Abstract
Hepatocellular carcinoma (HCC) is the major lethal primary liver malignant worldwide. Although, melatonin has various antitumor bioactivities; there is a requirement for more investigations to elucidate the not discussed effects, and the controversial responses of the treatment with melatonin on targets mediated in HCC. To achieve the aim of the present study, HCC-HepG2 cells were treated with different concentrations of melatonin at various time intervals. The selected minimal proliferation inhibition doses of melatonin were then incubated with cells to examine the arresting effect of melatonin on dividing cells using flow cytometry. Furthermore, the molecular patterns of genes that contributed to apoptosis, drug resistance development, antioxidation, and melatonin crossing were quantified by qRT-PCR. Additionally, the Human inflammation antibody array membrane (40 targets) was used to check the anti-inflammatory effect of melatonin. Our results validated that, melatonin shows anti-proliferative action through preserving cells in G0/G1 phase (P < 0.001) that is associated with a highly significant increase in the expression level of the P53 gene (P < 0.01). On contrary, as a novelty, our data recorded decreases in expression levels of genes involved in the pro-apoptotic pathway; with a significant increase (P < 0.05) in the expression level of an anti-apoptotic gene, Bcl2. Interestingly, we detected observed increases in the expression levels of genes responsible for conferring drug resistance including ABCB1, ABCC1, and ABCC5. Our study proved the anti-inflammatory activity of 1 mM melatonin in HCC-HepG2 cells. Accordingly, we can conclude that melatonin facilitates the anti-proliferation of cells at doses of 1 mM, and 2.5 mM after 24 h. This action is initiated through cell cycle arrest at G0/G1 phase via increasing the expression of P53, but independently on apoptosis. Collectively, melatonin is an effective anti-inflammatory and anti-proliferative promising therapy for the treatment of HCC. However, its consumption should be cautious to avoid the development of drug resistance and provide a better treatment strategy.
Similar content being viewed by others
Introduction
Hepatocellular carcinoma (HCC) is the most common cancer among all primary liver cancers, accounting for more than 70% of cases, and be the third leading cause of cancer-related death in 2020, with expected increased incidences, and deaths each year, as predicted by the World Health Organization1. As HCC is usually late diagnosed at advanced stages, the effective treatment options are so limited. Thus, searching for effective and safe antitumor treatments is an essential requirement2. Moreover, the selection of specific drugs which attenuate the cancer growth mechanisms, including cell division acceleration via suppressing cell cycle proliferation, has emerged as a promising need for developing treatments for cancers3,4. Besides, it has been reported that HCC cells can confer resistance to chemotherapeutic drugs5, and this resistance may exist before treatment (intrinsic) or develop after therapy (acquired). The different mechanisms of drug resistance were discussed in many works of literature6,7, in particular, which depend on ATP-binding cassette transporters (ABCs). Therefore, the complexity of drug resistance development suggests that antitumor therapies which should consider ATP might provide better strategies and improved efficacy for combating drug resistance in cancer8.
Melatonin (N-acetyl-5-methoxytryptamine) is an indoleamine neurohormone that is naturally produced principally by the pineal gland, as well as the liver, from the amino acid tryptophan. Nevertheless, its secretion was found to be decreased in the elderly, so many populations consume melatonin as a supplement that regulates circadian rhythmicity at night. Melatonin works through independent and dependent ways of binding to G protein-coupled receptors MT1 and MT29 in human cells, including hepatocytes, upon their expression induction by melatonin administration10. Many in vivo and in vitro studies have illustrated the physiological and pharmacological activities of melatonin, which include inhibition of proliferation, anti-inflammation, management of cellular redox status, modulation of autophagy, regulation of apoptosis, and cell cycle. Consequently, melatonin was suggested as a safe antitumor agent, either alone or in combination with other anti-cancer drugs, which would form a novel strategy for the treatment of various cancers by affecting multiple carcinogenic signaling pathways11,12. Meanwhile, there are few investigations have addressed the mechanistic role of melatonin in liver carcinoma13; therefore, the present work aimed to elucidate the dual function and the controversial responses of the treatment with melatonin on bioactive targets contributed to the proliferation, apoptosis, inflammation, and drug resistance of HCC cells.
Since, the human HCC cell line (HepG2) was the most widely used in vitro model for studying, and performing explorations of liver cancer cell therapeutic responses, and evaluating the cytotoxicity of many effective drugs14, we conducted our experiments on this type of permanent cells originally derived from a well-differentiated patient with HCC.
Material and methods
Cells propagation
The wild HepG2 cell line was purchased from the American Type Culture Collection (Rockville, MD, United States). The cells were cultured and maintained in Dulbecco’s Modified Eagle’s media (DMEM) (Invitrogen, USA) supplemented with 10% Fetal Bovine Serum (Invitrogen, USA), 1% (v/v) sodium pyruvate, 1% l-glutamine, and 100 Units/ml penicillin–streptomycin (Invitrogen, USA). The cultured cells were kept under the conditions of humidity, and at 37 °C in a 5% CO2 incubator2.
