Abstract
Olanzapine is a second-generation anti-psychotic drug used to prevent neuroinflammation in patients with schizophrenia. However, the long-term administration of olanzapine leads to insulin resistance (IR); the mechanisms of this effect remains poorly understood. Using cellular and rodent models of IR induced by olanzapine, we found that chronic olanzapine treatment induces differential inflammatory cytokine reactions in peripheral adipose and the central nervous system. Long-term treatment of olanzapine caused metabolic symptoms, including IR, by markedly elevating the plasma levels of pro-inflammatory cytokines, including IL-1ß, IL-6, IL-8 and TNFα; these findings are consistent with observations from schizophrenia patients chronically treated with olanzapine. Our observations of differential inflammatory cytokine responses in white adipose tissues from the prefrontal cortex in the brain indicated cell type-specific effects of the drug. These cytokines induced IR by activating NF-kB through the suppression of IkBα. Functional blockade of the components p50/p65 of NF-kB rescued olanzapine-induced IR in NIH-3T3 L1-derived adipocytes. Our findings demonstrate that olanzapine induces inflammatory cytokine reactions in peripheral tissues without adversely affecting the central nervous system and suggest that chronic olanzapine treatment of schizophrenia patients may cause inflammation-mediated IR with minimal or no adverse effects in the brain.
Similar content being viewed by others
Introduction
Schizophrenia is a common mental illness that causes obstacles in thinking, emotion and behavior and is characterized by incongruity between mental activities and the environment1,2. This severe psychosis has unknown causes with more than 1% incidence3 and has a lifelong impact on patients from its onset in young adulthood4,5. Schizophrenia seriously impacts patients’ cognitive, daily life and social functions, which impose many problems and burdens on patients’ families, community and society6. Schizophrenia was misunderstood for centuries, and there was no modern treatment for schizophrenia until the 1950s7.
The second generation antipsychotics (SGAs) are not limited to the blocking of dopamine D2 receptors; instead, they have a dual blocking effect on the dopamine D2 receptor and 5-hydroxytryptamine-2 (5HT2)3,8. Olanzapine, one of the most widely used SGAs, is effective for both the positive and negative symptoms of schizophrenia. Since 1996, olanzapine has effectively improved the qualities of patients’ lives and the mental aspects of the pathology with only mild to moderate sedation9,10. Due to its higher clinical efficacy and decreased EPS, olanzapine has been globally used in the treatment of other mental illnesses, such as bipolar disorder and major depression disorders (MDD)8,11,12.
Recent clinical studies and reviews have indicated that chronic olanzapine treatment is often associated with severe metabolic side effects, such as obesity, dyslipidemia and insulin resistance (IR), which increase the risk of type 2 diabetes, cardiovascular disease and noncompliance in schizophrenia patients13,14,15,16,17,18,19. However, the mechanisms that underlie chronic olanzapine-induced IR remain debatable, which, in turn, largely restrict olanzapine as a maintenance treatment against severe schizophrenia20,21.
Studies suggest that olanzapine binds with the neurotransmitter receptors H1 and M3 in the hypothalamus, which increases food intake and body weight leading to IR22,23,24,25. However, more recent clinical observations have indicated that chronic olanzapine treatment caused metabolic abnormalities and IR without weight gain26,27,28,29. These studies found that these receptors were also abundantly distributed in peripheral tissues, such as the pancreas and liver. It was stated that the acute administration of olanzapine could induce IR through increasing hepatic glucose production, decreasing glucose uptake, and rapidly inducing adverse metabolic reactions even before weight gain occurred.
Recent studies have proposed IR as an inflammatory disease30. Inflammation could activate serine but not threonine phosphorylation of the insulin receptor substrate (IRS), prevent PI3K activity and impair insulin signal transduction via dissociation of IRS-PI3K formation31,32. Consequently, serine phosphorylation could inhibit the translocation of glucose transporter 4(GLUT-4) to the plasma membrane and the uptake of glucose into adipocytes and muscle resulting in IR33. Numerous clinical and animal studies have shown that brain inflammation is closely related to schizophrenia pathophysiology34,35,36,37. More interestingly, olanzapine could prevent inflammatory mediation by reducing glial activity in primary glia cells cultured from rat newborn brains38,39. However, female rats that received olanzapine treatment had elevated plasma levels of IL-8 and IL-1β and increased macrophage infiltration in white adipose tissue in the peripheral system. Given that olanzapine is reported to induce the production and release of inflammatory factors from peripheral adipose tissue, we hypothesized that long-term olanzapine treatment induces IR by activating the inflammatory cytokine response in these tissues.
In the present study, proinflammatory factors were investigated in schizophrenia patients with long-term olanzapine treatment in different psychiatric hospitals. We then further explored the molecular mechanisms of olanzapine induced IR using peripheral adipose from animal models and cellular culture systems. Our results demonstrated the relationship between inflammatory cytokines and insulin resistance in clinical patients, olanzapine-treated mice and adipocytes. Moreover, our results demonstrated that long-term olanzapine application did not induce an inflammatory reaction in the central nervous system; however, it caused IR in adipose tissue via activation of the NF-κB inflammation cascades. The current study proposed new mechanisms underlying olanzapine induced IR and may provide alternative ways of modifying olanzapine therapy for schizophrenia patients.
Results
Schizophrenia Patients Developed IR after Long-term Olanzapine Maintenance Treatments
Clinical patients from different hospitals were enrolled in this study. The body weight, fasting blood glucose and insulin levels were measured, and the insulin resistance index was calculated. To fulfill our investigation purpose, we selected 14 patients with less or no insulin index change compared to the average levels in the normal subjects, grouped as OS, and 14 additional patients with a significantly higher insulin index, referred to as OR (Table 1). Compared with OS, the patients in the OR group had significantly increased body weight, fasting blood glucose and insulin levels, and the HOMA-IR significantly increased, which indicated an insulin resistance status (Table 1).
To determine whether inflammation is closely related to insulin resistance in OR patients, we collected plasma after long-term olanzapine treatments from both groups. ELISA experiments showed that the plasma levels of TNF-α, IL-6, IL-1β and IL-8 in the OR group were significantly higher than those in the OS group (Fig. 1A, p < 0.05). Linear regression statistical analyses demonstrated that the HOMA-IR index changes were closely correlated with these inflammatory factors (Supplemental Table 2), including TNF-α (Fig. 1B, r2 = 0.5104, p < 0.001), IL-6 (Fig. 1C, r2 = 0.3995, p < 0.001), IL-1β (Fig. 1D, r2 = 0.5407, p < 0.001), and IL-8 (Fig. 1E, r2 = 0.4508, p < 0.001).
