Abstract
Interest in medical cannabis and cannabis-based medicinal products (CBMPs) has increased greatly in recent years. Two cannabinoids are of principal importance; delta-9-tetrahydrocannabinol (∆9-THC), the primary psychoactive component, and also cannabidiol (CBD), considered non-intoxicating. Each has distinct mechanisms of action and different therapeutic potentials. CBMPs differ in their ∆9-THC and CBD components; predominantly ∆9-THC, balanced formulations with equivalent ∆9-THC and CBD elements, and CBD-predominant products. In this narrative review, we evaluate the published evidence for the clinical benefits of CBMPs and overall benefits in well-being. We also review the overall safety profile and discuss the potential for dependence with CBMPs. Evidence can be drawn from a wide range of randomized and other controlled studies and from observational real-world studies. Most data from observational registry studies are supportive of ∆9-THC-based products (∆9-THC-predominant or balanced CBMPs) in the management of chronic neuropathic pain. Balanced products are also effective in reducing spasticity in multiple sclerosis. Most CBMPs show benefit in providing symptomatic benefits in reducing anxiety, nausea, and in improving sleep, but the place of specific products is more subtle, and choice guided by specific circumstances. Symptomatic improvements are accompanied by improved quality of life and well-being. Safety data indicate that CBMPs are generally well tolerated in most patients without specific contraindications. The majority of adverse effects are non-serious, and transient; most are principally associated with ∆9-THC and are dose-dependent. In contrast to recreational cannabis use, there is little evidence from clinical studies that CBMPs have any potential for dependence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
There is continued interest in use of medical cannabis and cannabis-based medicinal products (CBMPs) in the management of a diverse range of symptoms. A wide range of products exist, chiefly differentiated by the major active agent; i.e., delta-9-tetrahydrocannabinol (∆9-THC)-based, cannabidiol (CBD)-based, and more balanced ∆9-THC/ CBD formulations. |
There is a clear need for improved training and education of healthcare professionals to help inform patients about medical cannabis and CBMPs. This review describes the existing evidence from clinical studies and real-world data for the use of CBMPs in clinical practice. |
There is a place for ∆9-THC-based products in chronic neuropathic pain management in some patients, and ∆9-THC/CBD products in spasticity. CBMPs can also provide symptomatic relief in various conditions (e.g., nausea and vomiting, sleep disturbance, and anxiety). |
CBMPs are generally well tolerated, and most adverse effects are minor and short-lived. Although specific data are limited, there is little evidence for any addictive potential. |
Introduction
Until relatively recently, clinical use of medicinal cannabis and allied cannabis-based or related medicinal products (called here CBMPs) was rather restricted, chiefly to use of a small number of licensed medications in specific indications [1,2,3,4]. Such agents are now increasingly studied for their therapeutic effects in a diverse range of clinical conditions and symptoms [5,6,7], and interest and use are expanding, particularly for managing neuropathic and chronic non-cancer pain [8,9,10,11], symptomatic relief in multiple sclerosis (MS) [12, 13], in supportive cancer care and in palliative care [14,15,16,17]. In part, this reflects legislative evolutions surrounding recreational cannabis use and a global shift in positive attitudes towards use of medicinal cannabis/CBMPs by medical professionals [18,19,20,21] and by patients [22,23,24,25,26,27,28,29,30,31]. As a reminder, recreational cannabis use has been formally legalized in some countries, e.g., Canada, Uruguay, and Malta, and across many jurisdictions within the United States (US), with more regulated legal supply also allowed in e.g., Switzerland and the Netherlands [32]. Furthermore, recreational cannabis use has been decriminalized (i.e., the removal of criminal penalties) in more than 30 countries, including Australia and Israel [33]. This has been accompanied by legislative changes allowing broader regulated use of medicinal cannabis in many countries such as the United States, Canada, Israel, and Australia [21, 34,35,36,37]. Within Europe, although access to medicinal cannabis remains more restricted, prescribed use is allowed in a number of countries including Italy, France, Germany, the United Kingdom (UK), Greece, the Netherlands, Denmark, and Luxembourg [38,39,40].
Consequently, medical cannabis and CBMPs are increasingly used by patients with a wide range of chronic medical conditions for symptom relief and to improve quality of life (QoL). In the US, the proportion of patients hospitalized with chronic pain reporting cannabis use doubled between 2011 and 2015, while in Canada, one large survey of patients living with chronic pain reported the prevalence of cannabis use for pain management was 30.1% [22, 23]. Surveys of patients with cancer conducted in the US, Canada, and in Europe reported use in between 13% and 70% of patients [24,25,26,27,28]. Principal reasons of this use was relief of various physical symptoms (e.g., pain or nausea and vomiting during active anticancer therapy) and also for broader psychological support (reducing anxiety/stress or improving mood and sleep) [24, 25, 41]. Note that although patients may report use for a potential anti-cancer effect [24, 27], with some supportive preclinical data [42,43,44,45], there are a lack of clinical data for any such benefit [42, 45]. Medical cannabis and CBMP use has also been described in patients with MS. A recent survey conducted in more than 3000 patients within the North American Research Committee on Multiple Sclerosis (NARCOMS) Registry found that 31% reported cannabis use at some point of their health pathway to treat their MS symptoms, with 20% reporting current use [31]. Surveys conducted in Canada, Spain, and France also reported use in between 19% and 23% of patients with MS [29, 46]. In these patients, use of medical cannabis or CMBPs was chiefly for symptomatic relief, mainly pain, spasticity, and sleep disruption, with greater use observed in patients with more severe symptoms [29, 31, 46,47,48].
These observational data require clinicians to be fully informed on benefits and risks to help decision-making when considering prescribing medical cannabis or CBMP, and to provide appropriate patient guidance. However, clinician surveys conducted across a range of countries indicate that knowledge is often inadequate, with clinicians often uncomfortable in patient discussions and enquiries [49,50,51,52]. There is thus a clear need for improved training and education of HCPs to help inform patients about medical cannabis and CBMPs.
As outlined below, such uncertainty around medicinal cannabis and CBMPs arises from a number of factors, including firstly the diverse range of agents and preparations used and the accompanying terminology, and secondly the interpretation of the relevant literature. The two principal bioactive components within Cannabis sativa and most medicinal cannabis preparations and CBMPs are delta-9-tetrahydrocannabinol (∆9-THC), the primary highly psychoactive component, and cannabidiol (CBD), considered as low psychoactive and non-intoxicating [53]. Other components include terpenes and flavonoids, as yet mainly investigated in the preclinical setting [54], and cannabigerol (often used as a nutritional supplement) although clinical data are limited [55, 56]. Medical cannabis and CBMPs vary in their constituent ∆9-THC and CBD components and concentrations, and in their source, i.e., whether derived from natural botanical extracts (‘phytocannabinoids’) or as manufactured synthetic analogs (‘synthetic cannabinoids’) [53]. These are available either as licensed medical agents [1,2,3,4], or within a diverse range of prescribed ‘medical cannabis’ and CBMPs (often given under conditional, regulated medicinal use, e.g., in patient registries) [57,58,59,60]. Note that a variety of terms are used in the supporting literature, and to some extent in the present review. There is no single standard definition. Here we chiefly use ‘medical cannabis’ in the context of those preparations containing ∆9-THC and/or CBD, and where the study authors use this same terminology in their reporting. Similarly, for CBMPs, in this review we focus on ∆9-THC and/or CBD preparations, again where the study authors use similar terminology. While to some extent these terms (medical cannabis and CBMPs) can be interchangeable, it remains important to specify the nature of each (in terms of their 9-THC and CBD components) to provide the necessary context to the clinical effects we report.
The existing evidence base for benefit and risks associated with medical cannabis and CBMPs use is large and extensively evaluated, with a recent umbrella review reporting across 101 metanalyses of clinical studies [61]. Alongside this, there has been a dramatic increase in the number of clinical studies evaluating medical cannabis and CBMPs in recent years [62]. The sheer volume of existing and emerging data, often involving diverse agents utilizing different ∆9-THC and CBD combinations (sometimes at uncertain concentrations and unclear dosing details), can be difficult to interpret [61, 63]. Indeed, this is often cited by poorly experienced physicians when trying to provide patient guidance [20, 64]. One concern relates to product safety, in particular the potential for adverse effects and any potential for dependance or addiction associated with the ∆9-THC component [39, 65, 66].
The aim of the present narrative review is to synthesize the current knowledge regarding some benefits of medical cannabis and CBMPs and the safety including all potential risks associated with their use. In this, our focus will be on phytocannabinoid preparations incorporating ∆9-THC and CBD derived as natural extracts, rather than synthetic ∆9-THC agents (dronabinol, nabilone) [1, 2]. Also, while a natural purified CBD oil extract (Epidiolex®) is currently used for seizure control in some pediatric seizure disorders [3], our review will focus on medical cannabis and CBMPs use in adults. Hence, the focus will be on certain medical conditions including pain, multiple sclerosis, cancer and palliative care, but not epilepsy.
Search Strategy
To inform the review, an electronic search of PubMed was performed between 11 and 13 March 2023 using different combinations of MeSH terms and keywords with Boolean operators to identify and retrieve articles spanning three areas of interest: (1) efficacy of phytocannabinoids in neuropathic pain, spasticity and cancer symptoms; (2) safety profile of these cannabinoids in these conditions; and (3) addictive potential in all indications and comparative safety of medical versus recreational cannabis. The process is fully described in the Supplementary Appendix and Supplementary Table 1. Additionally, subsequent ad hoc searches, along with continued citation chasing and snowball sampling, was used to remain up to date with emerging literature. Although comprehensive, this approach is not formally systematic and is not presented or reported as such, since the aim is to identify the most relevant literature to ultimately develop a broad current overview of efficacy and safety for clinical use of natural extracts of cannabis among cannabis products. This article is based on previously conducted studies and does not contain any studies with human participants or animals performed by any of the authors.
Overview on the Medical Use of Cannabis Natural Extracts
Mode of Action of Cannabinoids
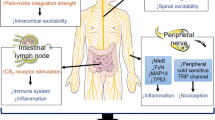
Cannabinoids exert their effects principally by acting on receptors within the endogenous cannabinoid system (ECS) [53, 67,68,69]. Specific ECS receptors are mainly cannabinoid-1 receptor (CB1), expressed preferentially across much of the central nervous system and also within the peripheral nervous system, and cannabinoid-2 receptor (CB2), expressed chiefly by leucocytes and within immune tissues (e.g., thymus, spleen, and bone marrow) [69]. ∆9-THC acts as a strong CB1 and a low CB2 agonist, with numerous downstream effects. CB1 agonism impacts gamma-aminobutyric acid, glutamine, and dopamine physiology in the brain, largely responsible for ∆9-THC’s psychoactive effects (e.g., intoxication, euphoria, or increased appetite), but also with putative antinociceptive effects on persistent pain [53, 68]. Such actions are also responsible for many of the recognized adverse effects including anxiety, sedation, and potential increased risk for cannabis use disorder. The mechanism of action for CBD is more complex and less fully understood, and less direct [69, 70]. It is a relatively low agonist of CB1, and while it may act by indirectly blocking ∆9-THC-mediated CB1 stimulation, its actions and interactions also involve a broad range of receptors within the ECS and other pathways within the central nervous system, including an agonistic central effect on serotonin 5HT-1A and dopamine D2 receptors and a peripheral effect on TRP receptor family [69, 70]. As discussed later, while some observational data suggest that CBD may attenuate any acute psychotropic effect of ∆9-THC with some supportive evidence of a benefit in clinical studies [71, 72], possibly through an indirect effect on CB1 agonism, recent data from small RCTs indicate that the resulting effect of such interaction is limited [73,74,75].
Characteristics of Medical Cannabis and CBMPs
Much of the uncertainty around the clinical use of medical cannabis and CBMPs relates to the substantial heterogeneity of available product types. Indeed, what constitutes “medical cannabis” can be unclear or confusing at times, as definitions and terminology often span a range of product formulations, with widely different ∆9-THC and CBD components, concentrations, delivery, and absolute dosing [57, 58, 63, 76, 77]. In alignment with others, medical cannabis and CBMPs are each used as broad terms in the present review, in part to reflect terms used across different studies and reviews [63, 78], although where possible, with qualifications as to relevant ∆9-THC and CBD components, concentration, and dosage. Some medical cannabis preparations are predominantly ∆9-THC-based, while others (generally referred to as hemp products) are almost exclusively CBD (with < 0.3% ∆9-THC) [5, 34, 79]. One particular concern is the ∆9-THC component of medicinal cannabis and CBMPs, with potential for adverse effects and even dependance issues [39, 65], a consideration that may only increase, given the trend towards greater ∆9-THC concentrations in medical cannabis preparations in some countries [80,81,82]. CBD-predominant products are generally subject to less restrictive regulation, chiefly as CBD products have no obvious intoxicating or psychodysleptic effects [83,84,85], and so less concerns exist [39]. Indeed, CBD-rich products with minimal or no ∆9-THC are widely available as non-prescribed over-the-counter (OTC) preparations in many countries [86,87,88].
