Abstract
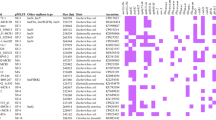
The emergence of the mobile colistin-resistance genes mcr-1 has attracted significant attention worldwide. This study aimed to investigate the genetic features of mcr-1-carrying plasmid among carbapenem-resistant Enterobacterales (CRE) isolates and the potential genetic basis governing transmission. Seventeen mcr-harboring isolates were analyzed based on whole genome sequencing using short-read and long-read platforms. All the mcr-1-carrying isolates could be conjugatively transferred into a recipient Escherichia coli UB1637. Among these 17 isolates, mcr-1 was located on diverse plasmid Inc types, consisting of IncX4 (11/17; 64.7%), IncI2 (4/17; 23.53%), and IncHI/IncN (2/17; 11.76%). Each of these exhibited remarkable similarity in the backbone set that is responsible for plasmid replication, maintenance, and transfer, with differences being in the upstream and downstream regions containing mcr-1. The IncHI/IncN type also carried other resistance genes (blaTEM-1B or blaTEM-135). The mcr-1-harboring IncX4 plasmids were carried in E. coli ST410 (7/11; 63.6%) and ST10 (1/11; 9.1%) and Klebsiella pneumoniae ST15 (1/11; 9.1%), ST336 (1/11; 9.1%), and ST340 (1/11; 9.1%). The IncI2-type plasmid was harbored in E. coli ST3052 (1/4; 25%) and ST1287 (1/4; 25%) and in K. pneumoniae ST336 (2/4; 50%), whereas IncHI/IncN were carried in E. coli ST6721 (1/2; 50%) and new ST (1/2; 50%). The diverse promiscuous plasmids may facilitate the spread of mcr-1 among commensal E. coli or K. pneumoniae strains in patients. These results can provide information for a surveillance system and infection control for dynamic tracing.
Similar content being viewed by others
Introduction
The global spread of carbapenem-resistant Enterobacterales (CRE) has become a leading public health concern due to the rapidly increasing prevalence of carbapenemase gene carriage by Enterobacterales, with most carbapenem resistance conferred by carbapenem-degrading enzymes (carbapenemase) such as K. pneumoniae carbapenemase (blaKPC), New Delhi metallo-β-lactamase (blaNDM), and OXA-48-like carbapenemase1,2.
The lack of accessible treatment has resulted in the use of colistin, an outmoded antibiotic, as a last-resort therapeutic drug for human infections by Gram-negative bacteria. The widespread use of colistin in humans and animals has led to the emergence of colistin resistance in Gram-negative bacteria, with rates of resistance continuously increasing3,4. A classic mechanism of colistin resistance is thought to be associated with chromosomal mediation5. The discovery of plasmid-mediated colistin resistance encoded by mcr genes revealed high prevalence in human and animal isolates harboring these genes and the transmission of mcr is of global concern6. Up to the present, 10 variants of mcr (mcr-1 through mcr-10) have been reported7,8. Of particular concern is the spread of mcr genes into CRE, which would create strains that are potentially pan-drug resistant. The coexistence of mcr and carbapenemase genes, such as blaNDM, blaOXA-48-like, and blaIMP, in CRE isolates has been described worldwide9,10,11,12.
The global prevalence of mcr genes revealed that mcr-1 (4917/5191; 94.7%) is a common gene and has a wider distribution than mcr-2 through to mcr-84. Human infections with CRE isolates carrying mcr-1 have been reported10,11,12,13,14 and the prevalence of mcr-1 has been increasing in Thailand13. The mcr-carrying plasmids identified consist of IncX4, IncI2, IncHI2, IncF, IncP, IncY, and ColE10-like ones, most of which are conjugative plasmid15.
Collectively, information regarding the genetic context of mcr-1 plasmid and its organization in the genome is still limited in Thailand. One study revealed the general characteristics of mcr-1 harboring CRE isolated from patients in Thailand13. However, genomic analysis has not yet determined insights to plasmidome in the CRE harboring mcr-1. Thus, this study aimed to determine the complete genomic sequences to provide insight into plasmidome and to compare plasmid harboring mcr-1- among CRE isolates from human patients in Thailand.
Materials and methods
Bacterial isolates
This study used 17 CRE carrying mcr-1 isolates, consisting of 12 isolates (E. coli = 8; K. pneumoniae = 4)) in a previous study13 and 5 isolates (E. coli = 4; K. pneumoniae = 1) sent by hospitals in Thailand for further confirmation by the Public Health Microbiological Laboratory of the Faculty of Public Health, Kasetsart University Chalermphrakiat Sakon Nakhon Province Campus under the Emerging Antimicrobial Resistant Bacterial Surveillance Program (EARB) during 2016–2019 (Table 1). The presence of mcr-1–mcr-916 and carbapenemase genes (blaIMP, blaKPC, blaNDM, and blaOXA‐48‐like)17 was confirmed in these CRE isolates using Multiplex polymerase chain reaction (PCR), as previously described.
Ethical approval
Ethical review and approval were not required because no human specimens or data were used in the current study.