Insulin resistance in patients increased along with levels of plasma inflammatory cytokines. Inflammatory cytokines were correlated to insulin resistance indexes. (A) Plasma TNF-α, IL-6, IL-1β and IL-8 levels in patients. (B) Correlation between TNF-α and HOMA-IR index. (C) Correlation between IL-6 and HOMA-IR index. (D) Correlation between IL-1β and HOMA-IR index. (E) Correlation between IL-8 and HOMA-IR index. OS, olanzapine sensitive; OR, olanzapine resistance. n = 14 per group. Student t-test was used for comparisons between OS and OR groups. The Pearson correlation coefficient scores were calculated among plasma TNF-α, IL-6, IL-1β and IL-8 levels and HOMA-IR index. Data are presented as mean ± SD. *p < 0.05.
Rodent Models with Chronic Olanzapine Treatment Mimic Inflammatory Reactions in Peripheral System but not in Central Nervous System
To further confirm whether long-term application of olanzapine induces inflammation, we tested this hypothesis in mouse and rat models. Following intraperitoneal injection of olanzapine, 10 mg/kg for 8 weeks, the fasting blood glucose and insulin were measured, and the IR index was calculated. Compared with the control group (CG group in mouse or BL in rat), the mice in the olanzapine treatment group (OL group in mice) did not exhibit a significant increase in the body weight; however, the rats in the olanzapine treatment (IR group in rats) had a significant increase in the body weight (Supplemental Table 1). The levels of fasting blood glucose and insulin and the IR index significantly increased for both the OL and IR groups. In the oral glucose tolerance test (OGTT analysis), the area under the blood glucose curve was significantly increased in the OL or IR group compared with the control group (Supplemental Table 1).
The levels of TNF-α, IL-6, IL-8 and IL-1β in the plasma and adipose tissue of the mice were detected by ELISA. The expressions of TNF-α, IL-6, IL-8 and IL-1β mRNA in the adipose tissue were detected by quantitative real-time PCR. Compared with the CG group, the plasma levels of TNF-α, IL-6, IL-1β and IL-8 in the OL group significantly increased (Fig. 2A, P < 0.05). The TNF-α, IL-6, IL-1β and IL-8 in the adipose tissue were also significantly increased (Fig. 2B, p < 0.05). Compared with the CG group, the expressions of TNF-α, IL-6, IL-8 and IL-1β mRNA in the adipose tissue of the OL group were also significantly increased (Fig. 2C, p < 0.05). Moreover, Pearson’s correlation analysis showed that all inflammatory factors in the plasma were correlated with the serum insulin levels (Supplemental Fig. 1a–d and Supplemental Table 3.).
Chronic olanzapine treatment altered inflammatory cytokines in mice. Inflammatory cytokines were correlated to IR. (A) Plasma levels of TNF-α, IL-6, IL-8 and IL-1β in mice. (B) Levels of TNF-α, IL-6, IL-8 and IL-1β in adipose tissue in mice. (C) Relative mRNA expression of TNF-α, IL-6, IL-8 and IL-1β in adipose tissue in mice. Student t-test was used for comparisons of inflammatory cytokines between mouse groups. Data are presented as mean ± SD. *p < 0.05.
Brain inflammation is closely related to schizophrenia pathophysiology, and olanzapine could prevent the neuroinflammation of schizophrenia brains in clinical studies32. Thus, we hypothesized that olanzapine may have distinct activities in peripheral adipose and central nervous systems. We detected several major inflammatory factors in chronic olanzapine-treated rat models. Compared to the age-matched control group, the ELISA quantitative data demonstrated that olanzapine could induce significant increases in inflammatory cytokines, including TNF-α, IL-6, and IL-1β, in the plasma and white adipose tissues (Fig. 3A–C). Interestingly, there were no differences in the levels of TNF-α, IL-6, and IL-1β in the prefrontal cortex (PFC) between the olanzapine-treated and age-matched rat brains. Our results suggested that olanzapine induced inflammatory gene overexpression in peripheral adipose tissues, but not in the central nervous system.
Chronic olanzapine treatment significantly triggered release of inflammatory cytokines in rat adipose tissue, but did not induce inflammation reactions in brains. (A) Levels (pg/ml) of TNF-α, IL-6 and IL-1β in rat plasma were detected using ELISA. (B) levels (pg/g) of TNF-α, IL-6 and IL-1β in rat white adipose tissue were tested using ELISA. (C) Levels (pg/g) of TNF-α, IL-6 and IL-1β in rat prefrontal cortex tissue (PFC) using ELISA. Student t-test was used for comparisons of inflammatory cytokines between mouse groups. Data are presented as mean ± SD. *p < 0.05.
Olanzapine Inhibited the Glucose Utilization of Adipocytes by Inducing IR via NF-κB Activity Activation
NF-κB plays a key role in initiating and regulating inflammatory responses1. NF-κB typically exists as homodimers or heterodimers, among which the p50/p65 dimer is the most widely distributed and has important physiological functions2. To determine the potential pathway of olanzapine induced IR through NF-kB cascades in white fat tissue, we first incubated 3T3-L1 adipocytes with a series of olanzapine concentrations (0, 1, 2, 5, or 10 µM) for 48 h to investigate the effects of olanzapine on insulin sensitivity and NF-κB activity. As shown in the left panel of Fig. 4A, 1 µM olanzapine had no significant effect on the insulin-stimulated glucose uptake or the NF-κB (p65) activity compared with the control group (Fig. 4A right panel). Olanzapine significantly inhibited insulin-stimulated glucose uptake, increased the NF-κB activity and decreased the IκBα protein expression at 5 µM (Fig. 4A right panel). When the concentration was increased to 10 µM, the effect of olanzapine did not further increase (Fig. 4A). These results show that olanzapine dose-dependently inhibits the action of insulin and increases the activity of NF-κB, and there are good correlations between the decrease of insulin action and the increase of NF-κB activity or the decreased expression levels of IkBa (Fig. 4B).
Olanzapine inhibited insulin-stimulated glucose utilization, induced NF-κB activity in a dose-dependent and time-dependent manner and did not inhibit cell survival. (A) Olanzapine dose-dependently inhibited insulin-stimulated glucose uptake and induced NF-κB activity. (B) Correlation between the decrease of insulin action and the increase of NF-κB activity. (C) Olanzapine inhibited insulin-stimulated glucose uptake over time and did not inhibit cell survival. Data in plot graphs are presented as mean ± SD. The Pearson correlation scores were calculated between p65 or IkBa expression and glucose uptake inhibitory ratio. One-way ANOVA statistical analyses, post hoc t-test, were performed for multiple comparisons. *p < 0.05.
