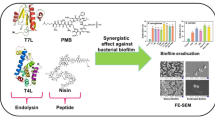
Abstract
Antibiotic resistance and the ability to form biofilms of Enterococcus faecalis have compromised the choice of therapeutic options, which triggered the search for new therapeutic strategies, such as the use of phage endolysins and antimicrobial peptides. However, few studies have addressed the synergistic relationship between these two promising options. Here, we investigated the combination of the phage endolysin Ply2660 and the antimicrobial peptide LL-37 to target drug-resistant biofilm-producing E. faecalis. In vitro bactericidal assays were used to demonstrate the efficacy of the Ply2660–LL-37 combination against E. faecalis. Larger reductions in viable cell counts were observed when Ply2660 and LL-37 were applied together than after individual treatment with either substance. Transmission electron microscopy revealed that the Ply2660–LL-37 combination could lead to severe cell lysis of E. faecalis. The mode of action of the Ply2660–LL-37 combination against E. faecalis was that Ply2660 degrades cell wall peptidoglycan, and subsequently, LL-37 destroys the cytoplasmic membrane. Furthermore, Ply2660 and LL-37 act synergistically to inhibit the biofilm formation of E. faecalis. The Ply2660–LL-37 combination also showed a synergistic effect for the treatment of established biofilm, as biofilm killing with this combination was superior to each substance alone. In a murine peritoneal septicemia model, the Ply2660–LL-37 combination distinctly suppressed the dissemination of E. faecalis isolates and attenuated organ injury, being more effective than each treatment alone. Altogether, our findings indicate that the combination of a phage endolysin and an antimicrobial peptide may be a potential antimicrobial strategy for combating E. faecalis.
Similar content being viewed by others
Introduction
Enterococcus faecalis is an opportunistic pathogen that has emerged as a major cause of healthcare-associated infections with high mortality rates1. This Gram-positive bacterium is able to survive under harsh conditions, making it well adapted to the hospital environment2,3. In addition, the worldwide spread of multidrug-resistant isolates, especially the emergence of vancomycin-resistant E. faecalis, puts huge economic pressure on the current healthcare systems because of the increasing risk of treatment failure and death4,5. Compared to the closely related species Enterococcus faecium, E. faecalis shows lower levels of intrinsic and acquired antibiotic resistance but is more virulent and more often isolated from hospitals4,5. It is considered the third-most prevalent nosocomial bacterial pathogen worldwide6. The U.S. Centers for Disease Control and Prevention listed vancomycin-resistant Enterococcus among the serious threat pathogens7.
Of great concern is that E. faecalis infections are usually linked to biofilm formation. Biofilms are dense multicellular communities of bacteria that form on biotic or abiotic surfaces, including human tissues, medical devices, and other materials8. Biofilm formation is a cyclic process involving initial attachment on a surface, microcolony formation, biofilm maturation, and dispersion9,10. Bacteria growing in the biofilm state are physiologically different from their planktonic cells, and their antibiotic tolerance can increase up to 1000-fold11,12. In addition, bacteria within biofilms are protected from the host defense, may persist for expanded time periods, and represent a reservoir for antibiotic resistance13,14. Biofilm-producing E. faecalis isolates occur worldwide. In Italy, biofilm production was identified among 87% of E. faecalis clinical isolates10,15. A study from the United States reported that 93% of 163 E. faecalis clinical and fecal isolates were classified as biofilm producers16. In China, 50.4 % of 113 E. faecalis isolates collected from urinary tract infections (UTI) produced biofilms17. Investigators from Japan have reported that all 352 E. faecalis isolates derived from UTI patients were able to form biofilms18. A study from Iran showed that 91 of the 95 E. faecalis isolates (95.8 %) produced biofilms19. Biofilm-producing E. faecalis isolates are often observed in a number of infections, including urinary tract infections, intra-abdominal and pelvic infections, catheter-related infections, surgical wounds, and endocarditis10,13. Thus, biofilm formation may be an important factor in the pathogenesis of E. faecalis infection.
The worsening antibiotic crisis and the prevalence of biofilm-producing E. faecalis underscore the necessity for the development of new therapeutic strategies. Antimicrobial peptides are bioactive small molecules produced by diverse organisms, which act as the first line of host defense against bacterial infections20. Among them, LL-37 is a 37-amino acid cationic peptide and the sole human member of the cathelicidin family21. This peptide is produced by many cell types, including epithelial cells, neutrophils, macrophages, and natural killer (NK) cells22. LL-37 displays outstanding antimicrobial activity and is active against a broad spectrum of microorganisms, including bacteria, viruses, and fungi23. In addition to its broad-spectrum antimicrobial activities, LL-37 has potent and multifarious immunomodulatory properties, including chemoattractant function, the release of pro-inflammatory cytokine, inhibition of neutrophil apoptosis, stimulation of angiogenesis, and tissue regeneration22,24. LL-37 also can augment the release of anti-inflammatory cytokines, neutralize bacterial LPS, and limit the expansion of inflammation25,26. Therefore, it has attracted much interest and is considered a promising agent to combat multidrug-resistant bacteria.
Another novel antibacterial strategy involves the use of phages and phage endolysins to control drug-resistant bacterial pathogens. Phages are viruses that can infect and kill bacteria. When following a lytic cycle, phages reorganize the host cell machinery to produce their own progeny. Phage endolysins are produced in phage-infected bacterial cells at the end of the phage replication cycle to destroy the cell walls and enable the release of the phage progeny27. Therefore, endolysins can be developed as antibacterial agents as they can cleave covalent bonds in the peptidoglycan cell wall of Gram-positive bacteria and induce cell death28. Compared to phages, endolysins as potential antimicrobial agents have distinct advantages. Phages usually infect specific bacteria with specificity, whereas several phage endolysins exhibit a broad lytic spectrum. For instance, PlyV12 has the capacity to kill enterococcal, streptococcal, and staphylococcal isolates29. In addition, endolysins are convenient for genetic engineering to improve the lytic activity30, expand the lytic spectrum31, or enhance the intracellular bactericidal activity32. Endolysins have better safety profiles as therapeutic agents as these enzymes exhibit non-cytotoxicity and a low probability of resistance development33,34. In contrast to broad-spectrum antibiotics, the antibacterial spectrum of endolysins is rather narrow, and, therefore, they do not destroy the physiological microbiota35. In addition, it appeared that the application of endolysins was an efficient strategy for preventing and eliminating biofilm-related infections36,37.
Combination therapy involving an antimicrobial peptide and a phage endolysin is considered to be a promising strategy to resolve the current clinical problem of severe antibiotic resistance in many pathogenic bacteria38. However, only limited data are currently available about the therapeutic efficacy of such combinations, and not all combinations are suitable for all bacteria. Thus, targeted approaches are necessary, which must be tailor-made for each bacterial pathogen. In this study, we explored the antibacterial and antibiofilm activities of the combination of the phage endolysin Ply2660, originating from a Streptococcus suis prophage, and the antimicrobial peptide LL-37 against E. faecalis in vitro, and evaluated the efficacy of this combination against vancomycin-resistant E. faecalis in a murine model of peritoneal septicemia.
Results
In vitro activity of combined Ply2660 and LL-37 against E. faecalis
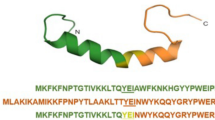
The antimicrobial peptide LL-37 displays an α-helical amphipathic structure, with higher hydrophobic residues and a net positive charge distributed on each side (Supplementary Fig. 1a). Ply2660 has a typical organization characteristic of phage endolysins targeting Gram-positive bacteria, including an N-terminal cysteine–histidine-dependent amidohydrolase/peptidase (CHAP) catalytic domain and a C-terminal cell wall-binding domain of SH3b (Supplementary Fig. 1b). The three-dimensional (3D) structure of Ply2660 was simulated using that of phage lysin Ly7917 (PDB code 5D74) as a template. Automated molecular modeling of the 3D structure generated a homology model consisting of six α-helices and six β-sheets in the CHAP domain, and eight β-sheets in the SH3 domain (Supplementary Fig. 1c). To examine the bacteriolytic activity, full-length Ply2660 was overexpressed in Escherichia coli BL21 (DE3) as a soluble protein, and the recombinant protein was purified using Ni2+-affinity chromatography. Successful purification was confirmed by sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE, Supplementary Fig. 1d).
