Abstract
Though many individuals in the United States of America and worldwide identify as LGBTQ + (lesbian, gay, bisexual, transgender, queer, intersex, asexual, and other identities), educational programs for allied health professions often do not adequately cover LGBTQ + issues. The literature clearly identifies a dearth of LGBTQ + information in undergraduate, graduate, and continuing education for allied health professionals. This lack of education and training causes real and perceived prejudice and discrimination by healthcare professionals against people who identify as LGBTQ +. Pertinent issues for people who identify as LGBTQ + and the language used to refer to these individuals changes over time so the LGBTQ + content that allied health education programs cover should be periodically reevaluated. This article summarizes the current state of education on LGBTQ + issues in allied health professions education and suggests contemporary LGBTQ + content that should be included in allied health professions education.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
The Lesbian, Gay, Bisexual, Transgender, and Queer (LGBTQ +) communities encounter significant challenges in receiving adequate healthcare due to systemic barriers to healthcare access, societal stigma, and potential biases from the healthcare providers [16]. Most studies that aim to close these healthcare gaps in the LGBTQ + communities focused on medical professionals, such as physicians and nurses. However, the allied health professionals have close contact with the communities and are uniquely positioned to improve the quality of healthcare for the LGBTQ + population. Here, we argue that allied health professionals are an essential component for promoting better health outcomes for the LGBTQ + communities, and therefore training programs should include LGBTQ + -related education in their curriculum. We then review the current state of LGBTQ + curricula for allied health professionals and provide a brief overview of the topics that should be covered within these curricula.
The Association of Schools Advancing Health Professions (ASAHP) defined allied health professions as being distinct from medicine and nursing. It can include a variety of professionals “who use scientific principles and evidence-based practice for the diagnosis, evaluation and treatment of acute and chronic diseases; promote disease prevention and wellness for optimum health and apply administration and management skills to support health care systems in a variety of settings” [4]. A few examples of allied health professionals are physical therapists, occupational therapists, and athletic trainers. A significant proportion of healthcare interactions are provided by allied health professionals. It was estimated that around 60% of the healthcare workforce in the United States consists of allied health professionals [4]. Therefore, allied health professionals are an integral component in ensuring equitable healthcare services.
1.1 Importance of LGBTQ + inclusive care in allied health professions
Although LGBTQ + individuals face similar health concerns as the general population, LGBTQ + individuals face unique healthcare challenges, including access to healthcare coverage, difficulties in finding culturally competent care, and federal and state policies that reinforce stigmatization and marginalization [14]. LGBTQ + identifying individuals experience worse mental and physical health outcomes in comparison to the general population, have worse access to healthcare, and engage in fewer health promoting behaviors because of these unique experiences [11, 14].
To reduce the health disparities experienced by LGBTQ + individuals, one needs to address both the immediate environment, the patient provider relationship with provider education, and the structural barriers to healthcare such as healthcare insurance coverage [1]. Allied health professions are uniquely positioned to address health disparities experienced by LGBTQ + individuals by affecting both the interpersonal environment and healthcare access. Many allied health professionals have more points of contact with their patients than physicians, as they often provide services outside of strictly clinical settings, such as hospitals or other primary care facilities. For instance, occupational therapists often work in school settings where LGBTQ + identifying or questioning adolescents are accessing services. Physical therapists may be working directly in patients’ homes.
Many LGBTQ + identifying individuals distrust medical professionals due to experiencing heteronormative microaggressions and stigmatization by their healthcare providers [16, 51]. In contrast, LGBTQ + individuals who had positive relationships with a health professional talked about an enhanced sense of well-being and health [29]. Being able to disclose sexual orientation and gender identities when interacting with a healthcare professional may reduce stress and improve mental health, and increase access to supportive services unique to their LGBTQ + identity [21]. Allied health professionals who have frequent contact with their patients or clients have the potential to provide positive and affirming experiences to LGBTQ + individuals and therefore enhance their health through the interpersonal environment.