Cell viability assay
After preparation of different concentrations (0–10 mM) of melatonin (Sigma Aldrich, St. Louis, MO, United States) dissolved in 0.5% dimethyl sulfoxide (DMSO) (Molecular Biology Grade; Serva, Germany), the seeded HepG2 cells onto a 96-well plate at a density of 1 × 104 cells/well were incubated with melatonin concentrations for a time interval of 24 h, 48 h, and 72 h. The viability of cells was measured using MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide) colorimetric assay. MTT (Serva, Germany) working solution (5 mg/ml) was added to each well and incubated for 90 min at 37 °C. After that, DMSO (100 µl/well) was added to dissolve the formazan crystals with shaking for 10 min. The optical density of each well was measured using a microplate reader (Tristart lb 942 microplate reader; Berthold, Germany) at 492 nm against a blank (no cells). Cell viability was calculated as the percentage of viable cells in the melatonin-treated cells versus the untreated control cells. The different cytotoxic concentrations of the compound that are corresponding to decreased cell viability were calculated from the cell viability (cytotoxicity) curve using fitting into a non-linear regression equation on Prism 8 (GraphPad Software Inc; San Diego, CA, United States)15.
Cell cycle distribution by flow cytometry
Cell cycle distribution was analyzed by a method of DNA content staining using propidium iodide (PI). Wild HepG2 cells were grown at a density of 1 × 106 cells/well in a 6-well plate, and then treated with the calculated minimal inhibition doses of 1 mM and 2.5 mM of melatonin for 24 h. Following, the cells were washed with (Dulbecco’s phosphate buffered saline) DPBS, trypsinized using 0.05% trypsin–EDTA, fixed in 60% ethanol in DPBS, and then kept at 4 °C overnight. Cells were incubated with 10 µg/ml PI (Thermo Scientific, USA) containing 50 µg/ml RNase A in the dark for 30 min at 37 °C16. Cells were then analyzed using an FL2 (λex/em 535/617 nm) signal detector (ACEA Novocyte™ flow cytometer, ACEA Biosciences Inc., San Diego, CA, USA). For each sample, 12,000 events are acquired. The percentage of cells in the G0/G1, S, G2/M, and sub-G1 phases of the cell cycle was calculated using ACEA NovoExpress™ software (ACEA Biosciences Inc., San Diego, CA, USA). The experiment was repeated 3 independent times.
RT-PCR quantitative analysis of the genes contributed to apoptosis, drug efflux, anti-oxidation, and melatonin crossing
After seeding of HepG2 cells onto a 6-well plate with a density of 300,000 cells/well, cells were treated with the calculated minimal proliferation inhibition dose of melatonin (1 mM) for 24 h. Then, cells were lysed with Qiazol Reagent (Qiagen, Germany) for RNA extraction. By following the manufacturer's instructions for the SensiFAST SYBR No-ROX one-step kit (Bioline, USA), genes expression levels were amplified and quantified by qRT-PCR (MiniOpticon Real-Time PCR System, Bio-Rad, France). Briefly, RT-PCR program steps was set up as shown in Table 1, for a sample with total volume of 15 µl containing 7.5 µl 2× sensiFAST SYBR No-ROX mix, 0.3 µl Ribosafe RNase Inhibitor, 0.15 µl Reverse transcriptase, 3.85 µl H2O, 2 µl RNA sample, and 0.6 µl of each specific primer sequence as indicated in Table 2. All RT-PCRs were performed in duplicate, and the gene copy numbers were normalized to 100,000 copies of the housekeeping beta-actin gene15.
Human inflammation antibody array membrane (40 targets) for quantification detection of inflammatory mediators in a response to 1 mM melatonin treatment
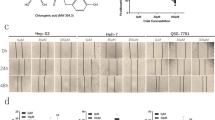
According to Hamed et al.15, after HepG2 cells were seeded onto 6-well plates (300,000 cells/well), cells were treated with 1 mM melatonin for 24 h, and then lysed with RIPA lysis buffer supplemented with protease inhibitor cocktail (Invitrogen, USA) for total protein extraction. Total protein concentration was estimated using the BCA protein assay kit (Cat# 23225; Thermo scientific, USA) by following the manufacturer’s instructions. The protein concentration of each sample was calculated from the Bovine Serum Albumin (BSA) standard curve using Prism 8 (GraphPad Software Inc; San Diego, CA, United States). Human inflammation antibody array membrane (cat# ab 134003, Abcam, USA) was used for the quantification of forty inflammatory factors involved in inflammatory pathway signaling. The protocol steps of the array were followed as; after blocking the array membrane, a final sample concentration of 140 µg/ml was incubated with the blocked membrane overnight at 4 °C. Then, the membrane was incubated with 1X Biotin-Conjugated Anti-Cytokines overnight at 4˚C after excessive washing steps. Gentle washing was done with buffers I, and II provided in the kit. Later on, the membrane was incubated with diluted HRP-Conjugated Streptavidin for 2 h at RT. After washing the membrane, an equal volume of detection buffer C, and detection buffer D was mixed and then incubated with the membrane for 2 min at RT before Chemiluminescence detection, and imaging of the spots signals' by a CCD camera of chemiluminescence imager (UVP, UK). The raw densitometry data was measured with the Image Studio Lite software, (https://www.licor.com/). Then, the background signals were subtracted, and normalization to the positive control was calculated before comparing analyte-by-analyte to determine relative differences in cytokine expression in each sample.