The bactericidal activities of LL-37 and/or Ply2660 against five E. faecalis isolates, including vancomycin-resistant and multidrug-resistant clinical isolates, were subsequently determined in vitro (Fig. 1a). No significant reduction in the number of viable bacteria was observed when LL-37 was applied at a concentration of 4 μM (Fig. 1a, b), at which it could effectively kill other bacteria, including E. coli, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, Staphylococcus aureus, and Enterococcus faecium39. When evaluating the effects of Ply2660 alone in the absence of LL-37, Ply2660 at a concentration of 1.6 μM resulted in a minor reduction in the number of viable bacteria, only decreasing 0.7-log10 colony forming units (CFU) within 30 min. When the treating time prolonged to 120 min, Ply2660 achieved a reduction of 1.2-log10 CFU (Fig. 1b). Treatment with the Ply2660+LL-37 combination at the same concentration led to a decrease of 2.3-log10 CFU within 30 min and a 3.6-log10 decrease within 120 min (Fig. 1b). The concentration-kill experiments showed that 0.8 μM Ply2660 kills 0.5-log10 CFU of viable bacteria after treatment for 60 min, and a decrease of 2.0-log10 CFU of E. faecalis is observed when treated with 3.2 μM of Ply2660 (Fig. 1c). However, no significant reduction in the number of viable bacteria was observed when Ply2660 was applied to E. faecium isolates at a concentration of 3.2 μM (Supplementary Fig. 2). The Ply2660+LL-37 combination exhibited the enhanced bactericidal activity against E. faecalis in a dose-dependent manner (Fig. 1c). Within 60 min, the combination of Ply2660 (3.2 μM) and LL-37 (8 μM) showed high activity against E. faecalis, with a reduction of 4.5-log10 CFU (Fig. 1c). These results suggested that LL-37 can potentiate the bactericidal effect of Ply2660 on E. faecalis.
a Enterococcus faecalis strains were treated with LL-37, Ply2660, or a mixture of both and incubated for 1 h at 37 °C. Tenfold serial dilutions of each sample after different treatments were spotted onto BHI agar and incubated at 37 °C for 18 h. Controls were treated with PBS alone. These assays were repeated three times on independent occasions with similar results, and representative experiments are shown. b Time-dependent killing efficacy of LL-37 or/and Ply2660 against E. faecalis V583. Bacterial cells were washed with PBS and treated with 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both for different times (30, 60, 90, and 120 min); the viable cell number after each treatment is determined by plating on brain heart infusion (BHI) agar. c Dose-dependent killing efficacy of LL-37 or/and Ply2660 against E. faecalis V583. Bacterial cells were washed with PBS and treated with 2–8 μM of LL-37, 0.8–3.2 μM of Ply2660, or a mixture of both for 60 min, the viable cell number after each treatment is determined by plating on BHI agar. The data are presented as the means ± SD from three independent assays; error bars represent the standard deviation. Statistical significance was calculated using two-way ANOVA followed by Tukey’s multiple comparison test. *P < 0.05; **P < 0.01; ***P < 0.001; ns, not significant.
Morphological changes of E. faecalis treated with the combination of Ply2660 and LL-37
To investigate the possible mechanisms underlying this synergy of Ply2660 and LL-37, the morphological changes of E. faecalis V583 upon exposure to Ply2660 and/or LL-37 were determined using transmission electron microscopy (TEM). As shown in Fig. 2a, untreated E. faecalis showed intact cells with a regular spherical shape, containing a uniform cell wall and cytoplasmic membrane and a heterogeneous electron density in the cytoplasm. LL-37 alone caused no visible morphological changes in E. faecalis, including cell wall and membrane ultrastructure (Fig. 2a). However, a small number of cells of E. faecalis treated with Ply2660 showed altered morphology with an irregular shape, a swollen and destructed appearance, and a significant decrease in electron-dense molecules in the cytoplasm (Fig. 2a). Treatment with the Ply2660+LL-37 combination led to dramatic morphological alterations of E. faecalis, resulting mainly in cell lysis (Fig. 2a). Most E. faecalis cells exhibited cytoplasmic retraction, and the intracellular content appeared granulated or clumped, or it leaked out from the ruptured sites. Considerable breakage in the cell wall and cytoplasmic membrane caused by the Ply2660+LL-37 combination could be visualized, resulting in the presence of some “ghost” cells. Moreover, a large amount of cellular debris was observed, and numerous bleb-like structures were present in the visual field. Approximately 26% of cells were damaged cells after Ply2660 treatment, whereas the Ply2660+LL-37 combination led to approximately 77% of abnormal cells (Fig. 2b). The data indicated that the loss of viability in E. faecalis following exposure to the combination of Ply2660 and/ LL-37 was due to their bacteriolytic properties.
a TEM analysis of E. faecalis V583 in the mid-logarithmic phase or after exposure to LL-37, Ply2660, or a mixture of both was conducted. Controls were treated with PBS alone. Varying degrees of lysed morphology and leakage of contents are shown in E. faecalis after the different treatments. Scale bar, 500 nm. b Averages and standard deviations are shown for three independent counts, and the number of cells for each count was 100 (n = 100); error bars represent standard deviation. Statistical significance was calculated using one-way ANOVA followed by Tukey’s multiple comparison test. ***P < 0.001; ns, not significant.
Mode of action of the combination of Ply2660 and LL-37 against E. faecalis
To understand how LL-37 potentiates the bactericidal effect of Ply2660 on E. faecalis, the effects of LL-37 and/or Ply2660 on the cell wall and cytoplasmic membrane were analyzed. The purified cell wall of E. faecalis strain V583 was treated with LL-37, Ply2660, or a mixture of both, and the turbidity was monitored. Similar to the untreated control, LL-37 did not affect the turbidity. However, in the presence of Ply2660, the turbidity of the cell wall suspension decreased gradually as time elapsed. In addition, the Ply2660+LL-37 combination degraded the cell wall similarly to Ply2660 alone (Fig. 3a). These data indicated that Ply2660 is sufficient for the degradation of the cell wall. Subsequently, membrane damage of E. faecalis following exposure to Ply2660 and/or LL-37 was assessed with propidium iodide (PI), which can pass only through damaged membranes to stain nucleic acids. As shown in Fig. 3b, in the absence of Ply2660, LL-37 hardly facilitated the entry of PI into the bacteria. After the addition of Ply2660, the fluorescence intensity of PI was almost fourfold increased. This result suggested that LL-37 alone could not penetrate the cytoplasmic membrane of E. faecalis, unless the cell wall was degraded with the aid of Ply2660. Therefore, the outstanding bactericidal activity of the combination of Ply2660 and LL-37 is based on Ply2660-induced cell wall degradation and subsequent LL-37-mediated membrane damage.
a Degradation of cell walls of E. faecalis V583 after different treatments. Cell walls were prepared from E. faecalis in the logarithmic growth phase and diluted with fresh PBS. LL-37, Ply2660, a mixture of both, or mutanolysin, was added into the cell wall suspension, and samples were incubated at 37 °C. Controls were treated with PBS alone. OD600 was measured at various time points to determine turbidity. The data are presented as the means ± SD from three independent assays; error bars represent the standard deviation. b Membrane damage of E. faecalis V583 after different treatments. Enterococcus faecalis was treated with LL-37, Ply2660, a mixture of both, or mutanolysin, and incubated at 37 °C for 1 h. Controls were treated with PBS alone. Membrane permeability was measured by detecting the fluorescence intensity of PI. The data are presented as the means ± SD from two independent assays with three biological replicates in each assay; error bars represent standard deviation. Statistical significance was calculated using Brown–Forsythe and Welch ANOVA tests followed by Dunnett’s T3 multiple comparison test. ***P < 0.001; ns, not significant.