On a systemic barrier level, allied health professions also include health administrators, who are responsible for navigating the insurance policies and ensure that patients can access medical care services with affordable costs. Many transgender individuals carry a heavy burden in simply accessing basic healthcare [41]. For instance, if a patient’s gender marker is changed from female to male, a healthcare administrator may need to go the extra distance in ensuring that basic checkup services, such as a pap smear, are still provided to the patient. Often, even if gender-affirming services are covered by an insurance policy, significant barriers exist for transgender individuals in navigating the complex insurance authorization process. Education on the common scenarios that LGBTQ + individuals face can improve health administrators’ proficiency in ensuring insurance covered services for this population.
Inclusion about LGBTQ + individuals and health are significant not only to teaching cisgender heterosexual allied health students regarding the topic, but also to retain students with LGBTQ + identities within such fields. LGBTQ + students within the allied health fields may be better able to serve the LGBTQ + community as allied health professionals, due to possible similarities in identity, background, and experiences. Studies regarding patient preference of LGBTQ + individuals have found that they are more comfortable when speaking with providers who are competent about LGBTQ + identities [28]. Hence, the involvement and retention of LGBTQ + within allied health fields is crucial when aiming to provide inclusive healthcare to LGBTQ + patients.
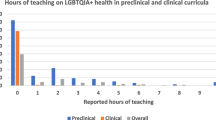
To provide more equitable care to LGBTQ + individuals, allied health students must also learn to combat heteronormative assumptions. Heteronormative assumptions can result in discrimination against LGBTQ + populations. For example, asserting that partners are always of opposite sex, may posit the notion that one’s identity as LGBTQ + is immoral. Until now, in the health curriculum in the U.S. has ignored LGBTQ + health related issues. For example, within U.S. medical schools, it was previously reported that medical students in their preclinical years spent a median of only 5 h on LGBTQ + health related issues [39]. The inadequate preparedness of physician to handle situation with LGBTQ + heath often poses challenges in practitioner patient interaction. Health care professionals who exhibited heteronormativity in their approach also perpetuates already existing health disparities for LGBTQ + communities [44]. This also results in avoidance of health care in LGBTQ + community due to existing health disparities [26].
1.2 Current state of allied health professions education
The current state of allied health professions education reflects biases against people who identify as LGBTQ + . These biases are not historical—dozens of transphobic and homophobic laws have been proposed or passed since 2020 alone [22]. Healthcare providers in all fields will encounter LGBTQ + people so it is essential for all healthcare providers to appreciate the social context that their patients experience. For centuries, Western healthcare systems have overwhelmingly pathologized gender diversity and same-sex contact [12]. Castration, the forced sex reassignment of children without their consent, and refusal to provide life-saving medically necessary care were, and in many places still are, the norm for LGBTQ + people [12, 15]. These identities were viewed as disorders, resulting in systematic prejudice and discrimination against gender and sexual minorities that persists today. Healthcare providers in all fields will encounter LGBTQ + people, so it is essential for all healthcare providers to appreciate the social context that their patients experience.
This prejudice against LGBTQ + people is visible in the curricula that allied healthcare educational programs use, the legal responsibilities that healthcare providers have toward LGBTQ + people, and in interpersonal interactions with healthcare providers. Sweeping statements about the state of allied healthcare professions education are difficult because of the diversity of educational requirements, clinical standards, and certifying organizations across allied health disciplines [3, 43, 47]. Some trends across the allied healthcare professions literature include reduced healthcare access and utilization for LGBTQ + people and poorer healthcare quality when healthcare services are accessed.
The literature comprehensively shows that the amount of education that healthcare providers receive is inadequate to provide competent services to people who identify as LGBTQ + [9, 23, 31, 36]. Even allied healthcare fields with longer duration of education such as audiology, which requires around 8 years of higher education, do not typically provide adequate content on LGBTQ + people [34, 36]. The level of training and provider comfort in working with LGBTQ + patients varies by discipline, and allied healthcare providers may be more comfortable with LGBTQ + people than medical and nursing fields [52]. Clinical preparedness, number of LGBTQ + patients seen, and basic knowledge varies by field but is generally even worse in allied health professions than the medical field which has many clearly demonstrated disparities [38] though some allied healthcare providers may be more comfortable with LGBTQ + people than medical and nursing fields [52]. Research has comprehensively shown that more education on LGBTQ + issues increases provider competence with this population—more training in the allied healthcare fields are clearly needed [8, 10]. Didactic education for students and continuing education for already-practicing professionals have both been suggested as routes to provide LGBTQ + competence training and subsequently improve care for LGBTQ + individuals seeing allied healthcare providers [6, 25, 52].
