Abstract
Background
Amidst growing evidence of the intricate link between physical and mental health, this study aims to dissect the relationship between the waist-to-weight index (WWI) and suicidal ideation within a representative sample of the US population, proposing WWI as a novel metric for suicide risk assessment.
Methods
The study engaged a sample of 9500 participants in a cross-sectional design. It employed multivariate logistic and linear regression analyses to probe the association between WWI and suicidal ideation. It further examined potential nonlinear dynamics using a weighted generalized additive model alongside stratified analyses to test the relationship's consistency across diverse demographic and health variables.
Results
Our analysis revealed a significant positive correlation between increased WWI and heightened suicidal ideation, characterized by a nonlinear relationship that persisted in the adjusted model. Subgroup analysis sustained the association's uniformity across varied population segments.
Conclusions
The study elucidates WWI's effectiveness as a predictive tool for suicidal ideation, underscoring its relevance in mental health evaluations. By highlighting the predictive value of WWI, our findings advocate for the integration of body composition considerations into mental health risk assessments, thereby broadening the scope of suicide prevention strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is a genuinely severe philosophical problem, and that is suicide [1], a profound societal crisis. Annually, approximately 700,000 individuals end their own lives [2]. According to the US Centers for Disease Control and Prevention (CDC), in 2021, there were 48,183 suicides in the US, a figure that escalated to 49,449 in 2022, indicating a 2.6% increase [3]. The complexity of suicide prevention is attributed to its multifaceted causes, including societal (e.g., familial responsibilities), political (e.g., policies on minimum wage), cultural (e.g., stereotypes of masculinity), and economic factors (e.g., unemployment, lower socioeconomic status) [4]. Identified risk factors encompass mental health disorders, substance abuse, chronic pain, a history of suicide in the individual or family, experiences of aggression, access to firearms at home, and recent discharge from incarceration [5,6,7,8,9]. Additionally, witnessing suicidal behaviors in others can heighten suicide risk [10]. Despite demographic variances among groups such as adolescents, sexual minorities, and adults, research consistently shows that individuals harboring suicidal thoughts face a greater risk of suicide completion than those without such thoughts [11,12,13,14]. Despite efforts across medical, socioeconomic, and political domains to mitigate and prevent suicide, a significant reduction in the prevalence of suicidal ideation remains elusive [15], highlighting the critical need for an in-depth examination of suicidal ideation.
Obesity represents a widespread, severe, and financially burdensome chronic condition affecting both adults and children. In 2022, the CDC reported that the prevalence of adult obesity in the US had escalated, with 22 states having an adult obesity prevalence at or above 35%, an increase from 19 states in 2021[16]. Obesity is a significant risk factor for a variety of severe health conditions, including hypertension, cardiovascular diseases, diabetes mellitus, asthma, joint disorders, cholelithiasis, as well as gallbladder disease. [5, 17, 18]. Doctors believe that obesity is a complex, heterogeneous chronic disease that manifests differently in patients and, therefore, requires individualized long-term management [19]. Consequently, identifying accurate and reliable metrics for evaluating obesity is critically essential.
Body mass index (BMI) has long been a widely accepted standard for identifying levels of obesity. However, BMI cannot distinguish excess fat, muscle, or bone mass. BMI cannot differentiate between locations of fat [20, 21]. It is generally accepted that abdominal (visceral) fat is more closely associated with health risks than fat in other body parts [22,23,24,25]. The weight-adjusted-waist index (WWI) represents a novel metric for obesity assessment, demonstrating enhanced precision in quantifying lean muscle and adipose tissue mass when juxtaposed with traditional measures such as BMI and waist circumference (WC) [26, 27]. The literature suggests that WWI is associated with a variety of conditions, including fatty liver, cognitive function, hyperuricemia, diabetes mellitus, kidney stones, dyslipidemia, and urinary incontinence [28, 27, 29,30,31,32,33]. It may serve as a more accurate predictor of risk.
