Abstract
Introduction
Posaconazole is superior to fluconazole (FLU) and itraconazole (ITRA) in the prevention of invasive fungal diseases (IFDs) in neutropenic patients with acute myelogenous leukemia (AML) and myelodysplastic syndrome (MDS). A new tablet formulation of posaconazole with improved pharmacokinetic and pharmacodynamic properties compared to posaconazole oral solution has recently been approved. The objective of this study is to estimate the cost-effectiveness of the newly developed posaconazole tablets versus FLU oral suspension or ITRA oral solution for preventing IFDs in high-risk neutropenic patients with AML or MDS and from the perspective of the Spanish National Health System (NHS).
Methods
A previously validated economic model was used. The probabilities of experiencing an IFD, an IFD-related death or death from other causes over 100 days were based on clinical trial data and input into a decision tree. Surviving patients were entered into a Markov model to calculate total costs, number of IFDs and number of life-years gained per patient over a lifetime horizon in each disease and treatment group. Two health states, alive and dead, were considered. Health effects were discounted using a rate of 3%. Univariate and probabilistic sensitivity analyses were conducted.
Results
During the first 100 days, posaconazole tablets were associated with a lower risk of IFDs (0.046 vs. 0.111), longer life expectancy (2.92 vs. 2.69 years) and lower total costs (€5906.06 vs. €7847.20 per patient) over the patients’ lifetimes compared to FLU or ITRA treatments. Thus, posaconazole tablets were more effective and less costly than FLU or ITRA. Probabilistic sensitivity analysis indicated that there was a 79.9% probability of posaconazole tablets being cost-saving compared to FLU or ITRA.
Conclusion
From the Spanish NHS perspective, posaconazole tablets are cost-effective compared to FLU or ITRA in AML or MSD patients with chemotherapy-induced neutropenia and at high risk for IFDs.
Funding
MSD Sharp & Dohme.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with acute myelogenous leukemia (AML) or myelodysplastic syndrome (MDS) who receive intense chemotherapy are at a considerably increased risk of acquiring life-threatening invasive fungal diseases (IFDs) due to drug-induced neutropenia [1, 2]. To date, yeast have been considered the main cause of IFDs, most attributed to Candida albicans [3, 4]; however, recently, epidemiological findings have indicated an increasing number of infections caused by molds [5, 6], with Aspergillus spp. the main pathogen, in addition to other opportunistic fungal pathogens such as Fusarium spp. and Zygomycetes [7, 8]. IFDs have been associated with decreased overall survival (OS) and reduced chances of achieving complete remission (CR) in AML patients [9,10,11]. Although the prognosis for patients with IFDs has improved considerably in recent years, it still remains a significant cause of death among hematologic cancer patients [12].
Over the past 20 years, increasingly more active and less toxic antifungal agents have been developed and used as standard antifungal prophylaxis, including fluconazole (FLU) or itraconazole (ITRA), reducing overall fungal-related morbidity and mortality [13, 14]. Posaconazole is a new-generation oral wide-spectrum azole that has demonstrated superiority in terms of efficacy and safety compared to FLU and ITRA for preventing IFDs in patients with neutropenia who were undergoing remission–induction chemotherapy for AML or MDS [15]. It appears in recognized international guidelines for antifungal prophylaxis with the highest grade of recommendation (AI level/strong recommendation, high-quality evidence/ 1), for patients with AML or MDS treated with intensive chemotherapy and for allogeneic stem cell recipients with graft versus host disease receiving intensive immunosuppression [16,17,18]. From a cost-effectiveness perspective, oral posaconazole has been found to be a potentially cost-saving IFD prophylactic strategy compared to ITRA and FLU in high-risk AML or MDS neutropenic patients due to its lower cost and greater efficacy [19].
A new formulation of oral posaconazole has recently been approved (posaconazole solid tablets), which offers several advantages over oral suspension, such as dosage; posaconazole tablets are dosed at 200 mg once daily, while the posaconazole oral suspension (300 mg) needs to be taken three times per day with a full meal [20]. In addition, the tablet formulation is associated with less interpatient pharmacokinetic variability, better systemic availability, absorption that is unaffected by changes in gastric pH or motility and higher and more consistent plasma drug concentrations [21]. Further, posaconazole tablets once daily is well tolerated and has demonstrated a safety profile similar to that reported for posaconazole oral solution [22].
