Abstract
Immunological memory is critical for immune protection, particularly at epithelial sites, which are under constant risk of pathogen invasions. To counter invading pathogens, CD8+ memory T cells develop at the location of infection: tissue-resident memory T cells (TRM). CD8+ T-cell responses are associated with type-1 infections and type-1 regulatory T cells (TREG) are important for CD8+ T-cell development, however, if CD8+ TRM cells develop under other infection types and require immune type-specific TREG cells is unknown. We used three distinct lung infection models, to show that type-2 helminth infection does not establish CD8+ TRM cells. Intracellular (type-1) and extracellular (type-3) infections do and rely on the recruitment of response type-matching TREG population contributing transforming growth factor-β. Nevertheless, type-1 TREG cells remain the most important population for TRM cell development. Once established, TRM cells maintain their immune type profile. These results may have implications in the development of vaccines inducing CD8+ TRM cells.
Similar content being viewed by others
Introduction
Epithelial barriers are prime portals for microbial invasion. Organ structure, such as a multilayer of epithelial cells in the skin, provides additional protection against invasion. Other organs, such as the intestine and lung require optimal exchange of nutrients, liquids, and gasses that necessitate a single epithelial cell layer. It is highly beneficial to the host to contain invading pathogens at the site of entry and swiftly clear any pathogens and their products to avoid tissue damage and systemic dissemination of infectious or toxic material. For this reason, the immune response is tailored to the identity of the invading microbe, towards intracellular (type-1), helminths (type-2), or extracellular (type-3) pathogens. Understanding how tissue immunity is established following distinct responses has conceivable therapeutic potential with the ability to modulate tissue-specific immunity, from vaccination strategies to tumour treatment.
The development of immunological memory is a pillar of adaptive immunity and an efficacious way to prevent the development of disease caused by pathogen entry. Memory T lymphocytes are functionally and phenotypically classified in at least three subsets. Central memory (TCM) and effector memory (TEM) T cells recirculate throughout lymphoid and non-lymphoid organs respectively1. TEM cells actively scout for pathogens, entering and exiting organs via the circulation and lymph, while TCM cells are more quiescent and are reactivated in secondary lymphoid organs, faster than, but not dissimilarly from, naïve T cells2,3. Although these cells provide significant protection from recurrent infections due to increased antigen-specific numbers and speed of activation, they require a systemic immune reaction for triggering and may not be sufficiently efficacious against pathogen entry. Tissue-resident memory (TRM) T cells reside in tissues, especially those at the host/environment interface. TRM cells actively survey the tissues for signs of infection, able to react rapidly and thereby swiftly eliminate infected cells without the need for a systemic immune reaction1.
CD8+ TRM cells are characterised by the expression of different markers and transcription factors, which depend on their activation status and on the tissue type they home to4. Most TRM cells constitutively express CD69, which antagonises the egress receptor S1P receptor 1, thus maintaining tissue residency5,6,7, with organ specificity8. The integrins CD103 and CD49a are additional markers of tissue residency, although TRM cells negative for CD103 have been reported and CD49a may reflect activation status9,10,11,12. CD103, integrin αE pairing with β7, is mostly present on epithelial residing TRM cells, providing support for tissue homing and maintenance via epithelial cell E-cadherin binding, while potentiating cytolytic activity. Of additional importance is the absence of Killer Cell Lectin Like Receptor G1 (KLRG1), typically described as a terminal differentiation marker on effector T cells13,14. KLRG1 may compete with CD103 for the binding to E-cadherin, with its downregulation contributing to TRM cell residency15.
A transcriptional programme, distinct from other CD8+ T-cell subsets, drives surface markers and function of TRM cells. TRM cells express low levels of Tbox protein expressed in T cells (Tbet) and Krüppel-like Factor 2 (KLF2), while Eomesodermin (Eomes) is absent6,14,16. Instead, TRM cells express high levels of arylhydrocarbon receptor (AhR) in gut and skin, Hobit and Blimp-117,18. In addition, TRM cells are maintained in a semi-activation state and distinct metabolic wiring takes place, ensuring rapid full activation when required19,20.Thus, TRM cells patrol non-lymphoid organs and perform immunosurveillance by killing infected cells and producing cytokines to recruit other immune cells to quickly eliminate the pathogen21,22.
Exacerbated T-cell responses can result in tissue damage, and a balance between pathogen elimination and immunopathology needs to be maintained. Regulatory T cells (TREG), characterised by the expression of Forkhead box protein 3 (Foxp3) transcription factor, play an important role in reducing excessive immune responses. TREG can influence the transition of effector CD8+ T cells to memory cells by limiting interleukin (Il)−2 availability, producing Il-10 and cytotoxic T-lymphocyte associate protein-4 (CTLA-4)23,24,25. Of importance, TREG cells can adopt a transcriptional programme in line with the type of inflammation and the CD4+ T helper (TH) subset involved. Besides Foxp3, TREG cells can co-express the TH1 cell (type-1) factor Tbet, the TH2 cell (type-2) factor Gata-3, and the TH17 cell (type-3) factor Rorγt, to take on characteristics of one of these TH cell ineages22,26,27,28.
We previously showed that type-1 TREG cells, recruited via their Tbet-dependent expression of the chemokine receptor CXCR3, supply and activate transforming growth factor (TGF)β locally, thereby efficiently facilitating the generation of TRM cells14. However, although TRM cells were found reduced in several organs, the link between their generation and type-1 TREG cells was established in the intestine and during a type-1 immune response. This raises the question of whether the establishment of TRM cells in another organ is also dependent on type-1 TREG cells, and more importantly, whether TRM cell development during other types of infection is dependent on the corresponding type of TREG cell or remains dependent on type-1 TREG cells. Here, we show that, in the lung, type-1 TREG cells are required to establish TRM cells upon type-1 infection, while a type-2 infection does not establish a robust TRM cell population. Furthermore, type-3 infection in the same organ requires type-3 TREG cells and their provision of TGFβ for efficient TRM cell establishment.
Results
Type-1 immunity induces TRM cells in lungs
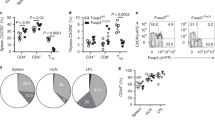
In the absence of type-1 TREG, there is a reduction in CD8+ TRM cells in the intestine, lungs, and liver, due to inhibition of their generation14. To establish a robust infection model in the lungs, we infected Foxp3WT mice with influenza H3N2 (X-31). A week after influenza infection, a robust influx of CD4+ and CD8+ T cells is observed (Supplementary Fig. 1a–d). Influenza challenge results in a strongly polarised type-1 response with production of interferon (IFN)-γ and dominance of CXCR3-expressing CD4+ and CD8+ T cells, with no other polarised T-cell response observed (Fig. 1a–d; Supplementary Fig. 1e–h). In addition to the type-1 response of CD4+ and CD8+ T cells, predominantly type-1 TREG cells expressing CXCR3 (Fig. 1e–f) are recruited to the site of inflammation.
