening whether telomere shortening could initiate an inflammatory response activating microglia and revert it to priming condition [29]. It is well-known that telomere shortening leads to the re-localization of RAP1—a protein structural component of telomeres—from telomeres to extratelomeric genomic sites which may affect gene transcription [30]. Indeed, mice expressing extratelomeric RAP1 show increased production of pro-inflammatory cytokines and chemokines through the NF-kb pathway in brain tissues [31]. However, Raj et al. concluded that telomere shortening does not impair the phenotypic and functional properties of microglia and does not result in microglia priming [29]. Thus, the exact role of microglia telomere dysfunction in CNS neurodegeneration remains elusive, and further research is necessary to clarify this association.
The Role of Microglia Telomere Shortening in Alzheimer’s Disease
It was hypothesized that telomere shortening is paramount in the onset and progression of neurodegenerative diseases such as Alzheimer’s and Parkinson’s disease through mechanisms that impede the function of glia, especially microglial cells [32]. Alzheimer’s dementia (AD) is a neurodegenerative disorder that has been inextricably linked to aging [21, 22]. It is characterized by cognitive impairment, neural cell death, and loss of neuronal synapses due to Aβ amyloid accumulation and neurofibrillin tangles, aggregates of hyperphosphorylated tau proteins [33].
Microglia senescence is considered a major risk factor for AD maintenance and progression, as glial cells lose their neuroprotective capacity during this state [15, 32]. Rolyan et al. using transgenic mouse models demonstrated that, even though telomere shortening is correlated with aged microglia and was expected to precipitate the progression of the disease, it impeded the neurodegenerative phenotype and Αβ plaque accumulation [34]. However, Hu et al. provided evidence of AD pathology associated with a group of senescent microglia cells (the so-called diseased-associated microglia) and that microglial proliferation (linked to telomere shortening) constitutes a risk factor for neurodegeneration. Early-stage inhibition of microglial proliferation in AD-like pathological mice impaired the onset of microglia senescence and diminished amyloid-induced pathology [35].
Given that deficiency of folate, the co-enzyme involved in homocysteine metabolism and nucleotide synthesis is associated with neurodegenerative disorders, including AD, folic acid (the therapeutic form of folate) could be a therapeutic approach for these disorders [36]. Interestingly, recent preliminary in vitro data demonstrate that folic acid decreases astrocyte apoptosis by preventing DNA oxidative stress-induced damage and telomere attrition [37]. Although further studies are needed to confirm these findings in vivo, this study introduced a link between folate deficiency and astrocyte telomere dysfunction in AD [37].
The Role of Microglia Telomere Shortening in Parkinson’s Disease
Parkinson’s disease (PD) is a multifactorial neurodegenerative disorder with a prevalence of 1% in individuals older than 60. The predominant pathophysiological feature of PD is the neuronal loss in the dopaminergic nucleus pars compacta at the substantia nigra, bearing the typical histological finding of Lewy bodies [38]. Five major genes have been associated with familial PD, the most important are the synuclein gene (SNCA), the parkin gene (PARK 2), and the ubiquitin C terminal hydrolase L1 gene (PARK 5). Crucial in the disease pathogenesis is the aggregation of misfolded synuclein proteins within Lewy bodies and Lewy neurites [38].
The association of PD with aging among other established risk factors unfolds a promising landscape to investigate the role of cellular aging in its pathogenesis. A study conducted by Scheffold et al. in a PD mouse model with telomere shortening phenotype (TERC knockout) indicated that earlier onset of synuclein aggregation had taken place with documented defective microglial immune response in the aged brain [39]. Thus, the study introduces the contribution of microglia telomere attrition in PD pathogenesis and adds to the hypothesis that telomere erosion with aging may be a risk factor in neurodegenerative disorders [40].
The Role of Glia Telomere Dysfunction in Glioma Pathogenesis
Genes Involved in Telomere Regulation Are Implicated in Gliomagenesis
According to a case–control study by Wang et al., telomere length in peripheral blood leukocytes correlates with glioma risk [41], which has also been proven in the Mendelian Association and Genome-Wide Association Studies [42,43,44]. More specifically, these studies attribute an increased risk for the development of glioma to genetically increased leukocyte telomere length and identify also numerous polymorphisms in telomere-regulating genes, including, among others, members of the shelterin complex, such as POT1, and the TERT and TERC subunits of telomerase itself. Another notable identified glioma risk locus regarding leukocyte telomere length is PARP1, known not only for its role in DNA repair but also for its ability to regulate the binding of TRF2 (Telomeric repeat-binding factor 2), a shelterin subunit, to telomeric DNA [45]. Additionally, SNPs in the RTEL1 locus—a helicase heavily implied in telomere maintenance—have been associated with high-grade glioma risk [46].
The Role of TERT Promoter and ALT Pathway in Gliomagenesis
Telomere alterations related to gliomagenesis take place via two main pathways: (i) telomerase reactivation and (ii) alternative lengthening of telomeres (ALT). Telomerase reactivation occurs mainly via changes on the TERT gene promoter. Mutations on the TERT promoter itself, among which C228T and C250T are the most common in CNS malignancies, have been shown to create new binding sites for transcription factors, activating, thus, the telomerase synthesis pathway [47]. Additionally, changes outside the TERT gene and its promoter can increase TERT expression, as is the case of THOR (TERT hypermethylated oncological region) hypermethylation [48] (Fig. 1).
Telomerase re-activation as a telomere elongation pathway in cancer. C250T and C228T are the two most common TERT promotor mutations that lead to the creation of new transcription factor binding sites, thus promoting telomerase expression. THOR (TERT hypermethylated oncologic region) is located upstream of the TERT promoter. Its hypermethylation can be enhanced by 2-hydroxyglutarate produced from α-ketoglutarate (α-KG) by mutant IDH1 and induces TERT transcription (created with Biorender.com)
Isocitrate dehydrogenase (IDH) exists in three isoforms (IDH1, IDH2, IDH3) and normally converts isocitrate to α-ketoglutarate (α-KG). When IDH is altered (usually via the R132H gene mutation), it generates 2-hydroxyglutarate (2-HG) from α-KG, which participates in abnormal DNA methylation and ROS-mediated damage. These alterations have been related with tumorigenesis in gliomas [49,50,51]. IDH1 mutations occur in lower-grade astrocytomas and secondary glioblastomas affecting young patients with a generally good prognosis [52]. It has been found that mutant IDH1 astrocytes exhibit an infinite replication potential due to telomere stabilization and high levels of telomerase and c-Myc/Max transcription factor binding on the TERT promoter [51, 53]. Interestingly, epidermal growth factor receptor (EGFR) inhibition in human glioblastoma cells results in a reduction of telomerase activity and telomere shortening and is associated with slower tumor progression in mice in a dose-dependent manner [54].
The ALT pathway accommodates a telomerase-independent, telomere expansion via homologous recombination (Fig. 2). The ALT phenotype includes ALT-associated PML (promyelocytic leukemia) bodies (APBs) on recombination sites, extrachromosomal telomeric ssDNA (C-circles) and telomeric sister chromatid exchange (T-SCEs) [55]. One of the main mutations found in the ALT phenotype is the inactivation of ATRX, which participates in the ATRX/DAXX (alpha-thalassemia/mental retardation syndrome X-linked/death domain-associated protein) chromatin remodeling complex. IDH1 mutations can directly suppress ATRX expression resulting in ALT [56]. Experiments in SV40-transformed fibroblasts indicate that ATRX knockdown increases the percentage of culture immortalization, whereas combined ATRX and DAXX downregulation reduces the time required for immortalization [57]. Thus, ATRX may be an ALT repressor; furthermore, loss of ATRX function cooperates with one or more as-yet-unidentified genetic or epigenetic alterations to activate ALT [57]. ATRX loss has been shown to be associated with ALT in adult and pediatric GBMs [56, 58]. Additionally, IDH1 mutation is necessary for the induction of the ALT phenotype in p53/pRb-deficient ATRX-knockout astrocytes, which acquire the feature of growth on soft agar (a hallmark of glioma) [59]. Moreover, mutant IDH1 is associated with RAP1 (Ras-proximate-1) gene and XRCC1 (X-ray repair cross-complementing 1) gene (responsible for DNA break repair and non-homologous end joining) downregulation which have been proven to play a role in driving the ALT phenotype during gliomagenesis [59].