Antimicrobial susceptibility testing
The minimal inhibitory concentration (MIC) of colistin was determined in 5 CRE carrying mcr-1 isolates using the broth microdilution method according to 2021 Clinical and Laboratory Standards Institute guidelines18. The broth microdilution method was conducted using cation-adjusted Mueller–Hinton broth (Becton, Dickinson and Company, Sparks, MD, USA). MIC values ≤ 2 µg/ml were interpreted as intermediate susceptibility, whereas an MIC of ≥ 4 µg/ml was considered resistant. Antimicrobial susceptibility to ampicillin, gentamicin, amikacin, amoxicillin/clavulanic acid, amoxicillin/sulbactam, pipercillin-tazobactam, trimethoprime/sulfamethoxazole, cefepime, cefotaxime, ciprofloxacin, levofloxacin, ertapenem, imipenem, meropenem, doripenem, ceftazidime, ceftriaxone, cefoxitin, and netilmicin was performed with a Vitek® 2 automated system (Clinical Microbiology Laboratory, Sakon Nakhon Hospital).
Conjugation assay
Conjugation assay was performed in all 17 mcr-1-carrying CRE isolates consisting of E. coli (n = 12) and K. pneumoniae (n = 5) isolates, as previously described19,20. The mcr-harboring CRE strains (donor) and streptomycin-resistant E. coli UB1637 (recipient) were mixed in a ratio of 1:25. The mixtures were collected and then plated on MacConkey agar containing streptomycin (3200 μg/ml) and colistin (4 μg/ml). The transconjugants harboring mcr genes were confirmed using PCR16.
Complete genome sequencing
Bacterial genomic DNA samples were extracted using ZymoBIOMICS DNA Kits (Zymo Research, CA, USA) according to manufacturer’s instructions. Only 12 isolates from the previous study were sequenced by Oxford Nanopore Technologies (ONT)13, while 5 isolates were sequenced using the ONT and Illumina platforms. Library preparation for ONT sequencing followed the rapid barcoding DNA sequencing protocol with the SQK-RBK004 kit without DNA size selection (to preserve the plasmid DNA) and the libraries were sequenced using a single R9.4.1/FLO-MIN106 flow cell on a MinION Mk1B sequencer. We base-called and demultiplexed the raw data using Guppy v3.4.5 (ONT), specifying the high-accuracy model (-c dna_r9.4.1_450bps_hac.cfg). The ONT adapters were trimmed using Porechop v0.2.4 (https://github.com/rrwick/Porechop). Quality control of ONT reads was undertaken using Nanoplot v1.28.1 (https://github.com/wdecoster/NanoPlot).
For the Illumina platform, the sequencing library was generated using a NEBNext Ultra II DNA Library Prep Kit for Illumina (New England Biolabs, UK), following the manufacturer’s recommendations. The genomic DNA was randomly fragmented to a size of 350 bp and the fragments were A-tailed and ligated with the adapter. Libraries were sequenced using the Illumina HiSeq platform with the 150 paired-end sequencing strategy. We applied Fastp v0.19.521 with default parameters for the quality filtering of Illumina reads. Adapters were trimmed using Skewer v0.2.222. The quality checking of Illumina reads was performed using FastQC v0.11.8 (https://www.bioinformatics.babraham.ac.uk/ projects/fastqc/). Hybrid assemblies with the ONT and Illumina data were performed using Unicycler v0.4.823 and the genome sequences of all 17 isolates were checked for quality using QUAST v5.0.224. Genome sequences were submitted to the NCBI Prokaryotic Genome Annotation Pipeline (PGAP v4.12) for annotation. The default parameters were used for all software unless otherwise specified.
Bioinformatics analysis
Identification of antimicrobial resistance genes was analyzed using ResFinder 4.125 and the Comprehensive Antibiotic Resistance Database (CARD)26. Determination of the mcr-1-carrying plasmid was carried out using PlasmidFinder27. Phylogrouping for E. coli and the KL type of K. pneumoniae were performed using ClermonTyping28 and Kaptive29, respectively. Multilocus sequence typing (MLST) analysis of mcr-1-carrying E. coli and K. pneumoniae was determined using MLST 2.030.
To search for the genetically closest relatives to the mcr-carrying isolates, a modular single genome analysis was conducted following the core genome multilocus sequence typing approach by BacWGSTdb 2.031. The genetically closest relatives were chosen for 5–10 strains based on small numbers of allelic differences with selection thresholds of 100–500, depending on the strains under current study. The phylogenetics of the mcr-carrying CRE isolates and the closest relatives selected from BacWGSTdb were conducted using a reference genome-based, single-nucleotide polymorphism (SNP) strategy with REALPHY32. The phylogenetic tree was visualized using the iTOL V4 software33. E. coli K12 substrain MG1655 (accession no. U00096) and K. pneumoniae WCHKP9G2 (accession no. NBYD01000091) were used as the reference sequences for SNP analysis. In addition, phylogenetic analysis of plasmid-harboring mcr-1 was conducted using the Mashtree program, following the program’s instructions34.
Accession number
The assembled genomic sequences were deposited under the BioProject accession number PRJNA525849. The accession numbers for each mcr-1-harboring isolate are provided in Table 1.
