Abstract
Background
Antibiotic resistance has been listed as one of the biggest threats to global health today. A recent study has shown that treating febrile urinary tract infections with temocillin instead of cefotaxime leads to a reduced selection of antibiotic-resistant bacteria. However, a potential challenge with prioritizing temocillin over cefotaxime is the cost consequences.
Objective
This study aimed to assess the cost effectiveness of using temocillin compared to cefotaxime in treating febrile urinary tract infections in a model that takes the emergence of antibiotic resistance into account.
Methods
We used a Markov cohort model to estimate the costs and health effects of temocillin and cefotaxime treatment in febrile urinary tract infections in a Swedish setting. Health effects were assessed in terms of quality-adjusted life-years, and the primary outcome was the cost per quality-adjusted life-year gained with temocillin compared to cefotaxime. We used a 5-year time horizon.
Results
The model results showed that temocillin treatment led to better health outcomes at a higher total cost. The cost per quality-adjusted life-year gained was approximately 38,400 EUR. Results from the sensitivity analysis suggested a 63% probability of temocillin being cost effective at a threshold of 50,000 EUR. Furthermore, results showed that the cost effectiveness of temocillin in febrile urinary tract infections is highly dependent on the drug cost.
Conclusions
As antibiotic consumption is a driving force of resistance, it is essential to consider the development of resistance when studying the health economic consequences of antibiotic treatments. In doing so, this study found temocillin to be cost effective for febrile urinary tract infections.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Temocillin is cost effective in patients with febrile urinary tract infections, compared with cefotaxime, when taking indirect effects such as the development of resistance into account. |
When cost-effectiveness analyses of antibiotic treatments are used for decision making and prioritization, indirect effects of antibiotic treatment are important to consider. |
1 Introduction
The World Health Organization has listed antibiotic resistance (ABR) as one of the biggest threats to global health today [1, 2]. As a part of the work to stem the development of antibiotic resistance, health economic evaluations could support decision makers when prioritizing between interventions. To date, most economic research has focused on quantifying the total cost and consequences of ABR nationally or globally. In contrast, only a few studies have focused on the cost effectiveness of interventions that aim to affect ABR development.
Urinary tract infections (UTIs) are among the most common bacterial infections worldwide [3]. Escherichia coli is the most common pathogen in both lower and febrile UTI [4]. Furthermore, UTI caused by E. coli with a production of extended-spectrum beta-lactamase (ESBL) has been estimated to double in incidence by 2050 in Sweden [5]. In a recent randomized clinical study by Edlund et al. [6], the authors compared in-hospital treatment with temocillin, a narrow-spectrum antibiotic, to cefotaxime, a broad-spectrum antibiotic, for patients with febrile UTI, with respect to the potential risk of colonization with resistant bacteria after treatment. Results suggested that patients treated with temocillin harbored less resistant bacteria (Enterobacterales with reduced susceptibility to third-generation cephalosporins [here referred to as 3GCR-E]) after treatment than patients treated with cefotaxime [6]. Safety and clinical efficacy were non-inferior between treatments. Thus, the study showed that temocillin was a favorable alternative to cefotaxime in reference to the emergence of resistance. Furthermore, this implies that the spread of the difficult-to-treat ESBL-producing Enterobacterales among hospitalized patients could potentially be reduced.
Interventions to decrease the development of resistance, such as stewardship programs, often refer to more appropriate use of antibiotics, for example, through shortening treatment duration or a different choice of drug with a lower risk of developing resistance [7]. Several antibiotics could be equally effective in treating an infection, but with varying features from a resistance development perspective. Including indirect effects, such as the risk of secondary infections caused by resistant bacteria, in cost-effectiveness analyses (CEAs) are of great importance to accurately evaluate the impact of antibiotic treatment on the development of resistance. Furthermore, to assess the economic consequences of antibiotic use to society, it is also desirable to include indirect effects in the CEA.
The need to include indirect effects of antibiotic treatment, such as the emergence of resistance, as a complement to the direct effect of the treatment has been discussed in previous studies. For example, in a paper from 2010, Leibovici and Andreassen [8] suggested a model to estimate the cost and health effects of different antibiotic treatments. They concluded that if a model does not include the cost of resistance to future patients, the model will benefit the most effective treatment regardless of any indirect effects or implications for the development of resistance [8].