The alternative lengthening of telomeres pathway in cancer. Loss of shelterin proteins exposes telomeres and allows them to interact with other DNA strands. Homologous recombination at these sites can then occur between sister chromatids which leads to DNA synthesis at telomere ends and thus telomere elongation (created with Biorender.com)
Additionally, general control non-depressible 5 (GCN5) and P300/CBP-associated factor (PCAF) are two largely homologous proteins with opposite effects on the alternative lengthening of telomeres process in human glioma cells [60]. GCN5 binds to ubiquitin-specific peptidase 22 (USP22) which deubiquitinates and thus salvages the telomeric repeat-binding factor 1 (TRF1) shelterin protein. Therefore, telomeres are protected from undergoing structural changes and homologous recombination. Conversely, PCAF increases telomeric instability and may regulate ABP formation, inducing the ALT phenotype [60].
It is worth noting that the activation of the telomere maintenance mechanism (TMM) is dynamic and reflects the plasticity and oncogenicity of tumor cells under internal and external pressures to survive. Thus, TMM in gliomas cannot be defined solely by the combination of telomerase activity and ALT. In fact, during the progression of the disease, gliomas have the capacity to switch from one telomere maintenance mechanism to another [61]. In a comprehensive retrospective cohort study by Kim et al., the TMM landscape unfolded across distinct groups—telomerase-positive, ALT-positive, negative for both telomerase and ALT, and a subset exhibiting both activities contributing to profound intratumoral heterogeneity. Contrary to conventional assumptions, neither TERT promoter mutations nor ATRX loss reliably predicted TMM categories. These findings underscore the intricate and evolving nature of TMM in gliomas suggesting a complex interplay of factors influencing TMM [61]. Importantly, recent findings in pediatric high-grade gliomas (pHGGs) like diffuse intrinsic pontine glioma (DIPG), and telomere maintenance mechanisms exhibit a noteworthy heterogeneity. The coexistence of telomerase and ALT pathways within the same tumor underscores the intricate nature of intratumoral heterogeneity in telomere length and maintenance mechanisms [62].
Diagnostic and Predictive Significance of Telomere Biology in Gliomas
It is of vital importance to differentiate between histologic and genetic subtypes of brain tumors that carry different prognoses and treatment options. In terms of diagnosis, the mutational burden of genes relevant to telomere regulation can be highlighted in tumor histology. Such genetic signatures have been proven useful in the histologic and prognostic classification of gliomas. More specifically, I-CF (IDH1/CIC/FUBP1) tumors are of oligodendroglial origin and carry IDH and at least one of CIC, FUBP1 (far upstream element binding protein 1) or 1p/19q mutations, whereas ATRX and IDH alterations define I-A (IDH1/ATRX) tumors, characterized by astrocytic histology, ALT mutations, and younger age at diagnosis. Furthermore, a heterogeneous category of IDH and ATRX wild-type tumors like glioblastoma multiforme (GBM) was defined as I-X [63]. More recently, analysis of ependymomas suggested that only the loss of ATRX immunoreactivity may be used as evidence against the diagnosis of ependymoma, as these tumors do not exhibit the ALT phenotype [64].
Telomeric G quadruplexes are nucleic acid structures formed between guanine bases and may represent a reliable biomarker in tumors since their formation is more pronounced in the ALT pathway [65]. This enables distinguishing low-grade gliomas in terms of their telomere maintenance mechanism (TMM) in a quick and reliable manner, using Naptho-Template assembled synthetic G-quartet (N-TASQ) probes through immunohistochemistry. ALT-dependent glioma diagnosis could also be achieved by c-circle assay, with the additional advantage of low DNA requirements [66]. 1H-magnetic resonance spectroscopy represents another promising non-invasive strategy, by detecting biomarkers specific to the tumor’s genetic subclassification or benign findings such as gliosis. Hyperpolarized [1-13C]-alanine is metabolized in vivo in either lactate, when the TERT pathway is activated, or pyruvate which is indicative of the ALT pathway [67].
Contrary to previous reports [68, 69], recent data show that activation of the ALT pathway or failure to identify a specific telomere maintenance mechanism is associated with poorer prognosis for glioblastoma patients [70]. However, ATRX loss associated with the ALT phenotype may be another promising marker with prognostic significance, as it is the hallmark of a favorable type of IDH-mutant astrocytomas [71, 72]. Moreover, recent findings introduce the potential existence of different types of ALT based on the level of activity of the pathway as identified by c-circle since the younger patients (25–30 years) with IDH-mutant ATRX-lost anaplastic astrocytoma display higher intensity of ALT compared with 66–70 years-old patients [73]. On the other hand, glioblastomas having progressed from anaplastic astrocytomas do not demonstrate this correlation [73]. Interestingly, further data show the development of ALT without ATRX loss in a subgroup of pediatric high-grade gliomas introducing germline variants in mismatch repair (MMR) genes as the possible cause of increased occurrence of ALT in these patients [74]. In this line, a study in pilocytic astrocytomas demonstrates that ALT-positive/ATRX-negative anaplastic pilocytic astrocytomas are a distinct category of gliomas which is associated with worse overall and recurrence/progression-free survival [75].
TERT promoter mutational status has a prognostic impact in gliomas which is different among the various subtypes of gliomas [47, 72]. Specifically, TERT promoter mutation has been significantly associated with worse survival in IDH-wildtype astrocytomas. In contrast, TERT mutation has been significantly associated with better survival in IDH-mutant astrocytomas and 1p/19q-codeleted oligodendrogliomas [72, 76]. Nevertheless, novel data define molecular subgroups of IDH-wildtype glioblastomas, including a telomerase-positive subgroup driven by TERT structural rearrangements and an ALT-positive subgroup with mutations in ATRX or SMARCAL1 which demonstrate poorer survival compared with IDH-mutant/TERT-wildtype GBMs [77]. In addition, certain TERT polymorphisms are associated with an increased risk of developing GBM, and an association between somatic TERT promoter mutations also results in a reduced OS of patients with primary glioblastoma [78]. Long telomere length and the TERT mutations C228T and C250T are not only indicators of poor survival but also of radioresistance in gliomas [79]. In a previous cohort however, the unfavorable prognosis of glioblastoma patients with TERT activation had been attributed to the older age of the patients and not to the subsequent telomerase activation per se [80]. Importantly, recent evidence confirms the relationship between telomerase activation and the older age of patients with gliomas [61]. Although TERT promoter mutations are extremely rare in pediatric gliomas, increased TERC and TERT expression are associated with decreased ΟS in high-grade tumors [81]. Also, in cerebellar glioblastomas TERT promoter mutation and/or EGFR amplification, ATRX loss, and ALT pathway activation have been reported as independent prognostic factors with ATRX loss of expression, and ALT positivity to associated with a better outcome and TERT/EGFR alterations with a worse outcome of the patients [82].
Shelterin protein expression is also of prognostic and predictive significance for gliomas. Higher-grade gliomas are characterized by increased expression of ACD, a protein known for its involvement in shelterin complex assembly and interaction with telomerase. Upregulation of ACD is associated with poor prognosis and radiosensitivity in glioblastoma [83]. Furthermore, expression of POT1 (protection of telomeres protein 1), another shelterin component, and telomere length are also independent predictors of poor response to photon irradiation for GBM patients [84]. Exome sequencing of glioma patients from families with multiple affected members has identified rare inherited mutations in POT1 as high-penetrance glioma risk factors [85].