Results
Antimicrobial susceptibility of mcr-1-harboring CRE isolates
In a previous study, 4516 (64.5%) CRE were identified from 6996 multidrug-resistant isolates. Of these, 4235 (93.7%) isolates were classified as carbapenemase-producing Enterobacterales (CPE) and carried carbapenemase genes including blaNDM, blaOXA-48-like, blaIMP, or coexisting carbapenemase genes according to the modified carbapenem inactivation method (mCIM) and PCR results13. Of all the CPE isolates, 13 (0.3%) carried mcr genes13. That study did not detect mcr-1 in other species of Enterobacterales except E. coli and K. pneumoniae13. In the current study, five additional Enterobacterales isolates from the EARB program were included. Unfortunately, one isolate of the previous study was unrecovered. Therefore, a total of 17 isolates were conducted to their completed genome and further analysis.
PCR confirmed the presence of mcr-1 in all 17 isolates, with one isolate (no. 54715) coexisting with mcr-3. Five additional mcr-1-carrying isolates in the current study presented carbapenemase genes including blaNDM-1 in three isolates (strain nos. 2509, 2117, and V417), whereas in two isolates (strain nos. P24-5 and P36.8) the carbapenemase genes were not detected (Fig. 1). Only five isolates carrying mcr-1 isolates included in this study were determined for antimicrobial susceptibility because the other 12 CRE isolates had already been described elsewhere13. All 17 mcr-1-harboring E. coli (n = 12) and K. pneumoniae (n = 5) isolates were resistant to colistin (MIC values 4–16 µg/ml), ampicillin and ampicillin/sulbactam (Table 2). Fifteen isolates (88.24%) of the mcr-1-harboring strains were resistant to carbapenems. Among the five isolates carrying mcr-1 isolates included in this study, three were resistant to ampicillin, ampicillin/sulbactam, Piperacillin/tazobactam, cefepime, cefotaxime, cefoxitin, imipenem, meropenem, ertapenem, ciprofloxacin, and levofloxacin. Two mcr-1-carrying E. coli isolates (P24-5 and P36.8) were resistant only to ampicillin, ampicillin/sulbactam, gentamicin, levofloxacin, and ciprofloxacin whereas they were susceptible to the carbapenems (Table 2).
Agarose gel electrophoresis of PCR-amplified products of carbapenemase and mcr-1 genes from five mcr-1-carrying E. coli and K. pneumoniae isolates. Positive control of blaIMP (lane 1), blaOXA-48-like (lane 2), blaNDM (lane 3), blaKPC (lane 4), mcr-1 (lane 5), K. pneumoniae strain no. 2509 (lane 6), E. coli strain no. 2117 (lane 7), V417 (lane 8), P24-5 (lane 9), and P36.8 (lane 10), negative control (lane 11). A 100-bp DNA ladder is shown in lane M.
Conjugative transfer of the mcr-1 gene
As shown in Fig. 2 and Table 3, all 17 mcr-1-carrying CRE isolates could be conjugatively transferred into E. coli UB1637. One coexisted of mcr-1 and mcr-3 E. coli (isolate no. 54715), transferring both. Colistin resistance was also detected in 14 E. coli recipient (82.35%) with MIC values in the range 4–16 µg/ml, whereas the rest were susceptible (Table 3). This suggested that mcr-1 in all 17 CRE isolates carried on the conjugative plasmids.
Agarose gel electrophoresis of PCR-amplified products from the transconjugants E. coli UB1637. Conjugation assay was performed in mcr-1-carrying CRE isolates. The transconjugants were collected nine colonies in each sample and confirmed the mcr-1 gene using PCR. Positive control (lane 1), E. coli strain no. 58967 (lane 2–10), negative control (lane 11), E. coli strain no. 56511 (lane 12–20), negative control (lane 22). A 100-bp DNA ladder is shown in lane M.
Genomic characterization of mcr-harboring CRE isolates
Table 1 summarizes the antimicrobial-resistant genes in all 17 mcr-1 carrying isolates. Five additional mcr-1-carrying isolates in the current study presented an associated β-lactamase gene: blaCTX-M-15, blaCTX-M-55, blaSHV-106, blaCMY-2, blaTEM-1B, and blaTEM-135. Of these, three isolates were coexisting carbapenemase genes including blaNDM-1 (Table 1 and Fig. 1). Other antimicrobial-resistance genes in the five isolates are shown in Table 1. Finally, β-lactamase-encoding genes in mcr-carrying isolates were located on different plasmid replicon types: IncFIA, IncFIB, IncFII, IncC, or IncI1-I (Table 1).
Based on MLST analysis, we detected 4 different STs in five additional mcr-1 carrying isolates; ST410, ST15, ST6726, and new ST (Table 1). Clermont phylotyping of four mcr-harboring E. coli isolates showed phylogroups C (2/4; 50%), A (1/4; 25%), and Clade III (1/4; 25%) while eight E. coli isolates in the previous study revealed 5 phylogroup C and 2 and 1 for phylogroups A and D, respectively13. We concluded that the predominant phylogroup in all 17 isolates was C, accounting for 41.18% (7/17).