To further investigate whether the effect of olanzapine is time dependent, we incubated 3T3-L1 adipocytes with 5 µM olanzapine for 0, 12, 24, 48 and 72 h. The results are shown in Fig. 4C; insulin-stimulated glucose uptake inhibited by olanzapine increased with time, which reached its maximum inhibition at 48 h. After incubation for 72 h, the inhibitory effect of olanzapine on insulin-stimulated glucose uptake did not increase significantly further. To rule out that long-term olanzapine treatment might disturb cell growth and survival, we conducted a CCK-8 experiment, which is an indicator of cell proliferation. The results showed that olanzapine 5 µM and 3T3-L1 adipocytes co-incubated for 48 h had no significant inhibitory effect on the survival of 3T3-L1 (Fig. 4C right panel). These results show that olanzapine inhibits insulin-stimulated glucose uptake by 3T3-L1 adipocytes over time, not because of the inhibition of cell survival.
Olanzapine Stimulated NF-κB Activity through Dissociating NF-kB - IkBα Complex
IκBα is a specific inhibitor of NF-κB40. At rest, IκBα binds to p65/p50 as an inactive complex in the cytoplasm; once activated, IκB kinase phosphorylates IκBα and dissociates it from NF-κB. Free NF-κB translocates into the nucleus and binds to DNA to activate the transcriptions of genes that encode inflammatory cytokines. To elucidate the effect of olanzapine on NF-κB activity, we specifically inhibited NF-κB using small interfering RNAs (p65 siRNA and IκBα siRNA). We compared the effects of olanzapine, p65 siRNA and IκBα siRNA on NF-κB activities. First, we transfected cells with IκBα siRNA and p65 siRNA, respectively (Supplemental Table 3). The mRNA and protein expressions of IκBα and p65 after transfection were detected by PCR and western blots. The results showed that p65siRNA could significantly knock-down p65 mRNA over 75% (Fig. 5A left panel) and substantially inhibited the protein expression to a 90% lower level (Fig. 5A right panel). Similarly, IκBα siRNA significantly inhibited the IκBα gene transcription close to 70% (Fig. 5B right panel), as well as the protein expression to 90% (Fig. 5B left panel).
siRNA transfection significantly inhibited protein and mRNA expression, and interfered with NF-κB activity. (A) Effect of p65 siRNA transfection on p65 protein and mRNA expression. (B) Effect of IκBα siRNA transfection on IκBαprotein and mRNA expression. (C) Effect of olanzapine (upper 6#; lower 3#), IκBα siRNA (upper 9#; lower 6#) and co-incubation of olanzapine and p65 siRNA (upper 8#; lower 5#) on NF-κB activity. Upper panel: lane 1, Negative controal without cellular extracts; lane 2, Positive control with nuclear extract; lane 3, Competition assays with cold NF-κB oligonucleotides; lane 4, Vector control without Control siRNA and olanzapine; lane 5, Control siRNA transfected; lane 6, olanzapine treatment; lane 7, Control siRNA transfected and olanzapine treatment; lane 8, p65 siRNA transfected and olanzapine treatment; lane 9, IκBα siRNA transfected. Lower panel: lane 1, Vector control without Control siRNA and olanzapine; lane 2, Control siRNA transfected; lane 3, olanzapine treatment; lane 4, Control siRNA transfected and olanzapine treatment; lane 5, p65 siRNA transfected and olanzapine treatment; lane 6, IκBα siRNA transfected.One-way ANOVA statistical analyses, post hoc t-test, were performed for multiple comparisons. Data are expressed as mean ± SD. *p < 0.05 compared with control group; #p < 0.05 compared with olanzapine group.
To investigate the direct effect of olanzapine on NF-κB activities, NF-κB binding to DNA was performed by EMSA; NIH 3T3-L1 derived adipocytes were treated with olanzapine, IκBα siRNA, or along with p65 siRNA, and EMSA was performed using the nucleoproteins extracted from these cells. The results demonstrated that both olanzapine and IκBα siRNA significantly increased the binding of NF-κB to nuclear DNAs, which suggests that it could substantially activate cytokine production compared with the control group (Fig. 5C upper panel, lanes 4–7 and 9, and lower panel). As expected, the results showed that p65 siRNA significantly inhibited olanzapine-induced NF-κB activity (Fig. 5C upper panel, lane 8, and lower panel).
IκBα Overexpression and p65 siRNA Rescued Insulin-stimulated Glucose Uptake and GLUT4 Membrane Transfer on Olanzapine-induced Adipocyte IR
To elucidate the role of NF-κB in olanzapine-induced IR, we transfected p65 siRNA into 3T3-L1 adipocytes. We also transfected IκBα siRNA into 3T3-L1 adipocytes to determine whether increasing the NF-κB expression could cause IR. As shown in Fig. 6A, olanzapine significantly inhibited insulin-stimulated glucose uptake by as much as 30.8% after incubation for 48 h. However, 3T3-L1 adipocytes transfected with p65 siRNA followed by olanzapine treatment prevented olanzapine-induced decreases in insulin-stimulated glucose uptake. In addition, 3T3-L1 adipocytes transfected with IκBα siRNA prevented insulin-stimulated glucose uptake by 25.4% (p < 0.05) compared with the control group.
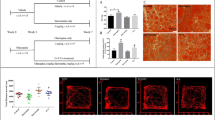
IκBα and p65 siRNA Rescued Insulin-stimulated Glucose Uptake and GLUT4 Membrane Translocation on Olanzapine-induced Adipocyte IR. (A) Effect of transfection reagents on insulin-stimulated glucose uptake (black bar) in olanzapine-treated adipocytes (olanzapine (lane 3), IκBα siRNA (lane 5), co-incubation of olanzapine and p65 siRNA (lane 6)). (B) Effect of transfection reagents (olanzapine (3# both left and right), IκBα siRNA (5#), co-incubation of olanzapine and p65 siRNA (6#) on insulin-stimulated GLUT4 translocation in olanzapine-treated adipocytes. (C) Effect of transfection reagents (olanzapine (3# both upper and lower panels), IκBα siRNA (5#), co-incubation of olanzapine and p65 siRNA (6#)) on p-IRS1 protein expression in olanzapine-treated adipocytes. (D) Effect of transfection reagents (olanzapine (3# both upper and lower panels), IκBα siRNA (5#), co-incubation of olanzapine and p65 siRNA (6#)) on p-AKT protein expression in olanzapine-treated adipocytes. lane 1, Control without Control siRNA and olanzapine; lane 2, Control siRNA transfected; lane 3, olanzapine treatment; lane 4, Control siRNA transfected and olanzapine treatment; lane 5, IκBα siRNA transfected; lane 6, p65 siRNA transefected and olanzapine treatment. One-way ANOVA statistical analyses, post hoc t-test, were performed for multiple comparisons of levels of plasma GLUT4, p-AKT, or p-IRS-1 among different treatments. Data in bar graphs are expressed as mean ± SD. *p < 0.05 compared with insulin group; #p < 0.05 compared with olanzapine and insulin treatment group.