Significance of Telomere Biology in Gliomas Treatment
Thousands of genes, among which telomere-regulating genes, have been found to affect sensitivity to temozolomide (TMZ), the standard chemotherapeutic treatment for glial tumors [86]. Telomerase, as one of the main contributors to telomere maintenance, was one of the first to be targeted for treatment purposes in GBM [87]. It is well known that telomerase is involved in TMZ resistance in GBM [88]. GRN163L (Imetelstat) is a common telomerase antagonist capable of crossing the BBB to shorten telomeres and induce cell cycle arrest and cell death, increasing survival [89,90,91]. It also shows synergistic effects with TMZ and radiation therapy [90]. Similarly, the synergistic effect of TMZ combined with the telomerase inhibitor BIBR1532 in vitro, based on a bioinformatical analysis, exhibits anti-proliferative properties in glioma cell lines on its own and especially in combination with TMZ [86]. Interestingly, several telomere or telomerase-targeting treatments have shown effect on tumor cell lines or animal models without affecting telomere length. After short-term treatment with the telomerase inhibitor MST-312, glioma cell lines undergo cell cycle arrest and apoptosis but subsequent adaptations after long-term treatment lead to increased aggressiveness [92]. MST-312 has also been shown to reduce pediatric ependymoma cell populations harvested from surgical specimens [93].
In addition, utilization of modern gene editing tools, such as CRISPR (Clustered Regularly Interspaced Short Palindromic Repeats) methodologies and antisense oligonucleotides pave the way for the application of gene therapy. These techniques, although they are still limited to preclinical studies, are a great example of the feasibility of precise correction of TERT mutations to inhibit CNS tumor growth [94] or hTERT knockdown via AON-Ex726-mediated targeting of the hTERT pre-mRNA splicing mechanism [95]. Promising approaches to TERT targeting for brain tumors including glioblastomas are very thoroughly reviewed recently by Patel et al. [47].
The inhibition of TRF1, a protein of the shelterin complex which is upregulated in GBM by multiple pathways [96], has been detected to impair tumor growth in GBM mouse models without disturbing normal brain function [96, 97]. G quadruplex stabilizers at telomeric ends—with telomestatin being the most representative—have also been studied as therapeutic targets in brain tumors. Specifically, glioma tumor cells are more sensitive to telomestatin than the normal brain parenchyma [98]. In addition, the acridine derivative BRACO-19—one of the most effective and specific ligand for telomeric G4—has been shown to disassemble telomere binding and shelterin proteins leading to telomere damage and reduced glioma cell growth, without affecting normal astrocytes [99]. Another interesting mechanism is that of the G quadruplex ligand CX5461 which reduces telomerase activity by interfering with its transcript splicing process. In this way, GBM cell lines undergo cell cycle arrest and a decrease in their proliferation [100]. Finally, G quadruplex stabilizers may have a synergistic effect with irradiation, as is the case of pentacyclic acridine (RHPS4) in glioblastoma cells [101], whereas TAC, a G-quadruplex ligand, reduces previously radioresistant GBM masses [102].
Arsenic has specific telomere-binding properties and thus arsenic-based compounds constitute another studied strategy. Arsenic trioxide generates reactive oxygen species (ROS) that activate DNA damage response at the telomeres and reduce telomerase activity, thus causing glioma cell senescence, apoptosis, and reduction of their migration and invasion [103]. Previously, Woo et al. had suggested that sodium meta-arsenite (KML001) affects telomere length, as they observed DNA-damage mediated apoptosis and reduction of xenograft tumor burden in combination with temozolomide and irradiation, without systemic toxicities in glioblastoma cells [104].
A common problem in cancer treatment is its recurrence after initial remission. A common mechanism of glioma recurrence is mediated by glioma stem cells (GSCs), a group of non-dividing chemoresistant cells which may however be reactivated after tumor removal. TRF1 [75] and TRF2 [105] inhibition can reduce stemness and increase survival in xenografted mice. Telomestatin selectively dissociates TRF2 from GSCs telomeres leading to telomeric DNA damage in GSCs but not in non-stem glioma cells (NSGCs) [106] and introduces telomeric and non-telomeric DNA damage in the context of failed repair mechanisms, thus reducing their self-renewal capacity and survival in vitro [98]. Similar results in terms of cell viability occur after the introduction of the nucleoside 6-thio-2′deoxyguanosine in stem cells derived from pediatric brain tumors including diffuse gliomas [107]. Recently, low-intensity pulsed ultrasound, a non-invasive method in human use, increased GSC sensitivity to temozolomide in vivo and in vitro by converting oxygen molecules to singlet oxygen that induces telomere shortening [108]. Importantly, recent data associate the ALT pathway with elevated glycolytic flux and demonstrate the ability of [6,6′-2H]-glucose to non-invasively assess tumor burden and response to therapy in astrocytomas [109].
A few research efforts targeting the telomere maintenance mechanism have been translated into early-phase clinical trials in gliomas, with limited success so far [87]. Specifically, NCT01836549 was A phase II clinical trial of imetelstat in various recurrent pediatric CNS tumors, which had to be prematurely terminated, following the death of two of 42 patients due to thrombocytopenia-related intracranial hemorrhage [110]. A telomerase 540–548 peptide vaccine in combination with the granulocyte–macrophage colony-stimulating factor sargamostim has reached phase I studies for adult and pediatric brain tumors and sarcoma but has not yet posted results (NCT00069940). Two additional ongoing trials utilizing telomere-related technologies are worth mentioning: NCT03491683 and NCT04280848. The former is investigating the biological agent INO-5401 comprised of three DNA plasmids each targeting a specific gene in glioblastoma patients, including hTERT. This agent is to be used in combination with another DNA plasmid expressing IL12 and an anti-PD1 monoclonal antibody. NCT04280848 on the other hand is a Phase 2 trial for GBM evaluating UCPVax, a cancer vaccine which relies on the introduction of two hTERT-derived peptides to activate CD4 + T-cells against cancer and have already shown to be safe and highly immunogenic in recent early-phase trial on non-small cell lung cancer [111].
The Role of Glia Telomere Shortening in Traumatic Brain Injury
Traumatic brain injury (TBI) includes a vast category of neurological conditions. The main mechanism of TBI is external mechanical forces to the brain and is of major concern in adolescents of both sexes [112]. TBI is most manifested as mild traumatic brain injury (mTBI) and repeated mTBI (RmTBI), also known as concussion. mTBIs and RmTBIs have been associated with persisting cognitive deficits and increased incidence of neurodegenerative disease [113, 114]. The primary traumatic incident is followed by a secondary injury comprising a neurometabolic cascade which interferes with the initiation of an acute inflammatory response and oxidative stress as well as activation and infiltration of microglia [115, 116].
Relevant literature documents a positive correlation between telomere shortening and mTBI [117, 118]. Specifically, shorter telomeres have been associated with poorer performance in contrast to longer telomeres which have been associated with better performance in juvenile rats following a concussion/mild traumatic brain injury [117]. Furthermore, findings from an injury model of RmTBI in adolescent rats demonstrate a link between RmTBI and significantly shorter telomere length independent of sex [118]. More data highlight the presence of worse sensorimotor deficits and shorter telomeres, in brain specimens of middle-aged TBI rats compared to young ones [119]. However, it is worth mentioning that molecular mechanisms pertaining to telomere maintenance are active in the injured brain since microglia can maintain telomere length via telomerase during periods of high proliferation in vivo [120].
Additional research conducted by Hehar and Mychasiuk demonstrates a strong correlation between telomere length in brain tissues and peripheral skin cells which provides easily obtained samples [117]. It remains to be elucidated if there is a potential clinical use of telomere length as an injury prognosis biomarker. Although recent data are promising for the use of telomere length as a non-invasive biomarker for TBI, RmTBI, and concussion prognosis [117, 118], there are still obstacles to overcome in both pre-clinical models and humans before validated clinical results are acquired. Longitudinal studies with human populations should examine the baseline of telomere length since literature indicates telomere length is responsive to environmental manipulations and inter-individual factors such as prenatal stress [121] and dietary intake [122]. In accordance with this latest finding, a molecular analysis of Mychasiuk et al. demonstrated that diet-induced epigenetic pathways exist and are associated with differences in individual predisposition and resiliency to post-concussion syndrome [122].