Several studies identified associations between obesity and suicide risk, depressive symptoms, and mood problems [34,35,36,37], and they have all used BMI as an indicator for determining obesity. Notwithstanding, the relationship between WWI and the prevalence of suicidal ideation has not yet been investigated. Consequently, the present study seeks to elucidate the potential correlation between WWI and suicidal ideation within the representative sample of the US population, employing data sourced from the National Health and Nutrition Examination Survey (NHANES) from 2013 to 2018.
Methods
Data source and study participants
Our investigation leveraged datasets obtained from NHANES, a project spearheaded by the National Center for Health Statistics (NCHS) in the United States. This comprehensive survey collates physical assessments and interview responses to gather extensive data on demographics, socioeconomic status, and health-related information. Focused on the NHANES data from 2013 to 2018, our study sought to secure a current and emblematic sample of the US population. The data acquisition process was governed by stringent ethical protocols, including the endorsement from the NCHS's Research Ethics Review Board and the acquisition of informed, written consent from all contributors. This groundwork enables our examination of health patterns and supports formulating informed health policy recommendations.
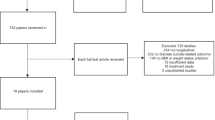
In this investigation, we employed a stratified, multistage probability sampling approach to ensure the comprehensive inclusion of participants. The initial participant pool comprised 29,400 individuals enrolled in the NHANES from 2013 to 2018. After excluding participants with incomplete data sets (N = 19,900), the analytical sample was refined to 9500 individuals (Fig. 1).
Definition of exposure variable
WWI is an anthropometric measure to assess central obesity. It derives from an individual’s WC and body weight. Each participant’s WWI is calculated using a specific formula: WC divided by the square root of body weight, with the outcome rounded to two decimal places (WWI = WC/√body weight, where WC is measured in cm and body weight in kg).
Assessment of suicidal ideation
Within the context of the survey’s Mental Health—Depression Screener segment, participants responded to a critical inquiry aimed at evaluating the presence of suicidal ideation: “Over the last two weeks, how often have you been troubled by thoughts of being better off dead, or by thoughts of self-harm?” Responses indicating such thoughts on “Several days”, “More than half the days”, or “Nearly every day” were interpreted as markers of suicidal ideation.
Covariates
We incorporated a comprehensive set of covariates: age, sex, race, education, marital status, smoking status, alcohol consumption, hypertension, diabetes, angina pectoris, arthritis, cancer, and asthma. Education was divided into two categories: individuals with qualifications higher than high school. Smoking status encompassed those who have smoked at least 100 cigarettes in their lifetime. Alcohol consumption was defined as having at least 12 alcoholic beverages annually.
Statistical analysis
We meticulously analyzed the demographic characteristics of participants, differentiated by the presence of suicidal ideation, employing weighted Chi-square tests for categorical variables and t-tests for continuous ones. The relationship between WWI and suicidal ideation was explored through multivariate logistic regression analyses. In contrast, the correlation between WWI and the level of suicidal ideation was examined using multivariate linear regression analyses. To uncover any potential nonlinear dynamics between WWI and suicidal ideation, we applied a weighted generalized additive model complemented by smooth curve fitting techniques. Additionally, stratified analyses and interaction tests were conducted to investigate the consistency of the WWI–suicidal ideation relationship across various subgroups. On a two-tailed basis, a p-value of less than 0.05 indicated statistical significance. All statistical analyses were performed using R Statistical Software (Version 4.2.2, available at http://www.R-project.org, developed by The R Foundation) and the Free Statistics analysis platform (Version 1.8, based in Beijing, China).
Results
Characteristics of the study participants
A total of 9500 participants were included in our research, with 9173 not exhibiting suicidal ideation and 327 reporting suicidal ideation. The overall prevalence of suicidal ideation was 3.44% (weighted proportion) (Table 1). A key finding from Table 1 is the statistically significant difference in WWI between groups (p < 0.001), with individuals exhibiting SI having a higher mean WWI than those without. This suggests that WWI may be a relevant factor in understanding suicidal ideation. Conversely, BMI does not significantly differ between groups (p = 0.401).