The inadequate amount of education on LGBTQ + issues in allied health professions often results in negative patient experiences when patients interact with healthcare providers. Some healthcare providers refuse outright to provide services to LGBTQ + identified patients, reducing the healthcare utilization by this population [7, 40, 46]. Once a patient has found a provider that is willing to work with them, lack of education on LGBTQ + identity causes difficulty in providing affirming healthcare services to LGBTQ + people. This lack of affirming care has been shown to lead to LGBTQ + patients feeling like they must educate their healthcare providers about their identities and results in many of these patients feeling that they are not treated respectfully by their healthcare providers [2, 30]. Bias and microaggressions are present in many providers, damaging the patient-provider relationship of allied healthcare providers seeing LGBTQ + individuals [13, 20, 35].
Due to health providers not being fully aware of LGBTQ + identities, patients may be prone to not disclose their identity or sexuality to their provider. Nondisclosure of identity to providers is common when accessing healthcare [17, 18]. There have been instances of LGBTQ + patients being refused care or facing prejudice from healthcare providers when they discussed their identity [5, 48]. Over one-third of LGBTQ + individuals in the U.S. did not disclose their identity to providers, either due to providers' assumptions regarding sexuality, maintaining privacy, and not feeling as if their identity was relevant to the healthcare they wished to receive [45]. Many, however, did mention that they did not share their identity with their provider due to fear of being treated differently due to their sexuality [45]. Because of providers' lack of competency regarding LGBTQ + identities and personal bias, they may be likelier to marginalize LGBTQ + individuals further or provide non-affirming care [5, 50]. Due to the current allied health curriculum, many healthcare professionals automatically assume that a patient is cisgender heterosexual or provide care from a heteronormative perspective [5, 18, 50]. As a result, LGBTQ + individuals may feel unwelcome and thus become hesitant to seek care in the future.
1.3 Essential LGBTQ + content for allied health professionals
1.3.1 Allied health curriculum
When re-envisioning the allied health curriculum to include LGBTQ + identities, it is important to consider the current courses offered that discuss this topic. Some universities offer courses that discuss the social and health issues of gender and sexual minorities. For example, the University of California, Irvine (UCI) currently offers both undergraduate and graduate level courses that discuss sexual and gender identity. However, none of these courses are directed completely at allied health students. Allied health students may not take these courses as electives. Moreover, it is important to note that these courses will differ from university to university. Courses offered in a more liberal setting, such as California, may differ from a university located in a more conservative area. This may further marginalize LGBTQ + individuals who reside or attend school is such areas.
Diverse course offerings can help to improve retention of LGBTQ + students in allied health fields. Providing instruction and an inclusive curriculum would allow LGBTQ + students and cisgender heterosexual students to participate in academic conversations across various fields such as sociology and anthropology, which can further improve diversity among allied health fields to better understand and approach social determinants of health. The inclusion of LGBTQ + courses within allied health can affirm the LGBTQ + identity of those within this field. Educators wishing to incorporate more LGBTQ + content into their curricula may find existing guidelines and literature on LGBTQ + education in the health sciences beneficial (for example, [9, 19, 33, 37].
1.4 Support on campus for LGBTQ + individuals
In addition to improving the curriculum, support groups and student centers for LGBTQ + individuals can improve the belonging and retention of LGBTQ + students within the allied health disciplines. Support groups or LGBTQ + resource centers are important sources of support for LGBTQ + college students [24, 27, 42]. The availability of a safe space where students can learn, study, and converse with those of a similar identity provides solidarity and inclusion. These resource centers on campus can improve awareness and education regarding LGBTQ + identities among those who do not identify with this community. This can help build some groundwork regarding LGBTQ + identities for those students who may not be as aware of these identities.