Some CBMPs comprise both THC and CBD in more equivalent ratios [89]. Of these, nabiximols, formulated as an oromucosal spray containing balanced quantities of both ∆9-THC and CBD, is most widely studied and clinically used [4, 90,91,92]. Nabiximols is licensed for the treatment of spasticity in a broad range of European countries [4, 93] (although not available in France [48]), and also licensed in Canada and elsewhere (e.g., Israel, Brazil, Colombia, Chile, New Zealand) [4]. However, for other CBMPs, and indeed some products described as medical cannabis preparations, this distinction as to whether a product is ∆9-THC-rich, CBD-rich, or equivalent, is less clear-cut, as is the most optimal ∆9-THC:CBD ratio, which are often poorly documented or reported in clinical studies [63, 65, 89]. In addition, ∆9-THC and CBD ratios and concentrations are only one consideration [63, 94]. Products with specific ∆9-THC and CBD concentrations may deliver vastly different absolute doses depending on the formulation (tablet or capsule, oil, resin, or flower preparation) and administration route, oral (ingestion, mucosal spray, or sublingual tablet) or inhalation (smoking or vaporization), which each influence pharmacokinetics (onset and duration of effect) [95]. In general, inhalation (whether smoked or vaporized) has a more rapid absorption and onset (within 5–10 min and lasting for 2–4 h) than oral routes, with oromucosal delivery more rapid than oral ingestion (within 15–45 min and 1–3 h respectively), each lasting for 6–8 h [95].
These various aspects present a challenge when evaluating efficacy and safety outcomes from clinical studies, in particular where details on ∆9-THC and CBD concentrations, ratios, and absolute dosing are limited [63, 89]. This is especially true in real-world studies where individuals take one or more preparations during such studies, and often use multiple administration routes [57, 58].
The Evidence Base for Medical Cannabis and CBMP Use
There is a wealth of data from clinical studies pertaining to the benefits and risks of medical cannabis and CBMPs. Numerous randomized and observational studies have been reported and evaluated further via systematic reviews or/with meta-analysis, particularly examining efficacy and safety in chronic pain [7, 10, 11, 96,97,98,99,100,101,102,103,104,105,106,107,108], cancer-associated pain [14, 102, 104, 107, 109,110,111], and in symptomatic management of MS [12, 13, 90, 92]. This list is by no means exhaustive, and encompasses data from hundreds of RCTs and controlled or observational studies (see Solmi et al. [61]). While such data provide supportive evidence into the benefits and risks of CBMPs discussed below, many studies evaluate short-term use, which may not reflect real-word use. Furthermore, studies are highly heterogeneous in terms of design and sample size (usually small), CBMP characteristics, and in outcomes and assessments. Overall, the quality of evidence from such studies has been considered to be relatively low [10, 63]. Inadequate blinding and high expectations on treatment effect from study participants may moreover impact self-reported outcome measures evaluating pain or other outcomes [101, 112, 113].
Additional insight can be gained from observational data reported from medical cannabis registries that prospectively collect longitudinal data from individuals provided prescribed medicinal cannabis products. Numerous registries are now in place worldwide, often involving and reporting on substantial patient numbers [114]. For example, one commercially sponsored registry in the United States has reported on patient characteristics on over 60,000 patients (although to date outcome data are not reported) [115]. In Canada, the Quebec Cannabis Registry (QCR) involves almost 3000 patients [59], while the Australian Emyria Clinical e-Registry (AECeR) reports on over 4000 patients [116], and an extensive registry in Israel involves more than 10,000 patients, many > 65 years of age [34, 57, 58]. Others such as the UK Medical Cannabis Registry (UKMCR) also report outcomes on large patient numbers [60], while the Project Twenty21 collaboration in both the UK and Australia also report data [117,118,119,120]. As described below, these registries provide valuable insight for benefits and safety of medical cannabis products in all its forms in real-world use [77]. Some usual caveats should however be considered. Registries often provide and report on a diverse range of cannabis preparations, with different Δ9-THC and CBD compositions (in broad terms, Δ9-THC-rich, CBD-rich, and balanced formulations), often as specific commercially available medical cannabis products. Moreover, these products often deliver a range of absolute Δ9-THC and CBD doses delivered in different forms and routes (e.g., inhaled either smoked or as vaporized flowers, or sublingual oils), and patients may use a combination of products. For example, one important registry in Israel includes over 10,000 patients with chronic medical conditions, including cancer, many of whom are elderly using a suite of medical cannabis preparations [34, 57, 58]. Some are Δ9-THC-rich (between 18% and 28% Δ9-THC with minimal CBD), some with equal Δ9-THC and CBD concentrations (approximately 15% of each), and others are exclusively CBD [57, 58]. Some are inhaled (smoked or vaporized), delivering high Δ9-THC and CBD doses of between 54 and 57 mg Δ9-THC and 39 mg CBD per administration; others are given as sublingual oils or gels, delivering lower doses (approximately 10% of inhaled doses) (Table 1). Finally, the majority of these patients take more than one form, and frequency of use varies [57, 58]. Other registries that report clinical outcomes also use a range of products, where patients may use more than one specific form [59, 60, 116,117,118, 121,122,123,124,125,126,127].
While reporting outcome data from such registries, defining and interpreting the benefits and safety of specific preparations (and drawing comparisons on the benefit and safety of Δ9-THC-rich, CBD-rich, and balanced formulations) is challenging. An additional caveat is that related to existing recreational/non-prescribed cannabis use by patients within such registries. While some such as the AECeR report almost exclusively on individuals not currently taking cannabis prior to entry [116], others such as the UKMCR include often substantial numbers of previous or current consumers, and who may continue with such use [60]. While this may influence some outcomes and can obscure conclusions from some of the findings, on balance it would seem of some value to report on these. All these points should be taken into account when considering the data reported below.
Benefits in Pain Management
Neuropathic and Chronic Pain
Numerous studies have evaluated medical cannabis or CBMPs to alleviate neuropathic and other forms of chronic non-cancer pain, appraised in a large number of recent systematic reviews (and meta-analyses) [7, 10, 96,97,98,99,100,101,102,103,104,105,106]. These studies span a wide range of products and ∆9-THC and CBD formulations and composition. Overall, greater benefit would seem to be associated with ∆9-THC-predominant products. This is borne out by systematic reviews and meta-analyses of RCTs evaluating synthetic ∆9-THC oral formulations such as nabilone, where one recent meta-analysis has shown this to be associated with moderate improvement in pain, with a mean reduction in severity scores (rated between 0 and 10) of – 1.59 (95% CI, – 2.49 to – 0.82] [10].
Looking specifically at plant-based extracts, studies evaluating predominantly ∆9-THC medical cannabis products report benefits in pain reduction. One meta-analysis of RCTs evaluating use of inhaled medical cannabis found this provides short-term relief in patients with chronic neuropathic pain, with one in five patients reporting ≥ 30% improvement from baseline pain VAS scores [108]. Observational data from registries also report improvements with ∆9-THC-rich products. One study from Israel, reporting on use of different CBMPs although predominantly ∆9-THC-rich CBMPs (mostly inhaled) over 6-months in over 2000 patients with neuropathic pain, found that treatment success (defined as a moderate or significant improvement in pain without treatment cessation or serious AE) was reported in 77.4% of patients, with reduced use of opioid or other analgesic medications [58]. While most outcomes were not reported in terms of specific products, a sub-group analysis showed better outcomes in patients using ∆9-THC-predominant preparations than with CBD-rich forms [58]. The UKMCR also reports pain improvements in patients with chronic pain using chiefly ∆9-THC-predominant regimens [123]. In one report from the UK Project Twenty21 collaboration, reduction in chronic pain with 9-THC-dominant flower and oil preparations were observed, and where over 50% of patients discontinued opioid use [117]. Some benefit in other specific chronic pain conditions such as fibromyalgia has also been reported. While randomized studies show generally little evidence of benefit [128, 129], Israel registry data report use of predominantly 9-THC-rich products (oral/inhaled) resulted in significant improvements in pain intensity NRS scores from baseline (from 9.0 to 5.0), in particular in those with intense pain prior to treatment, and where opioid use also reduced significantly [130].
Balanced ∆9-THC: CBD agents such as nabiximols also show improvements in chronic pain in placebo-controlled studies [131]. Recent metanalyses of RCTs have found small improvements with nabiximols in mean pain scores compared with placebo, although relatively small (mean reduction in severity scores rated between 0 and 10 of between 0.4 and 0.5) [10, 132]. Data from observational studies and patient registries also show benefits in alleviating chronic pain, and can provide a greater understanding of mixed ∆9-THC/CBD formulations. For example, nabiximols may be useful as an adjunctive therapy; the German Pain e-Registry has reported on such use in 800 patients with refractory chronic pain, where significant improvements in pain measures were observed, with 67% reporting ≥ 50% improvement in pain intensity rates after 12 weeks [133]. Benefit was greater in those patients with neuropathic pain, where ≥ 50% improvement was reported in 94% [133]. A reduction in analgesic use was also observed, including opioids [131, 133]. Nabiximols also shows benefit in patients with MS, where in addition to alleviating spasticity scores (described further below) RCTs and observational studies also show significant reduction in pain intensity scores, although mainly small (between 0.5 and 2.7 points on a 0 to 10 NRS) [131]. A recent Australian study evaluating real-world use of balanced ∆9-THC and CBD doses (25 mg daily) over 3 months found that 32.9% of patients reported a meaningful improvement in pain intensity scores [134].
Studies evaluating CBD-predominant products show more mixed results. RCTs examining such products for use in the management of neuropathic pain are limited and few conclusions can be made [10, 85, 105, 135]. Some smaller studies evaluating investigational CBD-rich oral or inhaled products have shown improvements in patient-reported outcomes (PROs) related to pain intensity/severity in patients with chronic pain including fibromyalgia [136, 137]. Some registries report on outcomes in patients with chronic pain receiving a mixture of ∆9-THC-rich and CBD-rich formulations (but where overall CBD dosage is higher). In Australia, the AECeR has reported on 1651 patients with pain receiving a median total daily oral dose of 10 mg ∆9-THC and 22.5 mg CBD. Across the overall cohort, significant improvements of approximately 25% were observed for both pain interference and severity, sustained for up to 2 years [116]. One recent study from the UKMCR registry reported on the use of different oral products (mean initial starting dose of 20 mg CBD and 2.0 mg ∆9-THC) with 25% receiving flower preparations, with statistically significant improvements compared to baseline seen at 1, 3, and 6 months across a range of pain PROs, including the BPI, VAS pain scores, and Short-Form McGill Pain Questionnaire-2 [121]. Another study reporting outcomes on those receiving more balanced CBD-predominant oils (median daily dosing of 20 mg CBD and 10 mg ∆9-THC) also showed similar improvements in these measures after 6 months [123]. In this latter study, benefits were similar regardless of any current recreational cannabis use [123]. Another retrospective observational study evaluating use of exclusively CBD-rich products within a specialized clinic in Canada (with 75% managed for chronic pain), reported significant improvements in Edmonton Symptom Assessment Scale-revised version (ESAS-r) pain scores after 3 months of treatment, with improvements greater in those with more severe baseline pain [138].
In summary, although evidence from randomized clinical studies is limited, data from real-word observational studies suggest that THC-rich natural extracts of cannabis may provide an often substantial benefit on pain and its consequences in some patients with chronic neuropathic pain.
Cancer Pain
Overall, the evidence from randomized studies for the benefit of CBMPs in alleviating cancer pain is more limited [16]. Most randomized studies have investigated nabiximols (with comparable ∆9-THC and CBD) and while some have found improved pain scores (either as a change in Numerical Rating Scale [NRS] scores from baseline, or reduction in pain intensity scores) [139, 140], others have found no benefit [141]. One recent meta-analysis of RCTs found no significant difference in mean NRS pain scores between nabiximols and placebo [110]. Similar conclusions can be drawn from other such reviews [14, 102, 107, 109]. There is a lack of RCT data for other CBMPs [16].
Observational real-world use provides some support for ∆9-THC-rich and balanced ∆9-THC/CBD CBMPs. For example, a large prospective study from the Israel registry involving 2970 patients (over 90% receiving a ∆9-THC-rich product, although administration was not stated) reported a significant reduction in the number of patients reporting intense pain after 6 months (4.6%) compared to treatment initiation (52.9%) [57]. Opioid and other analgesic use was also lower at this time-point, with 36% of patients stopping opioid use [57]. In Canada, the QCR has reported on use of both ∆9-THC-rich, balanced ∆9-THC:CBD and CBD-dominant products (orally, inhaled or both) in patients with cancer with significant pain in a number of publications [125, 126]. These report statistically significant decreases in a range of indicators of pain intensity and severity at 3 months, sustained for up to 12 months with all three product types [125, 126], although more frequently seen with balanced ∆9-THC:CBD product, with a reduction in analgesic and opioid use also observed [126].
Benefits in Multiple Sclerosis
Efficacy in MS spasticity has been extensively investigated in RCTs and longitudinal studies evaluating nabiximols, with a wealth of real-world data [4, 7, 12, 13, 90, 103]. These indicate substantial benefit. Up to 40% of those patients showing an initial response (considered as those with ≥ 20% improvement in their baseline spasticity NRS score within 4 weeks) will achieve durable responses. Continued treatment (mean dosages of 6–7 sprays/day) results in sustained improvement (≥ 30% improvement from baseline NRS) for response) [4, 7, 12, 90, 103]. A recent post hoc analysis of two RCTs (GWSP0604 [142] and SAVANT [143]) found that use of nabiximols as an adjunct to baclofen led to a significant, sustained reduction in spasticity NRS scores over 12 weeks, and reduced average daily spasm count by 19–35% compared with placebo [144]. A systematic review of real-world observational studies evaluating nabiximols found that the proportion of patients achieving ≥ 20% reduction from baseline spasticity NRS scores ranged from 41.9% to 82.9% after 4 weeks, with benefits maintained over 6–12 months [13]. Spasticity improvement was also accompanied by improvement in pain intensity scores [131].