Association between WWI and suicidal ideation
Table 2 details the results from multivariate logistic regression analyses conducted using two distinct models. These analyses identified a strong and statistically significant positive association between WWI and the likelihood of suicidal ideation, consistent across both models. After comprehensive adjustment, individuals with a one-unit increase in WWI were found to have a 67.9% heightened risk of experiencing suicidal ideation [OR: 1.679, 95% CI 1.532–1.969]. Moreover, when analyzing WWI by quartiles, those in the highest quartile of WWI faced a risk increase of 1.761 times compared to individuals in the lowest quartile [OR: 2.761, 95% CI 2.062–3.698], as shown in Table 2. A generalized model incorporating smooth curve fitting was also utilized to validate the nonlinear association between WWI and suicidal ideation. The analysis confirmed a nonlinear positive relationship between WWI and suicidal ideation (Fig. 2), with the observed patterns remaining consistent across both genders (Fig. 3).
The association between WWI and suicidal ideation of different genders. The solid red line represents the smooth curve fit of females between variables. The solid blue line represents the smooth curve fit of males between variables. The shadow area represents the 95% confidence interval from the fit: weight-adjusted-waist index, WWI
Association between WWI and the level of suicidal ideation
Table 3 elucidates the significant association between WWI and the level of suicidal ideation, treating both variables as continuous. Initial findings from the unadjusted Model 1 reveal an exponentiated coefficient of 2.770 (95% CI 1.011–1.028), highlighting a statistically significant positive relationship. The adjusted Model 2, which considers a range of health behaviors and conditions, presents an exponentiated coefficient of 1.023 (95% CI 1.012–1.035), indicating a significant link between higher WWI and increased suicidal ideation levels (p < 0.01). Quartile analysis further corroborates these findings, with the highest WWI quartile (Q4) demonstrating a notably elevated risk (p for trend < 0.001). These insights underscore the vital connection between WWI and the severity of suicidal thoughts.
Subgroup analyses
To assess the uniformity of the association between WWI and suicidal ideation across the representative sample of the US population and to pinpoint any parameters specific to subpopulations, we undertook a detailed subgroup analysis alongside interaction tests. Table 4 examines the odds ratio (OR) for suicidal thoughts across different demographics and health conditions, indicating no significant interaction effects based on sex, age, education level, smoking status, alcohol consumption, hypertension, diabetes, angina pectoris, arthritis, cancer, or asthma. The odds ratios suggest a relatively consistent association across these subgroups, with variations in the magnitude of risk but no statistically significant differences in the pattern of association. In parallel, Table 5 explores the exponentiated coefficient for the level of suicidal ideation across similar subgroups, again showing no significant interaction effects, which implies a uniform relationship between WWI and the severity of suicidal ideation across different demographic and health-related categories.
Discussion
We sought to elucidate the association between WWI and the propensity for suicidal ideation within the representative sample of the US population. Conducting a comprehensive cross-sectional analysis with 9500 participants, we discerned a significant correlation that elevated WWI was significantly associated with increased suicidal ideation and increased levels of suicidal ideation. This study unveiled a nonlinear positive correlation between WWI and the incidence of suicidal thoughts, a relationship that persisted even after complete adjustments in our model. Subsequent subgroup analyses revealed that the predictive validity of WWI for suicidal ideation remained unaffected across various demographic and health-related factors, including smoking status, alcohol intake, and the presence of chronic conditions such as hypertension, diabetes, and asthma. These insights collectively affirm the potential of WWI as an efficacious predictor for suicidal ideation, underscoring its utility in mental health assessments.