Statistical analysis
As our data were determined to be normally distributed after assessing their normality by the Shapiro–Wilk test, Q-Q (Quantile–Quantile) plot, and charts; the data were assumed to be parametric with equal sample sizes and variances. Accordingly, a student’s t-test was calculated using Microsoft Excel (version of 2007, Microsoft Corporation, USA) to detect the significant differences among the treated cells.
P-values of < 0.05 were considered significant (*) and P-values of < 0.01 were considered highly significant (**). All data were calculated as mean ± standard error of the mean (SEM). All data were reproducible, and each test was done in triplicates. GraphPad Prism version 5.0 (GraphPad Software Inc., San Diego, CA, USA) was used for statistical analyses and establishing of the figure charts.
Ethical approval
This investigation has complete compliance with ethical standards.
Results
Effect of melatonin doses on HepG2 cell viability, and proliferation of cells
As shown in Fig. 1, various concentrations of melatonin ranged from 0 to 10 mM for 24 h, 48 h, and 72 h were found to reduce the viability of HepG2 cells in a time-concentration dependent manner. The calculated 50% inhibition concentrations (IC50) of melatonin were 4.8 mM, 2.7 mM, and 2.3 mM at 24, 48 h, and 72 h, respectively. The concentrations of melatonin used in the next experiment were selected according to the minimal anti-proliferative doses of melatonin, which decreased cell viability percentage after 24 h. Therefore, 1 mM and 2.5 mM melatonin were used to test their effects on cell cycle distribution by flow cytometry.
The anti-proliferative activity of melatonin toward HCC cells. (A) Dose–response curve shows the cytotoxic effect of melatonin on wild HepG2 cells viability using MTT assay. Wild HCC cells (HepG2) were treated with various concentrations of melatonin (0–10 mM) for 24 h, 48 h, and 72 h. Melatonin was found to reduce the % viability of HepG2 cells in a time and concentration-dependent manner. GraphPad Prism version 8.0 (non-linear regression model) was used to calculate IC50 values of melatonin for each time interval. The experiment was performed in octuplets. (B) A column chart shows the calculated IC50 doses of melatonin for each incubation time (24 h, 48 h, and 72 h). Data are presented as mean ± SEM. “a” represents p < 0.01, and “b” represents p < 0.001, as compared to control.
Counting of accumulated cells in cell cycle phases by flow cytometry
To examine the effect of both melatonin concentrations 1 mM, and 2.5 mM on HepG2 cell cycle distribution after incubation time of 24 h. Our results determined a highly significant accumulation (P < 0.001) of cells in G0/G1-phase with a medium (n = 3) percentage of 70.20%, and 75.70% for 1 mM, and 2.5 mM, respectively (Fig. 2, and Table 3) in comparison to the control vehicle cells. G0/G1-phase denotes the non-proliferating cells. Compounds with anti-proliferative effects (regardless of their cytotoxicity) are expected to increase this cell population significantly17. Accordingly, our results confirm the antiproliferative properties of melatonin at the minimal inhibition concentration of 1 mM in comparison to 2.5 mM after 24 h incubation. Additionally, our estimation detected accumulated cells (2.62%) in a sub-G1 phase of 2.5 mM treated HepG2 cells after 24 h, and this phase represents cells with fragmented DNA that will undergo apoptosis18.
The cell cycles arrest induction by melatonin treatment. The effect of melatonin doses (1 mM, and 2.5 mM) for 24 h on HepG2 cell cycle distribution using flowcytometry is shown in representative charts (a) Cell cycle distribution in control vehicle untreated HepG2 cells, (b) cell cycle distribution in 1 mM melatonin treated HepG2 cells, (c) cell cycle distribution in 2.5 mM melatonin treated HepG2 cells, (d) the cell cycle distribution column chart of 1 mM melatonin-treated HepG2 cells, and (e) the cell cycle distribution column chart of 2.5 mM melatonin-treated HepG2 cells. Melatonin was detected to increase the accumulation of HepG2 cells in the G0/G1 phase of the cell cycle in percentages of 70.20% and 75.70% at melatonin concentrations of 1 mM and 2.5 mM, respectively. The experiment was repeated in triplicate. ***P < 0.001, **P < 0.01, and *P < 0.05 as compared to control.