There are at present limited data from patient registry data for patients with MS [116, 145]. Some insight can be gained from reports of real-world use in patients with MS, with surveys recently conducted in the United States, Canada, and in Europe (Spain, France) reporting current use of medicinal cannabis products in between 20% and 50% of patients surveyed, chiefly to alleviate spasticity symptoms [31, 46,47,48, 146]. Although outcome data are not always described, and details on product type are lacking, improvement in spasticity symptoms are reported in 70% of respondents in Canada and in France, with over 75% of French respondents also reporting improvement in pain and in sleep [47, 48]. In summary, there is evidence from randomized and observational studies for improvement in spasticity symptoms in some patients with MS using CMBPs.
Additional Symptomatic Benefits
Beyond the use of CBMPs to alleviate specific symptoms (e.g., chronic pain, spasticity), there is some evidence for a benefit in a broader range of symptoms in chronic pain, cancer, and MS such as chemotherapy-induced nausea or vomiting (CINV), anxiety, depression, and sleep disturbance. Much of this can be drawn from reports of real-world use within cannabis registries, although again with the caveat that as these often utilize a range of products with different ∆9-THC and CBD quantities.
Registry reports indicate benefits in reducing nausea, as measured by patient-reported improvement and a concomitant reduction in anti-emetic agent use. For example, reports from the Israel registry, which utilizes mainly inhaled ∆9-THC-rich preparations, indicate substantial improvements in nausea (as measured by the number of patients reporting reduced or cessation of symptoms and reduced use of anti-emetics) in patients with chronic pain and also within the palliative cancer care setting [57, 58]. In patients with cancer, symptom improvement was reported by 91% of patients after 6 months, with 67% discontinuing anti-emetic use [57]. This registry also reports improvements in psychological symptoms, where 84% of patients with cancer reported improvement in anxiety and depressive symptoms, and approximately 25% reporting stopping anxiolytic medications [57].
Benefits of a reduction in anxiety is also widely reported from registries using CBMPs. In the German pain registry, 84% of patients with neuropathic pain receiving nabiximols reported ≥ 50% improvement in anxiety scores [133]. Recent reports from the UKMCR on individuals with generalized anxiety disorder have shown that use of either ∆9-THC-rich, balanced or CBD-rich preparations in individuals with generalized anxiety disorder led to significant improvement in the EQ-5D-5L depression and anxiety subscale scores and in Generalized Anxiety and Depression-7 (GAD-7) scores after 3 months, with greatest benefit in those receiving CBD-rich oil preparations [147]. Other reports from this registry have shown a reduction in these outcomes after 3 months in patients with chronic pain receiving ∆9-THC-rich and/or CBD predominant preparations [121, 123, 124]. In Australia, the AECeR reports that use of combined oral CBMPs (approximately 2:1 ratio for CBD and ∆9-THC) for 12 months led to small improvements in Depression Anxiety Stress Scale scores, with these observed as early as 3 months, and sustained over 24 months [116]. Data from Canada suggests that in addition to pain relief, use of CBD-predominant products in patients with cancer is also associated with improved ESAS-r anxiety and depression symptoms scores over 12 months [125, 126], and that use of exclusively CBD-rich products can reduce anxiety and depression scores in patients with chronic non-cancer pain [138]. Beyond these data, studies evaluating any benefit of CBMPs for overt depression are sparse. One recent case series from the UKMCR reporting on patients with a primary diagnosis of depression receiving a mixture of ∆9-THC-rich and CBD-rich products reported statistically significant reductions in Patient Health Questionnaire-9 (PHQ-9) scores at 1, 3, and 6 months as well as improvements in EQ-5D-5L anxiety/depression subscale scores and GAD-7 scores [148].
Patients often take CBMPs for sleep improvement, but the literature on the place of cannabinoids in sleep disturbance is conflicting [149]. Some reviews conclude that cannabinoids have a limited effect [150, 151], and indeed may adversely impact sleep and may trigger or exacerbate insomnia, in particular ∆9-THC-rich products [149, 151]. Systematic reviews with meta-analysis of RCTs spanning a range of ∆9-THC products have concluded that there is some benefit in individuals with chronic pain [152, 153]. These found significant improvements in sleep quality in those with chronic neuropathic pain and also cancer-associated pain, although these were considered relatively small, involving < 10% of patients [152, 153]. Data from studies evaluating sleep improvement with nabiximols as a secondary outcome show inconsistent findings. Some benefit is reported in patients with MS and cancer-associated pain [140, 154, 155], and longer-term observational data from the German Pain e-Registry reports improved sleep in 70% of patients with neuropathic pain [133]. Similarly, a small Australian study evaluating ∆9-THC and CBD doses (each at 25 mg daily) reported that 49.3% of patients reported a meaningful improvement in sleep over 3 months [134]. Note that this study also reported improved fatigue in 39% [134]. For CBD alone, results are inconsistent, although one recently reported RCT evaluating CBD found that 15 mg of CBD taken at night reduced self-reported sleep disturbance over 4 weeks [156]. Sleep improvement is anyway widely reported in cannabis registry cohorts. In Israel, sleep improvement (less disturbance) was reported in 87% of patients with cancer (receiving predominantly inhaled ∆9-THC-rich preparations), and with reduced use of sedative medications [57]. Similar findings were subsequently reported across a larger cohort, involving both patients with chronic pain and with cancer (with 89% reporting improved sleep) [58]. In patients receiving chiefly CBD-predominant regimens such as those with chronic pain included in the AECeR (median total daily oral dose of 10 mg ∆9-THC and 22.5 mg CBD), a significant sustained reduction in sleep disturbance of approximately 35% was observed over 24 months [116]. Data from the UKMCR also show improved sleep, as measured using the Sleep Quality Scale (SQS), with this reported across a large patient cohort with a range of chronic conditions receiving ∆9-THC-rich and/or CBD-predominant preparations [60]. Sleep improvement was also observed in several specific conditions including chronic pain [121, 123, 124], generalized anxiety disorder, and depressive illness [147, 148].
Overall, clinical evidence and observations strongly suggest that CBMPs may improve sleep quality in a substantial number of patients, mainly those using these treatments for the improvement of other symptoms in chronic cancer and non-cancer pain and MS.
Impact on Quality of Life and Well-being
The benefits of CBMPs in alleviating specific symptoms we describe above have an impact on patients’ QoL. This can be assessed using formal QoL instruments e.g., EQ-5D-5L and EQ-5D-5L VAS, while further insight can be gained from instruments evaluating a more holistic benefit such as the Patient Global Impression of Change (PGIC). Relatively few randomized or controlled studies evaluating CBMPs formally evaluate QoL, with systematic reviews concluding that the evidence from such studies for any impact is relatively weak, even when symptom improvements are observed, with a rather small impact on physical function and little if any on mental well-being [102, 157]. For most randomized studies evaluating nabiximols in MS, the observed benefit in spasticity and pain outcomes is not accompanied by significant improvements in overall QoL scores; in some, improvement in physical functioning scores is observed, the greatest improvements in overall QoL measures being restricted to patients considered as treatment responders [158]. More supportive data for nabiximols in improving well-being is seen in observational studies. In the German pain registry, 55% of patients with neuropathic pain reported ≥ 50% improvement in physical QoL and 24% reported similar improvement in mental well-being. Using the PGIC, 76% reported that their overall situation was “much better” or “very much better” after 12 weeks (Table 2) [133].
A greater understanding of the impact on QoL and patient well-being can be gained from studies reporting from cannabis registries. The UKMCR routinely reports on EQ-5D-5L and PGIC outcomes in patients receiving an array of ∆9-THC-rich, balanced, and CBD-dominant products (which can make identification of the relative impact of ∆9-THC and CBD challenging, although in general patients received greater ∆9-THC dosing) [60, 121,122,123,124, 148]. The broad pattern, however, is that in addition to the symptom improvement described above, significant improvements in overall EQ-5D-5L scores (and most instrument subscales) as well as improved GAD-7 scores are observed, sustained over as much as 12 months of follow-up, along with supportive PGIC scores [60, 121,122,123,124, 148]. Although improvement was greater in those individuals declaring current consumption of recreational cannabis, benefit was also reported in otherwise cannabis-naïve individuals [60]. In those prospective registry studies from Israel (chiefly using ∆9-THC-rich inhalation formulations), QoL was measured using a five-point Likert scale. These report significant increases in the proportion of patients reporting good QoL after 6 months of receiving cannabis preparations [57, 58]. In the study reporting specifically on patients with cancer, while only 18.7% of patients reported good quality of life prior to treatment initiation, after 6 months this proportion increased to 69.5% [57]. A similar finding was observed in the later study reporting on use for chronic pain in cancer (approximately 50% in each category), with the proportion reporting good QoL increasing from 12.9% at baseline to 69.9% at 6 months [58].
Benefits are also evident for CBD-predominant products. Australian registry data in patients with chronic pain receiving a range of products (although chiefly delivering greater CBD doses) report improved quality of life (SF-36) scores sustained over 24 months, with particular improvement in mental health items [116]. Another retrospective case series study from Australia specifically evaluated QoL in a large cohort (> 3000 patients). While patients received a mix of products, balanced and CBD or ∆9-THC-predominant, which varied across the study, the overall pattern over 2 years was chiefly CBD (approx. 70 mg daily) with lower ∆9-THC doses (titrated up to approx. 20–25 mg daily). This study found substantial improvements from in QoL (SF-36) for all physical and mental domains sustained over 2 years, with the greatest effect observed for mental and emotional well-being [159]. Improved EQ-5D-5L and ESAS-r well-being scores are also reported in chronic pain and cancer cohorts in Canada receiving mixed or CBD-rich CBMPs, although such improvements were relatively small [125, 126, 138].
Safety Profile and Adverse Effects
Therapeutic benefits of medical cannabis and CBMPs must be considered in the context of any potential negative impact, considering not only the conventional safety profile but also regarding any ‘addictogenic’ potential. Systematic evaluations of safety are often reported across different CBMPs products and formulations given to different patient populations [11, 107, 160, 161]]. While this brings some uncertainty when drawing specific conclusions, some broad observations can be made. Most studies and observational data report a relatively high prevalence of AEs, indeed in as much as over 90% individuals in longer-term studies, although this varies widely [11], and generally less frequent in registry cohorts: 34% in Israel over 6 months [58], 37% within the AECeR over 2 years [116], and 17% over 12 months within the larger UKMCR cohort [60]. In most instances, AEs are mild to moderate and transient, and serious AEs are uncommon [37, 160]. A recent systematic review of longitudinal observational studies reporting on long-term (up to 18 months) safety of medical cannabis and CBMPs reported that discontinuation due to AEs ranged from 0 to 27%, while the prevalence of serious AEs was 1.2% (95% CI, 0.1–3.1%) [11]. The most common AEs, occurring in up to 20% of patients, are dizziness, drowsiness/sedation or fatigue, dry mouth, nausea, and gastrointestinal upset [37, 95, 160]. Other effects such as euphoria, dysphoria, confusion, or cognitive impairment are less common, occurring in between 1% and 10% of subjects [11, 91, 92, 162, 163].
Most side effects are principally associated with ∆9-THC and are dose-dependent [37, 95, 160]. One recent systematic evaluation of synthetic ∆9-THC cannabis-based medications (nabilone and dronabinol) in placebo-controlled trials found that dizziness, drowsiness, dry mouth, and headache were most frequently reported, with a far-greater prevalence compared with placebo [162]. Although less common, there is a recognized association between tachycardia and Δ9-THC [37, 160, 164]. For nabiximols, randomized and observational studies and also longer-term registry data indicate a common pattern of AEs, although prevalence varies across studies: dizziness (1–22%), nausea (4–20%), fatigue (1–9%), and drowsiness (1–12%), most were considered mild or moderate and transient [91, 92, 163, 165]. Safety evaluations of CBD given at dosing up to 600 mg daily in clinical trials indicate gastrointestinal upset as the main AE, reported in up to 60% of individuals, principally diarrhea and nausea/vomiting [83, 85, 166]. Others include drowsiness (17%), fatigue (11%), and reduced appetite (16%) [166]. We should mention that elevated liver enzymes are observed in individuals taking higher CBD doses (including children for seizure control) [83]. However, this relates to far higher CBD dosage than that used in routine practice (e.g., in cancer registries, with daily dosing of between 10 and 240 mg); most studies evaluating CBD dosing of up to 600 mg daily in adults indicating no such concerns [37, 83]. Moreover, elevated liver enzymes are not present in patients receiving nabiximols [91, 92].