Insulin regulates glucose uptake by inducing GLUT4 from intracellular vesicles to the cell surface in adipose tissue. Thus, we examined the expression of GLUT4 in 3T3-L1 adipocytes. As shown in Fig. 6B, the total GLUT4 expression of 3T3-L1 adipocytes was not significantly different in the different groups. However, olanzapine treatment and IκBα siRNA transfection significantly reduced insulin-induced GLUT4 translocation as assessed by GLUT4 contents on the cell membrane (Fig. 6B right panel: olanzapine, 75.3%, p < 0.05; IκBα siRNA, 56.5%, p < 0.05). P65 siRNA transfection blocked the inhibitory effect of olanzapine on insulin-induced GLUT4 membrane translocation.
To further elucidate the role of NF-κB in olanzapine-induced IR, we subsequently examined the effects of olanzapine and siRNA treatment on insulin signaling proteins. As shown in Fig. 6C (upper and lower panels) and Fig. 6D (upper and lower panels), olanzapine significantly increased IRS-1 phosphorylation by 2-fold (p < 0.05) and decreased Akt phosphorylation by 68.8% (p < 0.05), whereas p65 siRNA treatment largely blocked the effect of olanzapine on IRS-1 and Akt. Compared with the control group, IκBα siRNA transfection significantly increased IRS-1 phosphorylation by 1-fold (p < 0.05) and decreased Akt phosphorylation by 37.5% (p < 0.05).
Discussion
Olanzapine has been widely prescribed as a maintenance treatment for severe schizophrenia illness. Olanzapine is also widely used for the treatment of MDD and bipolar disorders; however, it is facing increasing noncompliance due to its reverse metabolic symptoms and insulin-resistance (IR), which are strong risk factors for type-2 diabetes. To uncover olanzapine induced IR, we investigated the effects of inflammatory cytokines in schizophrenia patients and demonstrated that inflammation is a key player of olanzapine induced IR using rodent mouse and rat models. We further explored the effects of olanzapine on NF-κB and insulin activities based on the 3T3-L1 adipocyte system. Our results indicated that olanzapine ignites inflammatory responses in peripheral adipose tissues by dissociating the NF-κB – IkBα complex to free NF-kB, which transduces into adipocyte nuclei to prompt the expression of inflammatory cytokines (Fig. 7). Furthermore, our results imply that activated NF-kB might induce the serine phosphorylation of insulin receptor substrate-1 (IRS-1) to downphosphorylate Akt and subsequently inhibits the translocation of GLUT4 to the adipose cell membrane and inhibits insulin utilization. We have also confirmed that the inhibition of NF-κB could significantly diminish IR and alleviate the inhibitory effect of olanzapine on insulin-stimulated glucose uptake in the adipocyte system. More interestingly, our current study, for the first time, showed that olanzapine induces no inflammatory response in the central nervous system, although it initiates strong inflammatory cytokine reactions in peripheral adipose tissue to induce IR.
The schematic diagram shows possibility of the NF-kB-IkBa complex contributes to olanzapine-induce IR. (A) IkBα binds to NF-Kb inhibiting NF-Kb transduction into adipose nuclei in physiological conditions. (B) Olanzapine may physically block the formation of NF-Kb-IKbα complex, leading to activate inflammatory reactions in adipose tissue. (C) Olanzapine may activate phosphorylation of IkBα and then free NF-Kb from their complex, leading to activate inflammatory reactions in adipose tissue.
Many cohort studies have shown that approximately 30% of diabetes or IR were induced by antipsychotics41,42. Schizophrenia patients from our clinical olanzapine long-term treatments showed a similar IR incidence and had significantly increased plasma glucose levels and HOMA-IR index, with a clear IR state that worsened glucose control in the OR patients compared to the OS or normal control subjects. Our clinical data proved that chronic olanzapine treatment induces IR and increases the risk of hyperglycemia, consistent with previous studies43,44. To clarify whether inflammation is a common player in IR, we examined the plasma inflammatory cytokine levels in the 14 OR and 14 OS patients and found that TNF-α, IL-6, IL-8 and IL-1β were significantly upregulated in the OR group compared with the OS group; these findings indicate an inflammatory response as an authentic indicator of IR (Table 1 and Fig. 1). Fountaine et al.45 also found that serum inflammatory factors, the levels of TNF-α and PAI-1, were significantly elevated in healthy male subjects after long-term application of olanzapine (5–10 mg/d)45. Major recent studies have suggested that inflammation could also be a mechanism for inducing IR46,47. However, for the first time, our results indicated that long-term olanzapine may induce hyperglycemia and IR by activating an inflammatory response in the peripheral adipose system.
We chose female rodent mice and rats to mimic the model of clinical long-term olanzapine treatment. Peripheral adipose tissue was comprehensively examined for pro-inflammatory factors, and our results clearly demonstrated that the plasma glucose and insulin levels were significantly increased in these established rodent models after 8 weeks of olanzapine treatment. The HOMA-IR index and the AUC in the OGTT were also significantly increased, which indicates that long-term olanzapine induced IR in the adipose system. Moreover, there was no significant difference in the body weight between the non-IR and IR animal groups, which indicates that long-term olanzapine treatments induced IR independent of weight gain in these rodent models (Supplemental Table 2 and Fig. 2). These data are consistent with recent clinical reports that weight-gain might not be a clue of olanzapine induced IR43.