Several studies documented that the prevalence of suicidal ideation or depressive symptoms increases with BMI [34, 35, 38, 39]. However, due to BMI's limitations, including its inability to differentiate between excess fat, muscle, or bone mass, and its failure to discern body fat distribution across different locations, some studies are beginning to experiment with other indicators. A study showed a significant relationship between WC, waist–height ratio, and suicidal ideation among US adult women. A Korean survey showed that BMI, WC, waist-to-hip ratio, and percent body fat were not significantly associated with suicidal ideation. In contrast, sarcopenia was strongly associated with an increased risk of suicidal ideation in older men [40]. It has also been shown that sarcopenic obesity is significantly associated with suicidal ideation [40]. Low height and perceived obesity are associated with suicidal ideation in Korean adolescents [41]. These studies also imply WWI's potential as a novel index of obesity. However, the validity of these indicators needs to be confirmed by more extensive clinical studies. In recent years, it has been found that WWI is a superior predictor of non-alcoholic fatty liver disease [33], low cognitive performance [27], hyperuricemia [28], diabetic kidney disease [42], kidney stones [30], stress urinary incontinence [31], and depressive symptoms [43]. WWI has excellent potential as an anthropometric indicator because of its easy computation and strong ability to forecast disease onset [44].
There may be multiple mechanisms for the interaction between obesity and suicidal ideation. First, the coexistence of obesity with other medical diseases may exacerbate the situation, or chronic health challenges may lead to increased mental stress, which in turn produces higher levels of suicidal ideation. It has been established that the coexistence of overweight or obesity and depression exacerbates the inflammatory response, leading to a worse prognosis and increased risk of suicide in adolescents with major depressive disorder [37]. In the setting of fibromyalgia and concomitant obesity, prior research points to a distinct (i.e., irrespective of depressive symptomatology and sleep quality) relationship between pain catastrophizing and suicidal thoughts [45]. Another research found that BMI is a risk factor for the development of severe anxiety symptoms in patients with severe anxiety disorder with comorbid dyslipidemia [46]. In addition, in patients with bipolar disorder, elevated BMI is associated with worsening clinical features, including higher rates of suicide, comorbidities, and core depressive symptoms. Second, obesity is associated with biochemical changes in the body, which may impact mood and behavior. It has been shown that obesity is associated with elevated levels of inflammation in the body [47,48,49], and inflammation is thought to be a possible mechanism that leads to depression and other mood disorders [50]. Some researchers believe that obesity may lead to insulin imbalance, and insulin resistance has been linked to depression [51]. There is also evidence that adipose tissue produces and releases various chemicals called adipokines, which directly affect other body parts, including the brain [52]. As a result, evaluating obesity is essential to estimating the likelihood of suicidal thoughts, and this study’s results suggest that WWI may be an effective indicator of obesity.
WWI combines body weight and waist measurements for a nuanced overview of fat distribution, offering advantages over BMI and WC, which overlook crucial aspects of body composition and total weight. From a pathophysiological perspective, WWI might provide a more explicit link to metabolic and cardiovascular risks associated with obesity. Abdominal fat, as measured by WC, is a known risk factor for metabolic syndrome, type 2 diabetes, and cardiovascular disease, which may be due to adipose gene expression of the effector genes [53], its proximity to vital organs and its role in producing inflammatory adipokines [54, 55]. However, incorporating the weight component could enhance the predictive power by indicating the overall load on the body, including the strain on bones, joints, and organs [56, 57]. Furthermore, the integrated approach of WWI better reflects the adiposity-related biochemical stress on the body. This includes the effects of fat mass on cytokine production [58], insulin resistance [59], and lipid metabolism [60], all of which are crucial for understanding the physiological basis for depression and suicidal ideation linked to obesity.
Social workers can effectively utilize WWI in their practice to identify individuals more accurately at high risk of suicide. By providing psychological support and counseling, establishing support systems, promoting education on healthy lifestyles, assisting in accessing medical and nutritional resources, and providing crisis intervention and referrals, social work can not only help the obese population improve their mental health but also improve their quality of life, thus playing a pivotal role in suicide prevention.