Cannabis registries provide a wealth of safety data in real-world long-term use, although due to the wide array of products used within registries, determining specific association with Δ9-THC or CBD elements can be challenging. One broad pattern is that most AEs are of mild or moderate severity, often transient, rarely cause treatment discontinuation, and that preparations are generally well tolerated [57, 58, 60, 116, 121, 125]. Those using primarily Δ9-THC-rich preparations, e.g., as in Israel, report a broad range of side effects: most frequently dizziness (8.2%), dry mouth (6.7%), increased appetite (4.7%), sleepiness (4.4%). Cognitive effects included euphoria (4.3%), confusion (1.7%), hallucinations (1.2%), and restlessness in 1.4%, although anxiety was uncommon (0.3%) [58]. Cardiac palpitations were infrequent (0.8%) [58]. A similar profile has recently been reported from a smaller Australian cohort receiving a Δ9-THC-rich product, with dizziness, fatigue, and increased appetite each reported by 10%, although with dry mouth reported by 24% [127]. This cohort, which also evaluated AEs observed with balanced and CBD-dominant products, allows a useful comparison. While dizziness, fatigue, and increased appetite observed with balanced Δ9-THC and CBD products were each reported at a relatively similar frequency as seen for Δ9-THC-dominant products, 10% also reported nausea and diarrhea, while 24% reported a sedative effect, with broadly similar patterns seen with patients receiving a CBD-dominant product [127].
From the data we describe above, it would appear that CBMPs have a favorable safety profile, although some differences exist depending on the cannabinoid involved. ∆9-THC is associated with a greater number and broader range of side effects than CBD, and it is likely that it is the ∆9-THC component of medical cannabis that carries the greater risk of AEs, in particular psychoactive effects including euphoria. Incorporation of CBD into ∆9-THC-rich regimens may attenuate any acute intoxicating effects of ∆9-THC and reduce any treatment-associated anxiety [167]. Most studies evaluating this interaction are heterogeneous regarding dosing routes and study populations (chiefly involving recreational cannabis users rather than for medical use) [89, 168]. Some supportive data exist, however, for use of CBD at high doses, leading to reduced euphoria in individuals using recreational cannabis, although conversely concomitant use of lower CBD doses may enhance intoxicating effects [71, 72]. However, some small RCTs have shown no evidence for CBD in modulation of acute ∆9-THC effects of ∆9-THC in recreational cannabis users [73,74,75]. While it seems possible, even likely, that there may be some genuine effect of adding CBD to ameliorate such effects, at present, however, the benefits remain uncertain [65, 169]. This said, such an approach remains part of some treatment recommendation strategies [95]. Finally, oral CBMPs have an inherently safer profile than inhaled formulations, where, drawing from studies of recreational cannabis use, it is likely that inhaled CBMPs may confer a greater risk of respiratory disease compared to other routes [164, 170, 171].
Contraindications for Use
Beyond this generally favorable profile, some additional points regarding safety concerns should be made. Firstly, the use of any cannabis product is generally contraindicated in pregnancy or while breastfeeding [160]. Although specific data for medical use are lacking, data for recreational cannabis point to adverse neurodevelopmental outcomes, with counseling and risk-reduction interventions important aspects of pre-natal care [172]. Some consider caution when considering use in younger adults < 25 years of age (or consider this a relative, even absolute contraindication) [160, 173], though it should be noted that some cannabis registries also include such individuals with no untoward safety signals [59, 60, 116]. Although associations are complex, the use of ∆9-THC is also contraindicated in individuals with specific psychiatric comorbidity, notably schizophrenia and other psychosis-related disorders [37, 160].
Other safety considerations include interactions with concomitant medications. Cannabinoids are metabolized in the liver by enzymes within the cytochrome P450 family, and so ∆9-THC and CBD may inhibit or induce the biological activity of a broad range of medications, including warfarin, phenobarbital, digoxin, and fluconazole (see review by MacCallum et al.) [173]. In turn, the use of a broad range of medications may impact ∆9-THC and CBD pharmacokinetics to increase or decrease bioavailability [160, 164, 173]. These considerations are particularly important in patients with renal/hepatic disease and the elderly, where close monitoring may be necessary [160, 164, 173]. Furthermore, CBMPs should be used with some caution in patients with well-controlled cardiovascular disease (arrythmia or coronary artery disease) and avoided completely in those with unstable cardiovascular disease [173].
While there is no evidence for any abuse potential for exclusively CBD products [65, 174, 175], ∆9-THC products are also contraindicated in individuals with overt substance-abuse disorders [37, 160]. In this context, there is growing interest in the role of CBMPS as a useful adjunct to harm reduction strategies with substance abuse [176, 177]. Although data are limited, some but not all studies have shown that nabiximols or high doses of CBD may have benefits in reducing cannabis use in frequent recreational users and in those with overt cannabis use disorder [176, 178,179,180]. However, this a complex and much-debated topic beyond the scope of the present article.
Guiding the Initiation of Medical Cannabis or CBMPs
Safety and tolerability guides recommended CBMP treatment-initiation strategies. Most guidance on this matter adopts a “start slow, go slow, and stay low” approach, beginning with low doses and gentle up-titration to reach symptom relief with fewest unwanted side effects [160, 173]. This is in keeping with the general recognition that AEs associated with medical cannabis and CBMPs (and indeed any potential for addiction) are dependent on dose and duration of use [65, 160, 173]. Slow up-titration of ∆9-THC allows some element of tolerance to build up and reduce the risk of AEs and impairment. This is a well-established practice for nabiximols [91, 92]. For other products, a variety protocols have been reported [173, 181, 182]. Some recommend routinely always beginning with CBD, e.g., at initial oral dosing of 5–10 mg daily, then increasing dosage by 10 mg every 2–3 days up to a daily dose of 40 mg if necessary [181, 182]. Only then if adequate symptom relief is not achieved should the addition of ∆9-THC be considered, beginning with 2.5 mg daily, titrating upwards in weekly 2.5-mg increments, to a maximal of 40 mg daily [181, 182]. An alternative approach involves beginning with CBD and ∆9-THC together, each at 5 mg daily, with up-titration of ∆9-THC and/or CBD by 2.5 mg every 2 or 3 days, while similar protocols utilizing only ∆9-THC (given orally or inhaled) along these same principles are also used [173, 181, 182]. Again, a maximal ∆9-THC daily dosage of 40 mg is recommended, with a general caveat that where higher dosing is desired, an alternative medication should be considered [173, 181, 182]. Ultimately, dosing should be tailored towards the individual’s needs at the holistic level. Obviously, ∆9-THC dosing is often far higher in patients treated in some of the cannabis registries we describe above. For these, specific protocols are not reported, but follow similar overall approach of titrating ∆9-THC and CBD dosing using a variety of products and administration routes to accommodate patient response and tolerance.
Addictive Potential of Medical Cannabis and CMBPs
A wealth of evidence exists that recreational cannabis use is associated with risk of dependence (which includes psychological and physical aspects) and addiction [65, 183]. Critical influencing factors include age at onset of cannabis use, with adolescent initiation in adolescents a particular risk factor, especially in males [183, 184]. Other factors are frequency of use and use of greater ∆9-THC concentrations [65, 183]. The administration route is also important, with greater bioavailability and more rapid onset of effects with inhaled cannabis compared to oral consumption (especially with vaporized products) [65, 185, 186].
This raises concerns around the possibility of dependence with medical cannabis and CBMPs containing ∆9-THC [65]. To date, although some studies have highlighted potential risks [187, 188], with greater risk in individuals with severe depressive illnesses [189, 190], few studies have formally examined potential or actual dependence, and there remains a need to better evaluate potential risks [191]. However, some observations can be made. Firstly, despite the acute intoxicating effects observed in clinical trials evaluating synthetic ∆9-THC agents or nabiximols, there were no signals for any potential for psychological dependance with standard recommended doses, although many studies were of relatively short duration [65, 163, 192, 193]. Data from longer-term studies indicate some potential for dependence, although it is low. One systematic review reporting on dependence-related AEs found a pooled prevalence for psychological dependence of 4.4% (95% CI 0–19.9%) and a pooled prevalence for withdrawal syndrome of 2.1% (95% CI, 0–8.2%) [11]. Some reassurance may be gained from those observational studies from the larger medical cannabis registries, where there are few, if any, safety signals around dependence, misuse or addiction reported. For example, the AECeR reporting on almost 4000 patients receiving CBMPs over 2 years (with a median daily dose of 10 mg ∆9-THC) found no evidence of addictive or dependence behavior [116]. Other large registries often reporting on patients receiving large doses of ∆9-THC (up to 170–220 mg in Israel, while as mentioned earlier the UKMCR allows continued recreational cannabis use) report little evidence of addiction [57, 58, 60].
These aspects should also be considered in the context of alternative agents, namely opioids for chronic pain management, with a well-established risk for addiction and dependence [194]. However, some caution remains for patients seeking medical cannabis therapies. As well as poorer general health, individuals using medical cannabis have different patterns of use than non-medical use (recreational or otherwise). In medical use, daily use is common (and often multiple times a day), especially in patients with chronic pain whereas frequency in recreational users varies widely, but often far less. Although such frequency is not in itself necessarily a concern, this points towards potential for dependence. Indeed some data suggest that ‘problematic use’ may be relatively high in those patients with chronic pain receiving CBMPs (up to 21.2% based on DSM-IV criteria), and that such use may be influenced by psychological factors, e.g., severe depression, although it is worth noting that in those with chronic pain receiving opioids, problematic use was even greater (52.6%) [189, 190]. A further consideration is that, although data are lacking, it may be anticipated that use of higher ∆9-THC concentrations, especially vaporized or smoked, carries a greater potential risk for dependence than lower-dose oral products [65]. Clearly, more research is required in this critical area.
Discussion
In this narrative review, we evaluated the evidence for some therapeutic benefits and the safety profile of medical cannabis and CBMPs. These agents span an enormous range of product and formulations, dosage, and administration, and there remain substantial knowledge gaps with regards to optimal formulations, dosage, and administration routes for specific clinical indications. Furthermore, as we have outlined, often at great length, in real-world use, individual patients often (indeed usually) receive both ∆9-THC and CBD components within their treatment regimens, though the relative predominance, concentrations, and dosing of each may change (as may the administration route). These factors hinder evaluating and quantifying the benefits and safety specifically associated with these individual ∆9-THC and CBD components. While this hampers making recommendations for specific CBMP regimens, some broad conclusions can be proposed. While CBMPs as a group show some efficacy in reducing chronic pain, there are more supportive data for ∆9-THC-predominant products and for balanced ∆9-THC/CBD preparations, although some data indicate that CBD-rich products also may provide pain reduction. Balanced products are also most effective in reducing spasticity in MS, and while most formulations show benefit in providing symptomatic benefits in reducing anxiety, nausea, and in improving sleep, the place of specific ∆9-THC or CBD-dominant and balanced products is more subtle and choice guided by specific circumstances.
Safety and tolerability would appear to be quite acceptable, a valid observation both for agents such as nabiximols [91, 92], and for the range of CBMP products in real-world use in cannabis registries [57, 58, 60, 116, 121, 125]. Although psychoactive and cognitive effects may be problematic in a small number of patients receiving ∆9-THC, this may be attenuated by concomitant CBD use [89, 167] and by gradual up-titration as described above [173, 181, 182]. Furthermore, in contrast to recreational cannabis use, where dependence is well documented [65, 183, 184], there seems little if any evidence from the larger cannabis registries in Israel and Australia involving more than 14,000 patients to indicate any such concerns with prescribed CBMPs [57, 58, 116].
One important finding in many real-world studies is that benefits were accompanied by reductions in symptomatic medication use and an increase of overall well-being. This was particularly observed for chronic pain populations where pain reduction was accompanied by substantial reduction in opioid use [57, 58, 117, 126, 131, 133]. However, data for the benefits of CBMPs in reducing opioid needs remain inconsistent. Some evidence commentaries [195], and a number of systematic reviews and meta-analysis have concluded that there is no evidence from randomized studies [111, 196]. However, one recent meta-analysis, which also evaluated observational study data, reported substantial impact on opioid use; the pooled prevalence for opioid reduction in observational studies being 85% (95% CI, 64–92.8%) while opioid cessation was found in 39% of patients (95% CI, 15–64%) [104]. In addition, a prospective study reporting the use of different ∆9-THC and CBD regimens over 6 months, in which with significant improvements in pain scores and QoL outcomes were observed, reported substantial reductions in opioid use, both in the number of patients using opioids and in dosage used [197]. However, one must be cautious when considering this issue. While some reduction in opioid use is observed in some patient populations (e.g., patients with chronic pain) when given medical cannabis/CBMPs, the supportive evidence for any such benefit is highly heterogeneous. Further research is necessary to inform clinicians on this matter. Furthermore, we do not suggest that medical cannabis or CBMPs be used specifically to reduce concomitant opioid use (although that may be a benefit for some patients).
All these patterns are important when considering the overall risk–benefit analysis accommodating symptomatic relief (and reduced symptomatic medication use), and broader benefits in improved well-being and QoL, with safety and tolerability aspects. Safety and potential for harmful effects remain a primary consideration when recommending and monitoring use of any medical cannabis product [61, 173]. One recent report from clinicians experienced in both pain management and/or CBMP use considered these elements within a multicriteria decision analysis model to evaluate comparative risks and benefits of a wide range of analgesics, including opioids of different potency, and of oral CBMPs in the management of chronic neuropathic pain [198]. It was observed that the most favorable benefit–safety balance was seen for CBMPs rather than conventional analgesics, with balanced products favored marginally over CBD-dominant or ∆9-THC-dominant products [198]. Nevertheless, there remains a need for further clinical studies, ideally RCTs, to better define the risk–benefit profiles of the many various CBMPs preparations in specific patient populations.