Mice were infected or not intranasally with 1000 plaque-forming units (PFU) of Influenza A X-31 strain (H3N2). 10 days post-infection lungs were collected, and cells were isolated and analysed via flow cytometry for cytokine production. a Numbers of activated (CD44+) CD4+ T cells producing indicated cytokines (p(Non-infected vs. Influenza H3N2) < 0.000001) and (b) representative flow cytometry plots (n = 6, non-infected, n = 7 infected, N = 3). c Numbers of activated CD8+ T cells producing indicated cytokines (p(Non-infected vs. Influenza H3N2) = 0.000013) and d representative flow cytometry plots (n = 6, non-infected, n = 7 infected, N = 3). e, f Foxp3WT mice (n = 6, non-infected, n = 7 infected, N = 3) were assessed for e percentage (p(Non-infected vs. Influenza H3N2) <0.000001), and f numbers of chemokine receptors CXCR3, ST2 (IL-33R) and CCR6 expression (p(Non-infected vs Influenza H3N2): CXCR3, p = 001415; ST2, p = 0.000502; CCR6, p = 0.001132), on TREG cells (n = 6, non-infected, n = 8 infected, N = 3). g, h Mice analysed via flow cytometry for g percentages of total CD8+ T cells and h numbers of TRM cells, defined as CD69+KLRG1− CD8+ T cells, p(Non-infected vs Influenza H3N2) < 0.0001 (n = 6, N = 3). i Foxp3WT and Foxp3ΔTbx21 mice received CD8CD45.1 T cells intravenously, one day prior to infection. 14 days post infection, lung cells were assessed by flow cytometry for the percentage of TRM cells (CD69+KLRG1-CD103+) in the transferred population (Foxp3WT n = 17, Foxp3ΔTbx21 n = 10, N = 4), p(Foxp3WT vs Foxp3ΔTbx21) <0.0001. Two-sided Mann–Whitney analysis was applied to compare groups. Data are presented as bars of mean ± SEM with single data points.
Influenza infection results in the establishment of a substantial CD8+ TRM cell population (Fig. 1g–h). To understand if their establishment in the lungs upon influenza infection is dependent on type-1 TREG cells we make use of our previously setup transfer model whereby CD45.1 expressing CD8+ T cells (CD8CD45.1) are transferred into control Foxp3Wt mice or Foxp3ΔTbx21 mice that miss type-1 TREG14. Cells are readily recovered in the spleens, and the characteristic weight loss is observed (Supplementary Fig. 1i–k). As previously shown in the small intestine, the absence of type-1 TREG cells reduces the establishment of CD8+ TRM cells, after CD8CD45.1 transfer. We now extend this observation to the lungs upon influenza infection where compared to controls (Foxp3WT), the absence of type-1 TREG cells leads to reduced efficiency of CD8+ TRM cell development (Fig. 1i).
Type-2 immunity does not induce de novo CD8+ TRM cells in lungs
Establishment of CD8+ TRM cells in the lung with similar requirements to the small intestine may still rely on the type-1 inflammation induced by an intracellular pathogen as influenza virus. We subsequently used the helminth Nippostrongylus brasiliensis, widely used as a model to elicit strong type-2 immunity in the lungs29. A week after infection we observe a strong activation of CD4+ T cells, CD44hi, and a response characterised by TH2 cells in the lungs expressing IL-4 and IL-13 (Fig. 2a, b; Supplementary Fig. 2a, b)30. However, the CD8+ T-cell compartment shows a very limited effector CD44hi CD8+ T-cell response, without type-2 polarisation, with primarily IFN-γ produced (Fig. 2c, d). There is an influx of TREG cells, but without a polarisation towards any specific TREG subset (Fig. 2e, f). Although some endogenous CD8+ TRM cell accumulation is observed, the CD8 T-cell activation in the lungs is modest (Fig. 2g, h, Supplementary Fig. 2c, d).
Mice were subcutaneously infected or not with 300 stage L3 larvae of Nippostrongylus brasiliensis. 7 days post-infection lungs were collected, and cells were isolated and analysed via flow cytometry for cytokine production, and TRM cells. a Numbers of activated (CD44+) CD4+ T cells producing indicated cytokines, p(Non-infected vs Nippostrongylus brasiliensis): IFN-γ, p = 0.001749; IL-17, p = 0.002537; IL-4, p = 0.000048; IL-13, p = 0.000729, and b representative flow cytometry plots (non-infected n = 6, infected n = 9, N = 3). c Numbers of activated CD8+ T cells producing indicated cytokines and d Representative flow cytometry plots of cytokine production in CD8+ T cells (non-infected n = 6, infected n = 9, N = 3). e, f Foxp3WT mice were assessed for e percentage and f numbers of chemokine receptors CXCR3, ST2 (IL-33R) and CCR6 expression on TREG cells, p(Non-infected vs Nippostrongylus brasiliensis): CXCR3, p = 0.014118; ST2, p = 0.023778; CCR6, p = 0.028885, (non-infected n = 6, infected n = 9, N = 3). g, h CD69+KLRG1− CD8+ TRM cell g percentage of total CD8+ T cells, p(Non-infected vs Nippostrongylus brasiliensis) = 0.0004, and h number, p(Non-infected vs Nippostrongylus brasiliensis)= = 0.0016, in non-infected (control) and infected mice (non-infected n = 6, infected n = 9, N = 3). i–l Foxp3WT mice received CD8CD45.1 T cells intravenously, one day prior to infection. 14 days post-infection, lung cells were analysed via flow cytometry for i total number of CD8CD45.1 T cells, CD69+KLRG1− CD8+ TRM cell j percentage and k numbers, and l representative flow plot, within the CD8CD45.1 T-cell population (n = 7, N = 3). m, n Comparison of transferred CD8CD45.1 T-cell number in the (m) spleen, p(Influenza vs Nippostrongylus brasiliensis) = 0.0012, or (n) lungs, p(Influenza vs Nippostrongylus brasiliensis) = 0.0002, of mice infected with Influenza and N. brasiliensis (Influenza n = 9, N. brasiliensis n = 7, N = 3). 2-sided Mann–Whitney analysis was applied to compare the differences between groups. Data is presented as bars of mean ± SEM with single data points.
CD8CD45.1 and CD4CD45.1 T cells transferred into Foxp3Wt mice are recovered from the spleen, with robust numbers but without signs of activation with the majority of cells showing a naïve or TCM cell phenotype (Supplementary Fig. 2e–g). CD8CD45.1 T cells are few in the lungs upon infection, with CD8+ TRM cells rare and often below the detection threshold (Fig. 2i–l). CD4CD45.1 T cells are more numerous in the lungs upon infection, at cost of cell numbers in the spleen, with CD4+ TRM cell proportions much higher than CD8+ TRM cells (Supplementary Fig. 2g–h). This indicated robust CD4+ T-cell recruitment to the site of N. brasiliensis infection as opposed to CD8+ T cells. Comparing influenza and N. brasiliensis, CD8CD45.1 T cells remain abundant upon type-2 infection in the spleen, while transferred CD8+ T cells are recruited to the site of infection only after challenge with influenza (Fig. 2m, n). Although CD8+ TRM cell generation is efficient in lung tissue, with CD8+ T cells recruited and relying on type-1 TREG cell help during a type-1 immune response, a type-2 infection, despite a robust CD4+ T-cell response (Fig. 2a, b), does not result in de novo CD8+ T-cell recruitment, activation or polarisation, the recruitment of type-2 TREG cells, or the establishment of CD8+ TRM cells.
Type-3 immunity does induce CD8+ TRM cells in lungs
Besides intracellular pathogens resulting in robust CD8+ TRM cell development, we asked if extracellular pathogens, not helminths, would result in the generation of CD8+ TRM cells. Aspergillus fumigatus infection results in a robust response dominated by TH17 cells (Fig. 3a, b; Supplementary Fig. 3a, b)31. In contrast to a type-2 infection, a type-3 challenge shows a type-1 response with increased numbers of TH1 accompanied by a robust CD44hi effector CD8+ T-cell response, but with few expressing IFN-γ, yet IL-17 production is observed (Fig. 3c, d; Supplementary Fig. 3c, d).