Despite its contributions, our study is not without limitations. First, the cross-sectional nature of our analysis precludes us from elucidating the causal mechanisms and effects underlying the observed associations. Second, the potential for inaccuracies in the covariates included may impact the results' precision. Third, it is essential to note that the results of this study may not necessarily translate into clinical implications, mainly due to the large sample size, which can amplify minor variations. Fourth, our analysis does not account for the potential influence of weight reduction treatments [61] on WWI due to data constraints, which could affect the associations observed. Nonetheless, our research is strengthened by its foundation on a substantial and representative dataset derived from the NHANES, providing a robust basis for our findings. Moreover, we are the first to investigate the relationship between WWI and suicidal ideation, including a variety of subgroup analyses.
Conclusion
Elevated WWI was significantly associated with increased suicidal ideation. Relative to BMI, WWI demonstrates enhanced predictive efficacy for suicidal ideation. This facilitates the timely identification of suicide risk by social workers. Nonetheless, additional studies are necessary to validate these preliminary outcomes.
Availability of data and materials
The datasets analyzed during the current study are available in the NHANES [https://www.cdc.gov/nchs/nhanes/index.htm].
References
Camus A (2010) Le mythe de Sisyphe: [essai sur l’sabsurde]. Chicoutimi: J-M Tremblay.
World Health Organization (2024) Suicide prevention: World Health Organization. https://www.who.int/health-topics/suicide#tab=tab_1. Accessed 16 Mar 2024
U.S. Centers for Disease Control and Prevention (2023) Suicide Data and Statistics: U.S. Centers for Disease Control and Prevention. https://www.cdc.gov/suicide/suicide-data-statistics.html. Accessed 16 Mar 2024
Stack S (2021) Contributing factors to suicide: political, social, cultural and economic. Prev Med 152:106498
Aboumrad M, Shiner B, Riblet N, Mills PD, Watts BV (2018) Factors contributing to cancer-related suicide: a study of root-cause analysis reports. Psychooncology 27(9):2237–2244
Bailo P, Gibelli F, Celletti A, Caraffa A, Sirignano A, Ricci G (2023) The contributing factors to suicide in Italian prisons: an 11-year analysis (2010–2020). Crim Behav Ment Health 33(6):441–454
Crook M (2003) Out of the darkness: teens and suicide. Arsenal Pulp Press, Vancouver
Suicide HM (2012) Detroit. Greenhaven Press, New York
Murfree L, DeMaria AL, Schwab-Reese LM (2022) Factors contributing to filicide-suicide: differences between male and female perpetrators. Child Abuse Neglect 129:105637
Ong MS, Lakoma M, Gees Bhosrekar S, Hickok J, McLean L, Murphy M et al (2021) Risk factors for suicide attempt in children, adolescents, and young adults hospitalized for mental health disorders. Child Adolesc Mental Health 26(2):134–142
Power E, Coughlan H, Clarke M, Kelleher I, Lynch F, Connor D et al (2016) Nonsuicidal self-injury, suicidal thoughts and suicide attempts among sexual minority youth in Ireland during their emerging adult years. Early Interv Psychiatry 10(5):441–445
van Vuuren CL, van der Wal MF, Cuijpers P, Chinapaw MJM (2021) Sociodemographic differences in time trends of suicidal thoughts and suicide attempts among adolescents living in Amsterdam, The Netherlands. Crisis 42(5):369–377
van Wijnen LG, Boluijt PR, Hoeven-Mulder HB, Bemelmans WJ, Wendel-Vos GC (2010) Weight status, psychological health, suicidal thoughts, and suicide attempts in Dutch adolescents: results from the 2003 E-MOVO project. Obesity 18(5):1059–1061