Conclusions
Through the present narrative review, it can be stated that findings from clinical studies and real-world data provide some evidence for the use of medical cannabis and CBMPs as an adjunctive therapy in some patients in a range of chronic conditions including neuropathic pain, multiple sclerosis, oncologic supportive care, and palliative care. Medical cannabis and CBMPs are generally well tolerated and with an acceptable safety profile. As use of these agents are likely to increase, the observations reported here can help inform physicians and other professionals on use in their daily practice.
Data Availability
All data discussed and analyzed in this study are from publicly available peer-reviewed articles. Data were drawn from included articles in their original form and not modified. The original studies and investigators are duly cited in the reference list.
References
Badowski ME, Yanful PK. Dronabinol oral solution in the management of anorexia and weight loss in AIDS and cancer. Ther Clin Risk Manag. 2018;14:643–51. https://doi.org/10.2147/TCRM.S126849.
Ware MA, Daeninck P, Maida V. A review of nabilone in the treatment of chemotherapy-induced nausea and vomiting. Ther Clin Risk Manag. 2008;4(1):99–107. https://doi.org/10.2147/tcrm.s1132.
Talwar A, Estes E, Aparasu R, Reddy DS. Clinical efficacy and safety of cannabidiol for pediatric refractory epilepsy indications: a systematic review and meta-analysis. Exp Neurol. 2023;359: 114238. https://doi.org/10.1016/j.expneurol.2022.114238.
Chan A, Silvan CV. Evidence-based management of multiple sclerosis spasticity with nabiximols oromucosal spray in clinical practice: a 10-year recap. Neurodegener Dis Manag. 2022;12(3):141–54. https://doi.org/10.2217/nmt-2022-0002.
Legare CA, Raup-Konsavage WM, Vrana KE. Therapeutic potential of cannabis, cannabidiol, and cannabinoid-based pharmaceuticals. Pharmacology. 2022;107(3–4):131–49. https://doi.org/10.1159/000521683.
Schlag AK, O’Sullivan SE, Zafar RR, Nutt DJ. Current controversies in medical cannabis: Recent developments in human clinical applications and potential therapeutics. Neuropharmacology. 2021;191: 108586. https://doi.org/10.1016/j.neuropharm.2021.108586.
Whiting PF, Wolff RF, Deshpande S, et al. Cannabinoids for medical use: a systematic review and meta-analysis. JAMA. 2015;313(24):2456–73. https://doi.org/10.1001/jama.2015.6358.
Lee G, Grovey B, Furnish T, Wallace M. Medical cannabis for neuropathic pain. Curr Pain Headache Rep. 2018;22(1):8. https://doi.org/10.1007/s11916-018-0658-8.
Hill KP, Palastro MD, Johnson B, Ditre JW. Cannabis and pain: a clinical review. Cannabis Cannabinoid Res. 2017;2(1):96–104. https://doi.org/10.1089/can.2017.0017.
McDonagh MS, Morasco BJ, Wagner J, et al. Cannabis-based products for chronic pain : a systematic review. Ann Intern Med. 2022;175(8):1143–53. https://doi.org/10.7326/M21-4520.
Zeraatkar D, Cooper MA, Agarwal A, et al. Long-term and serious harms of medical cannabis and cannabinoids for chronic pain: a systematic review of non-randomised studies. BMJ Open. 2022;12(8): e054282. https://doi.org/10.1136/bmjopen-2021-054282.
Rice J, Cameron M. Cannabinoids for treatment of MS symptoms: state of the evidence. Curr Neurol Neurosci Rep. 2018;18(8):50. https://doi.org/10.1007/s11910-018-0859-x.
Akgun K, Essner U, Seydel C, Ziemssen T. Daily practice managing resistant multiple sclerosis spasticity with delta-9-tetrahydrocannabinol: cannabidiol oromucosal spray: a systematic review of observational studies. J Cent Nerv Syst Dis. 2019;11:1179573519831997. https://doi.org/10.1177/1179573519831997.
Hauser W, Welsch P, Klose P, Radbruch L, Fitzcharles MA. Efficacy, tolerability and safety of cannabis-based medicines for cancer pain: a systematic review with meta-analysis of randomised controlled trials. Schmerz. 2019;33(5):424–36. https://doi.org/10.1007/s00482-019-0373-3.
Sawtelle L, Holle LM. Use of cannabis and cannabinoids in patients with cancer. Ann Pharmacother. 2021;55(7):870–90. https://doi.org/10.1177/1060028020965224.
Lord S, Hardy J, Good P. Does cannabidiol have a benefit as a supportive care drug in cancer? Curr Treat Options Oncol. 2022;23(4):514–25. https://doi.org/10.1007/s11864-021-00934-0.
Worster B, Hajjar ER, Handley N. Cannabis use in patients with cancer: a clinical review. JCO Oncol Pract. 2022;18(11):743–9. https://doi.org/10.1200/OP.22.00080.
Weisman JM, Rodriguez M. A systematic review of medical students’ and professionals’ attitudes and knowledge regarding medical cannabis. J Cannabis Res. 2021;3(1):47. https://doi.org/10.1186/s42238-021-00100-1.
Gardiner KM, Singleton JA, Sheridan J, Kyle GJ, Nissen LM. Health professional beliefs, knowledge, and concerns surrounding medicinal cannabis - a systematic review. PLoS ONE. 2019;14(5): e0216556. https://doi.org/10.1371/journal.pone.0216556.
Ronne ST, Rosenbaek F, Pedersen LB, et al. Physicians’ experiences, attitudes, and beliefs towards medical cannabis: a systematic literature review. BMC Fam Pract. 2021;22(1):212. https://doi.org/10.1186/s12875-021-01559-w.
MacPhail SL, Bedoya-Perez MA, Cohen R, Kotsirilos V, McGregor IS, Cairns EA. Medicinal cannabis prescribing in Australia: an analysis of trends over the first five years. Front Pharmacol. 2022;13: 885655. https://doi.org/10.3389/fphar.2022.885655.
Orhurhu V, Urits I, Olusunmade M, et al. Cannabis use in hospitalized patients with chronic pain. Adv Ther. 2020;37(8):3571–83. https://doi.org/10.1007/s12325-020-01416-9.
Godbout-Parent M, Nguena Nguefack HL, Angarita-Fonseca A, et al. Prevalence of cannabis use for pain management in Quebec: a post-legalization estimate among generations living with chronic pain. Can J Pain. 2022;6(1):65–77. https://doi.org/10.1080/24740527.2022.2051112.
Pergam SA, Woodfield MC, Lee CM, et al. Cannabis use among patients at a comprehensive cancer center in a state with legalized medicinal and recreational use. Cancer. 2017;123(22):4488–97. https://doi.org/10.1002/cncr.30879.
Weiss MC, Hibbs JE, Buckley ME, et al. A Coala-T-Cannabis Survey Study of breast cancer patients’ use of cannabis before, during, and after treatment. Cancer. 2022;128(1):160–8. https://doi.org/10.1002/cncr.33906.
Martell K, Fairchild A, LeGerrier B, et al. Rates of cannabis use in patients with cancer. Curr Oncol. 2018;25(3):219–25. https://doi.org/10.3747/co.25.3983.
Oelen Y, Revenberg S, de Vos-Geelen J, et al. Cannabinoid consumption among cancer patients receiving systemic anti-cancer treatment in the Netherlands. J Cancer Res Clin Oncol. 2023;149(5):1863–72. https://doi.org/10.1007/s00432-022-04085-z.
Nielsen SW, Ruhlmann CH, Eckhoff L, Bronnum D, Herrstedt J, Dalton SO. Cannabis use among Danish patients with cancer: a cross-sectional survey of sociodemographic traits, quality of life, and patient experiences. Support Care Cancer. 2022;30(2):1181–90. https://doi.org/10.1007/s00520-021-06515-z.
Schabas AJ, Vukojevic V, Taylor C, et al. Cannabis-based product use in a multiple sclerosis cohort. Mult Scler J Exp Transl Clin. 2019;5(3):2055217319869360. https://doi.org/10.1177/2055217319869360.
Guarnaccia JB, Khan A, Ayettey R, Treu JA, Comerford B, Njike VY. Patterns of medical cannabis use among patients diagnosed with multiple sclerosis. Mult Scler Relat Disord. 2021;50: 102830. https://doi.org/10.1016/j.msard.2021.102830.
Salter A, Fox RJ, Cutter G, et al. A survey of cannabis use in a large US-based cohort of people with multiple sclerosis. Int J MS Care. 2021;23(6):245–52. https://doi.org/10.7224/1537-2073.2021-036.
Kilmer B, Perez-Davila S. Nine Insights from 10 years of legal cannabis for nonmedical purposes. Clin Ther. 2023;45(6):496–505. https://doi.org/10.1016/j.clinthera.2023.03.005.
Eastwood N. Cannabis decriminalization policies across the globe. In: Decorte T, Lenton S, Wilkins C, editors. Legalizing cannabis experiences, lessons and scenarios. NY: Routledge; 2020. p. 133–53.
Abuhasira R, Shbiro L, Landschaft Y. Medical use of cannabis and cannabinoids containing products - regulations in Europe and North America. Eur J Intern Med. 2018;49:2–6. https://doi.org/10.1016/j.ejim.2018.01.001.
Mead A. Legal and regulatory issues governing cannabis and cannabis-derived products in the United States. Front Plant Sci. 2019;10:697. https://doi.org/10.3389/fpls.2019.00697.
Ablin J, Ste-Marie PA, Schafer M, Hauser W, Fitzcharles MA. Medical use of cannabis products: Lessons to be learned from Israel and Canada. Schmerz. 2016;30(1):3–13. https://doi.org/10.1007/s00482-015-0083-4.
Arnold JC. A primer on medicinal cannabis safety and potential adverse effects. Aust J Gen Pract. 2021;50(6):345–50. https://doi.org/10.31128/AJGP-02-21-5845.
Knoss W, van de Velde M, Sandvos C, Cremer-Schaeffer P. Key elements of legal environments for medical use of cannabis in different countries. Bundesgesundheitsblatt Gesundheitsforschung Gesundh. 2019;62(7):855–60. https://doi.org/10.1007/s00103-019-02969-z.
Freeman TP, Hindocha C, Green SF, Bloomfield MAP. Medicinal use of cannabis based products and cannabinoids. BMJ. 2019;365: l1141. https://doi.org/10.1136/bmj.l1141.
Fortin D, Marcellin F, Carrieri P, Mancini J, Barre T. Medical cannabis: toward a new policy and health model for an ancient medicine. Front Public Health. 2022;10: 904291. https://doi.org/10.3389/fpubh.2022.904291.
Vinette B, Cote J, El-Akhras A, Mrad H, Chicoine G, Bilodeau K. Routes of administration, reasons for use, and approved indications of medical cannabis in oncology: a scoping review. BMC Cancer. 2022;22(1):319. https://doi.org/10.1186/s12885-022-09378-7.
Mangal N, Erridge S, Habib N, Sadanandam A, Reebye V, Sodergren MH. Cannabinoids in the landscape of cancer. J Cancer Res Clin Oncol. 2021;147(9):2507–34. https://doi.org/10.1007/s00432-021-03710-7.
Cherkasova V, Wang B, Gerasymchuk M, Fiselier A, Kovalchuk O, Kovalchuk I. Use of cannabis and cannabinoids for treatment of cancer. Cancers (Basel). 2022;14(20):5142. https://doi.org/10.3390/cancers14205142.
Nahler G. Cannabidiol and other phytocannabinoids as cancer therapeutics. Pharmaceut Med. 2022;36(2):99–129. https://doi.org/10.1007/s40290-022-00420-4.
Abrams DI. Cannabis, cannabinoids and cannabis-based medicines in cancer care. Integr Cancer Ther. 2022;21:15347354221081772. https://doi.org/10.1177/15347354221081772.
Barre T, Testa D, Santos M, et al. Symptom severity is a major determinant of Cannabis-based products use among people with multiple sclerosis. J Clin Nurs. 2023. https://doi.org/10.1111/jocn.16674.
Santarossa TM, So R, Smyth DP, Gustavsen DS, Tsuyuki DRT. Medical cannabis use in Canadians with multiple sclerosis. Mult Scler Relat Disord. 2022;59: 103638. https://doi.org/10.1016/j.msard.2022.103638.
Barre T, Ramier C, Protopopescu C, Carrieri P, Radoszycki L. Symptom improvements following therapeutic use of cannabis-based products in French people with multiple sclerosis. Mult Scler Relat Disord. 2022;67: 104093. https://doi.org/10.1016/j.msard.2022.104093.
Cheng KYC, Harnett JE, Davis SR, Eassey D, Law S, Smith L. Healthcare professionals’ perspectives on the use of medicinal cannabis to manage chronic pain: a systematic search and narrative review. Pain Pract. 2022;22(8):718–32. https://doi.org/10.1111/papr.13161.
Bawa Z, McCartney D, Manocha R, McGregor IS. Knowledge, experiences, and attitudes of Australian General Practitioners towards medicinal cannabis: a 2021–2022 survey. BMC Prim Care. 2022;23(1):330. https://doi.org/10.1186/s12875-022-01946-x.
Rosenbaek F, Riisgaard H, Nielsen JB, et al. GPs’ prescription patterns, experience, and attitudes towards medicinal cannabis-a nationwide survey at the early stage of the Danish test scheme. BMC Prim Care. 2023;24(1):17. https://doi.org/10.1186/s12875-023-01971-4.
Barre T, Venturino H, Di Beo V, Carrieri P, Pelissier-Alicot AL. French general practitioners and medical cannabis: a need for training. Encephale. 2023;49(5):537–9. https://doi.org/10.1016/j.encep.2023.04.006.