Furthermore, recent studies in the UK have suggested additional “values” to be considered when assessing the cost effectiveness of new antibiotics [9,10,11]. These values refer to a greater access to effective antibiotics and potential indirect effects from treatments. For example, they suggest an indirect effect, referred to as the spectrum value, reflecting the benefits of narrow-spectrum antibiotics with less collateral damage to the microbiome, which minimizes opportunities for resistant organisms to thrive, compared to treatment with broad-spectrum antibiotics. However, to the authors’ knowledge, these additional values are not yet included in the evaluation process in the UK. Similar suggestions of including other values, i.e., indirect effects in a cost-effectiveness analysis have also been made in other countries [12]. However, no such values have been included in the health technology assessments to date.
In a Dutch study by Nguyen et al. from 2019, temocillin was considered cost effective, compared with meropenem, in patients with UTI [13]. The study considered the direct effects on the treated patient based on if resistant or susceptible bacteria caused the infection. However, they did not include the potential effect on the emergence of resistance. Because colonization with ESBL-producing bacteria increases the risk of future severe infections caused by ESBL-producing bacteria [14], such effects are important to consider. Furthermore, as previous studies have shown that ABR-related infections add additional costs than infections caused by susceptible bacteria, secondary effects could significantly impact the total costs [5].
The aim of our study was to evaluate the cost effectiveness of using temocillin, compared to cefotaxime, in adult patients with febrile UTI. To the authors’ knowledge, no previous CEAs of temocillin considered the positive effect of lower colonization levels of resistant strains. Thus, taking the risks for the emergence of ABR into account when conducting a CEA will be a novel approach when analyzing the cost effectiveness of temocillin. Furthermore, results from this study aim to support decision makers when prioritizing between interventions.
2 Methods
2.1 Model Specification
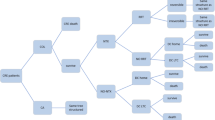
The overall reporting of this study follows the CHEERS framework for economic evaluations [15]. We used a Markov model to analyze the cost effectiveness of treating patients with febrile UTI with temocillin or cefotaxime in a Swedish setting. The Markov model approach was chosen to enable transmission between health states over a long period of time. The model, illustrated in Fig. 1, consists of five health states; febrile UTI, colonized with 3GCR-E (healthy, asymptomatic), healthy (not colonized with 3GCR-E), 3GCR-E-related bloodstream infection (BSI), and 3GCR-E-related UTI. In the health states colonized and healthy, individuals were assumed to be in full health without any symptoms, regardless of if they were colonized by 3GCR-E after initial treatment with temocillin or cefotaxime. Thus, the only thing separating these two health states was the risk of contracting a 3GCR-E-related infection after the initial treatment. Arrows illustrate possible transitions and directions between health states. At the start of the model, individuals in the febrile UTI health state, where persons had been treated with either temocillin or cefotaxime, transitions to the healthy or colonized health states. No other health states are populated from the beginning. For the following years, patients could move to another health state or stay in the current health state, depending on the transition probabilities described below.
The model was constructed to follow a yearly cohort of patients with febrile UTI over the modeled time horizon, set to 5 years in the base-case analysis. Cycle length was set to 1 year since transition probability data were measured on a yearly basis. The 5-year time horizon was chosen to enable the inclusion of indirect effects from contracting resistance-related infections if colonized with 3GCR-E, while still reflecting the relatively short time horizon that indirect effects related to initial treatment will occur. We used register data from the Swedish National Board of Health and Welfare for 2015–19 [16] to estimate the average annual number of cases in the adult population (aged 20 years and older) in hospital care, using the International Classification of Diseases 10th Revision code N10 Acute pyelonephritis. The database includes all hospitalized patients in Sweden.
Furthermore, in the base-case analysis, we applied a societal perspective, taking into account the effects of the health states on both healthcare consumption and production loss. In our data set, 34.8% of the population was considered working age, i.e., up to 64 years of age [16], while 65.2% were above the age of 65 years and considered retired. In a sensitivity analysis, we applied a healthcare perspective to analyze potential differences depending on the choice of perspective.