Yang C, Huebner ES, Tian L (2024) Prediction of suicidal ideation among preadolescent children with machine learning models: a longitudinal study. J Affect Disord 352:403–409
Karaye IM (2022) Differential trends in US suicide rates, 1999–2020: Emerging racial and ethnic disparities. Prev Med 159:107064
Centers for Disease Control and Prevention (2022) Nutrition, physical activity, and obesity: data, trends and maps. https://nccd.cdc.gov/dnpao_dtm/rdPage.aspx?rdReport=DNPAO_DTM.ExploreByTopic&islClass=OWS&islTopic=&go=GO. Accessed 16 Mar 2024
National Heart L, Blood Institute (1998) Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults
National Heart L, Blood Institute (2013) Managing overweight and obesity in adults: systematic evidence review from the obesity expert panel
Wharton S, Lau DCW, Vallis M, Sharma AM, Biertho L, Campbell-Scherer D et al (2020) Obesity in adults: a clinical practice guideline. CMAJ 192(31):E875–E891
Cole TJ, Faith MS, Pietrobelli A, Heo M (2005) What is the best measure of adiposity change in growing children: BMI, BMI %, BMI z-score or BMI centile? Eur J Clin Nutr 59(3):419–425. Erratum: 2005 June;59(6):807
Freedman DS, Woo JG, Ogden CL, Xu JH, Cole TJ (2019) Distance and percent distance from median BMI as alternatives to BMI z-score. Br J Nutr 124(5):493–500
Golan Shekhtman S, Boccara E, Ravona-Springer R, Inbar Y, Zelicha H, Livny A et al (2024) Abdominal fat depots are related to lower cognitive functioning and brain volumes in middle-aged males at high Alzheimer’s risk. Obesity. https://doi.org/10.1002/oby.24004
Haidar A, Srikanthan P, Watson K, Allison M, Kronmal R, Horwich T (2024) Associations between visceral fat, abdominal muscle, and coronary artery calcification: a cross-sectional analysis of the Multi-Ethnic Study of Atherosclerosis. Am J Cardiol. https://doi.org/10.1016/j.amjcard.2024.02.030
Ma M, Luo M, Liu Q, Zhong D, Liu Y, Zhang K (2024) Influence of abdominal fat distribution and inflammatory status on post-operative prognosis in non-small cell lung cancer patients: a retrospective cohort study. J Cancer Res Clin Oncol 150(3):111
Yoshida K, Kondo E, Ishida M, Ichikawa Y, Watashige N, Okumura A et al (2024) Visceral adipose tissue percentage compared to body mass index as better indicator of surgical outcomes in women with obesity and endometrial cancer. J Minim Invasive Gynecol. https://doi.org/10.1016/j.jmig.2024.02.009
Qin Z, Du D, Li Y, Chang K, Yang Q, Zhang Z et al (2022) The association between weight-adjusted-waist index and abdominal aortic calcification in adults aged ≥ 40 years: results from NHANES 2013–2014. Sci Rep 12(1):20354
Wang X-L, Feng H-L, Xu X-Z, Liu J, Han X (2024) Relationship between cognitive function and weight-adjusted waist index in people ≥ 60 years old in NHANES 2011–2014. Aging Clin Exp Res 36(1):30
Chen D, Lu C, Chen K, Liu T, Li Y, Shan Z et al (2024) Association between anthropometric indices and hyperuricemia: a nationwide study in China. Clin Rheumatol 43(3):907–920
Ding Y, Lv S, Xie R, Ye W, Luo Y, Li Y (2024) Association of weight-adjusted-waist index and diabetic kidney disease in type 2 diabetes mellitus. Endocr Connect. https://doi.org/10.1530/EC-23-0491
Gui Z, Yu L, Chen Y, Zhang M, He J, Hao Y (2023) Study from the United States: increased prevalence of kidney stones in patients with high weight-adjusted waist index. Front Nutr 10:1171775
Sun D, He H, Luo B, Xie B (2024) The association between weight-adjusted-waist index and stress urinary incontinence in female adults: a population-based study. Int Urol Nephrol. https://doi.org/10.1007/s11255-023-03928-z
Takhttavous A, Saberi-Karimian M, Hafezi SG, Esmaily H, Hosseini M, Ferns GA et al (2024) Predicting the 10-year incidence of dyslipidemia based on novel anthropometric indices, using data mining. Lipids Health Dis 23(1):33