The aim of this economic evaluation is to assess the cost-effectiveness of the newly developed posaconazole solid oral tablets compared to the oral formulations of FLU and ITRA for preventing IFDs among high-risk patients with AML or MDS and chemotherapy-induced neutropenia from the perspective of the Spanish National Healthcare System (NHS).
Methods
An economic model was constructed in Microsoft Excel 2003 for Windows® to assess the cost-effectiveness of posaconazole solid oral tablets versus fluconazole solid oral tablets or itraconazole oral solution as prophylactic treatment for IFDs in patients with AML or MDS and chemotherapy-induced neutropenia. Originally developed for another country, data were adapted to reflect usual clinical practice in the public health care system in Spain.
Structure
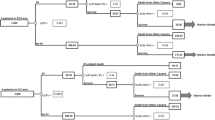
The model consisted of two integrated components: a decision tree and a Markov simulation model (Fig. 1). Based on the pivotal clinical trial designed to compare the efficacy and safety of posaconazole oral suspension versus ITRA or FLU in the prophylaxis of IFDs in patients with neutropenia [15], a hypothetical cohort of AML and MDS patients were entered into the decision tree and were randomly assigned to receive either posaconazole oral tablets or oral ITRA or FLU for 100 days. Four outcomes were possible: to develop an IFD, to die from an IFD, to survive an IFD or to die from causes unrelated to IFD. The probability of reaching any of the stipulated clinical events was taken from the same clinical trial [15]. Results were expressed in terms of the number of IFDs avoided, costs per IFD avoided and number of IFD-related and -unrelated deaths.
Following the initial 100 days, surviving patients were entered in a Markov model that extrapolated the results of the clinical trial to simulate the progression of the disease over the course of AML and MDS patients’ lifetimes, respectively. Two health states were defined: dead or alive. Transition probabilities were based on the estimated mortality rates for the general population in Spain [23] and for AML [24] and MDS [25] patients, respectively. The time horizon was the usual expected survival time for AML and MDS patients. The perspective for the analysis was that of the NHS in Spain. Results were expressed in terms of life-years gained (LYG) and of costs per LYG. Given that it was assumed that costs estimated for the first 100 days would remain unchanged throughout the rest of the model time horizon, a discount rate of 3% was applied only to clinical benefits [26].
Study Population
Patients included in the model had either AML or MDS and chemotherapy-induced neutropenia with a high risk for developing an IFD. The proportion of patients having MDS as the primary diagnosis was 14.45% patients (mean), based on the proportion enrolled in the clinical trial [15]. Likewise, the baseline characteristics of the population included in the model were based on those of the population from the original clinical study [15]. Hence, median age at the beginning of the prophylaxis treatment was different for each treatment arm (53 years for posaconazole, 52 for fluconazole and 54 for itraconazole); a mean value of 53 years was used in the model. Proportions of 52, 53 and 55% of patients treated with posaconazole, fluconazole anditraconazole, respectively, were male; a mean value of 52.82% was applied.
Clinical and Survival Data
Clinical data were also taken from the aforementioned clinical trial [15]. This was a prospective, randomized, multicenter study in which 304 patients were assigned to receive posaconazole [200 mg posaconazole in an oral suspension three times a day (total daily dose: 600 mg)] and 298 patients were given FLU (81%) [400 mg fluconazole in an oral suspension once a day (total daily dose: 400 mg)] or ITRA (19%) [200 mg itraconazole in an oral solution twice a day (total daily dose: 400 mg)]. Prophylaxis was administered with each chemotherapy cycle and was continued until recovery from neutropenia and complete remission or until occurrence of an IFD or for up to 12 weeks post-randomization, whichever came first. Clinical data used to feed into the model were extracted from the 100-day follow-up after randomization in the clinical trial, which already showed a significant improvement in the overall survival for patients receiving posaconazole relative to the fluconazole/itraconazole arms. Probability of death per year in each disease group was estimated by adding the mortality rate associated with an underlying diagnosis of AML or MDS, respectively, to the all-cause death rate in the general population in Spain [23,24,25]. All data used are summarized in Table 1.
Costs
Both the pharmacological costs of the prophylaxis treatment and the costs of treating an IFD episode were considered in the model.
Table 2 shows the estimated pharmacological costs per day for each antifungal agent and treatment duration. Costs of anti-fungals (ex-factory price) were taken from local sources for the costs of the drugs [27]. Treatment duration and dosing were based on clinical trials [15] and on the Summary of Product Characteristics (SmPC) [28,29,30].