Mice were intranasally challenged four times every 3 days with 106 spores of Aspergillus fumigatus. 10 days post-infection lungs were collected, and cells were isolated and analysed via flow cytometry for cytokine production, and TRM cells. a Numbers of activated (CD44+) CD4+ T cells producing indicated cytokines, p(Non-infected vs Aspergillus): IFN-γ, p = 0.005452; IL-17, p = 0.000733; IL-4, p = 0.007702; IL-13, p = 0.000005, and b representative flow cytometry plots of cytokine production in CD4+ T cells (non-infected n = 10, infected n = 12, N = 4). c Numbers of activated CD8+ T cells producing indicated cytokines, p(Non-infected vs Aspergillus): IFN-γ, p = 0.000951, and d representative flow cytometry plots of cytokine production in CD8+ T cells (non-infected n = 10, infected n = 14, N = 4). e, f TREG cells from Foxp3WT mice were assessed for expression in e percentage, p(Non-infected vs Aspergillus): Tbet, p = 0.018008; RORγt, p = 0.001023, and f numbers, p(Non-infected vs Aspergillus): Tbet, p = 0.022810; RORγt, p = 0.000093, of the transcription factors Tbet, GATA-3 and RORγt in (non-infected n = 6, infected n = 7, N = 3). g, h Analysis of CD69+KLRG1- CD8+ TRM cell (g) percentage, p(Non-infected vs Aspergillus) = 0.000017, within the total CD8+ T-cell population, and h number, p(Non-infected vs Aspergillus) = 0.002175 in the lungs of non-infected (control) and infected mice (n = 10, non-infected, n = 14 infected, N = 3). i Comparison of transferred CD8CD45.1 CD69+KLRG1− CD8+ TRM cell numbers in the lungs upon Nippostrongylus brasiliensis (N.b.) or Aspergillus fumigatus (A.f.) infection, p(Aspergillus vs Nippostrongylus brasiliensis)=0.0012, (n = 7, N = 3 for N.b.; n = 6 and N = 3 for A.f). Two-sided Mann-Whitney analysis was applied to compare the differences between groups. Data is presented as bars of mean ± SEM with single data points.
The influx of TREG cells shows skewing towards type-3 TREG at cost of type-1 TREG cells, with total TREG cell numbers increasing for all subsets (Fig. 3e, f). The TREG cell response reflects the CD4+ T-cell response, which shows strong skewing towards Rorγt+CCR6+ TH17 cells, but with increased numbers in all subsets (Supplementary Fig. 3e–g). The proportional distribution of CD8+ T cells remains similar to uninfected, but with total numbers of type-3 CD8+ T cells increasing (Supplementary Fig. 3h–j). Aspergillus infection increases endogenous host CD8+ TRM cell numbers in the lungs (Fig. 3g, h). Upon adoptive transfer of CD8CD45.1 T cells, in contrast to the type-2 infection used, newly established CD8+ TRM cells were more robustly detected upon Aspergillus challenge compared to N. brasiliensis infection (Fig. 3i). In summary, type-1 and 3 infections result in CD8+ TRM cell formation, which is not observed for a type-2 immune response.
Deletion of Rorγt in FoxP3+ cells ablates type-3 TREG cells
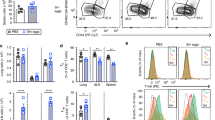
Our results using the type-3 immunity-inducing fungi Aspergillus indicate that CD8+ TRM cells are induced during type-3 infections. This raises the question if TREG cells are required and if the type of TREG cell needs to match the infection type to efficiently establish CD8+ TRM cells after type-3 infections. In order to address this, we generated Foxp3-yfp-Cre Rorγtf/f mice (Foxp3ΔRorγt), in which type-3 TREG cells are efficiently removed similarly as to type-1 TREG cells in Foxp3ΔTbx21 mice, in all tissues assayed (Fig. 4a, b)14. CD4+ or CD8+ T-cell proportions or numbers, including Rorγt-expressing subsets such as TH17 cells, or TREG subset proportions and numbers are not altered in Foxp3ΔRorγt mice compared to controls (Fig. 4b–d; Supplementary Fig. 4a–d). Since type-1 TREG cells are important in CD8+ TRM cell formation14, we also determined proportion and numbers of type-1 TREG cells and CXCR3 expression. These are similar between Foxp3Wt and Foxp3ΔRorγt mice (Fig. 4b, e, f; Supplementary Fig. 4c, e). In agreement with the presence of similar numbers of type-1 TREG cells, the number of intraepithelial lymphocytes (IELs) and CD8+ TRM cells in the lamina propria lymphocytes (LPL), lung, and liver, which differ in Foxp3ΔTbx21 mice14, were comparable between Foxp3Wt and Foxp3ΔRorγt mice (Fig. 4g; Supplementary Fig. 4f–h). Collectively, the data shows that efficient deletion of type-3 TREG cells is established without effects on other T-cell populations, as well as a noticeable effect on CD8+ TRM cells present at steady state.
Foxp3WT and Foxp3ΔRORγt mice were analysed at steady-state for TREG, CD4+, and CD8+ T cells in lung, spleen, small intestine lamina propria lymphocytes (LPL), and small intestine intraepithelial lymphocytes (IEL). a Representative flow plot of RORγt expression in LPL TREG cells in both mouse lines. b Percentage of LPL TREG cells expressing Tbet, GATA-3 or RORγt, p(Foxp3WT vs Foxp3ΔRORγt) < 0.000001, (Foxp3WT n = 8, Foxp3ΔRORγt n = 9, N = 3). c Percentage of RORγt expression in CD4+ and CD8+ LPL (Foxp3WT n = 8, Foxp3ΔRORγt n = 9, N = 3). d–f CD8+ T-cell proportions in the spleen were assessed for d naive (TN CD44−CD62L+), central memory (TCM, CD44+CD62L+) and effector memory/effector (TEM/TEFF, CD44+CD62L−) and e for CXCR3 expression on CD4+, CD8 and TREG cells, with f representative flow plot (n = 8, N = 3). g Percentage of CD69+KLRG1-CD103+ CD8+ TRM cell in small intestine LPL and IEL in both mouse lines (LPL Foxp3WT n = 7, Foxp3ΔRORγt n = 8, N = 3; IELs n = 6, N = 2). Two-sided Mann–Whitney analysis was applied to compare the differences between groups. Data is presented as bars of mean ± SEM with single data points.