Amin MR, Ali DW. Pharmacology of medical Cannabis. Adv Exp Med Biol. 2019;1162:151–65. https://doi.org/10.1007/978-3-030-21737-2_8.
Liktor-Busa E, Keresztes A, LaVigne J, Streicher JM, Largent-Milnes TM. Analgesic potential of terpenes derived from Cannabis sativa. Pharmacol Rev. 2021;73(4):98–126. https://doi.org/10.1124/pharmrev.120.000046.
Nachnani R, Raup-Konsavage WM, Vrana KE. The pharmacological case for cannabigerol. J Pharmacol Exp Ther. 2021;376(2):204–12. https://doi.org/10.1124/jpet.120.000340.
Russo EB, Cuttler C, Cooper ZD, Stueber A, Whiteley VL, Sexton M. Survey of patients employing cannabigerol-predominant cannabis preparations: perceived medical effects, adverse events, and withdrawal symptoms. Cannabis Cannabinoid Res. 2022;7(5):706–16. https://doi.org/10.1089/can.2021.0058.
Bar-Lev Schleider L, Mechoulam R, Lederman V, et al. Prospective analysis of safety and efficacy of medical cannabis in large unselected population of patients with cancer. Eur J Intern Med. 2018;49:37–43. https://doi.org/10.1016/j.ejim.2018.01.023.
Bar-Lev Schleider L, Mechoulam R, Sikorin I, Naftali T, Novack V. Adherence, safety, and effectiveness of medical cannabis and epidemiological characteristics of the patient population: a prospective study. Front Med (Lausanne). 2022;9: 827849. https://doi.org/10.3389/fmed.2022.827849.
Hachem Y, Moride Y, Castilloux AM, et al. A descriptive analysis of adverse event reports from the Quebec cannabis registry. Drug Saf. 2024;47(2):161–71. https://doi.org/10.1007/s40264-023-01379-0.
Olsson F, Erridge S, Tait J, et al. An observational study of safety and clinical outcome measures across patient groups in the United Kingdom Medical Cannabis Registry. Expert Rev Clin Pharmacol. 2023;16(3):257–66. https://doi.org/10.1080/17512433.2023.2183841.
Solmi M, De Toffol M, Kim JY, et al. Balancing risks and benefits of cannabis use: umbrella review of meta-analyses of randomised controlled trials and observational studies. BMJ. 2023;382: e072348. https://doi.org/10.1136/bmj-2022-072348.
Modaresi F, Talachian K. The Characteristics of clinical trials on cannabis and cannabinoids: a review of trials for therapeutic or drug development purposes. Pharmaceut Med. 2022;36(6):387–400. https://doi.org/10.1007/s40290-022-00447-7.
Inglet S, Winter B, Yost SE, et al. clinical data for the use of cannabis-based treatments: a comprehensive review of the literature. Ann Pharmacother. 2020;54(11):1109–43. https://doi.org/10.1177/1060028020930189.
Braun IM, Wright A, Peteet J, et al. Medical oncologists’ beliefs, practices, and knowledge regarding marijuana used therapeutically: a nationally representative survey study. J Clin Oncol. 2018;36(19):1957–62. https://doi.org/10.1200/JCO.2017.76.1221.
Schlag AK, Hindocha C, Zafar R, Nutt DJ, Curran HV. Cannabis based medicines and cannabis dependence: a critical review of issues and evidence. J Psychopharmacol. 2021;35(7):773–85. https://doi.org/10.1177/0269881120986393.
Freeman TP, Hall W. Benefits and risks of cannabinoids. BMJ. 2023;382:2113. https://doi.org/10.1136/bmj.p2113.
Zou S, Kumar U. Cannabinoid receptors and the endocannabinoid system: signaling and function in the central nervous system. Int J Mol Sci. 2018;19(3):833. https://doi.org/10.3390/ijms19030833.
Lucas CJ, Galettis P, Schneider J. The pharmacokinetics and the pharmacodynamics of cannabinoids. Br J Clin Pharmacol. 2018;84(11):2477–82. https://doi.org/10.1111/bcp.13710.
Peng J, Fan M, An C, Ni F, Huang W, Luo J. A narrative review of molecular mechanism and therapeutic effect of cannabidiol (CBD). Basic Clin Pharmacol Toxicol. 2022;130(4):439–56. https://doi.org/10.1111/bcpt.13710.
de Almeida DL, Devi LA. Diversity of molecular targets and signaling pathways for CBD. Pharmacol Res Perspect. 2020;8(6): e00682. https://doi.org/10.1002/prp2.682.
Solowij N, Broyd SJ, Beale C, et al. Therapeutic effects of prolonged cannabidiol treatment on psychological symptoms and cognitive function in regular cannabis users: a pragmatic open-label clinical trial. Cannabis Cannabinoid Res. 2018;3(1):21–34. https://doi.org/10.1089/can.2017.0043.
Solowij N, Broyd S, Greenwood LM, et al. A randomised controlled trial of vaporised Delta(9)-tetrahydrocannabinol and cannabidiol alone and in combination in frequent and infrequent cannabis users: acute intoxication effects. Eur Arch Psychiatry Clin Neurosci. 2019;269(1):17–35. https://doi.org/10.1007/s00406-019-00978-2.
Mokrysz C, Shaban NDC, Freeman TP, et al. Acute effects of cannabis on speech illusions and psychotic-like symptoms: two studies testing the moderating effects of cannabidiol and adolescence. Psychol Med. 2021;51(12):2134–42. https://doi.org/10.1017/S0033291720001038.
Lawn W, Trinci K, Mokrysz C, et al. The acute effects of cannabis with and without cannabidiol in adults and adolescents: a randomised, double-blind, placebo-controlled, crossover experiment. Addiction. 2023;118(7):1282–94. https://doi.org/10.1111/add.16154.
Englund A, Oliver D, Chesney E, et al. Does cannabidiol make cannabis safer? A randomised, double-blind, cross-over trial of cannabis with four different CBD:THC ratios. Neuropsychopharmacology. 2023;48(6):869–76. https://doi.org/10.1038/s41386-022-01478-z.
Halamish N, Schleider LB, McGuire S, Novack V. Can we predict the treatment doses of THC and CBD and does it matter? Eur J Intern Med. 2023;112:100–8. https://doi.org/10.1016/j.ejim.2023.03.028.
Schlag AK, Zafar RR, Lynskey MT, Athanasiou-Fragkouli A, Phillips LD, Nutt DJ. The value of real world evidence: the case of medical cannabis. Front Psychiatry. 2022;13:1027159. https://doi.org/10.3389/fpsyt.2022.1027159.
Hauser W, Finn DP, Kalso E, et al. European Pain Federation (EFIC) position paper on appropriate use of cannabis-based medicines and medical cannabis for chronic pain management. Eur J Pain. 2018;22(9):1547–64. https://doi.org/10.1002/ejp.1297.
Spindle TR, Bonn-Miller MO, Vandrey R. Changing landscape of cannabis: novel products, formulations, and methods of administration. Curr Opin Psychol. 2019;30:98–102. https://doi.org/10.1016/j.copsyc.2019.04.002.
Cash MC, Cunnane K, Fan C, Romero-Sandoval EA. Mapping cannabis potency in medical and recreational programs in the United States. PLoS ONE. 2020;15(3): e0230167. https://doi.org/10.1371/journal.pone.0230167.
Steuart SR. State variation in U.S. medical cannabis limits, restrictions, and therapeutic cannabis dosing. Cannabis. 2023;6(1):1–8. https://doi.org/10.26828/cannabis/2023.01.001.
Pennypacker SD, Cunnane K, Cash MC, Romero-Sandoval EA. Potency and therapeutic THC and CBD ratios: US Cannabis markets overshoot. Front Pharmacol. 2022;13:921493. https://doi.org/10.3389/fphar.2022.921493.
Chesney E, Oliver D, Green A, et al. Adverse effects of cannabidiol: a systematic review and meta-analysis of randomized clinical trials. Neuropsychopharmacology. 2020;45(11):1799–806. https://doi.org/10.1038/s41386-020-0667-2.
Iffland K, Grotenhermen F. An update on safety and side effects of cannabidiol: a review of clinical data and relevant animal studies. Cannabis Cannabinoid Res. 2017;2(1):139–54. https://doi.org/10.1089/can.2016.0034.
Arnold JC, McCartney D, Suraev A, McGregor IS. The safety and efficacy of low oral doses of cannabidiol: an evaluation of the evidence. Clin Transl Sci. 2023;16(1):10–30. https://doi.org/10.1111/cts.13425.
McGregor IS, Cairns EA, Abelev S, et al. Access to cannabidiol without a prescription: a cross-country comparison and analysis. Int J Drug Policy. 2020;85: 102935. https://doi.org/10.1016/j.drugpo.2020.102935.
Casanova C, Ramier C, Fortin D, Carrieri P, Mancini J, Barre T. Cannabidiol use and perceptions in France: a national survey. BMC Public Health. 2022;22(1):1628. https://doi.org/10.1186/s12889-022-14057-0.
Goodman S, Wadsworth E, Schauer G, Hammond D. Use and perceptions of cannabidiol products in Canada and in the United States. Cannabis Cannabinoid Res. 2022;7(3):355–64. https://doi.org/10.1089/can.2020.0093.
Zeyl V, Sawyer K, Wightman RS. What do you know about Maryjane? A systematic review of the current data on The THC:CBD ratio. Subst Use Misuse. 2020;55(8):1223–7. https://doi.org/10.1080/10826084.2020.1731547.
Conte A, Vila SC. Review of available data for the efficacy and effectiveness of nabiximols oromucosal spray (Sativex(R)) in multiple sclerosis patients with moderate to severe spasticity. Neurodegener Dis. 2021;21(3–4):55–62. https://doi.org/10.1159/000520560.
Prieto Gonzalez JM, Vila SC. Safety and tolerability of nabiximols oromucosal spray: a review of more than 15 years" accumulated evidence from clinical trials. Expert Rev Neurother. 2021;21(7):755–78. https://doi.org/10.1080/14737175.2021.1935879.
Prieto Gonzalez JM, Vila SC. Safety and tolerability of nabiximols oromucosal spray: a review of real-world experience in observational studies, registries, and case reports. Expert Rev Neurother. 2021;21(5):547–58. https://doi.org/10.1080/14737175.2021.1904896.
Carod-Artal FJ, Adjamian P, Vila Silvan C, Bagul M, Gasperini C. A systematic review of European regional and national guidelines: a focus on the recommended use of nabiximols in the management of spasticity in multiple sclerosis. Expert Rev Neurother. 2022;22(6):499–511. https://doi.org/10.1080/14737175.2022.2075263.
Campos DA, Mendivil EJ, Romano M, Garcia M, Martinez ME. A Systematic review of medical cannabinoids dosing in human. Clin Ther. 2022;44(12):e39–58. https://doi.org/10.1016/j.clinthera.2022.10.003.
MacCallum CA, Russo EB. Practical considerations in medical cannabis administration and dosing. Eur J Intern Med. 2018;49:12–9. https://doi.org/10.1016/j.ejim.2018.01.004.
Lynch ME, Ware MA. Cannabinoids for the treatment of chronic non-cancer pain: an updated systematic review of randomized controlled trials. J Neuroimmune Pharmacol. 2015;10(2):293–301. https://doi.org/10.1007/s11481-015-9600-6.
Stockings E, Campbell G, Hall WD, et al. Cannabis and cannabinoids for the treatment of people with chronic noncancer pain conditions: a systematic review and meta-analysis of controlled and observational studies. Pain. 2018;159(10):1932–54. https://doi.org/10.1097/j.pain.0000000000001293.
Bialas P, Fitzcharles MA, Klose P, Hauser W. Long-term observational studies with cannabis-based medicines for chronic non-cancer pain: a systematic review and meta-analysis of effectiveness and safety. Eur J Pain. 2022;26(6):1221–33. https://doi.org/10.1002/ejp.1957.
Meng H, Johnston B, Englesakis M, Moulin DE, Bhatia A. Selective cannabinoids for chronic neuropathic pain: a systematic review and meta-analysis. Anesth Analg. 2017;125(5):1638–52. https://doi.org/10.1213/ANE.0000000000002110.
Mucke M, Phillips T, Radbruch L, Petzke F, Hauser W. Cannabis-based medicines for chronic neuropathic pain in adults. Cochrane Database Syst Rev. 2018;3(3):CD012182. https://doi.org/10.1002/14651858.CD012182.pub2.
Fisher E, Moore RA, Fogarty AE, et al. Cannabinoids, cannabis, and cannabis-based medicine for pain management: a systematic review of randomised controlled trials. Pain. 2021;162(Suppl 1):S45–66. https://doi.org/10.1097/j.pain.0000000000001929.
Wang L, Hong PJ, May C, et al. Medical cannabis or cannabinoids for chronic non-cancer and cancer related pain: a systematic review and meta-analysis of randomised clinical trials. BMJ. 2021;374: n1034. https://doi.org/10.1136/bmj.n1034.
Bilbao A, Spanagel R. Medical cannabinoids: a pharmacology-based systematic review and meta-analysis for all relevant medical indications. BMC Med. 2022;20(1):259. https://doi.org/10.1186/s12916-022-02459-1.