The costs of IFD episodes included pharmacological costs, hospitalizations and laboratory tests, as described in an earlier Spanish publication [19]. All costs are expressed in terms of euros at October 2015 values [31].
Assumptions
As the clinical data used to feed into the model related to the first 100 days after the beginning of treatment, both the incidence of IFDs and the costs associated with prophylaxis for and management of the IFDs were assumed to occur during this period, remaining unchanged from then on. The survival rate for AML and MDS patients was obtained by extrapolating the 5-year relative survival data, assuming linear decrease throughout the modeling. Due to a lack of clinical evidence, the duration and efficacy of treatment with posaconazole solid oral tablets was assumed to be similar to that of its analogous oral suspension. In the authors’ opinion, the tablet formulation of itraconazole was not recommended as a substitute for the oral suspension or solution, so the latter was used for the analysis. Although tablets of fluconazole are a valid substitute in real clinical practice, in order to avoid unnecessary assumptions about efficacy, oral suspension of fluconazole was used for the analysis.
Data Validation
All the assumptions that were made as well as the clinical and economic data used to feed the model were validated by four of the authors (R.C., M.J., J.S., S.G.).
Base Case
For the base case, data summarized in Tables 1 and 2 were used to estimate the costs per IFD avoided during the first 100 days for the whole cohort and the costs per LYGs for AML and MDS patients over their lifetime.
Incremental Cost-Effectiveness
The cost-effectiveness of posaconazole tablets compared to oral ITRA or FLU was measured using the incremental cost-effectiveness ratio (ICER), which represents the incremental cost per incremental clinical benefit of one alternative versus another. In this case, both IFD avoided and LYGs were considered as units of clinical benefit. The decision tree was used to calculate the incremental cost per IFD avoided with posaconazole tablets compared to oral ITRA or FLU for the initial 100 days of therapy. The Markov simulation was used to estimate the incremental cost per LYG over the course of the patients’ lifetimes.
Sensitivity Analysis
One-way (OWSA) and probabilistic sensitivity analyses (PSA) were conducted to assess the stability of the results beyond the 100-day period under the uncertainty arising from the values adopted for the input parameters. For the OWSA, clinical data values varied between a ±25% minimum and maximum of the base-case value, while economic data changed ±10% from base-case. As an exception, some variables (5-year overall survival with AML or MDS, costs of IFDs, duration of treatment and discount rate) were assigned alternative values based on the literature review and the experts’ opinion (Table 3). For the PSA, the input parameters were assigned random values following a determined probability distribution (Tables 1, 2), and run for 1000 simulations to evaluate the ICER in each case. A scatterplot and an acceptability curve were used to graphically represent the variability of the cost-effectiveness results. The cost-effectiveness threshold of €30.000 per LYG was considered as the limit commonly accepted in Spain [35].
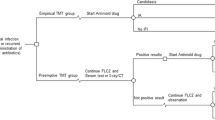
Additionally, three alternative scenarios were defined to test the consistency of the results in specific conditions in order to emulate more realistic clinical situations, in the opinion of the study’s experts. The 5-year relative survival data obtained from the bibliography [24, 25] for AML and MDS patients was used in the base scenario to estimate a 1-year relative survival rate, which was then extrapolated to the patients’ life expectancy. An assumption of linearity over time of the relative survival rate was questionable, so a first alternative scenario was designed to test economic results for a 5-year time horizon, avoiding the extrapolation (scenario 1). A second alternative scenario was designed using Kaplan–Meier curves, instead of the linear assumption made for relative survival, maintaining a 5-year time horizon (scenario 2). Finally, a third scenario was tested to introduce the use of intravenous formulations in patients who may be intolerant to the oral treatments for the first days of the chemotherapy cycle as frequently occurs in clinical practice (scenario 3). To build scenario 2, Kaplan–Meier curves (Figs. 2, 3) were obtained from the literature [36, 37] and approximated to logarithmic curves (R = 0.9193 and R = 0.9449, respectively). For scenario 3, the proportion of patients receiving IV anti-fungals and duration of the IV treatment was taken from the clinical trial [15]. Doses were taken from the corresponding SmPC, and costs of the IV formulation were obtained from local sources (Table 4). Loading doses and mean costs for different presentations were considered for the calculations.
Compliance with Ethics Guidelines
This article does not contain any new studies with human or animal subjects performed by any of the authors.