Furthermore, vitamin E, an antioxidant agent, has been thought to improve neurological recovery after brain injury and inhibit functional deterioration in aging. More specifically, vitamin E has been shown to increase microglia cell proliferation in vitro providing potential benefits of vitamin E supplementation on microglial renewal capacity during aging or after brain injury [123]. However, these results require further investigation before the effectiveness of vitamin E supplementation in vivo is proven.
The Role of Glial Telomere Length in Psychiatric Diseases
Two glia cell populations (oligodendrocytes and astrocytes) are characterized by differential resilience to biological stressors such as oxidative stress, known to play a role in accelerating telomere shortening [124]. Particularly, telomere lengths in white matter oligodendrocytes, but not astrocytes, from two areas of the brain, the frontal (Brodmann area 10) and temporal lobe (uncinate fasciculus), shown previously to demonstrate pathology in MDD patients, are significantly shorter in major depressive disorder (MDD) patients as compared to matched control donors suggesting a link between telomere shortening and white matter abnormalities described in MDD [124]. In addition, telomere length was found to be significantly reduced in oligodendrocytes from occipital cortical white matter and the immediate region of the locus coeruleus (LC) in the brainstem of MDD donors died by suicide as compared to control donors, in a study of Chandley et al. [125]. Likewise, although no difference of telomere length in the cerebellar gray matter derived from patients with MDD, bipolar disorder (BD), and schizophrenia, (SZ) compared to controls, was found; the telomere length has been detected as significantly shorter in MDD than in BD, SZ, and controls, in a study of Zhang et al. [126]. Moreover, Kronenberg et al. suggested a link between classical microglia activation with repression of telomere-associated genes in animal models of stroke, Alzheimer’s disease, and chronic stress. However, the effects of chronic stress in microglia activation were modest [127].
Previous studies have documented an abundance of shortened telomeres in peripheral blood samples (leukocytes and lymphocytes) of psychiatric patients as reviewed by Lindqvist et al. [128]. Nevertheless, further longitudinal studies in the human brain tissue, even though the limitations, are needed to enrich the knowledge concerning the relation between glial cells, telomere shortening, and possible clinical interventions in the field of psychiatric diseases. The role and implication of glial cell telomeres in neurodegenerative, and psychiatric diseases, gliomas, and traumatic brain injury are summarized in Fig. 3.
Neurodegenerative diseases: Top: schematic illustration of the topological relation between the glial cells and neurons in the CNS. Bottom: telomere shortening leads to microglial shortening and neuroinflammation; Brain tumors: Telomere-related biomarkers aiding in diagnosis, treatment, and prognosis of brain tumors; Psychiatric disorders: Glial telomere shortening is linked to various psychiatric disorders; Traumatic brain injury: Glial telomere length as a biomarker in traumatic brain injury
Conclusion
Although the exact role of glial telomere shortening in brain pathogenesis is—in many cases—yet to be elucidated, ongoing research is bound to offer new perspectives promoting glial cells as key elements in brain physiology and pathophysiology. Furthermore, the already established complex interplay between microglia, other glial cells, as well as neurons in their respective niche reiterates the need to analyze the interactions between cells in their microenvironment to dissect disease pathogenesis. Additional research is needed to detect the extent of telomere shortening and senescence in both glial and neuronal tissue and thus analyze their role in CNS pathology. Mapping the connectome between different cell phenotypes comprising the neural tissue and investigating their molecular state in health and disease will provide further insights in our quest to illuminate the substrate of CNS disorders in the era of precision medicine.
Availability of Data and Materials
Not applicable.
Abbreviations
- ACD:
-
Adrenocortical dysplasia protein homolog
- AD:
-
Alzheimer’s disease
- α-KG:
-
α-Ketoglutarate
- ALT:
-
Alternative lengthening of telomeres
- AON:
-
Antisense oligonucleotide
- APB:
-
ALT-associated promyelocytic leukemia bodies
- ATRX:
-
Alpha-thalassemia/mental retardation syndrome X-linked
- BBB:
-
Blood-brain barrier
- CAT:
-
Catalase
- CNS:
-
Central nervous system
- CRISPR:
-
Clustered regularly interspaced short palindromic repeats
- DAXX:
-
Death domain-associated protein
- DDR:
-
DNA damage response pathway
- EGFR:
-
Epidermal growth factor receptor
- FUBP1:
-
Far upstream element binding protein 1
- GBM:
-
Glioblastoma multiforme
- GPX1:
-
Intracellular glutathione peroxidase
- GCN5:
-
General control non-depressible 5
- GSC:
-
Glioma stem cells
- IDH:
-
Isocitrate dehydrogenase
- KO:
-
Knock-out
- LC:
-
Locus coeruleus
- MDD:
-
Major depressive disorder
- MGMT:
-
O6-methylguanine-DNA methyltransferase
- mTBI:
-
Mild traumatic brain injury
- mTL:
-
Mean telomere length
- NFκB:
-
Nuclear factor-κB
- N-TASQ:
-
Naptho-template assembled synthetic G-quartet
- OS:
-
Overall survival
- PARK 2:
-
Parkin gene 2
- PARK 5:
-
Parkin gene 5
- PCAF:
-
P300/CBP-associated factor
- PD:
-
Parkinson’s disease
- POT1:
-
Protection of telomeres 1
- Rap 1:
-
Ras-proximate-1 or Ras-related protein 1
- RAP1 :
-
Ras-proximate-1
- RmTBI:
-
Repeated mTBI
- ROS:
-
Reactive oxygen species
- SASP :
-
Senescence-associated secretory phenotype
- SOD1:
-
Cytoplasmic superoxide dismutase
- SOD2:
-
Mitochondrial superoxide dismutase
- SNCA:
-
Synuclein gene
- T/A:
-
Relative telomere lengths
- TBI:
-
Traumatic brain injury
- TERC:
-
Telomerase RNA component
- TERF2IP:
-
Telomeric repeat binding factor 2 interacting protein
- TERT:
-
Telomerase reverse transcriptase
- TIN2:
-
TRF1-interacting nuclear protein 2
- THOR :
-
TERT hypermethylated oncological region
- TMM:
-
Telomere maintenance mechanism
- TMZ :
-
Temozolomide
- TPP1:
-
Tripeptidyl-peptidase 1
- TRF1:
-
Telomeric repeat-binding factor 1
- T-SCE:
-
Telomeric sister chromatid exchange
- USP22:
-
Ubiquitin-specific peptidase 22
- XRCC1:
-
X-ray repair cross-complementing 1
References
Stewart JA, Chaiken MF, Wang F, Price CM (2012) Maintaining the end: roles of telomere proteins in end-protection, telomere replication and length regulation. Mutat Res 730(1–2):12–19. https://doi.org/10.1016/j.mrfmmm.2011.08.011
Smith EM, Pendlebury DF, Nandakumar J (2020) Structural biology of telomeres and telomerase. Cell Mol Life Sci 77(1):61–79. https://doi.org/10.1007/s00018-019-03369-x