Ply2660 and LL-37 act synergistically against E. faecalis biofilm
To investigate the antibiofilm activity of Ply2660 in combination with LL-37, two E. faecalis isolates were chosen on the basis of their ability to form biofilms. These isolates included E. faecalis V583, which is known as a biofilm producer40, and E. faecalis Y15, which displays an even stronger biofilm phenotype than V583 (Fig. 4a, b). In general, the minimal inhibitory concentration (MIC) value of Ply2660 against the planktonic form of E. faecalis isolates V583 and Y15 was 12.8 μM, and the MIC value of LL-37 was 32 μM. While the minimum biofilm inhibitory concentration (MBIC) values of Ply2660 ranged from 12.8 to 25.6 μM, and that of LL-37 was 64 μM. As shown in Fig. 4a, b, LL-37 alone did not show any inhibitory effect on the E. faecalis biofilm formation, except showing a minor inhibitory effect at the concentration of 32 μM. However, Ply2660 dose-dependently inhibited the biofilm at the higher concentrations (≥1.6 μM). A significant biofilm reduction was observed when Ply2660 was combined with LL-37 (Fig. 4a, b). In addition, as shown in Fig. 4c, d, LL-37 alone (at the concentrations of 4 and 8 μM) did not significantly alter the number of viable bacteria in biofilm compared to the untreated control. However, Ply2660 (at the concentrations of 1.6 and 3.2 μM) slightly reduced the number of viable bacteria (0.8 and 1.7-log10 CFU in V583 biofilm, 0.7 and 1.3-log10 CFU in Y15 biofilm). Conversely, the combination of both substances at the abovementioned concentrations led to a remarkable reduction in viable bacteria (3.7 and 4.6-log10 CFU in V583 biofilm, 3.6 and 4.5-log10 CFU in Y15 biofilm).
Biofilm inhibition was assessed by incubating LL-37 and/or Ply2660 with E. faecalis isolates in the wells of 96-well polystyrene microtiter plates for 24 h. Bacteria without any treatment were used as a control. The adhered biofilms of a V583 and b Y15 isolates were measured using crystal violet staining. OD600 values are the average of two independent assays with three biological replicates in each assay. The number of viable bacteria in the biofilms of c V583 and d Y15 isolates was examined. Results expressed as [log10 CFU/well]. The data are presented as the means ± SD from two independent assays with three biological replicates in each assay; error bars represent standard deviation. Statistical significance was calculated using one-way ANOVA followed by Tukey’s multiple comparison test. *P < 0.05; **P < 0.01; ***P < 0.001; ns, not significant.
Next, the abilities of LL-37 and/or Ply2660 against established (24 h) biofilms were investigated. As observed before, LL-37 alone had no effect on the number of viable bacteria in established biofilms of E. faecalis V583 and Y15 after 6 h exposure, and the effect of the Ply2660 on biofilm colony counts was less compared to those of the Ply2660+LL-37 combination (Fig. 5a, b). To better evaluate the effectiveness of the Ply2660–LL-37 combination on biofilm killing, mature biofilms were treated with LL-37 and/or Ply2660 and visualized by confocal laser scanning microscopy (CLSM) after the live/dead staining. SYTO 9 stains living bacterial cells with green fluorescence, and PI stains cells with impaired membranes with red fluorescence. As shown in Fig. 5c, after 24 h of incubation without treatment, E. faecalis Y15 displayed well-structured biofilms. LL-37 treatment did not show any obvious change compared to the untreated control. However, Ply2660 increased the number of dead bacteria in the biofilm. The combined treatment led to strikingly larger amounts of red-stained dead cells. These results demonstrated the synergistic effect of Ply2660 and LL-37 against E. faecalis biofilms. To determine whether LL-37 or Ply2660 directly affect biofilm extracellular matrix, E. faecalis Y15 biofilms after LL-37 and/or Ply2660 treatment were stained to visualize different components of the biofilm using Alexa Fluor 350-labeled Concanavalin A (polysaccharides) and SYPRO Ruby Biofilm Matrix stain (proteins) (Supplementary Fig. 3). LL-37 or Ply2660 alone, or their combination showed no obvious changes in fluorescence intensity (for either polysaccharides or protein respectively) from the CLSM images. These results suggested that the action of Ply2660 and LL-37 against E. faecalis biofilms is mainly due to the destruction of the biofilm-embedded cells.
Bactericidal activity of LL-37 and/or Ply2660 against preformed biofilms of E. faecalis isolates a V583 and b Y15. Biofilms were allowed to develop for 24 h and then treated with LL-37 and/or Ply2660 for 6 h at 37 °C. Bacteria without any treatment served as a control. Results are expressed as the number of viable bacteria [in log10 CFU/well]. The data are presented as the means ± SD from two independent assays with three biological replicates in each assay; error bars represent standard deviation. Statistical significance was calculated using one-way ANOVA followed by Tukey’s multiple comparison test. *P < 0.05; **P < 0.01; ***P < 0.001; ns, not significant. c Representative confocal microscope images of LIVE/DEAD-stained E. faecalis Y15 in 24-h-established biofilms after treatment with the indicated concentrations of LL-37, Ply2660, or a mixture of both at 37 °C for 6 h.
The combination of Ply2660 and LL-37 suppresses the dissemination of E. faecalis in infected mice
In light of the synergistic effect of the combination of Ply2660 and LL-37 on E. faecalis in vitro, we evaluated the therapeutic potential of this synergistic action. Before that, the hemolytic activities of LL-37 and Ply2660 against human red blood cells were determined as an indication of their toxicity toward mammalian cells. As shown in Supplementary Fig. 4, neither LL-37 nor Ply2660 exhibited notable hemolytic activity. Minor hemolytic effects (less than 13.5%) were observed for LL-37 at a concentration of 64 μM, whereas Ply2660 exhibited negligible hemolytic activity. To further evaluate the safety of LL-37 and Ply2660 in vivo, LL-37 and/or Ply2660 at the therapeutic dose were intraperitoneally injected into mice, and the changes in body weight were monitored for 14 days. The results showed that all mice from each group remained healthy, as indicated by the gradual increase in body weight during the observation period (Supplementary Fig. 5a). At 14 days after injection, lung, liver, kidney, and spleen were collected to observe whether or not these organs suffer from toxic damage. As shown in Supplementary Fig. 5b, LL-37 or Ply660 alone or the combination of both did not cause pathologic injuries.
Thereafter, the therapeutic effect of the Ply2660+LL-37 combination was evaluated in a murine model of peritoneal septicemia. Accordingly, BALB/c mice were infected with a high dose (1.8 × 109 CFU) of E. faecalis V583 by intraperitoneal injection, and PBS, LL-37, Ply2660, or the Ply2660+LL-37 combination was administered 1 h post-infection. As shown in Fig. 6a, almost all mice in the PBS-treatment group died within 24 h. LL-37 barely had a therapeutic effect against intraperitoneal challenge with E. faecalis, whereas treatment with Ply2660 was able to rescue 58.3% of the infected mice. The combination of Ply2660 and LL-37 showed improved survival rates, rescuing 83.3% of the infected mice.
a Survival curves of mice infected intraperitoneally with E. faecalis V583 (high dose, 1.8 × 109 CFU) and treated with a single dose of LL-37, Ply2660, a combination of LL-37 and Ply2660, or PBS via intraperitoneal injection (n = 12 for each group). For examination of bacterial loads in the b lung, c liver, and d kidney, mice were infected intraperitoneally with a lower dose (8 × 107 CFU) of E. faecalis V583 and treated as above (n = 5 for each group). The bacterial load was calculated by plating the samples on BHI agar. The data are presented as the means ± SD from five mice; error bars represent the standard deviation. Statistical significance was calculated using one-way ANOVA followed by Tukey’s multiple comparison test. **P < 0.01; ***P < 0.001; ns, not significant. e Bacterial detection (arrows) in tissue sections with H&E staining. Scale bars, 20 μm.