Results
Base Case Analysis
For the base case scenario, the analysis of the initial 100 days of prophylaxis treatment indicated a reduction in the probability of having an IFD with posaconazole tablets compared to oral ITRA or FLU (0.046 vs. 0.111), with total costs also decreasing with oral posaconazole (€5906.06 vs. €7854.43). The Markov simulation showed that life-expectancy increased (2.922 vs. 2.694 years) with posaconazole oral tablets compared to oral ITRA or FLU. In consequence, given the gains in health benefits and its comparatively lower cost, prophylaxis with posaconazole oral tablets was a dominant alternative compared to oral ITRA or FLU in AML or MDS neutropenic patients at high risk of developing IFDs in the Spanish NHS (cost-effectiveness ratio of €8545.5 per LYG) (Table 5).
One-Way Sensitivity Analysis
IFD costs were the only factor compromising the dominance of posaconazole oral tablets in the OWSA, showing that oral posaconazole might be more efficacious although more expensive than oral ITRA or FLU when the cost of IFDs decreased below €39,750 (−43%). Even when the alternative value for the cost of IFDs was considered (€19,900) [34], the ICER was still €5615.08/LYG, well below the threshold value of €30,000 (Table 6).
Other parameters that may jeopardize the dominance of posaconazole tablets were the probability of an IFD, the probability of non-IFD-related death and the daily cost of posaconazole, although at variances of more than 40% from the base-case value (Table 7). The rest of the parameters were not found to be compromising relative to their natural extreme values.
Probabilistic Sensitivity Analysis
Under the clinical and economic conditions posed in the model, the scatterplot (Fig. 4) shows that posaconazole oral tablets have a 79.9% probability of being dominant (i.e. more effective and less expensive than oral fluconazole or itraconazole formulations) and a 19.2% probability of being more effective albeit more costly than oral ITRA or FLU. The acceptability curve (Fig. 5) indicates that posaconazole oral tablets would have a 97.2% probability of being the cost-effective alternative in Spain, when the threshold value of €30,000/LYG is considered.
Cost-effectiveness scatterplot of posaconazol tablets versus oral FLU/ITRA. The scatter plot represents the value of one variable against the value of another to show the relationship between two variables (incremental costs against incremental LYG of posaconazol tablets compared to FLU/ITRA oral formulations). The cloud of dots in the southeast quadrant indicates more LYG at lower costs for posaconazole tablets for the vast majority of the clinical cases modeled and represented by each individual dot)
Alternative Scenarios
Scenario 1
When a time horizon of 5 years was considered, the incremental number of LYGs for posaconazole tablets versus oral FLU/ITRA was reduced from 0.234 to 0.183, from 0.195 to 0.164 and from 0.228 to 0.180 for patients with AML, with MDS and with both AML and MDS, respectively, as compared to the base-case scenario. However, total costs remained unchanged and posaconazole oral tablets remained dominant compared to oral ITRA or FLU.
Scenario 2
When survival of AML and MDS patients during a time horizon of 5 years was estimated using an approximation of the OS curves obtained from the literature, incremental LYGs were reduced from 0.234 to 0.139, from 0.195 to 0.103 and from 0.228 to 0.134 for patients with AML, with MDS and with both AML and MDS, respectively, compared to the base-case scenario. Again, total costs remain unchanged and posaconazole oral tablets remained dominant compared to oral ITRA or FLU.
Scenario 3
Use of IV formulation was taken into account in this scenario (Table 4). Considering the use of the intravenous formulation for some patients who were intolerant to the oral route during the first days of the chemotherapy cycle slightly increased the total costs of the prophylaxis treatment (from €5906.06 to €5956.16 for posaconazole, and from €7854.43 to €7863.61 for FLU or ITRA). Thus, the use of intravenous formulations for some of the days of the prophylactic treatment and for a proportion of patients intolerant to the oral administration [15] led to slightly increased total costs for both comparator arms, but still resulted in posaconazole being cost-effective.
Discussion
The results of our analysis showed that, for the prevention of IFD in patients with AML/MDS treated with intensive chemotherapy, the new formulation of posaconazole tablets was more efficacious (59%) and less costly (25%) in comparison with ITRA or FLU, maintaining its cost-effective advantage under varying or uncertain conditions.