NF-κB is a key regulator of the transcription of inflammatory cytokines. At rest, NF-κB binds to IκBα in the cytoplasm. After stimulation, phosphorylated IκBα degrades and dissociates with NF-κB. After dissociation, NF-κB enters the nucleus and binds to DNA, inducing the transcription of inflammatory cytokines32. In the current study, 3T3-L1 derived adipocytes treated with olanzapine showed that olanzapine concentration-dependently inhibited insulin-stimulated glucose uptake in the 1–5 µM range, consistent with the findings of Vestri et al.44. Our results also demonstrated the effect of olanzapine on increasing insulin and NF-κB in a time-dependent manner. Our results have shown that olanzapine significantly decreased the IκBα expression and increased the NF-κB expression and activity in 3T3-L1 adipocytes. Consistent with our findings, Sarvari et al. demonstrated that olanzapine significantly induced the expression of NF-κB and its target genes, such as TNF-α, IL-1β and IL-8, in human adipocytes in vitro48. These observations from cellular and molecular levels further confirmed that the IκBα- NF-κB complex pathway plays a pivotal role in olanzapine induced IR. These observations from cellular and molecular levels further confirmed that the IκBα- NF-κB complex pathway plays a pivotal role in olanzapine induced IR. Whether olanzapine physically blocks IkBa or activates IkBa to release free NF-kB leading to IR warrants additional studies.
To further confirm the IκBα- NF-κB complex pathway mechanism in IR, transfected 3T3-L1 adipocytes with p65 siRNA did show significantly downregulated NF-κB expression to relieve the IR status. The results showed that olanzapine and IκBα siRNA significantly induced NF-κB activity, inhibited insulin-stimulated glucose uptake and GLUT4 membrane translocation, and inhibited insulin signaling. The p65 siRNA can inhibit the activity of NF-κB to partially block the effect of olanzapine on NF-κB and IR. However, compared with IκBα siRNA transfection, olanzapine induced a more significant inhibition on insulin activity in the current study. Co-incubation with p65 siRNA did not fully rescue insulin-stimulated glucose uptake. These observations suggest that IR by olanzapine may have more signaling pathways other than NF-κB-dependent pathways.
These results indicate that long-term olanzapine-induced IR is related to the upregulation of inflammatory cytokines and inflammation, which suggests that NF-κB may be a potential target for the prevention and alleviation of olanzapine-induced IR. The most important finding of the current study is the first-time demonstration that olanzapine induced the expressions of inflammatory cytokines in the peripheral but not in the central nervous system. Although the increased adipose IL-6 levels were consistent with the findings from the Calevro29 group, the same animals showed cortical region-specific changes in the microglia density and activation state49, which indicates further investigation is required to link the microglial activation between peripheral and central cytokines after chronic olanzapine treatment. However, this current work could imply a new era to illuminate the mechanism by which olanzapine or other antipsychotic drugs may have differential effects on the central nervous system and peripheral adipose system.
Methods
Patient Recruitment Process and Sample Collection
This study recruited schizophrenia patients with long-term administration of olanzapine, whom were diagnosed positive, negative and cognitive impairment or emotional syndrome, according to the PNASS factor scores. Inclusion criteria: (1) age 18–60 years old;(2) no infectious disease, no chronic cardiovascular, digestive tract, endocrine, immune system and respiratory diseases within two weeks before blood sampling; (3) no family history of diabetes and no major liver or kidney disease; no bad habits, such as addiction and alcohol abuse; (4) nonpregnancy or lactation; (5) treatment with other mood stabilizers or other atypical antipsychotics (with olanzapine as the primary drug), but no antihypertensive drugs or typical antipsychotics; (6) informed consent; (7) patients treated mainly with olanzapine over 2 months and without hypoglycemic drugs. This clinical study was approved by the Tongji Medical College Ethics Committee of Huazhong University of Science and Technology (HUST).
We called clinical patients with long-term administration of olanzapine from different hospitals to conduct this study, which included measuring the body weight, fasting blood glucose, and insulin levels and calculating the insulin resistance index (HOMA-IR index). In this study, we mainly relied on experienced clinicians to determine the grouping of patients. In clinical practice, they assessed the patient’s metabolic status and insulin sensitivity based on changes in body weight and fasting blood glucose after long-term olanzapine treatment. Based on the HOMA-IR index values, the patients were divided into the OS group (the insulin resistance index has similar variations as the average levels in normal subjects, data not shown) and the OR group (the insulin resistance index is significantly higher than that of the average levels in normal subjects).
All experiments were performed according to the guidelines and regulations under HUST. The demographic and clinical details of the samples are provided in Table 1.
After overnight fasting, 10-ml blood samples were obtained from the patients and placed in a test tube that contained EDTAK2 anticoagulant. Following centrifugation at 3000 rpm for 10 min, the plasma was stored at −80 °C for later use.
Animals, Drug Treatment and Examination of Inflammatory Factors
Adult female Balb/c mice and Sprague Dawley rats (purchased from Beijing Huafu Kang Biotechnology Co., Ltd., animal license number: SCXK (Beijing) 2014–0004) were group-housed and maintained in the SPF animal room of the Animal Experiment Center of HUST with a 12-hour light/dark cycle. The animal use and procedures were in accordance with the HUST Animal Ethics Committee regulations and requirements. All experiments were performed under HUST animal guidelines and regulations.
The appropriate amount of olanzapine (TCI, Japan) was dissolved with 0.1 M hydrochloric acid solution, with 1 M sodium hydroxide solution to adjust the pH to 6.0. Olanzapine was intraperitoneally injected with dose justification as described and discussed in Wu, et al.50. Briefly, the injection doses were 10 mg/kg, injection volume of 10 ml/kg, with 0.1 M hydrochloric acid as the control. One week after the rodent animals were adaptively fed, they were randomly divided into two groups: the olanzapine treatment group and the control group. The olanzapine and control solvent were orally administered at 8:30 a.m. to 9 a.m. daily for 8 weeks.
After 8 weeks of administration, the body weight, fasting blood glucose and insulin levels were measured, and the Homeostasis model assessment insulin resistance (HOMA-IR) was calculated as shown in Supplemental Table S2. HOMA-IR = fasting blood glucose (mmol/L) * fasting insulin (mU/L) /22.5. The oral glucose tolerance test (OGTT) was performed after the end of the administration, and the area under the blood glucose curve was calculated. Orbital blood samples were obtained in heparin-added EP tubes, plasma was collected, and white adipose tissue was carefully separated. The prefrontal cortex of the rat brains from the OS and OR groups were dissected and immediately stored at −80 °C for later use.
Blood glucose was measured by a blood glucose detector. Insulin and inflammatory cytokines (TNF-α, IL-6, IL-8 and IL-1β) were measured using ELISA Kits (Neobioscience, China).
Adipocyte Cell Line and Differentiation Process
3T3-L1 fibroblasts (Shanghai Meixuan Biotechnology Co., Ltd.) were cultured in DMEM medium (which contained 4 mM L-glutamine, 4.5 g/L glucose and 10% fetal bovine serum) in a 5% CO2 incubator. After 2 days of fusion, the cells were stimulated for fat synthesis in DMEM medium that contained 25 mmol/L glucose, 0.5 mmol/L isobutylmethylxanthine, 1 mmol/L dexamethasone, 10 mg/ml insulin and 10% fetal bovine serum. After 3 days, the cells were changed using DMEM medium with 10 mg/ml insulin and 10% FBS. The medium was changed every 2 days during 10–14 day experiment, when 90–95% cells showed adipocyte phenotype.