All 12 mcr-1-harboring E. coli isolates carried the virulence genes gad (glutamate decarboxylase) and terC (tellurium ion resistance protein). Five mcr-1-harboring K. pneumoniae isolates carried fyuA (siderophore receptor), iutA (ferric aerobactin receptor), and irp2 (iron regulatory protein), as shown in Fig. 3. An additional single K. pneumoniae isolate included in the current study was KL type 28, whereas 3 KL25 and 1 KL15 were detected in K. pneumoniae in the previous study13.
Phylogenetic tree based on single nucleotide polymorphisms (SNP) using the neighbor-joining method, sequence types (STs) and virulence gene patterns in E. coli. Virulence genes are represented by respective blue-colored shapes. The tree was visualized and annotated using Interactive Tree of Life (iToL).
The genetic relationships based on the SNPs phylogeny of these mcr-1-harboring isolates are shown in Fig. 3 and Fig. 4. E. coli strain no. 2117 was closely related with strains from China (accession no. CP035123.1). Isolate no. P36.8 was closely related with the reference strain K12 and clustered with P24-5 (new ST), as shown in Fig. 3. K. pneumoniae strain no. 2509 was closely related with the K. pneumoniae SIKP199 strain from Thailand (accession no. GCA_004833525.1) (Fig. 4).
Analysis of mcr-1-bearing plasmids
Three different plasmid replicon types were identified in the 17 mcr-1-harboring isolates (Figs. 5 and 6). The most frequent plasmid replicons were IncX4 (11/17; 64.7%), IncI2 (4/17; 23.53%), and IncHI2/IncN (2/17; 11.76%), respectively (Figs. 5 and 6). The sizes of the 11 IncX4 carrying mcr-1 plasmids were in the range 33,309–45,011 bp, whereas the 4 IncI2 carrying mcr-1 plasmids were in the range 60,960–67,526 bp. The 2 IncHI/IncN were 270,820 bp and 273,765 bp. As shown in Fig. 5, there was high similarity among the IncX4 plasmids, although some of had different positions of the mcr-1 gene (nos. 56511 and 59990). In contrast, IncI2 and IncHI2/IncN, each had mcr-1 positions. We found that IncX4-type plasmids were carried on E. coli STs 410 (7/11;63.6%) and ST10 (1/11; 9.1%) and on K. pneumoniae ST15 (1/11; 9.1%), ST336 (1/11; 9.1%), and ST340 (1/11; 9.1%). IncI2 was harbored in ST3052 (1/4;25%), ST1287 (1/4;25%) in E. coli and in K. pneumoniae ST336 (2/4; 50%), whereas IncHI/IncN were carried by E. coli ST6721 (1/2; 50%) and the new ST (1/2; 50%).
Alignment of plasmids carrying mcr-1 genes. Horizontal red arrows indicate location, size, direction of transcription, and orientation of open reading frames. The red color code indicates mcr-1. Homologous segments generated by a BLASTn comparison are shown as gray blocks that are connected across plasmids.
Figure 6 demonstrated diversity in the upstream and downstream coding sequences flanking mcr-1 in each type of plasmid. The IncHI2/IncN carrying mcr-1 plasmids showed the repressor gene TnpA and the conjugative transfer gene TraN upstream and the tellurium resistance genes downstream of mcr-1. The IncI2 carrying mcr-1 plasmids revealed the same integrase gene downstream but different genes upstream. In contrast with 11 IncX4-carrying plasmids, the flanking coding sequences or genes were similar in 9 plasmids containing the gene RepB family plasmid initiator replication protein upstream (nos. 2117, 2509, 58967, 62122, 59990, 60220) and downstream (nos. 53037, 53060, 60000) or peptidyl-arginine deaminase downstream, whereas 2 IncX4 plasmids (V417 and 56511) had different genes upstream and downstream of mcr-1 (Fig. 6). Isolates with nos. 2117, 2509, 62122, and 60220 showed high genetic organization similarity in the plasmids (Figs. 5 and 6).
Among the mcr-1- harboring plasmids, other antimicrobial-resistant genes (blaTEM-135 or blaTEM-1B) than mcr-1 were detected in IncHI2/IncN (P24-5 and P36.8) that are first reported in this study. All IncX4 and IncI2 plasmids contained only mcr-1; no other antimicrobial resistant genes were detected.
As shown in Fig. 7, plasmid phylogeny demonstrated diversity among the mcr-1 harboring-plasmids. Most IncX4 carrying mcr-1 plasmid were grouped in three clusters. The first cluster comprised strain 59990 which was related to the pTB602 plasmid of Salmonella sp. SSDFZ69 from China (NZ_CP034833.1). The second cluster contained strains 58967, 50220, 2509, 62122, and 2117 that related to the plasmids pKPNH54.3 (NZ_CP024919.1) of K. pneumoniae NH54, and PN42 (MG557854.1) of E. coli PN42, both from Thailand. The third cluster consisted of 53360 and 53037 which related to the plasmid pEC931 (CP049122.1) of E. coli EC931 from China. We found that the other IncX4-type plasmids carrying mcr-1 of strains 56511, 60000, and V417 were not clustered and were located on different branches (Fig. 7).