Deletion of type-3 TREG cells impacts CD8+ TRM cell formation
Segmented filamentous bacteria (SFB) are known inducers of TH17 cells32. However, in our hands, there was a modest induction of TH17 cells, accompanied by TH1 cells as well, resulting in a mixed type-1/type-3 response (Supplementary Fig. 5a, b). In accordance, TREG cell recruitment was similar among the major three subsets (Supplementary Fig. 5c, d). Foxp3ΔRorγt mice mount a similar TH1 and TH17 cell response compared to Foxp3Wt controls (Supplementary Fig. 5e, f). SFB infection results in substantial CD8+ TRM cell establishment, but with reduced development in the absence of type-3 TREG cells (Fig. 5a, b). However, the chronicity of SFB in the intestinal tract prohibits the further assessment of memory T-cell responses32.
a, b In Foxp3WT and Foxp3ΔRORγt mice, CD45.1+ CD8+ T cells were transferred one day prior to infection with 100 mg of segmented filamentous bacteria (SFB)-containing feces, organs were assessed for their TRM cell phenotype (CD69+Eomes-CD103+) 14 days later. Small intestine LPL were collected and assessed for the T-cell phenotype of CD45.1+ CD8+ TRM cells. a Representative flow cytometry plots and b percentages of TRM cells, p(Foxp3WT vs Foxp3ΔRORγt) = 0.0357, (Foxp3WT n = 3, Foxp3ΔRORγt n = 5, N = 3). c, d Intranasal challenge with 1000 PFU of Influenza X-31 strain (H3N2). Lungs were collected and transferred T cells were analysed. c Representative flow cytometry plots of TRM cells within transferred T cells and d percentages of TRM cells in indicated mouse lines (Foxp3WT n = 17, Foxp3ΔRORγt n = 6, N = 4). e–g Mice were infected by four intranasal challenges with 106 spores of Aspergillus fumigatus. Lungs were collected and e total CD4+ T cells (Foxp3WT n = 7, Foxp3ΔRORγt n = 6, N = 3), f total TREG cells, p(Foxp3WT vs Foxp3ΔRORγt)=0.0043, and g subsets of TREG cells based on their transcription factor expression, p(Foxp3WT vs Foxp3ΔRORγt) = 0.000001, were analysed (Foxp3WT n = 6 Foxp3ΔRORγt n = 5, N = 3). h, i Mice were transferred with indicated condition receiving control or TGFβ1–deficient TREG cells prior to the first of four intranasal challenges with 106 spores of Aspergillus fumigatus. Lungs were collected and transferred CD45.1 CD8 T cells were analysed. h Representative flow cytometry plots of TRM cells within transferred CD45.1 CD8 T cells and i percentages of TRM cells in all conditions, p(Foxp3WT vs Foxp3ΔRORγt) = 0.0087, p(Foxp3ΔRORγt vs Foxp3ΔRORγt+WT Tregs) = 0.0173, p(Foxp3ΔRORγt vs Foxp3ΔRORγt+TregΔTGFβ1) = 0.0043 (Foxp3WT; Foxp3ΔRORγt n = 6, N = 4; Foxp3ΔRORγt + TREGWT n = 5, N = 2; Foxp3ΔRORγt + TREGΔTGFβ1 n = 5, N = 2). Multiple unpaired t test was used for g, other panels two-sided Mann-Whitney analysis was applied to compare groups. Data is presented as bars of mean ± SEM with single data points.
Influenza virus causes a strong type-1 response and establishment of CD8+ TRM cells in the lung, dependent on type-1 TREG cells (Fig. 1). Upon infection, Foxp3ΔRorγt and Foxp3Wt animals showed a similarly robust development of CD8+ TRM cells (Fig. 5c, d), in stark contrast to Foxp3ΔTbx21 mice (Fig. 1i), indicating primarily a dependency on type-1 TREG cells for CD8+ TRM cell development. This raised the question if Aspergillus infection, resulting in a strong type-3 response (Fig. 3), requires type-3 TREG cells for optimal CD8+ TRM cell development. Upon Aspergillus infection the influx of CD4+ T cells is similar between Foxp3Wt and Foxp3ΔRorγt animals (Fig. 5e). However, the recruitment of TREG cells is significantly lower (Fig. 5f), explained by the absence of type-3 TREG cells (Fig. 5g). This is similar to our previous observations in type-1 infections in Foxp3ΔTbx21 animals14. Genetic ablation of type-3 TREG cells in Foxp3ΔRorγt animals resulted in a marked reduction of CD8+ TRM development compared with Foxp3Wt animals (Fig. 5g, h). Importantly, and in line with previous results obtained with type-1 pathogens (Fig. 1)14, co-transfer of control TREG cells into type-3 TREG–deficient hosts prior to a type-3 infection is able to restore CD8+ TRM cell development and numbers to the level seen in control mice, which also for type-3 responses relies on TREG cell provision of TGFβ (Fig. 5i, Supplementary Fig. 5i).
Collectively, our data suggest that there appears to exist a matching of pathogen type and TREG subset during type-1 and type-3 infections. Influenza, SFB and Aspergillus, show a dominant dependency of the equivalent TREG subset for efficient CD8+ TRM cell development.
CD8+ TRM cell identity is maintained after infection
Eimeria vermiformis (Ev) is a small intestinal single-cell intracellular parasite that invades small intestine epithelial cells, it is mouse-specific and self-limiting, making it an ideal tool to study TRM cell development14. It undergoes at least three rounds of asexual replication, each time bursting out of an infected epithelial cell to reach distal uninfected epithelial cells33. Its clearance depends on a type-1 inflammatory response, as we showed previously, and establishes type-1 TREG-dependent CD8+ TRM cells14. We tested if the establishment of CD8+ TRM cells is inhibited by the absence of type-3 TREG cells in Foxp3ΔRorγt mice. Foxp3ΔRorγt mice do show reduced CD8+ TRM cell development compared to Foxp3Wt controls, although the decrease is not as marked as in the absence of type-1 TREG. (Fig. 6a, b)14.
Mice were transferred with CD45.1+ CD8+ T cells one day prior to oral gavage infection. 14 days after transplant, tissues were collected and assessed for their TRM phenotype. a, b Infection with 5000 oocysts of Eimeria vermiformis, a representative flow cytometry plots TRM cells (CD69+Eomes-CD103+) and b percentages of TRM cells in both mouse lines, p(Foxp3WT vs Foxp3ΔRORγt) = 0.0020, (Foxp3WT n = 4, Foxp3ΔRORγt n = 10, N = 3). c, d Mice were challenged four times intranasally with 106 spores of Aspergillus fumigatus. Lungs were collected and transferred T cells were analysed, c representative flow cytometry plots of TRM cells and d percentages of TRM cells in both mouse lines, p(Foxp3WT vs Foxp3ΔTbet) = 0.0238 (Foxp3WT n = 6, N = 4, Foxp3ΔTbx21 n = 3, N = 3). e, f Mice were transferred with CD45.1 CD8 T cells prior to the first of four intranasal challenges with 106 spores of Aspergillus fumigatus. Lungs were collected and transferred CD45.1 CD8+ TRM cells were analysed for e IFNγ or f IL-17 production (Foxp3WT n = 4, Foxp3ΔRORγt n = 7, Foxp3ΔTbx21 n = 4, N = 3). Two-sided Mann–Whitney analysis was applied to compare groups. Data is presented as bars of mean ± SEM with single data points.
CD8+ T cells are strongly associated with type-1 responses. We observed IFNγ-producing CD8+ T cells also in type-2 and type-3 infections (Figs. 2c, d, 3c, d). Hence, we next questioned if, in a strong type-3 infection model such as Aspergillus, the subsequent CD8+ TRM cell establishment that is dependent on type-3 TREG cells (Fig. 5e, f), shows any dependency on type-1 TREG cells as is the case with Ev infection (Fig. 6a, b). In the case of Aspergillus, the absence of either type-3 or type-1 has marked effects on the generation of CD8+ TRM cells (Figs. 5e, f, 6c, d).