Regulation of the expressed genes controlling apoptosis, drug efflux, anti-oxidation, and melatonin crossing in 1 mM melatonin-treated cells
Consequently to the significant antiproliferative effect of 1 mM melatonin in HepG2 cells after 24 h, as this dose was found to induce cell cycle arrest at G0/G1 phase, we preferred to choose this concentration to elucidate the effect of such minimal inhibition concentration of melatonin on the expression of some genes contributed to apoptosis, drug resistance, anti-oxidation, and melatonin entrance through the cell membranes. Our data reported a highly significant increase (P < 0.01) in the P53 gene expression level as compared to the control. This result proves the role of elevated expressed P53 in cell cycle arrest and accumulation of cells in the G0/G1 phase. On the other hand, we detected that the cytotoxic, and anti-proliferative action of melatonin is independent of apoptosis. As our apoptotic gene expression profiles indicated a significant increase (P < 0.05) in the expression level of the anti-apoptosis Bcl2 gene, and a slightly decrease in pro-apoptotic caspase-3, caspase-7, and Bax genes. Surprisingly, our outcomes recorded an increase in the expression levels of genes involved in drug resistance development including ABCB1, ABCC1, and ABCC5 (Fig. 3). Nevertheless, ABCG2 was found to be expressed in lower levels than the control, as for the anti-oxidation mediator NRF2 gene. These cells don't express ABCC2, and the levels of melatonin receptors᾿ expressive genes were recorded to be not significant.
The gene expression pattern verification by qRT-PCR. The effect of 1 mM melatonin for 24 h on genes expressions of wild HepG2 cells using qRT-PCR shows a highly significant increase in the P53 gene expression level (P < 0.01), and a significant increase in the Bcl2 gene level (P < 0.05) that is associated with a slightly decreases in the expression levels of pro-apoptotic genes caspase-3, caspase-7, and BAX. Observed increases in the expression levels of genes contributed to drug resistance including ABCB1, ABCC1, and ABCC5 are additionally shown.
The effect of 1 mM melatonin on the expression levels of inflammatory factors involved in the inflammation pathway
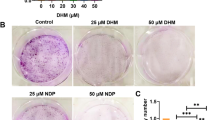
As illustrated in Fig. 4a–c, our antibody array membrane results approved the anti-inflammatory effect of the minimal growth inhibition dose of melatonin, 1 mM. All inflammatory molecules (Table 4) were detected to be mediated in lower levels after 24 h exposure to 1 mM melatonin, as a comparison to their expression in control cells.
The inhibitory effect of 1 mM melatonin on the inflammation. a. Human inflammation antibody array membranes detect signal spots of 40 targets/membrane. (A) The array membrane of vehicle control (DMSO treated) HepG2 cells, (B) The array membrane of 1 mM melatonin-treated HepG2 cells for 24 h. After development of the membranes, the imaging of the spots signals' was detected by Chemiluminescence using CCD camera of chemiluminescence imager (UVP, UK), and the raw densitometry data was measured with the Image Studio Lite software, (https://www.licor.com/), b. The anti-inflammatory effect of 1 mM melatonin. The graph shows the effect of 1 mM melatonin for 24 h on the mean expression levels of normalized inflammatory mediators in HepG2 cells, in a comparison to the control untreated cells. After subtracting the background signals, each spot was normalized to the positive control before comparing analyte-by-analyte to determine relative differences in inflammatory factors expression for each sample. All cytokines were expressed in non-significant varied lower levels as compared to control untreated HepG2 cells. The data were calculated as a mean of duplicate ± SEM, and c. the calculated fold changes (of 40 inflammatory factors expressed in 1 mM melatonin-treated HCC-HepG2 cells after incubation time of 24 h) to control. The chart displays the decreasing of the expression levels of all detected inflammatory mediators with the lowest expression levels were calculated for interleukin (IL)-7, and IL-13.
Discussion
Hepatocellular carcinoma (HCC) is the primary life-threatening liver malignancy in males, and females, globally. Additionally, it is one of the most challenging tumors to be treated. Thus, there is an emerging necessity to find alternatives or even complementary drugs that will improve the available treatment strategies. Melatonin is a natural hormone that was detected to be secreted by a few organs of the human body for the regulation of physiological processes through diverse actions. Recently, some studies have examined the antitumor activities of melatonin against several cancers. However, more investigations are required to underlie the effective functions, mediated regulatory mechanisms, and the conflicted responses of melatonin treatment in HCC13,19.