The IncHI2/IncN harboring mcr-1 plasmids of strains P24-5 and P36.8 were clustered together with plasmids pMCR_WCHEC050613 of E. coli and WCHEC050613 from China (NZ_CP019214.3). Among the IncI2 type plasmids harboring the mcr-1, strain 54881 was related to the p1002-MCR-1 plasmid (NZ_CP021205.1) of E. coli Z1002 from China, whereas it was a distant relative from strains 2514-18, 61843, and 54715. However, strains 2514-18 and 1843 were grouped together with two plasmids (p5CRE51-MCR-1 of E. coli 5CRE51 from Taiwan (NZ_CP021176.1) and pMCR-H9 (NZ_CP029184.1) of E. coli H9Ecoli from China).
Discussion
The high prevalence of human Enterobacterales isolates harboring mcr genes is of global concern. A recent report revealed the overall average prevalence of mcr genes was 4.7% (0.1–9.3%) in 47 countries across 6 continents4; as many as 10 variants of the mcr genes (mcr-1 through to mcr-10) have been documented7,8. A recent study reported 1.03% and 0.12% mcr-harboring carbapenem-resistant E. coli and K. pneumoniae, respectively13. Up to the present, 15 Inc-type mcr-1-carrying plasmids have been documented, consisting of IncFII, IncHI1, IncHI2, IncI2, IncP1, IncX4, IncY, IncF, IncK, IncFIB, IncI1-1Y, IncN, IncFIIs, IncO111, and syncretic35. Most plasmids carrying mcr-1 are transferable and IncX4, IncHI2, and IncI2 are predominant worldwide34,35,36,38. In the current study, mcr-1 was located on 3 different plasmids (IncX4, IncI2, and IncHI/IncN), mainly on IncX4 and IncI2 that was concordant with previous reporting39. Our single stain of K. pneumoniae carrying mcr-1 on the IncX4 plasmid was genetically almost identical to the mcr-1-carrying IncX4 plasmid pMCR_WCHEC1618 recovered from K. pneumoniae in healthy adults40. According to several reports in Thailand, the major plasmid types carrying mcr-1 in Enterobacterales isolates were IncX4 and IncI2, although other plasmid replicons have been documented, including IncI, IncFIB, IncFrepB, IncY13,40,41,42,44. These results suggested that IncX4 and IncI2 bearing mcr-1 mediated major transmission of colistin resistance in Enterobacterales in Thailand.
The conjugation experiment in the current study revealed that all mcr-1-harboring plasmids were successfully transferred from the donor to the E. coli recipient; according to the plasmid Inc types, they are conjugative plasmids39. Among such plasmids in our study, the IncX4 and IncI2 plasmid types were genetically similar, with the least variability, whereas the IncHI2/IncN plasmid type was divergent due to the fact that this type of double-Inc type plasmid contains multiple antimicrobial-resistant genes. This was consistent with the results of the two plasmids merging to perhaps increase the range of host species, plasmid fitness, and/or the acquisition of multiple antimicrobial-resistant genes45. Another study demonstrated that IncHI2-type plasmids are genetically divergent due to containing an MDR region which comprises a variable combination of antimicrobial-resistance genes and insertion sequences, such as Tn6330, in the IncHI2 type that is still highly active and is often transposable37. Our IncHI2/IncN plasmid also showed multiple antimicrobial-resistant genes. In addition, mcr-1 was stably located on IncX4 and IncI2 without cut-paste transposition37, which could explain that why mcr-1 was commonly distributed in these plasmids.
Plasmid phylogenetic analysis in the current study showed that most of our IncX4-type plasmids carrying mcr-1 were grouped, although some were diverse. Notably, 5 isolates carrying mcr-1 on the IncX4-type plasmid were clustered with mcr-1-IncX4 plasmids from either E. coli or K. pneumoniae from Thailand, indicating that they are close relatives and this type of plasmid is circulating in Thailand. In contrast, the other mcr-1 plasmid replicon types in our study were mostly related to several plasmid carrying mcr-1 types from China, perhaps suggesting that they are widely distributed in this region and they may have originated from the same source or ancestor.
The STs of mcr-1-harboring E. coli isolates in this study were mainly disseminated through local clonal expansion with a high-risk international clone ST410 that can cause several types of infection highly resistant to antibiotics and a global distribution46. The mcr-1-carrying IncX4 plasmids have also been identified in E. coli ST410 recovered from human blood47. This may suggest a possible association between E. coli ST410 and the carriage of mcr-1-IncX4 plasmids. In contrast, the most globally common ST of E. coli carrying mcr-1 is ST104. However, previous study in Thailand revealed the mcr-1 carrying E. coli isolates from humans had diverse STs42. In the current study, K. pneumoniae ST336 was predominant. ST336 belongs to clonal complex 17, predominant in carbapenem-resistant K. pneumoniae and is considered an international clone frequently associated with global spread47,48,50. The K. pneumoniae ST15 isolates associated with the spread of multiple drug-resistance genes include ESBLs and mcr-140,48.