Nielsen S, Picco L, Murnion B, et al. Opioid-sparing effect of cannabinoids for analgesia: an updated systematic review and meta-analysis of preclinical and clinical studies. Neuropsychopharmacology. 2022;47(7):1315–30. https://doi.org/10.1038/s41386-022-01322-4.
Johal H, Devji T, Chang Y, Simone J, Vannabouathong C, Bhandari M. Cannabinoids in chronic non-cancer pain: a systematic review and meta-analysis. Clin Med Insights Arthritis Musculoskelet Disord. 2020;13:1179544120906461. https://doi.org/10.1177/1179544120906461.
Nugent SM, Morasco BJ, O’Neil ME, et al. The effects of cannabis among adults with chronic pain and an overview of general harms: a systematic review. Ann Intern Med. 2017;167(5):319–31. https://doi.org/10.7326/M17-0155.
Hauser W, Petzke F, Fitzcharles MA. Efficacy, tolerability and safety of cannabis-based medicines for chronic pain management - an overview of systematic reviews. Eur J Pain. 2018;22(3):455–70. https://doi.org/10.1002/ejp.1118.
Andreae MH, Carter GM, Shaparin N, et al. Inhaled cannabis for chronic neuropathic pain: a meta-analysis of individual patient data. J Pain. 2015;16(12):1221–32. https://doi.org/10.1016/j.jpain.2015.07.009.
To J, Davis M, Sbrana A, et al. MASCC guideline: cannabis for cancer-related pain and risk of harms and adverse events. Support Care Cancer. 2023;31(4):202. https://doi.org/10.1007/s00520-023-07662-1.
Boland EG, Bennett MI, Allgar V, Boland JW. Cannabinoids for adult cancer-related pain: systematic review and meta-analysis. BMJ Support Palliat Care. 2020;10(1):14–24. https://doi.org/10.1136/bmjspcare-2019-002032.
Noori A, Miroshnychenko A, Shergill Y, et al. Opioid-sparing effects of medical cannabis or cannabinoids for chronic pain: a systematic review and meta-analysis of randomised and observational studies. BMJ Open. 2021;11(7): e047717. https://doi.org/10.1136/bmjopen-2020-047717.
Gedin F, Blome S, Ponten M, et al. Placebo response and media attention in randomized clinical trials assessing cannabis-based therapies for pain: a systematic review and meta-analysis. JAMA Netw Open. 2022;5(11): e2243848. https://doi.org/10.1001/jamanetworkopen.2022.43848.
Gertsch J. The intricate influence of the placebo effect on medical cannabis and cannabinoids. Med Cannabis Cannabinoids. 2018;1(1):60–4. https://doi.org/10.1159/000489291.
Banerjee R, Erridge S, Salazar O, et al. Real World evidence in medical cannabis research. Ther Innov Regul Sci. 2022;56(1):8–14. https://doi.org/10.1007/s43441-021-00346-0.
Mahabir VK, Merchant JJ, Smith C, Garibaldi A. Medical cannabis use in the United States: a retrospective database study. J Cannabis Res. 2020;2(1):32. https://doi.org/10.1186/s42238-020-00038-w.
Vickery AW, Roth S, Ernenwein T, Kennedy J, Washer P. A large Australian longitudinal cohort registry demonstrates sustained safety and efficacy of oral medicinal cannabis for at least two years. PLoS ONE. 2022;17(11): e0272241. https://doi.org/10.1371/journal.pone.0272241.
Lynskey MT, Schlag AK, Athanasiou-Fragkouli A, Badcock D, Nutt DJ. Characteristics of and 3-month health outcomes for people seeking treatment with prescribed cannabis: real-world evidence from Project Twenty21. Drug Sci Policy Law. 2023;9:20503245231167372.
O’Brien K, Beilby J, Frans M, et al. Medicinal cannabis for pain: Real-world data on three-month changes in symptoms and quality of life. Drug Sci Policy Law. 2023;9:20503245231172536.
Sakal C, Lynskey M, Schlag AK, Nutt DJ. Developing a real-world evidence base for prescribed cannabis in the United Kingdom: preliminary findings from Project Twenty21. Psychopharmacology. 2022;239(5):1147–55. https://doi.org/10.1007/s00213-021-05855-2.
Schlag AK. An evaluation of regulatory regimes of medical cannabis: what lessons can be learned for the UK? Med Cannabis Cannabinoids. 2020;3(1):76–83. https://doi.org/10.1159/000505028.
Harris M, Erridge S, Ergisi M, et al. UK Medical Cannabis registry: an analysis of clinical outcomes of medicinal cannabis therapy for chronic pain conditions. Expert Rev Clin Pharmacol. 2022;15(4):473–85. https://doi.org/10.1080/17512433.2022.2017771.
Ergisi M, Erridge S, Harris M, et al. An Updated analysis of clinical outcome measures across patients from the UK medical cannabis registry. Cannabis Cannabinoid Res. 2022. https://doi.org/10.1089/can.2021.0145.
Tait J, Erridge S, Holvey C, et al. Clinical outcome data of chronic pain patients treated with cannabis-based oils and dried flower from the UK Medical Cannabis Registry. Expert Rev Neurother. 2023;23(4):413–23. https://doi.org/10.1080/14737175.2023.2195551.
Erridge S, Leung O, Holvey C, et al. An observational study of clinical outcome measures in patients treated with cannabis-based medicinal products on the UK Medical Cannabis Registry. Neuropsychopharmacol Rep. 2023;43(4):616–32. https://doi.org/10.1002/npr2.12403.
Vigano A, Moride Y, Hachem Y, et al. The Quebec cannabis registry: investigating the safety and effectiveness of medical cannabis. Cannabis Cannabinoid Res. 2022. https://doi.org/10.1089/can.2022.0041.
Aprikian S, Kasvis P, Vigano M, Hachem Y, Canac-Marquis M, Vigano A. Medical cannabis is effective for cancer-related pain: Quebec Cannabis Registry results. BMJ Support Palliat Care. 2023. https://doi.org/10.1136/spcare-2022-004003.
Kalaba M, Eglit GML, Feldner MT, et al. longitudinal relationship between the introduction of medicinal cannabis and polypharmacy: an Australian Real-World Evidence Study. Int J Clin Pract. 2022;2022:8535207. https://doi.org/10.1155/2022/8535207.
Cameron EC, Hemingway SL. Cannabinoids for fibromyalgia pain: a critical review of recent studies (2015–2019). J Cannabis Res. 2020;2(1):19. https://doi.org/10.1186/s42238-020-00024-2.
Kurlyandchik I, Tiralongo E, Schloss J. Safety and efficacy of medicinal cannabis in the treatment of fibromyalgia: a systematic review. J Altern Complement Med. 2021;27(3):198–213. https://doi.org/10.1089/acm.2020.0331.
Sagy I, Bar-Lev Schleider L, Abu-Shakra M, Novack V. Safety and efficacy of medical cannabis in fibromyalgia. J Clin Med. 2019;8(6):807. https://doi.org/10.3390/jcm8060807.
Uberall MA. A review of scientific evidence for THC:CBD oromucosal spray (nabiximols) in the management of chronic pain. J Pain Res. 2020;13:399–410. https://doi.org/10.2147/JPR.S240011.
Dykukha I, Malessa R, Essner U, Uberall MA. Nabiximols in chronic neuropathic pain: a meta-analysis of randomized placebo-controlled trials. Pain Med. 2021;22(4):861–74. https://doi.org/10.1093/pm/pnab050.
Ueberall MA, Essner U, Mueller-Schwefe GH. Effectiveness and tolerability of THC:CBD oromucosal spray as add-on measure in patients with severe chronic pain: analysis of 12-week open-label real-world data provided by the German Pain e-Registry. J Pain Res. 2019;12:1577–604. https://doi.org/10.2147/JPR.S192174.
Abelev S, Warne LN, Benson M, Hardy M, Nayee S, Barlow J. Medicinal cannabis for the treatment of chronic refractory pain: an investigation of the adverse event profile and health-related quality of life impact of an oral formulation. Med Cannabis Cannabinoids. 2022;5(1):20–31. https://doi.org/10.1159/000521492.
Sholler DJ, Schoene L, Spindle TR. Therapeutic efficacy of cannabidiol (CBD): a review of the evidence from clinical trials and human laboratory studies. Curr Addict Rep. 2020;7(3):405–12. https://doi.org/10.1007/s40429-020-00326-8.
Yassin M, Oron A, Robinson D. Effect of adding medical cannabis to analgesic treatment in patients with low back pain related to fibromyalgia: an observational cross-over single centre study. Clin Exp Rheumatol. 2019;37(Suppl 116):13–20.
Capano A, Weaver R, Burkman E. Evaluation of the effects of CBD hemp extract on opioid use and quality of life indicators in chronic pain patients: a prospective cohort study. Postgrad Med. 2020;132(1):56–61. https://doi.org/10.1080/00325481.2019.1685298.
Rapin L, Gamaoun R, El Hage C, Arboleda MF, Prosk E. Cannabidiol use and effectiveness: real-world evidence from a Canadian medical cannabis clinic. J Cannabis Res. 2021;3(1):19. https://doi.org/10.1186/s42238-021-00078-w.
Johnson JR, Burnell-Nugent M, Lossignol D, Ganae-Motan ED, Potts R, Fallon MT. Multicenter, double-blind, randomized, placebo-controlled, parallel-group study of the efficacy, safety, and tolerability of THC:CBD extract and THC extract in patients with intractable cancer-related pain. J Pain Symptom Manage. 2010;39(2):167–79. https://doi.org/10.1016/j.jpainsymman.2009.06.008.
Portenoy RK, Ganae-Motan ED, Allende S, et al. Nabiximols for opioid-treated cancer patients with poorly-controlled chronic pain: a randomized, placebo-controlled, graded-dose trial. J Pain. 2012;13(5):438–49. https://doi.org/10.1016/j.jpain.2012.01.003.
Fallon MT, Albert Lux E, McQuade R, et al. Sativex oromucosal spray as adjunctive therapy in advanced cancer patients with chronic pain unalleviated by optimized opioid therapy: two double-blind, randomized, placebo-controlled phase 3 studies. Br J Pain. 2017;11(3):119–33. https://doi.org/10.1177/2049463717710042.
Novotna A, Mares J, Ratcliffe S, et al. A randomized, double-blind, placebo-controlled, parallel-group, enriched-design study of nabiximols* (Sativex((R)) ), as add-on therapy, in subjects with refractory spasticity caused by multiple sclerosis. Eur J Neurol. 2011;18(9):1122–31. https://doi.org/10.1111/j.1468-1331.2010.03328.x.
Markova J, Essner U, Akmaz B, et al. Sativex((R)) as add-on therapy vs further optimized first-line ANTispastics (SAVANT) in resistant multiple sclerosis spasticity: a double-blind, placebo-controlled randomised clinical trial. Int J Neurosci. 2019;129(2):119–28. https://doi.org/10.1080/00207454.2018.1481066.
Nicholas J, Lublin F, Klineova S, et al. Efficacy of nabiximols oromucosal spray on spasticity in people with multiple sclerosis: treatment effects on spasticity numeric rating scale, muscle spasm count, and spastic muscle tone in two randomized clinical trials. Mult Scler Relat Disord. 2023;75: 104745. https://doi.org/10.1016/j.msard.2023.104745.
Kawka M, Erridge S, Holvey C, et al. Clinical outcome data of first cohort of chronic pain patients treated with cannabis-based sublingual oils in the United Kingdom: analysis from the UK medical cannabis registry. J Clin Pharmacol. 2021;61(12):1545–54. https://doi.org/10.1002/jcph.1961.
Salter A, Cutter G, Marrie RA, et al. Sources of cannabis information and medical guidance for neurologic use: NARCOMS survey of people living with multiple sclerosis. Neurol Clin Pract. 2022;12(2):102–12. https://doi.org/10.1212/CPJ.0000000000001155.
Murphy M, Erridge S, Holvey C, Coomber R, Rucker JJ, Sodergren MH. A cohort study comparing the effects of medical cannabis for anxiety patients with and without comorbid sleep disturbance. Neuropsychopharmacol Rep. 2023. https://doi.org/10.1002/npr2.12407.
Mangoo S, Erridge S, Holvey C, et al. Assessment of clinical outcomes of medicinal cannabis therapy for depression: analysis from the UK Medical Cannabis Registry. Expert Rev Neurother. 2022;22(11–12):995–1008. https://doi.org/10.1080/14737175.2022.2161894.
Babson KA, Sottile J, Morabito D. Cannabis, cannabinoids, and sleep: a review of the literature. Curr Psychiatry Rep. 2017;19(4):23. https://doi.org/10.1007/s11920-017-0775-9.
Spanagel R, Bilbao A. Approved cannabinoids for medical purposes - comparative systematic review and meta-analysis for sleep and appetite. Neuropharmacology. 2021;196: 108680. https://doi.org/10.1016/j.neuropharm.2021.108680.
Kolla BP, Hayes L, Cox C, Eatwell L, Deyo-Svendsen M, Mansukhani MP. The effects of cannabinoids on sleep. J Prim Care Community Health. 2022;13:21501319221081276. https://doi.org/10.1177/21501319221081277.
McParland AL, Bhatia A, Matelski J, et al. Evaluating the impact of cannabinoids on sleep health and pain in patients with chronic neuropathic pain: a systematic review and meta-analysis of randomized controlled trials. Reg Anesth Pain Med. 2023;48(4):180–90. https://doi.org/10.1136/rapm-2021-103431.