In the current study, HCC-in vitro wild HepG2 cells were used and treated with a scale range of melatonin doses (0–10 mM) at interval incubation times (24 h, 48 h, and 72 h). Our results indicated the decrease in % cell viability that was dependent on incubation time, and dose of melatonin, with minimal effective inhibition doses at 1 mM, and 2.5 mM after 24 h. Numerous studies were conducted in different cell types of HCC, including HepG22,19,20,21,22, Hep3B23, HuH-74, and SMMC-772121, and treated with different concentrations of melatonin (10–6, 1, 2, 2.5 mM) at incubation times ranged from 24 to 96 h, agree with our findings. The antiproliferative effect of our administrated doses of melatonin was associated with an inhibition of the cell cycle at the G0/G1 phase, and a highly significant increase in the expression level of the P53 gene which controls the cell cycle progression. This inhibition activity was confirmed by other supportive studies in various cancers22,24,25,26. Additional studies reported cell cycle arrest at the G2/M phase2,27. The higher doses of melatonin could be the cause of cell cycle arrest and accumulation of cells at the G2/M phase28.
As a dichotomous action of 1 mM melatonin after 24 h treatment in our investigation, we recorded a significant increase in the expression level of the anti-apoptotic Bcl2 gene, besides a non-significant down-regulation of pro-apoptotic caspase-3, caspase-7, and Bax genes. Authors of previous publications were in contrast to our results, as they detected apoptotic effects for melatonin treatment that depend on the activation of caspases, and reduction of Bcl22,11,19,26,29,30. However, only a few reports referred to the anti-apoptotic role of melatonin. In human hexokinase 2 (HK2) cells, an immortalized proximal tubule epithelial cell line, melatonin was found to counteract the lethal effects of cisplatin, by inducing its anti-apoptotic actions. The intermediate events in this process were observed to be mediated through the regulation of expression BAX/Bcl-2 ratio and disruption of mitochondrial membrane potential31. Additionally, Shen et al. supposed that pathways other than those associated with apoptosis or necrosis inhibited the proliferation of ovarian cancer cell lines (OVCAR-429 and PA-1), as they indicated non-significant increases in the percentage of cells undergoing necrosis, apoptosis or caspase 3 activation after 4 h of melatonin treatment at 400 to 800 μM28. The controversial behavior of this indole regarding apoptosis depends on the difference in treatment time and doses of melatonin.
Interestingly, our flow cytometric data estimated started appearing of a low percentage of cells (2.62%) in the sub-G1 phase after treatment of HepG2 cells with 2.5 mM of melatonin. The sub-G1 phase represents cells with fragmented DNA content and will undergo apoptosis32. Cellular arrest mediated by melatonin in this phase of the cell cycle is in favor of pro-apoptotic and anti-proliferative effects for this indole on HCC19. Accordingly, the cellular apoptotic induction by melatonin could be dependent on the elevated doses of this indole28. More research is needed to elucidate this suppose.
Although inflammation is important for cancer proliferation and metastasis33, multiple studies confirmed the anti-inflammatory role of melatonin treatment in various in vitro cancer models treated with 1 mM melatonin for 24 h via down-regulation of individual inflammatory mediators, such as NF-kB34, IL-1α, IL-1β, TNF-α, COX-2, IL-8 and MCP-19, the present study is the first one which indicates the anti-inflammatory effect of 1 mM melatonin through targeting forty inflammatory mediated factors by using Human inflammation antibody array membrane. This inhibition could be mediated through the increased expression level of the P53 gene, as p53 has been reported to inhibit inflammatory responses, and functional loss of p53 causes excessive inflammatory reactions15,33.
While Colombo and the co-working team reported a decrease in the expression of NF-kB in breast cells after exposure to 1 mM melatonin for 24 h, they detected an increase in the same inflammatory transcription factor in HepG2 cells. So, they concluded that this double role in the expression of NF-kB depends on the cell type34.
Unfortunately, our results showed for the first time a somewhat increase in the expression of ATP-binding cassette transporters (ABCB1, ABCC1, and ABCC5) which mediate the drug efflux outside the cells and facilitate the development of drug resistance phenomena. Nevertheless, the expression of ABCG2 was quantified to be reduced. The reduction in the expression level of ABCG2 is a result of the methylation of its promoter by the action of melatonin to overcome drug resistance35.
In contrast to the majority of studies that approved melatonin as an anti-oxidant agent that can induce the expression of NRF230,36,37. Our data reported NRF2 to be expressed at lower levels after the treatment of cells by melatonin. This cellular behavior could be explained according to the status of oxidative stress dose level. Consequently, we can predict that the unexpected action of melatonin in the present wild HCC-HepG2 cells could be due to temporary signaling of the autophagy process upon induction by melatonin30, which is negatively regulated by the apoptosis mechanism38. Despite the detected significant increase in Bcl2 expression level, it has recently doesn't found to directly affect autophagy processing39. Generation of ATP was reported to be associated with autophagy40,41, thus it is expected to estimate higher expression levels of ATP-binding cassette transporters42.