Olanzapine Treatment of Adipocytes
After 3T3-L1 adipocytes (or transfected cells) were incubated with serum-free, high glucose, DMEM medium and olanzapine at the indicated concentrations were applied for the indicated time, the samples were incubated with 100 nM insulin or blank control solution without insulin for 30 min, and the supernatants were collected. The GOD-POD kit (Nanjing Jiancheng Bioengineering Institute, China) was used to determine the glucose content in the supernatants. The initial glucose content in the medium was subtracted from the glucose content in the supernatant to obtain the glucose content absorbed by the cells. The control cells were incubated with solvent only.
Examination of Influence on Adipocyte Growth
After the 3T3-L1 adipocytes were treated with olanzapine under the specified conditions, 10 µL CCK-8 solution was added, and the cells were incubated in an incubator at 37 °C for 2 h. The absorbance at 450 nm was measured using a microplate reader to calculate the effect of olanzapine on cell growth.
Gene Expression and Knock-down
IκBα siRNA and P50/p65 siRNA were synthesized by Shanghai Gemma (Ribobio, China). Briefly, prior to transfection, cells were harvested by trypsinization and collected, and the cell density was adjusted to 2 × 105/ml. Corresponding siRNAs were transfected into 3T3-L1 adipocytes using Lipofectamine rTM2000. The positive and vector siRNA were used to assess the transfection and knock-down efficiency. The levels of mRNA and protein expression of the target genes were detected after 48 hours.
Western Blotting Analyses
All cell lysates were collected via low-speed centrifugation. Briefly, cells were incubated ice-cooled lysis buffer for 30 minutes, vortexed and extracted the protein via centrifugation; the protein concentration was determined using the BCA method. SDS-PAGE electrophoresis and western blotting procedures were performed. Inflammation activates serine but not threonine phosphorylation of the insulin receptor substrate (IRS-1). Thus, the specific rabbit anti serine p-IRS1 antibody was purchased and applied in the present study, Cat:#2385, CST, USA, 1:500; the other corresponding protein primary antibodies used in this study were as follows: p65, (Cat:#8242, CST, USA, 1:2000); IκBα, (Cat:ab32518, Abcam, England, 1:2000); GLUT4, (Cat:ab33780, Abcam, England, 1:1000); p-AKT, (Cat:#4060, CST, USA, 1:2000); and GAPDH, (Cat:ab37168, Abcam, England, 1:10000). All primary antibodies were raised from rabbits; thus, a secondary antibody (HRP-Goat anti Rabbit, Cat:AS1107, ASPEN, USA, 1:10000) was used for each western blot analysis. Gel imager detection was performed with an X-ray film reader (Kodak, Japan). A cell membrane GLUT4 assay using a membrane protein extraction kit was used to determine the GLUT4 protein expression.
Quantitative Real-Time PCR
Approximately 100 mg of mouse adipose tissue was obtained and extracted by Trizol extraction (15596–026, Invitrogen™). The extracted RNA was added to the reverse transcription reaction system for reverse transcription. The primers for TNF-α were 5′-TCCCCAAAGGGATGAGAAGTT-3′ and 5′-GAGGAGGTTGACTTTCTCCTGG-3′. The primers for IL-6 were 5′-CTGGGAAATCGTGGAAATGAG-3′ and 5′-AAGGACTCTGGCTTTGTCTTTCT-3′. The primers for IL-1β were 5′-GGGCCTCAAAGGAAAGAATCT-3′ and 5′-GAGGTGCTGATGTACCAGTTGG-3′. The primers for IL-8 were 5′-GGCCCAATTACTAACAGGTTCC-3′ and 5′-TGACTTCACTGGAGTCCCGTAG-3′. The primers for GAPDH were 5′-TGAAGGGTGGAGCCAAAAG-3′ and 5′-AGTCTTCTGGGTGGCAGTGAT-3′. Real-time PCR was performed on a StepOne™ Real-Time PCR instrument using the SYBR® Premix Ex Taq™ kit (RR047A, TaKaRa, Japan). The calculation formula was as follows: ΔCt = Ct value of the target gene - Ct value of the reference gene; ΔΔCt = ΔCt of control group - ΔCt of the experimental group; the relative expression value of the target gene in the sample of the experimental group is 2ΔΔCt.
Electrophoretic Mobility Shift Assay
Following the cell intervention experiment, the nucleoprotein was extracted, and the protein concentration was determined with the purchased kit. Gel was prepared. After the gel was completely solidified, it was electrophoresed for 1 h at 100 v. After the pre-electrophoresis was completed, the precooled electrophoresis buffer was replaced, and 5 µl of 5x sample buffer was added to the sample mixture. Electrophoresis was then immediately performed at 150 v for 30–45 minutes. The positively charged nylon membrane was placed in a 0.5 x TBE for 10 minutes. After the electrophoresis was completed, the entire block of the sample was removed and transferred. After the membrane was completed, the membrane was marked and cross-linked under UV for 10 min. The membrane was blocked with blocking solution for 15 minutes. After being diluted 300-fold with blocking solution, the antibody was fully reacted with the membrane for 15 minutes. The membrane was subsequently washed and balanced. The image to the protein side of the membrane was taken. The film was scanned and analyzed with the AlphaEaseFC system. The oligos were AGTTGAGGGGACTTTCCCAGGC(5′−3′) and TCAACTCCCCTGAAAGGGTCCG(5′−3′).
Statistical Analyses
The PANSS scaling was used to measure the symptom severity of the patients with schizophrenia. The minimum scores for the positive, negative and general scales are 7, 7, and 16 and are used for the matched controls. Student’s t test was used to compare two groups for continuous variables. A Chi-square test was used to compare two groups for binary variables.
SPSS19.0 (SPSS Inc., IBM, USA) was used to process all animal and cell experimental data as mean ± SD. Analysis of variance (ANOVA) was used to compare multiple groups, and the least significant difference (LSD) was used for comparisons among groups. A logistic regression model was used for variables of each inflammatory factor with covariates of the HOMA-IR index. Pearson correlation scores were calculated for every inflammatory factor and the normalized HOMA-IR index values.
Statistical significance was set at p < 0.05. All experiments were repeated at least 3 times.