Next, BALB/c mice were infected with a lower dose (8 × 107) of E. faecalis V583, and the treatment protocol was the same as before. After 24-h treatment, samples were collected from harvested organs for quantification of E. faecalis. As shown in Fig. 6b–d, high bacterial burdens were detected in the lung, liver, and kidney of mice in the PBS-treated group, indicating E. faecalis dissemination from the peritoneal cavity to multiple organs. Treatment with LL-37 alone did not cause a significant reduction in bacterial burden compared to the PBS-treated group. In contrast, treatment with Ply2660 reduced the bacterial burden in the lungs by approximately 1.1-log10 CFU compared to the PBS-treated group (Fig. 6b). A similar effect was observed in the liver and kidney (Fig. 6c, d). Moreover, the Ply2660+LL-37 combination caused a significant reduction in the bacterial burden compared to each treatment alone. Compared with the PBS-treated group, on average, a more than 3.0-log10 CFU reduction in bacterial burden was detected in the Ply2660+LL-37 group (Fig. 6b–d). As seen in Fig. 6e, a lot of coccus-shaped bacteria appeared in lung, liver, and kidney of mice from PBS-treated group and LL-37-treated group, whereas the number of such bacteria decreased in the organs of mice of the Ply2660-treated group, and few or no cocci were seen in those of mice of the Ply2660+LL-37 group. These results showed that the combination of Ply2660 and LL-37 demonstrated higher efficacy against E. faecalis dissemination than each treatment alone.
The combination of Ply2660 and LL-37 attenuates organ injury in E. faecalis-infected mice
The therapeutic effects of LL-37 and/or Ply2660 were also confirmed by histological analysis. The hematoxylin and eosin (H&E)-stained sections (Fig. 7a) showed dramatic pathological damage in tissues of mice treated with PBS, including a high degree of inflammatory cell infiltration, severe blood stasis and hemorrhage, thickened respiratory membranes, hepatocyte degeneration and necrosis, hepatic sinusoidal dilation and congestion, renal tubular interstitial congestion with blurred brush border and clearly visible cast formation. However, LL-37 or Ply2660 treatment partially alleviated the tissue damage that occurred due to the E. faecalis infection. Remarkably, combined therapy with Ply2660+LL-37 almost completely abolished the inflammation damage induced by E. faecalis (Fig. 7a). Organ histological score analysis (Fig. 7b–d) confirmed these findings; the injury scores of lung, liver, and kidney from mice in the combined therapy group were significantly lower than those of the mice in the other groups, illustrating the contribution of the combination of Ply2660 and LL-37 to the restoration of E. faecalis-induced organ injury.
a Samples of the lung, liver, and kidney from mice with different treatments were fixed in 4% formalin, and tissue sections were prepared for H&E staining. Scale bars, 50 μm. Pathological scores of the b lung, c liver, and d kidney were evaluated from three random fields by two independent scientists. The data are presented as the means ± SD; error bars represent the standard deviation. Statistical significance was calculated using one-way ANOVA followed by Tukey’s multiple comparison test. *P < 0.05; **P < 0.01; ***P < 0.001; ns, not significant.
Discussion
Enterococcus faecalis commonly causes difficult-to-treat infections because of intrinsic and acquired resistance to a wide range of antibiotics4. Especially during the COVID-19 pandemic, E. faecalis co-infection in hospitalized COVID-19 patients increased the risk of treatment failure and death41,42. Moreover, when linezolid and daptomycin received licensing for the treatment of infections caused by vancomycin-resistant enterococci, resistant isolates began to appear in clinical settings since then43,44. Novel alternative antimicrobial agents and therapeutic strategies are urgently needed to combat E. faecalis infections. In this context, antimicrobial peptides and phage endolysins are considered promising candidates, and efforts to achieve clinical application are currently accelerating.
Enterococcus faecalis is protected by a thick mesh of peptidoglycan that maintains cellular integrity45. Nevertheless, this bacterium can be attacked by phage endolysins, which are efficient enzymes that directly cleave covalent bonds within the cell wall peptidoglycan and eventually cause bacterial lysis and death46. The endolysin Ply2660 has attracted our attention because it has a cell wall-binding domain of SH3b similar to that of the endolysin PlyV12 from an enterococcal phage29, implying the probability of Ply2660 targeting E. faecalis. In this study, the phage endolysin Ply2660 was found to degrade the peptidoglycan of E. faecalis and, thus, kill this bacterium. In addition, Ply2660 also exhibited lytic activities to vancomycin-resistant isolates, which are responsible for nosocomial infections to some extent. However, Ply2660 did not kill E. faecium isolates. As far as we know, several of the so far reported E. faecalis endolysins could also lyse E. faecium, such as IME-EF147, PlyV1229, and ORF9 of phage ΦEF24c48. However, the endolysin LysEF-P10 derived from an E. faecalis phage also did not kill E. faecium49. The peptidoglycan compositions of E. faecalis and E. faecium show minor differences. They have the same pentapeptide stem linked to the N-acetylmuramic acid but differ in the cross-linking bridge. The bridge is L-Ala-L-Ala in the peptidoglycan of E. faecalis, but D-Asp in that of E. faecium50,51,52, which may be the reason why E. faecium cannot be killed by Ply2660. Ply2660 possesses a CHAP catalytic domain, which can serve as N-acetylmuramoyl-L-alanine amidase or endopeptidase53. Since the cleavage site of N-acetylmuramoyl-L-alanine amidase is the same in E. faecalis and E. faecium, it is very likely that Ply2660 exerted endopeptidase activity, leading to its different bactericidal ability against E. faecalis and E. faecium, but this needs to be further ascertained.
It is well documented that the human antimicrobial peptide LL-37 exerts bactericidal activity against a variety of bacteria20,39. However, the findings in our study indicated that E. faecalis could resist the killing by LL-37. Moreover, E. faecalis is likely to be resistant not just to LL-37, but also to other antimicrobial peptides of host or bacterial origin. A previous study revealed that E. faecalis displays high intrinsic resistance against bacitracin, an antimicrobial peptide isolated from a strain of Bacillus54. It has been reported that E. faecalis gelatinase can cleave LL-37, which may be an important strategy exploited by E. faecalis to resist the killing of antimicrobial peptides55. In addition, we speculated whether some so far undiscovered surface-associated proteins of E. faecalis might hinder the access of antimicrobial peptides to the cytoplasmic membrane. Similarly, the surface-associated M1 protein of Streptococcus pyogenes has been demonstrated to sequester and neutralize LL-37 antimicrobial activity through its N-terminal domain56. However, additional studies are required to ascertain whether a similar mechanism applies to E. faecalis. From the perspective of pathogen-host interactions, the resistance of E. faecalis against antimicrobial peptides might be important for the successful invasion of this bacterium into the human host. In this study, we showed that although LL-37 alone did not kill E. faecalis, the addition of Ply2660 could trigger the antibacterial activity of LL-37 against E. faecalis, and the combination of both showed high efficacy at low concentrations, which might encourage their combined use for the control of E. faecalis. The synergy between Ply2660 and LL-37 could be explained as follows: degradation of the cell wall by Ply2660 makes the cytoplasmic membrane of E. faecalis more accessible to LL-37 (Fig. 8).
Enterococcus faecalis is protected against LL-37 by a thick mesh of peptidoglycan. However, Ply2660 degrades the cell wall peptidoglycan of E. faecalis, making the cytoplasmic membrane more accessible to LL-37. Subsequently, LL-37 interacts with the cytoplasmic membrane and inserts itself into lipid bilayers, leading to pore formation in the lipid membranes and lysis of E. faecalis. Thus, the combination of Ply2660 and LL-37 exerts synergistic antimicrobial effects against E. faecalis.
The ability of E. faecalis to form biofilms can exacerbate the pathogenicity that leads to life-threatening infections. Furthermore, when biofilms are produced by multidrug-resistant E. faecalis, the chances of successfully eradicating them are even smaller13. Previous studies have demonstrated that phage therapy was more effective in some cases for combating E. faecalis than conventional antibiotics, particularly when it comes to infections with multidrug-resistant biofilm-producing isolates57,58. Moreover, several phage endolysins, such as lys08 and ϕEf11 ORF28, showed antibiofilm activity against E. faecalis biofilms59,60. Similar to these previous studies, Ply2660 also exhibited antibiofilm activity against E. faecalis biofilms to some extent. Compared to the single Ply2660 treatment, the Ply2660+LL-37 combination showed distinctly higher antibiofilm activity against E. faecalis biofilms. Notably, Ply2660 and LL-37 did not destroy the main component of the biofilm extracellular matrix. The ability of Ply2660+LL-37 combination to inhibit biofilm formation is most likely attributable to their powerful bactericidal activity before biofilm formation. In addition, the Ply2660+LL-37 combination also exhibited excellent bactericidal efficacy in established biofilms. By adopting a biofilm lifestyle, bacteria grow slowly or do not grow due to a deficiency of nutrients that results in tolerance to antibiotics14. The mode of action of Ply2660 and LL-37, which is unlike antibiotics, does not require the metabolic machinery of the cell as they target the peptidoglycan and cytoplasmic membrane. Thus, the Ply2660+LL-37 combination could kill dormant cells in biofilm as well as planktonic cells. Furthermore, since both endolysins and antimicrobial peptides have low molecular weight, it is probable that they can penetrate more easily into deeper layers of the biofilm. It has been reported previously that the catalytic domain of an endolysin can help it penetrate into the biofilm61.