Yu C, He S, Kuang M, Wang C, Huang X, Sheng G et al (2024) Association between weight-adjusted waist index and non-alcoholic fatty liver disease: a population-based study. BMC Endocr Disord 24(1):22
Law S, Dong S, Zhou F, Zheng D, Wang C, Dong Z (2023) Bariatric surgery and mental health outcomes: an umbrella review. Front Endocrinol 14:1283621
Meshkat S, Liu Y, Jung H, Tassone VK, Pang H, Janssen-Aguilar R et al (2024) Temporal associations of BMI and glucose parameters with depressive symptoms among US adults. Psychiatry Res 332:115709
Mowoh DPM, Cole R, Sarvepalli S, Grover K, Abbas M, Khaitan L (2024) Bariatric surgery efficacy in patients with mood disorders. Surgery. https://doi.org/10.1016/j.surg.2023.11.032
Ninla-Aesong P, Puangsri P, Kietdumrongwong P, Jongkrijak H, Noipha K (2023) Being overweight and obese increases suicide risk, the severity of depression, and the inflammatory response in adolescents with major depressive disorders. Front Immunol 14:1197775
Kim MS, Kim JY, Song YS, Hong S, Won HH, Kim WJ et al (2024) Association of bariatric surgery with indicated and unintended outcomes: an umbrella review and meta-analysis for risk-benefit assessment. Obes Rev 25(3):e13670
Xu B, Chen C, Wang D (2024) Current psychotic-like experiences among Chinese college students: prevalence, correlates, and its relationship with suicidal ideation. Psychol Res Behav Manag 17:799–811
Cho Y, Shin SY, Shin MJ (2015) Sarcopenic obesity is associated with lower indicators of psychological health and quality of life in Koreans. Nutr Res 35(5):384–392
Kim B, Kim HS, Park S, Kwon JA (2023) BMI and perceived weight on suicide attempts in Korean adolescents: findings from the Korea Youth Risk Behavior Survey (KYRBS) 2020 to 2021. BMC Public Health 23(1):1107
Ding Y, Lv S, Xie R, Ye W, Luo Y, Li Y (2024) Association of weight-adjusted waist index and diabetic kidney disease in type 2 diabetes mellitus. Endocr Connect 13(4):e230491
Liu H, Zhi J, Zhang C, Huang S, Ma Y, Luo D et al (2024) Association between Weight-Adjusted Waist Index and depressive symptoms: a nationally representative cross-sectional study from NHANES 2005 to 2018. J Affect Disord 350:49–57
Ding Y, Xu Z, Zhou X, Luo Y, Xie R, Li Y (2023) Association between weight-adjusted-waist index and the risk of hyperuricemia in adults: a population-based investigation. Front Endocrinol 14:1236401
Varallo G, Scarpina F, Arnison T, Giusti EM, Tenti M, Rapelli G et al (2024) Suicidal ideation in female individuals with fibromyalgia and comorbid obesity: prevalence and association with clinical, pain-related, and psychological factors. Pain Med 25(3):239–247
Yin H, Zhang Q, Li Y, Ma J (2023) Prevalence and correlates of severe anxiety in patients with first hospitalization for major depressive disorder combined with dyslipidemia: a large sample cross-sectional study. Front Psychiatry 14:1289614
Freitas R, Vasques ACJ, da Rocha FG, Ribeiro FB, Solar I, Shivappa N et al (2024) Gut bacterial markers involved in association of dietary inflammatory index with visceral adiposity. Nutrition 122:112371
Liu Y, Dong Y, Wang X, Xu X (2024) Association between metformin treatment and coronary artery inflammation based on pericoronary adipose tissue attenuation in type 2 diabetes mellitus patients. J Clin Hypertens. https://doi.org/10.1111/jch.14777
Poynter ME, Mank MM, Ather JL (2024) Obesity-associated inflammatory macrophage polarization is inhibited by capsaicin and phytolignans. Am J Physiol Regul Integr Comp Physiol. https://doi.org/10.1152/ajpregu.00161.2023
Capuron L, Miller AH (2011) Immune system to brain signaling: neuropsychopharmacological implications. Pharmacol Ther 130(2):226–238
