Abstract
Alport syndrome is a hereditary disorder characterized by renal impairment, hearing loss, and ocular symptoms and is caused by COL4A3, COL4A4, and COL4A5 mutations. Here, we report the case of 3-year-old boy with isolated hematuria detected in routine preventative urinary screening conducted in 3-year-old children. He carried a novel variant, NM_033380.3:c. 1032 + 1 G > A, which caused a splicing abnormality in COL4A5. He was diagnosed with X-linked Alport syndrome.
Similar content being viewed by others
Alport syndrome is a hereditary disorder characterized by renal impairment, hearing loss, and ocular symptoms1 and is caused by COL4A3, COL4A4, and COL4A5 mutations. Historically, Alport syndrome has been diagnosed on the basis of either a combination of histopathological examination and genetic analysis or histopathological examination followed by genetic analysis. In recent years, because of advances in genetic analysis technology, the diagnosis can be made either by histopathological examination preceding genetic analysis or by genetic analysis alone2.
In patients with Alport syndrome, renal impairment progresses, leading to end-stage renal failure. Previously, no treatment was administered to prevent renal impairment. However, in recent years, the protective effect of angiotensin-converting enzyme (ACE) inhibitors on renal function has been reported3,4, and new drugs such as bardoxolone and gene therapy are under development5,6. Early diagnosis and treatment are crucial to improve renal function prognosis.
In Japan, routine urinary screening in 3-year-old children is useful to detect congenital anomalies of the kidneys and urinary tract. Proteinuria is considered to be a significant indicator, whereas hematuria is considered a clinically less useful indicator because serious illness is not often found in children with isolated hematuria7.
We report here the case of a 3-year-old child who was diagnosed with X-linked Alport syndrome by genetic analysis after hematuria was detected in routine urinary screening. This case demonstrates the usefulness of genetic analysis and urinary screening in the early diagnosis and treatment of Alport syndrome.
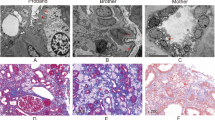
A 3-year-old boy was referred to Fujita Health University Hospital for further examination after isolated hematuria was identified in a routine urinary screening for 3-year-old children. His height was 93.8 cm, his weight was 12.7 kg, and his blood pressure was 70/54 mmHg. Physical examination revealed no abnormalities on chest auscultation or edema. Laboratory findings demonstrated normal renal function (estimated glomerular filtration rate, 108 ml/min/1.73 m2)8. Urinalysis showed occult blood (3+), 50–99 RBCs/high power field, and a protein/creatinine ratio of 0.16 g/gCr (Table 1). Various types of casts were observed. His mother had had hematuria with normal renal function since childhood, and his maternal grandmother had undergone hemodialysis for end-stage renal failure owing to diabetic nephropathy (Fig. 1).
After genetic counseling, we obtained consent for genetic analysis from the patient’s parents, and we performed genetic analysis of COL4A3, COL4A4, and COL4A5 using a next-generation sequencing. The results revealed a novel hemizygous variant NM_033380.3:c. 1032 + 1 G > A, in COL4A5. No variants were found in the COL4A3 or COL4A4 genes. The patient was genetically diagnosed with X-linked Alport syndrome. No renal biopsy was performed. Treatment with an ACE inhibitor was initiated.
The hemizygous variant revealed in this patient was novel because it was not present in the Human Genetic Variation Database, Genome Aggregation Database, or ClinVar. Based on the American College of Medical Genetics and Genomics standards and guidelines, the variant was classified as pathogenic since it is categorized as a PVS1 null variant (canonical + 1 splice site)9 and might cause a splicing abnormality. In the present case, Alport syndrome was suspected because the patient already had marked hematuria at the age of 3 years and his mother had hematuria10. Although renal biopsy is preferred for the diagnosis of Alport syndrome, it is not generally indicated for isolated hematuria or hematuria with a small amount of urinary protein10,11. Furthermore, in Japan, the genetic analysis of Alport syndrome has been covered by public medical insurance since 2020 and can be performed in general clinical practice. Therefore, we elected to perform a genetic analysis first. The recommended timing of treatment for Alport syndrome depends on the type of inheritance and patient sex2. In boys with X-linked Alport syndrome, treatment is recommended after the onset of proteinuria; however, in recent years, some authors have recommended treatment from the time of diagnosis even without the onset of proteinuria2. Therefore, the identification of the type of inheritance is clinically useful. The patient was diagnosed with X-linked Alport syndrome before the onset of proteinuria owing to the identification of a novel variant in COL4A5. Genetic analysis of Alport syndrome is useful for the early diagnosis, treatment, and prognosis of Alport syndrome.