Combined therapy offers a promising tool to cope with the rising global crisis of antibiotic resistance62. Phage endolysins and antimicrobial peptides have been found to act synergistically in the treatment of infections due to antibiotic-resistant bacteria38,63. The combined application of phage endolysins and antimicrobial peptides against antibiotic-resistant bacteria is an interesting research area that is still in its infancy38. In this study, we showed that the combination of Ply2660 and LL-37 not only displayed synergistic activity against E. faecalis in vitro but also elicited synergistic effects in vivo, increasing the survival rate, reducing the bacterial burden and alleviating tissue inflammation in E. faecalis-infected mice. Despite our study verifying the therapeutic effect only in the E. faecalis-induced murine model of peritoneal septicemia, the potential of the Ply2660+LL-37 combination is clear. This combination may be able to treat intra-abdominal and pelvic infections. However, it is necessary to pay attention to the possibility of an immune response caused by Ply2660 after systemic administration, and further studies involving its clinical application need to be carried out. In addition, it also remains to be established whether the combined Ply2660 and LL-37 could be coated on the catheter surfaces to avoid catheter-related infections, which are of major relevance among E. faecalis infections.
Natural antimicrobial peptides often have cytotoxic effects, which limit their clinical application. Although LL-37 has entered the phase II clinical trial64, it indeed shows minor hemolytic activity at a high concentration, but its therapeutic dose in this study did not cause toxicity in mice. Although Ply2660 does not exhibit hemolytic activity in vitro, its possible immunogenicity cannot be excluded. Combination therapy may be a suitable strategy to fight E. faecalis infection in vivo by maximizing effectiveness and minimizing the side effects of Ply2660 and LL-37. On the one hand, the high production cost is another limitation of the clinical application of endolysins and antimicrobial peptides. To reduce production costs, future studies should consider further increasing the solubility and expression level of endolysins, as well as choosing more cost-effective expression systems, or developing prodrugs fusing the endolysins and antimicrobial peptides. Our ongoing research is also designing new antimicrobial peptides with smaller molecular weights to reduce costs, improve antibacterial activity, and reduce toxicity. Thereby, we expect to find safer antimicrobial peptides for optimized combinations.
In conclusion, this work shows the potential of the synergistic interaction between the phage endolysin Ply2660 and the antimicrobial peptide LL-37 to develop a more efficient antimicrobial combination therapy against infections caused by vancomycin-resistant and multidrug-resistant E. faecalis. The high efficacy of this combination therapy is based on the mode of action of Ply2660-induced cell wall degradation and subsequent LL-37-mediated membrane damage. Overall, this strategy provides a promising antibiotic-free alternative approach to combat drug-resistant bacteria and opens a new path for the treatment of life-threatening bacterial diseases. Further studies are needed to exploit the potential of this combination for optimizing health outcomes.
Methods
Bacterial strains and growth conditions
The E. faecalis isolates used in the present study were the reference strain ATCC 29212, the vancomycin-resistant reference strain ATCC 5129965, the vancomycin-resistant clinical isolate V58366, the multidrug-resistant clinical isolate SY-167, and the Y15 isolate (resistance to erythromycin, gentamicin, and streptomycin) isolated from bovine feces with the capacity of producing biofilm in this study. The E. faecium isolates used in the present study were the vancomycin-resistant reference strain ATCC 700221, the vancomycin-resistant EFM30 isolate, and the vancomycin-susceptible EFM171 isolate, which were isolated from bovine feces in this study. All E. faecalis and E. faecium isolates were grown in Trypticase soy broth (TSB), BHI broth, or BHI agar (Difco, Detroit, MI, USA) at 37 °C.
Bioinformatics analysis
The 3D structure of LL-37 was obtained from the RCSB Protein Data Bank68. Protein domains of Ply2660 were identified using SMART69. Protein structure homology modeling of Ply2660 was conducted by SWISS-MODEL70. The structures of LL-37 and Ply2660 were presented using PyMOL (DeLano Scientific, San Carlos, CA, USA).
Protein expression and purification
The ply2660 gene (GenBank accession number CP031379.1) was chemically synthesized, and inserted into the pET22b plasmid (Novagen, San Diego, CA, USA) by BGI Biotech (Beijing, China). The recombinant plasmid pET22b-ply2660 was sequenced for confirmatory reasons and transformed into competent Escherichia coli BL21 (DE3) cells. Protein expression was induced by 0.5 mM of isopropyl 1-thio-β-D-galactopyranoside (Sigma-Aldrich, St. Louis, MO, USA) with shaking for 12 h at 16 °C. The cultures were then centrifuged, and the cell pellets were resuspended in binding buffer (20 mm Tris-HCl, pH 7.9, 0.5 m NaCl, and 20 mm imidazole). Then, the cells were disrupted by sonication, and supernatants were collected by centrifugation at 10,000×g for 10 min. His-tagged protein was purified using a Ni-SepharoseTM 6 Fast Flow column (GE Healthcare, Uppsala, Sweden) according to the manufacturer’s instructions. The elution buffer was changed to PBS using a PD-10 desalting column (GE Healthcare, Uppsala, Sweden). The purified protein was analyzed using 12% SDS-PAGE. All gels derive from the same experiment and were processed in parallel. The protein concentration was determined using a bicinchoninic acid protein assay kit (Beyotime, Shanghai, China).
Determination of minimal inhibitory concentration
The MICs of LL-37 and Ply2660 were determined using the standard broth microdilution method recommended by the Clinical and Laboratory Standards Institute71. Briefly, a final bacterial suspension of 5 × 105 CFU/ml in cation-adjusted Mueller–Hinton broth (Becton Dickinson, Sparks, MD, USA) was exposed to LL-37 or Ply2660 in a series of twofold serial dilutions in 96-well polypropylene microtiter plates (Nest, Wuxi, China). Cells were challenged with 0.5–256 μM of LL-37, or 0.2–51.2 μM of Ply2660 in triplicate. The MIC value was defined as the lowest concentration of LL-37 or Ply2660 that inhibited visible growth.
Bactericidal assays
Enterococcus faecalis isolates were grown in BHI broth at 37 °C to an optical density at 600 nm (OD600) of 0.8. Each isolate was harvested and diluted in PBS (pH 7.4) to a concentration of 2 × 106 CFU/ml. Then, 25 μl of bacterial suspensions (5 × 104 CFU) were added into the 96-well polypropylene microtiter plates (Nest, Wuxi, China), and incubated in the presence of 4 μM of LL-37 (GL peptide Inc., Shanghai, China, purity > 98%), 1.6 μM of Ply2660, or a mixture of both in a total volume of 200 μl PBS. As an untreated control, bacteria were incubated in PBS. After incubation for 1 h at 37 °C, each sample was serially diluted, and 10 μl aliquots of the serial dilutions were spotted onto BHI agar. The plates were incubated at 37 °C for 18 h.
For time-kill experiments, E. faecalis V583 (1 × 105 CFU) was incubated in the presence of 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both in PBS in polypropylene tubes in a total volume of 500 μl. After incubation at 37 °C for 30 to 120 min, each sample was serially diluted, and 100 μl aliquots of the serial dilutions were plated on BHI agar for CFU counting. For concentration-kill experiments, E. faecalis V583 (1 × 105 CFU) was incubated in the presence of 2–8 μM of LL-37, 0.8–3.2 μM of Ply2660, or a mixture of both in a total volume of 500 μl at 37 °C for 60 min. Aliquots were serial diluted and plated to assess viability.
Enterococcus faecium isolates (1 × 105 CFU) were incubated in the presence of 3.2 μM of Ply2660 in a total volume of 500 μl at 37 °C for 60 min. Aliquots were serial diluted and plated to assess viability.