2.2 Transition Probabilities
Transition probabilities between health states were collected from the published literature. According to Edlund et al. [6], the clinical treatment effect on febrile UTI was the same for temocillin and cefotaxime. However, the risk of being colonized with 3GCR-E after treatment differed after the study period. We used these probabilities to transit to a health state with or without colonization with 3GCR-E. The annual probability of getting a BSI [14] or UTI (unpublished data extracted from the dataset used in [14] [J Isendahl, personal communication, 1 October, 2021]) when colonized with 3GCR-E was 4.25 and 4.51%, respectively. For probabilities of transition from colonized to 3GCR-E-related infection (BSI or UTI), the average annual risk was used to account for decreasing risks over time. According to a study by Titelman et al., 43% of persons colonized with ABR remain colonized 1 year after the primary infection [17]. We used this information to calculate the probability of transit from colonized with 3GCR-E to the healthy state by accounting for the proportions that remain colonized for another cycle or get a secondary infection caused by 3GCR-E. Treatment effects and transition probabilities are presented in Table 1.
We included a probability of death for all health states, except for febrile UTI, as the effect of treatment and, hence, the probability of death did not differ between treatments [6]. Disease-specific death risks for different health states were collected from the literature [18, 19] (see Table 1). We used the natural death risks for asymptomatic health states, weighted by 5-year age groups [16, 20]. Furthermore, the probability for these states was the same independent of if the subject was colonized with 3GCR-E or not. For each health state, we included costs, measured in EUR, and health effects, measured as quality-adjusted life-years (QALYs). We ran the model separately for temocillin and cefotaxime, and results from each model were compared at the end as an incremental cost-effectiveness ratio (ICER). We used a threshold of 50,000 EUR per QALY gained as this was within the range of thresholds used in many European countries [21].
2.3 Costs and Resource Use
Costs for each health state were divided into healthcare costs and costs of production loss, measured as production loss caused by the time of sickness. As the number of patients in the starting state was the same, independent of treatment choice, we only included the cost for the different antibiotic treatments. Other costs, such as costs for general hospital care, were assumed to be the same because the clinical efficacy of treatment of the UTI did not differ between interventions [6]. Costs were estimated in 2021 price levels and adjusted using the consumer price index if needed [22].
At the time of this study, temocillin was available in five European countries (Belgium, France, Germany, Luxembourg, and the UK) [23]. To estimate the cost of treatment, we used the average market price in the UK and Belgium as these were the only countries where prices of both treatments were publicly available. As a result, the price of temocillin was estimated to be 22.89 EUR per 1 gFootnote 1, while the price of cefotaxime was estimated to be 3.74 EUR per 1 gFootnote 2 [24,25,26]. The dosage of temocillin was 2 g three times a day, according to EUCAST clinical breakpoints [27]. Cefotaxime was assumed to be administered 1 g three times a day [28]. To estimate the treatment time for both temocillin and cefotaxime, we used the average length of hospital stay from the National Board of Health and Welfare database, which was 4.5 days for patients with the ICD-10 code N10 in 2015–19 [16].
No costs were assumed for the asymptomatic health states, independent of whether the person was colonized with resistant bacteria or not. Healthcare costs for health states with an infection caused by 3GCR-E (BSI or UTI) were estimated from a previous study on the healthcare costs of antibiotic resistance [5]. However, as this study only estimated the additional costs because of resistance, we added a fixed daily treatment cost for patients in the infection ward [29]. All costs are presented in Table 1.
Production loss was estimated as the number of days absent from work because of an infection caused by a resistant infection. In a previous study, Larsson et al. [30] estimated the average number of additional long-term sick leave days, using the human capital method, for an episode of infection caused by a resistant bacteria, compared to infections caused by susceptible bacteria, to 8.2 days. Furthermore, they estimated the average number of days for infections caused by susceptible bacteria to be 5.7 days. Therefore, we estimated the total number of long-term sick leave days due to 3GCR-E-related infections to be 13.9 (i.e., 5.7+8.2) days. To calculate the cost of production loss, we used the average salary in Sweden (including social fees, which includes pension provisions for the employee) [31, 32]. Furthermore, production loss was only estimated for people of working age (20–64 years), which amounted to about 35% of the sample according to data from the National Board of Health and Welfare [16]. All costs were discounted by 3% annually.