Kan C, Silva N, Golden SH, Rajala U, Timonen M, Stahl D et al (2013) A systematic review and meta-analysis of the association between depression and insulin resistance. Diabetes Care 36(2):480–489
Trayhurn P (2022) Adipokines: inflammation and the pleiotropic role of white adipose tissue. Br J Nutr 127(2):161–164
Aberra YT, Ma L, Björkegren JLM, Civelek M (2023) Predicting mechanisms of action at genetic loci associated with discordant effects on type 2 diabetes and abdominal fat accumulation. Elife 12:e79834
Tadiotto MC, Corazza PRP, de Menezes-Junior FJ, Tozo TAA, de Moraes-Junior FB, Brand C et al (2024) Moderating role of 1-minute abdominal test in the relationship between cardiometabolic risk factors and adiponectin concentration in adolescents. BMC Pediatr 24(1):75
Tremblay EJ, Tchernof A, Pelletier M, Joanisse DR, Mauriège P (2024) Plasma adiponectin/leptin ratio associates with subcutaneous abdominal and omental adipose tissue characteristics in women. BMC Endocr Disord 24(1):39
Bahramian M, Arjmand N, El-Rich M, Parnianpour M (2023) Effect of obesity on spinal loads during load-reaching activities: a subject- and kinematics-specific musculoskeletal modeling approach. J Biomech 161:111770
Singhal V, Huynh C, Nimmala S, Mitchell DM, Pedreira CC, Bader A et al (2022) Load-to-strength ratio at the radius is higher in adolescent and young adult females with obesity compared to normal-weight controls. Bone 164:116515
Brydon L, Wright CE, O’Donnell K, Zachary I, Wardle J, Steptoe A (2008) Stress-induced cytokine responses and central adiposity in young women. Int J Obes 32(3):443–450
Dhokte S, Czaja K (2024) Visceral adipose tissue: the hidden culprit for type 2 diabetes. Nutrients 16(7):1015
Soedono S, Sharlene S, Vo DHN, Averia M, Rosalie EE, Lee YK et al (2024) Obese visceral adipose dendritic cells downregulate regulatory T cell development through IL-33. Front Immunol 15:1335651
Nazzaro P, Amatuzio A, Baranello S, Corvinelli M, Di Cienzo G, Principe F et al (2023) Renal damage and obesity: a silent pairing. G Ital Nefrol 40(3):2023
Acknowledgements
We want to thank Yihui Zhao for his help with data processing.
Funding
This work was supported by the Kunshan Traditional Chinese Medicine Hospital Youth Science and Technology Fund [Grant numbers: 2020QNJJ03].
Author information
Authors and Affiliations
Contributions
G.S. and Q.G.: methodology, formal analysis, writing—original draft; C.Q. and Y.G.: conceptualization, methodology, supervision, writing—review and editing.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The data acquisition process was governed by stringent ethical protocols, including the endorsement from the NCHS's Research Ethics Review Board and the acquisition of informed, written consent from all contributors. NHANES adheres to moral norms and standards that prioritize participant consent, privacy and data protection, IRB approval, compliance with laws and guidelines, including the Declaration of Helsinki and HIPAA, and minimization of risk to ensure the welfare and rights of participants while maintaining the scientific integrity and accuracy of the research. Human Ethics and Consent to Participate declarations: not applicable. Details can be found at https://www.cdc.gov/nchs/nhanes/irba98.htm.
Documented consent to participate was obtained from participants. Details can be found at https://www.cdc.gov/nchs/nhanes/irba98.htm.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests that pertain to this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Guo, S., Qing, G., Chen, Q. et al. The relationship between weight-adjusted-waist index and suicidal ideation: evidence from NHANES. Eat Weight Disord 29, 37 (2024). https://doi.org/10.1007/s40519-024-01666-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40519-024-01666-4