Since memory T cells are maintained to offer protection against future challenges, we wished to know if CD8+ TRM cells developed under polarising conditions of type-1 or type-3 infections reflected the original skewing. We assessed the endogenous CD8+ TRM cell population after the clearance of infection. Upon influenza infection, the established CD8+ TRM cells show a predominant skewing towards the original type-1 response, with the cells mainly able to produce IFNγ (Supplementary Fig. 6a–c). Upon an Aspergillus infection, the remaining CD8+ TRM cells are fewer and the skewing is less apparent. The recall response shows IL-17 production, in line with the initial type-3 immune response, but there is the presence of IFNγ-producing CD8+ TRM cells as well (Supplementary Fig. 6d–f). To analyse the polarisation of newly recruited CD8+ T cells upon an Aspergillus challenge at the site of infection, we made use of our CD45.1 T-cell adoptive transfer model. The Aspergillus challenge shows a mixed type-1 and type-3 polarisation of established CD8+ TRM cells, indicating their polarisation is maintained after TRM cell development (Fig. 6e–f). Furthermore, this model allows the assessment of the role of TREG cell types on TRM cell polarisation. Although type-1 and type-3 TREG cells enhance the establishment of TRM cells upon Aspergillus infection (Fig. 5), the absence of either type-1 or type-3 TREG cells does not alter the polarisation toward the production of IFNγ or IL-17 (Fig. 6e, f).
Our data suggest that CD8+ TRM cell formation occurs predominantly during type-1 immune responses, largely depending on type-1 TREG cell recruitment and action. Type-3 infections do give rise to CD8+ TRM cells as well, but these are more modest in numbers. Although there is preferential recruitment of infection-type-matching TREG cells, there is redundancy between TREG populations, especially when polarisation is less dominant. After establishment, CD8+ TRM cells maintain their original profile, determined by the infection type, after pathogen clearance.
Discussion
Non-lymphoid tissue immunity is important to guard against reinfection, local containment of invaders and to reduce the chance of systemic dissemination34. This is established after primary infection and is of great interest for vaccine strategies. TREG cells are a critical component in the management of immune responses, maintaining self-tolerance and homoeostasis. Different populations of TREG cells exist and co-localise with the corresponding CD4+ Th cell subsets, with similar transcriptional programmes and associated expression of chemokine receptors27,35,36. Our previous data showed the requirement of type-1 TREG cell recruitment to the site of inflammation to release and make available TGFβ, thereby facilitating CD8+ TRM cell development. The work focussed on an intestinal intracellular parasite infection, Eimeria vermiformis, invoking a type-1 dominated response with CD8+ TRM cell development dependent on type-1, Tbet- and CXCR3-expressing, TREG cells14. Mirroring of transcription programmes and chemokine receptor expression raised the question that particular TREG subsets may control immune responses within the context of the pathogen encountered. This suggests that the development of CD8+ TRM cells may require a match between type of infection and TREG subset to be recruited22.
Localised infections result in strong CD8+ TRM cell development, require inflammation-mediated lymphocyte trafficking and the cognate antigen to be present in the local microenvironment14,34,37,38. Our results are obtained using three distinct infection models in the lungs. In each of the models, CD4+ T cells are recruited to the site of inflammation, and each type of infection is dominated by the corresponding TH cell subset, in numbers and proportions; Influenza by TH1 cells (IFNγ), N. brasiliensis by TH2 cells (IL-4, IL-13), and A. fumigatus by TH17 cells (IL-17). A potential limitation of our analysis is that we did not in vivo label the studied cells, a method used to identify circulating cells. However, this method has some disadvantages as it does not address migration properties and, in a highly vascular organ such as the lungs, the inflammatory context might result in tissue permeability and affect the results39.
We tested the role of type-3 TREG cells in the establishment of CD8+ TRM cells after a type-3 infection by genetically removing them using Foxp3ΔRorγt animals. We successfully used this approach with Foxp3ΔTbx21 animals14. In Foxp3ΔRorγt animals, the total number of TREG cells, including type-1 TREG cells that contribute to CD8+ TRM cell development, TH17 cells, and CD8+ T cells expressing Rorγt were not altered. This confirms that the Foxp3-Cre-driven deletion is TREG-specific and attests to the careful genotyping of mice used. Conform our previous results in the small intestine14, predominantly type-1 TREG cells are recruited upon a viral infection in the lung, which are required to enhance the establishment of CD8+ TRM cells. CD8 T cells are also recruited to the site of the influenza infection and are nearly exclusively IFNγ-producers. Although we observe a robust TH2 cell response upon N. brasiliensis infection, and although more TREG cells are recruited, we did not see a predominance of type-2 TREG cells at the site of infection. In addition, CD8+ T cells are marginally recruited to, and activated at, the site of infection, although the presence of more endogenous CD8+ TRM cells was observed. It is not clear if these cells are an expansion of the local CD8+ TRM cell population responding to a local inflammation or if these are pathogen-specific. However, using CD45.1 adoptive transfers, it is clear that few naïve CD8+ T cells are recruited to the site of infection, while CD4+ T cells are. The cytokine expression profile of CD8+ T cells did not differ from non-infected controls, and the characteristic type-2 cytokines IL-4 and IL-13 were not detected. CD8+ T cells are not associated with type-2 or anti-helminth responses40. There are suggestions that helminths may themselves reduce the CD8+ T-cell response41. Therefore, our results may be applicable to helminth-induced type-2 responses but not represent allergic responses.
Type-3-dominated infections, represented by A. fumigatus and SFB, do result in preferential recruitment of type-3 TREG cells as well as the recruitment of CD8+ T cells. However, and in contrast to CD4+ T cells, the CD8+ T cells recruited are less numerous compared to influenza. IL-17-producing CD8+ T cells are present after type-3 infection, but constitute a small population. CD8+ TRM cell development does take place, but is not as efficient as observed during a type-1 response. In contrast to Foxp3ΔTbx21 animals in which we observe a marked decrease in CD8+ TRM cells under steady-state conditions without known infection, Foxp3ΔRorγt animals have numbers of CD8+ TRM cells comparable to controls. This indicates that type-3 TREG cell recruitment does not make a critical contribution to the overall development of CD8+ TRM cells. Upon infection with A. fumigatus or SFBs, however, the absence of type-3 TREG cells makes CD8+ TRM cell development less efficient.
We confirm that the development of CD8+ TRM cells during a type-1 infection, such as influenza, does not depend on type-3 TREG cells but on type-1 TREG cell recruitment exclusively. Less polarised responses or non-type-1 dominated infections are less dependent on specific TREG subset recruitment to facilitate CD8+ TRM cell development. This is in agreement with the T cells detected during the A. fumigatus or SFB infection showing a type-1 and type-3 identity, hence relying on type-1 and type-3 TREG cell recruitment for CD8+ TRM cell establishment. Infections are often a mixed response with type-1 responses playing an important role in most42. This may reflect the involvement of CD8+ T cells, which show an overwhelming type-1 dominated response. In accordance, the development of CD8+ TRM cells during type-3 responses is not exclusively dependent on type-3 TREG cell recruitment, but also on type-1 TREG cells. However, the polarisation of CD8+ TRM cells is determined by the infection and not by the recruitment of type-1 or type-3 TREG cells. In the context of any invader, the establishment of a tissue-resident T-cell memory pool will be an advantage to locally contain the infection, independent of antigen specificity43.
The functional relevance of mismatched CD8+ TRM cells during a reinfection is speculative but type-3 responses are flexible and can be converted to give rise to type-1 cells44. Although largely observed on CD4+ T cells, a mixed type-1/-3 response can be beneficial to reduce pathogen load and pathology in subsequent infections45,46,47,48,49. In addition, tissue repair can be enhanced by type-2 responses and type-3 CD8+ TRM cells have been reported in the context of signals from injury and exposure to inflammatory mediators to release type-2 cytokines50. The physiological and clinical relevance of this mixed response, especially for CD8+ TRM cells, is currently not clear but a subject for future investigation.