mcr-1 was widely distributed in many bacterial species such as E. coli, K. pneumoniae, Salmonella enterica, Shigella spp., Enterobacter cloacae, Pseudomonas spp., Aeromonas spp., Citrobacter freundii, Kluyvera ascobarta, Raulotella ornitholytica, Proteus mirabilis, and Acinetobacter lwoffi51. E. coli is the most prevalent species among the mcr-harboring isolates, accounting for approximately 91% of the total mcr-carrying isolates, followed by Salmonella enterica (~ 7%) and K. pneumoniae (~ 2%)52. In Thailand, mcr harboring E. coli and K. pneumoniae has been reported approximately 1.03–2% and 0.12–1% of isolates during 2014–2019, respectively13,53. The mcr genes have been reported high prevalence rate (3.3%, 24/724) in Salmonella clinical isolates associated with mcr-3 (91.67%, 22/24) and mcr-1 (8.33, 2/24) in Thailand54. A previous study reported that the dissemination of 26 mcr-1-carrying enterobacterial strains (23 E. coli and 3 K. pneumoniae) isolated from contact surfaces (such as handrails and vending machines) on public transportation routes suggested a possible transmission vector of these organisms from one location to another, thereby posing a broader public health risk55. These results demonstrated that plasmids are the major vehicle involved in the dissemination of resistance or virulence genes. Notably, mcr-1-carrying enterobacterial strains were recovered from samples collected from hospitals in the current and the previous studies13, indicating that these isolates could be of nosocomial origin and thus highlighting the need for strong infection control implementation to prevent transmission of mcr-gene-containing bacteria capable of causing potential outbreaks.
The prevalence and dissemination of mcr-1-harboring Enterobacterales isolates from animals (food animals, pet animals, and wildlife), humans (healthy populations and patients) and the environment (farms, urban and rural communities, and natural environments) have been mentioned globally36. Control of their dissemination among humans, animals, and the environment based on the “One-health approach” is necessary. In addition, the judicious use of antibiotics is advisable to minimize the development and dissemination of colistin resistance in human isolates.
Data availability
The assembled genomic sequences during the current study were deposited under the BioProject with accession number JAJBZQ000000000, JAJBZP000000000, JAJGBP000000000, JAJBZO000000000, and JAJGBO000000000.
Change history
13 December 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41598-022-26127-9
References
Kumarasamy, K. K. et al. Emergence of a new antibiotic resistance mechanism in India Pakistan, and the UK: A molecular, biological, and epidemiological study. Lancet Infect. Dis. 10, 597–602 (2010).
Munoz-Price, L. S. et al. Clinical epidemiology of the global expansion of Klebsiella pneumoniae carbapenemases. Lancet Infect. Dis. 13, 785–796 (2013).
Kempf, I., Jouy, E. & Chauvin, C. Colistin use and colistin resistance in bacteria from animals. Int. J. Antimicrob. Agents 48, 598–606 (2016).
Elbediwi, M. et al. Global burden of colistin-resistant bacteria: Mobilized colistin resistance genes study (1980–2018). Microorganisms 7, E461 (2019).
Meletis, G. & Skoura, L. Polymyxin resistance mechanisms: From intrinsic resistance to mcr genes. Recent Pat. Antiinfect. Drug Discov. 13, 198–206 (2018).
Liu, Y. Y. et al. Emergence of plasmid-mediated colistin resistance mechanism MCR-1 in animals and human beings in China: A microbiological and molecular biological study. Lancet Infect. Dis. 16, 161–168 (2016).
Gharaibeh, M. H. & Shatnawi, S. Q. An overview of colistin resistance, mobilized colistin resistance genes dissemination, global responses, and the alternatives to colistin: A review. Vet. World. 12, 1735–1746 (2019).
Wang, C. et al. Identification of novel mobile colistin resistance gene mcr-10. Emerg. Microbes Infect. 9, 508–516 (2020).
Huang, H. et al. Colistin-resistance gene mcr in clinical carbapenem-resistant Enterobacteriaceae strains in China, 2014–2019. Emerg. Microbes Infect. 9, 237–245 (2020).
Mediavilla, J. R. et al. Colistin- and carbapenem-resistant Escherichia coli harboring mcr-1 and blaNDM-5, causing a complicated urinary tract infection in a patient from the United States. MBio 7, e01191-e1116 (2016).
Arabacı, Ç., Dal, T., Başyiğit, T., Genişel, N. & Durmaz, R. Investigation of carbapenemase and mcr-1 genes in carbapenem-resistant Klebsiella pneumoniae isolates. J. Infect. Dev. Ctries. 13, 504–509 (2019).
Kananizadeh, P. et al. Emergence of carbapenem-resistant and colistin-susceptible Enterobacter cloacae complex co-harboring blaIMP-1 and mcr-9 in Japan. BMC Infect. Dis. 20, 282 (2020).
Paveenkittiporn, W., Kamjumphol, W., Ungcharoen, R. & Kerdsin, A. Whole-genome sequencing of clinically isolated carbapenem-resistant Enterobacterales harboring mcr genes in Thailand, 2016–2019. Front. Microbiol. 11, 3393 (2021).
Mendes, A. C. et al. mcr-1 in carbapenemase-producing Klebsiella pneumoniae with hospitalized patients, Portugal, 2016–2017. Emerg. Infect. Dis. 24, 762–766 (2018).
Madec, J. Y. & Haenni, M. Antimicrobial resistance plasmid reservoir in food and food-producing animals. Plasmid 99, 72–81 (2018).