Previous literature has presented that faculty can contribute to positive influence on the inclusion and success of students In a study on 60 LGBTQ + students, it was found that a strong relationship between faculty and students resulted in the students feeling a sense of support within and outside of the classroom [32]. Within the classroom, it was found that faculty who utilized inclusive and affirming language and challenged heteronormative perspectives allowed students to express their opinions and have a positive learning environment [32]. Some participants discussed support outside the classroom, including advising LGBTQ + students or LGBTQ + organizations [32]. This also left students feeling like they belonged on campus and could navigate their campus environment with the guidance of a faculty who would support them. Faculties acting as allies to LGBTQ + students can further motivate LGBTQ + students to stay in school, combat discrimination, and attain a fulfilling higher education experience.
1.5 Patient contact and the current allied health curriculum
Provider ally-ship and understanding are essential to decrease inequity and discrimination and increase healthcare utilization by LGBTQ + individuals. Knowing and respecting an individual's preferred pronouns can be a crucial element in terms of patient contact and can be a mode to for healthcare professionals to communicate and build trust with their patients. It is recommended to ask for a patient’s preferred pronoun and name in a confidential and private setting at the beginning of a clinical conversation. When caring for younger patients, it is important to ask their pronouns in a sensitive manner. Also, it is essential to ask if they would prefer to use their affirmed pronouns in front of others, such as their parents and guardians.
Professionals must also be mindful of microaggressions when providing care to LGBTQ + patients. Microaggressions contribute to persistent barriers in LGBTQ + health care scenario. Microaggression is defined as “brief and commonplace daily verbal, behavioral, and environmental indignities, whether intentional or unintentional, that communicate hostile, derogatory, or negative racial, gender, sexual-orientation, and religious slights and insults to the target person and group” [49]. Environmental microaggressions against the LGBTQ + people are still common in organizational materials, art or other medias. For example, lack of gender-neutral washroom or gender-neutral words exaggerates the heteronormative microaggression in medical spaces. Unless the measures to reduce microaggressions come in practice in both health professional training, microaggressions will continue to affect patient—provider relationships.
1.6 Change is crucial
Change within the allied health curriculum is vital to warrant the inclusion and promotion of LGBTQ + health. Basic core competencies that allied health programs may include in their curricula are reported in Fig. 1. By integrating information regarding gender and sexual minorities into the allied health curriculum, students within the field will progress the necessary tools to provide efficient care to this population. By teaching students about gender and sexual minorities, they will be able to address this community more effectively and competently upon graduating from their allied health program.
Campus life for LGBTQ + students has improved in the U.S as this group becomes more and more integrated into society. However, LGBTQ + students are still at an increased risk for discrimination and prejudice due to their identities. Nevertheless, students expand and develop their identities through coursework, activism, and participation and collaboration on campus. Hence, aligning programming, curriculum, and pedagogy is vital to supporting LGBTQ + students.
2 Conclusion
Allied health professions represent both a source of challenges for LGBTQ + people attempting to access healthcare, and an opportunity to improve care for LGBTQ + individuals by improving education for these allied health professions. Education and support for allied health professionals can take place in undergraduate and graduate curriculums, and in continuing education targeted to the unique context of each allied health professions field. Improved care for LGBTQ + people is essential to reduce historic and continuing inequality for this population, and all allied health professions must be invested in providing affirming care to all LGBTQ + people.
References
Aleshire ME, Ashford K, Fallin-Bennett A, Hatcher J. Primary care providers’ attitudes related to LGBTQ people: a narrative literature review. Health Promot Pract. 2019;20(2):173–87. https://doi.org/10.1177/1524839918778835.
Alpert AB, Cichoskikelly EM, Fox AD. What lesbian, gay, bisexual, transgender, queer, and intersex patients say doctors should know and do: a qualitative study. J Homosex. 2017;64(10):1368–89. https://doi.org/10.1080/00918369.2017.1321376.
Arena RA, Goldberg LR, Ingersoll CD, Larsen DS, Shelledy D. Research in the allied health professions: why fund it? A report of the ASAHP Research Committee. J Allied Health. 2011;40(3):161–6.
Association of Schools Advancing Health Professions. (2020). What is Allied Health? https://www.asahp.org/what-is.