2.4 Health Effects
We used QALYs to measure the health effects. Patients with febrile UTI were assumed to have a QALY weight of 0.74 based on previous studies on quality of life in patients with severe UTI in the USA and Canada [33], independent of whether resistant or susceptible bacteria caused UTI. Quality-adjusted life-years in healthy people were estimated to be 0.82, using the average weight of male and female individuals from a study on QALYs in the general Swedish population by Burström et al. [34]. Patients with BSI caused by resistant bacteria were assumed to have a QALY weight of 0.64, based on a Scottish study of patients with sepsis [35]. Quality-adjusted life-years were estimated using EQ-5D in all studies [33,34,35]. All health effects were discounted by 3% annually.
2.5 Sensitivity Analysis
To analyze the robustness of the main results, we conducted a probabilistic sensitivity analysis, which takes the uncertainty of different parameter values into account. All parameters are varied simultaneously by sampling from probability distributions reflecting the uncertainty of the parameters. Statistical parameters and distribution are included in Table 1. Cost parameters followed a gamma distribution, while probabilities of events and QALY weights followed a beta distribution [36]. Standard errors were assumed to be one eighth of the mean if not presented in the original study. We ran a thousand simulations to estimate a joint distribution of the incremental cost and health effects of using temocillin compared to cefotaxime. Results are presented in a cost-effectiveness acceptability curve, which illustrates the probability of temocillin being cost effective, compared to treatment with cefotaxime, at different levels of a cost-effectiveness threshold.
In a deterministic sensitivity analysis (DSA), we studied the effect of different time horizons on the result from the base-case analysis, using a 10-year and a lifetime time horizon, respectively (but with the same 1-year cycle period). Furthermore, as the price of temocillin differed significantly in Belgium and the UK, we also conducted a DSA on the price of antibiotic treatment. This analysis included prices in Belgium, the UK, and Sweden. Sweden was added to show the effect in a country where temocillin is not marketed, and therefore the use has been limited to special licenses. According to register data, the license price of temocillin in Sweden in 2020 was approximately 871 SEK (84 EUR) per 1 g [37, 38].
3 Results
The cohort consisted of 8789 patients with febrile UTI in total. The mean age in this sample was 67 years. Results from the simulation suggest that 2329 patients were colonized with 3GCR-E after initial treatment with temocillin, compared with 4254 patients when treated with cefotaxime. In addition, over the 5-year time horizon, secondary infection with 3GCR-E because of colonization occurred in 342 patients initially treated with temocillin (166 BSI, 176 UTI). Comparable numbers for patients initially treated with cefotaxime was 626 patients with a secondary infection (304 BSI, 322 UTI).
The average healthcare costs for the cohort treated with temocillin over the 5-year time horizon were about 922 EUR per patient, compared with 566 EUR per patient initially treated with cefotaxime. In comparison, the average production loss costs were about 22 and 40 EUR per patient for temocillin and cefotaxime, respectively.
Results from the base-case analysis showed that temocillin treatment in patients with febrile UTI would lead to an increased cost of about 2,970,000 EUR and a gain of 77 QALY compared with cefotaxime. Furthermore, this resulted in an ICER of about 38,500 EUR per QALY. Temocillin was, thus, considered cost effective from a societal perspective with a cost-effectiveness threshold of 50,000 EUR per QALY gained. Using a healthcare perspective, the ICER was slightly higher than in base case (40,500 EUR per QALY); however, the production loss was only a small fraction of the total cost, and, hence, the perspective chosen does not affect the ICER to any greater extent. Results are presented in Table 2.
3.1 Sensitivity Analysis
According to the probabilistic sensitivity analysis, there was about a 63% probability of temocillin being cost effective at a threshold of 50,000 EUR per QALY gained. At a threshold of 100,000 EUR, the probability increased to 88% that temocillin is cost effective in treating patients with febrile UTI. Results are illustrated in a cost-effectiveness acceptability curve, presented in Fig. 2.
Using a DSA on the time horizon, we found that a time horizon of 10 years resulted in a lower ICER of about 23,000 EUR per QALY. A further extension to a lifetime time horizon resulted in an ICER of about 11,700 EUR per QALY. The additional effect on the ICER was mainly owing to the health effects from most patients recovered to a healthy (non-colonized) state. At the same time, the costs were relatively low in the later years of the model.
The DSA on antibiotic treatment costs showed that using the price of temocillin and cefotaxime in Belgium resulted in an ICER of about 18,300 EUR per QALY gained, while the ICERs using prices in UK and Sweden were about 58,700, and 227,300 EUR per QALY gained, respectively. Results from the DSA on both time horizon and antibiotic treatment costs are combined in Table 3.