The analysis of cost-effectiveness beyond the initial prophylaxis treatment resulted in an ICER of €8545.50 per LYG for posaconazole tablets versus oral ITRA or FLU, which is far below the accepted ICER threshold in Spain (€30.000 per LYG). These findings confirmed posaconazole tablets as a highly cost-effective alternative for prophylactic treatment of high-risk AML or MDS neutropenic patients, as previously reported [19, 38].
The robustness of the cost-effectiveness evaluation was further enhanced by probabilistic and one-way sensitivity analyses along with the use of three alternative scenarios to the base-case. In this regard, when a more realistic time horizon was evaluated in the Markov simulation, avoiding extrapolation (scenario 1) and the assumption of linearity (scenario 2) over the lifetimes of AML and MDS patients, posaconazole also proved to be dominant compared to oral ITRA or FLU. Furthermore, when intravenous formulations were applied for the proportion of patients intolerant to the oral administration in scenario 3, the cost-effectiveness of posaconazole remained despite the cost increase associated with IV therapy.
Results from the probabilistic sensitivity analysis indicated that the likelihood for posaconazole oral tablets losing its dominance over oral ITRA and FLU is fairly low under the conditions defined for the base-case scenario. In similar healthcare cost environments in which both drug costs and overall IFD treatment costs are high, posaconazole tablets are a cost-effective alternative to oral ITRA or FLU in the prevention of IFD [38, 39]. Increasing the costs of oral posaconazole would make it more expensive than oral ITRA or FLU, but it would still remain cost-effective in most cases given its clinical superiority. Recent evidence shows that posaconazole prophylaxis lowered total medical costs and even provided a saving in costs during the hospitalization of patients surviving IFDs (p = 0.010) [40].
In the one-way sensitivity analysis, the incremental cost-effectiveness ratio was more sensitive to changes in the costs of IFD; however, the ICER stayed well below the threshold value of €30,000 (€5615.08/LYG), revealing that routine use of posaconazole oral tablets would be a cost-saving prophylactic alternative when the likelihood of IFD or the cost of treatment medications are expected to be particularly high. This result aligned with other similar conclusions in other health care systems [41]. Posaconazole tablets would lose their dominance if the cost of the management of IFD goes under the €39,750 used in our analysis of the costs of IFD. Costs of IFDs vary across health care settings, which can cause cost-effectiveness calculations for oral posaconazole to fluctuate depending upon the distinct characteristics of the organization of each health care system [34, 42]. However, it has been found to be the most cost-effective alternative across several economic evaluations [19, 22, 38, 39, 43,44,45]. This may mean that, although it is sensitive to conditioning factors such as the costs of IFD, the magnitude of the incremental clinical and economic benefits of oral posaconazole compared to oral ITRA or FLU compensates for differences in the costs of IFD across health care systems.
A growing body of evidence on the large clinical and economic benefits of the new azoles has emerged in recent years [46,47,48], showing that posaconazole use is associated with a significant decrease in the number of febrile days, the incidence rate of IFDs and the duration of hospitalizations [49]. This improvement in survival relates to the reduction in the long-term death rate that has been reported in hematologic cancer patients who have either never experienced an IFD during their illness trajectory or who have successfully recovered from it because of a timely initiation of prophylaxis [50].
This study has some limitations that need to be taken into account. Firstly, clinical data on which we based our analysis were taken from posaconazole oral suspension instead of tablet formulation. In this context, we conservatively assumed that the clinical benefits of posaconazole tablets were similar to those of the oral suspension, as recent evidence indicates improved pharmacokinetics and a low IFD rate (1/210) are associated with the tablet formulation [22].
The intrinsic limitations of decision models should also be mentioned. Decision trees can only partially mimic “real life” due to their static nature. In addition, some significant clinical variables, such as adverse events of antifungals, the risk of recurrence of an IFD due to disease-related complications or relapses or the overall health status deterioration that usually takes place in these patients, were not incorporated in the model. The inclusion of these variables might have contributed to a more realistic representation of the added value of IFD preventive treatments.
Conclusion
Our study adds to previous evidence on the cost-effectiveness of oral posaconazole, showing that the new solid tablet formulation of posaconazole is highly cost-effective compared to FLU or ITRA in AML and MSD patients with chemotherapy-induced neutropenia and high risk of IFD.
References
Pagano L, Caira M. Risks for infection in patients with myelodysplasia and acute leukemia. Curr Opin Infect Dis. 2012;25(6):612–8.