Beehler GP. Confronting the culture of medicine: Gay men’s experiences with primary care physicians. J Gay Lesbian Med Assoc. 2001;5(4):135–41. https://doi.org/10.1023/A:1014210027301.
Block RG, Sampson A, Gagliardi J, Augusto B, Santiago-Datil W, Schabath MB, Vadaparampil ST, Quinn GP. The LOvE ECHO training: developing a web-based LGBTQ cultural competency training module for oncology allied health professionals. J Adolesc Young Adult Oncol. 2022;2021:159. https://doi.org/10.1089/jayao.2021.0159.
Bradford J, Reisner SL, Honnold JA, Xavier J. Experiences of transgender-related discrimination and implications for health: results from the Virginia transgender health initiative study. Am J Public Health. 2013;103(10):1820–9. https://doi.org/10.2105/AJPH.2012.300796.
Burgwal A, Gvianishvili N, Hård V, Kata J, Nieto IG, Orre C, Smiley A, Vidić J, Motmans J. The impact of training in transgender care on healthcare providers competence and confidence: a cross-sectional survey. Healthcare. 2021;9(8):967. https://doi.org/10.3390/healthcare9080967.
Burton CW, Nolasco K, Holmes D. Queering nursing curricula: understanding and increasing attention to LGBTQIA+ health needs. J Prof Nurs. 2021;37(1):101–7. https://doi.org/10.1016/j.profnurs.2020.07.003.
Choi SK, Meyer I. LGBT aging: a review of research findings, needs, and policy implications. The Williams Institute. https://williamsinstitute.law.ucla.edu/wp-content/uploads/LGBT-Aging-Aug-2016.pdf.
Committee on Understanding the Well-Being of Sexual and Gender Diverse Populations, Committee on Population, Division of Behavioral and Social Sciences and Education, & National Academies of Sciences, Engineering, and Medicine. Understanding the Well-Being of LGBTQI+ Populations. In: Patterson CJ, Sepúlveda MJ, White J (eds). National Academies Press. 2020; p. 25877. https://doi.org/10.17226/25877.
Connors J, Casares MC, Honigberg MC, Davis JA. LGBTQ health disparities. In: The equal curriculum. Berlin: Springer; 2020. p. 13–31.
Crisp C. Beyond Tolerance: An Examination of LGBTQ+ Cultural Competence in Eating Disorder Treatment Centers [Psy.D., Pepperdine University]. In ProQuest Dissertations and Theses (2567945972). ProQuest Dissertations & Theses A&I; ProQuest Dissertations & Theses Global. 2021; https://www.proquest.com/dissertations-theses/beyond-tolerance-examination-lgbtq-cultural/docview/2567945972/se-2?accountid=14509.
Daniel H, Butkus R, The Health and Public Policy Committee of the American College of Physicians*. Lesbian, gay, bisexual, and transgender health disparities: executive summary of a policy position paper From the American College of Physicians. Annal Intern Med. 2015;163(2):135–7. https://doi.org/10.7326/M14-2482.
Davis G. Contesting intersex: the dubious diagnosis. New York University Press; 2015.
Dean MA, Victor E, Guidry-Grimes L. Inhospitable healthcare spaces: why diversity training on LGBTQIA issues is not enough. J Bioethical Inquiry. 2016;13(4):557–70. https://doi.org/10.1007/s11673-016-9738-9.
Durso LE, Meyer IH. Patterns and predictors of disclosure of sexual orientation to healthcare providers among lesbians, gay men, and bisexuals. Sexual Res Soc Policy. 2013;10(1):35–42. https://doi.org/10.1007/s13178-012-0105-2.
Eliason MJ, Schope R. Does “don’t ask don’t tell” apply to health care? Lesbian, gay, and bisexual people’s disclosure to health care providers. J Gay Lesbian Med Assoc. 2001;5(4):125–34. https://doi.org/10.1023/A:1014257910462.
Emory Nursing Professional Development Center. Caring for the LGBTQI+ Community. https://capacity.ce.emorynursingexperience.com/courses/caring-for-the-lgbtqi-community. 2022.