Transmission electron microscopy
Enterococcus faecalis V583 was cultivated in 5 ml of BHI broth at 37 °C until the mid-logarithmic phase. The cultures were washed three times and resuspended in PBS at a concentration of 5 × 108 CFU/ml, and exposed to 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both at 37 °C. Bacteria without any treatment were used as control. After 1 h, the samples were fixed with 2.5% glutaraldehyde overnight and then post-fixed with 2% osmic acid at 4 °C for 2 h. Following dehydration in upgraded ethanol, the samples were embedded in SPI-Pon 812 resin. Polymerization was done at 70 °C for 2 days, and 65–70-nm sections were cut using a UC6 ultra-microtome (Leica Microsystems, Vienna, Austria) and post-stained with uranyl acetate and lead citrate. Electron micrographs were visualized by an H-7650 transmission electron microscope (Hitachi, Tokyo, Japan).
Cell wall degradation assay
The effect of LL-37 and/or Ply2660 on the degradation of E. faecalis cell walls was examined by measuring the turbidity of the bacterial suspension. Enterococcus faecalis strain V583 was grown in 500 ml of BHI broth at 37 °C to the mid-logarithmic phase and washed three times with PBS. The bacterial pellet was resuspended in 14 ml of 4% SDS and boiled for 30 min. The cell wall was isolated by centrifugation at 10,000 × g for 15 min, washed four times with distilled water, and then incubated in 10 ml of buffer (0.5 mg/ml trypsin in 0.1 M Tris-HCl, pH 6.8, and 20 mM CaCl2) at 37 °C for 18 h. Thereafter, the sample was washed four times with distilled water, resuspended in 2 ml 10% trichloroacetic acid, and incubated at 4 °C for 6 h. The cell wall was further washed four times with distilled water and resuspended in PBS. The purified E. faecalis cell wall suspension was incubated in the presence of 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both at 37 °C. The cell wall-degrading enzyme mutanolysin (Sigma-Aldrich, St. Louis, MO, USA) was used as a positive control. The OD600 was monitored for 5 h at 1-h intervals.
Detection of membrane permeability
Bacterial cell membrane damage induced by the different treatments was monitored by detecting PI uptake. Briefly, mid-logarithmic phase cultures of E. faecalis strain V583 were resuspended in PBS to 1 × 106 CFU/ml and incubated in the presence of 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both at 37 °C for 1 h. Then, 10 μl PI (Invitrogen, Eugene, OR, USA) was added to a final concentration of 4 μg/ml, and samples were incubated for 20 min at 25 °C. Fluorescence was detected using an EnSpire Multiscan Spectrum (PerkinElmer, Massachusetts, USA), at an excitation wavelength of 535 nm and an emission wavelength of 617 nm.
Inhibition of biofilm formation
Mid-logarithmic growth-phase cultures of E. faecalis V583 and Y15 were diluted in TSB medium to 1 × 108 CFU/ml. Fifty microliters of this bacterial suspension were exposed to the various concentrations of LL-37 and/or Ply2660, then added to 96-well polypropylene microtiter plates (Corning, NY, USA). Bacteria without any treatment served as a control. After 24-h incubation at 37 °C, planktonic bacteria were washed from the biofilms. The biofilms were stained with 1% crystal violet (Sigma-Aldrich, St. Louis, MO, USA) for 20 min, washed, and solubilized with 33% acetic acid. The optical density at 600 nm was determined by a microplate spectrophotometer. Minimum biofilm inhibitory concentration (MBIC) is defined as the lowest concentration at which there were no detectable biofilms after 24-h incubation72. The number of viable bacteria in biofilms exposed to the indicated concentrations of LL-37 and/or Ply2660 was also quantified by plate colony counts.
Treatment of established biofilm
Mid-logarithmic growth-phase cultures of E. faecalis V583 and Y15 were diluted and added to 96-well polypropylene microtiter plates (Corning, NY, USA) without treatment and incubated for 24 h at 37 °C to allow biofilm formation. Afterward, planktonic bacteria were removed, and the biofilms were gently washed twice with PBS. Thereafter, the adhered biofilms were treated with the indicated concentrations of LL-37 and/or Ply2660. Bacteria without any treatment were used as a control. After 6-h incubation at 37 °C, the medium was removed, and the biofilm was gently washed three times with PBS. To assess the biofilm-killing efficacy of the different treatments, the number of viable bacteria in the biofilm was quantified by plate colony counts.
For confocal microscopy analysis, 24-h-established biofilms were formed by inoculating 2 ml of an E. faecalis Y15 cell suspension containing approximately 2 × 106 CFU/ml in glass-bottom microwell dishes (Nest, Wuxi, China). After washing twice, biofilms were exposed to 4 μM of LL-37, 1.6 μM of Ply2660, or a mixture of both for 6 h at 37 °C. At the end of the treatment, biofilms were washed twice with PBS and stained with the Live/Dead® BacLightTM kit (Invitrogen, Eugene, OR, USA). For exopolysaccharide visualization, biofilms were stained with Alexa Fluor 350-labeled Concanavalin A (Invitrogen, Eugene, OR, USA). The proteins in the biofilms were stained with SYPRO Ruby Biofilm Matrix stain (Invitrogen, Eugene, OR, USA). Samples were visualized using a confocal scanning laser microscope (Zeiss LSM 880, Jena, Germany).
Hemolysis assay
Human red blood cell suspensions (4% (w/v)) in PBS (pH 7.4) were incubated with various concentrations of LL-37 or Ply2660 for 1 h at 37 °C. Following this, the samples were centrifuged at 500 × g for 10 min, and the supernatant absorbance was read at 415 nm. A 1% Triton X-100 (Sigma-Aldrich, St. Louis, MO, USA) solution served as positive Control (Atriton). The percentage of hemolysis was calculated using the following formula: hemolysis % = [(Asample − APBS) / (Atriton − APBS)] × 100.
Toxicity to BALB/c mice
All of the experiments involving mice were conducted in accordance with the guidelines and policies of Laboratory Animals of the Ministry of Science and Technology of China. The protocols were reviewed and approved by the Animal Ethics Committee of the Harbin Veterinary Research Institute of the Chinese Academy of Agricultural Sciences (200811-03). Six-week-old specific pathogen-free BALB/c mice (Vital River, Beijing, China) were divided into four groups, with five mice in each group. LL-37 (10 mg/kg), Ply2660 (16 mg/kg), a combination of LL-37 (10 mg/kg) and Ply2660 (16 mg/kg), or PBS as control was injected intraperitoneally into mice. The mice were weighed every 24 h for 14 days. Then, the mice were euthanized, and the organs were collected for observation of gross lesions change.
Combined therapy in the murine model of peritoneal septicemia
Six-week-old specific pathogen-free BALB/c mice (Vital River, Beijing, China) were injected intraperitoneally with 8 × 107 CFU of E. faecalis strain V583 suspended in 100 μl of BHI broth with 6% mucin. The treatment experiment was performed 1 h after the E. faecalis challenge. The infected mice were divided into four groups, with five mice in each group. LL-37 (10 mg/kg), Ply2660 (16 mg/kg), a combination of LL-37 (10 mg/kg) and Ply2660 (16 mg/kg), or PBS was injected intraperitoneally into mice. The mice were euthanized after 24-h treatment, and lung, liver, and kidney of each mouse were harvested, weighed, homogenized, and plated on agar for CFU counting. For histopathological analysis, lung, liver, and kidney samples were fixed in 4% formalin. After paraffin embedding, 4-μm tissue sections were stained with H&E according to the standard protocol and examined by light microscopy. Pathological scores based on the severity of hemorrhages and inflammation were respectively assigned as follows: normal (score = 0), minimal (<5% of focal areas; score = 1), mild (5–10% of focal areas; score = 2), moderate(11–30% of focal areas; score = 3), or severe (>30% of focal areas; score = 4). To determine the efficacy of LL-37 and/or Ply2660 on the survival rate of mice, an additional experiment was performed by injecting intraperitoneally a high dose (1.8 × 109 CFU) of E. faecalis V583, and the following treatment protocol was the same as before, but with 12 mice in each group. The survival rate for each experimental group was monitored every 6 h for the first 24 h and then every 12 h for 7 days.