Khanawapee, A. et al. Distribution and molecular characterization of Escherichia coli harboring mcr genes isolated from slaughtered pigs in Thailand. Microb. Drug Resist. 27, 971–979 (2021).
Hatrongjit, R., Kerdsin, A., Akeda, Y. & Hamada, S. Detection of plasmid-mediated colistin-resistant and carbapenem-resistant genes by multiplex PCR. MethodsX. 5, 532–536 (2018).
Clinical Laboratory Standard Institute. Performance standards for antimicrobial susceptibility testing—the 31st edition. CLSI document M100-S30. Clinical and Laboratory Standards Institute, Wayne PA, (2021).
Mobasseri, G., The, C. S. J., Ooi, P. T. & Thong, K. L. The emergence of colistin-resistant Klebsiella pneumoniae strains from swine in Malaysia. J. Glob. Antimicrob. Resist. 17, 227–232 (2019).
Phetburom, N. et al. Klebsiella pneumoniae Complex harboring mcr-1, mcr-7, and mcr-8 isolates from slaughtered pigs in Thailand. Microorganisms 9, 2436 (2021).
Chen, S., Zhou, Y., Chen, Y., & Gu, J. fastp: an ultra-fast all-in-one FASTQ preprocessor. Bioinformatics 34(17), i884–i890. https://doi.org/10.1093/bioinformatics/bty560 (2018).
Jiang, H., Lei, R., Ding, S. W. & Zhu, S. Skewer: A fast and accurate adapter trimmer for next-generation sequencing paired-end reads. BMC Bioinform. 15, 182 (2014).
Wick, R. R., Judd, L. M., Gorrie, C. L. & Holt, K. E. Unicycler: Resolving bacterial genome assemblies from short and long sequencing reads. PLoS Comput. Biol. 13, e1005595 (2017).
Gurevich, A., Saveliev, V., Vyahhi, N. & Tesler, G. QUAST: Quality assessment tool for genome assemblies. Bioinformatics 29, 1072–1075 (2013).
Bortolaia, V. et al. ResFinder 4.0 for predictions of phenotypes from genotypes. J. Antimicrob. Chemother. 75, 3491–3500 (2020).
Alcock, B. P. et al. CARD 2020: Antibiotic resistome surveillance with the comprehensive antibiotic resistance database. Nucleic Acids Res. 48, 517–525 (2020).
Carattoli, A. et al. In silico detection and typing of plasmids using PlasmidFinder and plasmid multilocus sequence typing. Antimicrob. Agents Chemother. 58, 3895–3903 (2014).
Beghain, J., Bridier-Nahmias, A., Le Nagard, H., Denamur, E. & Clermont, O. ClermonTyping: An easy-to-use and accurate in silico method for Escherichia genus strain phylotyping. Microb. Genom. 4, e000192 (2018).
Wick, R. R., Heinz, E., Holt, K. E. & Wyres, K. L. Kaptive Web: User-friendly capsule and lipopolysaccharide serotype prediction for Klebsiella genomes. J. Clin. Microbiol. 56, e00197-e218 (2018).
Larsen, M. V. et al. Multilocus sequence typing of total-genome-sequenced bacteria. J. Clin. Microbiol. 50, 1355–1361 (2012).
Feng, Y., Zou, S., Chen, H., Yu, Y. & Ruan, Z. BacWGSTdb 2.0: A one-stop repository for bacterial whole-genome sequence typing and source tracking. Nucleic Acids Res. 49, D644–D650 (2021).
Bertels, F., Silander, O. K., Pachkov, M., Rainey, P. B. & Van Nimwegen, E. Automated reconstruction of whole-genome phylogenies from short-sequence reads. Mol. Biol. Evol. 31, 1077–1088 (2014).
Letunic, I. & Bork, P. Interactive tree of life (iTOL) v3: An online tool for the display and annotation of phylogenetic and other trees. Nucleic Acids Res. 44, W242–W245 (2016).
Katz, L. S. et al. Mashtree: A rapid comparison of whole genome sequence files. J. Open Source Softw. 4, 1762 (2019).
Xiaomin, S. et al. Global impact of mcr-1-positive Enterobacteriaceae bacteria on “one health”. Crit. Rev. Microbiol. 46, 565–577 (2020).
Wu, R. et al. Fitness advantage of mcr-1-bearing IncI2 and IncX4 plasmids in vitro. Front. Microbiol. 9, 331 (2018).
Li, R., Xie, M., Lv, J., Wai-Chi Chan, E. & Chen, S. Complete genetic analysis of plasmids carrying mcr-1 and other resistance genes in an Escherichia coli isolate of animal origin. J. Antimicrob. Chemother. 72, 696–699 (2017).
Doumith, M. et al. Detection of the plasmid-mediated mcr-1 gene conferring colistin resistance in human and food isolates of Salmonella enterica and Escherichia coli in England and Wales. J. Antimicrob. Chemother. 71, 2300–2305 (2016).
Li, W. et al. Genomic characterization of conjugative plasmids carrying the mcr-1 gene in foodborne and clinical strains of Salmonella and Escherichia coli. Food Control 125, 108032 (2021).