4 Discussion
Results from our base-case analysis imply that temocillin was a cost-effective treatment in patients febrile UTI, compared with cefotaxime, when taking indirect effects such as the development of resistance into account and assuming a drug price based on the average of Belgian and UK prices. Overall, this means that the favorable effects of temocillin on colonization with Enterobacterales with reduced susceptibility to 3GC [6] were large enough to motivate a higher price than cefotaxime. However, the sensitivity analysis showed that the price level of temocillin had a significant effect on the expected ICER. For example, using temocillin on special licenses in Sweden would not be cost effective at current price levels, independent of the time horizon used.
The cost-effectiveness threshold varies between countries [21, 39]. We used a cost-effectiveness threshold of 50,000 EUR per QALY gained as this was within the range of thresholds used in many European countries [21]. However, as previous studies suggested, the threshold could vary depending on the need for treatment options and the severity of the disease [40,41,42,43]. In this matter, it could be argued that the cost-effectiveness threshold for antibiotic treatments could be higher if there are few treatment options and a high severity of disease. Additionally, if a specific antibiotic shows less impact on the development of AMR compared with other treatment, then the threshold may be higher.
In addition, this study highlights the importance of including indirect effects, such as one treatment with less tendency to select for pathogens with resistance mechanisms compared with another. As the primary effect of the treatment was comparable between the treatments, the analysis would have been a cost-minimization analysis if indirect effects were not included in the CEA. In this case, temocillin would be more expensive than cefotaxime and hence not recommended to use as a primary treatment option.
There are some limitations to this study. For example, the level of colonization, from Edlund et al. [6], was measured after the initial use of temocillin and cefotaxime but before the use of complementary oral treatment. Their results suggest no significant difference after the additional use of oral treatment. However, when it comes to reducing healthcare-associated infections, it is essential to reduce the probability of transmitter ABR bacteria while the patient is still in the hospital. Because temocillin reduces colonization with 3CGR-E, the risk for spreading this in the hospital environment is most likely reduced. Another limitation is that we only included production loss for people in working age (defined as 20–64 years). In addition, it is reasonable to believe that production loss would occur for persons aged 65 years and older, owing to for example informal work at home. However, because of the uncertainties surrounding such estimations, we decided to exclude it. This exclusion probably led to an underestimation of the true cost-effectiveness of temocillin. Furthermore, input values and transmission probabilities were collected from different studies and combined in this study. Preferably, values should have been collected from the same study or cohort, which imposes uncertainty on the results.
5 Conclusions
Temocillin was more expensive than cefotaxime in the simple price comparison. However, it is important to consider health effects in addition to costs to allocate societal resources most effectively. According to our results, temocillin would lead to fewer secondary infections caused by resistant bacteria than cefotaxime when treating patients with febrile UTI. This reduction in infections could, in extension, reduce the pressure on antibiotic use, hence, the spread and development of antibiotic resistance. Overall, taking such effects into account, temocillin was found to be cost effective in this study setting. In addition, this study shows the importance of including all relevant effects when prioritizing healthcare interventions related to infections and resistance.
In conclusion, this study emphasizes the importance of taking indirect effects into account to make the most accurate analysis possible. It is even more important in the case of antibiotic treatments as antibiotic consumption is a driving force of ABR [1, 44]. Hence, the development of resistance will be an essential factor to consider when analyzing the health economic impact of antibiotic use.
Change history
19 October 2022
Missing Open Access funding information has been added in the Funding Note
Notes
Temocillin price in Belgium was 16.89 EUR per 1 gram for inpatient use 24.Rijksinstituut voor ziekte- en invaliditeitsverzekering (RIVIZ), Vergoedbare geneesmiddelen. 2022., and in UK 25.45 GBP (=30.48 EUR) per 1 gram for hospital use 25.British National Formulary, Drugs. 2021, 26.European Central Bank, Pound sterling (GBP). Conversion rate: 1 GBP = 1.1976 EUR (Average in January 2022). 2022.
Cefotaxime price in Belgium was 3.28 EUR per 1 gram for inpatient use 24.Rijksinstituut voor ziekte- en invaliditeitsverzekering (RIVIZ), Vergoedbare geneesmiddelen. 2022., and in UK 3.50 GBP (=4.19 EUR) per 1 gram for hospital use 25.British National Formulary, Drugs. 2021, 26.European Central Bank, Pound sterling (GBP). Conversion rate: 1 GBP = 1.1976 EUR (Average in January 2022). 2022.