Statistical analysis
Statistical analysis was conducted and graphs were generated using GraphPad Prism version 9.0 (GraphPad Software). The number of replicates is given in the respective figure legends. Statistical significance was analyzed using one-way analysis of variance (ANOVA), two-way ANOVA, Brown–Forsythe and Welch ANOVA, or unpaired t-tests. P-values of less than 0.05 were considered to be statistically significant.
Data availability
All data supporting the findings of this study are included in the article and its Supplementary file. Additional data are available from the corresponding authors upon request.
References
Cattoir, V. The multifaceted lifestyle of enterococci: genetic diversity, ecology and risks for public health. Curr. Opin. Microbiol. 65, 73–80 (2022).
Byappanahalli, M. N., Nevers, M. B., Korajkic, A., Staley, Z. R. & Harwood, V. J. Enterococci in the environment. Microbiol. Mol. Biol. Rev. 76, 685–706 (2012).
Guzman Prieto, A. M. et al. Global emergence and dissemination of enterococci as nosocomial pathogens: attack of the clones? Front. Microbiol. 7, 788 (2016).
Garcia-Solache, M. & Rice, L. B. The Enterococcus: a model of adaptability to its environment. Clin. Microbiol. Rev. 32, e00058–18 (2019).
van Harten, R. M., Willems, R. J. L., Martin, N. I. & Hendrickx, A. P. A. Multidrug-resistant enterococcal infections: new compounds, novel antimicrobial therapies? Trends Microbiol. 25, 467–479 (2017).
Torres, C. et al. Antimicrobial resistance in Enterococcus spp. of animal origin. Microbiol. Spectr. 6, 4 (2018).
Ayobami, O., Willrich, N., Reuss, A., Eckmanns, T. & Markwart, R. The ongoing challenge of vancomycin-resistant Enterococcus faecium and Enterococcus faecalis in Europe: an epidemiological analysis of bloodstream infections. Emerg. Microbes Infect. 9, 1180–1193 (2020).
Stewart, P. S. & Costerton, J. W. Antibiotic resistance of bacteria in biofilms. Lancet 358, 135–138 (2001).
Sauer, K. et al. The biofilm life cycle: expanding the conceptual model of biofilm formation. Nat. Rev. Microbiol. 20, 608–620 (2022).
Mohamed, J. A. & Huang, D. B. Biofilm formation by enterococci. J. Med. Microbiol. 56, 1581–1588 (2007).
Jefferson, K. K. What drives bacteria to produce a biofilm? FEMS Microbiol. Lett. 236, 163–173 (2004).
Hall, C. W. & Mah, T. F. Molecular mechanisms of biofilm-based antibiotic resistance and tolerance in pathogenic bacteria. FEMS Microbiol. Rev. 41, 276–301 (2017).
Ch’ng, J. H., Chong, K. K. L., Lam, L. N., Wong, J. J. & Kline, K. A. Biofilm-associated infection by enterococci. Nat. Rev. Microbiol. 17, 82–94 (2019).
Ciofu, O., Moser, C., Jensen, P. O. & Hoiby, N. Tolerance and resistance of microbial biofilms. Nat. Rev. Microbiol. 20, 621–635 (2022).
Dupre, I., Zanetti, S., Schito, A. M., Fadda, G. & Sechi, L. A. Incidence of virulence determinants in clinical Enterococcus faecium and Enterococcus faecalis isolates collected in Sardinia (Italy). J. Med. Microbiol. 52, 491–498 (2003).
Mohamed, J. A., Huang, W., Nallapareddy, S. R., Teng, F. & Murray, B. E. Influence of origin of isolates, especially endocarditis isolates, and various genes on biofilm formation by Enterococcus faecalis. Infect. Immun. 72, 3658–3663 (2004).
Zheng, J. X. et al. Characterization of biofilm formation by Enterococcus faecalis isolates derived from urinary tract infections in China. J. Med. Microbiol. 67, 60–67 (2018).
Seno, Y., Kariyama, R., Mitsuhata, R., Monden, K. & Kumon, H. Clinical implications of biofilm formation by Enterococcus faecalis in the urinary tract. Acta Med. Okayama 59, 79–87 (2005).
Kaviar, V. H. et al. Survey on phenotypic resistance in Enterococcus faecalis: comparison between the expression of biofilm-associated genes in Enterococcus faecalis persister and non-persister cells. Mol. Biol. Rep. 49, 971–979 (2022).
Pachon-Ibanez, M. E., Smani, Y., Pachon, J. & Sanchez-Cespedes, J. Perspectives for clinical use of engineered human host defense antimicrobial peptides. FEMS Microbiol. Rev. 41, 323–342 (2017).
Sorensen, O. E. et al. Human cathelicidin, hCAP-18, is processed to the antimicrobial peptide LL-37 by extracellular cleavage with proteinase 3. Blood 97, 3951–3959 (2001).
Hancock, R. E., Haney, E. F. & Gill, E. E. The immunology of host defence peptides: beyond antimicrobial activity. Nat. Rev. Immunol. 16, 321–334 (2016).
Lazzaro, B. P., Zasloff, M. & Rolff, J. Antimicrobial peptides: application informed by evolution. Science 368, eaau5480 (2020).
Hilchie, A. L., Wuerth, K. & Hancock, R. E. Immune modulation by multifaceted cationic host defense (antimicrobial) peptides. Nat. Chem. Biol. 9, 761–768 (2013).
Yu, X. et al. LL-37 inhibits LPS-induced inflammation and stimulates the osteogenic differentiation of BMSCs via P2X7 receptor and MAPK signaling pathway. Exp. Cell Res. 372, 178–187 (2018).
Yang, B. et al. Significance of LL-37 on immunomodulation and disease outcome. Biomed. Res. Int. 2020, 8349712 (2020).
Rodriguez-Rubio, L. et al. Phage lytic proteins: biotechnological applications beyond clinical antimicrobials. Crit. Rev. Biotechnol. 36, 542–552 (2016).
Mondal, S. I., Draper, L. A., Ross, R. P. & Hill, C. Bacteriophage endolysins as a potential weapon to combat Clostridioides difficile infection. Gut Microbes 12, 1813533 (2020).
Yoong, P., Schuch, R., Nelson, D. & Fischetti, V. A. Identification of a broadly active phage lytic enzyme with lethal activity against antibiotic-resistant Enterococcus faecalis and Enterococcus faecium. J. Bacteriol. 186, 4808–4812 (2004).
Diez-Martinez, R. et al. Improving the lethal effect of Cpl-7, a pneumococcal phage lysozyme with broad bactericidal activity, by inverting the net charge of its cell wall-binding module. Antimicrob. Agents Chemother. 57, 5355–5365 (2013).
Yang, H. et al. A chimeolysin with extended-spectrum streptococcal host range found by an induced lysis-based rapid screening method. Sci. Rep. 5, 17257 (2015).
Rohrig, C. et al. Targeting hidden pathogens: cell-penetrating enzybiotics eradicate intracellular drug-resistant Staphylococcus aureus. mBio 11, e00209-20 (2020).
Nithya, S. et al. Preparation, characterization and efficacy of lysostaphin-chitosan gel against Staphylococcus aureus. Int. J. Biol. Macromol. 110, 157–166 (2018).
Rios, A. C. et al. Alternatives to overcoming bacterial resistances: state-of-the-art. Microbiol. Res. 191, 51–80 (2016).
Lusiak-Szelachowska, M., Weber-Dabrowska, B. & Gorski, A. Bacteriophages and lysins in biofilm control. Virol. Sin. 35, 125–133 (2020).
Sharma, U., Vipra, A. & Channabasappa, S. Phage-derived lysins as potential agents for eradicating biofilms and persisters. Drug Discov. Today 23, 848–856 (2018).
Sass, P. & Bierbaum, G. Lytic activity of recombinant bacteriophage phi11 and phi12 endolysins on whole cells and biofilms of Staphylococcus aureus. Appl. Environ. Microbiol. 73, 347–352 (2007).
Mirski, T., Lidia, M., Nakonieczna, A. & Gryko, R. Bacteriophages, phage endolysins and antimicrobial peptides: the possibilities for their common use to combat infections and in the design of new drugs. Ann. Agric. Environ. Med. 26, 203–209 (2019).