We obtained through our experiments that, the mediated actions of melatonin were independent of melatonin receptors (MT1, MT2, and MT3) which were found to be insignificantly expressed upon induction with 1 mM melatonin for 24 h. On the other hand, studies13,27 suggested that the growth and migration suppressive activity of 1 mM, 2 mM, and 2.5 mM doses of melatonin could be mediated through the expression induction of different levels of MT1/MT2/MT3 receptors in Huh7 and HepG2 cell lines after incubation times ranged from 2 to 6 days. However, Wang et al.13 recommended further studies to identify the specific receptors through which melatonin mediates its antitumor activities. The induction of melatonin receptors depends on the treatment time and the melatonin dose administered to the HepG2 tumor cells27. In addition, studies conducted in breast, and colon cancers stated that the low sensitivity to melatonin treatments of 1 mM, and 2 mM was due to the low expressing levels of MT1/MT2 receptors43,44.
Melatonin is an effective anti-proliferative drug that can inhibit cell cycle progression in a mechanism that is independent of apoptosis. Moreover, melatonin is a promising candidate for targeting the inflammatory pathway. In conclusion, Melatonin could be administrated individually or in combination with other chemotherapies to introduce a better treatment strategy for HCC patients, but its consumption should be cautious to avoid the controversial responses of the treatment. The controversial effect of melatonin could be mediated through other alternative types of programmed cell death such as autophagy. As a result of ATP production, which is associated with autophagy, there was an increase in the ATP- binding cassette transporters (ABCs).
Data availability
All are available in the current research paper.
References
Zhang, H., Zhang, W., Jiang, L. & Chen, Y. Recent advances in systemic therapy for hepatocellular carcinoma. Biomark. Res. 10, 3. https://doi.org/10.1186/s40364-021-00350-4 (2022).
Ammar, O. A., El-Missiry, M. A., Othman, A. I. & Amer, M. E. Melatonin is a potential oncostatic agent to inhibit HepG2 cell proliferation through multiple pathways. Heliyon 8(1), e08837. https://doi.org/10.1016/j.heliyon.2022.e08837 (2022).
Mortezaee, K. et al. Modulation of apoptosis by melatonin for improving cancer treatment efficiency: An updated review. Life Sci. 228, 228–241 (2019).
Lin, S. et al. Melatonin promotes sorafenib-induced apoptosis through synergistic activation of JNK/c-jun pathway in human hepatocellular carcinoma. J. Pineal Res. https://doi.org/10.1111/jpi.12398 (2017).
Jin, Y. D., Ren, Y., Wu, M. W., Chen, P. & Lu, J. Effect of shikonin on multidrug resistance in HepG2: The role of SIRT1. Pharm. Biol. 53, 1016–1021 (2015).
Khaled, J., Kopsida, M., Lennernäs, H. & Heindryckx, F. Drug resistance and endoplasmic reticulum stress in hepatocellular carcinoma. Cells 11(4), 632. https://doi.org/10.3390/cells11040632 (2022).
Bukowski, K., Kciuk, M. & Kontek, R. Mechanisms of multidrug resistance in cancer chemotherapy. Int. J. Mol. Sci. 21(9), 3233. https://doi.org/10.3390/ijms21093233 (2020).
Wang, X., Zhang, H. & Chen, X. Drug resistance and combating drug resistance in cancer. Cancer Drug Resist. 2, 141–160. https://doi.org/10.20517/cdr.2019.10 (2019).
Tian, Q.-X. et al. Melatonin inhibits migration and invasion in LPS-stimulated and -unstimulated prostate cancer cells through blocking multiple EMT-relative pathways. J. Inflamm. Res. 14, 2253–2265 (2021).
Sato, K. et al. Melatonin and circadian rhythms in liver diseases: Functional roles and potential therapies. J. Pineal Res. 68(3), e12639. https://doi.org/10.1111/jpi.12639 (2020).
Mehrzadi, S., Pourhanifeh, M. H., Mirzaei, A., Moradian, F. & Hosseinzadeh, A. An updated review of mechanistic potentials of melatonin against cancer: Pivotal roles in angiogenesis, apoptosis, autophagy, endoplasmic reticulum stress and oxidative stress. Cancer Cell Int. 21, 188. https://doi.org/10.1186/s12935-021-01892-1 (2021).
Shrestha, S. et al. Melatonin potentiates the antitumor effect of curcumin by inhibiting IKKβ/NF-κB/COX-2 signaling pathway. Int. J. Oncol. 51(4), 1249–1260 (2017).