In summary, we extend previous work that TREG cells, critical in preventing autoimmunity and immunopathology, have an important role in efficiently generating tissue-resident memory T cells from effector or memory precursors. We show that type-2 helminth infections are unlikely to result in robust de novo CD8+ TRM cell formation. Type-3 infections result in CD8+ TRM cell development, but less robust than type-1 infections. Type-1 TREG cell recruitment is required for CD8+ TRM cell development during type-1 infections, although type-3 TREG cells may assist in less type-1 dominated responses, resulting in a predominantly IFNγ–producing CD8+ TRM cell population. During type-3 infection, both type-1 and -3 TREG cells play an important role, resulting in the establishment of a CD8+ TRM cell population containing a mix of IFNγ- and IL-17-producing cells. Excluding helminths, independently of the type of pathogen encountered, CD8+ TRM cells are generated, offering enhanced protection against future challenges.
Methods
Mice
C57BL/6 J CD45.1 mice were purchased from Charles River, France. Tbx21fl/fl (Tbx21tm2Srnr) were kindly provided by Dr. Steven Reiner51, Foxp3eYFP-Cre (Foxp3tm4(YFP/icre)Ayr) was kindly provided by Dr. Alexander Rudensky52, Rosa26-tdRFP was kindly provided by Dr. Hans Jörg Fehling53. RORγtfl/fl mice were obtained on Jackson Laboratories, Foxp3eYFP-Cre TGFβ1-/- mice were kindly provided by Dr. Julien Marie14. Mice were bred at the Instituto de Medicina Molecular, Lisbon, Portugal. Male and female mice, aged and sex-matched, at 12–25 weeks of age were used. Animals were housed in IVC cages with temperature-controlled conditions under a 12-h light/dark cycle with free access to drinking water and food. All mice were kept in specific pathogen-free conditions. All mice in the Foxp3eYFP-Cre Rosa26-tdRFP lines were stringently genotyped by PCR and those in which a knockout allele was detected were discarded (~20%). In addition, mice were counter-screened for inappropriate expression of RFP in relation to eYFP (~10% discarded). All animal experimentation complied with regulations and guidelines of, and was approved by, the Direção-Geral de Alimentação e Veterinária Portugal and the local ethical review committee (Orbea).
Cell isolation
ntestine was flushed with PBS to remove contents and opened longitudinally. After cutting into 1 cm pieces, it was incubated in PBS containing 20 mM Hepes, 100 U/ml penicillin, 100 µg/ml streptomycin, 1 mM Pyruvate, 10% FCS, 100 μg/ml polymyxin B and 10 mM EDTA for 30 min at 37 °C while shaking to release IELs. IEL single-cell suspensions were further purified using 37.5% isotonic Percoll. To isolate LPLs, intestinal tissue was then digested in IMDM medium containing 0.5 mg/ml of Collagenase D (Roche) and 0.2 mg/ml of DNaseI (Roche) for 25 min at 37 °C while shaking.
Lungs were perfused with 20 mL of PBS before being shredded in small pieces with scissors and digested in IMDM medium containing 5% FBS and 0.5 mg/ml Collagenase D, 37 °C during 30 min while shaking. The cell suspension containing the lymphocytes was passed through a 50 μm cell strainer, incubated for 2 min in ACK solution, and lymphocytes were obtained after a 6-min wash with PBS at 500 g centrifugation.
Adoptive cell transfers
CD8α+ T cells and/or CD25+ cells (TREG cells) were purified from a single-cell suspension of spleen and lymph nodes. Briefly, cells were labelled with anti-CD8a-APC or anti-CD25-APC antibodies and selected with anti-APC MACS microbeads, according to the manufacturer’s instructions. After counting, purity was determined by flow cytometry, and cell numbers were adjusted. To ensure a wide TCR diversity in the population transferred a minimum of 2 × 106 CD8+ T cells were used. Some of the recipient mice received in addition 0.6–1 × 106 TREG cells. Infection was performed one day after cell transfer (day 0).
Influenza X-31 preparation and infection
Reverse genetics A/X-31 (PR8-HK4 and 6) were used as model viruses. Reverse genetics derived chimeric PR8 containing the segment 4 from A/Hong Kong/1/1968, seg4-HK68 (PR8-HK4), or the segment 6 (PR8-HK6) were produced as previously described54,55,56. pDual plasmids were a kind gift from Dr. Ron Fouchier (Erasmus MC, Netherlands). PR8 NA-E229A57 was generated by reverse genetics after site-directed mutagenesis of pDual::segment 6. All viruses were amplified in embryonated chicken eggs and titrated using plaque assay as previously described58,59. A viral load of 1000 PFU was administered in 30 μL PBS intranasally to mice. Mouse weight was monitored daily during the experiment to certify welfare, with mice going lower than 25% initial weight being sacrificed.
Eimeria vermiformis infection
Animals were infected with Eimeria vermiformis (Ev) as previously described in detail33. Briefly, oocysts were washed three times with deionized water, floated in sodium hypochloride and counted using a Fuchs-Rosenthal chamber. Mice received 5000 oocysts of E. vermiformis by oral gavage in 100 μl of water.
N. brasiliensis infection
N. brasiliensis worms were propagated as previously described30. Infective L3 larvae were kindly provided by Brian Chan at Dr Judith E Allen’s laboratory. Briefly, the larvae were obtained by cutting the filter paper in which they were provided around the borders (~0.5 cm), emerging it around gauze in a Falcon tube with 40 mL of PBS at 37 °C for 10 min (Baermann’s method). After this, larvae were allowed to pool down by gravity for 10 min, with the bottom 10–15 mL containing them being transferred to a 15 mL tube. The larvae were then purified by performing three washes at 168 g with minimum break. Mice were then injected with 300 L3s subcutaneously.
A. fumigatus preparation and infection
Fungal isolate A. fumigatus strain Af293 was purchased from the Fungal Genetics Stock Center (Kansas City, MO, United States). The fungal strain was cultivated on T-flasks containing sabouraud dextrose agar (SDA). Cultures were incubated in the dark, for 3–4 days, at 37 °C. Asexual spores (conidia) were harvested using glass beads and a saline solution B (0.85% NaCl, 0.1% Tween-20), washed twice with a saline solution A (0.85% NaCl), and collected after passing through three layers of miracloth filter. The harvested conidia were resuspended in a phosphate-buffered saline solution (0.01 M phosphate buffer, 0.0027 M potassium chloride, 0.137 M sodium chloride, pH 7.4), and kept at 4 °C until mice infection (same day). Prior to infection, conidia were counted with a hemacytometer and subsequently resuspended to a concentration of 3.3 × 107 conidia/mL−1, 30 µL were used for mice infection (106 conidia). Mice were submitted to 4 intranasal challenges with 106 conidia every 3 days over 2 weeks.
SFB fecal transplant
SFB-containing feces were kindly provided by Dr. Gérard Eberl at Pasteur Institute, Paris. Fecal pellets were collected and kept at −20 °C to maintain integral microbiota. On the day of the fecal transplant, feces were defrosted, mashed, and suspended in filtered tap water at a concentration of 100 mg/mL. Mice then received a fecal transplant of 200 μL of this suspension by oral gavage.