References
World Health Organization (WHO). Antibiotic resistance. 2020. https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance. Accessed 21 Jul 2022.
Murray CJL, et al. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Lancet. 2022;399(10325):629–55.
Ozturk R, Murt A. Epidemiology of urological infections: a global burden. World J Urol. 2020;38(11):2669–79.
Flores-Mireles AL, et al. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol. 2015;13(5):269–84.
Larsson, S., et al., A microsimulation model projecting the health care costs for resistance to antibacterial drugs in Sweden. Eur J Public Health. 2018.
Edlund C, et al. The clinical and microbiological efficacy of temocillin versus cefotaxime in adults with febrile urinary tract infection, and its effects on the intestinal microbiota: a randomised multicentre clinical trial in Sweden. Lancet Infect Dis. 2021.
Dellit TH, et al. Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America guidelines for developing an institutional program to enhance antimicrobial stewardship. Clin Infec Dis. 2007;44(2):159–77.
Leibovici L, Paul M, Andreassen S. Balancing the benefits and costs of antibiotic drugs: the TREAT model. Clin Microbiol Infect. 2010;16(12):1736–9.
Gordon J, et al. Estimating the value of new antimicrobials in the context of antimicrobial resistance: development and application of a dynamic disease transmission model. Pharmacoeconomics. 2020;38(8):857–69.
Rothery CW, Schmitt L, Claxton K, Palmer S, Sculpher M. Framework for value assessment of new antimicrobials: implications of alternative funding arrangements for NICE appraisal. 2018.
Karlsberg Schaffer SWP, Towse A, Henshall C, Mestre-Ferrandiz J, Masterton R, Fischer A. Assessing the value of new antibiotics: additional elements of value for health technology assessment decisions. 2017.
Persson UOS, Althin R. Värdering av och betalning för antibiotika: litteraturöversikt och utarbetande av förslag för tillämpning i Sverige. IHE Rapport. 2021;1:2021.
Nguyen CP, et al. Clinical cure rate and cost-effectiveness of carbapenem-sparing beta-lactams vs. meropenem for Gram-negative infections: systematic review, meta-analysis, and cost-effectiveness analysis. Int J Antimicrob Agents. 2019;54(6):790–7.
Isendahl J, et al. Temporal dynamics and risk factors for bloodstream infection with extended-spectrum β-lactamase-producing bacteria in previously-colonized individuals: national population-based cohort study. Clin Infect Dis. 2019;68(4):641–9.
Husereau D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. Pharmacoeconomics. 2013;31(5):361–7.
The National Board of Health and Welfare (Socialstyrelsen). Statistical database, in-patient care diagnoses. ICD-10 code: N10. 2020.
Titelman E, et al. Faecal carriage of extended-spectrum β-lactamase-producing Enterobacteriaceae is common 12 months after infection and is related to strain factors. Clin Microbiol Infect. 2014;20(8):O508–15.
Eliakim-Raz N, et al. Risk factors for treatment failure and mortality among hospitalized patients with complicated urinary tract infection: a multicenter retrospective cohort study (RESCUING Study Group). Clin Infect Dis. 2018;68(1):29–36.
Isendahl J, et al. Risk factors for community-onset bloodstream infection with extended-spectrum β-lactamase-producing Enterobacteriaceae: national population-based case-control study. Clin Microbiol Infect. 2019;25(11):1408–14.
Statistics Sweden (SCB). Dödstal per 1000 av medelfolkmängden efter ålder och kön. År 2015-2019.
Cameron D, Ubels J, Norström F. On what basis are medical cost-effectiveness thresholds set? Clashing opinions and an absence of data: a systematic review. Glob Health Action. 2018;11(1):1447828.
Statistics Sweden (SCB). Konsumentprisindex (1980=100), fastställda tal.
European Medicines Agency (EMA). Public data from Article 57 database.
Rijksinstituut voor ziekte: en invaliditeitsverzekering (RIVIZ), Vergoedbare geneesmiddelen. 2022.
British National Formulary. Drugs. 2021.
European Central Bank, Pound sterling (GBP). Conversion rate: 1 GBP = 1.1976 EUR (average in January 2022). 2022.