Wang, T. H. et al. Melatonin inhibits the progression of hepatocellular carcinoma through microRNA Let7i-3p mediated RAF1 reduction. Int. J. Mol. Sci. 19(9), 2687. https://doi.org/10.3390/ijms19092687 (2018).
Gerets, H. H. et al. Characterization of primary human hepatocytes, HepG2 cells, and HepaRG cells at the mRNA level and CYP activity in response to inducers and their predictivity for the detection of human hepatotoxins. Cell Biol. Toxicol. 28, 69–87 (2012).
Hamed, A. R., Yahya, S. M. & Nabih, H. K. Anti-drug resistance, anti-inflammation, and anti-proliferation activities mediated by melatonin in doxorubicin-resistant hepatocellular carcinoma: In vitro investigations. Naunyn-Schmiedeberg’s Arch. Pharmacol. https://doi.org/10.1007/s00210-023-02385-w (2023).
Yahya, S. M. M. et al. Possible role of microRNA-122 in modulating multidrug resistance of hepatocellular carcinoma. Indian J. Clin. Biochem. 33(1), 21–30. https://doi.org/10.1007/s12291-017-0651-8 (2018).
Thangaraj, K. et al. Orientin induces G0/G1 cell cycle arrest and mitochondria mediated intrinsic apoptosis in human colorectal carcinoma HT29 cells. Biomolecules 9(9), 418. https://doi.org/10.3390/biom9090418 (2019).
Plesca, D., Mazumder, S. & Almasan, A. DNA damage response and apoptosis. Methods Enzymol. 446, 107–122. https://doi.org/10.1016/S0076-6879(08)01606-6 (2008).
Mortezaee, K. Human hepatocellular carcinoma: Protection by melatonin. J. Cell Physiol. 233, 6486–6508 (2018).
Colombo, J., Maciel, J. M. W., Ferreira, L. C., Da Silva, R. F. & Zuccari, D. Effects of melatonin on HIF-1α and VEGF expression and on the invasive properties of hepatocarcinoma cells. Oncol. Lett. 12(1), 231–237 (2016).
Fan, L., Sun, G., Ma, T., Zhong, F. & Wei, W. Melatonin overcomes apoptosis resistance in human hepatocellular carcinoma by targeting survivin and XIAP. J. Pineal Res. 55(2), 174–183 (2013).
Martín-Renedo, J. et al. Melatonin induces cell cycle arrest and apoptosis in hepatocarcinoma HepG2 cell line. J. Pineal Res. 45, 532–540. https://doi.org/10.1111/j.1600-079X.2008.00641.x (2008).
Prieto-Domínguez, N. et al. Melatonin-induced increase in sensitivity of human hepatocellular carcinoma cells to sorafenib is associated with reactive oxygen species production and mitophagy. J. Pineal Res. 61(3), 396–407. https://doi.org/10.1111/jpi.12358 (2016).
Song, J. et al. Melatonin induces the apoptosis and inhibits the proliferation of human gastric cancer cells via blockade of the AKT/MDM2 pathway. Oncol. Rep. 39, 1975–1983 (2018).
Nooshinfar, E. et al. Melatonin promotes ATO-induced apoptosis in MCF-7 cells: Proposing novel therapeutic potential for breast cancer. Biomed. Pharmacother. 83, 456–465. https://doi.org/10.1016/j.biopha.2016.07.004 (2016).
Nyamsambuu, A., Khan, M. A., Zhou, X. & Chen, H.-C. Molecular mechanism of inhibitory effects of melatonin on prostate cancer cell proliferation, migration and invasion. PLoS ONE 17(1), e0261341. https://doi.org/10.1371/journal.pone.0261341 (2022).
Carbajo-Pescador, S. et al. Changes in the expression of melatonin receptors induced by melatonin treatment in hepatocarcinoma HepG2 cells. J. Pineal Res. 47(4), 330–338 (2009).
Shen, C.-J., Chang, C.-C., Chen, Y.-T., Lai, C.-S. & Hsu, Y.-C. Melatonin suppresses the growth of ovarian cancer cell lines (OVCAR-429 and PA-1) and potentiates the effect of G1 arrest by targeting CDKs. Int. J. Mol. Sci. 17(2), 176. https://doi.org/10.3390/ijms17020176 (2016).
Li, M. et al. Melatonin sensitises shikonin-induced cancer cell death mediated by oxidative stress via inhibition of the SIRT3/SOD2-AKT pathway. Redox Biol. 36, 101632 (2020).
Favero, G. et al. Promising antineoplastic actions of melatonin. Front. Pharmacol. https://doi.org/10.3389/fphar.2018.01086 (2018).