Flow cytometry
Single-cell suspensions from spleen, intestine, and lung were prepared and stained with antibodies (Supplementary Table 1), according to the agreed standards60. For intracellular cytokine staining, cells were pre-stimulated with PDBU (Phorbol 12,13-dibutyrate) (0.5 µg/mL) and ionomycin (0.5 μg/mL), in the presence of Brefeldin A (2 μg/mL) (all from Sigma) for 2 h at 37 °C. Samples were run on a Fortessa X20 cytometer (BD Biosciences) and analysed with FlowJo X software (TreeStar) (Supplementary Fig. 7).
Statistical analysis
In the present work, statistical analyses were performed using GraphPad Prism Software (GraphPad Prism version 9 for Windows, GraphPad Software, San Diego, California USA), details described in each figure legend where applicable. N denotes the number of independent biological repeats and n the total number of samples (mice). Error bars represent S.E.M. Mann–Whitney analysis was applied to compare ranks between two groups with a p value of 0.05. *P < 0.05, **P < 0.01, ***P < 0.001.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The authors declare that data supporting the findings of this study are available within the paper and its supplementary information files. Source data are provided with this paper. Additional materials or data that support the findings of this study are available from the corresponding authors. Source data are provided with this paper.
References
Konjar, S., Ferreira, C., Blankenhaus, B. & Veldhoen, M. Intestinal barrier interactions with specialized CD8 T cells. Front. Immunol. 8, 1281 (2017).
Masopust, D., Vezys, V., Marzo, A. L. & Lefrancois, L. Preferential localization of effector memory cells in nonlymphoid tissue. Science 291, 2413–2417 (2001).
Reinhardt, R. L., Khoruts, A., Merica, R., Zell, T. & Jenkins, M. K. Visualizing the generation of memory CD4 T cells in the whole body. Nature 410, 101–105 (2001).
Konjar, S., Ficht, X., Iannacone, M. & Veldhoen, M. Heterogeneity of tissue resident memory T cells. Immunol. Lett. 245, 1–7 (2022).
Shiow, L. R. et al. CD69 acts downstream of interferon-alpha/beta to inhibit S1P1 and lymphocyte egress from lymphoid organs. Nature 440, 540–544 (2006).
Skon, C. N. et al. Transcriptional downregulation of S1pr1 is required for the establishment of resident memory CD8+ T cells. Nat. Immunol. 14, 1285–1293 (2013).
Mackay, L. K. et al. Cutting edge: CD69 interference with sphingosine-1-phosphate receptor function regulates peripheral T-cell retention. J. Immunol. 194, 2059–2063 (2015).
Walsh, D. A. et al. The functional requirement for CD69 in establishment of resident memory CD8(+) T cells varies with tissue location. J. Immunol. 203, 946–955 (2019).
Ray, S. J. et al. The collagen binding alpha1beta1 integrin VLA-1 regulates CD8 T cell-mediated immune protection against heterologous influenza infection. Immunity 20, 167–179 (2004).
Mackay, L. K. et al. The developmental pathway for CD103(+)CD8+ tissue-resident memory T cells of skin. Nat. Immunol. 14, 1294–1301 (2013).
Cheuk, S. et al. CD49a expression defines tissue-resident CD8(+) T cells poised for cytotoxic function in human skin. Immunity 46, 287–300 (2017).
Reilly, E. C. et al. TRM integrins CD103 and CD49a differentially support adherence and motility after resolution of influenza virus infection. Proc. Natl. Acad. Sci. USA 117, 12306–12314 (2020).
Herndler-Brandstetter, D. et al. KLRG1(+) effector CD8(+) T cells lose KLRG1, differentiate into all memory T-cell lineages, and convey enhanced protective. Immunity 48, 716–729.e718 (2018).
Ferreira, C. et al. Type 1 Treg cells promote the generation of CD8(+) tissue-resident memory T cells. Nat. Immunol. 21, 766–776 (2020).
Bottois, H. et al. KLRG1 and CD103 expressions define distinct intestinal tissue-resident memory CD8 T-cell subsets modulated in Crohn’s disease. Front. Immunol. 11, 896 (2020).
Mackay, L. K. et al. T-box transcription factors combine with the cytokines TGF-beta and IL-15 to control tissue-resident memory T-cell fate. Immunity 43, 1101–1111 (2015).
Zaid, A. et al. Persistence of skin-resident memory T cells within an epidermal niche. Proc. Natl. Acad. Sci. USA 111, 5307–5312 (2014).
Mackay, L. K. et al. Hobit and Blimp1 instruct a universal transcriptional program of tissue residency in lymphocytes. Science 352, 459–463 (2016).
Konjar, S. et al. Mitochondria maintain controlled activation state of epithelial-resident T lymphocytes. Sci. Immunol. 3, eaan2543 (2018).
Konjar, S. & Veldhoen, M. Dynamic metabolic state of tissue resident CD8 T cells. Front. Immunol. 10, 1683 (2019).
Ariotti, S. et al. Tissue-resident memory CD8+ T cells continuously patrol skin epithelia to quickly recognize local antigen. Proc. Natl. Acad. Sci. USA 109, 19739–19744 (2012).
Barros, L., Ferreira, C. & Veldhoen, M. The fellowship of regulatory and tissue-resident memory cells. Mucosal Immunol. 15, 64–73 (2022).
de Goer de Herve, M. G., Jaafoura, S., Vallee, M. & Taoufik, Y. FoxP3(+) regulatory CD4 T cells control the generation of functional CD8 memory. Nat. Commun. 3, 986 (2012).
Pace, L. et al. Regulatory T cells increase the avidity of primary CD8+ T-cell responses and promote memory. Science 338, 532–536 (2012).
Laidlaw, B. J. et al. Production of IL-10 by CD4(+) regulatory T cells during the resolution of infection promotes the maturation of memory CD8(+) T cells. Nat. Immunol. 16, 871–879 (2015).
Miyao, T. et al. Plasticity of Foxp3(+) T cells reflects promiscuous Foxp3 expression in conventional T cells but not reprogramming of regulatory T cells. Immunity 36, 262–275 (2012).
Duhen, T., Duhen, R., Lanzavecchia, A., Sallusto, F. & Campbell, D. J. Functionally distinct subsets of human FOXP3+ Treg cells that phenotypically mirror effector Th cells. Blood 119, 4430–4440 (2012).
Levine, A. G. et al. Stability and function of regulatory T cells expressing the transcription factor T-bet. Nature 546, 421–425 (2017).
Harvie, M. et al. The lung is an important site for priming CD4 T-cell-mediated protective immunity against gastrointestinal helminth parasites. Infect. Immun. 78, 3753–3762 (2010).
Lawrence, R. A., Gray, C. A., Osborne, J. & Maizels, R. M. Nippostrongylus brasiliensis: cytokine responses and nematode expulsion in normal and IL-4-deficient mice. Exp. Parasitol. 84, 65–73 (1996).
Zelante, T. et al. IL-23 and the Th17 pathway promote inflammation and impair antifungal immune resistance. Eur. J. Immunol. 37, 2695–2706 (2007).
Ivanov, I. I. et al. Induction of intestinal Th17 cells by segmented filamentous bacteria. Cell 139, 485–498 (2009).
Figueiredo-Campos P, Ferreira C, Blankenhaus B, Veldhoen M. Eimeria vermiformis infection model of murine small intestine. Bio. Protoc. 8, e3122 (2018).
Gebhardt, T. et al. Memory T cells in nonlymphoid tissue that provide enhanced local immunity during infection with herpes simplex virus. Nat. Immunol. 10, 524–530 (2009).
Chaudhry, A. et al. CD4+ regulatory T cells control TH17 responses in a Stat3-dependent manner. Science 326, 986–991 (2009).