Featherston R, Downie LE, Vogel AP, Galvin KL. Decision making biases in the allied health professions: a systematic scoping review. PLoS ONE. 2020;15(10):e0240716. https://doi.org/10.1371/journal.pone.0240716.
Follmer KB, Sabat IE, Siuta RL. Disclosure of stigmatized identities at work: an interdisciplinary review and agenda for future research. J Organ Behav. 2020;41(2):169–84. https://doi.org/10.1002/job.2402.
Freedom for All Americans. Legislative Tracker: Anti-Transgender Legislation Filed for the 2022 Legislative Session. Freedom for All Americans. 2022. https://freedomforallamericans.org/legislative-tracker/anti-transgender-legislation/.
Gisondi MA, Bigham B. LGBTQ + health: a failure of medical education. Can J Emerg Med. 2021;23(5):577–8. https://doi.org/10.1007/s43678-021-00185-w.
Goodenow C, Szalacha L, Westheimer K. School support groups, other school factors, and the safety of sexual minority adolescents. Psychol Sch. 2006;43(5):573–89. https://doi.org/10.1002/pits.20173.
Hawala-Druy S, Hill MH. Interdisciplinary: cultural competency and culturally congruent education for millennials in health professions. Nurse Educ Today. 2012;32(7):772–8. https://doi.org/10.1016/j.nedt.2012.05.002.
Heck JE, Sell RL, Gorin SS. Health care access among individuals involved in same-sex relationships. Am J Public Health. 2006;96(6):1111–8.
Hill RL, Nguyen DJ, Kilgo CA, Lange AC, Shea HD, Renn KA, Woodford MR. How LGBTQ+ students thrive in college. J Student Affairs Res Pract. 2021;58(3):267–81. https://doi.org/10.1080/19496591.2020.1738241.
Hoffman ND, Freeman K, Swann S. Healthcare preferences of lesbian, gay, bisexual, transgender and questioning youth. J Adolesc Health. 2009;45(3):222–9. https://doi.org/10.1016/j.jadohealth.2009.01.009.
Hudson KD, Mehrotra GR. “That is when I changed and my whole life changed”: turning points in health perceptions among LGBTQ adults of color. J Ethn Cult Divers Soc Work. 2022;31(2):84–95. https://doi.org/10.1080/15313204.2020.1839616.
Kattari SK, Bakko M, Hecht HK, Kattari L. Correlations between healthcare provider interactions and mental health among transgender and nonbinary adults. SSM Popul Health. 2020;10:100525. https://doi.org/10.1016/j.ssmph.2019.100525.
Korpaisarn S, Safer JD. Gaps in transgender medical education among healthcare providers: a major barrier to care for transgender persons. Rev Endocr Metab Disord. 2018;19(3):271–5. https://doi.org/10.1007/s11154-018-9452-5.
Linley JL, Nguyen D, Brazelton GB, Becker B, Renn K, Woodford M. Faculty as sources of support for LGBTQ college students. Coll Teach. 2016;64(2):55–63. https://doi.org/10.1080/87567555.2015.1078275.
Llayton CK, Caldas LM. Strategies for inclusion of lesbian, gay, bisexual, transgender, queer, intersex, and asexual (LGBTQIA+) education throughout pharmacy school curricula. Pharm Pract. 2020;18(1):1862. https://doi.org/10.18549/PharmPract.2020.1.1862.
Mahendra N. Integrating lesbian, gay, bisexual, transgender, and queer issues into the multicultural curriculum in speech-language pathology: instructional strategies and learner perceptions. Perspect ASHA Spl Interest Groups. 2019;4(2):384–94. https://doi.org/10.1044/2019_PERS-SIG14-2018-0007.
Marcelin JR, Siraj DS, Victor R, Kotadia S, Maldonado YA. The impact of unconscious bias in healthcare: how to recognize and mitigate it. J Infect Dis. 2019;220(Supplement_2):S62–73. https://doi.org/10.1093/infdis/jiz214.
McCabe HA, Kinney MK. LGBTQ+ individuals, health inequities, and policy implications. Creighton L Rev. 2018;52:427.
MedEdPORTAL. (n.d.). MedEdPORTAL. Retrieved December 8, 2022, from https://www.mededportal.org/.