Lim CJ, Cech TR (2021) Shaping human telomeres: from shelterin and CST complexes to telomeric chromatin organization. Nat Rev Mol Cell Biol 22(4):283–298. https://doi.org/10.1038/s41580-021-00328-y
Turner KJ, Vasu V, Griffin DK (2019) Telomere biology and human phenotype cells. 8(1):73.https://doi.org/10.3390/cells8010073
D’Adda Di Fagagna F, Reaper PM, Clay-Farrace L et al (2003) A DNA damage checkpoint response in telomere-initiated senescence. Nature 426(6963):194–198. https://doi.org/10.1038/nature02118
Victorelli S, Passos JF (2017) Telomeres and cell senescence - size matters Not. EBioMedicine 21:14–20. https://doi.org/10.1016/j.ebiom.2017.03.027
Zhu Y, Liu X, Ding X, Wang F, Geng X (2019) Telomere and its role in the aging pathways: telomere shortening, cell senescence and mitochondria dysfunction. Biogerontology 20(1):1–16. https://doi.org/10.1007/s10522-018-9769-1
Liu J, Wang L, Wang Z, Liu JP (2019) Roles of telomere biology in cell senescence, replicative and chronological ageing. Cells 8(1):54. https://doi.org/10.3390/cells8010054
Zeng X, Rao MS (2007) Human embryonic stem cells: long term stability, absence of senescence and a potential cell source for neural replacement. Neuroscience 145(4):1348–1358. https://doi.org/10.1016/j.neuroscience.2006.09.017
Villa A, Navarro-Galve B, Bueno C, Franco S, Blasco MA, Martinez-Serrano A (2004) Long-term molecular and cellular stability of human neural stem cell lines. Exp Cell Res 294(2):559–570. https://doi.org/10.1016/j.yexcr.2003.11.025
Rakic P (1985) DNA synthesis and cell division in the adult primate brain. Ann NY Acad Sci 457:193–211. https://doi.org/10.1111/j.1749-6632.1985.tb20806.x
Jessen KR (2004) Glial cells. Int J Biochem Cell Biol 36(10):1861–1867. https://doi.org/10.1016/j.biocel.2004.02.023
Tomita K-I, Aida J, Izumiyama-Shimomura N et al (2018) Changes in telomere length with aging in human neurons and glial cells revealed by quantitative fluorescence in situ hybridization analysis. Geriatr Gerontol Int 18:1507–1512. https://doi.org/10.1111/ggi.13500
Flanary BE, Streit WJ (2004) Progressive telomere shortening occurs in cultured rat microglia, but not astrocytes. Glia 45:75–88. https://doi.org/10.1002/GLIA.10301
Flanary B (2005) The role of microglial cellular senescence in the aging and Alzheimer diseased brain. Rejuvenation Res 8:82–85. https://doi.org/10.1089/REJ.2005.8.82
Colonna M, Butovsky O (2017) Microglia function in the central nervous system during health and neurodegeneration. Annu Rev Immunol 35:441–468. https://doi.org/10.1146/annurev-immunol-051116-052358
Cornejo F, von Bernhardi R (2016) Age-dependent changes in the activation and regulation of microglia. Adv Exp Med Biol 949:205–226. https://doi.org/10.1007/978-3-319-40764-7_10
Baron R, Babcock AA, Nemirovsky A et al (2014) Accelerated microglial pathology is associated with Ab plaques in mouse models of Alzheimer’s disease. Aging Cell 584–595.https://doi.org/10.1111/acel.12210
Angelova DM, Brown DR (2019) Microglia and the aging brain: are senescent microglia the key to neurodegeneration? J Neurochem. 151(6):676–688. https://doi.org/10.1111/jnc.14860
Herbig U, Jobling WA, Chen BP, Chen DJ, Sedivy JM (2004) Telomere shortening triggers senescence of human cells through a pathway involving ATM, p53, and p21(CIP1), but not p16(INK4a). Mol Cell 14(4):501–513. https://doi.org/10.1016/s1097-2765(04)00256-4
Liu RM (2022) Aging, cellular senescence, and Alzheimer’s disease. Int J Mol Sci. 23(4):1989. https://doi.org/10.3390/ijms23041989
Saez-Atienzar S, Masliah E (2020) Cellular senescence and Alzheimer disease: the egg and the chicken scenario. Nat Rev Neurosci. 21(8):433–444. https://doi.org/10.1038/s41583-020-0325-z
van Olst L, Verhaege D, Franssen M et al (2020) Microglial activation arises after aggregation of phosphorylated-tau in a neuron-specific P301S tauopathy mouse model. Neurobiol Aging. 89:89–98. https://doi.org/10.1016/j.neurobiolaging.2020.01.003
Hu Y, Fryatt GL, Ghorbani M et al (2021) Replicative senescence dictates the emergence of disease-associated microglia and contributes to Aβ pathology. Cell Rep 35(10):109228. https://doi.org/10.1016/j.celrep.2021.109228
Mendelsohn AR, Larrick JW (2018) Cellular senescence as the key intermediate in Tau-mediated neurodegeneration. Rejuvenation Res 21(6):572–579. https://doi.org/10.1089/rej.2018.2155
Khan AM, Babcock AA, Saeed H et al (2015) Telomere dysfunction reduces microglial numbers without fully inducing an aging phenotype. Neurobiol Aging 36:2164–2175. https://doi.org/10.1016/J.NEUROBIOLAGING.2015.03.008
Norden DM, Godbout JP (2013) Review: microglia of the aged brain: primed to be activated and resistant to regulation. Neuropathol Appl Neurobiol 39(1):19–34. https://doi.org/10.1111/j.1365-2990.2012.01306.x
Li J-W, Zong Y, Cao X-P et al (2018) Microglial priming in Alzheimer’s disease. Ann Transl Med 6:176–176. https://doi.org/10.21037/ATM.2018.04.22
Raj DDA, Moser J, van der Pol SMA et al (2015) Enhanced microglial pro-inflammatory response to lipopolysaccharide correlates with brain infiltration and blood-brain barrier dysregulation in a mouse model of telomere shortening. Aging Cell 14:1003–1013. https://doi.org/10.1111/ACEL.12370
Martinez P, Gomez-Lopez G, Pisano DG, Flores JM, Blasco MA (2016) A genetic interaction between RAP1 and telomerase reveals an unanticipated role for RAP1 in telomere maintenance. Aging Cell 15(6):1113–1125. https://doi.org/10.1111/acel.12517
Stock AJ, McDevitt RA, Puligilla C et al (2022) Aberrant expression and localization of the RAP1 shelterin protein contribute to age-related phenotypes. PLoS Genet 18(11):e1010506. https://doi.org/10.1371/journal.pgen.1010506
Spittau B (2017) Aging microglia—phenotypes, functions and implications for age-related neurodegenerative diseases. Front Aging Neurosci 9:194. https://doi.org/10.3389/FNAGI.2017.00194
Weller J, Budson A (2018) Current understanding of Alzheimer’s disease diagnosis and treatment. F1000Res 7:F1000 Faculty Rev-1161. https://doi.org/10.12688/f1000research.14506.1
Rolyan H, Scheffold A, Heinrich A et al (2011) Telomere shortening reduces Alzheimer’s disease amyloid pathology in mice. Brain 134:2044–2056. https://doi.org/10.1093/BRAIN/AWR133
Hu Y, Fryatt GL, Ghorbani M et al (2021) Replicative senescence dictates the emergence of disease-associated microglia and contributes to Aβ pathology. Cell Rep 35(10):109228. https://doi.org/10.1016/J.CELREP.2021.109228
Kao TT, Chu CY, Lee GH et al (2014) Folate deficiency-induced oxidative stress contributes to neuropathy in young and aged zebrafish - implication in neural tube defects and Alzheimer’s diseases. Neurobiol Dis 71:234–244. https://doi.org/10.1016/j.nbd.2014.08.004
Li W, Ma Y, Li Z et al (2020) Folic acid decreases astrocyte apoptosis by preventing oxidative stress-induced telomere attrition. Int J Mol Sci 21:62. https://doi.org/10.3390/ijms21010062