Koch, M. A. et al. T-bet(+) Treg cells undergo abortive Th1 cell differentiation due to impaired expression of IL-12 receptor beta2. Immunity 37, 501–510 (2012).
Mackay, L. K. et al. Long-lived epithelial immunity by tissue-resident memory T (TRM) cells in the absence of persisting local antigen presentation. Proc. Natl. Acad. Sci. USA 109, 7037–7042 (2012).
Khan, T. N., Mooster, J. L., Kilgore, A. M., Osborn, J. F. & Nolz, J. C. Local antigen in nonlymphoid tissue promotes resident memory CD8+ T-cell formation during viral infection. J. Exp. Med. 213, 951–966 (2016).
Anderson, K. G. et al. Intravascular staining for discrimination of vascular and tissue leukocytes. Nat. Protoc. 9, 209–222 (2014).
Wong, P. & Pamer, E. G. CD8 T-cell responses to infectious pathogens. Annu. Rev. Immunol. 21, 29–70 (2003).
Actor, J. K. et al. Helminth infection results in decreased virus-specific CD8+ cytotoxic T-cell and Th1 cytokine responses as well as delayed virus clearance. Proc. Natl. Acad. Sci. USA 90, 948–952 (1993).
Kiner, E. et al. Gut CD4(+) T-cell phenotypes are a continuum molded by microbes, not by TH archetypes. Nat. Immunol. 22, 216–228 (2021).
Ariotti, S. et al. T-cell memory. Skin-resident memory CD8(+) T cells trigger a state of tissue-wide pathogen alert. Science 346, 101–105 (2014).
Hirota, K. et al. Fate mapping of IL-17-producing T cells in inflammatory responses. Nat. Immunol. 12, 255–263 (2011).
Bai, H. et al. IL-17/Th17 promotes type 1 T-cell immunity against pulmonary intracellular bacterial infection through modulating dendritic cell function. J. Immunol. 183, 5886–5895 (2009).
Borkner, L., Curham, L. M., Wilk, M. M., Moran, B. & Mills, K. H. G. IL-17 mediates protective immunity against nasal infection with Bordetella pertussis by mobilizing neutrophils, especially Siglec-F(+) neutrophils. Mucosal Immunol. 14, 1183–1202 (2021).
Nguyen, N. et al. Th1/Th17 T-cell tissue-resident immunity increases protection, but is not required in a vaccine strategy against genital infection with chlamydia trachomatis. Front. Immunol. 12, 790463 (2021).
Dhume, K. et al. Bona fide Th17 cells without Th1 functional plasticity protect against influenza. J. Immunol. 208, 1998–2007 (2022).
Omokanye, A. et al. Clonotypic analysis of protective influenza M2e-specific lung resident Th17 memory cells reveals extensive functional diversity. Mucosal Immunol. 15, 717–729 (2022).
Harrison O.J. et al. Commensal-specific T-cell plasticity promotes rapid tissue adaptation to injury. Science 363, eaat6280 (2019).
Intlekofer, A. M. et al. Requirement for T-bet in the aberrant differentiation of unhelped memory CD8+ T cells. J. Exp. Med. 204, 2015–2021 (2007).
Rubtsov, Y. P. et al. Regulatory T cell-derived interleukin-10 limits inflammation at environmental interfaces. Immunity 28, 546–558 (2008).
Luche, H., Weber, O., Nageswara Rao, T., Blum, C. & Fehling, H. J. Faithful activation of an extra-bright red fluorescent protein in “knock-in” Cre-reporter mice ideally suited for lineage tracing studies. Eur. J. Immunol. 37, 43–53 (2007).
Marjuki, H. et al. An investigational antiviral drug, DAS181, effectively inhibits replication of zoonotic influenza A virus subtype H7N9 and protects mice from lethality. J. Infect. Dis. 210, 435–440 (2014).
Matrosovich, M., Matrosovich, T., Garten, W. & Klenk, H. D. New low-viscosity overlay medium for viral plaque assays. Virol. J. 3, 63 (2006).
Moskovich, O. & Fishelson, Z. Quantification of complement C5b-9 binding to cells by flow cytometry. Methods Mol. Biol. 1100, 103–108 (2014).
Luster, A. D. & Leder, P. IP-10, a -C-X-C- chemokine, elicits a potent thymus-dependent antitumor response in vivo. J. Exp. Med. 178, 1057–1065 (1993).
Miwa, T. et al. Deletion of decay-accelerating factor (CD55) exacerbates autoimmune disease development in MRL/lpr mice. Am. J. Pathol. 161, 1077–1086 (2002).
Miwa, T. et al. Decay-accelerating factor ameliorates systemic autoimmune disease in MRL/lpr mice via both complement-dependent and -independent mechanisms. Am. J. Pathol. 170, 1258–1266 (2007).
Cossarizza, A. et al. Guidelines for the use of flow cytometry and cell sorting in immunological studies (second edition). Eur. J. Immunol. 49, 1457–1973 (2019).
Acknowledgements
We would like to thank the excellent contributions from the iMM flow cytometry, rodent, and microscopy facilities. The project that gave rise to these results has received funding from the following sources:”la Caixa” Foundation under the grant agreement LCF/PR/HR19/52160005; European Union’s Horizon 2020 Research and Innovation Programme under grant agreements No 667824; FCT - Portuguese Foundation for Science and Technology under grant agreements (PD/BD/138847/2018) (COVID/BD/152538/2022) (L.B.) SFRH/BD/131605/2017 (P.F-C), COMPETE LISBOA-01-0145-FEDER-028003, and 2021.01136.CEECIND (C.F), FCT - Fundação para a Ciência e a Tecnologia, I.P., under the project LA/P/0082/2020, for work in the Veldhoen laboratory: and FCT PD/BD/135481/2018 (D.P.), UIDB/04612/2020, UIDP/04612/2020 and LA/P/0087/2020 for work in the Silva Pereira laboratory; FCG - Fundação Calouste Gulbenkian within the Post-Graduation Programme for Science and Development (N.S.), FCT CEECIND/02373/2020 and FCG, FCT and ”la Caixa” Foundation under the grant agreement HR22-00722 for work in the Amorim laboratory. The authors wish to acknowledge Brian Chan and Pedro Papotto, Lydia Becker Institute for Immunology & Inflammation, Faculty of Biology, Medicine & Health, Manchester Academic Health Science Centre, University of Manchester, United Kingdom for the delivery of N. brasiliensis.
Author information
Authors and Affiliations
Contributions
L.B., C.F. performed the experiments and analysis, with additional technical help from P.F.-C., S.A., J.F., S.R., M.B., and S.A. Aspergillus were grown and quality checked by D.P. and C.S.P. Influenza virus stocks and technical help from N.S. and M.J.A. C.F. and M.V. conceived and design the project. C.F., M.J.A., C.S.P., and M.V. supervised the work. All authors contributed to the data discussion and the writing of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Lalit Beura and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Barros, L., Piontkivska, D., Figueiredo-Campos, P. et al. CD8+ tissue-resident memory T-cell development depends on infection-matching regulatory T-cell types. Nat Commun 14, 5579 (2023). https://doi.org/10.1038/s41467-023-41364-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-023-41364-w
- Springer Nature Limited
This article is cited by
-
Tissue-resident memory T cells: decoding intra-organ diversity with a gut perspective
Inflammation and Regeneration (2024)
-
Mucosal T-cell responses to chronic viral infections: Implications for vaccine design
Cellular & Molecular Immunology (2024)