Xie, F. et al. Differential abilities of mammalian cathelicidins to inhibit bacterial biofilm formation and promote multifaceted immune functions of neutrophils. Int. J. Mol. Sci. 21, 1871 (2020).
Hancock, L. E. & Perego, M. The Enterococcus faecalis fsr two-component system controls biofilm development through production of gelatinase. J. Bacteriol. 186, 5629–5639 (2004).
Giacobbe, D. R. et al. Enterococcal bloodstream infections in critically ill patients with COVID-19: a case series. Ann. Med. 53, 1779–1786 (2021).
Ramos-Martinez, A. et al. Hospital-acquired infective endocarditis during Covid-19 pandemic. Infect. Prev. Pract. 2, 100080 (2020).
Marshall, S. H., Donskey, C. J., Hutton-Thomas, R., Salata, R. A. & Rice, L. B. Gene dosage and linezolid resistance in Enterococcus faecium and Enterococcus faecalis. Antimicrob. Agents Chemother. 46, 3334–3336 (2002).
Munoz-Price, L. S., Lolans, K. & Quinn, J. P. Emergence of resistance to daptomycin during treatment of vancomycin-resistant Enterococcus faecalis infection. Clin. Infect. Dis. 41, 565–566 (2005).
Kumar, S., Mollo, A., Kahne, D. & Ruiz, N. The bacterial cell wall: from lipid II flipping to polymerization. Chem. Rev. 122, 8884–8910 (2022).
Gu, J., Xi, H., Cheng, M. & Han, W. Phage-derived lysins as therapeutic agents against multidrug-resistant Enterococcus faecalis. Future Microbiol. 13, 275–278 (2018).
Zhang, W. et al. Characterization of Enterococcus faecalis phage IME-EF1 and its endolysin. PLoS ONE 8, e80435 (2013).
Uchiyama, J. et al. Characterization of lytic enzyme open reading frame 9 (ORF9) derived from Enterococcus faecalis bacteriophage phiEF24C. Appl. Environ. Microbiol. 77, 580–585 (2011).
Cheng, M. et al. Endolysin LysEF-P10 shows potential as an alternative treatment strategy for multidrug-resistant Enterococcus faecalis infections. Sci. Rep. 7, 10164 (2017).
Yang, H., Singh, M., Kim, S. J. & Schaefer, J. Characterization of the tertiary structure of the peptidoglycan of Enterococcus faecalis. Biochim. Biophys. Acta Biomembr. 1859, 2171–2180 (2017).
Mainardi, J. L. et al. Unexpected inhibition of peptidoglycan LD-transpeptidase from Enterococcus faecium by the beta-lactam imipenem. J. Biol. Chem. 282, 30414–30422 (2007).
Bellais, S. et al. Aslfm, the D-aspartate ligase responsible for the addition of D-aspartic acid onto the peptidoglycan precursor of Enterococcus faecium. J. Biol. Chem. 281, 11586–11594 (2006).
Bateman, A. & Rawlings, N. D. The CHAP domain: a large family of amidases including GSP amidase and peptidoglycan hydrolases. Trends Biochem. Sci. 28, 234–237 (2003).
Gebhard, S. et al. Identification and characterization of a bacitracin resistance network in Enterococcus faecalis. Antimicrob. Agents Chemother. 58, 1425–1433 (2014).
Schmidtchen, A., Frick, I. M., Andersson, E., Tapper, H. & Bjorck, L. Proteinases of common pathogenic bacteria degrade and inactivate the antibacterial peptide LL-37. Mol. Microbiol. 46, 157–168 (2002).
LaRock, C. N. et al. Group A streptococcal M1 protein sequesters cathelicidin to evade innate immune killing. Cell Host Microbe 18, 471–477 (2015).
Khalifa, L. et al. Targeting Enterococcus faecalis biofilms with phage therapy. Appl. Environ. Microbiol. 81, 2696–2705 (2015).
Khalifa, L. et al. Phage therapy against Enterococcus faecalis in dental root canals. J. Oral Microbiol. 8, 32157 (2016).
Yang, D. et al. Characterization of a lytic bacteriophage vB_EfaS_PHB08 harboring endolysin Lys08 against Enterococcus faecalis biofilms. Microorganisms 8, 1332 (2020).
Zhang, H. et al. Bacteriophage phiEf11 ORF28 endolysin, a multifunctional lytic enzyme with properties distinct from all other identified Enterococcus faecalis phage endolysins. Appl. Environ. Microbiol. 85, e00555–19 (2019).
Shen, Y., Koller, T., Kreikemeyer, B. & Nelson, D. C. Rapid degradation of Streptococcus pyogenes biofilms by PlyC, a bacteriophage-encoded endolysin. J. Antimicrob. Chemother. 68, 1818–1824 (2013).
Tyers, M. & Wright, G. D. Drug combinations: a strategy to extend the life of antibiotics in the 21st century. Nat. Rev. Microbiol. 17, 141–155 (2019).
Gouveia, A. et al. Synthetic antimicrobial peptides as enhancers of the bacteriolytic action of staphylococcal phage endolysins. Sci. Rep. 12, 1245 (2022).
Ghosh, C., Sarkar, P., Issa, R. & Haldar, J. Alternatives to conventional antibiotics in the era of antimicrobial resistance. Trends Microbiol. 27, 323–338 (2019).
Swenson, J. M. et al. Molecular characterization and multilaboratory evaluation of Enterococcus faecalis ATCC 51299 for quality control of screening tests for vancomycin and high-level aminoglycoside resistance in enterococci. J. Clin. Microbiol. 33, 3019–3021 (1995).
Paulsen, I. T. et al. Role of mobile DNA in the evolution of vancomycin-resistant Enterococcus faecalis. Science 299, 2071–2074 (2003).
Yang, W. et al. Characterization of a novel RepA_N-family plasmid harbouring the phenicol-oxazolidinone resistance gene optrA in Enterococcus faecalis ST16 high-risk clone of goat origin. Vet. Microbiol. 266, 109340 (2022).
Berman, H. M. et al. The Protein Data Bank. Nucleic Acids Res. 28, 235–242 (2000).
Letunic, I., Khedkar, S. & Bork, P. SMART: recent updates, new developments and status in 2020. Nucleic Acids Res. 49, D458–D460 (2021).
Bienert, S. et al. The SWISS-MODEL Repository—new features and functionality. Nucleic Acids Res. 45, D313–D319 (2017).
Hecht, D. W. et al. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically. Clinical and Laboratory Standards Institute M07-A9 32 (CLSI, 2012).
Tan, F. et al. Bactericidal and anti-biofilm activity of the retinoid compound CD437 against Enterococcus faecalis. Front. Microbiol. 10, 2301 (2019).
Acknowledgements
This research was supported by grants from the National Natural Science Foundation of China (31873016), the Natural Science Foundation of Heilongjiang Province of China (YQ2019C031), and the German Federal Ministry of Education and Research (BMBF) under project number 01KI2009D as part of the Research Network Zoonotic Infectious Diseases. We thank Dr. S. Wang for technical assistance with the SEM experiments. We also thank Dr. Z. Zhang for technical assistance with the histopathological analysis.
Author information
Authors and Affiliations
Contributions
F.X., S.S., S.G.L., and W.J.Z. conceived and designed the experiments. H.H.Z., X.Y.Z., S.Y.L., and J.W. performed the experiments. H.H.Z., X.Y.Z., Y.Z., and F.X. analyzed the data. F.X., S.S., and H.H.Z. wrote the paper with input from all co-authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, H., Zhang, X., Liang, S. et al. Bactericidal synergism between phage endolysin Ply2660 and cathelicidin LL-37 against vancomycin-resistant Enterococcus faecalis biofilms. npj Biofilms Microbiomes 9, 16 (2023). https://doi.org/10.1038/s41522-023-00385-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41522-023-00385-5
- Springer Nature Limited
This article is cited by
-
LysSYL: a broad-spectrum phage endolysin targeting Staphylococcus species and eradicating S. aureus biofilms
Microbial Cell Factories (2024)
-
Repurposing fusidic acid as an antimicrobial against enterococci with a low probability of resistance development
International Microbiology (2024)