Menzin J, Meyers JL, Friedman M, et al. Mortality, length of hospitalization, and costs associated with invasive fungal infections in high-risk patients. Am J Health Syst Pharm. 2009;66:1711–7.
Marr KA. Invasive Candida infections: the changing epidemiology. Oncology (Williston Park). 2004;18(14 Suppl 13):9–14.
Montagna MT, De Giglio O, Napoli C, Lovero G, Caggiano G, Delia M, et al. Invasive fungal infections in patients with hematologic malignancies (aurora project): lights and shadows during 18-months surveillance. Int J Mol Sci. 2012;13(1):774–87.
Pagano L, Caira M, Candoni A, Offidani M, Fianchi L, Martino B, et al. The epidemiology of fungal infections in patients with hematologic malignancies: the SEIFEM-2004 study. Haematologica. 2006;91(8):1068–75.
Nucci M, Garnica M, Gloria AB, Lehugeur DS, Dias VC, Palma LC, et al. Invasive fungal diseases in haematopoietic cell transplant recipients and in patients with acute myeloid leukemia or myelodysplasia in Brazil. Clin Microbiol Infect. 2013;19(8):745–51.
Kontoyiannis DP, Lionakis MS, Lewis RE, Chamilos G, Healy M, Perego C, et al. Zygomycosis in a tertiary-care cancer center in the era of Aspergillus-active antifungal therapy: a case-control observational study of 27 recent cases. J Infect Dis. 2005;191(8):1350–60.
Girmenia C, Pagano L, Corvatta L, Mele L, del Favero A, Martino P. The epidemiology of fusariosis in patients with haematological diseases. Gimema Infection Programme. Br J Haematol. 2000;111(1):272–6.
Girmenia C, Micozzi A, Piciocchi A, et al. Invasive fungal diseases during first induction chemotherapy affect complete remission achievement and long-term survival of patients with acute myeloid leukemia. Leuk Res. 2014;38:469–74.
Michallet M, Bénet T, Sobh M, et al. Invasive Aspergillosis: an important risk factor on the short- and long-term survival of acute myeloid leukemia (AML) patients. Eur J Clin Microbiol Infect Dis. 2012;2012(31):991–7.
Even C, Bastuji-Garin S, Hicheri Y, et al. Impact of invasive fungal disease on the chemotherapy schedule and event-free survival in acute leukemia patients who survived to fungal disease. A case-control study. Haematologica. 2010;96:337–41.
Slobbe L, Polinder S, Doorduijn JK, et al. Outcome and medical costs of patients with invasive aspergillosis and acute myelogenous leukemia-myelodysplastic syndrome treated with intensive chemotherapy: an observational study. Clin Infect Dis. 2008;15:1507–12.
Ananda-Rajah MR, Grigg A, Downey MT, Bajel A, Spelman T, Cheng A, Thursky KT, Vincent J, Slavin MA. Comparative clinical effectiveness of prophylactic voriconazole/posaconazole to fluconazole/itraconazole in patients with acute myeloid leukemia/myelodysplastic syndrome undergoing cytotoxic chemotherapy over a 12-year period. Haematologica. 2012;97(3):459–63.
Pagano L, Caira M. The role of primary antifungal prophylaxis in patients with haematological malignancies. Clin Microbiol Infect. 2014;20(Suppl 6):19–26.
Cornely OA, Maertens J, Winston DJ, et al. Posaconazole vs. fluconazole or itraconazole prophylaxis in patients with neutropenia. N Engl J Med. 2007;356:348–59.
Patterson TF, Thompson GR 3rd, Denning DW, Fishman JA, Hadley S, Herbrecht R, Kontoyiannis DP, Marr KA, Morrison VA, Nguyen MH, Segal BH, Steinbach WJ, Stevens DA, Walsh TJ, Wingard JR, Young JH, Bennett JE. Practice guidelines for the diagnosis and management of Aspergillosis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;63(4):e1–60.
Maertens J, Marchetti O, Herbrecht R, et al. European guidelines for antifungal management in leukemia and hematopoietic stem cell transplant recipients: summary of the ECIL 3–2009 update. Bone Marrow Transplant. 2011;46:709–18.
National Comprehensive Cancer Network. Prevention and treatment of cancer-related infection. NCCN version 2.2017. NCCN Clinical Practice Guidelines in Oncology [serial on the Internet]. v.2. 2017. https://www.nccn.org/professionals/physician_gls/pdf/infections.pdf.