Samii A, Nutt JG, Ransom BR (2004) Parkinson’s disease. Lancet 363:1783–1793. https://doi.org/10.1016/S0140-6736(04)16305-8
Scheffold A, Holtman IR, Dieni S et al (2016) Telomere shortening leads to an acceleration of synucleinopathy and impaired microglia response in a genetic mouse model. Acta Neuropathol Commun 4(1):87. https://doi.org/10.1186/S40478-016-0364-X
Vellingiri B, Balasubramani K, Iyer M et al (2023) Role of telomeres and telomerase in Parkinson’s disease-a new theranostics? Adv Biol (Weinh) 17:e2300097. https://doi.org/10.1002/adbi.202300097
Wang S, Chen Y, Qu F et al (2014) Association between leukocyte telomere length and glioma risk: a case-control study. Neuro Oncol 16(4):505–512. https://doi.org/10.1093/neuonc/not240
Walsh KM, Codd V, Rice T et al (2015) Longer genotypically-estimated leukocyte telomere length is associated with increased adult glioma risk. Oncotarget 6(40):42468–77. https://doi.org/10.18632/oncotarget.6468
Saunders CN, Kinnersley B, Culliford R et al (2022) Relationship between genetically determined telomere length and glioma risk. Neuro Oncol 24(2):171–181. https://doi.org/10.1093/neuonc/noab208
Chen B, Yan Y, Wang H et al (2023) Association between genetically determined telomere length and health-related outcomes: a systematic review and meta-analysis of Mendelian randomization studies. Aging Cell 22(7):e13874. https://doi.org/10.1111/acel.13874
Gomez M, Wu J, Schreiber V et al (2006) PARP1 Is a TRF2-associated poly(ADP-ribose)polymerase and protects eroded telomeres. Mol Biol Cell 17(4):1686–1696. https://doi.org/10.1091/mbc.e05-07-0672
Wrensch M, Jenkins RB, Chang JS et al (2009) Variants in the CDKN2B and RTEL1 regions are associated with high-grade glioma susceptibility. Nat Genet 41(8):905–908. https://doi.org/10.1038/ng.408
Patel B, Taiwo R, Kim AH, Dunn GP (2020) TERT, a promoter of CNS malignancies. Neurooncol Adv 2(1):1–11. https://doi.org/10.1093/noajnl/vdaa025
Lee DD, Leão R, Komosa M et al (2019) DNA hypermethylation within TERT promoter upregulates TERT expression in cancer. J Clin Investig 129(1):223–229. https://doi.org/10.1172/JCI121303
Dang L, White DW, Gross S et al (2009) Cancer-associated IDH1 mutations produce 2-hydroxyglutarate. Nature 462(7274):739. https://doi.org/10.1038/nature08617
Zhang C, Moore LM, Li X et al (2013) IDH1/2 mutations target a key hallmark of cancer by deregulating cellular metabolism in glioma. Neuro Oncol 15:1114–1126. https://doi.org/10.1093/neuonc/not087
Ohba S, Hirose Y (2018) Association between mutant IDHs and tumorigenesis in gliomas. Med Mol Morphol 51:194–198. https://doi.org/10.1007/s00795-018-0189-8
Parsons DW, Jones S, Zhang X et al (1979) (2008) An integrated genomic analysis of human glioblastoma multiforme. Science 321(5897):1807–1812. https://doi.org/10.1126/science.1164382
Ohba S, Mukherjee J, Johannessen T et al (2016) Mutant IDH1 expression drives TERT promoter reactivation as part of the cellular transformation process. Cancer Res 76:6680–6689. https://doi.org/10.1158/0008-5472.CAN-16-0696
Tian XX, Pang JCS, Zheng J et al (2002) Antisense epidermal growth factor receptor RNA transfection in human glioblastoma cells down-regulates telomerase activity and telomere length. Br J Cancer 86:1328–1332. https://doi.org/10.1038/sj.bjc.6600244
Henson JD, Reddel RR (2010) Assaying and investigating alternative lengthening of telomeres activity in human cells and cancers. FEBS Lett 584:3800–3811. https://doi.org/10.1016/j.febslet.2010.06.009
Ferreira MS, Sørensen MD, Pusch S et al (2020) Alternative lengthening of telomeres is the major telomere maintenance mechanism in astrocytoma with isocitrate dehydrogenase 1 mutation. J Neurooncol 147(1):1–14. https://doi.org/10.1007/s11060-020-03394-y
Napier CE, Huschtscha LI, Harvey A et al (2015) ATRX represses alternative lengthening of telomeres. Oncotarget 6:16543–16558. https://doi.org/10.18632/oncotarget.3846
Schwartzentruber J, Korshunov A, Liu XY et al (2012) Driver mutations in histone H3.3 and chromatin remodelling genes in paediatric glioblastoma. Nature 482:226–231. https://doi.org/10.1038/nature10833
Mukherjee J, Johannessen TC, Ohba S et al (2018) Mutant IDH1 cooperates with ATRX loss to drive the alternative lengthening of telomere phenotype in glioma. Cancer Res 78:2966–2977. https://doi.org/10.1158/0008-5472.CAN-17-2269
Jeitany M, Bakhos-Douaihy D, Silvestre DC et al (2017) Opposite effects of GCN5 and PCAF knockdowns on the alternative mechanism of telomere maintenance. Oncotarget 8:26269–26280. https://doi.org/10.18632/oncotarget.15447
Kim S, Chowdhury T, Jong YuH et al (2022) The telomere maintenance mechanism spectrum and its dynamics in gliomas. Genome Med 14(1):88. https://doi.org/10.1186/s13073-022-01095-x
Umaru B, Sengupta S, Senthil Kumar S, Drissi R (2023) Alternative lengthening of telomeres in pediatric high-grade glioma and therapeutic implications. Cancers 15(12):3070. https://doi.org/10.3390/cancers15123070
Jiao Y, Killela PJ, Reitman ZJ et al (2012) Frequent ATRX, CIC, FUBP1 and IDH1 mutations refine the classification of malignant gliomas. Oncotarget 3(7):709–722. https://doi.org/10.18632/oncotarget.588
Brügger F, Dettmer MS, Neuenschwander M et al (2017) TERT promoter mutations but not the alternative lengthening of telomeres phenotype are present in a subset of ependymomas and are associated with adult onset and progression to ependymosarcoma. J Neuropathol Exp Neurol 76(1):61–66. https://doi.org/10.1093/jnen/nlw106
Yang SY, Chang EYC, Lim J et al (2021) G-quadruplexes mark alternative lengthening of telomeres. NAR Cancer 3(3):zcab031. https://doi.org/10.1093/narcan/zcab031
Fogli A, Demattei MV, Corset L et al (2017) Detection of the alternative lengthening of telomeres pathway in malignant gliomas for improved molecular diagnosis. J Neurooncol 135:381–390. https://doi.org/10.1007/s11060-017-2585-7
Viswanath P, Batsios G, Mukherjee J et al (2021) Non-invasive assessment of telomere maintenance mechanisms in brain tumors. Nat Commun 12:92. https://doi.org/10.1038/s41467-020-20312-y
Hakin-Smith V, Jellinek DA, Levy D et al (2003) Alternative lengthening of telomeres and survival in patients with glioblastoma multiforme. Lancet 361(9360):836–838. https://doi.org/10.1016/s0140-6736(03)12681-5
McDonald KL, McDonnell J, Muntoni A et al (2010) Presence of alternative lengthening of telomeres mechanism in patients with glioblastoma identifies a less aggressive tumor type with longer survival. J Neuropathol Exp Neurol 69(7):729–736. https://doi.org/10.1097/NEN.0b013e3181e576cf
Sung JY, Cheong JH (2021) Pan-cancer analysis of clinical relevance via telomere maintenance mechanism. Int J Mol Sci 22(20):11101. https://doi.org/10.3390/ijms222011101
Wiestler B, Capper D, Holland-Letz T et al (2013) ATRX loss refines the classification of anaplastic gliomas and identifies a subgroup of IDH mutant astrocytic tumors with better prognosis. Acta Neuropathol 126(3):443–451. https://doi.org/10.1007/s00401-013-1156-z