Nowaskie DZ, Patel AU, Fang RC. A multicenter, multidisciplinary evaluation of 1701 healthcare professional students’ LGBT cultural competency: Comparisons between dental, medical, occupational therapy, pharmacy, physical therapy, physician assistant, and social work students. PLoS ONE. 2020;15(8):e0237670. https://doi.org/10.1371/journal.pone.0237670.
Obedin-Maliver J, Goldsmith ES, Stewart L, White W, Tran E, Brenman S, Wells M, Fetterman DM, Garcia G, Lunn MR. Lesbian, gay, bisexual, and transgender–related content in undergraduate medical education. JAMA. 2011;306(9):971–7.
Paul S. Overcoming the challenges and mitigating the disparities in our LGBTQI+ patients. Am J Gastroenterol. 2021;116(9):1815–8. https://doi.org/10.14309/ajg.0000000000001359.
Peters MD, Ramsey I, Kennedy K, Sharplin G, Eckert M. Culturally safe, high-quality breast cancer screening for transgender people: a scoping review protocol. J Adv Nurs. 2022;78(1):276–81.
Pitcher EN, Camacho TP, Renn KA, Woodford MR. Affirming policies, programs, and supportive services: using an organizational perspective to understand LGBTQ+ college student success. J Divers Higher Educ. 2018;11(2):117–32. https://doi.org/10.1037/dhe0000048.
Rodger S, Webb G, Devitt L, Gilbert J, Wrightson P, McMeeken J. Clinical education and practice placements in the allied health professions: an international perspective. J Allied Health. 2008;37(1):53–62.
Röndahl G, Innala S, Carlsson M. Heterosexual assumptions in verbal and non-verbal communication in nursing. J Adv Nurs. 2006;56(4):373–81.
Rossman K, Salamanca P, Macapagal K. A qualitative study examining young adults’ experiences of disclosure and nondisclosure of LGBTQ identity to health care providers. J Homosex. 2017;64(10):1390–410. https://doi.org/10.1080/00918369.2017.1321379.
Rowe D, Ng YC, O’keefe LC. Addressing transgender patientsʼ barriers to access care. Nurse Pract. 2019;44(6):30–8. https://doi.org/10.1097/01.NPR.0000558155.38478.8f.
Spence D, Wicks T, Wojnakowski M, Plaus K. Benchmarking study on continuing certification in healthcare and allied health fields: program variables, commonalities, and trends. J Nurs Regul. 2021;12(2):34–40. https://doi.org/10.1016/S2155-8256(21)00054-5.
Stein GL, Bonuck KA. Physician–patient relationships among the lesbian and gay community. J Gay Lesbian Med Assoc. 2001;5(3):87–93. https://doi.org/10.1023/A:1011648707507.
Sue DW. Microaggressions, marginality, and oppression: an introduction. New York: Wiley; 2010.
Utamsingh PD, Richman LS, Martin JL, Lattanner MR, Chaikind JR. Heteronormativity and practitioner–patient interaction. Health Commun. 2016;31(5):566–74. https://doi.org/10.1080/10410236.2014.979975.
White Hughto JM, Reisner SL, Pachankis JE. Transgender stigma and health: a critical review of stigma determinants, mechanisms, and interventions. Soc Sci Med. 2015;147:222–31. https://doi.org/10.1016/j.socscimed.2015.11.010.
Wilson CK, West L, Stepleman L, Villarosa M, Ange B, Decker M, Waller JL. Attitudes toward LGBT patients among students in the health professions: influence of demographics and discipline. LGBT Health. 2014;1(3):204–11. https://doi.org/10.1089/lgbt.2013.0016.
Author information
Authors and Affiliations
Contributions
SAK conceived, recruited for, outlined, drafted, and reviewed the manuscript. DR and AX outlined, drafted, and reviewed portions of the manuscript. MM drafted and reviewed portions of the manuscript. All authours read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kirjava, S.A., Rawal, D., Xia, A. et al. Contemporary LGBTQ + content that should be included in allied health professions education. Discov Educ 2, 6 (2023). https://doi.org/10.1007/s44217-023-00029-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44217-023-00029-y