Grau S, de la Cámara R, Sabater FJ, et al. Cost-effectiveness of posaconazole versus fluconazole or itraconazole in the prevention of invasive fungal infections among high-risk neutropenic patients in Spain. BMC Infect Dis. 2012;12:83.
Merck & Co. Inc. Noxafil (posaconazole) [prescribing information]. Whitehouse Station, NJ: Merck, 2014.
McKeage K. Posaconazole: a review of the gastro-resistant tablet and intravenous solution in invasive fungal infections. Drugs. 2015;75:397–406.
Cornely OA, Duarte RF, Haider S, et al. Phase 3 pharmacokinetics and safety study of a posaconazole tablet formulation in patients at risk for invasive fungal disease. J Antimicrob Chemother. 2016;71:718–26.
INE. Mortality tables for the Spanish population by year, sex, age and functions. Instituto Nacional de Estadística. 2013. www.ine.es. Accessed: October 2015.
Howlader N, Krapcho M, Garshell J et al. SEER cancer statistics review, 1975–2011. Bethesda: National Cancer Institute 2013. http://seer.cancer.gov/archive/csr/1975_2011/. Accessed: October, 2015.
Greenberg PL, Tuechler H, Schanz J, et al. Revised international prognostic scoring system for myelodysplastic syndromes. Blood. 2012;120:2454–65.
López-Bastida J, Oliva J, Antoñanzas F, et al. Spanish recommendations on economic evaluation of health technologies. Eur J Health Econ. 2010;11:513–20.
Pharmacists Official College [Consejo General de Colegios Oficiales de Farmacéuticos]. https://botplusweb.portalfarma.com/. Accessed October 2015.
SmPC Posaconazole [Ficha técnica Posaconazol. Centro de Información online de Medicamentos (CIMA) de la Agencia Española de Medicamentos y productos Sanitarios (AEMPS)]. http://www.aemps.gob.es/cima/fichasTecnicas.do?metodo=buscar. Accessed October 2015.
SmPC Fluconazole [Ficha técnica Fluconazol. Centro de Información online de Medicamentos (CIMA) de la Agencia Española de Medicamentos y productos Sanitarios (AEMPS)]. http://www.aemps.gob.es/cima/fichasTecnicas.do?metodo=buscar. Accessed October 2015.
SmPC Itraconazole [Ficha técnica Itraconazol. Centro de Información online de Medicamentos (CIMA) de la Agencia Española de Medicamentos y productos Sanitarios (AEMPS)]. http://www.aemps.gob.es/cima/fichasTecnicas.do?metodo=buscar. Accessed: October, 2015.
CCEMG-EPPI-Centre Cost Converter. http://eppi.ioe.ac.uk/costconversion/default.aspx. Accessed October 2015.
National Cancer Institute. SEER cancer statistics review 1975–2003. Age-adjusted SEER incidence and US death rates and 5-year relative survival rates. 2006. http://seer.cancer.gov/archive/csr/1975_2003/. Accessed October 2015.
Kantarjian H, Beran M, Cortes J, et al. Long-term follow-up results of the combination of topotecan and cytarabine and other intensive chemotherapy regimens in myelodisplastic syndrome. Cancer. 2006;106:1099–109.
Papadopoulos G, Hunt S, Prasad M. Adapting a global cost-effectiveness model to local country requirements: posaconazole case study. J Med Econ. 2013;16:374–80.
Sacristán JA, Oliva J, Llano J, et al. What is an efficient health technology in Spain? Gac Sanit. 2002;16(4):334–43.
de Witte ST, Suciu G, Verhoef B, et al. Intensive chemotherapy followed by allogeneic or autologous stem cell transplantation for patients with myelodysplastic syndromes (MDSs) and acute myeloid leukemia following MDS. Blood. 2001;98:2326–31.
Burnett AK, Russell NH, Hills RK, et al. Optimization of chemotherapy for younger patients with acute Myeloid Leukemia: results of the medical research council AML15 Trial. J Clin Oncol. 2013;31:3360–8.
O’Sullivan AK, Pandya A, Papadopoulos G, et al. Cost-Effectiveness of posaconazole versus fluconazole or itraconazole in the prevention of invasive fungal infections among neutropenic patients in the United States. Value Health. 2009;12:666–73.