The European Committee on Antimicrobial Susceptibility Testing (EUCAST). Temocillin. Rationale for the EUCAST clinical breakpoints, version 1.0 2019.
The European Committee on Antimicrobial Susceptibility Testing (EUCAST). Cefotaxime. Rationale for the EUCAST clinical breakpoints, version 1.0 2010.
Public Health Agency of Sweden. Economic impact of antimicrobial resistance (in Swedish). 2014.
Larsson S, Svensson M, Ternhag A. Production loss and sick leave caused by antibiotic resistance: a register-based cohort study. BMC Public Health 22, 527 (2022). https://doi.org/10.1186/s12889-022-12947-x
Statistics Sweden (sv. SCB). Statistics database of mean income in Sweden (Swedish title: Sammanräknad förvärvsinkomst för boende i Sverige hela året efter region, kön, ålder och inkomstklass. År 1999 - 2019). 14 January, 2021. In Swedish: Inkomst/dag beräknat utifrån: Medelinkomst, År 2018, Ålder 20-64år, Alla kön. Available from: https://www.statistikdatabasen.scb.se/pxweb/sv/ssd/START__HE__HE0110__HE0110A/SamForvInk1/. Accessed 21 Jul 2022.
The Swedish Tax Agency. Businesses and employers. 21 January, 2021. Available from: https://skatteverket.se/servicelankar/otherlanguages/inenglish/businessesandemployers.4.12815e4f14a62bc048f5159.html. Accessed 21 Jul 2022.
Bermingham SL, Ashe JF. Systematic review of the impact of urinary tract infections on health-related quality of life. BJU Int. 2012;110(11 Pt C):E830–6.
Burström K, Johannesson M, Rehnberg C. Deteriorating health status in Stockholm 1998–2002: results from repeated population surveys using the EQ-5D. Qual Life Res. 2007;16(9):1547–53.
Cuthbertson BH, et al. Mortality and quality of life in the five years after severe sepsis. Crit Care. 2013;17(2):R70.
Briggs A. Probabilistic analysis of cost-effectiveness models: statistical representation of parameter uncertainty. Value Health. 2005;8(1):1–2.
The Swedish eHealth Agency. The Pharmaceutical Register.
European Central Bank, Swedish krona (SEK). Conversion rate: 1 SEK = 0.09655 (average in January 2022). 2022.
Thokala P, et al. Cost-effectiveness thresholds: the past, the present and the future. Pharmacoeconomics. 2018;36(5):509–12.
Svensson M, Nilsson FO, Arnberg K. Reimbursement decisions for pharmaceuticals in Sweden: the impact of disease severity and cost effectiveness. Pharmacoeconomics. 2015;33(11):1229–36.
Schwappach DLB. Resource allocation, social values and the QALY: a review of the debate and empirical evidence. Health Expect. 2002;5(3):210–22.
Shah KK. Severity of illness and priority setting in healthcare: a review of the literature. Health Policy. 2009;93(2):77–84.
Skedgel C, Wranik D, Hu M. The relative importance of clinical, economic, patient values and feasibility criteria in cancer drug reimbursement in Canada: a revealed preferences analysis of recommendations of the Pan-Canadian Oncology Drug Review 2011–2017. Pharmacoeconomics. 2018;36(4):467–75.
Bell BG, et al. A systematic review and meta-analysis of the effects of antibiotic consumption on antibiotic resistance. BMC Infect Dis. 2014;14:13.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Open access funding provided by University of Gothenburg.
Conflict of interest
Sofie Larsson, Charlotta Edlund, Pontus Nauclér, Mikael Svensson, and Anders Ternhag have no conflicts of interest that are directly relevant to the content of this article.
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for publication
Not applicable.
Availability of Data and Material
Data used in this study come from the published literature, please see Table 1 and the reference list for further information.
Code Availability
The model was shared for the peer review process. The authors can provide more details upon request.
Authors’ Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by SL, CE, and AT. SL performed the analysis. SL wrote the first draft of the manuscript, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Additional information
The original online version of this article was revised: The Open Access funding information was missed and published in the original version.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Larsson, S., Edlund, C., Nauclér, P. et al. Cost-Effectiveness Analysis of Temocillin Treatment in Patients with Febrile UTI Accounting for the Emergence of Antibiotic Resistance. Appl Health Econ Health Policy 20, 835–843 (2022). https://doi.org/10.1007/s40258-022-00748-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40258-022-00748-7