Reiter, R. J. et al. Advances in characterizing recently-identified molecular actions of melatonin: clinical implications. In Approaching Complex Diseases Human Perspectives in Health Sciences and Technology Vol. 2 (ed. Bizzarri, M.) (Springer, 2020). https://doi.org/10.1007/978-3-030-32857-3_14.
Kajstura, M., Halicka, H. D., Pryjma, J. & Darzynkiewicz, Z. Discontinuous fragmentation of nuclear DNA during apoptosis revealed by discrete “sub-G1” peaks on DNA content histograms. Cytometry A 71(3), 125–131 (2007).
Uehara, I. & Tanaka, N. Role of p53 in the regulation of the inflammatory tumor microenvironment and tumor suppression. Cancers 10(7), 219. https://doi.org/10.3390/cancers10070219 (2018).
Colombo, J. et al. Melatonin differentially modulates NF-кB expression in breast and liver cancer cells. Anticancer Agents Med. Chem. 18(12), 1688–1694. https://doi.org/10.2174/1871520618666180131112304 (2018).
Liu, M.-T. & Reiter, R. J. The impact of melatonin and carbon ion irradiation on cancer stem cells. Nucl. Med. Biomed. Imaging 2(3), 1–14. https://doi.org/10.15761/NMBI.1000127 (2017).
Miguel, F. M. et al. Melatonin attenuates inflammation, oxidative stress, and DNA damage in mice with nonalcoholic steatohepatitis induced by a methionine- and choline-deficient diet. Inflammation 45(5), 1968–1984. https://doi.org/10.1007/s10753-022-01667-4 (2022).
Tascioglu, A. A., Panieri, E., Stepanić, V., Gurer-Orhan, H. & Saso, L. Involvement of NRF2 in breast cancer and possible therapeutical role of polyphenols and melatonin. Molecules 26, 1853. https://doi.org/10.3390/molecules26071853 (2021).
Mariño, G., Niso-Santano, M., Baehrecke, E. H. & Kroemer, G. Self-consumption: The interplay of autophagy and apoptosis. Nat. Rev. Mol. Cell Biol. 15(2), 81–94. https://doi.org/10.1038/nrm3735 (2014).
Lindqvista, L. M., Heinleina, M., Huang, D. C. & Vaux, D. L. Prosurvival Bcl-2 family members affect autophagy only indirectly, by inhibiting Bax and Bak. PNAS 111(23), 8512–8517. https://doi.org/10.1073/pnas.1406425111 (2014).
Zhang, B. et al. Mechanically induced autophagy is associated with ATP metabolism and cellular viability in osteocytes in vitro. Redox Biol. 14, 492–498. https://doi.org/10.1016/j.redox.2017.10.021 (2018).
Zhang, P. et al. The role of autophagy in regulating metabolism in the tumor microenvironment. Genes Dis. https://doi.org/10.1016/j.gendis.2021.10.010 (2021).
Giddings, E. L. et al. Mitochondrial ATP fuels ABC transporter-mediated drug efflux in cancer chemoresistance. Nat. Commun. 12, 2804. https://doi.org/10.1038/s41467-021-23071-6 (2021).
Winczyk, K. et al. Effects of melatonin and melatonin receptors ligand N-[(4-methoxy-1H-indol-2-yl)methyl]propanamide on murine Colon 38 cancer growth in vitro and in vivo. Neuro Endocrinol. Lett. 23(Suppl. 1), 50–54 (2002).
Hill, S. M. et al. Melatonin and associated signaling pathways that control normal breast epithelium and breast cancer. J. Mammary Gland Biol. Neoplasia 16, 235–245 (2011).
Acknowledgements
We would like to thank Dr. Asmaa M. El-Fiky and Dr. Ghada A. Soliman for providing excellent experimental assistance with this work.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). This work was funded by the National Research Centre (Egypt)—project number (12060125).
Author information
Authors and Affiliations
Contributions
A.R.H. performed the cells propagations, cytotoxicity assays, and development of membranes of the inflammation antibody array. S.M.Y. contributed to the molecular genes profiling, and statistic calculations. H.K.N. carried out the flow cytometry, and inflammation antibody array experiment, contributed to qRT-PCR, and statistic calculations, and wrote the manuscript. All authors reviewed and approved the manuscript for submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nabih, H.K., Hamed, A.R. & Yahya, S.M.M. Anti-proliferative effect of melatonin in human hepatoma HepG2 cells occurs mainly through cell cycle arrest and inflammation inhibition. Sci Rep 13, 4396 (2023). https://doi.org/10.1038/s41598-023-31443-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-31443-9
- Springer Nature Limited
This article is cited by
-
Restoring microRNA-34a overcomes acquired drug resistance and disease progression in human breast cancer cell lines via suppressing the ABCC1 gene
Breast Cancer Research and Treatment (2024)