AminiLari M, Wang L, Neumark S, et al. Medical cannabis and cannabinoids for impaired sleep: a systematic review and meta-analysis of randomized clinical trials. Sleep. 2022. https://doi.org/10.1093/sleep/zsab234.
Rog DJ, Nurmikko TJ, Friede T, Young CA. Randomized, controlled trial of cannabis-based medicine in central pain in multiple sclerosis. Neurology. 2005;65(6):812–9. https://doi.org/10.1212/01.wnl.0000176753.45410.8b.
Rog DJ, Nurmikko TJ, Young CA. Oromucosal delta9-tetrahydrocannabinol/cannabidiol for neuropathic pain associated with multiple sclerosis: an uncontrolled, open-label, 2-year extension trial. Clin Ther. 2007;29(9):2068–79. https://doi.org/10.1016/j.clinthera.2007.09.013.
Saleska JL, Bryant C, Kolobaric A, et al. The safety and comparative effectiveness of non-psychoactive cannabinoid formulations for the improvement of sleep: a double-blinded, randomized controlled trial. J Am Nutr Assoc. 2024;43(1):1–11. https://doi.org/10.1080/27697061.2023.2203221.
Goldenberg M, Reid MW, IsHak WW, Danovitch I. The impact of cannabis and cannabinoids for medical conditions on health-related quality of life: a systematic review and meta-analysis. Drug Alcohol Depend. 2017;174:80–90. https://doi.org/10.1016/j.drugalcdep.2016.12.030.
Arroyo R, Vila C, Dechant KL. Impact of Sativex((R)) on quality of life and activities of daily living in patients with multiple sclerosis spasticity. J Comp Eff Res. 2014;3(4):435–44. https://doi.org/10.2217/cer.14.30.
Arkell TR, Downey LA, Hayley AC, Roth S. Assessment of medical cannabis and health-related quality of life. JAMA Netw Open. 2023;6(5): e2312522. https://doi.org/10.1001/jamanetworkopen.2023.12522.
Gottschling S, Ayonrinde O, Bhaskar A, et al. Safety considerations in cannabinoid-based medicine. Int J Gen Med. 2020;13:1317–33. https://doi.org/10.2147/IJGM.S275049.
Pratt M, Stevens A, Thuku M, et al. Benefits and harms of medical cannabis: a scoping review of systematic reviews. Syst Rev. 2019;8(1):320. https://doi.org/10.1186/s13643-019-1243-x.
Bajtel A, Kiss T, Toth B, et al. The safety of dronabinol and nabilone: a systematic review and meta-analysis of clinical trials. Pharmaceuticals (Basel). 2022. https://doi.org/10.3390/ph15010100.
Etges T, Karolia K, Grint T, et al. An observational postmarketing safety registry of patients in the UK, Germany, and Switzerland who have been prescribed Sativex((R)) (THC:CBD, nabiximols) oromucosal spray. Ther Clin Risk Manag. 2016;12:1667–75. https://doi.org/10.2147/TCRM.S115014.
Corso B, Bacle A, Demay E, et al. Place of therapeutic cannabis in France and safety data: a literature review. Ann Pharm Fr. 2023;81(4):583–95. https://doi.org/10.1016/j.pharma.2023.02.002.
Lichtman AH, Lux EA, McQuade R, et al. Results of a double-blind, randomized, placebo-controlled study of nabiximols oromucosal spray as an adjunctive therapy in advanced cancer patients with chronic uncontrolled pain. J Pain Symptom Manage. 2018;55(2):179-88 e1. https://doi.org/10.1016/j.jpainsymman.2017.09.001.
Souza JDR, Pacheco JC, Rossi GN, et al. Adverse effects of oral cannabidiol: an updated systematic review of randomized controlled trials (2020–2022). Pharmaceutics. 2022. https://doi.org/10.3390/pharmaceutics14122598.
Pennypacker SD, Romero-Sandoval EA. CBD and THC: do they complement each other like Yin and Yang? Pharmacotherapy. 2020;40(11):1152–65. https://doi.org/10.1002/phar.2469.
Freeman TP, Craft S, Wilson J, et al. Changes in delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD) concentrations in cannabis over time: systematic review and meta-analysis. Addiction. 2021;116(5):1000–10. https://doi.org/10.1111/add.15253.
Freeman AM, Petrilli K, Lees R, et al. How does cannabidiol (CBD) influence the acute effects of delta-9-tetrahydrocannabinol (THC) in humans? A systematic review. Neurosci Biobehav Rev. 2019;107:696–712. https://doi.org/10.1016/j.neubiorev.2019.09.036.
Martinasek MP, McGrogan JB, Maysonet A. A systematic review of the respiratory effects of inhalational marijuana. Respir Care. 2016;61(11):1543–51. https://doi.org/10.4187/respcare.04846.
Ghasemiesfe M, Ravi D, Vali M, et al. Marijuana use, respiratory symptoms, and pulmonary function: a systematic review and meta-analysis. Ann Intern Med. 2018;169(2):106–15. https://doi.org/10.7326/M18-0522.
Badowski S, Smith G. Cannabis use during pregnancy and postpartum. Can Fam Phys. 2020;66(2):98–103.
MacCallum CA, Lo LA, Boivin M. “Is medical cannabis safe for my patients?” A practical review of cannabis safety considerations. Eur J Intern Med. 2021;89:10–8. https://doi.org/10.1016/j.ejim.2021.05.002.
Schoedel KA, Szeto I, Setnik B, et al. Abuse potential assessment of cannabidiol (CBD) in recreational polydrug users: a randomized, double-blind, controlled trial. Epilepsy Behav. 2018;88:162–71. https://doi.org/10.1016/j.yebeh.2018.07.027.
Babalonis S, Haney M, Malcolm RJ, et al. Oral cannabidiol does not produce a signal for abuse liability in frequent marijuana smokers. Drug Alcohol Depend. 2017;172:9–13. https://doi.org/10.1016/j.drugalcdep.2016.11.030.
Romer Thomsen K, Thylstrup B, Kenyon EA, et al. Cannabinoids for the treatment of cannabis use disorder: new avenues for reaching and helping youth? Neurosci Biobehav Rev. 2022;132:169–80. https://doi.org/10.1016/j.neubiorev.2021.11.033.
Lo LA, MacCallum CA, Nanson K, et al. Cannabidiol as a harm reduction strategy for people who use drugs: a rapid review. Can J Psychiatry. 2023;68(8):557–71. https://doi.org/10.1177/07067437231183525.
Lintzeris N, Bhardwaj A, Mills L, et al. Nabiximols for the treatment of cannabis dependence: a randomized clinical trial. JAMA Intern Med. 2019;179(9):1242–53. https://doi.org/10.1001/jamainternmed.2019.1993.
Lintzeris N, Mills L, Dunlop A, et al. Cannabis use in patients 3 months after ceasing nabiximols for the treatment of cannabis dependence: results from a placebo-controlled randomised trial. Drug Alcohol Depend. 2020;215: 108220. https://doi.org/10.1016/j.drugalcdep.2020.108220.
Freeman TP, Hindocha C, Baio G, et al. Cannabidiol for the treatment of cannabis use disorder: a phase 2a, double-blind, placebo-controlled, randomised, adaptive Bayesian trial. Lancet Psychiatry. 2020;7(10):865–74. https://doi.org/10.1016/S2215-0366(20)30290-X.
Bhaskar A, Bell A, Boivin M, et al. Consensus recommendations on dosing and administration of medical cannabis to treat chronic pain: results of a modified Delphi process. J Cannabis Res. 2021;3(1):22. https://doi.org/10.1186/s42238-021-00073-1.
Busse JW, Vankrunkelsven P, Zeng L, et al. Medical cannabis or cannabinoids for chronic pain: a clinical practice guideline. BMJ. 2021;374: n2040. https://doi.org/10.1136/bmj.n2040.
Curran HV, Freeman TP, Mokrysz C, Lewis DA, Morgan CJ, Parsons LH. Keep off the grass? Cannabis, cognition and addiction. Nat Rev Neurosci. 2016;17(5):293–306. https://doi.org/10.1038/nrn.2016.28.
Kaur N, Bastien G, Gagnon L, et al. Variations of cannabis-related adverse mental health and addiction outcomes across adolescence and adulthood: a scoping review. Front Psychiatry. 2022;13: 973988. https://doi.org/10.3389/fpsyt.2022.973988.
Spindle TR, Cone EJ, Schlienz NJ, et al. Acute effects of smoked and vaporized cannabis in healthy adults who infrequently use cannabis: a crossover trial. JAMA Netw Open. 2018;1(7): e184841. https://doi.org/10.1001/jamanetworkopen.2018.4841.
Spindle TR, Cone EJ, Schlienz NJ, et al. Acute pharmacokinetic profile of smoked and vaporized cannabis in human blood and oral fluid. J Anal Toxicol. 2019;43(4):233–58. https://doi.org/10.1093/jat/bky104.
Ware MA, Martel MO, Jovey R, Lynch ME, Singer J. A prospective observational study of problematic oral cannabinoid use. Psychopharmacology. 2018;235(2):409–17. https://doi.org/10.1007/s00213-017-4811-6.
Zongo A, Lee C, El-Mourad J, et al. Substance use disorders and psychoactive drug poisoning in medically authorized cannabis patients: longitudinal cohort study. Can J Psychiatry. 2022;67(7):544–52. https://doi.org/10.1177/07067437211060597.
Feingold D, Goor-Aryeh I, Bril S, Delayahu Y, Lev-Ran S. Problematic use of prescription opioids and medicinal cannabis among patients suffering from chronic pain. Pain Med. 2017;18(2):294–306. https://doi.org/10.1093/pm/pnw134.
Feingold D, Brill S, Goor-Aryeh I, Delayahu Y, Lev-Ran S. Medical marijuana dependence among chronic pain patients suffering from depression and anxiety. Harefuah. 2019;158(7):438–44.
Cooper ZD, Abrams DI. Considering abuse liability and neurocognitive effects of cannabis and cannabis-derived products when assessing analgesic efficacy: a comprehensive review of randomized-controlled studies. Am J Drug Alcohol Abuse. 2019;45(6):580–95. https://doi.org/10.1080/00952990.2019.1669628.
Ware MA, St A-T. The abuse potential of the synthetic cannabinoid nabilone. Addiction. 2010;105(3):494–503. https://doi.org/10.1111/j.1360-0443.2009.02776.x.
Allsop DJ, Lintzeris N, Copeland J, Dunlop A, McGregor IS. Cannabinoid replacement therapy (CRT): Nabiximols (Sativex) as a novel treatment for cannabis withdrawal. Clin Pharmacol Ther. 2015;97(6):571–4. https://doi.org/10.1002/cpt.109.
Battaglia M, Groenewald CB, Campbell F, et al. We need to talk: the urgent conversation on chronic pain, mental health, prescribing patterns and the opioid crisis. J Psychopharmacol. 2023;37(5):437–48. https://doi.org/10.1177/02698811221144635.
National Center for Complementary and Integrative Health (NCCIH). Cannabis (Marijuana) and Cannabinoids: What You Need To Know. 2019. https://www.nccih.nih.gov/health/cannabis-marijuana-and-cannabinoids-what-you-need-to-know. Accessed 19 June 2024
Nielsen S, Sabioni P, Trigo JM, et al. Opioid-sparing effect of cannabinoids: a systematic review and meta-analysis. Neuropsychopharmacology. 2017;42(9):1752–65. https://doi.org/10.1038/npp.2017.51.
Lucas P, Boyd S, Milloy MJ, Walsh Z. Cannabis significantly reduces the use of prescription opioids and improves quality of life in authorized patients: results of a large prospective study. Pain Med. 2021;22(3):727–39. https://doi.org/10.1093/pm/pnaa396.
Nutt DJ, Phillips LD, Barnes MP, et al. A multicriteria decision analysis comparing pharmacotherapy for chronic neuropathic pain, including cannabinoids and cannabis-based medical products. Cannabis Cannabinoid Res. 2022;7(4):482–500. https://doi.org/10.1089/can.2020.0129.
Acknowledgements
Medical Writing Assistance
The authors would like to thank Newmed Publishing Services for supporting manuscript development (funded by Laboratoires Boiron). Iain Spray (Newmed Publishing Services, Paris, France) developed and conducted supportive literature searches. The authors also thank Iain O’Neill (freelance on behalf of Newmed Publishing Services, Paris, France) for providing medical writing support.
Funding
Laboratoires Boiron (Messimy, France) funded this review and all costs related to the development and publication of this manuscript, including the journal's Rapid Service fee.
Author information
Authors and Affiliations
Contributions
Both Gérard Mick and Pascal Douek contributed to the conceptualization, review, and writing of the manuscript, take responsibility for the integrity of the work as a whole, and have approved the final manuscript for submission.
Corresponding author
Ethics declarations
Conflict of Interest
Gérard Mick has received honoraria for consulting and advisory boards from Grunenthal, Laboratoires Boiron, Viatris, AbbVie, and UPSA (in the last 3 years). Pascal Douek has received honoraria for consulting or conference attendance from Almirall, Laboratoires Boiron, and Sanofi (in the last 3 years).
Ethical Approval
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Mick, G., Douek, P. Clinical Benefits and Safety of Medical Cannabis Products: A Narrative Review on Natural Extracts. Pain Ther 13, 1063–1094 (2024). https://doi.org/10.1007/s40122-024-00643-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40122-024-00643-0