Ethical approval and informed consent
The use of all human samples and blood tissues in this study complied with the guidelines and regulations of the Tongji Medical College Ethics Committee of Huazhong University of Science and Technology (HUST). All experiments on human samples were approved by the Tongji Medical College Ethics Committee of HUST.
All experiments on rodents were approved by the HUST Animal Ethics Committee and were performed under the HUST animal guidelines and regulations.
Data Availability
All raw data, charts, and figures in this manuscript are available as electronic files uploaded on internet resources of scientific reports.
References
Arnold, S. E. Cognition and neuropathology in schizophrenia. Acta Psychiatr. Scand. Suppl. 395, 41–50 (1999).
Schnur, D. B., Friedman, S., Dorman, M., Redford, H. R. & Kesselman, M. Assessing the family environment of schizophrenic patients with multiple hospital admissions. Hosp. Community Psychiatry 37, 249–252 (1986).
Kapur, S. & Remington, G. Atypical antipsychotics: new directions and new challenges in the treatment of schizophrenia. Annual review of medicine 52, 503–517, https://doi.org/10.1146/annurev.med.52.1.503 (2001).
Stenstrom, A. D., Christiansen, E., Dehlholm-Lambertsen, B., Nohr-Jensen, P. & Bilenberg, N. Rising incidence rates of schizophrenia among children and adolescents. Ugeskr. Laeger. 172, 2131–2135 (2010).
Castagnini, A. & Foldager, L. Variations in incidence and age of onset of acute and transient psychotic disorders. Soc. Psychiatry Psychiatr. Epidemiol. 48, 1917–1922, https://doi.org/10.1007/s00127-013-0726-7 (2013).
Jenkins, J. H. & Schumacher, J. G. Family burden of schizophrenia and depressive illness. Specifying the effects of ethnicity, gender and social ecology. The British journal of psychiatry: the journal of mental science 174, 31–38 (1999).
Benjamin, J., Sadock, V. A. S. & Pedro, R. Kaplan and sadock’s comprehensive textbook of psychiatry. (Wolters Kluwer, 2009).
Fujimaki, K., Takahashi, T. & Morinobu, S. Association of typical versus atypical antipsychotics with symptoms and quality of life in schizophrenia. PloS one 7, e37087, https://doi.org/10.1371/journal.pone.0037087 (2012).
Spanarello, S., Beoni, A. M., Mina, G., Amantini, K. & Colotto, A. Analysis of differential clinical profiles of different antipsychotic molecules in the first psychotic episode: a retrospective study. Encephale 31, 692–697 (2005).
Caro, J. J., Ward, A., Levinton, C. & Robinson, K. The risk of diabetes during olanzapine use compared with risperidone use: a retrospective database analysis. The Journal of clinical psychiatry 63, 1135–1139 (2002).
Jairam, R., Prabhuswamy, M. & Dullur, P. Do we really know how to treat a child with bipolar disorder or one with severe mood dysregulation? Is there a magic bullet? Depression research and treatment 2012, 967302 (2012).
Goldberg, J. F. et al. The American society of clinical psychopharmacology survey of psychopharmacologists’ practice patterns for the treatment of mood disorders. Depression and anxiety 32, 605–613 (2015).
Drici, M. D. & Priori, S. Cardiovascular risks of atypical antipsychotic drug treatment. Pharmacoepidemiol. Drug Saf. 16, 882–890 (2007).
Asenjo Lobos, C. et al. Clozapine versus other atypical antipsychotics for schizophrenia. Cochrane Database Syst. Rev. 10, CD006633 (2010).
Nashed, M. G., Restivo, M. R. & Taylor, V. H. Olanzapine-induced weight gain in patients with bipolar I disorder: a meta-analysis. Prim. Care Companion CNS Disord. 13, 11r01174 (2011).
Harvey, R. C., James, A. C. & Shields, G. E. A Systematic Review and Network Meta-Analysis to Assess the Relative Efficacy of Antipsychotics for the Treatment of Positive and Negative Symptoms in Early-Onset Schizophrenia. CNS drugs 30, 27–39 (2016).
Tek, C. et al. Antipsychotic-induced weight gain in first-episode psychosis patients: a meta-analysis of differential effects of antipsychotic medications. Early intervention in psychiatry 10, 193–202 (2016).
Weiden, P. J., Mackell, J. A. & McDonnell, D. D. Obesity as a risk factor for antipsychotic noncompliance. Schizophrenia research 66, 51–57 (2004).
Velligan, D. et al. Methodological challenges in psychiatric treatment adherence research. Clin. Schizophr. Relat. Psychoses 4, 74–91 (2010).
Serretti, A., De Ronchi, D., Lorenzi, C. & Berardi, D. New antipsychotics and schizophrenia: a review on efficacy and side effects. Current medicinal chemistry 11, 343–358 (2004).
Daurignac, E., Leonard, K. E. & Dubovsky, S. L. Increased lean body mass as an early indicator of olanzapine-induced weight gain in healthy men. Int. Clin. Psychopharmacol. 30, 23–28 (2015).
Gunes, A., Melkersson, K. I., Scordo, M. G. & Dahl, M. L. Association between HTR2C and HTR2A polymorphisms and metabolic abnormalities in patients treated with olanzapine or clozapine. J. Clin. Psychopharmacol. 29, 65–68 (2009).
Melkersson, K. I., Gunes, A. & Dahl, M. L. Impact of serotonin receptor 2A gene haplotypes on C-peptide levels in clozapine- and olanzapine-treated patients. Hum. Psychopharmacol. 25, 347–352 (2010).
Poyurovsky, M. et al. Olanzapine-induced weight gain in patients with first-episode schizophrenia: a double-blind, placebo-controlled study of fluoxetine addition. Am. J. Psychiatry 159, 1058–1060 (2002).
Ma, X. et al. HTR2C polymorphisms, olanzapine-induced weight gain and antipsychotic-induced metabolic syndrome in schizophrenia patients: a meta-analysis. International journal of psychiatry in clinical practice 18, 229–242 (2014).
Kowalchuk, C. et al. In male rats, the ability of central insulin to suppress glucose production is impaired by olanzapine, whereas glucose uptake is left intact. Journal of psychiatry & neuroscience: JPN 42, 424–431 (2017).
Dayabandara, M. et al. Antipsychotic-associated weight gain: management strategies and impact on treatment adherence. Neuropsychiatr. Dis. Treat. 13, 2231–2241 (2017).
Palaniyappan, L. et al. Cortical folding defects as markers of poor treatment response in first-episode psychosis. JAMA psychiatry 70, 1031–1040 (2013).