Sung AH, Marcella SW, Xie Y. An update to the cost-effectiveness of posaconazole vs fluconazole or itraconazole in the prevention of invasive fungal disease among neutropenic patients in the United States. Med Econ. 2015;18:341–8.
Cho SY, Lee DG, Choi JK. Cost–benefit analysis of posaconazole versus fluconazole or itraconazole as a primary antifungal prophylaxis in high-risk hematologic patients: a propensity score-matched analysis. Clin Ther. 2015;37:2019–27.
Rely K, Alexandre PK, Escudero GS. Cost effectiveness of posaconazole versus fluconazole/itraconazole in the prophylactic treatment of invasive fungal infections in Mexico. Value Health. 2011;14(Suppl 1):S39–42.
Fung M, Kim J, Martin FM, et al. Meta-analysis and cost comparison of empirical versus pre-emptive antifungal strategies in hematologic malignancy patients with high-risk febrile neutropenia. PLoS ONE. 2015;10:e0140930.
Athanasakis K, Petrakis I, Kyriopoulos J. Posaconazole vs fluconazole/itraconazole in the prophylaxis of invasive fungal infections in immunocompromised patients: a cost-effectiveness analysis in Greece. J Med Econ. 2013;16:678–84.
Stam WB, O’Sullivan AK, Rijnders B, et al. Economic evaluation of posaconazole vs. standard azole prophylaxis in high risk neutropenic patients in the Netherlands. Eur J Haematol. 2008;81:467–74.
Dranitsaris G, Khoury H. Posaconazole versus fluconazole or itraconazole for prevention of invasive fungal infections in patients undergoing intensive cytotoxic therapy for acute myeloid leukemia or myelodysplasia: a cost effectiveness analysis. Support Care Cancer. 2011;19:1807–13.
Hahn-Ast C, Glasmacher A, Mückter S, et al. Overall survival and fungal infection-related mortality in patients with invasive fungal infection and neutropenia after myelosuppressive chemotherapy in a tertiary care centre from 1995 to 2006. J Antimicrob Chemother. 2010;65:761–8.
Girmenia C, Frustaci AM, Gentile G, et al. Posaconazole prophylaxis during front-line chemotherapy of acute myeloid leukemia: a single-center, real-life experience. Haematologica. 2012;97:560–7.
Cuenca-Estrella M, Bernal-Martinez L, Buitrago MJ, et al. Update on the epidemiology and diagnosis of invasive fungal infection. Int J Antimicrob Agents. 2008;32:143–7.
Vehreschild JJ, Rüping MJ, Wisplinghoff H, et al. Clinical effectiveness of posaconazole prophylaxis in patients with acute myelogenous leukemia (AML): a 6 year experience of the Cologne AML cohort. J Antimicrob Chemother. 2010;65:1466–71.
Zhao YJ, Khoo AL, Tan G et al. Fluconazole, itraconazole, posaconazole and voriconazole in invasive fungal infection prophylaxis: network meta-analysis and pharmacoeconomic evaluation. In Antimicrob Agents Chemother 2015.
Acknowledgements
This study, article processing charges and open access fee were funded by MSD Sharp & Dohme. The sponsor had no influence on the evaluation of data, the preparation of the manuscript and the decision to submit it for publication. All authors had full access to all the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis. Medical writing assistance was provided by Irmina Gozalbo and Lucía Pérez-Carbonell of the independent research institution Outcomes 10’, which was funded by MSD Sharp & Dohme. As members of the scientific committee of the study, all authors oversaw the development of the study, reviewed the methodology, assisted in the identification of sources and data, and guided the adaptation of the economic model as well as the analysis and interpretation of results. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published.
Disclosures
Belén Aragón works at MSD Sharp & Dohme. Irmina Gozalbo works for an independent research institution and received payment for her contribution to the development of the project as well as to the drafting of this manuscript. Rafael Cámara, Manuel Jurado, Jaime Sanz and Santiago Grau have nothing to disclose.
Compliance with Ethics Guidelines
This article does not contain any new studies with human or animal subjects performed by any of the authors.
Data Availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/69F8F060600154E0.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Cámara, R., Gozalbo, I., Jurado, M. et al. Cost-Effectiveness of Posaconazole Tablets for Invasive Fungal Infections Prevention in Acute Myelogenous Leukemia or Myelodysplastic Syndrome Patients in Spain. Adv Ther 34, 2104–2119 (2017). https://doi.org/10.1007/s12325-017-0600-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-017-0600-1