Pekmezci M, Rice T, Molinaro AM et al (2017) Adult infiltrating gliomas with WHO 2016 integrated diagnosis: additional prognostic roles of ATRX and TERT. Acta Neuropathol 133(6):1001–1016. https://doi.org/10.1007/s00401-017-1690-1
Grandin N, Bruno Pereira B, Cohen C et al (2019) The level of activity of the alternative lengthening of telomeres correlates with patient age in IDH-mutant ATRX-loss-of-expression anaplastic astrocytomas. Acta Neuropathol Commun 7(1):175. https://doi.org/10.1186/s40478-019-0833-0
Stundon JL, Ijaz H, Gaonkar KS et al (2022) ALT in pediatric high-grade gliomas can occur without ATRX mutation and is enriched in patients with pathogenic germline MMR variants. Neuro Oncol noac278. https://doi.org/10.1093/neuonc/noac278
Rodriguez FJ, Brosnan-Cashman JA, Allen SJ et al (2019) Alternative lengthening of telomeres, ATRX loss and H3–K27M mutations in histologically defined pilocytic astrocytoma with anaplasia. Brain Pathol 29(1):126–140. https://doi.org/10.1111/bpa.12646
Heidenreich B, Sivaramakrishna Rachakonda P, Hosen I et al (2015) TERT promoter mutations and telomere length in adult malignant gliomas and recurrences. Oncotarget 6:10617–10633. https://doi.org/10.18632/oncotarget.3329
Diplas BH, He X, Brosnan-Cashman JA et al (2018) The genomic landscape of TERT promoter wildtype-IDH wildtype glioblastoma. Nat Commun 9(1):2087. https://doi.org/10.1038/s41467-018-04448-6
Mostrati MA, Malmström A, Lysiak M et al (2015) TERT promoter mutations and polymorphisms as prognostic factors in primary glioblastoma. Oncotarget 6:16663–16673. https://doi.org/10.18632/oncotarget.4389
Gao K, Li G, Qu Y et al (2016) TERT promoter mutations and long telomere length predict poor survival and radiotherapy resistance in gliomas. Oncotarget 7(8):8712–8725. https://doi.org/10.18632/oncotarget.6007
Lötsch D, Ghanim B, Laaber M et al (2013) Prognostic significance of telomerase associated parameters in glioblastoma: effect of patient age. Neuro Oncol 15(4):423–432. https://doi.org/10.1093/neuonc/nos329
Dorris K, Sobo M, Onar-Thomas A et al (2014) Prognostic significance of telomere maintenance mechanisms in pediatric high-grade gliomas. J Neurooncol 117(1):67–76. https://doi.org/10.1007/s11060-014-1374-9
Picart T, Poncet D, Barritault M (2023) Molecular characterization of adult tumors diagnosed as cerebellar glioblastomas identifies subgroups associated with prognosis. Am J Surg Pathol 47(1):131–144. https://doi.org/10.1097/PAS.0000000000001996
Polito F, Cucinotta M, Abbritti RV et al (2018) Silencing of telomere-binding protein adrenocortical dysplasia (ACD) homolog enhances radiosensitivity in glioblastoma cells. Transl Res 202:99–108. https://doi.org/10.1016/j.trsl.2018.07.005
Ferrandon S, Saultier P, Carras J et al (2013) Telomere profiling: toward glioblastoma personalized medicine. Mol Neurobiol 47(1):64–76. https://doi.org/10.1007/s12035-012-8363-9
Walsh KM, Wiencke JK, Lachance DH (2015) Telomere maintenance and the etiology of adult glioma. Neuro Oncol 17(11):1445–1452. https://doi.org/10.1093/neuonc/nov082
Cai HQ, Liu AS, Zhang MJ et al (2020) Identifying predictive gene expression and signature related to temozolomide sensitivity of glioblastomas. Front Oncol 10:669. https://doi.org/10.3389/fonc.2020.00669
Aquilanti E, Kageler L, Wen PY, Matthew Meyerson M (2021) Telomerase as a therapeutic target in glioblastoma. Neuro Oncol 23(12):2004–2013. https://doi.org/10.1093/neuonc/noab203
Kanzawa T, Germano IM, Kondo Y et al (2003) Inhibition of telomerase activity in malignant glioma cells correlates with their sensitivity to temozolomide. Br J Cancer 89:922–929. https://doi.org/10.1038/sj.bjc.6601193
Castelo-Branco P, Zhang C, Lipman T et al (2011) Neural tumor-initiating cells have distinct telomere maintenance and can be safely targeted for telomerase inhibition. Clin Cancer Res 17(1):111–121. https://doi.org/10.1158/1078-0432.CCR-10-2075
Marian CO, Cho SK, Mcellin BM et al (2010) The telomerase antagonist, imetelstat, efficiently targets glioblastoma tumor-initiating cells leading to decreased proliferation and tumor growth. Clin Cancer Res 16(1):154–163. https://doi.org/10.1158/1078-0432.CCR-09-2850
Barszczyk M, Buczkowicz P, Castelo-Branco P et al (2014) Telomerase inhibition abolishes the tumorigenicity of pediatric ependymoma tumor-initiating cells. Acta Neuropathol 128(6):863–77. https://doi.org/10.1007/s00401-014-1327-6
Andrade da Mota TH, Reis Guimarães AF, Silva de Carvalho AÉ et al (2021) Effects of in vitro short- and long-term treatment with telomerase inhibitor in U-251 glioma cells. Tumour Biol 43(1):327–340. https://doi.org/10.3233/TUB-211515
Wong VCH, Morrison A, Tabori U, Hawkins CE (2010) Telomerase inhibition as a novel therapy for pediatric ependymoma. Brain Pathol 20(4):780–786. https://doi.org/10.1111/j.1750-3639.2010.00372.x
Li X, Qian X, Wang B et al (2020) Programmable base editing of mutated TERT promoter inhibits brain tumour growth. Nat Cell Biol 22(3):282–288. https://doi.org/10.1038/s41556-020-0471-6
Wang F, Cheng Y, Zhang C et al (2019) A novel antisense oligonucleotide anchored on the intronic splicing enhancer of hTERT pre-mRNA inhibits telomerase activity and induces apoptosis in glioma cells. J Neurooncol 143(1):57–68. https://doi.org/10.1007/s11060-019-03150-x
Bejarano L, Schuhmacher AJ, Méndez M et al (2017) Inhibition of TRF1 telomere protein impairs tumor initiation and progression in glioblastoma mouse models and patient-derived xenografts. Cancer Cell 32(5):590–607. https://doi.org/10.1016/j.ccell.2017.10.006
Bejarano L, Bosso G, Louzame J et al (2019) Multiple cancer pathways regulate telomere protection. EMBO Mol Med 11(7):e10292. https://doi.org/10.15252/emmm.201910292
Miyazaki T, Pan Y, Joshi K et al (2012) Telomestatin impairs glioma stem cell survival and growth through the disruption of telomeric G-quadruplex and inhibition of the proto-oncogene, c-Myb. Clin Cancer Res 18(5):1268–1280. https://doi.org/10.1158/1078-0432.CCR-11-1795
Zhou G, Liu X, Li Y et al (2016) Telomere targeting with a novel G-quadruplex-interactive ligand BRACO-19 induces T-Loop disassembly and telomerase displacement in human glioblastoma cells. Oncotarget 7(12):14925–14939. https://doi.org/10.18632/oncotarget.7483
Li G, Shen J, Cao J et al (2018) Alternative splicing of human telomerase reverse transcriptase in gliomas and its modulation mediated by CX-5461. J Exp Clin Cancer Res 37:78. https://doi.org/10.1186/s13046-018-0749-8
Berardinelli F, Sgura A, Facoetti A et al (2018) The G-quadruplex-stabilizing ligand RHPS4 enhances sensitivity of U251MG glioblastoma cells to clinical carbon ion beams. FEBS J 285(7):1226–1236. https://doi.org/10.1111/febs.14415