Calevro, A. et al. Effects of chronic antipsychotic drug exposure on the expression of Translocator Protein and inflammatory markers in rat adipose tissue. Psychoneuroendocrinology 95, 28–33 (2018).
Schoiswohl, G. et al. Impact of Reduced ATGL-Mediated Adipocyte Lipolysis on Obesity-Associated Insulin Resistance and Inflammation in Male Mice. Endocrinology 156, 3610–3624 (2015).
Saltiel, A. R. & Kahn, C. R. Insulin signalling and the regulation of glucose and lipid metabolism. Nature 414, 799–806 (2001).
Leto, D. & Saltiel, A. R. Regulation of glucose transport by insulin: traffic control of GLUT4. Nat. Rev. Mol. Cell. Biol. 13, 383–396 (2012).
Yu, X. et al. Egr-1 decreases adipocyte insulin sensitivity by tilting PI3K/Akt and MAPK signal balance in mice. EMBO J. 30, 3754–3765 (2011).
De Picker, L. J., Morrens, M., Chance, S. A. & Boche, D. Microglia and brain plasticity in acute psychosis and schizophrenia illness course: a meta-review. Frontiers in psychiatry 8, 238 (2017).
MacDowell, K. S. et al. Risperidone normalizes increased inflammatory parameters and restores anti-inflammatory pathways in a model of neuroinflammation. Int. J. Neuropsychopharmacol. 16, 121–135 (2013).
Laskaris, L. E. et al. Microglial activation and progressive brain changes in schizophrenia. British journal of pharmacology 173, 666–680 (2016).
Limoa, E. et al. Electroconvulsive shock attenuated microgliosis and astrogliosis in the hippocampus and ameliorated schizophrenia-like behavior of Gunn rat. Journal of neuroinflammation 13, 230 (2016).
Valera, E., Ubhi, K., Mante, M., Rockenstein, E. & Masliah, E. Antidepressants reduce neuroinflammatory responses and astroglial alpha-synuclein accumulation in a transgenic mouse model of multiple system atrophy. Glia 62, 317–337 (2014).
Faour-Nmarne, C. & Azab, A. N. Effects of olanzapine on LPS-induced inflammation in rat primary glia cells. Innate immunity 22, 40–50 (2016).
Karin, M. & Ben-Neriah, Y. Phosphorylation meets ubiquitination: the control of NF-[kappa]B activity. Annu. Rev. Immunol. 18, 621–663 (2000).
Citrome, L. & Volavka, J. Consensus development conference on antipsychotic drugs and obesity and diabetes: response to consensus statement. J. Clin. Psychiatry 66, 1073–1074 (2005).
Rajkumar, A. P. et al. Endogenous and antipsychotic-related risks for diabetes mellitus in young people with schizophrenia: a danish population-based cohort study. Am. J. Psychiatry 174, 686–694 (2017).
Martins, P. J., Haas, M. & Obici, S. Central nervous system delivery of the antipsychotic olanzapine induces hepatic insulin resistance. Diabetes 59, 2418–2425 (2010).
Vestri, H. S., Maianu, L., Moellering, D. R. & Garvey, W. T. Atypical antipsychotic drugs directly impair insulin action in adipocytes: effects on glucose transport, lipogenesis, and antilipolysis. Neuropsychopharmacology: official publication of the American College of Neuropsychopharmacology 32, 765–772 (2007).
Fountaine, R. J. et al. Increased food intake and energy expenditure following administration of olanzapine to healthy men. Obesity 18, 1646–1651 (2010).
Keane, K. N., Cruzat, V. F., Carlessi, R., De Bittencourt, P. I. H. & Newsholme, P. Molecular events linking oxidative stress and inflammation to insulin resistance and β-cell dysfunction. Oxid. Med. Cell. Longev. 2015, 181643 (2015).
Khodabandehloo, H., Gorgani-Firuzjaee, S., Panahi, G. & Meshkani, R. Molecular and cellular mechanisms linking inflammation to insulin resistance and β-cell dysfunction. Transl. Res. 167, 228–256 (2016).
Sarvari, A. K., Vereb, Z., Uray, I. P., Fesus, L. & Balajthy, Z. Atypical antipsychotics induce both proinflammatory and adipogenic gene expression in human adipocytes in vitro. Biochemical and biophysical research communications 450, 1383–1389 (2014).
Cotel, M. C. et al. Microglial activation in the rat brain following chronic antipsychotic treatment at clinically relevant doses. Eur. Neuropsychopharmacol. 25, 2098–2107 (2015).
Wu, C. et al. An evaluation of the effects of the novel antipsychotic drug lurasidone on glucose tolerance and insulin resistance: a comparison with olanzapine. PloS one 9, e107116 (2014).
Acknowledgements
We thank Dr. Anil B Mukherjee for rewriting the abstract and Drs. Goutam Chandra and Guochang Fan for critical review of the manuscript and helpful suggestions. We also thank Dr. Chandra for proof-reading and editorial assistance in correcting and clarifying the entire manuscript. This work was supported by funds from the National Natural Science Foundation (No.: 81573509) granted to Weiyong Li and a Xinxiang Medical University endowment (No.: 505182) granted to Peng, S.
Author information
Authors and Affiliations
Contributions
Conception and design: Huqun Li, Weiyong Li, and Shiyong Peng. Design and performance in majority of experiments: Huqun Li, Shihong Li, Shouqing Liu, Yifan Lv, and Ni Yang. Composition of the Manuscript: Shiyong Peng, Huqun Li, Weiyong Li, and Zhongjian Zhang. Data analysis and interpretation: Huqun Li, Shihong Li, Shouqing Liu, Yifan Lv, Ni Yang, and Ya-Hui Deng. Collection and assembly of clinical data: Maosheng Fang, Yunxiang Huo, Ying Chen, and Taohua Sun. Manuscript writing: All authors, Final approval of manuscript: All authors
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, H., Peng, S., Li, S. et al. Chronic olanzapine administration causes metabolic syndrome through inflammatory cytokines in rodent models of insulin resistance. Sci Rep 9, 1582 (2019). https://doi.org/10.1038/s41598-018-36930-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-36930-y
- Springer Nature Limited
This article is cited by
-
Insulin effects on core neurotransmitter pathways involved in schizophrenia neurobiology: a meta-analysis of preclinical studies. Implications for the treatment
Molecular Psychiatry (2023)
-
Do proinflammatory cytokines play a role in clozapine-associated glycometabolism disorders?
Psychopharmacology (2021)
-
Olanzapine Induces Inflammation and Immune Response via Activating ER Stress in the Rat Prefrontal Cortex
Current Medical Science (2021)