Lu, J. et al. Prevalence and molecular epidemiology of mcr-1-positive Klebsiella pneumoniae in healthy adults from China. J. Antimicrob. Chemother. 75, 2485–2494 (2020).
Srijan, A. et al. Genomic characterization of nonclonal mcr-1-positive multidrug-resistant Klebsiella pneumoniae from clinical samples in Thailand. Microb. Drug Resist. 24, 403–410 (2018).
Shanmugakani, R. K. et al. PCR-dipstick-oriented surveillance and characterization of mcr-1- and carbapenemase-carrying Enterobacteriaceae in a Thai hospital. Front. Microbiol. 10, 149 (2019).
Kamjumphol, W. et al. Draft genome sequence of a colistin-resistant Escherichia coli ST226: A clinical strain harbouring an mcr-1 variant. J. Glob. Antimicrob. Resist. 16, 168–169 (2019).
Pungpian, C. et al. Colistin resistance and plasmid-mediated mcr genes in Escherichia coli and Salmonella isolated from pigs, pig carcass and pork in Thailand, Lao PDR and Cambodia border provinces. J. Vet. Sci. 22, e68 (2021).
Strepis, N. et al. Genetic Analysis of mcr-1-carrying plasmids from Gram-negative bacteria in a Dutch tertiary care hospital: Evidence for intrapatient and interspecies transmission events. Front. Microbiol. 12, 2570 (2021).
Roer, L. et al. Escherichia coli sequence type 410 is causing new international high-risk clones. mSphere 3, e00337-e418 (2018).
Rocha, I. V. et al. Ciprofloxacin-resistant and extended-spectrum β-lactamase-producing Escherichia coli ST410 strain carrying the mcr-1 gene associated with bloodstream infection. Int. J. Antimicrob. Agents. 49, 655–656 (2017).
Rodrigues, C., Machado, E., Ramos, H., Peixe, L. & Novais, Â. Expansion of ESBL-producing Klebsiella pneumoniae in hospitalized patients: A successful story of international clones (ST15, ST147, ST336) and epidemic plasmids (IncR, IncFIIK). Int. J. Med. Microbiol. 304, 1100–1108 (2014).
Novović, K. et al. Molecular epidemiology of colistin-resistant, carbapenemase-producing Klebsiella pneumoniae in Serbia from 2013 to 2016. Antimicrob. Agents Chemother. 61, e02550-e2616 (2017).
Palmieri, M. et al. Genomic epidemiology of carbapenem-and colistin-resistant Klebsiella pneumoniae isolates from Serbia: Predominance of ST101 strains carrying a novel OXA-48 plasmid. Front. Microbiol. 11, 294 (2020).
Anyanwu, M. U., Jaja, I. F. & Nwobi, O. C. Occurrence and characteristics of mobile colistin resistance (mcr) gene-containing isolates from the environment: A review. Int. J. Environ. Res. Public Health 17, 1028 (2020).
Nang, S. C., Li, J. & Velkov, T. The rise and spread of mcr plasmid-mediated polymyxin resistance. Crit. Rev. Microbiol. 45, 131–161 (2019).
Luk-In, S. et al. Occurrence of mcr-mediated colistin resistance in Salmonella clinical isolates in Thailand. Sci. Rep. 11, 1–10 (2021).
Eiamphungporn, W. et al. Prevalence of the colistin resistance gene mcr-1 in colistin-resistant Escherichia coli and Klebsiella pneumoniae isolated from humans in Thailand. J. Glob. Antimicrob. Resist. 15, 32–35 (2018).
Shen, C. et al. Transmission of mcr-1-producing multidrug-resistant Enterobacteriaceae in public transportation in Guangzhou China. Clin. Infect. Dis. 67, S217–S224 (2018).
Funding
This research was supported by the Kasetsart University Research and Development Institute, KURDI (R-M 52.63), Bangkok, and the Health Systems Research Institute (HSI), Thailand.
Author information
Authors and Affiliations
Contributions
P.B. was the primary investigator and wrote the main manuscript text. T.W. and P.J. assisted with whole genome sequencing using short-read and long-read platforms and analyzed mcr-1-bearing plasmids. P.C., R.H., and S.J. provided assistance with data interpretation. A.K. was the senior author for the manuscript and edited the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The Funding section in the original version of this Article was omitted. Full information regarding the corrections made can be found in the correction for this Article.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Boueroy, P., Wongsurawat, T., Jenjaroenpun, P. et al. Plasmidome in mcr-1 harboring carbapenem-resistant enterobacterales isolates from human in Thailand. Sci Rep 12, 19051 (2022). https://doi.org/10.1038/s41598-022-21836-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-21836-7
- Springer Nature Limited
This article is cited by
-
Genomic analysis of carbapenem- and colistin-resistant Klebsiella pneumoniae complex harbouring mcr-8 and mcr-9 from individuals in Thailand
Scientific Reports (2024)
-
Situation Report on mcr-Carrying Colistin-Resistant Clones of Enterobacterales: A Global Update Through Human-Animal-Environment Interfaces
Current Microbiology (2024)
-
Whole genome sequencing to study antimicrobial resistance and RTX virulence genes in equine Actinobacillus isolates
Veterinary Research (2023)