Merle P, Evrard B, Petitjean A et al (2011) Telomere targeting with a new G4 ligand enhances radiation-induced killing of human glioblastoma cells. Mol Cancer Ther 10(10):1784–1795. https://doi.org/10.1158/1535-7163.MCT-10-0664
Cheng Y, Li Y, Ma C et al (2016) Arsenic trioxide inhibits glioma cell growth through induction of telomerase displacement and telomere dysfunction. Oncotarget 7(11):12682–92. https://doi.org/10.18632/oncotarget.7259
Woo SR, Ham Y, Kang W et al (2014) KML001, a telomere-targeting drug, sensitizes glioblastoma cells to temozolomide chemotherapy and radiotherapy through DNA damage and apoptosis. Biomed Res Int 2014:747415. https://doi.org/10.1155/2014/747415
Bai Y, Lathia JD, Zhang P et al (2014) Molecular targeting of TRF2 suppresses the growth and tumorigenesis of glioblastoma stem cells. Glia 62(10):1687–1698. https://doi.org/10.1002/glia.22708
Hasegawa D, Okabe S, Okamoto K et al (2016) G-quadruplex ligand-induced DNA damage response coupled with telomere dysfunction and replication stress in glioma stem cells. Biochem Biophys Res Commun 471(1):75–81. https://doi.org/10.1016/j.bbrc.2016.01.176
Sengupta S, Sobo M, Lee K et al (2018) Induced telomere damage to treat telomerase expressing therapy-resistant pediatric brain tumors. Mol Cancer Ther 17(7):1504–1514. https://doi.org/10.1158/1535-7163.MCT-17-0792
Song S, Ma D, Xu L et al (2022) Low-intensity pulsed ultrasound-generated singlet oxygen induces telomere damage leading to glioma stem cell awakening from quiescence. iScience 25(1):103558. https://doi.org/10.1016/j.isci.2021.103558
Taglang C, Batsios G, Mukherjee J et al (2022) Deuterium magnetic resonance spectroscopy enables noninvasive metabolic imaging of tumor burden and response to therapy in low-grade gliomas. Neuro Oncol 24(7):1101–1112. https://doi.org/10.1093/neuonc/noac022
Salloum R, Hummel TR, Kumar SS et al (2016) A molecular biology and phase II study of imetelstat (GRN163L) in children with recurrent or refractory central nervous system malignancies: a pediatric brain tumor consortium study. J Neurooncol 129(3):443–451. https://doi.org/10.1007/s11060-016-2189-7
Adotévi O, Vernerey D, Jacoulet P et al (2023) Safety, immunogenicity, and 1-year efficacy of universal cancer peptide-based vaccine in patients with refractory advanced non-small-cell lung cancer: a phase Ib/phase IIa De-Escalation study. J Clin Oncol 41(2):373–384. https://doi.org/10.1200/JCO.22.00096
Jordan BD (2013) The clinical spectrum of sport-related traumatic brain injury. Nat Rev Neurol 9:222–230. https://doi.org/10.1038/nrneurol.2013.33
McInnes K, Friesen CL, MacKenzie DE et al (2017) Mild traumatic brain injury (mTBI) and chronic cognitive impairment: a scoping review. PLoS ONE 12(4):e0174847. https://doi.org/10.1371/journal.pone.0174847
Fehily B, Fitzgerald M (2017) Repeated mild traumatic brain injury: potential mechanisms of damage. Cell Transplant 26(7):1131–1155. https://doi.org/10.1177/0963689717714092
Lenzlinger PM, Morganti-Kossmann MC, Laurer HL, McIntosh TK (2001) The duality of the inflammatory response to traumatic brain injury. Mol Neurobiol 24(1–3):169–181. https://doi.org/10.1385/MN:24:1-3:169
Giza CC, Hovda DA (2014) The new neurometabolic cascade of concussion. Neurosurgery 75:S24–S33. https://doi.org/10.1227/NEU.0000000000000505
Hehar H, Mychasiuk R (2016) The use of telomere length as a predictive biomarker for injury prognosis in juvenile rats following a concussion/mild traumatic brain injury. Neurobiol Dis 87:11–18. https://doi.org/10.1016/j.nbd.2015.12.007
Wright DK, O’Brien TJ, Mychasiuk R, Shultz SR (2018) Telomere length and advanced diffusion MRI as biomarkers for repetitive mild traumatic brain injury in adolescent rats. Neuroimage Clin 18:315–324. https://doi.org/10.1016/j.nicl.2018.01.033
Sun M, Brady RD, Casillas-Espinosa PM et al (2019) Aged rats have an altered immune response and worse outcomes after traumatic brain injury. Brain Behav Immun 80:536–550. https://doi.org/10.1016/j.bbi.2019.04.038
Flanary BE, Streit WJ (2005) Effects of axotomy on telomere length, telomerase activity, and protein in activated microglia. J Neurosci Res 82(2):160–171. https://doi.org/10.1002/jnr.20636
Entringer S, Buss C, Wadhwa PD (2012) Prenatal stress, telomere biology, and fetal programming of health and disease risk. Sci Signal 5(248):pt12. https://doi.org/10.1126/scisignal.2003580
Mychasiuk R, Hehar H, Ma I, Esser MJ (2015) Dietary intake alters behavioral recovery and gene expression profiles in the brain of juvenile rats that have experienced a concussion. Front Behav Neurosci 9:1–17. https://doi.org/10.3389/fnbeh.2015.00017
Flanary BE, Streit WJ (2006) Alpha-tocopherol (vitamin E) induces rapid, nonsustained proliferation in cultured rat microglia. Glia 53(6):669–674. https://doi.org/10.1002/glia.20313
Szebeni A, Szebeni K, DiPeri T et al (2014) Shortened telomere length in white matter oligodendrocytes in major depression: potential role of oxidative stress. Int J Neuropsychopharmacol 17(10):1579–1589. https://doi.org/10.1017/S1461145714000698
Chandley MJ, Szebeni A, Szebeni K et al (2022) Markers of elevated oxidative stress in oligodendrocytes captured from the brainstem and occipital cortex in major depressive disorder and suicide. Prog Neuropsychopharmacol Biol Psychiatry 117:110559. https://doi.org/10.1016/j.pnpbp.2022.110559
Zhang D, Cheng L, Craig DW et al (2010) Cerebellar telomere length and psychiatric disorders. Behav Genet 40(2):250–254. https://doi.org/10.1007/s10519-010-9338-0
Kronenberg G, Uhlemann R, Schöner J et al (2017) Repression of telomere-associated genes by microglia activation in neuropsychiatric disease. Eur Arch Psychiatry Clin Neurosci 267:473–477. https://doi.org/10.1007/s00406-016-0750-1
Lindqvist D, Epel ES, Mellon SH et al (2015) Psychiatric disorders and leukocyte telomere length: Underlying mechanisms linking mental illness with cellular aging. Neurosci Biobehav Rev 55:333–64. https://doi.org/10.1016/j.neubiorev.2015.05.007
Funding
Open access funding provided by HEAL-Link Greece.
Author information
Authors and Affiliations
Contributions
MAP, AB, I-AL, and MA contributed to the study conception and design. Material preparation, data collection, and analysis were performed by MAP, AB, I-AL, and KB. The first draft of the manuscript was written by MAP, AB, I-AL, and all authors commented on previous versions of the manuscript. MA critically edited and reviewed the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Manthia A. Papageorgakopoulou, Angelina Bania, and Ioanna-Aglaia Lagogianni contributed equally to this manuscript as the first authors.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Papageorgakopoulou, M.A., Bania, A., Lagogianni, IA. et al. The Role of Glia Telomere Dysfunction in the Pathogenesis of Central Nervous System Diseases. Mol Neurobiol 61, 5868–5881 (2024). https://doi.org/10.1007/s12035-024-03947-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-024-03947-6