In the present case, hematuria was identified in the patient during a routine urinary screening performed in 3-year-old children, leading to the diagnosis of Alport syndrome and thus allowing early treatment initiation. In Japan, routine urinary screening in 3-year-old children is useful to identify congenital anomalies of the kidneys and urinary tract7. In Alport syndrome, hematuria is present from infancy12, and at 3 years of age, affected patients often have marked hematuria, even in the absence of proteinuria13. Therefore, it is possible to screen for Alport syndrome by identifying hematuria during routine urinary screening in 3-year-old children. However, because Alport syndrome was found in only 0.0032% of all urine samples from 3-year-old children7 and there was previously no known effective treatment, screening for Alport syndrome during routine urinalysis in 3-year-old children has never been considered. In recent years, the protective effect of ACE inhibitors on renal function has been reported. In addition, other drugs, such as bardoxolone and gene therapy, are under development5,6. This development indicates the recognition of the relevance of the disease and the need for an early diagnosis to improve renal prognosis. In most patients with Alport syndrome, renal function is preserved at the age of 3 years14; therefore, an early diagnosis of Alport syndrome based on hematuria in routine urinary screening in 3-year-old children is useful to preserve renal function. Thus, the significance of hematuria in the routine urinary screening of 3-year-old children should be reconsidered.
In conclusion, we identified a novel COL4A5 splicing variant causing X-linked Alport syndrome in a 3-year-old child, and we demonstrated the usefulness of genetic analysis and urinary screening in a 3-year-olds for the early diagnosis and treatment of Alport syndrome.
HGV database
The relevant data from this Data Report are hosted at the Human Genome Variation Database at https://doi.org/10.6084/m9.figshare.hgv.3219.
References
Nozu, K., Nakanishi, K., Abe, Y., Udagawa, T., Okada, S. & Okamoto, T. et al. A review of clinical characteristics and genetic backgrounds in Alport syndrome. Clin. Exp. Nephrol. 23, 158–168 (2019).
Kashtan, C. E. & Gross, O. Clinical practice recommendations for the diagnosis and management of Alport syndrome in children, adolescents, and young adults-an update for 2020. Pediatr. Nephrol. 36, 711–719 (2021).
Gross, O., Licht, C., Anders, H. J., Hoppe, B., Beck, B. & Tönshoff, B. et al. Early angiotensin-converting enzyme inhibition in Alport syndrome delays renal failure and improves life expectancy. Kidney Int 81, 494–501 (2012).
Gross, O., Tönshoff, B., Weber, L. T., Pape, L., Latta, K. & Fehrenbach, H. et al. German Pediatric Nephrology (GPN) Study Group and EARLY PRO-TECT Alport Investigators. A multicenter, randomized, placebo-controlled, double-blind phase 3 trial with open-arm comparison indicates safety and efficacy of nephroprotective therapy with ramipril in children with Alport’s syndrome. Kidney Int 97, 1275–1286 (2020).
Chertow, G. M., Appel, G. B., Andreoli, S., Bangalore, S., Block, G. A. & Chapman, A. B. et al. Study Design and Baseline Characteristics of the CARDINAL Trial: A Phase 3 Study of Bardoxolone Methyl in Patients with Alport Syndrome. Am. J. Nephrol. 52, 180–189 (2021).
Yamamura, T., Horinouchi, T., Adachi, T., Terakawa, M., Takaoka, Y. & Omachi, K. et al. Development of an exon skipping therapy for X-linked Alport syndrome with truncating variants in COL4A5. Nat. Commun. 11, 2777 (2020).
Yanagihara, T., Hamada, R., Ishikura, K., Uemura, O., Matsuyama, T. & Takahashi, S. et al. Urinary screening and urinary abnormalities in 3-year-old children in Japan. Pediatr. Int 57, 354–358 (2015).
Uemura, O., Nagai, T., Ishikura, K., Ito, S., Hataya, H. & Gotoh, Y. et al. Creatinine-based equation to estimate the glomerular filtration rate in Japanese children and adolescents with chronic kidney disease. Clin. Exp. Nephrol. 18, 626–633 (2014).
Richards, S., Aziz, N., Bale, S., Bick, D., Das, S. & Gastier-Foster, J. et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 17, 405–424 (2015).
Vivante, A., Calderon-Margalit, R. & Skorecki, K. Hematuria and risk for end-stage kidney disease. Curr. Opin. Nephrol. Hypertens. 22, 325–330 (2013).
Suzuki, H., Kikuchi, M., Koike, K., Komatsu, H., Matsuzaki, K. & Takahashi, K. et al. Committee of Clinical Practical Guideline for IgA Nephropathy 2020. A digest from evidence-based clinical practice guideline for IgA nephropathy 2020. Clin. Exp. Nephrol. 25, 1269–1276 (2021).
Kashtan, C. E. Familial hematuria. Pediatr. Nephrol. 24, 1951–1958 (2009).
Kumagai, N., Nakayama, M., Uchida, N., Kudo, H., Kigosi, T. & Matsuki, T. et al. Diagnostic opportunities and effects of treating in Alport syndrome in the Department of Pediatrics, Tohoku University. Hospital. Jpn J. Nephrpol 60, 561–566 (2018).
Jais, J. P., Knebelmann, B., Giatras, I., Marchi, M., Rizzoni, G. & Renieri, A. et al. X-linked Alport syndrome: natural history in 195 families and genotype- phenotype correlations in males. J. Am. Soc. Nephrol. 11, 649–657 (2000).
Acknowledgements
We would like to thank AJE (www.aje.com/jp/) for English language editing. There was no relevant funding for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kumagai, N., Matsumoto, Y., Kondoh, T. et al. A novel COL4A5 splicing variant causing X-linked Alport syndrome: A case report. Hum Genome Var 9, 30 (2022). https://doi.org/10.1038/s41439-022-00209-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41439-022-00209-6
- Springer Nature Limited